Chapter 2. What is health promotion?
Chapter Contents
Defining health promotion
17
Health gain, health improvement and health development
18
Health education, health promotion and social marketing
18
Multidisciplinary public health
19
Involvement in public health
20
The scope of health promotion
20
A framework for health promotion activities
24
Broad areas of competencies important to health promotion practice
25
Occupational standards in health promotion
26
Summary
This chapter starts with a discussion of the definitions of health promotion, and the related terms health gain, health improvement, health development, health education and social marketing. This is followed by an examination of the position of health promotion within the multidisciplinary public health movement. An outline of the scope of health promotion work is offered, with frameworks for activities for promoting health. Broad areas of practice covered by professional health promoters and the core competencies needed are set out with an outline of the framework for national occupational standards. Exercises are included to help you explore the range of health promotion activities and the extent of your own health promotion work.
Defining Health Promotion
Health promotion is about raising the health status of individuals and communities. Promotion in the health context means improving, advancing, supporting, encouraging and placing health higher on personal and public agendas.
Given that major socioeconomic determinants of health are often outside individual or even collective control, a fundamental aspect of health promotion is that it aims to empower people to have more control over aspects of their lives that affect their health.
These twin elements of improving health and having more control over it are fundamental to the aims and processes of health promotion. The World Health Organization (WHO) definition of health promotion as it appears in the Ottawa Charter has been widely adopted and neatly encompasses this: ‘Health promotion is the process of enabling people to increase control over, and to improve, their health’ (WHO 1986).
Health Gain, Health Improvement and Health Development
Health development, health improvement and health gain are terms that are also employed when discussing the process of working to improve people's health. Health development is defined as the process of continuous, progressive improvement of health status of individuals and groups in a population (Nutbeam 1998). The Jakarta Declaration (WHO 1997) describes health promotion as an essential element of health development. Health improvement is frequently used by national health agencies. For example, there is a health improvement section on the Department of Health (DoH) website (http://www.dh.gov.uk) and NHS Scotland calls itself Scotland's health improvement agency (http://www.healthscotland.com). A research study undertaken by Abbott (2002), however, found that people's understanding of health improvement varied and ranged from explaining the term primarily as a government strategy – as a set of activities for the NHS – or in terms of the overarching purpose of health improvement. One definition sees health improvement as covering a wide range of activity, principally focused on improving the health and wellbeing of individuals and communities (so much like health promotion) (http://www.suffolkcoastal.gov.uk).
The term health gain emerged in policy documents in the late 1980s (for example, Welsh Health Planning Forum 1989). One useful early definition said health gain was a measurable improvement in health status, in an individual or population, attributable to earlier intervention (Nutbeam 1998).
Measurable means that it should be possible to put a value, usually a numerical value, onto health status, in order to demonstrate that a change has occurred.
Attributable means proving that the change in health status is the result of the intervention. This can be difficult. How will you be certain, for example, that a specific programme to reduce smoking has been effective when so many influences can affect smoking habits?
An intervention means a planned activity designed to improve health. It could be treatment, a care service or a health promotion activity.
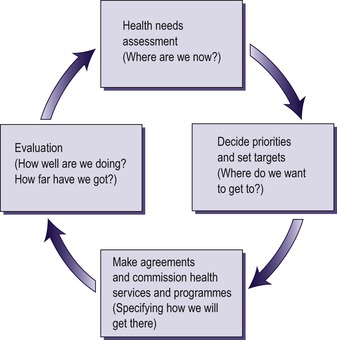
The role of health promoters in assessing health needs, deciding on priorities, setting objectives and targets, allocating resources, and monitoring and reviewing outcomes can be seen as a health gain cycle (Fig. 2.1). Health gain is a useful concept. It focuses attention on health outcomes and on how different choices or priorities can be compared by considering the extent to which they contribute to health gains for individuals or groups.
|
| Fig. 2.1
The health gain cycle.
|
Health Education, Health Promotion and Social Marketing
The WHO (1998) defined health education as the consciously constructed opportunities for learning involving some form of communication designed to improve health literacy, including improving knowledge, and developing life skills which are conducive to individual and community health (see Smith et al 2006 for updates on the WHO glossary of health promotion terms). In the 1970s the range of activities undertaken in the pursuit of better health began to diverge from health education (Scriven 2005). There was also criticism that the health education approach was too narrow, focused too much on individual lifestyle and could become victim-blaming (see Ch. 1, Improving Health – Historical Overview) and increasingly work was being undertaken on wider issues such as political action to change public policies. Such activities went beyond the scope of traditional health education.
Health promotion as a term was used for the first time in the mid 1970s (Lalonde 1974) and quickly became an umbrella term for a wide range of strategies designed to tackle the wider determinants of health. There is no clear, widely adopted consensus of what is meant by health promotion (see Scriven 2005 for a detailed discussion of the development and use of the term). Some definitions focus on activities, others on values and principles. The WHO (1986) definition defines health promotion as a process but implies an aim (enabling people to increase control over, and improve, their health) with a clear philosophical basis of self-empowerment.
Recently in the UK, health-related social marketing has emerged as a prominent health promoting strategy to achieve and sustain behaviour goals on a range of social issues. There are a number of definitions of social marketing, but the description most generally in use is the systematic application of marketing, alongside other concepts and techniques, to achieve specific behavioural goals, for a social good and to improve health and reduce inequalities (French & Blair-Stevens 2005). The exact relationship between social marketing and health promotion is currently being debated, so there is no consensus on whether social marketing comes under the health promotion umbrella of approaches to health gain.
Multidisciplinary Public Health
In the last decade, national and local policy has focused on the development of multidisciplinary public health (see Berridge 2007 for a critique and overview of these developments). Public health work has been defined by Acheson (DoH 1998) as the science and art of preventing disease, prolonging life and promoting health through the organised efforts of society. The Faculty of Public Health (FPH) also uses this definition but offers guidelines specifying that public health:
• Is population based.
• Emphasises collective responsibility for health, its protection and disease prevention.
• Recognises the key role of the state, linked to a concern for the underlying socioeconomic and wider determinants of health, as well as disease.
• Emphasises partnerships with all those who contribute to the health of the population (http://www.fphm.org.uk).
Three spheres of public health have been outlined by Griffiths et al (2005):
Health improvement
• Inequalities
• Education
• Housing
• Employment
• Family/community
• Lifestyles
• Surveillance and monitoring of specific diseases and risk factors.
Improving services
• Clinical effectiveness
• Efficiency
• Service planning
• Audit and evaluation
• Clinical governance
• Equity.
Health protection
• Infectious diseases
• Chemicals and poisons
• Radiation
• Emergency response
• Environmental health hazards.
It is clear from these definitions and explanations that public health requires a wide range of competencies (Evans & Dowling 2002), that it is a multidisciplinary activity involving people from many professions and backgrounds (DoH 2001, Coen & Wills 2007) and that health promotion activities overlap with and are an integral part of the UK public health function (DoH 2005).
Involvement in Public Health
See also Chapter 1, section on national initiatives, for more about this report.
There are three levels of involvement in public health (DoH 2001):
1. Teachers, social workers, voluntary sector staff and health workers all have a role in health improvement. They need to adopt a public health mind set and appreciate how their work can make a difference to health and wellbeing, and where more specialist support can be obtained locally.
2. A smaller number of hands-on public health professionals, such as health visitors and environmental health officers, who spend a major part, or all, of their time in public health practice working with communities and groups.
3. A still smaller group of public health specialists from medical and other professional backgrounds, who work at a senior level with responsibility to manage strategic change and lead public health initiatives. This group includes health promotion specialists and medically qualified public health doctors.
The roles of professionals who contribute to health promotion work are discussed in Chapter 4.
The Scope of Health Promotion
The questions in Exercise 2.1 give examples of the wide range of activities that may be classified as health promotion. Answering ‘yes’ to each one indicates a broad view of what may be included: mass media advertising, campaigning on health issues, patient education, self-help, environmental safety measures, public policy issues, health education, preventive and curative medical procedures, codes of practice on health issues, health-enhancing facilities in local communities, workplace health policies and social education for young people. Answering ‘no’ indicates that you identify criteria that you believe exclude these activities from the realms of health promotion. For example, you may have said ‘no’ to Item 2 because increasing tobacco taxation would place a heavier burden on smokers in poor financial circumstances, thus putting their health even more at risk.
EXERCISE 2.1
Exploring the scope of health promotion
Consider each of the following activities and decide whether you think each is, or is not, health promotion:
| Yes | No | |
|---|---|---|
| 1.Using TV advertisements to encourage people to be more physically active. | □ | □ |
| 2.Campaigning for increased tax on tobacco. | □ | □ |
| 3.Explaining to patients how to carry out their doctor's advice. | □ | □ |
| 4.Setting up a self-help group for people who have been sexually abused as children. | □ | □ |
| 5.Providing schools with a crossing patrol to help children across the road outside schools. | □ | □ |
| 6.Raising awareness of how poverty affects health. | □ | □ |
| 7.Giving people information about the way their bodies work. | □ | □ |
| 8.Immunising children against infectious diseases such as measles. | □ | □ |
| 9.Protesting about a breach in the voluntary code of practice for alcohol advertising. | □ | □ |
| 10.Running low-cost gentle exercise classes for older people at local leisure centres. | □ | □ |
| 11.Providing healthier menu choices at workplace canteens. | □ | □ |
| 12.Teaching a programme of personal and social education in a secondary school. | □ | □ |
| 13.Providing support to people with learning disabilities living in the community. | □ | □ |
| 14. Using social marketing tools to ensure behavioural change in a group of smokers. | □ | □ |
What were your reasons for saying ‘yes’ or ‘no’? Can you identify the criteria you are using for deciding whether an activity is ‘health promotion’?
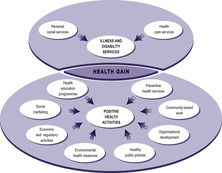
Attempts to provide frameworks and models for classifying activities have helped to clarify the scope of health promotion (see Naidoo & Wills 2000 for an overview). Drawing on these, Fig. 2.2 identifies the activities that contribute to health gain and maps out all those activities which aim to improve people's health. There are two sets of activities, those about providing services for people who are ill or who have disabilities, and positive health activities, which are about personal, social and environmental changes aiming to prevent ill health and develop healthier living conditions and lifestyles. These two sets of activities overlap, because they both contribute to health gain, and they are often closely related in practice. Ten categories of activities are identified, comprising two illness and disability services and eight types of positive health activities.
|
| Fig. 2.2
Activities for health gain.
|
Illness and Disability Services
Personal social services
This includes all those social services aimed at addressing the needs of sick people and people with disabilities or disadvantages whose health (in its widest sense) is improved by those services. This includes, for example, community care of mentally ill people and home help services for the elderly.
Healthcare services
This includes the major work of the health services: treatment, cure and care in primary care and hospital settings.
An important question when considering the boundaries of service provision by health promoters is: ‘If all illness and disability services improve health and produce varying amounts of health gain, are they all called health promotion?’ For example, is taking out someone's appendix or placing a child in a foster home health promotion?
It is helpful to go back to the WHO (1986) definition of health promotion, about enabling people to increase control over and improve their health. Things that need to be done to people (like taking out their appendix or placing them in foster homes) are excluded from this definition, so are generally not considered to be health promotion activities (although they are health gain activities). But those aspects of care and treatment that are about enabling people to take control over their health and improve it (such as educating patients in the skills of self-care, or educating foster parents in the skills of parenting) are legitimate areas of health promotion. So is creating a health promoting environment by, for example, modifying a home to make it suitable for a person with disabilities or providing affordable housing for homeless people with health problems.
Positive Health Activities
Health education programmes
These are planned opportunities for people to learn about health, and to undertake voluntary changes in their behaviour. Such programmes may include providing information, exploring values and attitudes, making health decisions and acquiring skills to enable behaviour change to take place. They involve developing self-esteem and self-empowerment so that people are enabled to take action about their health. This can happen on a personal one-to-one level such as health visitor/client, teacher/pupil, or in a group such as a smoking cessation group or exercise class, or reach large population groups through the mass media, health fairs or exhibitions.
See Chapter 10, Chapter 11, Chapter 12, Chapter 13 and Chapter 14 for detailed information on carrying out these health promotion activities.
Health education programmes may also be a part of healthcare and personal social services, and because of this it is useful to understand the concepts of primary, secondary and tertiary health education.
Primary health education
This would reflect McKinley's (1979) vision of upstream, preventative activity. It is directed at healthy people, and aims to prevent ill health arising. Most health education for children and young people falls into this category, dealing with such topics as sexual health, nutrition and social skills and personal relationships, and aiming to build up a positive sense of self-worth in children. Primary health education is concerned not merely with helping to prevent illness but with positive wellbeing.
Secondary health education
There is also often a major role for health education when people are ill. It may be possible to prevent ill health moving to a chronic or irreversible stage, and to restore people to their former state of health. This is known as secondary health education, educating patients about their condition and what to do about it. Restoring good health may involve the patient in changing behaviour (such as stopping smoking) or in complying with a therapeutic regime and, possibly, learning about self-care and self-help. Clearly, health education of the patient is of great importance if treatment and therapy are to be effective and illness is not to recur.
Tertiary health education
There are, of course, many patients whose ill health has not been, or could not be, prevented and who cannot be completely cured. There are also people with permanent disabilities. Tertiary health education is concerned with educating patients and their carers about how to make the most of the remaining potential for healthy living, and how to avoid unnecessary hardships, restrictions and complications. Rehabilitation programmes contain a considerable amount of tertiary health education with a focus on improving quality of life.
Quantenary health education
This concentrates on facilitating optimal states of empowerment and emotional, social and physical wellbeing during a terminal stage (see Hancock 2001, Scriven 2005).
It is not always easy to see where people fit into this primary, secondary or tertiary framework because a person's state of health is open to interpretation. For example, is educating an overweight person who appears to be perfectly well, despite being overweight, primary or secondary health education?
Social marketing
The National Social Marketing Centre (NSMC) identifies the primary aim of health-related social marketing as the achievement of a social good (rather than commercial benefit) in terms of specific, achievable and manageable behaviour goals, relevant to improving health and reducing health inequalities. Social marketing is a systematic process using a range of marketing techniques and approaches (a marketing mix) phased to address short-, medium- and long-term issues. The following six features and concepts are pertinent to understanding social marketing:
Customer or consumer orientation
A strong customer orientation with importance attached to understanding where the customer is starting from, their knowledge, attitudes and beliefs, along with the social context in which they live and work.
Behaviour and behavioural goals
Clear focus on understanding existing behaviour and key influences upon it, alongside developing clear behavioural goals. These can be divided into actionable and measurable steps or stages, phased over time.
Intervention mix and marketing mix
Using a mix of different interventions or methods to achieve a particular behavioural goal. When used at the strategic level this is commonly referred to as the intervention mix, and when used operationally it is described as the marketing mix.
Audience segmentation
Clarity of audience focus using audience segmentation to target effectively.
Exchange
Use of the exchange concept, understanding what is being expected of people, and the real cost to them.
Competition
This means understanding factors that impact on people and that compete for their attention and time (adjusted from http://www.nsmcentre.org.uk).
Social marketing uses the total process planning model summarised in Fig. 2.3. The front end scoping stage drives the whole process. The primary concern is establishing clear actionable and measurable behaviour goals to ensure focused development across the rest of the process. The ultimate effectiveness and success of social marketing rests on whether it is possible to demonstrate direct impact on behaviour. It is this feature that sets it apart from other communication or awareness raising approaches, such as health education, where the main focus is on imparting information and enabling people to understand and use it. The information on social marketing above has been adjusted from the NSMC website (http://www.nsmcentre.org.uk). For more details on how to engage in health-related social marketing, see Macdowall et al (2006) and NSMC (2007). To explore the effectiveness of social marketing as an approach, see McDermott et al (2005) and Stead et al (2007) and to examine in more detail the links between social marketing and health promotion, see NSMC (2008).

|
| Fig. 2.3
Social marketing uses a total process planning model.
(NSMC and Consumer Focus 2007. Reproduced with permission).
|
Preventive health services
These include medical services that aim to prevent ill health, such as immunisation, family planning and personal health checks, as well as wider preventive health services such as child protection services for children at risk of abuse.
Community-based work
This is a bottom-up approach to health promotion, working with and for people, involving communities in health work such as local campaigns for better facilities. It includes community development, which is essentially about communities identifying their own health needs and taking action to address them. The sort of activities that may result could include forming self-help and pressure groups, and developing local health-enhancing facilities and services.
See Chapter 15, Working with communities.
Organisational development
This is about developing and implementing policies within organisations to promote the health of staff and customers. Examples include implementing policies on equal opportunities, providing healthy food choices at places of work and working with commercial organisations to develop and promote healthier products.
See Chapter 16, Influencing and implementing policy.
Healthy public policies
Developing and implementing healthy public policies involves statutory and voluntary agencies, professionals and the public working together to develop changes in the conditions of living. It is about seeing the implications for health in policies about, for example, equal opportunities, housing, employment, transport and leisure. Good public transport, for example, would improve health by reducing the number of cars on the road, decreasing pollution, using less fuel and reducing the stress of the daily grind of travelling for commuters. It could also reduce isolation for those who do not own cars and enable people to have access to shopping and leisure facilities, all measures that improve wellbeing (See Scriven 2007 for a detailed overview of healthy public policies).
See Chapter 16, Influencing and implementing policy.
Environmental health measures
Environmental health is about making the physical environment conducive to health, whether at home, at work or in public places. It includes public health measures such as ensuring clean food and water and controlling traffic and other pollution.
Economic and regulatory activities
These are political and educational activities directed at politicians, policy makers and planners, involving lobbying for and implementing legislative changes such as food labelling regulations, pressing for voluntary codes of practice such as those relating to alcohol advertising or advocating financial measures such as increases in tobacco taxation.
A Framework for Health Promotion Activities
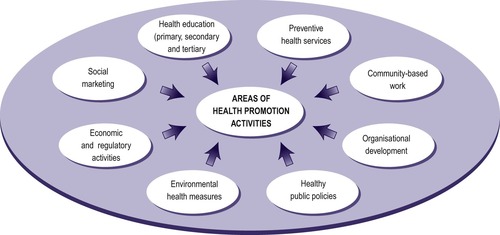
There are two important points to make about the use of the framework of health promotion activities in Fig. 2.4. The first is that activities do not always fall neatly into categories. For example, would a health visitor who was supporting a local women's health group be engaged in a health education programme because they provided health information to the group and set up stress management sessions, or in community-based work because some members of the group had got together to lobby their local health services for better sexual health advice clinics for young people?
|
| Fig. 2.4
A framework for health promotion activities.
|
Obviously areas of activity overlap, but this is not important. What is important is to appreciate the range of activities encompassed by health promotion, and the many ways in which you can contribute to health improvements.
The second point about using this framework is to note that it reflects planned, deliberate activities, and it is important to recognise that a great deal of health promotion happens informally and incidentally. For example, portrayal of damage caused by excessive drinking on television soaps and an advertising campaign to promote wholewheat breakfast cereals are all health promotion activities which are not likely to be planned with specific health promotion aims in mind. They may, however, be significant influences for change.
See Chapter 11, section on mass media.
Exercise 2.2 is designed to help you to identify your own contribution to health promotion.
EXERCISE 2.2
Identifying your health promotion work
Look at Fig. 2.4 again, which identifies eight major areas of health promotion activity. By each of the eight headings, note down any parts of your work you think come into that category. If you are not sure what each category includes, look back at the explanations. Then think about each category again, and consider whether there is scope for developing your work within each category.
Broad Areas of Competencies Important to Health Promotion Practice
In order to engage in the activities outlined in the framework in Fig. 2.4, health promoters require a range of competencies. There are two aspects of work to consider. One is the technical/specialist aspect such as immunising a child, taking a cervical smear test, recording blood pressure or undertaking microbiological tests for food hygiene purposes. All of these are the subject of specialist training, and outside the scope of this book.
The other aspect of your work is about working with people to promote health in many different situations with a variety of different aims. To do this, health promoters need to have knowledge of particular methods and acquire specialist competencies in the following areas:
Managing, planning and evaluating
All these are addressed in Part 2: Planning and managing for effective practice, Chapter 5, Chapter 6, Chapter 7, Chapter 8 and Chapter 9.
Managing resources for health promotion, including money, materials, oneself and other people, is crucial. Systematic planning is needed for effective and efficient health promotion. All health promotion work also requires evaluation, and different methods are appropriate for different approaches.
Communicating and educating
Communication and educating are addressed in Chapter 8, Chapter 9, Chapter 10, Chapter 11, Chapter 12, Chapter 13 and Chapter 14.
Health promotion is about people, so competence in communication is essential and fundamental. A high level of competence is needed in one-to-one communication and in working with groups in various ways, both formal and informal.
Effective communication is an educational competence, but health promoters also need to understand how people receive information and learn. For example, patient education requires communication and educational competencies.
Marketing and publicising
Marketing and publicising are addressed in Chapter 11.
This requires competence in, for example, marketing and advertising, using local radio and getting local press coverage of health issues. It may be used when undertaking any health promotion activities that would benefit from wider publicity.
Facilitating, networking, partnership working
This means enabling others to promote their own and other people's health, using various means such as sharing skills and information and building up confidence and trust. These competencies are particularly important when working with communities. They are also vital for working with other agencies and forming partnerships for health that cross barriers of organisations and disciplines.
Influencing policy and practice
Health promoters are in the business of influencing policies and practices that affect health. These can be at any level, from national (such as policies set by government or political parties about, for example, housing, transport and future directions for the NHS) to the level of day-to-day work of a health promoter (such as what sort of health promotion programmes will be run in a GP practice, or what resources will be devoted to specific health promotion activities in an environmental health department).
Influencing policy and practice is addressed in Chapter 16.
In order to influence policy and practice, you need to understand how power is distributed and exercised between people at any level, from a group of colleagues to those in positions of great authority or influence. You need to be able to use that knowledge to affect decisions. This includes working with statutory, voluntary and commercial organisations to influence them to develop health promoting policies for their staff and to produce health enhancing products and services. It also includes working for healthy public policies and economic and regulatory changes requiring lobbying and taking political action.
It is unrealistic to expect all health promoters to be highly competent in all aspects of health promotion. Practice nurses, for example, will work predominantly in health education and preventive health services, needing a high level of competence in communication and education. However, they also needs other competencies in order to plan and evaluate their work, market health promotion programmes to their patients, facilitate change in their patients and be able to refer them to a network of helpful contacts. They will also need to be able to influence the development of health promotion policy in their practice.
Occupational Standards in Health Promotion
At the time of writing there are a number of different initiatives taking place in the UK and in Europe that will result in a much clearer set of core competencies for health promotion. Currently in the UK competencies set out in the form of occupational standards are available for specialists and practitioners in public health (Skills for Health 2007). There is currently no agreed route through these standards for health promotion specialists or practitioners.
At an international level, the Galway Consensus Statement (http://www.sophe.org; see also Morales et al 2009) sets out eight domains of core competency in health promotion. They are: catalysing change, leadership, assessment, planning, implementation, evaluation, advocacy and partnerships. At the time of writing there is broad consultation on the consensus statement, so it will be interesting to monitor the development of both UK and international health promotion competency statements over the coming years.
The standards developed for specialist practice in public health set out in Box 2.1 are applicable (at least in part) to health promotion. It is useful to examine these standards and to think about the areas of health promotion work you are involved in and which standards are important for your work. It is also important to recognise the areas you do not use in your work and to think about the implications for working collaboratively with other professionals. Exercise 2.3 is designed to encourage you to think about your health promotion work and how it contributes to the wider public health function. It will also help you to think about the differences between health promotion and public health.
BOX 2.1
Overview of the national standards for public health (Skills for Health 2007)
Area 1: Surveillance and assessment of the population's health and wellbeing – see Chapter 6
1. Collect and form data and information about health and wellbeing and/or stressors to health and wellbeing.
2. Obtain and link data and information about health and wellbeing and/or stressors to health and wellbeing.
3. Analyse and interpret data and information about health and wellbeing and/or stressors to health and wellbeing.
4. Communicate and disseminate data and information about health and wellbeing and/or stressors to health and wellbeing.
5. Facilitate others’ collection, analysis, interpretation, communication and use of data and information about health and wellbeing and/or stressors to health and wellbeing.
6. Collect, structure and analyse data on the health and wellbeing and related needs for a defined population.
7. Undertake surveillance and assessment of the population's health and wellbeing.
Area 2: Promoting and protecting the population's health and wellbeing – see Chapter 5, Chapter 6, Chapter 7 and Chapter 16
1. Communicate with individuals, groups and communities about promoting their health and wellbeing.
2. Encourage behavioural change in people and agencies to promote health and wellbeing.
3. Work in partnership with others to promote health and wellbeing and reduce risks within settings.
4. Work in partnership with others to prevent the onset of adverse effects on health and wellbeing in populations.
5. Work in partnership with others to contact, assess and support individuals in populations who are at risk from identified hazards to health and wellbeing.
6. Work in partnership with others to protect the public's health and wellbeing from specific risks.
7. Promote and protect the population's health and wellbeing.
Area 3: Developing quality and risk management within an evaluative culture – see Chapter 7
1. Develop one's own knowledge and practice.
2. Contribute to the development of the knowledge and practice of others.
3. Support and challenge workers on specific aspects of their practice.
4. Manage the performance of teams and individuals.
5. Contribute to improvements at work.
6. Develop quality and risk management within an evaluative culture.
Area 4: Collaborative working for health and wellbeing – see Chapter 4, Chapter 9, Chapter 10, Chapter 11, Chapter 12, Chapter 13 and Chapter 14
1. Build relationships within and with communities and organisations.
2. Develop, sustain and evaluate collaborative work with others.
3. Represent one's own agency at other agencies’ meetings.
4. Work in partnership with communities to improve their health and wellbeing.
5. Enable the views of groups and communities to be heard through advocating on their behalf.
6. Provide information and advice to the media about health and wellbeing and related issues.
7. Improve health and wellbeing through working collaboratively.
Area 5: Developing health programmes and services and reducing inequalities – see Chapter 5, Chapter 6, Chapter 7 and Chapter 8
1. Work in partnership with others to plan, implement and review programmes and projects to improve health and wellbeing.
2. Manage change in organisational activities.
3. Develop people's skills and roles within community groups/networks.
4. Assess, negotiate and secure sources of funding.
5. Develop health programmes and services and reduce inequalities.
Area 6: Policy and strategy development and implementation to improve health and wellbeing – see Chapter 16
1. Work in partnership with others to plan, implement, monitor and review strategies to improve health and wellbeing.
2. Work in partnership with others to assess the impact of policies and strategies on health and wellbeing.
3. Work in partnership with others to develop policies to improve health and wellbeing.
4. Appraise policies and recommend changes to improve health and wellbeing.
5. Improve health and wellbeing through policy and strategy development and implementation.
Area 7: Working with and for communities to improve health and wellbeing – see Chapter 15
1. Facilitate the development of people and learning in communities.
2. Create opportunities for learning from practice and experience.
3. Support communities to plan and take collective action.
4. Facilitate the development of community groups/networks.
5. Enable people to address issues related to health and wellbeing.
6. Enable people to improve others’ health and wellbeing.
7. Work with individuals and others to minimise the effects of specific health conditions.
8. Improve health and wellbeing through working with and for communities.
Area 8: Strategic leadership for health and wellbeing – see Chapters 8 and 13
1. Use leadership skills to improve health and wellbeing.
2. Promote the value of, and need for, health and wellbeing.
3. Lead the work of teams and individuals to achieve objectives.
4. Design learning programmes.
5. Enable learning through presentations.
6. Evaluate and improve learning and development programmes.
7. Strategically lead the improvement of health and wellbeing and the reduction of inequalities.
Area 9: Research and development to improve health and wellbeing – see Chapter 7
1. Plan, undertake, evaluate and disseminate research and development about improving health and wellbeing.
2. Develop and maintain a strategic overview of developments in knowledge and practice.
3. Develop, implement and evaluate strategies to advance knowledge and practice.
4. Commission, monitor and evaluate projects to advance knowledge and practice.
5. Contribute to the evaluation and implementation of research and development outcomes.
6. Improve health and wellbeing through research and development.
Area 10: Ethically managing self, people and resources to improve health and wellbeing – see Chapter 3, Chapter 5, Chapter 6, Chapter 7, Chapter 8 and Chapter 9
1. Promote people's equality, diversity and rights.
2. Prioritise and manage own work and the focus of activities.
3. Manage the use of financial resources.
4. Monitor and review progress with learners.
5. Facilitate individual learning and development through mentoring.
6. Enable individual learning through coaching.
7. Ethically manage self, people and resources to improve health and wellbeing.
EXERCISE 2.3
Mapping your health promotion work against the standards for specialist practice in public health
Study the areas identified as specialist public health practice and tick the level of activity you are involved in. Look at Box 2.1 for details of the work covered by each area of activity.
Note the areas you work in and the areas that are outside your current job responsibilities or which you are not trained to do.
Compare this mapping with that of colleagues or other health workers.
| Area of public health practice | Very high level of activity | High level of activity | Fair level of activity | Some level of activity | No activity in this area |
|---|---|---|---|---|---|
| Area 1: Surveillance and assessment of the population's health and wellbeing. | □ | □ | □ | □ | □ |
| Area 2: Promoting and protecting the population's health and wellbeing. | □ | □ | □ | □ | □ |
| Area 3: Developing quality and risk management within an evaluative culture. | □ | □ | □ | □ | □ |
| Area 4: Collaborative working for health and wellbeing. | □ | □ | □ | □ | □ |
| Area 5: Developing health programmes and services and reducing inequalities. | □ | □ | □ | □ | □ |
| Area 6: Policy and strategy development and implementation to improve health and wellbeing. | □ | □ | □ | □ | □ |
| Area 7: Working with and for communities to improve heath and wellbeing. | □ | □ | □ | □ | □ |
| Area 8: Strategic leadership for health. | □ | □ | □ | □ | □ |
| Area 9: Research and development. | □ | □ | □ | □ | □ |
| Area 10: Ethically managing self, people and resources. | □ | □ | □ | □ | □ |
Standards taken from Skills for Health (2007)
Using the National Occupational Standards
Broadly speaking there are three uses for the national occupational standards:
1. Employers and managers can use the standards to improve the quality of the performance of their staff. An organisation can map what it is trying to achieve against the areas and sub-areas of practice. It can then look at its service specifications and its management of human resources through job specifications, staff appraisal and performance review. The standards could also be used as the basis for auditing a service and checking whether it meets quality standards.
Audit is discussed in more detail in Chapter 7.
2. Individuals can use the standards to improve their competence through identifying their key areas of work, assessing their own performance, identifying their learning needs and defining the learning outcomes needed to meet the national standards.
3. Education and training providers can use the standards to modify their programmes to enable practitioners to develop appropriate competencies, or use the standards as the basis of their programme design.
PRACTICE POINTS
▪ Health promotion practice encompasses a wide range of approaches that are united by the same goal, to enable people to increase control over and improve their health.
▪ It is important for you to identify the full scope of your health promotion work and to see how this fits with the work of your organisation or employer and the wider remit of public health.
▪ The national standards for specialist practice in public health provide a map which can be used by organisations, managers, education and training providers, and individuals to improve the quality of public health and health promotion work.
References
Abbott, S, The meaning of health improvement,
Health Education Journal
61
(4) (2002) 299–308
.
Berridge, V, Multidisciplinary public health: what sort of victory?
Public Health
121
(6) (2007) 404–408
.
Coen, C; Wills, J, Specialist health promotion as a career choice in public health,
The Journal of the Royal Society for the Promotion of Health
127
(5) (2007) 231–238
.
Department of Health,
Independent inquiry into inequalities in health
. (1998) The The Stationery Office, London
.
Department of Health,
Chief Medical Officer's report to strengthen the public health function of England
. (2001) The The Stationery Office, London
.
Department of Health,
Shaping the future of public health: Promoting health in the NHS
. (2005) The Stationery Office, London
.
Evans, D; Dowling, S, Developing a multi-disciplinary public health specialist workforce: training implications of current UK policy,
Journal of Epidemiology and Community Health
56
(2002) 744–747
.
French, J; Blair Stevens, C,
Social marketing pocket guide
. (2005) National Social Marketing Centre for Excellence, London
;
http://www.nsms.org.uk
.
Griffiths, S; Jewell, T; Donnelly, P, Public health in practice: the three domains of public health,
Public Health
119
(2005) 907–913
.
Hancock T 2001 Healthy people in healthy communities in a healthy world: the science, art and politics of public health in the 21st century. Paper presented at the launch of the OU School of Health and Social Welfare Health Promotion and Public Health Research Group, 12 September. Milton Keynes, The Open University.
Lalonde, M,
A new perspective on the health of Canadians
. (1974) Information Canada, Ottawa
.
Macdowall, W; Bonell, C; Davies, M, Social marketing, In: (Editors: Macdowall, W; Bonell, C; Davies, M)
Health promotion practice
(2006) Open University Press, Maidenhead
.
McDermott, L; Stead, M; Hastings, GB;
et al.
,
A systematic review of the effectiveness of social marketing nutrition and food safety interventions – final report prepared for Safefood. Stirling
. (2005) Institute for Social Marketing, University of Stirling
.
McKinley, JB, A case for refocusing upstream: the political economy of health, In: (Editor: Javco, EG)
Patients, physicians and illness
(1979) Macmillan, Basingstoke
.
Morales, AS-M; Battel-Kirk, B; Barry, MM;
et al.
, Perspectives on health promotion competencies and accreditation in Europe,
Global Health Promotion
16
(2) (2009) 21–30
.
Naidoo, J; Wills, J, Models and approaches to health promotion, In: (Editors: Naidoo, J; Wills, J)
Public health and health promotion practice: foundations for health promotion
3rd edn (2000) Elsevier, London
.
National Social Marketing Centre,
Big pocket guide: social marketing
. (2007) NSMC, London
.
National Social Marketing Centre,
Social marketing for health and specialised health promotion: stronger together – weaker apart
. (2008) NSMC, London
.
Nutbeam, D, Health promotion glossary,
Health Promotion International
13
(4) (1998) 349–364
.
Scriven, A, Promoting health: policies, principles and perspectives, In: (Editor: Scriven, A)
Health promoting practice: the contribution of nurses and allied health professions
(2005) Palgrave, Basingstoke
.
Scriven, A, Healthy public policies: rhetoric or reality, In: (Editors: Scriven, A; Garman, G)
2007 Public health: social context and action
(2007) Open University Press, Maidenhead
.
Skills for Health, Public health national occupational standards – practice and specialist,
http://www.skillsforhealth.org.uk/competences/~/media/Resource-Library/Word/PHstdstracking6.ashx (2007)
.
Smith, BJ; Cho Tang, K; Nutbeam, D, WHO health promotion glossary: new terms,
Health Promotion International
21
(4) (2006) 340–345
.
Stead, M; Hastings, G; McDermott, L, The meaning, effectiveness and future of social marketing,
Obesity Reviews
8
(1) (2007) 189–193
.
Welsh Health Planning Forum,
Strategic intent and direction for the NHS in Wales
. (1989) Welsh Office, Cardiff
.
World Health Organization,
The Ottawa charter for health promotion
. (1986) WHO, Geneva
;
http://www.who.int/hpr/NPH/docs/ottawa_charter_hp.pdf
.
World Health Organization,
The Jakarta declaration on health promotion in the 21st century
. (1997) WHO, Geneva
.
World Health Organization,
List of basic terms. Health promotion glossary
. (1998) WHO, Geneva
.