Bowel Elimination
- • Define the key terms and key abbreviations in this chapter.
- • Describe normal defecation and the observations to report.
- • Identify the factors affecting bowel elimination.
- • Explain how to promote comfort and safety during defecation.
- • Describe the common bowel elimination problems.
- • Describe bowel training.
- • Explain why enemas are given.
- • Describe the common enema solutions.
- • Describe the rules for giving enemas.
- • Describe how to care for a person with an ostomy.
- • Perform the procedures described in this chapter.
- • Explain how to promote PRIDE in the person, the family, and yourself.
Key Terms
colostomy A surgically created opening (stomy) between the colon (colo) and the body's surface
constipation The passage of a hard, dry stool
defecation The process of excreting feces from the rectum through the anus; a bowel movement
dehydration The excessive loss of water from tissues
diarrhea The frequent passage of liquid stools
enema The introduction of fluid into the rectum and lower colon
fecal impaction The prolonged retention and buildup of feces in the rectum
fecal incontinence The inability to control the passage of feces and gas through the anus
feces The semi-solid mass of waste products in the colon that is expelled through the anus; also called a stool or stools
flatulence The excessive formation of gas or air in the stomach and intestines
flatus Gas or air passed through the anus
ileostomy A surgically created opening (stomy) between the ileum (small intestine [ileo] ) and the body's surface
ostomy A surgically created opening that connects an internal organ to the body's surface; see “colostomy” and “ileostomy”
peristalsis The alternating contraction and relaxation of intestinal muscles
stoma A surgically created opening seen on the body's surface; see “colostomy” and “ileostomy”
suppository A cone-shaped, solid drug that is inserted into a body opening; it melts at body temperature
Key Abbreviations
| BM | Bowel movement |
| CMS | Centers for Medicare & Medicaid Services |
| GI | Gastro-intestinal |
| ID | Identification |
| IV | Intravenous |
| mL | Milliliter |
| oz | Ounce |
| SSE | Soapsuds enema |
Bowel elimination is a basic physical need. Wastes are excreted from the gastro-intestinal (GI) system (Chapter 10). Many factors affect bowel elimination—privacy, habits, age, diet, exercise and activity, fluids, drugs, disability. Problems easily occur. Normal bowel elimination is important. You assist patients and residents to meet elimination needs.
See Body Structure and Function Review: The Gastro-Intestinal Tract.
Normal Bowel Elimination
Some people have a bowel movement (BM) every day. Others do so every 2 to 3 days. Some people have 2 or 3 BMs a day. Many people have a BM after breakfast. Others do so in the evening.
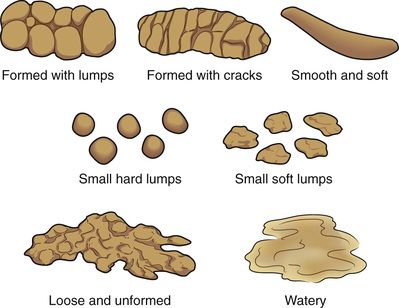
Stools are normally brown. Bleeding in the stomach and small intestine causes black or tarry stools. Bleeding in the lower colon and rectum causes red-colored stools. So do beets, tomato juice or soup, red Jell-O, and foods with red food coloring. Green vegetables can cause green stools. Diseases and infection can cause clay-colored or white, pale, orange-colored, or green-colored stools and stools with mucus. Figure 26-2, p. 424 shows a color chart for stools.

Stools are normally soft, formed, moist, and shaped like the rectum. They have a normal odor caused by bacteria in the intestines. Certain foods and drugs also cause odors.
See Focus on Children and Older Persons: Normal Bowel Elimination, p. 424.
Observations
Your observations are used for the nursing process. Ask the nurse to observe abnormal stools. Report and record the following.
Factors Affecting BMs
These factors affect BM frequency, consistency, color, and odor. They are part of the nursing process to meet the person's elimination needs. Normal, regular elimination is the goal.
- • Privacy. Lack of privacy can prevent a BM despite the urge. Odors and sounds are embarrassing. Some people ignore the urge when people are present.
- • Habits. Many people have a BM after breakfast. Some drink a hot beverage, read, or take a walk. These activities are relaxing. A BM is easier when a person is relaxed, not tense.
- • Diet—high-fiber foods. High-fiber foods leave a residue for needed bulk to prevent constipation (p. 426). Fruits, vegetables, and whole-grain cereals and breads are high in fiber. Many people do not eat enough fruits and vegetables. Some cannot chew these foods. They may not have teeth. Or dentures fit poorly. Some people think that they cannot digest fruits and vegetables. So they refuse to eat them. Sometimes bran is added to cereal, prunes, or prune juice.
- • Diet—other foods. Milk and milk products can cause constipation in some people and diarrhea in others. Chocolate and other foods cause similar reactions. Spicy foods can irritate the intestines, causing frequent stools or diarrhea. Gas-forming foods stimulate peristalsis, aiding BMs. Such foods include onions, beans, cabbage, cauliflower, radishes, and cucumbers.
- • Fluids. Feces contain water. Stool consistency depends on the amount of water absorbed in the colon. Fluid intake, urine output, and vomiting are factors. Feces harden and dry when large amounts of water are absorbed or from poor fluid intake. Hard, dry feces move slowly through the colon. Constipation can occur. Drinking 6 to 8 glasses of water daily promotes normal BMs. Warm fluids—coffee, tea, hot cider, warm water—increase peristalsis.
- • Activity. Exercise and activity maintain muscle tone and stimulate peristalsis. Constipation is a risk from inactivity and bedrest. Inactivity may result from disease, surgery, injury, and aging.
- • Drugs. Drugs can prevent constipation or control diarrhea. Other drugs have diarrhea or constipation as side effects. Pain-relief drugs often cause constipation. Antibiotics (used to fight or prevent infections) often cause diarrhea. Diarrhea occurs when the antibiotics kill normal flora in the colon. Normal flora is needed to form feces. (See “Normal Flora” in Chapter 16.)
- • Disability. Some people cannot control BMs. They have a BM whenever feces enter the rectum. A bowel training program is needed (p. 430).
- • Aging. Age affects bowel elimination.
See Focus on Children and Older Persons: Factors Affecting BMs.
Safety and Comfort
The care plan has measures for meeting elimination needs. It may involve diet, fluids, and exercise. The measures in Box 26-1 promote safety and comfort.
Common Problems
Common problems include constipation, fecal impaction, diarrhea, fecal incontinence, and flatulence.
Constipation
Constipation is the passage of a hard, dry stool. The person strains to have a BM. Stools are large or marble-sized. Large stools cause pain as they pass through the anus. Constipation occurs when feces move slowly through the bowel. This allows more time for water absorption. Common causes of constipation include:
- • A low-fiber diet
- • Ignoring the urge to have a BM
- • Decreased fluid intake
- • Inactivity
- • Drugs
- • Aging
- • Certain diseases
Diet changes, fluids, and activity prevent or relieve constipation. The doctor may order 1 or more of the following.
- • Stool softeners. These drugs soften feces. A BM is easier when feces are soft.
- • Laxatives. Laxative comes from the Latin word that means to loosen. A laxative is a drug that promotes bowel elimination. It increases the bulk of feces, softens feces, and lubricates the intestinal wall.
- • Suppositories (p. 430).
- • Enemas (p. 431).
 Fecal Impaction
Fecal Impaction
A fecal impaction is the prolonged retention and buildup of feces in the rectum. Feces are hard or putty-like. Fecal impaction results if constipation is not relieved. The person cannot have a BM. More water is absorbed from the already hard feces. Liquid feces pass around the hardened fecal mass in the rectum and seep from the anus.
The person tries many times to have a BM. Abdominal discomfort, abdominal distention (swelling), nausea, cramping, and rectal pain are common. Older persons may have poor appetite or confusion. Some persons have a fever. Report such signs and symptoms to the nurse.
The nurse does a digital (finger) exam to check for an impaction. A lubricated, gloved finger is inserted into the rectum to feel for a hard mass in the lower rectum (Fig. 26-5). Sometimes it is out of reach higher in the colon. The digital exam often causes the urge to have a BM. The doctor may order drugs, suppositories, or enemas to remove the impaction.
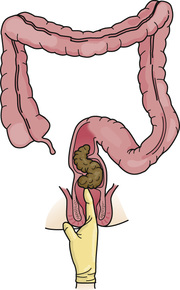
Sometimes digital removal of an impaction is done. A lubricated, gloved finger is hooked around a piece of feces. Then the finger and feces are removed. The stool is dropped into the bedpan. The process is repeated as needed. The procedure can be uncomfortable and embarrassing.
Checking for and removing impactions are very dangerous. The vagus nerve can be stimulated. Stimulation of the vagus nerve slows the heart rate. The heart rate can slow to unsafe levels in some persons.
See Focus on Long-Term Care and Home Care: Fecal Impaction.
See Delegation Guidelines: Fecal Impaction.
See Promoting Safety and Comfort: Fecal Impaction.
See procedure: Checking For and Removing a Fecal Impaction, p. 428.
Diarrhea
Diarrhea is the frequent passage of liquid stools. Feces move through the intestines rapidly. This reduces the time for fluid absorption. The need for a BM is urgent. Some people cannot get to a bathroom in time. Abdominal cramping, nausea, and vomiting may occur.
Causes of diarrhea include infections, some drugs, irritating foods, and microbes in food and water. Diet and drugs are ordered to reduce peristalsis. You need to:
- • Assist with elimination needs promptly.
- • Dispose of stools promptly. This prevents odors and the spread of microbes.
- • Give good skin care. Liquid stools irritate the skin. So does frequent wiping with toilet tissue. Skin breakdown and pressure ulcers are risks.
Fluid lost through diarrhea must be replaced to prevent dehydration. Dehydration is the excessive loss of water from tissues. The person has pale or flushed skin, dry skin, and a coated tongue. Urine is dark and scant in amount (oliguria). Thirst, weakness, dizziness, and confusion also occur. Falling blood pressure and increased pulse and respirations are serious signs. Death can occur. The nursing process is used to meet fluid needs. The doctor may order IV (intravenous) fluids in severe cases (Chapter 28).
Microbes can cause diarrhea. Preventing the spread of infection is important. Always follow Standard Precautions and the Bloodborne Pathogen Standard when in contact with stools.
Fecal Incontinence
Fecal incontinence is the inability to control the passage of feces and gas through the anus. Causes include:
- • Intestinal diseases.
- • Nervous system diseases and injuries.
- • Fecal impaction or diarrhea.
- • Some drugs.
- • Chronic illness.
- • Aging.
- • Mental health problems or dementia (Chapters 48 and 49). The person may not recognize the need for or the act of having a BM.
- • Unanswered call lights.
- • Not getting to the bathroom in time. The person may have mobility problems or may walk slowly. The bathroom may be too far away or occupied by another person.
- • Problems removing clothes.
- • Not finding the bathroom in a new setting.
Fecal incontinence affects the person emotionally. Frustration, embarrassment, anger, and humiliation are common. The person may need:
- • Bowel training
- • Help with elimination after meals and every 2 to 3 hours
- • Incontinence products to keep garments and linens clean
- • Good skin care
See Focus on Children and Older Persons: Fecal Incontinence.
Flatulence
Gas and air are normally in the stomach and intestines. They are expelled through the mouth (burping, belching, eructating) and anus. Gas or air passed through the anus is called flatus. Flatulence is the excessive formation of gas or air in the stomach and intestines. Causes include:
- • Swallowing air while eating and drinking. This includes chewing gum, eating fast, drinking through a straw, and drinking carbonated beverages. Tense or anxious people may swallow large amounts of air when drinking.
- • Bacterial action in the intestines.
- • Gas-forming foods—onions, beans, cabbage, cauliflower, radishes, and cucumbers.
- • Constipation.
- • Bowel and abdominal surgeries.
- • Drugs that decrease peristalsis.
If flatus is not expelled, the intestines swell or enlarge (distend) from the pressure of gases. Abdominal cramping or pain, shortness of breath, and a swollen abdomen occur. Bloating is a common complaint. Exercise, walking, moving in bed, and the left side-lying position often expel flatus. Doctors may order enemas and drugs to relieve flatulence.
Bowel Training
Bowel training has 2 goals.
- • To gain control of BMs.
- • To develop a regular pattern of elimination. Fecal impaction, constipation, and fecal incontinence are prevented.
Meals, especially breakfast, stimulate the urge for a BM. The person's usual time for a BM is noted on the care plan. So is toilet, commode, or bedpan use. Offer help with elimination at the times noted. The care plan includes a high-fiber diet, increased fluids, warm fluids, activity, and privacy. The nurse tells you about a person's bowel training program.
Suppositories
A suppository is a cone-shaped, solid drug that is inserted into a body opening. It melts at body temperature. A rectal suppository is inserted into the rectum (Fig. 26-6). A BM occurs about 30 minutes later.
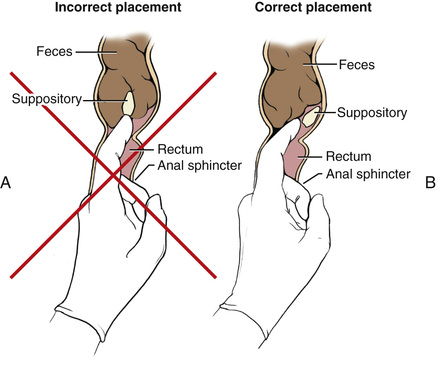
The doctor may order a suppository for:
See Delegation Guidelines: Suppositories.
See Promoting Safety and Comfort: Bowel Elimination, p. 423.
Enemas
An enema is the introduction of fluid into the rectum and lower colon. Doctors order enemas to:
- • Remove feces.
- • Relieve constipation, fecal impaction, or flatulence.
- • Clean the bowel of feces before certain surgeries and diagnostic procedures.
Safety and comfort measures for bowel elimination are practiced when giving enemas (see Box 26-1). So are the rules in Box 26-2.
The doctor orders the enema solution. The solution depends on the enema's purpose—cleansing, constipation, fecal impaction, or flatulence.
- • Tap water enema—is obtained from a faucet.
- • Saline enema—a solution of salt and water. For adults, 1 or 2 teaspoons of table salt is added to 500 to 1000 mL (milliliters) of tap water.
- • Soapsuds enema (SSE)—for adults, 3 to 5 mL of castile soap is added to 500 to 1000 mL of tap water.
- • Small-volume enema—the adult size has about 120 mL (4 ounces [oz]) of solution. The child size has about 60 mL (2 oz).
- • Oil-retention enema—has mineral, olive, or cottonseed oil. The adult size has about 120 mL (4 oz) of solution. Children usually receive 60 mL (2 oz).
Other enema solutions may be ordered. Consult with the nurse and use the agency's procedure manual to safely prepare and give enemas. You do not give enemas that contain drugs. Nurses give them.
See Delegation Guidelines: Enemas, p. 432.
See Promoting Safety and Comfort: Enemas, p. 432.
 The Cleansing Enema
The Cleansing Enema
Cleansing enemas clean the bowel of feces and flatus. They relieve constipation and fecal impaction. They are given before certain surgeries and diagnostic procedures. Cleansing enemas take effect in 10 to 20 minutes.
The doctor orders a tap water, saline, or soapsuds enema. An enemas until clear order means that enemas are given until the return solution is clear and free of stools. Agency policy may allow repeating enemas 2 or 3 times. The nurse tells you what enema to give and how many times to repeat the enema.
- • Tap water enema. The colon may absorb some of the water into the bloodstream. This creates a fluid imbalance. Only 1 tap water enema is given. Do not repeat the enema. Repeated enemas increase the risk of excessive fluid absorption.
- • Saline enema. The solution is similar to body fluid. However, some of the salt solution may be absorbed, causing a fluid imbalance. The body retains water from the excess salt.
- • Soapsuds enema. The SSE irritates the bowel's mucous lining. Repeated enemas can damage the bowel. So can using more than 3 to 5 mL of castile soap or stronger soaps.
See Focus on Children and Older Persons: The Cleansing Enema.
See procedure: Giving a Cleansing Enema.
 The Small-Volume Enema
The Small-Volume Enema
Small-volume enemas irritate and distend the rectum. This causes a BM. They are ordered for constipation or when the bowel does not need complete cleansing.
These enemas are ready to give. This solution is usually given at room temperature. To give the enema, squeeze and roll up the plastic container from the bottom. Do not release pressure on the bottle. Otherwise, solution is drawn from the rectum back into the bottle.
Urge the person to retain the solution until he or she needs to have a BM. This usually takes 5 to 10 minutes. Staying in the Sims' or left side-lying position helps retain the enema.
See procedure: Giving a Small-Volume Enema.
 The Oil-Retention Enema
The Oil-Retention Enema
Oil-retention enemas relieve constipation and fecal impaction. The oil softens feces and lubricates the rectum so feces pass with ease. The oil is retained for 30 minutes to 1 to 3 hours. Most oil-retention enemas are ready-to-use.
See Promoting Safety and Comfort: The Oil-Retention Enema.
See procedure: Giving an Oil-Retention Enema.
The Person With an Ostomy
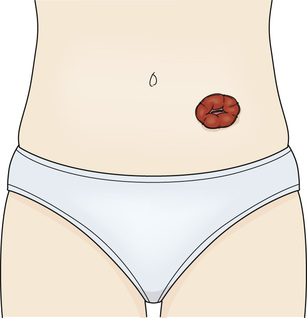
Sometimes part of the intestines is removed surgically. Cancer, bowel disease, and trauma (stab or bullet wounds) are common reasons. An ostomy is sometimes necessary. An ostomy is a surgically created opening that connects an internal organ to the body's surface. The surgically created opening seen on the body's surface is called a stoma (Fig. 26-10). A pouch is worn over the stoma to collect stools and flatus.
Colostomy
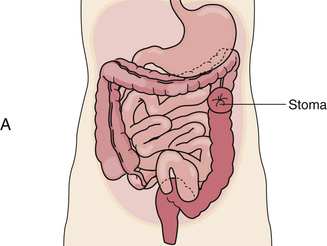
A colostomy is a surgically created opening (stomy) between the colon (colo) and the body's surface. Part of the colon is brought out onto the body's surface and a stoma is made. Feces and flatus pass through the stoma instead of the anus.
With a permanent colostomy, the diseased part of the colon is removed. A temporary colostomy gives the diseased or injured bowel time to heal. After healing, the bowel is surgically reconnected. The colostomy site depends on the site of disease or injury (Fig. 26-11). Stool consistency—liquid to formed—depends on the colostomy site. The more colon remaining to absorb water, the more solid and formed the stool. If the colostomy is near the end of the colon, stools are formed.
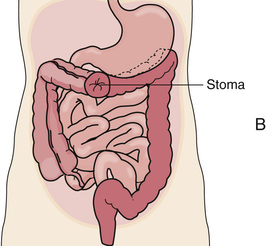
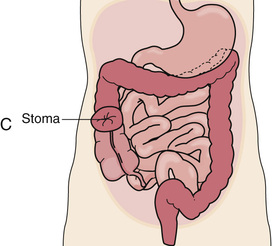
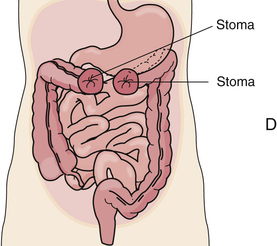
Stools irritate the skin. Skin care prevents skin breakdown around the stoma. The skin is washed and dried. Then a skin barrier is applied around the stoma. It prevents stools from having contact with the skin. The skin barrier is part of the pouch or a separate device.
Ileostomy
An ileostomy is a surgically created opening (stomy) between the ileum (small intestine [ileo]) and the body's surface. Part of the ileum is brought out onto the body's surface and a stoma is made. The entire colon is removed (Fig. 26-12, p. 438).
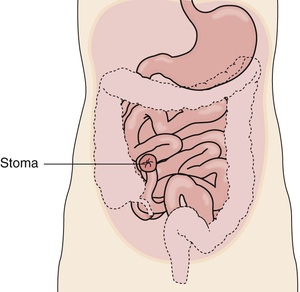
Liquid stools drain constantly from an ileostomy. Water is not absorbed because the colon was removed. Feces in the small intestine contain digestive juices that are very irritating to the skin. The ileostomy pouch must fit well. Stools must not touch the skin. Good skin care is required.
 Ostomy Pouches
Ostomy Pouches
A plastic pouch with an adhesive backing is applied to the skin. Some pouches are secured to ostomy belts (Fig. 26-13).
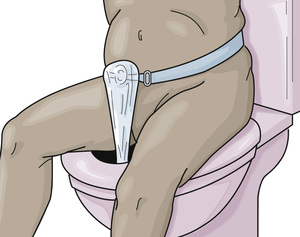
Pouches have a drain at the bottom that closes with a clip, clamp, or wire closure. The drain is opened to empty the pouch. The pouch is emptied when stools are present. It is opened when it balloons or bulges to release flatus. The drain is wiped with toilet tissue before closing.
The pouch is changed every 2 to 7 days and when it leaks. Frequent pouch changes can damage the skin.
Odors are prevented by:
- • Using odor-free pouches.
- • Performing good hygiene.
- • Emptying the pouch.
- • Avoiding gas-forming foods.
- • Putting deodorants into the pouch. The nurse tells you what to use.
The person wears normal clothes. However, tight garments can prevent feces from entering the pouch. Also, bulging from stools and flatus can be seen with tight clothes.
Peristalsis increases after eating and drinking. Therefore stomas are usually quiet after sleep. That is, expelling feces is less likely at this time. If the person showers or bathes with the pouch off, it is best done before breakfast. Showers and baths are delayed for 1 to 2 hours after applying a new pouch. This gives adhesive time to seal to the skin.
Do not flush pouches down the toilet. Follow agency policy for disposal.
See Focus on Children and Older Persons: Ostomy Pouches.
See Delegation Guidelines: Ostomy Pouches.
See Promoting Safety and Comfort: Ostomy Pouches.
See procedure: Changing an Ostomy Pouch.
Review Questions
Circle the BEST answer
a A person must have a BM every day.
b Stools are normally brown, soft, and formed.
c Diarrhea occurs when feces move slowly through the bowel.
d Constipation occurs when feces move quickly through the bowel.
2. Which should you ask the nurse to observe?
b The person's first BM of the day
d Liquid stool from an ileostomy
3. The prolonged retention and buildup of feces in the rectum is called
4. These measures promote normal BMs. Which is outside your role limits?
a Provide oral fluids according to the care plan.
b Assist with activity according to the care plan.
c Give drugs to control diarrhea.
d Provide privacy for bowel elimination.
5. A person has C. difficile. You should
a Disinfect care items with soap and water
b Use an alcohol-based hand rub before leaving the room
d Refuse to care for the person
a Bowel control and regular elimination
7. Your state and agency allow you to insert rectal suppositories. You insert a suppository
8. Which is used for a cleansing enema?
a Mineral, olive, or cottonseed oil
d Tap water, saline, or a soapsuds enema
9. Which is used for cleansing enemas in children?
b Place the person in the supine position
c Have the person void after giving the enema
11. In adults, the enema tube is inserted
12. A small-volume enema is retained
d Until the urge to have a BM is felt
13. Which care measure for an ostomy should you question?
b Perform good skin care around the stoma.
d Apply a skin barrier around the stoma.
14. An ostomy pouch is usually emptied
See Review Question Answers at the back of the text.






 inches in infants.
inches in infants.

