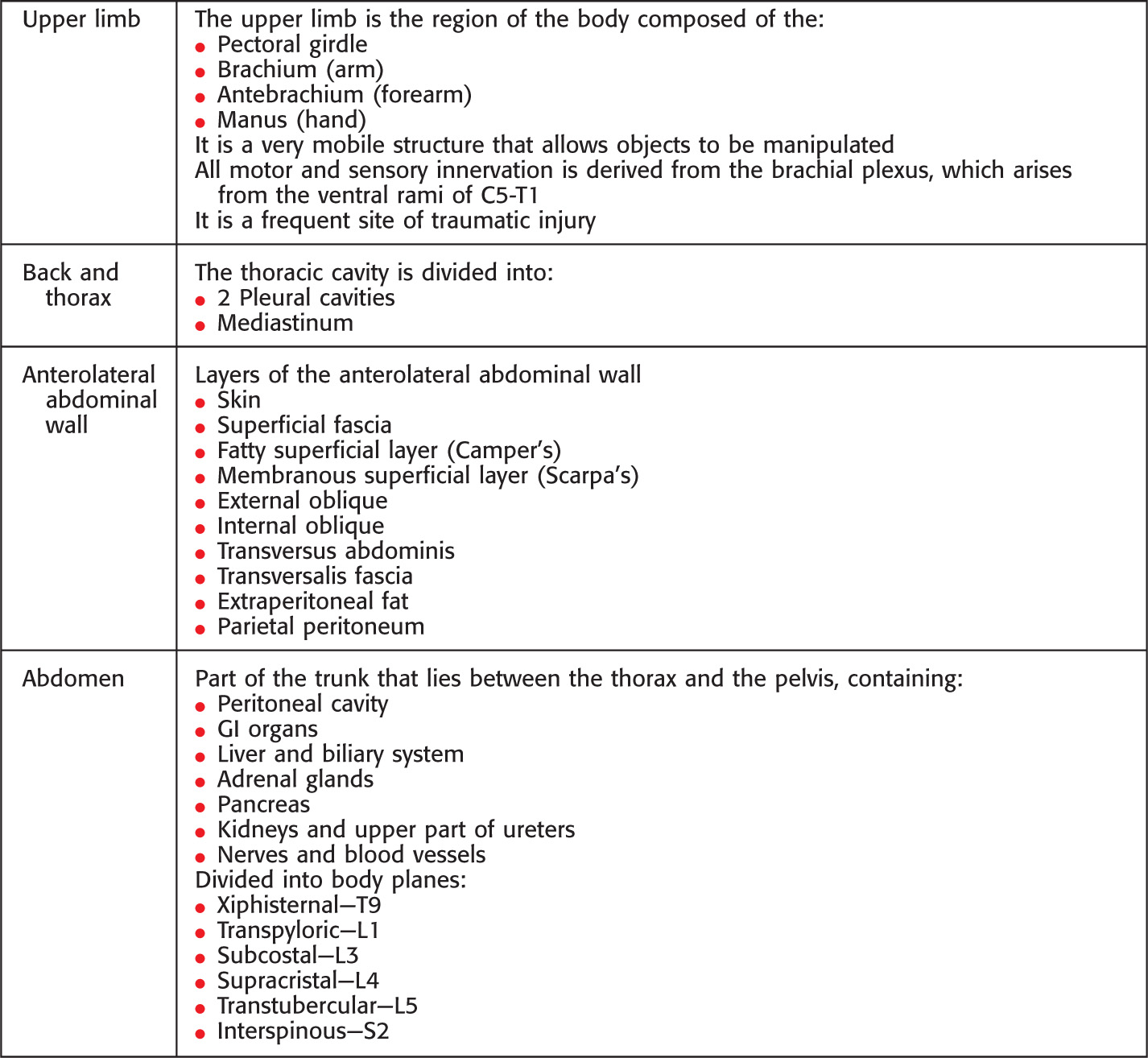
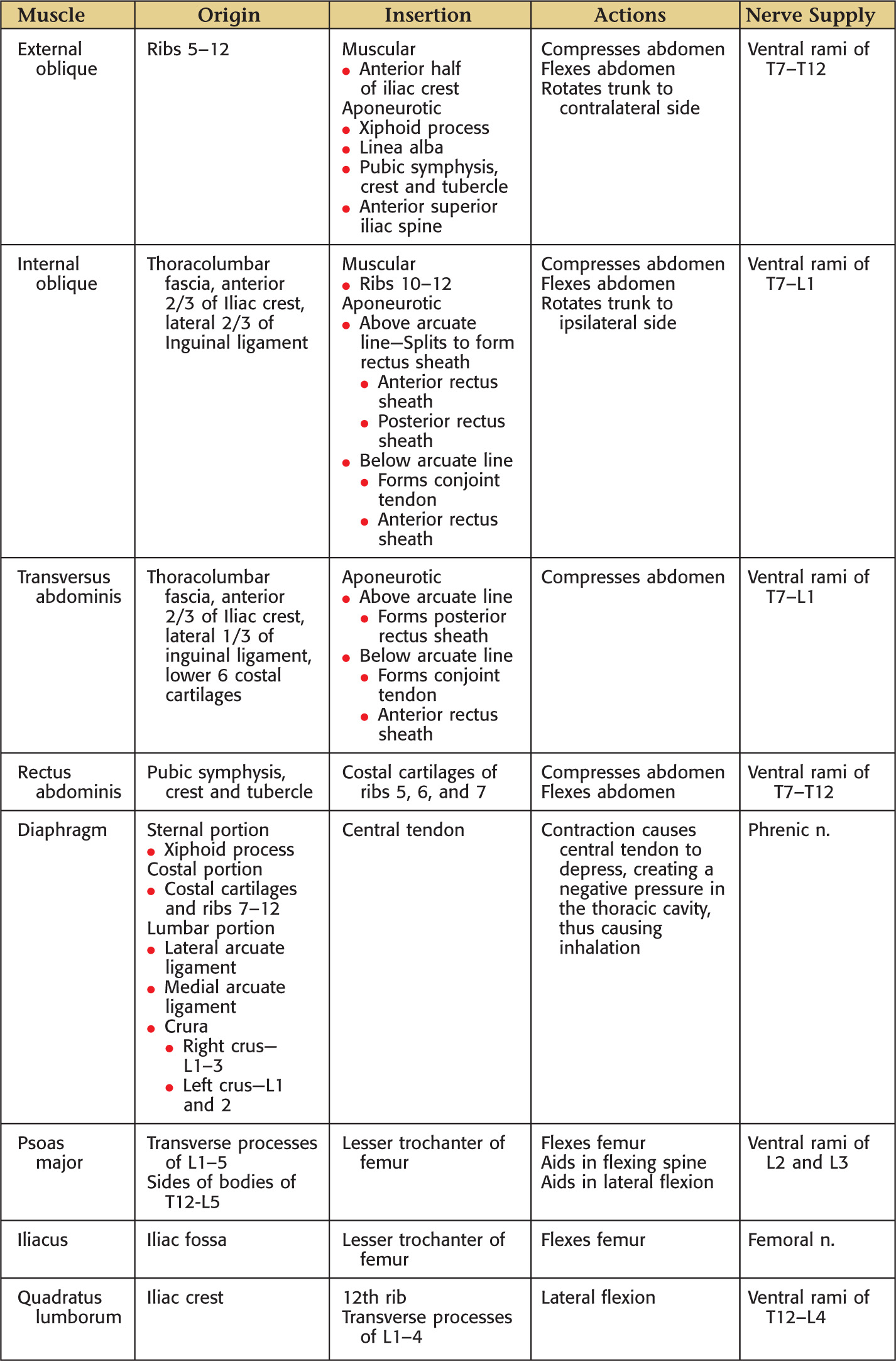
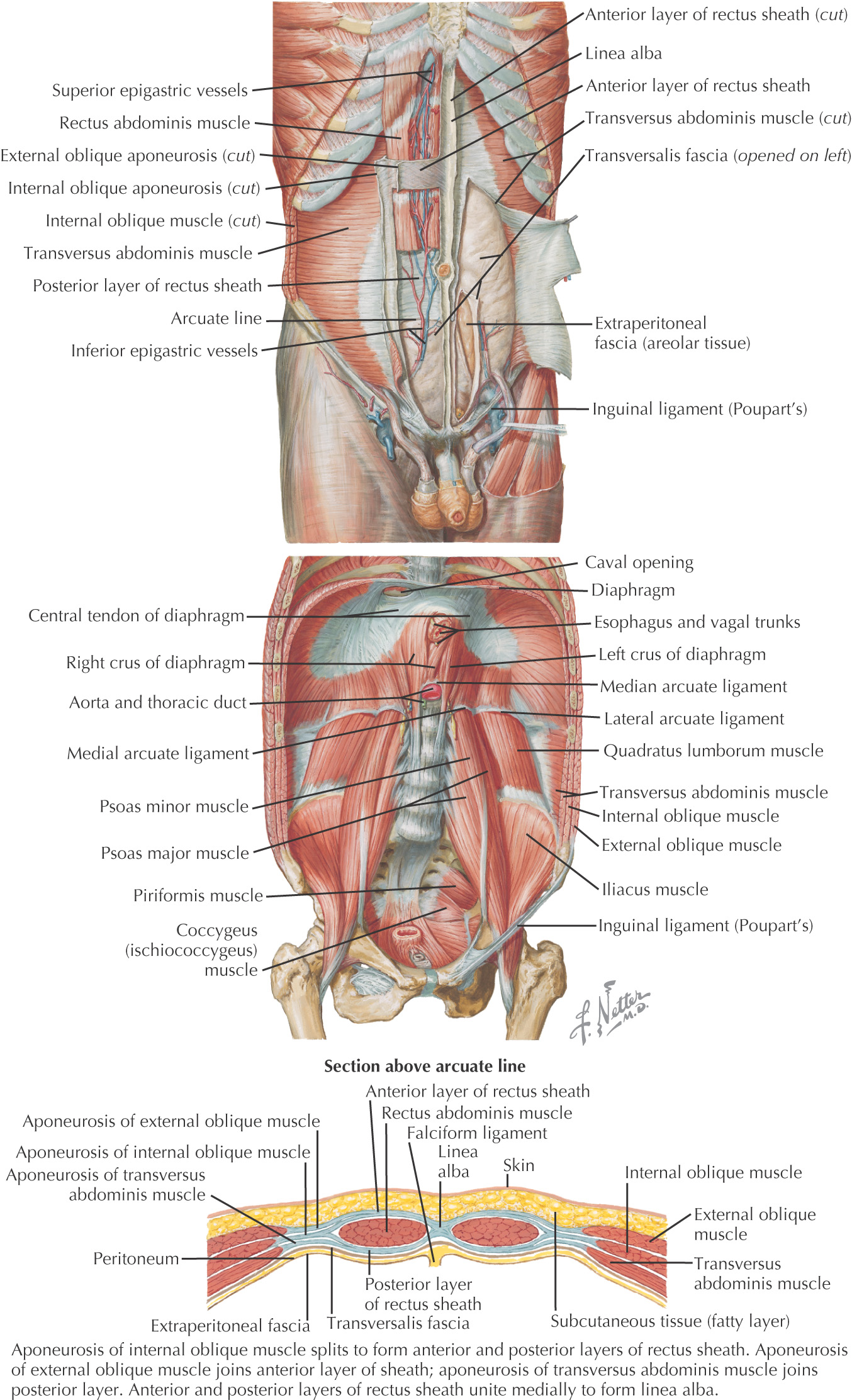
Overview and Topographic Anatomy

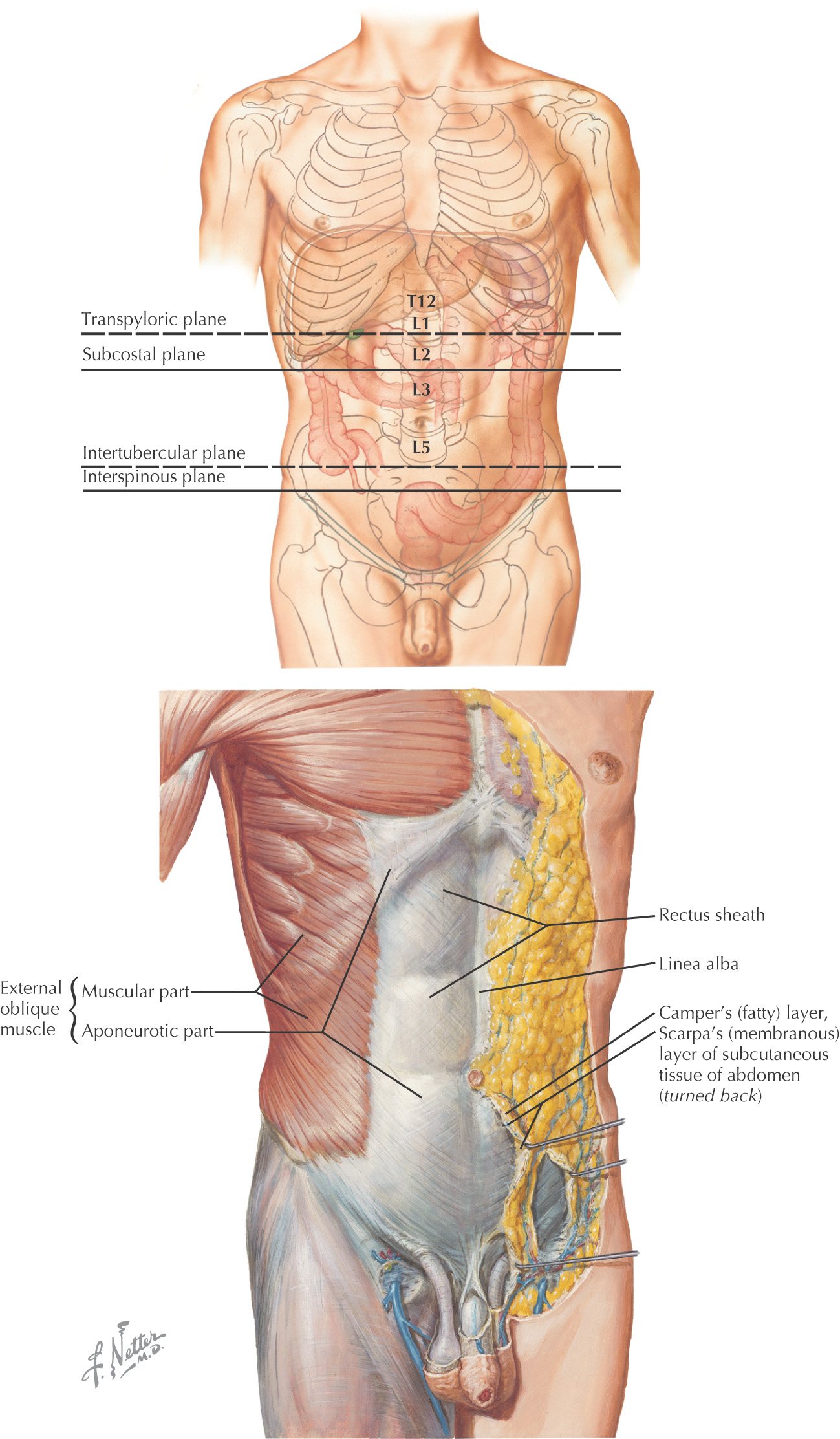
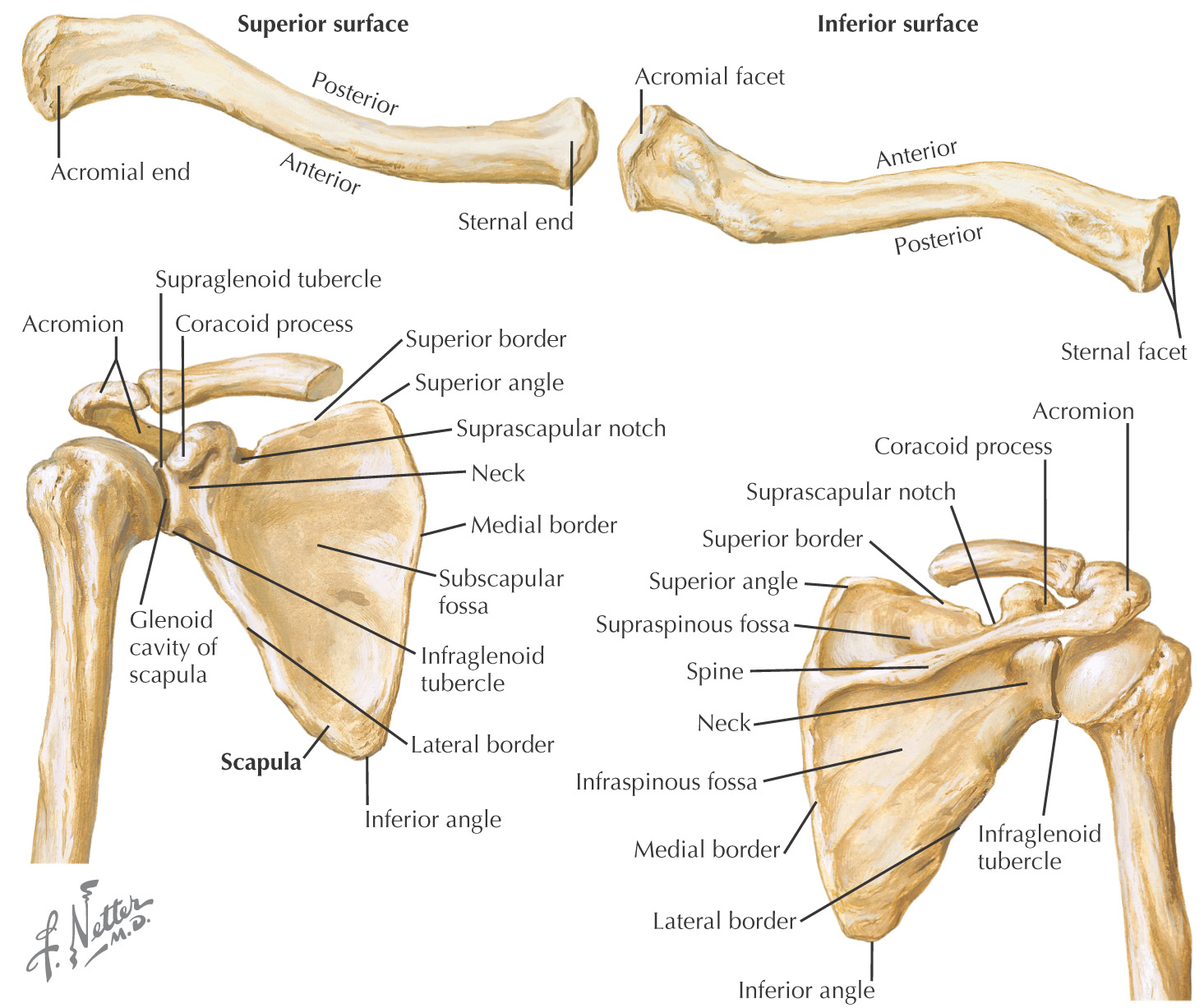
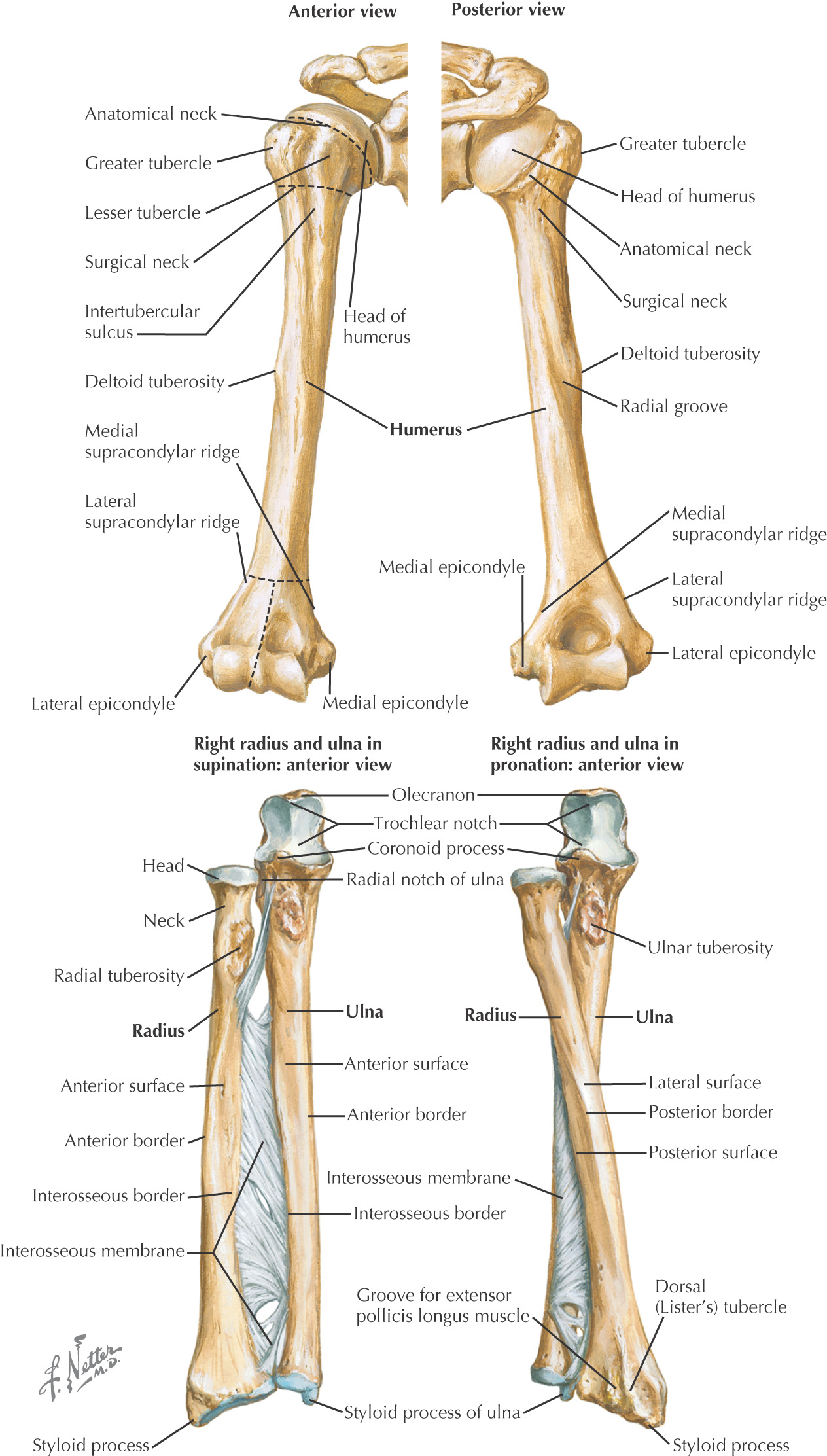
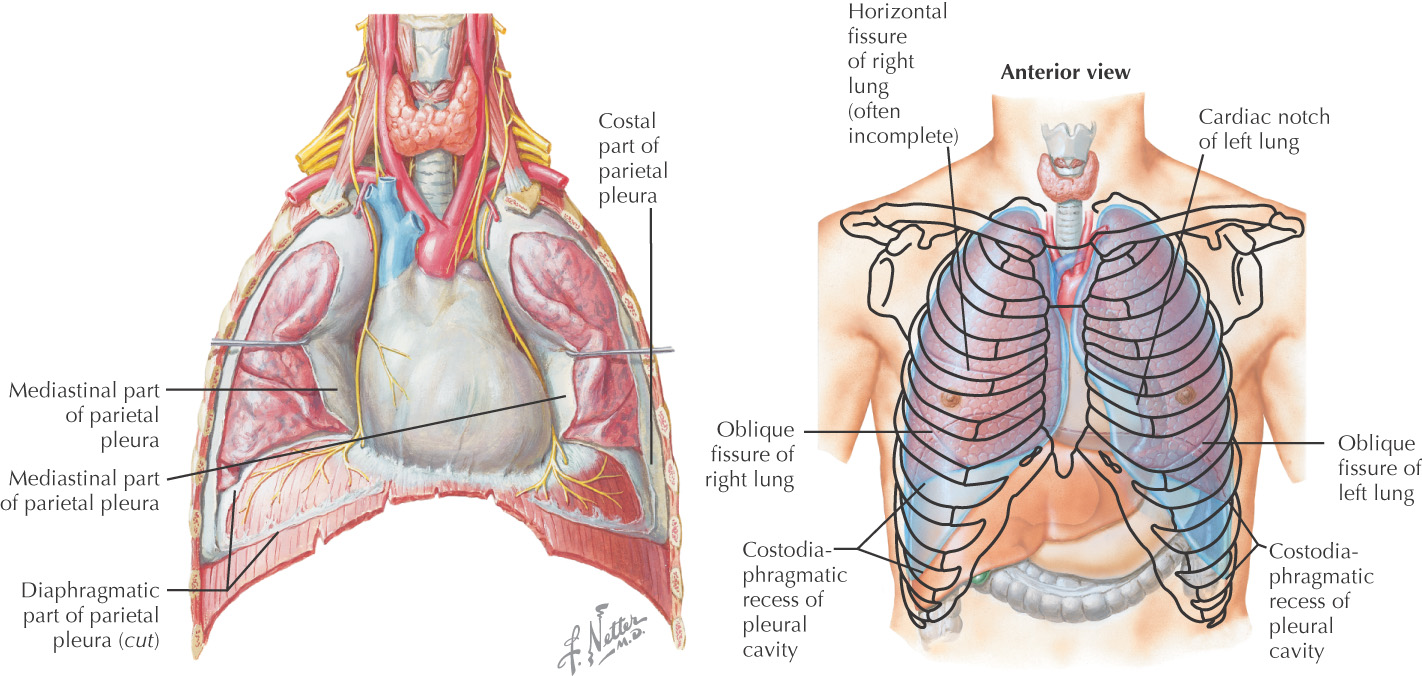
There are 2 pleural cavities
The cavity is composed of a 2-layered pleural sac that secretes a thin layer of serous fluid
• Visceral layer—lines the lung and fissures
• Parietal layer—lines the wall of the cavity
• Costal—lines the cavity along the ribs
• Mediastinal—lines the cavity along the mediastinum
• Diaphragmatic—lines the cavity along the diaphragm
• Cervical (cupula)—lines the cavity forming a dome in the ribs opposite the apex of the lung
Pleural reflections—Abrupt lines where the parietal pleura folds back or changes direction
• Vertebral (posterior)—where costal pleura is continuous with the mediastinal pleura at the vertebral column
• Costal (inferior)—where costal pleura is continuous with diaphragmatic pleura
• Sternal (anterior)—where costal pleura is continuous with the mediastinal pleura posterior to sternum
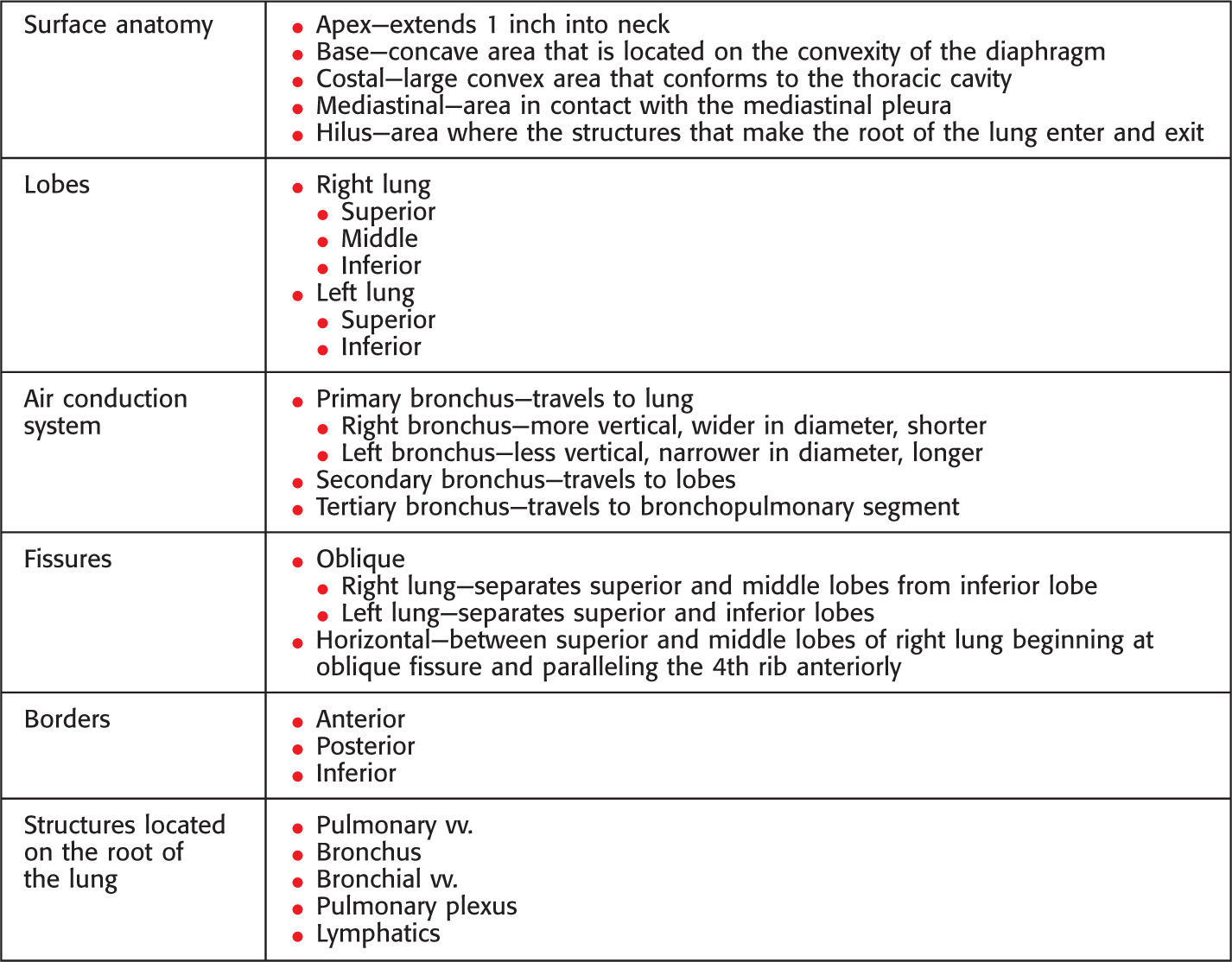
Boundaries
• Anterior midline—6th rib (right) 4th rib (left)
Inferior border of lungs in quiet respiration
• Anterior midline—6th rib (right) 4th rib (left)
Pleural recesses—potential spaces in the pleural cavity where parts of the parietal pleura contact one another during quiet respiration
• Costomediastinal—potential space where costal and mediastinal pleurae come together
• Costodiaphragmatic—potential space where costal and diaphragmatic pleurae come together
Pulmonary ligament—a fold created where the mediastinal pleura at the root of the lung come together and extend inferiorly
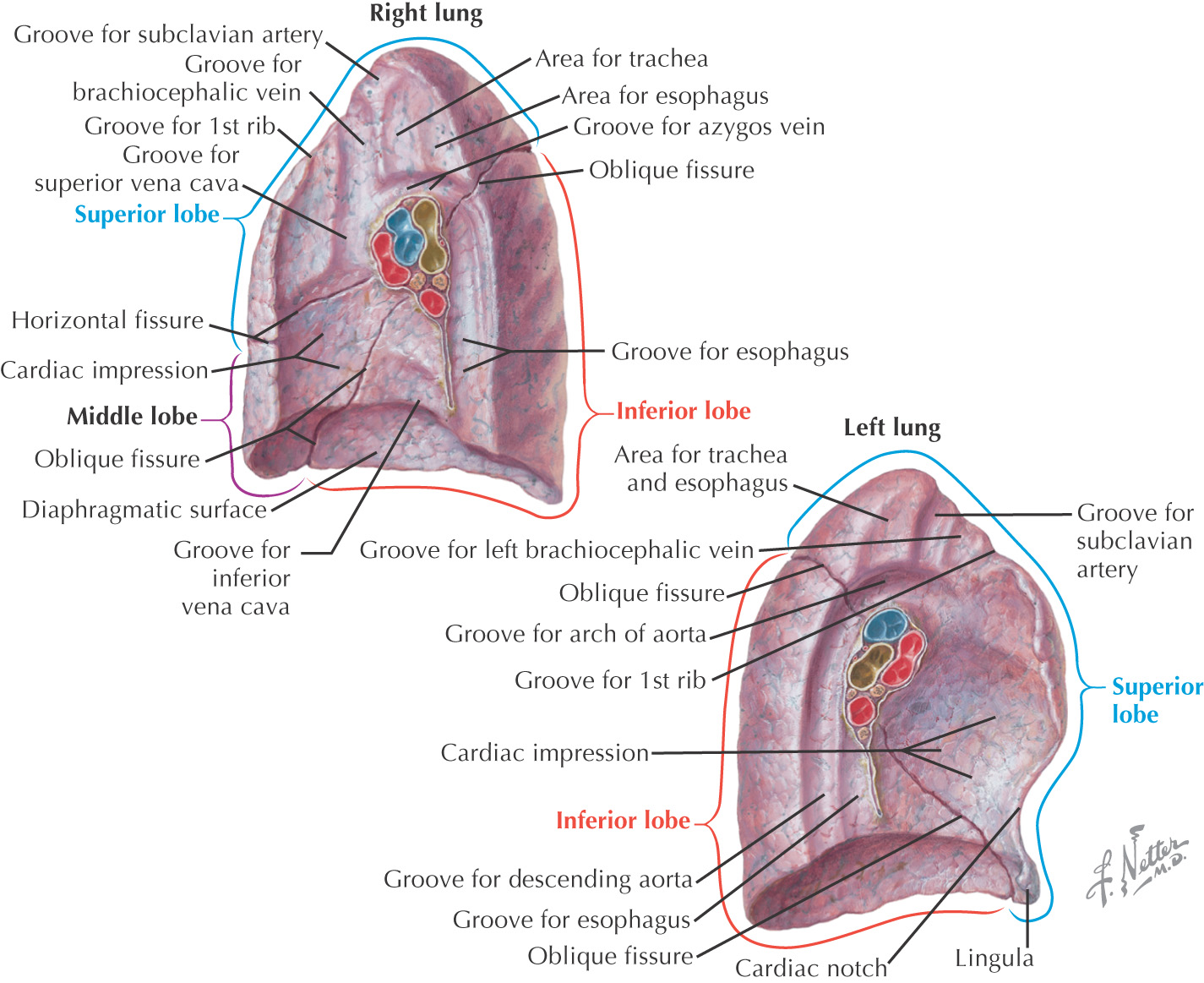
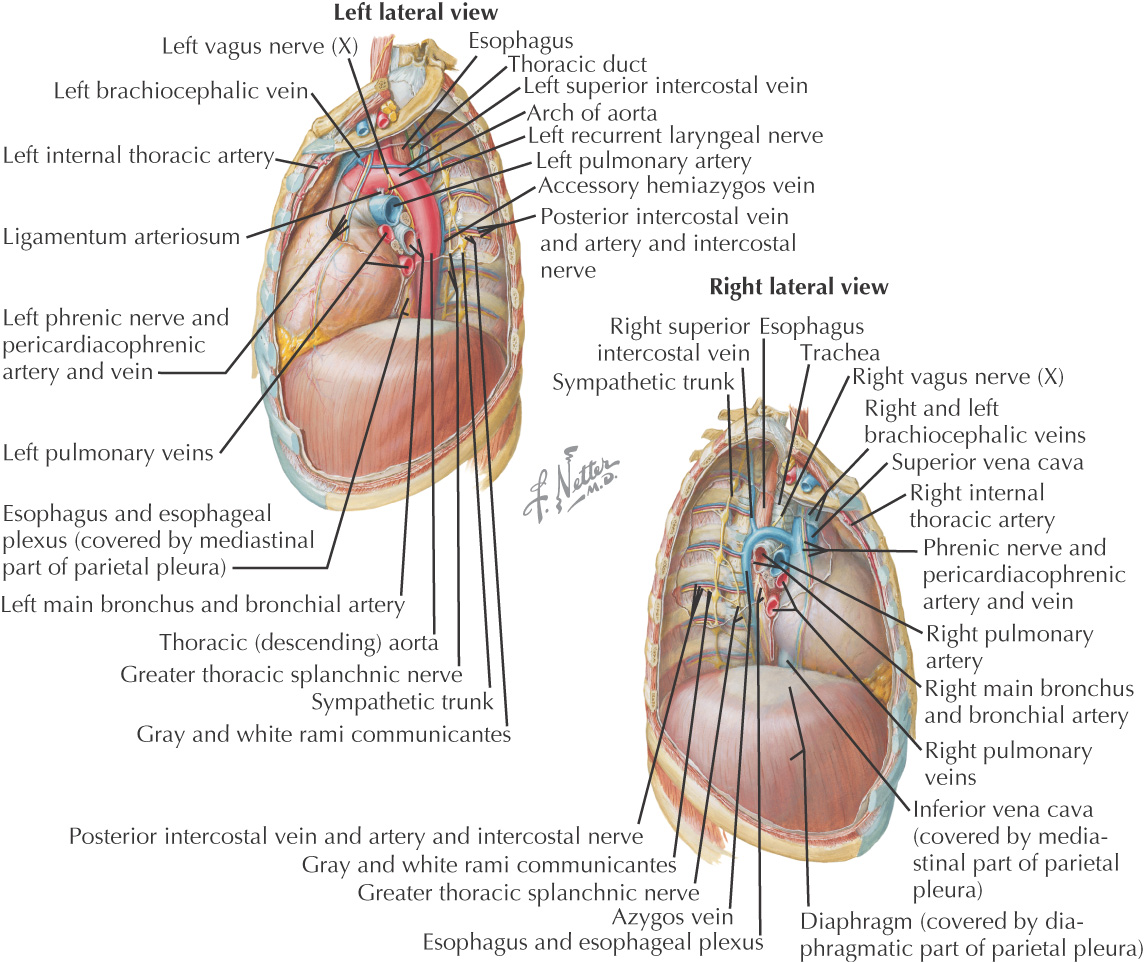
Region in the middle of the thorax between the two pleural sacs
Subdivided into superior and inferior
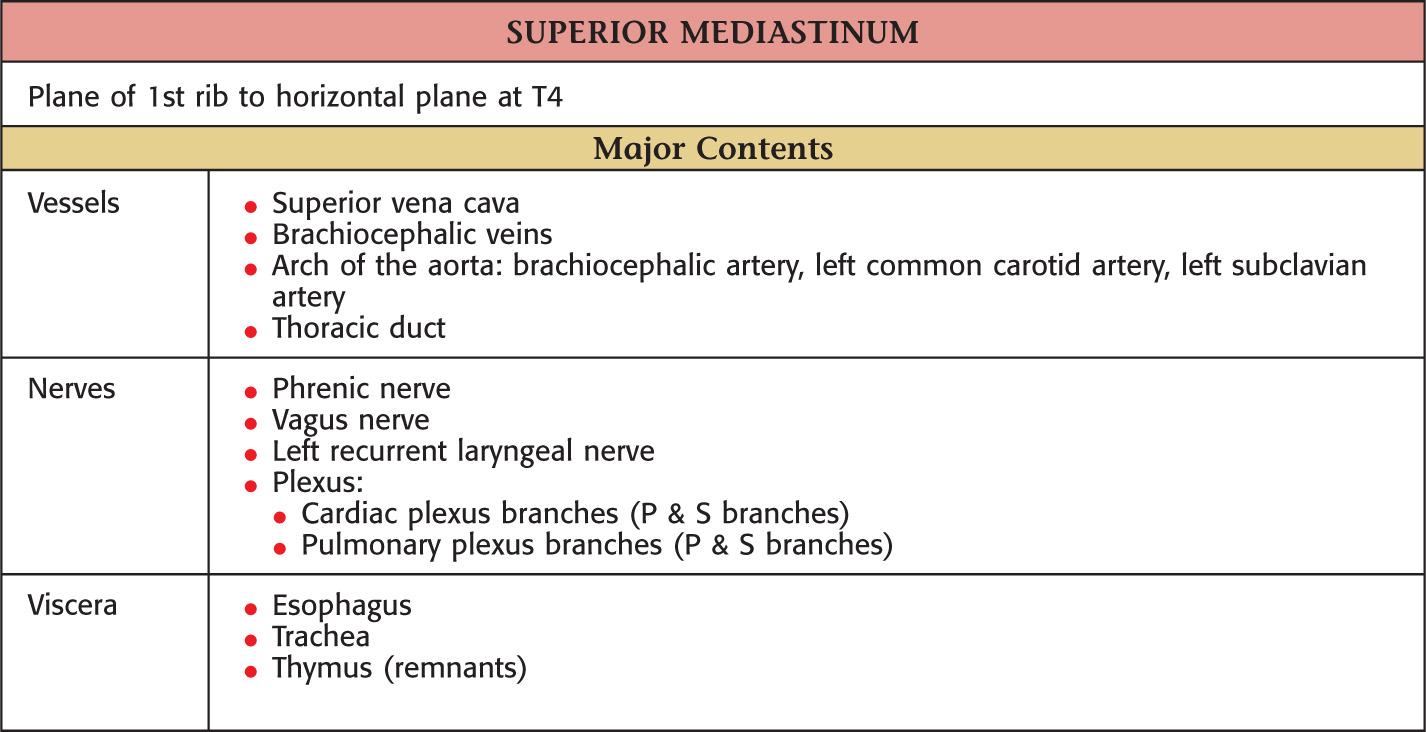
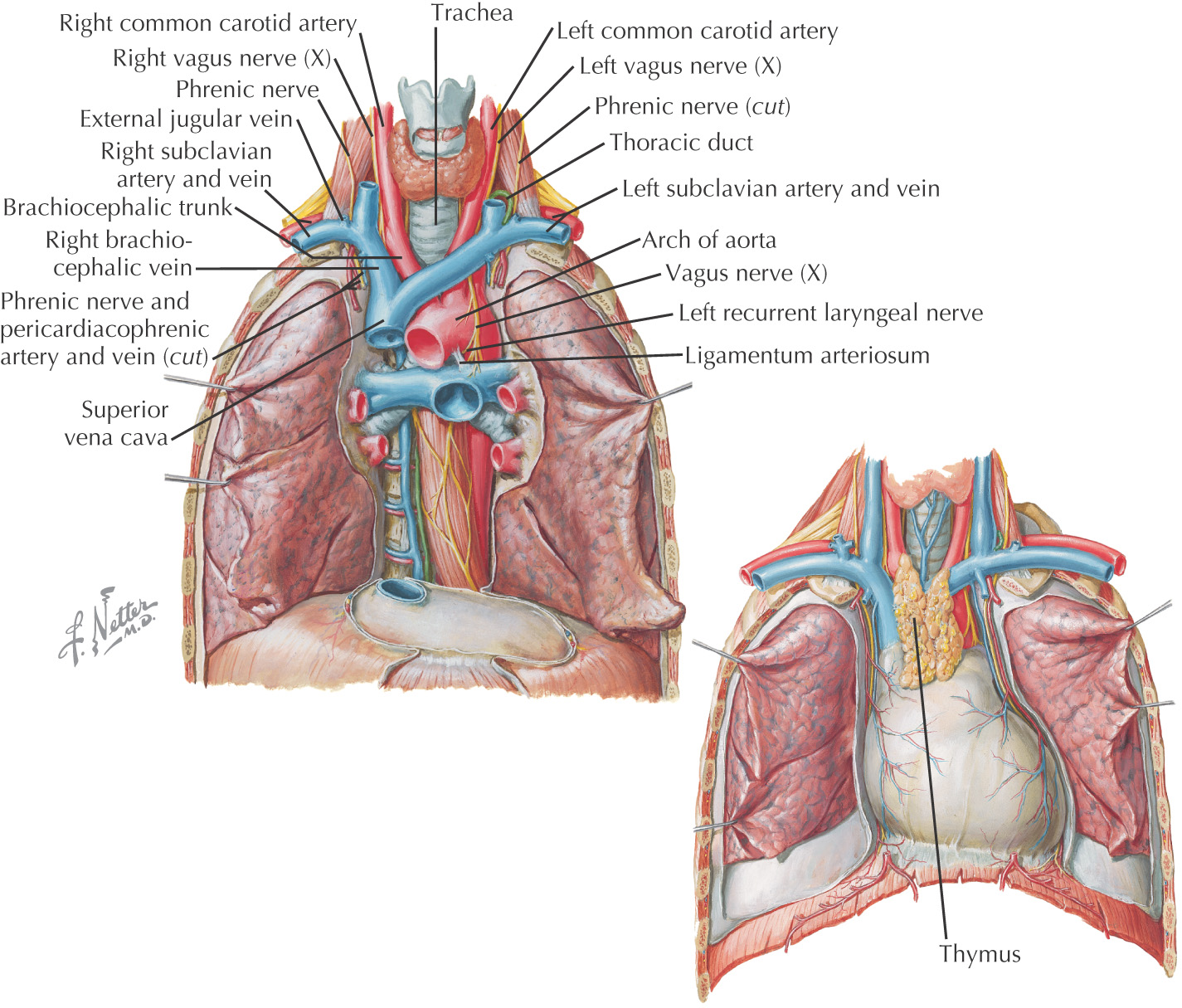
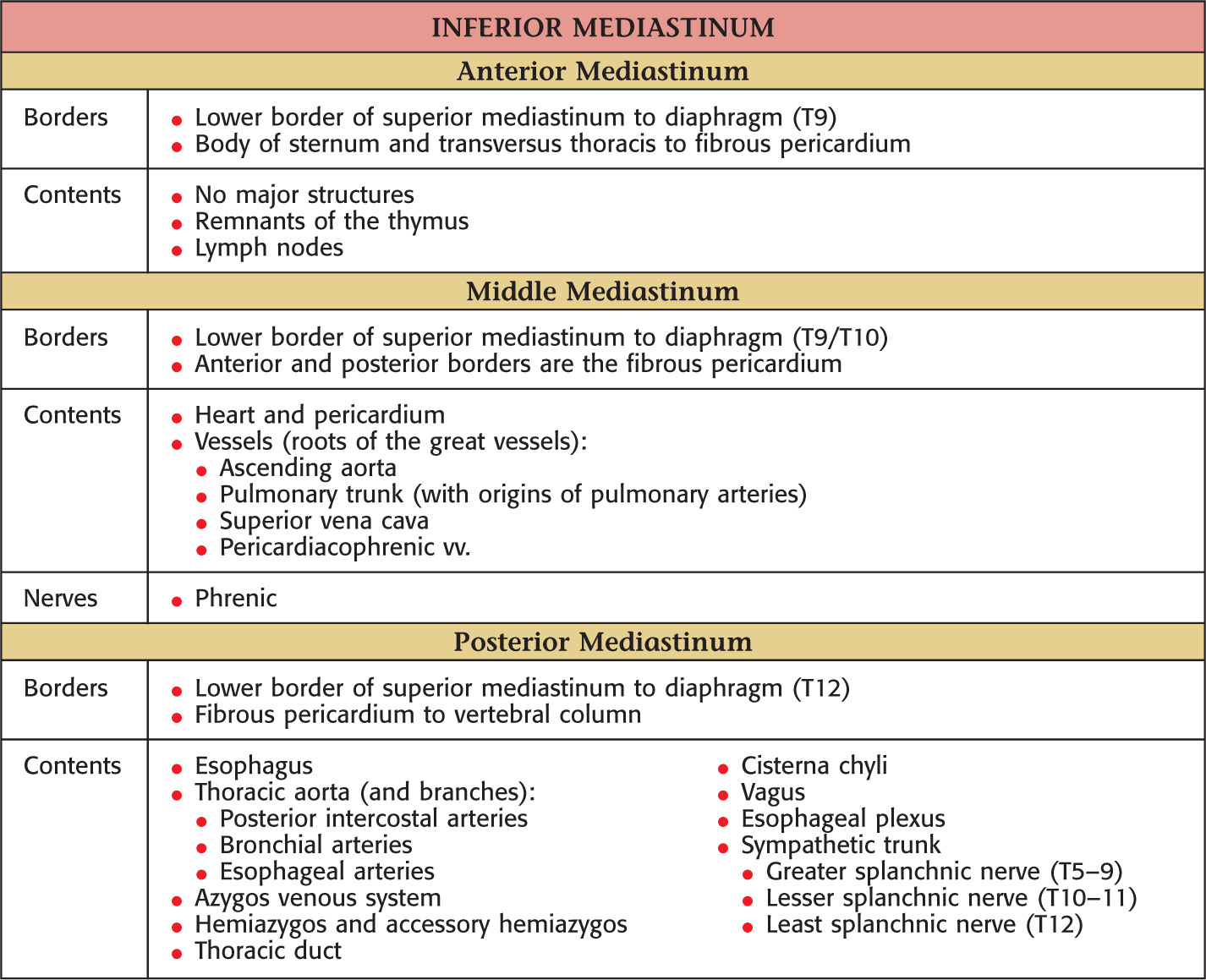
Part of the foregut
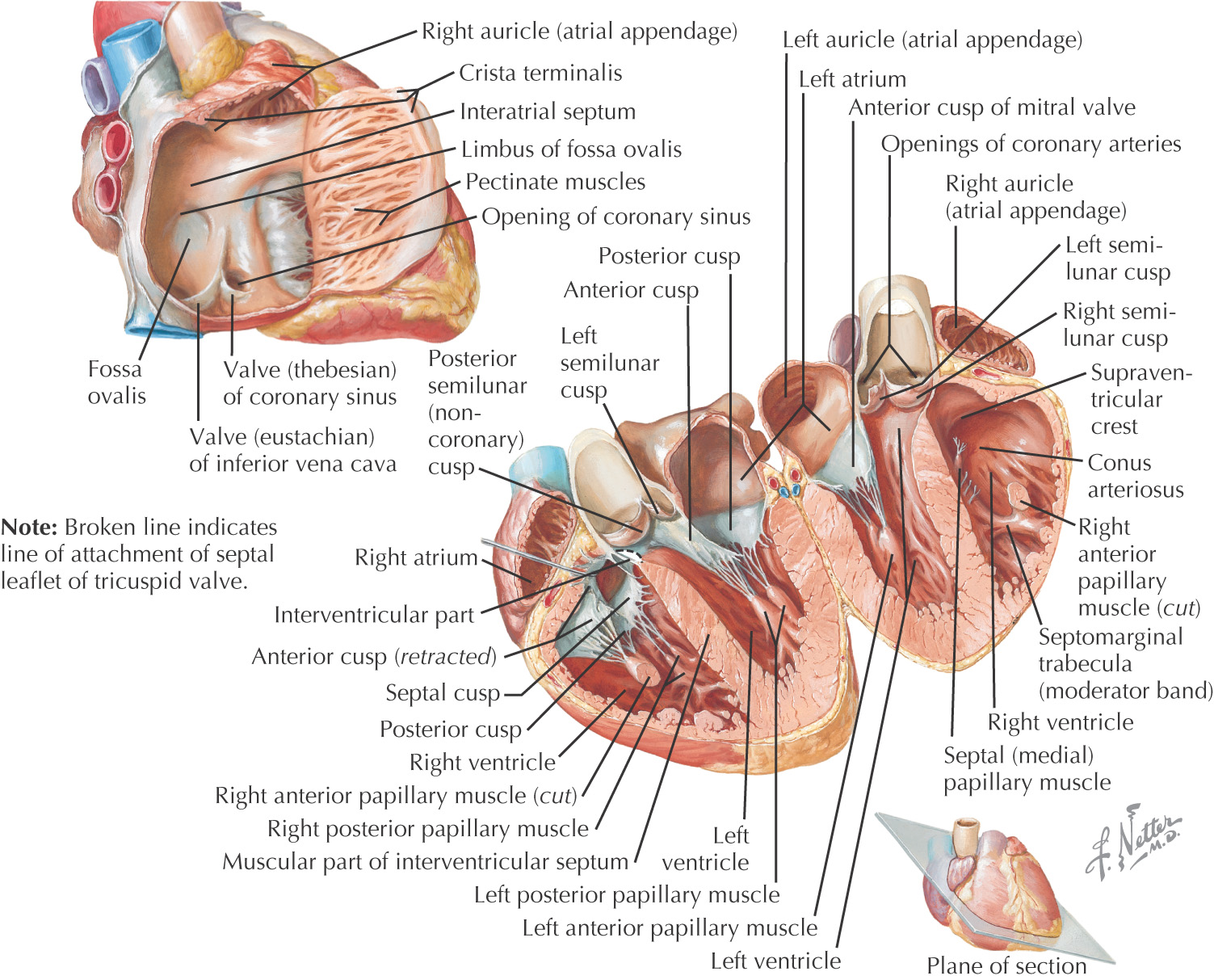
There are 4 anatomical parts of the stomach:
• Cardia—where esophagus enters the stomach
• Fundus—created by the superior portion of the greater curvature
• Pylorus—inferior portion that continues to narrow until reaching the pyloric sphincter
The mucosal lining of the stomach are raised elevations known as gastric rugae
There are 2 major curvatures:
• Greater curvature—provides attachment for some remnants of the dorsal mesogastrium:
• Lesser curvature—provides attachment for remnants of the ventral mesogastrium:
• Hepatogastric portion (hepatoduodenal portion does not attach to the stomach)
There are 2 sphincters associated with the stomach:
• Esophageal—not an anatomical sphincter
• Pyloric—has a thick muscular sphincter
Receives extensive autonomic nerve supply
Is supplied by branches of the celiac artery
Releases pepsin and hydrochloric acid to aid in digestion
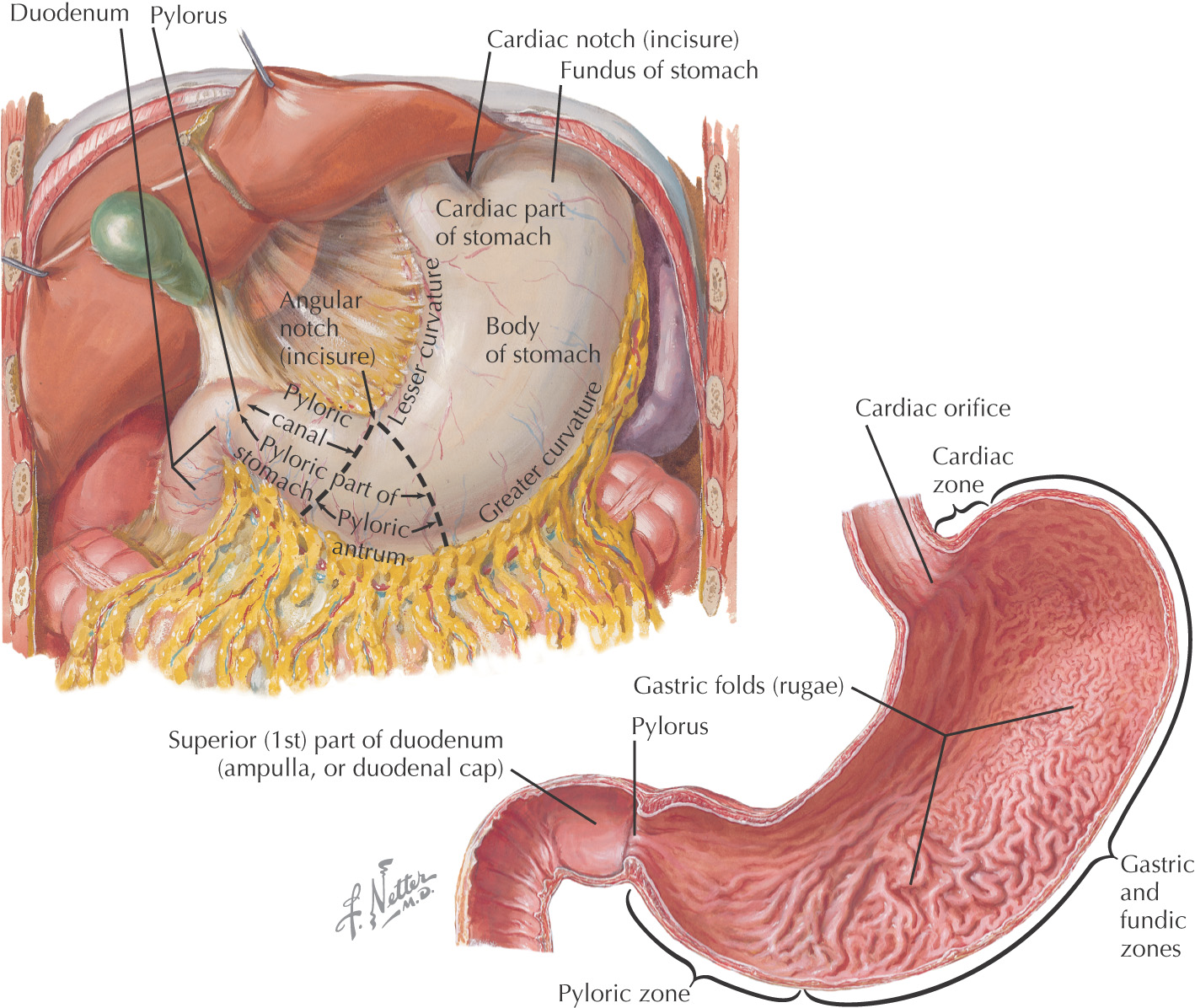
Is the first of the 3 parts of the small intestine:
Part of the foregut and midgut
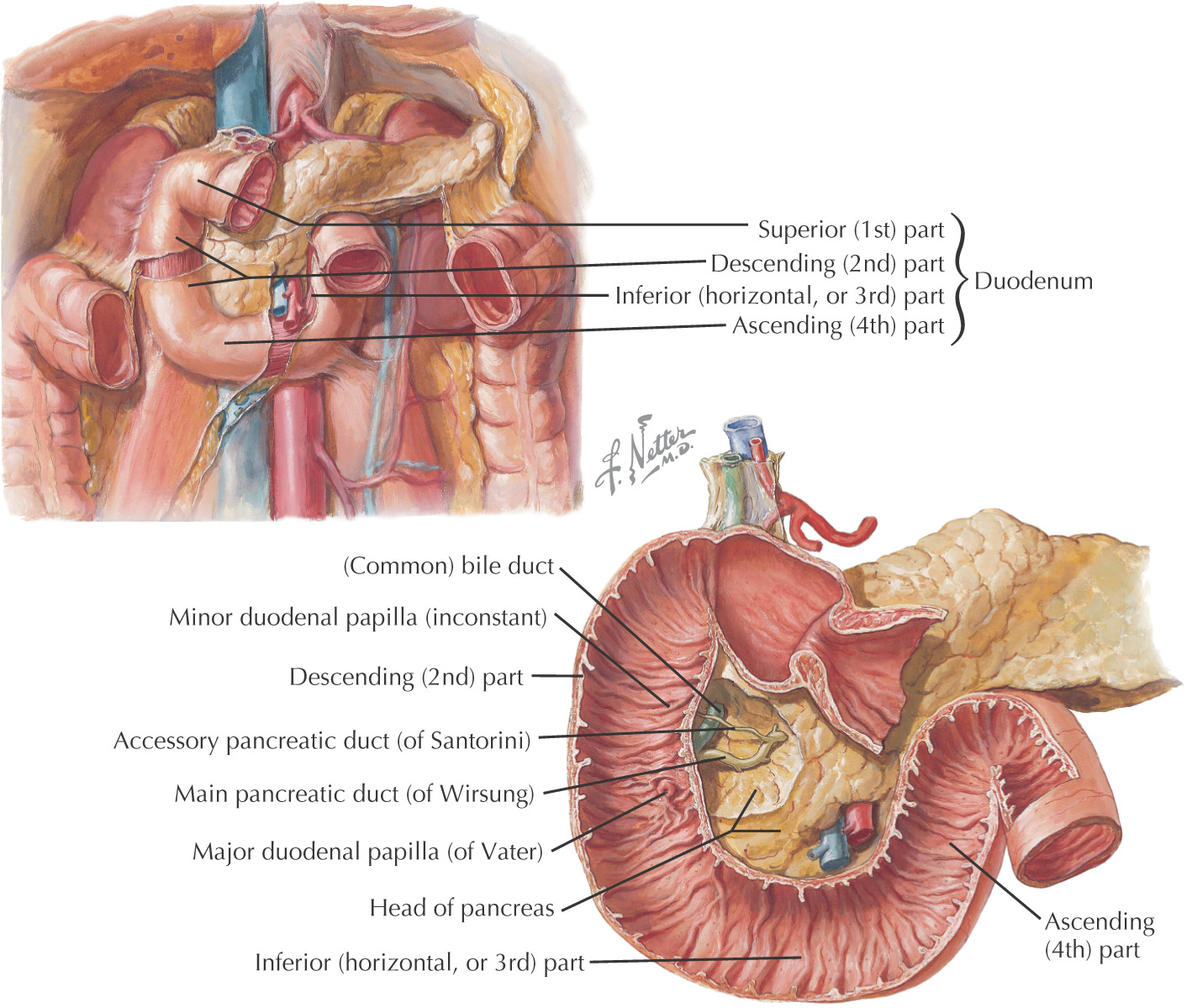
There are 4 anatomical parts of the duodenum:
• 1st part—intraperitoneal, part of foregut
• 2nd part—retroperitoneal, part of foregut
• Minor duodenal papilla—where accessory pancreatic duct (if present) drains
• Major duodenal papilla—where pancreas, liver, and gallbladder drain
• 3rd part—retroperitoneal, part of midgut
• 4th part—retroperitoneal, part of midgut
The mucosal lining of the duodenum are raised elevations known as plicae circulares
Receives extensive autonomic nerve supply
Is supplied by branches of the celiac and superior mesenteric arteries
Is the portion of the small intestine where the majority of chemical digestion occurs
A major histological feature is the presence of mucus-secreting glands, Brunner’s glands
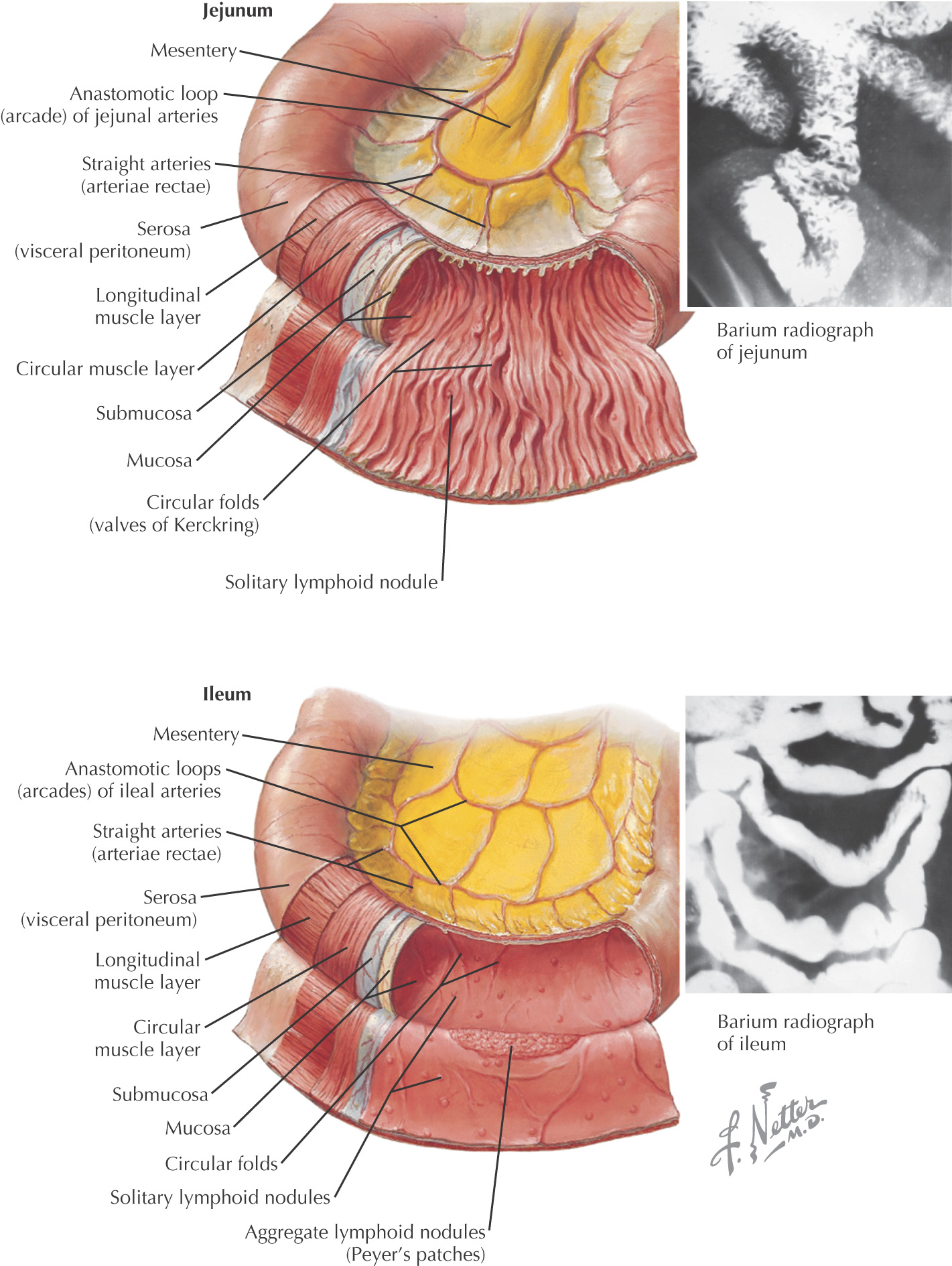
Are the final 2 parts of the small intestine:
Part of the midgut
Is intraperitoneal
Is suspended by the mesentery proper
The mucosal lining has raised elevations known as plicae circulares
Receives extensive autonomic nerve supply
Is supplied by branches of the superior mesenteric artery
Is about 7—8 feet in length
Has scattered lymphatic nodules and very few Brunner’s glands
Has prominent plicae circulares
Vascular supply has large prominent arterial arcades terminating with long vasa recta
Is about 6—12 feet in length
Ileum has extensive Peyer’s patches (lymphatic nodules)
Has fewer plicae circulares than the jejunum
Vascular supply has large smaller layers of arterial arcades terminating with short, compact vasa recta
Ends in the large intestine at the ileocecal valve
Is the embryological connection to the umbilicus via the vitelline duct; a Meckel’s diverticulum is a remnant of the duct in the adult
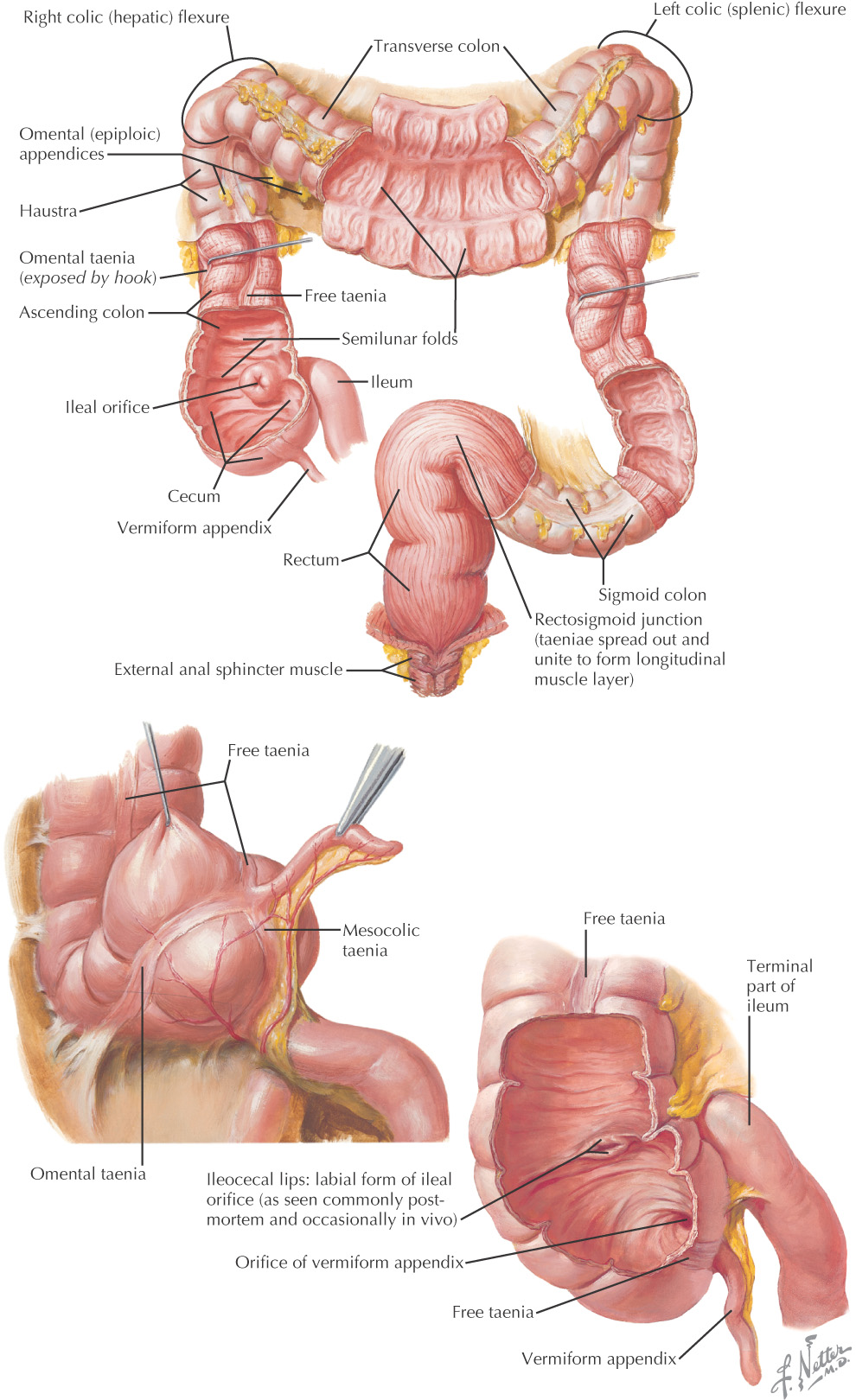
Is divided into:
Has the following characteristic features:
• Taeniae coli—3 separate bands of longitudinal muscle
• Haustra—pouch-like appearance caused by the contraction of the taeniae coli
• Epiploic appendages—small pouches of fat along the peritoneum
Part of the midgut and hindgut
Is intraperitoneal and retroperitoneal
The mucosal lining has raised elevations known as plicae semilunares
Receives extensive autonomic nerve supply
Is supplied by branches of the superior mesenteric and inferior mesenteric arteries
Major function is the absorption of water from the indigestible waste and expulsion from the body
Is intraperitoneal
Connects ileum to the large intestine at the ileocecal valve
Blind pouch
Appendix is a small (typically around 4 inches) blind tubular intraperironeal structure connected to the cecum
Is retroperitoneal
Begins at ileocecal valve and ascends
Makes a colic impression on the liver and makes a sharp turn to the left side of the body known as the right colic (hepatic) flexure before continuing as the transverse colon
Is intraperitoneal, suspended by the transverse mesocolon
Longest portion of the large intestine
At the area of the spleen, makes a sharp turn to travel inferiorly, known as the left colic (splenic) flexure before continuing as the descending colon
Is retroperitoneal
Descends until it ends at the sigmoid colon
Terminal portion of the descending colon is often called the iliac colon because it lies in the iliac fossa
Typically has a smaller diameter than the ascending colon
Is intraperitoneal, suspended by the sigmoid mesocolon
Begins at the level of the pelvic brim
Travels toward the midline, where it ends at the rectum
Begins as intraperitoneal, but is retroperitoneal until it passes through the pelvic floor
Is about 4—5 inches in length
Does not have taeniae coli as the separate bands merge to form a complete band of longitudinal muscle at the rectum
Ends at the anus
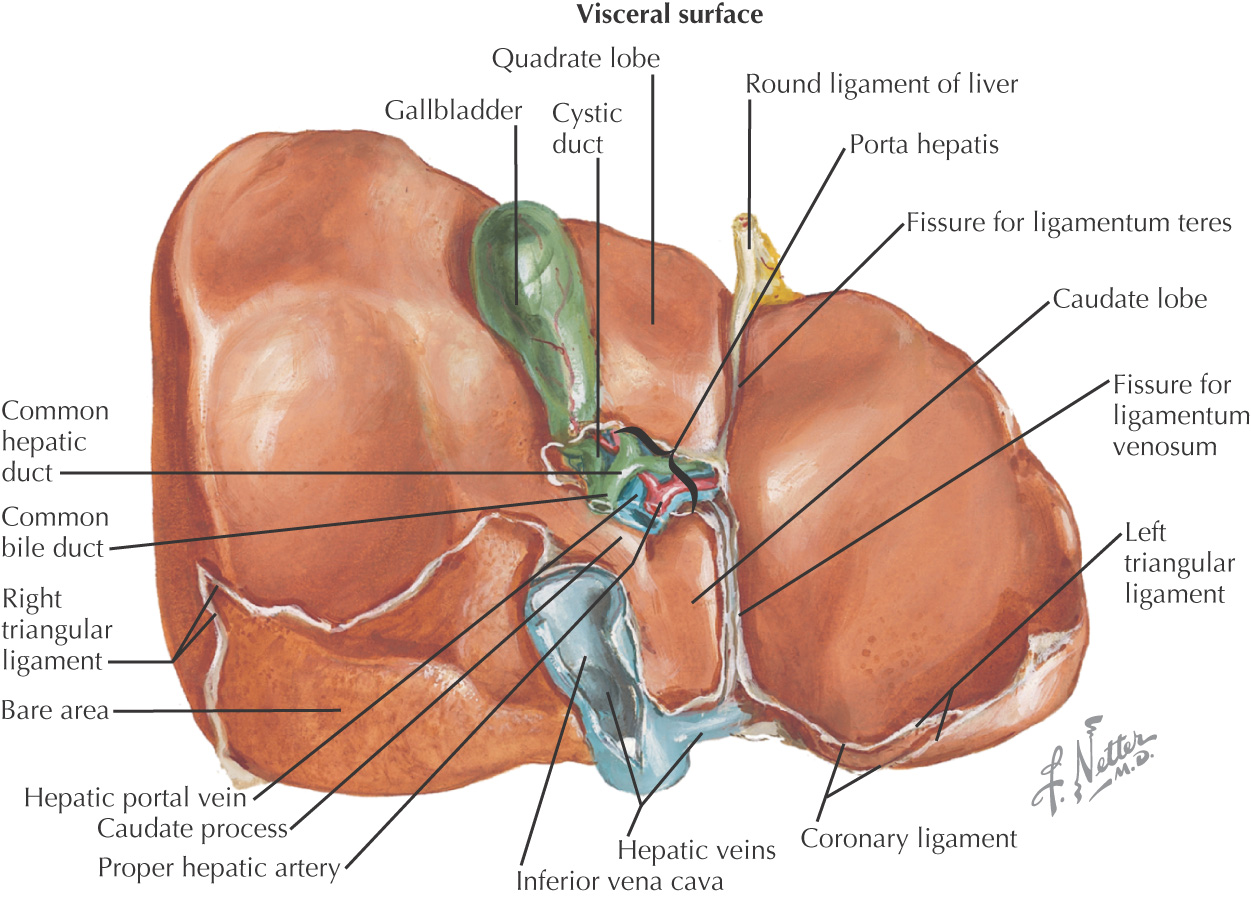
Large, multifunctional organ, including:
• Synthesis of plasma proteins
Divided into 4 anatomical lobes:
• Caudate—located between fissure for the ligamentum venosum and the inferior vena cava
• Quadrate—located between fissure for the ligamentum teres hepatis (round ligament of the liver) and the gallbladder
Is further subdivided into functional segments based on the vascular supply
Is completely covered by visceral peritoneum except an area where the liver connects with the diaphragm, known as the bare area
The porta hepatis is the central portion of the liver where the following structures enter and exit:
• Hepatic portal vein—provides 75% of the blood to the liver
• Proper hepatic artery—provides 25% of the blood to the liver
Is intraperitoneal
Is supplied by branches of the celiac artery
All remnants of the ventral mesentery attach to the liver:
The liver is subject to numerous pathologies, including:
The pancreas functions as 2 types of glands:
• Endocrine—Islets of Langerhans producing hormones
• Exocrine—Compound tubuloalveolar pancreatic acini producing digestive enzymes
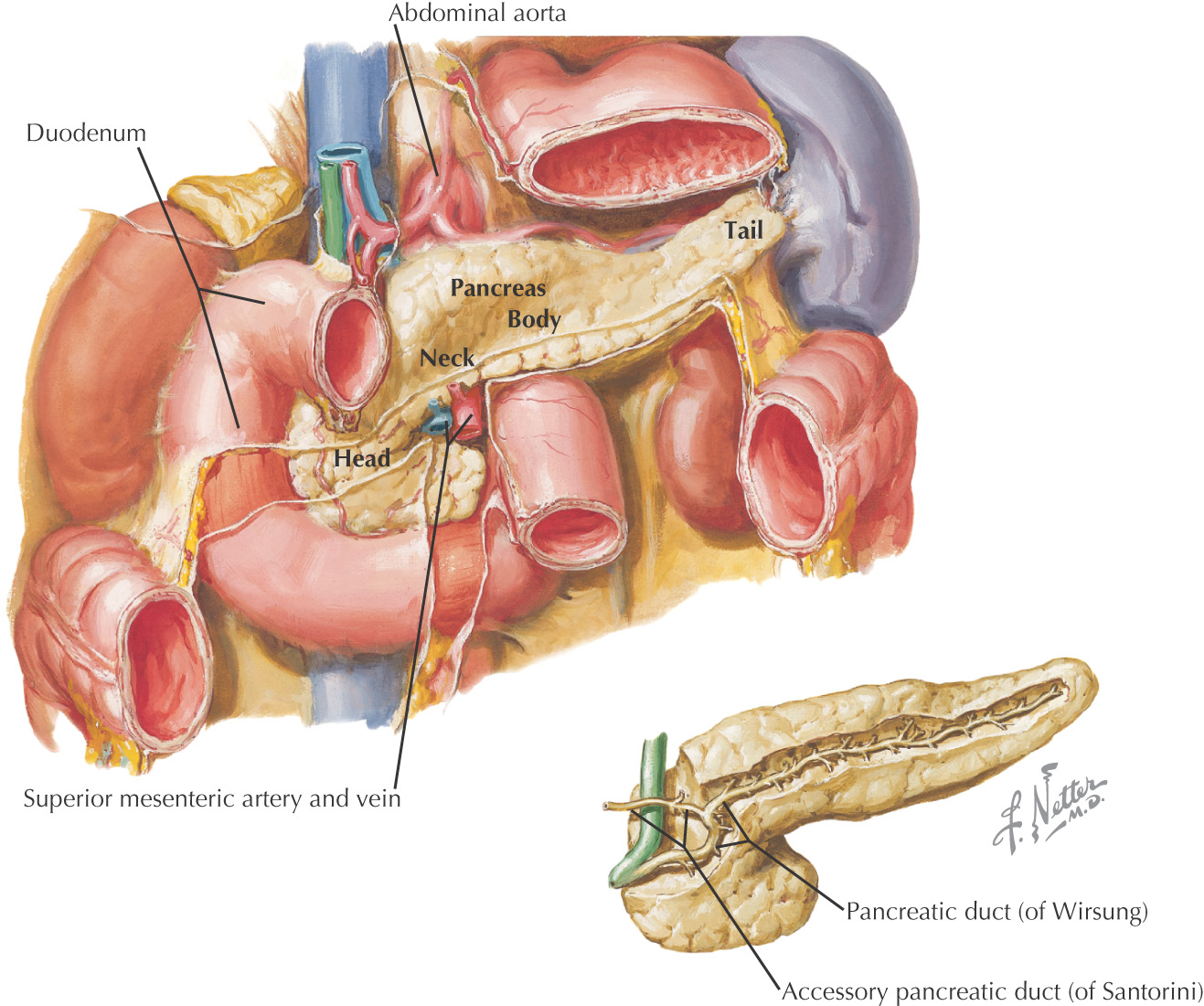
Comprised of 4 major parts:
• Head—is located in the “C” or curve formed by the duodenum; is retroperitoneal
• Uncinate process—an extension of the head crossed by the superior mesenteric vv.
• Neck—constricted portion of pancreas connecting the head to the body; is retroperitoneal
• Body—largest part of the pancreas separated from the stomach by the omental bursa, is retoperitoneal
• Tail—extends into the lienorenal ligament with the splenic vv. to the spleen
Is part of the foregut
Develops as 2 separate outgrowths from the 2nd part of the duodenum:
• Ventral pancreatic bud—an outgrowth of the hepatic bud
• Develops into the head and neck of the pancreas
• Dorsal pancreatic bud—a direct outgrowth of the 2nd of the duodenum
• Develops into the body and tail of the pancreas
Drains into the 2nd part of the duodenum
• Main pancreatic duct—drains into the major duodenal papilla by joining the common bile duct forming the hepatopancreatic ampulla
• Accessory pancreatic duct—drains into the minor duodenal papilla (if present and patent)
Is supplied by branches of the celiac and superior mesenteric arteries
Receives extensive autonomic nerve supply
Small intraperitoneal organ
Is part of the foregut
Stores and concentrates bile, which emulsifies fat during digestion
Is located in a fossa on the liver where the linea semilunaris attaches to the ribcage at the 9th costal cartilage
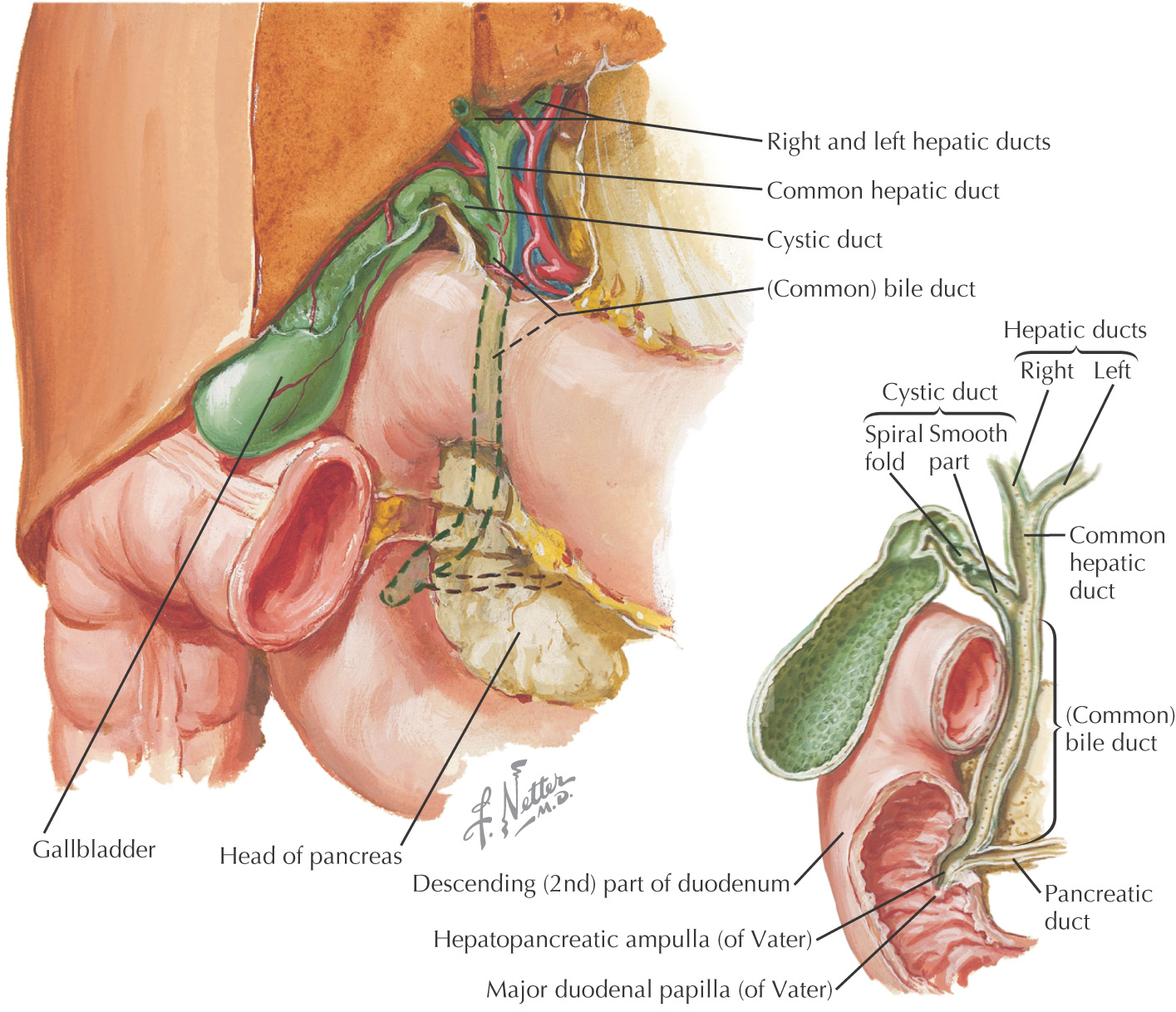
Divided into 3 parts:
Is supplied by branches of the celiac artery
Receives extensive autonomic nerve supply
The cystic duct joins the common hepatic duct to form the common bile duct
The common bile duct joins the main pancreatic duct within the substance of the pancreas to form the hepatopancreatic ampulla, which passes through the wall of the 2nd part of the duodenum into the major duodenal papilla
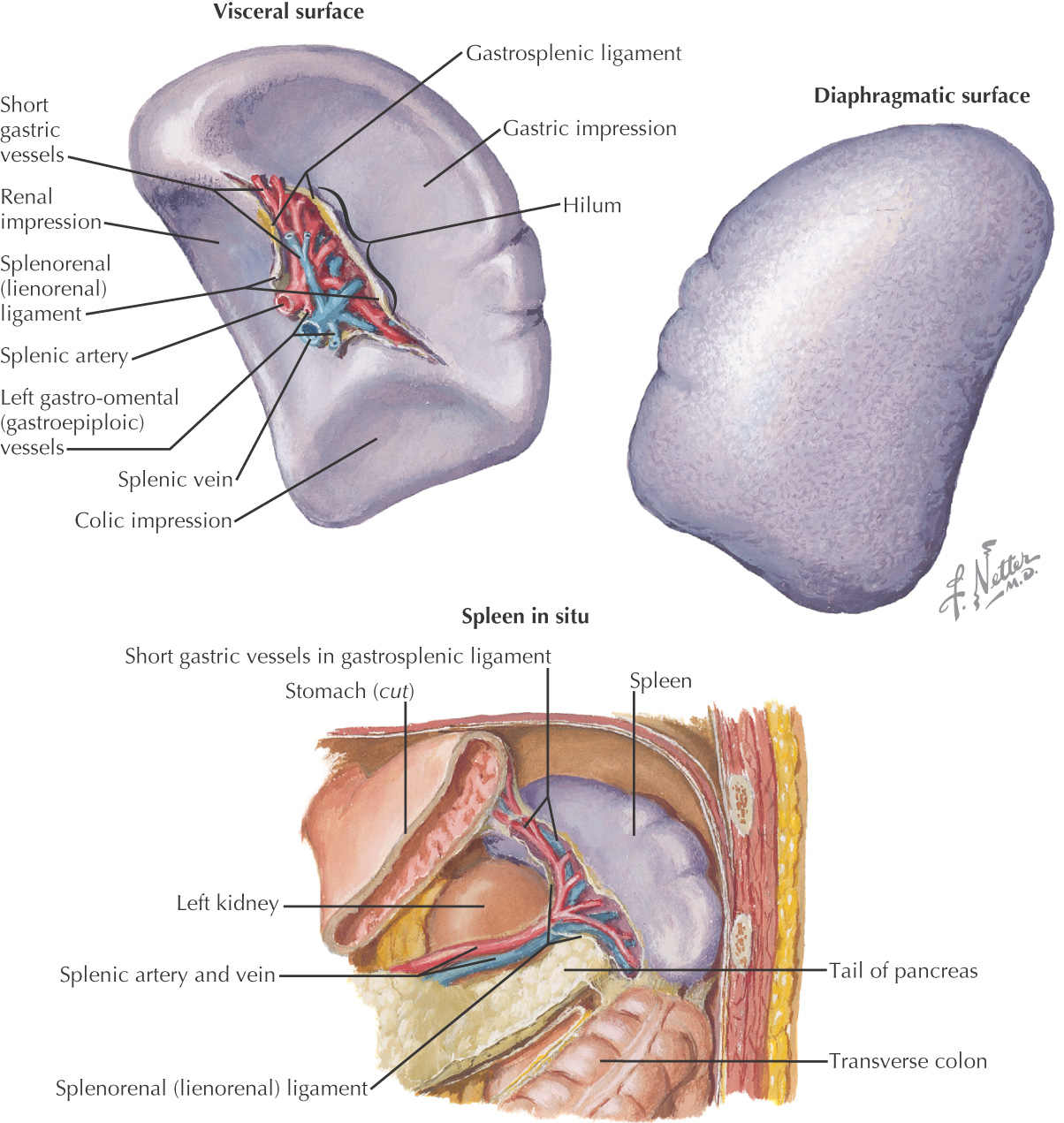
A lymphatic organ on the left side of the body divided into:
Is intraperitoneal
Is not a derivative of the foregut, although receives its arterial supply from branches of the celiac artery
Is located between the 9th and 11th ribs, paralleling the 10th rib
Has contact with 4 organs:
Is suspended by dorsal mesentery of the foregut:
• Lienorenal—contains tail of the pancreas and splenic vv.
• Gastrosplenic—contains short gastric vv. and left gastroepiploic vv.
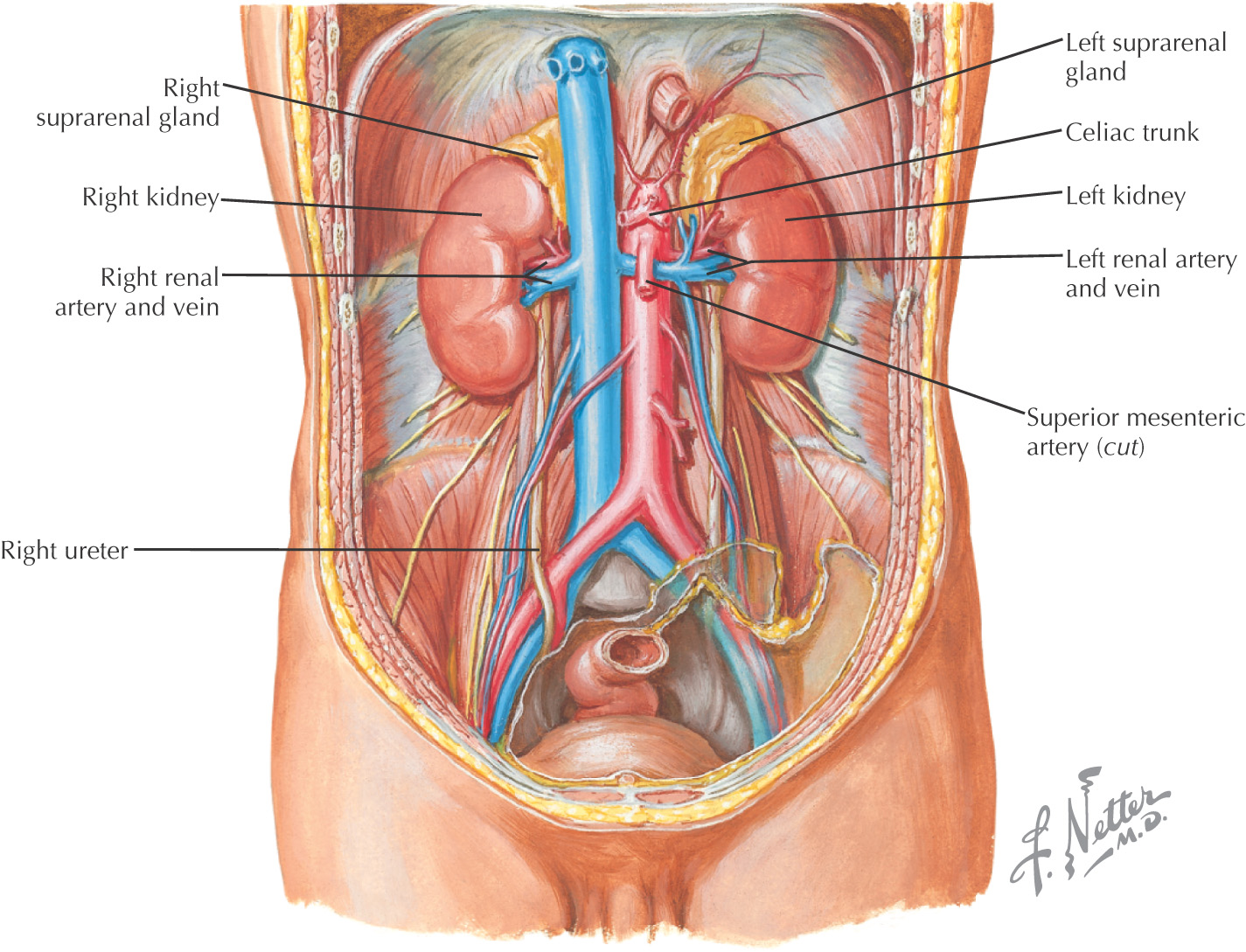
Paired organ
Is retroperitoneal
Has multiple functions, including:
Nephron is function unit
Located between T11—L3, with hilum at L1
Left kidney is slightly larger than the right kidney
Right kidney is slightly inferior to the left kidney due to the liver
Surrounded by a tough capsule
Divided into:
Receives arterial supply from renal vv.
Receives extensive autonomic nerve supply
Is retroperitoneal
Carries urine from kidney to the bladder
Begins at hilum, or L1 and travels inferior to the bladder
Common sites of kidney stones include:
• Crossing Iliac vv. on pelvis
Also known as adrenal gland
Are endocrine glands
Divided into:
• Cortex—responsible for production of mineralocorticoids, glucocorticoids, and androgens
• Medulla—responsible for catecholamines via sympathetic response (flight or flight)
Receives threefold arterial supply:
• Superior suprarenal—from inferior phrenic a.
• Middle suprarenal—from aorta
• Inferior suprarenal—from renal a.
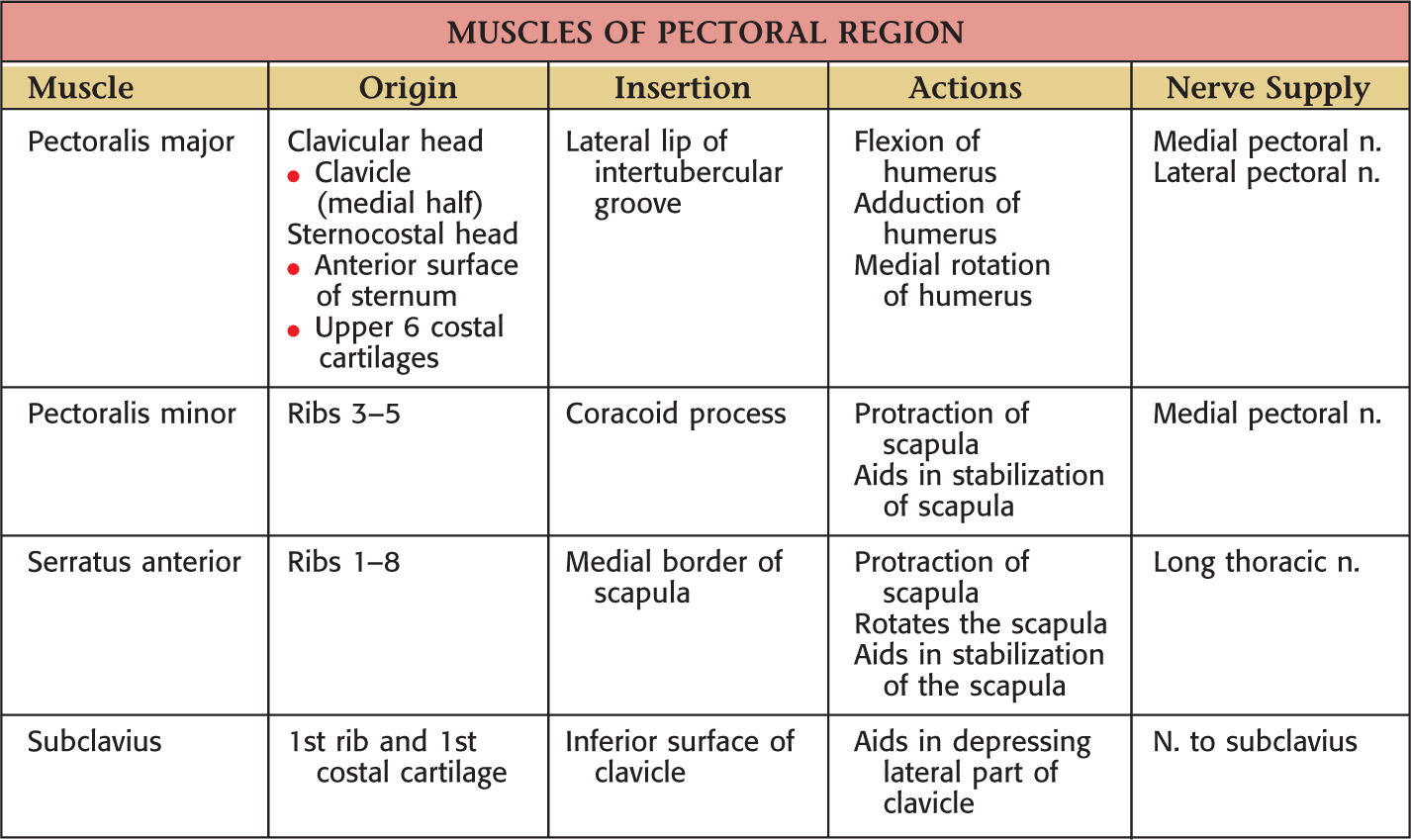
Axillary—is divided into 3 parts based on its relationship to the pectoralis minor
• Superior thoracic—supplies 1st two intercostal spaces
• Deltoid—accompanies cephalic v.
• Clavicular—helps supply acromioclavicular joint
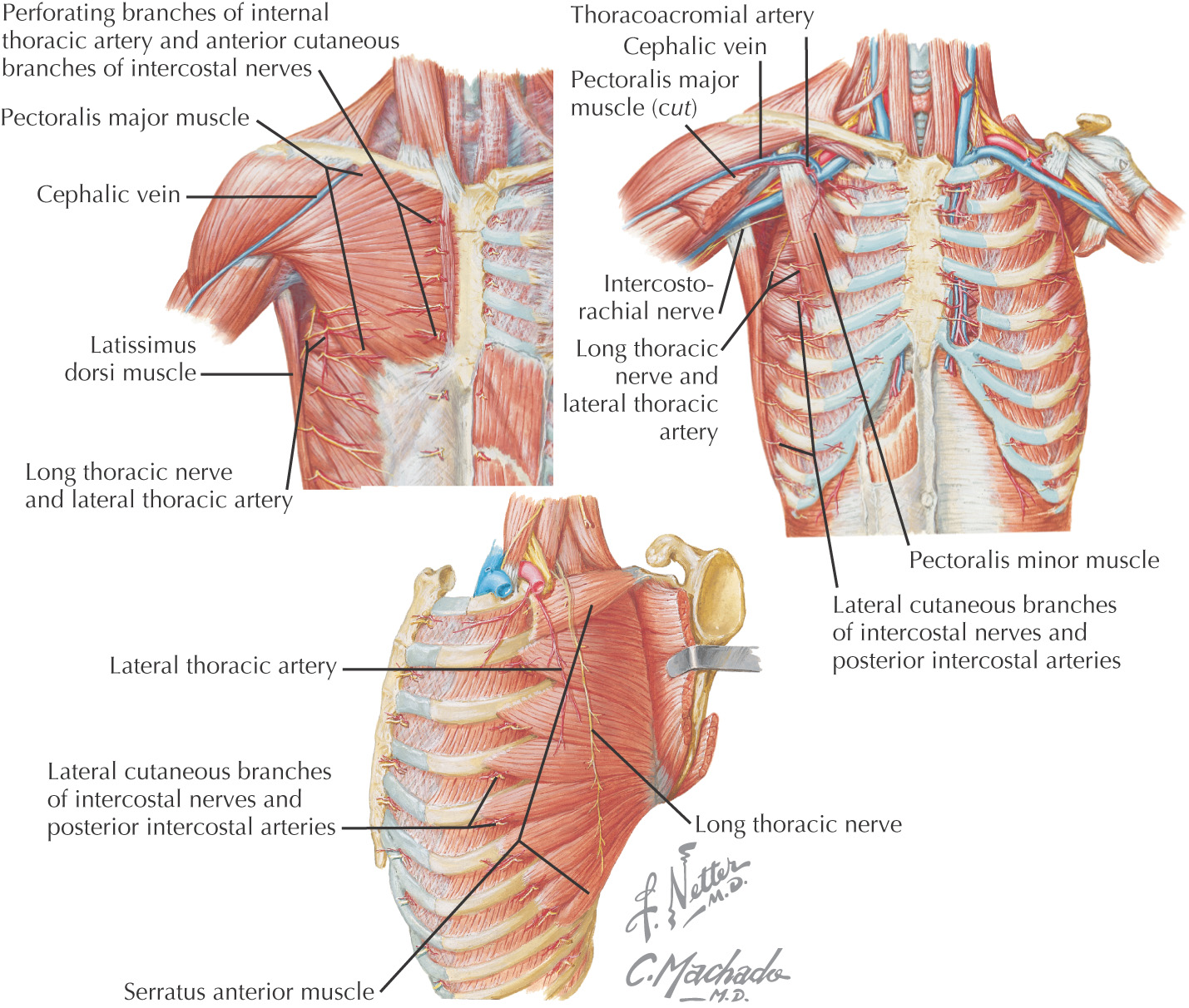
• Lateral thoracic—follows inferior border of pectoralis minor to thorax
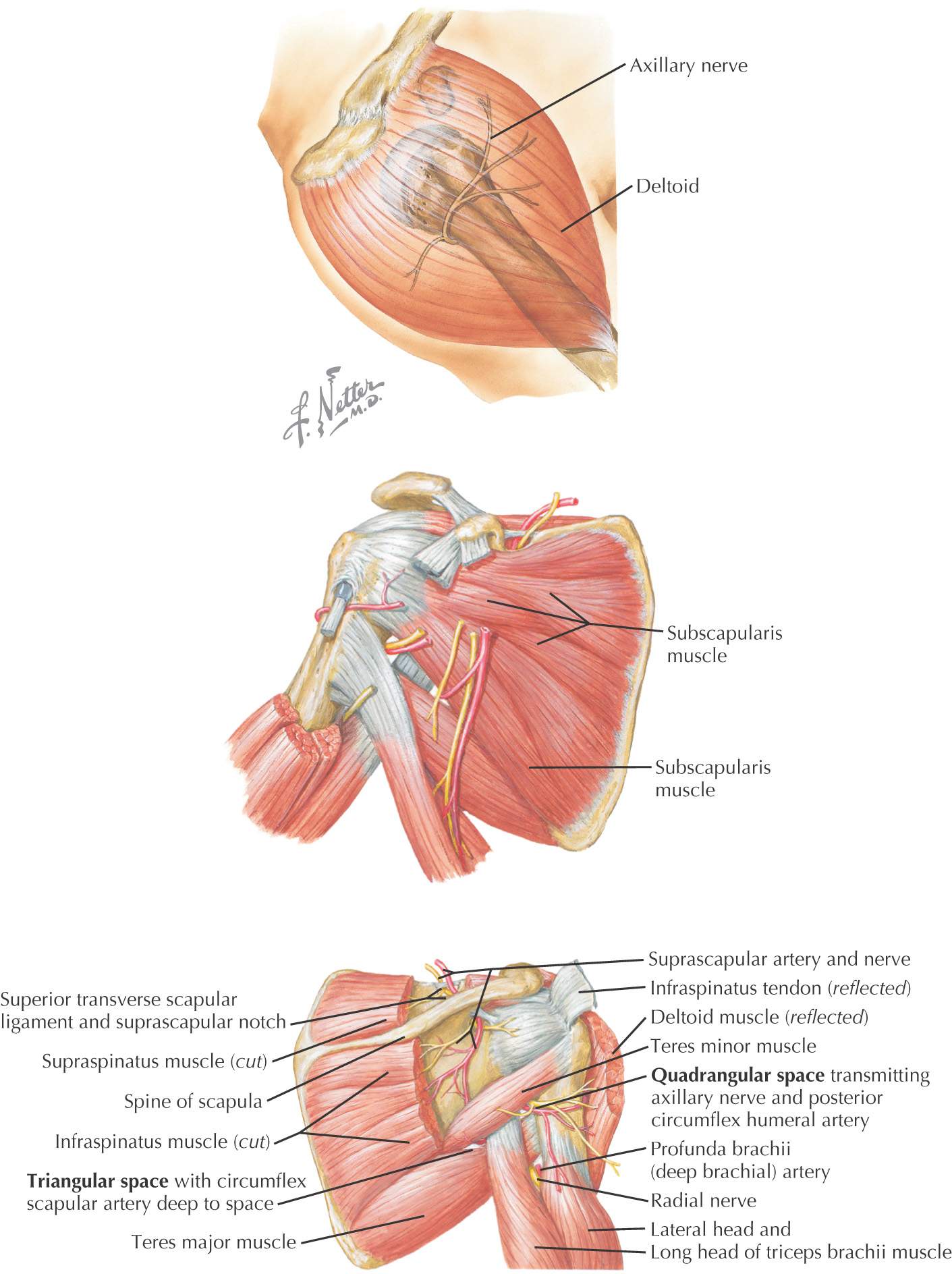
• Scapular circumflex—located in triangular space
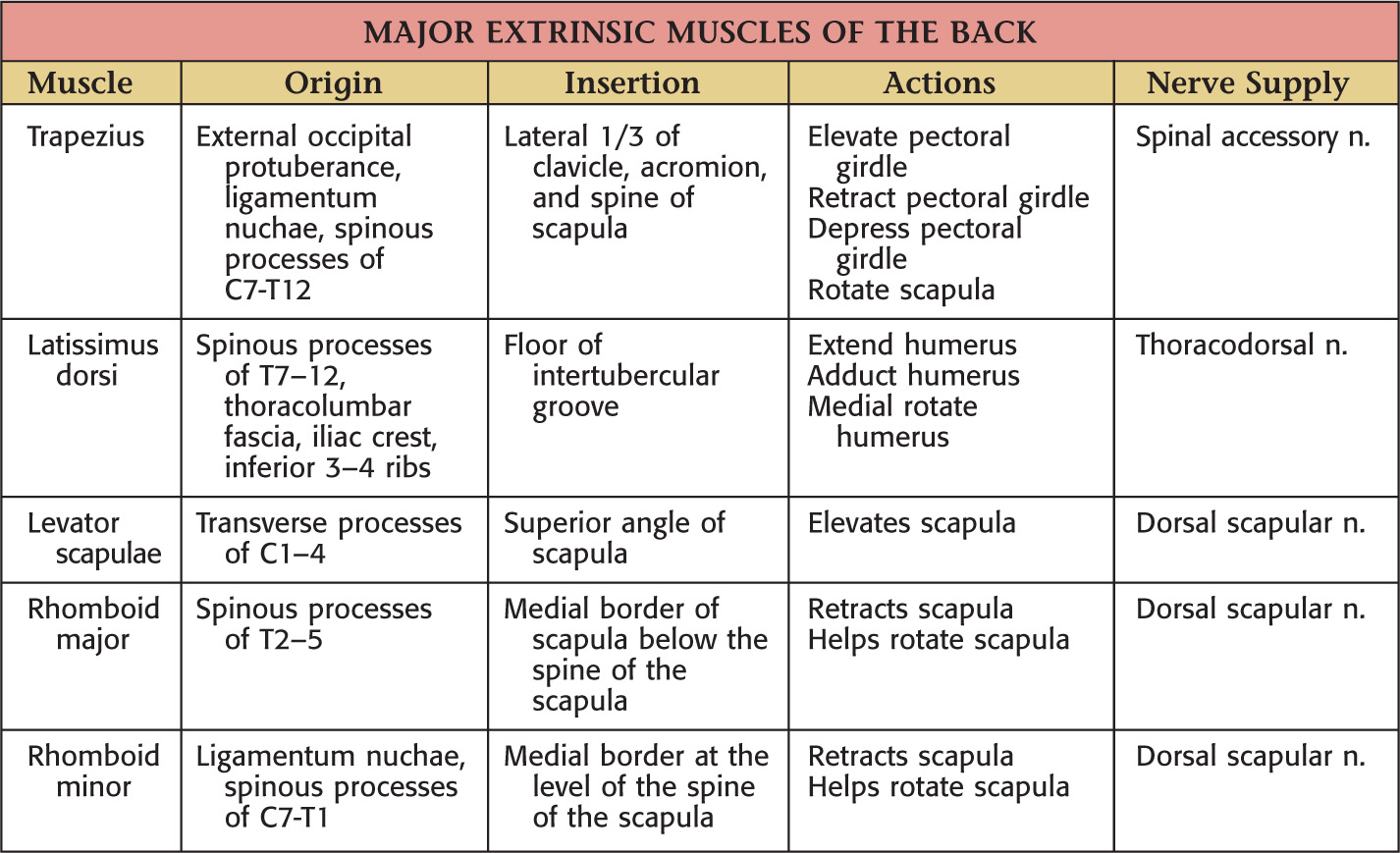
• Thoracodorsal—passes with thoracodorsal n. to latissimus dorsi
• Posterior humeral circumflex—travels in quadrangular space with axillary n.
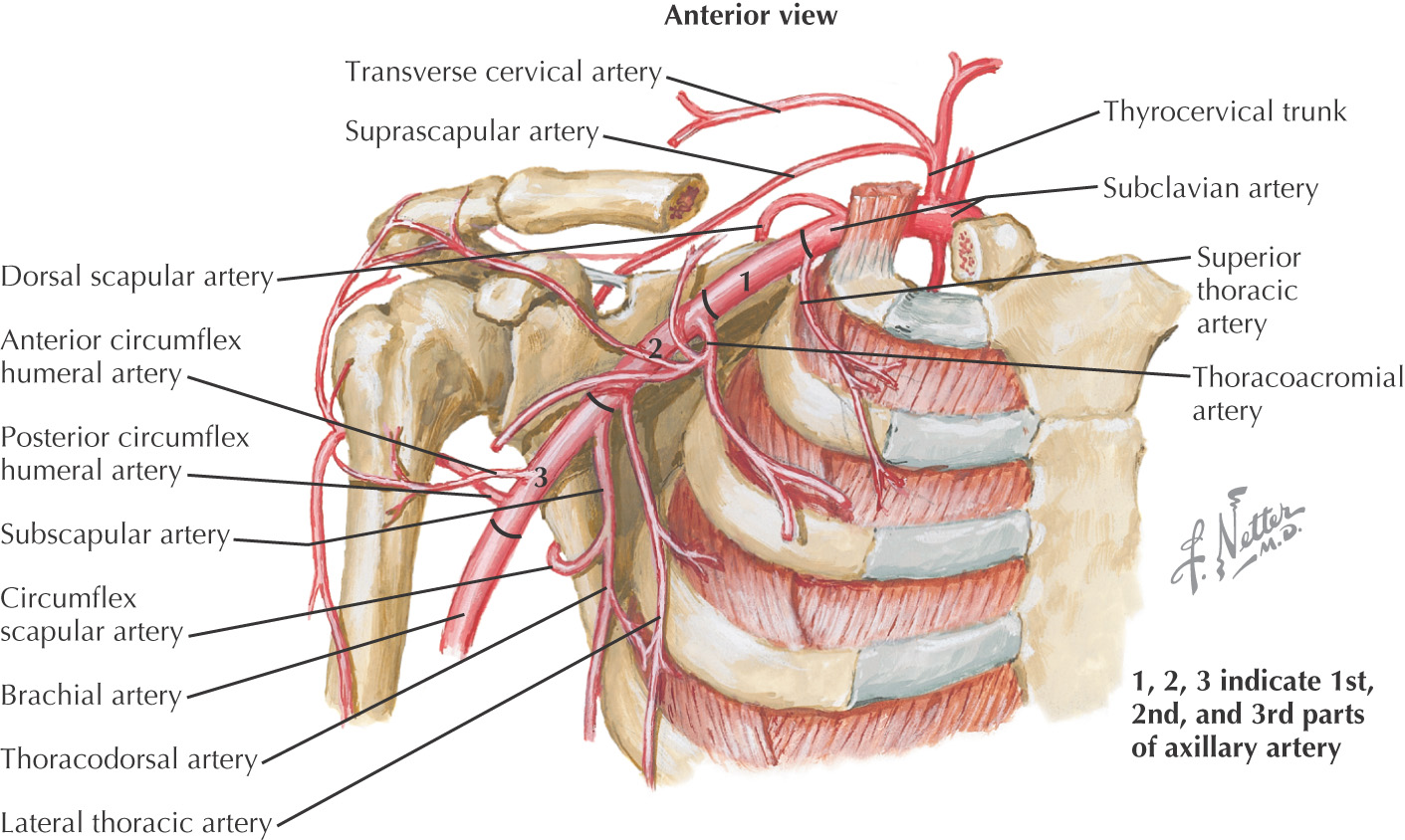
Brachial—begins at inferior border of teres major
• Superior ulnar collateral—passes with ulnar n. posterior to medial epicondyle
Brachial—divides into:
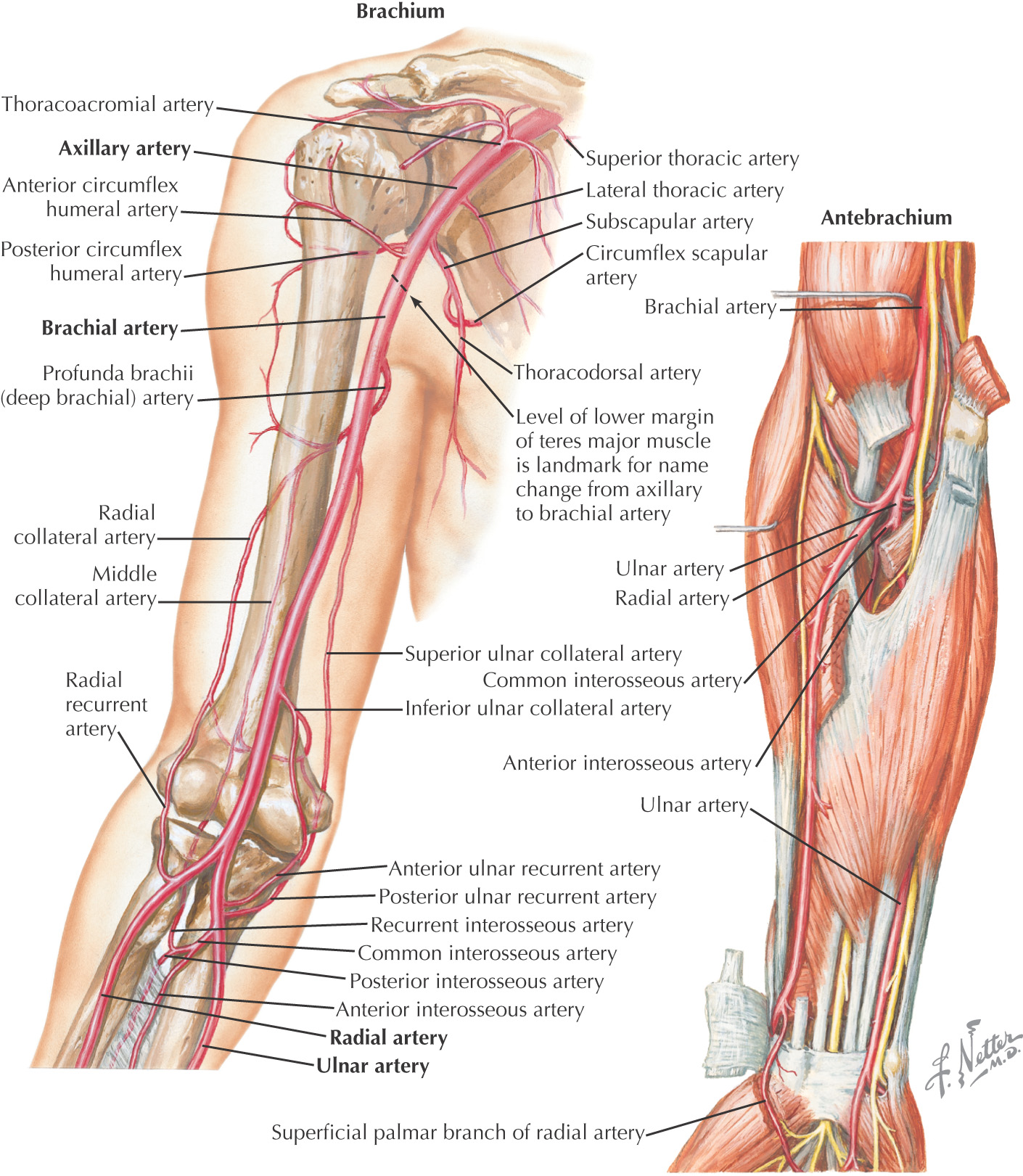
Ulnar
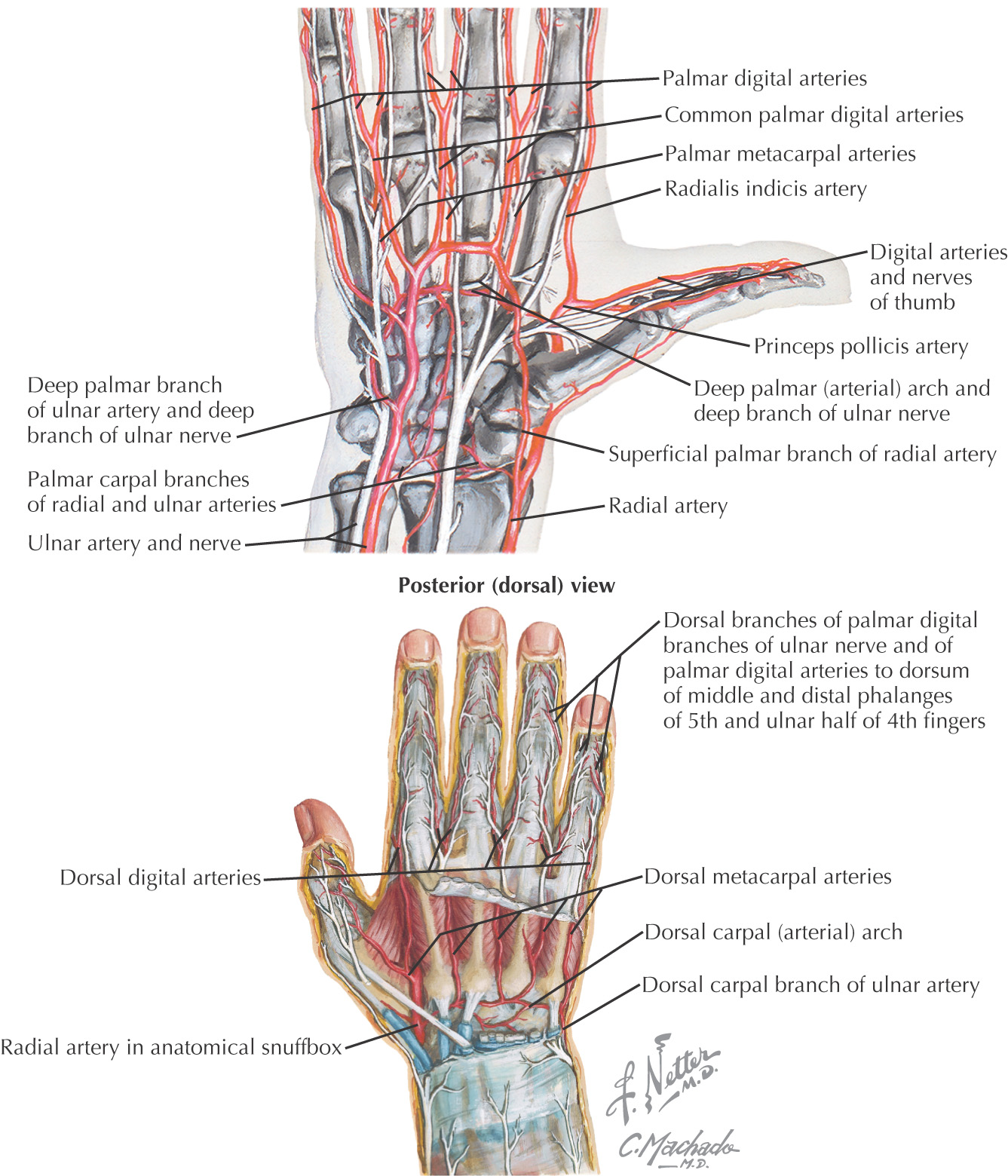
Radial
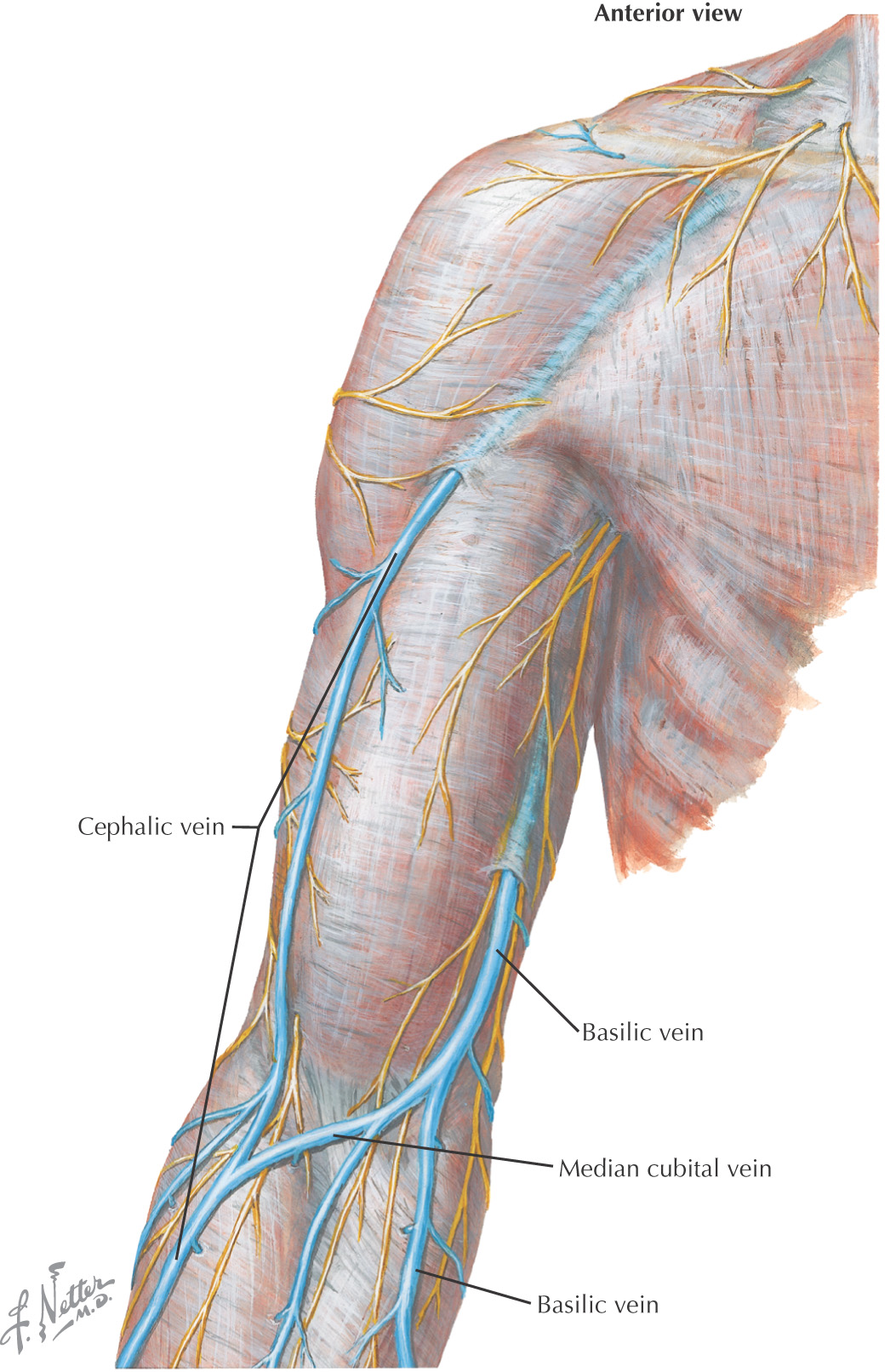
Two types of veins:
• Superficial—lie in superficial fascia
• Single similar-sized vein following the artery of the upper limb (e.g., subclavian vein or axillary vein)
• Vena comitans—accompanying vein
• A pairing of veins with both surrounding the artery
• Typically any veins that are distal to the axillary v. is a vena comitans (e.g., brachial veins, ulnar veins, and radial veins), which are paired around the artery of the same name
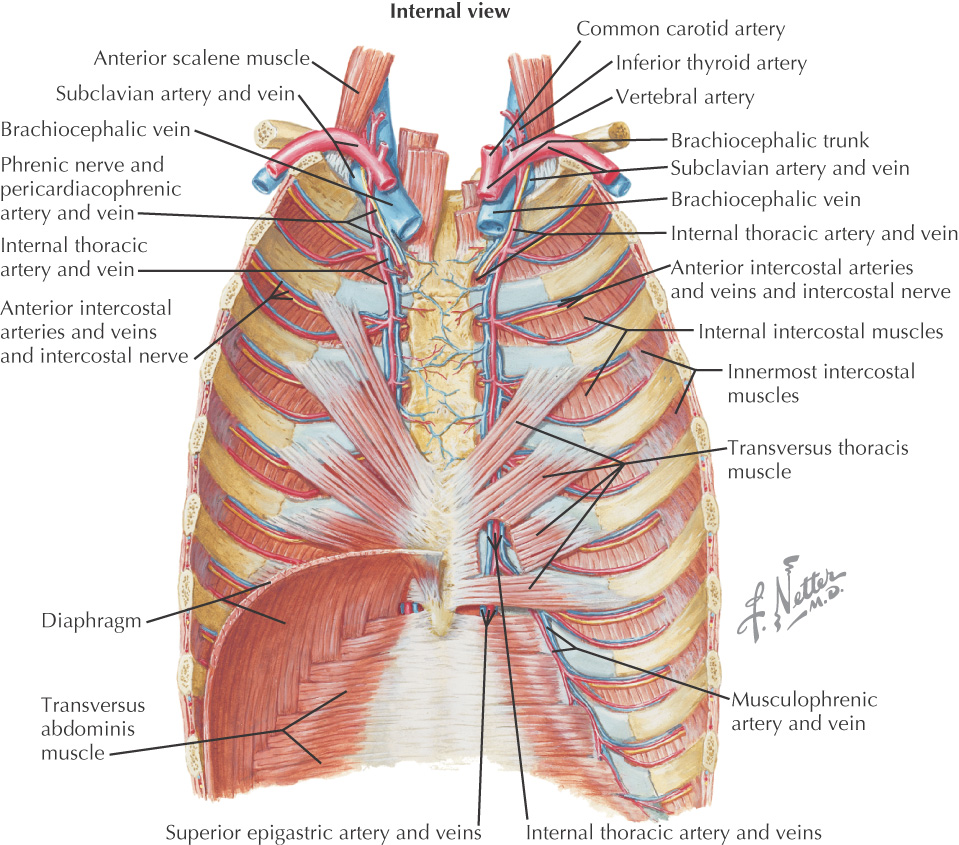
• Internal thoracic—arises from subclavian a.
• 1 Subcostal (thoracic aorta)
• Right (3rd posterior intercostal a.)
• Right supreme intercostal v.
• Right superior intercostal v.
• Left superior intercostal v.
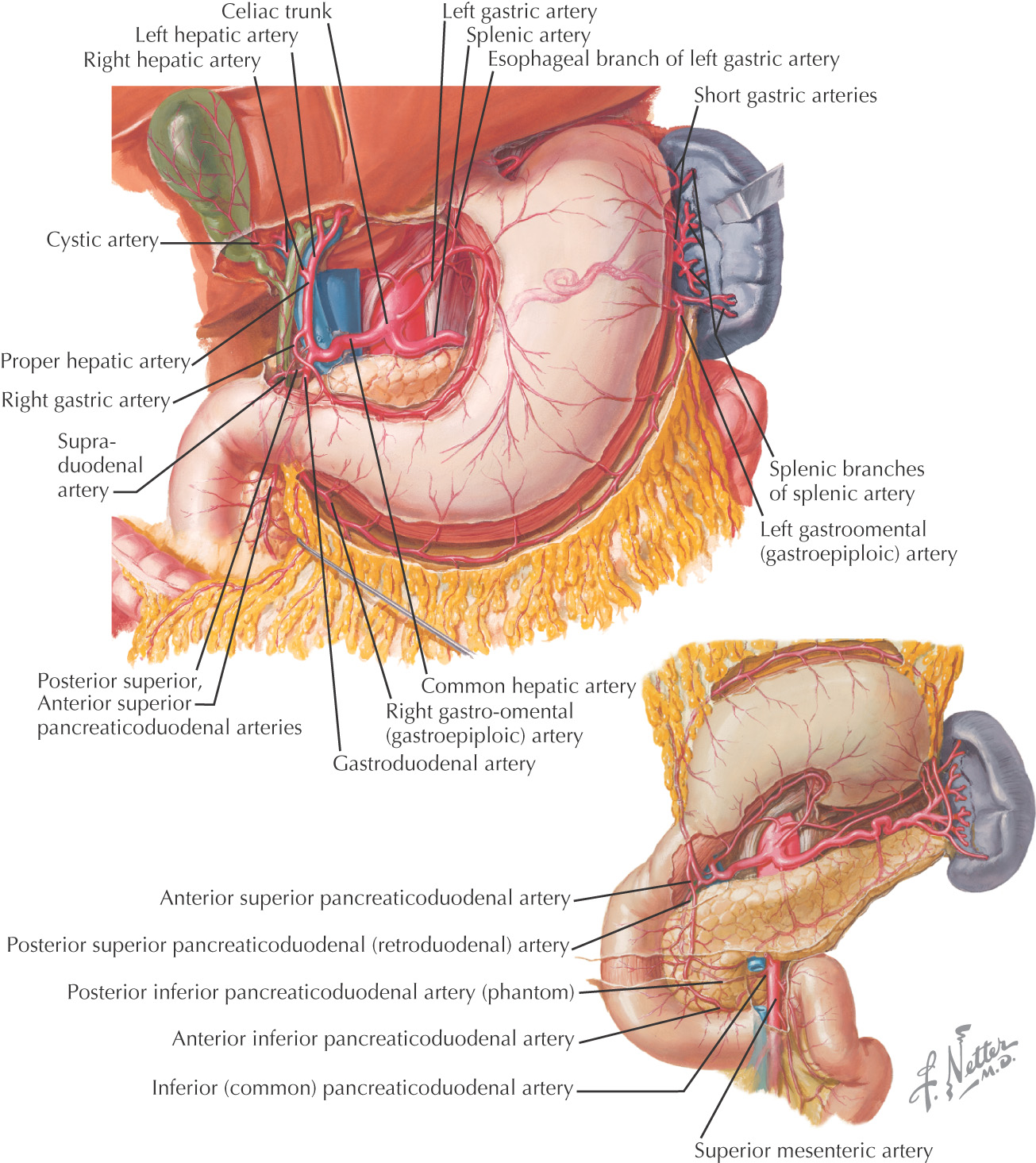
Celiac Artery (Artery of the Foregut)—arises at T12
• Anterior and posterior superior pancreaticoduodenal
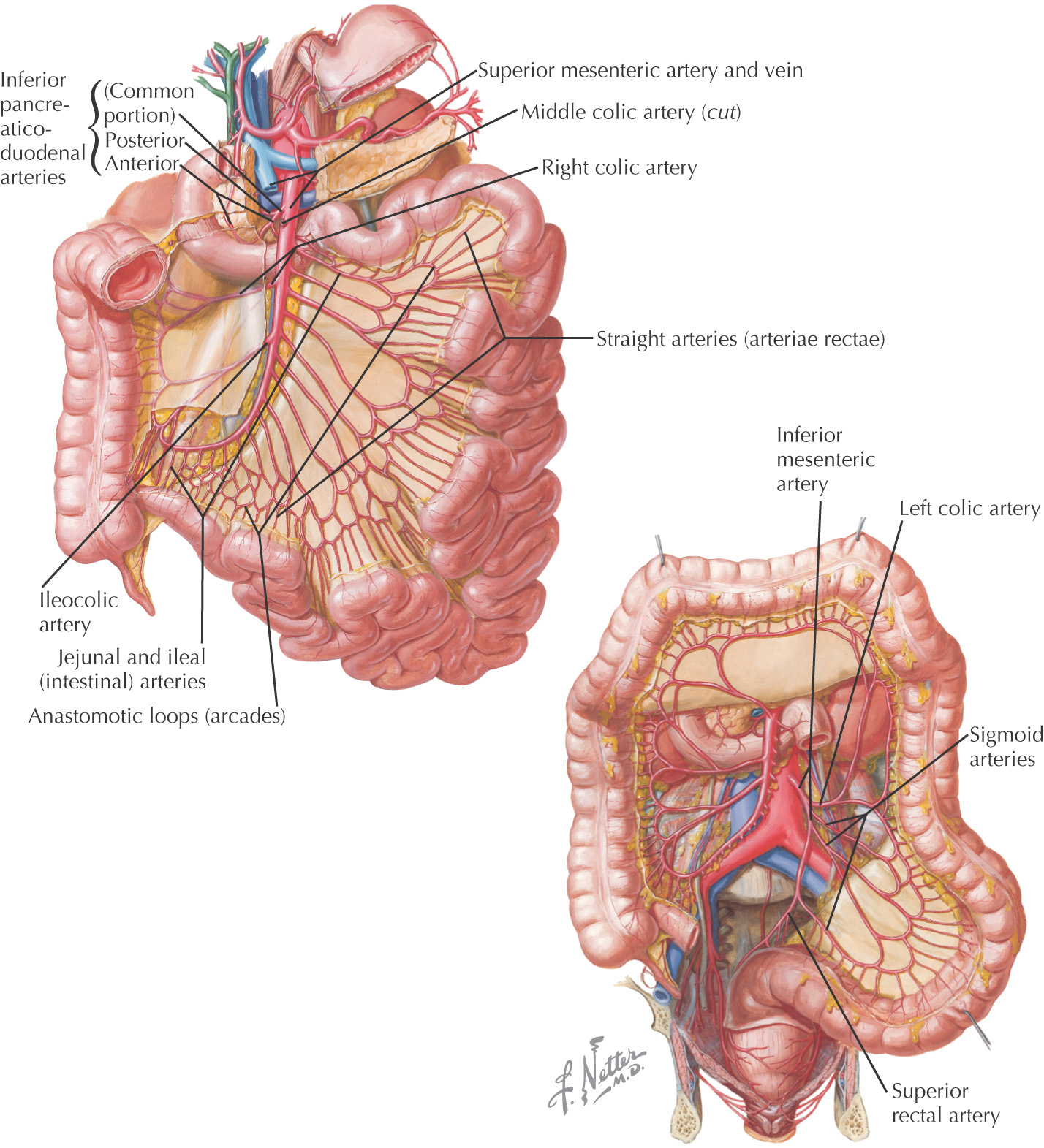
Superior Mesenteric Artery (Artery of the Midgut)—arises at L1
• Anterior and posterior inferior pancreaticoduodenal
• Arterial arcades and vasa recta
• Arterial arcades and vasa recta
Inferior Mesenteric Artery (Artery of the Hindgut)—arises at L3
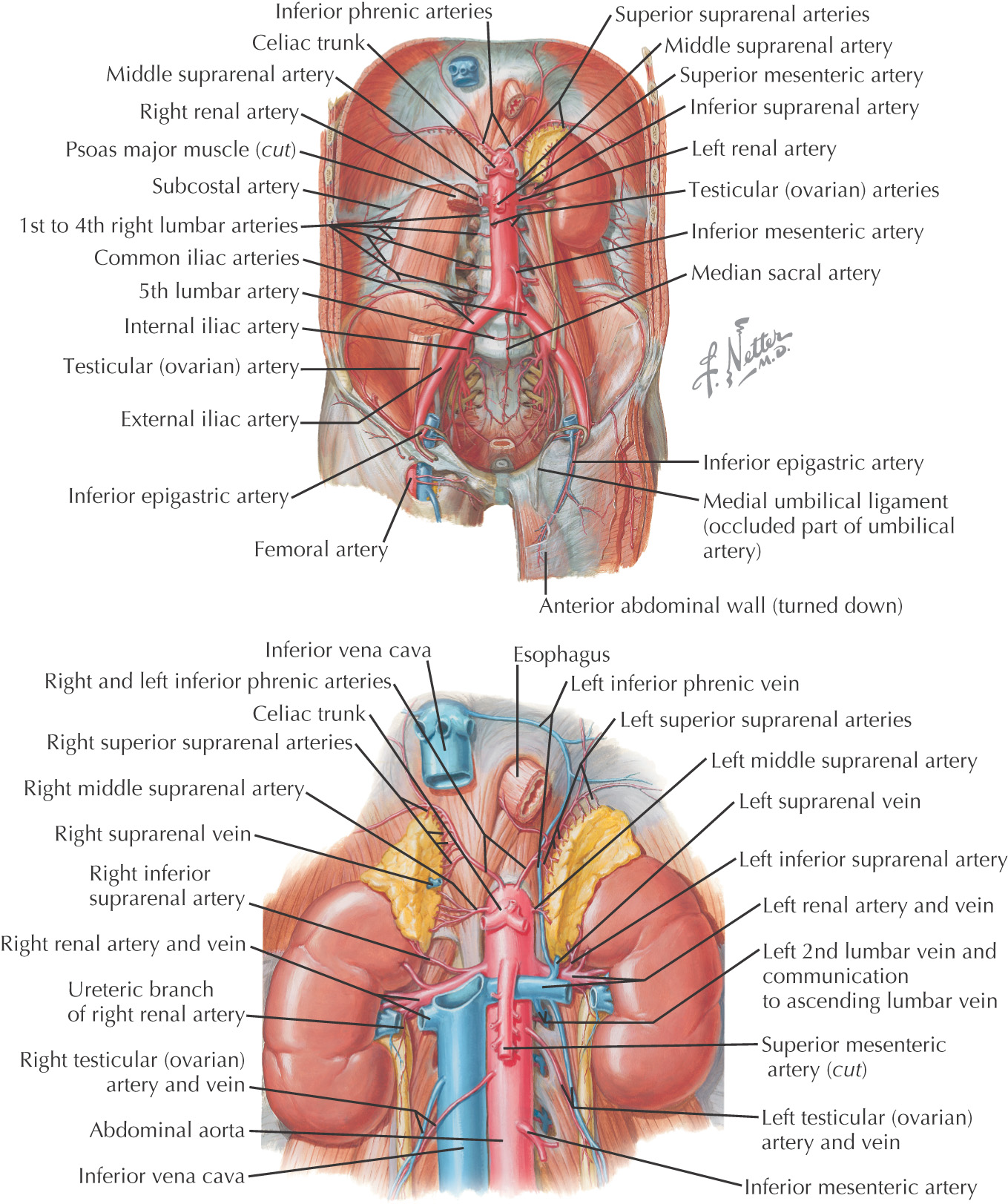
Paired Visceral Branches—paired branches supplying organs
• Gonadal—arises between L2 and L3
• Superior—arises from the inferior phrenic
• Middle—arises from the aorta
• Inferior—arises from the renal
Paired Parietal (Body Wall) Branches—paired branches supplying the wall
• Lumbar—4 arise from the aorta
Veins that drain the abdominal viscera closely follow the celiac, superior mesenteric, and inferior mesenteric arteries
These veins eventually drain into the hepatic portal vein, which passes into the liver, allowing the liver to clear the blood of any wastes and to store nutrients
The hepatic portal vein is formed by the:
After passing through the liver, the blood returns into the systemic system via hepatic veins into the inferior vena cava
Since the veins in this region lack valves, they take the path of least resistance
If there is an obstruction in the path of the hepatic portal vein, the blood will attempt to return the blood toward the heart by bypassing the block and utilizing anastomosis between the portal system and the systemic system (vena cava)
There are 4 major collaterals between the portal and systemic systems:
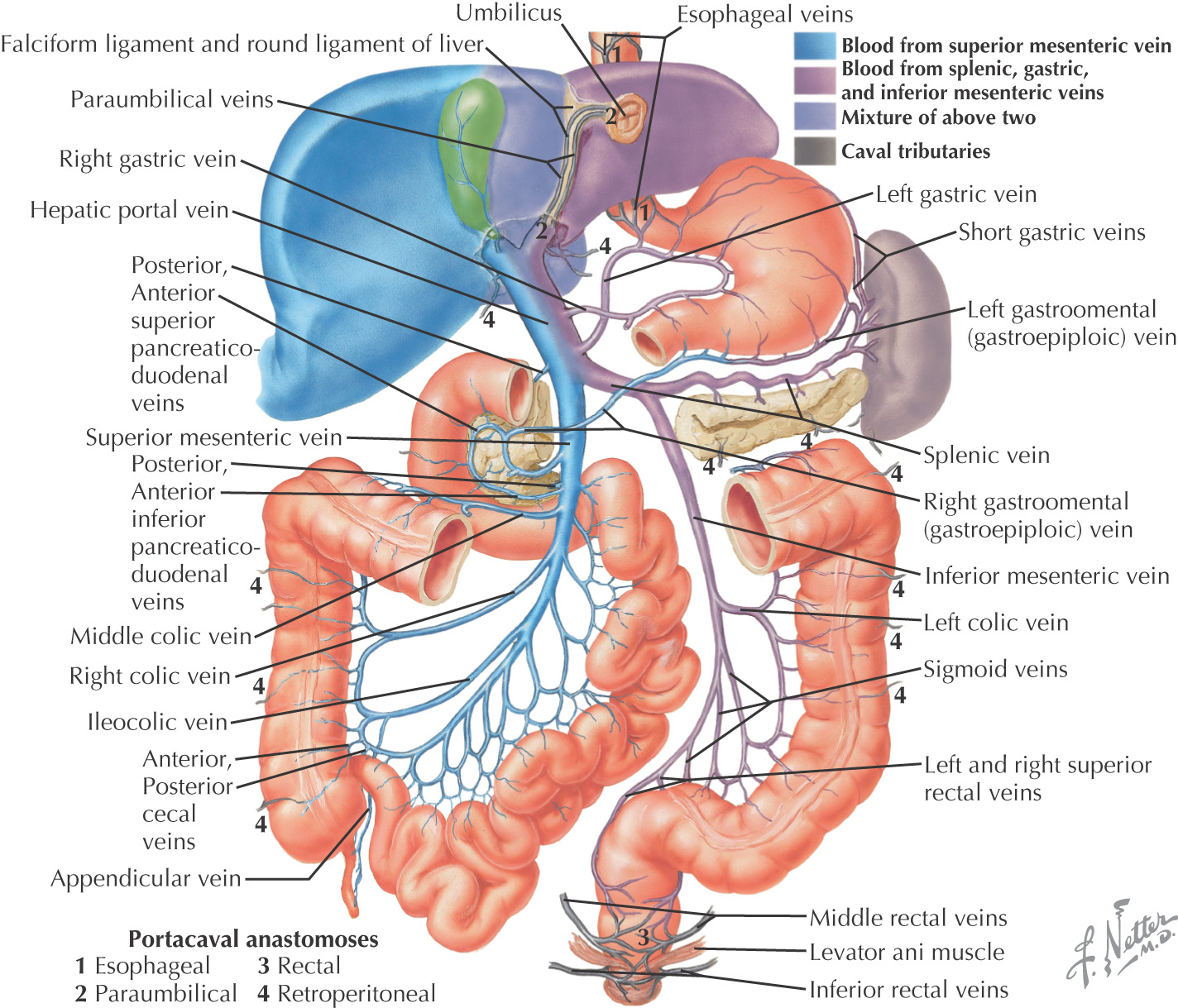
• Minor direct tributaries include:
• Posterior superior pancreaticoduodenal v.
• Anterior superior pancreaticoduodenal v.
• Anterior inferior pancreaticoduodenal v.
• Posterior inferior pancreaticoduodenal v.
• Inferior mesenteric—sometimes joins to form hepatic portal v.
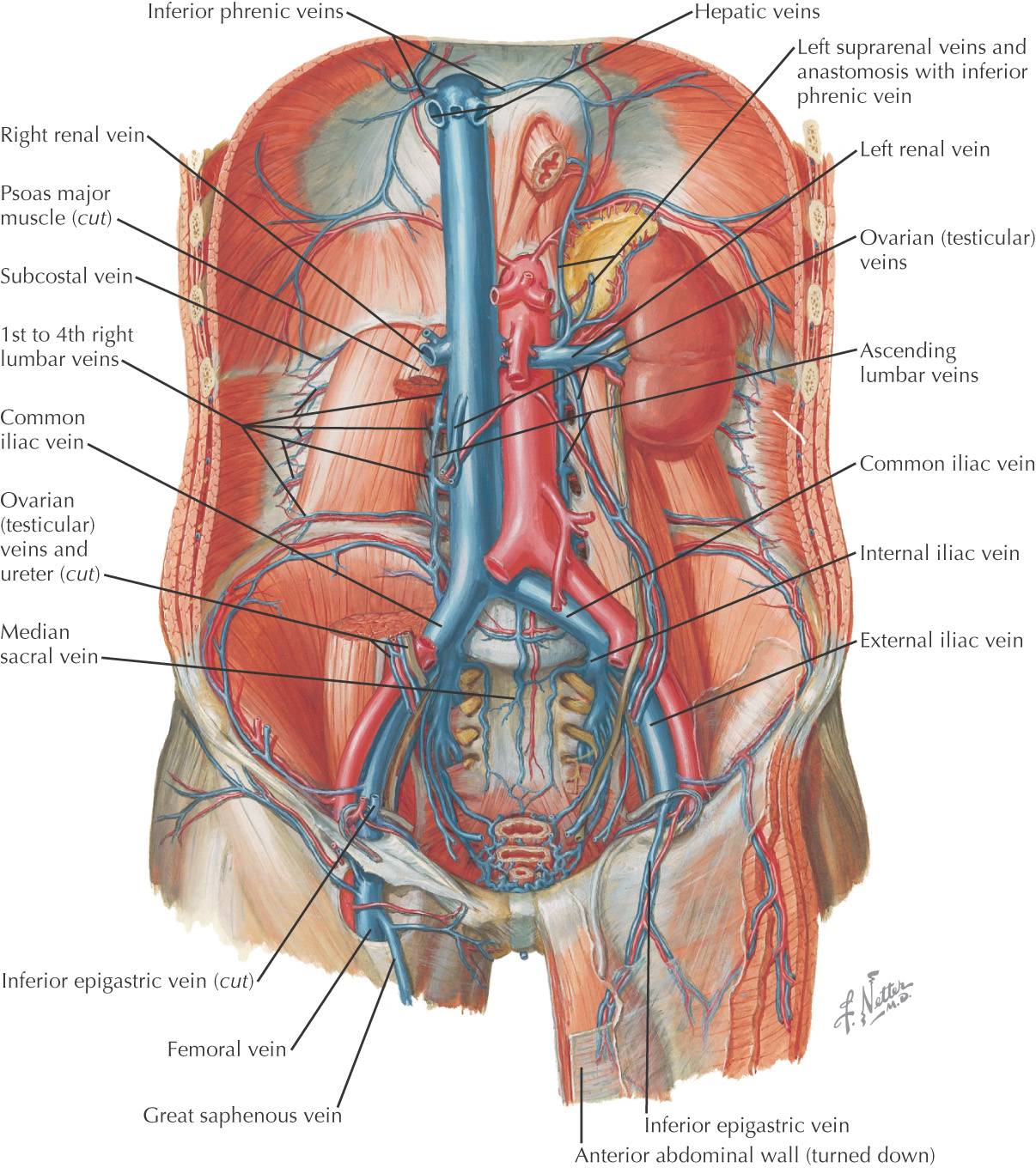
Veins of the posterior abdominal wall drain into the inferior vena cava
Tributaries include:
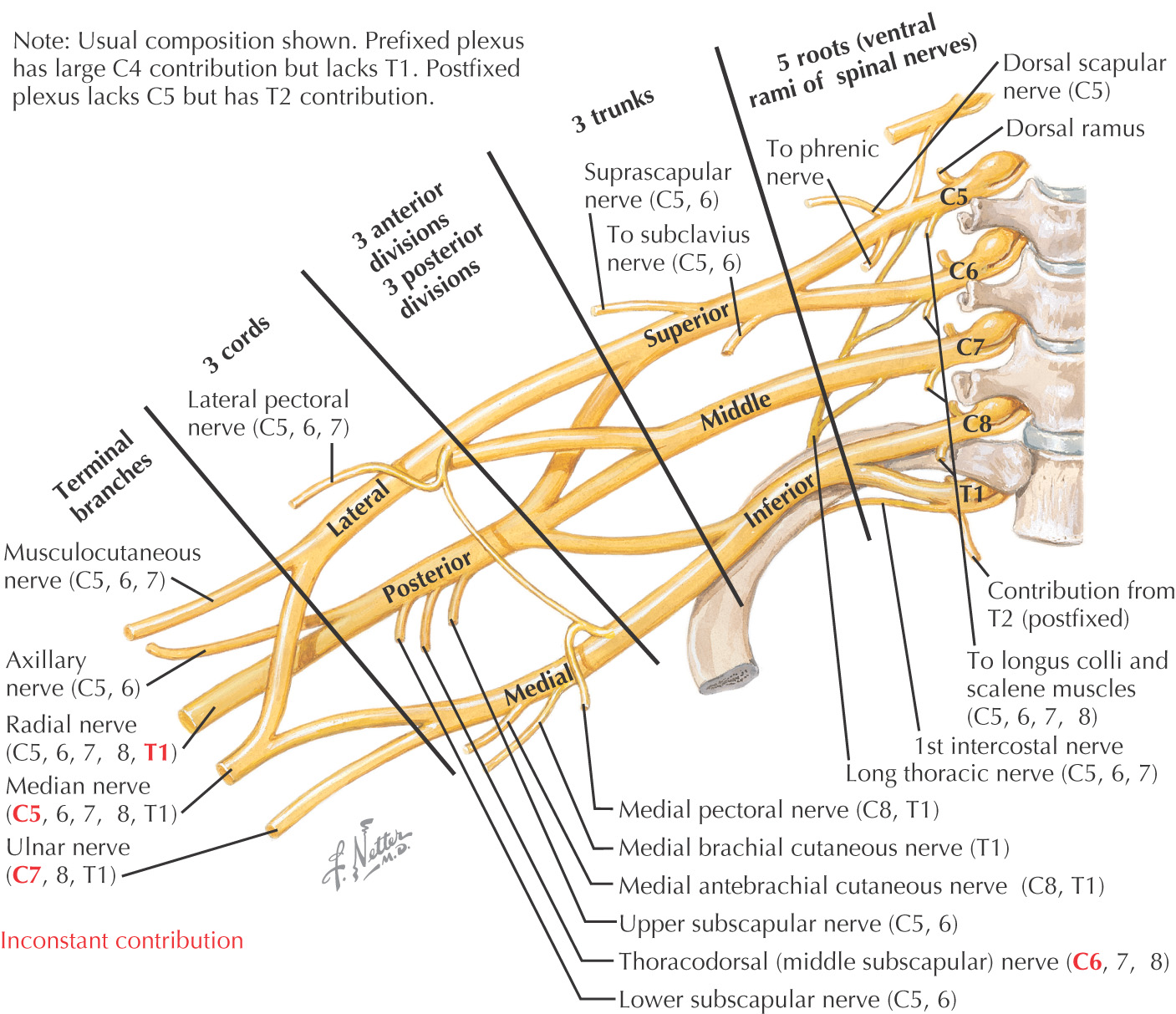
Alternating joining and branching of nerves to reorganize the terminal branches with contributions from multiple spinal cord levels
Origin from ventral rami of 5th to 8th cervical and 1st thoracic spinal nerves
General organization is:
Nerves to muscles on ventral and dorsal surfaces of upper limb are derived from anterior and posterior divisions, respectively.
Location and arterial relations:
• Rami and trunks—Posterior triangle of neck—Subclavian a.
• Divisions—Behind clavicle—Subclavian and 1st part of axillary a.
• Cords—Axilla—2nd part of axillary a.
• Branches—Axilla—3rd part of axillary a.
Key landmark of “M” formed by medial and lateral cords and terminal branches
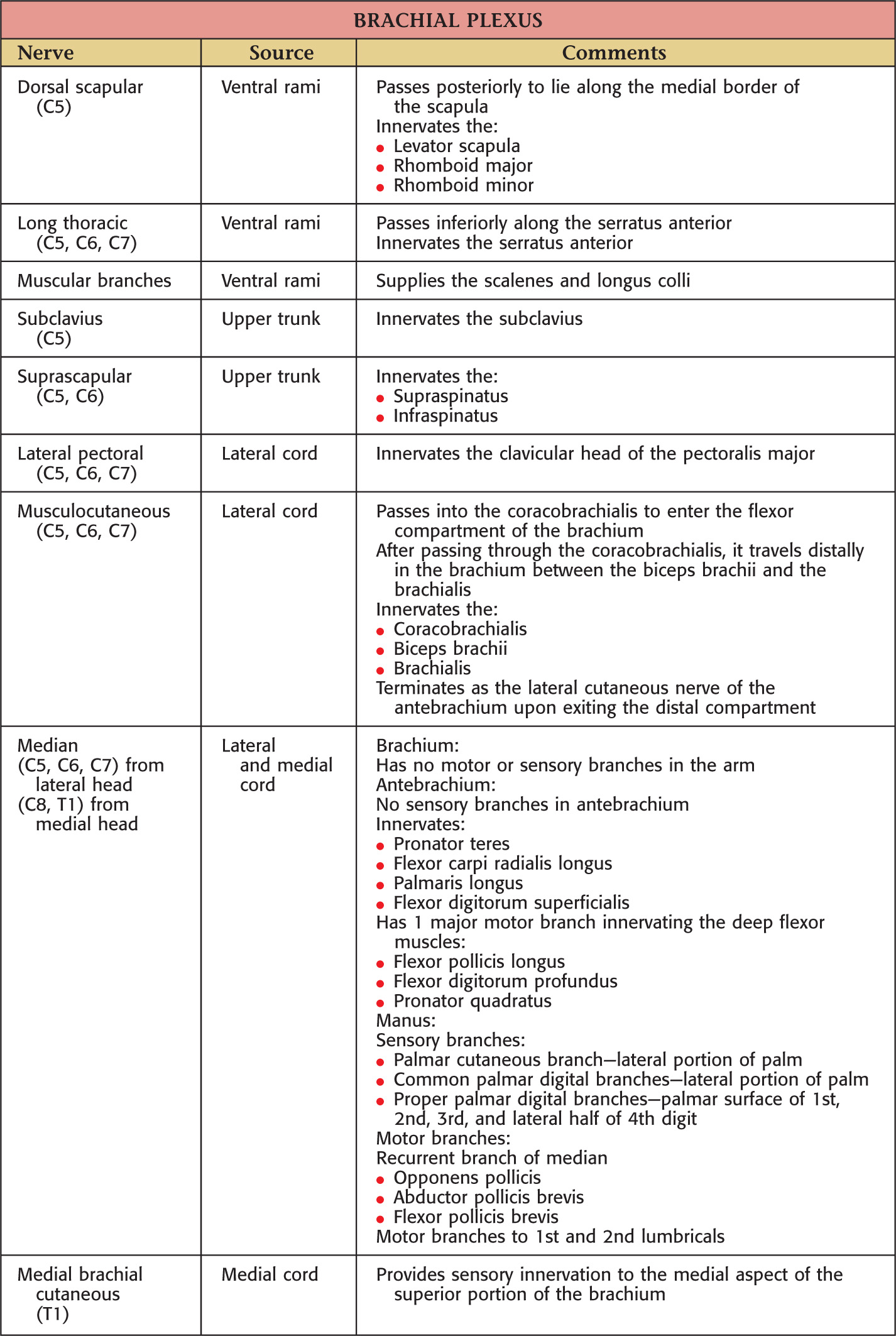
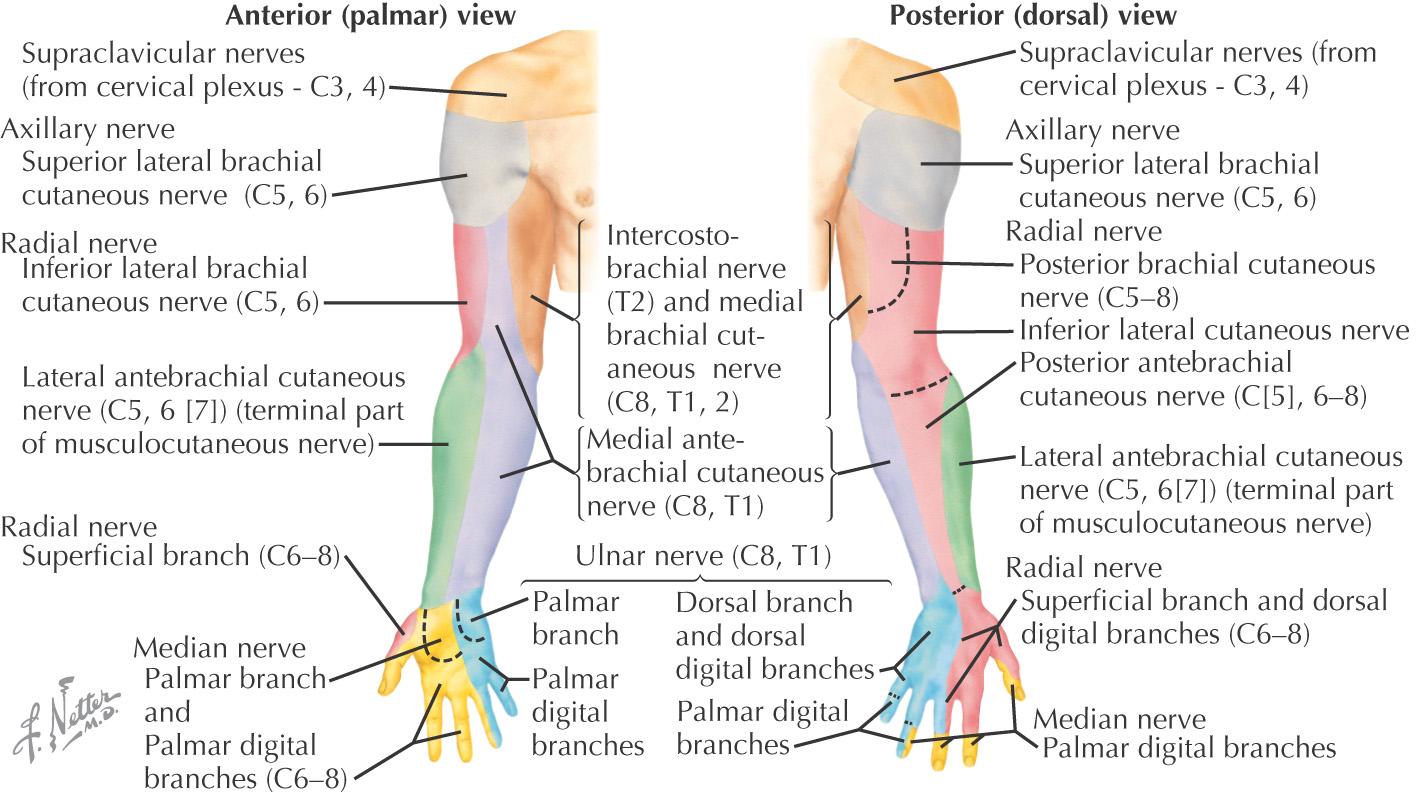
Nerves
• Lateral femoral cutaneous nerve—L2, L3