Grooming
- • Define the key terms and key abbreviations in this chapter.
- • Explain why grooming is important.
- • Explain how to safely provide grooming measures—hair care, shaving, nail and foot care, and changing garments.
- • Perform the procedures described in this chapter.
- • Explain how to promote PRIDE in the person, the family, and yourself.
Key Terms
anticoagulant A drug that prevents or slows down (anti) blood clotting (coagulate)
dandruff Excessive amounts of dry, white flakes from the scalp
infestation Being in or on a host
mite A very small spider-like organism
pediculosis Infestation with wingless insects; lice
pediculosis capitis Infestation of the scalp (capitis) with lice
pediculosis corporis Infestation of the body (corporis) with lice
pediculosis pubis Infestation of the pubic (pubis) hair with lice
scabies A skin disorder caused by a female mite—a very small spider-like organism
Hair care, shaving, nail and foot care, and clean garments prevent infection and promote comfort. Such measures affect love, belonging, and self-esteem needs.
People differ in their grooming measures. Some want only clean hair. Others want a certain hairstyle. Some want only clean hands. Others want polished nails. Men may shave and groom their beards. Likewise, women may shave their legs and underarms. Some women use hair removal methods for facial hair.
As with hygiene, the person performs grooming measures to the extent possible. This promotes independence and quality of life. The person may use adaptive devices (Fig. 23-1).
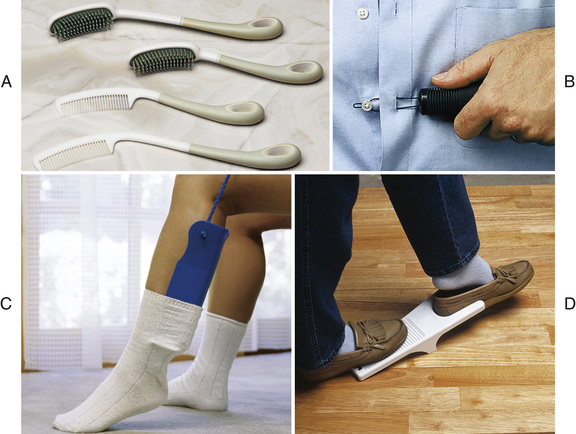
See Focus on Surveys: Grooming.
See Teamwork and Time Management: Grooming.
Hair Care
The look and feel of hair affect mental well-being. The nursing process reflects the person's culture, personal choice, skin and scalp conditions, health history, and self-care ability. You assist with hair care as needed.
See Focus on Long-Term Care and Home Care: Hair Care.
Skin and Scalp Conditions
Skin and scalp conditions include hair loss, excessive body hair, dandruff, lice, and scabies.
- • Alopecia means hair loss. Hair loss may be complete or partial. A result of heredity, male pattern baldness occurs with aging. Hair thins in some women with aging. Cancer treatments (radiation therapy to the head and chemotherapy) may cause alopecia in all age-groups. Skin disease, stress, poor nutrition, pregnancy, some drugs, and hormone changes are other causes. Except for hair loss from aging, hair usually grows back.
- • Hirsutism is excessive body hair. It can occur in men, women, and children. It results from heredity and abnormal amounts of male hormones.
- • Dandruff is the excessive amount of dry, white flakes from the scalp. Itching is common. Sometimes eyebrows and ear canals are involved. Medicated shampoos correct the problem.
- • Pediculosis (lice) is the infestation with wingless insects (Fig. 23-3). Infestation means being in or on a host. Lice attach their eggs (nits) to hair shafts. Nits are oval and yellow to white in color. They hatch in about 1 week. After hatching, they bite the scalp or skin to feed on blood. About the size of a sesame seed, adult lice are tan to gray-ish white in color. Lice easily spread to others through clothing, head coverings, furniture, beds, towels, bed linens, and sexual contact. They also are spread by sharing combs and brushes. Lice are treated with medicated shampoos, lotions, and creams specific for lice. Thorough bathing is needed. So is washing clothing and linens in hot water. Lice bites cause severe itching in the affected body area.
- • Pediculosis capitis is the infestation of the scalp (capitis) with lice. It is commonly called “head lice.”
- • Pediculosis pubis is the infestation of the pubic (pubis) hair with lice. This form of lice is also called “crabs.”
- • Pediculosis corporis is the infestation of the body (corporis) with lice.
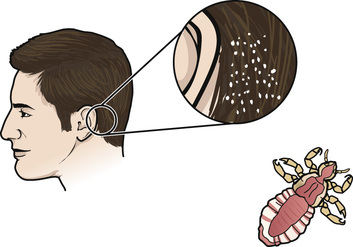 FIGURE 23-3 Head lice. (Redrawn from Medline Plus: Head lice. Bethesda, Md., National Institutes of Health.)
FIGURE 23-3 Head lice. (Redrawn from Medline Plus: Head lice. Bethesda, Md., National Institutes of Health.) - • Scabies is a skin disorder caused by a female mite (Fig. 23-4). A mite is a very small spider-like organism. The female mite burrows into the skin and lays eggs. After hatching, the females produce more eggs. Infested with mites, the person has a rash and intense itching. Common sites are between the fingers, the wrists, underarm areas, thighs, and genital area. Other sites include the breasts, waist, and buttocks. Highly contagious, scabies is transmitted to others by close contact. Persons in crowded living settings are at risk. So are persons with weakened immune systems. Special creams are ordered to kill the mites. The person's room is cleaned. Clothing and linens are washed in hot water.
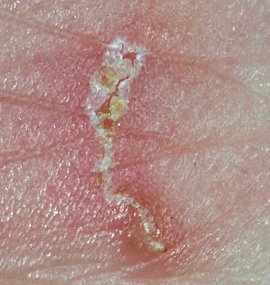 FIGURE 23-4 Scabies. (From Marks JG, Miller JJ: Lookingbill & Marks' principles of dermatology, ed 4, St Louis, 2006, Saunders.)
FIGURE 23-4 Scabies. (From Marks JG, Miller JJ: Lookingbill & Marks' principles of dermatology, ed 4, St Louis, 2006, Saunders.)
 Brushing and Combing Hair
Brushing and Combing Hair
Brushing and combing hair are part of early morning care, morning care, and afternoon care. Some people also do so at bedtime. Provide hair care when needed and before visitors arrive.
Encourage patients and residents to do their own hair care. The person chooses how to brush, comb, and style hair. Assist as needed. Provide hair care for those who cannot do so.
Brushing increases blood flow to the scalp. And it brings scalp oils along the hair shaft to help keep hair soft and shiny. Daily brushing and combing prevent tangled and matted hair. To brush and comb hair, start at the scalp. Then brush or comb to the hair ends.
Braiding prevents long hair from matting and tangling. You need the person's consent to braid hair. Report matted or tangled hair to the nurse. The nurse may have you comb or brush through the matting and tangling from the hair ends to the scalp. Never cut the person's hair.
Special measures are needed for curly, coarse, and dry hair. For curly hair, use a wide-tooth comb. Start at the neckline. Working upward, lift and fluff hair outward. Continue to the forehead. Wet hair or apply conditioner, petroleum jelly, or other hair care product as directed. This makes combing easier. Follow the care plan for coarse and dry hair.
The person may have certain hair care practices and products. They are part of the care plan. Also, let the person guide you when giving hair care.
See Caring about Culture: Brushing and Combing Hair.
See Focus on Children and Older Persons: Brushing and Combing Hair.
See Delegation Guidelines: Brushing and Combing Hair.
See Promoting Safety and Comfort: Brushing and Combing Hair.
See procedure: Brushing and Combing Hair, p. 370.
 Shampooing
Shampooing
People vary in shampoo frequency—1, 2, or 3 times a week or daily. Factors affecting frequency include hair and scalp condition, hairstyle, and personal choice.
Some persons use certain shampoos and conditioners. Others use medicated products ordered by the doctor.
The person may need help shampooing. The nurse tells you what method to use. The shampoo method depends on the person's condition, safety factors, and personal choice.
- • Shampoo during the shower or tub bath. You use a hand-held nozzle for persons in shower chairs or taking tub baths. Direct a spray of water at the hair.
- • Shampoo at the sink. The person sits or lies facing away from the sink. A folded towel placed over the sink edge protects the neck. The person's head is tilted back over the sink edge (Fig. 23-7). Use a water pitcher or hand-held nozzle to wet and rinse the hair.
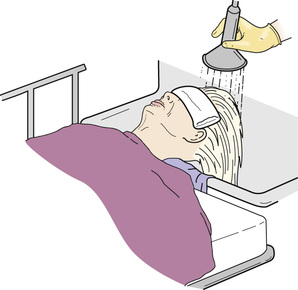 FIGURE 23-7 Shampooing while the person is on a stretcher. The stretcher is in front of the sink.
FIGURE 23-7 Shampooing while the person is on a stretcher. The stretcher is in front of the sink. - • Shampoo in bed. The person's head and shoulders are at the edge of the bed if possible. A shampoo tray is under the head to protect the linens and mattress from water. The tray drains into a basin on a chair by the bed (Fig. 23-8). Use a water pitcher to wet and rinse the hair. This method is used for persons:
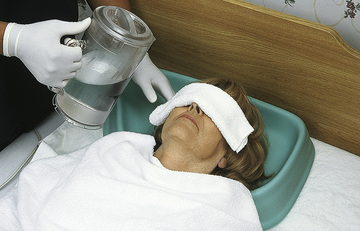 FIGURE 23-8 A shampoo tray for a person in bed. The tray is directed to the side of the bed so water drains into a collecting basin.
FIGURE 23-8 A shampoo tray for a person in bed. The tray is directed to the side of the bed so water drains into a collecting basin.
Some agencies have commercial shampoo caps. The cap has a cleaning agent that does not need rinsing. Some caps also have a conditioner. To use a shampoo cap:
- • Warm the package in a microwave oven or commercial warmer. Follow the manufacturer's instructions for microwave settings and warming times.
- • Check the temperature. The cap should be warm. Do not use a cap that is too hot.
- • Apply the cap to the person's head.
- • Massage the cap gently. Follow the manufacturer's instructions for how long to massage—usually 1 to 3 minutes. Longer hair may require more time.
- • Remove the cap. You do not need to rinse the hair. Dry the hair with a towel if needed.
- • Comb the hair.
Dry and style hair as soon as possible after the shampoo. Women may want hair curled or rolled up before drying. Check with the nurse before doing so.
See Focus on Children and Older Persons: Shampooing.
See Focus on Long-Term Care and Home Care: Shampooing, p. 372.
See Delegation Guidelines: Shampooing, p. 372.
See Promoting Safety and Comfort: Shampooing, p. 372.
See procedure: Shampooing the Person's Hair, p. 373.
 Shaving
Shaving
Many men shave for comfort and well-being. Many women shave their legs and underarms. Some women shave facial hair. Other hair removal methods include waxing, hair removal products, plucking, and threading. See Box 23-1 for shaving rules.
Safety razors or electric shavers are used (Fig. 23-9). Some persons have their own electric shavers. If the agency's shaver is used, clean it before and after use. To brush out whiskers or hair, follow the manufacturer's instructions. Also follow agency policy for cleaning electric shavers.

Safety razors (blade razors) have razor blades. They can cause nicks and cuts. Do not use safety razors on persons with healing problems or for those taking anticoagulant drugs. An anticoagulant is a drug that prevents or slows down (anti) blood clotting (coagulate). Bleeding occurs easily and is hard to stop. A nick or cut can cause serious bleeding. Electric shavers are used.
Soften the beard before shaving. To do so, apply a moist, warm washcloth or towel for a few minutes. Then pat dry the face and apply talcum powder if using an electric shaver. For a safety razor, lather the face with soap and water or shaving cream.
See Focus on Children and Older Persons: Shaving.
See Delegation Guidelines: Shaving.
See Promoting Safety and Comfort: Shaving.
See procedure: Shaving the Person's Face With a Safety Razor.
Caring for Mustaches and Beards
Mustaches and beards need daily care. Food can collect in the whiskers. So can mouth and nose drainage. Daily washing and combing are needed. Ask the person how to groom his mustache or beard. Never trim a mustache or beard.
Shaving Legs and Underarms
Many women shave their legs and underarms. This practice varies among cultures. Some women shave only the lower legs. Others shave to mid-thigh or the entire leg.
To shave legs and underarms:
- • Follow the rules in Box 23-1.
- • Collect shaving items with bath items.
- • Shave after bathing. The skin is soft at this time.
- • Use soap and water, shaving cream, or lotion for the lather. Follow the care plan.
- • Use the kidney basin to rinse the razor. Do not use bath water.
 Nail and Foot Care
Nail and Foot Care
Nail and foot care prevents infection, injury, and odors. Hangnails, ingrown nails (nails that grow in at the side), and nails torn away from the skin cause skin breaks. These breaks are portals of entry for microbes. Long or broken nails can scratch skin and snag clothing.
The feet are easily injured and infected. Dirty feet, socks, or stockings harbor microbes and cause odors. Shoes and socks provide a warm, moist environment for microbes to grow. Injuries occur from stubbing toes, stepping on sharp objects, or being stepped on. Poorly fitting shoes cause blisters.
Poor circulation prolongs healing. Diabetes and vascular diseases are common causes of poor circulation. Foot injuries or infections are very serious for older persons and persons with circulatory disorders. Gangrene and amputation are serious complications (Chapter 44).
Nails are easier to trim and clean right after soaking or bathing. Use nail clippers to cut fingernails. Never use scissors. Use extreme caution to prevent damage to nearby tissues.
Trimming and clipping toenails can easily cause injuries. Some agencies do not let nursing assistants cut or trim toenails. Follow agency policy.
See Teamwork and Time Management: Nail and Foot Care.
See Focus on Long-Term Care and Home Care: Nail and Foot Care.
See Delegation Guidelines: Nail and Foot Care.
See Promoting Safety and Comfort: Nail and Foot Care.
See procedure: Giving Nail and Foot Care, p. 378.
Changing Garments
Hospital patients usually wear patient gowns or other sleepwear. Nursing center residents wear street clothes during the day and sleepwear at bedtime. Garments are changed:
 Dressing and Undressing
Dressing and Undressing
When assisting with dressing and undressing, follow the rules in Box 23-2.
See Focus on Communication: Dressing and Undressing.
See Focus on Children and Older Persons: Dressing and Undressing.
See Focus on Long-Term Care and Home Care: Dressing and Undressing.
See Delegation Guidelines: Dressing and Undressing, p. 380.
See Promoting Safety and Comfort: Dressing and Undressing, p. 380.
See procedure: Undressing the Person, p. 380.
See procedure: Dressing the Person, p. 382.
 Changing Patient Gowns
Changing Patient Gowns
Many patients wear patient gowns. So do some nursing center residents. Gowns are usually worn for IV (intravenous) therapy (Chapter 28). Some agencies have IV therapy gowns that open along the sleeve and close with ties, snaps, or Velcro. Sometimes standard gowns are used.
For injury or paralysis, remove the gown from the strong arm first. Support the weak arm while removing the gown. Put the clean gown on the weak arm first and then on the strong arm.
See Delegation Guidelines: Changing Patient Gowns.
See Promoting Safety and Comfort: Changing Patient Gowns.
See procedure: Changing a Patient Gown on a Person With an IV.
Review Questions
Circle T if the statement is TRUE or F if it is FALSE.
2. T F Mustaches are trimmed weekly.
3. T F Feet are soaked for 5 to 10 minutes.
4. T F Fingernails are clipped straight across.
5. T F Wear gloves when giving nail care.
6. T F Clothing is removed from the weak side first.
7. T F The person chooses what to wear.
8. T F A person has poor circulation in the legs and feet. You can trim the person's toenails.
9. T F You can cut matted hair.
Circle the BEST answer.
10. A person with alopecia has
b Dry, white flakes from the scalp
11. Which prevents hair from matting and tangling?
12. A person's hair is not matted or tangled. When brushing hair, start at
a The forehead and brush backward
d The back of the neck and brush forward
14. A person requests a shampoo. You should
a Shampoo the hair during the person's shower
15. When shaving a person's face with a safety razor
a Discard the razor in the wastebasket when done
b Shave against the direction of hair growth
16. A person is nicked during shaving. Your first action is to
c To either the weak or the strong side first
d In the same way they are removed
20. When changing the gown on a person with an IV
a Keep the IV bag below the person's arm
b Stop the IV pump to change the gown
c Have the nurse check the flow rate afterward
d Disconnect the IV to change the gown
See Review Question Answers at the back of the text.






 (two-thirds) full with water. The nurse tells you what water temperature to use. (Measure water temperature with a bath thermometer. Or test it by dipping your elbow or inner wrist into the basin. Follow agency policy.) Also ask the person to check the water temperature. Adjust the water temperature as needed.
(two-thirds) full with water. The nurse tells you what water temperature to use. (Measure water temperature with a bath thermometer. Or test it by dipping your elbow or inner wrist into the basin. Follow agency policy.) Also ask the person to check the water temperature. Adjust the water temperature as needed. (two-thirds) full with water. See step 9 for water temperature.
(two-thirds) full with water. See step 9 for water temperature.










