Overview and Topographic Anatomy
The neck is the area between the base of the skull and inferior border of the mandible and the superior thoracic aperture
The anterior portion of the neck contains the major visceral structures between the head and the thorax:
• Thyroid and parathyroid glands
For descriptive purposes, the neck is divided into 2 triangles:
Skin is the most superficial structure covering the neck
The neck is surrounded by 2 main layers of cervical fascia that can be further subdivided:
• Superficial layer of deep cervical fascia (investing)
• Middle layer of deep fascia (includes muscular and visceral parts such as the pretracheal)
• Deep layer of deep fascia (includes prevertebral and alar)
Superficial fascia is deep to the skin and surrounds the platysma muscle
Sensory branches to the neck are located in the superficial fascia
Deep to the superficial fascia is the investing layer of deep cervical fascia
The superficial (or investing) layer of deep cervical fascia attaches posteriorly along the midline and passes anteriorly to surround the entire neck
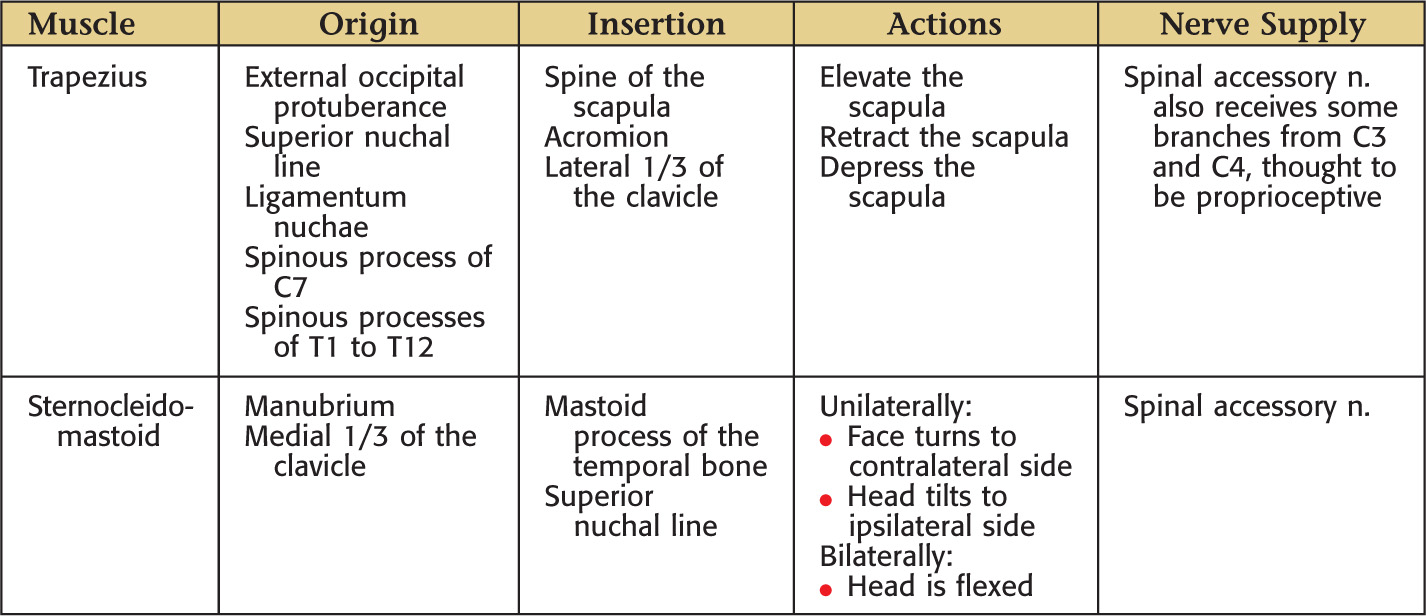
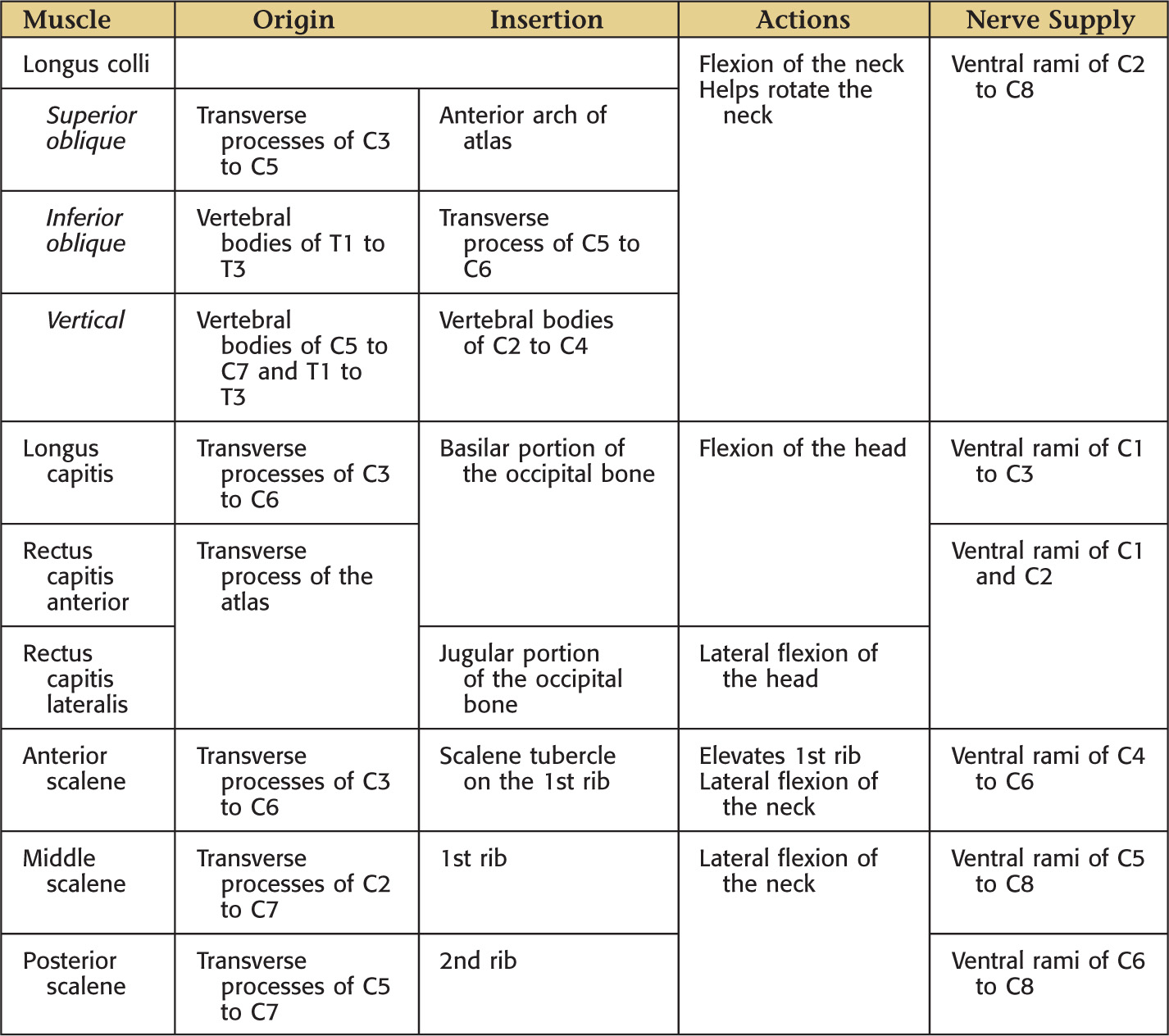
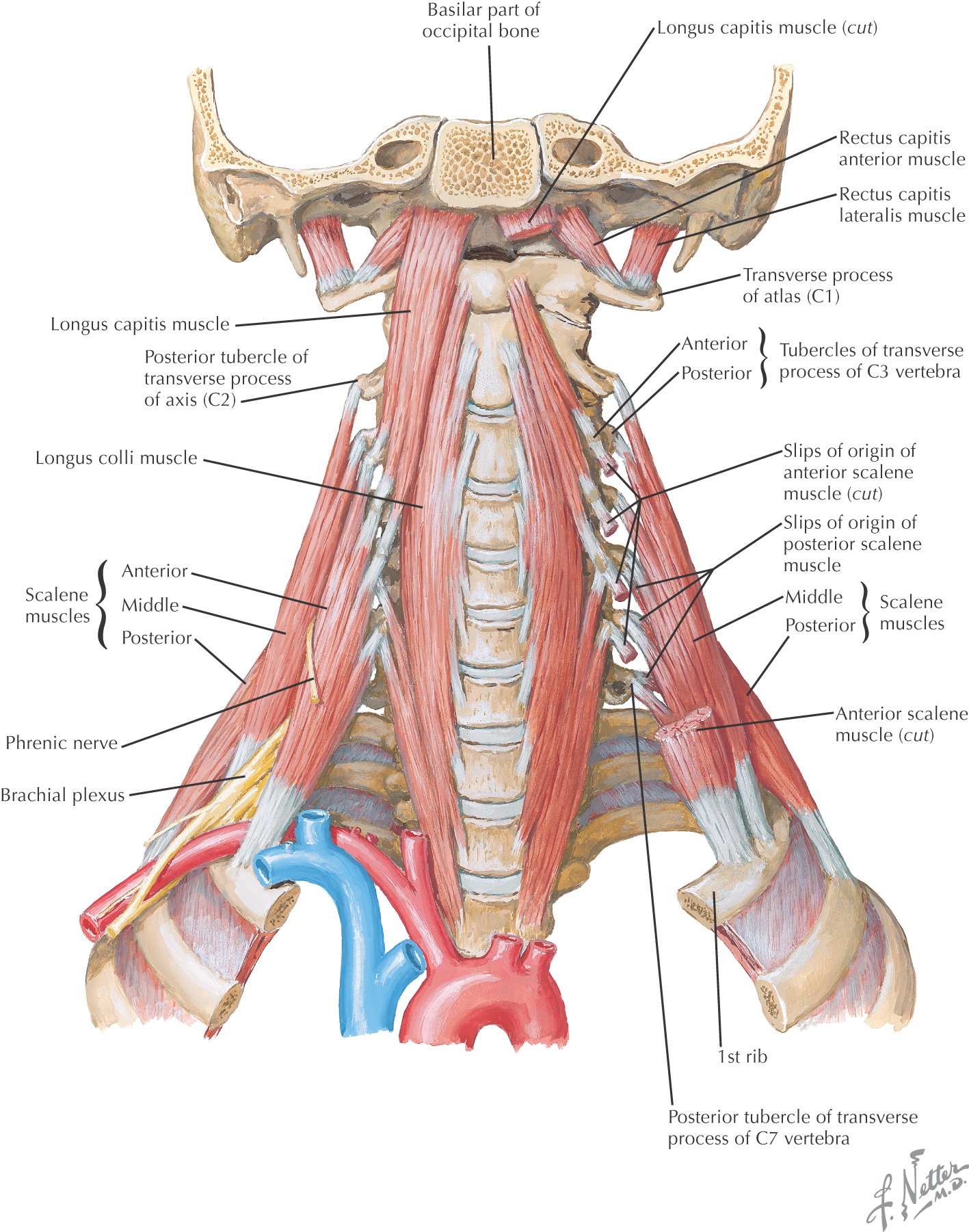
The superficial (or investing) layer of deep cervical fascia surrounds these muscles:

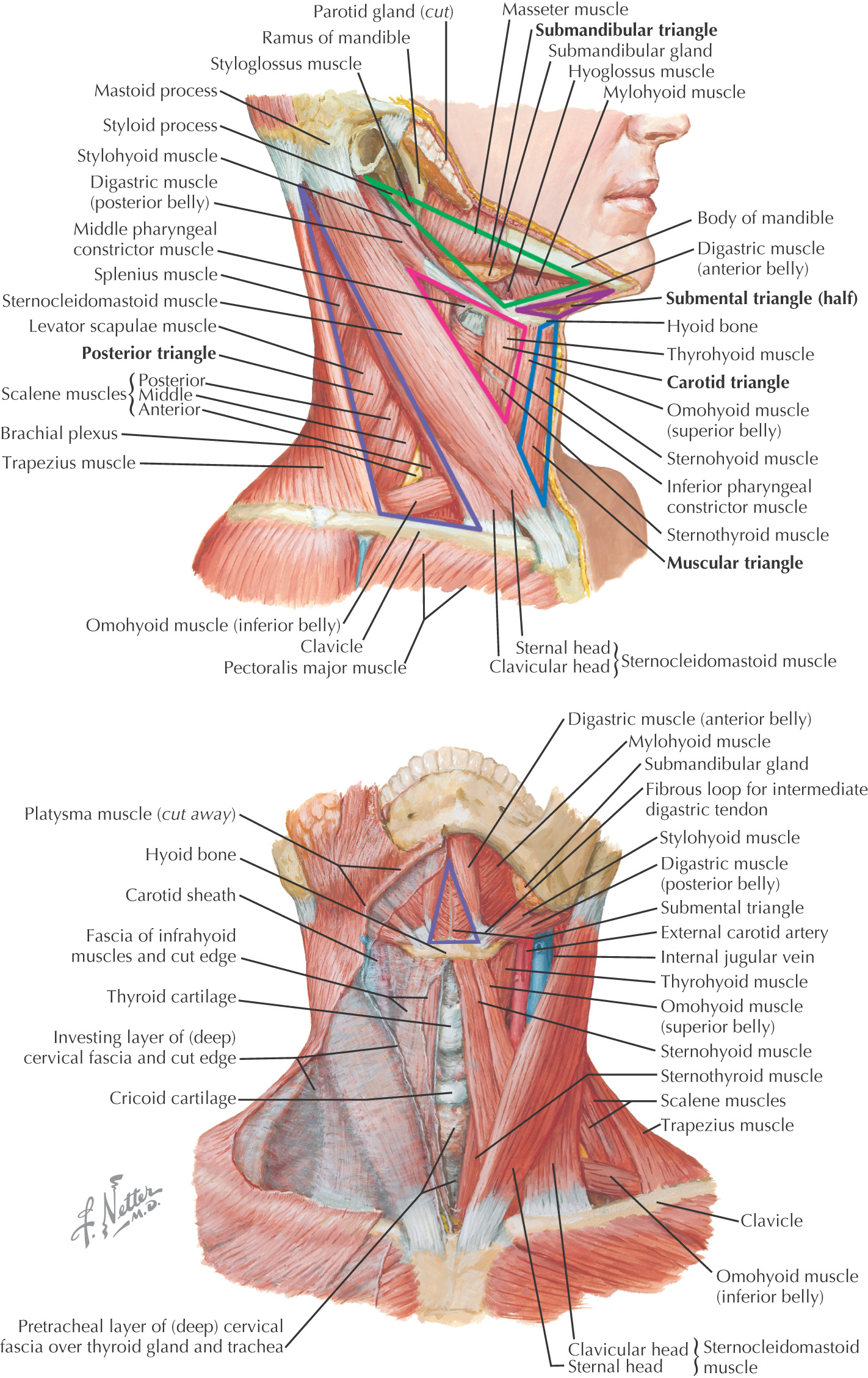
Borders of the anterior triangle:
• Anterior border of the sternocleidomastoid
• Inferior border of the mandible
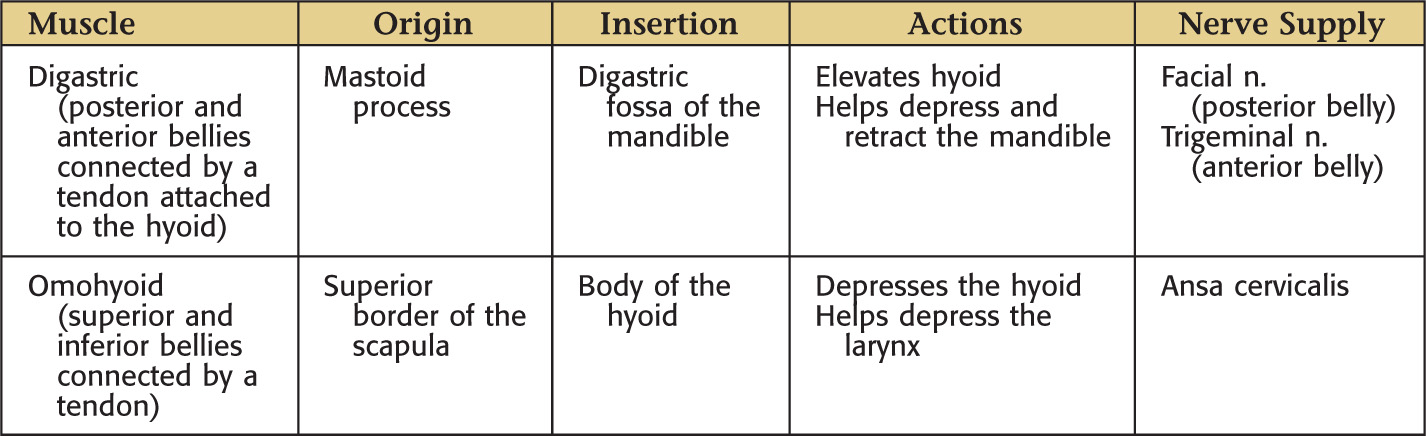
Using the hyoid as a keystone, the omohyoid and digastric muscles subdivide the anterior triangle into:
All of the triangles within the anterior triangle are paired except for the submental triangle, which spans the right and the left sides of the neck
Hyoid bone divides the anterior triangle into 2 areas: suprahyoid and infrahyoid regions
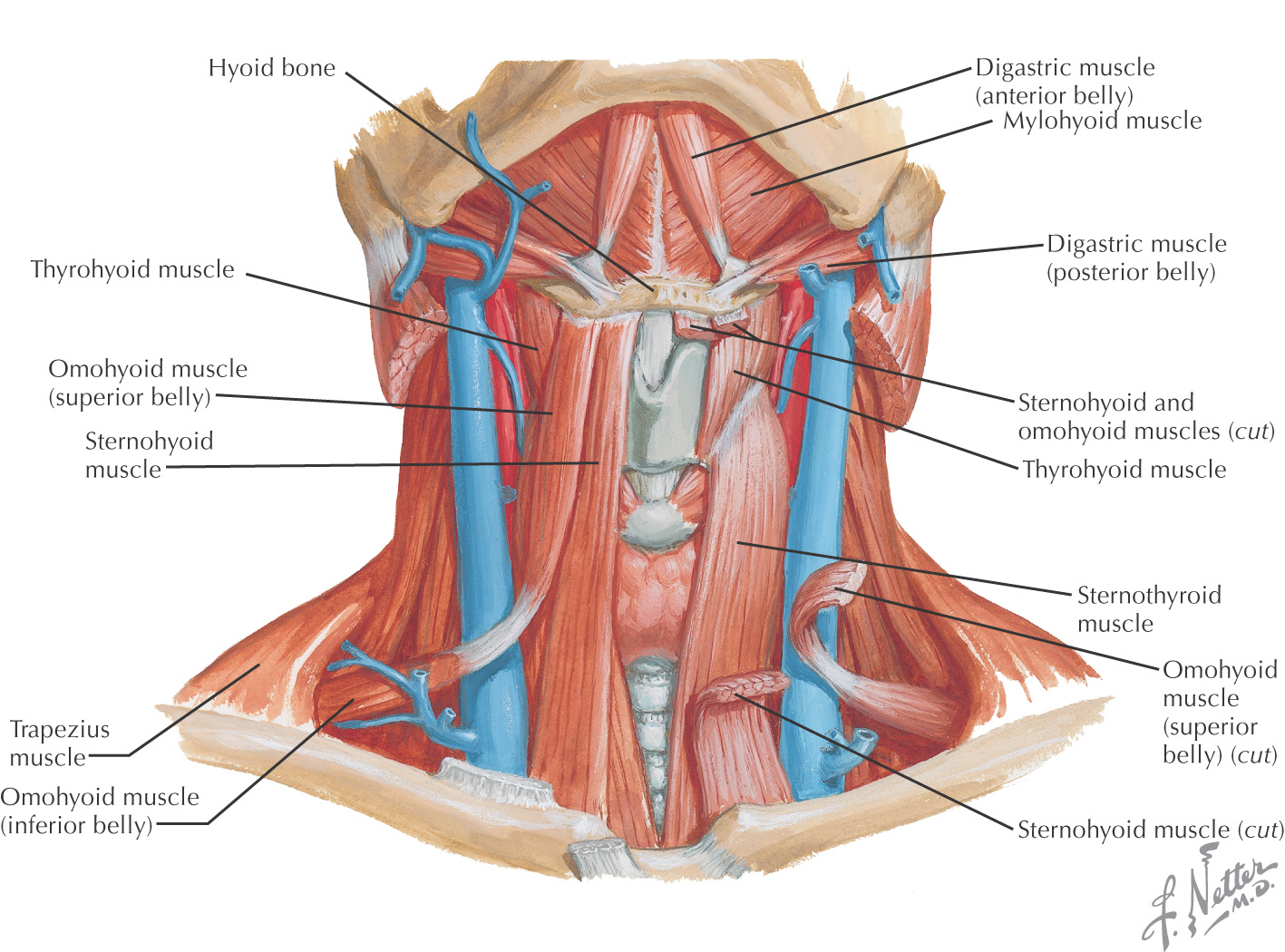
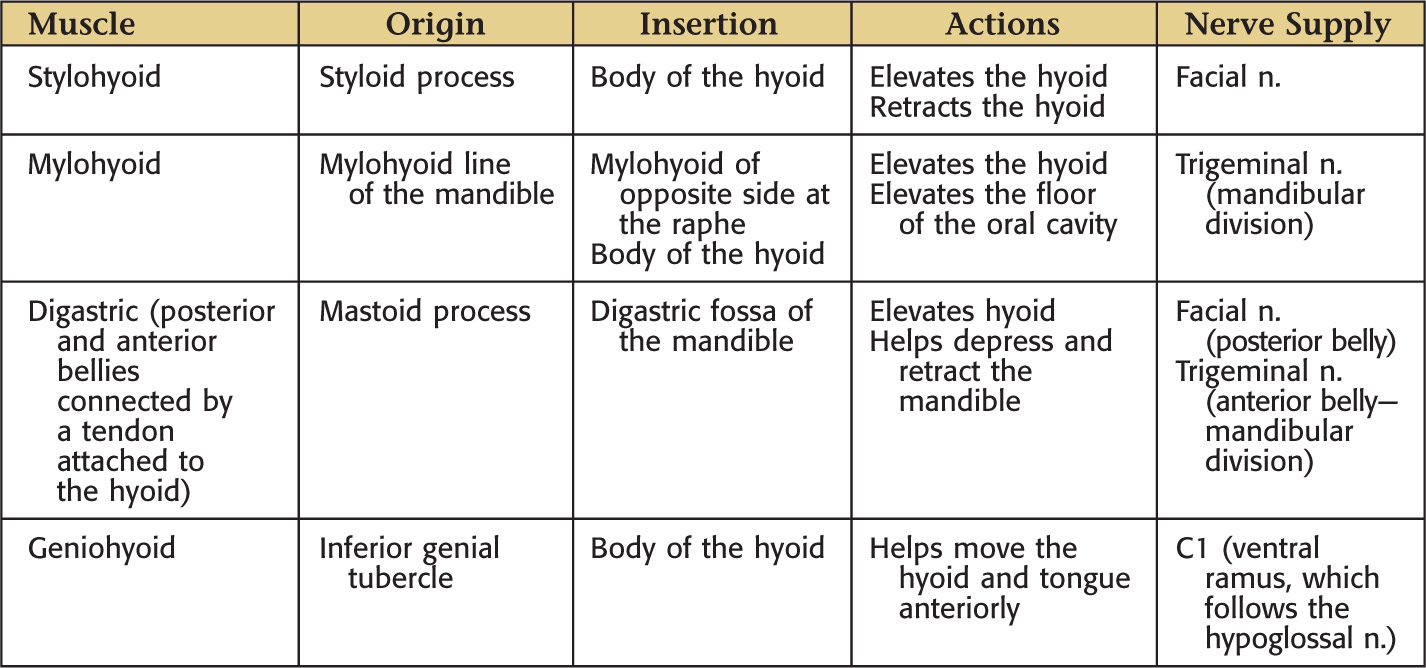
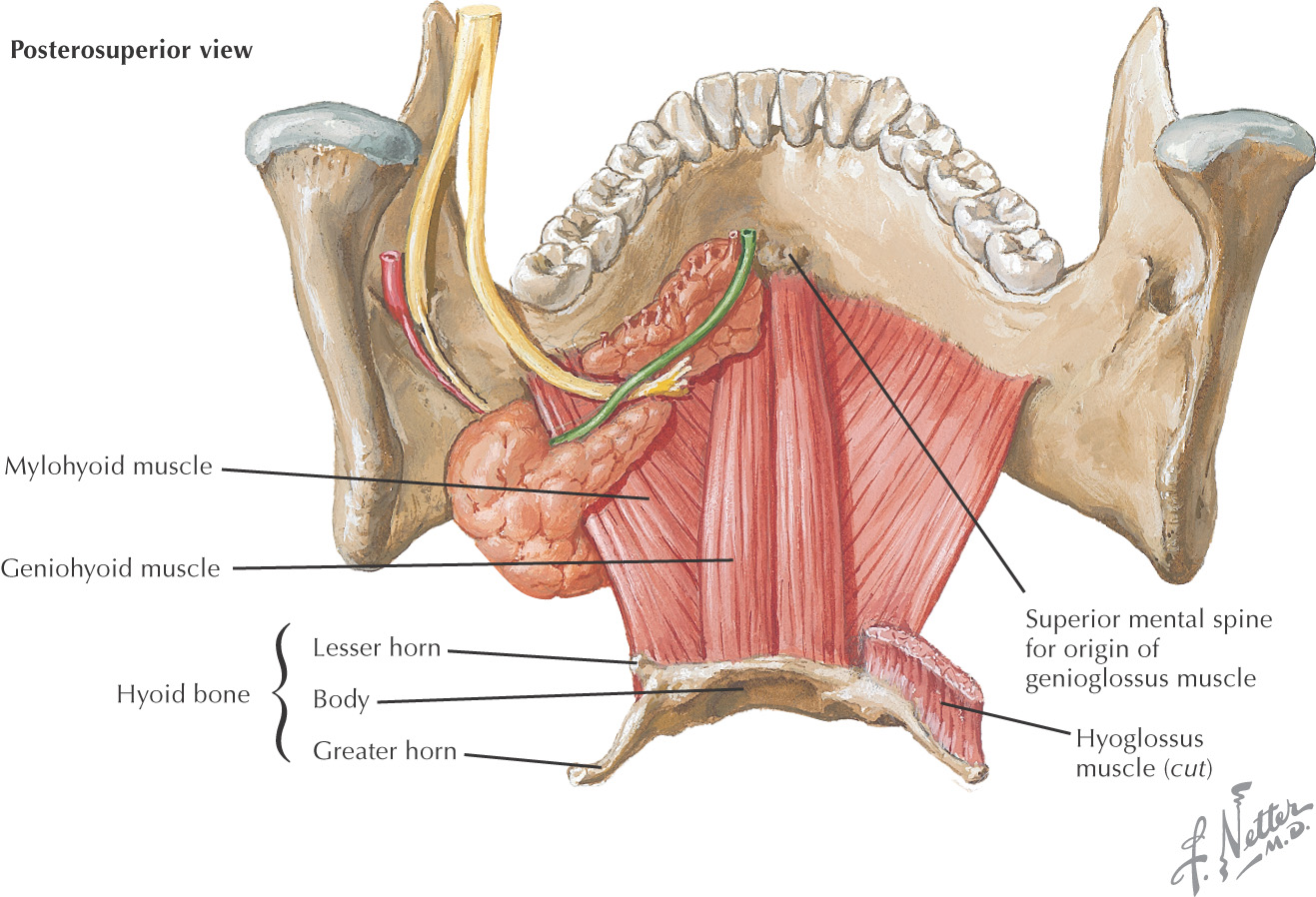
The suprahyoid region contains 4 muscles:
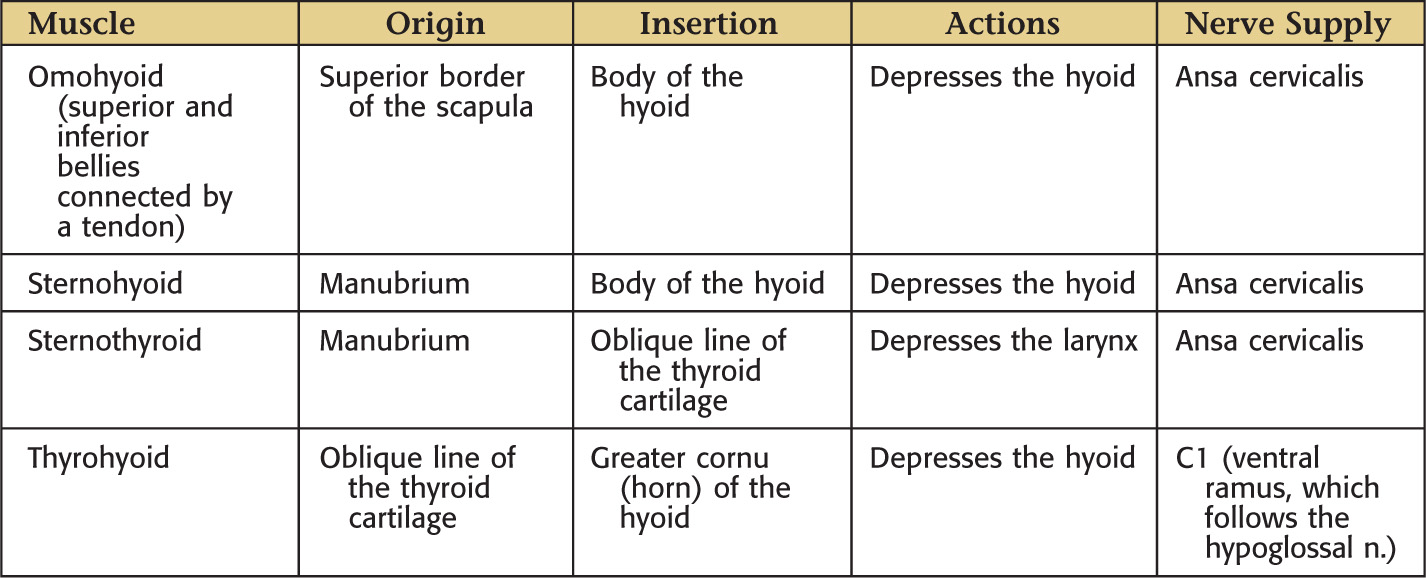
The infrahyoid region contains 4 muscles commonly called strap muscles:
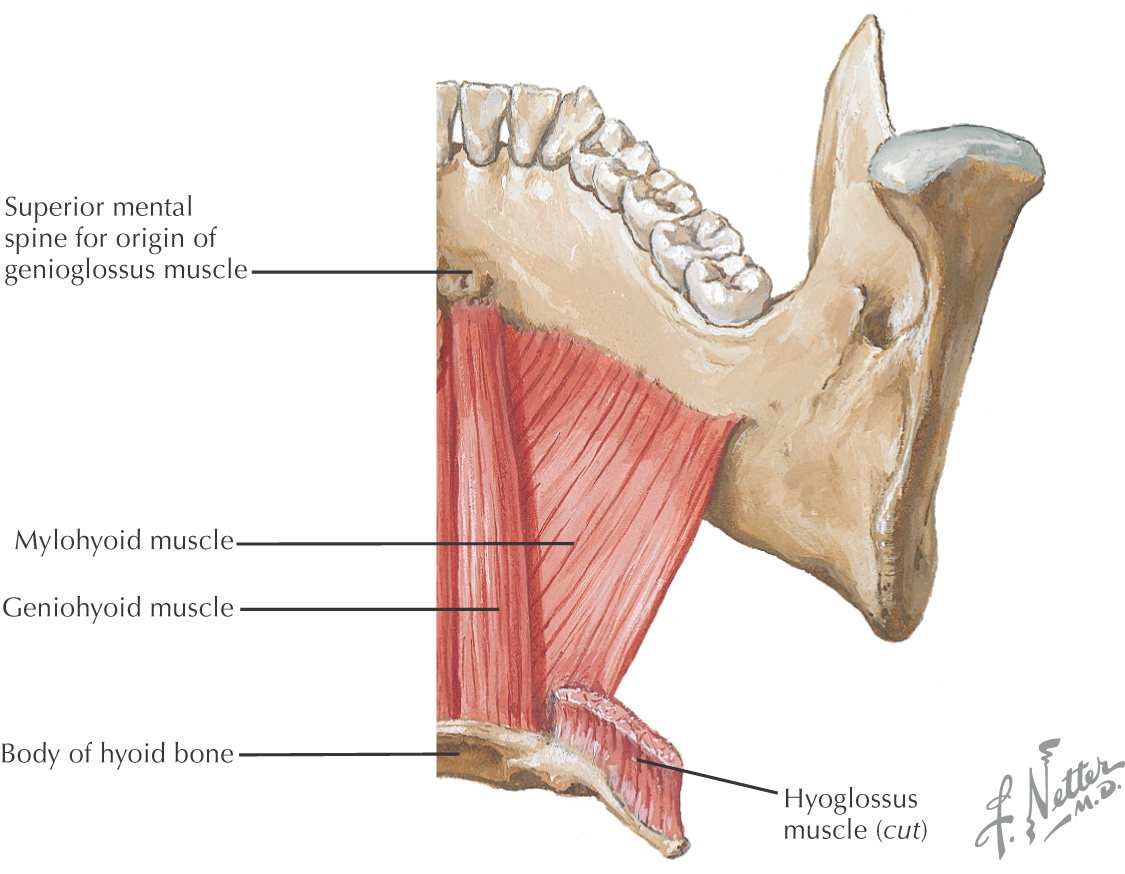
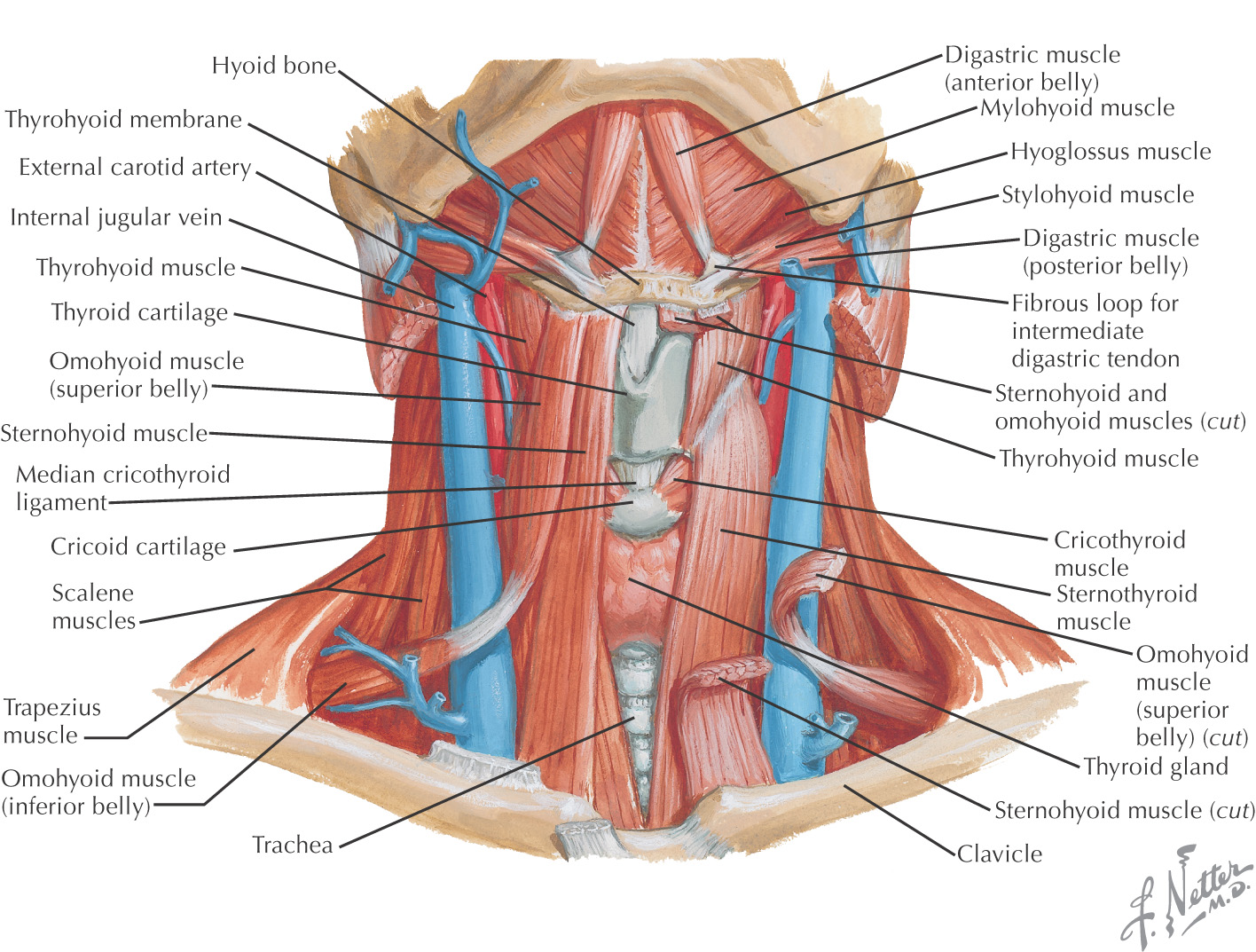
Often called the digastric triangle
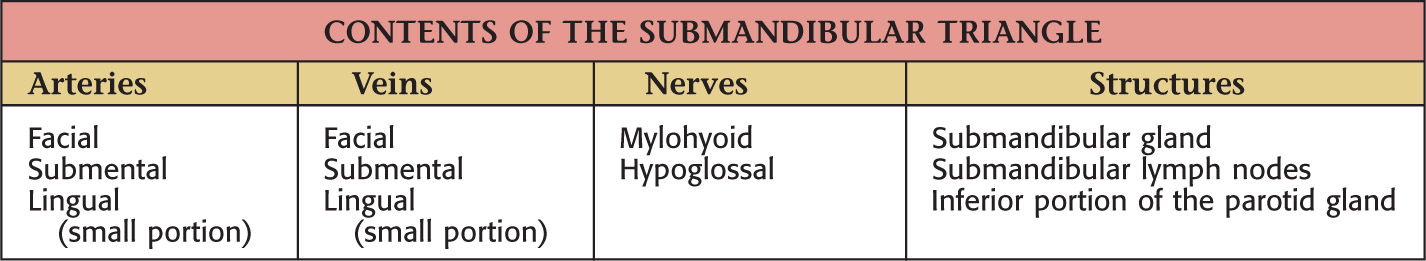
Borders of the submandibular triangle:
• Inferior border of the mandible
Floor of the triangle is composed of the:
Roof is made of the:
• Superficial fascia with platysma
Submandibular triangle is paired
Lesser’s triangle is a small subdivision of the submandibular triangle, which aids in identifying the lingual artery (especially for ligation)
Boundaries of Lesser’s triangle:

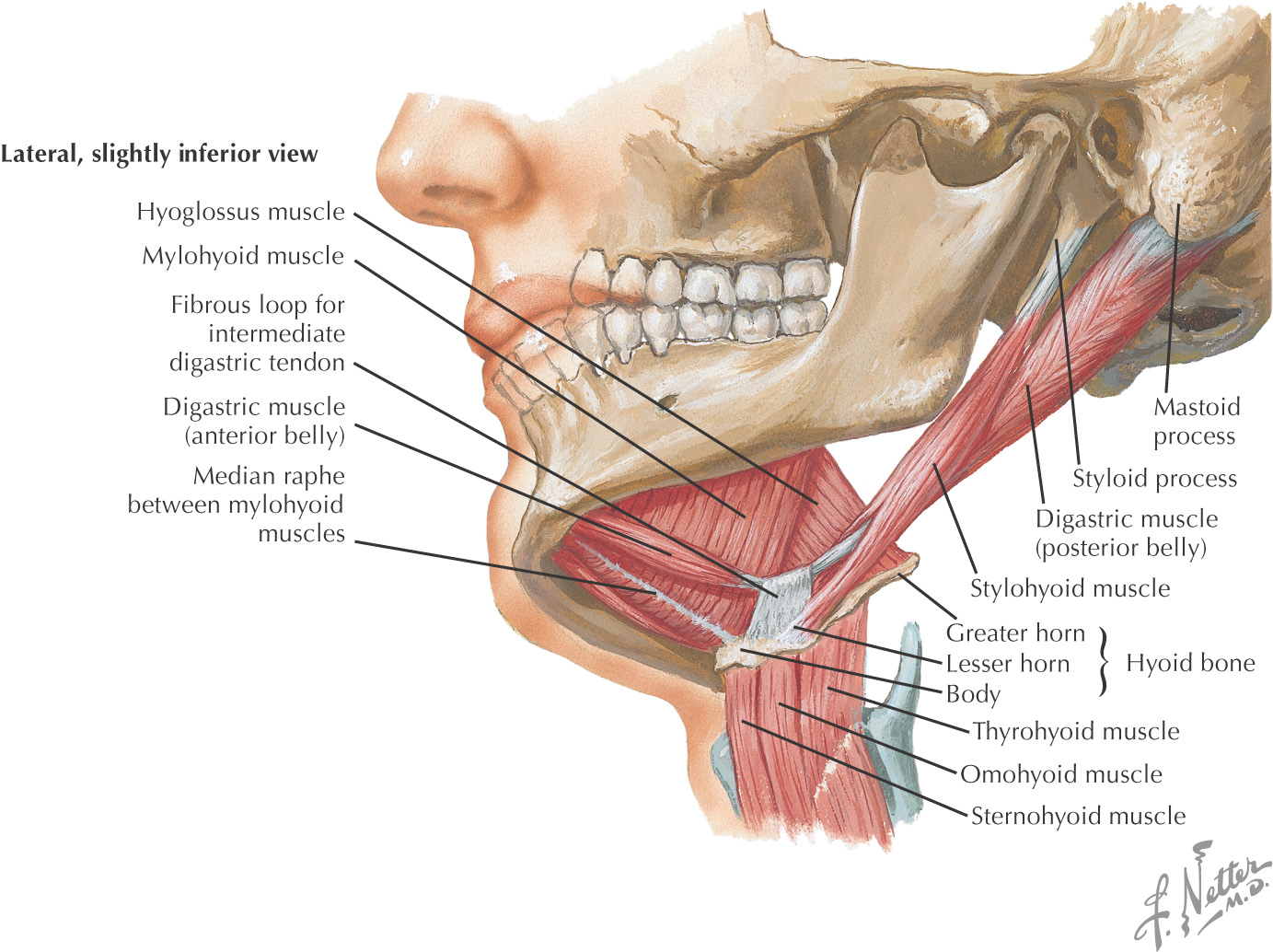
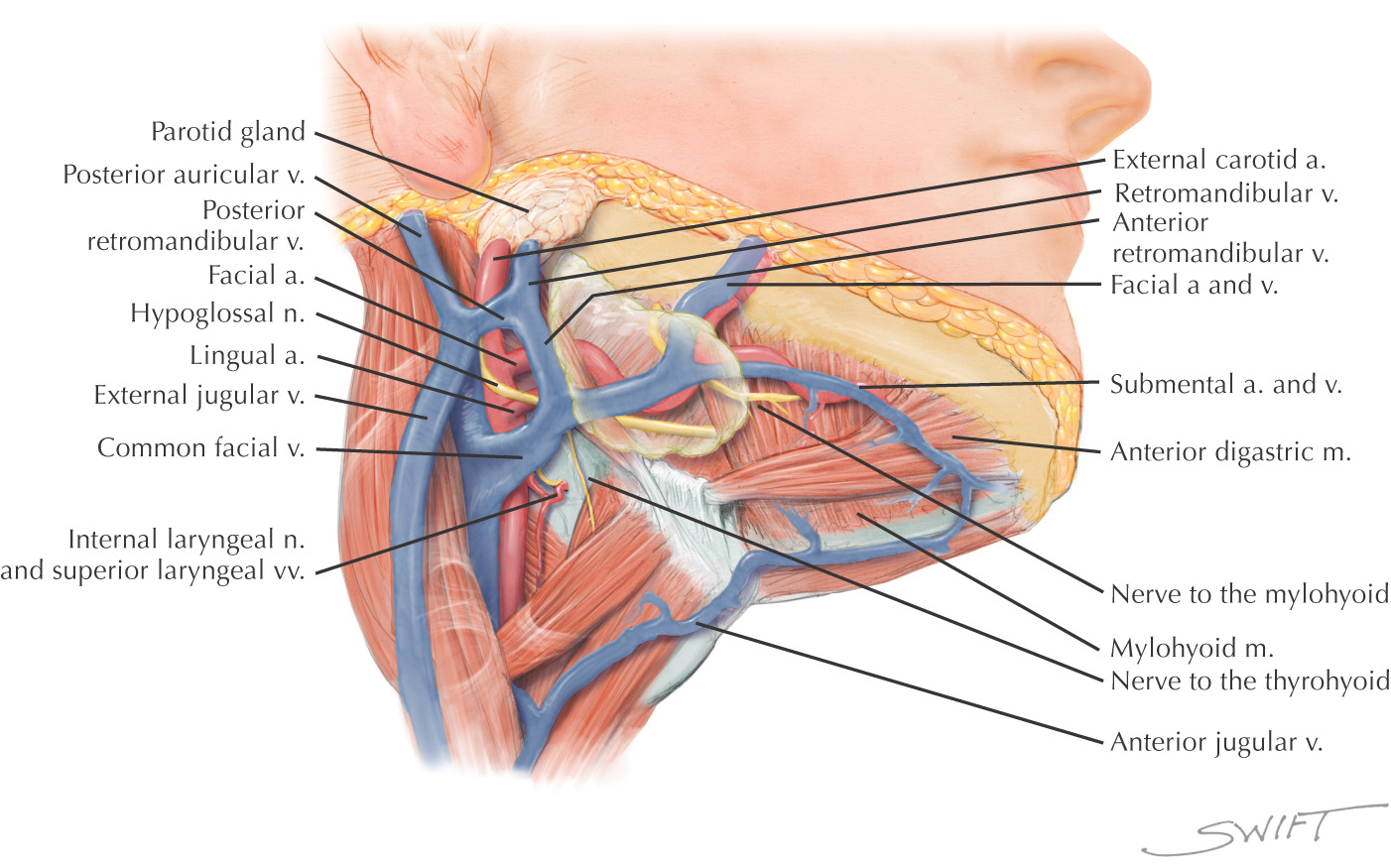
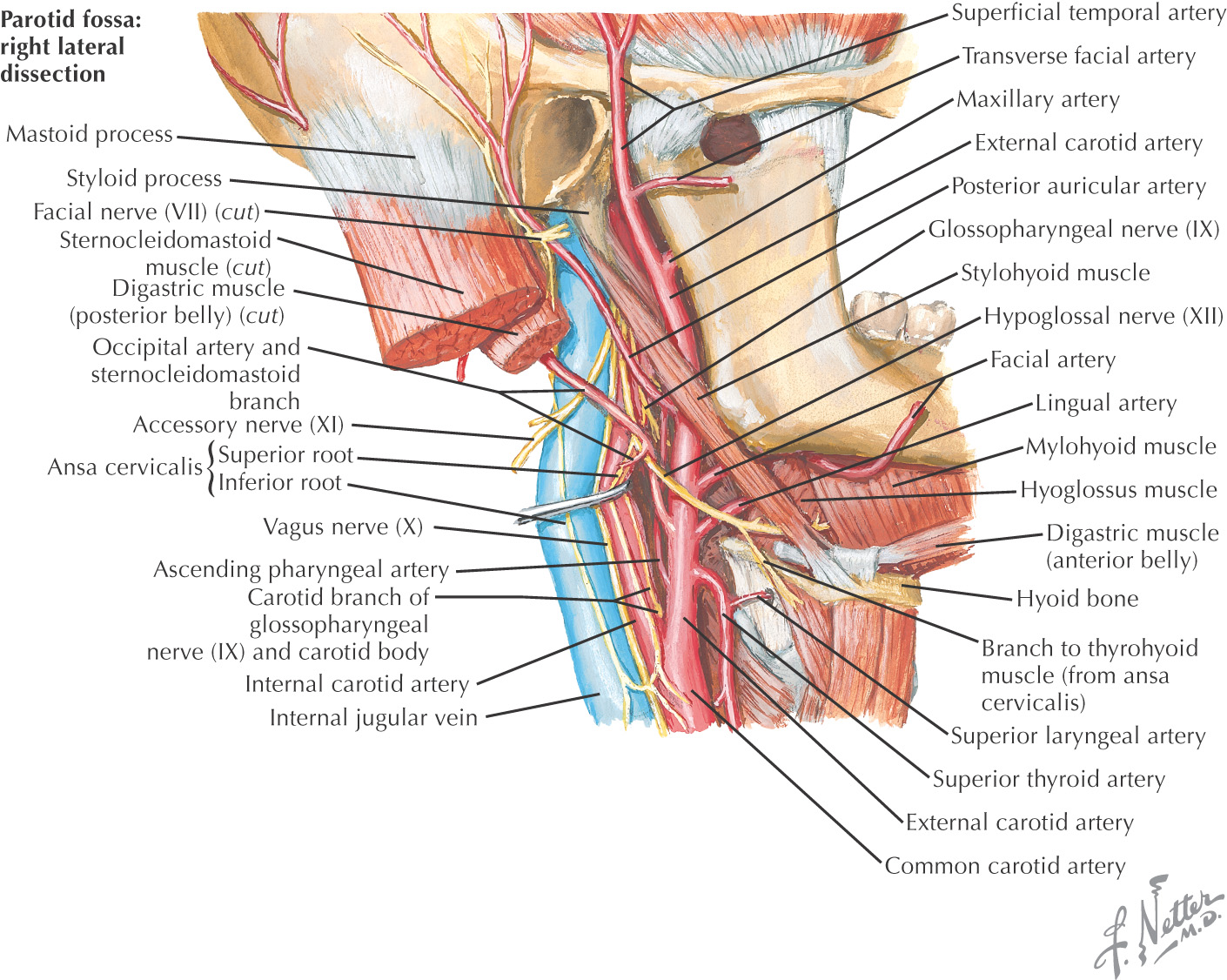
Named because parts of all three carotid arteries are located within it
Borders of the carotid triangle:
• Anterior border of the sternocleidomastoid
Floor of the triangle is composed of the:
Roof is made of the:
• Superficial fascia with platysma
Carotid triangle is paired
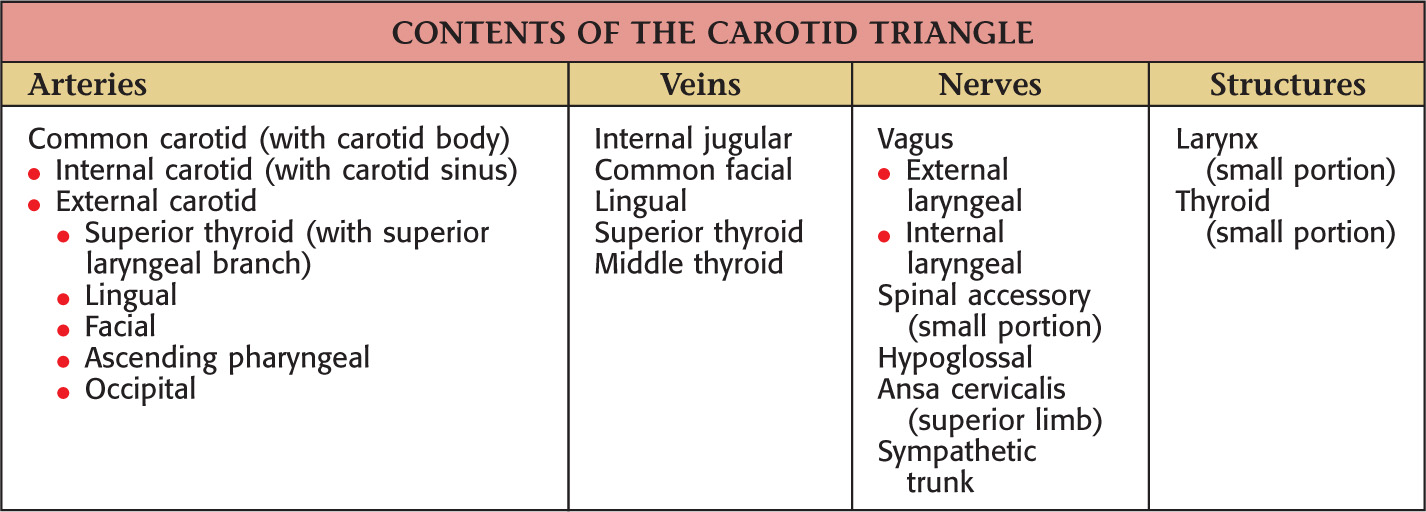
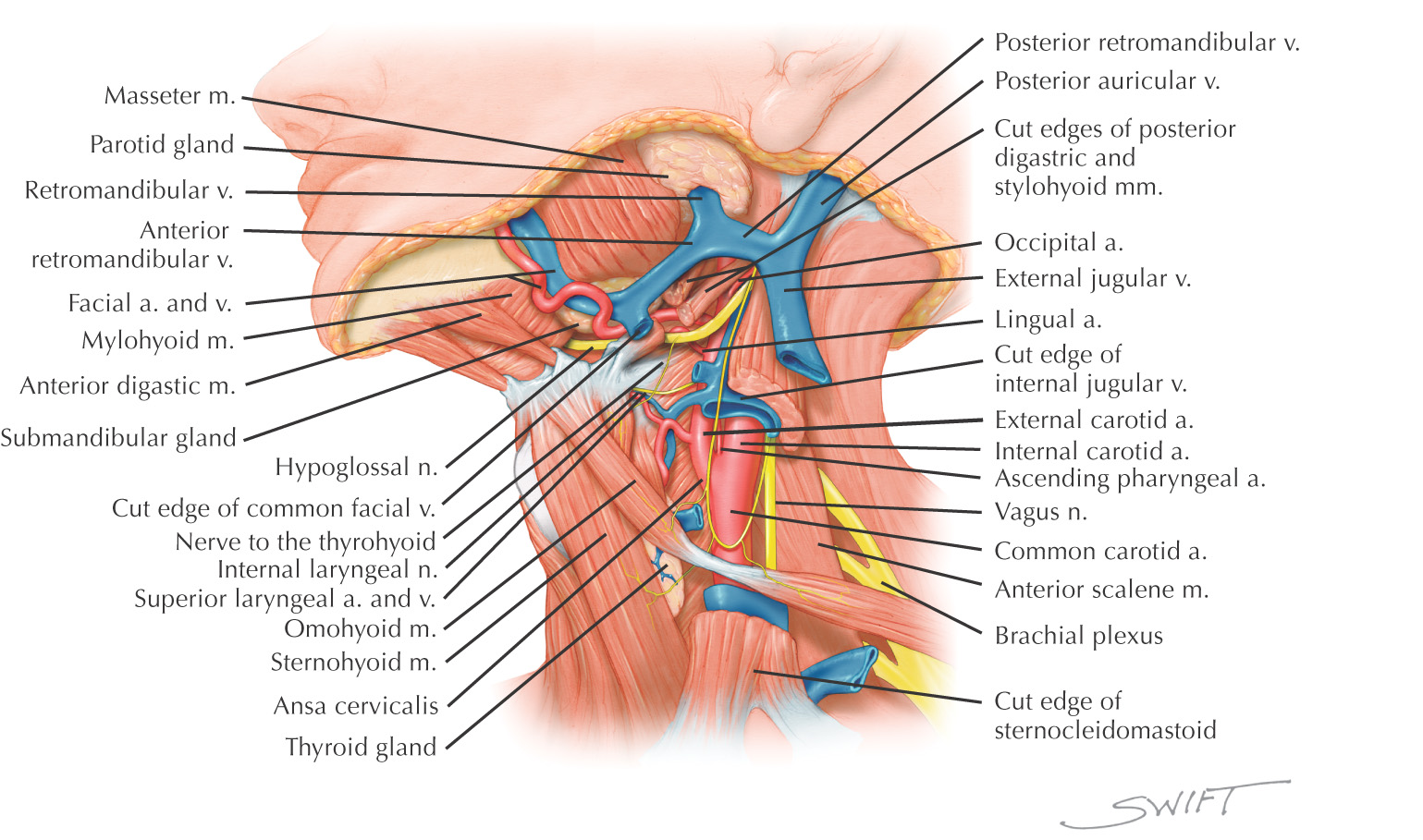
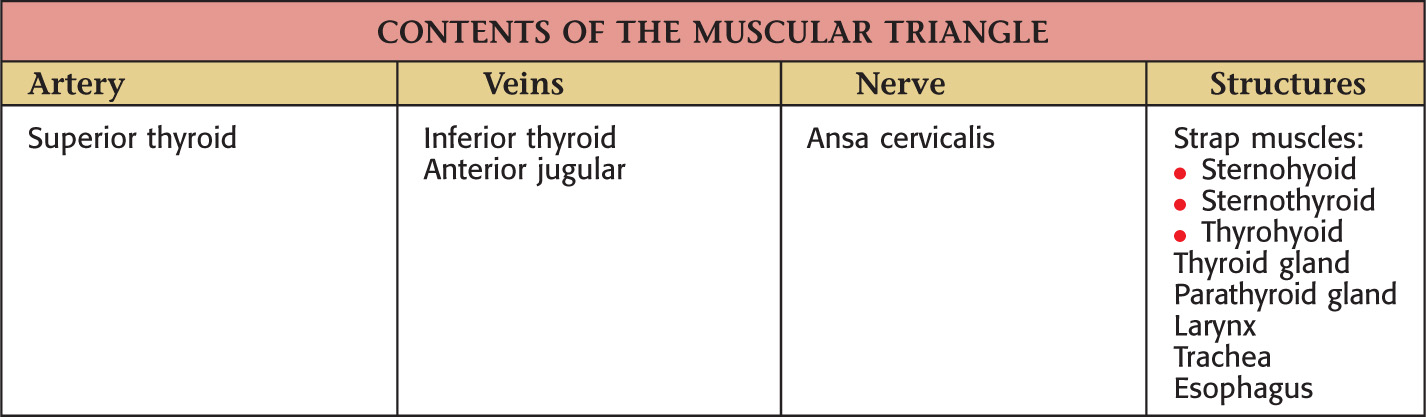
Borders of the muscular triangle:
• Anterior border of the sternocleidomastoid
Floor of the triangle is composed of the:
Roof is made of the:
• Superficial fascia with platysma
Muscular triangle is paired
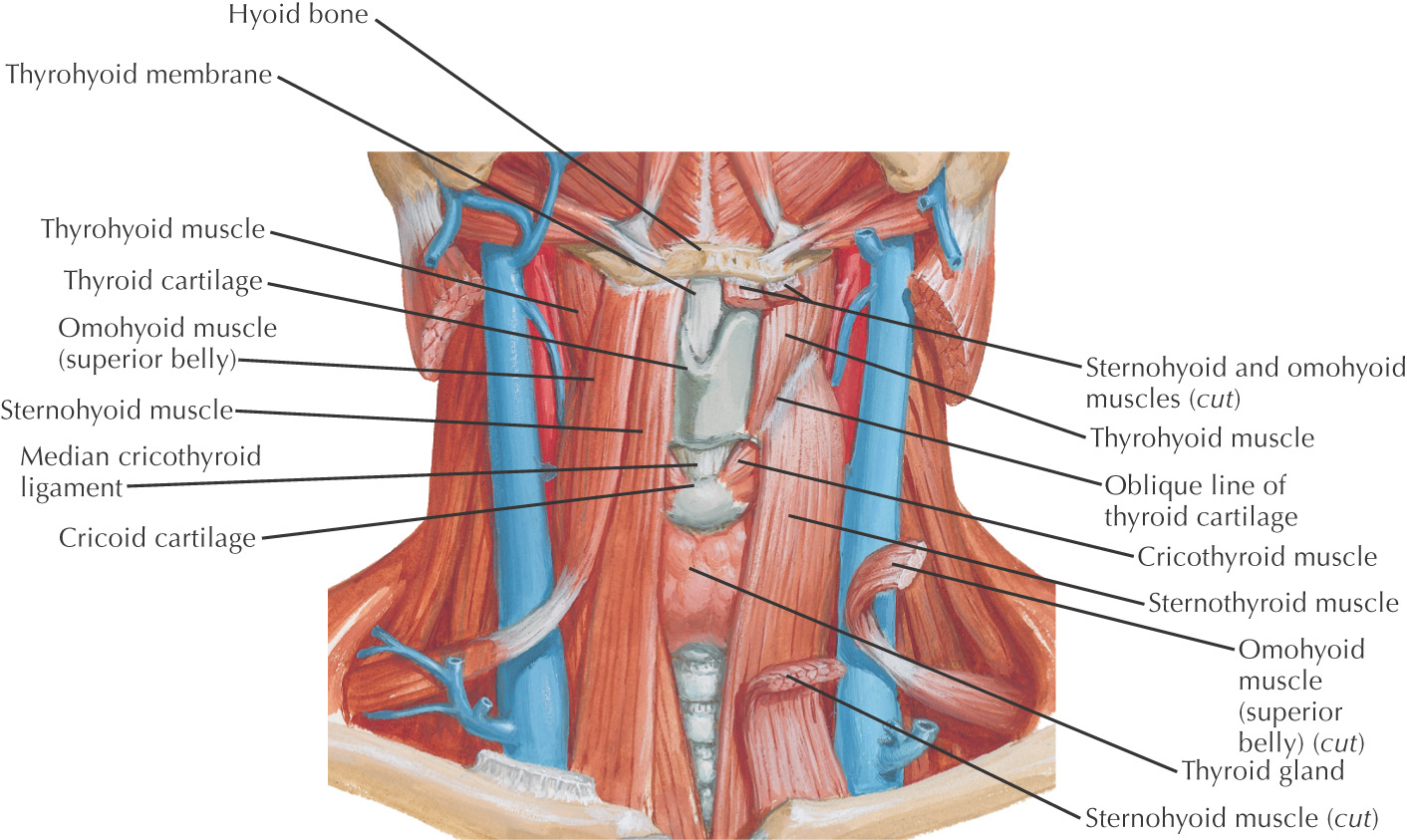
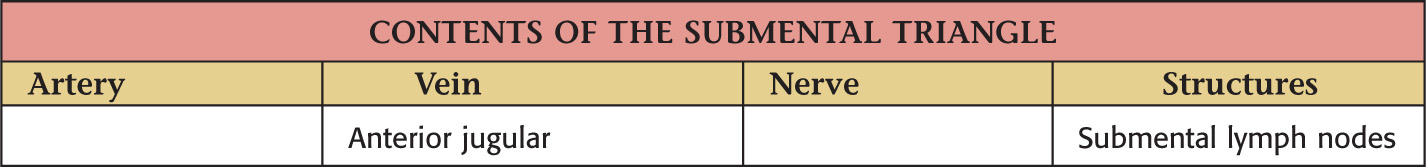
Borders of the submental triangle:
Floor of the triangle is composed of the:
Roof is made of the:
• Superficial fascia with platysma
Submental triangle is unpaired

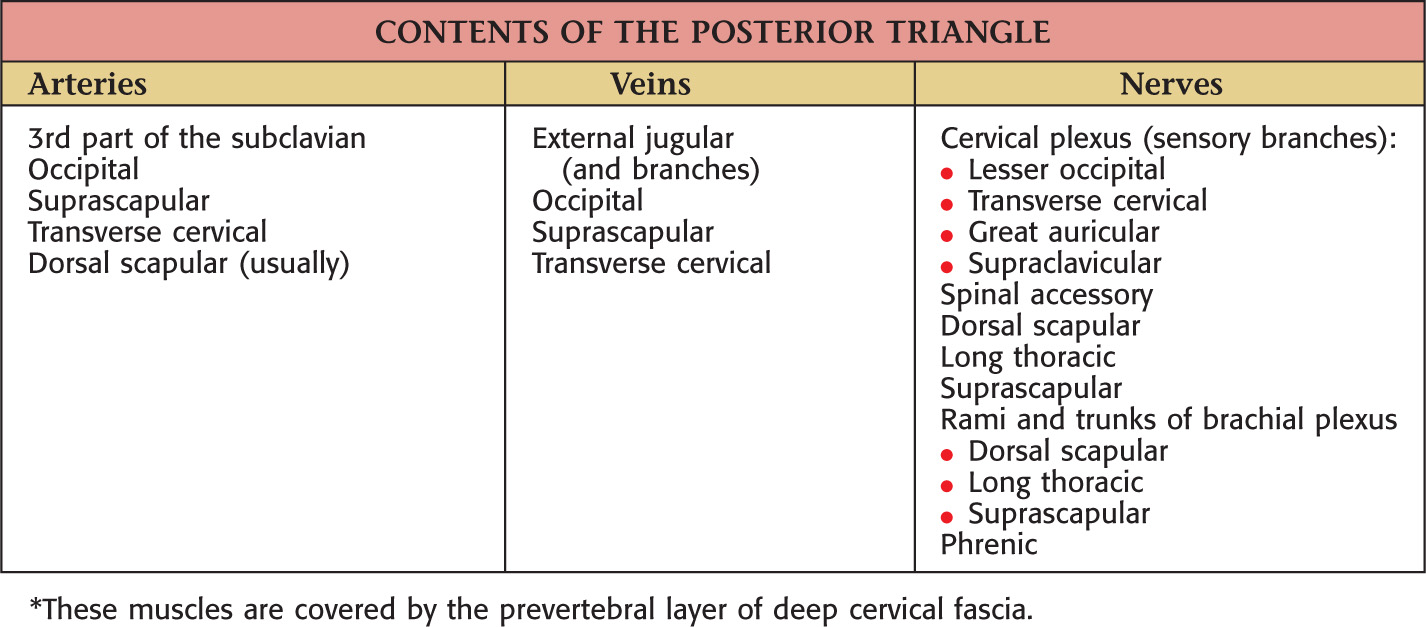
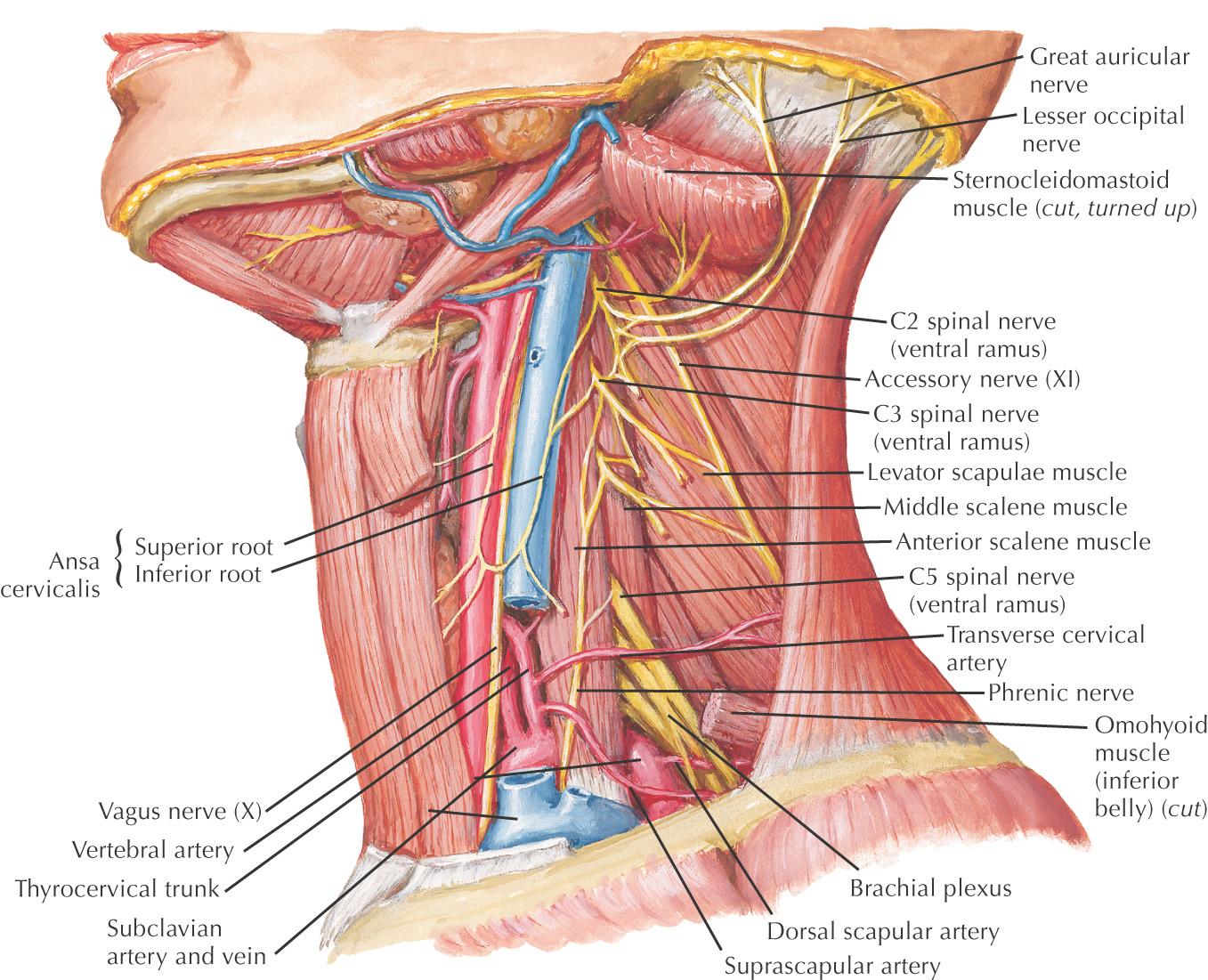
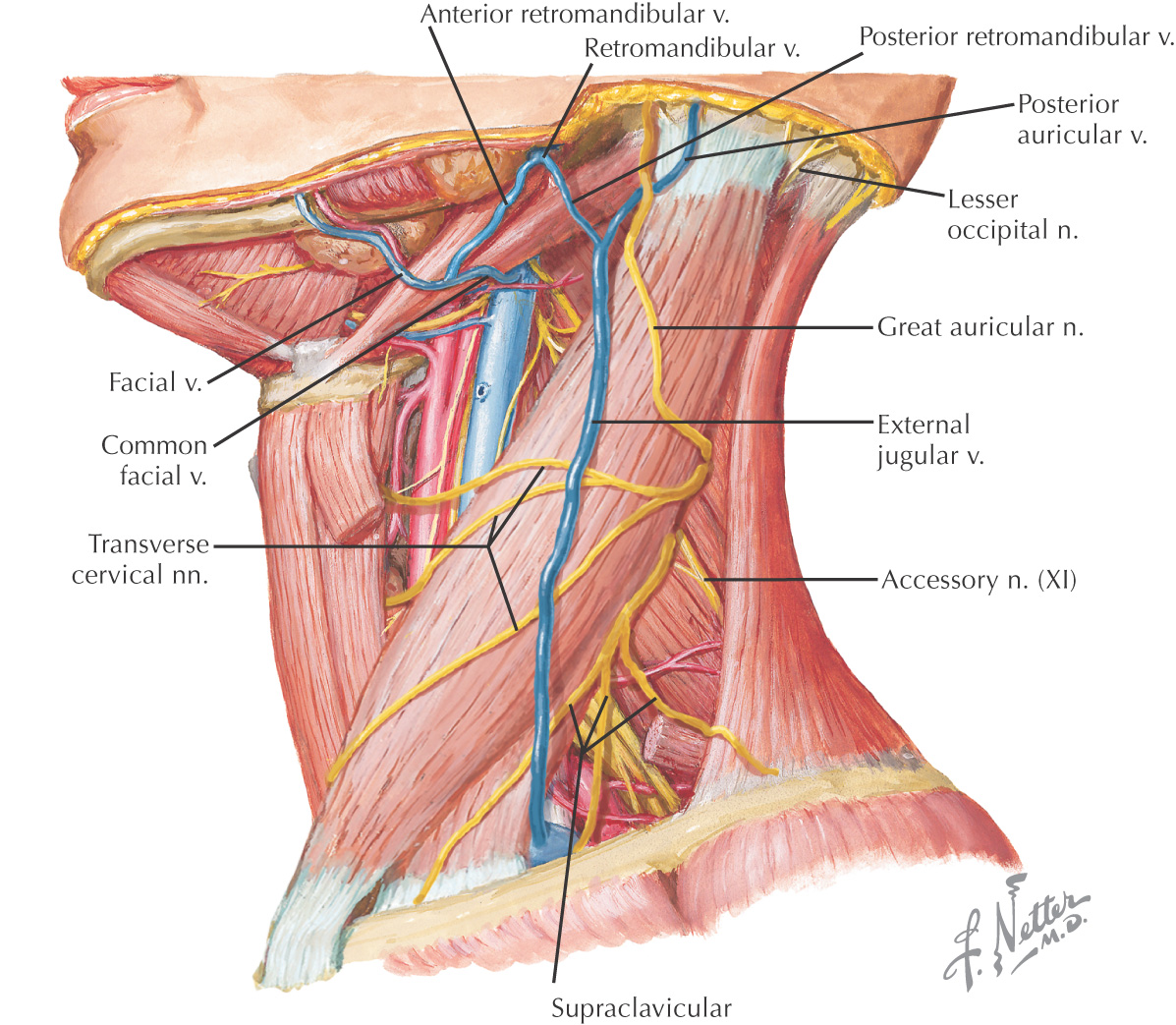
Borders of the posterior triangle:
• Posterior border of the sternocleidomastoid
• Middle third of the clavicle
• Anterior border of the trapezius
Located on the lateral side of the neck and spirals around the neck
Is subdivided into 2 triangles by the omohyoid:
• Omoclavicular (also called the supraclavicular triangle)
Roof of the posterior triangle includes:
• Superficial fascia with platysma
• Superficial (investing) layer of deep cervical fascia
Floor of the posterior triangle includes*:
Posterior triangle is paired
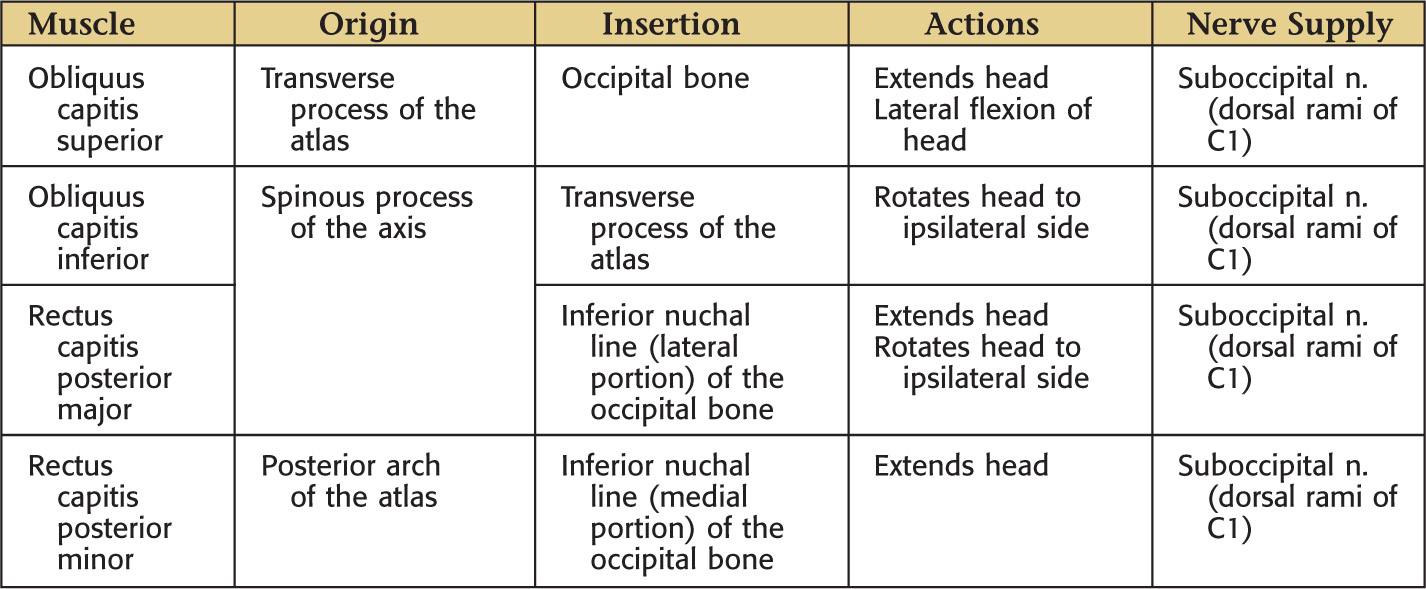
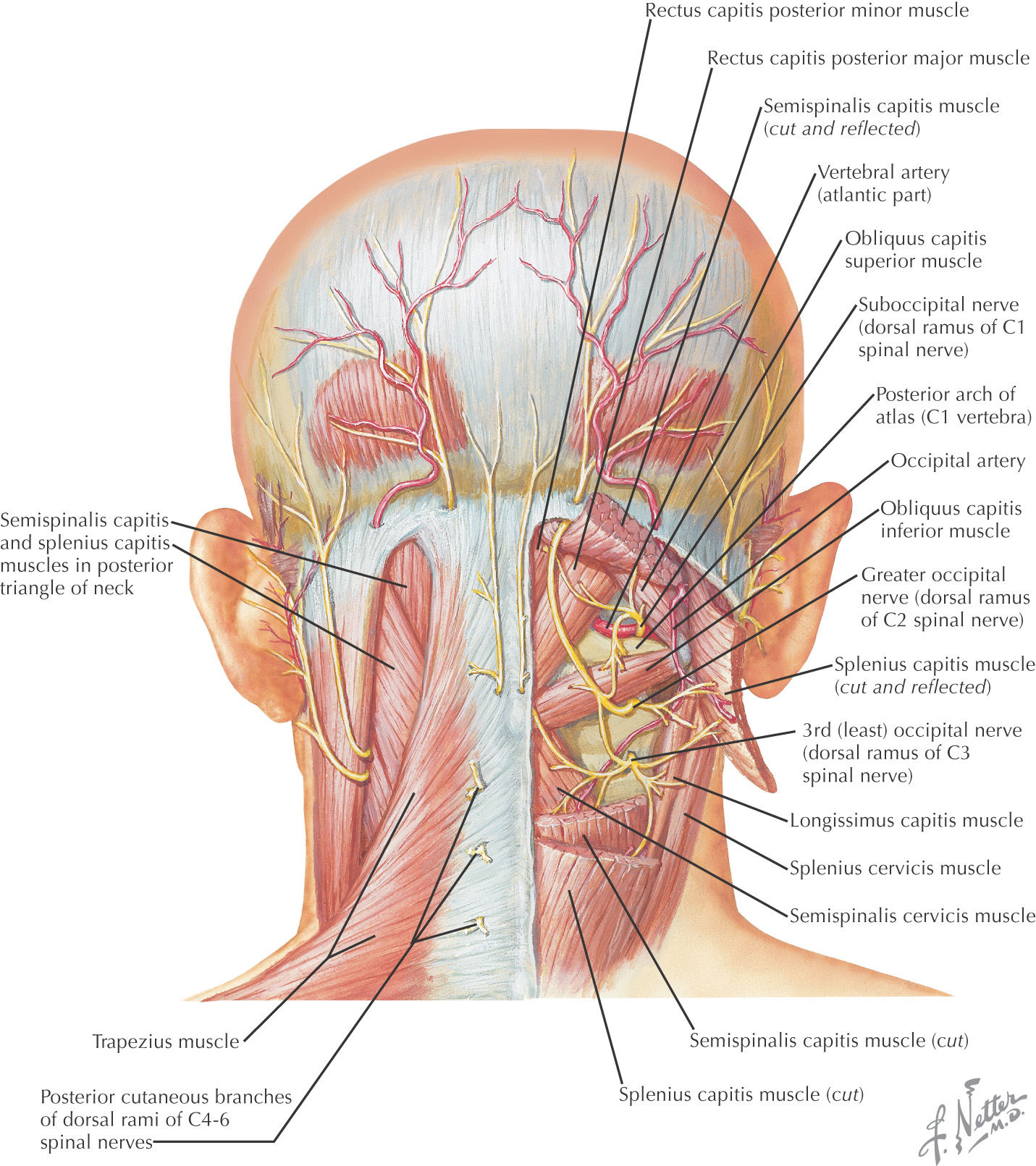
Borders of the suboccipital triangle:
• Rectus capitis posterior major
Roof of the suboccipital triangle includes:
Floor of the suboccipital triangle includes:
• Posterior atlanto-occipital membrane
Suboccipital triangle is paired
These vessels enter the foramen transversarium of the 6th cervical vertebra, emerging above the 1st cervical vertebra to enter the suboccipital triangle
They curve medially to lie in a groove on the posterior arch of the atlas
Pass through the posterior atlanto-occipital membrane to enter the vertebral canal

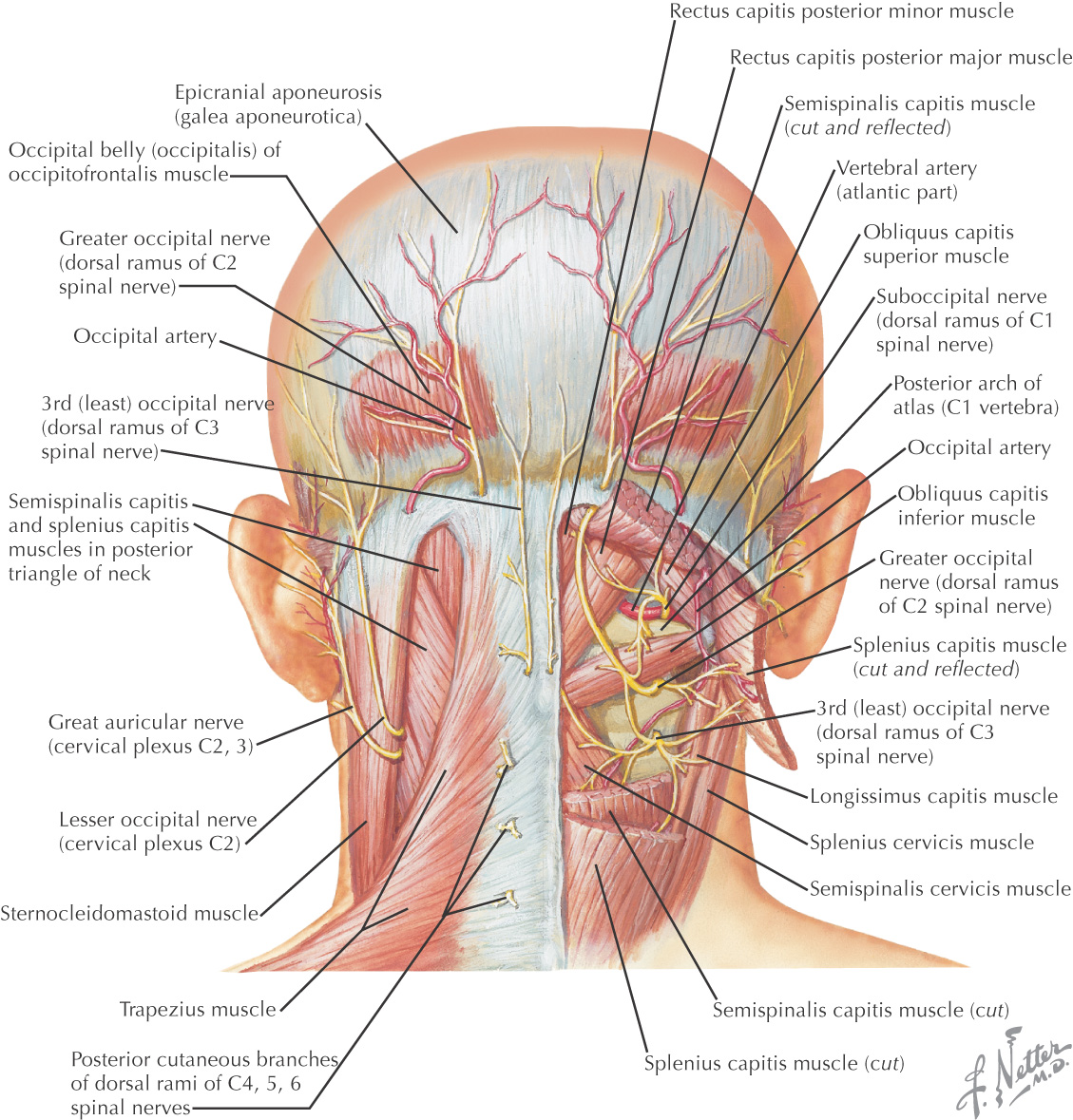
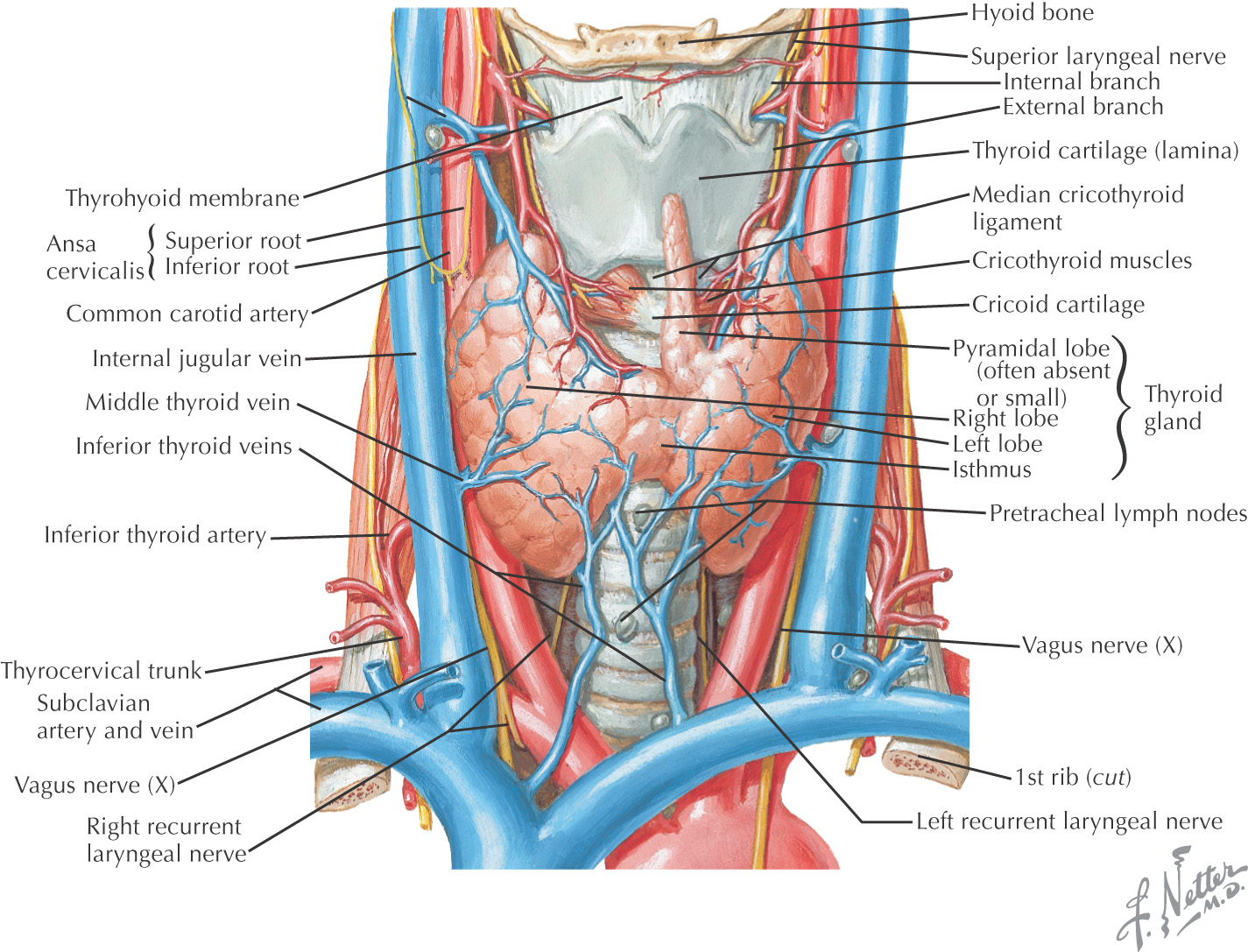
Highly vascular organ located on the anterior and lateral surfaces of the neck
Formed by a right and a left lobe connected in the midline by an isthmus
Lies roughly at a level between the 5th cervical and the 1st thoracic vertebrae
The isthmus crosses at the 2nd and 3rd tracheal rings
A pyramidal lobe often arises from the isthmus and extends superiorly
Arterial supply arises from the superior and inferior thyroid arteries, with the major portion from the inferior thyroid artery
A thyroidea ima vessel may supply the thyroid gland and arises from the brachiocephalic artery or as a direct branch from the aorta
Venous drainage forms from a plexus on the surface of the thyroid gland that drains into the superior, middle, and inferior thyroid veins
Microscopically, the thyroid is made of thyroid epithelial cells, which secrete thyroid hormones (thyroxine and triiodothyronine), and parafollicular (C cells), which secrete calcitonin
Parathyroid glands normally are 4 glands located on the posterior surface of the thyroid lobes
The superior parathyroids are supplied by the superior thyroid artery and the inferior parathyroids are supplied by the inferior thyroid artery
Microscopically, their cells are organized in cords and secrete parathyroid hormone
Connection between the pharynx and the trachea
Prevents foreign bodies from entering the airways
Designed for the production of sound (phonation)
Shorter in women and children
Formed by 9 cartilages: 3 paired and 3 unpaired
Located in the midline opposite the 3rd to 6th cervical vertebrae
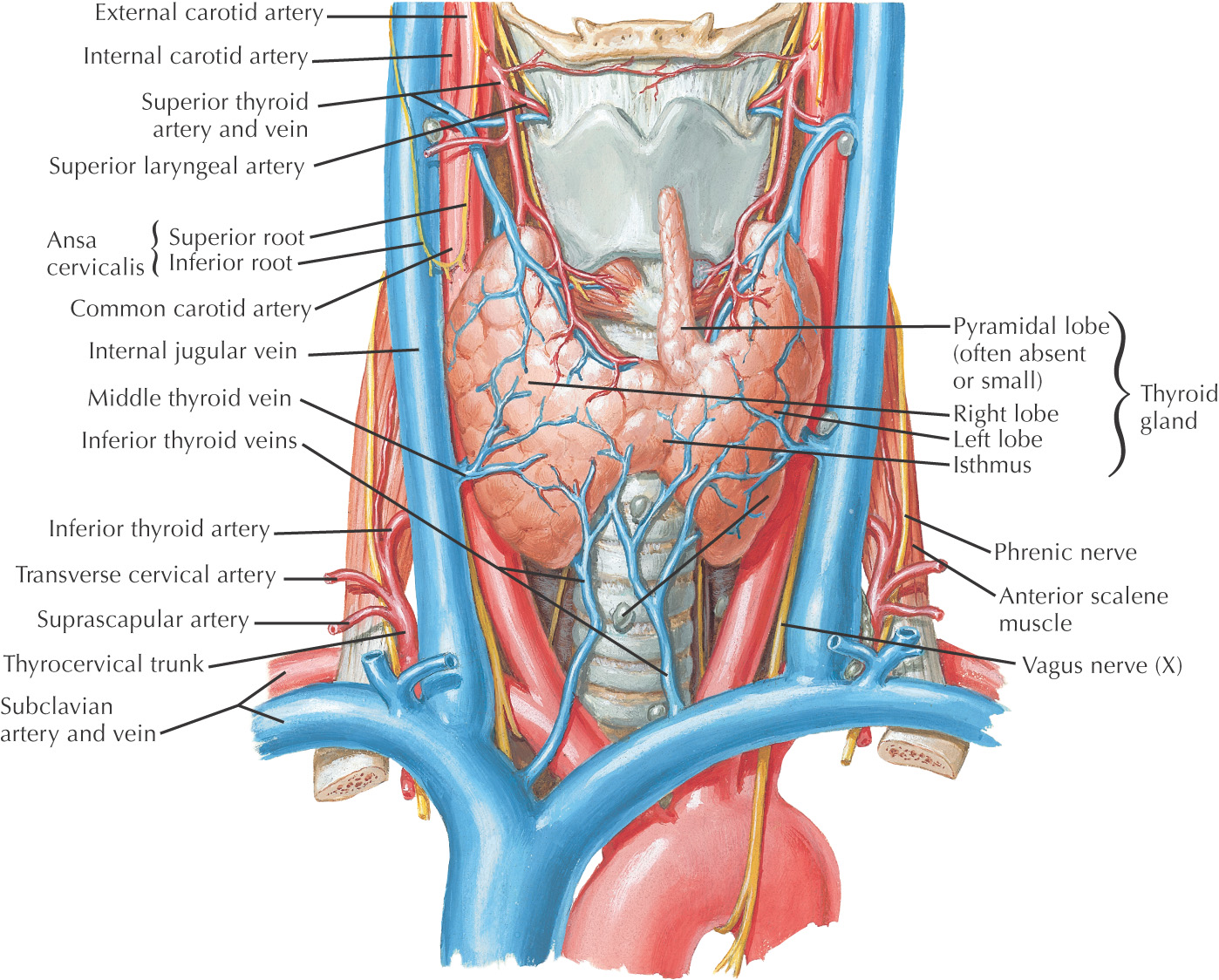
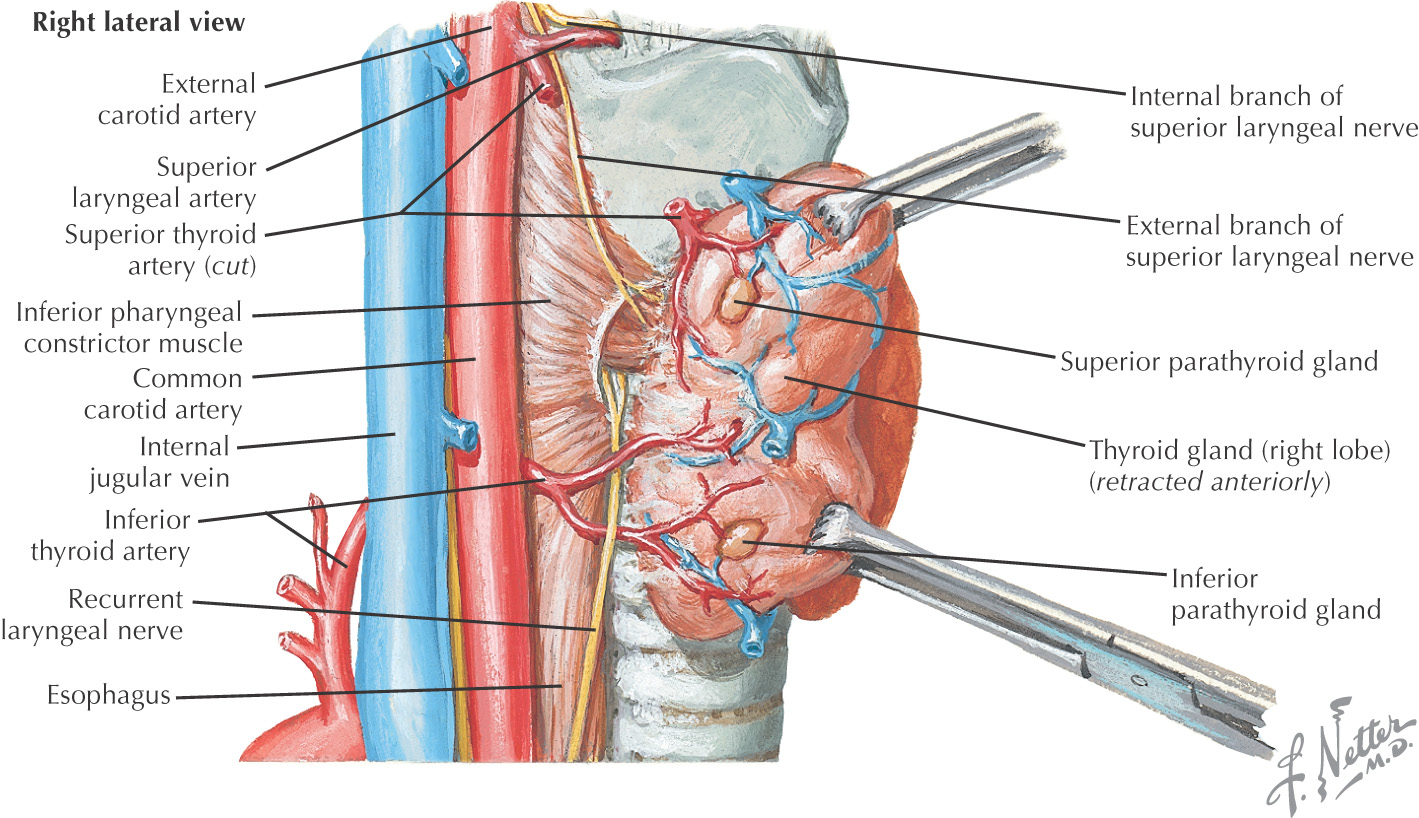
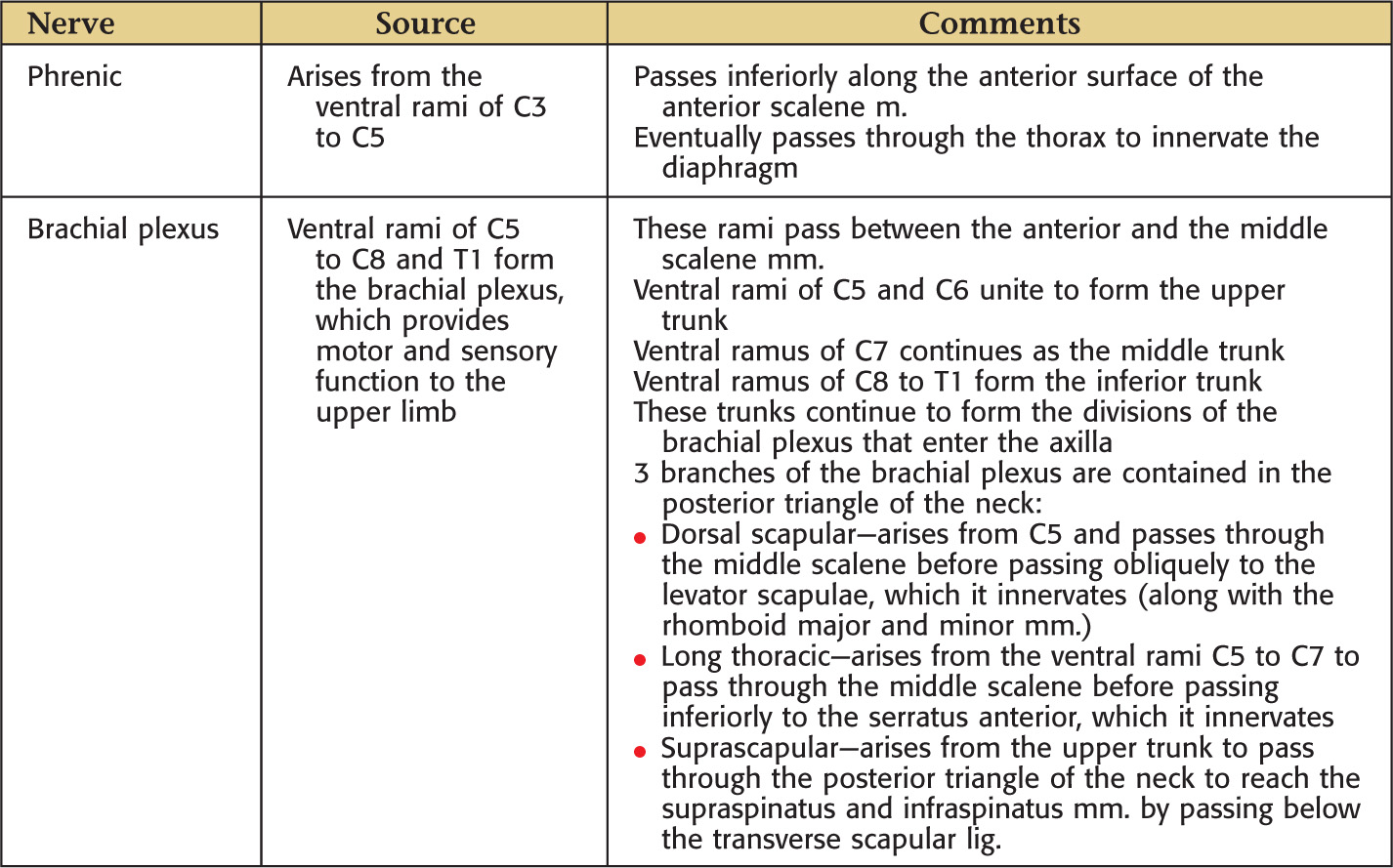
Root of the neck connects the structures of the neck with the thoracic cavity
The superior thoracic aperture is bounded by:
The apex of each lung extends into the root of the neck on the lateral side of the superior thoracic aperture
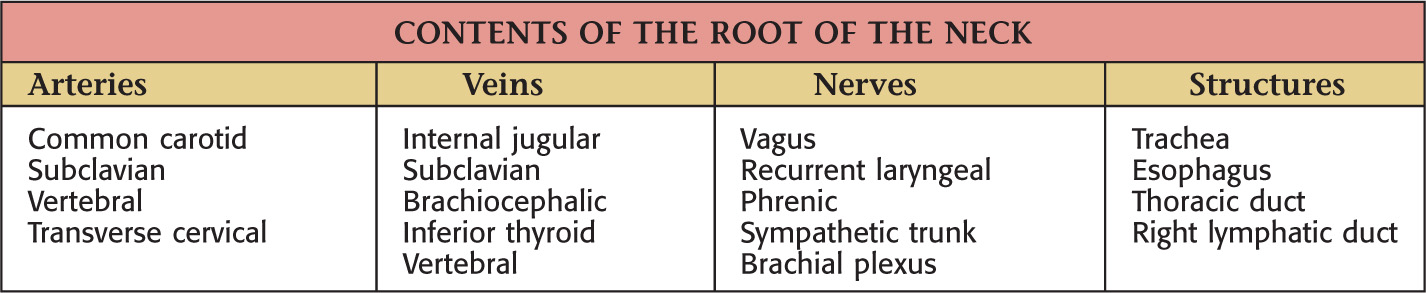
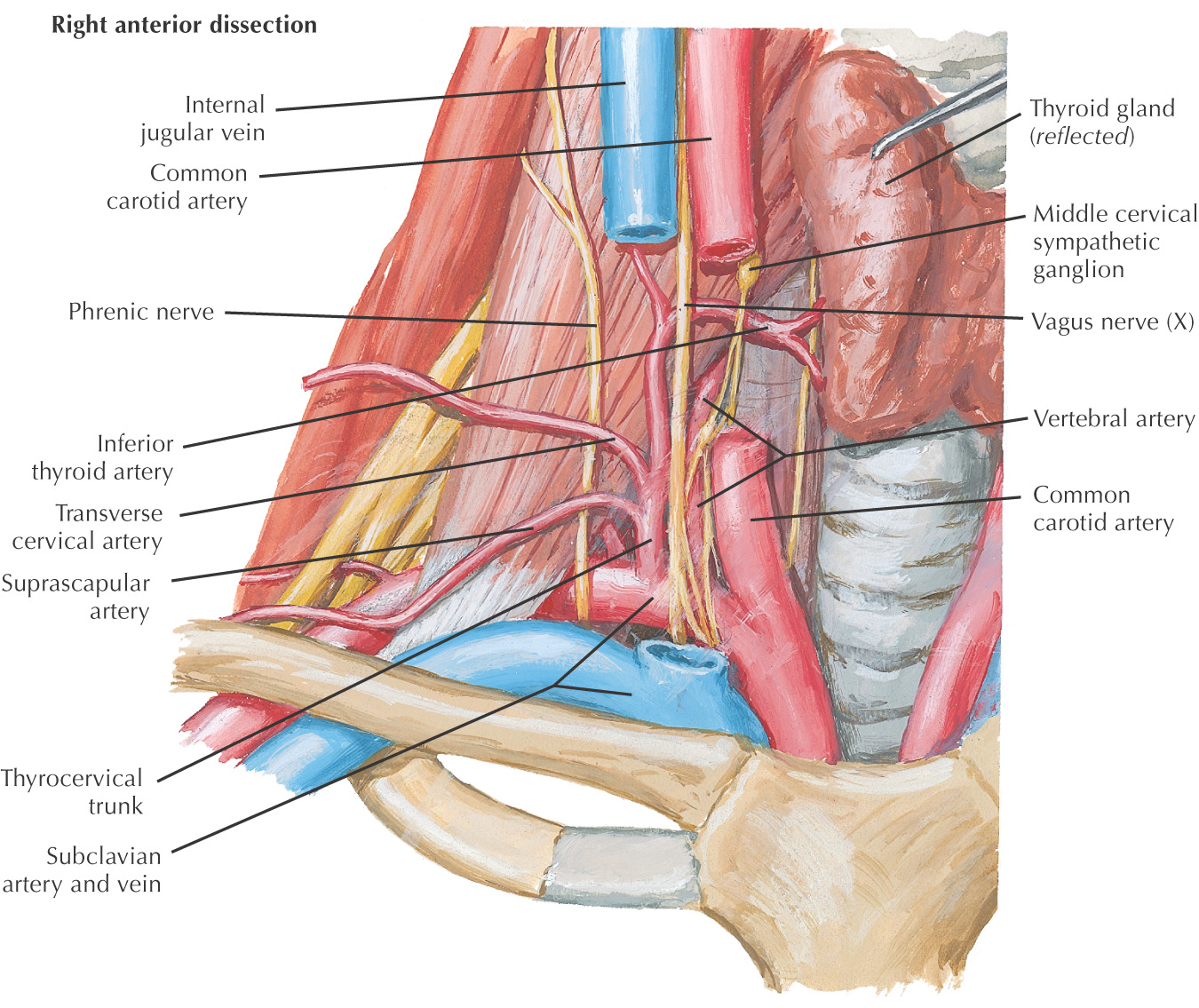
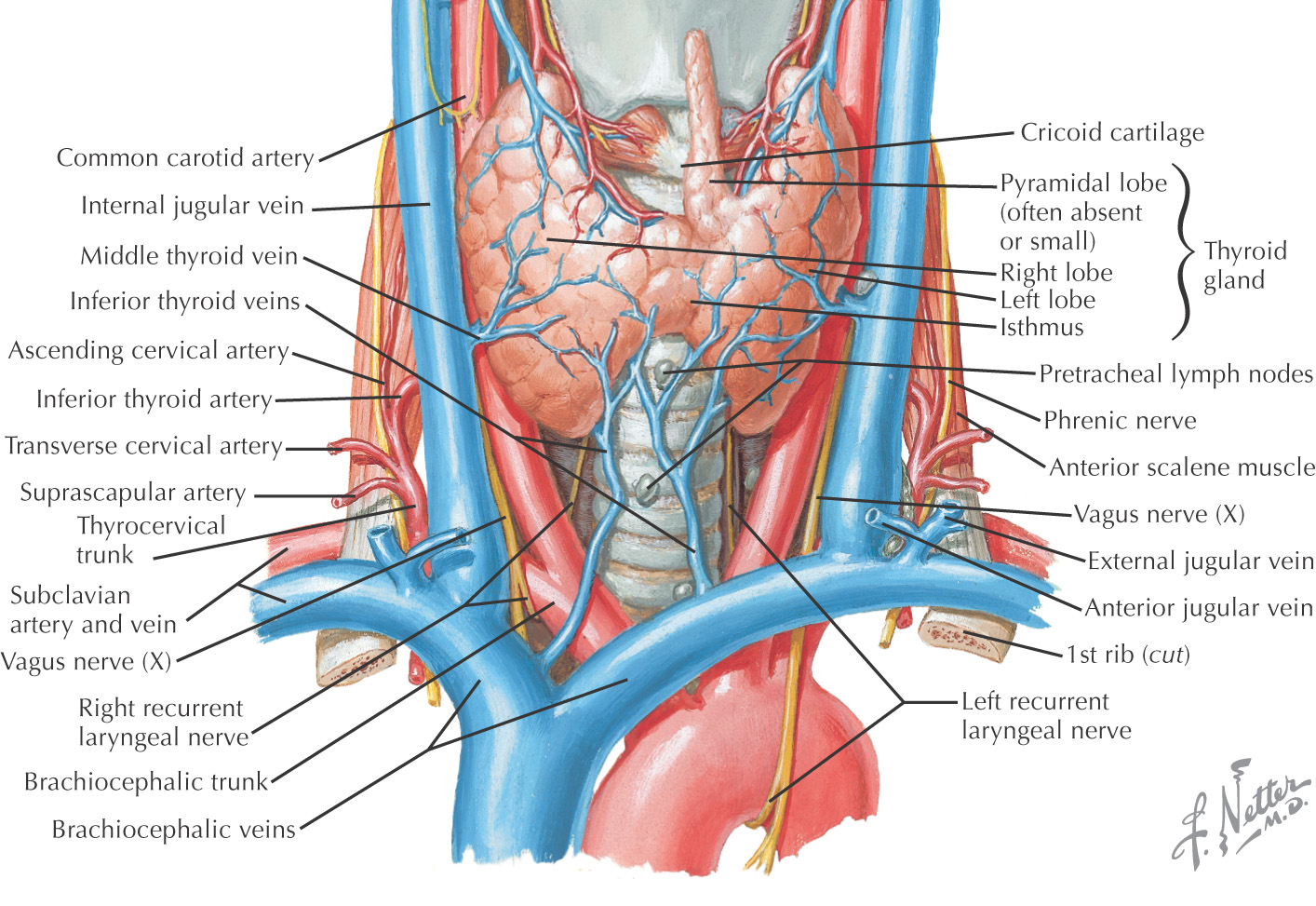
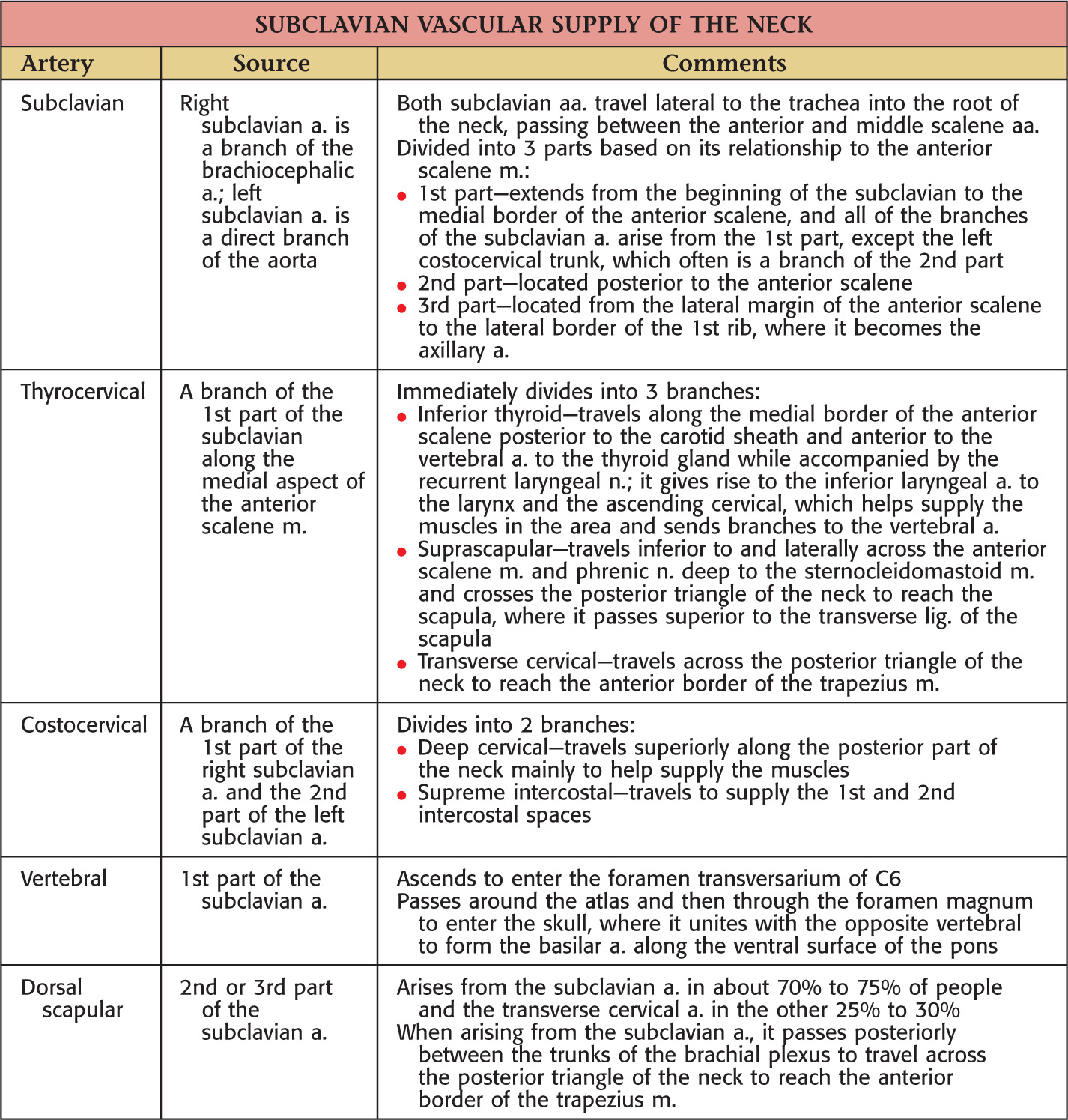
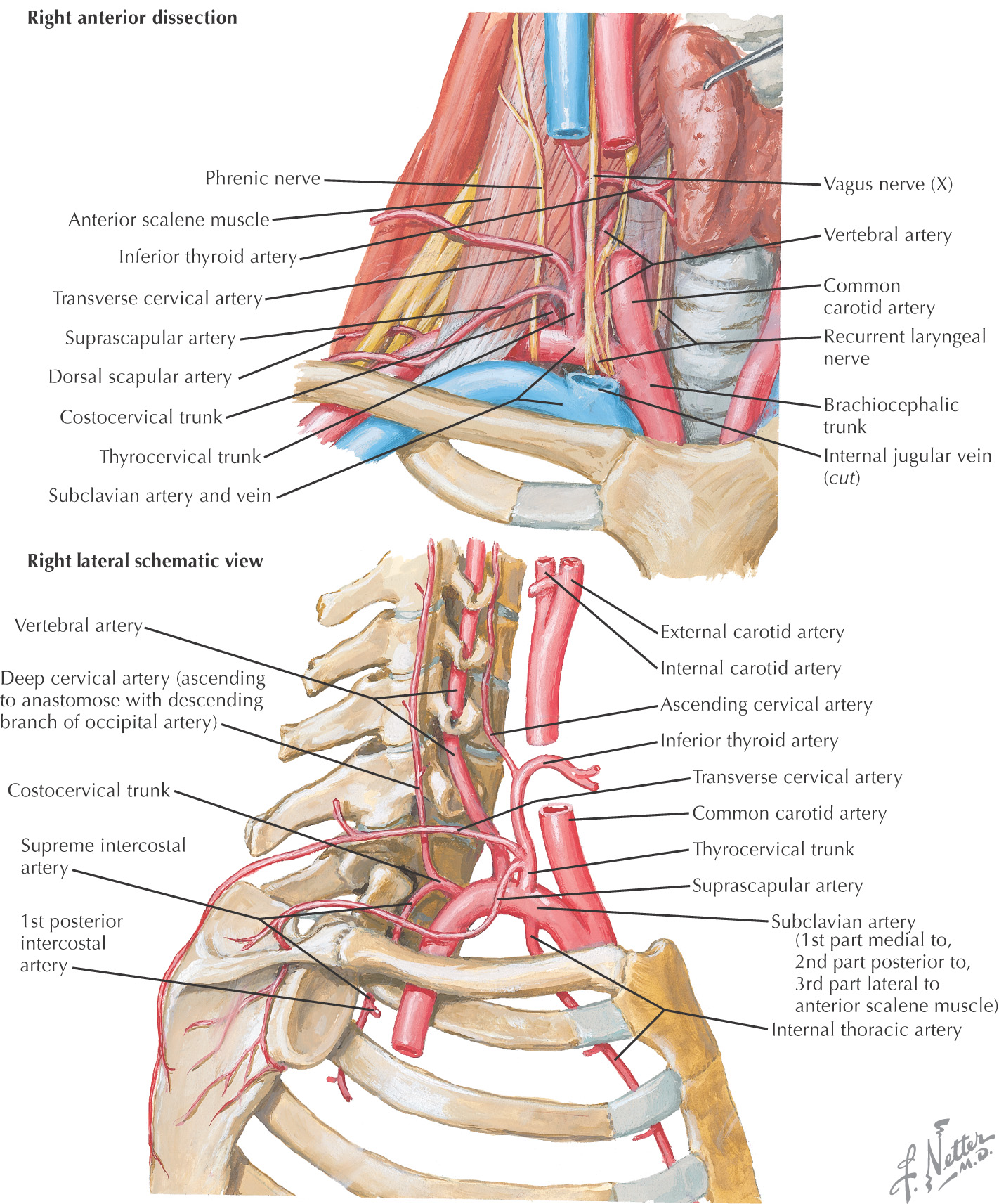
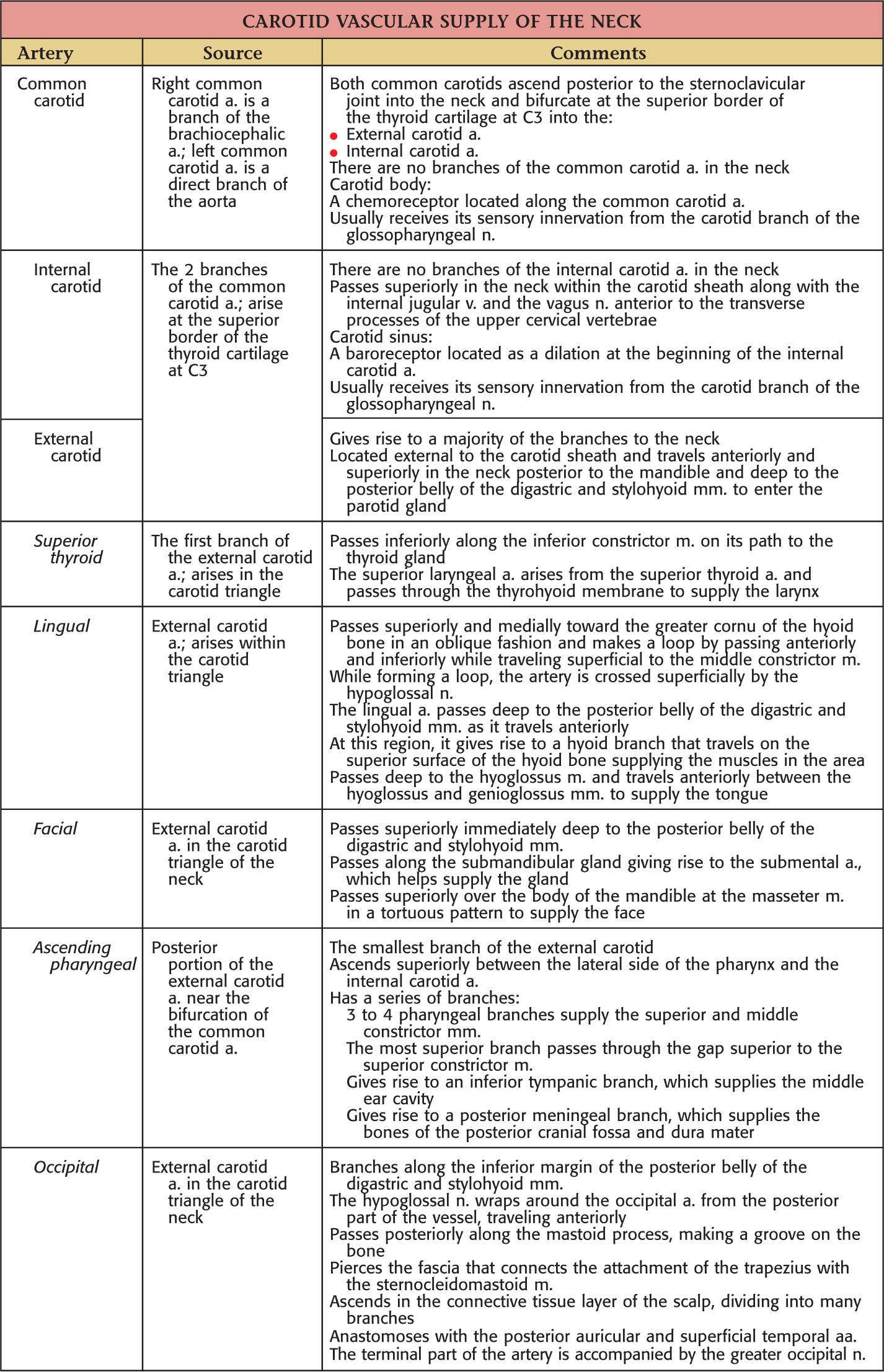
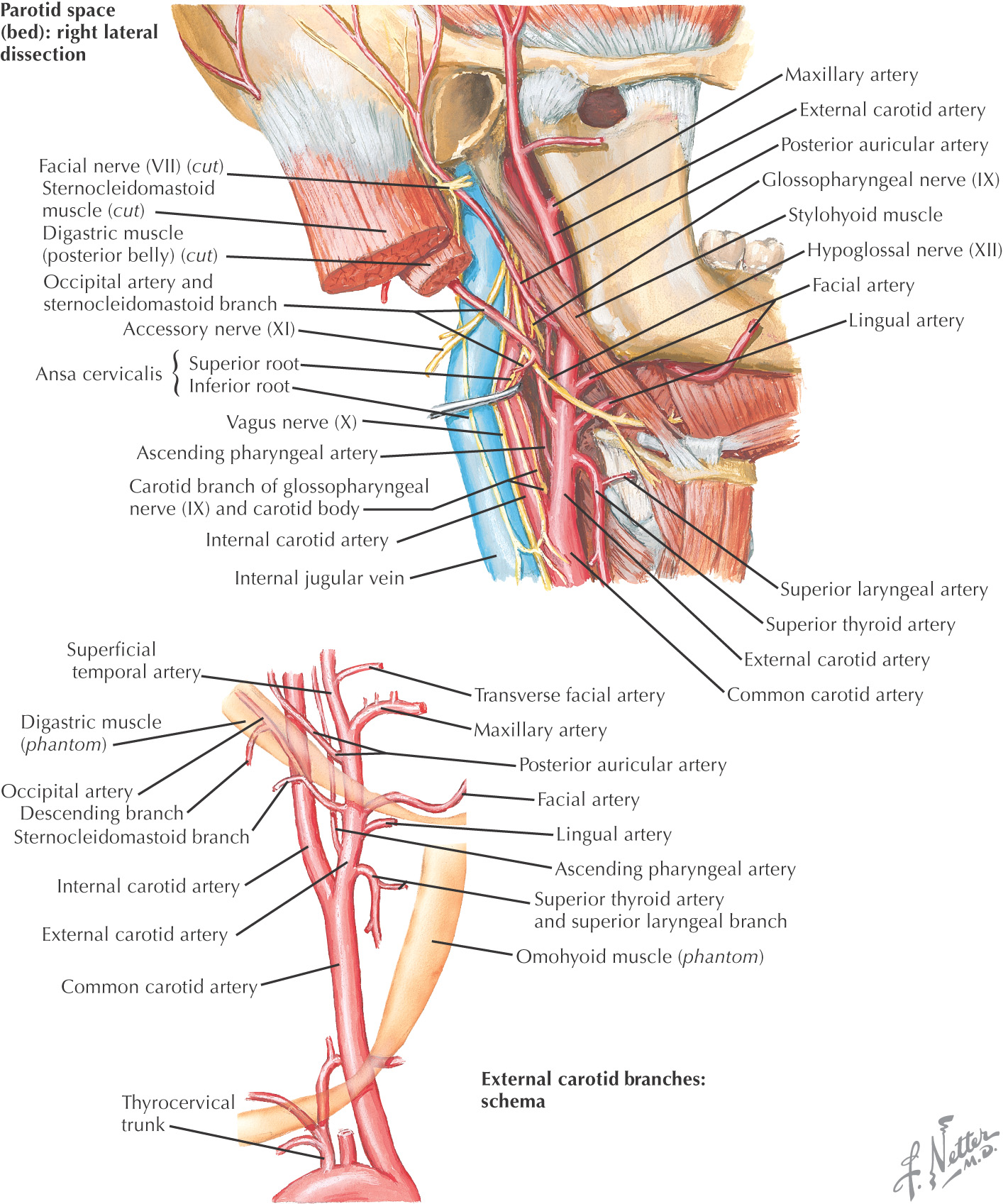
The major arteries of the neck are the common carotid and the subclavian arteries
(Internal thoracic artery is located in the thorax)
(Posterior auricular, maxillary, and superficial temporal arteries are located in the head)
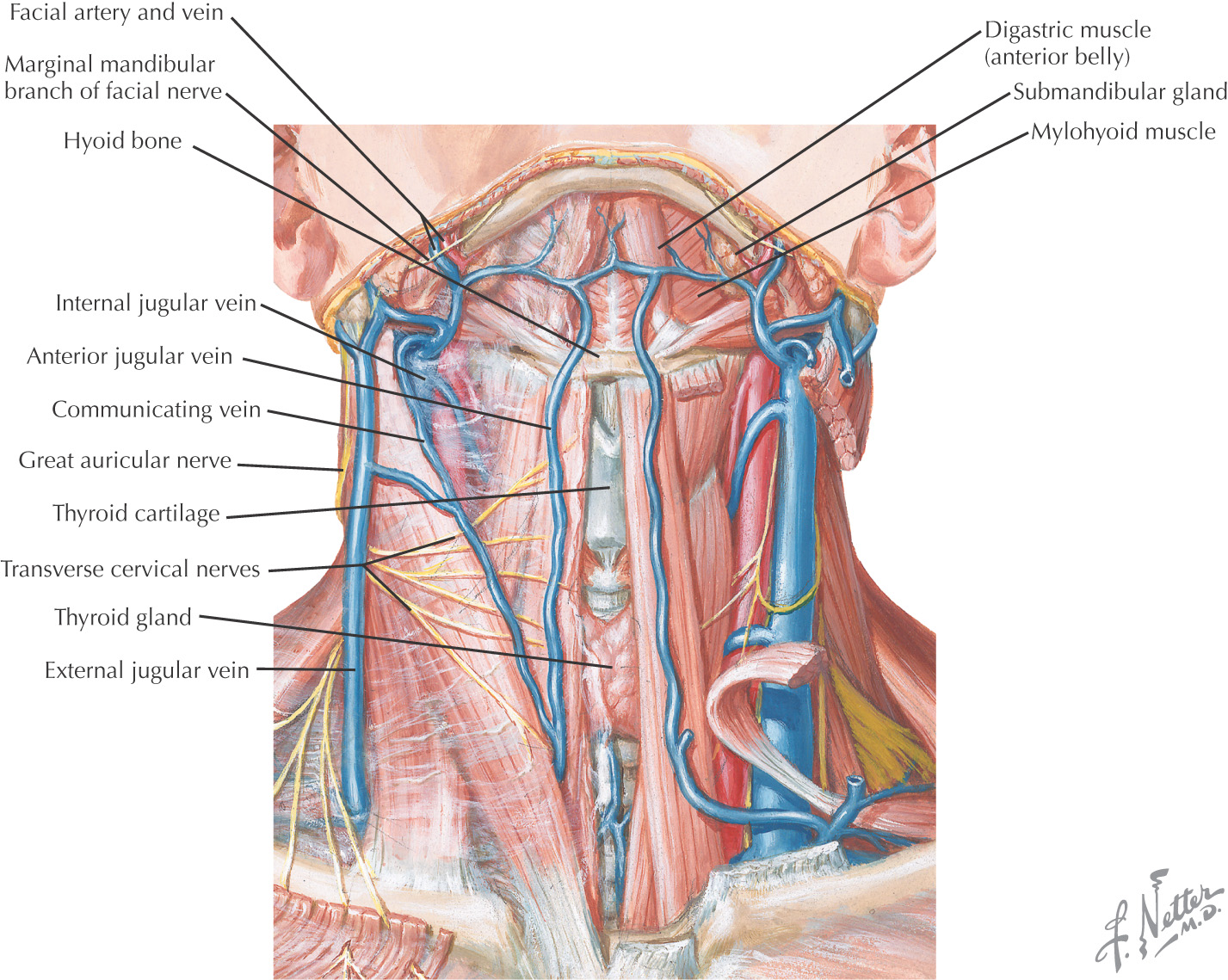
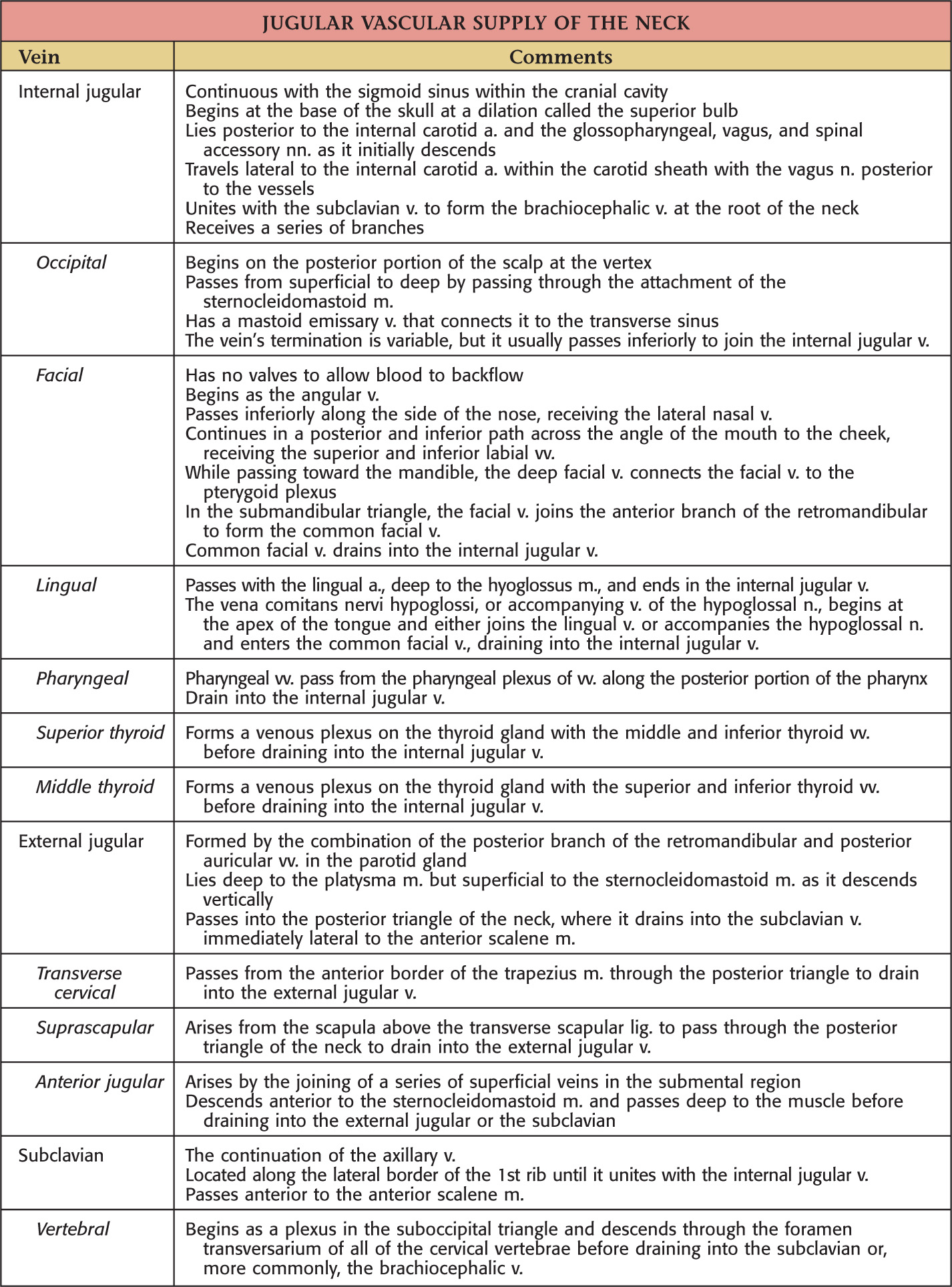
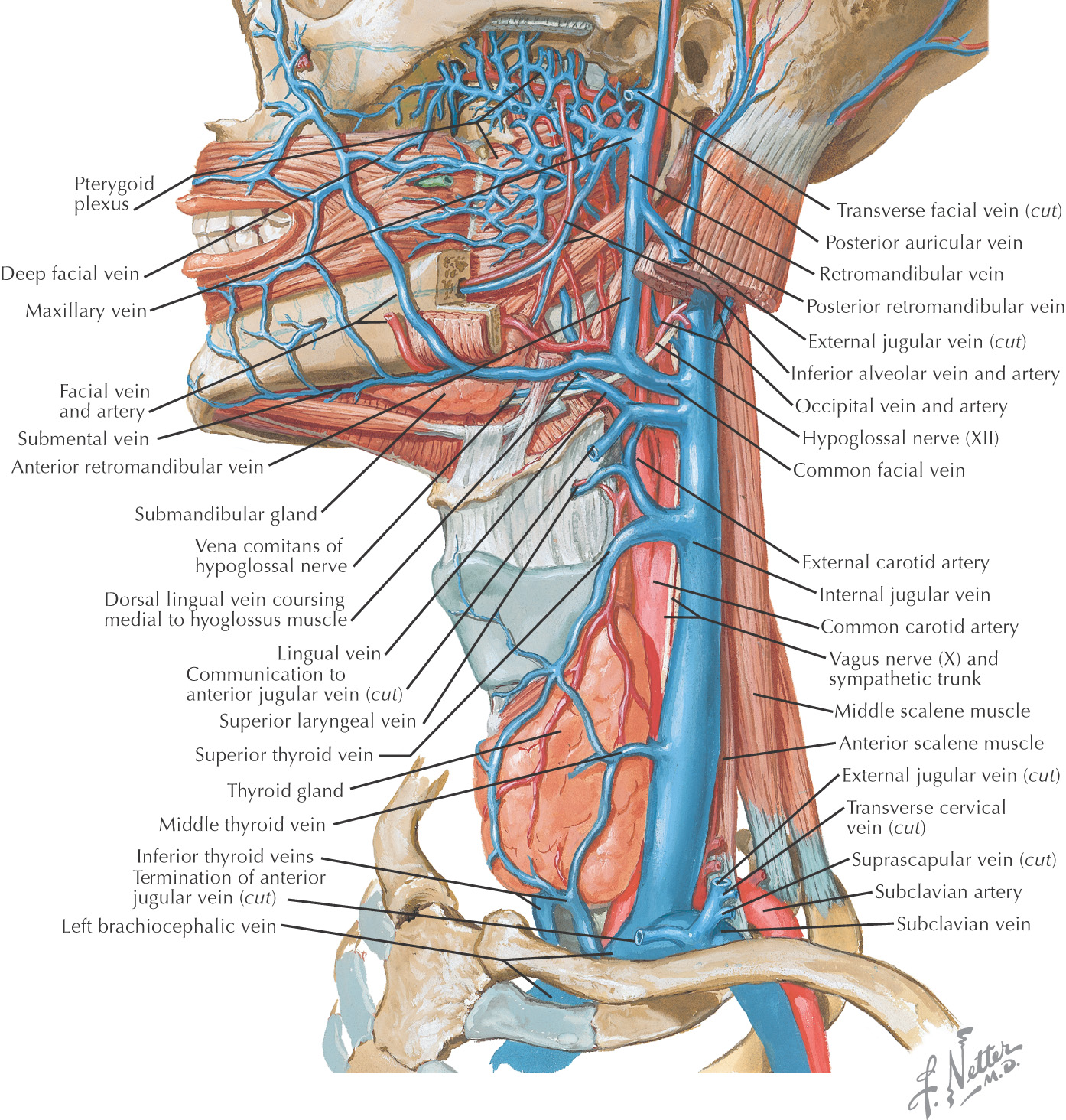
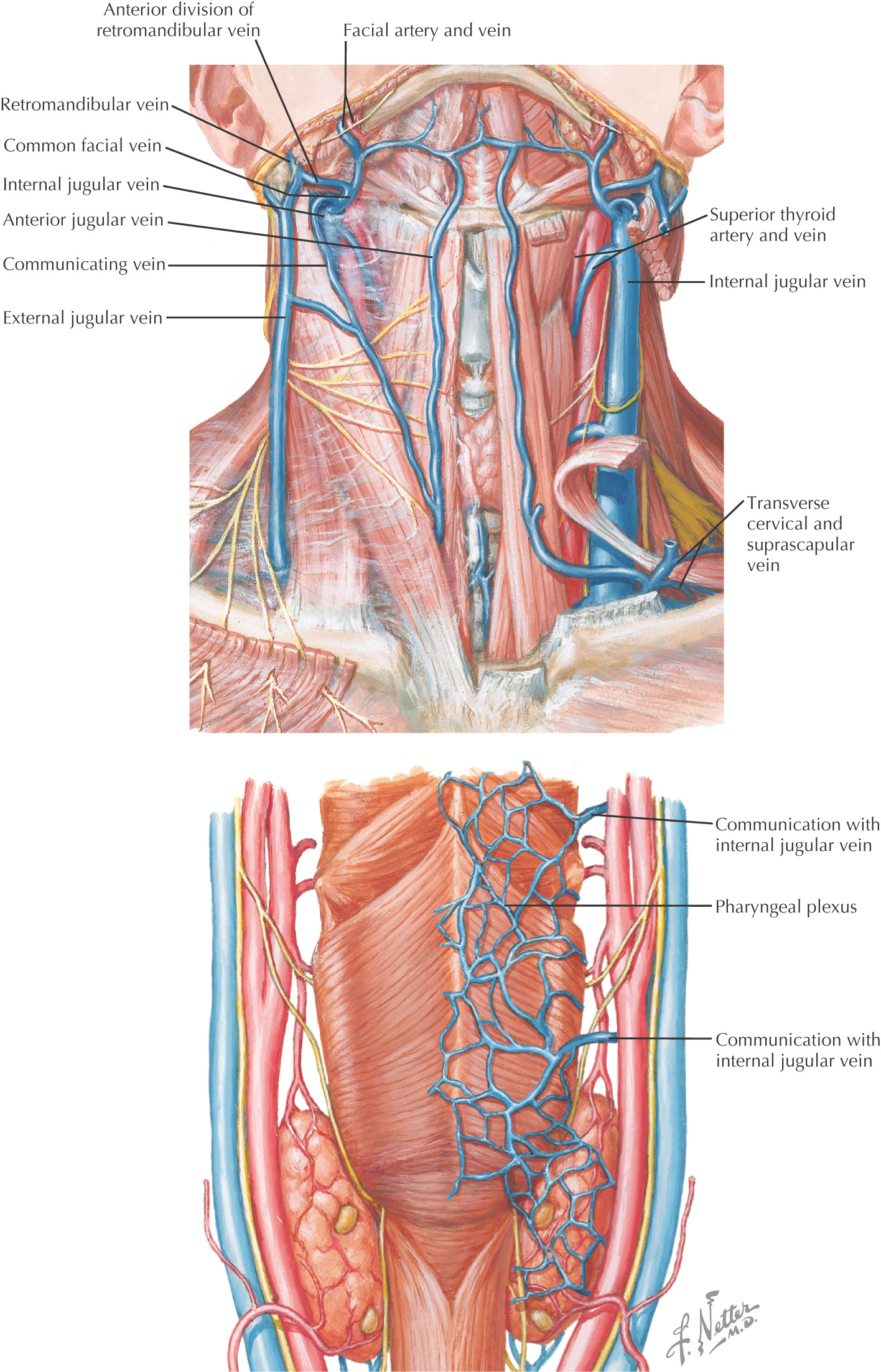
Highly variable with inconsistent drainage
Internal jugular
External jugular
Anterior jugular
Subclavian
The nerve supply to the neck is extensive; it is made up of:
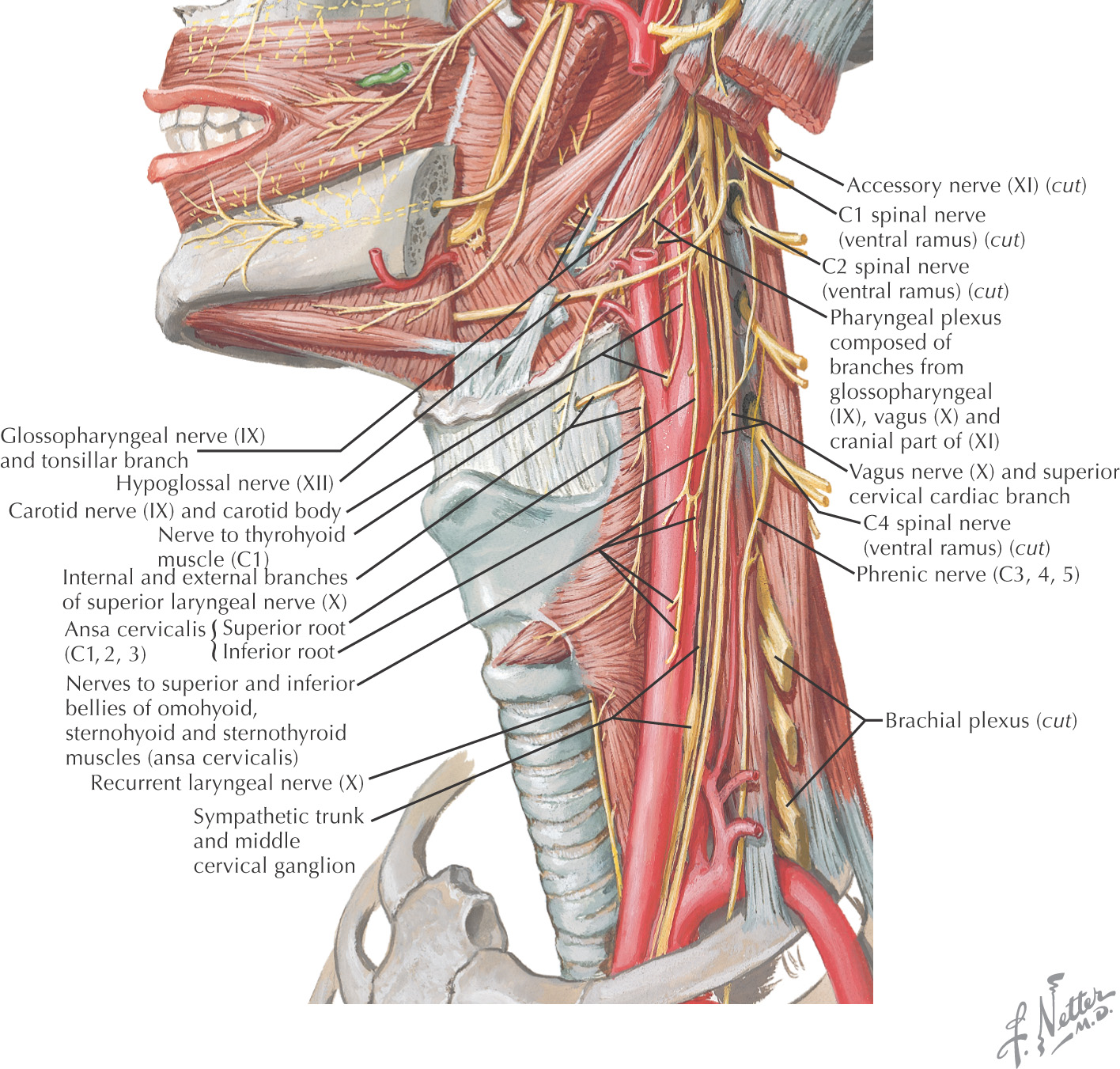
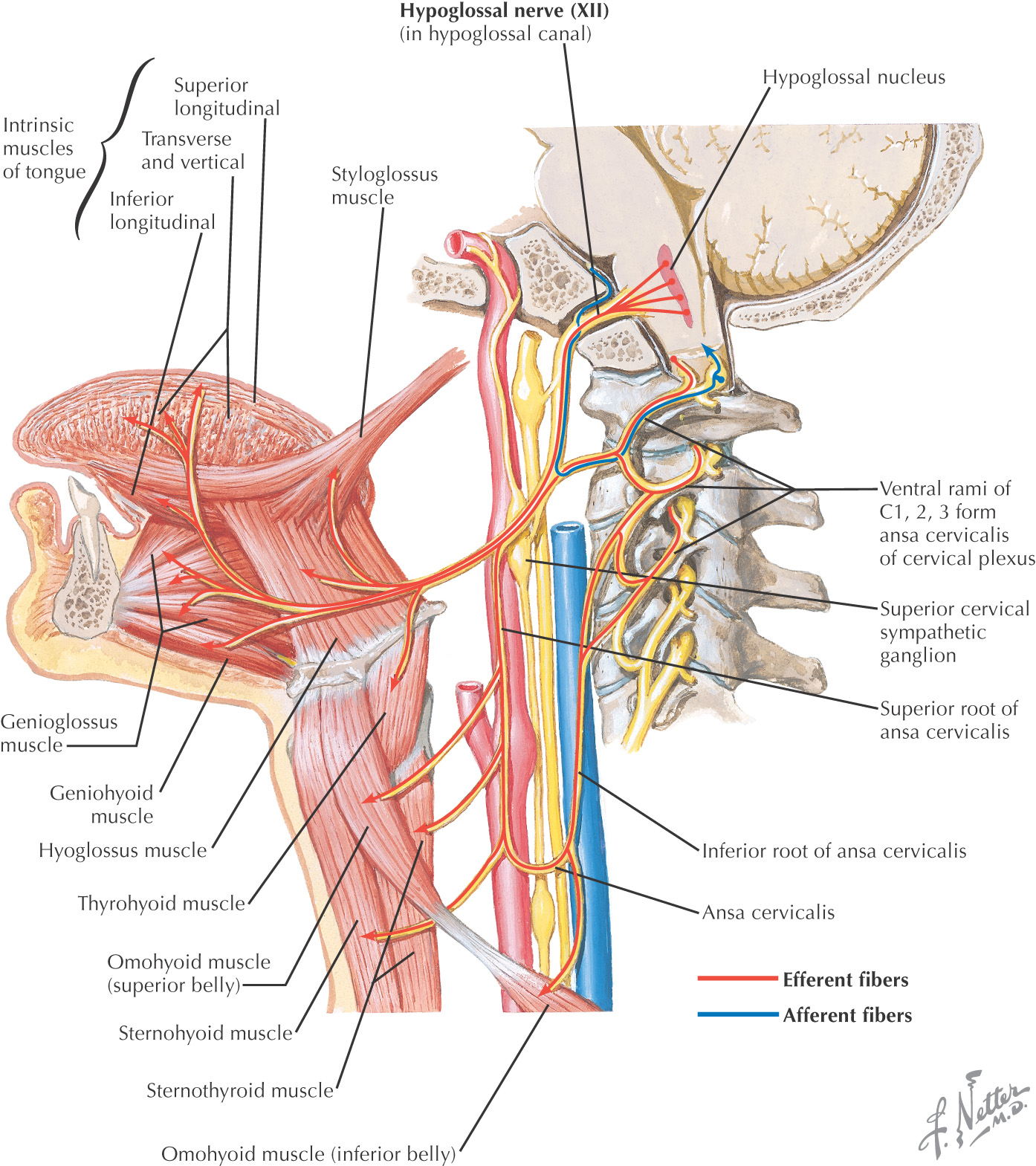
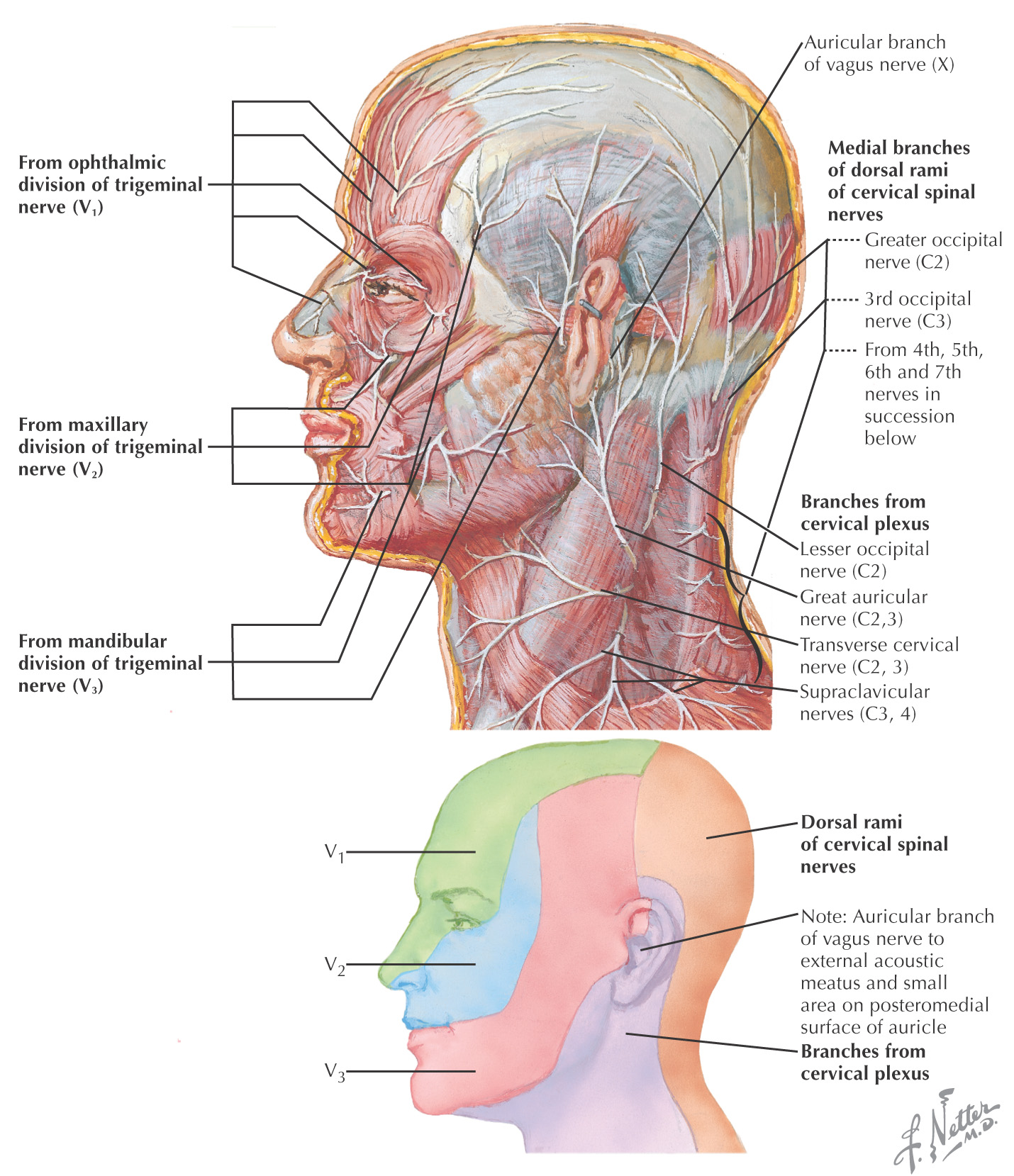
Skin of the neck receives sensory innervation from both dorsal and ventral rami
Dorsal ramus of C1 lacks sensory fibers and does not contribute to the sensory distribution to the neck
Dorsal rami of C6 to C8 lack sensory fibers and do not contribute to the sensory distribution to the neck
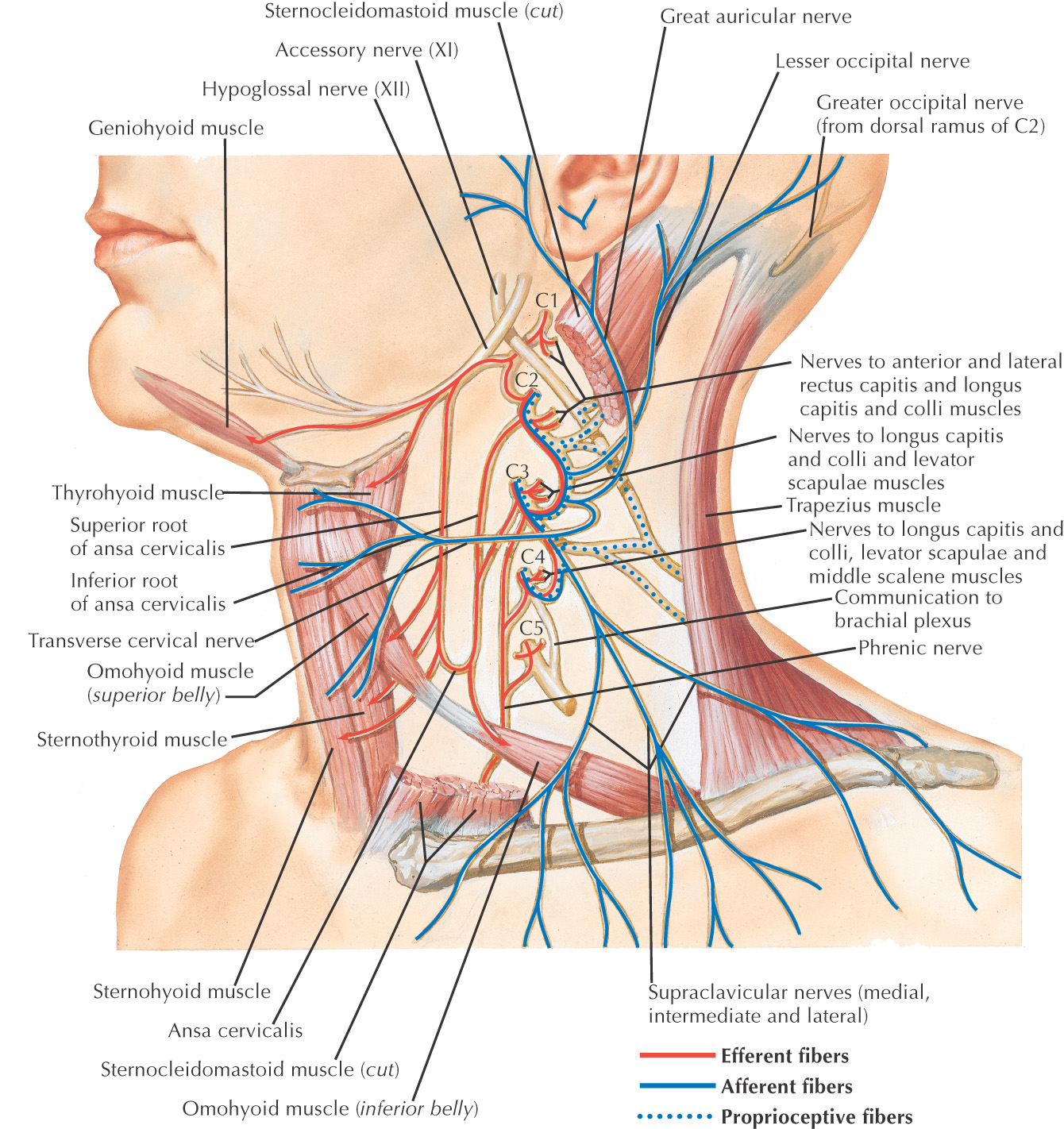
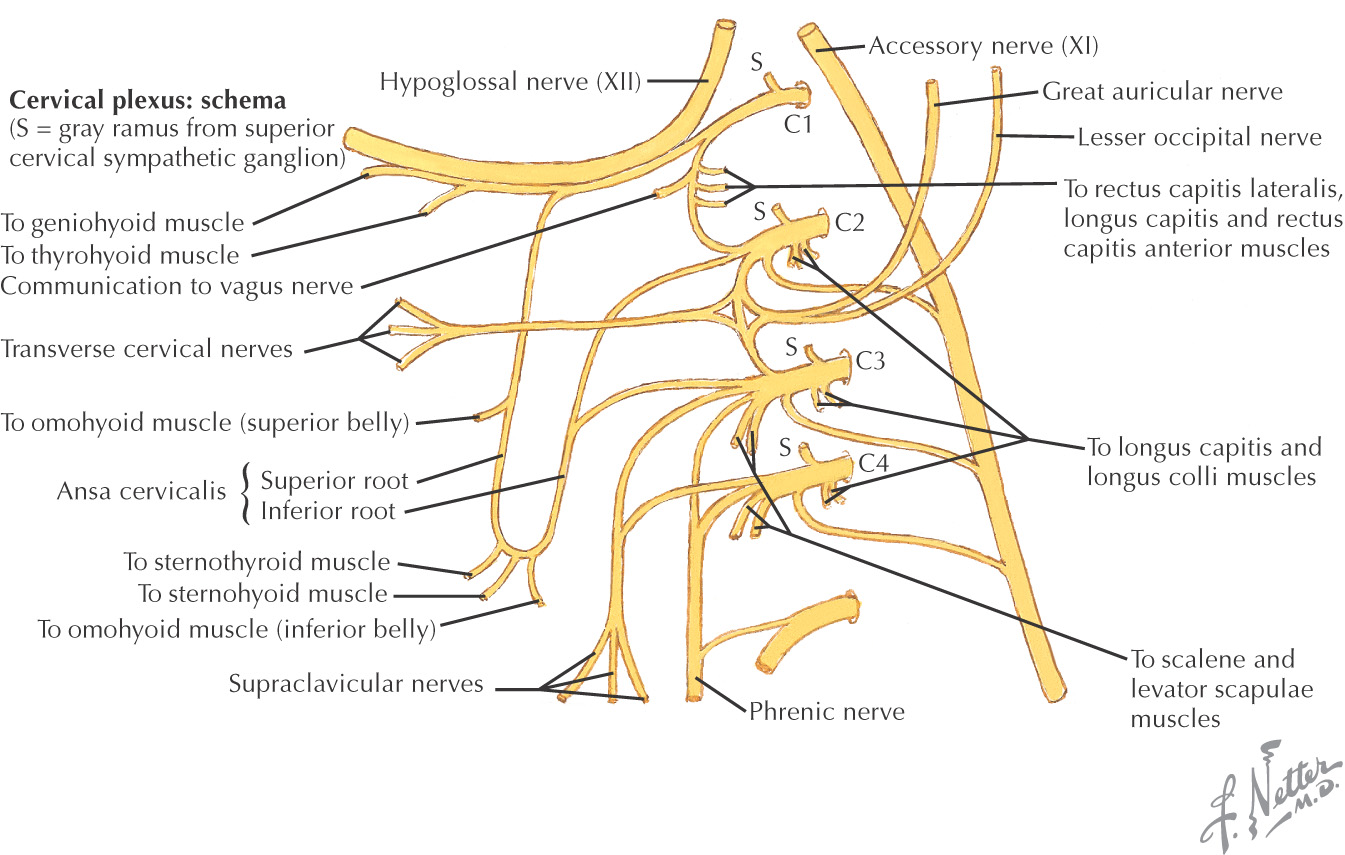
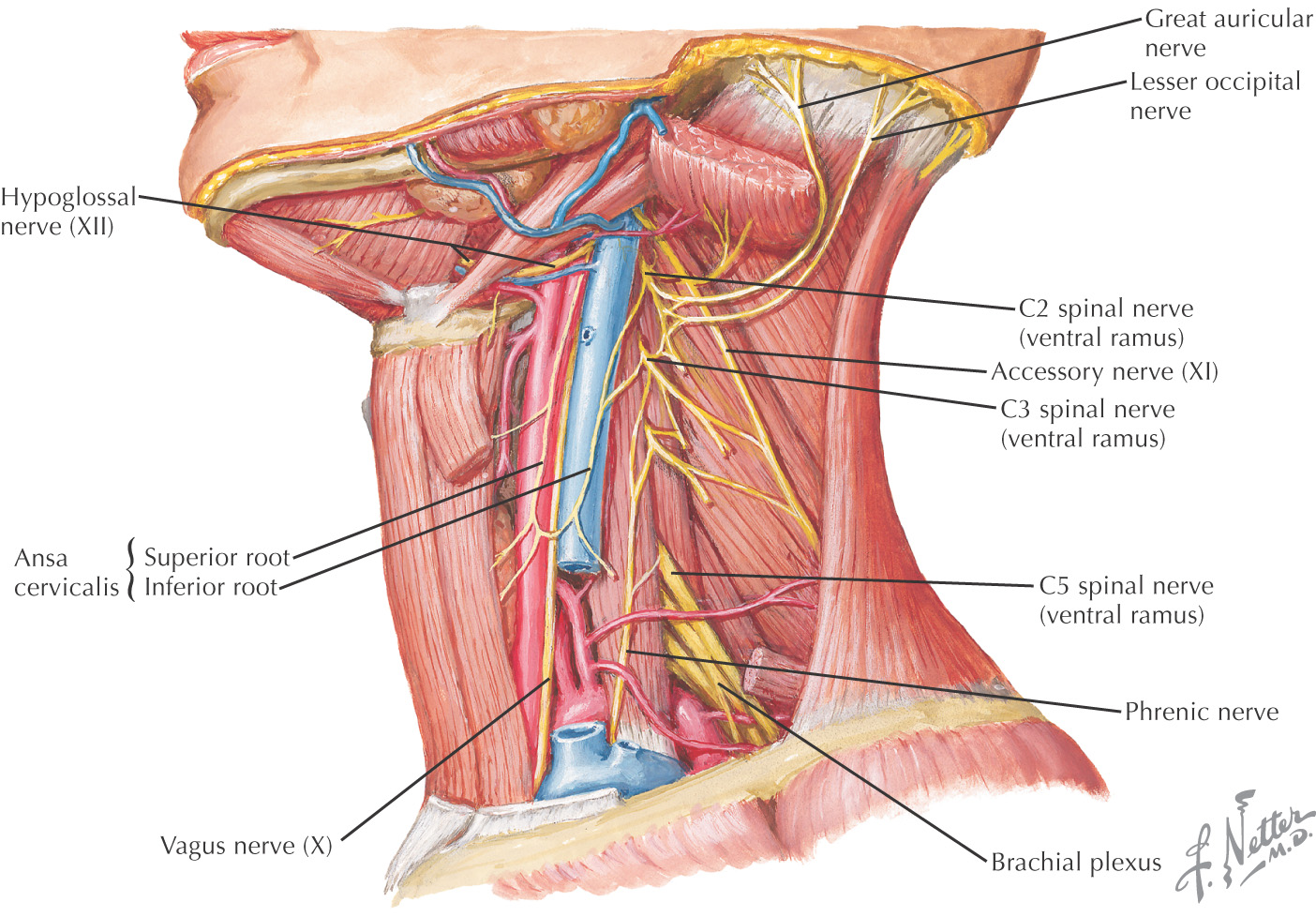
Ventral rami provide most of the sensory innervation to the neck through the sensory branches of the cervical plexus
Formed by C1 to C4 ventral rami
Originates deep to the sternocleidomastoid
Sensory branches pass along the posterior border of the muscle at Erb’s point to travel to their destinations
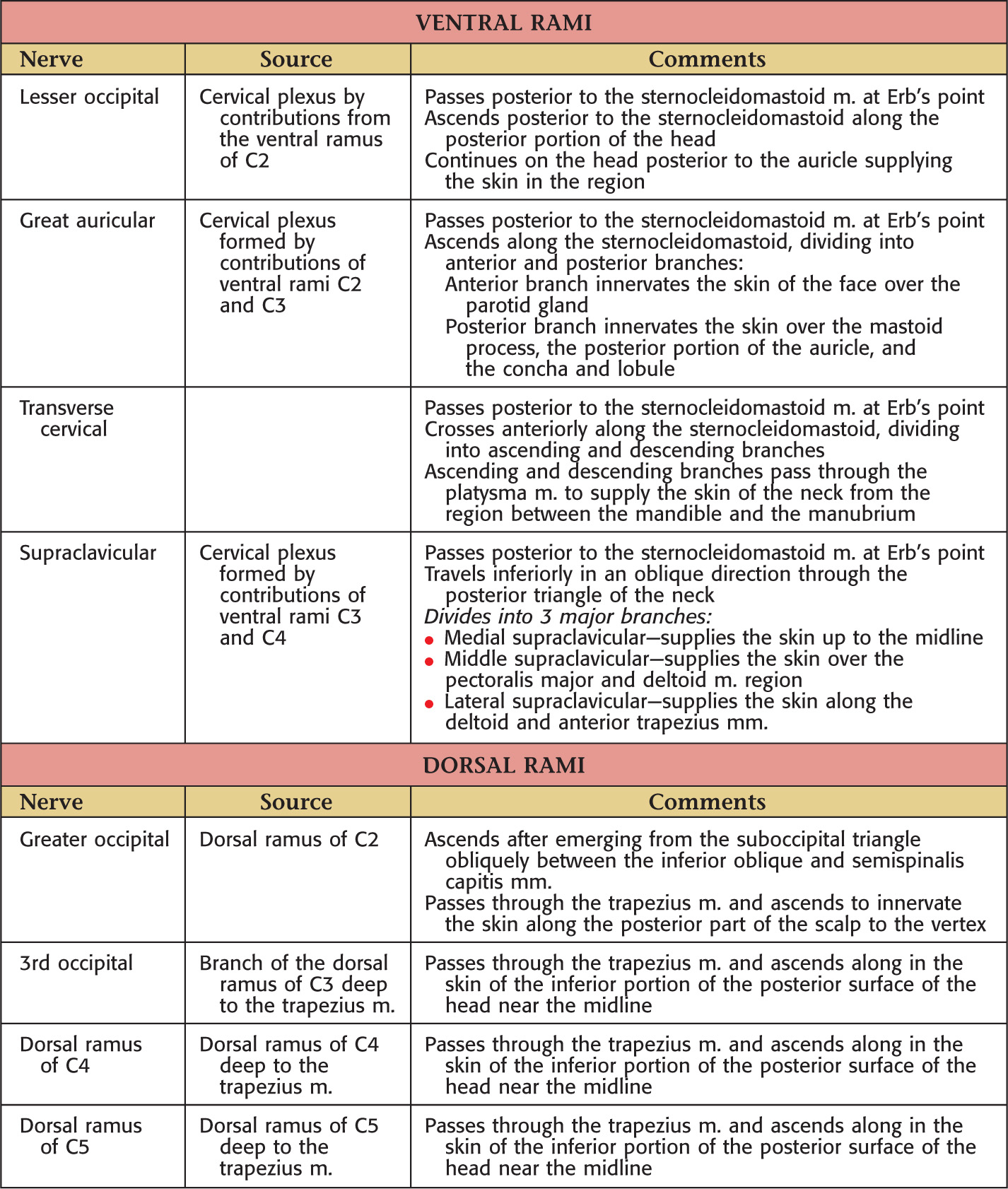
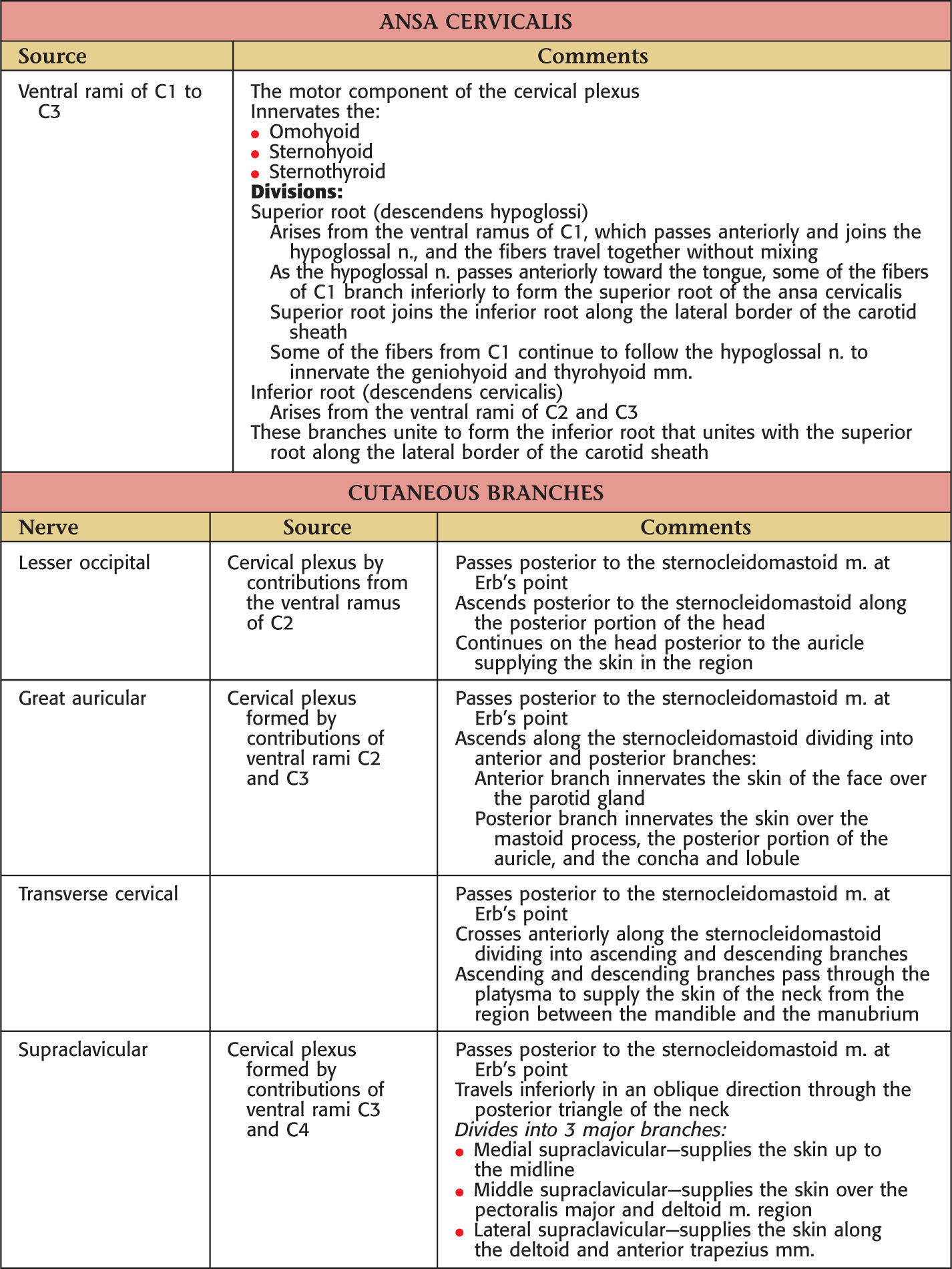
Arises from the ventral rami of C1 to C4
Divided into 2 parts:
• Ansa cervicalis (motor component)
• Cutaneous branches (sensory component):
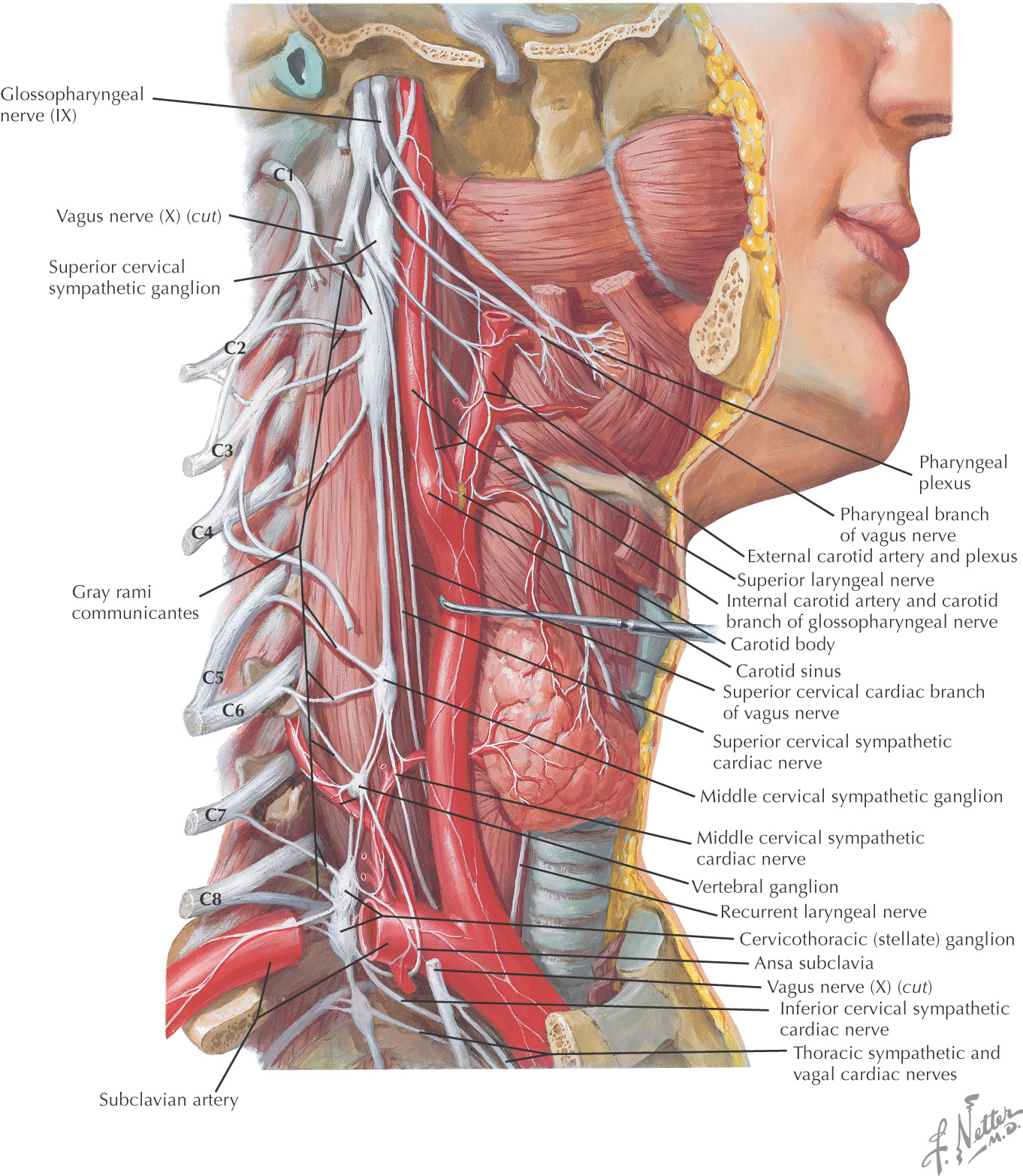
Sympathetic trunk extends into the neck from the thorax
In the neck, the sympathetic trunk typically has 3 ganglia:
• Superior cervical ganglion—located at the base of the skull
• Middle cervical ganglion—located at C6
• Inferior cervical ganglion—located immediately posterior to the vertebral artery near the vessel’s origin
Often the inferior cervical ganglion unites with the 1st thoracic ganglion to create the stellate ganglion
Sympathetics for the head and neck arise in the intermediolateral horn column of the spinal cord from T1 to T4
These preganglionic fibers ascend through the sympathetic trunk to reach the cervical ganglia and synapse with the postganglionic neurons
Postganglionic neurons follow either of 2 paths:
• May travel to the spinal nerves via the gray ramus
• May follow the arterial supply to the effector organs of the head
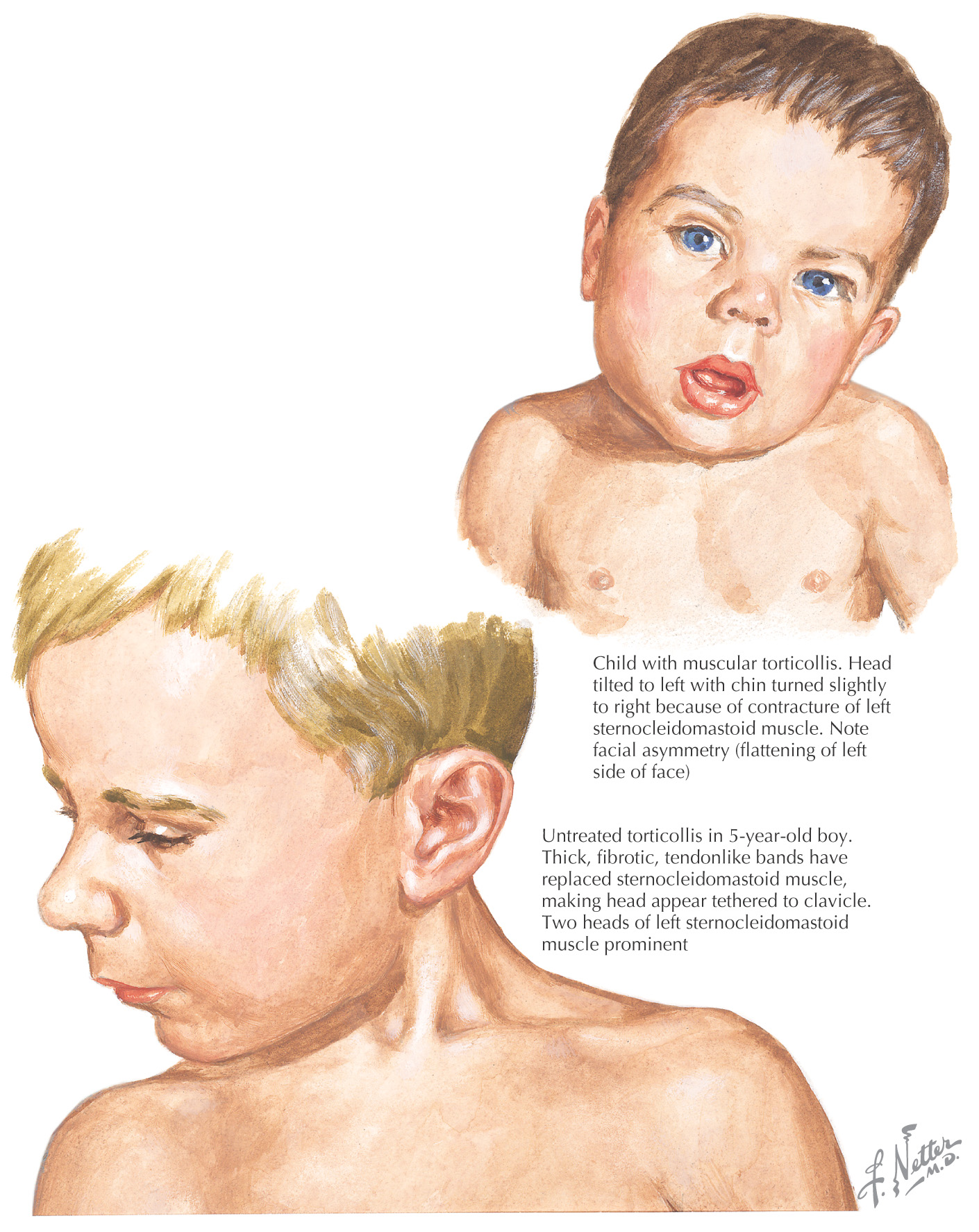
Torticollis, also known as „wryneck,” is a disorder in which the muscles of the neck are flexed, extended, or twisted in an abnormal position
The sternocleidomastoid is the most commonly affected muscle
The neck typically twists to one side, leading to abnormal movements and postures of the head
In congenital muscular torticollis, the bent neck is caused by a tight sternocleidomastoid on one side of the body
Early treatment is important in preventing permanent deformities
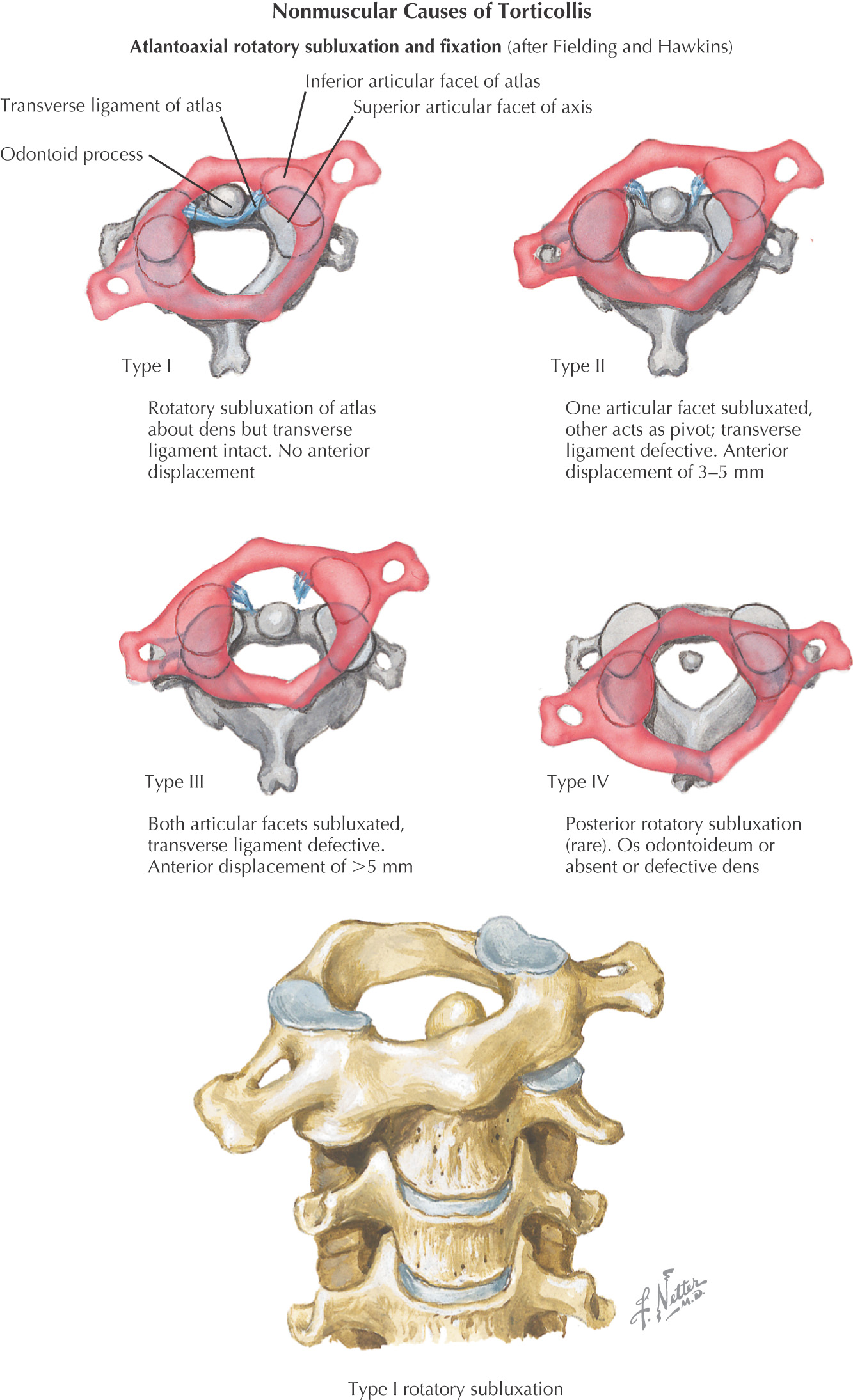
Certain drugs, such as neuroleptic agents, can cause dystonia, a condition in which involuntary muscle contraction occurs in the neck, back, and trunk
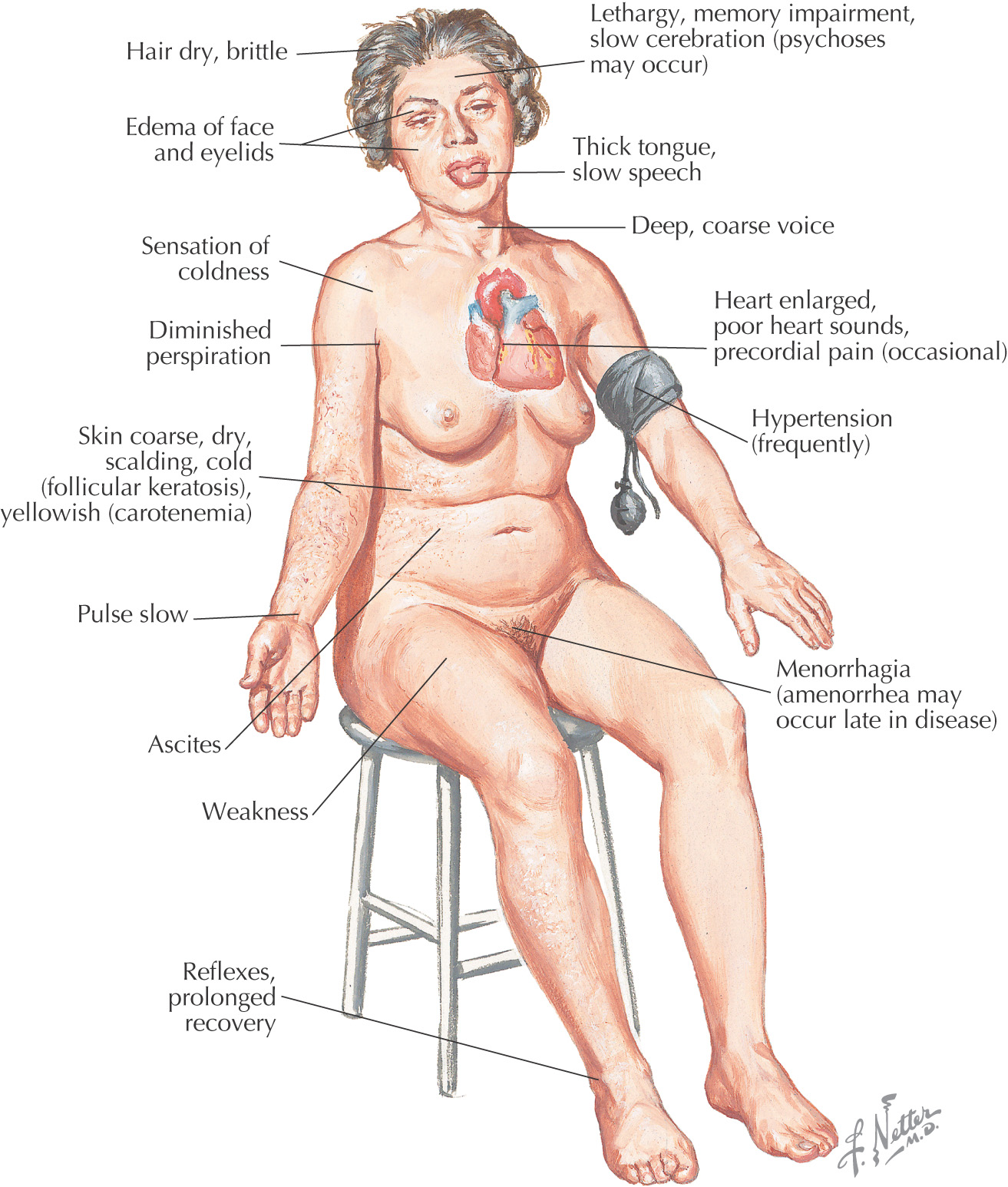
Hypothyroidism: a condition in which the thyroid gland does not produce enough thyroid hormones
The pituitary gland regulates the thyroid’s normal production of the hormones thyroxine and triiodothyronine
The lack of hormones leads to an overall slowing of mental and physical activities
Congenital hypothyroidism is known as cretinism
• Hashimoto’s thyroiditis–immune system of the body attacks the gland
• Surgical removal of the gland
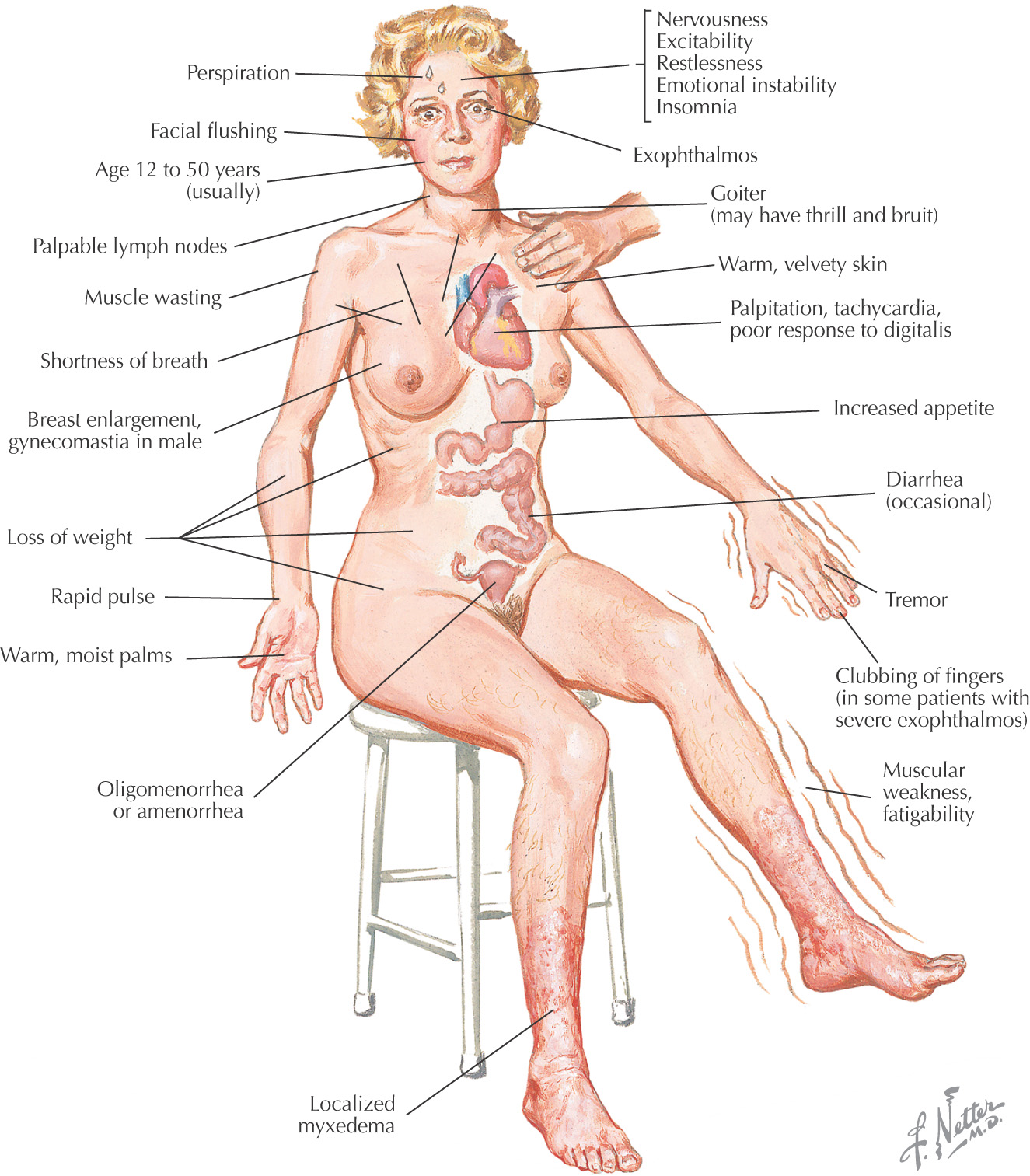
Hyperthyroidism: a condition characterized by hypermetabolism and elevated levels of thyroid hormones
Can lead to thyrotoxicosis, a toxic condition caused by excess thyroid hormones regardless of the cause
• Graves’ disease—most common cause (in greater than 80% of all cases of hyperthyroidism), in which the body produces antibodies that stimulate the thyroid to synthesize excess thyroid hormones
• Benign growths of the thyroid or pituitary gland
• Ingestion of excess thyroid hormones or iodine
• Radioactive iodine—but too much can lead to hypothyroidism
*These muscles are covered by the prevertebral layer of deep cervical fascia.