39: Pediatric nursing interventions and skills
Marilyn J. Hockenberry
Concepts
![]() http://evolve.elsevier.com/Perry/maternal
http://evolve.elsevier.com/Perry/maternal
General concepts related to pediatric procedures
Informed consent
Before undergoing any invasive procedure, the patient or the patient’s legal surrogate must receive sufficient information on which to make an informed health care decision. Informed consent should include the nature of the illness or condition, proposed care, or treatment; potential risks, benefits, and alternatives; and what might happen if the patient chooses not to consent. In addition, discussions should include the procedure team roles, including trainees involved in care (Firdouse, Wajchendler, Koyle, et al., 2017). To obtain valid informed consent, health care providers must meet the following three conditions:
- 1. The person must be capable of giving consent; he or she must be over the age of majority (usually age 18 years) and must be considered competent (i.e., possess the mental capacity to make choices and understand their consequences).
- 2. The person must receive the information needed to make an intelligent decision.
- 3. The person must act voluntarily when exercising freedom of choice without force, fraud, deceit, duress, or other forms of constraint or coercion.
The patient has the right to accept or refuse any health care. If a patient is treated without consent, the hospital or health care provider may be charged with assault and held liable for damages. In addition, consent is a two-way process that requires both the health care provider to share all required information and the patient to hear and understand the information. Health care providers must deliver information in the appropriate language and health literacy level for the patient and family. There must also be adequate time for questions and opportunity to clarify concerns. Informed consent and medical decision making is not a one-time event but an ongoing process that requires continual communication among the health care team, patient, and caregivers (American Academy of Pediatrics, Committee on Bioethics, 2016).
Requirements for obtaining informed consent
Written informed consent of the patient, parent, or legal guardian is usually required for medical or surgical treatment of a minor, including many diagnostic procedures. One universal consent is not sufficient. Separate informed permissions must be obtained for each surgical or diagnostic procedure, including the following:
- • Major surgery
- • Minor surgery (e.g., cutdown, biopsy, dental extraction, suturing a laceration [especially one that may have a cosmetic effect], removal of a cyst, closed reduction of a fracture)
- • Diagnostic tests with an element of risk (e.g., bronchoscopy, angiography, lumbar puncture [LP], cardiac catheterization, bone marrow aspiration)
- • Medical treatments with an element of risk (e.g., blood transfusion, thoracentesis or paracentesis, radiotherapy)
Other situations that require patient or parental consent include the following:
Decision making involving the care of older children and adolescents (older than 7 years of age with appropriate age, maturity, and psychologic state) should include the patient’s assent (if feasible) as well as the parent’s consent (Poston, 2016). Assent means that the child or adolescent has been informed about the proposed treatment, procedure, or research and is willing to permit a health care provider to perform it. If the child or adolescent merely fails to object, this does not equate assent. Assent should include the following:
- • Helping the patient achieve a developmentally appropriate awareness of the nature of his or her condition
- • Telling the patient what he or she can expect
- • Making a clinical assessment of the patient’s understanding
- • Soliciting an expression of the patient’s willingness to accept the proposed procedure
Health care providers should use multiple methods to provide information, including age-appropriate methods (e.g., videos, peer discussion, diagrams, written materials). The nurse should provide an assent form for the child to sign, and the child should keep a copy. By including the child in the decision-making process and gaining his or her acceptance, staff members demonstrate respect for the child. Assent is not a legal requirement but an ethical one to protect the rights of children. Chapter 36 provides further discussion on the dying child’s right to refuse treatment.
Eligibility for giving informed consent
Informed consent of parents or legal guardians
Parents have full responsibility for the care and rearing of their minor children, including legal control over them. As long as children are minors, their parents or legal guardians are required to give informed consent before medical treatment is rendered or any procedure is performed. If the parents are married to each other, consent from only one parent is required for nonurgent pediatric care. If the parents are divorced, consent usually rests with the parent who has legal custody (American Academy of Pediatrics, Committee on Bioethics, 2016). Emergency care of a pediatric patient should never be withheld due to the absence of a parent or legal guardian. Parents also have a right to withdraw consent later. If the legal caregivers disagree on the treatment course, it is within the health care providers’ scope to request consultation of a hospital ethics board to determine what care is in the best interest of the patient (Dahl, Sinha, Rosenberg, et al., 2015).
Evidence of consent
Regulations on obtaining informed consent vary from state to state, and policies differ at each health care facility. It is the physician’s legal responsibility to explain the procedure, risks, benefits, and alternatives. The nurse witnesses the patient’s, parent’s, or legal guardian’s signature on the consent form and may reinforce what the patient has been told. A signed consent form is the legal document that signifies that the process of informed consent has occurred. If parents are unavailable to sign consent forms, verbal consent may be obtained via the telephone in the presence of two witnesses. Both witnesses record that informed consent was given and by whom. Their signatures indicate that they witnessed the verbal consent. If the parents or legal guardians cannot be reached for an extended period, the nurse may request the assistance of social work or law enforcement officers to locate a legal guardian.
Informed consent of mature and emancipated minors
State laws differ with regard to the age of majority, the age at which a person is considered to have all the legal rights and responsibilities of an adult. In most states, 18 years is the age of majority. Competent adults can give informed consent on their own behalf. An emancipated minor is one who is legally under the age of majority but is recognized as having the legal capacity or social status of an adult under circumstances prescribed by state law, such as pregnancy, marriage, high school graduation, independent living, or military service. A mature minor exception to consent laws is recognized in a few states for children age 14 years and older who possess the maturity and cognitive abilities to understand all elements of informed consent and make a choice based on the information. Legal action may be required for designation as a mature minor (American Academy of Pediatrics, Committee on Bioethics, 2016).
Treatment without parental consent
Exceptions to requiring parental consent before treating minor children occur in situations in which children need urgent medical or surgical treatment and a parent is not readily available to give consent or refuses to give consent. For example, a child may be brought to an emergency department accompanied by a grandparent, child care provider, teacher, or others. In the absence of parents or legal guardians, persons in charge of the child may be given permission by the parents to give informed consent by proxy. A medical screening examination is required by federal law under the Emergency Medical Treatment and Active Labor Act for all patients presenting to an emergency center. In emergencies, including danger to life or the possibility of permanent injury, appropriate care should not be withheld or delayed because of problems obtaining consent (American Academy of Pediatrics, Committee on Bioethics, 2016). The nurse should document any efforts made to obtain consent.
Parental refusal to give consent for life-saving treatment or to prevent serious harm can occur and requires notification to child protective services to render emergency treatment. For example, Jehovah’s Witnesses commonly choose to avoid receiving blood products due to religious beliefs. In cases where a blood product is crucial for the child’s survival, it is important to work together with the family, medical team, and child protective services to determine the course of action that is in the best interest of the child. “Parental decision-making should primarily be understood as parents’ responsibility to support the interests of their child and to preserve family relationships, rather than being focused on their rights to express their own autonomous choices” (American Academy of Pediatrics, Committee on Bioethics, 2016). Evaluation for child abuse or neglect can occur without parental consent and without notification to the state before evaluation in most states.
Adolescents, consent, and confidentiality
The Health Insurance Portability and Accountability Act of 1996 (HIPAA) was passed to help protect and safeguard the security and confidentiality of health information. Because adolescents are not yet adults, parents have the right to make most decisions on their behalf and receive information. Adolescents, however, are more likely to seek care in a setting in which they believe their privacy will be maintained. All 50 states have enacted legislation that entitles adolescents to consent to treatment without the parents’ knowledge to one or more “medically emancipated” conditions such as sexually transmitted infections, mental health services, substance abuse and addiction, pregnancy, and contraceptive advice (American Academy of Pediatrics, Committee on Bioethics, 2016). Consent to abortion is controversial, and statutes vary widely by state. The Planned Parenthood Federation of America provides consent and notification law requirements listed by state. State law preempts HIPAA regardless of whether that law prohibits, mandates, or allows discretion about a disclosure.
Informed consent and parental right to the child’s medical chart
Some state statutes give parents the unrestricted right to a copy of their children’s medical records. In states without statutes, the best practice is to allow parents to review or have a copy of minors’ charts under reasonable circumstances. Practitioners should avoid restrictive requirements such as review permitted only in the presence of a clinician. Rather, an appropriate practitioner should be available to answer any questions that parents may have during their reviews. It is important for the nurse to check the state and health care institution’s policies surrounding providing printed copies of medical records to patients and families.
Preparation for diagnostic and therapeutic procedures
Technologic advances and changes in health care have resulted in more pediatric procedures being performed in a variety of settings. Many procedures are both stressful and painful experiences. For many procedures, the focus of care is psychologic preparation of the child and family. However, some procedures require the administration of sedatives and analgesics.
The child life specialist is an especially valued member of the health care team when preparing a child for diagnostic and therapeutic procedures. Child life specialists address the psychosocial concerns that accompany stressful life experiences by promoting optimal child development and minimizing adverse effects. Child life specialists receive advanced education and training in the developmental stages of childhood as well as strategies to cope with illness and injury. Therapeutic play, procedural preparation and support, developmentally appropriate education, and promoting normalcy are all significant ways in which the child life specialist can have a positive impact on the health care experience of the child and family. Child life specialists and nursing staff can work together to implement evidence-based interventions to decrease fear, anxiety, and discomfort experienced by children in the health care environment (Association of Child Life Professionals, 2021).
Psychologic preparation
Preparing children for procedures decreases their anxiety, promotes their cooperation, supports their coping skills and may teach them new ones, and facilitates a feeling of mastery in experiencing a potentially stressful event. Many institutions have developed preadmission teaching programs designed to educate the pediatric patient and family by offering hands-on experience with hospital equipment, the procedure performed, and departments they will visit. Preparatory methods may be formal, such as group preparation for hospitalization. Most preparation strategies are informal, focus on providing information about the experience, and are directed at stressful or painful procedures. The most effective preparation includes the provision of sensory-procedural information and helping the child develop coping skills, such as imagery, distraction, or relaxation.
The Applying Evidence to Practice boxes describe general guidelines for preparing children for procedures along with age-specific guidelines that consider children’s developmental needs and cognitive abilities. In addition to these suggestions, nurses should consider the child’s temperament, existing coping strategies, and previous experiences in individualizing the preparatory process. Stress point coping can be used to determine the child’s most stressful or upsetting part of previous procedural experiences (Thompson, 2018). Once the stress point is identified, coping strategies to address this specific point in the procedure can be discussed with the child. Children who are distractible and highly active or those who are “slow to warm up” may need individualized sessions—shorter for active children and more slowly paced for shy children. Whereas children who tend to cope well may need more emphasis on using their present skills, those who appear to cope less adequately can benefit from more time devoted to simple coping strategies, such as relaxing, breathing, counting, squeezing a hand, or singing. Children with previous health-related experiences still need preparation for repeat or new procedures; however, the nurse must assess what they know, correct their misconceptions, supply new information, and introduce new coping skills as indicated by their previous reactions. Especially for painful procedures, the most effective preparation includes providing sensory-procedural information and helping the child develop coping skills, such as imagery or relaxation (see Evidence-Based Practice boxes).
All experiences of childhood can affect development and influence the way in which a child responds to the health care environment, even into adulthood. Adverse childhood experiences can include abuse, neglect, substance abuse, or any other traumatic experiences and may result in negative health behaviors, chronic health conditions, and even early death (Centers for Disease Control and Prevention, 2019). While in the health care environment, children can experience medical traumatic stress during difficult or frightening medical events or from simply being present in the hospital environment. As care providers, it is important to practice trauma-informed care; consider the impact that past physical, mental, and emotional trauma may have on a patient; and adapt care appropriately. This may include reducing distress through pain control, offering choices, psychologic preparation for procedures, providing emotional support, and including the family in what health care providers may perceive as routine care (National Child Traumatic Stress Network, 2019).
| Words and Phrases to Avoid | Suggested Substitutions |
|---|---|
| Shot, bee sting, stick | Medicine under the skin, poke that will feel like a pinch |
| Organ | Place in body |
| Test | To see how (specify body part) is working |
| Incision, cut | Make an opening |
| Edema | Puffiness |
| Stretcher, gurney | Rolling bed, bed on wheels |
| Stool, urine | Child’s usual term |
| Dye | Medicine to help place in your body show up on a picture |
| Pain | Hurt, discomfort, “owie,” “boo-boo,” sore, achy, scratchy, pinch |
| Deaden, numb | Not feel body part as much |
| Fix | Make better |
| Take (as in “take your temperature”) | See how warm you are |
| Take (as in “take your blood pressure”) | Check your pressure, hug your arm |
| Put to sleep, anesthesia | Different kind of sleep so you won’t feel anything |
| Catheter | Soft tube, small straw |
| Monitor | Television screen |
| Electrodes | Stickers, ticklers |
| Specimen | Take some blood |
Children differ in their “information-seeking dimension.” Some actively ask for information about the intended procedure, but others characteristically avoid information. Parents can often guide nurses in deciding how much information is enough for the child because parents know whether the child is typically inquisitive or satisfied with short answers. Asking older children their preferences about the amount of explanation is also important.
The exact timing of the preparation for a procedure varies with the child’s age and developmental level and the type of procedure. No exact guidelines govern timing, but in general, the younger the child, the closer the explanation should be to the actual procedure to prevent undue fantasizing and worrying. Concurrent preparation is a strategy that can be used during a procedure to explain what a child can expect to occur and sense immediately before it happens (Thompson, 2018). This can be helpful for emergency procedures, for a highly anxious child, or for younger age groups where extensive prior preparation is not possible or beneficial. With complex procedures, more time may be needed for assimilation of information, especially with older children. For example, the explanation for an injection can immediately precede the procedure for all ages, but preparation for surgery may begin the day before for young children and a few days before for older children, although the nurse should elicit older children’s preferences.
Establish trust and provide support
The nurse who has spent time with and established a positive relationship with a child usually finds it easier to gain cooperation. If the relationship is based on trust, the child will associate the nurse with caregiving activities that give comfort and pleasure most of the time rather than discomfort and stress. If the nurse does not know the child, it is best for the nurse to be introduced by another staff person whom the child trusts. The first visit with the child should not include any painful procedure and ideally should focus on the child first and then on an explanation of the procedure. A simple way to begin the process of creating trust is by engaging in play with the patient through favorite activities or toys. Body language is another key element of promoting trust. Positive body language, such as sitting instead of standing, and avoiding the use of technical medical terminology in conversation can enhance the therapeutic caregiver relationship with the child and family (Lidgett, 2016).
Parental presence and support
Children need support during procedures, and for young children, the greatest source of support is the parents. They represent security, protection, safety, and comfort. Parental presence has a positive impact on the level of pain and negative behavior experienced by the child, as well as on parental distress and satisfaction (Saglik & Caglar, 2018). In addition, there is no difference in technical complications when parents remain with children. However, controversy exists regarding the role parents should assume during the procedure, especially if discomfort is involved. The nurse should assess the parents’ preferences for assisting, observing, or waiting outside the room, as well as the child’s preference for parental presence. Respect the child’s and parents’ choices. Give parents who wish to stay appropriate explanation about the procedure and coach them about where to sit or stand and what to say or do to help the child through the procedure. Support parents who do not want to be present in their decision and encourage them to remain close by so that they can be available to support the child immediately after the procedure. It can be helpful for parents to assist the health care team in identifying an alternative support person for their child, such as a child life specialist or nurse, if they are unable to be present during the procedure. Parents should know that someone will be with their child to provide support. Ideally, this person should inform the parents after the procedure about how the child did.
Provide an explanation
Age-appropriate explanations are one of the most widely used interventions for reducing anxiety in children undergoing procedures. Before performing a procedure, explain what is to be done, what sensations the child may feel, what is expected of the child, and why the procedure is being done. It is important that the child understand that the procedure is not punishment. The explanation should be short, simple, and appropriate to the child’s level of comprehension. Long explanations may increase anxiety in a young child. When explaining the procedure to parents with the child present, the nurse uses language appropriate to the child because unfamiliar words can be misunderstood (see Table 39.1). If the parents need additional preparation, it is done in an area away from the child. Teaching sessions are planned at times most conducive to the child’s learning (e.g., after a rest period) and for the usual span of attention.
Special equipment is not necessary for preparing a child, but for young children who cannot yet think conceptually, using objects to supplement verbal explanation is important. Children often learn through behavior modeling such as seeing a doll experience the procedure, watching a video, or seeing a picture. In addition, allowing children to handle actual items that will be used in their care, such as a stethoscope, sphygmomanometer, or oxygen mask, helps them develop familiarity with these items and reduces the fear often associated with their use. Miniature versions of hospital items such as gurneys and x-ray and intravenous (IV) equipment can be used to explain what the children can expect and permit them to safely experience situations that are unfamiliar and potentially frightening. Written and illustrated materials are also valuable aids to preparation.a
Physical preparation
One area of special concern is the administration of appropriate sedation and analgesia before stressful procedures.
Performance of the procedure
Supportive care continues during the procedure and can be a major factor in a child’s ability to cooperate. Ideally, the same nurse who explains the procedure should perform or assist with the procedure. The child may also benefit from a parent or trusted caregiver who can offer coaching techniques and support during the procedure. Before beginning, all equipment is assembled, and the room is readied to prevent unnecessary delays and interruptions that increase the child’s anxiety. Minimizing the number of people present and allowing one person to speak during the procedure also can decrease the child’s anxiety.
To promote long-term coping and adjustment, give special consideration to the patient’s age, coping skills, and procedure to be performed in determining where a procedure will occur. Treatment rooms should be used for procedures requiring sedation, such as bone marrow aspirates and LPs in younger children. Traumatic procedures should never be performed in “safe” areas, such as the playroom. If the procedure is lengthy, avoid conversation that could be misinterpreted by the child. As the procedure is nearing completion, the nurse may inform the child “this is the last piece of tape” or simply inform the child when the procedure is completed.
Expect success
Nurses who approach children with confidence and who convey the impression that they expect to be successful are less likely to encounter difficulty. It is best to approach a child as though cooperation is expected. Children sense anxiety and uncertainty in an adult and respond by striking out or actively resisting. Although it is not possible to eliminate such behavior in every child, a firm approach with a positive attitude tends to convey a feeling of security to most children.
Involve the child
Involving children helps gain their cooperation. Permitting choices gives them some measure of control. However, a choice is given only in situations in which one is available. Asking children, “Do you want to take your medicine now?” leads them to believe they have an option and provides them the opportunity to legitimately refuse or delay the medication. This places the nurse in an awkward, if not impossible, position. It is much better to state firmly, “It’s time to drink your medicine now.” Children usually like to make choices, but the choice must be one that they do indeed have (e.g., “It’s time for your medicine. Do you want to drink it plain or with a little water?”).
Many children respond to tactics that appeal to their maturity or courage. This also gives them a sense of participation and achievement. For example, preschool children will be proud that they can hold the dressing during the procedure or remove the tape. The same is true for school-age children, who often cooperate with minimal resistance.
Provide distraction
Distraction is a powerful coping strategy during painful procedures (Dastgheyb, Fishlock, Daskalakis, et al., 2018). It is accomplished by focusing the child’s attention on something other than the procedure. Singing favorite songs, listening to music with a headset, counting aloud, or blowing bubbles to “blow the hurt away” are effective techniques.
Allow expression of feelings
The child should be allowed to express feelings of anger, anxiety, fear, frustration, or any other emotion. It is natural for children to strike out in frustration or to try to avoid stress-provoking situations. The child needs to know that it is all right to cry. Behavior is children’s primary means of communication and coping and should be permitted unless it inflicts harm on them or those caring for them. Harmful behavior should be acknowledged, and appropriate limitations should be set to promote patient and caregiver safety.
Postprocedural support
After the procedure, the child continues to need reassurance that he or she performed well and is accepted and loved. If the parents did not participate, the child is united with them as soon as possible so that they can provide comfort.
Encourage expression of feelings
Planned activity after the procedure is helpful in encouraging constructive expression of feelings. For verbal children, reviewing the details of the procedure can clarify misconceptions and garner feedback for improving the nurse’s preparatory strategies. Play is an excellent activity for all children. Infants and young children should have the opportunity for gross motor movement. Older children are able to vent their anger and frustration in acceptable pounding or throwing activities. Play-Doh is a remarkably versatile medium for pounding and shaping. Dramatic play provides an outlet for anger and places the child in a position of control, in contrast to the position of helplessness in the real situation. Puppets also allow the child to communicate feelings in a nonthreatening way. One of the most effective interventions is therapeutic play, which includes well-supervised activities such as permitting the child to give an injection to a doll or stuffed toy to reduce the stress of injections (Fig. 39.1).

Three children with hand gloves sitting around the round table playing with hospital equipment in a hospital. A baby toy is placed on the table, which is in front of them. Among the three children, the one at the center is wearing a stethoscope.
Positive reinforcement
Children need to hear from adults that they did the best they could in the situation—no matter how they behaved. There should be specific acknowledgment of what aspect of the procedure the child performed well. It is important for children to know that their worth is not being judged based on their behavior in a stressful situation. Reward systems, such as earning stars, stickers, or a supportive care program such as Beads of Courage that celebrates a child’s milestones in medical treatment, are appealing to children.b
Returning to the child a short while after the procedure helps the nurse strengthen a supportive relationship. Relating with the child in a relaxed and nonstressful period allows him or her to see the nurse not only as someone associated with stressful situations but also as someone with whom to share pleasurable experiences.
Use of play in procedures
The use of play is an integral part of relationships with children. As such, its value in specific situations is discussed throughout this book, such as in Chapter 38 in relation to hospitalization. Many institutions have elaborate and well-organized play areas and programs under the direction of child life specialists. Other institutions have limited facilities. No matter what the institution provides for children, nurses can include play activities as part of nursing care. Play can be used to teach, express feelings, or achieve a therapeutic goal. Consequently, it should be included in preparing children for and encouraging their cooperation during procedures. Play sessions after procedures can be structured, such as directed toward needle play, or general, with a wide variety of equipment available for children to play with.
Routine procedures such as measuring blood pressure and oral administration of medication may be of concern to children. Box 39.1 describes suggestions for incorporating play into nursing procedures and activities for the hospitalized child that facilitate learning and adjustment to a new situation.
Preparing the family
The process of patient education involves giving the family information about the child’s condition, the regimen that must be followed and why, and other health teaching as indicated. The goal of this education is to enable the family to modify behaviors and adhere to the regimen that has been mutually established (see Evidence-Based Practice box).
If equipment will be needed at home (e.g., suction machines, syringes), begin making the necessary arrangements in advance so that discharge can proceed smoothly. Whenever possible, make arrangements for the family to use the same equipment in the home that they are using in the hospital. This allows them to become familiar with the items. In addition, the staff can help troubleshoot the equipment in a controlled environment. Plan the teaching sessions well in advance of the time the family will be responsible for performing the care. The more complex the procedure, the more time is needed for training.
Review the instructions with family members (see Evidence-Based Practice box). Encourage note taking if they desire. Allow ample practice time under supervision. At least one family member, but preferably two members, should demonstrate the procedure before they are expected to care for the child at home. Provide the family with the telephone numbers of resource individuals who are available to assist them in the event of a problem.
Surgical procedures
Preoperative care
Children experiencing surgical procedures require both psychologic and physical preparation. An important concern is restriction of food and fluids before surgery to avoid pulmonary aspiration during anesthesia. In addition, fasting for too long can cause discomfort, headache, dehydration, or hypoglycemia and can delay recovery and hospital discharge (Dolgun, Yavuz, Eroğlu, et al., 2017). Infants require special attention to fluid needs. They should not be without oral fluids for an extended period preoperatively to avoid glycogen depletion and dehydration. If surgical procedures are delayed, it is the nurse’s responsibility to communicate with the surgical team to adjust fasting guidelines appropriately (Williams, Johnson, Guzzetta, et al., 2014). Table 39.2 contains current preoperative fasting guidelines.
| Ingested Material | Minimum Fasting Period (h)b |
|---|---|
| Clear liquidsc | >2 |
| Breast milk | 4 |
| Infant formula | 6 |
| Nonhuman milkd | 6 |
| Light meale | 6 |
aThese recommendations apply to healthy patients who are undergoing elective procedures. They are not intended for women in labor. Following the guidelines does not guarantee that complete gastric emptying has occurred.
bFasting periods noted in chart apply to all ages.
cExamples of clear liquids include water, fruit juices without pulp, carbonated beverages, clear tea, and black coffee.
dBecause nonhuman milk is similar to solids in gastric emptying time, the amount ingested must be considered when determining appropriate fasting period.
eA light meal typically consists of toast and clear liquids. Meals that include fried or fatty foods or meat may prolong gastric emptying time. Both the amount and type of foods ingested must be considered when determining an appropriate fasting period.
(From American Society of Anesthesiologists, Committee on Standards and Practice Parameters. [2011]. Practice guidelines for preoperative fasting and the use of pharmacological agents to reduce the risk of pulmonary aspiration: Application to healthy patients undergoing elective procedures. Anesthesiology, 114[3], 495–511.)
In general, psychologic preparation is similar to that discussed earlier for any procedure and uses many of the same techniques used in preparing a child for hospitalization, such as films, books, brochures, play, and tours (see Chapter 38). Stress points before and after surgery include the admission process, blood tests, administration of preoperative medication (if prescribed), transport to the operating room, the mask on the face during induction, and the stay in the postanesthesia care unit. Wearing a hospital gown without the security of underpants or pajama bottoms can also be traumatic. Therefore these articles of clothing should be allowed to be worn into the operating room and removed after induction of anesthesia. Children are at higher risk of ineffective response to anesthesia and complications in the recovery period because of higher anxiety in the preoperative period associated with stranger anxiety (infants), separation anxiety (toddlers and preschoolers), and fear of injury or death (adolescents) (Al-Yateem, Brenner, Shorrab, et al., 2016).
Individualized psychologic intervention consisting of systematic preparation, rehearsal of the forthcoming events, and supportive care at each of these points has shown to be more effective than a single-session preparation or consistent supportive care without systematic preparation and rehearsal (Fortier, Kain, & Morton, 2015). A family-centered preoperative preparation program may consist of a tour of the perioperative areas with short explanations of the events 5 to 7 days before surgery, a video to take home and review a couple of times with additional explanations and demonstrations of perioperative processes, a mask to take home and practice with, pamphlets to guide parents on supporting children during induction, phone calls to coach parents on preparing children 1 or 2 days before surgery, toys and supplies in the holding area, and mobile phone applications with interactive tours and videos. In addition, the use of interactive electronic games, tablets, or therapy dogs in the preoperative setting can provide effective alternatives or complements to pharmacologic premedication. Therapeutic play is an effective strategy in preparing children, and increased familiarity with medical procedures can decrease anxiety.
Parental presence
Some institutions support parental presence during induction of anesthesia. Benefits of well-prepared children and parents along with parental presence during induction of anesthesia include reduced anxiety for children and parents, lower doses of postoperative analgesia, lower incidence of severe emergence delirium symptoms, decreased postoperative maladaptive behaviors, and shorter discharge time for short procedures (Fortier et al., 2015). Other studies have not supported a reduction in children’s anxiety (Erhaze, Dowling, & Devane, 2016; Manyande, Cyna, Yip, et al., 2015).
Concern exists regarding the appropriateness of parental presence during induction for all parents. Some parents may become upset by the rapid succession of induction events, by observing their child becoming limp, and by leaving the child in the care of strangers. Although parents who are anxious before surgery tend to become even more anxious after the induction, the reverse is true of parents with little anxiety. There is little evidence to suggest that parental presence during induction provides decreased anxiety for parents and caregivers (Al-Yateem et al., 2016). Appropriate education is essential to help parents understand the stages of anesthesia, what to expect, and how to support their child.
Preoperative sedation
The goals for using preoperative medications include anxiety reduction, amnesia, sedation, antiemetic effect, and reduction of secretions (Manworren & Fledderman, 2000). (Chapter 30 includes a discussion of pain management strategies for children undergoing surgery.) When drugs are administered, they should be delivered atraumatically via oral, intranasal, or IV routes. Numerous preanesthetic drug regimens are used with children, and no consensus exists on the optimal method. Some institutions promote distraction or parental support instead of medications due to the incidence of postoperative medication delirium (Batawi, 2015).
Intraoperative care
The role of the pediatric operating room nurse is to advocate for care of the patient in surgery through the verification of procedure and laterality, implants, skin preparation, necessary instrumentation, and supplies. The operating room nurse assesses, recognizes, and intervenes for the pediatric surgical patient at high risk for pressure injury due to patient diagnosis, patient anatomy, general anesthesia, intraoperative positioning, immobility, moisture, and nothing-by-mouth (NPO) status. Clear communication is used through collaboration with the interdisciplinary team (anesthesia, surgeon, scrub technician, nurses, radiology, etc.) to coordinate the intraoperative and postoperative disposition of the surgical patient. Family-centered care is provided through engaging the family in the preoperative procedure verification and updating them throughout the procedure (Herd & Rieben, 2014).
Postoperative care
Various psychologic and physical interventions and observations help prevent or minimize possible unpleasant effects from anesthesia and the surgical procedure. Although serious postoperative complications in healthy children undergoing surgery are rare, continuous monitoring of the child’s cardiopulmonary status is essential during the immediate postoperative period to reduce this risk (Pawar, 2012). Postanesthesia complications such as airway obstruction, postextubation croup, laryngospasm, and bronchospasm make maintaining a patent airway and maximum ventilation critical.
Monitoring the patient’s oxygen saturation and providing supplemental oxygen as needed, maintaining body temperature, and promoting fluid and electrolyte balance are important aspects of immediate postoperative care. Vital signs are continuously monitored, and each vital sign is evaluated in terms of side effects from anesthesia, shock, or respiratory compromise (Table 39.3).
A change in vital signs that demands immediate attention in the perioperative period is caused by malignant hyperthermia (MH), a potentially fatal pharmacogenetic disorder of muscle metabolism. In susceptible children, inhaled anesthetics and the muscle relaxant succinylcholine trigger the disorder, producing hypermetabolism. Symptoms of MH include hypercarbia (increasing end-tidal carbon dioxide [ETCO2]), elevated temperature, tachycardia, tachypnea, acidosis, muscle rigidity, hyperkalemia, and rhabdomyolysis. A family or previous history of sudden high fever associated with a surgical procedure and myotonia increase the risk for MH. Children who have successfully undergone prior surgery without adverse effects may still be considered susceptible (Salazar, Yang, Shen, et al., 2014).
Treatment of MH includes immediate discontinuation of the triggering agent, hyperventilation with 100% oxygen, and IV dantrolene sodium. If the child is hyperthermic, initiate cooling measures such as ice packs to the groin, axillae, and neck and iced nasogastric (NG) lavage. The surgery may be discontinued, or if it is emergent, it may be continued with a different anesthetic agent. The patient should be transferred to an intensive care unit for at least 36 hours and closely monitored for stabilization of vital signs, metabolic state, and possible recurrence of symptoms.
Managing pain is a major nursing responsibility after surgery. The nurse should assess pain frequently and administer analgesics to provide comfort and facilitate cooperation with postoperative care such as ambulation and deep breathing. Opioids are the most commonly used analgesics. Routinely scheduled IV analgesics, patient-controlled analgesia, regional blocks, and epidural infusions, rather than as-needed orders, provide excellent analgesia in postoperative pediatric patients.
Nonpharmacologic postoperative recovery interventions include the use of distraction, videos, interactive game applications, and therapy dogs. Therapy dogs can facilitate decreased pain perception, increase in activity, and emotional stabilization in the postoperative period (Calcaterra, Veggiotti, Palestrini, et al., 2015).
Because respiratory tract infections are a potential complication of anesthesia, make every effort to aerate the lungs and remove secretions. The lungs are auscultated regularly to identify abnormal sounds or any areas of diminished or absent breath sounds. To prevent pneumonia, encourage respiratory movement with incentive spirometers or other motivating activities (see Box 39.1). If these measures are presented as games, the child is more likely to comply. The child’s position is changed every 2 hours, and deep breathing is encouraged. Patients with preexisting pulmonary disease may be advised to begin incentive spirometry before the day of surgery (Azhar, 2015). Early respiratory movement can decrease the patient’s need for supplemental oxygen and promote discharge home sooner (Shaughnessy, White, Shah, et al., 2015).
During the recovery period, spend some time with the child to assess his or her perceptions of surgery. Play, drawing, and storytelling are excellent methods of discovering the child’s thoughts. With such information, the nurse can support or correct the child’s perceptions and boost his or her self-esteem for having endured a stressful procedure.
Many pediatric patients are discharged shortly after surgery. Preparation for discharge begins with the preadmission preparation visit. Thorough discharge processes and education can greatly assist in the prevention of unplanned readmissions (Payne & Flood, 2015). The nurse should discuss instructions for postoperative care and review them throughout the perioperative visit with the strategy that works best for the patient and family. After discharge, the nursing staff often makes phone calls to check the patient’s status. Patient education and compliance with discharge instructions can also be assessed during these phone calls (Flippo, NeSmith, Stark, et al., 2015) (see Evidence-Based Practice box).
Compliance
Compliance, also called adherence, refers to the extent to which the patient’s behavior coincides with the prescribed regimen in terms of taking medication, following diets, or executing other lifestyle changes. In developing strategies to improve compliance, the nurse must first assess level of compliance. Because many children are too young to assume partial or total responsibility for their care, parents are usually primarily responsible for home management.
Factors relating to the care setting are important in ensuring compliance and should be considered in planning strategies to improve compliance. Basically, any aspect of the health care setting that increases the family’s satisfaction with the physical setting and the relationship with the provider positively influences adherence to the treatment regimen. However, the more complex, expensive, inconvenient, and disruptive the treatment protocol, the less likely the family is to comply. During long-term conditions that involve multiple treatments and considerable rearrangement of lifestyle, compliance is severely affected.
Although it is helpful to know those factors that influence compliance, assessment must include more direct measurement techniques. When inquiring about a patient’s compliance, it can be helpful to ask details about how medication administration or other interventions are carried out instead of asking yes-or-no questions. For example, a health care provider could ask about what time of day patients perform their prescribed interventions, what beverages they prefer to take their medications with, or how many doses were missed this week. A number of methods exist, each with advantages and disadvantages. The most successful approach includes a combination of at least two of the following methods:
- Clinical judgment—This is subject to bias and inaccuracy unless the nurse carefully evaluates the criteria used in assessment.
- Self-reporting—Most people overestimate their compliance even when they admit to lapses.
- Direct observation—This is difficult to use outside the health care setting, and awareness of being observed frequently affects performance.
- Monitoring appointments—Keeping appointments indirectly indicates compliance with the prescribed care.
- Monitoring therapeutic response—Few treatments yield directly measurable results (e.g., decreased blood pressure, weight loss); record on a graph or chart.
- Pill counts—The nurse counts the number of pills remaining in the original container and compares the number missing with the number of times the medication should have been taken. Although this is a simple method, families may forget to bring the container or deliberately alter the number of pills to avoid detection. This method is also poorly suited to liquid medication. Another technique is the use of pill container caps that record every opening as a presumptive dose.
- Chemical assay—For certain drugs, such as digoxin, measurement of plasma drug levels provides information on the amount of drug recently ingested. However, this method is expensive, indicates only short-term compliance, and requires precise timing of the assay for accurate results.
Compliance strategies
Strategies to improve compliance involve interventions that encourage families to follow the prescribed treatment regimen. Some evidence suggests that higher levels of self-esteem and increased autonomy favorably affect adolescent compliance (Letitre, DeGroot, Draaisma, et al., 2014). In addition, anxiety, depression, and self-esteem can be negatively affected when treatment regimens are inadequately followed. However, family factors are important, and characteristics associated with good compliance include family support, family reminders, good communication, and expectations for successful completion of the therapeutic regimen. No one approach is always successful, and the best results occur when at least two strategies are used.
Organizational strategies involve the care setting and the therapeutic plan. This may involve increasing the frequency of appointments, designating a primary provider, reducing the cost of medication by prescribing generic brands, reducing the treatment’s disruption of the family’s lifestyle, and using “cues” to minimize forgetting. Numerous devices are available commercially or can be improvised for cueing, such as pill dispensers; watches with alarms; charts to record completed therapy; messages on the refrigerator or morning coffee pot; mobile phone applications; and individualistic, self-timed schedules that incorporate the treatment plan into the daily routine, such as physical therapy after the evening bath (Britto, Munafo, Schoettker, et al., 2012; Carbone, Zebrack, Plegue, et al., 2013).
The nurse instructs the family about the treatment plan. Although education is an important factor in enhancing compliance, and patients who are more knowledgeable about their condition are more likely to comply, education alone does not ensure compliant behavior. The nurse should incorporate teaching principles known to enhance understanding and retention of material. Written materials are essential, especially in any regimen requiring multiple or complex treatments, and they need to be understandable to the average individual, who reads at about the fourth-grade level. Learning disabilities can negatively affect medication adherence and should be routinely assessed along with health literacy (Dharmapuri, Best, Kind, et al., 2015). Individualized teaching strategies appropriate for developmental and cognitive levels of the individual, as well as involvement of the immediate and extended family (e.g., grandparents) in education sessions, may enhance compliance.
Treatment strategies relate to the child’s refusal or inability to take the prescribed medication. The family may also have difficulty following a prescribed treatment regimen. They may remember and understand the instructions but may not be able to give the medicine as prescribed. Assess the reason for refusal. For example, the child may not be able to swallow pills. In this case, perhaps pills could be crushed or a liquid medication substituted (always review medication to ensure that crushing is acceptable before giving this instruction).
Assess the treatment and medication schedule to determine whether it is reasonable for a home situation. Although an every-6-hour or every-8-hour schedule is reasonable for hospitals, a parent would have difficulty getting up once or twice nightly. Instead, the patient could take a medication during the day at times that would be easy to remember.
Behavioral strategies are designed to modify behavior directly. Nurses can use several effective strategies with children to encourage the desired behavior. Positive reinforcement is one strategy that strengthens the behavior. One example of this is the child earning stars or tokens, which can be exchanged for a special privilege or gift. Sticker charts also serve as a visual reminder of positive behavior and motivation to continue compliance. At times, however, disciplinary techniques, such as a time-out for young children or withholding privileges for older children, may be needed to improve compliance. The child life specialist can be especially helpful in determining behavioral compliance strategies across the developmental spectrum.
Skin care and general hygiene
Maintaining healthy skin
Maintaining an IV line, removing a dressing, positioning a child in bed, changing a diaper, using electrodes, and using restraints all have the potential to contribute to skin injury. General guidelines for skin care are listed in the Evidence-Based Practice box.
Assessment of the skin is easiest to accomplish during the bath. Examine for early signs of injury, including redness, flaking, decreased perfusion, or skin breakdown. Risk factors include impaired mobility, protein malnutrition, edema, incontinence, sensory loss, anemia, infection, failure to turn the patient, and intubation. Identification of risk factors helps determine children who need a more thorough skin assessment. Several risk assessment scales, such as the Braden Q Scale, the Neonatal Skin Risk Assessment Scale, the Waterlow Scale, and the Glamorgan Scale, are available for use in pediatrics (Razmus & Bergquist-Beringer, 2017). Initial assessment should occur on admission to identify pressure ulcers and wounds that occurred before admission. Skin assessment should be repeated every shift and at least every 4 hours in perfusion-compromised patients.
Pressure ulcers, a form of pressure injuries, are localized damage to the skin and/or underlying soft tissue due to decreased perfusion as a result of increased pressure. Pressure ulcers most often occur over bony prominences or related to medical or other devices. Pressure injuries are staged to classify the amount of tissue damage that has occurred.c Necrotic tissue must be removed so that the tissue depth can accurately be assessed. Accurate documentation of redness or obvious skin breakdown is essential. Color, size (diameter and depth), location, presence of sinus tracts, odor, exudate, and response to treatment are observed and recorded at least daily.
Pressure ulcers in children typically occur on the occiput, earlobes, sacrum, heels, and scapula (Schober-Flores, 2012); the heels and sacrum are common sites in adults. Critically ill children; children with sensory deficits, mobility deficits, or cardiopulmonary abnormalities; and bariatric patients are at a higher risk of pressure ulcers and skin breakdown because they often have several risk factors combined. Although pressure ulcers in hospitalized children are generally uncommon, the incidence in critically ill children can be significantly higher. Interventions found to prevent pressure ulcers in critically ill children include the following:
- • Assessing the patient’s skin from head to toe on admission and each shift
- • Turning children every 2 hours
- • Using pillows, blanket rolls, and positioning devices
- • Using draw sheets to minimize shear
- • Using pressure reduction surfaces (e.g., foam overlays, gel pads, specialty beds)
- • Allowing moisture reduction by using dry-weave diapers and disposable underpads
- • Using skin moisturizers
- • Conducting nutrition consults
Medical devices such as pulse oximeter probes, bilevel and continuous positive airway pressure masks, oxygen cannulas, tracheostomy tubes, orthotics, and casts can also cause pressure ulcers (Freundlich, 2017). In addition, both medical devices and special garments such as shoes, slippers, jewelry, hair ties, and restraints should be removed to inspect skin at least every shift.
Friction and shear contribute to pressure ulcers. Friction occurs when the surface of the skin rubs against another surface, such as bed sheets. The skin may have the appearance of an abrasion. The skin damage is usually limited to the epidermal and upper layers. It most often occurs over the elbows, heels, or occiput. Prevention of friction injury includes the use of foam mattresses that redistribute pressure; customized splinting or foam-padded boots over the heels; gel pillows; moisturizing agents; protective, transparent barrier dressings over susceptible areas; and soft, smooth bed linens and clothing (Freundlich, 2017). By itself, friction does not cause tissue necrosis, but when it acts with gravity, it results in shear injury.
Shear is the result of the force of gravity pushing down on the body and friction of the body against a surface, such as the bed or chair. For example, when a patient is in the semi-Fowler position and begins to slide to the foot of the bed, the skin over the sacral area remains in the same place because of the resistance of the bed surface. The blood vessels, bone, and muscle in the area are stretched and slide parallel to the stationary skin, which may cause small-vessel thrombosis and tissue death. Prevention of shear injury includes using lift sheets when repositioning a patient, elevating the bed no more than 30 degrees for short periods, and elevating the knees to interrupt the pull of gravity on the body toward the foot of the bed.
Epidermal stripping results when the epidermis is unintentionally removed when tape is pulled off the skin. These lesions are usually shallow and irregularly shaped. Babies are at increased risk for epidermal injury. Prevention includes using no tape when possible or securing dressings with laced binders (Montgomery straps) or stretchy netting (Spandage or stockinette). Using porous or low-tack tapes (e.g., Medipore, paper, hydrogel), using alcohol-free skin sealants (No Sting Barrier Film), or picture-framing wounds with hydrocolloid or wafer barriers (e.g., DuoDERM, Coloplast, Stomahesive) and then taping on top of the barrier also will reduce epidermal stripping.
Tape should be placed so that there is no tension, traction, or wrinkles on the skin. To remove tape, slowly peel the tape away while stabilizing the underlying skin. Adhesive remover may be used to break the adhesive bond but may be drying to the skin. Avoid adhesive removers in preterm neonates because absorption rates vary and toxicity may occur. Remove the adhesive with water to prevent absorption and irritation. Wetting the tape with water or alcohol-based foam hand cleansers may facilitate removal.
Chemical factors can also lead to skin damage. Fecal incontinence, especially when mixed with urine; wound drainage; or gastric drainage around gastrostomy tubes can erode the epidermis. The skin can quickly progress from redness to denudement if exposure continues. Moisture barriers, gentle cleansing with alcohol-free cleansers or wipes as soon after exposure as possible, and skin barriers can be used to prevent damage caused by chemical factors. For nonintact skin, a barrier cream with zinc oxide should be applied. It is important to cleanse only the stool and urine during diaper changes, not the paste. In addition, foam dressings that wick moisture away from the skin are helpful around gastrostomy tubes and tracheostomy sites.
Bathing
Most infants and children can be bathed at the bedside or in a standard bathtub or shower. Assess the child’s and family’s preferences for bath time frequency and family involvement. For infants and young children confined to bed, use commercially available bath cloths or the towel method. Immerse two towels in a dilute soap solution and wring them damp. With the child lying supine on a dry towel, place one damp towel on top of the child and use it to gently clean the body. Discard the towel, dry the child, and turn him or her prone. Repeat the procedure using the second damp towel. If bar soap is used, discard the basin and bar soap after a single bath because they can serve as a reservoir for pathogens in the hospital setting. Chlorhexidine is much less likely to harbor microbes, but it is generally not approved for use in infants younger than 2 months of corrected gestational age. Daily chlorhexidine gluconate bathing in the pediatric population can reduce bacteremia and prevent hospital-acquired infections (Karcz, Kelley, Conrad, et al., 2015; Raulji, Clay, Velasco, et al., 2015).
Infants and small children are never left unattended in a bathtub, and infants who are unable to sit alone are securely held with one hand during the bath. The nurse securely supports the infant’s head with one hand or grasps the infant’s farther arm while the head rests comfortably on the nurse’s arm. Children who are able to sit without assistance need only close supervision and a pad placed in the bottom of the tub to prevent slipping and loss of balance.
School-age children and adolescents may shower or bathe. Nurses need to use judgment regarding the amount of supervision the child requires. Some children can assume this responsibility unaided, but others need someone in constant attendance. Children with cognitive impairments, physical limitations such as severe anemia or leg deformities, or suicidal or psychotic problems (who may commit bodily harm) require close supervision.
Areas that require special attention are the ears, between skinfolds, the neck, the back, and the genital area. The genital area should be carefully cleansed and dried, with particular care given to skinfolds. In uncircumcised boys younger than 3 years of age, the foreskin is not fully retractile. For older males, the foreskin should be gently retracted, the exposed surfaces cleansed, and the foreskin then replaced. If the condition of the glans indicates inadequate cleaning, such as accumulated smegma, inflammation, phimosis (condition in which the foreskin cannot be retracted), or foreskin adhesions, teaching proper hygiene is indicated. Do not forcibly retract the foreskin to avoid trauma and further complications (Hunter, 2012). Notify the provider of abnormal clinical findings during genitourinary assessment. In the Vietnamese and Cambodian cultures, the foreskin is traditionally not retracted until adulthood. Older children have a tendency to avoid cleaning the genitalia; therefore they may need a gentle reminder.
Oral hygiene
Mouth care is an integral part of daily hygiene and should be continued in the hospital. Oral hygiene can prevent infection and promote comfort, adequate nutrition, and verbal communication. For some young children, this is their first introduction to the use of a toothbrush. Infants and debilitated children require the nurse or a family member to perform mouth care. For infants who do not yet have teeth, a soft moistened cloth or swab can be used to gently clean the gums. Children should begin brushing their teeth after the first teeth emerge around 6 months of age. For children younger than 3 years of age, a grain-sized amount of fluoride toothpaste should be used. For children 3 to 6 years of age, a pea-sized amount of fluoride toothpaste should be used (American Dental Association, 2017). Although young children can manage a toothbrush and are encouraged to use it, most need assistance to perform satisfactorily. Older children, although capable of brushing and flossing without assistance, sometimes need to be reminded.
Hair care
Children should have their hair brushed and combed at least once daily for hair and scalp health. The hair is styled for comfort and in a manner pleasing to the child and parents. The hair should not be cut without parental permission, although clipping hair to provide access to a scalp vein for IV insertion may be necessary.
If children are hospitalized for more than a few days, the hair may need shampooing. With infants, the hair may be washed during the daily bath or less frequently. For most children, washing the hair and scalp once or twice weekly is sufficient unless there is an indication for more frequent washing, such as after a high fever and profuse sweating. Adolescents normally have increased oily sebaceous secretions that require frequent hair care and more frequent shampoos.
Almost any child can be transported to an accessible sink for shampooing. Inspect the hair and scalp before shampooing using a fine toothcomb to assess for the presence of lice or other scalp abnormalities. Nits are a gray-white color, the size of a knot of thread, and difficult to remove from the scalp in comparison to dandruff. Adult lice are a red-black color and the size of a sesame seed and can live on the scalp for 3 to 4 weeks if untreated (Cummings, Finlay, & McDonald, 2018). If lice are suspected, an order for a pediculicide treatment and nit combing must be obtained. It is important for the nurse to don personal protective equipment, including a gown and cap, during the lice removal process. In addition, other members of the household should be evaluated for the presence of lice and the family educated on the importance of individual hair care products.
Patients who are unable to be transported can receive a shampoo in their beds with adequate protection, specially adapted equipment or positioning, or dry shampoo caps. Comb or brush the hair before washing. When necessary, a shampoo basin may be used or the child may be positioned near the edge of the bed, towels placed under the shoulders and neck, a large plastic garbage bag draped at the edge of the bed with one open end under the shoulders, and the hair placed inside the opening. The other end is opened and placed in a collection container. Water can be transported in a basin.
For children with curly hair, most standard combs are inadequate and may cause hair breakage and discomfort. Use a special comb with widely spaced teeth. It is also much easier to comb the hair after shampooing when it is wet. Use a special hair dressing or pomade, which usually has a coconut oil base. Rub the preparation on the hands and then transfer it to the hair to make it more pliable and manageable. Consult the child’s parents regarding the preparation to use on the child’s hair and ask if they can provide some for use during the child’s hospitalization. Petroleum jelly should not be used. If braiding or plaiting the hair, weave it loosely while the hair is damp. The hair tightens as it dries, which could result in tension folliculitis. Tight braids should be avoided, as braiding can increase pressure on the scalp or hide pressure injuries.
Feeding the sick child
Loss of appetite is a symptom common to most childhood illnesses. Decreased appetite can be a result of pain or discomfort, nausea and vomiting, emotional concerns, or loss of control. Because an acute illness is usually short, the nutritional state is seldom compromised. Urging food on the sick child may precipitate nausea and vomiting. In most cases, children can usually determine their own need for food.
Refusing to eat may also be one way children can exert power and control in an otherwise helpless situation. For young children, loss of appetite may be related to depression caused by separation from their parents. Parents’ concern with eating can intensify the problem. Forcing a child to eat meets with rebellion and reinforces the behavior as a control mechanism. Encourage parents to relax any pressure during an acute illness. Although it is best to provide high-quality, nutritious foods, the child may desire foods and liquids that contain mostly empty or nonnutritional calories. Some well-tolerated foods include gelatin, diluted clear soups, carbonated drinks, flavored ice pops, dry toast, and crackers. Even though these substances are not nutritious, they can provide necessary fluid and calories.
Dehydration is always a hazard when children have a fever or anorexia, especially when accompanied by vomiting or diarrhea. Fluids should not be forced, and the child should not be awakened to take fluids. Forcing fluids may create the same difficulties as urging the child to eat unwanted food. Gentle persuasion with preferred beverages will usually meet with success. Using play techniques can also be effective (see Evidence-Based Practice box).
An understanding of children’s feeding habits can also increase food consumption. For example, if children are given all their food at one time, they generally eat the dessert first. Likewise, if they are presented with large portions, they often push the food away because the amount overwhelms them. If young children are not supervised during mealtime, they tend to play with the food rather than eat it. Therefore nurses should present food in the usual order, such as soup first followed by small portions of meat, potatoes, and vegetables, and ending with dessert.
When the child is feeling better, appetite usually begins to improve. It is best to take advantage of any hungry period by serving high-quality foods and snacks. If the child still refuses to eat, offer nutritious fluids, such as prepared breakfast drinks. Parents can help by bringing in food items from home, especially if the family’s cultural eating habits differ from the hospital food. A clinical dietitian may be consulted for alternative food choices.
When children are placed on special diets, such as clear liquids after surgery or during episodes of diarrhea, assessment of their intake and readiness to advance to more complex foods is essential.
Regardless of the type of diet, charting the amount consumed is an important nursing responsibility. Descriptions need to be detailed and accurate, such as “4 ounces of orange juice, one pancake, and 8 ounces of milk.” Comments such as “ate well” or “ate poorly” are inadequate. Charting the percentage of the meal eaten is also inadequate unless food is measured before serving. For infants, assess the duration, amount, and frequency of breastfeeding or bottle-feeding and the possible addition of solid foods to determine whether nutrition is adequate.
If the parents are involved in the child’s care, encourage them to keep a list of everything the child eats. Using a premeasured cup for fluids ensures a more accurate estimate of intake. A comparison of the intake at each meal can isolate food deficiencies, such as insufficient intake of meat or vegetables. Behaviors associated with mealtime also identify possible factors influencing appetite. For example, the observation “Child eats well when with other children but plays with food if left alone in room” helps the nurse plan mealtime activities that stimulate the child’s appetite.
Although sick children’s appetites may be poor and not characteristic of their home eating habits, the hospital stay provides numerous opportunities for nurses to assess the family’s knowledge of good nutrition and to implement teaching as needed to improve nutritional intake.
Controlling elevated temperatures
An elevated temperature, most frequently from fever but occasionally caused by hyperthermia, is one of the most common symptoms of illness in children. This manifestation is a great concern to parents. To facilitate an understanding of fever versus hyperthermia, the following terms are defined:
- Set point—The temperature around which body temperature is regulated by a thermostat-like mechanism in the hypothalamus
- Fever (hyperpyrexia)—An elevation in set point such that body temperature is regulated at a higher level; may be arbitrarily defined as rectal temperature above 38°C (100.4°F)
- Hyperthermia—Body temperature exceeding the set point, which usually results from the body or external conditions creating more heat than the body can eliminate, such as in heat exhaustion, heatstroke, aspirin toxicity, seizures, or hyperthyroidism
Body temperature is regulated by a thermostat-like mechanism in the hypothalamus. This mechanism receives input from centrally and peripherally located receptors. When temperature changes occur, these receptors relay the information to the thermostat, which either increases or decreases heat production to maintain a constant set point temperature. However, during an infection, pyrogenic substances cause an increase in the body’s normal set point, a process that is mediated by prostaglandins. Consequently, the hypothalamus increases heat production until the core temperature reaches the new set point.
During the fever (febrile) state, shivering and vasoconstriction generate and conserve heat during the chill phase of fever, raising central temperatures to the level of the new set point. The temperature reaches a plateau when it stabilizes in the higher range. When the temperature is greater than the set point or when the pyrogen is no longer present, a crisis, or defervescence, of the temperature occurs.
Most fevers in children are of brief duration with limited consequences and are viral in origin (Patricia, 2014). Children may experience warm, flushed skin, chills, aches, malaise, or irritability during a fever. However, children who appear very ill, immunocompromised children, and neonates are at high risk for serious bacterial illness, such as urinary tract infections or bacteremia, and will likely receive a sepsis workup, antibiotics, and hospitalization.
Fever has physiologic benefits, including increased white blood cell activity, interferon production and effectiveness, and antibody production and enhancement of some antibiotic effects such as penicillin (Patricia, 2014). Contrary to popular belief, neither the rise in temperature nor its response to antipyretics indicates the severity or etiology of the infection, which casts doubt on the value of using fever as a diagnostic or prognostic indicator.
Therapeutic management
Treatment of elevated temperature depends on whether it is attributable to a fever or hyperthermia. Because the set point is normal in hyperthermia but increased in fever, different approaches must be used to lower body temperature successfully.
Fever
The principal reason for treating fever is the relief of discomfort. However, children with cardiopulmonary disease or immunocompromised children may not tolerate the increase in metabolic demand from a fever and should receive antipyretic therapy. Relief measures include pharmacologic and environmental intervention. The most effective intervention is the use of antipyretics to lower the set point.
Antipyretics include acetaminophen, aspirin, and nonsteroidal antiinflammatory drugs (NSAIDs). Acetaminophen is the preferred drug. Aspirin should not be given to children because of its association in children with influenza virus or chickenpox and Reye syndrome. One nonprescription NSAID, ibuprofen, is approved for fever reduction in children as young as 6 months of age.
Another antipyretic, acetaminophen, can be given every 4 hours but no more than five times in 24 hours due to the risk of hepatotoxicity. Because body temperature normally decreases at night, three or four doses in 24 hours will control most fevers. The temperature is usually retaken 30 to 60 minutes after the antipyretic is given to assess its effect but should not be measured repeatedly. The child’s level of discomfort is the best indication for continued treatment.
The nurse can use environmental measures to reduce fever if they are tolerated by the child and if they do not induce shivering. Shivering is the body’s way of maintaining the elevated set point by producing heat. Compensatory shivering greatly increases metabolic requirements above those already caused by the fever.
Traditional cooling measures, such as wearing minimum clothing; exposing the skin to air; reducing room temperature; increasing air circulation; and applying cool, moist compresses to the skin (e.g., the forehead), are effective if used approximately 1 hour after an antipyretic is given so that the set point is lowered. Cooling procedures such as sponging or tepid baths are ineffective in treating febrile children (these measures are effective for hyperthermia) either when used alone or in combination with antipyretics, and they cause considerable discomfort (Monsma, Richerson, & Sloand, 2015).
Seizures associated with a fever occur in 2% to 5% of all children, usually in those between 6 months and 5 years of age. About 30% to 50% of children have subsequent febrile seizures; a younger age at onset and a family history of febrile seizures are associated with increased incidence of recurring episodes. Evidence does not support the use of antipyretic drugs or anticonvulsants to prevent a second febrile seizure. Nursing interventions should focus on ways to provide care and comfort during a febrile illness. Simple febrile seizures lasting less than 10 minutes do not cause brain damage or other debilitating effects (Patricia, 2014).
Hyperthermia
Unlike in fever, antipyretics are of no value in hyperthermia because the set point is already normal. Consequently, cooling measures are used. If a child is severely hyperthermic with a core temperature above 40°C, it may be necessary to perform continuous monitoring of vital signs, including core temperature and urinary output, and administer IV fluids in a critical care environment (Chan & Mamat, 2015). Cool applications to the skin help reduce the core temperature. Cooled blood from the skin surface is conducted to inner organs and tissues, and warm blood is circulated to the surface, where it is cooled and recirculated. The surface blood vessels dilate as the body attempts to dissipate heat to the environment and facilitate this cooling process.
Commercial cooling devices, such as cooling blankets or mattresses, are available to reduce body temperature. Place the patient on the bed and cover with a sheet or lightweight blanket. Frequent temperature monitoring is essential to prevent excessive cooling of the body.
Traditionally, cool compresses decrease high temperature. For tepid tub baths, it is usually best to start with warm water and gradually add cool water until the desired water temperature of 37°C (98.6°F) is reached to acclimate the child to the lower water temperature. Generally, the temperature of the water has to be only 1°C (2°F) less than the child’s temperature to be effective. The child is placed directly in the tub of tepid water for 15 to 20 minutes while water is gently squeezed from a washcloth over the back and chest or gently sprayed over the body from a sprayer. In the bed or crib, cool washcloths or towels are used, exposing only one area of the body at a time. Continue sponging for approximately 20 minutes.
After the tub or sponge bath, the child is dried; dressed in lightweight pajamas, a nightgown, or a diaper; and placed in a dry bed. The child is dried by gently rubbing the skin surface with a towel to stimulate circulation. The temperature is retaken 30 minutes after the tub or sponge bath. The tub or sponge bath should not be continued or restarted until the skin surface is warm or if the child feels chilled. Chilling causes vasoconstriction, which defeats the purpose of the cool applications. In this condition, little blood is carried to the skin surface; the blood remains primarily in the viscera to become heated.
Whether a temperature elevation in the critically ill child is caused by fever or hyperthermia, it should be treated aggressively. The metabolic rate increases 10% for every 1°C increase in temperature and three to five times during shivering, thus increasing oxygen, fluid, and caloric requirements. If the child’s cardiovascular or neurologic system is already compromised, these increased needs are especially hazardous. In all children with an elevated temperature, attention to adequate hydration is essential. Most children’s needs can be met through additional oral fluids.
Family teaching and home care
Fever is one of the most common problems for which parents seek health care. High levels of parental anxiety (fever phobia) surrounding potential complications of fever such as seizures and dehydration are prevalent and can result in overusing antipyretics. Parents need to know that sponging is indicated for elevated temperatures from hyperthermia rather than fever and that ice water and alcohol are inappropriate, potentially dangerous solutions (Monsma et al., 2015). Parents should know how to take the child’s temperature, how to read the thermometer accurately, and when to seek professional care (see Family-Centered Care box). A dedicated thermometer should be used for the rectal route. Oral temperatures should not be taken within 15 minutes of the child eating or drinking hot or cold food. Some of the newer temperature-measuring devices, such as plastic strip or digital thermometers, may be better suited for home use. (See Chapter 29, Temperature.) If the use of acetaminophen or ibuprofen is indicated, the parents need instructions in administering the drug. Emphasize accuracy in both the amount of drug given and the time intervals at which the drug is administered. Along with reduced activity, encourage small, frequent sips of clear liquids. Dress the child in light clothing; use a light blanket for children who are cold or shivering (Monsma et al., 2015).
Safety
Safety is an essential component of any patient’s care, but children have special characteristics that require an even greater concern for safety. Because small children in the hospital are separated from their usual environment and do not possess the capacity for abstract thinking and reasoning, it is the responsibility of everyone who comes in contact with them to maintain protective measures throughout their hospital stay. Nurses need to understand the age level at which each child is operating and plan for safety accordingly.
Identification bands and the use of two patient identifiers are particularly important for children. Infants and unconscious patients are unable to tell or respond to their names. Toddlers may answer to any name or to a nickname only. Older children may exchange places, give an erroneous name, or choose not to respond to their own names as a joke, unaware of the hazards of such practices. In addition, allergy bands for medications and food should be worn by all patients, as should bands for other precautions such as fall risks or antineoplastic precautions.
Environmental factors
All of the environmental safety measures for the protection of adults apply to children, including good illumination, floors that are clear of fluid and objects that might contribute to falls, and nonskid surfaces in showers and tubs. All staff members should be familiar with the area-specific fire plan. Elevators and stairways should be made safe.
All windows should be secured. Window blind and curtain cords should be out of reach, with split cords to prevent strangulation. Pacifiers should not be tied around the neck or attached to an infant by a string.
Electrical equipment should be in good working order and used only by personnel familiar with its use. It should not be in contact with moisture or situated near tubs. Electrical outlets should have covers to prevent burns in small children, whose exploratory activities may extend to inserting objects into the small openings.
Staff members should practice proper care and disposal of small objects such as syringe caps, needle covers, and temperature probes. Staff also must carefully check bathwater before placing the child in it and never leave children alone in a bathtub. Infants are helpless in water, and small children (and some older ones) may turn on the hot water faucet and be severely burned.
Furniture is safest when it is scaled to the child’s proportions, is sturdy, and is well balanced to prevent its being easily tipped over. A special hazard for children is the danger of entrapment under an electronically controlled bed when it is activated to descend. Infants and small children must be securely strapped into infant seats, feeding chairs, and strollers. Baby walkers should not be used because they provide access to hazards, resulting in burns, falls, and poisonings. Infants; young children; and children who are weak, paralyzed, agitated, confused, sedated, or cognitively impaired should never be left unattended on treatment tables, on scales, or in treatment areas. Even premature infants are capable of surprising mobility; therefore portholes in incubators must be securely fastened when not in use. For patients at risk of suicide, it is necessary to remove all items such as sharp objects, cords, and plastic bags that can be used to impose self-harm. Depending on patient diagnosis, a one-to-one sitter should also be considered. In addition, visitors, personal items, and Internet access may be restricted to protect the patient.
Crib sides should always be raised and fastened securely. Use cribs that meet federal safety standards (https://www.cpsc.gov/safety-education/safety-education-centers/cribs). Anyone attending to an infant or small child on a stretcher or table should never turn away without maintaining hand contact with the child—that is, keeping one hand on the child’s back or abdomen to prevent rolling, crawling, or jumping from the open crib (Fig. 39.2). A child who is likely to climb over the sides of the crib is safest when placed in a specially constructed crib with a cover over the top. Never tie nets to the movable crib sides or use knots that do not permit quick release.

An infant is lying on the bed. A nurse standing near the bed is touching the infant with one hand, and her other hand is taking the glass from the table behind her.
The safest sleeping position to prevent sudden infant death syndrome is wholly supine until at least 1 year of age (American Academy of Pediatrics, Task Force on Sudden Infant Death Syndrome, 2016). No pillows should be placed in a young infant’s crib while the infant is sleeping. A firm sleep surface with no other bedding or any soft items in the crib in a shared room (not a shared bed) and the avoidance of overheating or exposure to tobacco smoke, alcohol, and illicit drugs further increase the safety of an infant’s sleeping environment. The use of car seats, strollers, swings, or other sitting devices should not be used for routine sleep. In addition, swaddling is not recommended for infants over 2 months of age due to the risk of death if the infant rolls into the prone position. In accordance with the American Academy of Pediatrics guidelines to avoid extra bedding in the crib, many institutions recommend an infant sleep sack for adequate warmth and safety.
Toys
Toys play a vital role in the everyday lives of children, and they are no less important in the hospital setting. Nurses are responsible for assessing the safety of toys brought to the hospital by well-meaning parents and friends. Toys should be appropriate to the child’s age, condition, and treatment. For example, if the child is receiving oxygen, electrical or friction toys or equipment are not safe because sparks can cause oxygen to ignite. Inspect toys to ensure that they are nonallergenic, washable, and unbreakable and that they have no small, removable parts that can be aspirated or swallowed or can otherwise inflict injury on a child. All objects within reach of children younger than 3 years of age should pass the choke tube test. A toilet paper roll is a handy guide. If a toy or object fits into the cylinder (items less than 1¼ inches across or balls less than 1¾ inches in diameter), it is a potential choking danger to the child. Latex balloons pose a serious threat to children of all ages. If the balloon breaks, a child may put a piece of the latex in his or her mouth. If it is aspirated or swallowed, the latex piece is difficult to remove, resulting in choking. Latex balloons should never be permitted in the hospital setting.
Preventing falls
Although children have a known predisposition to falls based on normal growth and development, falls risk identification and prevention for children with medical conditions is especially important due to greater risk for injury from a fall (Murray, Edlund, & Vess, 2016). Falls prevention begins with identification of children most at risk for falls. Pediatric hospitals use various methods to identify a child’s risk of falls. After a risk assessment is performed, multiple interventions are needed to minimize pediatric patients’ risk of falling, including education of patient, family, and staff.
To identify children at risk of falling, perform a falls risk assessment on patients on admission and throughout hospitalization. Risk factors for hospitalized children include the following:
- • Medication effects—Postanesthesia or sedation; analgesics or narcotics, especially in those who have never had narcotics in the past and in whom effects are unknown
- • Altered mental status—Secondary to seizures, brain tumors, or medications
- • Altered or limited mobility—Reduced skill at ambulation secondary to developmental age, disease process, tubes, drains, casts, splints, or other appliances; new to ambulation with assistive devices such as walkers or crutches
- • Postoperative children—Risk of hypotension or syncope secondary to large blood loss, a heart condition, or extended bed rest
- • History of falls
- • Infants or toddlers in cribs with side rails down or on the daybed with family members
- • Changes to the patient’s environment
Once children at risk of falls have been identified, alert other staff members by posting signs on the door and at the bedside, applying a special-colored armband labeled “Fall Precautions,” labeling the chart with a sticker, or documenting information on the chart.
Prevention of falls requires alterations in the environment, including the following:
- • Keep the bed in the lowest position with the brakes locked and the side rails up.
- • Place the call bell within reach and orient the patient and caregivers to the bed and room.
- • Ensure that all necessary and desired items are within reach (e.g., water, glasses, tissues, snacks).
- • Offer toileting on a regular basis, especially if the patient is taking diuretics or laxatives.
- • Keep lights on at all times, including dim lights while sleeping.
- • Lock wheelchairs before transferring patients.
- • Ensure that the patient has an appropriate-size gown and nonskid footwear. Do not allow gowns or ties to drag on the floor during ambulation.
- • Keep the floor clean and free of clutter. Post a “wet floor” sign if the floor is wet.
- • Ensure that the patient has glasses on if he or she normally wears them.
- • Use a gait belt during ambulation.
- • Keep the patient’s door open unless isolation status prohibits.
Preventing falls also relies on age-appropriate education of patients. Assist the child with ambulation even though he or she may have ambulated well before hospitalization. Patients who have been lying in bed need to get up slowly, sitting on the side of the bed before standing.
The nurse also needs to educate family members:
- • Call the nursing staff for assistance and do not allow patients to get up independently.
- • Keep the side rails of the crib or bed up whenever patient is in the crib or bed.
- • Do not leave infants on the daybed; put them in the crib with the side rails up.
- • When all family members need to leave the bedside, notify the staff and ensure that the patient is in the bed or crib with the side rails up and call bell within reach (if appropriate).
In the event of a fall, it is important to immediately respond to the needs of the patient; notify appropriate personnel, including caregivers; and document the event.
Infection control
According to the Centers for Disease Control and Prevention, nosocomial (health care-associated) infections pose a significant threat to patient safety. These infections occur when there is interaction among patients, health care personnel, equipment, and bacteria. Health care-associated infections include infections such as Clostridium difficile or hospital-onset methicillin-resistant Staphylococcus aureus, as well as central line-associated bloodstream infections (CLABSIs), catheter-associated urinary tract infections (CAUTIs), and some surgical site infections. Health care-associated infections can be preventable if caregivers practice meticulous cleaning and disposal techniques.
Standard Precautions synthesize the major features of Universal (blood and body fluid) Precautions (designed to reduce the risk of transmission of bloodborne pathogens) and body substance isolation (designed to reduce the risk of transmission of pathogens from moist body substances). Standard Precautions involve vigilant hand hygiene and the use of barrier protection, such as gloves, goggles, gown, or mask, to prevent contamination from (1) blood; (2) all body fluids, secretions, and excretions except sweat, regardless of whether they contain visible blood; (3) nonintact skin; and (4) mucous membranes. Standard Precautions are designed for the care of all patients to reduce the risk of transmission of microorganisms from both recognized and unrecognized sources of infection.
Transmission-Based Precautions are designed for patients with documented or suspected infection or colonization (i.e., presence of microorganisms in or on the patient but without clinical signs and symptoms of infection) with highly transmissible or epidemiologically important pathogens for which additional precautions beyond Standard Precautions are needed to interrupt transmission in hospitals. There are three types of Transmission-Based Precautions: Airborne Precautions, Droplet Precautions, and Contact Precautions. They may be combined for diseases that have multiple routes of transmission (Box 39.2). They are to be used in addition to Standard Precautions.
Airborne Precautions reduce the risk of airborne transmission of infectious agents. Airborne transmission occurs by dissemination of either airborne droplet nuclei (small-particle residue [<5 mm] of evaporated droplets that may remain suspended in the air for long periods) or dust particles containing the infectious agent. Microorganisms carried in this manner can be dispersed widely by air currents and may become inhaled by or deposited on a susceptible host within the same room or over a longer distance from the source patient, depending on environmental factors. Individuals who have not had direct face-to-face contact with the source individual may become infected. Special air handling and ventilation are required to prevent airborne transmission. Airborne Precautions apply to patients with known or suspected infection with pathogens transmitted by the airborne route such as measles, varicella, and tuberculosis.
Droplet Precautions reduce the risk of droplet transmission of infectious agents. Droplet transmission involves contact of the conjunctivae or the mucous membranes of the nose or mouth of a susceptible person with large-particle droplets (>5 mm) containing microorganisms generated from a person who has a clinical disease or who is a carrier of the microorganism. Droplets are generated from the source person primarily during coughing, sneezing, or talking and during procedures such as suctioning and bronchoscopy. Transmission requires close contact between source and recipient persons because droplets do not remain suspended in the air and generally travel only short distances, usually 3 feet or less but up to 10 feet, through the air. Because droplets do not remain suspended in the air, special air handling and ventilation are not required to prevent droplet transmission. Droplet Precautions apply to any patient with known or suspected infection with pathogens that can be transmitted by infectious droplets (see Box 39.2).
Contact Precautions reduce the risk of transmission of microorganisms by direct or indirect contact. Direct-contact transmission involves skin-to-skin contact and physical transfer of microorganisms to a susceptible host from an infected or colonized person, such as occurs when turning or bathing patients. Direct-contact transmission also can occur between two patients (e.g., by hand contact). Indirect contact transmission involves contact of a susceptible host with a contaminated intermediate object, usually inanimate, in the patient’s environment. Contact Precautions apply to specified patients known or suspected to be infected or colonized with microorganisms that can be transmitted by direct or indirect contact.
Nurses caring for young children are frequently in contact with body substances, especially urine, feces, and vomitus. Nurses need to exercise judgment concerning those situations when gloves, gowns, or masks are necessary. For example, wear gloves and possibly gowns for changing diapers when there are loose or explosive stools. Otherwise, the plastic lining of disposable diapers provides a sufficient barrier between the hands and body substances. During feedings or oral medication administration, wear gowns if the child is likely to vomit or spit up, which often occurs during burping. When wearing gloves, wash the hands thoroughly after removing the gloves because gloves fail to provide complete protection. The absence of visible leaks does not indicate that gloves are intact.
Another essential practice of infection control is that all needles (uncapped and unbroken) are disposed of in a rigid, puncture-resistant container located near the site of use. Consequently, these containers are installed in patients’ rooms. Because children are naturally curious, extra attention is needed in selecting a suitable type of container and a location that prevents access to the discarded needles. Puncture-resistant containers should be changed when three-quarters full or when the fill line marker on the container is reached (US Food and Drug Administration, 2018). The use of needleless systems allows secure syringe or IV tubing attachment to vascular access devices without the risk of needlestick injury to the child or nurse.
Transporting infants and children
Infants and children need to be transported within the unit and to areas outside the pediatric unit. Infants and small children can be carried for short distances within the unit, but for more extended trips, the child should be securely transported in a suitable conveyance.
Small infants can be held or carried in the horizontal position with the back supported and the thigh grasped firmly by the carrying arm (Fig. 39.3A). In the football hold, the infant is carried on the nurse’s arm with the head supported by the hand and the body held securely between the nurse’s body and elbow (see Fig. 39.3B). Both of these holds leave the nurse’s other arm free for activity. The infant also can be held in the upright position with the buttocks on the nurse’s forearm and the front of the body resting against the nurse’s chest. The infant’s head and shoulders are supported by the nurse’s other arm in case the infant moves suddenly (see Fig. 39.3C). Older infants are able to hold their heads erect but are still subject to sudden movements. Medically stable infants can be carried in a variety of ways for transport as long as their head is supported at all times.

A three-part image labelled A through C, depicts three different ways of transporting the infants. A: A nurse holding an infant in his arms. B: The nurse is holding the infant in his right arm facing in a supine position near the right nipple representing a football position. C: The nurse holding the infant close to his chest with one hand supporting the back of the infant.
The method of transporting children depends on their age, condition, and destination. Older children are safe in wheelchairs or on stretchers. Younger children can be transported in a crib, on a stretcher, in a wagon with raised sides, or in a wheelchair with a safety belt. Stretchers should be equipped with high sides and a safety belt, both of which are secured during transport.
Special care is needed in transporting critically ill patients in the hospital. Critically ill children should always be transported on a stretcher or bed (rather than carried) by at least two appropriately trained staff members with monitoring continued during transport. A blood pressure monitor (or standard blood pressure cuff), pulse oximeter, and cardiac monitor/defibrillator should accompany every patient (Alamanou & Brokalaki, 2014). Airway equipment, oxygen, and emergency medications should accompany the patient. The monitoring and staff members required for transport will vary depending on the acuity and clinical status of the patient. In addition, it is important for the nurse to be familiar with emergency transport of patients in the event of severe weather, fire, or security threats when power or elevators may be unavailable.
Restraining methods
The Centers for Medicare and Medicaid Services (2015) has established regulations to minimize the use of and ensure the safety of patients in restraints. It defines restraint as “any manual method, physical or mechanical device, material, or equipment that immobilizes or reduces the ability of a patient to move his or her arms, legs, body, or head freely... or a drug or medication when it is used as a restriction to manage the patient’s behavior or restrict the patient’s freedom of movement and is not a standard treatment or dosage for the patient’s condition.” A restraint should be applied only by a health care team member with demonstrated competency in restraint management. The physical force may be human, mechanical devices, or a combination of the two. Examples of restraints include limb restraints, elbow restraints, vest restraints, and tight tucking of sheets to prevent movement in bed.
Mechanical supports such as immobilizers for fractures, orthopedic devices to maintain proper body alignment, leg braces, protective helmets, and surgical dressings are not considered restraints. An armboard to secure a peripheral IV line is not considered a restraint unless it is tied to the bed or immobilizes the entire limb such that the patient cannot access his or her body. Hand mitts are not considered a restraint unless tied to the bed or used in conjunction with a wrist restraint. Developmentally age-appropriate safety interventions for infants, toddlers, and preschoolers, such as net enclosures on beds, crib domes, crib side rails, and high chair lap safety belts, are generally not considered restraints. Picking up, redirecting, or holding an infant, toddler, or preschooler is not considered restraint. Interventions that typically would be used by a child care provider outside a health care environment to ensure safety in young children are not considered restraints.
Before initiating restraints, the nurse completes a comprehensive assessment of the patient to determine whether the need for a restraint outweighs the risk of not using one. Restraints can result in loss of dignity, violation of patient rights, psychologic harm, physical harm, and even death. Consider alternative methods first and document them in the patient’s record. Some examples of alternative measures include bringing a child to the nurses’ station for continuous observation, providing diversional activities such as music, and encouraging the participation of the parents. The use of restraints can often be avoided with adequate preparation of the child; parental or staff supervision of the child; or adequate protection of a vulnerable site, such as an infusion device.
The nurse needs to assess the child’s development, mental status, potential to hurt others or self, and safety. The nurse is responsible for selecting the least restrictive type of restraint. Using less restrictive restraints is often possible by gaining the cooperation of the child and parents. An order must be obtained as soon as possible (during application or within a few minutes) after the initiation of restraints and specify the time frame in which they can be used, the reason they are being used, and reasons for discontinuation. Discontinuation of restraints should occur as soon as it is safe, even if the order time frame has not expired.
Restraints for violent, self-destructive behavior are limited to situations with a significant risk of patients physically harming themselves or others because of behavioral reasons and when nonphysical interventions are not effective. Before initiating a behavioral restraint, the nurse should assess the patient’s mental, behavioral, and physical status to determine the cause for the child’s potentially harmful behavior. If behavioral restraints are indicated, a collaborative approach involving the patient (if appropriate), the family, and the health care team should be used. Behavioral restraints can include personal restraints, such as a physical hold, or mechanical restraints, such as secured anklets and wristlets or bilateral arm immobilizers.
Unless state law is more restrictive, behavioral restraints for children must be reordered every 15 minutes for a personal restraint, every 1 hour for children under 9 years of age, and every 2 hours for children 9 to 17 years old; orders for adults 18 years and older are required every 4 hours. A licensed independent practitioner or specially trained nurse must conduct an in-person evaluation within 1 hour and at least every 24 hours to continue restraints.
Children in behavioral restraints must be observed and assessed according to facility policy—typically continuously, every 15 minutes, or every 2 hours. Assessment components include signs of injury associated with applying restraint, nutrition and hydration, circulation and range-of-motion of extremities, vital signs, hygiene and elimination, physical and psychologic status and comfort, and readiness for discontinuation of restraint. The nurse must use clinical judgment in setting a schedule within the facility’s policy for when each of these parameters needs to be evaluated.
Nonviolent and non-self-destructive patients may also require restraints to support medical healing. Examples of situations where a nonbehavioral restraint may be necessary for the patient’s safety include removal of an artificial airway or airway adjunct for delivery of oxygen, indwelling catheters, tubes, drains, lines, pacemaker wires, or disruption of suture sites. The medical-surgical restraint is used to ensure that safe care is given to the patient. Patient confusion, agitation, unconsciousness, and developmental inability to understand direct requests or instructions may warrant the use of nonbehavioral restraints to maintain patient safety. The potential risks of the restraint are offset by the potential benefit of providing safer care.
Nonbehavioral restraints can be initiated by an individual order or by protocol; the use of the protocol must be authorized by an individual order. The order for continued use of restraints must be renewed each day. Patients are monitored per facility policy, typically at least every 2 hours.
Restraints with ties must be secured to the stationary bed or crib frame, not the side rails. Suggestions for increasing safety and comfort while the child is in a restraint include leaving one fingerbreadth between skin and the device and tying knots that allow for quick release. The nurse can also increase safety by ensuring that the restraint does not tighten as the child moves and by decreasing wrinkles or bulges in the restraint. Placing jacket restraints over an article of clothing; placing limb restraints below waist level, below knee level, or distal to the IV; and tucking in dangling straps also increase safety and comfort. Do not place objects over a patient’s face to protect staff from being spit on or bitten. Masks and face shields should be readily available for staff to wear; some facilities also provide bite gloves and arm and hand wraps made of strong barrier materials such as Kevlar for staff to wear to prevent injury from bites and scratches.
Mummy restraint or swaddle
When an infant or small child requires short-term restraint for examination or treatment that involves the head and neck (e.g., venipuncture, throat examination, gavage feeding), a papoose board with straps or a mummy wrap effectively controls the child’s movements. When used only for the duration of the test or procedure, this is not considered a restraint. The mummy restraint or swaddle should not be used for behavior or long-term restraint. A blanket or sheet is opened on the bed or crib with one corner folded to the center. The infant is placed on the blanket with the shoulders at the fold and feet toward the opposite corner. With the infant’s right arm straight down against the body, the right side of the blanket is pulled firmly across the infant’s right shoulder and chest and secured beneath the left side of the body. The left arm is placed straight against the infant’s side, and the left side of the blanket is brought across the shoulder and chest and locked beneath the body on the right side. The lower corner is folded and brought over the body and tucked or fastened securely with safety pins. Safety pins can be used to fasten the blanket in place at any step in the process. To modify the mummy restraint for chest examination, bring the folded edge of the blanket over each arm and under the back and then fold the loose edge over and secure it at a point below the chest to allow visualization and access to the chest (Fig. 39.4A).
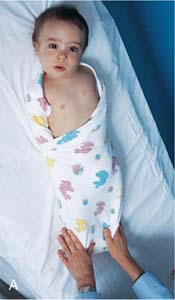
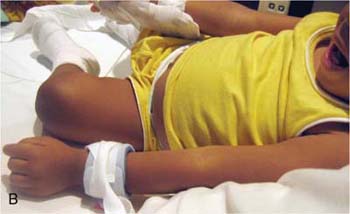

A three-part image labelled, A through C, depicts three examples of restraints from most restrictive to least restrictive. A: An infant covered with a towel is lying on a bed. Two human hands are shown touching the infant's legs. B: A smiling infant lying on a bed, wearing restrictive bands around both of her wrists. C: A child wearing an armband on both hands, is sitting on a bed.
Arm and leg restraints
Occasionally, the nurse needs to restrain one or more extremities or limit their motion. Several commercial restraining devices are available, including disposable wrist and ankle restraints (see Fig. 39.4B). Restraints must be appropriate to the child’s size and padded to prevent undue pressure, constriction, or tissue injury, and the extremity must be observed frequently for signs of irritation or impaired circulation. The ends of the restraints are never tied to the side rails because lowering the rail will disturb the extremity, frequently with a jerk that may hurt or injure the child.
Elbow restraint
Sometimes it is important to prevent the child from reaching the head or face (e.g., after cleft lip or palate surgery, when a scalp vein infusion is in place, or to prevent scratching in skin disorders). Bilateral elbow restraints fashioned from a variety of materials function well (see Fig. 39.4C). Commercial elbow restraints or immobilizers are available. They extend from just below the axilla to the wrist and are sometimes referred to as “no-no’s.” A shoulder strap to prevent slipping may be used in an awake, active older infant or toddler to prevent slippage but should not be used when sleeping.
Positioning for procedures
Infants and small children are unable to cooperate for many procedures. Therefore the nurse is responsible for minimizing their movement and discomfort with proper positioning. It can also be helpful to involve the caregivers or child life specialists during procedures to minimize distress in the child. Older children usually need only minimal, if any, positioning hold or movement restrictions. Careful explanation and preparation beforehand and support and simple guidance during the procedure are usually sufficient. For painful procedures, the child should receive adequate analgesia and sedation to minimize pain and the need for excessive restraint. For local anesthesia, use buffered lidocaine to reduce the stinging sensation or a topical anesthetic. (See Chapter 30, Pain Management.)
Femoral venipuncture
The nurse places the child supine with the legs in a frog position to provide extensive exposure of the groin area. A towel can also be placed under the hips. The infant’s legs can be effectively controlled by the nurse’s forearms and hands (Fig. 39.5). Only the side used for the venipuncture is uncovered, so the practitioner is protected if the child urinates during the procedure. Apply pressure to the site to prevent oozing from the site.

Close-up of two human hands holding the thighs of an infant lying supine on a bed with legs in a frog position. The left hand is being used to hold the left leg of the infant, while the thumb of the right hand is being pressed hard on the femoral vein of the infant, as the other fingers hold the right thigh of the infant.
Extremity venipuncture or injection
The most common sites of venipuncture are the veins of the extremities, especially the arm and hand. A convenient position is to place the child in the parent’s (or assistant’s) lap with the child facing the parent and in the straddle position. Next, place the child’s arm for venipuncture on a firm surface, such as a treatment table. The nurse can partially stabilize the child’s outstretched arm and have the parent hug the child’s upper body, preventing movement; the nurse can then use the parent’s arm to immobilize the venipuncture site. This type of comfort hold also comforts the child because of the close body contact, allows for distraction techniques for the child, and allows each person to maintain eye contact (Fig. 39.6).

A child sitting in the lap of a woman. The woman holds the child in a secure and comfortable position with her belly in a close physical contact with the back of the child. A nurse in front of them is engaging the child with a toy in her gloved hands, as she smiles and interact with the child.
Lumbar puncture
Pediatric LP sets contain smaller spinal needles, but sometimes the provider will specify a different size or type of needle depending on the child’s size or obesity. The technique for the LP procedure in infants and children is similar to that in adults, although modifications are suggested in neonates, who have less distress in a side-lying position with modified neck extension than in flexion or a sitting position.
Children can be positioned in a side-lying or sitting position. Children are usually easiest to control in the side-lying position, with the head flexed and the knees drawn up toward the chest. Even cooperative children need to be held gently under the knees and around the shoulders to prevent possible trauma from unexpected, involuntary movement. They can be reassured that, although they are trusted, holding will serve as a reminder to maintain the desired position. It also provides a measure of support and reassurance to them (Fig. 39.7).

An infant lying on the left side position, and a nurse holds the back of the infant with her hands. One of the hands is at the back of the neck of the infant while the other hand is at the lower back in the space surrounding the spinal column.
A flexed sitting position may be used, depending on the child’s ability to cooperate and whether sedation will be used. In the sitting position with the hips flexed and spine curved forward, the interspinous space is maximized between L3 and L5. The child is placed with the buttocks at the edge of the table. For an infant, the nurse’s hands immobilize the arms and legs. Neck flexion has not been shown to enhance the interspinous space opening in children.
Specimens and spinal fluid pressure are obtained, measured, and sent for analysis in the same manner as for adult patients. Take vital signs as ordered throughout and after the procedure and observe the child for any changes in level of consciousness, motor activity, and other neurologic signs. Post-LP headache may occur and can be related to larger needle size, prior history of headaches, and postural changes. There is insufficient evidence to support the use of bed rest after LP to reduce post-LP headaches (Rusch, Schulta, Hughes, et al., 2014). Treatment generally includes rest and oral analgesics, such as acetaminophen, that do not inhibit platelet function.
Bone marrow aspiration or biopsy
The position for a bone marrow aspiration or biopsy depends on the chosen site. In children, the posterior or anterior iliac crest is most frequently used, but in infants less than 18 months old, the tibia may be selected because the iliac crest has not yet ossified.
If the posterior iliac crest is used, the child is positioned prone, and if the anterior iliac crest is used, the child is typically positioned side-lying or supine. Sometimes a small pillow or folded blanket is placed under the hips to facilitate obtaining the bone marrow specimen. Children should receive adequate analgesia or anesthesia to relieve pain and should be monitored appropriately throughout the procedure. If the child might awaken, he or she may need to be held, preferably by two people—one person to immobilize the upper body and a second person to immobilize the lower extremities. A pressure dressing is applied to the puncture site on completion of the procedure. The dressing will be removed after 24 hours and the site assessed for infection.
Collection of specimens
Many of the specimens needed for diagnostic examination of children are collected in much the same way as they are for adults. Older children are able to cooperate if given proper instruction regarding what is expected of them. Infants and small children, however, are typically unable to follow directions or control body functions sufficiently to help in collecting some specimens.
Fundamental steps common to all procedures
The following steps are very important for every procedure and should be considered fundamental aspects of care. These steps, although important, are not listed in each of the specimen collection procedures.
- 1. Assemble the necessary equipment.
- 2. Introduce self to the family and verify the specimen that is to be collected.
- 3. Identify the child using two patient identifiers (e.g., patient name and medical record or birth date; neither identifier can be a room number). Compare the same two identifiers with the specimen container and order.
- 4. Perform hand hygiene, maintain aseptic technique, and follow Standard Precautions.
- 5. Explain the procedure to parents and child according to the developmental level of the child; reassure the child that the procedure is not a punishment.
- 6. Provide atraumatic care and position the child securely.
- 7. Prepare area with antiseptic agent.
- 8. Place specimens in appropriate containers with appropriate collection information such as date and time and apply a patient identification label to the specimen container in the presence of the child and family.
- 9. Discard puncture device in puncture-resistant container near the site of use.
- 10. Wash the procedural preparation agent off if povidone-iodine is used, if skin is sensitive, and for infants. Check that all collection supplies have been removed from the patient’s bed area to ensure patient safety.
- 11. Remove gloves and perform hand hygiene after the procedure. Have children wash their hands if they have helped.
- 12. Praise the child for helping.
- 13. Document pertinent aspects of the procedure, such as number of attempts, site, and amount of blood or urine withdrawn, as well as type of test performed.
Urine specimens
Many diagnostic situations warrant urine specimens. The age of the child will affect the collection technique, as will developmental considerations. Children will better understand what is expected if the nurse uses familiar terms, such as “pee-pee,” “wee-wee,” or “tinkle.” Preschoolers and toddlers are usually unable to void on request. It is often best to offer them water or other liquids that they enjoy and wait about 30 minutes until they are ready to void voluntarily. Some have difficulty voiding in an unfamiliar receptacle. Potty chairs or a potty hat placed on the toilet is usually satisfactory. Toddlers who have recently acquired bladder control may be especially reluctant because they undoubtedly have been admonished for “going” in places other than those approved by parents. Enlisting the parents’ help usually leads to success. School-age children are generally cooperative with collection methods but curious. They are concerned about the reasons behind things and are likely to ask questions about the disposition of their specimen and what one expects to discover from it. Self-conscious adolescents may be reluctant to carry a specimen through a hallway or waiting room and appreciate a paper bag for disguising the container. The presence of menses may be an embarrassment or a concern to teenage girls; therefore it is a good idea to ask them about this and make adjustments as necessary. The specimen can be delayed or a notation made on the laboratory slip to explain the presence of red blood cells.
At times, parents may be asked to bring a urine sample to a health care facility for examination, especially when infants are unable to void during an outpatient visit. In these instances, parents need instructions on applying the collection device and storing the specimen. Ideally, the specimen should be brought to the designated place as soon as possible. If there is a delay, the sample should be refrigerated and the lapsed time reported to the examiner.
Although it is a convenient and noninvasive collection method, direct urine aspiration from a diaper can alter the specimen results. Superabsorbent gel disposable diapers may absorb all urine and may also produce a false crystalluria. Direct aspiration from the diaper may not be suitable for all urine specimen tests. Nurses should verify collection procedures with the laboratory before collection.
Urine collection bags
For infants and toddlers who are not toilet trained, special urine collection bags with self-adhering material around the opening at the point of attachment may be used. To prepare the infant, the genitalia, perineum, and surrounding skin are washed and dried thoroughly because the adhesive will not stick to a moist, powdered, or oily skin surface. The collection bag is easiest to apply if attached first to the perineum, progressing to the symphysis pubis (Fig. 39.8). With girls, the perineum is stretched taut during application to ensure a leakproof fit. With boys, the penis and sometimes the scrotum are placed inside the bag. The adhesive portion of the bag must be firmly applied to the skin all around the genital area to avoid leakage. The bag is checked frequently and removed as soon as the specimen is available because the moist bag may become loosened on an active child.

A two-part image labelled, A and B, demonstrates the applications of a urine collection bag. A: Close-up of a nurse inserting a urine collection bag into the perineum of a female infant. B: Close-up of the infant with her legs apart, and the urine collection bag inserted into the perineum. A pair of hands is holding the legs of the infant.
The American Academy of Pediatrics guidelines (American Academy of Pediatrics, Subcommittee on Urinary Tract Infections, 2011) for diagnosis and management of urinary tract infections in infants 2 to 24 months old recommend that any positive screen obtained from a bag specimen be confirmed by culture via bladder catheterization or suprapubic aspiration due to an unacceptably high rate of false-positive results. Although the bag specimen collection method is less invasive and traumatic to an infant, some families and clinicians may prefer to collect only one definitive specimen and avoid additional delay in obtaining a second specimen. Urine bag specimens may be most appropriate for a urine dipstick or urinalysis, not urine cultures (Stein, Dogan, Hoebeke, et al., 2015).
Clean-catch specimens
Clean-catch specimen traditionally refers to a urine sample obtained for culture after the urethral meatus is cleaned and the first few milliliters of urine are voided (midstream specimen). In girls, the perineum is wiped with an antiseptic pad from front to back. In boys, the tip of the penis is cleansed. If the boy is uncircumcised, the foreskin is retracted and the glans is cleansed. It is important that the inside of the specimen cup or lid is not touched or contaminated during collection to ensure accurate results.
Twenty-four-hour collection
For a 24-hour collection, collection bags are required in infants and small children. Older children require special instruction about notifying someone when they need to void or have a bowel movement so that urine can be collected separately and is not discarded. Some older school-age children and adolescents can take responsibility for collection of their own 24-hour specimens and can keep output records and transfer each voiding to the 24-hour collection container.
The collection period always starts and ends with an empty bladder. At the time the collection begins, instruct the child to void and discard the specimen. All urine voided in the subsequent 24 hours is saved in a container with a preservative or is placed on ice. Twenty-four hours from the time the precollection specimen was discarded, the child is again instructed to void, the specimen is added to the container, and the entire collection is taken to the laboratory.
Infants and small children who are bagged for 24-hour urine collection require a special collection bag. Frequent removal and replacement of adhesive collection devices can produce skin irritation. A thin coating of sealant, such as Skin-Prep, applied to the skin helps protect it and aids adhesion (unless its use is contraindicated, such as in premature infants or children with irritated skin). Plastic collection bags with collection tubes attached are ideal when the container must be left in place for a time. These can be connected to a collecting device or emptied periodically by aspiration with a syringe. When such devices are not available, a regular bag with a feeding tube inserted through a puncture hole at the top of the bag serves as a satisfactory substitute. However, take care to empty the bag as soon as the infant urinates to prevent leakage and loss of contents. An indwelling catheter may also be placed for the collection period.