Community Health Planning, Implementation, and Evaluation
Diane C. Martins and Patricia M. Burbank*
Objectives
Upon completion of this chapter, the reader will be able to do the following:
1. Describe the concept “community as client.”
2. Apply the nursing process to the larger aggregate within a system’s framework.
3. Describe the steps in the health planning model.
4. Identify the appropriate prevention level and system level for nursing interventions in families, groups, aggregates, and communities.
5. Recognize major health planning legislation.
6. Analyze factors that have contributed to the failure of health planning legislation to control health care costs.
7. Describe the community health nurse’s role in health planning, implementation, and evaluation.
Key terms
certificate of need (CON)
community as client
health planning
Health Planning Model
Hill-Burton Act
key informant
National Health Planning and Resources Development Act
Partnership for Health Program (PHP)
Regional Medical Programs (RMPs)
Additional Material for Study, Review, and Further Exploration
Health planning for and with the community is an essential component of community health nursing practice. The term health planning seems simple, but the underlying concept is quite complex. Like many of the other components of community health nursing, health planning tends to vary at the different aggregate levels. Health planning with an individual or a family may focus on direct care needs or self-care responsibilities. At the group level, the primary goal may be health education, and, at the community level, health planning may involve population disease prevention or environmental hazard control. The following example illustrates the interaction of community health nursing roles with health planning at a variety of aggregate levels
.
Implementing such a comprehensive plan is time consuming and requires community involvement and resources. The nurse enlisted the aid of school officials and other community professionals. Time will reveal the plan’s long-term effectiveness in reducing teen pregnancy.
This example shows how nurses can and should become involved in health planning. Teen pregnancy is a significant health problem and often results in lower education and lower socioeconomic status, which can lead to further health problems. The nurse’s assessment and planned interventions involved individual teenagers, parents and families, the school system, and community resources.
This chapter provides an overview of health planning and evaluation from a nursing perspective. It also describes a model for student involvement in health planning projects and a review of significant health planning legislation.
Overview of health planning
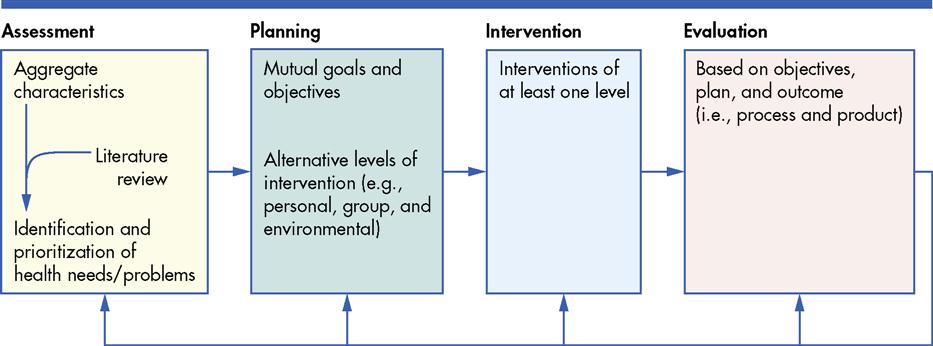
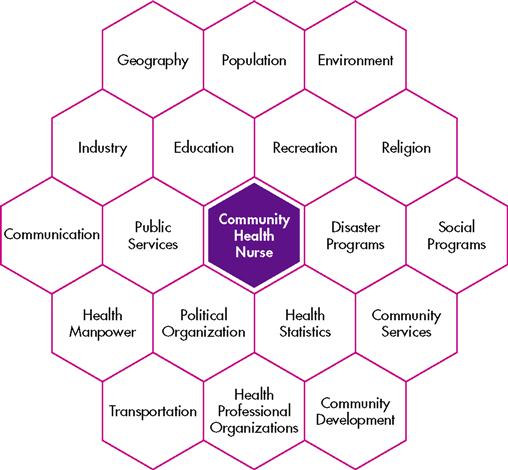
One of the major criticisms of community health nursing practice involves the shift in focus from the community and larger aggregate to family caseload management or agency responsibilities. When focusing on the individual or family, nurses must remember that these clients are members of a larger population group or community, and environmental factors influence them. Nurses can identify these factors and plan health interventions by implementing an assessment of the entire aggregate or community. Figure 7-1 illustrates this process.
The concept of “community as client” is not new. Lillian Wald’s work at New York City’s Henry Street settlement in the late 1800s exemplifies this concept. At the Henry Street settlement, Miss Wald, Mary Brewster, and other public health nurses worked with extremely poor immigrants.
The “case” element in Wald’s early reports received less and less emphasis; she instinctively went beyond the symptoms to appraise the whole individual. She observed that one could not understand the individual without understanding the family and saw that the family was in the grip of larger social and economic forces, which it could not control (Duffus, 1938).
The early beginnings of public health nursing incorporated visits to the homebound ill and applied the nursing process to larger aggregates and communities to improve health for the greatest number of people. Wald’s goals, and those of other public health nurses, were health promotion and disease prevention for the entire community (Silverstein, 1985). Health planning at the aggregate or community level is necessary to accomplish these goals.
Through the 1950s, public health nursing adopted Wald’s nursing concepts, which focused on mobilizing communities to solve local problems, treat the poor, and improve the environmental conditions that fostered disease. During the 1950s, social changes such as suburbanization, increased family mobility, and enhanced government health expenditures updated nursing roles. Since the mid-1960s, there has been a shift from public health nursing, which emphasizes community care, to community health nursing, which includes all nonhospital nursing activities. New trends constantly emerge through health care reform debates. It has become more important to use nurses as primary care providers in the health care system. A continued shift into the community requires that community health nurses become increasingly visible and vocal leaders of health care reform.
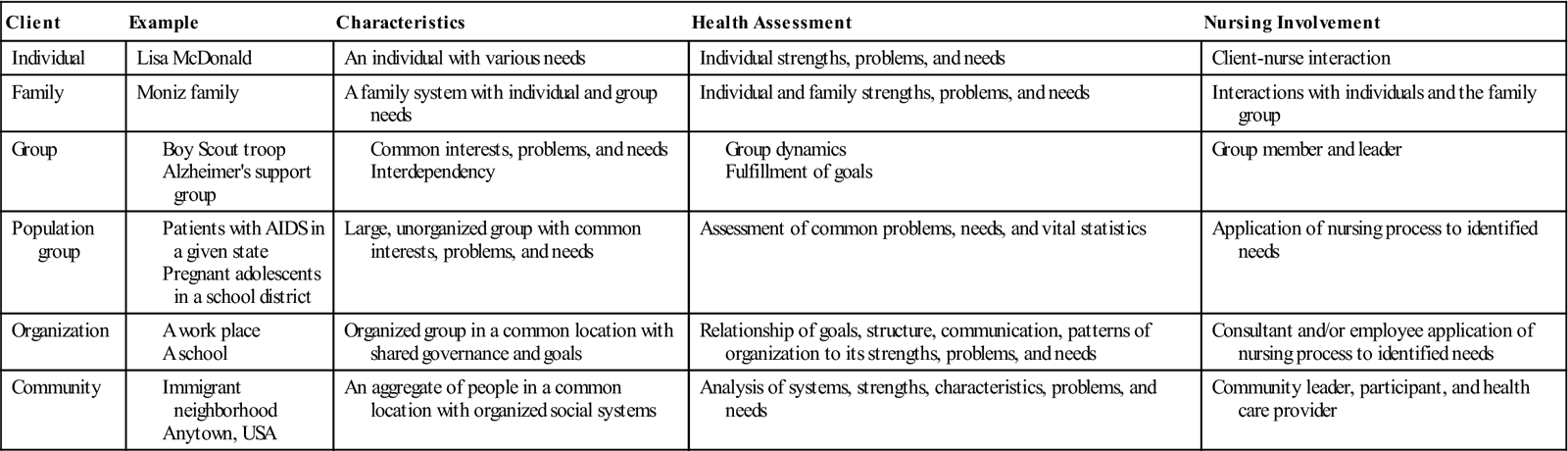
The increased focus on community-based nursing practice yields a greater emphasis on the aggregate becoming the client or care unit. However, the community health nurse should not neglect nursing care at the individual and family levels by focusing on health care only at the aggregate level. Rather, the nurse can use this community information to help understand individual and family health problems and improve their health status. Table 7-1 illustrates the differences in community health nursing practice at the individual, family, and community levels.
TABLE 7-1
Levels of Community Health Nursing Practice
However, before nurses can participate in health care planning, they must be knowledgeable about the process and comfortable with the concept of community as client or care focus. It is essential that undergraduate and graduate nursing programs integrate these concepts into the curricula. If basic and advanced nursing education includes health planning, the student becomes aware of the process and the professional involvement opportunities.
Early efforts to provide students with learning experiences in community health investigation included Hegge’s (1973) use of learning packets for independent study and Ruybal’s opportunities for students to apply epidemiological concepts in community program planning and evaluation (Ruybal, Bauwens, and Fasla, 1975). However, neither of these approaches presented a complete model that incorporated the nursing process into a health planning framework. Several other authors, including Budgen and Cameron (2003) and Shuster and Goeppinger (2008), described the community health planning process. However, none of these models uses practical examples for actual student implementation throughout the entire process.
Health planning model
A model based on Hogue’s (1985) group intervention model was developed in response to this need for population focus. The Health Planning Model aims to improve aggregate health and applies the nursing process to the larger aggregate within a systems framework. Figure 7-2 depicts this model. Incorporated into a health planning project, the model can help students view larger client aggregates and gain knowledge and experience in the health planning process. Nurses must carefully consider each step in the process, using this model. Box 7-1 outlines these steps. In addition, Box 7-2 provides the systems framework premises that nurses should incorporate.
Several considerations affect how nurses choose a specific aggregate for study. The community may have extensive or limited opportunities appropriate for nursing involvement. Additionally, each community offers different possibilities for health intervention. For example, an urban area might have a variety of industrial and business settings that need assistance, whereas a suburban community may offer a choice of family-oriented organizations such as boys and girls clubs and parent-teacher associations that would benefit from intervention.
A nurse should also consider personal interests and strengths in selecting an aggregate for intervention. For example, the nurse should consider whether he or she has an interest in teaching health promotion and preventive health or in planning for organizational change, whether his or her communication skills are better suited to large or small groups, and whether he or she has a preference for working with the elderly or with children. Thoughtful consideration of these and other variables will facilitate assessment and planning.
Assessment
To establish a professional relationship with the chosen aggregate, a community health nurse must first gain entry into the group. Good communication skills are essential to make a positive first impression. The nurse should make an appointment with the group leaders to set up the first meeting.
The nurse must initially clarify his or her position, organizational affiliation, knowledge, and skills. The nurse should also clarify mutual expectations and available times. Once entry is established, the nurse continues negotiation to maintain a mutually beneficial relationship.
Meeting with the aggregate on a regular basis will allow the nurse to make an in-depth assessment. Determining sociodemographic characteristics (e.g., distribution of age, sex, and race) may help the nurse ascertain health needs and develop appropriate intervention methods. For example, adolescents need information regarding nutrition, abuse of drugs and alcohol, and relationships with the opposite sex. They usually do not enjoy lectures in a classroom environment, but the nurse must possess skills to initiate small-group involvement and participation. An adult group’s average educational level will affect the group’s knowledge base and its comfort with formal versus informal learning settings. The nurse may find it more difficult to coordinate time and energy commitments if an organization is the focus group, because the aggregate members may be more diverse.
The nurse may gather information about sociodemographic characteristics from a variety of sources. These sources include observing the aggregate, consulting with other aggregate workers (e.g., the factory or school nurse, a Head Start teacher, or the resident manager of a high-rise senior-citizen apartment building), reviewing available records or charts, interviewing members of the aggregate (i.e., verbally or via a short questionnaire), and interviewing a key informant. A key informant is a formal or informal leader in the community who provides data that is informed by his or her personal knowledge and experience with the community.
In assessing the aggregate’s health status, the nurse must consider both the positive and negative factors. Unemployment or the presence of disease may suggest specific health problems, but low rates of absenteeism at work or school may suggest a need to focus more on preventive interventions. The specific aggregate determines the appropriate health status measures. Immunization levels are an important index for children, but nurses rarely collect this information for adults. However, the nurse should consider the need for influenza and/or pneumonia vaccines with the elderly. Similarly, the nurse would expect a lower incidence of chronic disease among children, whereas the elderly have higher rates of long-term morbidity and mortality.
The aggregate’s suprasystem may facilitate or impede health status. Different organizations and communities provide various resources and services to their members. Some are obviously health related, such as the presence or absence of hospitals, clinics, private practitioners, emergency facilities, health centers, home health agencies, and health departments. Support services and facilities such as group meal sites or Meals on Wheels (MOW) for the elderly and recreational facilities and programs for children, adolescents, and adults are also important. Transportation availability, reimbursement mechanisms or sliding-scale fees, and community-based volunteer groups may determine the use of services. An assessment of these factors requires researching public records (e.g., town halls, telephone directories, and community services directories) and interviewing health professionals, volunteers, and key informants (i.e., someone who is familiar with the community) in the community. The nurse should augment existing resources or create a new service rather than duplicating what is already available to the aggregate.
A literature review is an important means of comparing the aggregate with the norm. For example, children in a Head Start setting, day care center, or elementary school may exhibit a high rate of upper respiratory tract infections during the winter. The nurse should review the pediatric literature and determine the normal incidence for this age range in group environments. Further, the nurse should research potential problems in an especially healthy aggregate (e.g., developmental stresses for adolescents or work or family stresses for adults) or determine whether a factory’s experience with work-related injury is within an average range. Comparing the foregoing assessment with research reports, statistics, and health information will help determine and prioritize the aggregate’s health problems and needs.
The last phase of the initial assessment is identifying and prioritizing the specific aggregate’s health problems and needs. This phase should relate directly to the assessment and the literature review and should include a comparative analysis of the two. Most important, this step should reflect the aggregate’s perceptions of need. Depending on the aggregate, the nurse may consult the aggregate members directly or interview others who work with the aggregate (e.g., a Head Start teacher). Interventions are seldom successful if the nurse omits or ignores the clients’ input.
During the needs assessment, four types of needs should be assessed. The first is the expressed need or the need expressed by the behavior. This is seen as the demand for services and the market behavior of the targeted population. The second need is normative, which is the lack, deficit, or inadequacy as determined by expert health professionals. The third type of need is the perceived need expressed by the audience. Perceived needs include the population’s wants and preferences. The final need is the relative need, which is the gap showing health disparities between the advantaged and disadvantaged populations (Issel, 2009).
Finally, the nurse must prioritize the identified problems and needs to create an effective plan. The nurse should consider the following factors when determining priorities:
• Number of individuals in the aggregate affected by the health problem
• Severity of the health need or problem
• Availability of potential solutions to the problem
• Practical considerations such as individual skills, time limitations, and available resources
In addition, the nurse may further refine the priorities by applying a framework such as Maslow’s (1968) hierarchy of needs (i.e., lower-level needs have priority over higher-level needs) or Leavell and Clark’s (1965) levels of prevention (i.e., primary prevention may take priority for children, whereas tertiary prevention may take higher priority for the elderly).
Assessment and data collection are ongoing throughout the nurse’s relationship with the aggregate. However, the nurse should proceed to the planning stage once the initial assessment is complete. It is particularly important to link the assessment stage with other stages at this step in the process. Planning should stem directly and logically from the assessment, and implementation should be realistic.
An essential component of health planning is to have a strong level of community involvement. The nurse is responsible for advocating for client empowerment throughout the assessment, planning, implementation, and evaluation phase of this process. Community organization reinforces one of the field’s underlying premises as outlined by Nyswander (1956): “Start where the people are.” Moreover, Labonte (1994) stated that the community is the engine of health promotion and a vehicle of empowerment. He describes five spheres of an empowerment model, that focus on the following levels of social organization: interpersonal (personal empowerment), intragroup (small-group development), intergroup (community collaboration), interorganizational (coalition building), and political action. Attention to collective efforts and support of community involvement and empowerment, rather than focusing on individual efforts, will help ensure that the outcomes reflect the needs of the community and truly make a difference in people’s lives.
Labonte’s (1994) multilevel empowerment model allows us to consider both macro-level and micro-level forces that combine to create both health and disease. Therefore, it seems that both micro and macro viewpoints on health education provide nurses with multiple opportunities for intervention across a broad continuum. In summary, health education activities that have an “upstream” focus examine the underlying causes of health inequalities through multilevel education and research. This allows nurses to be informed by critical perspectives from education, anthropology, and public health (Israel et al., 2005).
Successful health programs rely on empowering citizens to make decisions about individual and community health. Empowering citizens causes power to shift from health providers to community members in addressing health priorities. Collaboration and cooperation among community members, academicians, clinicians, health agencies, and businesses help ensure that scientific advances, community needs, sociopolitical needs, and environmental needs converge in a humanistic manner.
Planning
Again, the nurse should determine which problems or needs require intervention in conjunction with the aggregate’s perception of its health problems and needs, and based on the outcomes of prioritization. Then the nurse must identify the desired outcome or ultimate goal of the intervention. For example, the nurse should determine whether to increase the aggregate’s knowledge level and whether an intervention will cause a change in health behavior. It is important to have specific and measurable goals and desired outcomes. This will facilitate planning the nursing interventions and determining the evaluation process.
Planning interventions is a multistep process. First, the nurse must determine the intervention levels (e.g., subsystem, aggregate system, and/or suprasystem). A system is a set of interacting and interdependent parts (subsystems), organized as a whole with a specific purpose. Just as the human body can be viewed as a set of interacting subsystems (e.g., circulatory, neurological, integumentary), a family, a worksite, or a senior high-rise can also be viewed as a system. Each system then interacts with, and is further influenced by, its physical and social environment, or suprasystem (for example, the larger community).
Second, the nurse should plan interventions for each system level, which may center on the primary, secondary, or tertiary levels of prevention. These levels apply to aggregates, communities, and individuals. Primary prevention consists of health promotion and activities that protect the client from illness or dysfunction. Secondary prevention includes early diagnosis and treatment to reduce the duration and severity of disease or dysfunction. Tertiary prevention applies to irreversible disability or damage and aims to rehabilitate and restore an optimal level of functioning. Plans should include goals and activities that reflect the identified problem’s prevention level.
Third, the nurse should validate the practicality of the planned interventions according to available personal as well as aggregate and suprasystem resources. Although teaching is often a major component of community health nursing, the nurse should consider other potential forms of intervention (e.g., personal counseling, policy change, or community service development). Input from other disciplines or community agencies may also be helpful. Finally, the nurse should coordinate the planned interventions with the aggregate’s input to maximize participation.
Goals and Objectives
Development of goals and objectives is essential. The goal is generally where the nurse wants to be, and the objectives are the steps needed to get there. Measurable objectives are the specific measures used to determine whether or not the nurse is successful in achieving the goal. The objectives are instructions about what the nurse wants the population to be able to do. In writing the objectives, the nurse should use verbs and include specific conditions (how well or how many) that describe to what degree the population will be able to demonstrate mastery of the task.
The objectives may be used to later measure learning outcomes, but the objectives need to be measurable. Objectives may also be referred to as behavioral objectives or outcomes because they describe observable behavior rather than knowledge. An example of the goals and measurable objectives for a city with a high rate of childhood obesity is shown in Box 7-3.
Intervention
The intervention stage may be the most enjoyable stage for the nurse and the clients. The nurse’s careful preliminary assessment and planning should help ensure the aggregate’s positive response to the intervention. Although implementation should follow the initial plan, the nurse should prepare for unexpected problems (e.g., bad weather, transportation problems, poor attendance, or competing events). If the nurse is unable to complete the intervention, the reasons for its failure should be analyzed. Interventions should be included from a range of strategies including mass media (public service announcements, radio, television, billboards), general information dissemination (e.g., pamphlets, DVDs, CDs, posters), electronic information dissemination (e.g., websites, blogs, tweets, video stream), and public forums (e.g., town meetings, focus groups, discussion groups).
Evaluation
Evaluation is an important component for determining the success or failure of a project and understanding the factors that contributed to its success or failure. The evaluation should include the participant’s verbal or written feedback and the nurse’s detailed analysis. Evaluation includes reflecting on each previous stage to determine the plan’s strengths and weaknesses (process evaluation). Process evaluation is also referred to as formative evaluation. It allows one to evaluate both positive and negative aspects of each experience honestly and comprehensively and whether the desired outcomes were achieved (product evaluation). Product evaluation is summative and can consist of end-of-intervention surveys and other tools that measure whether objectives have been met. Summative evaluation is another term for product evaluation and looks at outcomes. Evaluation should include adequacy, efficiency, appropriateness, and cost benefit. During both process and product evaluation, the nurse may ask the following questions:
• Was the assessment adequate?
• Were plans based on an incomplete assessment?
• Did the plan allow adequate client involvement?
• Were the interventions realistic or unrealistic in terms of available resources?
• Did the plan consider all levels of prevention?
• Were the stated goals and objectives accomplished?
• Were the participants satisfied with the interventions?
• Did the plan advance the knowledge level of the aggregate and the nurse?
The intervention may have limited impact if the nurse fails to communicate follow-up recommendations to the aggregate upon completion of the project. Although follow-up activity is not necessary for every plan, most require additional interventions within the aggregate using community agencies and resources. A comprehensive health planning project involves a close working relationship with the aggregate and careful consideration of each step. Long-term evaluation may need to be done by those professionals working continuously with the aggregate, to determine behavior changes and/or changes in health status
.
Health planning projects
Successful Projects
Student projects have used this health planning model with group, organization, population group, and community aggregates. Table 7-2 describes interventions with these aggregates at the subsystem, aggregate system, and suprasystem levels.
TABLE 7-2
Interventions by Type of Aggregate and System Level
| Project | Type of Aggregate | System Level for Intervention |
| Rehabilitation group | Group, organization | Subsystem and aggregate system |
| Textile industry | Population group | Aggregate system and suprasystem |
| Crime watch | Group, organization, and population group | Aggregate system and suprasystem |
| Bilingual students (case study) | Community | Aggregate system and suprasystem |
Textile Industry
Crime Watch
Rehabilitation Group
Unsuccessful Projects
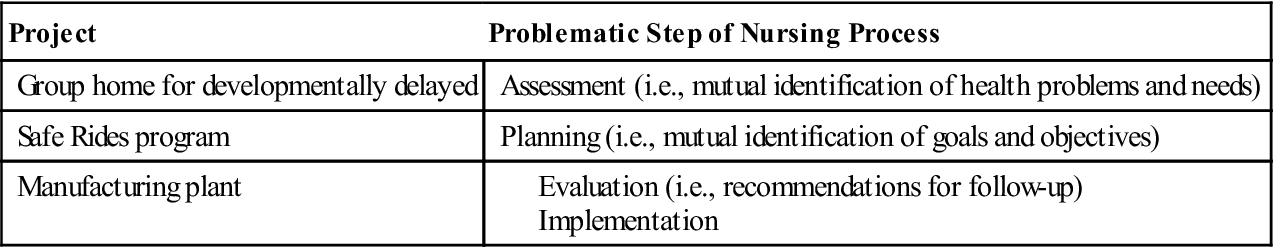
Project failure is usually caused by problems with one or more steps of the nursing process. Usually the student does not discover problems until the evaluation phase. The following unsuccessful projects illustrate failures at different steps in the nursing process. Table 7-3 summarizes the identified problem areas for these examples.
TABLE 7-3
Group Home for Developmentally Delayed Adults
Safe Rides Program
Manufacturing Plant
Discussion
Each of these projects attempted to address a particular level of prevention. Most of these examples focused on primary prevention and health promotion because they were student conducted and time limited. Table 7-4 lists these projects and their prevention levels. However, the full-time community health nurse working with an aggregate (e.g., in the occupational health setting) would target interventions for all three levels of prevention at a variety of system levels. It is useful to view nursing interventions with aggregates within a matrix structure to address all intervention opportunities. The matrix in Table 7-5 gives examples of how the occupational health nurse may intervene at all system levels and all prevention levels.
TABLE 7-4
Level of Prevention for Each Project
| Primary Prevention | Secondary Prevention | Tertiary Prevention |
| Textile industry | Textile industry | Rehabilitation group |
| Crime watch | Group home for developmentally delayed | |
| Manufacturing plant | ||
| Safe Rides program |
TABLE 7-5
Occupational Health: Levels of Prevention for System Levels
| System Level | Primary Prevention | Secondary Prevention | Tertiary Prevention |
| Subsystem | Yearly physical examination for each employee | Regular blood pressure monitoring and diet counseling for each employee with elevated blood pressure | Referral for job retraining for employee with a back injury |
| Aggregate and group system | Incentive program to encourage departments to use safety devices | Weight reduction group for overweight employees | Support group for employees who are recovering from problems with alcohol or drug use |
| Suprasystem | Health fair open to the community and employees | Counseling and referral of community members with elevated blood pressure or cholesterol on the basis of health fair findings | Media advertising to encourage people with substance abuse problems to seek help and use community resources that provide assistance |

In practice, most interventions occur at the individual level and include all prevention levels. Interventions at the aggregate level are usually less frequent. For many occupational health nurses, time does not allow intervention at the suprasystem level. However, industries are integral parts of the community system. Factors that affect community health also affect employee health and vice versa. Some industries take their reciprocal relationship with the surrounding community quite seriously. For nurses in these industries, interventions at the suprasystem level may become a reality and improve the health of the community and the workers. This is a good example of refocusing upstream by addressing the real source of problems. Although the chosen example is occupational health nursing, any nurse working with aggregate systems can construct a similar matrix for interventions.
These projects illustrate the variety of available opportunities for aggregate health planning. In addition, they exemplify the application of the nursing process within various aggregate types, at different systems levels, and at each prevention level. These examples demonstrate the vital importance of each step of the nursing process.
1. Aggregate assessments must be thorough. The textile industry project exemplifies this point. Assessments should elicit answers to key questions about the aggregate’s health and demographic profile and should compare this information with similar aggregates presented in the literature.
2. The nurse must complete careful planning and set goals that the nurse and the aggregate accept. The rehabilitation group project illustrates the importance of mutual planning.
3. Interventions must include aggregate participation and must meet the mutual goals. The Crime Watch project exemplifies this point.
4. Evaluation must include process and product evaluation and aggregate input.
Health planning federal legislation
Health planning at the national, state, and local levels is another example of aggregate planning. Planning at any of these levels can be a broader extension of the suprasystem level and affects the individual, family, group, population, and organization levels. Again, upstream change can occur on these levels; for example, individual consumers and consumer groups have protested some managed-care practices at the suprasystem level, because health policy can directly affect patient care.
Historically, nurses have influenced health planning only minimally at the community level, but health planning has a tremendous effect on nurses and nursing practice. It is necessary to understand planning on a suprasystem level; therefore the following section contains a review of past health planning efforts with projections for the future.
Hill-Burton Act
In 1946, Congress passed the Hospital Survey and Construc-tion Act (Hill-Burton Act, PL 79-725) to address the need for better hospital access. This act provided federal aid to states for hospital facilities. A state had to submit a plan documenting available resources and need estimates to qualify for hospital construction and modernization funds under the Hill-Burton Act (Sultz and Young, 2006). In addition, each state had to designate a single agency for the development and implementation of the hospital construction plan. The Hill-Burton Act caused the expenditure of vast sums of money and resulted in an increase in the number of beds, especially in general hospitals. Although the act and its amendments focused only on construction, it improved the quality of care in rural areas and introduced systematic statewide planning (Gourevitch, Caronna, and Kalkut, 2005).
Regional Medical Programs
The Hill-Burton Act provided construction-related planning, but it did not address coordination and care delivery directly. In response to recommendations from Dr. Michael DeBakey’s national commission, Heart Disease, Cancer, and Stroke Amendments of 1965 (PL 89-239) were enacted. This legislation was more comprehensive and established regional medical programs.
The Regional Medical Programs (RMPs) intended to make the latest technology for the diagnosis and treatment of heart disease, cancer, stroke, and related diseases available to community health care providers through the establishment of regional cooperative arrangements among medical schools, research institutions, and hospitals. The goals of these cooperative arrangements were to improve the health manpower and facilities available to the communities. The intent was to avoid interfering with methods of financing, hospital administration, patient care, or professional practice.
Although RMPs have been credited with the regionalization of certain services and the introduction of innovative approaches to organization and care delivery, some observers believed the reforms were not comprehensive enough. The RMPs did not partner with the existing federal and state programs; therefore, there were gaps and duplication in service delivery, personnel training, and research (Kovner, 2002).
Comprehensive Health Planning
Congress signed the Comprehensive Health Planning and Public Health Services Amendments of 1966 (PL 89-749) into law to broaden the previous legislation’s categorical approach to health planning. Combined with the Partnership for Health Amendments of 1967 (PL 90-174), these amendments created the Partnership for Health Program (PHP). The PHP provided federal grants to states to establish and administer a local agency program to enact local comprehensive health care planning. The PHP’s objectives were promoting and ensuring the highest level of health for every person and not interfering with the existing private practice patterns (Shonick, 1995).
To meet these objectives, the PHP formulated a two-level planning system. Under this system, each state had to designate a single health planning agency, or “A” agency. To play a statewide coordinating role, the “A” agency had to partner with an advisory council, which consisted largely of health care consumers. Meanwhile, the local “B” agencies formulated plans to meet designated local community needs, which could be any public or nonprofit private agency or organization. “A” agencies were to encourage the formation of local, comprehensive, health planning “B” agencies, and federal grants were made available for that purpose (Shonick, 1995).
Although the comprehensive health plans were the first of these programs to mandate consumer involvement, they may have failed in their basic intent. The possible failure may have resulted from funding shortage, conflict avoidance in policy formulation and goal establishment, political absence, and provider opposition (e.g., American Medical Association, American Hospital Association, and major medical centers) (Shonick, 1995).
Certificate of Need
In response to increased capital investments and budgetary pressures, state governments developed the idea of obtaining prior governmental approval for certain projects through the use of a certificate of need (CON). New York State passed the first CON law in 1964, which required government approval of hospitals’ and nursing homes’ major capital investments. Eventually all states supported this CON requirement, and it ultimately became a component of health legislation (PL 93-641). In practice, state CON programs differ in structure and goals. These differences include program focus, decision-making levels, review standard scope, and appeals process exemption (Sultz and Young, 2006).
National Health Planning and Resources Development Act
Given the perceived failure of the comprehensive health planning programs, the federal government focused on a new approach to health planning. The federal government was greatly concerned with the cost of health care, which escalated dramatically following the end of World War II; the uneven distribution of services; the general lack of knowledge of personal health practices; and the emphasis on more costly modalities of care. The National Health Planning and Resources Development Act of 1974 (PL 93-641) combined the strengths of the Hill-Burton Act, RMPs, and the comprehensive health planning program to forge a new system of single-state and area-wide health planning agencies (Harlow, 2006).
The goals and purposes of the new law were an increase in accessibility, acceptability, continuity, and quality of health services; control over the rising costs of health care services; and prevention of unnecessary duplication of health resources. The new law addressed the needs of the underserved and provided quality health care. The provider and consumer were to be involved in planning and improving health services, and it placed the system of private practice under scrutiny.
At the center of the program was a network of local health planning agencies, which developed a health systems plan for their geographic service area. The local agencies then submitted these plans to a state health planning and development agency, which integrated the plans into a preliminary state plan. The state agency presented this preliminary plan to a statewide health coordinating council for approval. The law required that the council consist of at least 16 governor-appointed members and that 50% of these members represent health system agencies and 50% represent consumers. One major function of this council was to prepare a state health plan that reflected the goals and purposes of the act. Once the council formulated a tentative plan, they presented it at public hearings throughout the state for discussion and possible revisions (Thorpe, 2002).
Despite careful deliberations by health planners with input from consumers, not all states accepted the health system plan at the grassroots level. A number of problems were encountered, and, in time, the legislation failed to effect major change in the health care system. A significant problem was that legislation grandfathered the entire health care system (i.e., health care delivery methods did not change). Although legislation mandated consumer involvement in the health system agency, it was often difficult to implement this aspect. Additionally, despite the mandated efforts by CON and required reviews, costs continued to rise, and the health care system remained essentially unchanged (Thorpe, 2002).
Comprehensive Health Reform
The Patient Protection and Affordable Care Act of 2010 includes several elements that involve health planning (Kaiser Family Foundation, 2010). Provisions from that act include:
• Creation of task forces on preventive services and commu-nity preventive services to develop, update, and disseminate evidence-based recommendations on health care delivery
• Establishment of the National Prevention, Health Promotion, and Public Health Council, an agency that will be charged with development of a national strategy to improve the nation’s health
• Creation of an innovation center within the Centers for Medicare and Medicaid Services
• Development of a national quality improvement strategy that will seek to improve delivery of health care services and population health
• Provision of billions of dollars for funding community health centers, school based clinics and the National Health Service Corps to improve access to care
• Establishment of an Independent Payment Advisory Board to make proposals to reduce the growth in Medicare spending
• Establishment of a workforce advisory committee to develop a national workforce strategy and to suggest ways to enhance the workforce supply by supporting education of health professionals through scholarships and loans
Many of these provisions will not be implemented for several years. Thus, the impact of these changes will not be realized for some time
Health Planning in Public Health
According to Issel (2009), many planning programs to address public health problems began as environmental planning of water and sewer systems. Additional population-based planning became necessary with the advent of immunizations. Blum (1974) was the first to suggest how public health planning should be done. Perspectives on health planning range from systematic problem solving and an epidemiological approach to a social awareness approach.
Beginning in the mid-1980s the Centers for Disease Control and Prevention (CDC) began to develop and promote systematic methods for health planning in public health. These models were important for a structured approach to public health planning.
PATCH
The Planning Approach to Community Health (PATCH) model was based on Green’s PRECEDE (Predisposing, Reinforcing, and Enabling factors in Community Education Development and Evaluation) (Green et al., 1980; Green and Kreuter, 2005). This model encouraged the idea that health promotion is a process that enables the population to have more control of its own health. An essential element of the PATCH model is community participation. Another element is the use of data to develop comprehensive health strategies. The PATCH model achieved this through mobilizing the community, collecting health data, selecting health priorities, developing a comprehensive intervention plan, and evaluating the process (Issel, 2009).
APEX-PH Program
The Assessment Protocol for Excellence in Public Health (APEX-PH) began in 1987 as a cooperative project of the American Public Health Association (APHA), the Association of Schools of Public Health (ASPH), the Association of State and Territorial Health Officials (ASTHO), the CDC, the National Association of County and City Health Officials (NACCHO), and the United States Conference of Local Health Officers (USCLHO). The APEX-PH is a voluntary process for organizational and community self-assessment, planned improvements, and continuing evaluation and reassessment. It is a true self-assessment and is intended to be more of a public endeavor involving the community, as well as the public organizations (CDC, 2009).
MAPP
More recently, the CDC and NACCHO have released the MAPP (Mobilizing for Action Through Planning and Partnerships) model. MAPP is a health planning model that helps public health leaders to facilitate community priorities about health issues and identify sources to address them. The first phase of MAPP is to mobilize the community, the second is to guide the community toward a shared vision for long-range planning, and the third is to conduct four assessments. The assessments are identifying community strengths, local health system, health status, and forces of change within the population (NACCHO, 2009).
Changing Focus of Health Planning
Health planning legislation is heavily influenced by the politics of the administration in power at any given time. The Reagan administration encouraged competition within the health care system. During the 1980s, the administration emphasized cost shifting and cost reduction with greater state power, less centralization of functions, and less national control. This approach represented the government’s philosophical shift and combined it with a funding cutback from the Omnibus Budget Reconcilia-tion Act in 1981. This resulted in a curtailment on federal health planning efforts at that time (Mueller, 1993). The cutbacks caused health system agencies to redefine their role, and the federal government recommended eliminating these agencies.
A reduction in federal funding and the influence of medical lobbies caused the closure of some health system agencies. Those that remained open experienced a decrease in staff, a resulting decrease in overall board functioning, and a reordering of priorities. In an effort to compensate for the decrease in federal funding, some health system agencies sought nonfederal funding or built coalitions to provide the necessary power base for change. Although the administration did not renew federal health planning legislation in the 1980s, it used other regulatory approaches to control costs. These included basing payments to Medicare on diagnosis- related groups and, in the 1990s, many individual states requiring their Medicaid recipients to enroll in health maintenance organizations (HMOs).
The Clinton administration’s plan for health care reform included mechanisms to revitalize planning at the national level. The failure of Congress to pass the plan in 1994 gave planning efforts back to state and local agencies. As a result, most states have become very involved in various aspects of health planning. Indeed, there is considerable variation as many have statewide health plans, local health plans, and some other type of local health planning (American Health Planning Association [AHPA], 2009).
At the beginning of the twenty-first century, 36 states and the District of Columbia still required CON reviews for selected expenditures that include nursing homes, psychiatric facilities, and expensive equipment (AHPA, 2009). However, within these programs, requirements for approval are more liberal, expedited reviews are conducted, and certain projects are exempted from review, which weakens the CON cost-containment mandate. Newer high-technology services (i.e., lithotripsy, gamma knives, and positron emission tomography) still need CON review in most states. Furthermore, it is anticipated that state CON programs will continue to assume a stronger role because states must increasingly monitor and report the quality, cost, and access to health care that managed care promised.
Health care system and health insurance reform were central issues in the 2008 presidential election. President Obama’s election, along with a Democratically controlled Congress, provided the opportunity to make dramatic changes in how health care is managed in the United States. Throughout most of 2009 and into 2010, Congress debated a number of different options, and the Patient Protection and Affordable Care Act became law in March 2010.
With full implementation of the Health Care Act, there should be enhanced emphasis on health promotion/health care and local, community-based approaches to health issues as opposed to emphasis on illness-oriented medical care to help defray costs and improve the overall health of the population. The Healthy People 2020 objectives support this notion. To help achieve improved health status for all, health planning needs a coordinated approach that combines public and private cooperation with an emphasis on supplies and services. Advances in planning models and the sophistication level of planners will impact future health planning efforts
.
Nursing implications
Nurses must work collaboratively with health planners to improve aggregate health. Nurses can influence health planning at the local and state, or community level by fusing current technology with their knowledge of health care needs and skills gained through working with individuals, families, groups, and population groups. This is an example of “upstream interventions.” Indeed, the nurse may become directly involved in the planning process by participating in CON reviews or gaining membership on health planning councils. Even as students, nurses can begin to participate by engaging in aggregate-level projects, such as those outlined in this chapter, and by tracking health care legislation and contacting their legislators about important issues.
Increased nursing involvement is one method of strengthening local and national health planning. Nurses can use the Health Planning Model presented in this chapter to facilitate a systematic approach to improve aggregate health care. Nurses can assess aggregates from small groups through population groups; identify the group’s health needs; and perform planning, intervention, and evaluations by applying this model. The health of individuals, families, and groups would improve if nurses reemphasized the larger aggregate.
Summary
Community health nurses are responsible for incorporating health planning into their practice. Nurses’ unique talents and skills, augmented by the comprehensive application of the nursing process, can facilitate population health improvement at various aggregate levels. Health planning policy and process constitute part of the knowledge base of the baccalaureate-prepared nurse. Systems theory provides one framework for nursing process application in the community. Interventions are possible at subsystem, system, and suprasystem levels using all three levels of prevention.
Learning activities
1. Assess a neighborhood or local community using the following exploratory techniques: Perform a windshield survey by driving through the area and identifying types of houses, schools, churches, health-related agencies, and businesses, and looking for potential environmental and safety hazards. Interview a town hall clerk, a senior citizen at a meal site or day care center, a newspaper reporter, a visiting nurse, a police officer, a social worker, or a school nurse regarding health issues in the community. Call the local, county, or state health department for morbidity and mortality statistics. Try to attend a town council or school committee meeting. Compare and contrast these findings with classmates’ findings.
2. Construct a matrix similar to Table 7-5 using interventions from a school setting.
3. In class, identify 10 to 15 questions that will elicit important health information from young adults. Each student must write answers to these questions. Tally the student responses, and draw conclusions from this assessment. Identify problems or potential problem areas, and construct a plan to solve or prevent these problems.
4. Attend a state or local health planning meeting. Observe the number of health care providers and consumers in attendance. Compare the meeting’s issues with the goals of improving care quality and reducing health care costs.