16. The evolving theory of clinical reasoning
Carolyn A. Unsworth
Overview
This chapter explores clinical reasoning in occupational therapy. It provides an overview of the development of clinical reasoning in occupational therapy, definitions of the different types of clinical reasoning, and explains how acquisition of expertise is promoted through clinical reasoning. A major review of clinical reasoning research is then presented. While it has long been established that clinical reasoning enables therapists to integrate theory into practice, the final section of the chapter examines the process of theory development and maps this against developments and research growth in the area of clinical reasoning in occupational therapy. Hence, this chapter builds an argument that clinical reasoning is developing into a theory.
• Clinical reasoning has been studied by occupational therapy researchers since 1982. Clinical reasoning is distinct from clinical decision-making.
• Many types or modes of clinical reasoning have been identified and described, including narrative, procedural, interactive, conditional, ethical and pragmatic reasoning.
• One of the hallmarks of expertise is the therapist's ability to reason rapidly and intuitively. The clinical reasoning of an expert is deeply internalized, and the therapist can draw appropriately on relevant ideas, solutions or information from an extensive knowledge bank and range of experiences.
• There have been over 30 empirical studies conducted to investigate the clinical reasoning of occupational therapists. Qualitative and quantitative findings from this research are slowly building a picture of occupational therapy reasoning.
• Clinical reasoning is evolving into a theory in its own right. Research evidence to support the evolving theory of clinical reasoning is slowly assembling. Further studies that build on existing work, organize this phenomenon into a conceptual framework and empirically test this framework are urgently required.
Introduction
In 1983, Schön (p.42) penned the following analogy:
In the varied topography of professional practice, there is a high hard ground in which practitioners can make effective use of the research-based theory and technique. Moreover, there is the swampy lowland in which situations are confusing ‘messes’ incapable of technical solution. The difficulty is that the problems of the high hard ground, however great their technical interest, are often relatively unimportant to clients or to the larger society, whereas in the swamp, the problems of greatest human concern are found.
This chapter welcomes you to the swamp!
The way we think and reason, in essence, makes us who we are as individuals. Furthermore, groups of people who come together for specific purposes often share patterns, modes and constellations of thinking and reasoning. As a professional group, occupational therapists share a mode of thinking and reasoning that is quite particular and quite different from that of other health professionals. Of course, many elements and aspects of this thinking are shared with other clinicians, but it is the way the thinking is constructed and how this reasoning enables our theories of human occupation to be practised that is unique. Writing about clinical reasoning in occupational therapy today is commonplace, and all of the introductory texts and compendia in the profession include material on clinical reasoning. Furthermore, I would guess that all occupational therapy education programmes internationally include some training or exposure to the idea of clinical reasoning. However, clinical reasoning has only been described in our profession over the past 25 years or so. Although the idea was first brought to the attention of therapists by Rogers and Masagatani, 1982 and Rogers, 1982 and Rogers’ Eleanor Clarke Slagle lectureship the following year (1983), it was not till the American Journal of Occupational Therapy released its special edition on clinical reasoning in November 1991, and Mattingly and Fleming published their text, Clinical Reasoning: Forms of Inquiry in a Therapeutic Practice, in 1994 that the idea of clinical reasoning entered mainstream practice and became the buzz word of the early 1990s. News of this concept spread rapidly around the occupational therapy world, and there was an ‘ah-ha’ moment as the profession collectively recognized clinical reasoning as a way of naming and explaining all the hidden elements of practice that were so essential in the art (as opposed to the science) of occupational therapy practice. Early scholarly activities investigating clinical reasoning revealed that our thinking was indeed special and unique, and construction of a language to describe the tacit as well as overt elements of practice commenced. But what exactly is clinical reasoning? How does a therapist do it? What can make a therapist better at it? Some ideas to answer these questions are provided in this chapter, commencing with the first section, which provides an overview of what clinical reasoning is.
What is clinical reasoning?
Issues in arriving at a definition
It is not easy to put forth a simple definition of clinical reasoning, since this is quite a complex construct. To start, we must acknowledge that clinical reasoning is also described in the occupational therapy literature as ‘therapeutic reasoning’ (Kielhofner & Forsyth 2002), ‘professional reasoning’ (Schell & Schell 2008) and ‘occupational reasoning’ (Rogers 2010). All of these are also excellent terms. The terms ‘professional reasoning’ and ‘therapeutic reasoning’ acknowledge that occupational therapy practice is not confined to the clinic. Using the term ‘occupational reasoning’ ensures that our thinking is targeted to the ‘systematic method of thinking about the occupational engagement of humans that supports the occupational therapy process’ (Rogers 2010, p.57). But renaming the clinical reasoning rose does not make it smell any sweeter. Therefore, while this chapter adopts the traditional term that is so easily recognized, the reader is asked to consider that other terms can also be used.
The second issue to raise, before a definition is offered, concerns the intertwined nature of clinical reasoning and clinical decision-making. In discussing reasoning and decision-making in occupational therapy practice, Harries and Duncan (2009) observed that, in the occupational therapy literature, clinical reasoning tends to be used to cover all the thinking processes that involve reasoning, problem-solving judgement and decision-making. These authors go on to present material on two theories of judgement and decision-making from cognitive psychology, cognitive continuum theory (Hammond & Brehmer 1973) and dual-processing theory (Stanovich & West 2000), and show how these theories can further our understanding of occupational therapy practice. Harries and Duncan describe how, within dual-processing theory, two thinking systems are outlined that have been shown to be neurologically different (Goel et al 2000). The S1 system, as it is called, is a fast automatic form of processing. Through the S1 system, judgements are largely tacit. On the other hand, the slower and more deliberate S2 system is more analytical, focuses on one task at a time, and considers the outcome of different decisions from a more objective basis. The S1 system is more focused on the art of clinical reasoning, and the S2 on the science of objective decision-making. Ideally, we need both these elements in a successful clinical practice, and we need to explore both literatures to gain an understanding of what these approaches offer us. However, it is beyond the size and introductory nature of this chapter to explore both these concepts. This chapter focuses on the more context-dependent, phenomenologically grounded clinical reasoning. Texts that delve deeper into clinical reasoning in the allied health literature include those by Schell and Schell (2008) and Higgs et al (2008). The chapter will refer to, but not describe, decision-making in any detail. To gain an appreciation of the full complexity of the science of judgement and decision-making, the reader is referred to Klein et al., 1993 and Dowie and Elstein, 1988 or Hardman (2009).
Definition of clinical reasoning
It is hard to be succinct when defining clinical reasoning. The Oxford Dictionary defines reasoning as ‘the intellectual faculty by which conclusions are drawn from premises … [and] to reach conclusions by connected thought’ (Thompson 1995, p.1144). But this definition does not convey the scope or complexity of clinical reasoning in occupational therapy. Higgs and Jones (2000, p.11) define clinical reasoning as ‘a process in which the clinician, interacting with significant others (client, caregivers, healthcare team members), structures meaning, goals and health management strategies based on clinical data, client choices, and professional judgment and knowledge’. In occupational therapy, clinical reasoning can be defined as the reflexive thinking associated with engaging in a client-centred professional practice. This includes the thinking when planning to be with the client (and their caregivers and other health professionals), when the therapist is with the client and afterwards when reflecting on time with the client. Clinical reasoning draws on empathy, intuition, judgement and common sense. Clinical reasoning is constantly changing in response to a multitude of hidden and overt influences and contextual factors, which may be inhibitory or enabling. Clinical reasoning plays out in the occupational therapist's mind in narratives and images (adapted from Unsworth 1999). Within the clinical reasoning construct, many modes or types of reasoning have been identified. These are described in the next section of the chapter.
A language to describe the modes of clinical reasoning
Cheryl Mattingly (a medical anthropologist) and Maureen Fleming (an occupational therapist) worked with a large team of experts, including Gilette, Schön and Cohen, to conduct the first large-scale enquiry into the clinical reasoning of occupational therapists. The American Occupational Therapy Foundation funded a study between and 1986 and 1988 involving 14 therapists at a 900-bed acute care facility in a large city in the USA. The two major findings of the study were an understanding of the practice cultures that occupational therapists work within and the beginnings of a language to describe the modes of reasoning used by occupational therapists (Mattingly & Fleming 1994). Many refinements and additions have been made to this framework, but the fundamental ideas laid out in Mattingly and Fleming's text provide the foundation for understanding clinical reasoning in occupational therapy. The language that has now developed in occupational therapy in the field of clinical reasoning has been drawn from medicine, philosophy, anthropology and sociology.
An overview of these different modes of clinical reasoning and related terminology used in the field are provided below, and Table 16.1 provides a detailed examination of the language of clinical reasoning in occupational therapy. The third column in the table provides an example of how this language might be used in clinical practice in the narrative (first-person) form. The use of narrative examples to illustrate how therapists reason is now quite popular in occupational therapy texts. Mattingly and Fleming's text came to life through the use of these narratives, and several occupational therapy writers have since adopted this approach to illustrate texts with both what and how a therapist thinks (see, for example, Unsworth, 1999, Kielhofner, 2008 and Crepeau et al., 2009). This approach helps students and novice therapists to learn both what a particular therapy technique is, and, very importantly, what a therapist thinks as they engage in practice.
| Mode of thinking | Description (and examples of researchers who coined/use this term) | Clinical example |
|---|---|---|
| Narrative reasoning | The use of storytelling and creation to explore therapy. Used when therapists work in a more phenomenological practice sphere where the emphasis is on the meaning of the client's illness and illness experience (Mattingly & Fleming 1994) | Robyn enters the hospital's allied health staff lunch room and flops into a chair. Her colleagues, Dana, Matty and Pip, are already there. Pip observes that Robyn looks exhausted. Robyn replies: ‘I've just been working with the new lad. He's only four, but he spent the whole session wailing for his mum. The puppets caught his attention for a few minutes and I made a start but that was about it. His leg muscles are so tight, but I'm sure the [tendon release] surgery will make a huge difference in the long run … I just need to find what will turn on the light and get him interested and motivated. I'm going to try and call his mum later and get some more information from her …’ |
| Scientific reasoning | The process of hypothesis generation and testing that generally is referred to as hypothetico-deductive reasoning. Used to make a diagnosis of the client's medical condition. Although more concerned with identifying the client's occupational problems rather than the medical diagnosis, therapists do draw on the ideas of scientific reasoning when reasoning procedurally (Schell & Cervero 1993) | Saran reports on her initial assessment of 73-year-old Peter at the team meeting. ‘I assessed the new client, Peter, yesterday in terms of ability to complete personal ADLs. I found him to be independent with verbal supervision for all tasks such as toileting, showering, dressing and grooming. He plans to return to his home without any support and use public transport to get to the shops, visit his doctor and do his banking. Given what I observed yesterday, I doubt he will be independent in all these activities by next week. I will commence an IADL assessment today, and intervention will aim at facilitating his independence and also putting local community supports in place.’ |
| Diagnostic reasoning | Used to identify underlying impairments or occupational performance issues, define desired outcomes, set goals, develop intervention/solutions (Rogers & Holm 1991) | Brian has been working in acute care for only a few months and has used a hypothesis testing approach (Unsworth 1999) to determine the underlying cognitive impairments that are limiting his client's ability to make a cup of tea. ‘He presents as really confused, and so I was very cautious in putting everything out on the bench and I didn't have the water in the kettle any hotter than tap water. He started by breaking open the teabag and tipping the tea into the cup. Then he tipped in half the sugar from the sugar pot, played around with this for a while and then filled the cup with milk. Before the session, I was wondering what was going on and whether he had some complex perceptual problems. But over the session it became clear that he has ideational apraxia. This hypothesis fits with the fact that he has left brain damage as a result of the stroke and has quite severe receptive aphasia as well.’ |
| Procedural reasoning | The thinking associated with the procedural aspects of therapy, such as the evaluations and interventions to be used with the client, and how the client is performing. Procedural reasoning represents the more scientific components of practice, which include systematic data collection, hypothesis formation and testing (Mattingly & Fleming 1994) | Alex works on a stroke ward. His new client has cognitive and perceptual problems. ‘So I did a dressing assessment with Mr P this morning and the hypotheses were just flying around my head. He has so many cognitive and perceptual problems but hardly any physical ones … so I just watched him and tried a few things as we went. He looks as if he has a unilateral neglect and some short-term memory problems, as well as complex perceptual problems … but I've got to check for homonymous hemianopia too. So I'm just trying to work out which standardized assessments to do … maybe the RPAB [Rivermead Perceptual Assessment Battery] or LOTCA [Lowenstein Occupational Therapy Cognitive Assessment] and the BIT [Behavioural Inattention Test] … but I probably don't have enough time for all three, so maybe just the LOTCA and some confrontation testing to check for neglect versus homonymous hemianopia versus both.’ |
| Interactive reasoning | Concerned with how the therapist interacts with the client. Referred to as the underground practice by Mattingly and Fleming, since the therapists they studied were able to describe what they had done with the client but generally not their interactions. Therapists use interactive reasoning to engage the client in therapy, and consider the best approach to communicate with the client, to understand the client as a person, understand the client's problems from the client's point of view, individualize therapy, convey a sense of acceptance/trust/hope to the client, break tension through the use of humour, build a shared language of actions and meanings, and monitor how the treatment session is going (Mattingly & Fleming 1994) | Dana describes to her fieldwork student some of her interactive reasoning as she gets to know her clients during an initial interview. As Dana will get to know these clients over several months, she reasons that she has this time to use the initial interview to ‘go deep’. ‘So what I do is just start off with the initial interview structure but explore any directions the client's responses take me in. I don't want to limit this opportunity to get to know the client by sticking to the form, as the sooner I can get my head around understanding who this person is and what makes them tick, the better the therapy plans we make will be. I try to keep it light and friendly so the client feels at ease and that it's an open and sharing environment. If there is an opportunity to share a joke I will … or if the client becomes upset or distressed, then I take time to support them through this and slowly we move on. I guess what I'm aiming for is to get the clients to see me as someone who is going to be useful in their recovery and someone they can trust.’ |
| Conditional reasoning | Takes into account the whole of the client's condition, as the therapist considers the client's temporal contexts (past, present and future) and their personal, cultural and social contexts. Hence, this type of reasoning is used when trying to understand what is meaningful to the client in their world by imagining what their life was like before the illness or disability, what it is like now and what it could be like in the future (Mattingly & Fleming 1994) | Maryella is reflecting on a session with Joseph, a 5-year-old boy with developmental delay. She started by interviewing Joseph and then undertook Ayres Clinical Observation to examine his motor skills. She completed this assessment about 12 months ago as well. ‘So I did this assessment last year and I haven't seen Joseph for over 6 months since his family moved away for his Dad's work. Now they're back so I'm just checking on where Joseph is up to with school and socially, and how he feels about coming home and so on. So we've had a chat and I can really tell he's made a lot of good gains. He's a bit anxious about starting back at his old school, so I've been reassuring him about that and now I'm just using Ayres Clinical Obs assessment to run through his current performance. He's made some nice gains over the time he's been away; he has more core trunk stability and I can really see changes compared with the last time I saw him in terms of balance, righting reactions and even fine motor coordination. I think we can work on some more advanced goals now with him, such as …’ |
| Ethical reasoning | The thinking that accompanies analysis of a moral dilemma where one moral conviction or action conflicts with another, and then generating possible solutions and selecting action to be taken (Rogers, 1983 and Barnitt and Partridge, 1997) | Alan had a head injury and attends a day therapy programme as an outpatient. His therapist, Kate, reflects on the fact that Alan takes illegal drugs (Unsworth 2004b): ‘So Alan still lives in his parents’ house, but he can't stay there much longer, and they want him out. Alan takes drugs and I find it a real dilemma. I have to help him find other housing, but he shares his drugs around, and I'm really worried that if I help him find a group home, then he could be putting other people at risk. I also feel really disappointed because he's made such amazing gains in therapy and he could do so much, but when he takes drugs he just loses all his cognition, basically. He just sits there and misses out on therapy, and it's a real shame. Sometimes I think the therapy I provide is going to waste … should I spend less time with him and more with my other clients who seem to make more gains? I try not to dwell on it but it's a bit disappointing, as if he didn't do drugs, then he could easily be living in a good home and making fantastic progress towards independent living and getting some part-time voluntary work. Anyway, it's his life and I try not to judge him. But I have to think some more about what kind of place he can live in so he doesn't put others at risk as well.’ |
| Generalization reasoning | Within the forms of procedural, interactive, conditional and pragmatic reasoning, therapists use generalization reasoning to draw on past experience or knowledge to assist them in making sense of a current situation or client circumstance. The kind of reasoning in force when a therapist thinks about a particular issue or scenario with a client, then reflects on their general experiences or knowledge (i.e. making generalizations) related to the situation, and then refocuses the reasoning back on the client (Unsworth 2005) | Max works in a short-stay residential facility, helping adolescents with intellectual disability to become more independent. ‘So Kate is making some good gains with her goal of grooming, which includes managing her long hair and doing some basic make-up. So often these kids have a kind of learned helplessness since their parents have often done everything for them. So with Kate, she asks for help all the time but really she can do it. So I think it's more about reassurance and just reinforcing what a great job she's doing. So that's what I'm focusing on with Kate in this session, supporting and reassuring her that she can do her hair and so on and that she's doing a great job.’ |
| Pragmatic reasoning/ management reasoning | Concerned with the therapist's practice and personal contexts. The practice context includes organizational, political environments and economic influences, such as resources and reimbursement. Personal context includes the reasoning surrounding the therapist's own motivation, negotiation skills, repertoire of therapy skills, ability to read the practice culture, and what Törnebohm (1991) described as life knowledge and assumptions (Schell and Cervero, 1993, Barris, 1987, Neuhaus, 1988 and Fondiller et al., 1990). Lyons and Crepeau (2001) labelled pragmatic (practice context) reasoning as management reasoning | Xui Sing works in community health with elderly clients living at home. ‘I really want to be able to provide my client, Mrs Beller, with an adjustable over-toilet frame, as I know her husband is having hip replacement surgery in 6 weeks and he's a lot bigger than her. So if I get an adjustable one, they can both use it. But our centre has just had a major policy change in equipment allocation, and I think I can only provide a seat that is a fixed height and suitable for her. Maybe they can afford to buy an adjustable one now, or maybe we'll have to worry about Mr Beller later when he has his surgery? I'll have to work out the best solution based on their needs now, their budget and what my centre can provide.’ |
| Embodiment | Our bodies, as well as our minds, gather a great deal of information as we work with clients. For example, we can smell if the client has not washed or if a wound is not healing well, and we use our sensation to feel the client's muscles and how their body moves. This is referred to as embodied knowledge and it is not always possible to put this knowledge into words. Although therapists have long recognized the importance of information from our bodies about our clients, the embodied nature of clinical reasoning is a relatively new area for research in occupational therapy (Schell & Harris 2008) | Helen describes how she knows when an autistic child begins to relax and settle into an activity. ‘Well, if I describe a typical client, then I could tell you about Paul. So let's say I've started with a warm-up activity outside climbing the rope ladder and swinging on the bars, so it's a gross motor activity using major muscle groups. And that's really helpful, so that when he comes inside I might then start with a large weighted floor puzzle. This kind of “heavy work”, with lots of joint compression seems to help kids like Paul to relax. And as he's moving the puzzle, I can see his whole body kind of slows and I can place my hands over his back or at his hips, and feel the tension releasing and his muscles relaxing.’ |
| Worldview | Defined in philosophy as ‘a global outlook on life and the world’ (Wolters, 1989 and Hooper, 1997). Worldview is the influence of the therapist's personal context on clinical reasoning. While some writers describe pragmatic reasoning as incorporating this personal context (e.g. Schell & Cervero 1993), others view this as a separate factor which has an impact on reasoning rather than being a separate form of reasoning (e.g. Unsworth 2004a) | Asher describes his worldview. ‘Well, I suppose my worldview makes me who I am, and I guess it colours everything I think and do. It's about my faith and what values I hold and my sense of right and wrong. Sometimes I'm aware of it but mostly I'm not. I guess I have to think about what my worldview is, when I'm confronted with it being different from the client's. It's times like these I really have to work at not making judgements about the client but try to see it from their point of view or try to accept that it's OK to have that particular worldview. When I have OT fieldwork students, they find this hard at times. Often you can't solve the dilemma for them, but at least you make them aware of what the problem is — in other words, you can at least look at it objectively for what the problem is, and also see that it's normal to have to work at understanding these issues and resolving or making peace with these differences.’ |
| Intuition | Defined as the ‘knowledge of a fact or truth, as a whole; immediate possession of knowledge; and knowledge independent of the linear reasoning process’ (Rew 1986, p.23). Within Cognitive Continuum Theory, Hammond (1996) posits that cognition can be ordered on a continuum from intuition to analysis | Fiona reflects on the development of her intuition and its value in her practice. ‘When I first started in mental health, working with depressed clients, I would have done A, B and C as I was taught and expected to do by others in the team. But now I'm 8 years on, and I do so many things differently based on that experience. And I'm really comfortable with what the A, B, C is, and I can see where it will work and where it will need to be changed. And I just trust my intuition. When I was new at this job, I didn't have the same “feel” or gut instinct for clients that I have now. But now I can just sense when something isn't quite right or when the client is going downhill … even if that isn't what they're telling me. And I trust this intuition.’ |
| Reflection | Involves reviewing performance and examining it in detail by relating it to past knowledge and experiences and relating it to future action, to enhance understanding. There are several types of reflection, including reflection about past experiences (reflection on action), reflecting in the present (reflection in action) and looking forward or anticipatory reflection (reflection for action). Reflection is a bridge to link theory and practice (Schön, 1983, Alsop and Ryan, 1996 and McKay, 2009) | Akhmed describes the value in setting aside time for reflection in his practice. ‘Each week I try to put some time aside on Friday to go back over the week and identify the highlights and low points, and I reflect on what worked well and the problems … both working with clients and with other staff. I don't keep a journal but some of my colleagues do. But I try to make some notes about events and feelings, and use this time to think about doing things differently or better. Then I also have professional supervision once a month, and I identify something from these “Friday reflections” to really go into more detail … and I find these sessions really useful. My mentor really pushes me to think about the issue from so many different angles and I use her approach when I'm thinking back over the week on my own.’ |
Narrative reasoning and chart talk
Mattingly documented how occupational therapy was a profession that sat comfortably between two practice cultures, and therefore described occupational therapy as a ‘two body practice’ (1994, p.37). On the one hand, occupational therapists work within a biomedical framework. Even when therapists do not work in a medical setting, our profession is primarily concerned about the relationship between health, occupation and well-being. Therefore, our concern with health connects us to medicine and a biomechanical understanding. Occupational therapists also have their own professional practice culture, which operates in the social, cultural and psychological sphere that is concerned with the client's experience of the illness and the meaning of the illness (Mattingly 1994). Usually, a biomechanical or scientific approach (the body as a machine) does not sit well alongside the more phenomenological sphere (the lived body). However, in occupational therapy, these two seem to make perfect sense. As Mattingly (1994) notes, occupational therapists seemed to have the ability to shift rapidly and easily between thinking about the client and the disease process and resulting occupational performance issues (for example), and developing an understanding of the person and the client's experience of the illness.
When therapists are thinking and working in a biomechanical sphere, they use chart talk to present information on the client and discuss evaluation and intervention issues. Hence, chart talk is generally used when the occupational therapist is talking about the client's medical problem, or writing case notes using brief and factual language. This kind of communication fits well in the biomedical world. However, when working in the more phenomenological practice sphere, occupational therapists use narrative reasoning to tell the story of therapy (Mattingly, 1994 and Unsworth, 2004a). Storytelling is never static. Stories can be told of the past and of the present and created for the future. Stories can be rewritten and changed mid-stream. Hence, thinking in narratives fits perfectly with the ever-changing therapy environment.
The therapist with the three-track mind
While narrative reasoning may be described as a core form of reasoning, Fleming (1994) went on to develop the idea of ‘the therapist with the three-track mind’ (p.119). The therapist with the three-track mind describes three dominant modes of reasoning found in the clinical reasoning study and confirmed in more recent research (Alnervik and Sviden, 1996 and Unsworth, 2004a). Fleming argued that therapists use these different kinds of reasoning when working in the different practice spheres. Therefore, procedural reasoning, which is similar to the problem-solving or hypothetico-deductive approach used in medical enquiry, fits well in the biomechanical sphere. The other forms of reasoning described by Fleming, interactive reasoning and conditional reasoning, fit more readily in the phenomenological or meaning making practice sphere (Fleming 1994). These forms of reasoning are all defined and described in Table 16.1. However, it is important to note how intertwined these are throughout the therapy process. Mattingly and Fleming (1994) described how the perspective gained from reasoning in one track might inform reasoning in another. This idea, that the different forms of reasoning interact and overlap, has been supported in subsequent clinical reasoning research (Unsworth 2004a).
Other modes of clinical reasoning and related terms
Early clinical reasoning researchers, such as Rogers and Masagatani, 1982 and Barris, 1987, as well as researchers following in the footsteps of Mattingly and Fleming, have also contributed terms to describe modes of clinical reasoning, or to describe constructs that fit with clinical reasoning. Some of these terms, such as ethical, scientific, pragmatic, generalization and diagnostic reasoning, and related constructs such as intuition, embodiment, worldview and reflection, are defined and illustrated in Table 16.1. It is important to note that some of these terms, such as procedural, interactive, conditional and pragmatic reasoning, fit better within an S1 or reasoning approach to understanding thinking processes. Other terms, such as scientific and diagnostic reasoning, fit better with an S2 approach.
Clinical reasoning and expertise
Differences between the clinical reasoning of novice and expert therapists
Research in occupational therapy on novice–expert differences has often portrayed this construct as a dichotomy. However, as described by Dreyfus and Dreyfus (1980) in their work on chess players and airline pilots, and then adapted for use in the health sciences by nursing researcher Benner (1984), expertise occurs on a continuum. It is now widely accepted that there are five phases one passes through on the journey from novice to expert, and these are novice, advanced beginner, competent, proficient and expert. It is also widely documented that increasing years of experience do not always equate with increasing expertise; some therapists never reach expert status but remain stuck at the level of competent or proficient practice (Benner et al., 1996, Gibson et al., 2000 and Unsworth, 2001). There have been several occupational therapy studies on the differences between novice and expert therapists (Hallin and Sviden, 1995, Strong and Gilbert, 1995, Robertson, 1996, Gibson et al., 2000, Unsworth, 2001 and Mitchell and Unsworth, 2005). One of the consistent findings from these studies and from studies of other health professionals is that experts think and reason differently from novices; experts know how (non-propositional or tacit knowledge) rather than know what (propositional or factual book-learned knowledge), their knowledge is embedded in action and experience, and much of their knowledge is automatic and intuitive (Dreyfus and Dreyfus, 1980 and Dreyfus and Dreyfus, 1986). Occupational therapy research in this area has revealed that, while novice and expert differences may be readily apparent, the differences between the other levels of expertise are not so apparent. Further research is required to help us identify the hallmarks and key reasoning patterns at each of the three mid-phases (advanced beginner, competent, proficient) so we can aid therapists who are ‘stuck’ at a particular level to move forward on their journey to expertise.
One of the goals of an occupational therapy educational programme is to ensure that students exit with the skills, tools, behaviours, attitudes and reasoning abilities needed to be excellent occupational therapists. Therefore, educators use novice–expert research findings to help students and novices to gain insights into expert thinking so they may hasten their journey on this continuum. However, expertise is not a point of arrival but rather a lifelong quest. This is because expertise is heavily context-dependent and a clinician who excels in one field of practice, such as psychiatry, may have novice skills only in working with clients who are recovering from stroke. In addition, clinicians who have attained expert status in a particular context must continue to expand and hone skills on their quest for professional excellence. Hence, novices and experts alike can benefit from undertaking an activity that has been shown as a key to enhancing clinical reasoning, and that is reflection.
Enhancing clinical reasoning skills through reflection
Reflection, as described in Table 16.1, is concerned with reviewing one's performance and examining it in detail by relating it to past knowledge and experiences and relating it to future action, to enhance understanding. Reflection is often referred to as the bridge that links theory and practice (Schön, 1983, Alsop and Ryan, 1996 and McKay, 2009). It is essential that all therapists, novices as well as experts, have the time and opportunity to reflect on practice both alone and with a supervisor or mentor. Reflective activities designed to enhance clinical reasoning include storytelling, pre-briefing and debriefing, reflective questions after working with a client, reflective journal writing, reviewing critical incidents with a mentor, participation in discussion groups, and videotaping and viewing sessions with clients. Additionally, activities with a reflective partner can also be helpful; together therapists can note significant similarities and differences between clients with similar disease processes or occupational performance issues and consider how these differences can influence treatment (Alsop and Ryan, 1996 and McKay, 2009). Therapists who take the time to reflect nurture their clinical reasoning skills, thus promoting excellent practice.
A review of empirical research on clinical reasoning in occupational therapy, 1982–2009
There have been over 100 journal articles, book chapters and books on clinical reasoning in occupational therapy written over the past 25 years. The sheer quantity of musings and research in this area reflects the value that our profession places on clinical reasoning and the commitment made to exploring and understanding it. While the reflective discussions and information presented in a lot of the writing on clinical reasoning provide a raft of ideas for research, this section of the chapter details the evidence or the empirical research published on clinical reasoning in occupational therapy. Occupational therapy practice requires a sound evidence base (Holm 2000). Evidence-based practice may be defined as the judicious use of evidence to make sound decisions about practice. Therefore, decision-making, thinking and reasoning are at the heart of putting evidence into practice. Occupational therapy urgently needs more empirical studies on clinical reasoning, so we are confident that we are judicious in putting the best evidence into practice. Hence, research into clinical reasoning where data were collected with occupational therapists and analysed in some way, either qualitatively or quantitatively, is summarized below. As a result of this process, we can more easily identify where work has been done, and clearly see how this can be built upon as we continue the mammoth task of exploring and understanding clinical reasoning in occupational therapy.
The literature between 1983 and 2009 was searched using the following databases: Medline, CINAHL, AMED and OTDBASE. The key terms used were ‘clinical reasoning’ or ‘reasoning’ or ‘thinking’ combined with ‘occupational therapy’. Reference lists of articles retrieved and many of the recent books or book chapters on clinical reasoning in the health professions were then searched by hand. Articles were included in the review if they met the following criteria:
1. They researched an element of clinical reasoning and hence the words clinical reasoning were included in either the title or abstract.
2. They were published in a peer-reviewed journal.
3. They included a sample that involved at least one occupational therapist.
4. Data analysis was undertaken.
5. Results were presented and a discussion on the findings was included.
Furthermore, articles were excluded if:
1. They focused on how to teach clinical reasoning to students.
2. They researched reasoning used or required in a particular area of practice and where the focus was on the area of practice.
3. They researched clinical decision-making rather than reasoning processes.
Hence, several of the articles by Maureen Neistadt on teaching clinical reasoning (see, for example, Neistadt, 1987 and Neistadt and Atkins, 1996) were excluded, while studies such as McKay and Ryan's (1995) work on the clinical reasoning used by students on fieldwork was included. Research examining the scientific decision-making processes of occupational therapists (S2 rather than S1 reasoning) was excluded, such as my own work (e.g. Unsworth et al 1995, Unsworth & Thomas 1993, Unsworth et al 1997, Unsworth 2007), and research by Priscilla Harries (e.g. Harries and Harries, 2001 and Harries and Gilhooly, 2006) and Medhi Rassafiani (Rassafiani and Ziviani, 2006 and Rassafiani and Ziviani, 2008). Research examining how clinical reasoning can be used to manage a particular area of practice was also excluded (e.g. Fortune & Ryan 1996). The empirical studies that met the selection criteria are presented in Table 16.2.
| Key | ||||
| AJOT = American Journal of Occupational Therapy; AOTJ = Australian Occupational Therapy Journal; BJOT = British Journal of Occupational Therapy; DR = Disability and Rehabilitation; FOHPE = Focus on Health Professional Education; IJTR = International Journal of Therapy and Rehabilitation; OTJR = Occupational Therapy Journal of Research; OTHC = Occupational Therapy in Health Care; PRI = Physiotherapy Research International; SJOT = Scandinavian Journal of Occupational Therapy | ||||
| AUS = Australia; CAN = Canada; NZ = New Zealand; SA = South Africa; UK = United Kingdom | ||||
| Year | Author Journal | Aim Setting | Sample of OTs Country | Main finding |
|---|---|---|---|---|
| 1982 | Rogers & Masagatani OTJR | To describe the clinical reasoning used to decide client problem area and treatment goals. Acute care physical setting. Focus on Assessment Physical rehabilitation | n = 10 USA | Data were analysed qualitatively and a six stage model was developed to describe the therapists' reasoning processes: 1. search for medical information, 2. select standard assessments, 3. implement assessment plan, 4. define client problems, 5. specify treatment objectives, and 6. evaluate the assessment process. Noted that therapists found it difficult to articulate their thinking |
| 1987 | Barris OTJR | To explore and describe the assessment processes used by therapists Mental health | n = 19 USA | Initial assessments varied between therapists in terms of format and content. There is a great deal of routinization in decisions made |
| 1990 | Fondiller et al OTJR | To identify values that influence clinical reasoning in occupational therapy using qualitative research methods Recognized experts from a variety of settings | n = 9 USA | Participants answered a series of open-ended questions in response to a case study. Eighteen value statements were reported that influence clinical reasoning and these were placed in two groups: therapist-related statements and treatment-related statements. Concluded that the pervasive presence of values in clinical reasoning must be acknowledged |
| 1991 | Fleming AJOT | To answer the question of what is clinical reasoning in occupational therapy Acute care physical setting | N = 14 USA | Identified the two-bodied practice of occupational therapy: the ‘lived body’ or phenomenological approach vs. the ‘body as a machine’ or biomechanical approach to working with clients. Developed a language for clinical reasoning, including the therapist with the three-track mind: procedural, interactive and conditional reasoning |
| 1993 | Sviden & Saljo AJOT | To examine the ways in which professional education affects occupational therapy students’ perceptions and descriptions of patients’ non-verbal behaviour Educational setting | n = 13 Sweden | Students found it difficult to discuss individual cases in relation to newly acquired theoretical knowledge. It was concluded that students would benefit more from increased opportunity to analyse individual cases by means of theoretical knowledge, rather than increased instruction in theory |
| 1995 | McKay & Ryan BJOT | To investigate the use of narrative reasoning by an occupational therapy student and an experienced therapist No information provided | n = 2 UK | The expert and novice told different narrative stories; however, it was found that the student's story could be enhanced to include more narrative by asking probing and reflective questions |
| Sviden OTRJ | To examine the different methods in which occupational therapy students report how they would respond to patients’ non-verbal communication of affect Educational setting | n = 13 Sweden | Students’ comments showed evidence of change after 1.5 years of occupational therapy education, when compared with the beginning of their course. The change may be regarded as cognitive in nature because comments became more differentiated and organized | |
| Creighton et al AJOT | To investigate experienced occupational therapists’ clinical reasoning as they presented and modified therapeutic activities to treat their clients Spinal cord injury | n = 4 USA | Consistent with previous research, the therapists demonstrated multilayered thinking. However, hierarchical structuring of knowledge also emerged unexpectedly as a dominant theme in their reasoning | |
| Strong et al BJOT | To use nominal group techniques to ascertain the differences between novice and expert therapist reasoning Mixed settings, including hospitals, schools, paediatric care and psychiatry | n = 19 Australia | The study revealed that, when making clinical decisions, a wider range of factors was considered by experts than by students. Clinical reasoning was also rated to be at a higher level by experts than by students. The factors identified by the experts as important in clinical reasoning were derived from both the scientific and narrative domains. Students identified the most important factors from the pragmatic and narrative domains, as well as one factor from the scientific domain | |
| Hallin & Sviden SJOT | To explore the differences in the way that expert occupational therapists reflect on practice. This study asked the experts to describe their impressions after viewing a videotape of a patient in three different scenarios Neurological rehabilitation | n = 6 Sweden | Five qualitatively different types of comment were revealed: confident, tentative, generalized, teaching and understanding. The extent to which individuals used these types of comment differed, which in turn varied in relation to the three different scenarios | |
| 1996 | Roberts BJOT | To examine the content and process of occupational therapists’ reasoning when given a referral letter. The study approached reasoning from the cognitive sciences, based on what is known about human cognition and information-processing theories Therapists were entering postgraduate study and came from a variety of settings | n = 38 UK | The content of therapists’ reasoning focused on gathering information about the client and suggesting intervention. The processes of thinking were found to be similar to those observed in studies of medical problem-solving, and there was an element of hypothetico-deductive reasoning, as has been observed in medicine. The process included problem-sensing, cue acquisition, problem formulation and problem solution |
| Hagedorn BJOT | To examine experienced occupational therapists’ clinical reasoning and decision-making processes when making a decision regarding the first intervention in a familiar type of case Physical rehabilitation | n = 6 UK | Occupational therapists used schematic processing to speed identification of problems and find solutions. Hagedorn found that theory had become so embedded in practice that therapists were no longer conscious of it. Schematic models representing therapists’ mental problem space were developed | |
| Alnervik & Sviden OTJR | To examine whether descriptions of treatment sessions conducted by occupational therapists differed cognitively, depending on whether they were involved in storytelling or reflection practice. Also to examine the frequency with which different types of reasoning were used in these practices Medical and neurological rehabilitation, hand surgery and rheumatology | n = 5 Sweden | Procedural reasoning (focused on treatment interventions) was found to predominate in both storytelling and reflection using both quantitative and qualitative analysis. Accounts of reflection on practice did not contain any features distinguishing them from storytelling. A much smaller number of comments were also categorized as conditional or interactive reasoning | |
| Mew & Fossey AOTJ | To explore the client-centred aspects of the clinical reasoning of an occupational therapist when using the Canadian Occupational Performance Measure Physical rehabilitation | n = 1 Australia | Three aspects of client-centred reasoning were discussed: collaboration to define problems and determine the goals of therapy; the therapist's acknowledgement of the client's feelings; and the therapist's understanding of the client | |
| Munroe BJOT | To investigate the scope and nature of clinical reasoning which required occupational therapists to describe the content and meaning of their thinking during routine interventions with clients and carers living in their own homes Community setting | n = 30 UK | Patterns of reasoning consisted of three elements: reflection, reasoning and decision-making. Reflection in action was commonplace during the home visits. Reasoning was found to be relativistic or pragmatic in response to contextual influences. The therapists tended to use coded meaning when explaining their thinking, which may in part account for the difficulties in articulating the reasoning that underpins clinical action. Decision-making was found to be concerned more with interactive as opposed to technical or procedural issues | |
| Robertson BJOT | To explore the differences in clinical reasoning in occupational therapy between student and clinicians No information provided | n = 67 New Zealand | Internal representations of clinical problems are changed by practical experience. Clinicians and students have access to the same information but this is more clearly defined and organized in the case of the clinician | |
| 1997 | Hooper AJOT | To explore the worldview of an occupational therapist and how her beliefs influence the delivery of service Physical setting | n = 1 USA | A therapist's worldview frames clinical practice and shapes delivery of service. The therapist's view of reality can be categorized into four areas: ‘(a) what she believes about ultimate reality; (b) what she believes about life, death, and eternity; (c) what she believes about human nature; and (d) what she believes about the nature of knowing’ (Hooper 1997, p.328). This worldview shapes the therapist's practice |
| Crabtree & Lyons BJOT | A single case study exploring an occupational therapist's clinical reasoning as they worked in a large public hospital Acute care setting | n = 1 Australia | The therapist demonstrated a range of clinical reasoning strategies, as outlined in previous literature. These strategies operated in harmony and conflicted at different times. The view that clinical reasoning is an extremely complex process was reinforced | |
| Barnitt & Partridge PRI | To describe qualitatively and then compare ethical dilemmas reported by eight occupational therapists and eight physiotherapists Variety of physical and mental health settings | n = 8 UK | Occupational therapists were found to use a narrative style when describing ethical reasoning. Dealing with ethical dilemmas was found to be a stressful but positive experience. Factors that influenced capacity to deal with the dilemma included previous experience, time for reflection and support from peers | |
| 1999 | Sviden & Hallin SJOT | To explore whether therapists’ clinical reasoning varied depending on their field of practice (rheumatology and neurology) Physical rehabilitation | n = 12 Sweden | Differences between these two groups of therapists were found, and it was proposed that differences in clinical reasoning may influence patient–therapist interaction. The analysis focused on the way the occupational therapists reasoned in order to make sense of the situation. Five qualitatively different groups of comment were identified: confident, tentative, understanding, generalized and teaching |
| 2000 | Gibson et al OTHC | To compare the clinical reasoning process of a novice and an experienced occupational therapist Inpatient hospital with a rehabilitation unit | n = 2 USA | Emerging themes included definitions of clinical reasoning, factors influencing clinical reasoning, sources used when reasoning, ability to prioritize, patient viewed as an individual, patients’ role in treatment, and clinical reasoning as an evolving process. Both similarities and differences between the therapists were also found |
| 2001 | Unsworth SJOT | To examine qualitatively and quantitatively the differences in clinical reasoning of novice and expert occupational therapists Physical rehabilitation | n = 5 Australia | Three expert and two novice occupational therapists working in rehabilitation settings wore a head-mounted video camera while completing assessment, treatment and discharge planning sessions. Differences were found between novices and experts in both the amounts and types of clinical reasoning used. The findings suggest that novice therapists could benefit from spending more time reflecting on the therapy process and discussing their therapy with expert colleagues |
| 2003 | Doumanov & Rugg IJTR | To explore clinical reasoning and compare the factors that influence it in qualified occupational therapists and support staff Community rehabilitation teams for older clients | n = 20 UK | Occupational therapists were more likely to take a holistic view to client care. Support staff followed the treatment plans developed by the occupational therapy staff, and sought approval from the therapist prior to making any treatment decision. Concluded that the thinking of these two groups of staff is necessarily different (owing to education rather than experience) and that support staff cannot be expected to perform the same duties as occupational therapists in community rehabilitation settings |
| Ward AJOT | To investigate the clinical reasoning of occupational therapists in group practice Mental health | n = 1 USA | Clinical reasoning used by the therapists in psychosocial task groups included interactive, narrative, conditional and pragmatic reasoning. The gestalt of their practice was uncovered through therapists’ descriptions of the multiple levels of consciousness used in the therapy environment and larger environmental context | |
| 2004 | Mitchell & Unsworth AOTJ | To present the findings of a survey that intended firstly to provide an overview of the occupational therapy role in community health centre settings, and secondly to gather some basic data on the nature of the clinical reasoning processes used during occupational therapy practice in this field Community healthcare | n = 36 Australia | Community health occupational therapists were mature in age and widely experienced. They undertook a wide range of roles. The expert therapists were confident of their skills in client-related tasks and were strongly client-centred in their reasoning. In general, the experts agreed on the reasoning needed for the case scenarios given |
| 2004a | Unsworth BJOT | To examine the relationship between client-centred practice and clinical reasoning, explore the concept of pragmatic reasoning and present a diagrammatic conceptualization of current knowledge of clinical reasoning Physical rehabilitation | n = 13 Australia | A diagram was presented to illustrate the results, which included the overlapping nature of the types of reasoning, that a reciprocal relationship seems to exist between client-centred practice and interactive reasoning, that pragmatic reasoning was only related to the therapist's practice context, and that all forms of reasoning were influenced by the therapist's worldview |
| 2005 | Mitchell & Unsworth BJOT | To examine the clinical reasoning of five expert and five novice occupational therapists when conducting home visits Community health care | n = 10 Australia | Differences were found in the amounts and types of clinical reasoning used by novices versus experts; novices used more procedural reasoning, whereas experts used more conditional and mixes of different reasoning types. Qualitative results illustrated the smooth flow of the home visits conducted by experts, whereas novices depended on external structure such as assessment forms to guide the process. Expert reasoning was more confident and clear, while novices were more awkward and self-conscious |
| Unsworth AJOT | To use a head-mounted video camera and debriefing interview to explore current conceptualizations of clinical reasoning in occupational therapy Physical rehabilitation | n = 13 Australia | The dominant forms of reasoning used were procedural, interactive and conditional. Therapists were also seen to be using aspects of pragmatic reasoning and used a newly identified form of reasoning termed generalization reasoning to draw on past experience or knowledge to assist them in making sense of a current situation or client circumstance | |
| 2007 | Nikopoulou-Smyrni & Nikopoulos DR | To develop and collect preliminary data on the application of ‘Anadysis’ (a new integrated clinical reasoning model), involving patients suffering from stroke or transient ischaemic attack. This approach was compared with a current clinical reasoning model Physical rehabilitation | n = 4 UK | Used pretest and post-test design, the reasoning of participants using the current reasoning model of their discipline and the new Anadysis model (n = 12, including 4 occupational therapists). Results revealed substantially higher median percentages of ‘correct’ responses in clinical reasoning among clinicians using the new integrated model when compared with the control group |
| 2008 | Kuipers & Grice AOTJ | To describe the repertory grid technique, to investigate the clinical reasoning of an experienced occupational therapist working in the area of upper limb hypertonia following brain injury Physical rehabilitation | n = 1 Australia | Qualitative results were presented in themes, including importance of clinical expertise and theoretical frameworks to guide practice, and the difference between ‘broad’ and ‘specific’ aspects of practice, as well as differentiation between ‘therapist and client-related’ aspects of the clinical situation. Quantitative analysis after the interview indicated that clinical reasoning was structured in terms of upper limb performance and client-centred aspects of the therapy process |
| 2009 | Kuipers & Grice AOTJ | To examine the impact of a protocol on the clinical reasoning of novice and expert occupational therapists when working with clients who have upper limb hypertonia following brain injury Physical rehabilitation | n = 21 Australia | Novice participants changed their reasoning after exposure to a protocol on treatment for upper limb hypertonia. Prior to exposure, novices relied on therapy tasks, the problem-solving process, environmental factors and standard practice to structure their reasoning. Following exposure, novices’ clinical reasoning changed to reflect more closely experts’ reasoning, which was a more collaborative model of care |
The table reveals that there have been relatively few (31) published empirical studies on clinical reasoning in occupational therapy. It is particularly notable that there are very few researchers who have published multiple or related papers. It also seems that the research does not seem to build on what has come before, but is rather fragmented. Hopefully, this will change as a new wave of international researchers and doctoral students publish their findings.
Building a theory of clinical reasoning through scholarship of practice
One of the central aims of the clinical reasoning study funded by the American Occupational Therapy Foundation was to discover the practical theories-in-use of the occupational therapy profession so that this tacit knowledge could be documented and passed on. Mattingly and Fleming (1994) were able to realize this goal because their research adopted a participatory action research approach within an ethnographic framework. The occupational therapists were not studied from a distance, but rather they became part of the research team as they examined their own practice, working with the researchers in what Schön (1983) refers to as a ‘scholarship of practice’. This term can be defined as ‘delivering and generating evidence for practice through a partnership between academia and practice’ (Melton et al 2009, p.13).
This approach to describing how theory can be generated from practice is quite distinct from the traditional basic science view that theory is generated prior to its application in the field. Over the past 15 years, many occupational therapy writers have identified how occupational therapists do seem to have a problem with integrating theory into practice (Duncan, 2006, Kielhofner, 2009 and Melton et al., 2009). It appears that therapists are somewhat disillusioned with the relevance of theory in daily practice. Therefore, the scholarship of practice approach has been identified as a way of growing relevant theory from within practice, to support and promote that practice (Argyris and Schön, 1974, Schön, 1983 and Creek and Ormston, 1996). This section of the chapter examines how theories evolve, and proposes that clinical reasoning is actually developing into a theory itself through scholarship of practice.
In Chapter 5 of this text and the previous edition (2006), Duncan describes not only the value and importance of having theory to underpin practice, but also the complexities surrounding our use and misuse of theory terms such as paradigm, conceptual practice model, frame of reference and approach. Since the idea that clinical reasoning in occupational therapy is developing into a theory in its own right is relatively new (Unsworth and Schell, 2006 and Schell et al., 2008), it is too early map out its structure, function and relationships to the core beliefs of the occupational therapy profession. It may transpire that clinical reasoning becomes incorporated into an existing occupational therapy theory, or it may become known as a frame of reference, since frames of reference link theory to practice and reasoning is often described in this way. Since it is premature to use any particular label at this stage, for the purposes of this chapter, the term ‘theory’ of clinical reasoning will be adopted and used in its broadest sense.
Theories may be defined as connected sets of ideas that form a base for practice or action. Theories attempt to explain and predict phenomena (Walker & Ludwig 2004), and help us to recognize what we know and to organize what we do (Mitcham 2003). Differing opinions concerning how theory is generated have also been proposed. In occupational therapy, Mitcham (2003) describes the process of theory generation as involving six sequential steps, starting with observation and ending with tested theory.
Steps of theory development
1. Observation of the phenomena over time.
2. Recognition that phenomena present themselves in certain ways.
3. Organization of the phenomena into a conceptual framework.
4. Empirical testing of the propositions and concepts that hold the conceptual framework together.
5. Refinement and retesting propositions and concepts.
6. Acceptance of the new theory (adapted from Mitcham 2003).
This description of theory development implies a coordinated, concerted approach to theory generation. What we know from the definitions of modes of clinical reasoning as presented in Table 16.1 and the research undertaken and summarized in Table 16.2, is that the approach to researching and understanding clinical reasoning has been far from coordinated. However, these stages of theory development do fit well with our understanding of clinical reasoning as a contextualized phenomenon that alters depending on the circumstances. In mapping the development of clinical reasoning as a theory against these steps, it is also important to note that the approach adopted here is to build on the foundation of clinical reasoning, as laid by Mattingly and Fleming (1994), rather than fragment research in this area by seeking out new interpretations of this phenomenon (Unsworth 2004a).
The first step in theory development is to observe the phenomena over time and recognize how clinical reasoning presents itself. The occupational therapy literature is rich with descriptive observations and explorations of clinical reasoning and how it is an interactive phenomenon that varies depending on the practice context and the broader social, cultural and political environment. What is required now is more directed effort to organize clinical reasoning into a conceptual framework for occupational therapy practice. Towards this end, models of clinical reasoning can be seen as emerging from the literature. Models describe a phenomenon in a familiar way so as to increase our understanding (Young & Quinn 1992).
Five models are presented here to explain the phenomenon of clinical/professional reasoning:
• Mattingly and Fleming's foundation research on clinical reasoning
• the model presented by Higgs and Jones, 2000 and Higgs and Jones, 2008
• Schell's ecological model of professional reasoning (Schell 2009)
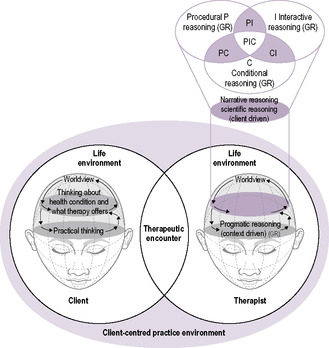 |
| Fig. 16.1 • The Occupational Therapy Model of Clinical Reasoning. This model is based on an earlier version (Unsworth 2004a), and attempts to draw in elements from the other models to work towards building a conceptual framework. |
Although Ryan (1998) also describes a narrative model of clinical reasoning, there is insufficient information on its components and definitions to describe it in any detail. Each of these models is outlined below. In these descriptions, note is taken of whether the model has an S1 focus (clinical reasoning), and also an S2 element (decision-making). Models reflecting an S2-only approach have not been included in this chapter.
Dewey, 1929 and Dewey, 1934: linear model of clinical reasoning (S1 and S2)
This is a classic description of general reasoning (Ryan 1998). It has many similarities to the hypothetico-deductive model of reasoning used in early medical research. This linear model consists of five stages, including reflecting on ideas, formulating hypotheses, evaluating hypotheses for truths, determining a course of action, and formulating a verbal statement to represent the hypothesis (Ryan 1998). The linear model has been widely adopted in medicine, as it fits well with the problem-solving approach required for medical diagnosis.
Mattingly and Fleming (1994): two-bodied practice and the therapist with the three-track mind (S1)
Although not articulated as a model, the documentation of the two-bodied practice and the therapist with the three-track mind none the less contributes to a developing model of clinical reasoning in occupational therapy. The eloquent description of the two-bodied practice (1994) reassures and supports occupational therapists in the belief that their practice is indeed complex, as it spans both the biomedical culture (in which we use chart talk) and the social, cultural and psychological issues surrounding the meaning of the illness (in which we use narrative reasoning). The notion of the therapist with the three-track mind provides an excellent description of three core modes of reasoning: procedural, interactive and conditional reasoning.
Higgs et al (2000, 2008): contextualized model of clinical reasoning (S1 and S2)
Higgs and Jones (2000) described an integrated, patient-centred model of clinical reasoning. They depicted an expanding spiral that reflected the clinician's growing understanding of the client and the clinical problem. At the beginning of the spiral was the clinician's encounter with the client and at the end was the final outcome. The tubing of the spiral represented the interaction of the six elements that make up the model: cognition, metacognition, the clinical problem, knowledge, the environment and the client's input. In the third edition of their text, Higgs et al (2008) describe clinical reasoning as a contextualized phenomenon, and add four meta-skills to the model, including the ability to derive knowledge and practise wisdom from reasoning and practice, the location of reasoning as relating to the selected practice model, the reflexive ability to promote personal growth in clients and self, and the use of critical creative conversations to make clinical decisions.
Schell et al., 2008 and Schell, 2009: the ecological model of professional reasoning (S1)
Schell describes professional reasoning and the resulting therapy action as the interface of the therapist, the client and the practice context. Each practitioner brings to the therapy situation knowledge and skills that are grounded in life experiences, including personal characteristics such as physical capacities, sensory profile, personality and intelligence profile, as well as enculturated factors such as values, beliefs and preferences. These form a personal self, which is an inescapable lens through which the therapist frames the therapy encounter. Layered over or entwined with this personal self is the professional self, which includes the therapist's professional knowledge from education, experiences from prior clients, and therapy beliefs, along with knowledge of specific technical skills and therapy routines available for use in the practice context (Fondiller et al., 1990, Törnebohm, 1991, Mattingly and Fleming, 1994 and Burk, 1997). The personal and professional selves act in concert to respond to various problems of practice. Clients also come to therapy with their own life experiences and contexts, which also shape the therapeutic encounter.
Unsworth, 2004a and Unsworth, 2005, Fig. 16.1): Occupational Therapy Model of Clinical Reasoning (S1)
Based on the research foundation laid by Mattingly and Fleming, 1994, Schön, 1983, Schön, 1988, Barris, 1987, Hooper, 1997, Schell and Cervero, 1993 and Unsworth, 2004a proposed a three-tier structure to depict clinical reasoning. At the top of Unsworth's model is worldview (moral beliefs and socio-cultural perspective) (Wolters 1989), which influences and modifies all other modes of reasoning. The middle level of the diagram contains the three main forms of reasoning: procedural, interactive and conditional. The fact that therapists also seemed to use two or three forms of procedural/interactive/conditional reasoning simultaneously is presented by the use of a Venn diagram, and generalization reasoning is included in each of these modes. The last level of the diagram contains pragmatic reasoning (dealing with what can be achieved, given the practical constraints or benefits of the environment). The arrows flow around the model to indicate that these modes of reasoning or influences on reasoning all have an impact on each other. In Unsworth (2004a), it was stated that this model operates in the client-centred practice of occupational therapy. This model is expanded here in Figure 16.1 to incorporate the practice and contextual elements that also influence clinical reasoning. This updated model includes the client, acknowledging that reasoning is shaped by the interactive nature of the clinical encounter. The client's reasoning is also shaped by their worldview, their thoughts about health status and expectations of what occupational therapy has to offer. Clients also have many practical issues to consider that affect their therapy, such as their finances and family politics. This kind of pragmatic thinking is influenced by the client's life environment, which exists for both clients and therapists. Life environment is concerned with the social, cultural and political systems in which we live. However, a great deal more research is required to test, modify and expand this model into a conceptual framework.
Directions for further research in clinical reasoning
The Occupational Therapy Model of Clinical Reasoning, as illustrated in Figure 16.1, attempts to bring together some of the concepts articulated in the other models in a more integrated fashion to begin work on the third step of theory-building, which is to organize the phenomena into a conceptual framework. Research to build this framework is required in the spirit of scholarship of practice. As proposed by Nixon and Creek (2006), we need to construct theory by ‘developing collaborative models of thoughtful practice that challenge assumptions and suggest new lines of inquiry’. Areas for research on the model include exploration of the relationship between pragmatic reasoning and worldview. Embodied knowledge is also not explicitly included in the model, and research is required to examine how a therapist reasons with their whole body. Research is also required to test empirically if the components of the model are sound and hold true across different environments and over time. Finally, there is a need for further longitudinal studies of clinical reasoning. Most of the research undertaken by occupational therapists provides snapshots of practice, and what we need now are studies that track therapists reasoning, and, importantly, shifts in reasoning, over time. We need to have a better understanding of the patterns of reasoning that promote the best therapy outcomes and gain further insights into how to share these patterns with novice therapists.
Summary
When visiting clinics around the world, I see occupational therapists striving to provide the best evidence-based therapy possible. This commitment and aspiration to achieve excellence are supported by clinical reasoning. Therefore, it is crucial in our profession that we continue to research and write about clinical reasoning. The clinical reasoning of occupational therapists is a multifaceted process and forms part of the central framework of the profession. In daily practice, clinical reasoning results from the complex interactions between the therapist's own worldview, modes of reasoning and life environment, as well as the worldview, life environment and reasoning of the client. This chapter has explored the concept of clinical reasoning in occupational therapy and related factors such as intuition, worldview, expertise and reflection. It is proposed that occupational therapy researchers and writers in the area of clinical reasoning are slowly contributing to the construction of a theory of clinical reasoning. The challenge now is to ensure that the theory is built using a systematic framework and that research undertaken benefits from a scholarship of practice approach.
• Use your own words to describe what clinical reasoning is, and differentiate clinical reasoning from clinical decision-making.
• Describe two of the most common modes of clinical reasoning you use in practice (or you used in your last fieldwork). Reflect on why you selected these two. Consider what other reasoning modes you might use to enhance your practice in the future.
• Many of the factors that shape our pragmatic reasoning have the potential to impact negatively on what we can do or offer clients. Can you think of an example or scenario that could lead to the kind of pragmatic reasoning that limits delivery of an ideal therapy service? What could you do to counteract the forces that lead to this kind of pragmatic reasoning?
• Identify an episode in your career (or while doing fieldwork) that has been difficult due to discordance between your worldview and something happening in the clinic or with a client. What happened, why, and what would you do differently next time?
• Models of clinical reasoning contributing to a theory of clinical reasoning are presented in the text. Describe a research study that you think might add to our understanding of clinical reasoning in occupational therapy and contribute to theory development in this field.
Acknowledgements
Many thanks to my research assistant, Adrian Kamer, for assistance in compiling the information presented in Table 16.2.
References
Alnervik, A.; Sviden, G., On clinical reasoning: patterns of reflection on practice, Occupational Therapy Journal of Research 16 (2) (1996) 98–110.
Alsop, A.; Ryan, S.E., Making the Most of Fieldwork Education: a Practical Approach. (1996) Stanley Thornes, Cheltenham.
Argyris, C.; Schön, D.A., Theory in Practice: Increasing Professional Effectiveness. (1974) Jossey-Bass, San Francisco.
Barnitt, R.; Partridge, C., Ethical reasoning in physical therapy and occupational therapy, Physiotherapy Research International 2 (1997) 178–194.
Barris, R., Clinical reasoning in psychosocial occupational therapy: the evaluation process, Occupational Therapy Journal of Research 7 (1987) 147–162.
Benner, P., From Novice to Expert. Excellence and Power in Clinical Nursing Practice. (1984) Addison–Wesley, Menlo Park, CA.
Benner, P.E.; Tanner, C.A.; Chesla, C.A., Expertise in Nursing Practice: Caring, Clinical Judgement and Ethics. (1996) Springer, New York.
Burke, J.P., Frames of meaning: An analysis of occupational therapy evaluations of young children, Dissertation Abstracts International 58 (03) (1997) 644.
Crabtree, M.; Lyons, M., Focal points and relationships: a study of clinical reasoning, British Journal of Occupational Therapy 60 (2) (1997) 57–64.
Creek, J.; Ormston, C., The essential elements of professional motivation, British Journal of Occupational Therapy 59 (1996) 7–10.
Creighton, C.; Dijkers, M.; Bennett, N.; Brown, K., Reasoning and the art of therapy for spinal cord injury, American Journal of Occupational Therapy 49 (1995) 311–317.
In: (Editors: Crepeau, E.B.; Cohn, E.S.; Boyt Schell, B.A.) Willard and Spackman's Occupational Therapyeleventh ed. (2009) Lippincott Williams & Wilkins, Baltimore.
Dewey, J., Experience and Nature. (1929) WW Norton, New York.
Dewey, J., Art as Experience. (1934) Minton & Balch, New York.
Doumanov, P.; Rugg, S., Clinical reasoning skills of occupational therapists and support staff: a comparison, International Journal of Therapy and Rehabilitation 10 (5) (2003) 195–203.
Dowie, J.; Elstein, A., Professional Judgement: a Reader in Clinical Decision Making. (1988) Cambridge University Press, Cambridge.
Dreyfus, H.L.; Dreyfus, S.E., Mind Over Machine: The Power of Human Intuition and Expertise in the Era of the Computer. (1986) Free Press, New York.
Dreyfus, S.E.; Dreyfus, H.L., In: A Five-Stage Model of the Mental Activities Involved in Directed Skill AcquisitionUnpublished report supported by the Air Force Office of Scientific Research (AFSC). USAF (Contract F49620-79-C-0063). (1980) University of California at Berkeley, Berkeley.
Duncan, E.A.S., An introduction to conceptual models of practice and frames of reference, In: (Editor: Duncan, E.A.S.) Foundations for Practice in Occupational Therapy (2006) Elsevier, Edinburgh.
Fleming, M.H., The therapist with the three-track mind, American Journal of Occupational Therapy 45 (1991) 1007–1014.
Fleming, M.H., The therapist with the three track mind, In: (Editors: Mattingly, C.; Fleming, M.H.) Clinical Reasoning: Forms of Inquiry in a Therapeutic Practice (1994) FA Davis, Philadelphia, pp. 119–136.
Fondiller, E.L.; Rosage, L.J.; Neuhaus, B.E., Values Influencing Clinical Reasoning in Occupational Therapy: An Exploratory Study, Occupational Therapy Journal of Research 10 (1990) 41–55.
Fortune, T.; Ryan, S., Applying Clinical Reasoning: a Caseload Management System for Community Occupational Therapists, British Journal of Occupational Therapy 59 (5) (1996) 207–211.
Gibson, D.B.; Velde, B.; Hoff, T.; et al., Clinical reasoning of a novice versus an experienced occupational therapist: a qualitative study, Occupational Therapy in Health Care 12 (4) (2000) 15–31.
Goel, V.; Buchel, C.; Frith, C.; et al., Dissociation of mechanisms underlying syllogistic reasoning, NeuroImage 12 (5) (2000) 504–514.
Hagedorn, R., Clinical decision making in familiar cases: a model of the process and implications for practice, British Journal of Occupational Therapy 59 (5) (1996) 217–222.
Hallin, M.; Sviden, G., On expert occupational therapists’ reflection-on-practice, Scandinavian Journal of Occupational Therapy 2 (1995) 69–75.
Hammond, K.R., Human Judgment and Social Policy: Irreducible Uncertainty, Inevitable Error, Unavoidable Injustice. (1996) Oxford University Press, New York.
Hammond, K.R.; Brehmer, B., Quasi rationality and distrust: implications for international conflict, In: (Editors: Summers, D.; Rappoport, L.) Human Judgement and Social Interaction. Holt (1973) Rinehart & Wonston, New York, pp. 338–391.
Hardman, D., Judgment and Decision Making: Psychological Perspectives. (2009) BPS Blackwell, Chichester.
Harries, P.; Duncan, E.A.S., Judgement and decision-making skills for practice, In: (Editor: Duncan, E.A.S.) Skills for Practice in Occupational Therapy (2009) Elsevier, Edinburgh, pp. 25–39.
Harries, P.; Gilhooly, K., Identifying occupational therapists’ referral priorities in community health, Occupational Therapy International 10 (2) (2006) 150–164.
Harries, P.; Harries, C., Studying clinical reasoning, Part 2: Applying social judgment theory, British Journal of Occupational Therapy 64 (6) (2001) 285–292.
Higgs, J.; Jones, M., Clinical Reasoning in the Health Professions. second ed. (2000) Butterworth–Heinemann, Melbourne.
Higgs, J.; Jones, M.; Loftus, S.L.; et al., Clinical Reasoning in the Health Professions. third ed. (2008) Butterworth–Heinemann, Melbourne.
Holm, M.B., Our mandate for the new millennium: evidence-based practice, American Journal of Occupational Therapy 54 (2000) 575–585.
Hooper, B., The relationship between pretheoretical assumptions and clinical reasoning, American Journal of Occupational Therapy 51 (5) (1997) 328–338.
Kielhofner, G., Model of Human occupation: Theory and Application. fourth ed. (2008) Lippincott Williams & Wilkins, Baltimore.
Kielhofner, G., Conceptual Foundations of Occupational Therapy. fourth ed. (2009) FA Davis, Philadelphia.
Kielhofner, G.; Forsyth, K., Thinking with theory: a framework for therapeutic reasoning, In: (Editor: Kielhofner, G.) Model of Human Occupation: Theory and Applicationthird ed. (2002) Lippincott Williams & Wilkins, Baltimore, pp. 162–178.
Klein, G.A.; Orasanu, J.; Calderwoon, R.; et al., Decision Making in Action: Models and Methods. (1993) Ablex, Norwood, NJ.
Kuipers, K.; Grice, J.W., Clinical reasoning in neurology: use of the repertory grid technique to investigate the reasoning of an experienced occupational therapist, Australian Occupational Therapy Journal 56 (4) (2008) 275–284.
Kuipers, K.; Grice, J.W., The structure of novice and expert occupational therapists’ clinical reasoning before and after exposure to a domain-specific protocol, Australian Occupational Therapy Journal 56 (6) (2009) 418–427.
Lyons, K.D.; Crepeau, E.B., The clinical reasoning of an occupational therapy assistant, American Journal of Occupational Therapy 55 (2001) 577–581.
Mattingly, C., Occupational therapy as a two-body practice: the body as machine, In: (Editors: Mattingly, C.; Fleming, M.H.) Clinical Reasoning: Forms of Inquiry in a Therapeutic Practice (1994) FA Davis, Philadelphia, pp. 37–63.
Mattingly, C.; Fleming, M.H., Clinical Reasoning: Forms of Inquiry in a Therapeutic Practice. (1994) FA Davis, Philadelphia.
McKay, E.A., Reflective practice: doing, being and becoming a reflective practitioner, In: (Editor: Duncan, E.A.S.) Skills for Practice in Occupational Therapy (2009) Churchill Livingstone, Edinburgh, pp. 55–72.
McKay, E.A.; Ryan, S., Clinical reasoning through story telling: examining a student's case story on a fieldwork placement, British Journal of Occupational Therapy 58 (6) (1995) 234–238.
Melton, J.; Forsyth, K.; Freeth, D., Using theory in practice, In: (Editor: Duncan, E.A.S.) Skills for Practice in Occupational Therapy (2009) Churchill Livingstone, Edinburgh, pp. 9–24.
Mew, M.M.; Fossey, E., Client-centred aspects of clinical reasoning during an initial assessment using the Canadian Occupational Performance Measure, Australian Occupational Therapy Journal 43 (1996) 155–166.
Mitcham, M.D., Integrating theory and practice: using theory creatively to enhance professional practice, In: (Editors: Brown, G.; Esdaile, S.A.; Ryan, S.E.) Becoming an Advanced Healthcare Practitioner (2003) Butterworth–Heinemann, New York, pp. 64–89.
Mitchell, R.; Unsworth, C.A., Role perceptions and clinical reasoning of community health occupational therapists undertaking home visits, Australian Occupational Therapy Journal 51 (1) (2004) 13–24.
Mitchell, R.; Unsworth, C.A., Clinical reasoning during community health home visits: expert and novice differences, British Journal of Occupational Therapy 68 (5) (2005) 215–223.
Munroe, H., Clinical reasoning in community occupational therapy, British Journal of Occupational Therapy 59 (5) (1996) 196–202.
Neistadt, M.E., Classroom as clinic: a model of teaching clinical reasoning in occupational therapy education, American Journal of Occupational Therapy 41 (1987) 631–637.
Neistadt, M.E.; Atkins, A., Analysis of the orthopedic content in an occupational therapy curriculum from a clinical reasoning perspective, American Journal of Occupational Therapy 50 (1996) 669–675.
Neuhaus, B.E., Ethical considerations in clinical reasoning: the impact of technology and cost containment, American Journal of Occupational Therapy 42 (1988) 288–294.
Nikopoulou-Smyrni, P.; Nikopoulos, C.K., A new integrated model of clinical reasoning: development, description and preliminary assessment in patients with stroke, Disability and Rehabilitation 29 (14) (2007) 1129–1138.
Nixon, J.; Creek, J., Towards a theory of practice, British Journal of Occupational Therapy 69 (2) (2006) 77–80.
Rassafiani, M.; Ziviani, J.; Rodger, S.; et al., Managing upper limb hypertonicity: factors influencing therapists’ decisions, British Journal of Occupational Therapy 69 (8) (2006) 373–378.
Rassafiani, M.; Ziviani, J.; Rodger, S.; et al., Occupational therapists’ decision-making in the management of clients with upper limb hypertonicity, Scandinavian Journal of Occupational Therapy 15 (2) (2008) 105–115.
Rew, L., Intuition: concept analysis of a group phenomenon, Advances in Nursing Science 8 (2) (1986) 21–28.
Roberts, A.E., Clinical reasoning in occupational therapy: idiosyncrasies in content and process, British Journal of Occupational Therapy 59 (8) (1996) 372–376.
Robertson, L., Clinical reasoning, Part 2: Novice/expert differences, British Journal of Occupational Therapy 59 (5) (1996) 212–216.
Rogers, J.C., Clinical reasoning: the ethics, science, and art, American Journal of Occupational Therapy 37 (1983) 601–616.
Rogers, J.C., Occupational reasoning, In: (Editors: Curtin, M.; Molineux, M.; Supyk-Mellson, J.) Occupational Therapy and Physical Dysfunction. Enabling Occupation (2010) Churchill Livingstone, Sydney, pp. 57–65.
Rogers, J.C.; Holm, M.B., Occupational therapy diagnostic reasoning: a component of clinical reasoning, American Journal of Occupational Therapy 45 (1991) 1045–1053.
Rogers, J.C.; Masagatani, G., Clinical reasoning of occupational therapists during initial assessment of physically disabled patients, Occupational Therapy Journal of Research 2 (1982) 195–219.
Rogers, J.C., Teaching Clinical Reasoning in Practice in Geriatrics, Physical and Occupational Therapy in Geriatrics 1 (3) (1982) 29–37.
Ryan, S., Influences that shape our reasoning, In: (Editor: Creek, J.) Occupational Therapy New Perspectives (1998) Whurr, London, pp. 47–65.
Schell, B.A.B., Professional reasoning in practice, In: (Editors: Crepeau, E.B.; Cohn, E.; Schell, B.A.B.) Willard and Spackman's Occupational Therapy (2009) Wolters Kluwer, Philadelphia, pp. 314–327.
Schell, B.A.B.; Cervero, R.M., Clinical reasoning in occupational therapy: an integrative review, American Journal of Occupational Therapy 47 (1993) 605–610.
Schell, B.A.B.; Harris, D., Embodiment: reasoning with the whole body, In: (Editors: Schell, B.A.B.; Schell, J.W.) Clinical and Professional Reasoning in Occupational Therapy (2008) Lippincott Williams & Wilkins, Philadelphia, pp. 69–87.
In: (Editors: Schell, B.A.B.; Schell, J.W.) Clinical and Professional Reasoning in Occupational Therapy (2008) Wolters Kluwer, Philadelphia.
Schell, B.A.B.; Unsworth, C.A.; Schell, J.W., Theory and practice: new directions for research in professional reasoning, In: (Editors: Schell, B.A.B.; Schell, J.W.) Clinical and Professional Reasoning in Occupational Therapy (2008) Lippincott Williams & Wilkins, Philadelphia, pp. 401–431.
Schön, D.A., The Reflective Practitioner: How Professionals Think in Action. (1983) Basic, New York.
Schön, D.A., Educating the Reflective Practitioner. (1988) Jossey-Bass, San Francisco.
Stanovich, K.E.; West, R.W., Individual differences in reasoning: implications for the rationality debate?Behavioral and Brain Sciences 23 (5) (2000) 645–726.
Strong, J.; Gilbert, J.; Cassidy, S.; et al., Expert clinicians’ and students’ views on clinical reasoning in occupational therapy, British Journal of Occupational Therapy 58 (3) (1995) 119–123.
Sviden, G., Responding to patients’ nonverbal communication of affect, Occupational Therapy Journal of Research 15 (2) (1995) 85–102.
Sviden, G.; Hallin, M., Differences in clinical reasoning between occupational therapists working in rheumatology and neurology, Scandinavian Journal of Occupational Therapy 6 (1999) 63–69.
Sviden, G.; Saljo, R., perceiving patients and their nonverbal reactions, American Journal of Occupational Therapy 47 (6) (1993) 491–497.
In: (Editor: Thompson, D.) Concise Oxford Dictionaryninth ed. (1995) Oxford Clarendon, Oxford.
Törnebohm, H., What is worth knowing in occupational therapy?American Journal of Occupational Therapy 45 (1991) 451–454.
Unsworth, C.A., Cognitive and Perceptual Disorders: A Clinical Reasoning Approach to Evaluation and Intervention. (1999) FA Davis, Philadelphia.
Unsworth, C.A., The clinical reasoning of novice and expert occupational therapists, Scandinavian Journal of Occupational Therapy 8 (2001) 163–173.
Unsworth, C.A., Clinical reasoning: how do worldview, pragmatic reasoning and client-centredness fit?British Journal of Occupational Therapy 67 (2004) 10–19.
Unsworth, C.A., How therapists think: Exploring therapists’ reasoning when working with patients who have cognitive and perceptual problems following stroke, In: (Editors: Gillen, G.; Burkhardt, A.) Stroke Rehabilitation: A Function-Based Approachsecond ed. (2004) Mosby, St Louis, pp. 358–375.
Unsworth, C.A., Using a head-mounted video camera to explore current conceptualizations of clinical reasoning in occupational therapy, American Journal of Occupational Therapy 59 (2005) 31–40.
Unsworth, C.A., Using social judgment theory to study occupational therapists’ use of information when making licensing recommendations to older and functionally impaired drivers, American Journal of Occupational Therapy 61 (5) (2007) 493–502.
Unsworth, C.A.; Schell, B.A., Clinical Reasoning: Development of a Theory-in-use, In: Proceedings of the 14th International Congress of the World Federation of Occupational Therapists, Sydney 24–28 July (2006).
Unsworth, C.A.; Thomas, S.A., Information use in discharge accommodation recommendations for stroke patients, Clinical Rehabilitation 7 (1993) 181–188.
Unsworth, C.A.; Thomas, S.A.; Greenwood, K.M., Rehabilitation team decisions concerning discharge housing for stroke patients, Archives of Physical Medicine and Rehabilitation 76 (1995) 331–340.
Unsworth, C.A.; Osberg, J.S.; Graham, A., Admitting pediatric trauma patients to rehabilitation following acute care: decision making practices in the U.S.A. and Australia, Journal of Pediatric Rehabilitation 1 (1997) 207–218.
Walker, K.F.; Ludwig, F.M., Perspectives on Theory for the Practice of Occupational Therapy. third ed. (2004) Pro-ed, Austin, TX.
Ward, J.D., The nature of clinical reasoning with groups: a phenomenological study of an occupational therapist in community mental health, American Journal of Occupational Therapy 57 (6) (2003) 625–634.
Wolters, A.M., On the idea of worldview and its relationship to philosophy, In: (Editors: Marshall, P.A.; Griffioen, S.; Mouw, R.) Stained Glass: Worldviews and Social Science (1989) University Press of America, New York, pp. 14–26.
Young, M.E.; Quinn, E., Theories and Principles of Occupational Therapy. (1992) Churchill Livingstone, London.