Abdomen
Dan L. Hobbs, MSRS, RT(R)(CT)(MR)
John P. Lampignano, MEd, RT(R)(CT), Kathy M. Martensen, BS, RT(R) and Barry T. Anthony, RT(R)
Radiographic Anatomy
Abdominal Radiography
This chapter covers the anatomy and positioning for what are sometimes called “plain films” (images) of the abdomen. The most common image is an anteroposterior (AP) supine abdomen, also sometimes called a KUB (kidneys, ureters, and bladder). These radiographs are taken without the use of contrast media. Plain radiographs of the abdomen (KUB) commonly are taken before abdominal examinations are performed with the use of contrast media to rule out certain pathologies.
Certain acute or emergency conditions of the abdomen may develop from conditions such as bowel obstruction, perforations involving free intraperitoneal air (air outside the digestive tract), excessive fluid in the abdomen, or a possible intra-abdominal mass. These acute or emergency conditions require what is commonly called an “acute abdominal series,” or a “two-way” or “three-way abdomen” series, wherein several abdominal radiographs are taken in different positions to demonstrate air-fluid levels or free air or both within the abdominal cavity.
Abdominal radiography requires an understanding of anatomy and relationships of the organs and structures within the abdominopelvic cavity.
Abdominal Muscles
Many muscles are associated with the abdominopelvic cavity. The three that are most important in abdominal radiography are the diaphragm and the right and left psoas (so′-es) major.
The diaphragm is an umbrella-shaped muscle that separates the abdominal cavity from the thoracic cavity. The diaphragm must be perfectly motionless during radiography of either the abdomen or the chest. Motion of the patient's diaphragm can be stopped when appropriate breathing instructions are given to the patient.
The two psoas major muscles are located on either side of the lumbar vertebral column. The lateral borders of these two muscles should be faintly visible on a diagnostic abdominal radiograph of a small to average-sized patient when correct exposure factors are used (see arrows, Fig. 3-1).
Abdominal Organ Systems
The various organ systems found within the abdominopelvic cavity are presented briefly in this chapter. Each of these systems is described in greater detail in later chapters devoted to the specific systems.
Digestive System
The digestive system, along with its accessory organs, the liver, gallbladder, and pancreas, fills much of the abdominal cavity. The pancreas is located posterior to the stomach and is not well visualized on this drawing.
The spleen (part of the lymphatic system) is also partially visible in the left upper abdomen posterior to the stomach. The six organs of the digestive system are as follows:
Stomach and Small and Large Intestines
The three digestive organs within the abdominal cavity are the stomach and small and large intestines.
The stomach is the first organ of the digestive system that is located within the abdominal cavity. The stomach is an expandable reservoir for swallowed food and fluids. The size and shape of the stomach vary depending on the volume of its contents and on the body habitus.
Gastro is a common combining form denoting a relationship to the stomach (the Greek word gaster means “stomach”). The term gastrointestinal (GI) tract or system describes the entire digestive system, starting with the stomach and continuing through the small and large intestines.
The small intestine continues from the stomach as a long, tubelike convoluted structure about 4.5 to 5.5 m (15 to 18 feet) in length. The three parts of the small intestine as labeled in Figs. 3-4 and 3-5 are as follows: duodenum (doo″o-de′-num) (A); jejunum (je-joo′-num) (B); ileum (il′-eum) (C).
The first portion of the small intestine, the duodenum, is the shortest but widest in diameter of the three segments. It is about 25 cm (10 inches) in length. When filled with contrast medium, the duodenum looks like the letter C. The proximal portion of the duodenum is called the duodenal bulb, or cap. It has a characteristic shape that usually is well seen on barium studies of the upper GI tract. Ducts from the liver, gallbladder, and pancreas drain into the duodenum.
The remainder of the small bowel lies in the central and lower abdomen. The first two-fifths following the duodenum is called the jejunum, and the distal three-fifths is called the ileum. The orifice (valve) between the distal ileum and the cecum portion of the large intestine is the ileocecal valve.
Radiograph of stomach and small intestine
Air seldom is seen filling the entire stomach or small intestine on a plain abdominal radiograph of a healthy, ambulatory adult. This radiograph shows the stomach, small intestine, and proximal large intestine because they are filled with radiopaque barium sulfate (see Fig. 3-5). Note the duodenal bulb and the long convoluted loops of the three labeled parts of the small intestine located in the midabdomen and lower abdomen.
The sixth and last organ of digestion is the large intestine, which begins in the right lower quadrant at the junction with the small intestine at the ileocecal valve. The portion of the large intestine below the ileocecal valve is a saclike area called the cecum. The appendix (vermiform appendix) is attached to the posteromedial aspect of the cecum.
The vertical portion of the large bowel above the cecum, the ascending colon, joins the transverse colon at the right colic (kol′-ik, referring to colon) flexure. The transverse colon joins the descending colon at the left colic flexure. Alternative secondary names for the two colic flexures are hepatic and splenic flexures based on their proximity to the liver and spleen, respectively.
The descending colon continues as the S-shaped sigmoid colon in the lower left abdomen. The rectum is the final 15 cm (6 inches) of the large intestine. The rectum ends at the anus, the sphincter muscle at the terminal opening of the large intestine.
As seen in body habitus drawings, the shape and location of the large intestine vary greatly, with the transverse colon located high in the abdomen on wide hypersthenic types and low in the abdomen on slender hyposthenic and asthenic types. This is demonstrated in Chapters 12 and 13.
Spleen
The spleen is the part of the lymphatic system that along with the heart and blood vessels is part of the circulatory system. It is an important abdominal organ that occupies a space posterior and to the left of the stomach in the left upper quadrant, as shown in Fig. 3-7.
The spleen may be visualized faintly on plain abdominal radiographs, particularly if the organ is enlarged. It is a fragile organ and is sometimes lacerated during trauma to the lower left posterior rib cage.
Accessory Digestive Organs
Three accessory organs of digestion, also located in the abdominal cavity, are the (1) pancreas, (2) liver, and (3) gallbladder.
The pancreas, which is not seen on a plain abdominal radiograph, is an elongated gland that is located posterior to the stomach and near the posterior abdominal wall, between the duodenum and the spleen. The average length is about 12.5 cm (6 inches). Its head is nestled in the C-loop of the duodenum, and the body and tail of the pancreas extend toward the upper left abdomen. This relationship of the duodenum and the head of the pancreas sometimes is referred to as “the romance of the abdomen.”
The pancreas is part of the endocrine (internal) secretion system and the exocrine (external) secretion system. The endocrine portion of the pancreas produces certain essential hormones, such as insulin, which aids in controlling the blood sugar level of the body. As part of its exocrine functions, the pancreas produces large amounts ( quarts [1500 mL] daily) of digestive juices that move to the duodenum through a main pancreatic duct as needed for digestion.
quarts [1500 mL] daily) of digestive juices that move to the duodenum through a main pancreatic duct as needed for digestion.
The liver is the largest solid organ in the body, occupying most of the right upper quadrant. The liver has numerous functions, one of which is the production of bile that assists in the digestion of fats. If bile is not needed for digestion, it is stored and concentrated for future use in the gallbladder.
The gallbladder is a pear-shaped sac located below the liver. The primary functions of the gallbladder are to store and concentrate bile and to contract and release bile when stimulated by an appropriate hormone. In most cases, the gallbladder cannot be visualized with conventional radiographic techniques without contrast media. This is because the gallbladder and the biliary ducts blend in with the other abdominal soft tissues and in most cases cannot be visualized. The anatomy of the gallbladder and biliary ducts is described in greater detail in Chapter 12. Only about 10% to 15% of all gallstones contain enough calcium to allow visualization on a plain abdominal radiographic image.
CT Cross-Sectional Images
Cross-sectional (axial) CT (computed tomography) images through various levels of the abdomen demonstrate anatomic relationships of the digestive organs and their accessory organs as well as the spleen.
Fig. 3-8 shows a sectional view of the upper abdomen at the level of T10 or T11 (tenth or eleventh thoracic vertebrae) just below the diaphragm. Note the proportionately large size of the liver at this level in the right upper abdomen and the cross-sectional view through the stomach to the left of the liver. The spleen is visualized posterior to the stomach in the left upper abdomen.
Fig. 3-9 is a cross-sectional image a little lower through the upper abdomen at the approximate level of L2 (second lumbar vertebra). The pancreas is seen adjacent to a portion of the duodenal loop posterior to the distal part of the stomach. Note the air-fluid level in the stomach with the heavy barium fluid mixture (white) in the posterior stomach. The dark air-filled portion of the stomach is on top (anteriorly), indicating that the patient was lying in a supine position for this CT scan.
Urinary System
The urinary system is another important abdominal system. Although this system is introduced in this chapter, it is discussed in detail in Chapter 14.
The urinary system comprises the following:
Each kidney drains via its own ureter to the single urinary bladder. The bladder, which is situated above and behind the symphysis pubis, stores urine. Under voluntary control, the stored urine passes to the exterior via the urethra. The two suprarenal (adrenal) glands of the endocrine system are located at the superomedial portion of each kidney. The bean-shaped kidneys are located on either side of the lumbar vertebral column. The right kidney usually is situated a little lower than the left one because of the presence of the large liver on the right.
Waste materials and excess water are eliminated from the blood by the kidneys and are transported through the ureters to the urinary bladder.
Excretory or Intravenous Urogram
The kidneys usually are seen faintly on a plain abdominal radiograph because of a fatty capsule that surrounds each kidney. The contrast medium examination shown in Fig. 3-11 is an excretory or intravenous urogram (IVU), which is a radiographic examination of the urinary system performed with intravenous contrast medium. During this examination, the hollow organs of this system are visualized with use of the contrast medium that has been filtered from the blood flow by the kidneys. The organs as labeled are the left kidney (A), the left proximal ureter (B), the left distal ureter (C) before emptying into the urinary bladder, and the right kidney (D).
NOTE: The term intravenous pyelogram (IVP) often was used in the past for this examination. However, this is not an accurate term for this examination because pyelo refers to the renal pelvis of the kidney, and an excretory or intravenous urogram includes a study of the entire urinary tract, which comprises the total collecting system. (The terms excretory urogram [EU] and intravenous urogram [IVU] are both current and correct terms, but intravenous urogram is the term that is used most commonly.)
The sectional CT image (Fig. 3-12) may appear confusing at first because of the numerous small, odd-shaped cross-sectional images that are visualized. However, as you study the relationships between these structures and imagine a thin “slice” view through the level of about L2-L3 of the drawings (see Fig. 3-10) and on the previous page (see Fig. 3-7), you should be able to identify each of these structures as labeled in Fig. 3-12. See how many of the structures labeled A through J you can identify without looking at the answers listed next.
Two major blood vessels of the abdomen are also seen, labeled K and L. K is the large abdominal aorta, and L is the inferior vena cava.
Abdominal Cavity
Four important terms that describe the anatomy of the abdominal cavity appear on the drawings to the right and are described subsequently. These four terms are:
Peritoneum
Most of the abdominal structures and organs as well as the wall of the abdominal cavity in which they are contained are covered to varying degrees by a large serous, double-walled, saclike membrane called the peritoneum. The total surface area of the peritoneum is about equal to the total surface area of the skin that covers the entire body.
A greatly simplified cross-section of the abdominal cavity is shown in Fig. 3-13. Two types of peritoneum exist: parietal and visceral. The two-layered peritoneum that adheres to the cavity wall is called parietal peritoneum, whereas the portion that covers an organ is called visceral peritoneum. The space or cavity between the parietal and visceral portions of the peritoneum is called the peritoneal cavity. This space is really only a potential cavity because normally it is filled with various organs. If all the loops of bowel and the other organs of the abdominal cavity were included in the drawing, little actual space would be left in the peritoneal cavity. This cavity contains some serous lubricating-type fluid, which allows organs to move against each other without friction. An abnormal accumulation of this serous fluid is a condition called ascites. (See Clinical Indications, p. 113.)
A layer of visceral peritoneum only partially covers certain organs that are more closely attached to the posterior abdominal wall (see Fig. 3-13). At this level, the ascending and descending colon, the aorta, and the inferior vena cava are only partially covered; therefore, this lining would not be considered mesentery, and these structures and organs are called retroperitoneal, as described on the following page.
Mesentery
The peritoneum forms large folds that bind the abdominal organs to each other and to the walls of the abdomen. Blood and lymph vessels and the nerves that supply these abdominal organs are contained within these folds of peritoneum. One of these double folds that hold the small intestine in place is called mesentery. Mesentery is the double fold of peritoneum that extends anteriorly from the posterior abdominal wall to envelop completely a loop of small bowel. Mesentery is the specific term for a double fold of peritoneum that loosely connects the small intestine to the posterior abdominal wall (Fig. 3-14).
Omentum
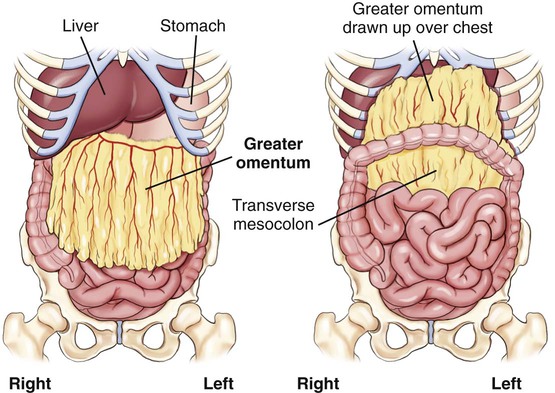
The term omentum refers to a specific type of double-fold peritoneum that extends from the stomach to another organ (see Fig. 3-14). The lesser omentum extends superiorly from the lesser curvature of the stomach to portions of the liver. The greater omentum connects the transverse colon to the greater curvature of the stomach inferiorly. The greater omentum drapes down over the small bowel then folds back on itself to form an apron along the anterior abdominal wall.
If one entered the abdomen through the midanterior wall, the first structure encountered beneath the parietal peritoneum would be the greater omentum. Varying amounts of fat are deposited in the greater omentum, which serves as a layer of insulation between the abdominal cavity and the exterior. This is sometimes called the “fatty apron” because of its location and the amount of fat contained therein (Fig. 3-15).
Mesocolon
The peritoneum that attaches the colon to the posterior abdominal wall is the mesocolon. Four forms of mesocolon exist, each named according to the portion of the colon to which it is attached: ascending, transverse, descending, and sigmoid or pelvic. The transverse mesocolon is shown in Fig. 3-15 as the visceral peritoneum that loosely connects the transverse colon to the posterior abdominal wall.
Greater Sac and Lesser Sac
The drawing in Fig. 3-16 shows the two parts of the peritoneal cavity. The major portion of the peritoneal cavity is called the greater sac and is commonly referred to as simply the peritoneal cavity. A smaller portion of the upper posterior peritoneal cavity located posterior to the stomach is called the lesser sac. This sac has a special name—the omentum bursa.
This drawing shows the mesentery connecting one loop of small intestine (ileum) to the posterior abdominal wall. A full drawing of a normal abdomen would have many loops of small bowel connected to the posterior wall by mesentery.
The prefix meso- is used to refer to mesentery-type folds from which other abdominal organs are suspended, such as the transverse mesocolon, which is shown to be connecting the transverse colon to the posterior abdominal wall.
Retroperitoneal and Infraperitoneal Organs
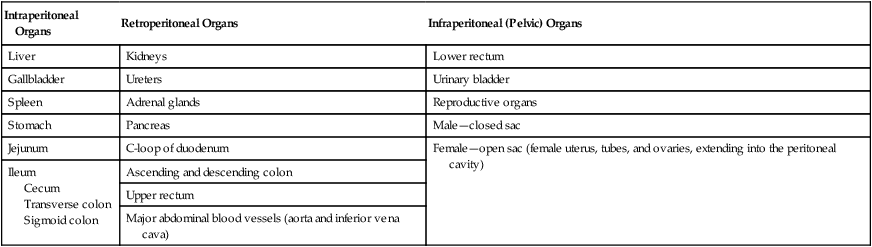
The organs shown in Fig. 3-17 are considered either retroperitoneal (retro, meaning “backward” or “behind”) or infraperitoneal (infra, meaning “under” or “beneath”).
Structures closely attached to the posterior abdominal wall that are retroperitoneal as shown on this drawing are the kidneys and ureters, adrenal glands, pancreas, C-loop of duodenum (aspect adjacent to head of pancreas), ascending and descending colon, upper rectum, abdominal aorta, and inferior vena cava.
These retroperitoneal structures are less mobile and move around less within the abdomen than other intraperitoneal organs. For example, Fig. 3-16 shows that the stomach, small intestine, and transverse colon are only loosely attached to the abdominal wall by long loops of different types of peritoneum and change or vary greatly in their position within the abdomen compared with retroperitoneal or infraperitoneal structures. (This is an important consideration in positioning of the GI system.)
Male Versus Female Peritoneal Enclosures
One significant difference exists between male and female peritoneal enclosures. The lower aspect of the peritoneum is a closed sac in the male but not in the female. In males, the lower peritoneal sac lies above the urinary bladder, totally separating the reproductive organs from the organs within the peritoneal cavity. In females, the uterus, uterine (fallopian) tubes, and ovaries pass directly into the peritoneal cavity (see Fig. 3-16).
Intraperitoneal Organs
Organs within the abdominal cavity that are partially or completely covered by some type of visceral peritoneum but are not retroperitoneal or infraperitoneal may be called intraperitoneal (intra, meaning “within”). These organs, which have been removed from the drawing in Fig. 3-17, include the liver, gallbladder, spleen, stomach, jejunum, ileum, cecum, and transverse and sigmoid colon.
Quadrants and Regions
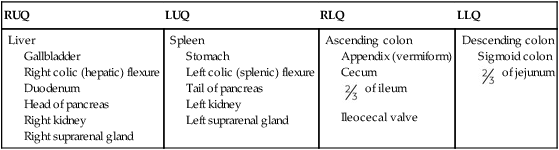
To facilitate description of the locations of various organs or other structures within the abdominopelvic cavity, the abdomen may be divided into four quadrants or nine regions.
Four Abdominal Quadrants
If two imaginary perpendicular planes (at right angles) were passed through the abdomen at the umbilicus (or navel), they would divide the abdomen into four quadrants. One plane would be transverse through the abdomen at the level of the umbilicus, which on most people is at the level of the intervertebral disk between L4 and L5 (fourth and fifth lumbar vertebrae), which is about at the level of the iliac crests on a female.
The vertical plane would coincide with the midsagittal plane or midline of the abdomen and would pass through both the umbilicus and the symphysis pubis. These two planes would divide the abdominopelvic cavity into four quadrants: right upper quadrant (RUQ), left upper quadrant (LUQ), right lower quadrant (RLQ), and left lower quadrant (LLQ).
NOTE: The four-quadrant system is used most frequently in radiography for localizing a particular organ or for describing the location of abdominal pain or other symptoms.
Nine Abdominal Regions
The abdominopelvic cavity also can be divided into nine regions through the use of two horizontal or transverse planes and two vertical planes. The two transverse/horizontal planes are the transpyloric plane and the transtubercular plane. The two vertical planes are the right and left lateral planes (Fig. 3-20).
The transpyloric plane is at the level of the lower border of L1 (first lumbar vertebra), and the transtubercular plane is at the level of L5. The right and left lateral planes are parallel to the midsagittal plane and are located midway between it and each anterior superior iliac spine (ASIS).
The names of these nine regions are given in the following list. Technologists should be familiar with the locations and names of these nine regions. However, in general, locating most structures and organs within the four-quadrant system is sufficient for radiographic purposes because of variables that affect specific locations of organs, such as body habitus, body position, and age (see organ outlines in Fig. 3-20 for general locations of organs within these nine regions).
Topographic Landmarks
Abdominal borders and organs within the abdomen are not visible from the exterior, and because these soft tissue organs cannot be palpated directly, certain bony landmarks are used for this purpose.
NOTE: Palpation must be done gently because the patient may have painful or sensitive areas within the abdomen and pelvis. Also, ensure that the patient is informed of the purpose of palpation before beginning.
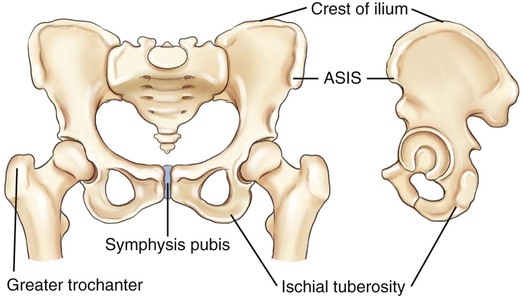
Seven Landmarks of the Abdomen
The following seven palpable landmarks are important in positioning the abdomen or locating organs within the abdomen. You should practice finding these bony landmarks on yourself before attempting to locate them on another person or on a patient for the first time.
Positioning for abdominal radiographs in AP or posteroanterior (PA) projections requires quick but accurate location of these landmarks on thin patients as well as on heavy-set or muscular patients, who require more firm palpation.
1. Xiphoid process (level of T9-T10): The tip of the xiphoid process is the most distal or inferior process of the sternum. This landmark can best be palpated by first gently pressing on the soft abdomen below the distal sternum, then moving upward carefully against the firm, distal margin of the xiphoid process. This landmark approximates the superior anterior portion of the diaphragm, which is also the superior margin of the abdomen. However, this is not a primary landmark for positioning the abdomen because of variation in body types and the importance of including all of the lower abdomen on most radiographic images of the abdomen.
2. Inferior costal (rib) margin (level of L2-L3): This landmark is used to locate upper abdominal organs, such as the gallbladder and stomach.
3. Iliac crest (level of L4-L5 vertebral interspace): The crest of the ilium is the uppermost portion of the curved border of the ilium. The iliac crest can be palpated easily by pressing inward and downward along the midlateral margin of the abdomen. The uppermost or most superior portion of this crest is the most commonly used abdominal landmark and corresponds approximately to the level of the midabdomen, which is also at or just slightly below the level of the umbilicus on most people. If the center of the cassette or image receptor (IR) is centered to this level, the lower abdominal area generally is included on the lower margin of the IR.
NOTE: Ensuring that the entire upper abdomen, including the diaphragm, is included on the IR requires centering about 5 cm (2 inches) above the level of the crest for most patients, which usually cuts off some of the important lower abdomen. A second IR centered lower would be required to include this lower region.
4. Anterior superior iliac spine (ASIS): The ASIS can be found by locating the iliac crest, then palpating anteriorly and inferiorly until a prominent projection or “bump” is felt (more prominent on females). This landmark is commonly used for positioning of pelvic and vertebral structures but can also serve as a secondary landmark for general abdominal positioning.
5. Greater trochanter: This landmark is more easily palpated on thin patients. Gentle but very firm palpation generally is required to feel the movement of the trochanter with one hand, while rotating the leg internally and externally at the knee area with the other hand. This is not as precise a landmark as the other bony landmarks of the pelvis, but the prominence of the greater trochanter is at about the same level as the superior border of the symphysis. With practice, the greater trochanter can be used as a secondary landmark for abdominal positioning.
6. Symphysis pubis: The symphysis pubis is the anterior junction (joint) of the two pelvic bones. The most superior anterior portion of the pubis can be palpated when the patient is in a supine position. This landmark corresponds to the inferior margin of the abdomen. However, palpation of this area may be embarrassing to some patients. With practice, the level of the symphysis pubis or the lower margin of the abdomen can be identified by palpating the greater trochanter with reference to the iliac crest as being at the level of the center of the cassette or IR; this places the lower margin of the IR at the symphysis pubis.
7. Ischial tuberosity: This landmark can be used to determine the lower margin on a PA abdomen with the patient in a prone position. These two bony prominences, which can be palpated most easily on thin patients, bear most of the weight of the trunk when one is seated. The lower margins of the ischial tuberosities are about 1 to 4 cm ( inches) below or distal to the symphysis pubis. This landmark may be used for positioning a PA projection of the colon when the rectal area is to be included on the IR. However, this may be uncomfortable and embarrassing for the patient, and other landmarks can and should be used when possible.
inches) below or distal to the symphysis pubis. This landmark may be used for positioning a PA projection of the colon when the rectal area is to be included on the IR. However, this may be uncomfortable and embarrassing for the patient, and other landmarks can and should be used when possible.
Radiographic Positioning
Patient Preparation
Patient preparation for abdominal radiography includes removal of all clothing and any opaque objects in the area to be radiographed. The patient should wear a hospital gown with the opening and ties in the back (if this type of gown is used). Shoes and socks may remain on the feet. Generally, no patient instructions are required before the examination unless barium studies are also scheduled.
Breathing Instructions
A key factor in good abdominal radiography is the prevention of motion. Motion may result from voluntary movement, such as breathing, or from involuntary movement, such as peristaltic action of the bowel. The difference between these two types of motion is illustrated in Chapter 1. However, to prevent any potential motion in abdominal radiography, the shortest exposure time possible should be used.
A second way to prevent voluntary motion is by providing careful breathing instructions to the patient. Most abdominal radiographs are taken on expiration; the patient is instructed to “take in a deep breath—let it all out and hold it—don't breathe.” Before making the exposure, ensure that the patient is following instructions and that sufficient time has been allowed for all breathing movements to cease.
Abdominal radiographs are exposed on expiration, with the diaphragm in a superior position for better visualization of abdominal structures.
Image Markers
Correctly placed R and L markers and “up side” markers, such as short arrows, are used for erect and decubitus projections and should be visible without superimposing abdominal structures. Likewise, markers used for patient identification information in screen-film (analog) systems should be placed so that they do not interfere with pertinent anatomy and should be clear and legible. The anatomic side marker must correspond with the patient's left or right side of the body. The marker must be placed on the IR before exposure. It is not acceptable practice to indicate the side of the body either digitally or with a marking pen following the exposure.
Radiation Protection
Good radiation protection practices are especially important in abdominal radiography because of the proximity of the radiation-sensitive gonadal organs.
For abdominal radiographs of small patients, some side collimation to skin borders is possible if it does not cut off abdominal anatomy.
Collimation on the top and bottom for adults should be adjusted directly to the margins of the IR or film holder, allowing for divergence of the x-ray beam. Essential anatomy is collimated off on average-sized adults if extra collimation margins are shown on the top and bottom borders of a typical 35 × 43-cm (14 × 17-inch) abdominal image.
For abdominal radiographs, gonadal shields should be used for male patients, with the upper edge of the shield carefully placed at the pubic symphysis (Fig. 3-24). For female patients, gonadal shields should be used only when such shields do not obscure essential anatomy in the lower abdominopelvic region. Generally, the decision to shield female gonads on abdominal radiographs should be made by a physician to determine whether essential anatomy would be obscured. The top of an ovarian shield should be at or slightly above the level of ASIS, and the lower border should be at the symphysis pubis.
Exposure Factors
The principal exposure factors for abdominal radiographs are as follows:
Correctly exposed abdominal radiographs on an average-sized patient should faintly visualize the lateral borders of the psoas muscles, lower liver margin, kidney outlines, and lumbar vertebrae transverse processes. Moderate contrast is required with medium kV exposure to allow for visualization of various abdominal structures, including possible small semiopaque stones in the gallbladder or kidneys.
Pediatric Applications
Acute abdomen routines for pediatric patients generally include only a supine and one horizontal beam projection to show air-fluid levels. For patients younger than 2 or 3 years of age, a lateral decubitus may be difficult to obtain, and an AP erect abdomen with an immobilization device such as a Pigg-O-Stat (Modern Way Immobilizers, Inc, Clifton, Tennessee) is preferred (see Chapter 16).
Motion prevention is of utmost importance in pediatric patients, and short exposure times and higher speed film and screens are essential. Children younger than 12 or 13 years of age require a reduction in kV and mAs. Confirmed technique factors for children of various sizes and ages for the equipment that is being used should always be available to minimize repeats because of exposure errors.
Geriatric Applications
Older patients often require extra care and patience in explaining what is expected of them. Careful breathing instructions are essential, as is assistance in helping patients move into the required position. Extra radiolucent padding under the back and buttocks for thin patients and blankets to keep patients warm add greatly to their comfort on supine abdomen radiographic procedures.
Digital Imaging Considerations
The guidelines that should be followed with digital imaging (CR and DR) of the abdomen as described in this chapter are summarized as follows:
1. Four-sided collimation: Collimation to the body part being imaged and accurate centering are most important in digital imaging of the abdomen.
2. Exposure factors: It is important that the ALARA (as low as reasonably achievable) principle be followed in regard to patient exposure to radiation and the lowest exposure factors required to obtain a diagnostic image be used. This includes the highest kV and the lowest mAs that result in desirable image quality. For digital imaging, some increase in kV may be required compared with film-screen imaging.
3. Post-processing evaluation of exposure indicator: The exposure indicator on the final processed image must be checked to verify that the exposure factors used were in the correct range to ensure optimal quality with the least radiation to the patient.
Alternative Modalities
CT and MRI
CT and MRI (magnetic resonance imaging) are very useful in the evaluation and early diagnosis of small neoplasms involving abdominal organs such as the liver and pancreas. With the use of intravenous, iodinated contrast media, CT imaging can discriminate between a simple cyst and a solid neoplasm.
Both CT and MRI also provide valuable information in assessing the extent to which neoplasms have spread to surrounding tissues or organs. For example, MRI may be used to demonstrate blood vessels within neoplasms and to assess their relationship and involvement with surrounding organs without the need for contrast media injection.
MRI is also used to visualize the biliary and pancreatic ducts. Endoscopic retrograde cholangiopancreatography (ERCP), a fluoroscopic procedure in which a contrast medium is injected endoscopically, is used to visualize the biliary and pancreatic ducts as well (described in Chapter 19).
Sonography
Ultrasound has become the method of choice when the gallbladder is imaged for detection of gallstones (in the gallbladder or bile ducts). Ultrasound is of limited use in the evaluation of the hollow viscus of the GI tract for bowel obstruction or perforation, but along with CT, it is very useful in detecting and evaluating lesions or inflammation of soft tissue organs such as the liver or pancreas. Ultrasound is widely used, along with CT, for demonstrating abscesses, cysts, or tumors involving the kidneys, ureters, or bladder.
Ultrasound with graded compression, in combination with clinical evaluation, can be used successfully to diagnose acute appendicitis. CT can be used to demonstrate an abscess or thickened wall surrounding the inflamed appendix.*
Nuclear Medicine
Nuclear medicine is useful as a noninvasive means of evaluating GI motility and reflux as related to possible bowel obstruction. It is also useful for evaluation of lower GI bleeding.
With the injection of specific radionuclides, nuclear medicine imaging can be used to examine the entire liver and the major bile ducts and gallbladder.
Clinical Indications
A plain AP supine radiograph of the abdomen (KUB) generally is taken before contrast medium is introduced into the various abdominal organ systems for evaluation and diagnosis of diseases and conditions involving these systems. Clinical indications and terms specifically related to each of these systems are provided in Chapters 12 and 13.
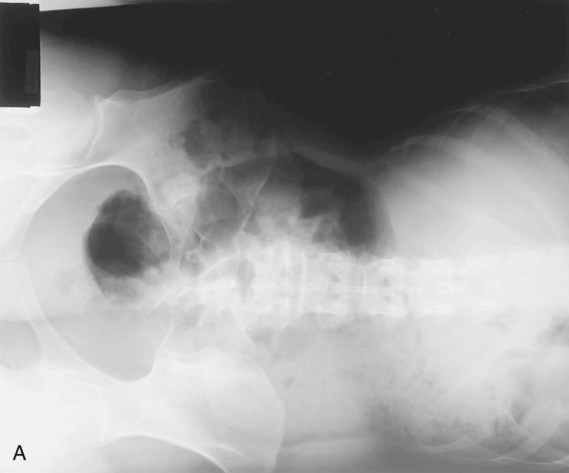
The acute abdomen series, as described in this chapter, is performed most commonly to evaluate and diagnose conditions or diseases related to bowel obstruction or perforation. This evaluation requires visualization of air-fluid levels and possible intraperitoneal “free” air with the use of horizontal beam erect or decubitus body positions. Following are terms and pathologic diseases or conditions that are related to the acute abdominal series examination.
Ascites (ah-si′-tez) is an abnormal accumulation of fluid in the peritoneal cavity of the abdomen. It generally is caused by long-standing (chronic) conditions such as cirrhosis of the liver or by metastatic disease to the peritoneal cavity.
Pneumoperitoneum refers to free air or gas in the peritoneal cavity. This is a serious condition for which surgery is required when it is caused by perforation of a gas-containing viscus, such as a gastric or duodenal ulcer. It also can be caused by trauma that penetrates the abdominal wall.
Small amounts of residual air may be evident radiographically 2 to 3 weeks after abdominal surgery. It is best demonstrated with a horizontal beam erect abdomen or chest radiograph, with which even a small amount of free air can be seen as it rises to the highest position under the diaphragm.
Dynamic (with power or force) or mechanical bowel obstruction is the complete or nearly complete blockage of the flow of intestinal contents. Causes include the following:
• Fibrous adhesions: The most common cause of mechanically based obstruction, in which a fibrous band of tissue interrelates with the intestine, creating a blockage.
• Crohn's (Kro-nz) disease: Also known as regional enteritis, a chronic inflammation of the intestinal wall that results in bowel obstruction in at least half of affected patients. The cause is unknown. Crohn's disease is most common in young adults and is characterized by loops of small intestine joined by fistulas or connected openings with adjacent loops of intestine. The two most common sites of intestinal involvement in Crohn's disease are the terminal ileum and proximal colon.*
• Intussusception: The telescoping of a section of bowel into another loop, which creates an obstruction. Intussusception is most common in the distal small intestine region (terminal ileum), and it is more common in children than in adults. This condition requires treatment within 48 hours to prevent necrosis (tissue death).
• Volvulus: The twisting of a loop of intestine, which creates an obstruction. Volvulus may require surgery for correction.
Ileus–nonmechanical bowel obstruction is categorized as adynamic (without power or force) ileus and most frequently is caused by peritonitis, or paralytic (paralysis) ileus, which is caused by a lack of intestinal motility. It occurs frequently in postoperative patients, usually 24 to 72 hours after abdominal surgery. In contrast to mechanical obstruction, it rarely leads to perforation, and the radiographic appearance is characterized by a large amount of air and fluid, with air-fluid levels visible in a greatly dilated small and large intestine and no visible distinct point of obstruction (in contrast to a mechanical obstruction).
Ulcerative colitis is a chronic disease involving inflammation of the colon that occurs primarily in young adults and most frequently involves the rectosigmoid region. In some cases, it becomes a very severe acute process, causing serious complications, such as a toxic megacolon (extreme dilation of a segment of colon) with potential perforation into the peritoneal cavity. Barium enema is strongly contraindicated with symptoms of toxic megacolon.
SUMMARY OF CLINICAL INDICATIONS
| CONDITION OR DISEASE | MOST COMMON RADIOGRAPHIC EXAMINATION | POSSIBLE RADIOGRAPHIC APPEARANCE | EXPOSURE FACTOR ADJUSTMENT* |
| Ascites | Acute abdomen series | General abdominal haziness | Increase, depending on severity (+ or + +) |
| Pneumoperitoneum (air in peritoneal cavity) | Acute abdomen series—erect chest or abdomen | Thin, crest-shaped radiolucency under dome of right hemidiaphragm on erect | Decrease (−) |
| Dynamic (Mechanical Bowel) Obstruction | |||
| Fibrous adhesions | Acute abdomen series | Distended loops of air-filled small intestine | Decrease, depending on severity of distention (− or − −) |
| Crohn's disease | Acute abdomen series | Distended loops of air-filled small intestine | Decrease, depending on severity of distention (− or − −) |
| Intussusception (most common in children) | Acute abdomen series | Air-filled “coiled spring” appearance | Decrease (−) |
| Volvulus (most common in sigmoid colon) | Acute abdomen series | Large amounts of air in sigmoid with tapered narrowing at site of volvulus | Slight decrease (−) |
| Ileus (nonmechanical obstruction), adynamic or paralytic | Acute abdomen series | Large amounts of air in entire dilated small and large intestine with air-fluid levels visualized | Decrease, depending on severity of distention (− or − −) |
| Ulcerative colitis | |||
| Severe case may lead to toxic megacolon and bowel perforation | Plain AP abdomen | Deep air-filled mucosal protrusions of colon wall, usually in rectosigmoid region | Decrease (−) |
| Acute abdomen series for possible free air (barium enema contraindicated) | Dilated loop of colon | Decrease (−) | |
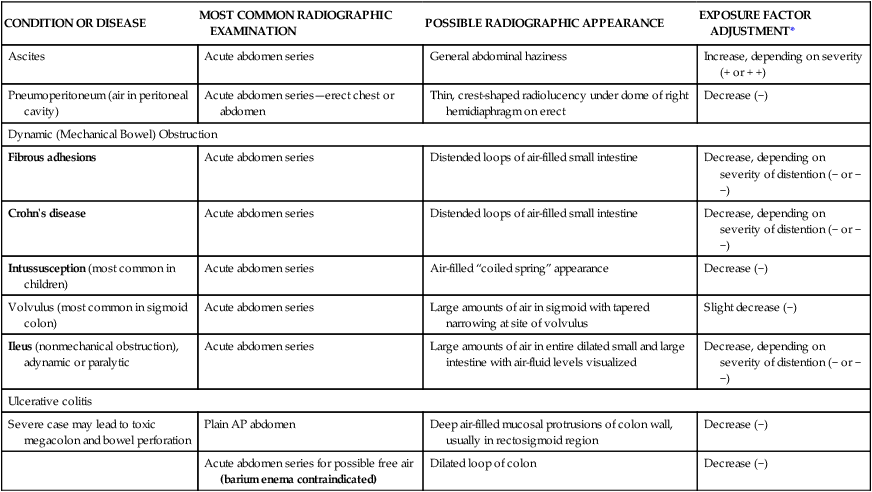
*Note: Automatic exposure control (AEC) systems are designed to correct exposure density (brightness) automatically for patient size variances and for these pathologic conditions. If they are calibrated correctly and are used as intended, manual adjustments generally are not needed when AEC systems are used. However, these exposure adjustments may be needed for more extreme cases, or for repeats, even with AEC. They are also important when manual exposure techniques are set, such as for tabletop or mobile examinations when AEC is not used.
Acute Abdomen Routine
In addition to the supine and erect or decubitus abdomen, the PA chest is included at some institutions to demonstrate free intraperitoneal air trapped under the diaphragm. Therefore, the three-way acute abdomen series (AP and erect abdomen plus PA chest) is presented as basic or routine. However, acute abdomen routines vary, depending on the institution. Students and technologists should determine the routine for their departments.
One reason the PA chest is commonly included in the three-way acute abdomen series is that the erect chest best visualizes free intraperitoneal air under the diaphragm. The erect abdomen also visualizes free air if the IR is centered high enough to include the diaphragm; however, the exposure technique for the chest best visualizes small amounts of this air if present.
AP Projection—supine Position: Abdomen
KUB
Technical Factors
• Minimum SID—40 inches (102 cm)
• IR size—35 × 43 cm (14 × 17 inches), lengthwise
• Analog and digital systems*—70 to 80 kV range
CR
Make exposure at end of expiration (allow about 1 second delay after expiration to allow involuntary motion of bowel to cease).
NOTES: A tall hyposthenic or asthenic patient may require two images placed lengthwise—one centered lower to include the symphysis pubis and the second centered high to include the upper abdomen and diaphragm.
PA Projection—prone Position: Abdomen
Clinical Indications
• Pathology of abdomen, including bowel obstruction, neoplasms, calcifications, ascites, and scout image for contrast medium studies of abdomen
NOTE: This projection is less desirable than AP if the kidneys are of primary interest because of the increased object image receptor distance (OID).
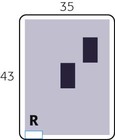
Lateral Decubitus Position (AP Projection): Abdomen
Clinical Indications
• Abdominal masses, air-fluid levels, and possible accumulations of intraperitoneal air are demonstrated.
• Small amounts of free intraperitoneal air are best demonstrated with chest technique on erect PA chest.
Important: Patient should be on his or her side a minimum of 5 minutes before exposure (to allow air to rise or abnormal fluids to accumulate); 10 to 20 minutes is preferred, if possible, for best visualization of potentially small amounts of intraperitoneal air.
Left lateral decubitus best visualizes free intraperitoneal air in the area of the liver in the right upper abdomen away from the gastric bubble.
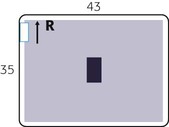
Patient Position
• Lateral recumbent on radiolucent pad, firmly against table or vertical grid device (with wheels on cart locked so as not to move away from table)
• Patient on firm surface, such as a cardiac or back board, positioned under the sheet to prevent sagging and anatomy cutoff
• Knees partially flexed, one on top of the other, to stabilize patient
Part Position 
• Adjust patient and cart so that center of IR and CR are approximately 2 inches (5 cm) above level of iliac crests (to include diaphragm). Proximal margin of IR is approximately at level of axilla.
• Ensure no rotation of pelvis or shoulders.
• Adjust height of IR to center midsagittal plane of patient to center of IR, but ensure that upside of abdomen is clearly included on the IR.
CR
• CR horizontal, directed to center of IR, at about 2 inches (5 cm) above level of iliac crest; use of a horizontal beam to demonstrate air-fluid levels and free intraperitoneal air
AP Projection—erect Position: Abdomen
CR
Exposure should be made at end of expiration.
Note: Patient should be upright a minimum of 5 minutes, but 10 to 20 minutes is desirable, if possible, before exposure for visualizing small amounts of intraperitoneal air. If a patient is too weak to maintain an erect position, a lateral decubitus should be taken. For hypersthenic patients, two crosswise IRs may be required to include the entire abdomen.
Dorsal Decubitus Position (Right or Left Lateral): Abdomen
Part Position 
• Adjust patient and cart so that center of IR and CR is at level of iliac crest (or 2 inches [5 cm] above iliac crest to include diaphragm).
• Ensure that no rotation of pelvis or shoulders exists (both ASIS should be the same distance from tabletop).
• Adjust height of IR to align midcoronal plane with centerline of IR.
Acute Abdominal Series: Acute Abdomen
Three-Way Abdomen: (1) AP Supine, (2) Erect (or Lateral Decubitus) Abdomen, (3) PA Chest
Specific Clinical Indications for Acute Abdominal Series
1. Ileus (nonmechanical small bowel obstruction) or mechanical ileus (obstruction of bowel from hernia, adhesions)
2. Ascites (abnormal fluid accumulation in abdomen)
3. Perforated hollow viscus (e.g., bowel or stomach, evident by free intraperitoneal air)
Take erect images first if patient comes to the department in an erect position.
CR to level of iliac crest on supine and approximately 5 cm (2 inches) above level of crest to include diaphragm on erect or decubitus
NOTES: Left lateral decubitus replaces erect position if the patient is too ill to stand.
For decubitus, patient should be upright or on the side for a minimum of 5 minutes before exposure (10 to 20 minutes preferred) to demonstrate potential small amounts of intraperitoneal air.
Radiographs for Critique
Each abdominal radiograph demonstrates at least one repeatable error. These as well as other radiographs for critique are available as part of the accompanying audiovisuals. Together, these tools provide a basis for classroom or positioning laboratory discussion on radiographic critique.
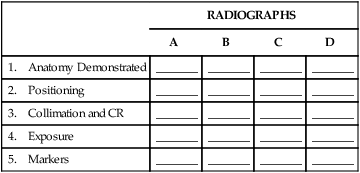
See whether you can critique each of these four radiographs based on the categories as described in the textbook and as outlined on the right. As a starting critique exercise, place a check in each category that demonstrates a repeatable error for that radiograph.
Answers are provided in the Appendix at the end of this textbook.
| RADIOGRAPHS | ||||
| A | B | C | D | |
| 1. Anatomy Demonstrated | _______ | _______ | _______ | _______ |
| 2. Positioning | _______ | _______ | _______ | _______ |
| 3. Collimation and CR | _______ | _______ | _______ | _______ |
| 4. Exposure | _______ | _______ | _______ | _______ |
| 5. Markers | _______ | _______ | _______ | _______ |
















 of ileum
of ileum of jejunum
of jejunum