Chapter 653 Disorders of the Sweat Glands
Eccrine glands are found over nearly the entire skin surface and provide the primary means, through evaporation of the water in sweat, of cooling the body. These glands have no anatomic relationship to hair follicles and secrete a relatively large amount of odorless aqueous sweat. In contrast, apocrine sweat glands are limited in distribution to the axillae, anogenital skin, mammary glands, ceruminous glands of the ear, Moll glands in the eyelid, and selected areas of the face and scalp. Each apocrine gland duct enters the pilosebaceous follicle at the level of the infundibulum and secretes a small amount of a complex, viscous fluid that, on alteration by microorganisms, produces a distinctive body odor. Some disorders of these two types of sweat glands are similar pathogenetically, whereas others are unique to a given gland.
Anhidrosis
Neuropathic anhidrosis results from a disturbance in the neural pathway from the control center in the brain to the peripheral efferent nerve fibers that activate sweating. Disorders in this category, which are characterized by generalized anhidrosis, include tumors of the hypothalamus and damage to the floor of the 3rd ventricle. Pontine or medullary lesions may produce anhidrosis of the ipsilateral face or neck and ipsilateral or contralateral anhidrosis of the rest of the body. Peripheral or segmental neuropathies, caused by leprosy, amyloidosis, diabetes mellitus, alcoholic neuritis, or syringomyelia, may be associated with anhidrosis of the innervated skin. Various autonomic disorders are also associated with altered eccrine sweat gland function.
At the level of the sweat gland, anticholinergics (drugs such as atropine and scopolamine) may paralyze the sweat glands. Acute intoxication with barbiturates or diazepam has produced necrosis of sweat glands, resulting in anhidrosis with or without erythema and bullae. Eccrine glands are largely absent throughout the skin or are present in a localized area among patients with anhidrotic ectodermal dysplasia or localized congenital absence of sweat glands, respectively. Infiltrative or destructive disorders that may produce atrophy of sweat glands by pressure or scarring include scleroderma, acrodermatitis chronica atrophicans, radiodermatitis, burns, Sjögren syndrome, multiple myeloma, and lymphoma. Obstruction of sweat glands may occur in miliaria and in a number of inflammatory and hyperkeratotic disorders, such as the ichthyoses, psoriasis, lichen planus, pemphigus, porokeratosis, atopic dermatitis, and seborrheic dermatitis. Occlusion of the sweat pore may also occur with the topical agents aluminum and zirconium salts, formaldehyde, or glutaraldehyde.
Diverse disorders that are associated with anhidrosis by unknown mechanisms include dehydration; toxic overdose with lead, arsenic, thallium, fluorine, or morphine; uremia; cirrhosis; endocrine disorders such as Addison disease, diabetes mellitus, diabetes insipidus, and hyperthyroidism; and inherited conditions such as Fabry disease, Franceschetti-Jadassohn syndrome, which combines features of incontinentia pigmenti and anhidrotic ectodermal dysplasia, and familial anhidrosis with neurolabyrinthitis.
Anhidrosis may be complete, but in many cases, what appears clinically to be anhidrosis is actually hypohidrosis caused by anhidrosis of many but not all eccrine glands. Compensatory, localized hyperhidrosis of the remaining functional sweat glands may occur, particularly in diabetes mellitus and miliaria. The primary complication of anhidrosis is hyperthermia, seen primarily in anhidrotic ectodermal dysplasia or in otherwise normal preterm or full-term neonates who have immature eccrine glands.
Hyperhidrosis
Etiology/Pathogenesis
Hyperhidrosis is excessive sweating beyond what is physiologically necessary for temperature control and occurs in 3% of the population with about half having axillary hyperhidrosis. The numerous disorders that may be associated with increased production of eccrine sweat may also be classified into those with neural mechanisms involving an abnormality in the pathway from the neural regulatory centers to the sweat gland and those that are non-neurally mediated and occur by direct effects on the sweat glands (Table 653-1).
Clinical manifestations
The average age at onset of hyperhidrosis is 14-25 yr. The excess sweating may be continuous or may occur in response to emotional stimuli. In severe cases, sweat may be seen to drip constantly from the hands.
Treatment
Excessive sweating of the palms and soles (volar hyperhidrosis) and axillary sweating may respond to 20% aluminum chloride in anhydrous ethanol applied under occlusion for several hours, iontophoresis (palms and soles only), injection with botulinum toxin, therapy with oral anticholinergics, or in severe, refractory cases, cervicothoracic or lumbar sympathectomy.
Miliaria
Etiology/Pathogenesis
Miliaria results from retention of sweat in occluded eccrine sweat ducts. The keratinous plug does not form until the later stages of the disease, and therefore, does not appear to be the primary cause of the sweat duct obstruction. The initial obstruction is postulated to be due to swelling of the ductal epidermal cells, perhaps from imbibition of water. Retrograde pressure may result in rupture of the duct and leakage of sweat into the epidermis and/or the dermis. The eruption is most often induced by hot, humid weather, but it may also be caused by high fever. Infants who are dressed too warmly may demonstrate this eruption indoors, even during the winter.
Clinical Manifestations
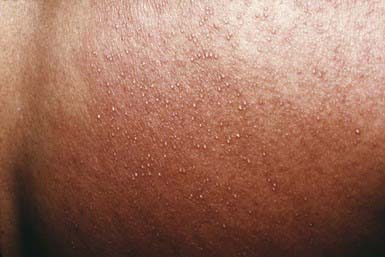
In miliaria crystallina, asymptomatic, noninflammatory, pinpoint, clear vesicles may suddenly erupt in profusion over large areas of the body surface, leaving brawny desquamation on healing (Fig. 653-1). This type of miliaria occurs most frequently in newborn infants because of the relative immaturity and delayed patency of the sweat duct and the tendency for infants to be nursed in relatively warm, humid conditions. It may also occur in older patients with hyperpyrexia.
Miliaria rubra is a less superficial eruption characterized by erythematous, minute papulovesicles that may impart a prickling sensation. The lesions are usually localized to sites of occlusion or to flexural areas, such as the neck, groin, and axillae, where friction may have a role in their pathogenesis. Involved skin may become macerated and eroded. Lesions of miliaria rubra, however, are extrafollicular.
Repeated attacks of miliaria rubra may lead to miliaria profunda, which is due to rupture of the sweat duct deeper in the skin, at the level of the dermal-epidermal junction. Severe, extensive miliaria rubra or miliaria profunda may result in disturbance of heat regulation. Lesions of miliaria rubra may become infected, particularly in malnourished or debilitated infants, leading to development of periporitis staphylogenes, which involves extension of the process from the sweat duct into the sweat gland.
Histology
Histologically, miliaria crystallina reveals an intracorneal or subcorneal vesicle in communication with the sweat duct, whereas in miliaria rubra, one sees focal areas of spongiosis and spongiotic vesicle formation in close proximity to sweat ducts that generally contain a keratinous plug.
Differential Diagnosis
The clarity of the fluid, superficiality of the vesicles, and absence of inflammation permit differentiation of miliaria crystalline from other blistering disorders. Miliaria rubra may be confused with or superimposed on other diaper area eruptions, including candidosis and folliculitis.
Treatment
All forms of miliaria respond dramatically to cooling of the patient by regulation of environmental temperatures and by removal of excessive clothing; administration of antipyretics is also beneficial to patients with fever. Topical agents are usually ineffective and may exacerbate the eruption.
Bromhidrosis
The excessive odor that characterizes bromhidrosis may result from alteration of either apocrine or eccrine sweat. Apocrine bromhidrosis develops after puberty as a result of the formation of short-chain fatty acids and ammonia by the action of anaerobic diphtheroids on axillary apocrine sweat. Eccrine bromhidrosis is caused by microbiologic degradation of stratum corneum that has become softened by excessive eccrine sweat. The soles of the feet and the intertriginous areas are the primary affected sites. Hyperhidrosis, warm weather, obesity, intertrigo, and diabetes mellitus are predisposing factors. Treatments that may be helpful include cleansing with germicidal soaps, topical clindamycin or erythromycin, or topical application of aluminum or zirconium. Treatment of any associated hyperhidrosis is mandatory.
Hidradenitis Suppurativa
Etiology/Pathogenesis
Hidradenitis suppurativa is a disease of the apocrine gland–bearing areas of the skin. Pathogenesis of hidradenitis suppurativa is controversial. It is now believed that it is a primary inflammatory disorder of the hair follicle and not solely an alteration of apocrine glands. It is considered a part of the follicular occlusion tetrad, along with acne conglobata, dissecting cellulites of the scalp, and pilonidal sinus. Bacterial infection, particularly with Staphylococcus aureus, Streptococcus milleri, Escherichia coli, and, possibly, anaerobic streptococci, appears to be important in the progressive dilatation below the obstruction, leading to rupture of the duct, inflammation, sinus tract formation, and destructive scarring.
Clinical Manifestations
Hidradenitis suppurativa is a chronic, inflammatory, suppurative disorder of the apocrine glands in the axillae, the anogenital area, and, occasionally, the scalp, posterior aspect of the ears, female breasts, and periumbilical area. Onset of clinical manifestations is sometimes preceded by pruritus or discomfort and usually occurs during puberty or early adulthood. Solitary or multiple painful erythematous nodules, deep abscesses, and contracted scars are sharply confined to areas of skin containing apocrine glands. When the disease is severe and chronic, sinus tracts, ulcers, and thick, linear fibrotic bands develop. Hidradenitis suppurativa tends to persist for many years, punctuated by relapses and partial remissions. Complications include cellulitis, ulceration, and burrowing abscesses that may perforate adjacent structures, forming fistulas to the urethra, bladder, rectum, or peritoneum. Episodic inflammatory arthritis develops in some patients.
Histology
Early lesions are characterized by a keratinous plug in the apocrine duct or hair follicle orifice and by cystic distention of the follicle. The process generally but not necessarily extends into the apocrine gland. Later changes include inflammation within and around apocrine glands and the presence of groups of cocci within apocrine glands and in the adjacent dermis. Scarring may obliterate skin appendages.
Differential Diagnosis
Early lesions of hidradenitis suppurativa are often mistaken for infected epidermal cysts, furuncles, scrofuloderma, actinomycosis, cat-scratch disease, granuloma inguinale, or lymphogranuloma venereum. Sharp localization to areas of the body that bear apocrine glands, however, should suggest hidradenitis. When involvement is limited to the anogenital region, the condition may be difficult to distinguish from Crohn disease.
Treatment
Conservative management includes cessation of smoking, weight loss, and avoidance of irritation of the affected area. Warm compresses and topical antiseptic or antibacterial soaps may also be helpful. For mild, early, disease, topical clindamycin 1% is the treatment of choice. For more severe disease therapy may be initiated with tetracycline (500 mg bid), doxycycline (100 mg bid), or minocycline (100 mg bid). Some patients require intermittent or long-term antibiotic treatment. Oral retinoids (1 mg/kg/day) for 5-6 mo may also be effective. Oral contraceptive agents, which contain a high estrogen : progesterone ratio and low androgenicity of the progesterone, are another alternative. Surgical measures may be required for control or cure.
Fox-Fordyce Disease
Clinical Manifestations
This disease is most common in females and manifests during puberty to the 3rd decade of life as pruritus in the axillae. Pruritus is exacerbated by emotional stress and stimuli that induce apocrine sweating. Dome-shaped, skin-colored to slightly hyperpigmented, follicular papules develop in the pruritic areas.
Gelbard CM, Epstein H, Hebert A. Primary pediatric hyperhidrosis: a review of current treatment options. Pediatr Dermatol. 2008;25:591-598.
Kineston DP, Martin KO. Pruritic axillary papules: Fox-Fordyce disease. Am Fam Physician. 2008;15:1735-1736.
Lam J, Krakowski AC, Friedlander SF. Hidradenitis suppurativa (acne inverse): management of a recalcitrant disease. Pediatr Dermatol. 2007;24:465-473.
Sellheyer K, Krahl D. What causes acne inverse (or hidradenitis suppurativa)?—the debate continues. J Cutan Pathol. 2008;35:701-703.