General Pathology of Infectious Diseases
Humans are prey to thousands of infectious agents ranging from submicroscopic viruses to several meters long tape worms. This chapter reviews the general principles of the pathogenesis of infectious disease and describes the characteristic histopathologic changes caused by different types of microbes. Infections that involve specific organs are discussed in other chapters of this book.
General Principles of Microbial Pathogenesis
Infectious diseases are an important health problem in the United States and worldwide despite the availability of effective vaccines and antibiotics for many types of infections. Influenza and pneumonia combined are the eighth leading cause of death in the United States. In low-income countries, limited access to healthcare, unsanitary living conditions, and malnutrition contribute to a massive burden of infectious diseases. Lower-respiratory infections, HIV/AIDS, and diarrheal diseases are the top three causes of death in developing countries, and malaria and tuberculosis are among the top ten. Infectious diseases are particularly important causes of death among children, older adults, individuals with chronic debilitating diseases and inherited or acquired immunodeficiency states (e.g., AIDS), and in patients receiving immunosuppressive drugs.
Categories of Infectious Agents
Infectious agents belong to a wide range of classes and vary greatly in size, ranging from prion protein aggregates of under 20 nm to tapeworms 10 meters in length (Table 9.1).
Table 9.1
Classes of Human Pathogens
| Taxonomic Category | Size | Propagation Site(s) | Example(s) | Disease(s) |
| Prions | <20 nm | Intracellular | Prion protein | Creutzfeldt-Jacob disease |
| Viruses | 20–400 nm | Obligate intracellular | Poliovirus | Poliomyelitis |
| Bacteria | 0.2–15 µm | Obligate intracellular | Chlamydia trachomatis | Trachoma, urethritis |
| Extracellular | Streptococcus pneumoniae | Pneumonia | ||
| Facultative intracellular | Mycobacterium tuberculosis | Tuberculosis | ||
| Fungi | 2–200 µm | Extracellular | Candida albicans | Thrush |
| Facultative intracellular | Histoplasma capsulatum | Histoplasmosis | ||
| Protozoa | 1–50 µm | Extracellular | Trypanosoma brucei | Sleeping sickness |
| Facultative intracellular | Trypanosoma cruzi | Chagas disease | ||
| Obligate intracellular | Leishmania donovani | Kala-azar | ||
| Helminths | 3 mm–10 m | Extracellular | Wuchereria bancrofti | Filariasis |
| Intracellular | Trichinella spiralis | Trichinosis |

Prions
Prions are composed of abnormal forms of a host protein termed prion protein (PrP). These agents cause transmissible spongiform encephalopathies, including kuru (associated with human cannibalism), hereditary or sporadic Creutzfeldt-Jakob disease (CJD), bovine spongiform encephalopathy (BSE) (better known as mad cow disease), and variant Creutzfeldt-Jakob disease (vCJD) (probably transmitted to humans through consumption of meat from BSE-infected cattle). PrP is found normally in neurons. Diseases occur when the PrP undergoes a conformational change that confers resistance to proteases. The protease-resistant PrP promotes conversion of the normal protease-sensitive PrP to the abnormal form, explaining the transmissable nature of these diseases. CJD can be transmitted from person to person iatrogenically, by surgery, organ transplantation, or blood transfusion. These diseases are discussed in detail in Chapter 23.
Viruses
Viruses are obligate intracellular parasites that depend on the host cell's metabolic machinery for their replication. They consist of a nucleic acid genome surrounded by a protein coat (called a capsid) that is sometimes encased in a lipid membrane. Viruses are classified by their nucleic acid genome (DNA or RNA, but not both), the shape of the capsid (icosahedral or helical), the presence or absence of a lipid envelope, their mode of replication, their preferred cell type for replication (called tropism), or the type of pathology they cause. Some viral components and particles aggregate within infected cells and form characteristic inclusion bodies, which may be seen with the light microscope and are useful for diagnosis (Fig. 9.1). For example, cytomegalovirus (CMV)-infected cells are enlarged and show a large eosinophilic nuclear inclusion and smaller basophilic cytoplasmic inclusions; herpesviruses form a large nuclear inclusion surrounded by a clear halo; and both smallpox and rabies viruses form characteristic cytoplasmic inclusions. However, many viruses (e.g., poliovirus) do not produce inclusions.
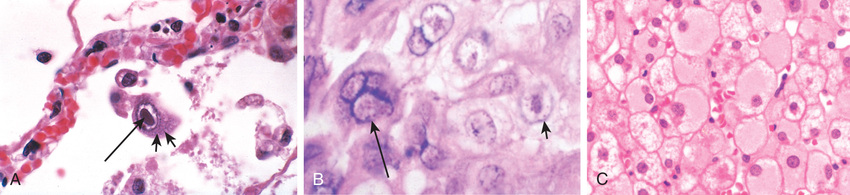
Accounting for a large share of human infections, viruses can cause disease in several ways (Table 9.2). Many viruses cause transient illnesses (e.g., colds, influenza). Other viruses are not eliminated from the body and persist within cells of the host for years, either continuing to multiply (e.g., chronic infection with hepatitis B virus [HBV]) or survive in some latent nonreplicating form, with the potential to be reactivated later. For example, herpes zoster virus, the cause of chickenpox, can enter dorsal root ganglia and establish latency at the site, with periodic reactivation at later times to cause shingles, a painful skin condition. Some viruses are involved in transformation of a host cell into a benign or malignant tumor (e.g., human papillomavirus [HPV]-induced benign warts and cervical carcinoma). Different species of viruses can produce the same clinical picture (e.g., adenovirus and rhinovirus causing upper respiratory infection); conversely, a single virus can cause different clinical manifestations depending on the age or immune status of the host (e.g., CMV causing congenital neurologic damage or gastroenteritis in the immunocompromised).
Table 9.2
Selected Human Viral Diseases and Their Pathogens
| Organ System | Pathogen | Disease(s) |
| Respiratory | Adenovirus | Upper- and lower-respiratory tract infections, conjunctivitis |
| Rhinovirus | Upper-respiratory tract infection | |
| Influenza viruses A, B | Influenza | |
| Respiratory syncytial virus | Bronchiolitis, pneumonia | |
| Digestive | Mumps virus | Mumps, pancreatitis, orchitis |
| Rotavirus | Childhood gastroenteritis | |
| Norovirus | Gastroenteritis | |
| Hepatitis A virus | Acute viral hepatitis | |
| Hepatitis B virus | Acute or chronic hepatitis | |
| Hepatitis D virus | With hepatitis B virus infection: acute or chronic hepatitis | |
| Hepatitis C virus | Acute or chronic hepatitis | |
| Hepatitis E virus | Acute viral hepatitis | |
| Systemic | ||
| With skin eruptions | Measles virus | Measles (rubeola) |
| Rubella virus | German measles (rubella) | |
| Varicella-zoster virus | Chickenpox, shingles | |
| Herpes simplex virus type 1 | Oral herpes (“cold sore”) | |
| Herpes simplex virus type 2 | Genital herpes | |
| With hematopoietic disorders | Cytomegalovirus | Cytomegalic inclusion disease in the newborn, gastroenteritis in transplant patients |
| Epstein-Barr virus | Infectious mononucleosis | |
| HIV-1 and HIV-2 | AIDS | |
| Skin/genital warts | Papillomavirus | Condyloma; cervical carcinoma |
| Central nervous system | Poliovirus | Poliomyelitis |
| JC virus | Progressive multifocal leukoencephalopathy (opportunistic) | |
| Zika virus | Congenital microcephaly |

Bacteria
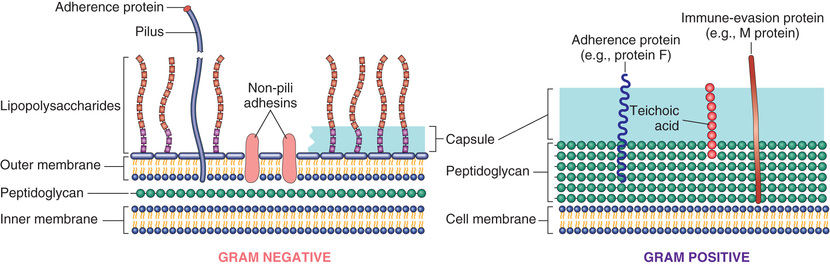
Bacteria are prokaryotes, meaning that they have a cell membrane but lack membrane-bound nuclei and other membrane-enclosed organelles. Most bacteria are bounded by a cell wall consisting of peptidoglycan, a polymer of long sugar chains linked by peptide bridges surrounding the cell membrane. There are two common forms of cell wall structure: a thick wall that retains crystal-violet stain (gram-positive bacteria) and a thin cell wall surrounded by an outer membrane (gram-negative bacteria) (Fig. 9.2). Bacteria are classified by Gram staining (positive or negative), shape (spherical, called cocci, or rod-shaped, called bacilli) (Fig. 9.3), and their requirement for oxygen (aerobic or anaerobic). Motile bacteria have flagella, long helical filaments extending from the cell surface that rotate and move the bacteria. Some bacteria possess pili, another kind of surface projection that can attach bacteria to host cells or extracellular matrix. Bacteria synthesize their own DNA, RNA, and proteins, but they depend on the host for favorable growth conditions. Many bacteria remain extracellular when they grow in the host, while others can survive and replicate both outside and inside of host cells (facultative intracellular bacteria such as mycobacteria), and some grow only inside host cells (obligate intracellular bacteria, such as rickettsia).
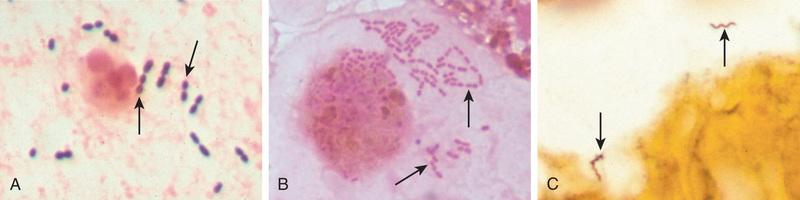
Bacteria cause a range of infections from common pharyngitis and urinary tract infections to rare diseases such as leprosy (Table 9.3). Chlamydia and Rickettsia are obligate intracellular bacteria that replicate inside membrane-bound vacuoles in epithelial and endothelial cells, respectively. These bacteria get most or all of their energy source, ATP, from the host cell. Chlamydia trachomatis is a frequent infectious cause of female sterility (by scarring and narrowing of the fallopian tubes) and blindness (by chronic inflammation of the conjunctiva that eventually causes scarring and opacification of the cornea). Rickettsiae injure the endothelial cells in which they grow, causing a hemorrhagic vasculitis, often visible as a rash, but they also may injure the central nervous system (CNS), with potentially fatal outcome, as in Rocky Mountain spotted fever and epidemic typhus. Rickettsiae are transmitted by arthropod vectors, including lice (in epidemic typhus), ticks (in Rocky Mountain spotted fever and ehrlichiosis), and mites (in scrub typhus).
Table 9.3
Selected Human Bacterial Diseases and Their Pathogens
| Microbiologic Category Clinical Category | Species | Frequent Disease Presentation(s) |
| Infections by pyogenic cocci | Staphylococcus aureus, Staphylococcus epidermidis | Abscess, cellulitis, pneumonia, sepsis |
| Streptococcus pyogenes | Pharyngitis, erysipelas, scarlet fever | |
| Streptococcus pneumoniae | Lobar pneumonia, meningitis | |
| Neisseria meningitidis | Meningitis | |
| Neisseria gonorrhoeae | Gonorrhea | |
| Gram-negative infections | Escherichia coli, Klebsiella pneumoniae, Enterobacter aerogenes, Proteus mirabilis, Serratia marcescens, Pseudomonas aeruginosa, Bacteroides fragilis | Urinary tract infection, wound infection, abscess, pneumonia, sepsis, shock, endocarditis |
| Legionella pneumophila | Legionnaires' disease | |
| Clostridial infections | Clostridium tetani | Tetanus (lockjaw) |
| Clostridium botulinum | Botulism (paralytic food poisoning) | |
| Clostridium perfringens, Clostridium septicum | Gas gangrene, necrotizing cellulitis | |
| Clostridium difficile | Pseudomembranous colitis | |
| Zoonotic bacterial infections | Bacillus anthracis | Anthrax |
| Yersinia pestis | Bubonic plague | |
| Francisella tularensis | Tularemia | |
| Brucella melitensis, Brucella suis, Brucella abortus | Brucellosis (undulant fever) | |
| Borrelia recurrentis | Relapsing fever | |
| Borrelia burgdorferi | Lyme disease | |
| Treponemal infections | Treponema pallidum | Syphilis |
| Mycobacterial infections | Mycobacterium tuberculosis, M. bovis | Tuberculosis |
| Mycobacterium leprae | Leprosy | |
| Mycobacterium kansasii, Mycobacterium avium complex | Pulmonary disease, lymphadenitis, disseminated disease | |
| Actinomycetal infections | Nocardia asteroides complex | Pulmonary disease, brain abscess |
| Actinomyces israelii | Head and neck abscess | |
| Contagious childhood bacterial diseases | Haemophilus influenzae | Meningitis, upper- and lower-respiratory tract infections |
| Bordetella pertussis | Whooping cough | |
| Corynebacterium diphtheriae | Diphtheria | |
| Enteric infections | Enteropathogenic E. coli, Shigella spp., Vibrio cholera, Campylobacter jejuni, Campylobacter coli, Yersinia enterocolitica, Salmonella spp. | Invasive or noninvasive gastroenterocolitis |
| Salmonella enterica serotype Typhi | Typhoid fever |

Mycoplasma and the related genus Ureaplasma are unique among extracellular bacterial pathogens in that they do not have a cell wall. These are the tiniest free-living organisms known (125 to 300 nm).
Fungi
Fungi are eukaryotes with thick cell walls composed of complex carbohydrates such as beta-glucans, chitin, and mannosylated glycoproteins. Calcofluor-white, a fluorescent stain that binds chitin, provides a useful way to identify fungi in patient specimens. Assays for beta-glucans in blood are used to diagnose disseminated fungal infections. Fungi can grow either as rounded yeast cells or as slender, filamentous hyphae. An important distinguishing characteristic is whether hyphae are septate (with cell walls separating individual cells) or aseptate. Some of the most important pathogenic fungi exhibit thermal dimorphism; that is, they grow as hyphal forms at room temperature but as yeast forms at body temperature. Fungi may produce sexual spores or, more commonly, asexual spores called conidia. The latter are produced on specialized structures or fruiting bodies arising along the hyphal filament.
Fungi may cause superficial or deep infections.
• Superficial infections involve the skin, hair, and nails. Fungal species that cause superficial infections are called dermatophytes. Infection of the skin is called tinea; thus, tinea pedis is “athlete's foot” and tinea capitis is scalp ringworm. Certain fungi invade the subcutaneous tissue, causing abscesses or granulomas. Chronic infections, often in the foot, are called mycetomas.
• Deep fungal infections can spread systemically and invade tissues, destroying vital organs in immunocompromised hosts, but usually resolve or remain latent in otherwise normal hosts.
Fungi are divided into endemic and opportunistic species.
• Endemic fungi are invasive species that are usually limited to particular geographic regions (e.g., Coccidioides in the southwestern United States, Histoplasma in the Ohio River Valley).
• Opportunistic fungi (e.g., Candida, Aspergillus, Mucor, Cryptococcus), by contrast, are ubiquitous organisms that either colonize individuals or are encountered from environmental sources but do not cause severe disease in healthy individuals. In immunodeficient individuals, opportunistic fungi give rise to life-threatening invasive infections characterized by vascular occlusion, hemorrhage, and tissue necrosis, with little or no inflammatory response (Fig. 9.4). Patients with AIDS are very susceptible to infection with the opportunistic fungus Pneumocystis jiroveci (previously called Pneumocystis carinii).
Protozoa
Protozoa are single-celled eukaryotes that are major causes of disease and death in developing countries. Protozoa can replicate intracellularly within a variety of cells (e.g., Plasmodium in red cells, Leishmania in macrophages) or extracellularly in the urogenital system, intestine, or blood. Trichomonas vaginalis organisms are sexually transmitted flagellated protozoal parasites that often colonize the vagina and male urethra. The most prevalent pathogenic intestinal protozoans, Entamoeba histolytica and Giardia lamblia, are ingested as nonmotile cysts in contaminated food or water and become motile trophozoites that attach to intestinal epithelial cells. Bloodborne protozoa (e.g., Plasmodium, Trypanosoma, Leishmania) are transmitted by insect vectors, in which they replicate before being passed to new human hosts. Toxoplasma gondii is acquired either through contact with oocyst-shedding cats or by eating cyst-ridden, undercooked meat.
Helminths
Parasitic worms are highly differentiated multicellular organisms. Their life cycles are complex; most alternate between sexual reproduction in the definitive host and asexual multiplication in an intermediate host or vector. Thus, depending on the species, humans may harbor adult worms (e.g., Ascaris lumbricoides), immature stages (e.g., Toxocara canis), or asexual larval forms (e.g., Echinococcus spp.). Once adult worms take up residence in humans, they usually do not multiply but they produce eggs or larvae that typically are passed in stool. Often, the severity of disease is proportional to the number of infecting organisms. For example, a burden of 10 hookworms is associated with mild or no clinical disease, whereas 1000 hookworms consume enough blood to cause severe anemia. In some helminthic infections, such as schistosomiasis, disease is caused by inflammatory responses to the eggs or larvae rather than the adult worms.
Helminths comprise three groups:
• Roundworms (nematodes) are circular in cross-section and nonsegmented. Intestinal nematodes include A. lumbricoides, Strongyloides stercoralis, and hookworms. Nematodes that invade tissues include the filariae, such as Wuchereria bancrofti and Trichinella spiralis (Fig. 9.5).
• Tapeworms (cestodes) have a head (scolex) and a ribbon of multiple flat segments (proglottids). They adsorb nutrition through their tegument and do not have a digestive tract. They include the fish, beef, and pork tapeworms that make their home in the human intestine. The larvae that develop after ingestion of eggs of certain tapeworms can cause cystic disease within tissues (Echinoccus granulosus larvae cause hydatid cysts; pork tapeworm larvae produce cysts called cysticerci in many organs).
• Flukes (trematodes) are leaf-shaped flatworms with prominent suckers that are used to attach to the host. They include liver and lung flukes and schistosomes.
Ectoparasites
Ectoparasites are insects (e.g., lice, bedbugs, fleas) or arachnids (e.g., mites, ticks, spiders) that cause disease by biting or by attaching to and living on or in the skin. Infestation of the skin by arthropods is characterized by itching and excoriations, such as pediculosis caused by lice attached to hairs, or scabies caused by mites burrowing into the stratum corneum. At the site of bites, mouth parts may be found associated with a mixed infiltrate of lymphocytes, macrophages, and eosinophils. Arthropods also can serve as vectors for other pathogens, such as Borrelia burgdorferi, the agent of Lyme disease, which is transmitted by deer ticks.
The Microbiome
The microbiome is the diverse microbial population of bacteria, fungi, and viruses found in or on the human body (e.g., in the intestinal tract, skin, upper airway, and vagina). While most of these organisms do not harm the healthy host, a few cause diseases such as skin and soft-tissue infections (Staphylococcus aureus and Streptococcus pyogenes), acne (Propionibacterium acnes), and tooth decay (Streptococcus mitus). The microbiome has important roles in normal health and development. In the intestinal tract, the normal flora are responsible for absorption of digested foods, for maintaining the integrity of the epithelium and the normal functioning of the intestinal immune system, and for competitively inhibiting invasion and colonization by potentially pathogenic microbes. The gut microbiome is also emerging as a regulator of nutritional status.
New techniques of bacterial identification relying on ribosomal RNA sequencing have dramatically improved our understanding of the microbiome:
• In healthy individuals, the microbiome is very diverse. For example, there are estimated to be over 1000 species of bacteria in the normal intestinal flora of an individual. In a healthy person, a part of the bacterial population at various body sites is relatively stable over time, but may be altered by diet and environment.
• The diversity of bacteria is greatest in the oral cavity and the stool, intermediate on the skin, and least in the vagina.
• The bacterial microbiomes at various body sites are partially similar in different individuals.
Dysbiosis refers to changes in composition of the microbiome that are associated with disease. These changes may result from therapies or various pathophysiologic conditions, including the following:
• Use of some antibiotics is an important risk factor for intestinal infections caused by toxin-producing Clostridium difficile. These antibiotics kill or inhibit normal commensal bacteria, allowing overgrowth of C. difficile. Restoration of the microbiome by duodenal infusion of stool containing commensal flora from healthy donors successfully treats C. difficile infection in many individuals who have relapsed after antibiotic therapy.
• The microbiome in the stool of obese individuals is less diverse than that of lean individuals, and the proportions of bacterial phyla differ as well. The proportions of these phyla in obese individuals who change their diet and lose weight shifts to resemble that of lean individuals. Experimental animals gain more weight when colonized with bacterial populations associated with a high-fat diet than when colonized with bacterial populations associated with a normal diet.
• The intestinal bacterial populations in individuals with inflammatory bowel disease are altered, with reduced diversity and changes in the proportions of bacterial phyla, compared to individuals without inflammatory bowel disease. Interestingly, inflammatory bowel disease also is associated with changes in the viral populations in stool. The specific roles of different viruses and bacteria in gastrointestinal dysbiosis is an area of very active investigation.
Techniques for Identifying Infectious Agents
There are several methods for identifying microorganisms in tissue and body fluids:
• Culture. Bacterial and fungal cultures remain essential for diagnostic testing, in conjunction with additional methods, but culture of viruses has been replaced to a great extent by alternative methods.
• Histology. Some infectious agents can be seen in hematoxylin and eosin (H&E)–stained sections (e.g., the inclusion bodies formed by CMV and herpes simplex virus (HSV); bacterial clumps, which usually stain blue; Candida and Mucor among the fungi; most protozoans; all helminths). Many infectious agents, however, are better visualized by special stains that identify organisms on the basis of particular characteristics of their cell wall or coat—Gram, acid-fast, silver, mucicarmine, and Giemsa stains—or after labeling with specific antibodies (Table 9.4). Organisms are usually best visualized at the advancing edge of a lesion rather than at its center, particularly if there is necrosis.
Table 9.4
Techniques for Identifying Infectious Agents
| Technique | Infectious Agent(s) |
| Gram stain | Most bacteria |
| Wet Mount/Calcofluor-white/Fungi-fluor | Fungi |
| Acid-fast stain | Mycobacteria, nocardiae (modified) |
| Silver stain | Fungi, legionellae, Pneumocystis |
| Periodic acid–Schiff stain | Fungi, amebae |
| Mucicarmine stain | Cryptococci |
| Giemsa stain | Leishmaniae, Plasmodium |
| Antibodies | All classes |
| Culture | All classes |
| DNA probes and polymerase chain reaction | All classes |
| Proteomic methods/mass spectrometry | Bacteria, mycobacteria, fungi |
• Serology. Acute infections can be diagnosed serologically by detecting pathogen-specific antibodies in the serum. The presence of specific immunoglobulin M (IgM) antibody shortly after the onset of symptoms is often diagnostic. Alternatively, specific antibody titers can be measured early (“acute”) and again at 4 to 6 weeks (“convalescent”) after infection; a 4-fold rise in titer usually is considered diagnostic. Assays for serum antibodies are very useful for the diagnosis of viral hepatitis. Antibodies that are not pathogen-specific are produced by patients with syphilis or infectious mononucleosis, and assays for these cross-reacting antibodies are used in diagnosis.
• Molecular diagnostics. Nucleic acid amplification techniques, such as polymerase chain reaction (PCR) and transcription-mediated amplification, are used for diagnosis of gonorrhea, chlamydial infection, tuberculosis, and herpes encephalitis. Molecular assays are much more sensitive than conventional testing for some pathogens. PCR testing of cerebrospinal fluid (CSF) for HSV encephalitis has a sensitivity of about 80%, whereas viral culture of CSF has a sensitivity of less than 10%. Similarly, nucleic acid tests for genital Chlamydia detect 10% to 30% more cases than conventional Chlamydia culture does. For other infections, such as gonorrhea, the sensitivity of nucleic acid testing is similar to that of culture. Quantitative PCR for BK virus, CMV, and Epstein-Barr virus (EBV) is used to assess viral loads in transplant recipients. Molecular panels for detection of 20 or more pathogens are now routinely used to diagnose respiratory bacterial and viral infections, as well as gastrointestinal bacterial, viral and parasitic infections. Quantitative assays for viral nucleic acids are used to guide the medical management of patients infected with human immunodeficiency virus (HIV), HBV, and hepatitis C virus (HCV). Next-generation sequencing, with or without initial PCR amplification, is being used for the detection of novel or rare pathogens, and for epidemiologic investigations.
• Proteomics. Mass spectrometry can be used to identify microorganisms based on protein content and has been introduced into routine clinical laboratories. It has the advantage of rapid identification of the bacterial species but is not useful for antibiotic sensitivity. That still requires culture.
Newly Emerging and Reemerging Infectious Diseases
A surprising number of new infectious agents continue to be discovered, and there are several reasons for this:
• Some pathogens were discovered due to improved methods of detection, although they have likely been present in humans for centuries. For example, Helicobacter pylori, which causes gastritis and peptic ulcer disease, was only discovered in the 1980s. More recently, a new cause of leprosy was discovered, Mycobacterium lepromatosis. This agent, identified by sequencing bacterial DNA from biopsy material of patients who died of leprosy, is a close relative of the previously known Mycobacterium leprae.
• Animals are a source of new pathogens that infect humans. Two coronaviruses that cause severe respiratory tract infections in humans, Middle East respiratory syndrome coronavirus (MERS CoV) and the severe acute respiratory syndrome (SARS) virus, likely spread to humans from animals and were first detected in 2003 and 2012, respectively. Other examples of pathogens that emerged in humans after being transmitted from animals include HIV and B. burgdorferi.
• Microorganisms can acquire genes that enhance virulence or overcome host defense. In 2011, almost 4000 individuals in Germany were infected with a new strain of highly virulent shiga-toxin producing Escherichia coli that spread in sprout seeds. The new strain was derived from a different type of E. coli that acquired a gene for the shiga-toxin from a bacteriophage.
• Other pathogens have become much more common because of immunosuppression caused by AIDS, or therapy to prevent transplant rejection or treat cancers (e.g., human herpes virus 8, Mycobacterium avium complex, P. jirovecii).
Additional clinical syndromes may be recognized after the pathogen has been known for some time, possibly due to new contributing factors. Although Zika virus was discovered in 1947 in Uganda, very few human cases were reported for many years, until the virus more recently spread through additional countries, expanding the range from Africa, Asia, and the Pacific to the Americas, causing newly recognized clinical cases. The virus is contracted primarily via the Aedes species mosquito but also via sexual transmission and possibly blood transfusion. Although many individuals infected have no or mild nonspecific symptoms, infection may be associated with Guillain-Barre syndrome, a form of rapid-onset muscle weakness caused by immune system damage to the nervous system. Infection with Zika virus during pregnancy is associated with birth defects, including microcephaly. Many more congenital cases were diagnosed in the 2015 outbreak beginning in Brazil compared to earlier outbreaks, creating a Public Health Emergency of International Concern. Further investigation is ongoing to determine if other variables may be contributing to the CNS effects such as genetics, co-infections, immunity from past infections, or yet to be defined environmental factors.
Several factors contribute to the emergence of infectious diseases:
• Human behavior affects the spread and demographics of infections. AIDS was first recognized in the United States as predominantly a disease of homosexual men and drug abusers, but heterosexual transmission is now more common. In sub-Saharan Africa, the area of the world with the highest number of AIDS cases, it is predominantly a heterosexual disease. The Ebola virus epidemic of 2014 spread to more countries than previous Ebola outbreaks due in part to the frequent movement of people across borders in West Africa, as well as burial practices that involved contact with the bodies of the deceased. SARS, mentioned earlier, spread very quickly to 24 countries due to human air travel before it was contained.
• Changes in the environment occasionally increase the incidence of infectious diseases. Regrowth of forests in the eastern United States with cessation of farming has led to massive increases in deer and mice, which carry the ticks that transmit Lyme disease, babesiosis, and ehrlichiosis. Global warming also has had an impact on the spread of infections. For example, the mosquitoes that carry Dengue fever and Zika viruses, which used to be confined to the U.S.-Mexican border, are now found in more than half of the states. Chikungunya virus transmitted by mosquitoes, which causes fever and joint pain that can be severe for some, was first seen in the Americas in 2013, and transmission of Dengue and Zika viruses has recently been reported in Florida.
• Infectious diseases that are common in one geographic area may be introduced into a new area due to increased travel or movement of infected animals, invertebrates, or birds. For example, West Nile virus has been common in Europe, Asia, and Africa for years but was first described in the United States in 1999, possibly transported by an infected mosquito or bird. Highly pathogenic H5 influenza viruses, which have led to death of some patients in Asia, have spread throughout the world during the last 2 decades in bird populations, due to their natural migration and transport of domestic birds.
• Pathogens adapt rapidly to selective pressures exerted by widespread use of antibiotics. Antibiotic resistance has developed and is now common in Mycobacterium tuberculosis, Neisseria gonorrhoeae, Klebsiella pneumoniae, and S. aureus. Similarly, development of drug-resistant parasites has dramatically increased the morbidity and mortality associated with Plasmodium falciparum infection in Asia, Africa, and Latin America.
Agents of Bioterrorism
Sadly, the anthrax attacks in the United States in 2001 transformed the theoretical threat of bioterrorism into reality. The Centers for Disease Control and Prevention (CDC) has evaluated the danger microorganisms pose as weapons on the basis of the efficiency with which disease can be transmitted, how difficult the microorganisms are to produce and distribute, what can be done to defend against them, and the extent to which they are likely to alarm the public and produce widespread fear. Based on these criteria, the CDC has ranked bioweapons into three categories, designated A, B, and C (Table 9.5).
Table 9.5
Potential Agents of Bioterrorism
Category A Diseases and Agents
Anthrax: Bacillus anthracis
Botulism: Clostridium botulinum toxin
Plague: Yersinia pestis
Smallpox: Variola major virus
Tularemia: Francisella tularensis
Viral hemorrhagic fevers: Ebola, Marburg, Lassa, others
Category B Diseases and Agents
Brucellosis: Brucella spp.
Epsilon toxin of Clostridium perfringens
Food safety threats: Salmonella spp., Escherichia coli O157:H7, Shigella, others
Glanders: Burkholderia mallei
Melioidosis: Burkholderia pseudomallei
Psittacosis: Chlamydia psittaci
Q fever: Coxiella burnetii
Ricin toxin from castor beans (Ricinus communis)
Staphylococcal enterotoxin B
Typhus fever: Rickettsia prowazekii
Mosquito-borne encephalitis viruses: Venezuelan equine encephalitis, Eastern equine encephalitis, Western equine encephalitis, others
Water safety threats: Vibrio cholerae, Cryptosporidium parvum, others
Category C Diseases and Agents
Emerging infectious disease threats: Nipah virus, hantavirus, others
Adapted from Centers for Disease Control and Prevention Information (http://emergency.cdc.gov).
The agents in the highest-risk category A can be readily disseminated or transmitted from person to person, typically cause diseases that carry a high mortality rate with potential for major public health impact, may cause pandemics leading to widespread panic and social disruption, and are likely to require special action for public health preparedness. For example, the smallpox virus is a category A agent because of its high transmissibility, case mortality rates of 30% or greater, and the lack of effective therapy. Smallpox readily spreads from person to person, mainly through respiratory secretions and by direct contact with virus in skin lesions. Since routine smallpox vaccination ended in the United States in 1972, immunity has waned, leaving the population highly susceptible. Concern that smallpox could be used for bioterrorism has led to reinstitution of vaccination for some medical and military personnel.
Category B agents are less easy to disseminate, cause disease associated with moderate morbidity but low mortality, and require specific diagnostic and disease surveillance. Many of these agents can be spread in food or water. Category C agents include emerging pathogens that could be engineered for mass dissemination because of ease of availability, production, and dissemination; the potential for high morbidity and mortality; and great impact on health.
Transmission and Dissemination of Microbes
Microbes can enter the host through several body surfaces and, once in the host, can disseminate by different routes.
Routes of Entry of Microbes
Microbes can enter the host through breaches in the skin, by inhalation or ingestion, or by sexual transmission. The first defenses against infection are intact skin and mucosal surfaces, which provide physical barriers and produce anti-microbial substances. In general, respiratory, gastrointestinal, or genitourinary tract infections that occur in otherwise healthy individuals are caused by relatively virulent microorganisms that are capable of damaging or penetrating intact epithelial barriers. By contrast, most skin infections in healthy individuals are caused by less virulent organisms that breach the skin through damaged sites (Table 9.6).
Table 9.6
Routes of Microbial Infection
| Site | Major Local Defense(s) | Basis for Failure of Local Defense | Pathogen/Disease (Examples) |
| Skin | Epidermal barrier | Mechanical defects (punctures, burns, ulcers) | Staphylococcus aureus, Candida albicans, Pseudomonas aeruginosa |
| Needle sticks | HIV, hepatitis viruses | ||
| Arthropod and animal bites | Yellow fever, plague, Lyme disease, malaria, rabies, Zika virus | ||
| Direct penetration | Schistosoma | ||
| Gastrointestinal tract | Epithelial barrier | Attachment and local proliferation of microbes | Vibrio chloerae, Giardia |
| Attachment and local invasion of microbes | Shigella, Salmonella, Campylobacter | ||
| Uptake through M cells | Poliovirus, certain pathogenic bacteria | ||
| Acidic secretions | Acid-resistant cysts and eggs | Many protozoa and helminths | |
| Bile and pancreatic enzymes | Resistant microbial external coats | Hepatitis A, Rotavirus, Norovirus | |
| Normal protective flora | Broad-spectrum antibiotic use | Clostridium difficile | |
| Respiratory tract | Mucociliary clearance | Attachment and local proliferation of microbes | Influenza viruses |
| Ciliary paralysis by toxins | Haemophilus influenzae, M. pneumoniae, Bordetella pertussis | ||
| Resident alveolar macrophages | Resistance to killing by phagocytes | M. tuberculosis | |
| Urogenital tract | Urination | Obstruction, microbial attachment, and local proliferation | E. coli |
| Normal vaginal flora | Antibiotic use | Candida albicans | |
| Intact epidermal/epithelial barrier | Microbial attachment and local proliferation | Neisseria gonorrhoeae | |
| Direct infection/local invasion | Herpes viruses, Zika virus, Treponema pallidum | ||
| Local trauma | Various sexually transmitted diseases (e.g., human papilloma virus) |

Skin
The dense, keratinized outer layer of skin is a natural barrier to infection; furthermore, the low pH of the skin (less than 5.5) combined with the presence of fatty acids inhibit growth of microorganisms other than the normal bacteria and fungi. Included among these normal flora are potential opportunists, such as S. aureus and Candida albicans.
Cutaneous infections are typically acquired by entry of microbes through breaks in the skin, including wounds or surgical incisions (Staphylococci), burns (Pseudomonas aeruginosa), and diabetic and pressure-related foot sores (multibacterial infections). Intravenous catheters in hospitalized patients provide portals for local or systemic infection. Needle sticks can expose the recipient to infected blood and transmit HBV, HCV, or HIV. Some pathogens penetrate the skin via an insect or animal bite. Bites by fleas, ticks, mosquitoes, mites, and lice break the skin and transmit arboviruses (causes of yellow fever and encephalitis), bacteria (plague, Lyme disease, Rocky Mountain spotted fever), protozoa (malaria, leishmaniasis), and helminths (filariasis). Animal bites can lead to infections with bacteria, such as Pasteurella, or viruses, such as rabies. Only a few microorganisms are able to cross the skin barrier directly. For example, Schistosoma larvae released from freshwater snails penetrate swimmers' skin by releasing enzymes that dissolve the extracellular matrix, traversing unbroken skin. Similarly, certain fungi (dermatophytes) can infect intact stratum corneum of the skin, hair, and nails.
Gastrointestinal Tract
Gastrointestinal pathogens are transmitted by food or drink contaminated with fecal material. When hygiene fails, as may occur with natural disasters such as floods and earthquakes, diarrheal disease becomes rampant. Acidic gastric secretions are important defenses and are lethal for many gastrointestinal pathogens. Healthy volunteers do not become infected by Vibrio cholerae unless they are fed 1011 organisms, but neutralizing the stomach acid reduces the infectious dose by 10,000-fold. By contrast, some ingested agents, such as Shigella and Giardia cysts, are relatively resistant to gastric acid, so fewer than 100 organisms can cause illness.
Other normal defenses within the gastrointestinal tract include (1) the layer of viscous mucus covering the intestinal epithelium, (2) lytic pancreatic enzymes and bile detergents, (3) mucosal anti-microbial peptides called defensins, (4) normal flora, and (5) secreted IgA antibodies. IgA antibodies are made by plasma cells located in mucosa-associated lymphoid tissue (MALT). These lymphoid aggregates are covered by a single layer of specialized epithelial cells called M cells, which are important for transport of antigens to MALT. Numerous gut pathogens use M cells to enter the host from the intestinal lumen, including poliovirus, enteropathic E. coli, V. cholerae, Salmonella enterica serotype Typhi, and Shigella flexneri.
Infection via the gastrointestinal tract occurs when local defenses are weakened or the organisms develop strategies to overcome these defenses. Host defenses are weakened by low gastric acidity, by antibiotics that alter the normal bacterial flora (e.g., in pseudomembranous colitis due to C. difficile), or when there is stalled peristalsis or mechanical obstruction. Viruses that can enter the body through the intestinal tract (e.g., hepatitis A, rotavirus) are those that lack envelopes, because enveloped viruses are inactivated by bile and digestive enzymes.
Enteropathogenic bacteria cause gastrointestinal disease in several ways:
• Toxin production in food. S. aureus and Bacillus cereus can contaminate and grow in food, where they release powerful enterotoxins that, when ingested, cause food poisoning without any bacterial growth in the gut.
• Adhesion, local proliferation, and toxin production in the host. V. cholerae and enterotoxigenic E. coli bind to the intestinal epithelium and multiply in the overlying mucous layer, where they release exotoxins that cause epithelial cells to secrete large volumes of fluid, resulting in watery diarrhea.
• Invasion. Shigella, Salmonella, and Campylobacter invade locally and damage the intestinal mucosa and lamina propria, causing ulceration, inflammation, and hemorrhage—changes manifested clinically as bloody diarrhea (dysentery). S. enterica serotype Typhi passes from the damaged mucosa through Peyer patches and mesenteric lymph nodes and into the bloodstream, resulting in a systemic infection.
Fungal infections of the gastrointestinal tract occur in immunologically compromised individuals. Candida, part of the normal gastrointestinal flora, shows a predilection for stratified squamous epithelium, causing oral thrush or membranous esophagitis, but also may spread to the stomach, lower gastrointestinal tract, and other organs.
Most intestinal parasites enter the body by being ingested as cysts, eggs, or meat-borne larvae, but a few enter by penetrating the skin and finding their way to the intestine. Once in the intestine, these pathogens cause damage in several ways:
• G. lamblia attaches to the epithelial brush border, but does not invade into cells or tissue. Attachment of the organisms leads to blunting of villi, loss of brush border, malabsorption, and chronic inflammation through mechanisms that are poorly understood.
• Cryptosporidia are taken up by enterocytes, in which they replicate, leading to extensive mucosal damage, villous atrophy, and inflammation.
• E. histolytica kills host cells by contact-mediated cytolysis through a channel-forming pore protein, with consequent ulceration and invasion of the colonic mucosa.
• Intestinal helminths cause disease when they are present in large numbers or travel to ectopic sites. Large numbers of A. lumbricoides can obstruct the gut, and this organism can invade and damage the bile ducts as well.
• Helminths also cause disease by depriving the host of nutrients. Hookworms cause iron-deficiency anemia by sucking blood from intestinal villi; Diphyllobothrium, the fish tapeworm, causes anemia by depriving the host of vitamin B12.
Respiratory Tract
A large number of microorganisms, including viruses, bacteria, and fungi, are inhaled daily by every individual. In many cases, the microbes are inhaled in dust or aerosol particles. The distance these particles travel into the respiratory system is inversely proportional to their size. Large particles are trapped in the mucociliary blanket that lines the nose and the upper respiratory tract. Microorganisms trapped in the mucus secreted by goblet cells are transported by ciliary action to the back of the throat, where they are swallowed or coughed out. Particles smaller than 5 µm travel directly to the alveoli, where they are phagocytosed by alveolar macrophages or by neutrophils recruited to the lung by cytokines.
Microorganisms that invade the normal healthy respiratory tract have developed specific mechanisms to overcome mucociliary defenses or to avoid destruction by alveolar macrophages. Some successful respiratory viruses evade these defenses by attaching to and entering epithelial cells in the lower respiratory tract and pharynx. For example, influenza viruses possess hemagglutinin proteins that project from the surface of the virus and bind to sialic acid on the surface of epithelial cells. This attachment induces the host cell to engulf the virus, leading to viral entry and replication within the host cell.
Certain bacterial respiratory pathogens release toxins that paralyze cilia. Examples include Haemophilus influenzae, Mycoplasma pneumoniae, and Bordetella pertussis. Some bacteria lack the ability to overcome the defenses of the healthy lung and can cause respiratory infections only in compromised hosts. Streptococcus pneumoniae and S. aureus can cause pneumonia subsequent to influenza because the viral infection leads to the loss of the protective ciliated epithelium. Chronic damage to mucociliary defense mechanisms occurs in smokers and individuals with cystic fibrosis, while acute injury occurs in intubated patients and in those who aspirate gastric acid.
Some respiratory pathogens avoid phagocytosis or destruction after phagocytosis. M. tuberculosis, for example, gains a foothold in alveoli because it escapes killing within the phagolysosomes of macrophages. Opportunistic fungi infect the lungs when cellular immunity is depressed or when leukocytes are reduced in number (e.g., P. jiroveci in patients with AIDS, Aspergillus spp. after chemotherapy).
Urogenital Tract
The urinary tract is almost always invaded from the exterior by way of the urethra. The regular flushing of the urinary tract with urine serves as a defense against invading microorganisms. Urine in the bladder is normally sterile or contains only small numbers of fastidious bacteria; however, successful pathogens (e.g., N. gonorrhoeae, E. coli) adhere to the urinary epithelium, overcoming the host defense of regular flushing. Anatomy plays an important role in infection. Women have many more urinary tract infections than men because the distance between the urinary bladder and skin (i.e., the length of the urethra) is 5 cm in women, in contrast with 20 cm in men. Obstruction of urinary flow, as in benign prostatic hyperplasia, or reflux can compromise normal defenses and increase susceptibility to urinary tract infections. Urinary tract infections can spread further up from the bladder to the kidney and cause acute and chronic pyelonephritis.
From puberty until menopause, the vagina is protected from pathogens by a low pH resulting from catabolism of glycogen in the normal epithelium by lactobacilli. Antibiotics can kill the lactobacilli, allowing overgrowth of yeast, with resultant vaginal candidiasis.
Spread and Dissemination of Microbes Within the Body
Some microorganisms proliferate locally, at the site of initial infection, whereas others penetrate the epithelial barrier and spread to distant sites by way of the lymphatics, the blood, or nerves (Fig. 9.6). In contrast to those that disseminate, pathogens that cause superficial infections stay confined to the lumen of hollow viscera (e.g., V. cholerae) or interact exclusively with epithelial cells (e.g., papillomaviruses, dermatophytes).
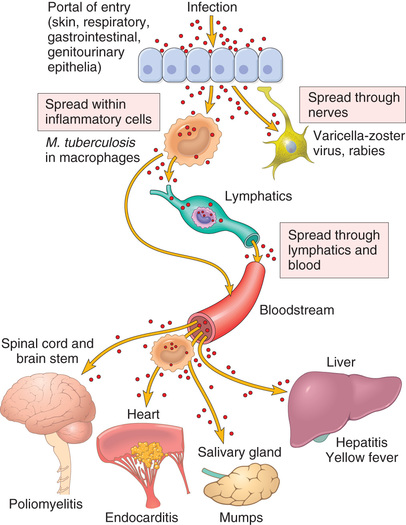
Microbes can spread within the body in several ways:
• Lysis and invasion. Some extracellular bacteria, fungi, and helminths secrete lytic enzymes that destroy tissue and allow direct invasion. For example, S. aureus secretes hyaluronidase, which degrades the extracellular matrix between host cells. Invasive microbes initially follow tissue planes of least resistance and drain to regional lymphatics. S. aureus may travel from a localized abscess to the draining lymph nodes. This can sometimes lead to bacteremia and spread to deep organs (heart, bone).
• Through blood and lymph. Microorganisms may be spread either in extracellular fluid or within host cells. Some viruses (e.g., poliovirus, HBV), most bacteria and fungi, some protozoa (e.g., African trypanosomes), and all helminths are transported in the plasma. Leukocytes can carry herpesviruses, HIV, mycobacteria, Leishmania, and Toxoplasma. The parasites Plasmodium and Babesia are found within red cells.
• Cell-to-cell transmission. Most viruses spread locally from cell to cell by replication and release of infectious virions, but others may propagate from cell to cell by causing fusion of host cells, or by transport within nerves (as with rabies virus and varicella-zoster virus).
The consequences of bloodborne spread of pathogens vary widely depending on the virulence of the organism, the magnitude of the infection, the pattern of seeding, and host factors such as immune status. Sporadic bloodstream invasion by low-virulence or nonvirulent microbes (e.g., during brushing of teeth) is common but is quickly controlled by normal host defenses. By contrast, disseminated viremia, bacteremia, fungemia, or parasitemia by virulent pathogens poses a serious danger and manifests as fever, hypotension, and multiple other systemic signs and symptoms of sepsis. Massive bloodstream invasion by bacteria can be rapidly fatal, even in previously healthy individuals.
The major manifestations of infectious disease may appear at sites distant from the point of microbe entry. For example, varicella-zoster and measles viruses enter through the airways but cause rashes in the skin; poliovirus enters through the intestine but kills motor neurons to cause paralysis. Schistosoma mansoni parasites penetrate the skin but eventually localize in blood vessels of the portal system and mesentery, damaging the liver and intestine. Schistosoma hematobium also penetrates the skin, but localizes to the urinary bladder and causes cystitis. The rabies virus travels from the site of a bite by a rabid animal to the brain by retrograde transport in sensory neurons, where it then causes encephalitis and death.
Transmission of Microbes
Transmission depends on the hardiness of the microbe. Some microbes can survive for extended periods in dust, food, or water. Bacterial spores, protozoan cysts, and thick-shelled helminth eggs can survive in a cool and dry environment. Less hardy microorganisms must be quickly passed from person to person, often by direct contact.
For transmission of disease, the mode of exit of a microorganism from the host's body is as important as entry into it. Every fluid or tissue that is normally secreted, excreted, or shed is used by microorganisms to leave the host for transmission to new victims.
• Skin. Skin flora, such as S. aureus and dermatophytes (fungi), are shed in the desquamated skin. Some sexually transmitted pathogens are transmitted from genital skin lesions, such as HSV and Treponema pallidum (causing syphilis).
• Oral secretions. Viruses that replicate in the salivary glands and are spread in saliva include mumps virus, CMV, and rabies virus.
• Respiratory secretions. Viruses and bacteria can be shed in respiratory secretions during talking, coughing, and sneezing. Most respiratory pathogens, including influenza viruses, spread in large respiratory droplets, which travel no more than 3 feet. However, a few organisms, including M. tuberculosis and varicella-zoster virus, are spread from the respiratory tract in small respiratory droplets or within dust particles that can travel long distances in the air. These properties determine the type of isolation precautions that are used to prevent the spread of infection.
• Stool. Organisms shed in stool include many pathogens that replicate in the lumen or epithelium of the gut, such as Shigella, G. lamblia, and rotavirus. Pathogens that replicate in the liver (hepatitis A virus) or gallbladder (S. enterica serotype Typhi) enter the intestine in bile and are shed in stool.
• Blood. Pathogens spread via blood may be transmitted by invertebrate vectors, medical practices (blood transfusion, reuse of equipment), or sharing of needles by intravenous drug abusers. Bloodborne parasites, including Plasmodium spp. and arboviruses, are transmitted by biting insects.
• Urine. Urine is the usual mode of exodus from the human host for only a few organisms, including S. haematobium, which grows in the veins of the bladder and releases eggs that reach the urine.
• Genital tract. Sexually transmitted infections (STIs) spread from the urethra, vagina, cervix, rectum, or oral pharynx. Organisms that cause STIs depend on direct contact for person-to-person spread because these pathogens cannot survive in the environment. Transmission of STIs often is by asymptomatic individuals who do not realize that they are infected. Infection with one STI increases the risk for additional STIs, mainly because the risk factors are the same for all STIs. STIs are described in Chapters 18 and 19.
• Vertical transmission. Transmission of infectious agents from mother to fetus or newborn child is a common mode of transmission for some pathogens, and may occur through several different routes. Placental-fetal transmission is most likely to occur when the mother is infected with a pathogen during pregnancy. Some of the resulting infections interfere with fetal development, and the degree and type of damage depend on the age of the fetus at the time of infection. For example, rubella infection during the first trimester can lead to heart malformations, mental retardation, cataracts, or deafness, while rubella infection during the third trimester has little effect. Congenital microcephaly and other CNS complications have been associated with Zika virus infection during pregnancy. Much is still unknown about timing of infection relative to the trimester of pregnancy. Transmission during birth is caused by contact with infectious agents during passage through the birth canal. Examples include gonococcal and chlamydial conjunctivitis. Postnatal transmission in maternal milk can transmit CMV, HIV, and HBV.
Microbes also can be transmitted from animal to human resulting in zoonotic infections, either through direct contact with or consumption of animal products or indirectly by an invertebrate vector.
How Microorganisms Cause Disease
Infectious agents establish infection and damage tissues by any of three mechanisms:
• They can contact or enter host cells and directly cause death of infected cells.
• They can release toxins that kill cells at a distance, release enzymes that degrade tissue components, or damage blood vessels and cause ischemic necrosis.
• They can induce host immune responses that, although directed against the invader, cause additional tissue damage. Thus, the defensive responses of the host can be a mixed blessing, helping to overcome the infection but also contributing to tissue damage.
Described next are some of the mechanisms whereby viruses and bacteria damage host tissues.
Mechanisms of Viral Injury
Viruses can directly damage host cells by entering them and replicating at the host's expense. The manifestations of viral infection are largely determined by the tropism of the virus for specific tissues and cell types. Tropism is influenced by a number of factors.
• Host receptors for viruses. Viruses are coated with surface proteins that bind with high specificity to particular host cell surface proteins. Entry of many viruses into cells commences with binding to normal host cell receptors. For example, HIV glycoprotein gp120 binds to CD4 and CXCR4 and CCR5 on T cells and macrophages (Chapter 5). Host proteases may be needed to enable binding of virus to host cells; for instance, a host protease cleaves and activates the influenza virus hemagglutinin.
• Specificity of transcription factors. The ability of the virus to replicate inside particular cell types depends on the presence of lineage-specific transcription factors that recognize viral enhancer and promoter elements. For example, the JC virus, which causes leukoencephalopathy (Chapter 23), replicates only in oligodendroglia in the CNS because the promoter and enhancer DNA sequences regulating viral gene expression are active in glial cells, but not in neurons or endothelial cells.
• Physical characteristics of tissues. Host environment and temperature can contribute to tissue tropism. For example, enteroviruses replicate in the intestine in part because they can resist inactivation by acids, bile, and digestive enzymes. Rhinoviruses infect cells only within the upper-respiratory tract because they replicate optimally at the lower temperatures characteristic of this site.
Once viruses are inside host cells, they can damage or kill the cells by a number of mechanisms (Fig. 9.7):
• Direct cytopathic effects. Viruses can kill cells by preventing synthesis of critical host macromolecules, by producing degradative enzymes and toxic proteins, or by inducing apoptosis. For example, poliovirus blocks synthesis of host proteins by inactivating cap-binding protein. HSV produces proteins that inhibit synthesis of cellular DNA and mRNA and other proteins that degrade host DNA. Viral replication also can trigger apoptosis of host cells by cell-intrinsic mechanisms, such as perturbations of the endoplasmic reticulum during virus assembly, which can activate caspases that mediate apoptosis.
• Anti-viral immune responses. Viral proteins on the surface of host cells may be recognized by the immune system, and lymphocytes may attack virus-infected cells. Cytotoxic T lymphocytes (CTLs) are important for defense against viral infections, but CTLs also can be responsible for tissue injury. Hepatitis B infection causes CTL-mediated destruction of infected hepatocytes, a normal response that is attempting to clear the infection.
• Transformation of infected cells. Different oncogenic viruses (e.g., HPV, EBV) can stimulate cell growth and survival by a variety of mechanisms, including hijacking the control of cell cycle machinery, anti-apoptotic strategies, and insertional mutagenesis (in which the insertion of viral DNA into the host genome alters the expression of nearby host genes). Mechanisms of viral transformation are discussed in Chapter 6.
Mechanisms of Bacterial Injury
Bacterial Virulence
Bacterial damage to host tissues depends on the ability of the bacteria to adhere to host cells, invade cells and tissues, or deliver toxins. Pathogenic bacteria have virulence genes that are frequently found grouped together in clusters called pathogenicity islands. A small number of virulence genes can determine whether a bacterium is harmful. The Salmonella strains that infect humans are so closely related that they are a single species, but only a few virulence genes determine whether an isolate of Salmonella causes life-threatening typhoid fever or self-limited gastroenteritis.
Plasmids (small independently replicating circular DNAs) and bacteriophages (viruses) are genetic elements that spread between bacteria and can carry virulence factors, including toxins or enzymes that confer antibiotic resistance. Exchange of these elements between bacteria can endow the recipient bacteria with a survival advantage and/or the capacity to cause disease. Plasmids or transposons encoding antibiotic resistance can convert an antibiotic-susceptible bacterium into a resistant one, making effective therapy difficult. Carbapenemase genes carried on plasmids have spread among gram-negative bacilli worldwide, resulting in strains for which there are no available effective antibiotics, causing the CDC to list these organisms as an urgent threat.
Populations of bacteria also can act together in ways that alter their virulence.
• Quorum sensing. Many species of bacteria coordinately regulate gene expression within a large population in which specific genes, such as virulence genes, are expressed after bacteria reach high concentrations. This in turn may allow bacteria growing in discrete host sites, such as an abscess or consolidated pneumonia, to overcome host defenses. S. aureus coordinately regulates virulence factors by secreting autoinducer peptides. As the bacteria grow to increasing concentrations, the level of the autoinducer peptide increases, stimulating exotoxin production.
• Biofilms. Communities of bacteria can live within a viscous layer of extracellular polysaccharides that adhere to host tissues or devices such as intravascular catheters and artificial joints. Biofilms make bacteria inaccessible to immune effector mechanisms and increase their resistance to anti-microbial drugs. Biofilm formation seems to be important in the persistence and relapse of infections such as bacterial endocarditis, artificial joint infections, and respiratory infections in individuals with cystic fibrosis.
Bacterial Adherence to Host Cells
Bacterial surface molecules that bind to host cells or extracellular matrix are called adhesins. Diverse surface structures are involved in adhesion of various bacteria (see Fig. 9.2). S. pyogenes has protein F and teichoic acid projecting from its cell wall that bind to fibronectin on the surface of host cells and in the extracellular matrix. Other bacteria have filamentous proteins called pili on their surfaces. Stalks of pili are structurally conserved, whereas amino acids on the tips of the pili vary and determine the binding specificity of the bacteria. Strains of E. coli that cause urinary tract infections uniquely express a specific P pilus that binds to a Gal(α1–4)Gal moiety expressed on uroepithelial cells. Pili on N. gonorrhoeae bacteria mediate adherence of the bacteria to host cells and also are targets of the host antibody response. Antigenic variation affecting the antigens expressed in the pili is an important mechanism by which N. gonorrhoeae escapes the immune response.
Bacterial Toxins
Any bacterial substance that contributes to illness can be considered a toxin. Toxins are subclassified as endotoxins, which are components of the bacterial cell, or exotoxins, which are proteins that are secreted by the bacterium.
Bacterial endotoxin is a lipopolysaccharide (LPS) that is a component of the outer membrane of gram-negative bacteria (see Fig. 9.2). LPS is composed of a long-chain fatty acid anchor, termed lipid A, connected to a core sugar chain, both of which are very similar in all gram-negative bacteria. Attached to the core sugar is a variable carbohydrate chain (O antigen), which is used to serotype strains of bacteria to aid in diagnosis. Lipid A binds to CD14 on the surface of host leukocytes, and the complex then binds to Toll-like receptor 4, a pattern recognition receptor of the innate immune system that transmits signals to promote cell activation and inflammatory responses. Responses to LPS can be both beneficial and harmful to the host. The response is beneficial in that LPS activates protective immunity through induction of important cytokines and chemoattractants (chemokines), as well as increased expression of costimulatory molecules, which enhance T-lymphocyte activation. However, high levels of LPS play an important role in septic shock, disseminated intravascular coagulation, and acute respiratory distress syndrome, mainly through induction of excessive levels of cytokines such as tumor necrosis factor (Chapter 4).
Exotoxins are secreted proteins that cause cellular injury and disease. They can be classified into broad categories by their mechanism and site of action.
• Enzymes. Bacteria secrete enzymes (proteases, hyaluronidases, coagulases, fibrinolysins) that act on their respective substrates in vitro, but their role in disease is understood in only a few cases. For example, exfoliative toxins are proteases produced by S. aureus that cleave proteins known to hold keratinocytes together, causing the epidermis to detach from the deeper skin.
• A-B toxins: Toxins that alter intracellular signaling or regulatory pathways. The two-component toxins have an active (A) component with enzymatic activity and a binding (B) component that binds cell surface receptors and delivers the A protein into the cell cytoplasm. The effect of these toxins depends on the binding specificity of the B domain and the cellular pathways affected by the A domain. A-B toxins are made by many bacteria including Bacillus anthracis, V. cholerae, and Corynebacterium diphtheriae. The mechanism of action of the A-B anthrax toxin is well understood (Fig. 9.8). Anthrax toxin has two alternate A components, edema factor (EF) and lethal factor (LF), which enter cells following binding to the B component, and each A component mediates specific pathologic effects.
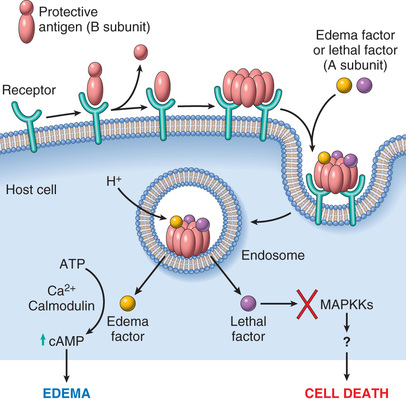
• Superantigens stimulate very large numbers of T lymphocytes by binding to conserved portions of the T cell receptor, leading to massive T lymphocyte proliferation and cytokine release. The high levels of cytokines lead to capillary leak and the systemic inflammatory response syndrome (Chapter 4). Superantigens made by S. aureus and S. pyogenes cause toxic shock syndrome.
• Neurotoxins produced by Clostridium botulinum and Clostridium tetani inhibit release of neurotransmitters, resulting in paralysis. These toxins do not kill neurons; instead, the A domains cleave proteins involved in secretion of neurotransmitters at the synaptic junction. Tetanus and botulism can result in death from respiratory failure due to paralysis of the chest and diaphragm muscles.
• Enterotoxins affect the gastrointestinal tract causing varied effects, including nausea and vomiting (S. aureus), voluminous watery diarrhea (V. cholerae), and bloody diarrhea (C. difficile).
Injurious Effects of Host Immune Responses
As mentioned earlier, the host immune response to microbes can sometimes be the cause of tissue injury. A few examples of types and mechanisms of injury are as follows:
• Granulomatous inflammation. Infection with M. tuberculosis results in a delayed hypersensitivity response and the formation of granulomas, which sequester the bacilli and prevent its spread, but also produce tissue damage (caseous necrosis) and fibrosis.
• T-cell–mediated inflammation. Damage from HBV and HCV infection of hepatocytes is due mainly to the immune response to the infected liver cells and not to cytopathic effects of the virus.
• Innate immune inflammation. Pattern recognition receptors bind to pathogen-associated molecular patterns (PAMPS) and to damage-associated molecular patterns (DAMPS) released from damaged host cells, activating the immune system and leading to inflammation (discussed in Chapter 5).
• Humoral immunity. Poststreptococcal glomerulonephritis can develop after infection with S. pyogenes. It is caused by antibodies that bind to streptococcal antigens and form immune complexes, which deposit in renal glomeruli and produce nephritis.
• Chronic inflammatory diseases. In the development of inflammatory bowel disease (Chapter 15), an important early event may be compromise of the intestinal epithelial barrier, which enables the entry of both pathogenic and commensal microbes and their interactions with local immune cells, resulting in inflammation. The cycle of inflammation and epithelial injury may be an important component of the disease, with microbes playing the central role.
• Cancer. Viruses, such as HBV and HCV, and bacteria, such as H. pylori, that are not known to carry or to activate oncogenes are associated with cancers, presumably because these microbes trigger chronic inflammation with subsequent tissue regeneration, which provides fertile ground for the development of cancer (Chapter 6).
Immune Evasion by Microbes
Humoral and cellular immune responses that protect the host from most infections are discussed in Chapter 5. Not surprisingly, microorganisms have developed many means to resist and evade the immune system (Fig. 9.9). These mechanisms of escaping the immune response are important determinants of microbial virulence and pathogenicity.
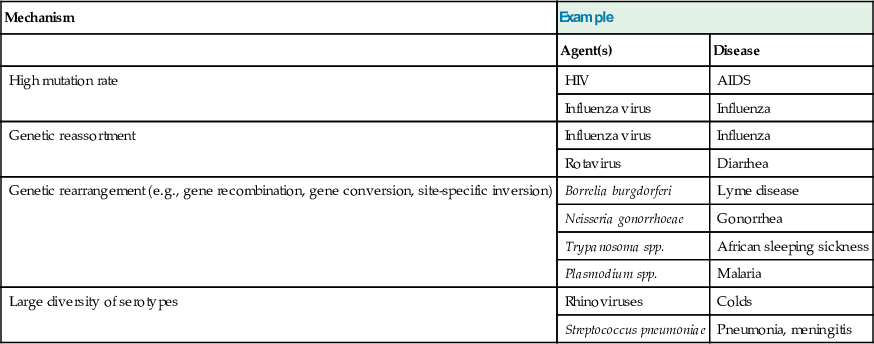
• Antigenic variation. Neutralizing antibodies against microbial antigens block the ability of microbes to infect cells and recruit immune cells to kill pathogens. To escape recognition, microbes use many strategies that involve genetic mechanisms for generating antigenic variation. The low fidelity of viral RNA polymerases (HIV and influenza virus) and reassortment of viral genomes (influenza viruses) create viral antigenic variation (Table 9.7). Borrelia species switch their surface antigens via gene rearrangement. Trypanosoma species have many genes for their major surface antigen, VSG, and vary the expression of this surface protein. There are more than 90 different serotypes of S. pneumoniae, each with a different capsular polysaccharide.
• Modification of surface proteins. Host cationic anti-microbial peptides, including defensins, cathelicidins, and thrombocidins, provide important initial defenses against invading microbes. These peptides bind the bacterial membrane and form pores, killing the bacterium by osmotic lysis. Bacterial pathogens (Shigella spp., S. aureus) avoid killing by making surface molecules that resist binding of anti-microbial peptides, or that inactivate or downregulate anti-microbial peptides.
• Overcoming antibodies and complement. Host defense includes coating of bacteria with antibodies or the complement protein C3b (opsonization) to facilitate phagocytosis by macrophages. However, the facultative intracellular pathogen M. tuberculosis subverts the complement response by activating the alternative complement pathway in the extracellular environment, and complement products coat the bacteria, resulting in uptake of the organism by monocytes; by this means, the organism reaches its site of replication. Many bacteria (such as Shigella, enteroinvasive E. coli, M. tuberculosis, M. leprae, S. enterica serotype Typhi) use the inside of cells as a “hideout” that allows them to escape from antibodies and complement. Listeria monocytogenes can manipulate the cell cytoskeleton to spread directly from cell to cell, thus allowing the bacteria to evade immune defenses.
• Resisting phagocytosis and bacterial killing in phagosomes. Phagocytosis and killing of bacteria by neutrophils and macrophages constitute a critical host defense against extracellular bacteria. The carbohydrate capsule on the surface of many bacteria that cause pneumonia or meningitis (S. pneumoniae, Neisseria meningitidis, H. influenzae) makes them more virulent by preventing phagocytosis of the organisms by neutrophils. Surface proteins that inhibit phagocytosis include proteins A (S. aureus) and M (S. pyogenes). Macrophages usually kill bacteria by fusion of the phagosome with the lysosome to form a phagolysosome. M. tuberculosis blocks fusion of the lysosome with the phagosome, allowing the bacteria to proliferate unchecked within the macrophage. Legionella produces a pore-forming protein called listeriolysin O and two phospholipases that degrade the phagosome membrane, allowing the bacteria to escape into the cytoplasm and avoid destruction in the macrophage. Legionella also secretes proteins that modulate small GTPases, master regulators of intracellular signaling to modify trafficking. Also, many bacteria make proteins that kill phagocytes, prevent their migration, or diminish their oxidative burst.
• Escaping the inflammasome. The activation of the cytosolic inflammasome is one pathway of innate immune responses to microbes. It is stimulated by microbial products and culminates in the activation of caspases, which induce the secretion of the pro-inflammatory cytokines IL-1 and IL-18 and induce a form of cell death called pyroptosis (Chapter 5). Both inflammation and cell death limit microbial virulence and replication. Some bacteria, such as Yersinia and Salmonella, express virulence proteins that inhibit the formation of the mature inflammasome, suppress caspase activation, block signaling pathways that are required for inflammasome activation, or limit the access of other bacterial proteins to the inflammasome. All these mechanisms serve to disable various components of this host anti-microbial defense reaction.
• Disruption of interferon pathways. Viruses have developed a large number of strategies to combat interferons (IFNs), which are mediators of early antiviral defense. Some viruses produce soluble homologues of IFN receptors that bind to and block the actions of secreted IFNs, or produce proteins that inhibit intracellular JAK/STAT signaling downstream of IFN receptors. RIG-I (RNA helicase retinoic acid inducible gene I protein) is a host cytoplasmic pattern recognition receptor for intracellular double-stranded RNA viruses. RIG-I inhibits signaling by this receptor, thus blocking the downstream IFN pathway and overcoming this host defense. Some viruses encode within their genomes homologs of cytokines, chemokines, or their receptors that act as competitive antagonists to inhibit immune responses. Finally, viruses have developed strategies to block apoptosis, which may give the viruses time to replicate, persist, or transform the infected host cell.
• Decreased T-cell recognition: DNA viruses (e.g., HSV, CMV, and EBV) can bind to or alter the localization of major histocompatibility complex (MHC) class I proteins, impairing peptide presentation to CD8+ cytotoxic T cells. Although downregulation of MHC class I molecules might cause virus-infected cells to be targets for NK cells, herpesviruses also express MHC class I homologuess that act as decoys that engage inhibitory receptors of NK cells. Herpesviruses can target MHC class II molecules for degradation, impairing antigen presentation to CD4+ helper T cells. Viruses also can infect leukocytes to directly compromise their function (e.g., HIV infects CD4+ T cells, macrophages, and dendritic cells).
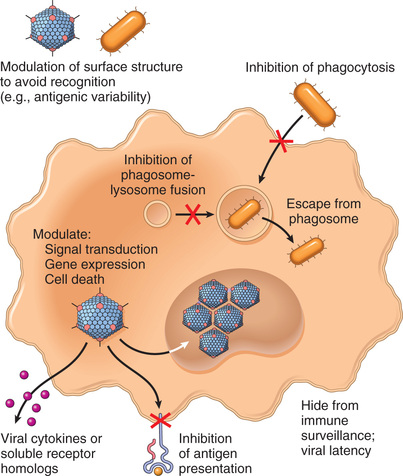
Table 9.7
Mechanisms of Anti-genic Variation
| Mechanism | Example | |
| Agent(s) | Disease | |
| High mutation rate | HIV | AIDS |
| Influenza virus | Influenza | |
| Genetic reassortment | Influenza virus | Influenza |
| Rotavirus | Diarrhea | |
| Genetic rearrangement (e.g., gene recombination, gene conversion, site-specific inversion) | Borrelia burgdorferi | Lyme disease |
| Neisseria gonorrhoeae | Gonorrhea | |
| Trypanosoma spp. | African sleeping sickness | |
| Plasmodium spp. | Malaria | |
| Large diversity of serotypes | Rhinoviruses | Colds |
| Streptococcus pneumoniae | Pneumonia, meningitis | |
Spectrum of Inflammatory Responses to Infection
In contrast with the vast molecular diversity of microbes, the morphologic patterns of tissue responses to microbes are limited, as are the mechanisms directing these responses. Therefore, many pathogens produce similar reaction patterns, and few features are unique to or pathognomonic for a particular microorganism, adding to the challenge in histopathologic diagnosis.
The interaction between the microbe and the host determines the histologic features of the response to the microbes. There are five major histologic patterns of tissue reaction in infections: suppurative, mononuclear/granulomatous, cytopathic-cytoproliferative, necrosis, and chronic inflammation/scarring. Suppurative inflammation is discussed in Chapter 3.
Mononuclear and Granulomatous Inflammation
Diffuse, predominantly mononuclear, interstitial infiltrates are a common feature of all chronic inflammatory processes, but sometimes they appear acutely in response to viruses, intracellular bacteria, or intracellular parasites. In addition, spirochetes and some helminths also provoke chronic inflammation. Eosinophilia can be prominent with some helminthic infections.
Cytopathic-Cytoproliferative Reaction
Cytopathic-cytoproliferative reactions usually are produced by viruses. The lesions are characterized by cell necrosis or cellular proliferation, usually with sparse inflammatory cells.
Tissue Necrosis
Clostridium perfringens and other organisms that secrete powerful toxins can cause such rapid and severe necrosis that tissue damage is the dominant feature.
Chronic Inflammation and Scarring
Many infections elicit chronic inflammation, which can either resolve with complete healing or lead to extensive scarring.
The patterns of tissue reactions described above are useful guidelines for analyzing microscopic features of infectious processes, but in practice it must be remembered that different types of host reactions often occur at the same time. For example, the lung of a patient with AIDS may be infected with CMV, which causes cytolytic changes, and, at the same time, by Pneumocystis, which causes interstitial inflammation. Similar patterns of inflammation also can be seen in tissue responses to physical or chemical agents and in other inflammatory conditions of unknown cause. Finally, in immunocompromised individuals, the absence of a host inflammatory response frequently eliminates some of the histologic clues about the potential nature of infecting microorganism(s). Because of this potential for mixed infections and/or lack of host response, other diagnostic tests for infection in addition to pathologic examination are essential to make a definitive diagnosis.
Infections in Individuals With Immunodeficiencies
Inherited or acquired defects in immunity (Chapter 5) often impair only part of the immune system, rendering the affected individuals susceptible to specific types of infections.
• Patients with antibody deficiency, as in X-linked agammaglobulinemia, contract severe bacterial infections by extracellular bacteria and a few viral infections (rotavirus and enteroviruses).
• Patients with T-cell defects are susceptible to infections with intracellular pathogens, notably viruses and some parasites.
• Patients with deficiencies in early complement components are particularly susceptible to infections by encapsulated bacteria, such as S. pneumoniae, whereas deficiencies of the late components of complement are associated with Neisseria infections.
• Deficiencies in neutrophil function lead to increased infections with S. aureus, some gram-negative bacteria, and fungi.
• Individuals with inherited deficiencies in specific components of innate and adaptive immunity sometimes show selective susceptibility to particular infections. These patterns reveal the essential roles of different molecules in mediating protective immunity to specific microorganisms. For example, patients with mutations in signaling molecules downstream of several TLRs are prone to pyogenic bacterial diseases, particularly with S. pneumoniae infections. Impaired TLR3 responses are associated with childhood HSV encephalitis. Inherited defects in IL-17 immunity (such as mutations in STAT3, a transcription factor needed for Th17 cell generation) are associated with chronic mucocutaneous candidiasis.
Acquired immunodeficiencies have a variety of causes, the most widely known being infection with HIV, which causes AIDS (Chapter 5). HIV infects and kills CD4+ helper T lymphocytes, leading to profound immunosuppression and a multitude of infections. Other causes of acquired immunodeficiency include infiltrative processes that suppress bone marrow function (e.g., leukemia), immunosuppressive drugs (such as those used to treat certain autoimmune diseases), and hemopoietic stem cell transplantation. Diseases of organ systems other than the immune system also can make patients susceptible to disease due to specific microorganisms. Individuals with cystic fibrosis and impaired respiratory clearance commonly get infections dominated by Pseudomonas aeruginosa. Lack of splenic function in individuals with sickle cell disease makes them susceptible to infection with encapsulated bacteria such as S. pneumoniae. Burns destroy skin, removing this barrier to microbes, allowing infection with pathogens such as P. aeruginosa. Finally, malnutrition impairs immune defenses.





