Health Promotion and Risk Factor Management Care Plans
This chapter is a new addition to Nursing Care Plans: Diagnoses, Interventions and Outcomes. It was written to address the challenges of working with patients who are seeking to increase their level of well-being. Typical nursing care plans focus on sick care, helping patients manage their medical illnesses. In these disease-focused care plans, nurses assume the more active role, with patients as the recipients of care. Thus this new chapter is unique in that it showcases patients who are actively engaged in health-seeking behaviors. The public is beginning to realize that almost half of all premature deaths in the United States are caused by lifestyle-related problems: unhealthy foods, overweight and obesity, tobacco smoking, poorly managed stress, sleep deficit, and sedentary lifestyle, to name a few. Nurses have always done an excellent job educating patients about health and disease; however, research is clear that education, though necessary, is not sufficient for making needed lifestyle changes. Making changes to one’s lifestyle is very complex. Helping a patient adopt new health behaviors requires attention to multifaceted, evidence-based strategies known to facilitate successful behavior change. These strategies include a combination of methods to enhance awareness of risk factors, increase motivation for change, set realistic goals, focus on tailoring the regimen, incorporate self-monitoring, enhance self-efficacy, provide skills in problem-solving, include social support and rewards, and address relapse prevention. Nurses are well-positioned to guide patients who are actively seeking to improve their health habits and environment to achieve their optimal level of health and wellness. These care plans demonstrate the important partnership nurses have with patients in assisting them to develop the knowledge and skills needed for making healthy lifestyle decisions and enacting healthy behaviors.
 Health-Seeking Behaviors
Health-Seeking Behaviors
![]() For additional care plans and an Online Care Plan Constructor, go to http://evolve.elsevier.com/Gulanick/.
For additional care plans and an Online Care Plan Constructor, go to http://evolve.elsevier.com/Gulanick/.
Definition: Active seeking (by a person in stable health) of ways to alter personal health habits and/or the environment in order to move toward a higher level of health
Health promotion activities include a wide range of topics such as smoking cessation; stress management; weight loss; proper diet for prevention of coronary artery disease, cancer, osteoporosis, and others diseases; exercise promotion; prenatal instruction; safe sex practices to prevent sexually transmitted infections; protective helmets to prevent head trauma; and practices to reduce risks for diabetes, stroke, and other diseases.
Patients of all ages may be involved in improving health habits. Social cognitive theory identifies factors (e.g., behavior, cognition and other personal factors, the environment) that influence how and to what extent people are able to change old behaviors and adopt new ones. Psychosocial factors such as stress and anxiety regarding perceived risk for disease, along with social support for engaging in the health-promoting behaviors, must be considered. The action plan must be tailored to fit with the patient’s values and belief systems. Opportunities for self-monitoring and receiving feedback enhance the behavior change process.
The setting in which health promotion activities occur may range from the privacy of someone’s home, group activities (e.g., weight maintenance groups or health clubs) or even the work setting (especially targeted programs for hypertension management and weight reduction). This care plan gives a general overview of health-seeking behaviors.



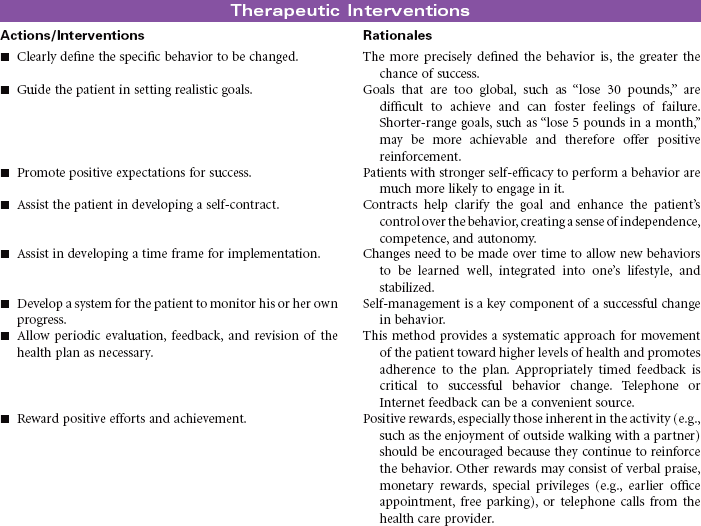

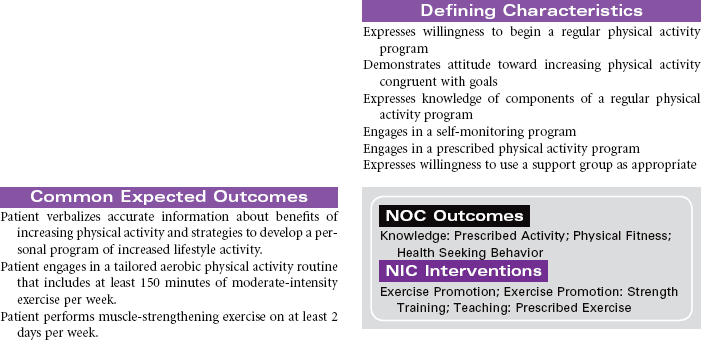
 Readiness for Engaging in a Regular Physical Activity Program
Readiness for Engaging in a Regular Physical Activity Program
The 2008 Physical Activity Guidelines for Americans provides an evidence-based prescription for assisting individuals with improving their health through regular physical activity. Based on the Aerobics Center Longitudinal Study, recommendations include both aerobic and muscle-strengthening activities in the following doses: at least 150 minutes per week of moderate aerobic physical activity to obtain general health benefits and muscle-strengthening activities using major muscle groups on 2 or more days per week. Additional health benefits can be achieved in a dose-response fashion, either by increasing the intensity to vigorous activity or by increasing the duration of moderate activity to 300 minutes per week. Health benefits can be achieved in intermittent episodes of even 10 minutes of moderate physical activity. Health benefits are attainable by individuals of all ages, even those with chronic medical problems. Stressful and busy lifestyles, socioeconomic factors, physical constraints, and lack of motivation are all barriers that can contribute to low physical activity. Nursing objectives are to educate patients on the importance of adopting an active lifestyle and to assist patients in finding ways to personalize the recommended exercise prescription.

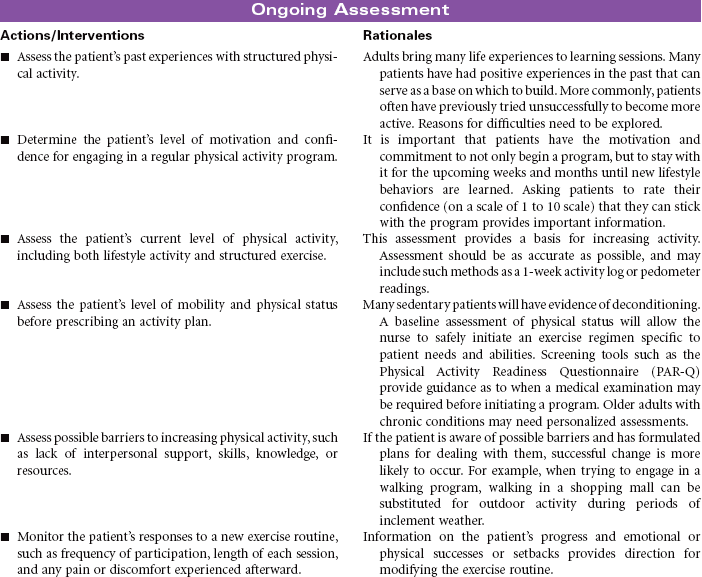





 Readiness for Enhanced Immunization Status
Readiness for Enhanced Immunization Status
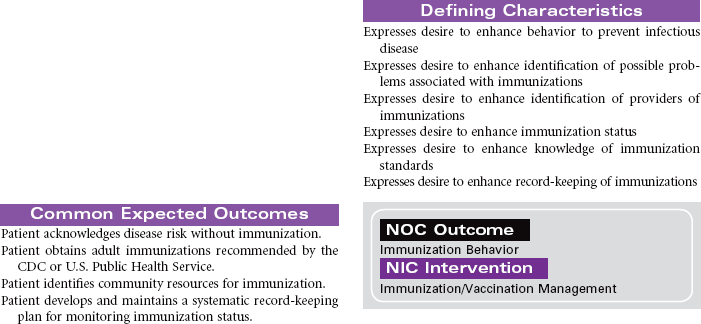
Definition: A pattern of conforming to local, national, and/or international standards of immunization to prevent infectious disease(s) that is sufficient to protect a person, family, or community and can be strengthened
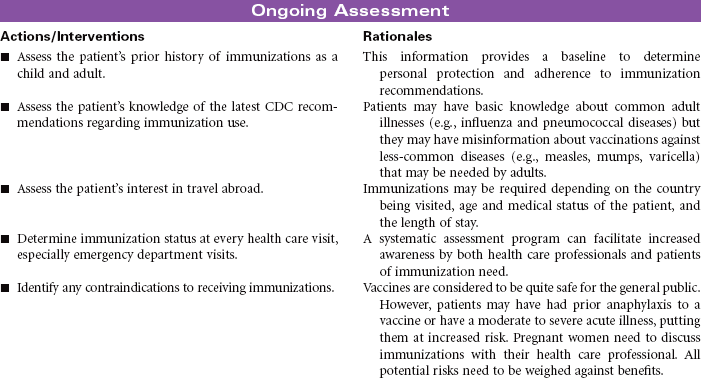
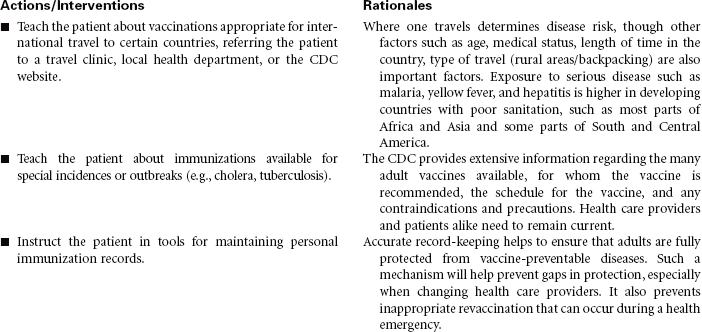
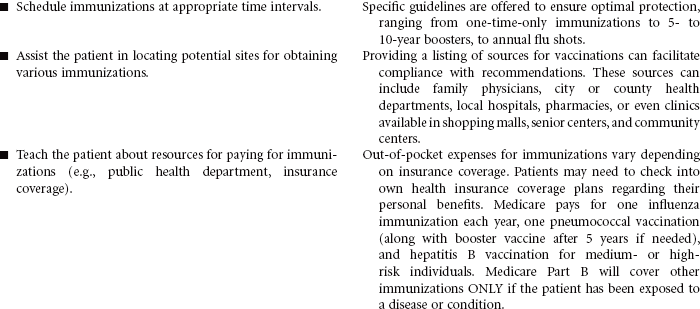
Every year, approximately 50,000 adults in the United States die from diseases that could have been prevented by vaccines. Influenza and pneumonia are the fifth leading cause of death in older adults in the United States. Immunizations are one of the safest, most cost-effective public health measures available to patients to preserve their health. Although many adults do support immunization programs for their children, they are often less informed about the many health benefits of vaccines as adults. The Centers for Disease Control and Prevention (CDC) recommendations clearly identify who is at risk for various diseases and who should be immunized to protect against them.





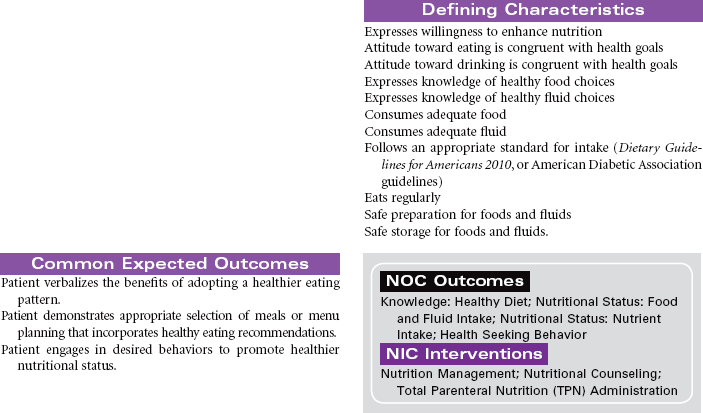
 Readiness for Enhanced Nutrition
Readiness for Enhanced Nutrition
Definition: A pattern of nutrient intake that is sufficient for meeting metabolic needs and can be strengthened.
Though people are living longer, living healthy is the more important goal. Eating a nutritious diet is essential for maintaining health, reducing the epidemic of obesity, and reducing the risk of major diseases such as heart disease, diabetes, osteoporosis, and some cancers. However, people who want to adopt a healthy eating pattern find it challenging in today’s fast-paced, fast-food, super-sized environment. Readiness to engage in a lifestyle of nutritious eating requires focused time, effort, and practice to learn how to make healthy food choices. National health guidelines, such as The Dietary Guidelines for Americans 2010, provide people with information about selecting healthy foods. These guidelines focus on three main components: balancing calories (portion control); eating a variety of nutritious foods from all the food groups (fruits, vegetables, whole-grains, low-fat milk products, seafood, lean meats, and poultry); and reducing the intake of saturated fat, added sugar, salt, and alcohol. Successful nutrition education programs also include information about identifying healthy packaged food products, reading food labels, and selecting healthy foods when eating in restaurants. Ensuring food safety is an additional principle for building healthy eating patterns and includes attention to food preparation, cooking, and storage.







 Readiness for Enhanced Sleep
Readiness for Enhanced Sleep
Definition: A pattern of natural, periodic suspension of consciousness that provides adequate rest, sustains a desired lifestyle, and can be strengthened.
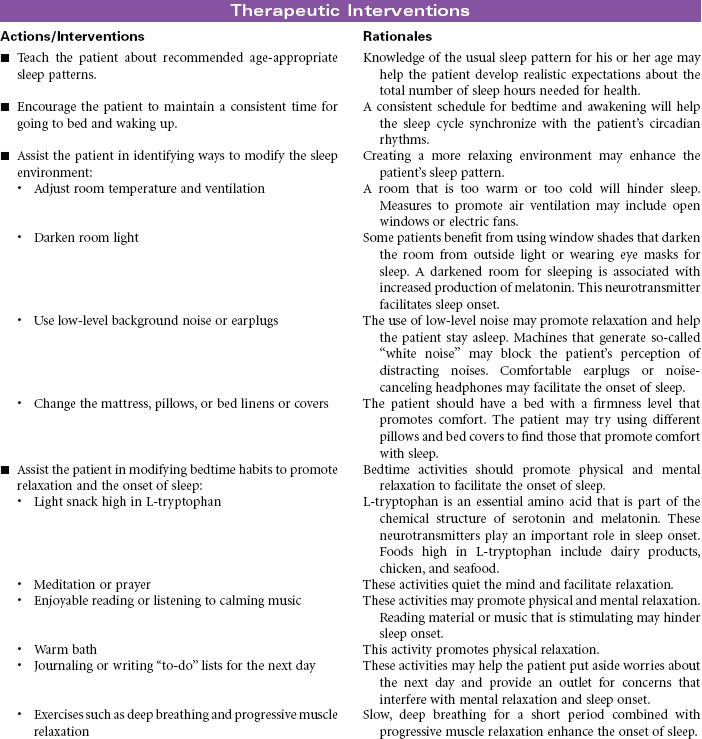
The sleep–wake cycle is a dynamic process regulated by complex interactions among neurotransmitters and hormones in the central nervous system. This cycle consists of normal changes in a person’s level of consciousness that include rapid eye movement (REM) sleep, non-REM (NREM) sleep, and wakefulness. NREM sleep consists of four stages and accounts for as much as 80% of total sleep time. Body processes decrease during NREM sleep, especially in stages 3 and 4. These changes in body function are related to sleep’s function in restoring energy, repairing tissues, and regulating hormone secretion. REM sleep occurs at 90-minute intervals. The length of each REM cycle increases during the night. During REM sleep, brain activity increases to that seen during wakefulness, yet the person is difficult to arouse. Dreams are associated with REM sleep. Research indicates that REM sleep is necessary for learning and memory formation in the brain.
Normal sleep patterns vary based on the person’s age. These variations include the total hours of sleep time, the length of each sleep cycle, and the time spent in each stage of the sleep cycle. The majority of healthy adults require 7 to 9 hours of sleep per day. Approximately 20% of sleep time is spent in REM sleep. As the adult ages, the amount of time spent in stage 4 NREM or deep sleep begins to decline. The older adult may have a decline in stage 3 NREM sleep and no stage 4 NREM sleep. As a result of spending more time in the lighter stages of NREM, the older adult may report more frequent night time awakenings. The length of each REM cycle becomes shorter with aging. Older adults sleep less during the night but may take more naps during the day to meet total sleep hour requirements. The quality of sleep for the older adult is affected by the presence of chronic health problems and the use of medications.








 Readiness for Managing Stress
Readiness for Managing Stress
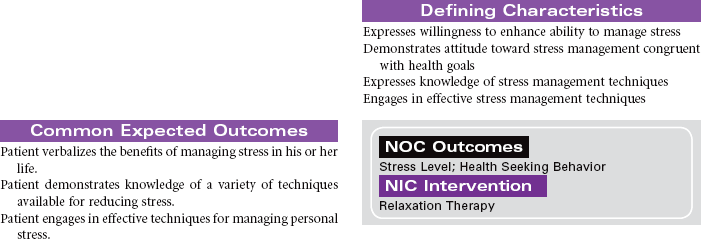
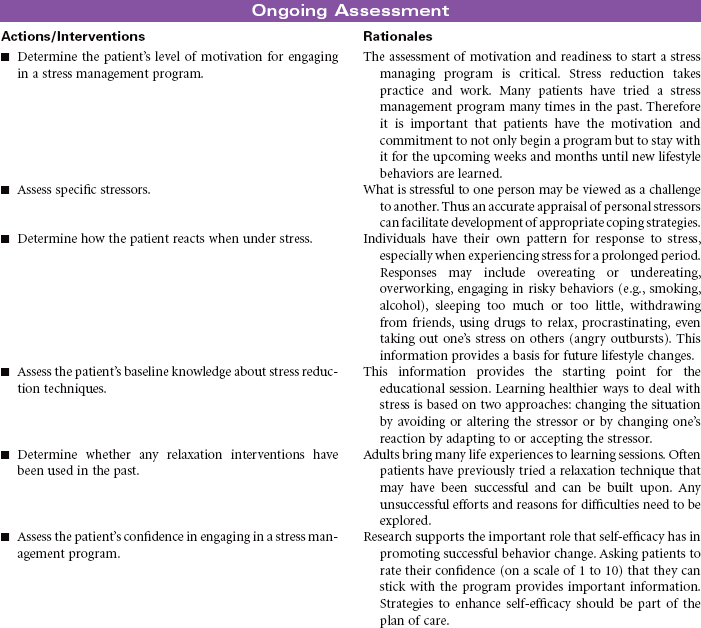
Stress is a state of physical and mental readiness. It is not an “event,” but rather an approach to an event. Stress is an inevitable part of life and something that cannot be completely eliminated; it should not be, because stress is a natural and important physiological and psychological response to a challenge about which a person is not sure. Living in today’s fast-paced, multitasking world, most people accept stress as normal and inevitable. Although stress itself is not harmful, one’s response to it can be overwhelming, and even harmful to the body. Prolonged physiological responses to stressors increase stimulation of the sympathetic nervous system and increase the release of cortisol from the adrenal cortex. These neuro-endocrine changes may impair cardiovascular and immune function and contribute to the development of chronic disease. The challenge for the individual person is to be able to reduce stress to a manageable and healthy level. Therefore successful stress reduction should be approached as a permanent lifestyle change, not simply a temporary response to a specific life event. Managing stress is about taking charge and not allowing it to control one’s life and behavior.
Readiness to engage in a stress management program is a key to success, as it takes focused time, effort, and practice to learn the many stress-reducing techniques. Mastering stress requires establishing a new mindset and habits that become a part of one’s everyday life. Different people may benefit from different approaches to stress management, but all successful programs contain the same core components: education, participating in ongoing self-monitoring, cognitive (behavioral) restructuring, incorporating relaxation training into one’s daily life, using support people or groups, and paying attention to maintaining lifestyle modifications.






 Readiness for Smoking Cessation
Readiness for Smoking Cessation
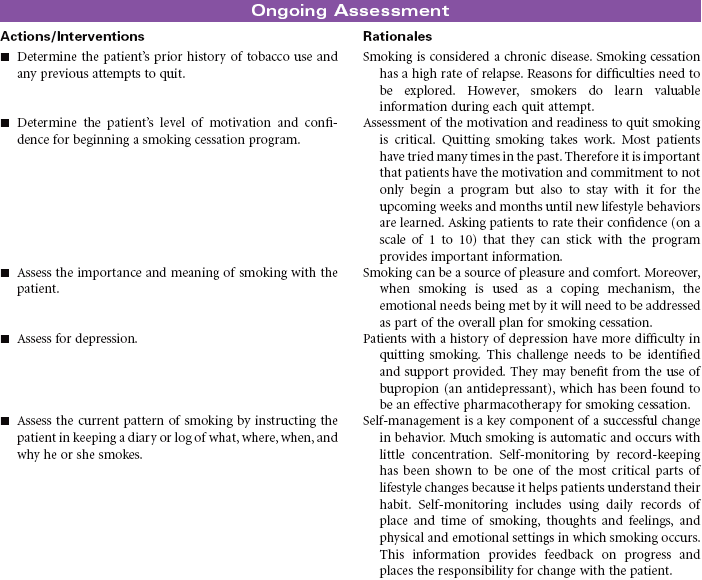
Approximately 30% of adults in America are currently smokers. The decision to quit smoking is one of the best things people can do to improve their health and add years to their life. Overall, about 70% of smokers say they are “interested” in quitting, but only 10% to 20% plan to quit in the next month. Most smokers try to quit on their own, with a success rate of 2% to 3%. Eventually, half of all smokers are able to quit.
Nicotine is one of the most powerful of all addictions to overcome. Nicotine causes changes in the brain that makes smokers want to use it more. As a result, it is very difficult for the person to stop the smoking habit. Besides the pleasant feeling of smoking, these individuals experience both physiological and psychological withdrawal from nicotine.
Fortunately, there is much evidence available on how to guide smokers in the cessation process. The U.S. Department of Health and Human Services has published clinical practice guidelines for tobacco cessation developed by the Treating Tobacco Use and Dependence Guideline Panel of 1996, 2000, and 2008. These guidelines describe five key steps (the 5 A’s) to use for patients willing to make a quit attempt. The 5 A’s include: (1) Ask—identify if individual uses tobacco; (2) Advise—deliver clear, strong, personal advice about the importance of quitting; (3) Assess—willingness to make a quit attempt; (4) Assist—aid the patient in quitting by setting a quit date and offering pharmacological and behavioral support; and (5) Arrange—for follow-up to prevent relapse.
A wide variety of programs and tools are available to assist the smoker through each stage of the quitting process. Many of these smoking cessation services are available online or through telephone quit lines. Evidence-based studies support that there is a strong dose-response relationship between the intensity of tobacco dependence counseling and its effectiveness. Numerous effective pharmacotherapies are now available. Recent guidelines recommend that all patients expressing an interest in quitting smoking should receive both counseling and pharmacotherapy as appropriate. This care plan is focused on the patient who is motivated to quit smoking.






 Readiness for Weight Management
Readiness for Weight Management
Overweight and obesity are common health problems in the United States, and their prevalence is growing globally. Although multiple factors contribute to overweight (genetics, the biology of one’s regulatory systems, environment, medications, psychological state), the fact remains that most people gain weight because they consume more calories than they expend. Many overweight people have tried short-term fad diets that resulted in temporary weight loss. However, they soon find that losing weight is much easier than keeping it off.
Successful weight management should be approached as a permanent lifestyle change, not simply a quick fix to lose a few pounds for a special event. Slow and gradual weight loss resulting in about 10% of body weight over a 6-month period is a reasonable expectation and one that has shown health benefits, such a reduced blood pressure and glucose and lipid levels.
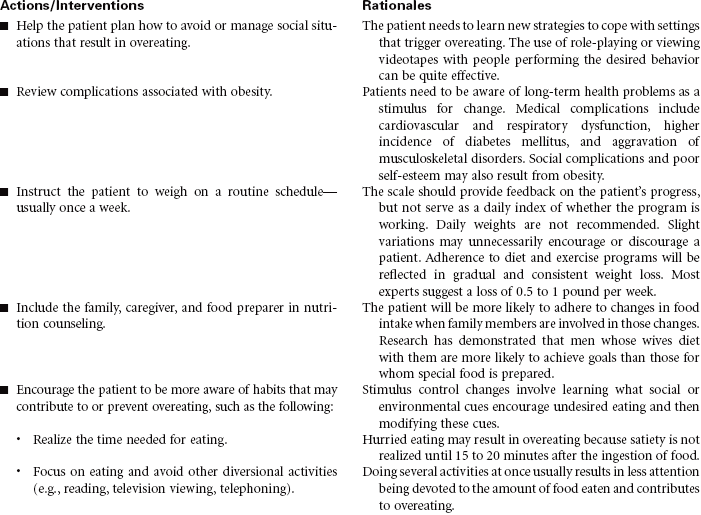
Weight loss readiness is a key to success, as it takes focused time and effort to begin a weight loss program. Making a healthy eating lifestyle change requires establishing a new mindset and habits that become a part of one’s everyday life. Different people may benefit from different approaches to weight loss, but all successful weight management programs contain the same core components: paying careful attention to a reduced-calorie, low-fat diet; participating in ongoing self-monitoring; incorporating physical activity into one’s daily life; using support people or groups; and paying attention to maintaining lifestyle modifications. Multifactorial programs that include behavioral interventions and counseling are more successful than education alone. This care plan focuses on individuals who are ready to begin a weight management program. Note that basic information about healthy food choices can be found in the care plan Readiness for Enhanced Nutrition. Obese individuals with more complex weight issues may benefit from information found in the Bariatric Surgery care plan.












 = Independent
= Independent  = Collaborative
= Collaborative
