27 Desensitization (tachyphylaxis) in signalling pathways
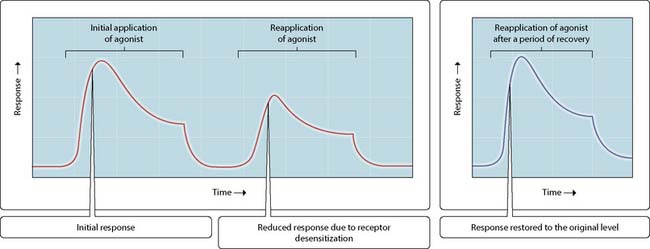
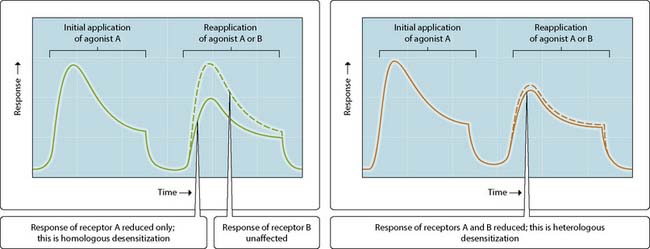
When cells are exposed continuously to an extracellular messenger or drug, they can often become increasingly resistant to stimulation. This loss of sensitivity is known as desensitization or tachyphylaxis when it occurs acutely over a few minutes, and tolerance or resistance when occurring over a period of days or weeks. Desensitization can take two forms. When sensitivity is lost to a single extracellular agonist, this is known as homologous desensitization (Fig. 3.27.1). When sensitivity is lost to multiple stimulating agonists in response to the presence of a single stimulating agonist, this is known as heterologous desensitization (Fig. 3.27.2).
Many mechanisms may contribute to cellular desensitization. At the level of the receptor, a change in receptor properties or a reduction in the number of receptors may bring about desensitization. Alternatively, metabolic desensitization could occur through exhaustion of a mediator within a signalling pathway, increased degradation of the extracellular signalling molecule and/or physiological adaptation to the raised levels of signalling molecule.
Receptor desensitization
Ligand-gated ion channels desensitize rapidly. When continually exposed to agonist, these receptors undergo a slow transition to a stable conformation that binds agonist with high affinity but in which the channel remains closed. Desensitization is reversed when the concentration of agonist falls and the agonist dissociates.
Desensitization of G-protein-coupled receptors can occur through modification of the activated receptor by phosphorylation, reversible removal of the receptor from the plasma membrane or irreversible removal and degradation of the receptor; the last is known as downregulation. Receptor phosphorylation may be in response to protein kinases activated by second messengers (e.g. cyclic AMP-dependent protein kinase (cA-PK) or protein kinase C) or specific G-protein-receptor protein kinases (e.g. β-adrenoceptor kinase) (Fig. 3.27.3).
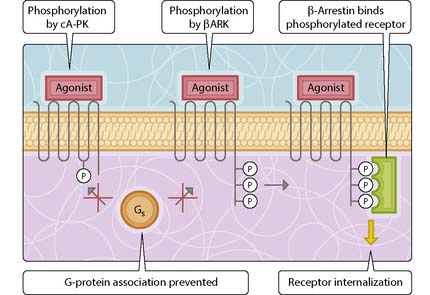
Fig. 3.27.3 Methods of desensitization. βARK, β-adrenoceptor kinase; cA-PK, cyclic AMP-dependent protein kinase.
Some activated receptors can be internalized by receptor-mediated endocytosis. A short period of desensitization results if the internalized receptors are sorted and recycled to the plasma membrane. On prolonged cell stimulation, receptors may become targeted to lysosomes where they are degraded; this results in receptor downregulation. The results of downregulation are reversed only by the synthesis of new receptors. It is noteworthy that downregulation of receptors can occur in response to molecules other than agonist. For example, ethanol and barbiturates, which are not receptor agonists, may lead to downregulation of G-protein-coupled receptors, an example of tolerance.
Cell supersensitivity
The sensitivity of a cell to an external stimulus may be increased by convergent cross-talk between signalling pathways. For example, glucagon and glucagon-like peptide do not stimulate release of insulin from beta-cells per se but potentiate the response to a given level of glucose through a cA-PK mechanism. Similarly, β-adrenergic stimulation in the heart can increase heart rate and force of contraction, again through a cA-PK mechanism via phosphorylation of L-type voltage-sensitive Ca2+ channels. This phosphorylation increases the probability that Ca2+ channels will open and, therefore, leads to a greater Ca2+ signal for a given depolarization.
Supersensitivity may also occur following interruption of normal signalling to the cell. This is often seen after denervation of peripheral tissues. The response in the postsynaptic cell can be to increase the number of receptors and to increase postjunctional responsiveness by increasing electrical excitability.
![]() Receptor desensitization and insulin resistance in diabetes
Receptor desensitization and insulin resistance in diabetes
In type 2 diabetes mellitus, tissues become resistant to insulin even though insulin may be present at raised levels. One contributory factor to insulin resistance is the downregulation of insulin receptors.
![]() Drug habituation and ‘rebound’ effects
Drug habituation and ‘rebound’ effects
Rebound effects on removal of drug therapy
Adaptive responses in cells in an attempt to overcome the effect of a drug during treatment may result in a rebound effect in response to natural agonists when therapy ceases. For example, sudden withdrawal of β-adrenoceptor antagonists can cause an increased sympathetic stimulation of the heart. The resulting increase in heart rate and force of contraction, and hence oxygen consumption, can lead to the development of angina pectoris and myocardial infarction.