1 Palpation
Definition, application and practice
Some definitions and concepts
Palpation: some definitions
The Oxford Dictionary of English defines the verb to palpate as: ‘to examine (a part of the body) by touch, especially for medical purposes’. Its derivative noun is ‘palpation’ (from the Latin verb ‘palpare’: to ‘feel or touch gently’). According to The Chambers Dictionary, the term ‘palp’ means ‘to feel, examine or explore by touch’; ‘palpare’ is defined as ‘to touch softly, stroke, caress or flatter’. Churchill’s Medical Dictionary defines palpation as ‘to stroke, caress; to explore or examine by touching and probing with the hands and fingers’.
Whilst ‘stroking’, ‘caressing’ or (tactile) ‘flattering’ represent practices (through ‘gentle touch’) that are essentially designed to give physiological and psychological ‘healing’ to the recipient, palpation, for the purposes of this text, is primarily a purposeful activity requiring considerable skill. It is associated with methodical exploration and detailed manual examination, the aim of which is to acquire objective information that will eventually lead to a reasoned medical diagnosis upon which a subsequent treatment regimen can be based. Gould’s Medical Dictionary makes the direct link between the activity of palpation and diagnosis by gentle touch which involves the detection of the ‘characteristics and condition of local tissues of the underlying organs or tumors’.
In The Oxford Dictionary of English, to examine is defined as ‘to test; to inquire into; to question; to look closely at or into; to inspect’. According to The Chambers Dictionary, to examine is to ‘inspect (someone or something) thoroughly in order to determine the nature of a condition’. The activity involves critical, reflective thinking: the systematic weighing up of evidence in an attempt to arrive at a balanced conclusion.
General characteristics of palpation
Palpation is a highly complex and sophisticated manual skill. Citing Frymann, Chaitow (2003) draws attention to the potential which palpation offers members of the healing professions:
The human hand is equipped with instruments to perceive changes in texture, surface texture, surface humidity, to penetrate and detect successively deeper tissue textures, turgescence, elasticity and irritability. The human hand, furthermore, is designed to detect minute motion, motion which can only be detected by the most sensitive electronic pick-up devices available. This carries the art of palpation beyond the various modalities of touch into the realm of proprioception, of changes in position and tension within our own muscular system.
As Frymann emphasizes, the hand is particularly well equipped to play the key role in this activity. With reference to palpation of the human body, Chaitow reminds us that different parts of the hand possess the ability to discriminate between variations in tissue features: ‘… relative tension, texture, degree of moisture, temperature and so on’. He then makes the important point that ‘This highlights the fact that an individual’s overall palpatory sensitivity depends on a combination of different perceptive (and proprioceptive) qualities and abilities’ (Chaitow 2003).
Touch
Some general characteristics
Palpation involves the use of one of the primary senses, that of touch, in order to investigate and obtain information or to supplement that already gained by other means, such as by visual and auditory input. As Poon (1995) points out:
The act of touching and the feeling of being touched are very powerful experiences … (and touch) is the earliest and most primitive form of communication.
Montague (1978) reminds us that:
Touch is the first of the senses to develop in the embryo and it plays a very important role in the birth process itself and in the early life of the individual.
Not only is it the earliest system to become functional in the human being but also touch is thought to be the last of the senses to be lost immediately prior to death.
Touch plays a very significant part in our everyday experience:
When the other senses are not wholly effective, we return to the sense of touch to rediscover reality. Clothing is felt to determine its quality, fruit is squeezed to determine its ripeness and paint is touched to test for dryness.
Experience suggests, however, that there are instances when touch is often subjugated in favour of reliance upon other sensory modalities. Only when an awareness of an alteration in incoming stimuli occurs do we become conscious of the sense of touch. An example of this phenomenon might be when picking up a garment, we recognize its unfamiliarity through its texture or ‘feel’; another example might be an awareness of the material of trousers touching the legs immediately after a long period of wearing shorts.
Touch may be divided into two distinct categories: instrumental and expressive. Touch is described as instrumental when it is associated with a deliberate action: locating an anatomical structure for the purposes of examination during a clinical assessment, for example. Touch is identified as expressive when it is associated with spontaneous, affective actions: touching a distressed person’s arm in order to convey sympathy and offer comfort (MacWhannell 1992, Poon 1995).
Touch can be experienced as safe or unsafe; physically comfortable or uncomfortable. It can be used to establish rapport: hand-shaking as a formal greeting at the beginning of a clinical interview or as a means of ending a treatment session. Communication by touch is specifically permitted within particular interpersonal relationships (see later). In certain contexts, however, permission to touch may be required, for example, at the commencement, and during the various stages of a clinical examination and treatment session. Touch is associated with psychological reactions: it is difficult to touch or be touched by those who elicit negative responses. The anticipation of touching or being touched can increase stress levels and these reactions may be influenced by personality, cultural and social factors: some female patients may deliberately avoid consulting a male therapist; some patients may be reluctant to remove clothing. It is important to remember that professional personnel are placed in an extremely powerful and privileged position in relation to others: they are given a license to touch and this power and privilege should never be abused.
The physiology of touch
All areas of the skin supplied with appropriate receptors are normally able to perceive a variety of sensations (pain, degrees of pressure, temperature changes, etc.) to a greater or lesser degree. Some areas, however, are more sensitive to stimuli than others because:
The degree of tactile sensitivity in any area is in direct proportion to the number of sensory units present and active in that area, as well as to the degree of overlap of their receptive fields, which vary in size. Small receptive fields with many sensory units therefore have the highest degree of discriminatory sensitivity.
Sensitivity to spatial discrimination is poor in the lumbar region, the legs and the back of the hands. In the back of the hands, for example, two points can only be perceived separately if they are more than 50–100 mm apart. The lips, tongue and fingertips, however, rate high (1–3 mm). Thus individuals with normal sensation in the fingertips should be able to distinguish between two points even when they are less than 6 mm apart. This is referred to as the ‘Two Point Discrimination Test’ (see Chaitow 2003, Evans 2000, Magee 1997). The significance of this is that only relatively large objects can be recognized by the receptors in the lumbar region, whereas fine point discrimination can be achieved when employing the fingertips.
Chaitow makes the further point that:
Not only is there a difference of perception relating to spatial accuracy, but also one relating to intensity. An indentation of 6 micrometers is capable of being registered on the finger pads, while 24 micrometers is needed before the sensors in the palm of the hand reach their threshold and perceive the stimulus.
Additionally, Evans (2000) contends that:
Under normal conditions, touch is an exploratory sense rather than purely receptive, and it is becoming increasingly evident that tactile acuity is enhanced in active exploration when compared with passive reception.
Citing Meyers, Etherington and Ashcroft (1958), Evans suggests that:
An early indication of the phenomenon may be seen in an examination of the parameters of perception required to read Braille. The dots are separated by 2.3 mm, which is close to the threshold value for two-point discrimination at the pad of the index finger. Reduction of the inter-dot space to 1.9 mm only moderately reduces the legibility of the Braille text.
While sighted Braille transcribers, relying solely on visual input, have been known to become proficient at reading Braille by the end of only three weeks, experience confirms that individuals attempting to conquer the system by touch are estimated to take an average of 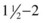 years to reach a speed suitable for serious study, even with regular practice. This is not due to lack of knowledge of the system; rather it is because the palpation and recognition of the signs using tactile input requires a considerable amount of dedicated time and practice in which to develop. As with all skills, the speed and quality of reading depends upon the frequency and amount of use. The ability to palpate with any finger or fingers can usually be developed, the use of the index finger being the most popular. Reading speed is further enhanced by using the fingers of both hands. In some cases, this skill never develops if the individual has not learnt to employ touch from an early age. In rare instances, people who have been unable to use their fingers have developed the same ability to read Braille by using their toes or even their lips! (see above). This means that regardless of the method by which this skill is acquired, the ability to increase the information received through sensory input can be improved, given time and serious dedication to regular practice. This can be of great benefit to the clinical practitioner who wishes to ‘read’ information that lies deep to the skin. The controlled use of pressure and movement, coupled with feedback and experience, unlocks a vast quantity of information that is often unavailable to the eye.
years to reach a speed suitable for serious study, even with regular practice. This is not due to lack of knowledge of the system; rather it is because the palpation and recognition of the signs using tactile input requires a considerable amount of dedicated time and practice in which to develop. As with all skills, the speed and quality of reading depends upon the frequency and amount of use. The ability to palpate with any finger or fingers can usually be developed, the use of the index finger being the most popular. Reading speed is further enhanced by using the fingers of both hands. In some cases, this skill never develops if the individual has not learnt to employ touch from an early age. In rare instances, people who have been unable to use their fingers have developed the same ability to read Braille by using their toes or even their lips! (see above). This means that regardless of the method by which this skill is acquired, the ability to increase the information received through sensory input can be improved, given time and serious dedication to regular practice. This can be of great benefit to the clinical practitioner who wishes to ‘read’ information that lies deep to the skin. The controlled use of pressure and movement, coupled with feedback and experience, unlocks a vast quantity of information that is often unavailable to the eye.
Obtaining information through touch is a skill, the practical significance of which is often not fully appreciated or valued until it is needed, perhaps to compensate for the impairment or loss of one of the other senses: sight or hearing, for example. Because of this, considerable practice is often required before the skill of palpation becomes developed to the point where it is of practical use to the individual concerned (see above). Initially, new techniques have to be devised and then undertaken slowly and carefully, with regular practice and evaluation, often involving feedback from other observers with consequent modification of behaviour. Efforts to recognize and accurately interpret tactile sensory input demand high levels of concentration which necessarily cause anxiety and additional stress to an individual who is unaccustomed to placing such reliance on this variety of incoming stimuli. These reactions are likely to be experienced by the novice clinical practitioner as well as by the recently disabled person and should be regarded as normal responses to the process of acquiring a new range of sophisticated psychomotor skills and personal strategies (Owen Hutchinson, Atkinson and Orpwood 1998).
In other non-medical contexts, touch-related skills are used to acquire general information about the environment such as establishing the temperature of water. A thermometer could be employed for this purpose, but it is often easier (and quicker) to test water temperature by utilizing the input from the sensory endings in the skin. While the results of this method of temperature testing are likely to be far less accurate than if a thermo- meter were to be used, they provide a range of potentially significant information upon which subsequent action could be based. The water temperature, for example, might be experienced as burning, scorching, boiling, extremely hot, very hot, fairly hot, hot, quite hot, very warm, blood heat, warm, fairly warm, slightly warm, cool, cold, quite cold, very cold, bitterly cold, freezing and icy cold. A temperature of 42°C read from a thermometer has little practical meaning as to whether something is too hot or too cold to touch.
The social significance of touch
The concept of the novice engaged in learning to interpret incoming stimuli received through touch extends, of course, into the realm of social interaction. As suggested above, touch can represent a powerful means of expressive communication (Nathan 1999). The way in which this communication is interpreted will be contingent upon such variables as personality, upbringing, culture and social situation and, in these contexts, it seems unhelpful to separate touch into mechanical and psychosocial categories. Referring to a medical intervention, Nathan contends that:
Touching a person’s body in a non-therapeutic context is not normally considered an act of merely mechanical significance. Nor is it a procedure of a technique – rather it is an act of self-expression, or occasionally self-assertion, or preservation.
The degree to which people will engage in touching will be dictated by the nature of the interpersonal relationship in which they are involved at the time. Nathan continues:
In the main, frequent touching is reserved for parent–child relationships, lovers and close friends. In these contexts it both signifies emotional intimacy and is emotionally significant.
Touch can be employed to communicate a variety of emotions. For example, affection may be conveyed by a gentle squeeze of the hand, whereas a loose handshake may imply indifference or even dislike. Touching and being touched can be extremely therapeutic. Montague summarizes the observations of many researchers who conclude that:
Cutaneous stimulation in the various forms in which the newborn and young receive it is of prime importance for their healthy physical and behavioural development …. It appears probable that for human beings, tactile stimulation is of fundamental significance for development of healthy, emotional and affectional relationships.
Montague quotes examples of cases that were studied by Lorna Marshall, a researcher who spent much time between 1950 and 1961 living among the Bushmen of the Kalahari Desert in Botswana, South West Africa. He observed that, within this society, the development of the newborn, infant, adolescent and adult appeared to be influenced by the way in which the child was handled in early life. Montague also refers to accounts by Margaret Mead, who studied the Arapesh and Mundugumor societies in New Guinea during the 1930s and documented the characteristics of their respective social practices. In the former tribe, the child was in contact with the mother for most of the day. The adults of this tribe were observed to be kind, happy and peace-loving people. In the latter tribe, the child had little human contact, being kept in a rough plaited basket which was usually suspended from the mother’s forehead. The adults of this tribe were observed to become unattractive, aggressive and cannibalistic.
The tendency to avoid close physical contact can be demonstrated in adults from certain cultures and within some social backgrounds of particular nationalities. Montague comments that ‘There exists not only cultural and national differences in tactile behaviour but also class differences.’ He cites the English upper class as a an example of a social group that is characterized by non-tactile social behaviour when compared with social groups of other nationalities: French and Italian people display more demonstrative behaviour when greeting one another and are observed to engage in more physical interpersonal contact.
When considering the practice of palpation skills, the significance of Montague’s observations cannot be underestimated. Not only is it crucial for us to recognize the relevance of culture, nationality and social class on the degree to which people communicate by touch, but also the impact of living in a multicultural society in which we are likely to encounter unfamiliar and potentially disconcerting practices. Additionally the effect of globalization on our patterns of non-verbal communication has been considerable.
In contrast to the somewhat reserved behaviour of English people in the 19th and early 20th centuries, we now regularly witness overt instances of emotion (love and friendship, happiness and sadness) through physical contact. Behaviour such as mutual embracing, hand-holding and kissing is frequently to be observed in public places. Sportspeople will leap in the air and hug each other following a winning achievement such as the scoring of a goal in football; equally, it is not uncommon for athletes to display tears of misery and frustration and to engage in mutually sympathetic embraces after a failure to attain high standards of performance.
Touch and clinical practice
Palpation, then, would seem to be a practice which involves a combination of many other skilled activities: the appropriate use of touch, the application of methodical investigatory techniques, accurate interpretation of sensory feedback (based upon sound general knowledge), the ability to draw on previous experience, to reflect, critically, upon findings and arrive at a reasoned conclusion.
Palpation is the art of feeling tissues with your hands in such a manner that changes in tension and position within these tissues can be readily noticed, diagnosed and treated.
A skill is attained and retained by its continual use, evaluation and modification of practice (Phillips 2004). The study and practice of manual contact techniques over a long period of time enables the practitioner to become highly skilled in the art of palpation. The development of this skill provides valuable supplementary information to that which can be obtained through observation and verbal questioning and is crucial to arriving at a meaningful clinical diagnosis. After many years experience of practising palpation skills, the moving, stretching and compression of tissues will be undertaken with precise control. This will enable the therapist to receive and interpret vital information from the patient and to apply and modify techniques as appropriate. Small changes in tension, temperature, dampness, movement and swelling will be identified by the sense of touch; these will then be noted and the appropriate course of action taken. Grieve states:
Of the entire objective examination of the vertebral column, the palpation examination of accessible tissues is probably the most informative and therefore the most valuable.
As has been noted above, however, learning to palpate is also associated with acquiring the skills to ‘read’, accurately, the patient’s problem. Citing Ford (1989) Chaitow reminds us that:
In days gone by, when a physician had to diagnose by touch a good practitioner did not feel a tumour at his fingertips but he projected his vibratory and pressure sensations into the patient. So we regularly project our sense of touch beyond our physical being and … merely make the ordinarily unconscious process available to our conscious mind. In so doing, we cross the delicate boundary between self and other, to explore, to learn, and ultimately to help.
Personal experience confirms that patients can easily distinguish between a novice and an expert practitioner. During the initial examination, both the practitioner and the person being palpated progress through a learning process in which each is engaged in assessing the other by the giving and receiving of information. Relatively little significant information can be obtained if one of the participants in this relationship is reluctant to communicate. This learning process takes time and it is often the case that an accurate picture of the underlying issues does not appear until much later in the treatment session. The reason for this is partly due to the need for each participant to become comfortable with the other, so permitting mutual reduction in anxiety and the relaxation of tension. It is also due to the need for both parties to become familiar with the learning process itself, so that each can benefit from the knowledge gained as a result of their participation in this two-way event. The skill of palpation, therefore, should not be regarded merely as an arbitrary form of physical intervention; rather it must be respected as a highly skilled investigative process which elicits specialized information to both participants. In our experience, the skill of palpation is estimated to be only 10% innate: the other 90% is acquired through dedicated practice.
Effects of palpation on the patient
Patient and person
It is far beyond the scope of this book to enter into the complexities of the mind–body debate, but its significance in relation to clinical diagnosis and management cannot be ignored. Traditionally, medical practice has been characterized by the biomedical model of health. This model is underpinned by the philosophical principles of dualism: the mind and body are regarded as separate and distinct entities that do not interact and, essentially, the practitioner is engaged in treating one or the other. The manual therapist would, in this context therefore, be regarded as being concerned only with the treatment of the patient’s body. Indeed, it is not uncommon to hear therapists refer to a patient as ‘a neck’ or ‘a back’. The body is considered to resemble a sophisticated machine; if part of that machine is malfunctioning, physical intervention is required in order to rectify the fault (Chaitow in Nathan 1999, Christensen, Jones and Edwards 2004, Owen Hutchinson 2004).
The 1990s, however, have witnessed significant changes in the approach towards illness and disability with the consequent development of the biopsychosocial model of disability which ‘is a way of conceptualizing the multifactorial and complex system that shapes a person’s experiences of pain and disability’ (Christensen, Jones and Edwards 2004). Citing various sources, Christensen, Jones and Edwards explain the biopsychosocial theory:
… the degree of disability a person develops will be based upon the reactions of that person to the pain experienced far more than on the physical experience of the pain itself. The biopsychosocial model places a complaint of pain into a more holistic context, and views the pain as important not in isolation, but in relation to any disability the person with pain is experiencing as a result of that pain.
(See also Ramsden 1999, Stevenson, Grieves and Stein-Parbury 2004.)
The last decade has also witnessed a growth in the popularity of complementary medicine, whose underlying holistic principles stand in direct contrast to those of orthodox medical practice. This trend would suggest that patients prefer to be treated as whole persons rather than as bodies requiring cures. When they seek consultation with a therapist, patients are asking for help with more than just a painful neck or back: they want far more than to be the passive recipient of skillfully performed physical techniques. Indeed, patients regard a satisfactory healing experience as one that acknowledges the inextricable links between mind and body and which therefore treats the whole person who is more than just the sum of a collection of constituent parts. Recognizing this, the therapist must adopt an empathic and sensitive approach to all input from the patient, both in terms of verbal and non-verbal communication. Social and cultural factors must also be taken into account.
The quality of all clinical interventions will improve dramatically if the person-centred approach to patient management is adopted. The therapist, however, should not underestimate the degree to which patients have learned the conventions associated with society in general and medicine in particular. During the session, patients will often choose to use language to conceal as well as to reveal emotional states: ‘That movement does not hurt any more’; ‘I feel much freer now’. It must always be remembered that the patient has this choice. It must also be borne in mind that some patients may not have recognized the link between physical and psychological states and may need to be encouraged to reflect upon their choice of language in order to gain insight into certain aspects of their emotional lives.
As has been suggested above, the act of touching and the feeling of being touched are very powerful experiences and the degree to which people engage in touching is largely contingent upon personality, cultural and social factors. Both patient and therapist may experience an increase in stress levels due to unfamiliarity within particular therapeutic contexts. The practitioner must demonstrate a respect for the patient as a person. Permission to touch should be obtained at the commencement, and during the various stages of a clinical intervention. Abuse of power and the privilege of being licensed to touch must be avoided.
The consultation process
For a variety of physical and psychosocial reasons, many patients remain reluctant to consult professional personnel on matters associated with their personal issues, especially those problems relating to their own bodies. Barriers may be erected by one or both participants in the therapist–patient relationship, although both must contribute to the dismantling of these barriers if effective communication and co-operation are to be achieved. Experience suggests that each patient usually presents with a combination of issues which are revealed by the identification of problems, the giving of information and the posing of a number of questions during the consultation process. Typically, no particular order of priority emerges except perhaps that associated with the overriding presence of pain. Some of the information provided by the patient may appear to be somewhat peripheral in relation to the practitioner’s objective of establishing a clinical diagnosis, but it nevertheless represents a vital component of the overall clinical picture and must be thoroughly evaluated before it can be discounted.
The practitioner must be sympathetically receptive to all forms of information offered by the patient. Standards governing all areas of professional practice demand that the clinician must objectively evaluate all clinical evidence and attempt to produce a comprehensive analysis of the presenting situation. On some occasions, a prescribed plan will be used to facilitate the compilation and evaluation of data; at other times, the practitioner will be expected to tailor the procedure according to the patient’s individual circumstances. The use of such strategies will enable the practitioner to arrive at a reasoned clinical diagnosis. Care must be taken, however, that any prescribed plan does not preclude the practitioner from obtaining relevant information from the patient; adherence to such standard pro forma can sometimes adversely affect the practitioner’s judgement and thus lead to an incorrect clinical assessment of the patient’s current problem.
It is crucial that the practitioner should manage the initial investigation with great care and sensitivity as this process is likely to have a significant influence on both parties during the subsequent clinical examination. The practitioner should exercise the same degree of tact and diplomacy when conducting the subsequent physical examination, which should be undertaken with equal care, precision and gentleness. Physical or verbal clumsiness at this stage of the proceedings could lead to a complete breakdown of the interpersonal relationship between the therapist and patient, who may become reluctant to communicate vital information. The therapist employs palpation techniques during the first contact with the patient and it is vital that efficient methods of obtaining information are employed at this time. Experience suggests that most patients have an expectation that a clinical examination involving the use of palpation techniques will take place; indeed, they would consider it to be unprofessional practice if such a procedure were not undertaken. Inevitably, each person will exhibit different reactions to being touched and it is important that the practitioner should establish and evaluate the patient’s unique reaction to such interventions at the earliest opportunity. An initial indication of the patient’s reaction to physical contact can be obtained by the act of hand-shaking at the commencement of the session. Additionally, information gained by the act of assisting the patient to and from a chair can provide the practitioner with valuable feedback relating to the patient’s degree of willingness or reluctance to accept help. Of course, such strategies represent only part of the range of techniques being employed during this initial session. The use of visual, auditory and olfactory input can also provide useful sources of relevant clinical information.
During the period of questioning, the practitioner is recommended to make sensitive and careful physical contact with the area of the patient’s pain. When these techniques are performed successfully, this encourages both parties to focus attention on the patient’s motivation in seeking the consultation. All movements should be tested carefully, palpation skills being employed simultaneously with continual observation of the ongoing situation, the therapist monitoring any reluctance on the part of the patient to perform movements due to tension, muscle spasm, joint anomalies and pain. Inadvertently eliciting symptoms of acute pain will inevitably destroy the patient’s confidence, resulting in an unwillingness to offer potentially significant information.
In most cases, the patient will gradually gain confidence and learn to trust the practitioner. Much of the apprehension of meeting will have passed during the initial contact. When the time comes for the therapist to undertake an objective physical examination of the patient’s movements, rapport should have been well established which overcomes that initial reluctance to seeking of medical advice.
Palpation continues throughout the examination and subsequent treatment. If it is carried out carefully and sympathetically, it reveals valuable information concerning the patient’s physical and psychological condition. Indeed, palpation has the potential to ‘unlock’ psychological issues which had hitherto been deliberately ignored or unrecognized by the patient as having any relevance to the presenting physical problem. Many practitioners will have experience of patients who seek medical consultation for a relatively minor physical ailment which, during the examination or treatment, will be found to be masking much deeper and more complex issues. All practitioners should be sensitive to this possibility and should note any incongruous sentiments that the patient may express during the session. Experience suggests that it is the physical contact with the patient which appears to facilitate the unveiling of these underlying issues, but the importance of recognizing this phenomenon is contingent upon the quality of the practitioner’s professional training.
That the patient must have confidence in the practitioner cannot be over-emphasized. This will promote the offering of information through both verbal and non-verbal communication methods. Throughout the consultation, the practitioner should be receptive to the patient; as the session progresses, continual evaluation of the patient’s verbal and non-verbal reactions to events should take place. Whether complex or simple, all treatment sessions should promote mutual trust and understanding. Experience indicates that the degree to which a patient contributes to the treatment session is directly proportional to the practitioner’s input; this reciprocal relationship is, however, contingent on the practitioner’s willingness to impart information and the patient’s genuine interest in receiving it.
Techniques of palpation
It is not enough merely to place the hands on the patient’s body and hope to receive the information required. Positive steps must be taken to search for the data. As has been noted above, palpation is associated with the seeking of information and all techniques must be approached in a rational and logical manner. The practitioner can gain very little by contacting a surface with the hands and remaining stationary. Movement of the hands is required so that structures can pass under the fingers in a controlled manner so that any alterations in skin temperature, surface tension, and bone structure can be evaluated and recorded. The practitioner’s speed of movement can be adjusted to facilitate the full interpretation of information. The importance of regularly modifying the speed of movement can be demonstrated by the following example. If the fingers are run over Braille script too quickly, dots can be felt but no information is obtained; if the individual adapts the speed accordingly, however, what initially appeared to be an incomprehensible mass of dots now becomes an intelligible text.
Sometimes palpation techniques need to be performed slowly and at considerable depth; at other times they should be carried out quickly and at a superficial level. For example, palpation of the transverse processes of the spines of the lumbar region or the hook of the hamate needs careful application of deep pressure, combined with slow movement and sensitivity to the patient’s reactions. Palpation of the spines of the thoracic vertebrae – particularly when counting downwards – is much easier if the fingertips are gently moved up and down three or four centimetres at a time, marking each spine with the finger of the other hand and holding it until the position of the next spine is confirmed. This type of palpation works in a similar way to a scanner using a beam to build up a clearer picture. The technique can be used to obtain a clearer picture of the rib cage, particularly from the posterior aspect.
In our experience, using one or even two complete palms and fingertips conveys more information regarding movement below the skin surface and about the patient’s general reaction to physical contact than if the fingertips alone were used. The application of the fingertips alone, for example, would be used for palpating a pulse. Generally, if the structures below the surface are stationary, the hands will have to be used in a controlled movement, whereas if the structures are mobile, the hands should remain stationary. The finer the movement below the surface, the more delicate the palpation technique must be: this is clearly demonstrated when searching for a faint pulse.
If joints are being manipulated to examine the quality of movement and to assess limiting factors, the hands should be moved as little as possible so as to avoid any feedback from the palpator’s own tissues which would obscure information from those of the patient. In fact, with this kind of palpation, a minimum of all other movements – with the exception of the joint being examined – is required. This involves adopting a stance which will avoid movement of the feet, applying a hold that will allow the full range of movement without change and also reducing all skin sliding by firm contact. Finally, the palpator must be absolutely sure that the patient’s position is stable and that the movement being tested is localized to the joint being examined and is in the plane around the axis required. It is not uncommon, when testing the movements of the upper or lower limb, for a ‘clicking’ or crepitus to occur and neither the patient nor the examiner are able to locate its source. Conversely, if the examiner’s thumb nails touch when pressure is being applied to the posterior aspect of the lateral mass of the atlas (C1), the patient may, erroneously, report a grinding sound located in the atlanto-occipital joint.
When examining the end-range of a joint, all variations must be known in advance so that movement, physiological and accessory, is tested accurately, noting the range available and the limiting factors. This is a highly skilled form of palpation, requiring a great deal of practice on normal joints in order to perfect the technique, considerable experience with abnormal joints to be able to recognize the variations and an expert knowledge of the various conditions to assess how much or how little testing should be undertaken. It is not suggested that this form of palpation should be employed by an expert only; on the contrary, the technique should be practised at the earliest opportunity and based on palpation of normal anatomy. Gradually, if care is taken and limits set, considerable skill can be gained.
Experience suggests that some palpators either under-employ the use of touch and try to compensate by observation, or they tend to palpate over-enthusiastically but fail to interpret the significance of what they feel. Some may also feel what they believe they are meant to feel. It is easy to be persuaded by an eager patient, by prior knowledge or by a more experienced observer that one can feel changes that are not actually present. An open and honest interpretation of what is beneath the fingertips is essential: remember Hans Andersen’s story of the Emperor’s new clothes!
Improving the art of palpation
Returning to the example of the Braille reader, improvement in palpation techniques can only be achieved with practice. As with all areas of knowledge, the motivation to learn is crucial. In relation to clinical practice, the learning of good palpation skills is contingent upon the need to know what lies beneath the surface of the body and the desire to find some means of offering help to patients. Practitioners frequently express the wish to be able to ‘see what is happening beneath the surface’. These sentiments confirm the importance of developing appropriate palpation techniques which can then be employed as a means of providing assistance. Inextricably linked with this process is the development of manual dexterity and sensitivity.
It is worth noting that, when practising any technique that necessarily involves the use of the hands, the quality of the information that is received through the sense of touch can often be enhanced by reducing the input from the other senses. Closing the eyes and using the hands to recognize different textures, weights, surfaces, liquids, coins, etc., often reveals hitherto unrecognized characteristics of what are regarded as familiar objects. The palpator must endeavour to obtain as much information from the sense of touch as possible. In order to develop this skill, different objects can be placed in a bag and identified only by using the hands. As the skill improves, less familiar objects can be chosen so that they are less recognizable: their shape might be more unusual and/or they may be smaller. All of these objects should be handled sensitively by the palpator who should attempt to identify their distinctive features (such as blemishes). Progression of this exercise would be to require the palpation and identification of the same objects through the material of the bag. The material of the bag could be chosen so that the exercise becomes progressively more difficult: beginning with a relatively thin surface such as fine plastic and gradually changing to a thicker material. Practise should be undertaken regularly during the course of everyday activities, the practitioner always noting the technique which is most suitable for the identification of each object. One suggestion would be habitually to identify the loose change in a pocket or purse before removing the correct amount to make a purchase. Recognition of coins is a relatively easy task and it should be unnecessary to use vision in order to verify the amount tendered. Take care: this could prove to be an expensive way to learn the art of palpation if adequate practice is not undertaken! Another exercise might be to select clothing on a daily basis using tactile and not visual input. It is a salutary point that all visually impaired people necessarily employ these tactual skills every day.
The development of the sense of touch needs to be nurtured. It is recommended that each contact with an object should be treated as if no visual or auditory input is available whilst attempting to obtain the maximum amount of information. Those who have the privilege of handling patients professionally possess a constant source of practice in their study of structure and function and examination of normal and abnormal phenomena. Those professionals are even more fortunate if they specialize in the use of massage, movement, mobilization and manipulation techniques as part of clinical practice. Individuals who have undertaken formal study and practice of the art of massage are indeed already well versed in the appropriate knowledge and skills relating to palpation. Their contribution to the increased public recognition of palpation as a crucial element in the diagnosis and treatment of clinical conditions cannot be underestimated. Indeed it is gratifying to note the increased status of all the manual therapies during the past decade: people are deliberately selecting practitioners who possess skills that rely on touch for their efficacy. It should never be forgotten, however, that all such therapists are required to demonstrate a serious commitment to Continuing Professional Development (CPD): they are required to revise and update their anatomical and physiological knowledge on a regular basis in order to maintain the high standards of professional practice demanded by their respective professional organizations.
Care of the hands
All skills in which complex manual techniques are employed in the performance of precise movements necessarily rely on the regular care and maintenance of the hands: their mobility, sensitivity and dexterity. Prior to engaging in any form of manual contact, however, the practitioner should ensure that the temperature of the skin is warm; patients do not appreciate being touched by therapists whose hands are cold!
Cleanliness is essential and its positive contribution to the quality of tactile input cannot be underestimated. Traces of grease, cream, dirt, dust, etc., effectively create an additional intervening layer between the sensory receptor organs and nerve endings in the hand and the object or subject to be palpated. It is significant that most Braille readers will make every effort to keep their hands clean while reading Braille; many tend to avoid eating anything sticky in order to prevent their fingers from losing sensitivity. A routine of washing the hands in warm water using a mild soap and drying them thoroughly after washing should be adopted; the use of additional creams or ointments is not recommended unless this is absolutely necessary. A good, oil-based hand cream can be used at night in order to maintain a smooth, soft condition of the skin; some authorities also recommend the regular use of Vaseline and sugar. Whichever maintenance routine is adopted, the hands must always be washed thoroughly prior to attempting palpation techniques. In addition, the nails should be kept clean and short so that the risks of injury or infection are avoided. No wrist or hand jewellery should be worn. The quality of the palpation depends, to a great extent, upon the texture and suppleness of the hands. They should look and feel good, thus promoting the patient’s confidence in the palpator. Poorly maintained hands which are dirty, stiff and with hard skin will be off-putting to patients: a reluctance to be touched will act as a barrier to the passage of information from the body of the patient to the receptors of the palpator.
The joints of the hands must be maintained in a supple condition with the musculature being firm and strong. Regular exercises should be practised in order to maintain joint mobility and increase muscle strength. Contact with all abrasive surfaces and detergents should be avoided as far as possible and gloves should be worn at all times when manual work is performed, particularly during activities such as washing-up, cleaning, gardening, car maintenance and building work. Many liquids, certain soaps and detergents, tend to remove the natural greases from the skin and the use of these should, therefore, be minimal. Any activity that is likely to lead to the production of blisters, finger calluses or general hard skin should also be minimized: examples might include such pastimes as rowing, playing a stringed musical instrument, rope-climbing and woodwork. Additionally, great care must be taken when using sharp instruments or engaging in any activity that is likely to cause trauma and/or skin infection. Lack of vigilance whilst performing any of these activities may prejudice the ability to perform high-quality palpation techniques.
Palpation of different tissues
Experience suggests that normal palpation when performed by the lay person – and even when undertaken by some professionals – is sometimes ineffective. It may enable the operator to differentiate between such tissues as bone, muscle or tendon, etc., but often does little more. By contrast, the skilled student practitioner will be able to distinguish different parts of bones, contrasting shapes and texture of muscles, identify their connections to tendons and trace them to their attachments. Such students will also be able to count vertebrae, palpate lumbar transverse processes and other deep bony structures, locate certain ligaments, palpate elusive pulses and determine abnormalities such as different types of swelling, misalignment and rupture. The expert clinician must progress far beyond this concept in order to complete the picture that lies hidden within the body. Bony landmarks should be studied, linking them together and obtaining a clear mental image of the skeletal layout. This programme should include studying rib angles, transverse processes and spines of all vertebrae including their differing features. For example, the bifid spinous processes of the cervical region contrast with the pointed spines in the thoracic and the rectangular-shaped spines of T12 and in the lumbar region. Alignment of one bone to another is relatively easily examined in the upper and lower limbs, whereas this is much more difficult to examine in the vertebral column. Defects in the contour of a bone can also be located and possible avulsions recognized.
Variations in muscle texture should be identifiable and note taken of differences occurring in normal muscle, enabling the examiner to recognize any abnormal variations. Some muscles, such as gluteus maximus and the middle fibres of deltoid, have a coarse structure due to the type of muscle fibres involved, whereas muscles such as the oblique abdominals and quadratus lumborum have a smoother texture. Fibrous tissue between the muscle fibres may give a stringy feel, while local areas of spasm are hard but regular in shape. The former tend to remain in the same position irrespective of what technique is performed on them; the latter will often disappear on applying either heat or massage. Both types of muscle spasm can be found in the rhomboid muscles between the scapula and spinous processes of the vertebral column.
Careful palpation will reveal where each muscle joins its tendon and where and how the tendon is attached. Palpation can also determine how tightly the muscle is bound down by fascia and whether the tendon is maintained in its position by a retinaculum. The extent of the retinacula can be examined and a study made of those structures which pass under or over them.
Swellings in muscle are often caused by bruising (contusion) and bleeding (haematoma) between the muscle fibres. These are normally contained within a localized area and become hard and painful, often warm to the touch and sometimes produce redness over the area. There is nearly always a history of trauma to the region. Care should be taken, however, when palpating any area of swelling as this symptom could be caused by other more serious conditions. It is important to be sensitive to local changes in temperature, noting whether these are higher or lower than expected. The condition of the underlying structures must be recorded and a knowledge of the possible causes of such variations will contribute to the establishment of a clinical diagnosis and subsequent treatment of the condition.
When palpating joints, other considerations must be taken into account. The precise location of the joint line is essential, the quality of this technique being based on the accurate identification of bony landmarks and measurements, taking into account the general size and shape of other bones and the patient’s posture at the time. A detailed knowledge of the structure and extent of the adjacent joint surfaces, as well as where ligaments may obscure the joint space, is essential. The presentation of tissue-filled joint spaces under differing circumstances – for example, whether fluid is contained within the joint capsule or within a bursa – together with a detailed knowledge of the surrounding tendons is also a necessary pre-requisite when examining joints. As Chaitow points out:
There are many important features to note during the examination of joints: the range and smoothness of movement, whether the axis varies according to the position of the joint and to what degree movement may be limited. Employing great care and skill, movement of joints can be examined indirectly through the bones of either side of that joint. The movement between the joint surfaces may be experienced as smooth or grinding; the restriction felt at ‘the end of a joint’s range of motion may be described as having a certain feel and this is called (the) ‘end-feel’.
In his discussion of barriers to joint movement Chaitow continues:
If there is, for any reason, a restriction in the range of motion then a pathological barrier would be apparent on active or passive movement in that direction. If the reason for the restriction involved interosseous changes (arthritis, for example) the end-feel would be sudden or hard. However, if the restriction involved soft tissue dysfunction the end-feel would have a softer nature.
Most joints possess additional movements which are of small range and not under voluntary control: these are essential for the efficient functioning of the joint. These are known as ‘accessory’ movements.
Accessory or joint play movements are those movements of a joint that cannot be performed actively by the individual. Such accessory movements include the roll, spin and slide which accompany a joint’s physiological movements.
A simple example of this type of movement would be found in the axle of a bicycle wheel. On each side, the axle is surrounded by a ring of ball-bearings maintained in position by a cone which screws on to the axle. When the cones are loose, they allow the wheel to be moved slightly from side to side; when the cones are tight, there is no side-to-side or accessory movement. When there is side-to-side movement, the wheel is free to turn; as the cones are tightened, the ball-bearings become ‘close packed’ and more difficult to turn so finally locking the wheel. The side-to-side (or accessory) movement is thus essential for the free turning of the wheel, since its elimination results in no movement.
Accessory movements are most demonstrable in human joints within a certain range of the joint movement: when the ligaments allow joint surfaces to be parted or when the surfaces are not congruent. This is termed the ‘loose packed’ position. When the ligaments of a joint become taut and its surfaces are congruent, no further movement is possible, either physiological or accessory. The joint is now said to be in a ‘close packed’ position (Standring 2004). If the accessory movements of a joint are lost, the joint becomes extremely difficult to move, similar to the cones of the bicycle wheel being tightened (see above). If, however, accessory movement is restored, as in loosening the cones in the bicycle wheel, normal movement is also restored. The restoration of accessory movements is an important principle underlying the practice of mobilization and manipulation techniques to restore normal movement in joints. With care and expertise, by using a combination of accessory and normal movements, joint function can be assessed and the treatment varied accordingly. The use of ‘quadrant’ techniques (combined movements at the end of range) is a good example of this testing. (For further information on the application of these types of examination and techniques, see Grieve 1986, Hengeveld and Banks 2005.)
Chaitow’s definition of ‘joint play’ is also useful:
Joint play refers to the particular movements between bones associated with either separation of the surfaces (as in traction) or parallel movement of joint surfaces (also known as translation or translatoric gliding).
This information is important in establishing the joints’ condition.
Swelling around a joint deforms its shape and contour, the extent of the deformity being dependent upon the degree of swelling involved. The bony features can usually be identified between the areas of swelling. In some instances, the swelling is so profuse that it is difficult to locate bony landmarks; on other occasions, the amount of fluid is so small that precise techniques have to be employed to palpate the swelling which is interfering with normal joint function. Most joint swelling is contained within the capsule, causing a build-up of pressure which results in increasing pain. The swelling may have to be removed surgically, although this is usually deferred until absolutely necessary because of the risk of infection into the joint. Blood can also escape into a joint space (haemarthrosis), resulting in a similar appearance, but this is usually accompanied by some discoloration and an increased local temperature. Any swelling can lead to severe damage to the mechanics of the joint; this damage may vary according to the type of fluid involved.
Careful palpation of the swelling can produce more information than at first thought. The swelling may appear soft and movable with the application of pressure; this often gives a fluid feel as it passes from one part of the joint cavity to another. Alternatively it may appear thick and pliable although difficult to move unless sustained pressure is applied. Swelling may appear to be a solid mass, pitting under pressure from the fingers but taking a considerable time before signs of movement are evident.
Summary
Palpation is a detailed examination using the hands as tools to enable the palpator to elicit information about structures beneath the skin and fascia. It is, in our opinion, still under-used and undervalued, mainly because of lack of practise and appreciation of its intrinsic value. In addition, its teaching and practice are time-consuming, requiring expert instruction from experienced practitioners, genuine interest, patience and commitment from students. While its techniques can be practised and developed, however, expertise, takes time and dedication to acquire.
Palpation is more than just a desire to ‘see’ through the skin and interpret the underlying anatomy. It can be developed in such a way that information can be imparted to the patient through the practitioner’s hands. It is not difficult to appreciate the ways in which the expert palpator can employ the art of instrumental and expressive touching in combination to obtain clinical diagnosis and establish sympathetic communication. Indeed, the philosophy that underpins the practice of many therapists emphasizes the intrinsic therapeutic qualities of touch per se (see for example Charman 2000, Dennis, Jones and Holey 1995, Everett 1997, Nathan 1999). Healers who practise the ‘laying on of hands’ and Therapeutic Touch also share this belief (see Krieger 1986, 1993, 1997, 2002, Macrae 1987, Sayre-Adams and Wright 2001). The increasing popularity of complementary therapies amongst the general public further confirms the general tendency to place considerable value in a holistic approach to patient care. Rather than relying solely on orthodox medical practice, patients and therapists alike are now recognizing the importance of healing in the management of chronic physical and psychological problems (Charman 2000, Nathan 1999).
Palpation must be learned, practised and developed before it can be applied professionally. The study of anatomy, physiology and the human sciences, together with the additional information obtained through the appropriate use of touch, are excellent ways of learning the art of palpation. Anatomy will become clearer and more understandable as the hands become more sensitive to what lies below the skin, leading to an enhancement of knowledge and improvement in assessment: an asset in therapeutic application. Finally, and perhaps most importantly, the skilled palpator should be aware of the patient’s reaction to movement. By observing the patient’s face, listening to the patient’s comments and being sensitive to all reactions in muscle and joint movement, a total picture of the patient’s condition becomes available. With care and sensitivity, a great deal of information can easily be obtained.
The following pages contain a detailed study of the surface markings of many of the body’s structures, including a guide to the palpation of particular areas. It must be remembered, however, that the development of effective palpation skills for the purposes of clinical intervention requires more than the acquisition of sound theoretical knowledge upon which to base practice. As Chaitow emphasizes, expertise in palpation techniques is achieved ‘… by application (and repetition) of hundreds of carefully designed exercises that are capable of refining palpation skills to an astonishing degree of sensitivity’ (Chaitow 2003).
Citing Frymann (1963) he adds:
… palpation cannot be learned by reading or listening; it can only be learned by palpation. This learning process is not just about hard dedicated labour; it should be fun and it should be exciting. The thrills to be experienced when taking this journey of exploration of the tissues of the human body is hopefully contagious …
We hope that readers will take inspiration from this and other related texts and strive to attain expertise in palpation skills in the interests of improving the quality of their clinical practice.