| Sequence |
Selected photos |
| Many of the assessments can be done with the person sitting in a chair. For some you may need to assist the person into bed. Make sure that the bed is at a comfortable level for the physical examination. |
|
| GENERAL SURVEY |
|
| On your way into the room, verify that any necessary markers or flags are in place at the doorway regarding such conditions as isolation precautions, latex allergies or fall precautions. Once in the room, introduce yourself as the patient’s nurse for the shift. Make direct eye contact and do not allow yourself to be distracted by IV pumps or other equipment as you ask how they are feeling, how they spent the previous shift and whether they are currently having any pain or discomfort (including chest pain). Refer to what you have heard from the previous shift in the process of your own questioning—this alleviates the person’s frustration at answering the same questions every time a new staff member walks through the door. |
 |
Offer water (if the patient is not nil orally) as a courtesy and note the data this gives you: the person’s ability to hear, follow directions and, especially, ability to swallow. As you collect this and subsequent history, note data on the general appearance. Complete your initial overview by verifying that the correct name band has been applied to the wrist.
At this time conduct a general check of equipment attached to the patient. Check:
• The IV bag/s against the medical orders including the solution type and rate of infusion
• The IV site for redness and swelling
• Oxygen/suction administration and equipment
• Drains/catheters and drainage equipment/containers
• Location and function of emergency equipment.
|
 |
| GENERAL APPEARANCE |
|
1 Facial expression, appropriate to the situation
2 Body position, relaxed and comfortable or tense, in pain
3 Level of consciousness, alert and oriented, attentive to your questions, responds appropriately
4 Skin colour, mucous membrane colour
5 Nutritional status, weight appears in healthy range, even fat distribution, hydration appears healthy
6 Speech: articulation clear and understandable, pattern fluent and even, content appropriate
7 Hearing, responses and facial expression consistent with what you have said
8 Personal hygiene, ability to attend to hair, make-up, shaving
|
 |
| MEASUREMENT |
|
Done at prescribed time intervals—note changes from previous assessment or trends in the assessment findings.
1 Temperature
2 Pulse
3 Respiration
4 Blood pressure (note to avoid an arm because of surgery or venous access on that side)
5 Pulse oximetry
6 Rate pain level on 1 to 10 scale, and note ability to tolerate pain
7 If pain medication given, note response in 15 minutes for IV administration to 1 hour for oral administration.
|
 |
| MENTAL STATUS |
|
Commonly performed postsurgery/anaesthetic on return to ward; following head injury, stroke or neurological surgery or after any change in conscious state; where there is a history of mental illness, confusion or delirium.
1 General appearance and demeanour
2 Behaviour
3 Thought processes and perceptions
|
|
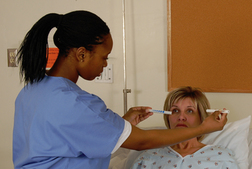
| NEUROLOGICAL AND SENSORY FUNCTION |
|
Commonly performed postsurgery/anaesthetic on return to ward; following head injury, stroke or neurological surgery or after any change in conscious state. This may involve the recording of frequent assessments using the Glasgow Coma Scale on a neurological assessment chart.
1 Eyes open spontaneously to name
2 Motor response
3 Verbal response
4 Pupil size in mm and reaction, R and L
5 Muscle strength, R and L upper
6 Muscle strength, R and L lower
7 Any ptosis, facial droop
8 Sensation
9 Communication (including vision and hearing)
10 Ability to swallow
|
 |
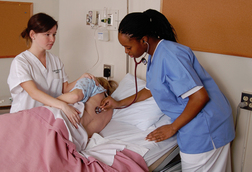
| RESPIRATORY FUNCTION |
|
Commonly performed postsurgery/anaesthetic on return to ward; following chest surgery or trauma; in the person with a chest infection, asthma or chronic lung disease; or in the person who is at risk of ineffective airway clearance.
1 Oxygen by mask, nasal prongs, check fitting
2 Note FIo2
3 Respiratory effort
4 Auscultate breath sounds comparing side to side: Posterior lobes: left upper, right upper, left lower, right lower
Note: if not able to sit up, have another nurse hold patient side to side Anterior lobes: right upper, left upper, right middle and lower, left lower
5 Cough and deep breath; any mucus? Check colour and amount.
|

 |
| CARDIOVASCULAR FUNCTION |
|
Commonly performed postsurgery/anaesthetic on return to ward; in the person with chest pain or myocardial infarction; postcardiac or vascular surgery; vascular assessments are also performed post orthopaedic surgery or trauma.
1 Auscultate rhythm at apex: regular, irregular?
2 Check apical pulse against radial pulse, noting perfusion of all beats
3 Assess apical heart sounds
4 Check capillary refill for prompt return
5 Check pretibial oedema
6 Palpate posterior tibial pulse, right and left
7 Palpate dorsalis pedis pulse, right and left
Note: Be prepared to assess pulses in the lower extremities by Doppler imaging if you cannot find them by palpation
8 Assess fluid intake and output balance.
|


 |
| SKIN |
|
Commonly performed postsurgery/anaesthetic on return to ward; as part of an assessment of fluid balance, wound assessment and to assess risk of skin breakdown.
1 Note skin colour
2 Palpate skin temperature; expect warm and dry
3 Pinch up a fold of skin under the clavicle or on the forearm to note mobility and turgor
4 Note skin integrity, any lesions and the condition of any wound/dressings
5 Complete any standardised scales used to quantify the risk of skin breakdown
6 Verify that any air loss or pressure loss surfaces being used are properly applied and operating at the correct settings
|
 |
| NUTRITION AND METABOLISM |
|
Commonly performed postsurgery/anaesthetic on return to ward; and to monitor nutritional intake and blood sugar levels.
1 Assess type and amount of food and fluid intake
2 Assess appropriateness of diet for person’s situation
3 Check nasogastric feeds/drainage
4 Perform blood sugar monitoring if relevant.
|
|
ABDOMEN/BOWEL FUNCTION
Commonly performed postsurgery/anaesthetic on return to ward; to assess bowel sounds prior to commencement of food and/or fluids; to assess risk for constipation.
1 Assess contour of abdomen: flat, rounded, protuberant
2 Listen to bowel sounds in all four quadrants
3 Check any tube placement for drainage and insertion site integrity
4 Assess bowel or urinary stoma (if applicable) for colour and moisture, size and shape, oedema, periostomal skin integrity, protrusion (spouting) and output
5 Inquire whether passing flatus or stool and rating according to the Bristol stool form scale.
|
 |
| RENAL/BLADDER FUNCTION |
|
Commonly performed postsurgery/anaesthetic on return to ward; to assess bowel sounds prior to commencement of food and/or fluids.
1 Assess fluid intake compared with output in the last 24 hours. Check fluid balance over past days
2 Inquire about voiding frequency
3 Check urine for colour, clarity and amount
4 If urine output is below the expected value, perform a bladder scan according to agency protocol. Is the problem in the production of urine or its retention?
|
|
| MUSCULOSKELETAL FUNCTION |
|
1 Assist patient to sitting up level, move to chair
2 Note any assistance needed, how tolerates movement, distance walked to chair, ability to turn
3 Need for any ambulatory aid or equipment
4 Complete any standardised scales used to quantify the patient’s risk for falling
5 Note patient’s need for rest/sleep, presence of fatigue.
|
 |













