3 Preparation for placement learning
Introduction
You are now aware of what a medical ward is and how it works but what can you do in preparation for your medical ward placement? This chapter aims to give you some tips and preparation activities to ensure that you start your medical ward placement feeling confident and ready to learn. Remember that your practice learning opportunities make up 50% of your nurse training programme and you need to recognise the importance and value of this learning opportunity. You are an adult learner and there will be an expectation that you take personal responsibility for directing your own learning and making the best use of the learning opportunities available. You may worry that the medical ward may not be the right place for you to achieve the learning outcomes, however let us reassure you – care is always taken to place students in wards that allow them to meet their learning outcomes and placements are linked very closely to your curriculum.
Student reflection
The first day I started practice I had not much confidence at all. I thought ‘how can I do this and help a patient?’ I put myself in the mindset of a role as a nurse and this mindset helped me a lot throughout my time on practice, but I also talked to my mentor about my concerns and worries and they gave me some guidance and then, in time, my confidence grew and I was able to perform to the best of my abilities.
During your practice placement, your learning outcomes will be assessed by a registered nurse who is a qualified mentor who has undertaken a specific course that is recognised by the Nursing and Midwifery Council (NMC). Sometimes a team of mentors will support you and this may also include co-mentors or associate mentors who have not undertaken the recognised mentor course but are expected to contribute to your learning.
There are a number of aspects that you should consider when preparing for your placement:
Practicalities
First of all, when you find out the name of the ward and the location, the Website at your university will probably have placement profile information. This may contain information about the ward, who to contact, phone numbers, shift times and general advice. Do they advise any special preparation activities? It is important to contact the ward at least 2 weeks before your placement to ensure that you know when to start and, even better, if you can arrange to visit the ward before you start (Sharples 2009).
Once you find out the shift times, you need to think about the practicalities of getting to your placement on weekdays and weekends and for the inevitable early starts and late finishes. For example, what are the transport links like and is there parking available for students? You may care for someone at home such as a relative or a child and need to make arrangements for this while you are on placement. It is important to clarify what the expectations of you are regarding attendance in placement and you will find this information in your student handbook. In some universities you will be expected to work the shifts that the ward staff works, and in other placements this might be more flexible.
If you are a more senior student, you may need to work some night shifts or weekends to cover the expectations of your professional body for registration. Ward managers will need to know if you have any special off duty requests so that they can ensure you are allocated to an appropriate mentor who can work with you for the required amount of time to facilitate learning and assessment in practice. Even though you are supernumerary, nursing is fundamentally a practical job and you can only learn with hands-on practice and will need to be there for patient handover to ensure you are fully informed of the patient caseloads.
The university will probably have an identified lecturer who will link with your ward and it is important that you know how to contact this person and the times and dates that they visit the ward. It is also important to consider whether you have any learning needs that require discussion prior to your placement to enable the ward staff to support you appropriately. You will need to find out if there is a planned induction or welcome meeting that you need to attend and if there is a student notice board somewhere locally or centrally within the hospital. The ward will want to keep you safe while you are in your placement and you need to inform them of any adjustments or risk assessments that need to be carried out. For example, if you are pregnant you will be able to achieve your learning outcomes but will need a risk assessment outlining any adjustments required.
If this is your first placement, this is a good time to look through your learning outcomes and consider what your priorities might be and if you have any transferable skills that you can bring to the placement. If this is not your first placement, you should look at the feedback you received from your mentors in your last placement, focusing on areas of strength and areas for development, and consider what your learning objectives are for this ward.
Student reflection
My first placement was an experience that I will never forget, but before my first day of placement I prepared myself by watching the clinical skills DVD, reading the clinical skills book, reading the biology and anatomy books and also reading the lecture notes from previous lectures.
Log on to your university Website and find out about your placement. Consider the practicalities involved using the questions in Box 3.1.
Box 3.1 What are the practicalities of this placement?
Look up the ward profile on the student Website:
1. Is there any information about your learning outcomes for this placement on the student Website?
2. Who can be your mentor? If you are a final placement student you will need a sign off mentor (NMC 2008b).
3. What shifts does the ward work?
4. What shifts do you need to work to meet the university's expectations.
5. Do you have any special off duty requests?
6. How do you get to the placement – what are the transport links like?
7. Is there a lecturer from the university who links with the placement?
8. Is there an induction planned?
9. Do you have any learning needs that require discussion with the placement before you arrive?
10. What were the strengths and areas for development highlighted in your previous placement?
11. Do you have transferable skills?
12. What do you want to achieve in this placement?
13. What is the uniform policy?
14. Who do you inform at the university if you are sick or absent from placement?
15. Do you need to make arrangements to see your personal tutor while you are on placement?
16. Are there any university lectures, exams or assignments that you need to plan into your time?
17. Have you attended all the mandatory training at the university prior to your placement?
18. Are you pregnant? If so, have your read the university maternity policy and understand that you will require a risk assessment?
Professional standards and behaviour
As a student nurse you will not only be expected to develop clinical skills but also a certain level of professional attitude and behaviour (Parker 2009). These attributes will be assessed as part of your course and your mentors in the clinical environment will play a key part in your assessment in this area.
A Website worth looking at is:
NMC Guidance (NMC 2009): http://www.nmc-uk.org/Documents/Guidance/NMC-Guidance-on-professional-conduct-for-nursing-and-midwifery-students.pdf (accessed July 2011).
It is expected that, as a student nurse, you will act in a professional manner at all times. This means not just within the clinical area but in public places as well. It is essential that people feel they can trust nurses, and any behaviour which may damage the respect and credibility of the profession in the eyes of the general public could be detrimental to how safe patients feel when they are admitted to hospital (Levett-Jones & Bourgeois 2009). This may sound daunting but there is plenty of guidance and support available to help you. This chapter aims to help you understand what is expected of you and how to use the support of your mentors in the clinical area to help you develop your professional behaviour.
Good health, good character and fitness to practise
The NMC sets out what they expect from student nurses in their Guidance on Professional Conduct for Nursing and Midwifery Students (NMC 2009). At the end of your nursing course your university is required to inform the NMC that you have not only met the educational and clinical requirements of your course but also that you are in good health and are of good character. It is essential that you read this and adhere to it, and discuss it with your mentor at the start of your placement learning experience.
What does good health mean? It means that you are capable of safe and effective practice without supervision. It does not mean the absence of any disability or health condition.
What does good character mean? It is based on your conduct, behaviour and attitude. It takes account of any convictions and cautions you may have that may bring the profession into disrepute.
Both of these elements are required for you to be deemed fit to practise and join the nursing register.
1. What do members of the public think when they see a nurse in uniform smoking a cigarette in a public place?
2. What do they think about a nurse doing their shopping in the local supermarket in their uniform?
3. What do they think when they overhear nurses giggling and laughing about their patients?
The areas of concern highlighted in Box 3.2 are also cited by the NMC as aspects of your personal life that may influence your ability to be judged as having good health and good character.
Box 3.2 Aspects of your personal life that may influence your ability to be judged as having good health and character
 Aggressive, violent or threatening behaviour.
Aggressive, violent or threatening behaviour.
 Criminal conviction or caution.
Criminal conviction or caution.
 Dishonesty, e.g. misrepresentation of qualifications, fraudulent CV.
Dishonesty, e.g. misrepresentation of qualifications, fraudulent CV.
 Health concerns, e.g. putting others at risk by not seeking help for medical problems or not recognising own limitations.
Health concerns, e.g. putting others at risk by not seeking help for medical problems or not recognising own limitations.
Now that you have read about behaviour that is not acceptable for a nurse to display, list the positive attributes and behaviours you would expect to see in a nurse and consider how you can ensure that these are displayed in your personal and professional life.
The NMC Code (2008a) in the UK is a set of strict standards that registered nurses must adhere to. The sooner you become familiar with these, the easier it will be to ensure that your practice and behaviour are meeting the standards required for registration. Other countries will have similar guidance and standards, so ensure you are familiar with the requirements of the country you are registering in.
Accountability
Accountability is a word you may hear your mentor and other registered nurses use. It is integral to nursing practice and, although the level of accountability expected of you as a student differs from that which will be expected of you as a registered nurse, it is important that you understand what it means to you and to your practice.
Accountability can be described as (Thompson et al 2006, p. 84):
The ability to give account of one's actions, in particular to give a coherent, rational and ethical justification for what one has done.
Registered nurses are accountable in four ways:
Professional accountability
The NMC Code (2008a) states that:
As a professional, you are personally accountable for actions and omissions in your practice and must always be able to justify your decisions.
Your mentors are accountable for passing or failing you – they need to be able to justify their decisions. At the heart of their decision will be patient safety. Patients have expectations of nurses – that we are registered, educated to a certain level, keep up to date and that we will not harm them. Patients do not expect us to know everything but they expect us to acknowledge when we cannot do something competently and to seek assistance and advice if we are ever unsure.
In our daily lives we have expectations of other registered practitioners. For example, if a gas fire is not working we would only employ someone who is a registered up-to-date gas fitter to come and fix it, as anyone else could harm us and our families.
So what should patients expect from a registered nurse? This is a good starting point:
• To know who is looking after them each shift.
• To know when the shift changes.
• To know what's happening to them and when.
• That care is evidence-based.
• That nurses work to policies/guidelines.
• That nurses are not afraid to challenge poor practice.
• That nurses work in a team for their benefit.
• That nurses monitor the standards of care ensuring quality, safety and efficiency.
The roles and responsibilities of those who can support you doing your medical practice placement
The mentor
During your practice placement, your learning outcomes will be assessed by a registered nurse who is a qualified mentor who has undertaken a specific course that is recognised by the NMC (NMC 2008b). The mentor who assesses you must be registered within the same field of practice as you and have attended a mentor update within the last year. The placement holds registers of mentors and their updates and is expected to be able to produce this evidence for the NMC. Each mentor also has a triennial review to ensure that they are meeting the NMC Standards and a record of this is kept by each placement. Your curriculum documentation will often have a section that requires the mentor to print and sign their name, year of registered mentor course and the last update they attended to ensure the validity of your assessments.
You are expected to work with your mentor for 40% of your placement time and this must be evident through the duty roster (NMC 2008b, 2011). Your mentor may work weekends, nights, 7.5-hour or 12.5-hour shifts and your allocated duties should follow this. Mentors will also have annual leave and study days themselves, so sometimes this will be difficult to achieve and you may be allocated more than one mentor. Sometimes a team of mentors will support you and this may also include co-mentors or associate mentors who have not undertaken the recognised mentor course but are expected to contribute to your learning (NMC 2008a). Associate or co-mentors are registered nurses who you will often work with and learn from, and they will often provide feedback on your performance to your main mentor. They may do this verbally or by writing in your record of achievement, for example in a mentor comment page. However, they will not be able to assess you until they have undertaken the recognised mentor course.
The sign-off mentor
The role of the sign-off mentor is to ‘sign off’ that a student has met all of the NMC Standards and Competencies at the end of their NMC pre-registration nurse programme for entry to the register. The sign-off mentor has completed the NMC mentor course but has been further assessed against the NMC Standards for Learning and Assessment in Practice (NMC 2008b) and has met the criteria to be a sign-off mentor. The sign-off mentor in your final placement will assess and supervise your learning but will also be making judgements based on decisions of other mentors who have supervised you earlier in your final year. It is important that you make sure that there is sufficient evidence from other mentors to allow your sign-off mentor to be satisfied that you have been assessed sufficiently within your recent placements. The sign-off mentor will only sign you off as proficient if they are satisfied that you are fit to practise and for purpose and safe to practise as they hold that responsibility and accountability. The NMC (2010) emphasises the requirement for a record of achievement for each student which documents comments from mentors and is passed from one placement to another. This record of achievement is shared with academic staff, and if there are any concerns in practice, there is an expectation that the placement mentors and academic staff from the university will work in partnership to address these.
A useful resource for mentoring and mentors is:
http://www.rcn.org.uk/__data/assets/pdf_file/0008/78677/002797.pdf (accessed July 2011).
The practice experience/education facilitator or practice experience manager
At the end of the 1990s the role of the practice experience/education facilitator or practice experience manager was developed to support the increasing numbers of students in practice (Department of Health 1999, United Kingdom Central Council for Nursing, Midwifery and Health Visiting (UKCC; now the NMC) 1999). These roles have many titles within organisations, but for the purposes of this chapter will be called the practice education facilitator. The role of the practice education facilitator is to provide a quality learning environment for students which involves supporting them in their practice placements and preparing and facilitating mentors to assess the students. The practice education facilitator also links with the university and will spend time meeting with programme leaders, personal tutors, placement units and link lecturers to ensure that the quality of learning is sustained.
The practice education facilitator will often provide inductions, evaluations, workshops, organise teaching for you and your mentors and, in partnership with the university, undertake educational audits of the environments within which you are placed to ensure and enhance the quality of placement learning (Lauder et al 2008).
A Website you might like to visit:
Nursing and midwifery in Scotland: being fit for practice. The report of the Evaluation of Fitness For Practice Pre-Registration Nursing and Midwifery Curricula Project 2008: http://www.nes.scot.nhs.uk/media/6962/ffpfinalreportsept082.pdf (accessed July 2011).
The link lecturer
The role of the link lecturer is to ensure that there are strong links between the university and the placement and to support students and mentors in these areas. For the majority of their role, a link lecturer will continue to teach and have responsibilities at the university, however one aspect of their job will be to link with a number of areas within organisations. Link lecturers will often work closely with the practice education facilitator to support students and mentors within their placements. Some organisations have lecturer/practitioner roles which are 50:50 practice/lecturer roles employed by the NHS 50% of the time and the university 50% of the time.
The personal tutor
When you join university you will be given a personal tutor normally for the duration of your training who will play a key role in supporting your progression throughout. They keep all of your records for your training and will monitor your progress and attendance throughout the course. They will book appointments to see you regularly throughout your programme, and you should contact them if you have any issues or worries as they have a key role in providing pastoral support for you and will be the person that can refer you to other agencies if you need help. Universities normally have an outline of the role of the personal tutor and these can differ from one university to another.
Make an appointment to see your personal tutor and ask them what their role is, what they expect from you and what you can expect from them.
Meetings with your mentors/sign-off mentors
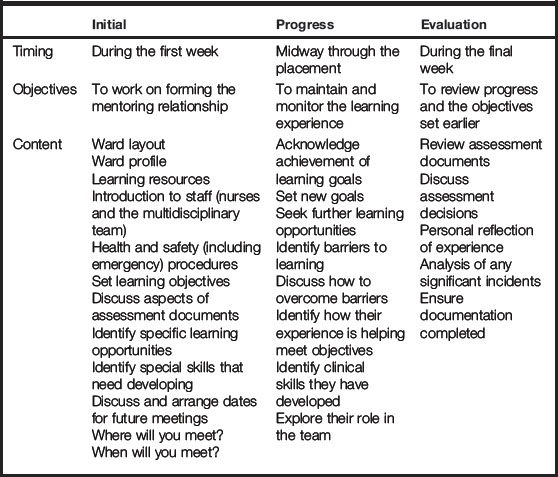
Within each of your placements you should have three meetings with your mentors:
1. An initial meeting – this should occur within your first week of placement.
2. An interim meeting – this should occur midway through your placement.
3. An endpoint meeting – this should occur at the end of your placement.
See Table 3.1 for what should occur within these meetings.
Student reflection
Every time I came on duty I would make beds, assist patients bathing and feeding and following my mentor when doing drug rounds. I thought that was not enough and wanted to do something more challenging than that. I gradually developed a skill of learning by negotiation. I put my objectives in writing so that when I am on duty I would show my mentor and ask if it was possible to follow my objectives. This helped me to achieve my objectives in time. I would sit down with my mentor and discuss how my objectives would be met. I learnt that we can learn through various ways like observing someone doing something or by practically doing it.
It is important to remember to inform your mentor of any adjustments that you require during your practice learning experience. You may have learning needs, for example dyslexia, dyspraxia or dyscalculia, that you have shared with your personal tutor at university to ensure that adjustments and support are offered for your academic work. Remember that you continue to learn within your placement and it is important that your mentors are aware so that they can make reasonable adjustments in practice to ensure that you receive the support you require. The practice experience facilitator will be working closely with the university and will be able to provide further support to you and the mentor.
The following Website can help:
http://www.rcn.org.uk/__data/assets/pdf_file/0003/333534/003835.pdf (accessed July 2011).
This is a Royal College of Nursing (2010) publication which has been developed for students as well as qualified nurses and others. in particular, it is a supportive publication which would be reassuring for any student with any of these three learning difficulties to negotiate assistance both before and during placement.
Practice assessment decisions
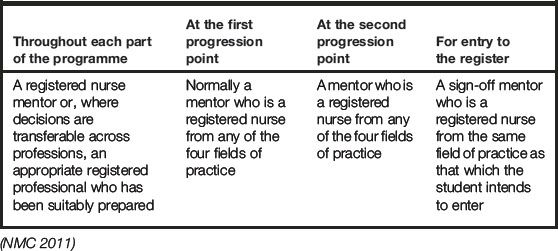
An area that can be confusing to students is who can assess them in practice. The standards introduce a flexible approach to the assessment of practice learning, and Table 3.2 summarises who is required to make assessment decisions at various stages of the programme.
Consider Table 3.2 and where you are in your nurse programme. Look at your learning outcomes together with your medical placement learning opportunities to understand who could possibly assess and help you to meet these outcomes.
As a senior student, you will be working alongside junior students. The NMC expects all nurses to mentor junior colleagues and it is important for you to adopt this role as you prepare to be a registered nurse (NMC 2008b,2010):
All nurses must continue their professional development, supporting the professional and personal development of others, demonstrating leadership, reflective practice, supervision, quality improvement and teaching skills.
(NMC 2010)
Combined with this, there is an expectation that the student nurse will progress to registered nurse with the ability to display leadership, management and team working (NMC 2010). You will find that a more junior student will often come to you before they will approach a registered nurse. It is important that you role model professional behaviour, are approachable and refer anything that you are unsure of. You will find that your knowledge base is required to be up-to-date in your final year of training and registered nurses will find it useful if you share any new knowledge or information.
When you are a registered nurse you will find that nurses often become link nurses for specialist areas, for example tissue viability, continence and infection. They will attend meetings run by clinical nurse specialists and they will have an obligation to share any new knowledge with their colleagues for practice to remain evidence-based, enabling patients to receive the best care possible.
As teaching will be a learning outcome for you, it is important that you speak to your mentor about how you can achieve this on the medical ward. Your mentor has undertaken a formal NMC recognised qualification to prepare to support learning and assessment within practice and should be able to help you develop your teaching skills. In your university modules in the final year, it is normal to find mentorship and teaching others as one of the main topics in preparation for you to make the transition from student to registered nurse.
Your mentor will understand where there will be opportunities to teach more junior colleagues and will support you with this. Your mentor may be able to suggest some areas for development that staff have identified. You may feel a lack of confidence and worry that you don't know enough to teach, however with adequate preparation and support from your mentor you should be able to achieve this. It may help you to think about students who have taught you in your first year and how knowledgeable they seemed. You could speak to junior colleagues and explain that you would like to undertake a teaching session and ask if there is anything they are struggling with or would like to learn.
Teaching within practice can take place formally or informally. Sometimes teaching is opportunistic and unplanned. For example, you might be handing over a group of patients and a junior colleague asks you what a term means, for example COPD. You might be planning discharge and someone might ask you why the patient needs a district nurse. Often junior students will be unclear about the plans of care for patients and will often struggle with nursing models and care planning.
Learning often takes place during professional discussions. For example, as you discuss patients with the multidisciplinary team, there are opportunities to clarify and reflect in and on care. Learning is not always formal or planned and it is important to take time at the end of the day to think about what you have learnt. You can document this in your reflective diary/journal.
When undertaking a formal teaching session for a few junior colleagues, ask your mentor how she plans her teaching? You will find examples of teaching plans within many books/articles, and once you have decided what to teach it is helpful to plan your teaching. Planning is an essential component for effective teaching (Fry et al 2001) and provides a clear framework even when the process is informal:
• It is important to consider where teaching can take place – most wards have an area where meetings take place and you may be able to book this space for your teaching.
• Make sure that you find out what is available – is there a white board, flip chart, does the ward have a laptop and projector? Your mentor will be able to help you with this.
• Is your session practical (e.g. taking manual blood pressure) and does the ward have enough sphygmomanometers and stethoscopes available?
• Think about the timing of your teaching and the knowledge level of your students. Do you want this to be an interactive session and do you want to assess their knowledge base at the beginning of the session? Sometimes a quiz can help with this. For example, do the students know the normal values for blood pressure?
• What is the aim of your teaching? Set specific objectives. What will they learn and what will they do? How will you evaluate what they have learnt? What resources do you need?
Take time to share your ideas with your mentor and listen to their advice. Try to ensure that your mentor observes your teaching and take time to reflect on your mentor's feedback. Your link lecturer may also be able to help you – remember that you have a lot of support. Ensure that this becomes one of your objectives.
Transferable skills
Whether this is your first ever placement or one of your final placements, you will have a wealth of transferable skills – skills you have acquired elsewhere that can be utilised in your new placement. It is worth spending some time thinking about what these skills may be before you commence your placement. This will give you an opportunity to reflect on your previous experiences and strengths and help build your confidence when starting in a new placement area.
It is not always easy to identify what your transferable skills may be, and this section aims to help you identify those relevant to your medical placement and give you some guidance as to how you can put them into practice.
Communication skills
Your communication skills will be wide ranging and probably quite advanced, even at an early stage in your training. They are the cornerstone of good nursing practice and you would not have been selected for your course if you had not already shown you had the potential to be a good communicator. They will be included within your learning outcomes as communication and interpersonal skills are a key NMC competency domain (NMC 2010). They are also part of the NMC Competencies for entry to the register and form part of the essential skills clusters (NMC 2010), whatever field of practice you are in.
Graduate nurses must have ‘presence’ demonstrated through the energy and quality of their interaction. They must communicate safely and effectively with individuals and groups of all ages, using a variety of complex skills and interventions including communication technologies. Communication must be characterised at all times by respect for the individual differences, care, compassion and dignity.
(NMC 2010)
Make a list of all the situations in your day-to-day life that require you to exercise your communication skills.
You may have thought of some of the following:
• Using the telephone to give information, make enquiries, confirm arrangements.
• Giving instructions to others, your children.
• Listening to the views, worries and concerns of family and friends.
• Making small talk with strangers, neighbours.
• Judging the mood of others from their body language, tone of voice.
• Asking questions to find out information from strangers, family and friends.
• Dealing with members of the public in current or previous jobs.
Now consider how your communication skills in each of these situations could be of benefit on your medical placement.
All of your communication skills will be of benefit to you on your placement. Telephone skills are essential and you will be expected to be able to answer the telephone as soon as you commence your first shift. It won't matter if you aren't able to answer the query on the other end of the line, but being able to answer politely and transfer the call and a message to someone who is able to help is essential. Being able to listen effectively to patients and other members of staff is vital if you are to carry out your duties well, and the ability to ask questions if you are not clear about instructions or information will be expected of you.
An awareness of your own body language and the ability to interpret that of others is very important, especially as patients may not always feel they are able to talk honestly about their feelings when they are feeling vulnerable. An ability to pick up on subtle non-verbal cues will be a skill you develop throughout your training, but even from your first placement you will have some ability to judge the mood and feelings of others as we are attuned to do this with our own family and friends. Have confidence that your communication skills are already in the process of developing and the time you spend on the medical ward will be invaluable in continuing this process.
Managing information
From the moment you step onto the ward you will find yourself bombarded with information. This may include the nursing handover at the start of the shift, giving you vital information about the patients you will be caring for; it may be instructions and advice from staff on where you will be working and what will be expected of you. Also, as mentioned before, it may be information given directly to you from patients, relatives or other members of the team that needs to be communicated to others. Whatever this information is, you need to be able to manage it appropriately and use it to get the best out of your placement.
It is your first day on your medical ward placement and within the first hour of your shift you have been given the following information:
 Name and role of all the staff on duty.
Name and role of all the staff on duty.
 Ward layout and location of emergency equipment.
Ward layout and location of emergency equipment.
 The name of your mentor and when they will be on duty.
The name of your mentor and when they will be on duty.
 Name, age, diagnosis and progress update for 26 patients.
Name, age, diagnosis and progress update for 26 patients.
 Instructions from the nurse in charge as to which patients you will be looking after, who you will be working with and what you will be expected to do.
Instructions from the nurse in charge as to which patients you will be looking after, who you will be working with and what you will be expected to do.
 Requests for pain relief from two patients.
Requests for pain relief from two patients.
 A telephone call from a relative wanting to know how their loved one is.
A telephone call from a relative wanting to know how their loved one is.
Consider what your strategies would be for managing all of this information.
There are a number of different skills you will employ to manage the information given to you and many of them will come naturally to you. The situation in the activity above may seem daunting to some but you are probably used to managing this amount of information in your everyday life.
Think about how often you are juggling information in your day-to-day life:
A common way to manage information – especially that which is important or unfamiliar to us – is to write it down. This will be an essential strategy to use on your medical placement. Different placement areas will have different policies on what patient information may be written down for your personal use, so it is important that you are familiar with local policy and procedures regarding this. A working understanding of the confidentiality policy of your placement area and the Data Protection Act is also necessary.
Information such as your shift patterns, meetings with your mentor and other study sessions you need to attend while on placement can all be written down and kept somewhere safely, as this sort of information is not necessary for you to remember at all times. Information pertaining to the patients you are looking after, requests from patients and messages or instructions from others will need to be close at hand on your shift and possibly dealt with immediately. Again, don't be afraid of writing down the seemingly small things as well as those that seem very important, as having the information to hand when someone asks for it will give you confidence.
Think carefully about where you write things down and how. Lots of scraps of paper with different bits of information on may only make you more confused, although, if you write everything in the same place (in a notebook for example) and this becomes mislaid, you have lost all your important information. Probably a combination of the two is the better option. Use a notebook for things you may want to reflect on or use later, and use separate pieces of paper for messages to be passed on or information that can be discarded appropriately after use. You must be careful what you write down to ensure that a patient cannot be identified, in case you ever misplace it, to protect patient confidentiality (NMC 2009).
Find out how confidential waste is managed in your placement area so you can dispose of anything with patient details on in the right manner.
As you become more confident and familiar with your medical placement and as you proceed through your training, the way you manage information will change as managing previously unfamiliar information becomes the norm. Managing information such as blood test results and vital signs can be difficult unless you have a good understanding of how these things are measured and what the normal value ranges are. Similarly the names of conditions being experienced and investigations your patients may need may be very unfamiliar. It is worth doing some revision on the sorts of conditions you are likely to meet on the medical ward to prepare yourself and build your confidence when handling this kind of information (see Ch. 1 for suggestion on what to revise).
Another challenge will be ensuring that any information you pass on or is passed to you can be understood. For this, it is essential that you are able to make clear written notes that both you and others will be able to understand later on. Abbreviations are useful when you are taking down a lot of information in a short amount of time, but be sure that you will remember what you meant later on. Try to avoid the use of abbreviations when passing on information to others as they can often mean different things to different people. If you have been taught abbreviations in a previous placement, check that they mean the same thing in your medical placement, as different specialties will often use the same abbreviation to mean different things. If the person giving you information is using abbreviations, don't be afraid to stop and ask them what they mean – they will assume you understand if you don't say anything.
Technology
Nursing practice is becoming increasingly reliant on technology as a way of sharing information and monitoring the progress of a patient's condition. You no doubt will already have at least basic computer skills and considerable experience using a range of electronic equipment at home. All of these skills will be invaluable to you on your placement. Your placement organiser will probably arrange for you to have training and access to the computer systems used locally, but you will need to ask your mentor to guide you in the most appropriate use of these systems in your placement area. If you have already been on a placement within the same hospital or institution, then your transferable skills in this area will be considerably greater and you may even be able to use your knowledge to support students who are on their first placements.
Other pieces of equipment do vary though, so even if you are working in the same hospital as your previous placement, the equipment being used may be different or the same piece of equipment may be being used in a different way. Ensure you ask your mentor about which equipment you need to be trained to use.
Caring for patients
Providing direct care to patients is the essential business of nursing but can also be the most daunting when you commence a new placement and especially your first placement. You will have many transferable skills in this area that you probably don't even realise you have.
If this is your first placement then a good rule of thumb is to think about how you would want to be cared for if you were a patient in hospital. When providing personal care such as help with washing, dressing or toileting, then protecting your patient's dignity is the most important thing you can do and all the other necessary skills will soon follow. Asking your patient what they would like you to help with is the best way to start and be guided by them at all times if they are able to tell you.
If you have had previous placements in other areas then this may be an area you feel considerably more confident in. This placement may then be an opportunity for you to develop your skills in this area, such as enhancing your assessment skills when helping with personal care and teaching junior students.
Many clinical skills are also taught in a simulated environment such as a skills lab prior to commencing a placement. This will enhance your confidence and competency in such situations as helping to provide direct care to patients, moving and handling, resuscitation, bed making, taking vital signs and many more.
The routine on a medical placement is likely to be different to that of other specialties, so ensure you ask your mentor about the routine and what is seen as priority on the ward. For example, some wards may record the patients’ vital signs before breakfast; other places will record them at 10 a.m. if they had been recorded at 6 a.m. by the night shift. Understanding the routine of the medical placement will help you use your transferable skills to the best of your ability.
Local knowledge and information
If you live in or close to the area of the hospital you are placed in then your knowledge of the local environment and population will be very useful when seeking to understand the problems faced by many of your patients. It will also serve as a talking point to break the ice when meeting patients for the first time. Having an awareness of the demography of your local population, prominent cultures, religions and languages and socioeconomic status is an important starting point in providing direct care to your patients, ensuring you have a greater understanding of their problems and can ensure they are treated with dignity and respect. If you speak any of the languages used in your local area then this will be a skill you may often be called upon to use.
If you don't know the local area well, there are plenty of ways to find this out. Talk to other students or friends who may know the area better. Your university tutors and placement organiser will have a good knowledge of the hospital and the area it is situated in.
Summary
Throughout your placement you will continue to gain skills that you will be able to take with you to your next placement and on through your career in nursing. You wouldn't be undertaking your nursing training if you didn't already have the beginnings of the essential skills required to be a good nurse, so be confident in yourself and the skills you have gained from all aspects of your life and don't be afraid to ask questions!
Department of Health. Making a Difference. Strengthening the nursing, midwifery and health visiting contribution to health and healthcare. London: Department of health; 1999.
Fry H., Ketteridge S., Marshall S. A handbook for teaching & learning in higher education : enhancing academic practice. London: Kogan Page; 1999.
Lauder W., Holland K., Roxburgh M., et al. Measuring competence, self reported competence and self-efficacy in preregistration students. Nursing Standard. 2008;22:35–44.
Levett- Jones T., Bourgeois S. The Clinical Placement A Nursing survival guide, 2nd ed. London: Elsevier; 2009.
Nursing and Midwifery Council. The code: standards of conduct, performance and ethics for nurses and midwives. London: NMC; 2008.
Nursing and Midwifery Council. Supporting assessment and learning in practice. London: NMC; 2008.
Nursing and Midwifery Council. Guidance on professional conduct for nursing and midwifery students. London: NMC; 2009.
Nursing and Midwifery Council. Standards for pre-registration nursing education. London: NMC; 2010.
Nursing and Midwifery Council. Advice and supporting information for implementing NMC standards for pre-registration nursing education. London: NMC; 2011.
Parker P. Why should we assess in practice? J. Nursing Management. 2009;17:559–569.
Royal College of Nursing. Dyslexia, dyspraxia and dyscalculia: a toolkit for nursing staff. London: RCN; 2010.
Sharples K. Learning to learn in practice: a guide for nursing students. Transforming nursing practice. Exeter: Learning Matters; 2009.
Thompson I.E., Melia K.M., Boyd K.M., et al. Nursing ethics, 5th ed. Edinburgh: Churchill Livingstone; 2006.
United Kingdom Central Council for Nursing, Midwifery and Health Visiting. Peach report. UKCC Commission for Nursing and Midwifery and Education fitness for practice. London: UKCC; 1999.
Ball M.J. Nursing informatics: where caring and technology meet, 4th ed. New York: Springer; 2010.
Benbow W., Jordan G. A handbook for student nurses: introducing key issues relevant for practice. Exeter: Reflect Press; 2009.
Burton R., Ormrod G. Nursing: transition to professional practice. Oxford: Oxford University Press; 2011.
Holloway I., Wheeler S. Qualitative research in nursing and health care, third ed. Oxford: Wiley–Blackwell; 2010.
Nursing and Midwifery Council. Annex 1. Confirmation of resources to support achievement of intended programme outcomes. London: NMC; 2011. Online. Available at: http://www.nmc-uk.org/Documents/Circulars/2011Circulars/nmcCircular03_2011_Annexe1-Confirmation-of-resources.pdf (accessed July 2011)
Peate I. Compendium of clinical skills for student nurses. London: Whurr; 2005.
Richardson R., ed. Clinical skills for student nurses: theory, practice and reflection. Exeter: Reflect Press, 2008.
Roberts D. How you will learn in practice. In: Hart S., ed. Nursing: study and placement learning skills. Oxford: Oxford University Press, 2010.
Roberts P.M., Priest H. Healthcare research: a handbook for students and practitioners. Oxford: Wiley–Blackwell; 2010.
http://www.nmc-uk.org/Students/Guidance-for-students/. (accessed July 2011)
http://www.nmc-uk.org/Students/Good-Health-and-Good-Character-for-students-nurses-and-midwives/. (accessed July 2011)
There are a number of helpful publications for student nurses at the Royal College of Nursing Website which would be helpful to read prior to undertaking any clinical placement experience:.
Helping students get the best from their practice placements (2004: reprinted with amendments in 2006). Please keep in mind when reading it that the NMC have now amended their standards for pre-registration nursing education (NMC 2010). http://www.rcn.org.uk/development/publications/publicationsA-Z?78808_result_page=H#H. (accessed July 2011)
An ageing population: education and practice preparation for nursing students learning to work with older people. A resource pack for nursing students (RCN 2008). A very useful publication based on a research project which will help students understand the specific needs of older people in any healthcare setting. http://www.rcn.org.uk/__data/assets/pdf_file/0005/149558/003222.pdf. (accessed July 2011)
Benchmarks for children's orthopaedic nursing care. RCN guidance (RCN 2007). An excellent publication relating to children's nursing care in an orthopaedic context which also has sections relating to surgical nursing, pre- and post-operative care. http://www.rcn.org.uk/__data/assets/pdf_file/0007/115486/003209.pdf. (accessed July 2011)
Dignity in health care for people with learning disabilities (RCN 2010). Another excellent publication offering examples of best practice in caring for people with learning disabilities in various healthcare settings, including being in hospital. http://www.rcn.org.uk/__data/assets/pdf_file/0010/296209/003553.pdf. (accessed July 2011)
Dyslexia, dyspraxia and dyscalculia: a toolkit for nursing staff (2010). This is a publication which has been developed for students as well as qualified nurses and others. It is a particularly supportive one which would be reassuring for any student with any of these learning difficulties to negotiate assistance, both before and during placement. http://www.rcn.org.uk/__data/assets/pdf_file/0003/333534/003835.pdf. (accessed July 2011)