Oral Cavities and Gastrointestinal Tract
The gastrointestinal tract is a hollow tube consisting of the esophagus, stomach, small intestine, colon, rectum, and anus. Each region has unique, complementary, and highly integrated functions that together serve to regulate the intake, processing, and absorption of ingested nutrients and the disposal of waste products. The intestines also are the principal site at which the immune system interfaces with a diverse array of antigens present in food and gut microbes. Thus, it is not surprising that the small intestine and colon frequently are involved by infectious and inflammatory processes. Finally, the colon is the most common site of gastrointestinal neoplasia in Western populations. In this chapter, we discuss the diseases that affect each section of the gastrointestinal tract. Disorders that typically involve more than one segment, such as Crohn disease, are considered with the most frequently involved region. We begin our discussion with diseases of the oral cavity, since that is where the journey of food begins.
Oral Cavity
Pathologic conditions of the oral cavity can be broadly divided into diseases affecting teeth their support structures, oral mucosa, salivary glands, and jaws. Discussed next are the more common conditions affecting these sites. Odontogenic cysts and tumors (benign and malignant), which are derived from the epithelial and/or mesenchymal tissues associated with tooth development, are also discussed briefly.
Diseases of Teeth and Supporting Structures
Caries
Dental caries results from focal demineralization of tooth structure (enamel and dentin) caused by acids generated during the fermentation of sugars by bacteria. Worldwide, caries is the main cause of tooth loss before 35 years of age. The prevalence of caries used to be very high in developed countries where there is ready access to processed and refined foods containing large amounts of carbohydrates. However, the rate of caries has dropped markedly in countries such as the United States, where oral hygiene has improved and fluoridation of the drinking water is widespread. Fluoride is incorporated into the crystalline structure of enamel, forming fluoroapatite, which is resistant to degradation by bacterial acids. In contrast, with the globalization of the world's economy, processed foods are being increasingly consumed in developing nations; as a result, the rate of caries is increasing in these regions of the world.
Gingivitis
Inflammation involving the squamous mucosa, or gingiva, and associated soft tissues that surround teeth is defined as gingivitis. Poor oral hygiene, which facilitates buildup of dental plaque and calculus between and on the surfaces of teeth, is the most frequent cause of gingivitis. Dental plaque is a sticky biofilm composed of bacteria, salivary proteins, and desquamated epithelial cells. As it accumulates, plaque becomes mineralized to form calculus, or tartar. In chronic gingivitis, this is accompanied by gingival erythema, edema, and bleeding. Gingivitis may occur at any age but is most prevalent and severe in adolescence, where it is present in 40% to 60% of individuals, after which the incidence tapers off. Fortunately, gingivitis can be reversed, primarily by regular brushing and flossing of teeth which reduces accumulation of plaque and calculus.
Periodontitis
Periodontitis is an inflammatory process that affects the supporting structures of the teeth (periodontal ligaments), alveolar bone, and cementum. With progression, periodontitis may result in destruction of periodontal ligament and alveolar bone and eventual tooth loss. Periodontitis is associated with poor oral hygiene that affects the composition of gingival bacteria. Facultative Gram-positive organisms are found at healthy sites, while anaerobic and microaerophilic Gram-negative bacteria colonize plaque within areas of active periodontitis. Although about 300 bacterial species reside within the oral cavity, periodontitis is most closely associated with Aggregatibacter (Actinobacillus) actinomycetemcomitans, Porphyromonas gingivalis, and Prevotella intermedia.
Oral Inflammatory Lesions
Aphthous Ulcers (Canker Sores)
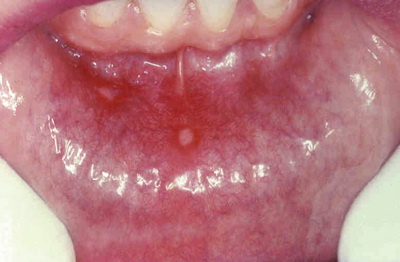
These common superficial mucosal ulcerations affect up to 40% of the population. They are more frequent in the first 2 decades of life, extremely painful, and often recur. Although the cause of aphthous ulcers is unknown, they tend to be familal and may be associated with celiac disease, inflammatory bowel disease, and Behçet disease. Ulcers can be solitary or multiple; typically, they are shallow, with a hyperemic base covered by a thin exudate and rimmed by a narrow zone of erythema (Fig. 15.1). In most cases they resolve spontaneously in 7 to 10 days but can recur.
Herpes Simplex Virus Infections
Herpes simplex virus causes a self-limited primary infection that can be reactivated when there is a compromise in host resistance. Most orofacial herpetic infections are caused by herpes simplex virus type 1 (HSV-1), with the remainder being caused by HSV-2 (genital herpes). With changing sexual practices, oral HSV-2 is becoming increasingly common. Primary infections typically occur in children between 2 and 4 years of age and are often asymptomatic. However, in 10% to 20% of cases the primary infection manifests as acute herpetic gingivostomatitis, with abrupt onset of vesicles and ulcerations throughout the oral cavity. Most adults harbor latent HSV-1, and the virus can be reactivated, resulting in a so-called “cold sore” or recurrent herpetic stomatitis. Factors associated with HSV reactivation include trauma, allergies, exposure to ultraviolet light and extremes of temperature, upper-respiratory tract infections, pregnancy, menstruation, and immunosuppression. Recurrent lesions, which occur at the site of primary inoculation or in adjacent mucosa innervated by the same ganglion, typically appear as groups of small (1- to 3-mm) vesicles. The lips (herpes labialis), nasal orifices, buccal mucosa, gingiva, and hard palate are the most common locations. Although lesions typically resolve within 7 to 10 days, they can persist in immunocompromised patients, who may require systemic anti-viral therapy. Morphologically, the lesions resemble those seen in esophageal herpes (see Fig. 15.8 later in the chapter) and genital herpes (Chapter 19). The infected cells become ballooned and have large eosinophilic intranuclear inclusions. Adjacent cells commonly fuse to form large multinucleated polykaryons.
Oral Candidiasis (Thrush)
Candidiasis is the most common fungal infection of the oral cavity. Candida albicans is a normal component of the oral flora and only produces disease under unusual circumstances. Predisposing factors include the following:
Broad-spectrum antibiotics that alter the normal microbiota can promote oral candidiasis. The three major clinical forms of oral candidiasis are pseudomembranous, erythematous, and hyperplastic. The pseudomembranous form is most common and is known as thrush. This condition is characterized by a superficial, curdlike, gray to white inflammatory membrane composed of matted organisms enmeshed in a fibrinosuppurative exudate that can be readily scraped off to reveal an underlying erythematous base. In mildly immunosuppressed or debilitated individuals, such as diabetics, the infection usually remains superficial, but it may spread to deep sites in association with more severe immunosuppression, that may be seen in organ or hematopoietic stem cell transplant recipients, and in patients with neutropenia, chemotherapy-induced immunosuppression, or AIDS.
Proliferative and Neoplastic Lesions of the Oral Cavity
Fibrous Proliferative Lesions
Fibromas are submucosal nodular fibrous tissue masses that are formed when chronic irritation results in reactive connective tissue hyperplasia (Fig. 15.2A). They occur most often on the buccal mucosa along the bite line. Treatment is complete surgical excision and removal of the source of irritation.
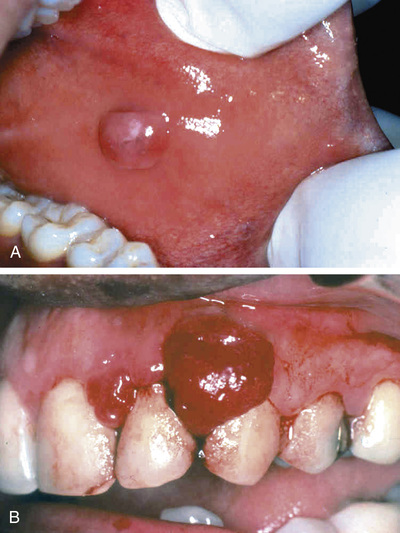
Pyogenic granuloma (Fig. 15.2B) is an inflammatory lesion typically found on the gingiva of children, young adults, and pregnant women (pregnancy tumor). These lesions are richly vascular and typically ulcerated, which gives them a red to purple color. In some cases, growth can be rapid and raise fear of a malignant neoplasm. However, histologic examination demonstrates a proliferation of immature vessels similar to that seen in granulation tissue. Pyogenic granulomas may regress, mature into dense fibrous masses, or develop into a peripheral ossifying fibroma. Complete surgical excision is definitive treatment.
Leukoplakia and Erythroplakia
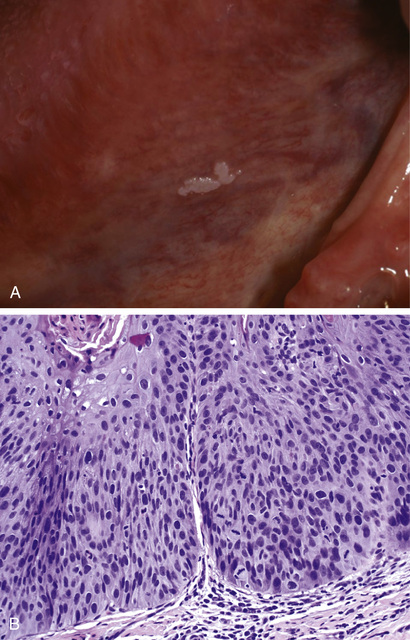
Leukoplakia is defined by the World Health Organization as “a white patch or plaque that cannot be scraped off and cannot be characterized clinically or pathologically as any other disease.” This description is reserved for lesions that arise in the oral cavity in the absence of any known cause (Fig. 15.3A). Accordingly, white patches caused by obvious irritation or entities such as lichen planus and candidiasis are not considered leukoplakia. Approximately 3% of the world's population has leukoplakic lesions, of which 5% to 25% are dsyplastic and at risk for progression to squamous cell carcinoma. Thus, until proved otherwise by means of histologic evaluation, all leukoplakias must be considered precancerous. A related but less common entity, erythroplakia, is a red, velvety, sometimes eroded lesion that is flat or slightly depressed relative to the surrounding mucosa. Erythroplakia is associated with a much greater risk for malignant transformation than leukoplakia. While leukoplakia and erythroplakia may be seen in adults at any age, they typically affect individuals between 40 and 70 years of age, with a 2:1 male predominance. Although the etiology is multifactorial, tobacco use (cigarettes, pipes, cigars, and chewing tobacco) is the most common risk factor for leukoplakia and erythroplakia.
Squamous Cell Carcinoma
Approximately 95% of cancers of the oral cavity are squamous cell carcinomas, with the remainder largely consisting of adenocarcinomas of salivary glands. Squamous cell carcinoma, an aggressive epithelial malignancy, is the sixth most common neoplasm in the world today. Despite numerous advances in treatment, the overall long-term survival rate has remained less than 50% for the past 50 years. This dismal outlook is due to several factors, in large part because oral cancer often is diagnosed at an advanced stage.
Multiple primary tumors may be present at initial diagnosis but more often are detected later, at an estimated rate of 3% to 7% per year; patients who survive 5 years after diagnosis of the initial tumor have up to a 35% chance of developing at least one new primary tumor within that interval. The development of these secondary tumors can be particularly devastating for individuals whose initial lesions were small. Therefore, surveillance and early detection of new premalignant lesions are critical for the long-term survival of patients with oral squamous cell carcinoma.
The elevated risk for development of additional primary tumors in these patients has led to the concept of “field cancerization.” This hypothesis suggests that multiple primary tumors develop independently as a result of years of chronic mucosal exposure to carcinogens such as alcohol or tobacco (described next).
Pathogenesis
Squamous cancers of the oropharynx arise through two distinct pathogenic pathways, one involving exposure to carcinogens, and the other related to infection with high risk variants of human papilloma virus (HPV). Carcinogen exposure mainly stems from chronic alcohol and tobacco (both smoked and chewed) use. In India and Southeast Asia, chewing of betel quid and paan are important predisposing factors. Betel quid is a “witch's brew” containing araca nut, slaked lime, and tobacco, all wrapped in betel nut leaf. It is likely that these tumors arise by a pathway similar to that characterized for tobacco use–associated tumors in the West. Deep sequencing of these cancers has revealed frequent mutations that bear a molecular signature consistent with exposure to carcinogens in tobacco. These mutations frequently involve TP53 and genes that regulate cell proliferation, such as RAS. The HPV-related tumors tend to occur in the tonsillar crypts or the base of the tongue and harbor oncogenic “high-risk” subtypes, particularly HPV-16. These tumors carry far fewer mutations than those associated with tobacco exposure and often overexpress p16, a cyclin-dependent kinase inhibitor.
It is conservatively predicted that the incidence of HPV-associated oropharyngeal squamous cell carcinoma will surpass that of cervical cancer by 2020, in part because the anatomic sites of origin—tonsillar crypts, base of tongue, and oropharynx—are not readily accessible or amenable to cytologic screening (unlike the cervix). The prognosis for patients with HPV-positive tumors is better than for those with HPV-negative tumors. The HPV vaccine, which is protective against cervical cancer, offers hope to limit the increasing frequency of HPV-associated oropharyngeal squamous cell carcinoma.
The incidence of oral cavity squamous cell carcinoma (particularly in the tongue) has been on the rise in individuals younger than 40 years of age who have no known risk factors. The pathogenesis in this group of patients, who are nonsmokers and are not infected with HPV, is unknown
Diseases of Salivary Glands
There are three major salivary glands—parotid, submandibular, and sublingual—as well as innumerable minor salivary glands distributed throughout the oral mucosa. Inflammatory or neoplastic disease may develop within any of these.
Xerostomia
Xerostomia is defined as a dry mouth resulting from a decrease in the production of saliva. Its incidence varies among populations but has been reported in more than 20% of individuals older than 70 years of age. It is a major feature of the autoimmune disorder Sjögren syndrome, in which it usually is accompanied by dry eyes (Chapter 5). A lack of salivary secretions is also a major complication of radiation therapy. However, xerostomia is most frequently observed as a side effect of many common classes of medications including anti-cholinergic, anti-depressant/anti-psychotic, diuretic, anti-hypertensive, sedative, muscle relaxant, analgesic, and anti-histaminic agents. The oral cavity may reveal only dry mucosa and/or atrophy of the papillae of the tongue, with fissuring and ulcerations, or, in Sjögren syndrome, concomitant inflammatory enlargement of the salivary glands. Complications of xerostomia include increased rates of dental caries and candidiasis, as well as difficulty in swallowing and speaking.
Sialadenitis
Inflammation of the salivary glands, referred to as sialadenitis, may be induced by trauma, viral or bacterial infection, or autoimmune disease. The most common form of viral sialadenitis is mumps, which may produce enlargement of all salivary glands but predominantly involves the parotids. Mumps produces interstitial inflammation marked by a mononuclear inflammatory infiltrate. While mumps in children is most often a self-limited benign condition, in adults it can cause pancreatitis or orchitis; the latter sometimes causes sterility.
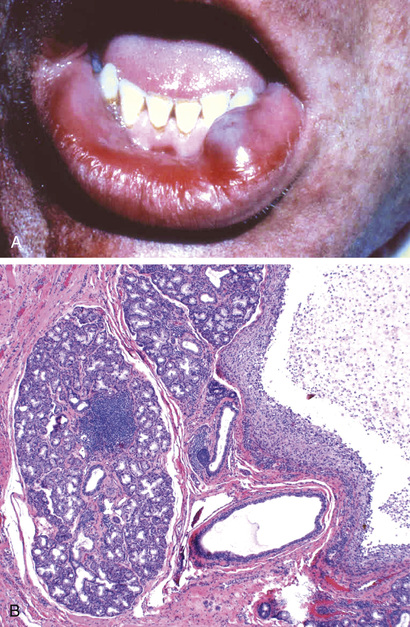
The mucocele is the most common inflammatory lesion of the salivay glands and results from either blockage or rupture of a salivary gland duct, with consequent leakage of saliva into the surrounding connective tissue stroma. Mucocele occurs most often in toddlers, young adults, and older adults, and typically manifests as a fluctuant swelling of the lower lip that may change in size, particularly in association with meals (Fig. 15.5A). Histologic examination demonstrates a cystlike space lined by granulation tissue or fibrous connective tissue that is filled with mucin and inflammatory cells, particularly macrophages (Fig. 15.5B). Complete excision of the cyst and the minor salivary gland constitutes definitive treatment.
Bacterial sialadenitis is a common infection that most often involves the major salivary glands, particularly the submandibular glands. The most frequent pathogens are Staphylococcus aureus and Streptococcus viridans. Duct obstruction by stones (sialolithiasis) is a common antecedent to infection; it may also be induced by impacted food debris or by edema consequent to injury. Dehydration and decreased secretory function can also predispose to bacterial invasion. Systemic dehydration, with decreased salivary secretions, may predispose to suppurative bacterial parotitis in older adult patients following major thoracic or abdominal surgery. Such obstruction and bacterial invasion lead to nonspecific inflammation of the affected glands that may be largely interstitial or, when induced by staphylococci or other pyogens, may be associated with suppurative necrosis and abscess formation.
Autoimmune sialadenitis, better known as Sjögren syndrome, is discussed in Chapter 5.
Neoplasms
Despite their relatively simple morphology, the salivary glands give rise to at least 30 histologically distinct tumors (Table 15.1). A small number of these neoplasms account for more than 90% of tumors. Overall, salivary gland tumors are relatively uncommon and represent less than 2% of all human tumors. Approximately 65% to 80% arise within the parotid, 10% in the submandibular gland, and the remainder in the minor salivary glands, including the sublingual glands. Approximately 15% to 30% of tumors in the parotid glands are malignant. By contrast, approximately 40% of submandibular, 50% of minor salivary gland, and 70% to 90% of sublingual tumors are cancerous. Thus, the likelihood that a salivary gland tumor is malignant is inversely proportional, roughly, to the size of the gland.
Table 15.1
Histopathologic Classification and Prevalence of the Most Common Benign and Malignant Salivary Gland Tumors
| Benign | Malignant |
| Pleomorphic adenoma (50%) | Mucoepidermoid carcinoma (15%) |
| Warthin tumor (5%) | Acinic cell carcinoma (6%) |
| Oncocytoma (2%) | Adenocarcinoma NOS (6%) |
| Cystadenoma (2%) | Adenoid cystic carcinoma (4%) |
| Basal cell adenoma (2%) | Malignant mixed tumor (3%) |
Salivary gland tumors usually occur in adults, with a slight female predominance, but about 5% occur in children younger than 16 years of age. Whatever the histologic pattern, parotid gland neoplasms produce swelling in front of and below the ear. Benign tumors may be present for months to several years before coming to clinical attention, while cancers more often come to attention promptly, probably because of their more rapid growth. However, there are no reliable criteria to differentiate benign from malignant lesions on clinical grounds, and histopathologic evaluation is essential.
Pleomorphic Adenoma
Pleomorphic adenomas are benign tumors that consist of a mixture of ductal (epithelial) and myoepithelial cells, so they exhibit both epithelial and mesenchymal differentiation. Epithelial elements are dispersed throughout the matrix, which may contain variable mixtures of myxoid, hyaline, chondroid (cartilaginous), and even osseous tissue. In some pleomorphic adenomas, the epithelial elements predominate; in others, they are present only in widely dispersed foci. This histologic diversity has given rise to the alternative, albeit less preferred, name mixed tumor.
Pleomorphic adenomas represent about 60% of tumors in the parotid, are less common in the submandibular glands, and are relatively rare in the minor salivary glands. They present as slow-growing, painless, mobile discrete masses. They recur if incompletely excised. Recurrence rates approach 25% after simple enucleation of the tumor, but are only 4% after wider resection. In both settings, recurrence stems from a failure to recognize minute extensions of tumor into surrounding soft tissues.
Carcinoma arising in a pleomorphic adenoma is referred to variously as a carcinoma ex pleomorphic adenoma or malignant mixed tumor. The incidence of malignant transformation increases with time from 2% of tumors present for less than 5 years to almost 10% for those present for more than 15 years. The cancer usually takes the form of an adenocarcinoma or undifferentiated carcinoma. Unfortunately, these are among the most aggressive malignant neoplasms of salivary glands, with mortality rates of 30% to 50% at 5 years.
Mucoepidermoid Carcinoma
Mucoepidermoid carcinomas are composed of variable mixtures of squamous cells, mucus-secreting cells, and intermediate cells. These neoplasms represent about 15% of all salivary gland tumors, and while they occur mainly (60%–70%) in the parotids, they account for a large fraction of salivary gland neoplasms in the other glands, particularly the minor salivary glands. Overall, mucoepidermoid carcinoma is the most common form of primary malignant tumor of the salivary glands.
Clinical course and prognosis depend on histologic grade. Low-grade tumors may invade locally and recur in about 15% of cases but metastasize only rarely and afford a 5-year survival rate of over 90%. By contrast, high-grade neoplasms and, to a lesser extent, intermediate-grade tumors are invasive and difficult to excise. As a result, they recur in 25% to 30% of cases, and about 30% metastasize to distant sites. The 5-year survival rate is only 50%.
Odontogenic Cysts and Tumors
Odontogenic cysts usually are derived from remnants of odontogenic epithelium present within the jaws. In contrast to the rest of the skeleton, epithelium-lined cysts are quite common in the jaws. These cysts are subclassified as either inflammatory or developmental. Only the most common lesions are considered here, starting with developmental cysts.
The dentigerous cyst originates around the crown of an unerupted tooth and is thought to be the result of degeneration of the dental follicle (primordial tissue that makes the enamel surface of teeth). They are lined by a thin, stratified squamous epithelium that typically is associated with a dense chronic inflammatory infiltrate in the underlying connective tissue. Complete removal is curative.
Odontogenic keratocysts can occur at any age but are most frequent in individuals between 10 and 40 years of age, have a male predominance, and typically are located within the posterior mandible. Differentiation of the odontogenic keratocyst from other odontogenic cysts is important because it is locally aggressive and has a high recurrence rate. On histologic examination, the cyst lining consists of a thin layer of parakeratinized or orthokeratinized stratified squamous epithelium with a prominent basal cell layer and a corrugated luminal epithelial surface. Treatment requires aggressive and complete removal; recurrence rates of up to 60% are associated with inadequate resection.
In contrast with the developmental cysts just described, the periapical cyst has an inflammatory etiology. These extremely common lesions occur at the tooth apex as a result of long-standing pulpitis, which may be caused by advanced caries or trauma. Necrosis of the pulpal tissue, which can traverse the length of the root and exit the apex of the tooth into the surrounding alveolar bone, can lead to a periapical abscess. Over time, granulation tissue (with or without an epithelial lining) may develop. Periapical inflammatory lesions persist as a result of bacterial infection or necrotic tissue in the area. Successful treatment, therefore, necessitates the complete removal of the offending material followed by restoration or extraction of the tooth.
Odontogenic tumors are a complex group of lesions with diverse histologic appearances and clinical behaviors. Some are true neoplasms, either benign or malignant, while others are thought to be hamartomas. Odontogenic tumors are derived from odontogenic epithelium, ectomesenchyme, or both. The two most common and clinically significant tumors are ameloblastoma and odontoma.
Ameloblastomas arise from odontogenic epithelium. They are typically cystic, slow-growing and, despite being locally invasive, have an indolent course. The cysts are lined by palisading columnar epithelium that overlies a loose stroma with stellate cells. Odontoma, the most common type of odontogenic tumor, arises from epithelium but shows extensive deposition of enamel and dentin. Odontomas are cured by local excision.
Esophagus
The esophagus develops from the cranial portion of the foregut. It is a hollow, highly distensible muscular tube that extends from the epiglottis to the gastroesophageal junction, located just above the diaphragm. Acquired diseases of the esophagus run the gamut from lethal cancers to the persistent “heartburn” of gastroesophageal reflux that may be chronic and incapacitating or merely an occasional annoyance.
Obstructive and Vascular Diseases
Mechanical Obstruction
Atresia, fistulas, and duplications may occur in any part of the gastrointestinal tract. When they involve the esophagus, they are discovered shortly after birth, usually because of regurgitation during feeding. Prompt surgical repair is required. Absence, or agenesis, of the esophagus is extremely rare. Atresia, in which a thin, noncanalized cord replaces a segment of esophagus, is more common. It occurs most frequently at or near the tracheal bifurcation and usually is associated with a fistula connecting the upper or lower esophageal pouches to a bronchus or the trachea. This abnormal connection can result in aspiration, suffocation, pneumonia, or severe fluid and electrolyte imbalances.
Esophageal stenosis may be congenital or more commonly acquired. When acquired the narrowing generally is caused by fibrous thickening of the submucosa and atrophy of the muscularis propria. Stenosis due to inflammation and scarring may be caused by chronic gastroesophageal reflux, irradiation, ingestion of caustic agents, or other forms of severe injury. Stenosis-associated dysphagia usually is progressive; difficulty eating solids typically occurs long before problems with liquids.
Functional Obstruction
Efficient delivery of food and fluids to the stomach requires coordinated waves of peristaltic contractions. Esophageal dysmotility interferes with this process and can take several forms, all of which are characterized by discoordinated contraction or spasm of the muscularis. Because it increases esophageal wall stress, spasm also can cause small diverticula to form. Esophageal dysmotility can be separated into several forms depending on the character of the contractile abnormalities.
Achalasia is characterized by the triad of incomplete lower esophageal sphincter (LES) relaxation, increased LES tone, and esophageal aperistalsis. Primary achalasia is caused by failure of distal esophageal inhibitory neurons and is, by definition, idiopathic. Degenerative changes in neural innervation, either intrinsic to the esophagus or within the extraesophageal vagus nerve or the dorsal motor nucleus of the vagus, may lead to secondary achalasia. This occurs in Chagas disease, in which Trypanosoma cruzi infection causes destruction of the myenteric plexus, failure of LES relaxation, and esophageal dilatation. Duodenal, colonic, and ureteric myenteric plexuses also can be affected in Chagas disease. Achalasia-like disease may be caused by diabetic autonomic neuropathy, infiltrative disorders such as malignancy, amyloidosis, or sarcoidosis, and lesions of dorsal motor nuclei, which may be produced by polio or surgical ablation.
Ectopia
Ectopic tissues (developmental rests) are common in the gastrointestinal tract. The most frequent site of ectopic gastric mucosa is the upper third of the esophagus, where it is referred to as an inlet patch. Although the presence of such tissue generally is asymptomatic, acid released by gastric mucosa within the esophagus can result in dysphagia, esophagitis, Barrett esophagus, or, rarely, adenocarcinoma. Gastric heterotopia, small patches of ectopic gastric mucosa in the small bowel, particularly within a Meckel diverticulum, or colon, may present with occult blood loss due to local injury caused by acid secretion.
Esophageal Varices
Instead of returning directly to the heart, venous blood from the gastrointestinal tract is delivered to the liver via the portal vein before reaching the inferior vena cava. This circulatory pattern is responsible for the first-pass effect, in which drugs and other materials absorbed in the intestines are processed by the liver before entering the systemic circulation. Diseases that impede portal blood flow cause portal hypertension, which can lead to the development of esophageal varices, an important cause of massive and frequently life-threatening bleeding.
Pathogenesis
One of the few sites where the splanchnic and systemic venous circulations can communicate is the esophagus. Portal hypertension induces development of collateral channels that allow portal blood to shunt into the caval system. However, these collateral veins enlarge the subepithelial and submucosal venous plexi within the distal esophagus. These vessels, termed varices, develop in 50% of cirrhotic patients, most commonly in association with alcoholic liver disease. Worldwide, hepatic schistosomiasis is the second most common cause of varices. A more detailed consideration of portal hypertension is given in Chapter 16.
Clinical Features
Varices often are asymptomatic, but their rupture can lead to massive hematemesis and death. Variceal rupture therefore constitutes a medical emergency. Despite intervention, as many as half of the patients die from the first bleeding episode, either as a direct consequence of hemorrhage or due to hepatic coma triggered by the protein load that results from intraluminal bleeding as well as hypovolemic shock. Among those who survive, additional episodes of hemorrhage, each potentially fatal, occur in as many as 20% of cases.
Esophagitis
Esophageal Lacerations, Mucosal Injury, and Infections
The most common esophageal lacerations are Mallory- Weiss tears, which are often induced by severe retching or vomiting. Normally, a reflex relaxation of the gastroesophageal musculature precedes the anti-peristaltic contractile wave associated with vomiting. This relaxation may fail during prolonged vomiting, with the result that refluxing gastric contents cause the esophageal wall to stretch and tear. Patients usually present with hematemesis.
The roughly linear lacerations of Mallory-Weiss syndrome are longitudinally oriented and usually cross the gastroesophageal junction (Fig. 15.8A). These superficial tears generally heal quickly without surgical intervention. By contrast, severe, transmural esophageal tears (Boerhaave syndrome) result in mediastinitis, are catastrophic, and require prompt surgical intervention.
Chemical and Infectious Esophagitis
The stratified squamous mucosa of the esophagus may be damaged by a variety of irritants including alcohol, corrosive acids or alkalis, excessively hot fluids, and heavy smoking. Medicinal pills, most commonly doxycycline and bisphosphonates, may adhere to the esophageal lining and dissolve in the esophagus rather than passing immediately into the stomach, resulting in pill-induced esophagitis. Esophagitis due to chemical injury generally causes only self-limited pain, particularly odynophagia (pain with swallowing). Hemorrhage, stricture, or perforation may occur in severe cases. Iatrogenic esophageal injury may be caused by cytotoxic chemotherapy, radiation therapy, or graft-versus-host disease. The morphologic changes are nonspecific, consisting of ulceration and acute inflammation. Irradiation causes blood vessel damage adding an element of ischemic injury.
Infectious esophagitis may occur in otherwise healthy individuals but is most frequent in those who are debilitated or immunosuppressed. In these patients, esophageal infection by herpes simplex viruses, cytomegalovirus (CMV), or fungal organisms is common. Among fungi, Candida is the most common pathogen, although mucormycosis and aspergillosis may also occur. The esophagus may also be involved in desquamative skin diseases such as bullous pemphigoid and epidermolysis bullosa and, rarely, Crohn disease.
Infection by fungi or bacteria can be primary or complicate a preexisting ulcer. Nonpathogenic oral bacteria frequently are found in ulcer beds, while pathogenic organisms, which account for about 10% of infectious esophagitis cases, may invade the lamina propria and cause necrosis of overlying mucosa. Candidiasis in its most advanced form is characterized by adherent, gray-white pseudomembranes composed of densely matted fungal hyphae and inflammatory cells covering the esophageal mucosa.
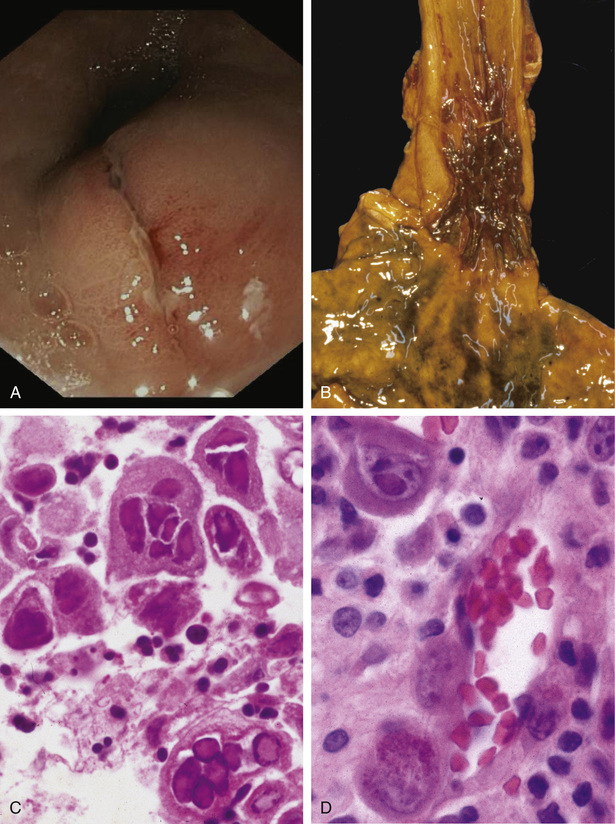
The endoscopic appearance often provides a clue to the identity of the infectious agent in viral esophagitis. Herpesviruses typically cause punched-out ulcers (Fig. 15.8B), and histopathologic analysis demonstrates nuclear viral inclusions within a rim of degenerating epithelial cells at the ulcer edge (Fig. 15.8C). By contrast, CMV causes shallower ulcerations. Biopsy of these lesions show the characteristic nuclear and cytoplasmic inclusions within capillary endothelium and stromal cells (Fig. 15.8D). Immunohistochemical staining for viral antigens can be a useful ancillary diagnostic tool.
Reflux Esophagitis
Reflux of gastric contents into the lower esophagus is the most frequent cause of esophagitis and the most common gastrointestinal ailment with which patients present in the out patient setting in the United States. The associated clinical condition is termed gastroesophageal reflux disease (GERD). The stratified squamous epithelium of the esophagus is resistant to abrasion from foods but is sensitive to acid. The submucosal glands of the proximal and distal esophagus contribute to mucosal protection by secreting mucin and bicarbonate. More important, high lower esophageal sphincter tone protects against reflux of acidic gastric contents, which are under positive pressure.
Pathogenesis
Reflux of gastric juices is central to the development of mucosal injury in GERD. In severe cases, duodenal bile reflux may exacerbate the damage. Conditions that decrease lower esophageal sphincter tone or increase abdominal pressure contribute to GERD and include alcohol and tobacco use, obesity, central nervous system depressants, pregnancy, hiatal hernia (discussed later), delayed gastric emptying, and increased gastric volume. In many cases, no definitive cause is identified.
Clinical Features
GERD is most common in those over 40 years of age but also occurs in infants and children. The most frequently reported symptoms are heartburn, dysphagia, and, less often, noticeable regurgitation of sour-tasting gastric contents. Rarely, chronic GERD is punctuated by attacks of severe chest pain that may be mistaken for heart disease. Treatment with proton pump inhibitors reduces gastric acidity and typically provides symptomatic relief. While the severity of symptoms is not closely related to the degree of histologic damage, the latter tends to increase with disease duration. Complications of reflux esophagitis include esophageal ulceration, hematemesis, melena, stricture development, and Barrett esophagus, a precursor lesion to esophageal carcinoma.
Hiatal hernia is characterized by separation of the diaphragmatic crura and protrusion of the stomach into the thorax through the resulting gap. Congenital hiatal hernias are recognized in infants and children, but many are acquired in later life. Hiatal hernia is symptomatic in fewer than 10% of adults; symptoms when present resemble GERD since hiatal hernia can cause LES incompetence.
Eosinophilic Esophagitis
Eosinophilic esophagitis is a chronic immunologically mediated disorder that is being increasingly recognized. Symptoms include food impaction and dysphagia in adults and feeding intolerance or GERD-like symptoms in children. The cardinal histologic feature is epithelial infiltration by large numbers of eosinophils, particularly superficially (Fig. 15.9B) and at sites far from the gastroesophageal junction. Their abundance can help to differentiate eosinophilic esophagitis from GERD, Crohn disease, and other causes of esophagitis. Endoscopically evident rings in the upper and mid portions of the esophagus (Fig. 15.9C), may also help to distinguish eosinophilic esophagitis from GERD. Patients with eosinophilic esophagitis are typically refractory to high-dose proton pump inhibitor treatment. Most patients are atopic, and many have atopic dermatitis, allergic rhinitis, asthma, or modest peripheral eosinophilia. Treatments include dietary restrictions to prevent exposure to food allergens, such as cow milk and soy products, and topical or systemic corticosteroids.
Barrett Esophagus
Barrett esophagus is a complication of chronic GERD that is characterized by intestinal metaplasia within the esophageal squamous mucosa. The incidence of Barrett esophagus is rising; it is estimated to occur in as many as 10% of individuals with symptomatic GERD. White males are affected most often and typically present between 40 and 60 years of age. The greatest concern in Barrett esophagus is that it confers an increased risk for development of esophageal adenocarcinoma. Molecular studies suggest that Barrett epithelium may be more similar genetically to adenocarcinoma than to normal esophageal epithelium, consistent with the view that Barrett esophagus is a direct precursor of cancer. In keeping with this, epithelial dysplasia, considered to be a preinvasive lesion, develops in 0.2% to 1% of individuals with Barrett esophagus each year; its incidence increases with duration of symptoms and increasing patient age. Although the vast majority of esophageal adenocarcinomas are associated with Barrett esophagus, it should be noted that most individuals with Barrett esophagus do not develop esophageal cancer.
Clinical Features
Diagnosis of Barrett esophagus is usually prompted by GERD symptoms and requires endoscopy and biopsy. The best course of management is a matter of debate, but most clinicians recommend periodic surveillance endoscopy with biopsy to screen for dysplasia. Dysplasia is often treated and more advanced lesions, including high-grade dysplasia and intramucosal carcinoma, always require therapeutic intervention. Available modalities include surgical resection (esophagectomy); newer approaches include photodynamic therapy, radiofrequency ablation, and endoscopic mucosectomy.
Esophageal Tumors
Two morphologic variants account for a majority of esophageal cancers: adenocarcinoma and squamous cell carcinoma. Worldwide, squamous cell carcinoma is more common, but adenocarcinoma is on the rise. Other rare tumors are not discussed here.
Adenocarcinoma
Esophageal adenocarcinoma typically arises in a background of Barrett esophagus and long-standing GERD. Risk for development of adenocarcinoma is greater in patients with documented dysplasia and in those who use tobacco, are obese, or who have had previous radiation therapy. In the United States, esophageal adenocarcinoma occurs most frequently in whites and shows a strong gender bias, being seven times more common in men than in women. However, the incidence varies by a factor of 60-fold worldwide, with rates being highest in Western countries, including the United States, the United Kingdom, Canada, Australia, and the Netherlands, and lowest in Korea, Thailand, Japan, and Ecuador. In countries where esophageal adenocarcinoma is more common, the incidence has increased markedly since 1970, more rapidly than for almost any other cancer. As a result, esophageal adenocarcinoma, which represented less than 5% of esophageal cancers before 1970, now accounts for half of all esophageal cancers in some Western countries, including the United States.
Pathogenesis
Molecular studies suggest that the progression of Barrett esophagus to adenocarcinoma occurs over an extended period through the stepwise acquisition of genetic and epigenetic changes. This model is supported by the observation that epithelial clones identified in nondysplastic Barrett metaplasia persist and accumulate mutations during progression to dysplasia and invasive carcinoma. Chromosomal abnormalities and TP53 mutation are often present in the early stages of esophageal adenocarcinoma. Additional genetic changes and inflammation are thought to contribute to tumor progression.
Clinical Features
Patients most commonly present with pain or difficulty in swallowing, progressive weight loss, chest pain, or vomiting. By the time signs and symptoms appear, the tumor usually has invaded submucosal lymphatic vessels. As a result of the advanced stage at diagnosis, the overall 5-year survival rate is less than 25%. By contrast, 5-year survival approximates 80% in the few patients with adenocarcinoma limited to the mucosa or submucosa.
Squamous Cell Carcinoma
In the United States, esophageal squamous cell carcinoma typically occurs in adults older than 45 years of age and affects males four times more frequently than females. Risk factors include alcohol and tobacco use, poverty, caustic esophageal injury, achalasia, Plummer-Vinson syndrome, frequent consumption of very hot beverages, and previous radiation therapy to the mediastinum. It is nearly six times more common in African Americans than in whites—a striking risk disparity that cannot be accounted for by differences in rates of alcohol and tobacco use. The incidence of esophageal squamous cell carcinoma can vary by more than 100-fold between and within countries, being more common in rural and underdeveloped areas. The countries with highest incidences are Iran, central China, Hong Kong, Argentina, Brazil, and South Africa.
Pathogenesis
A majority of esophageal squamous cell carcinomas in Europe and the United States are at least partially related to the use of alcohol and tobacco, the effects of which synergize to increase risk. However, esophageal squamous cell carcinoma also is common in some regions where alcohol and tobacco use are uncommon due to religious or societal norms. In these areas, nutritional deficiencies, as well as exposure to polycyclic hydrocarbons, nitrosamines, and other mutagenic compounds, such as those found in fungus-contaminated foods, are suspected to be the risk factors. HPV infection also has been implicated in esophageal squamous cell carcinoma in high-risk but not in low-risk regions. The molecular pathogenesis of esophageal squamous cell carcinoma remains incompletely defined.
Clinical Features
Clinical manifestations of squamous cell carcinoma of the esophagus begin insidiously and include dysphagia, odynophagia (pain on swallowing), and obstruction. As with other forms of esophageal obstruction, patients may unwittingly adjust to the progressively increasing obstruction by altering their diet from solid to liquid foods. Extreme weight loss and debilitation may occur as consequences of both impaired nutrition and tumor-associated cachexia. As with adenocarcinoma, hemorrhage and sepsis may accompany tumor ulceration. Occasionally, squamous cell carcinomas of the upper and mid esophagus present with symptoms caused by aspiration of food via a tracheoesophageal fistula.
Increased use of endoscopic screening has led to earlier diagnosis of esophageal squamous cell carcinoma. Early detection is critical, because 5-year survival rates are 75% for patients with superficial esophageal carcinoma but much lower for patients with more advanced tumors. The overall 5-year survival rate remains a dismal 9%.
Stomach
Disorders of the stomach are a frequent cause of clinical disease, with inflammatory and neoplastic lesions being particularly common. In the United States, symptoms related to gastric acidity account for nearly one third of all health care spending on gastrointestinal disease. In addition, despite a decreasing incidence in certain locales, including the United States, gastric cancer remains a leading cause of death worldwide.
The stomach is divided into four major anatomic regions: the cardia, fundus, body, and antrum. The cardia is lined mainly by mucin-secreting foveolar cells that form shallow glands. The antral glands are similar but also contain endocrine cells, such as G cells, that release gastrin to stimulate luminal acid secretion by parietal cells within the gastric fundus and body. The well-developed glands of the body and fundus also contain chief cells that produce and secrete digestive enzymes such as pepsin.
Gastropathy and Acute Gastritis
Gastritis results from mucosal injury. When neutrophils are present, the lesion is referred to as acute gastritis. When cell injury and regeneration are present but inflammatory cells are rare or absent, the term gastropathy is applied. Agents that cause gastropathy include nonsteroidal anti-inflammatory drugs, alcohol, bile, and stress-induced injury. Acute mucosal erosion or hemorrhage, such as Curling ulcers or lesions following disruption of gastric blood flow, for example, in portal hypertension, can also cause gastropathy that typically progresses to gastritis. The term hypertrophic gastropathy is applied to a specific group of diseases exemplified by Ménétrier disease and Zollinger-Ellison syndrome (discussed later).
Both gastropathy and acute gastritis may be asymptomatic or cause variable degrees of epigastric pain, nausea, and vomiting. In more severe cases, there may be mucosal erosion, ulceration, hemorrhage, hematemesis, melena, or, rarely, massive blood loss.
Pathogenesis
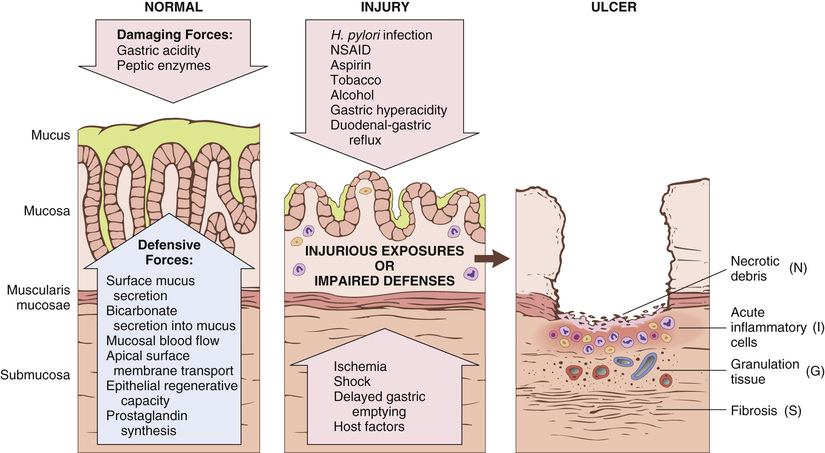
The gastric lumen is strongly acidic, with a pH close to 1—more than 1 million times more acidic than the blood. This harsh environment contributes to digestion but also has the potential to damage the mucosa. Multiple mechanisms have evolved to protect the gastric mucosa (Fig. 15.13). Mucin secreted by surface foveolar cells forms a thin layer of mucus that prevents large food particles from directly touching the epithelium. The mucus layer also promotes formation of an “unstirred” layer of fluid over the epithelium that protects the mucosa; it has a neutral pH as a result of secretion of bicarbonate ions by surface epithelial cells. Finally, the rich blood supply of the gastric mucosa efficiently buffers and removes protons that back-diffuse into the lamina propria. Gastropathy, acute gastritis, and chronic gastritis can occur after disruption of any of these protective mechanisms. The main causes include:
• Nonsteroidal anti-inflammatory drugs (NSAIDs) inhibit cyclooxygenase (COX)-dependent synthesis of prostaglandins E2 and I2, which stimulate nearly all of the above defense mechanisms including mucus and bicarbonate secretion, mucosal blood flow, and epithelial restitution. Although COX-1 plays a larger role than COX-2, both isoenzymes contribute to mucosal protection. Thus, while the risk for development of NSAID-induced gastric injury is greatest with nonselective inhibitors, such as aspirin, ibuprofen, and naproxen, selective COX-2 inhibition, for example, by celecoxib, can also result in gastropathy or gastritis.
• The gastric injury that occurs in uremic patients and those infected with urease-secreting H. pylori may be due to inhibition of gastric bicarbonate transporters by ammonium ions.
• Reduced mucin and bicarbonate secretion have been suggested as factors that explain the increased susceptibility of older adults to gastritis.
• Hypoxemia and decreased oxygen delivery may account for an increased incidence of gastropathy and acute gastritis at high altitudes.
• Ingestion of harsh chemicals, particularly acids or bases, either accidentally or in a suicide attempt, leads to severe gastric mucosal damage as a result of direct injury to epithelial and stromal cells. Direct cellular damage also contributes to gastritis induced by excessive alcohol consumption, NSAID use, and radiation therapy. Agents that inhibit DNA synthesis or the mitotic apparatus, including those used in cancer chemotherapy, may cause generalized mucosal damage due to insufficient epithelial renewal.
Stress-Related Mucosal Disease
Stress-related gastric injury occurs in patients with severe trauma, extensive burns, intracranial disease, major surgery, serious medical disease, and other forms of severe physiologic stress. More than 75% of critically ill patients develop endoscopically visible gastric lesions during the first 3 days of their illness. In some cases, the associated ulcers are given specific names based on location and clinical associations. Examples are as follows:
• Stress ulcers affecting critically ill patients with shock, sepsis, or severe trauma.
• Curling ulcers occur in the proximal duodenum and are associated with severe burns or trauma.
• Cushing ulcers arise in the stomach, duodenum, or esophagus of those with intracranial disease and have a high incidence of perforation.
Pathogenesis
The pathogenesis of stress-related gastric mucosal injury is most often due to local ischemia. This may be caused by systemic hypotension or reduced blood flow resulting from stress-induced splanchnic vasoconstriction. Upregulation and increased release of the vasoconstrictor endothelin-1 also contributes to ischemic gastric mucosal injury, while increased COX-2 expression appears to be protective. Cushing ulcers are thought to be caused by direct stimulation of vagal nuclei resulting acid hypersecretion. Systemic acidosis may also contribute to mucosal injury by lowering the intracellular pH of mucosal cells.
Clinical Features
Most critically ill patients admitted to hospital intensive care units have histologic evidence of gastric mucosal damage. Ulcers are associated with nausea, vomiting, melena, and coffee-ground hematemesis. Bleeding from superficial gastric erosions or ulcers that may require transfusion develop in 1% to 4% of these patients. Other complications, including perforation, also may occur. Prophylaxis with proton pump inhibitors may blunt the impact of stress ulceration, but the most important determinant of outcome is the severity of the underlying condition.
Chronic Gastritis
The most common cause of chronic gastritis is infection with the bacillus Helicobacter pylori. Autoimmune gastritis, typically associated with gastric atrophy, represents less than 10% of cases of chronic gastritis but is the most common cause in patients without H. pylori infection. Chronic NSAID use is a third important cause of gastritis in some populations, as discussed later. Less common causes include radiation injury and chronic bile reflux.
The signs and symptoms associated with chronic gastritis typically are less severe but more persistent than those of acute gastritis. Nausea and upper-abdominal discomfort may occur, sometimes with vomiting, but hematemesis is uncommon.
Helicobacter pylori Gastritis
The discovery of the association of H. pylori with peptic ulcer disease revolutionized the understanding of chronic gastritis. These spiral-shaped or curved bacilli are present in gastric biopsy specimens from almost all patients with duodenal ulcers and a majority of those with gastric ulcers or chronic gastritis. Acute H. pylori infection is subclinical in most cases; rather, it is the chronic gastritis that ultimately brings the afflicted person to medical attention. H. pylori infection most often presents as an antral gastritis with increased acid production. The increased acid production may give rise to peptic ulcer disease of the duodenum or stomach.
While in most cases H. pylori gastritis is limited to the antrum, in some individuals it progresses to involve the gastric body and fundus, resulting in reduced parietal cell mass and acid secretion. Reduced acid output results in hypergastrinemia, as in autoimmune atrophic gastritis. In addition, extension of the gastritis to the gastric body and fundus results in intestinal metaplasia and increased risk of gastric cancer.
Epidemiology
In the United States, H. pylori infection is associated with poverty, household crowding, limited education, residence in areas with poor sanitation, and birth outside of the United States. Infection is typically acquired in childhood and may then persist for life. Improved sanitation in many areas likely explains why H. pylori infection rates among younger individuals today are markedly lower than they were in similarly aged individuals 30 years ago. In the United States, the prevalence of H. pylori infection is also higher in African Americans and Mexican Americans. Worldwide, colonization rates vary from less than 10% to more than 80% as a function of age, geography, and social factors.
Pathogenesis
H. pylori organisms have adapted to the ecologic niche provided by gastric mucus. Although H. pylori may invade the gastric mucosa, the contribution of invasion to disease pathogenesis is not known. Four features are linked to H. pylori virulence:
• Flagella, which allow the bacteria to be motile in viscous mucus
• Urease, which generates ammonia from endogenous urea, thereby elevating local gastric pH around the organisms and protecting the bacteria from the acidic pH of the stomach
• Adhesins, which enhance bacterial adherence to surface foveolar cells
• Toxins, such as that encoded by cytotoxin-associated gene A (CagA), that may be involved in ulcer or cancer development
These factors allow H. pylori to create an imbalance between gastroduodenal mucosal defenses and damaging forces that overcome those defenses.
Clinical Features
In addition to histologic identification of the organism, several diagnostic tests have been developed including a noninvasive serologic test for anti–H. pylori antibodies, a stool test for the organism, and the urea breath test, based on the generation of ammonia by bacterial urease. Gastric biopsy specimens also can be analyzed by the rapid urease test, bacterial culture, or polymerase chain reaction (PCR) assay for bacterial DNA. Effective treatments include combinations of antibiotics and proton pump inhibitors. Patients with H. pylori gastritis usually improve after treatment, although relapses can follow incomplete eradication or reinfection.
Autoimmune Gastritis
Autoimmune gastritis accounts for less than 10% of cases of chronic gastritis. In contrast H. pylori-associated gastritis, autoimmune gastritis typically spares the antrum and induces marked hypergastrinemia (Table 15.2). Autoimmune gastritis is characterized by the following:
• Antibodies to parietal cells and intrinsic factor that can be detected in serum and gastric secretions
• Reduced serum pepsinogen I levels
• Antral endocrine cell hyperplasia
• Vitamin B12 deficiency leading to pernicious anemia and neurologic changes
Table 15.2
Characteristics of Helicobacter pylori–Associated and Autoimmune Gastritis
| Feature | H. pylori–Associated | Autoimmune |
| Location | Antrum | Body |
| Inflammatory infiltrate | Neutrophils, subepithelial plasma cells | Lymphocytes, macrophages |
| Acid production | Increased to slightly decreased | Decreased |
| Gastrin | Normal to markedly increased | Markedly increased |
| Other lesions | Hyperplastic/inflammatory polyps | Neuroendocrine hyperplasia |
| Serology | Antibodies to H. pylori | Antibodies to parietal cells (H+,K+-ATPase, intrinsic factor) |
| Sequelae | Peptic ulcer, adenocarcinoma, lymphoma | Atrophy, pernicious anemia, adenocarcinoma, carcinoid tumor |
| Associations | Low socioeconomic status, poverty, residence in rural areas | Autoimmune disease; thyroiditis, diabetes mellitus, Graves disease |
Pathogenesis
Autoimmune gastritis is associated with immune-mediated loss of parietal cells and subsequent reductions in acid and intrinsic factor secretion. Deficient acid secretion stimulates gastrin release, resulting in hypergastrinemia and hyperplasia of antral gastrin-producing G cells. Lack of intrinsic factor disables ileal vitamin B12 absorption, leading to B12 deficiency and a particular form of megaloblastic anemia called pernicious anemia (Chapter 12). Reduced serum concentration of pepsinogen I reflects chief cell loss. Although H. pylori can cause hypochlorhydria, it is not associated with achlorhydria or pernicious anemia, because the parietal and chief cell damage is not as severe as in autoimmune gastritis.
Clinical Features
Antibodies to parietal cells and intrinsic factor are present early in the disease, but B12 deficiency and pernicious anemia develop in only a minority of patients. The median age at diagnosis is 60 years, and there is a slight female predominance. Autoimmune gastritis often is associated with other autoimmune diseases but is not linked to specific human leukocyte antigen (HLA) alleles.
Complications of Chronic Gastritis
There are three important complications of chronic gastritis: Peptic ulcer disease, mucosal atrophy and intestinal metaplasia, and dysplasia. Each of these is discussed shortly.
Peptic Ulcer Disease
Peptic ulcer disease (PUD) most often is associated with H. pylori infection or NSAID use. The imbalances of mucosal defenses and damaging forces that cause chronic gastritis (see Fig. 15.13) are also responsible for PUD. In the United States, NSAID use is becoming the most common cause of gastric ulcers as H. pylori infection rates are falling and low-dose aspirin use in the aging population is increasing. PUD may occur in any portion of the gastrointestinal tract exposed to acidic gastric juices but is most common in the gastric antrum and first portion of the duodenum. Peptic (acid-induced) injury may occur in the esophagus as a result of acid reflux (GERD) or acid secretion by ectopic gastric mucosa. Peptic injury in the small intestine may also be associated with gastric heterotopia, including that within a Meckel diverticulum.
Epidemiology
PUD is common and is a frequent cause of physician visits worldwide. It leads to treatment of over 3 million individuals, 190,000 hospitalizations, and 5000 deaths in the United States each year. The lifetime risk for developing an ulcer is approximately 10% for males and 4% for females.
Pathogenesis
H. pylori infection and NSAID use are the primary underlying causes of PUD. More than 70% of PUD cases are associated with H. pylori infection and in these individuals PUD generally develops on a background of chronic gastritis. Because only 5% to 10% of H. pylori–infected individuals develop ulcers, it is probable that host factors as well as variation among H. pylori strains also contribute to the pathogenesis.
Gastric acid is fundamental to the pathogenesis of PUD. Hyperacidity may be caused by H. pylori infection, parietal cell hyperplasia, and excessive secretory responses. Insufficient inhibition of stimulatory mechanisms such as gastrin release may also contribute. For example, Zollinger-Ellison syndrome, characterized by multiple peptic ulcerations in the stomach, duodenum, and even jejunum, is caused by uncontrolled release of gastrin by a tumor and the resulting massive acid production. Cofactors in peptic ulcerogenesis include chronic NSAID use, as noted; cigarette smoking, which impairs mucosal blood flow and healing; and high-dose corticosteroids, which suppress prostaglandin synthesis and impair healing. Peptic ulcers are more frequent in individuals with alcoholic cirrhosis, chronic obstructive pulmonary disease, chronic renal failure, and hyperparathyroidism. In the latter two conditions, hypercalcemia stimulates gastrin production and thereby increases acid secretion.
Clinical Features
Peptic ulcers are chronic, recurring lesions that occur most often in middle-aged to older adults without obvious precipitating conditions, other than chronic gastritis. A majority of peptic ulcers come to clinical attention after patient complaints of epigastric burning or aching pain, although a significant fraction manifest with complications such as iron deficiency anemia, frank hemorrhage, or perforation. The pain tends to occur 1 to 3 hours after meals during the day, is worse at night, and is relieved by alkali or food. Nausea, vomiting, bloating, and belching may be present. Healing may occur with or without therapy, but the tendency to develop subsequent ulcers remains.
PUD causes much more morbidity than mortality. A variety of surgical approaches were formerly used to treat PUD, but current therapies are aimed at H. pylori eradication with antibiotics and neutralization of gastric acid, usually through use of proton pump inhibitors. These efforts have markedly reduced the need for surgical management, which is reserved primarily for treatment of ulcers with uncontrollable bleeding or perforation.
Mucosal Atrophy and Intestinal Metaplasia
Long-standing chronic gastritis may be associated with intestinal metaplasia, recognized by the presence of goblet cells. This is strongly associated with increased risk for development of gastric adenocarcinoma. In addition, the achlorhydria of gastric mucosal atrophy, which is commonly associated with intestinal metaplasia, permits overgrowth of bacteria that produce carcinogenic nitrosamines. Intestinal metaplasia caused by chronic H. pylori gastritis may regress after eradication of the organism.
Dysplasia
Chronic gastritis exposes the epithelium to inflammation-related free radical damage and proliferative stimuli. Over time, this can lead to the accumulation of genetic alterations that result in carcinoma. Preinvasive in situ lesions can be recognized histologically as dysplasia, which is marked by variations in epithelial size, shape, and orientation along with coarse chromatin texture, hyperchromasia, and nuclear enlargement. These overlap with and are sometimes difficult to distinguish from injury-associated regenerative changes.
Gastric Polyps and Tumors
Gastric Polyps
Polyps are nodules or masses that project above the level of the surrounding mucosa. They are identified in up to 5% of upper gastrointestinal tract endoscopies. Polyps may develop as a result of epithelial or stromal cell hyperplasia, inflammation, ectopia, or neoplasia. Although many different types of polyps can occur in the stomach, only hyperplastic and inflammatory polyps, fundic gland polyps, and adenomas are considered here.
Inflammatory and Hyperplastic Polyps
Up to 75% of all gastric polyps are inflammatory or hyperplastic polyps. In the stomach, inflammatory and hyperplastic polyps represent opposite ends of the morphologic spectrum of a single entity; the distinction is based solely on the degree of inflammation. They most commonly affect individuals between 50 and 60 years of age, usually arising in a background of chronic gastritis that initiates the injury and reactive hyperplasia that cause polyp growth. If associated with H. pylori gastritis, polyps may regress after bacterial eradication.
The frequency with which dysplasia, a precancerous in situ lesion, develops in these polyps correlates with size; there is a significant increase in risk with polyps larger than 1.5 cm.
Fundic Gland Polyps
Fundic gland polyps occur sporadically and in individuals with familial adenomatous polyposis (FAP) Polyps associated with FAP (but not sporadic) may show dysplasia, but they almost never progress to become malignant. The incidence of sporadic lesions has increased markedly as a result of the widespread use of proton pump inhibitors. This likely results from increased gastrin secretion, in response to reduced acidity, and glandular hyperplasia driven by gastrin. Fundic gland polyps are nearly always asymptomatic, and are usually an incidental finding. These well-circumscribed polyps occur in the gastric body and fundus, often are multiple, and are composed of cystically dilated, irregular glands lined by flattened parietal and chief cells.
Gastric Adenoma
Gastric adenomas represent up to 10% of all gastric polyps. Their incidence increases with age and varies among different populations in parallel with that of gastric adenocarcinoma. Patients usually are between 50 and 60 years of age, and males are affected three times more often than females. Adenomas almost always occur on a background of chronic gastritis with atrophy and intestinal metaplasia. All gastrointestinal adenomas exhibit epithelial dysplasia, which can be classified as low- or high-grade. The risk for development of adenocarcinoma in gastric adenomas is related to the size of the lesion and is particularly elevated with lesions greater than 2 cm in diameter. Overall, the malignant potential of gastric adenomas is far greater than that of their colonic counterparts. Carcinoma may be present in up to 30% of gastric adenomas.
Gastric Adenocarcinoma
Adenocarcinoma is the most common malignancy of the stomach, comprising more than 90% of all gastric cancers. Early symptoms resemble those of chronic gastritis, including dyspepsia, dysphagia, and nausea. As a result, the cancer is often diagnosed at advanced stages when clinical manifestations such as weight loss, anorexia, altered bowel habits, anemia, and hemorrhage trigger diagnostic evaluation.
Epidemiology
Gastric cancer rates vary markedly with geography. The incidence is up to 20 times higher in Japan, Chile, Costa Rica, and Eastern Europe than in North America, northern Europe, Africa, and Southeast Asia. Mass endoscopic screening programs have been successful in regions of high incidence, such as Japan, where 35% of newly detected cases are early gastric cancer (i.e., tumors limited to the mucosa and submucosa). Unfortunately, mass screening programs are not cost-effective in regions in which the incidence is low, and less than 20% of cases are detected at an early stage in North America and northern Europe.
Gastric cancer is more common in lower socioeconomic groups and in individuals with multifocal mucosal atrophy and intestinal metaplasia. PUD does not impart an increased risk for development of gastric cancer, but patients who have had partial gastrectomies for PUD have a slightly higher risk for developing cancer in the residual gastric stump as a result of hypochlorhydria, bile reflux, and chronic gastritis.
In the United States, gastric cancer rates have dropped by more than 85% during the 20th century. Similar declines have been reported in many other Western countries, reflecting the importance of environmental and dietary factors. Despite this decrease in overall gastric adenocarcinoma incidence, cancer of the gastric cardia is on the rise. This trend probably is related to increased rates of Barrett esophagus and may reflect the growing prevalence of obesity and chronic GERD.
Pathogenesis
Gastric cancers are genetically heterogeneous, but certain molecular alterations are common. We will consider these first to be followed by the role of H. pylori–induced chronic inflammation and the association of a subset of gastric cancers with EBV infection.
• Mutations. While the majority of gastric cancers are not hereditary, mutations identified in familial gastric cancer have provided important insights into the mechanisms of carcinogenesis in sporadic cases. Germ line mutations in CDH1, which encodes E-cadherin, a protein that contributes to epithelial intercellular adhesion, are associated with familial gastric cancers, usually of the diffuse type. By comparison, mutations in CDH1 are present in about 50% of sporadic diffuse gastric tumors, while E-cadherin expression is drastically decreased in the rest, often by methylation of the CDH1 promoter. Thus, the loss of E-cadherin function seems to be a key step in the development of diffuse gastric cancer.
In contrast to CDH1, patients with FAP who have germ line mutations in adenomatous polyposis coli (APC) genes have an increased risk for development of intestinal-type gastric cancer. Sporadic intestinal-type gastric cancer is associated with several genetic abnormalities including acquired mutations of β-catenin, a protein that binds to both E-cadherin and APC protein; microsatellite instability; and hypermethylation of genes including TGFβRII, BAX, IGFRII, and p16/INK4a. TP53 mutations are present in a majority of sporadic gastric cancers of both histologic types.
• H. pylori. Chronic gastritis, most commonly due to H. pylori infection, promotes the development and progression of cancers that may be induced by diverse genetic alterations (Chapter 6). As is the case with many forms of chronic inflammation, H. pylori–induced chronic gastritis is associated with increased production of proinflammatory proteins, such as interleukin-1β (IL-1β) and tumor necrosis factor (TNF). It is therefore not surprising that polymorphisms of genes that encode such factors and enhance production of these cytokines confer increased risk for development of chronic gastritis-associated gastric cancer in those with coexisting H. pylori infection.
• Epstein-Barr virus (EBV). While H. pylori is most commonly associated with gastric cancer, approximately 10% of gastric adenocarcinomas are associated with Epstein-Barr virus (EBV) infection. Although the precise role of EBV in the development of gastric adenocarcinomas remains to be defined, it is notable that EBV episomes in these tumors frequently are clonal, suggesting that infection preceded neoplastic transformation. Further, TP53 mutations are uncommon in EBV-positive gastric tumors, suggesting that the molecular pathogenesis of these cancers is distinct from that of other gastric adenocarcinomas. Morphologically, EBV-positive tumors tend to occur in the proximal stomach and most commonly have a diffuse morphology with a marked lymphocytic infiltrate.
Clinical Features
Intestinal-type gastric cancer predominates in high-risk areas and develops from precursor lesions such as dysplasia and adenomas. The mean age at presentation is 55 years, and the male-to-female ratio is 2:1. By contrast, the incidence of diffuse gastric cancer is relatively uniform across countries, there are no identified precursor lesions, and the disease occurs at similar frequencies in males and females. Of note, the decrease in gastric cancer incidence applies only to the intestinal type, which is most closely associated with atrophic gastritis and intestinal metaplasia. As a result, the incidences of intestinal and diffuse types of gastric cancers are now similar in some regions.
The depth of invasion and the extent of nodal and distant metastasis at the time of diagnosis remain the most powerful prognostic indicators for gastric cancer. Local invasion into the duodenum, pancreas, and retroperitoneum is also characteristic. When possible, surgical resection remains the preferred treatment for gastric adenocarcinoma. After surgical resection, the 5-year survival rate for early gastric cancer can exceed 90%, even if lymph node metastases are present. By contrast, the 5-year survival rate for advanced gastric cancer remains below 20%, in large part because current chemotherapy regimens are have limited impact. This is changing slowly with individualized therapies. For example, patients whose tumors over-express the epidermal growth factor receptor HER2 benefit from agents that inhibit HER2 signaling. Nevertheless, most gastric cancers are discovered at advanced stage in the United States, and the overall 5-year survival rate is less than 30%.
Lymphoma
Although extranodal lymphomas can arise in virtually any tissue, they do so most commonly in the gastrointestinal tract, particularly the stomach. In allogeneic hematopoietic stem cell and organ transplant recipients, the bowel also is the most frequent site for Epstein-Barr virus–positive B cell lymphoproliferations. Nearly 5% of all gastric malignancies are primary lymphomas, the most common of which are indolent extranodal marginal zone B-cell lymphomas. In the gut, these tumors often are referred to as lymphomas of MALT, or MALTomas. This entity and the second most common primary lymphoma of the gut, diffuse large B cell lymphoma, are discussed in Chapter 12.
Neuroendocrine (Carcinoid) Tumor
Neuroendocrine tumors, also referred to as carcinoid tumors, arise from neuroendocrine organs (e.g., the endocrine pancreas) and neuroendocrine-differentiated gastrointestinal epithelia (e.g., G cells). A majority of these tumors are found in the gastrointestinal tract, and more than 40% occur in the small intestine. The tracheobronchial tree and lungs are the next most commonly involved sites. Gastric neuroendocrine tumors may be associated with endocrine cell hyperplasia, chronic atrophic gastritis, and Zollinger-Ellison syndrome. These tumors were called “carcinoid” because they are slower growing than carcinomas. The most current WHO classification describes these as low- or intermediate-grade neuroendocrine tumors. High-grade neuroendocrine tumors, termed neuroendocrine carcinoma, resemble small cell carcinoma of the lung (Chapter 13) and, in the gastrointestinal tract, are most common in the jejunum.
Clinical Features
The peak incidence of neuroendocrine tumors is in the sixth decade, but they may appear at any age. Symptoms are determined by the hormones produced. For example, the carcinoid syndrome is caused by vasoactive substances secreted by the tumor that cause cutaneous flushing, sweating, bronchospasm, colicky abdominal pain, diarrhea, and right-sided cardiac valvular fibrosis. When tumors are confined to the intestine, the vasoactive substances released are metabolized to inactive forms by the liver—a “first-pass” effect similar to that seen with oral drugs. Thus, carcinoid syndrome occurs in less than 10% of patients and is strongly associated with metastatic disease.
The most important prognostic factor for gastrointestinal neuroendocrine tumors is location:
• Foregut neuroendocrine (carcinoid) tumors found within the stomach, duodenum proximal to the ligament of Treitz, and esophagus, rarely metastasize and are generally cured by resection. Rare duodenal gastrin-producing neuroendocrine tumors, also termed gastrinomas, may present with symptoms related to increased acid production, including pain and/or bleeding from gastroduodenal ulcers, refractory gastroesophageal reflux, and diarrhea due to inactivation of pancreatic enzymes by excessive gastric acid.
• Midgut neuroendocrine (carcinoid) tumors arise in the jejunum and ileum, are often multiple and tend to be aggressive. In these tumors, depth of local invasion, size, and the presence of necrosis and mitoses are associated with poor outcome.
• Hindgut neuroendocrine (carcinoid) tumors arising in the appendix and colorectum are typically discovered incidentally. Those in the appendix occur at any age and are almost uniformly pursue a benign course. Rectal tumors tend to produce polypeptide hormones and may manifest with abdominal pain and weight loss. Because they are usually discovered when small, metastasis of rectal neuroendocrine tumors is uncommon.
Gastrointestinal Stromal Tumor
Gastrointestinal stromal tumor (GIST) is the most common mesenchymal tumor of the abdomen, and more than half of these tumors occur in the stomach. A wide variety of other mesenchymal neoplasms may arise in the stomach. Many are named according to the cell type they most resemble; for example, smooth muscle tumors are called leiomyomas or leiomyosarcomas, nerve sheath tumors are termed schwannomas, and those resembling glomus bodies in the nail beds and at other sites are termed glomus tumors. These tumors are all rare and are not discussed here.
Pathogenesis
The most common genetic change underlying the pathogenesis of GISTs is gain-of-function mutations of the gene encoding the tyrosine kinase KIT, the receptor for stem cell factor. These are present in 75% to 85% of all GISTs. An additional 8% of GISTs have mutations that activate a related tyrosine kinase, platelet-derived growth factor receptor A (PDGFRA). The term stromal reflects historical confusion about the origin of this tumor, which is now recognized to arise from the interstitial cells of Cajal, or pacemaker cells, of the gastrointestinal muscularis propria. For unknown reasons, GISTs bearing PDGFRA mutations are overrepresented in the stomach. KIT and PDGFRA gene mutations are mutually exclusive, reflecting their activities within the same signal transduction pathway. Germ line mutations in these same genes are present in rare familial GISTs, in which patients develop multiple GISTs and may also have diffuse hyperplasia of Cajal cells.
Both sporadic and germ line mutations result in constitutively active KIT or PDGFRA receptor tyrosine kinases and produce intracellular signals that promote tumor cell proliferation and survival (Chapter 6). In GISTs without KIT or PDGFRA mutations, genes encoding components of the mitochondrial succinate dehydrogenase (SDH) complex are most commonly affected. These mutations result in loss of SDH function and confer increased risk for both GIST and paraganglioma. One mutant allele is often inherited, with the second copy of the gene being either mutated or otherwise lost in the tumor. The loss of SDH causes a number of metabolic changes, including increased production of reactive oxygen species, activation of hypoxia induced factor (HIF), and increased dependency on glycolysis for ATP production, but how these alterations lead to transformation is uncertain.










