Assessment of maternal and neonatal vital signs
Neurological assessment
Learning outcomes
Having read this chapter, the reader should be able to:
Neurological assessment may be undertaken when there are concerns about actual or possible alterations in a woman's level of consciousness (e.g. post-seizure, magnesium toxicity, meningitis, head injury). Initially a doctor with neurological experience will complete the neurological assessment evaluating level of consciousness, pupillary reaction, motor (including reflexes), sensory and cerebellar function and vital signs. A reduced assessment of level of consciousness, motor signs (limb movement), pupillary assessment in conjunction with vital signs – respiration, heart rate, blood pressure, temperature and oxygen saturation – can be undertaken by the midwife. The midwife must be appropriately trained to enable her to complete a neurological assessment competently and safely, as it provides invaluable information regarding the woman's condition. The Modified Early Obstetric Warning Scoring (MEOWS) chart may contain some of the components of neurological assessment, e.g. alertness, response to stimulation (p. 66) This chapter focuses on the principles of neurological assessment and the midwife's role in relation to undertaking this assessment.
Frequency of observations
NICE (2014) recommend that neurological observations should be completed every 30 minutes until the GCS is 15, when they can then be recorded hourly for 4 hours, then every 2 hours, reverting to 30-minute assessments if the condition deteriorates.
Glasgow Coma Scale
The GCS was developed in 1974 and revised in 1979 to provide a quick and objective assessment of eye opening, verbal response and motor ability, enabling the level of consciousness to be monitored effectively and is accepted as the ‘gold standard’ assessment tool (Palmer & Knight 2006). Each of these three categories has four to six different responses and each response is scored. The three scores are totalled to score between 15 (fully conscious) and 3 (no response) to provide a rapid assessment of the woman's condition and response to treatment. NICE (2014) state that a GCS >12 indicates a normal or minimally impaired level of consciousness. The score should be recorded as a fraction using 15 as the denominator (e.g. 10/15). NICE (2014) recommend that information about the three separate GCS responses should also be recorded, e.g. a score of 12/15 based on scores of 3 on eye opening, 4 on verbal response, and 5 on motor ability should be recorded as E3, V4, M5.
Eye opening
Eye opening is the first GCS measurement of consciousness, as without this cognition does not occur; however, it does not indicate the neurological system is intact (Iankova 2006). Okamura (2014) states it is assessing the integrity of the reticular activating system found in the brainstem. It cannot be used if there has been damage to the eyes resulting in swelling, as it is unlikely the eyes will open easily, rendering this aspect of the assessment unreliable until the swelling subsides. Jevon (2008) recommends recording this as ‘C’.
The midwife should look at the woman to see if her eyes are opening spontaneously (score 4). If the eyes remain closed, the midwife should speak to the woman, which should provoke the eyes to open (score 3). Waterhouse (2009) suggests a greater response is achieved by asking the woman if she ‘wants a cup of tea’ rather than saying her name.
If the eyes continue to remain closed, a painful peripheral stimulus is used – this may be a gentle shake but if no response a deeper stimulus is needed. Pressure is applied using a pen positioned just below the lateral outer aspect of the second or third interphalangeal joint for 10–15 seconds (Iankova 2006, Okamura 2014, Waterhouse 2009) (score 2). Painful stimulation should be applied slowly up to a maximum of 15 seconds. Pressure should not be applied to the nail bed because of the risk of bruising (Edmunds et al 2011).
If there is no response using a painful peripheral stimulus, a central painful stimulus is used. Central stimulation involves the application of a noxious painful stimulus to the core of the nervous system via the cranial nerves to elicit a complete motor response (Waterhouse 2009). However, the woman may grimace while keeping her eyes closed, and so it is not generally used unless the midwife has been appropriately trained. It is important to use the same stimulus on each assessment. A score of 1 is given if the eyes remain closed.
Jevon (2008) recommends squeezing the trapezium muscle using a thumb and two fingers and Edmunds et al (2011) advise twisting 3–5 cm of muscle from where the neck and shoulders meet for up to 30 seconds to stimulate the spinal accessory nerve (XI), although this is difficult on large or obese women. Waterhouse (2009) considers this to be the safer technique for inexperienced staff. Alternatively the supraorbital nerve, part of the trigeminal nerve (V), can be stimulated by applying pressure to the supraorbital ridge provided there is no suspected or confirmed facial fracture or glaucoma (Palmer & Knight 2006) but bradycardia may occur. This is achieved by placing the thumb into the indentation below the eyebrow, close to the nose, and applying gradual pressure for up to 30 seconds (Okamura 2014). Sternal rubs are used with caution because they can cause bruising and the flat of the hand should be used, not the knuckles. It should not be used for repeated assessments (Edmunds et al 2011).
Waterhouse (2009) recommends central painful stimulus, rather than peripheral pain stimulus, is used as it can result in both an eye opening response and assess motor ability. The type and site of the stimulus used should be documented.
Verbal response
Assessing the verbal response is an assessment of the integrity of the higher, cognitive and interpretive centres of the brain (Okamura 2014). The midwife should ascertain the level of verbal response by asking questions that require answers to show clarity and understanding – What is your name? Where are you? What day is it? – an accurate answer scores 5. If the woman is able to speak using full sentences but the answers are incorrect, a score of 4 is given. If only words and incomplete sentences are given, the score is 3, regardless of whether the words are appropriate. A score of 2 is given if incomprehensible sounds (e.g. grunts, groans) are made. If no sound is made in response to verbal or painful central stimuli, 1 is scored.
It is important to take into account the language spoken by the woman; if she does not speak English, an interpreter should be used.
Motor ability
The response of the upper limbs is tested to determine the integrity of the motor strip within the cerebral cortex (Okamura 2014), as the lower limbs can also be affected by spinal function. The midwife should ask the woman to bend then hold out her arms and squeeze the midwife's hands with both of her hands. The midwife can then determine that both arms can be moved and the elbows flexed, the power and release of grip from each hand can be noted.
A score of 6 is given if the woman is able to complete these movements and 1 if there is no response despite painful central stimuli. Scores of 2–5 are given according to the degree of movement and flexion occurring as a result of painful stimulus: the arm moving towards the stimuli to try to remove it (5), arm bends at the elbow without rotation of the wrist (4) or with wrist rotation and forearm rotation (3), the arm extends at the elbow while the wrist flexes (2).
Pupillary assessment
While this is not part of the GCS, it is a separate and important component of the neurological assessment. The size and shape of each pupil and reaction to light are assessed. The midwife should look at the pupils to determine if they are the same shape and whether the eyes are working together. The diameter of each pupil is then measured – the normal range is 2–6 mm (Dawson 2000) – and they are usually equal in size (unequal pupils are a late sign associated with raised intracranial pressure, but may be of little significance if the woman is alert and orientated and small differences in pupil size are often normal). Pupil reaction is assessed by shining a bright light from a pen torch into one eye, then the other – approach from the side rather than directly in front. The pupils should decrease in size and the speed at which this occurs is recorded. If there is no response, the pupil is fixed and suggests the midbrain may be suffering from pressure as constriction and dilation of the pupils is controlled by the oculomotor nerve (cranial nerve III). Pupils that are slow to respond or which dilate suddenly and unequally indicate that cerebral oedema or haematoma is worsening (Waterhouse 2005). The level of sedation administered to the woman will affect pupil reaction – pupils measuring 1–2 mm can occur when barbiturates or opiates have been used. Edmunds et al (2011) suggest that if the pupil size is equal but they are pinpoint in size, opiates or a Pontine lesion may be the cause whereas when they are equal but small and reactive, there be metabolic encephalopathy, equal-sized and fixed may be due to a midbrain lesion and equal, mid-sized pupils may be caused by a metabolic lesion. They also advise that when pupils are unequal, dilated, and unreactive, a cranial nerve III palsy may be responsible and unequal, small, reactive pupils may be a result of Horner's syndrome (Edmunds et al 2011).
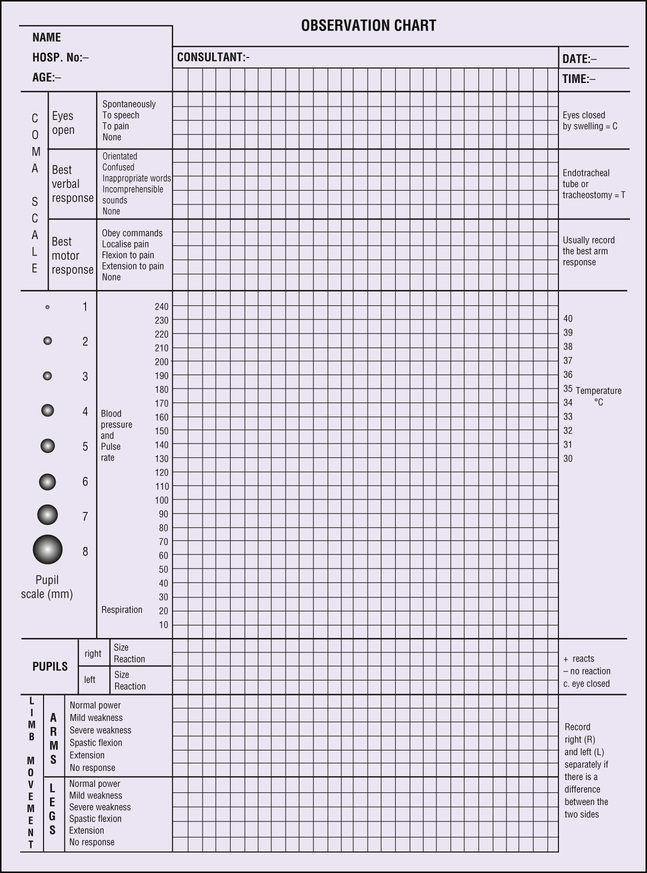
The findings of the neurological assessment should be recorded on a neurological observation chart (Fig. 7.1) in conjunction with the MEOWS, vital signs including temperature (see Chapter 3), pulse (see Chapter 4), blood pressure (see Chapter 5), and respiratory rate (see Chapter 6). Blood oxygen saturation should also be monitored (NICE 2014) (see p. 65). While the total GCS score is recorded, it is also important to record separately the scores of the three different categories, as each one is assessing different areas of the brain. A decreasing score indicates the woman's condition is deteriorating and referral is indicated.
The doctor should be informed if there is a severe or increasing headache, persistent vomiting, new or evolving neurological signs and symptoms (e.g. pupil inequality), a reduction to 3 or less points in eye opening or verbal responses or 2 in motor responses, agitation or abnormal behaviour as these can indicate deterioration of the woman's neurological status.
PROCEDURE: Neurological assessment
• Gather equipment and take to the bedside:
• Inform the woman of the procedure and gain consent if conscious and responsive.
• Complete vital signs: temperature, blood pressure, pulse, respiration and arterial oxygen saturation.
• Assess level of consciousness by talking with the woman and asking her who she is, what day it is and where she is; use peripheral or central painful stimulus if no response.
• Assess motor function by asking the woman to bend and lift her arms and to squeeze both your hands.
• Assess the size and shape of the pupils and movement of the eyes.
• Assess pupillary reaction by:
▪ darkening the room if necessary
▪ holding one eyelid open, move the pen torchlight towards and across the eye, moving the light from side to side
▪ assess the degree and speed at which the pupil constricts
▪ then with both eyelids held open, shine the light into one eye – the pupil in the other eye should also be observed to constrict
• Ensure the woman is covered and comfortable.
Summary
• Neurological assessment is undertaken where there are actual or potential altering levels of consciousness.
• The GCS determines the level of consciousness by assessing the woman's response to the three categories of eye opening, verbal response and motor ability.
• The midwife who has been appropriately trained can undertake the GCS and recording of vital signs as part of the woman's neurological assessment to determine any changes to her condition.
• Additionally, the doctor will evaluate motor and sensory function as required.
Self-assessment exercises
The answers to the following questions may be found in the text: