CHAPTER 44 Community-based care
At the completion of this chapter and with further reading, students should be able to:
• Explain the role of public health in community-based care
• Describe the role of the community health nurse
• Identify the models of care used in community health practice
• Explain the issues that affect nurses who are involved in home care
• Describe the common competencies and skills of the community health nurse
There has been a gradual change in Australian and New Zealand healthcare policies with an increased focus on primary healthcare in the community. These changes have occurred as a result of public health policies aimed at maintaining health and preventing illness, a consumer push for more healthcare options, earlier discharge from acute hospitals and containment of costs.
This chapter discusses the diverse role of the nurse who works in the community in Australia and New Zealand. It also explains the principles of primary healthcare and how they are practised in the context of the public health paradigm. Community health and healing are also explored. The factors that impact the health of individuals, families and communities are discussed. The role, skills and competencies of the community health nurse are broadly examined. Reference is made to the literature and research on the topic, in deference to evidence-based principles.
My daughter is 63 years of age and has been diagnosed with dementia. She used to help me with my housework and gardening. She never married and has worked for years for a local factory. Her condition has worsened and she had to leave work. A month ago she moved in with me. Now I find myself having to take care of her. She needs help with nearly everything and wanders about the house at night. I am 85 years old, almost legally blind and have severe osteoarthritis. I never thought I would be in this situation, having people come in to my house to look after one of my own.
COMMUNITY HEALTHCARE
Community healthcare has been changing. More attention is directed to the provision of disease-recovery nursing care for transitioning clients as they move out of the hospital environment and into the community context. Early intervention measures for people living with chronic conditions are focused on preventing re-admission into the acute healthcare system (van Loon 2008a). Community nurses increasingly assist clients and their carers/families to self-manage their health situation within their home environment and thus require a person-centred approach to care (van Loon 2008b).
A social view of health considers other determinants of health such as economic and social factors (Fleming & Parker 2009). The social determinants of health have been recognised and asserted by the World Health Organization (WHO 1978). ‘Health for all’, a philosophy developed by the WHO, has been promoted in many countries (WHO 1978). These philosophies impact on the provision of care for people in the community.
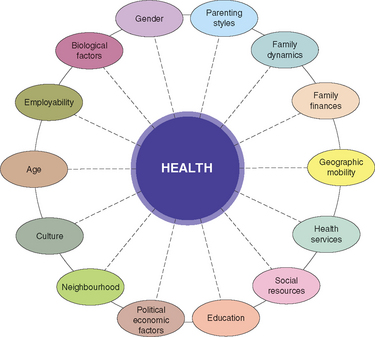
Illness is influenced by how an individual experiences medically-diagnosed pathophysiology which may have characteristic signs and symptoms (McMurray & Clendon 2011). The interactions between factors affecting health are illustrated in Figure 44.1.
According to Moore (2009), the ‘extension of health services beyond the medical treatment model to a social model, and beyond the institutional to the community context, has seen “patients” now described also by terms used in social settings as “clients”’. Service users include the client and their primary carers who access a service with the client’s consent. In Australia, community-based services are moving from being population-based to focusing on specific at-risk sub-groups (Chapman et al 2008).
The health of a community
Baisch (2009) suggests that ‘community health is grounded in philosophical beliefs of social justice and empowerment … and … is achieved through participatory, community development processes based on ecological models that address broad determinants of health’. Community nurses are critical in helping individuals, families and communities become whole by acting as a conduit or facilitator for positive change. This concept is illustrated in the model for community healing in Figure 44.2.
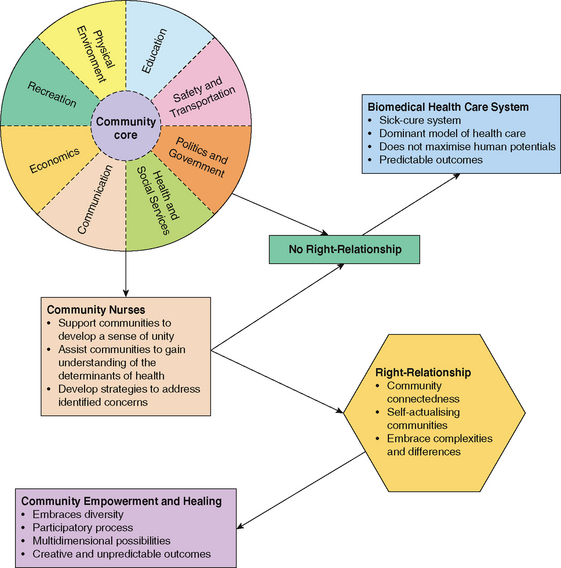
Figure 44.2 Model for community healing
(Francis K, Chapman Y, Hoare K, Mills J, Community as Partner: Theory and Practice in Nursing, Lippincott Williams & Wilkins, NSW, 2008. Reproduced with permission from Wolters Kluwer Health via Rightslink)
According to Maddock (2008) factors which impact on the context of community care include:
• The changing and diverse complexity of illness and disease comorbidities that people experience as they live longer
• The increasing number of people who want to be cared for in their homes
• Healthcare delivery that is becoming more complex with multiple services that require multidisciplinary team approaches to care provision and complex policy and strategic guidance to ensure quality and safe outcomes.
People with chronic illness face many challenges. Helping a patient or client to be more empowered is a role of any nurse. Empowerment is beneficial as it enhances a person’s capacity to develop personal resources to manage their particular situation.
Public health
Public health philosophy strives to reorientate health systems towards health and wellness rather than disease and illness. Philosophically, the values for public health are based on notions of health for all, social justice and equity (Keleher 2009).
The Public Health Association of Australia vision for a healthy population is ‘healthy people living in a healthy society and a sustaining environment, improving and promoting health for all’ (PHAA 2011). Fleming and Parker (2009) suggest that ‘public health is about preventing disease, illness and injury, together with promoting the quality of life of human populations. This is a very complex process and requires the committed skills and expertise of many different professional disciplines’. These authors have summarised the roles and functions of the public health workforce as:
• Understanding the context for public health activity and its role and functions
• Providing clarity around political impacts on public health
• Able to apply a range of methodological approaches to understand data
• Having a theoretical understanding of the disciplines that underpin public health and their contribution to strategy selection
• Understanding a range of skills around surveillance, prevention, promotion and restoration of the population’s health
• Developing and analysing policy
• Planning, implementation and evaluation
• Using evidence-based practice
• Using advocacy, communication and negotiation skills
• Working intersectorally and with multidisciplinary groups
• Demonstrating ethical practice (Fleming & Parker 2009).
Community health nursing and primary healthcare
Community-based nursing services comprise continuing nursing care, which may be preventive, curative, rehabilitative, supportive or palliative. Community health nursing focuses on promoting and preserving the health of population groups (Hales 2010a). Community nurses have a role in promoting community health through primary healthcare. Primary healthcare is a model of community-based health service delivery that is part of the publicly funded health system in Australia. Community nursing in Australia draws much of its revenue from a complex mix of health, community, veterans’ and aged care programs which are funded by different levels and arms of government (Taylor 2008).
Primary healthcare reflects care that transitions health system boundaries and focuses attention on community needs (van Loon 2008b). Primary healthcare takes a client-centred approach which minimises the potential for harm, because the consumer’s values and preferred approaches to health are respected (Eckermann et al 2010). The outcomes of primary healthcare, apart from better health, should be empowerment and self-reliance. Primary healthcare every day, according to Eckermann et al (2010), should be holistic in its approach. This involves:
• High levels of trust and community participation
• Shifting the power and control to those whose health is at stake.
Community-based healthcare is a primary healthcare system that provides holistic health-related services within the context of people’s daily lives, and is directed towards a specific group within the geographic neighbourhood. To be effective it needs to:
• Be flexible in responding to the care needs that individuals and families identify
• Promote care between and among healthcare agencies through improved communication mechanisms
• Provide appropriate support for family caregivers, and
• Be affordable (Hales 2010a).
A range of services delivered in community-based settings in Victoria are designed to provide early intervention to maximise health and wellbeing outcomes and prevent or slow the progression of ill health. These services are funded by the state and federal governments, private services and volunteer-led and community-based organisations and they play an important role in meeting the needs of people with, or at risk of, poorer health (Department of Health Victoria 2012). Australia also has the not-for-profit home nursing organisation, the Royal District Nursing Service (RDNS), which delivers general and specialised nursing and health care in clients’ homes, and which is ‘committed to improving and maintaining our clients’ quality of life and independence by providing tailored care to meet their individual needs’ (RDNS).
In Aotearoa (New Zealand), the primary health nurse is a registered nurse with knowledge and expertise in primary healthcare practice. A primary healthcare nurse works autonomously and collaboratively to promote, improve and restore health. Primary healthcare nursing encompasses population health, health promotion, disease prevention, wellness care, first point of contact care and disease management across the life span. The setting and the ethnic and cultural grouping of the people determine models of practice. Partnerships with people—individuals, whānau, communities and populations—to achieve the shared goal of health for all is central to primary healthcare nursing (Ministry of Health 2005).
According to Woods (2010), recent health reform in Australia which seeks to curtail the burden of chronic disease by adopting a primary healthcare approach challenges community health nurses to demonstrate their understanding and capacity to practise according to primary healthcare principles. Woods suggests that there is a need to formulate an Australian model for community nurses and national competencies through a national professional body. Community health nursing competencies are discussed later in this chapter.
COMMUNITY HEALTH NURSE ROLE
Competencies integral for community health nurse care is discussed later in this chapter; however, the following community health nurse competency statement from Queensland Health (2009) encapsulates the role of the community health nurse in Australia.
The community health nurse is a professional who delivers evidence-based nursing care to individuals, families, significant others and defined communities, underpinned by the principles of primary healthcare and health promotion, supporting self-reliance in recovery from illness, enhancement of health or management of chronic and terminal conditions, in a setting which is optimal for the client or community.
The Community Nurses Special Interest Group and Department of Health in Western Australia (2001) developed the following occupational statement about the community health nurse:
Community health nurses practise primary healthcare in a diverse range of settings. They provide continuous monitoring of the health status of communities and respond to episodic health needs. Community health nurses need to be creative, adaptable and responsive to a variety of norms, cultures and value systems whether they are working with individuals, families or community groups.
In New Zealand, community health nurses provide overall care to the population in the form of Plunket Nurses and Tamariki Ora Nurses for 0–5 year olds, public health nurses for school-age children and district nurses for home care (Chapman et al 2008). In New Zealand people enrol with a primary health organisation (PHO) which provides primary healthcare services in local communities. Primary health organisations are not-for-profit organisations funded through district health boards. This model of care removes barriers and creates a continuous health service by the provision of primary (community-based) and secondary (mostly hospital-based) health professionals working together collaboratively and with patients to provide effective healthcare (Ministry of Health 2011).
Teamwork in community care
Community nurses base their practice on the concepts of partnership, collaboration and empowerment (Francis et al 2008). Partnerships between community members and healthcare professionals are critical for collaborative decisions that promote awareness and understanding of a community’s health needs (Chapman et al 2008).
A study by O’Neill and Cowman (2008) investigated community nurses’ understanding of an interdisciplinary team-based approach to primary care using a qualitative research design. Their conclusions were that nurses can contribute significantly to the re-orientation and development of primary care services. Collective team efforts enhance patient care and effective teamwork requires a greater understanding of group processes and team development.
As well as community nurses there are many other healthcare workers who provide community-based healthcare, both in centres and in people’s homes. Some of these include occupational therapists, physiotherapists, social workers, dietitians, general practitioners, home care workers, volunteers, personal carers and home maintenance workers. Collaborative working relationships between healthcare workers, institutions and agencies are essential for providing coordinated care for clients in the community. Competencies identified as being vital for collaboration include effective communication skills, mutual respect and trust and a team decision-making process with shared responsibility for the outcome (Hales 2010a).
Home care
The terms used to describe the provision of nursing care in clients’ homes varies but can include domiciliary nursing, ambulatory care, community health nursing, district nursing, hospital in the home and home care. Regardless of the title, home care requires specialised skill sets of advanced nursing care as nurses may work in an environment which necessitates that they work independently, and includes coordination of services, provision of direct care, client assessment, consulting, education, administration and research activities (Hales 2010b).
The registered nurse working in home care may also be responsible for the direction and supervision of unregulated care workers. The role of the home health nurse includes being: advocate, carer, educator, case manager or coordinator. The home care nurse also needs to consider other perspectives related to working in the client’s environment: client safety, legal and ethical issues, infection prevention and control and nurse safety (Hales 2010b).
MODELS OF CARE IN COMMUNITY HEALTH
Various approaches are emerging to address community health, such as integrated health, community initiatives, coalitions, managed care, case management and outreach programs (Hales 2010a). The following is a summary of these models of care:
• Integrated healthcare system—makes all levels of care—primary, secondary and tertiary—available in an integrated form
• Community initiatives—members of the community establishing health priorities, goals and actions to achieve goals
• Community coalitions—individuals and groups having a shared purpose of improving community health
• Managed care—multidisciplinary teams working together to provide cost-effective and quality healthcare across the care continuum with the managed care organisation liaising between client, provider and payer
• Case management—tracks clients’ needs, and helps them access services through a variety of care settings to ensure continuity. Case management is defined as a collaborative process of assessment, planning, facilitation and advocacy for options and services to meet an individual’s health needs through communication and available resources to promote quality cost-effective outcomes. It is a dominant model used in community mental healthcare
• Outreach programs—link people who have difficulty accessing services with the formal healthcare system
• Solution-focused nursing—considers the sociocultural as well as the individual world of a client with nurses being proactive in promoting health and wellbeing rather than reacting to palliate symptoms (Aged and Community Care Services Australia & Case Management Society of Australia 2006; Henderson & Walter 2009; Hales 2010a; McAllister 2010).
Clinical Scenario Box 44.1
Effectiveness of a new community nursing model of care—research
The researchers Edwards and colleagues undertook a study to determine the effectiveness of a new community nursing model of care on quality of life, morale, depression, self-esteem, social support, healing, pain and functional ability of clients with chronic venous leg ulcers. A randomised controlled trial was used with participants randomised to either a Leg Club model of care which emphasises socialisation and peer support, or the traditional community nursing model of home visits by a registered nurse. Participants in the Leg Club model demonstrated significantly improved outcomes in quality of life, self-esteem, healing, pain and functional ability.
In New Zealand, other models used in community health include rural nurse specialist, nurse-led youth health clinic, mental health primary care liaison nurse, community care nurse-led acute care team, primary healthcare neighbourhood nurse and mobile community ear clinic (Ministry of Health 2005).
ISSUES FOR COMMUNITY HEALTH NURSES IN HOME CARE
Isolation is an issue for some community nurses. Rural and remote community nurses work in diverse settings, often in isolated practice in resource-poor environments with their practice influenced by the geography of the community, issues of transportation, communication and personal safety (Francis & Chapman 2008).
In addition to incident management and reporting, the community nurse has mandatory reporting requirements as part of their duty of care to the client. These requirements include reporting all:
• Suspected incidences of child abuse and neglect
• Suspected incidences of elder abuse
• Cases of inappropriate use and storage of firearms
• Unexpected deaths (Maddock & Trowbridge 2008).
Giving culturally safe care is also an integral requirement in community healthcare. Cultural safety is an outcome experienced by the person receiving care and is described as ‘the effective nursing of a person/family from another culture by a nurse who has undertaken a process of reflection on own cultural identity and recognises the impact of the nurse’s culture on own nursing practice’ (Te Kaunihera Tapuhi o Aotearoa Nursing Council of New Zealand). Culturally safe nurses accommodate and respect a diverse range of views on health and healing (Stein-Parbury 2009).
Clinical Scenario Box 44.2
Program snapshot: Refugee Health Nurse Program, Victoria
The Refugee Health Nurse Program provides a coordinated approach using community nurses who have expertise in working with culturally and linguistically diverse and marginalised communities. These nurses work in community health services with high refugee populations. The program has three aims: increase refugee access to primary health services; improve the response of health services to refugees’ needs; enable individuals, families and refugee communities to improve their health and wellbeing.
Aboriginal health workers are vital in Aboriginal health services as they are the most appropriate people to deal with their own people and help bridge the gap with non-Aboriginal health professionals in their community (Eckermann et al 2010). As stated by Eckermann and colleagues (2010), ‘some Aboriginal people maintain that the cornerstones of their culture are lore, law, language and land, which forms the basis of their identity’.
Personal safety is an important consideration for the nurse who makes home visits. Strategies to eliminate or manage risks must be implemented. Risks include: working as a sole practitioner; being ‘on-call’ in remote communities; the gender bias (most community health nurses are female); dealing with hazards in the home such as obstructions and debris; aggressive dogs; having to use mobile telephones especially in rural Australia; dealing with angry and aggressive clients and domestic violence; driving; needlestick incidents; and working alone (Henderson 2010; Newman & Berens 2010).
Skills and competencies of the community nurse
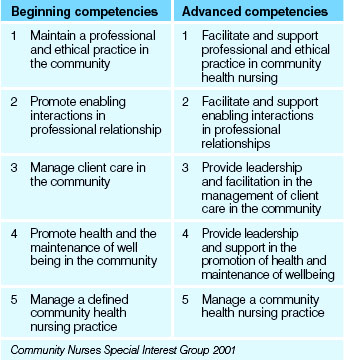
The competencies of community health nursing that make it a unique specialty are actually attributes that are desirable in nursing practice, regardless of the setting (DeBrew & Lutz 2010). Community nurses must be compliant with the legal and regulatory requirements of the jurisdictions in which they practise. Enrolled nurses who work in community health must work within their scope of practice under the supervision of the registered nurse. The Community Nurses Special Interest Group and Department of Health, Western Australia (2001) developed competency standards for the community health nurse (see Table 44.1). They make the distinction between the competencies of the beginning practitioner and the practitioner with advanced skills.
Queensland Health with the Institute of Primary Health & Ambulatory Care and the Institute of Women’s & Children’s Health, Townsville Health Service District (2009) developed community health nursing competency and skills checklists designed to support the transition of nurses into community health nursing. These competency and skills checklists were derived by reviewing a number of services, categorising and summarising competency, competency units and skills and consulting with stakeholders, A refined list of competencies emerged to reflect community nursing in the Townsville Health Service District. Standards and competencies that exist from national, state and organisational levels take precedence—with the competency and skills framework intended to fill a gap and add refinement to a specific area of nursing practice. Five competency units and 17 skills are described (see Clinical Interest Box 44.1).
CLINICAL INTEREST BOX 44.1 Community health nurse competencies and skills
(Copyright Townsville Health Service District, Queensland Health 2009)
| Competency Unit 1 Community health appraisal and screening | |
| Skill 1 | Surveillance |
| Skill 2 | Disease and other health event investigation |
| Skill 3 | Outreach |
| Skill 4 | Screening |
| Skill 5 | Case finding |
| Competency Unit 2 Healthcare delivery | |
| Skill 6 | Referral and follow-up |
| Skill 7 | Case management |
| Skill 8 | Delegated functions (assessment, nursing diagnosis, planning, implementation, evaluation) |
| Competency Unit 3 Education and support | |
| Skill 9 | Health teaching |
| Skill 10 | Counselling |
| Skill 11 | Consultation |
| Competency Unit 4 Community development | |
| Skill 12 | Collaboration |
| Skill 13 | Coalition building |
| Skill 14 | Community organising |
| Competency Unit 5 Political action | |
| Skill 15 | Advocacy |
| Skill 16 | Social marketing |
| Skill 17 | Policy development and policy enforcement |
Generic competencies for public health in Aotearoa
A coalition of public health disciplines collaborated with the Public Health Association of New Zealand to determine generic competencies for public health which would assist with keeping people healthy and improving the health of populations (Public Health Association of New Zealand). Generic competencies define the minimum level of ability in areas of public health to guide discipline-specific and specialist practitioners who have advanced and expert levels of competencies. There are twelve topic areas which each comprise a set of competency statements with accompanying performance requirements. The topic areas are organised into two main descriptors: public health knowledge (five topics) and public health practice (seven topics) (see Table 44.2).
THE NURSING PROCESS AND COMMUNITY NURSING
The nursing process is used in community health and community-based nursing, as in many other areas of nursing care. As a logical framework for nursing care, the steps of assessment, nursing identification of issues, planning, implementation and evaluation are particularly useful for clients receiving care in the community. The nursing process is instructive in providing a formalised and documented problem-solving strategy (Luxford & Avery 2010). Using tools designed to help in decision making, such as the nursing practice flowchart developed by the Australian Nursing and Midwifery Council in 2007 and now available from the Nursing and Midwifery Board of Australia (NMBA), is recommended (NMBA 2010). Nurses in community care also use critical thinking skills to resolve issues, manage risks and make appropriate referrals (Luxford & Avery 2010). Community nurses need to reflect at the analytical and personal levels about their clients and the larger community, and also about themselves and their own role and function in the community they serve.
Nurses working in the home setting have the opportunity to observe clients in their own environment, enabling a more holistic assessment (see Clinical Interest Box 44.2). The focus on client choice and autonomy means that clients and families are encouraged to participate actively in the nursing process. As a result, the client and their family may be more proactive in the implementation phase, significantly contributing to the success of the care plan as they work towards their own goals.
CLINICAL INTEREST BOX 44.2
Rebecca is an enrolled nurse who works in a community-based nursing service. In a typical day Rebecca sees 10–15 clients in their homes. The activities she is involved in include hygiene assistance, wound care, monitoring blood glucose levels and assisting clients with the application of compression stockings.
Rebecca is responsible for organising her own day, which starts at the office base with a handover and ends there with time allowed to debrief with the coordinator and other staff. Rebecca’s days are not often the same and she finds herself regularly involved in providing education and emotional support to clients and carers, as well as information on other services that are available in the community.
Summary
There has been an increased focus on preventative care and wellbeing promotion in recent years. Community care is increasingly helping clients transition from acute services to care and enabling services in the community. The philosophy of public healthcare and the practice of primary healthcare underpin the delivery of community health services in Australia and New Zealand. Integral to this service is empowering communities to become healthy while addressing the non-traditional determinants of health such as social and economic factors. Community nurses have particular competencies and skills which are now being formally recognised. Nurses providing care in the community, and in particular home care, have specific issues which impact on their practice. The nursing process informs care delivery along with applying critical thinking strategies and decision-making tools to assist to manage risks and resolve problems. Several case studies illustrate particular aspects of community-based healthcare.
1. Mr Jobe, 32, is homeless and spends most nights sleeping in the park. He has asthma and chronic bronchitis. Sometimes he drops in at the local charity food kitchen. He likes to pay his way and usually offers to help with the clean-up. Recently he has been short of breath. What interventions would you consider to improve Mr Jobe’s health and quality of life?
2. Consider the community health nurse competencies described in this chapter. Which of the competencies would be within the scope of practice of the enrolled nurse?
1. What is meant by a social view of health?
2. What are the philosophical values of public health?
3. List some models of care used in community health.
4. Define community health nurse as an occupation.
5. What are some of the issues community nurses face in home care?
References and Recommended Reading
Aged and Community Care Services Australia & Case Management Society of Australia. Case Management and Community Care: A Discussion Paper. Online. Available: www.cmsa.org.au, 2006.
Baisch M. Community health: an evolutionary concept analysis. Journal of Advanced Nursing. 2009;65(11):2264–2276.
Chapman Y, Francis K, Hoare K. Building healthy and healing communities. In: Francis K, Chapman Y, Hoare K, et al. Community as Partner: Theory and Practice in Nursing. Broadway, NSW: Wolters Kluwer Health/Lippincott Williams & Wilkins, 2008. Australia and New Zealand edn
Community Nurses Special Interest Group. Competency Standards for the Community Health Nurse, 2nd edn. Western Australia: Department of Health, 2001.
DeBrew J, Lutz J. Looking through a community lens: innovative ways to integrate community health nursing competencies into all settings of care. Issues in Mental Health Nursing. 2010;31:64–67.
Department of Health (Victoria). Primary and Community Health. Online. Available: www.health.vic.gov.au, 2012.
Department of Human Services. Community Health Services—Program Snapshots. Melbourne: State Government of Victoria, 2005.
Eckermann A, Dowd T, Chong E, et al. Binan Goonj: Bridging Cultures in Aboriginal Health, 3rd edn. Sydney: Elsevier, 2010.
Edgecombe G. Maternal and child health. In: Kralik D, van A. Community Nursing in Australia. Oxford: Blackwell Publishing, 2008.
Edwards H, Courtney M, Finlayson K, et al. A randomized controlled trial of a community nursing intervention: improved quality of life and healing for clients with chronic leg ulcers. Journal of Clinical Nursing. 2009;18:1541–1549.
Fleming M, Parker E. Introduction to Public Health. Sydney: Elsevier, 2009.
Francis K, Chapman Y, Hoare K, et al. Primary health care. In: Francis K, Chapman Y, Hoare K, et al. Community as Partner: Theory and Practice in Nursing, Australia and New Zealand edn. Broadway, NSW: Wolters Kluwer Health/Lippincott Williams & Wilkins, 2008.
Francis K, Chapman Y. Rural and remote community nursing. In: Kralik D, van Loon A. Community Nursing in Australia. Oxford: Blackwell Publishing, 2008.
Hales M, Community health nursing. Berman A, Snyder S, Kozier B, et al, eds. Kozier and Erb’s Fundamentals of Nursing, Vol 1. Pearson, Frenchs Forest, NSW, 2010.
Hales M, Home care. Berman A, Snyder S, Kozier B, et al, eds. Kozier and Erb’s Fundamentals of Nursing, Vol 1. Frenchs Forest, NSW: Pearson, 2010.
Henderson S. Community child health (CCH) nurses’ experience of home visits for new mothers: A quality improvement project. Contemporary Nurse. 2009–2010;34(1):66–76.
Henderson J, Walter B. Organising care for the mentally ill in Australia. In: Willis E, Reynolds L, Keleher H. Understanding the Australian Health Care System. Sydney: Elsevier, 2009.
Jackson D, Edgecombe G. Caring for children and adolescents in the community. In: Kralik D, van Loon A. Community Nursing in Australia. Oxford: Blackwell Publishing, 2008. (2008)
Keleher H. Public health. In: Willis E, Reynolds L, Keleher H. Understanding the Australian Health Care System. Sydney: Elsevier, 2009.
Luxford Y, Avery A, Critical thinking and the nursing process. Berman A, Snyder S, Kozier B, et al, eds. Kozier and Erb’s Fundamentals of Nursing, Vol 1. Pearson, Frenchs Forest, NSW, 2010.
Maddock A. Clinical governance. In: Kralik D, Trowbridge K, Smith J. A Practice Manual for Community Nursing in Australia. UK: Wiley-Blackwell, 2008.
Maddock A, Trowbridge K. Incident management and mandatory reporting. In: Kralik D, Trowbridge K, Smith J. A Practice Manual for Community Nursing in Australia. UK: Wiley-Blackwell, 2008.
Martin-McDonald K. Empowering partnerships: Nurses and those they care for. In: Rogers-Clark C, Martin-McDonald K, McCarthy A. Living with Illness: Psychosocial Challenges for Nursing. Sydney: Elsevier, 2005.
McAllister M. Solution focused nursing: A fitting model for mental health nurses working in a public health paradigm. Contemporary Nurse. 2010;34(2):149–157.
McMurray A, Clendon J. Community Health and Wellness: Primary Health Care in Practice, 4th edn. Sydney: Elsevier, 2011.
Ministry of Health. Evolving Models of Primary Health Care Nursing Practice. Wellington: Ministry of Health, 2005.
Ministry of Health. Better, Sooner, More Convenient Health Care in the Community. Wellington: Ministry of Health, 2011.
Moore E. Systems diversity: definitions and archetypes. In: Moore E, ed. Case Management for Community Practice. Melbourne: Oxford University Press, 2009.
Newman B, Berens H. Occupational health-related experiences in rural Tasmania. British Journal of Community Nursing. 2010;15(7):355–359.
Nursing and Midwifery Board of Australia. Codes and Guidelines. Online. Available www.nursingmidwiferyboard.gov.au/Codes-and-Guidelines.aspx, 2010.
O’Neill M, Cowman S. Partners in care: investigating community nurses’ understanding of an interdisciplinary team-based approach to primary care. Journal of Clinical Nursing. 2008;17:3004–3011.
Public Health Association Australia. Annual Report 2010–2011 of the Public Health Association of Australia Incorporated. Online. Available: www.phaa.net.au, 2011.
Public Health Association of New Zealand. Generic Competencies for Public Health in Aotearoa–New Zealand. Public Health Association of New Zealand, 2007.
Queensland Health. Community Health Nursing Competency and Skills. Townsville Health Service District, Queensland Health, 2009.
Royal District Nursing Service (RDNS). (nd) What we do. Online. Available: www.rdns.com.au.
Stein-Parbury J. Patient and Person: Interpersonal Skills in Nursing, 4th edn. Sydney: Elsevier, 2009.
Taylor B. Economic and political context of Australian community nursing. In: Kralik D, van Loon A. Community Nursing in Australia. Oxford: Blackwell Publishing, 2008.
van Loon A. The changing professional role of community nurses. In: Kralik D, van Loon A. Community Nursing in Australia. Oxford: Blackwell Publishing, 2008.
van Loon A. Approaches to community nursing care. In: Kralik D, van Loon A. Community Nursing in Australia. Oxford: Blackwell Publishing, 2008.
Woods M. Public health intervention model: impact on Australian community and mental health nursing students’ practice. International Journal of Nursing Education Scholarship. 2010;7(1):1–19. Article 17
World Health Organization (WHO). Declaration of Alma-Ata. Online. Available www.who.int/publications/almaata_declaration_en.pdf, 1978.
Department of Health Victoria, Primary and Community Health, http://health.vic.gov.au/communityhealth/about_chs.htm.
Plunket, www.plunket.org.nz.
Public Health Association of Australia, www.phaa.net.au.
Public Health Association of New Zealand, www.pha.org.nz.
Queensland Health, www.health.qld.gov.au.
Royal District Nursing Service, www.rdns.com.au.
Te Kaunihera Tapuhi o Aotearoa Nursing Council of New Zealand. www.nursingcouncil.org.nz.