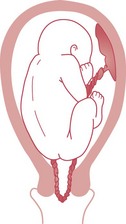
Chapter 67 Presentation and prolapse of the umbilical cord
Introduction
In approximately 0.1–0.6% of births, the umbilical cord descends below the presenting part (RCOG 2008). The cord vessels may become occluded by pressure of the descending presenting part, potentially resulting in irreversible brain damage, stillbirth or neonatal death. There are three variants:
Causes
Presentation and prolapse of the umbilical cord may occur in any situation which results in a poorly fitting presenting part: normally, the well-flexed fetal head enters the pelvis in late pregnancy or early labour, fitting snugly, to prevent the descent of the cord.
Risk factors
(Dilbaz et al 2006, Kahana et al 2004, RCOG 2008, Sheiner et al 2004).
Diagnosis
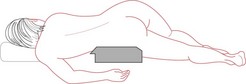
Vaginal examination may reveal a cord presentation, the cord being palpated through the fetal membranes. Pulsation, synchronous with the fetal heart, may be felt. If the presenting part is high, the cord may float away from the examining fingers. Uterine arterial pulsation will be felt in the vaginal fornices, synchronous with the maternal pulse. Therefore, the midwife should auscultate the fetal heart and simultaneously take the maternal pulse if she is unsure of the source of pulsation. If a cord presentation is suspected, the midwife must aim to keep the membranes intact and should attempt to reduce any cord compression by placing the mother in an exaggerated Sims’ position with the hips and buttocks elevated by a wedge or pillows (Squire 2002) (Fig. 67.3). Medical assistance should be called at once and the midwife must stay with the woman. Elevating the maternal pelvis may encourage the umbilical cord to move, but if the cord presentation persists, the fetus will be delivered by caesarean section.
When the membranes rupture, the fetal heart must be auscultated and a vaginal examination made in order to diagnose cord prolapse. The risk of cord prolapse should be borne in mind whenever there is a high head, malpresentation or malposition, polyhydramnios or multiple pregnancy. The prolapsed cord may be palpated in the cervical canal, in the vagina or may be visible at the vulva. The midwife should assess cervical dilatation and the descent of the presenting part, as management of this condition depends upon the stage of labour.
Dangers
Umbilical cord prolapse has a perinatal mortality rate of 50% (Dilbaz et al 2006). There may also be considerable morbidity from hypoxic-ischaemic encephalopathy and cerebral palsy (RCOG 2008).
The main risks to the fetus are:
The prognosis for the fetus depends upon prompt recognition of the prolapse and speedy delivery.
Management of cord prolapse
The management will depend upon the stage of labour and whether the fetus is alive or dead.
Key points
Absence of both cord pulsation and fetal heart are suggestive of fetal death, but this should be confirmed by ultrasound scan. If fetal death is confirmed, labour will proceed without intervention, as a caesarean section would not be performed for a dead baby. If the fetus is known or suspected to be alive, the treatment is immediate delivery, which may be instrumental or by caesarean section. The midwife must attempt to keep the fetus in good condition until delivery is effected.
Prelabour and first stage
Obstetric, anaesthetic and paediatric assistance is summoned urgently and the time that the prolapse was detected is noted.
If this emergency occurs at home, the midwife should call the paramedic ambulance service at once.
Meanwhile, the midwife must manage the emergency and conserve the fetal condition:
There is insufficient evidence to recommend the practice of umbilical cord replacement (funic reduction) in managing cord prolapse (RCOG 2008).
The obstetrician may prescribe an intravenous infusion of a tocolytic drug such as terbutaline to arrest uterine contractions.
Bladder filling
An effective alternative to digital pressure to displace the presenting part is bladder filling, especially if there may be a delay between the cord prolapse and delivery, such as may occur in the community (Houghton 2006, RCOG 2008). Either the foot of the bed should be elevated to provide a head-down tilt or the woman placed in the Trendelenburg position (Fig. 67.4). A 16G self-retaining (Foley) catheter is passed into the bladder. Sterile normal saline (0.9%) is instilled, using a bag for intravenous infusion and an intravenous fluid administration set connected to the catheter. This procedure has been shown to dislodge the fetal head to 2 cm above the ischial spines and should relieve pressure on the umbilical cord. The amount of fluid required is assessed by the degree of elevation of the presenting part but would probably be a minimum of 500 mL. The fetal condition should be continuously monitored and response to this intervention assessed (Katz et al 1988, RCOG 2008, Runnebaum & Katz 1999). Once the bladder has been filled, the woman’s position should be altered to achieve a lateral tilt and avoid supine hypotension, which would exacerbate the fetal hypoxia. It is unsafe to attempt an ambulance transfer of a woman in the knee–chest position, and the left lateral position should be used (RCOG 2008).
The urinary catheter is secured by filling the self-retaining balloon and remains in situ until the woman is in theatre and the obstetric surgeon requests that the bladder is drained. Delivery will be by caesarean section, preferably under regional anaesthesia (RCOG 2008).
Second stage
If the cervix is fully dilated and there is no evidence of cephalopelvic disproportion or malpresentation, an immediate instrumental delivery is performed. Late in second stage, the midwife should make an episiotomy and encourage the woman’s expulsive efforts in order to effect a quick delivery. Caesarean section may be the preferred mode of delivery even in second stage if there is evidence of malpresentation which would require correction or if the presentation is breech with the buttocks high in the pelvis.
Reflective activity 67.1
Locate and read your local policy for management of umbilical cord presentation and prolapse. What instructions does it give with regard to midwifery management of such incidents at home and in the community?
Psychological care
The midwife should remember that the woman and her partner are likely to be confused and frightened by the sudden nature of the emergency and the speed with which delivery is effected. This has implications for informed consent in this situation.
Careful explanations should be given as soon as the midwife is aware of the possibility of cord presentation or prolapse. Even if the outcome is good, feelings of powerlessness may cause the couple to feel resentful or angry. The midwife should ensure that she makes the time to discuss the events with them.
Reflective activity 67.2
What are the possible emotional/psychological consequences for the woman and her family following prolapse of the umbilical cord? If you have cared for a woman who has experienced this, reflect on what you observed in her, and her interaction with the baby. What were her perceptions of what happened and how did these match with the ‘professional’ perceptions of events? If there are radical differences, why would this be?
Conclusion
Prolapse of the umbilical cord threatens the life of the fetus. The midwife must be aware of potential high-risk situations and be able to take the appropriate action when this emergency is suspected or detected. The psychological and support needs of the woman and her partner must not be forgotten in the haste to save the life of the baby. The safe management of this emergency demands a high level of clinical and interpersonal skills from the midwife.