Atrial Fibrillation: Clinical Features, Mechanisms, and Management
Fred Morady, Douglas P. Zipes
Electrocardiographic Features
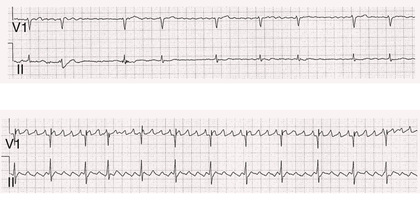
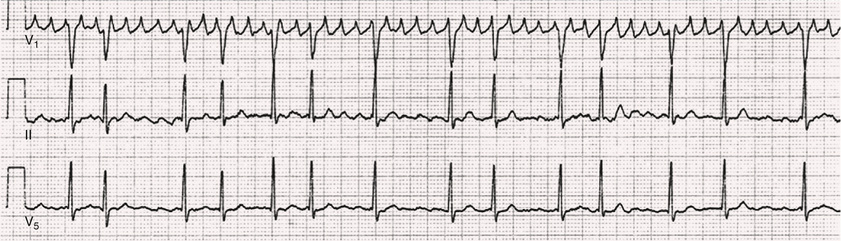
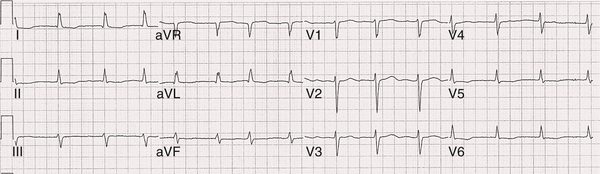
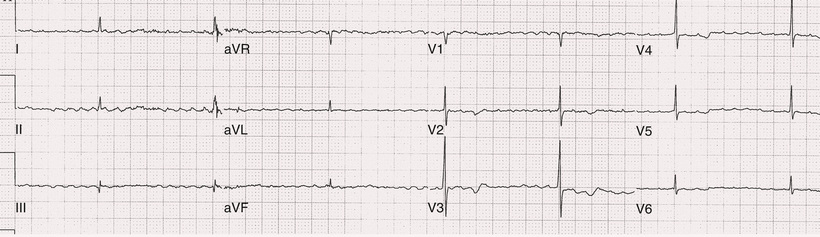
Atrial fibrillation (AF) is a supraventricular arrhythmia characterized electrocardiographically by low-amplitude baseline oscillations (fibrillatory or f waves from the fibrillating atria) and an irregularly irregular ventricular rhythm. The f waves, 300 to 600 beats/min, are variable in amplitude, shape, and timing. Atrial flutter waves have a rate of 250 to 350 beats/min and are constant in timing and morphology (Fig. 38.1). In lead V1, f waves sometimes appear uniform and can mimic flutter waves (Fig. 38.2). In some patients, f waves are very small and not perceptible on the electrocardiogram, and the diagnosis of AF is based on the irregularly irregular ventricular rhythm (Fig. 38.3).
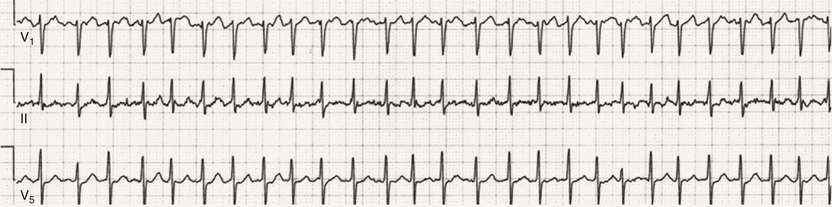
The ventricular rate during untreated AF typically is 100 to 160 beats/min. Patients with the Wolff-Parkinson-White (WPW) syndrome can experience ventricular rates during AF exceeding 250 beats/min because of conduction over the accessory pathway (see Chapter 37). The ventricular rate during AF can appear more regular when the rate is extremely rapid (>170 beats/min) (Fig. 38.4), when a junctional tachycardia independently controls the ventricles, when there is high-degree atrioventricular (AV) block with a regular escape rhythm (Fig. 38.5), or when the QRS complexes are fully paced. In these cases the diagnosis of AF is based on the presence of f waves. Infrequently, a junctional tachycardia can exhibit a Wenckebach exit block (often during digitalis toxicity) to cause a regularly irregular ventricular rate.
Classification of Atrial Fibrillation
Atrial fibrillation that terminates spontaneously within 7 days is termed paroxysmal, and AF present continuously for more than 7 days is called persistent. AF that persists for longer than 1 year is termed longstanding persistent, whereas longstanding AF refractory to cardioversion is termed permanent. However, “permanent AF” is not necessarily permanent in the literal sense because it may be successfully eliminated by surgical or catheter ablation.
Some patients with paroxysmal AF occasionally can have episodes that are persistent, and vice versa. The predominant form of AF determines how it should be categorized.
A confounding factor in the classification of AF is cardioversion and antiarrhythmic drug (AAD) therapy. For example, if a patient undergoes transthoracic cardioversion 24 hours after AF onset, it is unknown whether the AF would have persisted for more than 7 days. Furthermore, AAD therapy can change persistent AF into paroxysmal AF. It is generally thought that the classification of AF should not be altered on the basis of the effects of electrical cardioversion or AAD therapy.
Lone atrial fibrillation refers to AF that occurs in patients younger than 60 years who do not have hypertension or any evidence of structural heart disease. This designation is clinically relevant because patients with lone AF are at lower risk of thromboembolic complications, eliminating the necessity for anticoagulation. They also may be more likely to have familial or genetic causes. In addition, the absence of structural heart disease allows the safe use of rhythm-control drugs such as flecainide in patients with lone AF.
Paroxysmal AF also can be classified clinically on the basis of the autonomic setting in which it most often occurs. Approximately 25% of patients with paroxysmal AF have vagotonic AF, during which AF is initiated in the setting of high vagal tone, typically in the evening when the patient is relaxing or during sleep. Drugs exerting a vagotonic effect (e.g., digitalis) can aggravate vagotonic AF, and drugs with a vagolytic effect (e.g., disopyramide) may be particularly appropriate for prophylactic therapy. Adrenergic AF occurs in approximately 10% to 15% of patients with paroxysmal AF in the setting of high sympathetic tone, as during strenuous exertion. In patients with adrenergic AF, beta blockers not only provide rate control but can prevent the onset of AF. Most patients have a mixed or random form of paroxysmal AF, with no consistent pattern of onset. In some, alcohol can be a precipitant.
Epidemiology of Atrial Fibrillation
Atrial fibrillation is the most common arrhythmia treated in clinical practice and the most common arrhythmia for which patients are hospitalized; approximately 33% of arrhythmia-related hospitalizations are for AF. AF is associated with approximately a fivefold increase in the risk of cerebrovascular accident (stroke) and a twofold increase in the risk of all-cause mortality.1 AF also is associated with the development of heart failure and has been linked to sudden death.
The incidence of AF is age and gender related, ranging from 0.1% per year before age 40 to more than 1.5% per year in women and more than 2% per year in men older than 80. Congestive heart failure, aortic and mitral valve disease, left atrial enlargement, hypertension, and advanced age are independent risk factors for the development of AF, as are obesity and obstructive sleep apnea2 (see Chapter 87). Another risk factor is psoriasis, which, when severe, triples the risk of AF in patients younger than 50.3
A community-based cohort study in Olmstead County, Minnesota, reported that the age-adjusted incidence of AF per 1000 person-years increased significantly between 1980 and 2000 from 4.4 to 5.4 in men and from 2.4 to 2.8 in women.4 There was a relative increase of 0.6% per year in the age-adjusted AF incidence. An increase in obesity accounted for 60% of the age-adjusted increase in AF incidence. The number of patients with AF in the United States was estimated to be 3.2 million in 1980 and 5.1 million in 2000 and was projected to be 12.1 to 15.9 million in 2050, all of which are higher than previous estimates.
Mechanisms of Atrial Fibrillation
The mechanisms responsible for AF are complex. Triggering events may differ from maintenance mechanisms. In addition, the clinical phenotypes of paroxysmal, persistent, and longstanding persistent have different electrophysiologic characteristics because of remodeling and different clinical modulators that affect the substrate, such as heart failure, atrial stretch and ischemia, sympathovagal influences, inflammation, and fibrosis.
The two likely electrophysiologic mechanisms of AF are one or more automatic, triggered, or microreentrant foci, so-called drivers, which fire at rapid rates and cause fibrillation-like activity, and multiple reentrant circuits meandering throughout the atria, annihilating and reforming wavelets that perpetuate the fibrillation. In many studies the left atrium contains the site of dominant frequency discharge, with a left-to-right gradient. Both mechanisms may be present simultaneously and can change as the atria remodel. In the CONFIRM trial, computational maps were obtained in patients by signal processing of multiple electrograms recorded simultaneously during AF.5 This technique can reveal rotors and focal sources. A mean of 2.1 sources was found in 97% of 101 patients, with 70% being rotors and 30% being focal sources.
Rapid discharges from the pulmonary veins are the most common triggers of AF and also may play a perpetuating role, more so in paroxysmal AF than in persistent AF. This is why pulmonary vein isolation is particularly effective for elimination of paroxysmal AF. In persistent AF, changes in the atrial substrate, including interstitial fibrosis that contributes to slow, discontinuous, and anisotropic conduction, may give rise to complex fractionated atrial electrograms (CFAEs) and reentry. Therefore, pulmonary vein isolation alone often is insufficient to eliminate persistent AF (see Chapter 36).
Genetic Factors
Several mutations that are responsible for familial AF and that predispose to AF have been identified. These mutations cause a gain of function of repolarization potassium currents that results in shortening of atrial refractoriness and facilitation of atrial reentry. Multiple polymorphisms associated with idiopathic AF or structural heart disease or occurring postoperatively also have been identified.6 These polymorphisms are in genes that affect potassium and sodium channels, sarcolipin, the renin-angiotensin system, connexin-40, endothelial nitric oxide synthase, and interleukin-10. The end results are changes in calcium handling, fibrosis, conduction, and inflammation that predispose to AF.
Causes of Atrial Fibrillation
The majority of patients with AF have hypertension (usually with left ventricular hypertrophy; Chapters 46 and 47) or some other form of structural heart disease. In addition to hypertensive heart disease, the most common cardiac abnormalities associated with AF are ischemic heart disease (Chapter 58), mitral valve disease (Chapter 69), hypertrophic cardiomyopathy (Chapter 78), and dilated cardiomyopathy (Chapter 77). Less common causes of AF are restrictive cardiomyopathies such as amyloidosis (Chapter 77), constrictive pericarditis (Chapter 83), and cardiac tumors (see Chapter 95). Severe pulmonary hypertension often is associated with AF (Chapter 85).
Obstructive sleep apnea and obesity are associated with each other, and both independently increase the risk of AF (see Chapter 87). The possible mechanisms of AF in patients with sleep apnea include hypoxia, surges in autonomic tone, and hypertension.2 Available data suggest that atrial dilation and an increase in systemic inflammatory factors are responsible for the relationship between obesity and AF. Obesity also is associated with increased deposits of epicardial fat (see Chapter 50). The most likely mechanisms by which epicardial fat predisposes to AF are slow or anisotropic conduction caused by adipocyte infiltration into atrial muscle, atrial fibrosis caused by adipokines secreted by epicardial fat, and the local secretion of proinflammatory factors (e.g., IL-6, IL-8, TNF-α).7 The LEGACY study demonstrated that sustained weight loss and exercise can reduce the AF burden.8
AF can have causes that are temporary or reversible. The most common temporary causes are excessive alcohol intake (“holiday heart”), open heart or thoracic surgery, myocardial infarction (see Chapters 58 and 59), pericarditis (Chapter 83), myocarditis (Chapter 79), and pulmonary embolism (Chapter 84). The most common correctable cause is hyperthyroidism (Chapter 92).
AF is sometimes caused by tachycardia. Patients with tachycardia-induced AF most often have AV nodal reentrant tachycardia or a tachycardia related to WPW syndrome that degenerates into AF. AF in a patient with a history of rapid and regular palpitations before the onset of irregular palpitations or with a WPW electrocardiographic pattern should suggest tachycardia-induced AF. Treatment of the tachycardia that triggers the AF often (but not always) prevents recurrences of AF.
Clinical Features
The symptoms of AF range from none to severe and functionally disabling. The most common symptoms are palpitations, fatigue, dyspnea, effort intolerance, and lightheadedness. Polyuria can occur because of release of atrial natriuretic peptide. Many patients with symptomatic paroxysmal AF also have asymptomatic episodes, and some patients with persistent AF have symptoms only intermittently, making it difficult to assess accurately the frequency and duration of AF on the basis of symptoms.
An estimated 25% of patients with AF are asymptomatic, more often elderly patients and patients with persistent AF. Such patients sometimes are erroneously classified as having “asymptomatic” AF despite having symptoms of fatigue or effort intolerance. Because fatigue is a nonspecific symptom, it may not be clearly caused by persistent AF. A “diagnostic cardioversion” may be helpful by maintaining sinus rhythm for at least a few days to determine whether a patient feels better in sinus rhythm. This can provide a basis to pursue a rhythm-control versus rate-control strategy.
Syncope, an uncommon symptom of AF, can be caused by a long sinus pause on termination of AF in a patient with the sick sinus syndrome. Syncope also can occur during AF with a rapid ventricular rate because of neurocardiogenic (vasodepressor) syncope triggered by the tachycardia or because of a severe drop in blood pressure caused by a reduction in cardiac output.
Asymptomatic or minimally symptomatic AF patients are not prompted to seek medical care and can present with a thromboembolic complication such as stroke or the insidious onset of heart failure symptoms, eventually presenting in florid congestive heart failure.
The hallmark of AF on physical examination is an irregularly irregular pulse. Short R-R intervals during AF do not allow adequate time for left ventricular diastolic filling, resulting in a low stroke volume and the absence of palpable peripheral pulse. This results in a “pulse deficit,” during which the peripheral pulse is not as rapid as the apical rate. Other manifestations of AF on the physical examination are irregular jugular venous pulsations and variable intensity of the first heart sound.
Diagnostic Evaluation
In a patient who describes irregular or rapid palpitations suggestive of paroxysmal AF, ambulatory monitoring is useful to document whether AF is responsible for the symptoms. If the symptoms occur on a daily basis, a 24-hour Holter recording is appropriate. However, extended monitoring for 2 to 4 weeks with an event monitor or by mobile cardiac outpatient telemetry is appropriate for patients whose symptoms are sporadic (see Chapter 32).
The history should be directed at determination of the type and severity of symptoms, the first onset of AF, whether the AF is paroxysmal or persistent, the triggers of AF, whether the episodes are random or occur at particular times (e.g., during sleep), and the frequency and duration of episodes. When it is unclear from the history, 2 to 4 weeks of ambulatory monitoring with an autotrigger event monitor or by mobile cardiac outpatient telemetry is useful to determine whether AF is paroxysmal or persistent and to quantitate the AF burden in patients with paroxysmal AF. The history also should be directed at identification of potentially correctible causes (e.g., hyperthyroidism, excessive alcohol intake), structural heart disease, and comorbidities.
Laboratory testing should include thyroid, liver, and renal function tests. Echocardiography always is appropriate to evaluate atrial size and left ventricular function and to look for left ventricular hypertrophy, congenital heart disease (see Chapter 75), and valvular heart disease (Chapters 68 and 69). Chest radiography is appropriate if the history or physical examination is suggestive of pulmonary disease (Chapter 15). A stress test is appropriate for evaluation of ischemic heart disease in at-risk patients (Chapter 13).
Prevention of Thromboembolic Complications
Risk Stratification
A major goal of therapy in patients with AF is to prevent thromboembolic complications such as stroke. Warfarin and other oral anticoagulants are more effective than aspirin for prevention of thromboembolic complications.9 However, because of the risk of hemorrhage from anticoagulants, their use should be limited to patients whose risk of thromboembolic complications is greater than the risk of hemorrhage. Therefore, it is useful to risk stratify patients with AF to identify appropriate candidates for anticoagulation.
The strongest predictors of ischemic stroke and systemic thromboembolism are a history of stroke or transient ischemic episode and mitral stenosis. When patients with AF and a prior ischemic stroke are treated with aspirin, the risk of another stroke is very high, in the range of 10% to 12% per year. At the other end of the risk spectrum are patients with lone AF, whose cumulative 15-year risk of stroke is in the range of 1% to 2%. Aside from prior stroke, the best-established risk factors for stroke in patients with nonvalvular AF are diabetes (relative risk [RR], 1.7), hypertension (RR, 1.6), heart failure (RR, 1.4), and age 70 or older (RR, 1.4 per decade).2
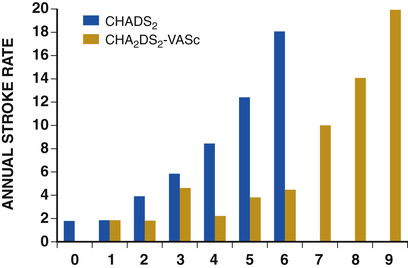
A simple clinical scheme to risk stratify patients on the basis of the major risk factors is the CHADS2 (cardiac failure, hypertension, age, diabetes, stroke) score. Each of the first four risk factors counts as 1 point, and a prior stroke or transient ischemic event is 2 points. There is a direct relationship between the CHADS2 score and the annual risk of stroke in the absence of aspirin or warfarin therapy. The clinical value of the CHADS2 score lies in its simplicity and predictive value. However, the CHADS2 score has been superseded by the CHA2DS2-VASc score because it more accurately discriminates low-risk from intermediate-risk patients.10 In this risk-scoring system, cardiac failure, hypertension, diabetes, vascular disease, age 65 to 74 years, and female gender are 1 point each, and age 75 or older and prior stroke or transient ischemic event are 2 points. The annual risk of stroke is zero or close to zero when the CHA2DS2-VASc score is 0, compared to approximately 2% when the CHADS2 score is 0.11 A score of 1 is associated with an annual stroke risk of approximately 3% with the CHADS2 score, compared to 0.7% with the CHA2DS2-VASc score (Fig. 38.6).
Renal failure also is an independent risk factor for stroke in patients with AF.12 The relative risk of a thromboembolic event in the absence of anticoagulation was 1.4 in patients with non–end-stage chronic kidney disease and 1.8 in patients requiring hemodialysis or a renal transplant. The predictive strength of chronic kidney disease for a thromboembolic event appears to be equivalent to that of heart failure and advanced age. Therefore, it may be appropriate to take into account chronic kidney disease in evaluating the risk profile of a patient with AF.
By definition, the burden of AF is greater in patients with persistent AF than in patients with paroxysmal AF. It may seem reasonable to assume that the risk of stroke is lower in patients with occasional episodes of self-limited AF than in patients with AF continuously. However, the available data in fact indicate that the risk of thromboembolic complications is the same in patients with paroxysmal and persistent AF. Accordingly, guideline recommendations for anticoagulation are the same in patients with paroxysmal and persistent AF.2,13
Current dual-chamber pacemakers and implantable cardioverter-defibrillators (ICDs) are capable of detecting short episodes of asymptomatic AF that otherwise would not have been detected clinically. In a recent multicenter prospective study, subclinical atrial tachyarrhythmias (atrial rate >190 beats/min for >6 minutes) were detected by device interrogation in 10.1% of patients 65 years or older with hypertension and no history of AF who received a pacemaker or ICD.14 Subclinical atrial tachyarrhythmias were independently associated with a 2.5-fold increase in the risk of stroke.
An important consideration in patients treated with an oral anticoagulant is the risk of bleeding. Several risk-scoring systems have been developed to assess a patient's susceptibility to hemorrhagic complications. The scoring system with the best balance of simplicity and accuracy is the HAS-BLED score.15 The components of this score are hypertension, abnormal renal or liver function, stroke, bleeding history or predisposition, labile international normalized ratio (INR), elderly (>75 years), and concomitant drug (antiplatelet agent or nonsteroidal anti-inflammatory drug) or alcohol use. Each of these components is 1 point. As the score increases from 0 to the maximum of 9, there is a stepwise increase in the risk of bleeding in patients treated with warfarin. For example, in one study the annual rate of major bleeds was 1.1% in patients with a HAS-BLED score of 0, 3.7% with a score of 3, and 12.5% with a score of 5.16
In two large-scale cohort studies of 132,372 and 170,292 patients with nonvalvular AF, the CHA2DS2-VASc and HAS-BLED scores were calculated for each patient.17,18 The net clinical benefit of warfarin was defined as the number of strokes off warfarin minus the number of intracranial bleeds on warfarin. In both studies, warfarin was associated with a net clinical benefit except when the CHA2DS2-VASc score was 0. In patients with a CHA2DS2-VASc score of 1 or more, the risk of stroke in the absence of warfarin exceeded the number of bleeding complications during treatment with warfarin.
Despite the results of these large cohort studies, the decision to anticoagulate a patient in clinical practice should be individualized. At times it may be appropriate not to anticoagulate a patient with a CHA2DS2-VASc score 1 or greater. For example, the annual risk of stroke in a patient with a CHA2DS2-VASc score of 2 is approximately 2%, which usually justifies the use of warfarin. However, if that patient has a HAS-BLED score of 5 or more, which is associated with an annual risk of major bleeding of 12% or greater, it would be imprudent to treat that patient with warfarin.
The HAS-BLED score was developed and validated in patients anticoagulated with warfarin. Except for labile INR, the components of the HAS-BLED score likely also apply to patients who are anticoagulated with one of the novel (new) oral anticoagulants (NOACs), either a direct thrombin inhibitor or factor Xa inhibitor. However, clinical trials have indicated that the risk of major bleeding is lower with NOACs than with warfarin (see later). Accordingly, the benefit of anticoagulation with warfarin is estimated to be greater than the risk of bleeding when the annual stroke risk is at least 1.7%, compared to an annual stroke risk of at least 0.9% in patients treated with a NOAC.19
Aspirin and Other Antithrombotic Agents
Aspirin does not prevent thromboembolic complications as effectively as warfarin or NOACs in patients with AF. In a meta-analysis of five randomized clinical trials, aspirin did not significantly reduce the risk of stroke compared to placebo in patients with AF.9 In a large cohort study of patients with non-valvular AF, aspirin had no therapeutic efficacy for preventing strokes.17 Therefore, if aspirin is used for prophylactic therapy, this should be only in patients at lowest risk of thromboembolic complications (CHA2DS2-VASc score of 0). However, the 2014 American College of Cardiology (ACC), American Heart Association (AHA), and /Heart Rhythm Society (HRS) guidelines for management of patients with AF recommend that for patients with nonvalvular AF and a CHA2DS2-VASc score of 0, it is reasonable to omit all antithrombotic therapy, including aspirin. When the CHA2DS2-VASc score is 1, the guidelines recommend that either no antithrombotic therapy or treatment with an oral anticoagulant or aspirin may be considered.2 Because of the negligible therapeutic effect of aspirin, a risk of bleeding complications that is close to the risk of oral anticoagulants, and the ability of the CHA2DS2-VASc score to accurately identify low-risk patients, the most recent guidelines of the European Society of Cardiology (ESC) recommend no antithrombotic therapy when the CHA2DS2-VASc score is 0 and an individualized decision between no antithrombotic therapy versus an oral anticoagulant when the CHA2DS2-VASc score is 1.20
If aspirin is used for stroke prevention in patients with AF, the appropriate daily dose is 81 to 325 mg/day. No data indicate superiority of a particular dose for prevention of thromboembolism.
In patients with a CHADS2 score greater than 1 who are not able to tolerate anticoagulation with warfarin or a NOAC, combination therapy with aspirin and the platelet inhibitor clopidogrel is more efficacious than aspirin alone for prevention of thromboembolic complications.21 The potential benefit of combination therapy with aspirin plus clopidogrel may outweigh the increased risk of bleeding complications in high-risk patients who are not suitable candidates for warfarin or a NOAC.
Warfarin and Direct Thrombin Inhibitors
A meta-analysis of the major randomized clinical trials that compared warfarin with placebo for prevention of thromboembolism in patients with AF demonstrated that warfarin reduced the risk of all strokes (ischemic and hemorrhagic) by approximately 60%.9 The target INR should be 2.0 to 3.0. This range of INRs provides the best balance between stroke prevention and hemorrhagic complications. In clinical practice, maintenance of the INR in therapeutic range has been challenging, and a large proportion of patients often have an INR of less than 2.0. A large prospective study of community-based practices demonstrated that the mean time in therapeutic range in patients treated with warfarin was only 66% and that the time in therapeutic range was less than 60% in 34% of patients.22 Maintaining the INR at a level of 2.0 or higher is important because even a relatively small decrease in INR from 2.0 to 1.7 more than doubles the risk of stroke.
The annual risk of a major hemorrhagic complication during anticoagulation with warfarin is in the range of 1% to 2%, and a strong predictor of major bleeding events is an INR greater than 3.0. For example, the risk of intracranial bleeding is approximately twice as high at an INR of 4.0 than 3.0. This emphasizes the importance of maintaining the INR in the range of 2.0 to 3.0.
Some studies have indicated that advanced age can be a risk factor for intracranial hemorrhage in patients with AF treated with warfarin. The concern of hemorrhagic complications may lead some clinicians to favor the use of aspirin over warfarin or one of the NOACs in elderly patients. However, the available data indicate that the risk-to-benefit ratio of warfarin and the NOACs is more favorable than that of aspirin even in patients older than 75.23
It is well established that genetic factors influence the dose of warfarin required to maintain the INR within therapeutic range. Several single-nucleotide polymorphisms that affect warfarin metabolism have been identified. Algorithms based on pharmacogenetic and clinical factors improve the accuracy of warfarin dose initiation compared with algorithms based only on clinical factors.24 Additional studies are required to determine whether the clinical benefits of genotyping of warfarin candidates justify the cost of genetic testing (see Chapter 8).
Novel Oral Anticoagulants
Direct thrombin inhibitors and factor Xa inhibitors have several advantages over vitamin K antagonists such as warfarin, the most notable being a fixed dosing regimen that eliminates the need for monitoring of a laboratory test such as the INR. Dabigatran, an oral direct thrombin inhibitor, and rivaroxaban and apixaban, factor Xa inhibitors, are approved by the U.S. Food and Drug Administration (FDA) for prevention of stroke/embolism in patients with nonvalvular AF. Randomized clinical trials demonstrated that each of these three NOACs is noninferior or superior to warfarin in efficacy and safety in patients with nonvalvular AF who had risk factors for stroke.25 One of the most serious risks of anticoagulation is intracranial hemorrhage. Recent studies have indicated that the risk of intracranial hemorrhage is about 50% lower with NOACs compared to warfarin.26
The NOACs, in addition to eliminating the need for laboratory monitoring, have other advantages over warfarin: fewer drug interactions, no food interactions, and rapid onset of action that obviates the need for bridging therapy. However, they also have some disadvantages compared to warfarin: higher cost, more gastrointestinal side effects in the case of dabigatran, twice-daily dosing for dabigatran and apixaban, and the absence of a readily available laboratory test to verify compliance. Furthermore, these agents cannot be used safely in patients with severe renal disease. Another limitation is that there are no specific reversal agents for all the NOACs. The FDA recently approved idarucizumab, an antibody fragment that reverses the anticoagulant effects of dabigatran within minutes.27 Prothrombin complex concentrate can reverse the anticoagulant effect of the NOACs,28 but specific and rapid-acting antidotes for rivaroxaban and apixaban are not yet available. Nonetheless, for many patients with AF, the advantages of the newer anticoagulants outweigh the disadvantages.
Older studies showed underutilization of warfarin in patients with AF and risk factors for stroke. The inconvenience and potential risks of warfarin likely contributed to its underutilization. However, underutilization of an oral anticoagulant in patients with AF continues to be the case even with the advent of NOACs and even in patients with a CHA2DS2-VASc score 3 or higher.29
The major professional societies have incorporated recommendations regarding the use of the factor Xa and direct thrombin inhibitors into their most recent updated guidelines for the management of AF. The ACC/AHA/HRS practice guidelines recommend dabigatran, rivaroxaban, and apixaban as useful alternatives to warfarin for prevention of stroke or systemic embolism in patients with nonvalvular paroxysmal or persistent AF and risk factors for stroke.2 This recommendation is limited to patients without a prosthetic valve, with creatinine clearance higher than 15 mL/min, and without impaired clotting function from advanced liver disease. The ESC guidelines recommend dabigatran, rivaroxaban, or apixaban for patients with AF in whom maintenance of a therapeutic INR during treatment with warfarin is difficult and state that one of these NOACs should be considered instead of dose-adjusted warfarin for most patients with nonvalvular AF, based on their net clinical benefits.13 These guidelines recommend that the NOACs not be used in patients with a creatinine clearance of less than 30 mL/min.
The results of a prospective randomized clinical trial and post hoc analysis of three other randomized clinical trials indicate that the NOACs are as effective as warfarin for prevention of thromboembolic complications associated with cardioversion.30 This is the case regardless of whether a transesophageal echocardiogram is performed before cardioversion to look for left atrial thrombus.
The onset of action of dabigatran, rivaroxaban, and apixaban is approximately 1.5 to 2 hours after a dose. The half-life of dabigatran and apixaban ranges between 10 and 16 hours, and that of rivaroxaban is 5 to 9 hours. These anticoagulants lose most of their effect by 24 hours after discontinuation. The rapid onset of action and washout eliminates the need for bridging therapy with heparin when treatment with one of the NOACs is interrupted for a surgical or invasive procedure. Recent data indicate that the risk of major periprocedural complications does not differ significantly between patients who undergo radiofrequency catheter ablation of AF during uninterrupted therapy with warfarin and patients anticoagulated with a NOAC when the last dose of the NOAC is 1 to 2 days before the procedure and dosing is restarted 6 hours after the procedure, without bridging therapy.31
Low-Molecular-Weight Heparin
Low-molecular-weight heparin (LMWH) has a longer half-life than unfractionated heparin and a predictable antithrombotic effect that is attained with a fixed dosage administered subcutaneously twice daily. Because LMWH can be self-injected outside the hospital, it is a practical alternative to unfractionated heparin for initiation of anticoagulation with warfarin in patients with AF. Bridging therapy with LMWH be continued until the INR is 2.0 or higher.
Because of its high cost, LMWH rarely is used in clinical practice as a substitute for long-term conventional anticoagulation. LMWH typically is used as a temporary bridge to therapeutic anticoagulation when therapy with warfarin is initiated or in high-risk patients for a few days before and after a medical or dental procedure when anticoagulation with warfarin has been suspended.
Excision or Closure of the Left Atrial Appendage
Approximately 90% of left atrial thrombi form in the left atrial appendage (LAA), and therefore successful excision or closure of the LAA should greatly reduce the risk of thromboembolic complications in patients with AF. Surgical techniques consist of either excision or closure by suturing or stapling. The efficacy of these techniques is variable and probably dependent on both the technique and the operator.32 Transesophageal echocardiography (TEE) should be performed after surgical closure of the LAA to confirm successful closure before discontinuation of anticoagulation.
In recent years, several percutaneous LAA occlusion and suturing devices have been developed as alternatives to surgical closure techniques. These devices have their greatest utility in high-risk AF patients who cannot tolerate or who refuse to take an oral anticoagulant.
The only percutaneous occlusion device approved by the FDA specifically for stroke prevention as an alternative to warfarin is the WATCHMAN (Boston Scientific, Marlborough, Massachusetts). This nitinol plug covered with fenestrated fabric became widely available for clinical use after FDA approval in 2015. After implantation of the WATCHMAN using femoral vein access and transseptal catheterization, anticoagulation with warfarin is necessary for at least 45 days, at which time anticoagulation can be discontinued if there is no TEE evidence of peridevice flow. The most recent clinical trial and registry data indicated an implantation success rate of 95% and a procedural complication rate of approximately 2% to 3%, the most common complication being pericardial effusion requiring drainage.32 Approximately 95% of patients are able to discontinue warfarin at 45 days after implant. Clinical trial data have demonstrated noninferiority of the WATCHMAN compared to warfarin for stroke prevention and a significantly lower risk of hemorrhagic stroke during long-term follow-up.32
Another device used in the United States for LAA occlusion is the LARIAT (Sentreheart, Redwood City, California). This device has FDA approval as a method for soft tissue approximation (not stroke prevention) and has been used “off label” in clinical practice in the United States and Europe for LAA occlusion. A guidewire with a magnetic tip is inserted into the left atrium after transseptal catheterization and is positioned at the tip of the LAA and functions as a rail for an epicardial snare. Entry into the pericardial space is attained using a percutaneous approach. A snare with a pretied suture is inserted into the pericardial space and guided toward the LAA. The pretied suture then is tightened to occlude the LAA. In a large multicenter registry, complete LAA closure was achieved in 94% of 712 patients.33 There was one procedure-related death, and cardiac perforation occurred in 3.4% of patients, with open heart surgery required to repair the perforation in 1.4% of patients.33 Clinical trial data demonstrating efficacy of the LARIAT for stroke prevention are lacking.
Acute Management of Atrial Fibrillation
Patients who present to the emergency department because of AF often have a rapid ventricular rate, and control of the ventricular rate is most rapidly achieved with intravenous diltiazem or esmolol. If the patient is hemodynamically unstable, immediate transthoracic cardioversion may be appropriate. Cardioversion should be preceded by TEE to rule out a left atrial thrombus if the AF has been present for longer than 48 hours or if the duration is unclear and the patient is not already anticoagulated.
If the patient is hemodynamically stable, the decision to restore sinus rhythm by cardioversion is based on several factors, including symptoms, prior AF episodes, age, left atrial size, and current AAD therapy. For example, in an elderly patient whose symptoms resolve once the ventricular rate is controlled and who already has had early recurrences of AF despite rhythm-control drug therapy, further attempts at cardioversion usually are not appropriate. On the other hand, cardioversion usually is appropriate for patients with symptomatic AF who present with a first episode of AF or who have had long intervals of sinus rhythm between prior episodes.
If cardioversion is decided for a hemodynamically stable patient who presents with AF that does not appear to be self-limited, two management decisions must be made: early versus delayed cardioversion and pharmacologic versus electrical cardioversion.
The advantages of early cardioversion are rapid relief of symptoms, avoidance of the need for TEE or therapeutic anticoagulation for 3 to 4 weeks before cardioversion if cardioversion is performed within 48 hours of AF onset, and possibly a lower risk of early AF recurrence because of less atrial remodeling (see Chapter 36). A reason to defer cardioversion is the unavailability of TEE in an unanticoagulated patient with AF of unclear duration or duration more than 48 hours. Other reasons include a left atrial thrombus by TEE (see Chapter 14), a suspicion (based on prior AF episodes) that AF will convert spontaneously within a few days, or a correctable cause of AF (e.g., hyperthyroidism).
When cardioversion is performed early in the course of an episode of AF, there is the option of either pharmacologic or electrical cardioversion. Pharmacologic cardioversion has the advantage of not requiring general anesthesia or deep sedation. In addition, the probability of an immediate recurrence of AF is lower with pharmacologic cardioversion than with electrical cardioversion. However, pharmacologic cardioversion is associated with the risk of adverse drug effects and is not as effective as electrical cardioversion. Pharmacologic cardioversion is unlikely to be effective if the duration of AF is longer than 7 days.
Drugs that can be administered intravenously for cardioversion of AF consist of ibutilide, procainamide, and amiodarone. For AF episodes less than 2 to 3 days in duration, efficacy is approximately 60% to 70% for ibutilide, 40% to 50% for amiodarone, and 30% to 40% for procainamide. To minimize the risk of QT prolongation and polymorphic ventricular tachycardia (torsades de pointes; see Chapter 39), the use of ibutilide should be limited to patients with an ejection fraction greater than 35%.
Acute pharmacologic cardioversion of AF also can be attempted with oral drugs in patients without structural heart disease. The most common oral agents for acute conversion of AF are propafenone (300 to 600 mg) and flecainide (100 to 200 mg). It is prudent to administer these drugs under surveillance at first use. If no adverse drug effects are observed, the patient may then be an appropriate candidate for episodic, self-administered AAD therapy on an outpatient basis.
The efficacy of transthoracic cardioversion is approximately 95%. Biphasic waveform shocks convert AF more effectively than monophasic waveform shocks and allow the use of lower energy shocks, resulting in less skin irritation. An appropriate first-shock strength using a biphasic waveform is 150 to 200 J, followed by higher output shocks if needed. If a 360-J biphasic shock is unsuccessful, ibutilide should be infused before another shock is delivered because it lowers the defibrillation energy requirement and improves the success rate of transthoracic cardioversion.
Transthoracic cardioversion can fail to restore sinus rhythm. An increase in shock strength or infusion of ibutilide often results in successful repeat cardioversion. The second type of failure is an immediate recurrence of AF within a few seconds of successful conversion to sinus rhythm. This occurs in approximately 25% for episodes less than 24 hours in duration and 10% for episodes more than 24 hours in duration. For this type of cardioversion failure, an increase in shock strength is of no value. If the patient has not been receiving an oral rhythm-control agent, infusion of ibutilide may be helpful to prevent an immediate recurrence of AF.
Regardless of whether cardioversion is performed pharmacologically or electrically, therapeutic anticoagulation is necessary for 3 weeks or more before cardioversion to prevent thromboembolic complications if the AF has been ongoing for more than 48 hours. If the time of onset of AF is unclear, for the sake of safety, the AF duration should be assumed to be more than 48 hours. These patients should be therapeutically anticoagulated for 4 weeks after cardioversion to prevent thromboembolic complications that may occur because of atrial stunning. If the duration of AF is known to be less than 48 hours, cardioversion can be performed without anticoagulation. To improve the safety margin, it may be appropriate to use a 24-hour cutoff for the AF duration that allows safe cardioversion without anticoagulation. Postcardioversion atrial stunning and thromboembolic events are possible in patients with comorbidities even when the AF duration is less than 48 hours, and anticoagulation for 4 weeks is appropriate when the CHA2DS2-VASc score is more than 2.34
When AF duration exceeds 48 hours or is unclear, an alternative to 3 weeks of therapeutic anticoagulation before cardioversion is anticoagulation with heparin and TEE to check for a left atrial thrombus. If no thrombi are seen, the patient can be cardioverted safely but still requires 4 weeks of therapeutic anticoagulation after cardioversion to prevent thromboembolism related to atrial stunning. The major clinical benefit of the TEE-guided approach over the conventional approach is that sinus rhythm is restored several weeks sooner. Compared with the conventional approach, the TEE approach has not been found to reduce the risk of stroke or major bleeding or to affect the proportion of patients still in sinus rhythm at 8 weeks after cardioversion.
Long-Term Management of Atrial Fibrillation
Pharmacologic Rate Control Versus Rhythm Control
Several randomized studies have compared a rate-control strategy with a rhythm-control strategy in patients with AF. Overall, these studies have demonstrated a significantly lower rate of rehospitalization with a rate-control strategy, but no significant differences in other major outcomes, such as all-cause mortality, strokes, bleeding events, worsening heart failure, or quality of life.35
The results of these randomized studies should not be applied systematically to all patients with AF. It is important to note that many patients in the rhythm-control arms of these studies continued to have AF, and that the possible beneficial effects of sinus rhythm over AF could have been negated by adverse effects of the AADs. Furthermore, many of the patients included in these studies were elderly and had minimal or no symptoms from the AF.
The decision to pursue a rhythm-control strategy versus a rate-control strategy should be individualized with consideration of several factors. These include the nature, frequency, and severity of symptoms; the length of time that AF has been present continuously in patients with persistent AF; left atrial size; comorbidities; the response to prior cardioversions; age; the side effects and efficacy of the AADs already used to treat the patient; and the patient's preference.
The randomized studies convincingly demonstrated that a rate-control strategy is preferable to a rhythm-control strategy in asymptomatic or minimally symptomatic patients age 65 or older. When the AF is persistent, it is reasonable to restore sinus rhythm with AAD therapy or transthoracic cardioversion at least once in patients younger than 65 and in patients 65 or older who are symptomatic from the AF despite adequate heart rate control. If the AF has been continuous for more than 1 year or if the left atrial diameter is very large (>5.0 cm), there is a high probability of an early recurrence of AF, and this should be taken into account in deciding on the best strategy. After cardioversion, the decision to maintain the patient on AAD therapy to delay the next episode of AF is based on the patient's preference, the perceived risk of an early recurrence of AF, and the duration of sinus rhythm between prior cardioversions. Treatment by cardioversion without daily AAD therapy is acceptable if episodes of AF are separated by at least 6 months. Treatment with a rhythm-control drug usually is appropriate when AF recurs within a few months of cardioversion.
The most realistic goal of AAD therapy in patients with persistent AF is to delay the onset of the next episode by at least several months, not for several years. It often is appropriate to continue therapy with a particular AAD at a constant dosage if recurrences of AF are limited to approximately one episode per year.
In patients with symptomatic paroxysmal AF, the aggressiveness with which a rhythm-control strategy is pursued should be dictated by the frequency and severity of symptoms and how well AAD therapy is tolerated. Drug therapy is more likely to be judged successful when patients are reminded that the goal of therapy is not complete suppression of AF but a clinically meaningful reduction in frequency, duration, and severity of episodes.
A pharmacologic rhythm-control strategy does not necessarily require daily AAD therapy. Episodic drug therapy (the “pill-in-the-pocket” approach) is useful for patients whose episodes of AF are relatively infrequent. Episodic drug therapy is a reasonable option for patients who are clearly aware of the onset and termination of AF episodes and who have lone AF or only minimal structural heart disease. A typical AAD regimen consists of a class IC drug (flecainide or propafenone) plus a short-acting beta blocker (e.g., propranolol) or calcium channel blocker (e.g., verapamil) for rate control. Many patients with infrequent episodes prefer this approach because it eliminates the inconvenience, cost, and possible side effects of daily prophylactic therapy. However, patients who are disabled by severe symptoms during AF may prefer daily prophylactic therapy even if episodes are infrequent.
Many patients with symptomatic AF also have asymptomatic episodes. Therefore, daily antithrombotic therapy to prevent thromboembolic events is appropriate for all patients being treated for recurrent AF, whether it is persistent or paroxysmal and whether a rhythm-control or rate-control strategy is employed. The choice of no therapy, an oral anticoagulant, aspirin, or aspirin plus clopidogrel should be dictated by an analysis of risk factors.
Pharmacologic Rate Control
An excessively rapid ventricular rate during AF often results in uncomfortable symptoms and decreased effort tolerance and can cause a tachycardia-induced cardiomyopathy if it is sustained for several weeks to months. Optimal heart rates during AF vary with age and should be similar to the heart rates that a patient would have at a particular degree of exertion during sinus rhythm. Heart rate control must be assessed both at rest and during exertion. At rest, the ideal ventricular rate during AF is in the range of 60 to 80 beats/min. During mild to moderate exertion (e.g., rapid walking), the target rate should be 90 to 115 beats/min. During strenuous exercise, the ideal rate is in the range of 120 to 160 beats/min. Optimal assessment of the degree of heart rate control is provided by an ambulatory 24-hour Holter recording or an exercise test.
Oral agents available for long-term heart rate control in patients with AF are digitalis, beta blockers, calcium channel antagonists, and amiodarone. The first-line agents for rate control are beta blockers and the calcium channel antagonists verapamil and diltiazem. A combination is often used to improve efficacy or to limit side effects by allowing the use of smaller dosages of the individual drugs. In patients with sinus node dysfunction and tachycardia-bradycardia syndrome, the use of a beta blocker with intrinsic sympathomimetic activity (pindolol, acebutolol) may provide rate control without aggravating sinus bradycardia.
Digitalis may adequately control the rate at rest but often does not provide adequate rate control during exertion. However, its use for rate control of AF is controversial because digitalis has been shown to increase the risk of all-cause mortality, particularly among patients with AF.36
Amiodarone is much less frequently used for rate control than the other negative dromotropic agents because of the risk of organ toxicity associated with long-term therapy. Amiodarone can be an appropriate choice for rate control if the other agents are not tolerated or are ineffective. For example, amiodarone would be an appropriate choice for a patient with persistent AF, heart failure, and reactive airway disease who cannot tolerate either a calcium channel antagonist or a beta blocker and who has a rapid ventricular rate despite treatment with digitalis.
Strict heart rate control can be difficult to achieve pharmacologically. Based on the results of a single randomized study that demonstrated no significant differences in major outcomes between a lenient rate-control strategy (resting rate <110 beats/min) and a strict rate-control strategy (resting heart rate <80 beats/min, rate during moderate exercise <110 beats/min), a lenient rate-control strategy is reasonable if the patient remains asymptomatic and left ventricular systolic function is not compromised.2 However, strict rate control often still is an appropriate goal for relief of symptoms, improvement in functional capacity, and avoidance of tachycardia-induced cardiomyopathy during long-term follow-up.
Pharmacologic Rhythm Control
The results of published studies on the efficacy of AADs for AF suggest that all the available drugs except amiodarone have similar efficacy and are associated with a 50% to 60% reduction in the odds of recurrent AF during 1 year of treatment. The one drug that stands out as having higher efficacy than the others is amiodarone. In studies that directly compared amiodarone with sotalol or class I drugs, amiodarone was 60% to 70% more effective in suppressing AF. However, because of the risk of organ toxicity, amiodarone is not appropriate first-line drug therapy for many patients with AF. Because the efficacy of rhythm-control agents other than amiodarone is in the same general range, the selection of an AAD to prevent AF often is dictated by the issues of safety and side effects.
Ventricular proarrhythmia from class IA agents (quinidine, procainamide, disopyramide) and class III agents (sotalol, dofetilide, dronedarone, amiodarone) is manifested as QT prolongation and polymorphic ventricular tachycardia (torsades de pointes). Risk factors for this type of proarrhythmia include female gender, left ventricular dysfunction, and hypokalemia. The risk of torsades de pointes appears to be much lower with dronedarone and amiodarone than with the other class III drugs. The ventricular proarrhythmia from class IC agents (flecainide and propafenone) manifests as monomorphic ventricular tachycardia, sometimes associated with widening of the QRS complex during sinus rhythm but not QT prolongation. Drugs most likely to result in ventricular proarrhythmia are quinidine, flecainide, sotalol, and dofetilide. In controlled studies, these agents increased the risk of ventricular tachycardia by a factor of 2 to 6.
Adverse drug events or side effects resulting in discontinuation of drug therapy are fairly common with rhythm-control drugs, with discontinuation rates reported to be as high as 40%.37
The best options for drug therapy to suppress AF depend on the patient's comorbidities. In patients with lone AF or minimal heart disease (e.g., mild left ventricular hypertrophy), flecainide, propafenone, sotalol, and dronedarone are reasonable first-line drugs, and amiodarone and dofetilide can be considered if the first-line agents are ineffective or not tolerated. In patients with substantial left ventricular hypertrophy (left ventricular wall thickness >15 mm), the hypertrophy heightens the risk of ventricular proarrhythmia, and the safest choices for drug therapy are amiodarone and dronedarone.2 In patients with coronary artery disease (CAD), several of the class I drugs have been found to increase the risk of death, and the safest first-line options are dofetilide and sotalol, with amiodarone reserved for use as a second-line agent. In patients with heart failure, several AADs have been associated with increased mortality, and the only two drugs known to have a neutral effect on survival are amiodarone and dofetilide (see Chapter 36).
At the time of FDA approval, it was known that dronedarone increases mortality in NYHA Class IV heart failure or patients with a recent episode of decompensated heart failure. After approval, the categories of patients in which dronedarone is contraindicated expanded based on the results of a randomized clinical trial that was discontinued prematurely because of major adverse drug effects.38 Dronedarone should be avoided in patients age 65 or older with permanent AF and CAD, prior stroke, or symptomatic heart failure and in those age 75 or older with hypertension and diabetes.
Rhythm Control with Agents Other Than Antiarrhythmic Drugs
Experimental studies indicate that angiotensin-converting enzyme (ACE) inhibitors and angiotensin receptor blockers (ARBs) have favorable effects on electrical and structural remodeling (see Chapter 34). This explains why some studies have shown that ACE inhibitors and ARBs prevent AF. However, other studies have demonstrated that these agents do not prevent AF. A meta-analysis demonstrated that the strongest beneficial effects have been observed with ARBs and in patients with heart failure.39 However, the quality of the data in the meta-analysis studies was low, and at present, there is insufficient evidence to support the use of ACE inhibitors and ARBs for the sole purpose of preventing AF.
Some evidence indicates that statins prevent AF, perhaps because of their anti-inflammatory effects. A systematic review of 16 observational studies demonstrated a 12% reduction in the relative risk of new-onset AF and a 15% reduction in recurrent AF in patients treated with statins.40 However, a meta-analysis of 11 randomized clinical trials concluded that statins do not prevent AF in patients who have not undergone open heart surgery.40 Therefore, the available data do not support the use of statins for the prevention of AF.
Omega-3 polyunsaturated fatty acids (PUFAs) have anti-inflammatory and antioxidant effects and also can have direct ion channel effects. Epidemiologic studies suggested that fish oil could prevent AF, which lead to several randomized clinical trials that assessed the efficacy of PUFAs for AF prevention. These trials reported conflicting results, but the predominance of the data indicate that the daily intake of PUFAs or fish oil does not prevent recurrent AF after cardioversion or episodes of paroxysmal AF.41
Nonpharmacologic Management of Atrial Fibrillation
Pacing to Prevent Atrial Fibrillation
Multiple studies have been performed to determine whether various atrial pacing strategies can prevent or terminate AF. Overall, there has been no convincing evidence that any atrial pacing strategy is effective in preventing or terminating episodes of AF, and therefore atrial pacing is not indicated for prevention of AF in patients without bradycardia. In patients with a bradycardia indication for a pacemaker and paroxysmal AF or recurrent episodes of persistent AF, the available data clearly support the use of atrial-based pacing and programming to minimize the amount of ventricular pacing.42
Catheter Ablation of Atrial Fibrillation
Catheter ablation reliably and permanently eliminates several types of arrhythmias, such as atrioventricular nodal reentrant tachycardia (AVNRT) and accessory pathway–mediated tachycardias (see Chapters 36 and 37). Success rates greater than 95% are attainable when the arrhythmia substrate is well defined, localized, and temporally stable. In contrast, the arrhythmia substrate of AF is not well understood, usually is widespread, is variable between patients, and may be progressive. Furthermore, several factors that promote AF cannot be addressed simply by catheter ablation, including comorbidities (e.g., hypertension, obesity, obstructive sleep apnea), structural remodeling of the atria, inflammatory factors, and genetic factors (see Chapter 7). Therefore, whereas late recurrences of AVNRT or accessory pathway conduction are very rare, AF can recur more than 2 or 3 years after an initially successful ablation procedure.
Selection of Patients
Given the limitations of catheter ablation of AF, it usually is appropriate to treat the patient with at least one rhythm-control drug before catheter ablation is considered. This is particularly true if the AF is persistent because the efficacy of catheter ablation is lower for persistent AF than for paroxysmal AF. The most appropriate candidates for catheter ablation have symptomatic AF affecting quality of life and not adequately responding to drug therapy. The ideal candidate has lone AF or only minimal structural heart disease. The recommendation for catheter ablation should depend on the severity of symptoms, AF burden, prior responses to drug therapy or transthoracic cardioversion, and estimated probability of success. Catheter ablation is least likely to be successful when the left atrium is extremely dilated or if the AF has been persistent for more than 3 or 4 years.
Catheter ablation of AF usually is contraindicated in patients who have a left atrial thrombus or who cannot tolerate anticoagulation for at least 6 to 8 weeks after ablation. Catheter ablation usually is also inappropriate in asymptomatic individuals with a CHA2DS2-VASc score greater than 1 whose only motivation to undergo the procedure is to eliminate the need for anticoagulation.
Although usually reserved for patients who have not responded adequately to ADD treatment, catheter ablation of AF can also be appropriate first-line therapy in patients younger than 35 with symptomatic AF, patients with sinus node dysfunction in whom ADD therapy is likely to create the need for a permanent pacemaker, and patients who express a strong preference for catheter ablation over drug therapy.
Radiofrequency Catheter Ablation
A commonly used energy for catheter ablation of AF is radiofrequency (RF) energy. RF energy is delivered point by point, typically in association with a three-dimensional electroanatomic mapping system as a navigation guide and to create a visual record of the sites that already have been ablated (Fig. 38.7). To improve anatomic accuracy, the electroanatomic map of the left atrium can be merged with a computed tomography scan or magnetic resonance image of the left atrium and pulmonary veins (PVs) or with an ultrasound image generated by intracardiac echocardiography. An important determinant of lesion depth and durability is contact force, and the newest generation of RF ablation catheters provides the operator with immediate feedback on contact force.
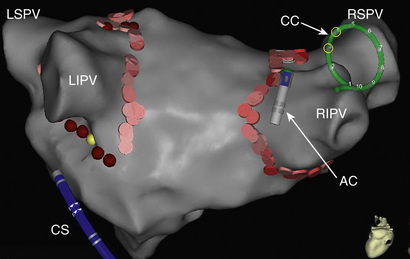
Because of their important role in triggering and maintaining episodes of AF, almost all ablation strategies include electrical isolation of the PVs (Fig. 38.8). This is often sufficient for patients with paroxysmal AF and sometimes sufficient for patients with persistent AF. Pulmonary vein (PV) isolation can be accomplished by either ostial ablation or wide-area ablation 1 to 2 cm away from the ostia, in the antral regions of the PVs. Most of the available data indicate that wide-area ablation is more effective than ostial ablation, probably because it also targets drivers that are in the antrum, outside the PV itself.43 Triggers of AF can also arise from other thoracic veins, such as the superior vena cava, coronary sinus, and the vein of Marshall. After the PVs have been isolated, infusion of isoproterenol is helpful to determine whether any non–PV triggers are present.
A variety of ablation strategies have been used for persistent AF after the PVs have been isolated: linear ablation across the left atrial roof, mitral isthmus, or cavotricuspid isthmus; ablation of complex fractionated atrial electrograms (CFAEs) in the left atrium, coronary sinus, or right atrium; various combinations of linear and CFAE ablation; and ablation of ganglionated plexi.43 The endpoint of catheter ablation of persistent AF is either completion of a prespecified lesion set (in which case sinus rhythm is restored by cardioversion) or stepwise ablation until the AF converts to sinus rhythm. Recent randomized studies have demonstrated that antral PV isolation is as effective as PV isolation plus linear ablation and/or ablation of CFAEs.44,45
A novel approach to ablation of AF is based on the hypothesis that AF is sustained by localized sources, either rotors or focal impulses.5 Signal processing using proprietary software allows identification of focal impulses and rotors that are targeted for RF ablation during ongoing episodes of AF. In one of the first clinical studies using this approach, AF termination or slowing was successfully achieved by ablation of the localized sources in 86% of cases. At a median of 9 months of follow-up, 82% of patients were free of AF, compared to 45% of patients in a control group who underwent conventional ablation.5 These early results suggested that focal impulse and rotor modulation can improve outcomes of catheter ablation of AF. However, more recent studies in patients with paroxysmal, persistent, and longstanding persistent AF have not confirmed the initial results of ablation of rotors and/or focal impulses. The single-procedure freedom from AF/atrial tachycardia (AT) off AADs at 6 to 18 months of follow-up was only 17% to 21% in these studies.46,47 Therefore, although focal impulse and rotor modification is potentially an important step forward in understanding the mechanism of AF, its clinical value in patients undergoing catheter ablation of AF is unsettled.
When the efficacy of catheter ablation of AF is evaluated, recurrences of AF in the first 3 months after ablation usually are ignored. A 3-month blanking period excludes early recurrences that are caused by a transient inflammatory response or incomplete lesion maturation. Even in patients with symptomatic AF, postablation recurrences can be asymptomatic. Therefore, accurate assessment of efficacy requires monitoring for at least 7 days and preferably for 1 month with a device capable of detecting asymptomatic episodes of AF. Ideally, the monitoring should be performed at 6 and 12 months. Continuous monitoring for recurrent AF is possible in patients who have a pacemaker or ICD and an atrial lead. A miniaturized insertable cardiac monitor with wireless telemetry for remote monitoring (Reveal LINQ, Medtronic, Minneapolis, Minnesota) also allows for intense monitoring for postablation AF.48
A wide range of success rates has been reported for RF catheter ablation of AF. When the latest-generation ablation catheters are used by experienced operators, 12-month freedom from AF/AT off AADs after a single procedure generally is 70% to 75% for paroxysmal AF49,50 and 50% to 60% for persistent AF.44,45
Recurrent AF after PV isolation in patients with paroxysmal AF most often is attributable to electrical reconnection of one or more PVs but sometimes is caused by triggers or drivers of AF originating in structures such as the superior vena cava or coronary sinus or in the atria themselves. After reisolation of the PVs and ablation of triggers outside the PVs, 12-month efficacy of 85% to 90% can be expected.
Redo ablation procedures in patients with persistent AF usually consist of re-isolation of the PVs if necessary, and additional ablation directed at substrate modification by targeting CFAEs or creating lines of conduction block at sites such as the left atrial roof or mitral isthmus.43 A 12-month success rate of 75% to 85% typically is achieved after multiple ablation procedures for persistent AF.
Most recurrences of AF after RF catheter ablation occur within the first year of follow-up. However, recurrences continue to occur at a rate of approximately 10% per year at 1 to 3 years, then approximately 4% to 5%/year at 3 to 12 years after ablation.51 The predictors of late recurrences of AF include a history of persistent AF before the initial ablation procedure, age, left atrial size, diabetes, valvular heart disease, cardiomyopathy, and sleep apnea.43 In addition, obesity and lack of cardiovascular conditioning have been reported to predispose to recurrences of postablation AF. Treatment of sleep apnea, weight loss, and improvement in cardiovascular fitness have been found independently to reduce the risk of recurrent AF after an ablation procedure.52,53
Atrial tachyarrhythmias that occur after catheter ablation of AF can take the form of atrial tachycardia/flutter that can be either focal or reentrant. When the ablation strategy consists only of PV isolation, postablation focal ATs often are attributable to partial recovery of PV conduction. The incidence of reentrant AT/flutter after ablation is related to the extent of ablation at atrial sites other than around the PVs. When extensive ablation is performed in the left atrium or in both atria, AT/flutter can occur during follow-up in up to 50% or more of patients. These arrhythmias do not respond well to AAD therapy and often require another ablation procedure for elimination.
The risk of a major complication from RF catheter ablation of AF is reported to be 5% to 6%.54,55 The most common major complications are cardiac tamponade, PV stenosis, and cerebral thromboembolism, each with a prevalence of approximately 1%. The risk of a femoral vascular injury is reported to be 1% to 2%. The risk of a major complication is more than twofold higher when the annual operator volume is less than 25 cases compared to more than 25 cases.54
The risk of esophageal perforation is reported in the range of 0.01% to 0.02%.56 Despite its rarity, this complication is of great concern because it often is lethal. Patients typically present 3 to 14 days after ablation with one of more of the following: dysphagia, odynophagia, fever, leukocytosis, bacteremia, and septic, thrombotic, or air emboli. Computed tomography of the chest with intravenous contrast is the diagnostic test of choice. The presence of contrast in the esophagus or air in the mediastinum or cardiac chambers is indicative of esophageal perforation or fistula formation. Instrumentation of the esophagus should be avoided.
Monitoring of the position of the esophagus and intraluminal esophageal temperature monitoring have been used to prevent esophageal injury during ablation along the posterior wall. Although these maneuvers may reduce the risk, they clearly do not prevent all cases of esophageal injury, since 90% of patients with an esophageal perforation had undergone monitoring of the esophageal position or temperature.56 There is evidence that limiting the power of RF energy applications to 20 to 25 watts for less than 30 seconds when ablating along the posterior left atrial wall and the use of periprocedural proton pump inhibitors reduce the risk of esophageal injury.57
Based on the results of a recent global survey, 72% of patients with an esophageal perforation had evidence of an atrial-esophageal fistula, and mortality among these patients was 79%. In contrast, among the 28% of patients with an esophageal perforation who did not have an atrial-esophageal fistula, mortality was 13%.56 This highlights the importance of early diagnosis and treatment of esophageal perforations. Early surgical intervention is appropriate regardless of whether an atrial-esophageal fistula is present.
A recently recognized complication of RF ablation is silent cerebral ischemic lesions. Cerebral magnetic resonance imaging has demonstrated silent cerebral ischemic lesions in 2% to 14% of patients in whom an irrigated-tip RF ablation catheter is used.58 The long-term clinical significance of these lesions is unclear.
Recent randomized clinical trials have demonstrated that RF catheter ablation of AF is superior to AAD therapy for prevention of AF. In previously untreated patients with paroxysmal AF, there was an absolute difference of 18% in the 12-month risk of recurrent AF in favor of RF catheter ablation over AAD therapy.59 Among patients with persistent AF, there was an absolute difference of 27% in the 12-month risk of recurrent AF in favor of RF catheter ablation over AAD therapy.60
Cryoballoon Ablation
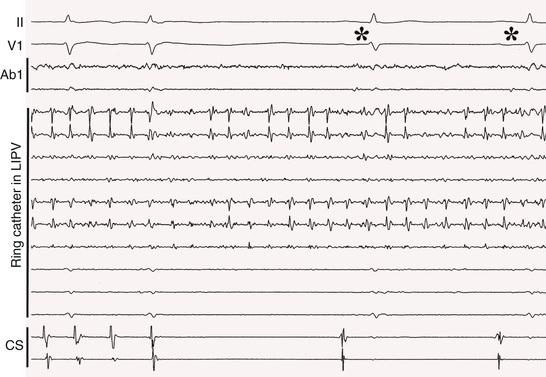
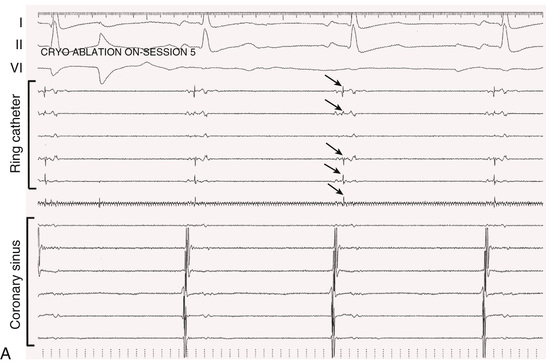
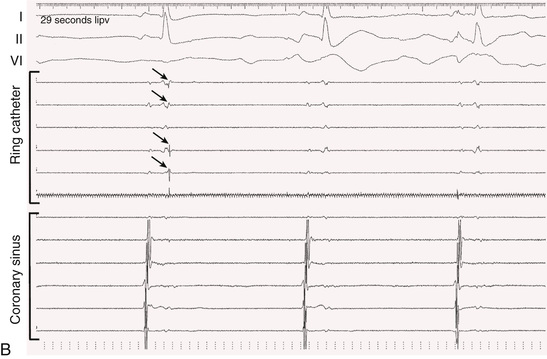
In 2010 a cryoballoon catheter designed to isolate PVs became widely available for use in the United States. In contrast to point-by-point RF ablation around the PVs, the cryoballoon was designed to fit into the antrum of a PV and to create a circumferential ablation lesion using cryoenergy. Cryoenergy is delivered through the entire distal half of the second-generation cryoballoon catheter currently in clinical use. Complete occlusion of the PV by the inflated balloon is necessary for reliable PV isolation (Fig. 38.9). Two 4-minute applications of cryoenergy initially were recommended for each of the PVs. With the second-generation cryoballoon catheter, a single 3- or 4-minute application of cryoenergy often is sufficient to create durable PV isolation in a majority of PVs (Fig. 38.10). Among patients with paroxysmal AF, with a mean of 1.1 to 1.7 applications of cryoenergy per PV, 1-year freedom from recurrent AF was 80% to 82% using a single-freeze protocol.61,62
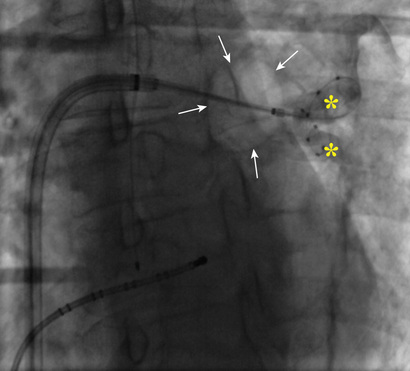
Avoidance of entry of the cryoballoon into the luminal portion of a PV is important to avoid PV stenosis. The most commonly used cryoballoon catheter has a 28-mm diameter when the balloon is fully inflated. The relatively large size of the balloon typically allows occlusion of a PV from the antrum. With use of the 28-mm balloon, up to 40% of the posterior wall between the left and right PVs is rendered electrically silent.63
A multielectrode catheter inserted through a central lumen of the cryoballoon catheter often allows recording of PV potentials during an application of cryoenergy. Disappearance or dissociation of PV potentials within the first minute of a cryoenergy application is a strong independent predictor of durable PV isolation64 (Fig. 38.10). Other independent predictors are achieving a balloon temperature of −40°C in less than 60 seconds during an application of cryoenergy and an interval thaw time to 0°C of longer than 10 seconds on completion of a cryoenergy application.64,65
There is a lower clinical success rate with use of the cryoballoon catheter in patients with persistent AF than in those with paroxysmal AF. Among patients with persistent AF who undergo PV isolation using the 28-mm cryoballoon catheter, freedom from AF at 12 months of follow-up was 60%.66 This is similar to the clinical results achieved in similar patients when wide-area circumferential PV isolation is performed by point-by-point RF catheter ablation.66
Possible complications associated with the cryoballoon catheter have the same risk as with RF catheter ablation of AF, including cardiac tamponade (approximately 1%) and femoral vascular injury (1% to 2%).
The most common complication of cryoballoon ablation is phrenic nerve injury. During early experience with the cryoballoon catheter, the incidence of right phrenic nerve injury was approximately 10%, with the injury resolving within 12 months in almost all patients.67 Injury to the left phrenic nerve is possible but rare. It now is standard clinical practice to pace the phrenic nerve with a catheter positioned in the superior vena cava or right subclavian vein during cryoballoon ablation at the right PVs. Various strategies are available to monitor diaphragmatic contraction or phrenic nerve function during phrenic nerve pacing, including direct palpation of diaphragmatic contraction and monitoring the diaphragmatic compound motor action potential.68 The immediate discontinuation of an application of cryoenergy on the first evidence of phrenic nerve injury greatly reduces the risk of long-lasting or permanent injury. In recent experience with the 28-mm cryoballoon catheter, the risk of right phrenic nerve injury is as low as 1.5% to 2%.62,69
A small number of case reports have made it clear that death from an atrial-esophageal fistula is a potential complication of cryoballoon ablation. Measures to minimize the risk of esophageal injury are appropriate, including the periprocedural use of a proton pump inhibitor and monitoring of intraluminal esophageal temperature during cryoablation. It is common practice to discontinue cryoablation if the esophageal temperature drops to 30°C. This provides a large safety margin for avoiding esophageal injury.70
Radiofrequency Catheter Ablation Versus Cryoballoon Ablation for Atrial Fibrillation
A small number of randomized studies have compared the efficacy of RF catheter ablation versus cryoballoon ablation to isolate the PVs. These studies have shown no major differences in outcomes. The largest multicenter, randomized clinical trial that compared the safety and efficacy of RF catheter ablation versus cryoballoon ablation was performed in 693 patients with paroxysmal AF who underwent PV isolation using either an irrigated-tip radiofrequency ablation catheter (n = 341) or a cryoballoon catheter (n = 341).71 Ideally, the most advanced versions of these catheters would have been used in all patients; however in the cryoablation arm, 82% of the cases were performed using the second-generation balloon, but in the RF ablation arm, only 26% of cases were performed using a contact-force-sensing catheter.
Designed to be a noninferiority trial,71 the primary efficacy endpoint was a combination of recurrence of an atrial tachyarrhythmia longer than 30 seconds, AAD prescription, or a repeat ablation procedure. The primary safety endpoint was a combination of death, stroke, or a treatment-related serious adverse event. A primary efficacy endpoint occurred by 12 months of follow-up in 35.9% of patients in the RF catheter ablation arm and 34.6% of patients in the cryoablation arm. There was also no significant difference in the incidence of primary safety endpoints between the two groups (13.6% in RF catheter ablation arm versus 11.0% in cryoballoon ablation arm). The prevalence of serious adverse events did not differ significantly between the RF catheter ablation group (9%) and the cryoablation group (7.5%). The mean procedure time was 16 minutes shorter in the cryoballoon ablation arm. This study demonstrated that cryoballoon ablation is not inferior to RF catheter ablation in regard to efficacy or safety.
Given that outcomes are similar with point-by-point RF ablation and cryoballoon ablation, the most important factor in deciding which approach to use is operator preference. The advantages of RF catheter ablation include greater versatility, with the ability to ablate AF triggers or drivers that are outside the pulmonary venous antral regions; greater flexibility in energy delivery (e.g., being able to cut back on power delivery when ablating close to esophagus); a lower risk of phrenic nerve injury; ability to use the same catheter to ablate other arrhythmias (e.g., atrial flutter, AVNRT); and lower cost. The advantages of cryoballoon ablation include a shorter learning process, less demand for technical expertise in catheter manipulation, and a shorter procedure time.
Remote Magnetic Navigation
Two systems currently are available for remote navigation of an RF ablation catheter. One system has large magnets positioned on each side of the patient and small magnets embedded in the tip of the ablation catheter that allow remote navigation by shifting the magnetic field vectors. The other has an ablation catheter navigated remotely by a robotic steerable sheath system. The advantages of these systems are improved catheter stability, marked reduction in radiation exposure to the operator, and avoidance of the technical challenges of manual catheter manipulation. The experience to date with remote magnetic navigation for catheter ablation of AF suggests that safety and efficacy outcomes are similar to the outcomes achieved with manual RF catheter ablation.72
Ablation of the Atrioventricular Node
Radiofrequency catheter ablation of the AV node results in complete AV nodal block and substitutes a regular, paced rhythm for an irregular and rapid native rhythm. It is a useful strategy in patients who are symptomatic from AF because of a rapid ventricular rate that cannot be adequately controlled pharmacologically as a result of inefficacy or intolerance to rate-control drugs, and who either are not good candidates for AF ablation or already have undergone unsuccessful attempts at ablation. AV node ablation also can be helpful in patients with heart failure and AF to maximize the benefits of cardiac resynchronization therapy (CRT) if there already is not 100% ventricular pacing.73
In patients with AF and an uncontrolled ventricular rate, AV node ablation improves the left ventricular ejection fraction (EF) if there is a tachycardia-induced cardiomyopathy. AV node ablation also has been shown to improve symptoms, quality of life, and functional capacity and to reduce the use of health care resources.74
The disadvantages of AV node ablation are that it creates a lifelong need for ventricular pacing and does not restore AV synchrony. Although symptoms and functional capacity typically improve after AV node ablation in patients with AF and an uncontrolled ventricular rate, some patients may not feel as well as during sinus rhythm.
Atrioventricular node ablation is a technically simple procedure with an acute and long-term success rate of 98% or higher and a very low risk of complications. In patients with persistent AF, a ventricular pacemaker is implanted. A dual-chamber pacemaker is appropriate if the AF is paroxysmal. Most patients have a good clinical outcome with right ventricular pacing, but in patients with left ventricular dysfunction, biventricular pacing for CRT is appropriate.75 In patients with an ischemic or nonischemic cardiomyopathy and EF of 30% to 35% or lower, an ICD may be appropriate for primary prevention of sudden death. However, a pacemaker without the ICD often is adequate for patients with a borderline EF (30% to 35%) and a rapid ventricular rate because the EF is likely to improve after the ventricular rate has been controlled by AV node ablation.74 His bundle pacing can be considered in some patients to avoid problems with right ventricular pacing.
Surgical Approaches to Atrial Fibrillation
The most effective surgical procedure for AF is the “cut-and-sew” maze procedure developed by Cox in 1987. This operation involves multiple atrial incisions to isolate the PVs and to create lines of block in the left atrium and right atrium. In addition, the left and right atrial appendages are excised. In a study from a highly experienced surgical center in patients who underwent periodic 24-hour Holter monitoring during follow-up, there was 83% freedom from AF off drugs at a median follow-up of 5.9 years after the most recent version of the cut-and-sew maze procedure (Cox maze III).76 However, because continuous monitoring for only 24 hours at a time often is insufficient to detect recurrent episodes of AF, the 83% long-term freedom from AF likely was an overestimate.
The cut-and-sew Cox maze procedure has not been widely performed because it requires cardiopulmonary bypass, is technically difficult, and is associated with a mortality rate of 1% to 2%.
A large variety of surgical ablation tools have been developed to simplify the Cox maze III procedure. These tools allow the surgeon to substitute an ablation line for a surgical incision. Some surgeons use a minimally invasive approach in which the ablation tools are inserted through small incisions between the ribs, and thoracoscopic video-assisted epicardial ablation is performed. Several different types of energy have been used for surgical ablation: RF energy, cryoenergy, microwave, laser, and high-intensity focused ultrasound. The tool that most consistently produces transmural ablation lesions is a clamp device developed to isolate the PVs using bipolar RF energy.
Various surgical ablation strategies have been used, including PV isolation, left atrial ablation, and the Cox maze lesion set (Cox maze IV) in which a combination of RF and cryothermal ablation lines replace most of the surgical incisions. In a large series of patients with AF who underwent the Cox maze IV procedure, freedom from AF off AADs at 5 years was 66%, with no difference in efficacy between patients with paroxysmal versus persistent AF or between patients with a stand-alone procedure versus a concomitant procedure.77
Surgical therapy for AF is appropriate as a concomitant procedure in patients with symptomatic AF undergoing open heart surgery for CAD or valvular disease. A stand-alone surgical procedure for AF is an option for patients who have not had a successful outcome from catheter ablation, who are not good candidates for catheter ablation, or who prefer a surgical approach over catheter ablation.
Hybrid Approach to Ablation of Atrial Fibrillation
Some AF ablation centers use a hybrid approach that combines surgical and catheter ablation, either on the same day or staged, with the two components separated by days to weeks. The rationale for the hybrid approach is that it capitalizes on the strengths of the two approaches and minimizes their limitations.78 The surgical component is performed first, allowing exclusion of the left atrial appendage, direct visualization of the antrum of the PVs, access to epicardial structures such as the ligament of Marshall and ganglionated plexi, and avoidance of damage to the esophagus and phrenic nerve. A subsequent catheter ablation procedure consists of additional ablation as needed, for PV isolation, conduction block across epicardial ablation lines, ablation of complex fractionated electrograms or rotors, and ablation of sites that are not accessible from the epicardium, such as the tricuspid or mitral isthmus.
The 12-month freedom from AF off AADs after the hybrid approach has varied widely, from as low as 37% to as high as approximately 80%.78 This wide range of success rates likely is attributable to differences in patient selection, operator skill, specific technologies used for ablation, and lesion sets.
In the absence of data from prospective randomized studies, the incremental value of the hybrid approach over surgical or catheter ablation alone has remained unclear.
Specific Clinical Syndromes
Postoperative Atrial Fibrillation
Atrial fibrillation is common after open heart surgery and is reported to occur in 25% to 40% of patients who undergo coronary artery bypass graft (CABG) surgery or valve replacement (see Chapter 11). AF is associated with a twofold increase in the risk of postoperative stroke and is the most common reason for prolonged hospitalization. The incidence of AF peaks on the second postoperative day. The pathogenesis of postoperative AF is multifactorial and probably involves adrenergic activation, inflammation, atrial ischemia, electrolyte disturbances, and genetic factors. Several risk factors for AF after open heart surgery have been identified, including age over 70 years, history of prior AF, male gender, left ventricular dysfunction, left atrial enlargement, chronic lung disease, diabetes, and obesity.
The AADs that decrease the risk of postoperative AF are amiodarone and sotalol by 50% to 65%, and beta blockers by approximately 30%.79 Hypomagnesemia is common after open heart surgery and can heighten the risk of AF. Magnesium administration is reported to decreases the risk of postoperative AF by 20% to 40%.79
Right atrial or biatrial pacing using temporary electrodes attached to the right and left atrium is reported to reduce the risk of postoperative AF by approximately 40%.79
Colchicine, atorvastatin, and steroids also have been demonstrated in randomized studies to reduce the risk of AF after open heart surgery by approximately 35% to 40%.79,80 The main mechanism by which these agents prevent AF probably is an anti-inflammatory effect. Omega-3 PUFAs also have an anti-inflammatory effect, but randomized studies on their efficacy for preventing postoperative AF have reported conflicting results.79
A novel approach to the prevention of AF after cardiac surgery is injection of botulinum toxin into the four major epicardial fat pads at operation. This causes temporary autonomic blockade and has been shown to reduce the incidence of AF after CABG to less than 10%.81
Patients who develop postoperative AF can be managed using a rate- or rhythm-control strategy. In a randomized comparison of rate- and rhythm-control strategies in patients with AF after cardiac surgery, there were no significant differences between the two strategies in the number of days of hospitalization, mortality, or adverse events.81 The decision on which type of strategy to employ in these patients should be based on the severity of symptoms, hemodynamic effects of the AF, and the patient-specific risk of side effects or adverse reactions to the various rate- and rhythm-control drugs.
AF that occurs after cardiac surgery often resolves within 3 months. In a randomized comparison of rate control versus rhythm control in patients with new-onset AF after cardiac surgery, approximately 95% of patients in both groups were in sinus rhythm at 60 days and had not experienced AF during the prior 30 days.81 Treatment with an oral anticoagulant should be continued after discharge. Because new-onset AF after cardiac surgery often does not recur after 60 to 90 days, rhythm-control medications can be discontinued at that time, and if there is no subsequent evidence of symptomatic or asymptomatic AF, as confirmed by monitoring (e.g., 3- to 4-week autotrigger event monitor), anticoagulation can be safely discontinued unless needed for another indication.
New-onset AF occurs postoperatively in less than 5% of patients undergoing major noncardiac surgery. Some of the possible mechanisms of postoperative AF after cardiac surgery (e.g., sympathetic activation, electrolyte abnormalities, hypoxia) most likely also play a role in AF after noncardiac surgery. Beta blockers have been shown to reduce the risk of AF after major noncardiac surgery by approximately 25%.79
Wolff-Parkinson-White Syndrome
Patients with the WPW syndrome and an accessory pathway with a short refractory period can experience a very rapid ventricular rate during AF (see Chapters 36 and 37). Ventricular rates greater than 250 to 300 beats/min can result in loss of consciousness or precipitate ventricular fibrillation and a cardiac arrest. Patients with WPW syndrome who present in AF with a rapid ventricular rate should undergo transthoracic cardioversion if there is hemodynamic instability. If the patient is hemodynamically stable, intravenous procainamide or ibutilide can be used for pharmacologic cardioversion. Procainamide may be preferable to ibutilide because it blocks accessory pathway conduction and slows the ventricular rate before AF has converted to sinus rhythm. Digitalis and calcium channel antagonists are contraindicated in patients with WPW syndrome and AF. These agents selectively block conduction in the AV node and can result in acceleration of conduction through the accessory pathway.
The preferred therapy for patients with WPW syndrome and AF with a rapid ventricular rate is catheter ablation of the accessory pathway. The efficacy of catheter ablation is 95% or higher for most types of accessory pathways, and the risk of a major complication is very low. AF typically no longer recurs after successful accessory pathway ablation, probably because AF in the WPW syndrome often is induced by tachycardia and a result of atrioventricular reciprocating tachycardia (AVRT).
Congestive Heart Failure
Atrial fibrillation is a common arrhythmia in patients with heart failure, with a prevalence ranging from 10% in patients with New York Heart Association (NYHA) functional Class I up to 50% in Class IV patients (see Chapters 24 and 25). AF may be the cause of heart failure in patients who present with a nonischemic cardiomyopathy and AF with a rapid ventricular rate. Occasionally, AF causes left ventricular dysfunction and heart failure even when the ventricular rate is not rapid. In patients with structural heart disease and preexisting left ventricular dysfunction, AF can worsen the heart failure. The deleterious hemodynamic effects of AF are mediated by a rapid and/or irregular ventricular rate and loss of AV synchrony.
The most appropriate rate-control drugs in patients with systolic heart failure are beta blockers and digitalis. If necessary, amiodarone also can be used for rate control. In patients with diastolic heart failure, nondihydropyridine calcium antagonists can be used safely for rate control. Amiodarone and dofetilide are the only two rhythm-control drugs that are not associated with an increased risk of death in patients with heart failure.
As in other patients with AF, the decision to pursue a rate-control or a rhythm-control strategy in patients with heart failure should be individualized. If the heart failure is a result of AF, a rhythm-control strategy should be employed. In patients with heart failure who develop AF, there are no significant differences in all-cause mortality, cardiovascular mortality, or worsening heart failure between patients treated with a rate-control strategy or a pharmacologic rhythm-control strategy.2 However, although symptoms improve with both a rate- and rhythm-control strategy, sinus rhythm is associated with greater improvement in NYHA functional class and quality of life.82
A limitation of a pharmacologic rhythm-control strategy is that many patients continue to experience episodes of AF. Catheter ablation is more effective than AADs for preventing recurrent AF and therefore could have incremental benefit over drug therapy in patients with heart failure and AF. In patients with heart failure and persistent AF who were randomly assigned to either catheter ablation or treatment with amiodarone, freedom from AF at 24 months was 70% in the catheter ablation group compared to 34% in the amiodarone group, and the relative risks of unplanned hospitalizations and mortality were reduced by 45% to 55% in the catheter ablation group.83 The EF increases by approximately 13% when AF is successfully eliminated in patients with left ventricular dysfunction.84
Four small-scale randomized studies (sample sizes of 41 to 81 patients) compared catheter ablation to either pharmacologic rate control or AV junction ablation in patients with left ventricular dysfunction, and NYHA Class II to IV heart failure.85 A majority of the patients had persistent AF. Freedom from AF ranged from 50% to 81% at 6 months and was 88% at 12 months after catheter ablation. Compared to rate control, catheter ablation was associated with significantly greater improvements in EF, functional capacity, brain natriuretic peptide levels, and quality of life.
These results suggest that maintenance of sinus rhythm is preferable to rate control in patients with heart failure and that catheter ablation of the AF should be considered if sinus rhythm is not maintained by amiodarone or dofetilide. Large-scale multicenter trials currently are in progress and will be helpful in clarifying the role of catheter ablation in patients with heart failure and AF.
A rate-control strategy is appropriate for patients who do not respond adequately to amiodarone or dofetilide and either are not suitable candidates for catheter ablation of the AF or have had an unsuccessful outcome from ablation. AV node ablation is appropriate for patients when ventricular rate during AF is not adequately controlled by drug therapy. Because left ventricular dysfunction and heart failure can be aggravated by right ventricular pacing, biventricular pacing should be performed after AV node ablation. The decision to implant a biventricular pacemaker versus a biventricular ICD is based on clinical judgment. If it seems likely that the EF will remain less than 30% to 35% after optimal heart rate control, a biventricular ICD is appropriate for primary prevention of sudden cardiac death.
In patients with heart failure who undergo CRT, AF often results in intrinsic and/or fused QRS complexes even when the rate is considered to be adequately controlled. This can limit the extent of biventricular capture. If this is the case in a patient with heart failure and AF, AV node ablation can maximize the benefit of CRT by resulting in 100% biventricular capture.73
Hypertrophic Cardiomyopathy
Atrial fibrillation occurs in approximately 25% of patients with hypertrophic cardiomyopathy (HCM) and can cause severe hemodynamic impairment because of an inadequate diastolic filling time and loss of atrial-ventricular synchrony. Because of a high risk of thromboembolic complications, anticoagulation is indicated in AF patients with HCM, independent of the CHA2DS2-VASc score.
Severe left ventricular hypertrophy increases the risk of drug-induced torsade de pointes, and the only rhythm-control agents recommended for patients with HCM and a wall thickness greater than 1.5 cm are dronedarone and amiodarone.2 Catheter ablation of AF also is an option. However, the responses to drug therapy and catheter ablation often are suboptimal because of the extensive atrial remodeling that may be present in patients with HCM.
Eight observational cohort studies reported on the results of RF catheter ablation of AF in patients with HCM.86 The median follow-up in these studies was 18 to 19 months, and the rate of redo ablation procedures was 43%. Freedom from AF in these studies was a median of 66% to 86% for patients with paroxysmal AF and 42% to 65% for patients with persistent AF. These results indicate that catheter ablation is a reasonable option in patients with HCM and AF who do not respond well to AAD therapy. However, because of the prominent structural atrial abnormalities that can be associated with HCM, AF is likely to recur during long-term follow-up in many of these patients.
Percutaneous Coronary Intervention for Coronary Artery Disease
In patients with stable ischemic heart disease, treatment with aspirin plus clopidogrel (double-antiplatelet [-antithrombotic] therapy, DAPT) is recommended for a minimum of 1 month after placement of a bare metal stent and for a minimum of 6 months after placement of a drug-eluting stent. In patients with an acute coronary syndrome who undergo percutaneous coronary intervention with either a bare metal stent or a drug-eluting stent, DAPT is recommended for at least 12 months.
In patients who require long-term anticoagulation for AF, the addition of DAPT increases the risk of serious bleeding. The results of a randomized clinical trial indicated that therapy with a vitamin K inhibitor plus clopidogrel after stent placement reduces the risk of major bleeding events compared to therapy with a vitamin K inhibitor plus DAPT, without increasing the risk of adverse outcomes such as myocardial infarction, death, or stent thrombosis.87
Pregnancy
The prevalence of AF during pregnancy is very low, approximately 60/100,000 pregnancies. When it occurs, AF often is in the setting of underlying congenital or valvular heart disease, thyrotoxicosis, or electrolyte abnormalities. Pregnancy is associated with a hypercoagulable state, but no data indicate that pregnancy increases the risk of thromboembolic complications related to AF. In women with paroxysmal AF before pregnancy, the frequency of episodes may or may not increase during pregnancy.
The decision to anticoagulate a pregnant woman with AF should be made using the same criteria as in nonpregnant women. If anticoagulation is deemed necessary, warfarin (not an NOAC) is recommended from the second trimester until 1 month before the due date, and subcutaneous low-molecular-weight heparin is recommended during the first trimester and during the final month of pregnancy.
Transthoracic cardioversion is considered safe at all stages of pregnancy. The recommended pharmacologic agents for acute management of AF consist of intravenous metoprolol for rate control and flecainide or sotalol for conversion to sinus rhythm. If ongoing therapy is deemed necessary, the recommended rate-control drug is digoxin. If ineffective, a beta blocker can be used, but only after the first trimester. If there is no structural heart disease, flecainide and sotalol are recommended for long-term rhythm control.88 In the patient with structural heart disease, amiodarone is recommended for rhythm control.
Future Perspectives
The ideal antiarrhythmic drug to prevent atrial fibrillation would affect only the atrium, thereby eliminating the potential for ventricular proarrhythmia. Such AADs are under development and may improve the safety and efficacy of pharmacologic therapy for AF. It is likely that drugs that modify a single channel will not be as effective as those with multiple actions, and targeting nonchannel functions (e.g., prevention of atrial fibrosis) may prove useful.
In the past few years, significant progress has been made in the field of catheter ablation of AF, but much room remains for improvement in efficacy and procedure duration. The failure to create enduring pulmonary vein isolation often accounts for recurrences of AF after both radiofrequency catheter ablation and cryoballoon ablation. The development of new ablation tools that improve the ability safely to create transmural lesions could reduce the need for redo ablation procedures. The cryoballoon catheter has improved the efficiency of PV isolation compared to point-by-point RF ablation. However, its use is limited to the antral regions of the PVs. The development of ablation catheters that ablate large areas of atrial myocardium with single applications of energy could improve the efficiency of catheter ablation of persistent AF.
In patients with persistent AF, a better understanding of AF mechanisms could result in more efficient and successful ablation strategies. The identification of presumptive localized sources of AF (focal impulses and/or atrial rotors) by computed signal analysis in humans in the past few years possibly represents an important step in this direction.5 However, the excellent early clinical results have not been consistently reproduced in subsequent studies.46,47 Better understanding of AF mechanisms in humans is clearly needed. Several studies have shown that a rhythm-control strategy in patients with AF provides no advantages in outcomes over a rate-control strategy. The results of these studies most likely were influenced by the suboptimal safety and efficacy of the drugs used for rhythm control.
To date, no randomized trials have demonstrated that catheter ablation of AF improves outcomes such as stroke or survival. An ongoing trial, Catheter Ablation versus Antiarrhythmic Drug Therapy for Atrial Fibrillation (CABANA), has a primary endpoint of mortality and secondary endpoints of cardiovascular mortality and stroke. If this study shows improved outcomes with AF ablation, it will strengthen the case for rhythm control by ablation.
Guidelines
Atrial Fibrillation
Fred Morady and Douglas P. Zipes
Recent updates have been incorporated into the comprehensive guidelines for the management of atrial fibrillation (AF) published in 2006 by the American College of Cardiology/American Heart Association (ACC/AHA) Task Force on Practice Guidelines and the European Society of Cardiology Committee for Practice Guidelines.1 The following classification system was used for recommendations and for the level of evidence on which the recommendations are based:
- Class I: conditions for which there is evidence and/or general agreement that the test is useful and effective
- Class IIa: weight of evidence or opinion is in favor of usefulness/efficacy
- Class IIb: usefulness or efficacy is less well established by evidence or opinion
- Class III: conditions for which there is evidence and/or general agreement that the test is not useful or effective and in some cases may be harmful
- Level A recommendations are derived from data from multiple randomized clinical trials.
- Level B recommendations are derived from a single randomized trial or nonrandomized studies.
- Level C recommendations are based on the consensus opinion of experts.
The guidelines do not necessarily define the standard of care. Management decisions must be individualized on the basis of the particular circumstances of a patient, and there are situations in which a deviation from the guidelines may be appropriate.
Classification of Atrial Fibrillation
The terminology used to classify AF in the guidelines is as follows: paroxysmal AF is defined as episodes of AF that last less than 7 days; persistent AF is defined as AF that lasts more than 7 days; and longstanding AF refers to AF that has been persistent for more than 1 year. These designations are not altered by termination of AF by drug therapy or electrical cardioversion. AF that is resistant to electrical cardioversion is referred to as permanent AF. AF is considered recurrent after two or more episodes have occurred.
Some patients with paroxysmal AF occasionally have episodes that are persistent, and vice versa. In this event, the AF should be categorized on the basis of the predominant form. Lone AF refers to AF in patients younger than 60 years who do not have structural heart disease or hypertension. AF that is secondary to acute myocardial infarction (MI), cardiac surgery, pericarditis, myocarditis, hyperthyroidism, or an acute pulmonary process is considered separately because the AF often resolves after treatment of the underlying disorder.
Management of Atrial Fibrillation
The guidelines address five aspects of the management of AF: pharmacologic rate control, prevention of thromboembolic complications, cardioversion, maintenance of sinus rhythm, and special considerations, including postoperative AF, MI, Wolff-Parkinson-White (WPW) syndrome, hyperthyroidism, pregnancy, hypertrophic cardiomyopathy (HCM), and pulmonary disease.
An important aspect in the management of patients with AF that is not specifically addressed in the guidelines is how to decide on a rate-control strategy versus a rhythm-control strategy. Several clinical trials have demonstrated that pharmacologic rhythm-control and rate-control strategies result in similar outcomes, even in patients with AF who have left ventricular dysfunction and heart failure. On the other hand, a randomized trial of left atrial radiofrequency catheter ablation versus atrioventricular (AV) node ablation and biventricular pacing demonstrated significantly greater improvement in left ventricular (LV) function, exercise capacity, and quality of life in patients with heart failure who were treated by ablation. It is possible that the side effects from the drugs used for rhythm control offset the benefits of sinus rhythm. Specific recommendations regarding rhythm-control versus rate-control strategies are difficult to provide because the decision must be individualized on the basis of several factors, including age, symptom severity, functional limitations, patient preference, comorbidities, sinus node function, and response to drug therapy.
Pharmacologic Rate Control During Atrial Fibrillation (Table 38G.1)
In addition to specific recommendations on the use of particular drugs for control of the ventricular rate, the guidelines recommend that the effects of drug therapy on ventricular rate be measured at rest and during exercise to ensure adequate heart rate control. The criteria used for rate control are rates of 60 to 80 beats/min at rest and 90 to 115 beats/min during moderate exercise.
TABLE 38G.1
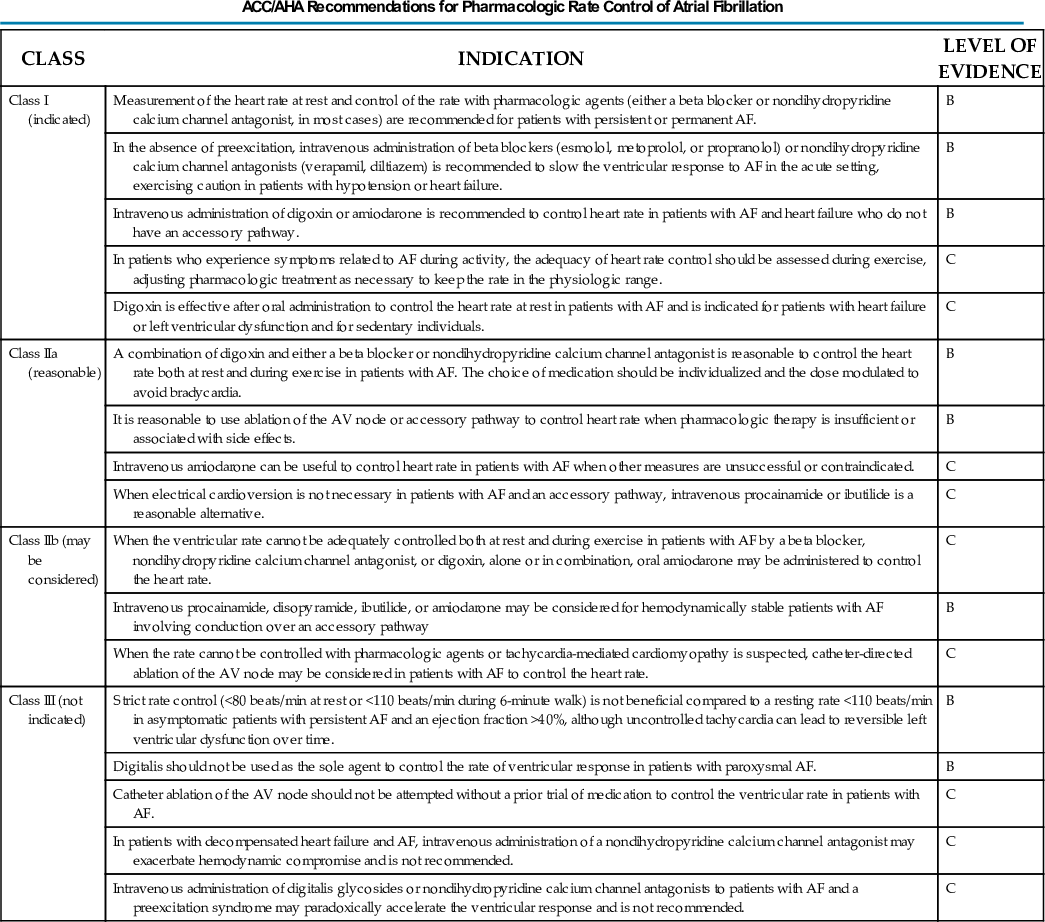
A 2011 recommendation states that a resting rate of less than 110 beats/min is a reasonable rate-control target in patients with persistent AF and no arrhythmia-related symptoms who have an ejection fraction (EF) greater than 40%. However, the guidelines caution that tachycardia can result in a decline in LV function over time.
Digitalis is much less effective for control of the ventricular rate during exercise than at rest and is indicated for patients with heart failure or LV dysfunction and for sedentary patients. A combination of digitalis and either a beta blocker or nondihydropyridine calcium channel antagonist is appropriate to control the rate at rest and during exercise. The guidelines recommend that digitalis not be used as the sole agent for rate control in patients with paroxysmal AF. Catheter ablation of the AV node should be reserved for patients whose ventricular rate cannot be adequately controlled by drug therapy because of either inefficacy or drug intolerance.
Prevention of Thromboembolism (Table 38G.2)
The 2006 guidelines recommend antithrombotic therapy with either aspirin or a vitamin K antagonist such as warfarin for all patients with AF except those who have lone AF or contraindications. An updated 2011 recommendation is that the direct thrombin inhibitor dabigatran is a useful alternative to warfarin for stroke/embolism prevention in patients with AF. The choice between aspirin and an anticoagulant is based on the patient's risk profile. The factors associated with the highest risk of thromboembolism are a prior thromboembolic event and rheumatic mitral stenosis, and warfarin or dabigatran is recommended for patients with one of these risk factors. The risk factors associated with a moderate risk of thromboembolism are age 75 years or older, hypertension, heart failure, EF of 35% or less, and diabetes. Aspirin is recommended if none of these risk factors is present, and an anticoagulant is recommended for patients with one or more of these risk factors. In patients with only one of the moderate risk factors, either aspirin or an anticoagulant is reasonable, and the choice should be individualized.
TABLE 38G.2
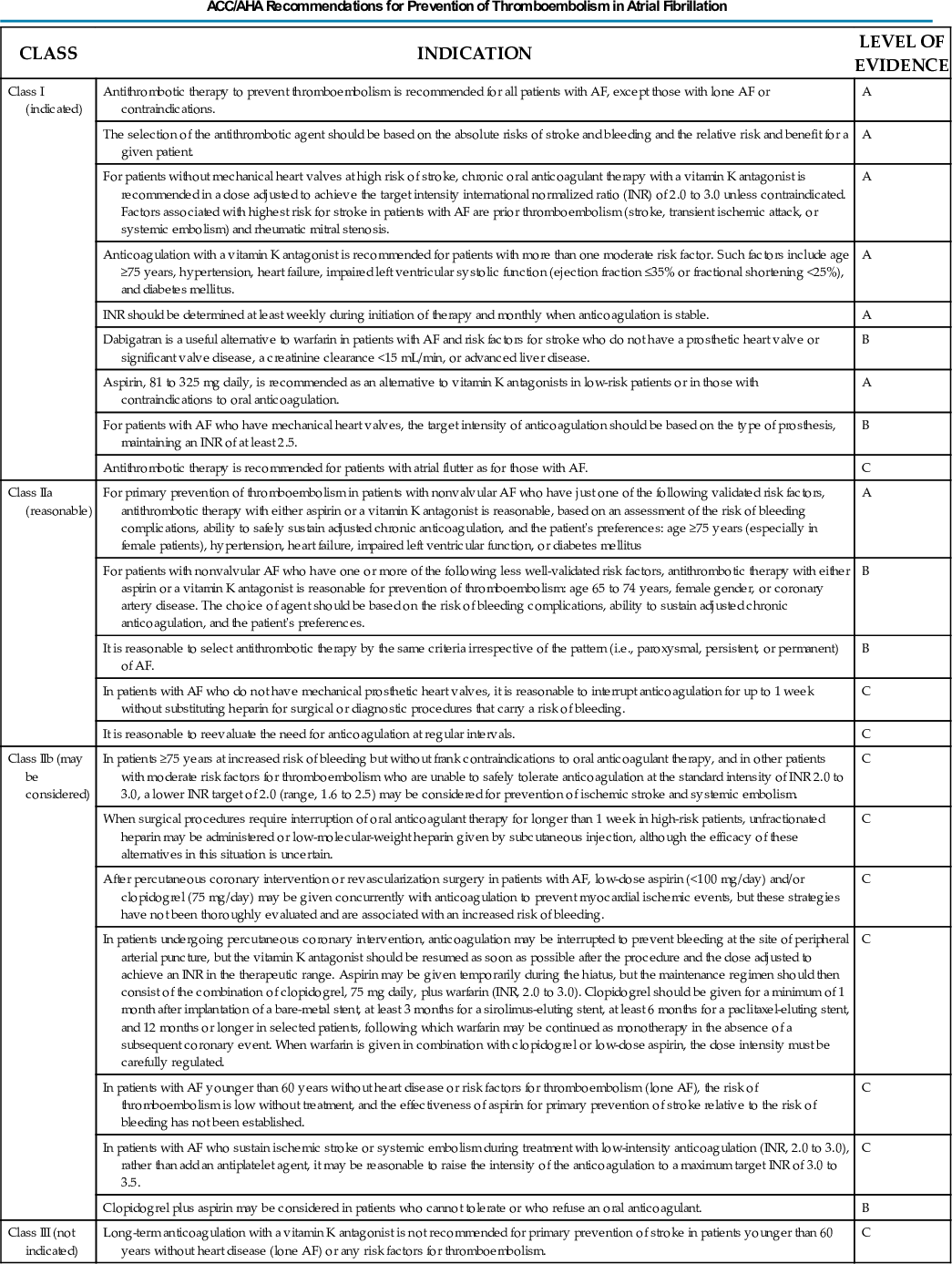
Rivaroxaban was approved by the FDA in 2011, after publication of the updated guidelines dealing with dabigatran. It seems appropriate to generalize the recommendations regarding dabigatran to the factor Xa inhibitor rivaroxaban.
Another update to the 2006 guidelines addresses combination therapy with aspirin and clopidogrel. This combination has been demonstrated to be less effective than warfarin for preventing strokes, but more effective than aspirin alone. The guidelines now recommend that aspirin plus clopidogrel be considered for stroke prevention in patients who cannot tolerate or refuse to take an oral anticoagulant.
Cardioversion of Atrial Fibrillation (Table 38G.3)
The first-line drugs recommended for cardioversion are flecainide, dofetilide, propafenone, and ibutilide. Amiodarone is considered a reasonable option. The guidelines state that digoxin and sotalol may be harmful when they are used for cardioversion and recommend against use of these agents for that purpose.
TABLE 38G.3
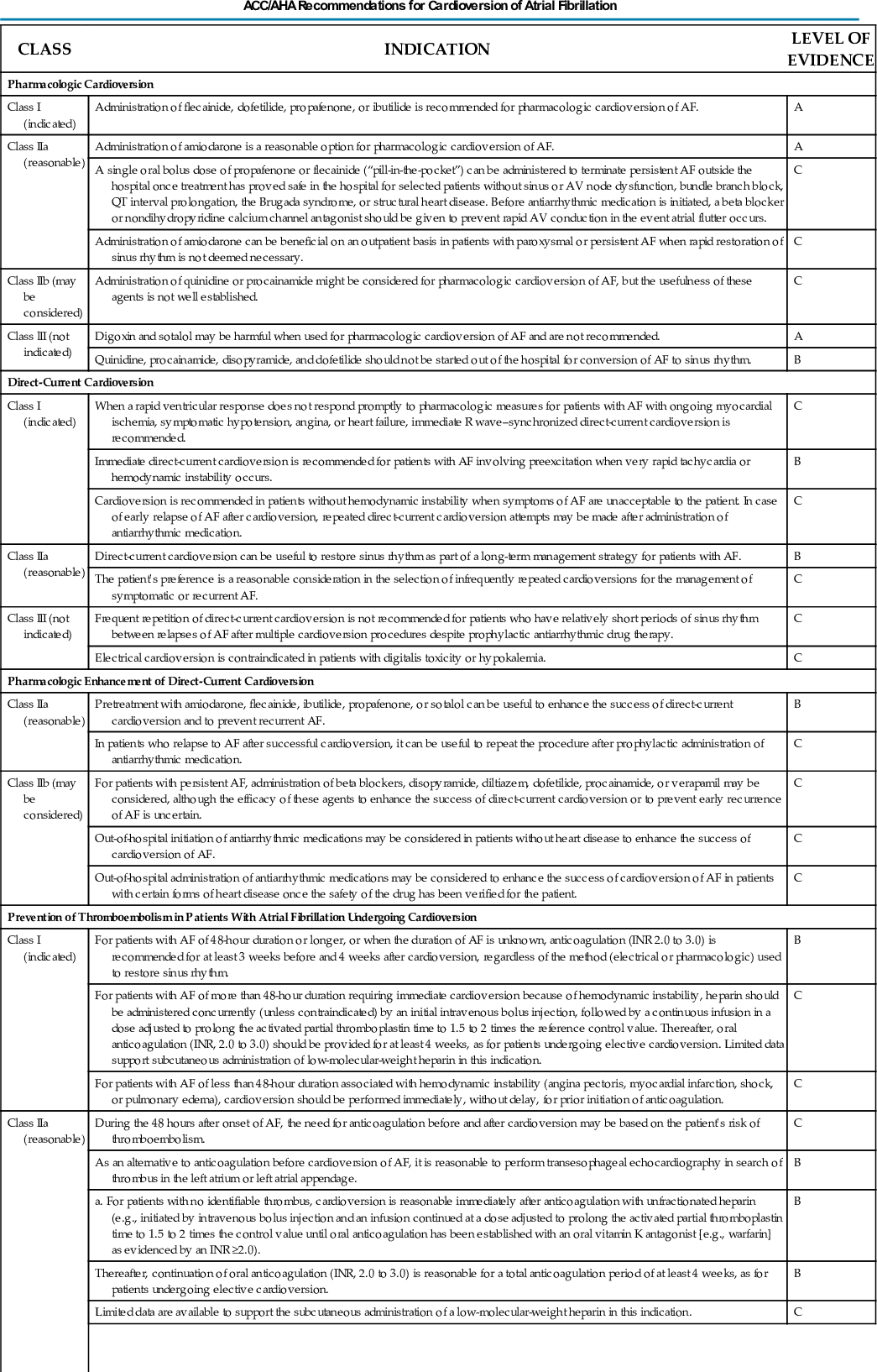

Direct-current (DC) cardioversion is recommended when there is a rapid ventricular rate that does not respond quickly to drug therapy in patients with myocardial ischemia, hypotension, or heart failure and in patients with the WPW syndrome and AF with a very rapid rate or hemodynamic instability. If there is an early recurrence of AF after DC cardioversion, repeated cardioversion is recommended after treatment with an antiarrhythmic drug (AAD).
If AF has been present for more than 48 hours or if the duration is unknown, anticoagulation with warfarin and an international normalized ratio (INR) of 2 to 3 is recommended for 3 weeks or longer before cardioversion, whether pharmacologic or electrical, and for 4 weeks afterward. It is reasonable to presume that dabigatran or rivaroxaban are suitable alternatives to warfarin.
When cardioversion is performed within 48 hours of the onset of AF, anticoagulation before and after cardioversion may be based on the patient's risk profile.
In patients with AF for more than 48 hours or in whom the duration is unknown, an alternative to anticoagulation for 3 or more weeks before cardioversion is to perform transesophageal echocardiography, to anticoagulate the patient with heparin, to initiate oral anticoagulation, and to proceed with immediate cardioversion if no thrombi are present in the left atrium or left atrial appendage. In patients receiving warfarin, heparin should be continued until the INR is 2, and oral anticoagulation with an INR of 2 to 3 should be continued for 4 weeks or longer. In patients treated with dabigatran or rivaroxaban, heparin can be discontinued 3 to 4 hours after the first oral dose. As with warfarin, anticoagulation therapy should be continued for 4 weeks or longer.
Maintenance of Sinus Rhythm (Table 38G.4)
A reasonable outcome of AAD therapy is infrequent recurrences of well-tolerated AF. Initiation of a rhythm-control medication is reasonable on an outpatient basis in patients without heart disease when the medication is well tolerated. The updated guidelines now recommend dronedarone as being a reasonable option in patients with paroxysmal AF or after conversion of persistent AF. The guidelines recommend catheter ablation of symptomatic paroxysmal AF for patients who have failed treatment with an AAD and have little or no left atrial enlargement and normal or mildly reduced LV function.
TABLE 38G.4
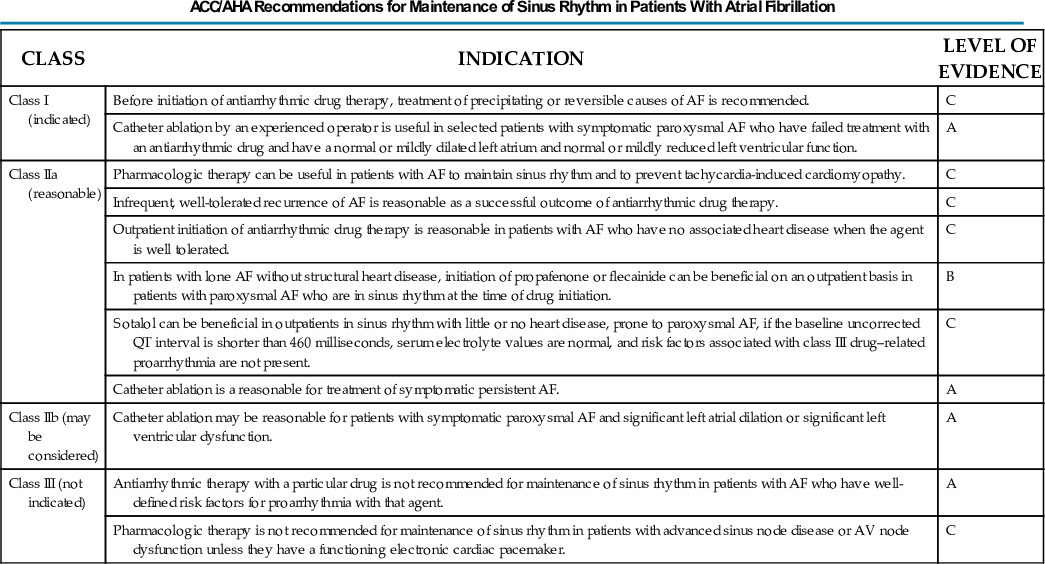
Special Considerations (Table 38G.5)
Postoperative Atrial Fibrillation
The guidelines recommend prophylactic treatment with an oral beta blocker to prevent postoperative AF in patients undergoing cardiac surgery. Preoperative amiodarone also is considered to be appropriate prophylactic therapy to prevent postoperative AF. The use of cardioversion, rhythm-control medications, and antithrombotic medication should be based on the same considerations as in nonsurgical patients.
TABLE 38G.5
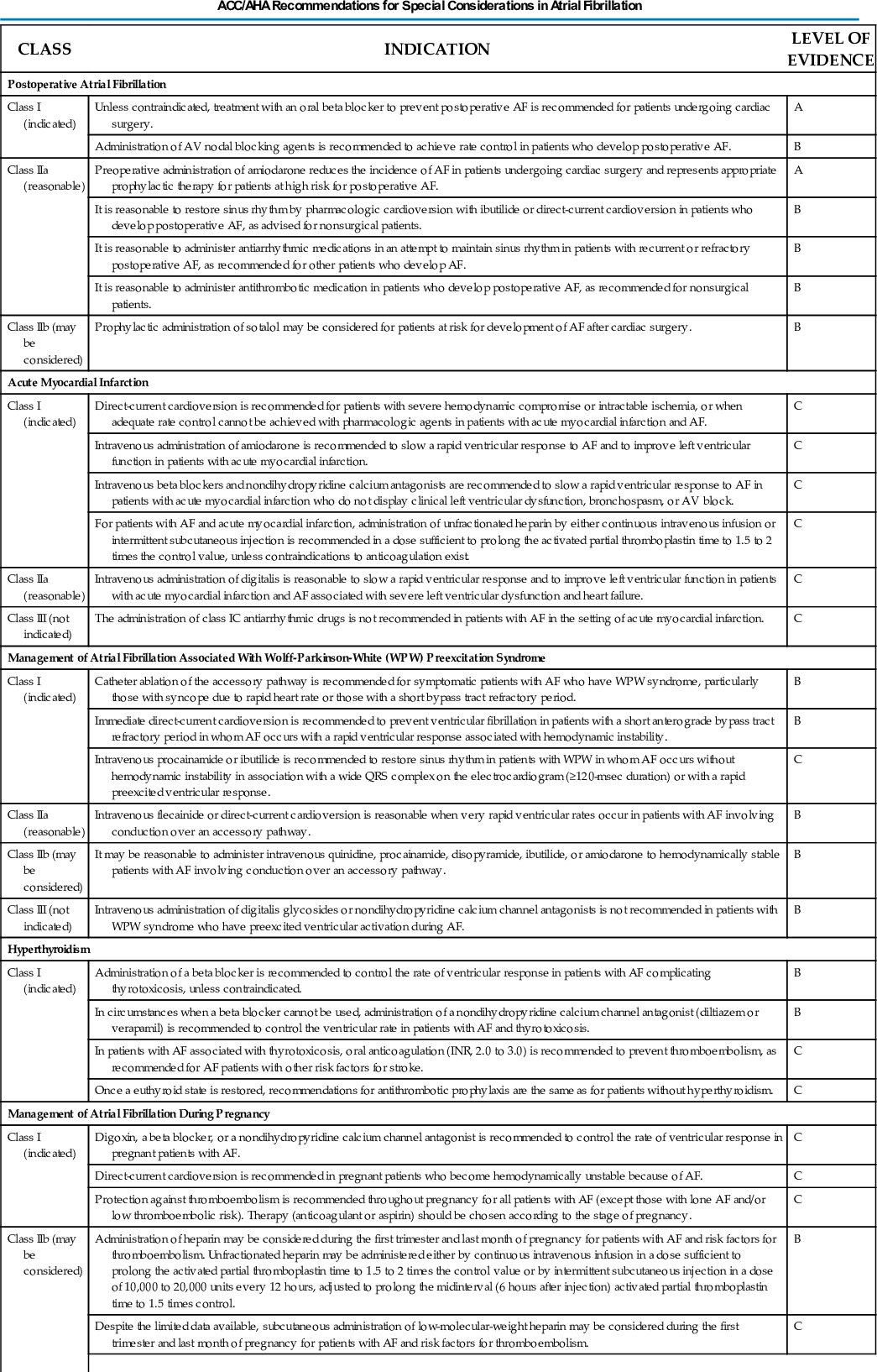

Acute Myocardial Infarction
Electrical cardioversion is recommended if there is hemodynamic compromise or ongoing ischemia or when adequate rate control cannot be achieved with drug therapy. The guidelines recommend intravenous (IV) amiodarone or digitalis to slow the ventricular rate in patients and to improve LV function in patients with an acute MI. If there is no LV dysfunction, bronchospasm, or AV block, an IV beta blocker or nondihydropyridine calcium antagonist is recommended for rate control.
Atrial Fibrillation in Wolff-Parkinson-White Syndrome
Catheter ablation of the accessory pathway is recommended in patients with symptomatic AF and the WPW syndrome. Immediate electrical cardioversion is recommended if there is AF with a rapid ventricular rate and hemodynamic instability. If the patient is hemodynamically stable, IV procainamide or ibutilide is recommended for pharmacologic conversion of AF. IV digitalis and nondihydropyridine calcium channel antagonists should be avoided in patients with ventricular preexcitation during AF.
Hyperthyroidism
The guidelines recommend a beta blocker as first-line therapy for rate control in patients with AF and thyrotoxicosis. If a beta blocker cannot be used, verapamil or diltiazem should be used for rate control. Recommendations for therapy to prevent thromboembolic complications are as for patients without hyperthyroidism.
Atrial Fibrillation During Pregnancy
The guidelines recommend digoxin, a beta blocker, or a nondihydropyridine calcium channel antagonist for rate control of AF during pregnancy. DC cardioversion is recommended if there is hemodynamic instability.
Except in patients with a low-risk profile, either aspirin or an anticoagulant is recommended for prevention of thromboembolic complications, depending on the stage of pregnancy (see Chapter 90). Unfractionated or low-molecular-weight heparin can be considered during the first trimester and last month of pregnancy in patients with risk factors for thromboembolism, and an oral anticoagulant can be considered during the second trimester in patients at high risk of thromboembolism.
When AF occurs during pregnancy, quinidine or procainamide can be considered for pharmacologic cardioversion in hemodynamically stable patients.
Hypertrophic Cardiomyopathy
The guidelines point out that there are not adequate data on the best rhythm-control medication to use for AF in the setting of HCM. The preferred therapy is either disopyramide plus a beta blocker, verapamil, or diltiazem for rate control or amiodarone by itself.
Pulmonary Disease
The primary therapy for AF in the setting of an acute pulmonary illness or exacerbation of chronic pulmonary disease should be correction of hypoxemia and acidosis. Verapamil or diltiazem is recommended for rate control in patients with obstructive pulmonary disease. Theophylline and beta-adrenergic agonists are not recommended in patients with bronchospastic disease, and beta blockers, sotalol, propafenone, and adenosine are not recommended in patients with obstructive lung disease.
Reference
1. Fuster V, Ryden LE, Cannom DS, et al. 2011 ACCF/AHA/HRS focused updates incorporated into the ACC/AHA/ESC 2006 guidelines for the management of patients with atrial fibrillation: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Circulation. 2011;123:e269–e367.