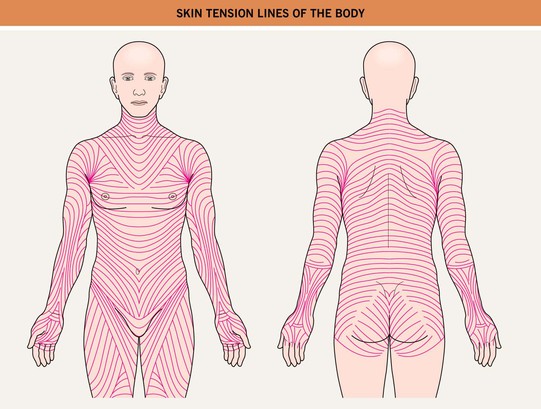
Other Papulosquamous Disorders
Parapsoriasis
• Chronic, usually asymptomatic patches or thin plaques with fine scale whose color varies from pink to red-brown; may have associated epidermal atrophy and occasionally poikiloderma (large plaque parapsoriasis).
• Two major forms of parapsoriasis are small plaque (lesions usually <5 cm in diameter) and large plaque (usually >5 cm); digitate dermatosis is a form of the former, whereas retiform parapsoriasis is a variant of the latter (Figs. 7.1 and 7.2).
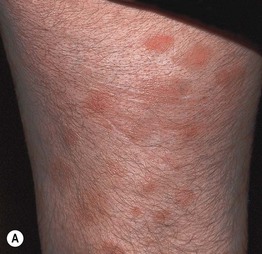
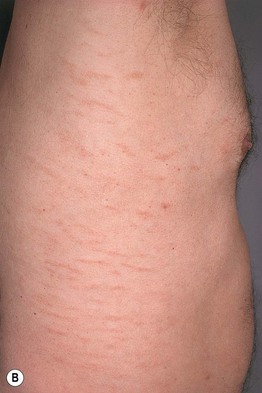
Fig. 7.1 Small plaque parapsoriasis. A Small (<5 cm), pink slight scaly patches. B Digitate dermatosis with elongated finger-like lesions on the flank. Digitate dermatosis is the exception to the 5-cm rule as the lesions may measure 10 cm or more along their long axes. A, Courtesy, Gary Wood, MD, and George Reizner, MD.
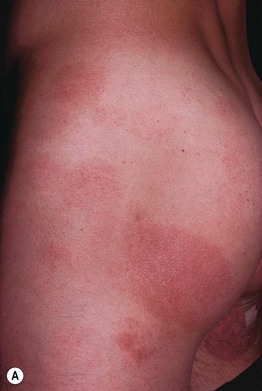
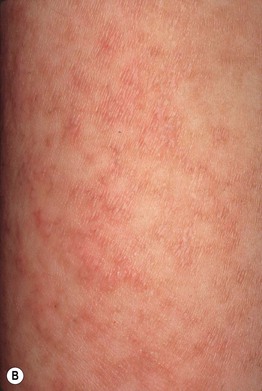
Fig. 7.2 Large plaque parapsoriasis. A Large, red-brown patches in the bathing trunk region – a classic clinical presentation. B Retiform parapsoriasis with pink-brown lesions forming a net-like pattern, hence the term retiform; note the associated wrinkling due to epidermal atrophy.
• While the distribution may be limited or more generalized, there is a tendency for an increase in extent over time; large plaque parapsoriasis can favor the sun-protected ‘girdle’ area; both forms usually occur in adults.
• Controversy exists regarding the percentage of cases of large plaque parapsoriasis that eventually evolve into mycosis fungoides.
• Histologically, parakeratosis and nonspecific spongiotic dermatitis is seen in small and large plaque; large plaque may have a more lichenoid infiltrate.
• Infiltrate of CD4+ T lymphocytes, often clonal, in large plaque > small plaque, leading to the term ‘clonal dermatitis’.
• DDx: small plaque – pityriasis rosea (PR), PR-like drug eruption, pityriasis lichenoides chronica, guttate psoriasis, secondary syphilis; large plaque parapsoriasis – patch stage mycosis fungoides (MF), MF-like drug eruption; if a few lesions, consider tinea corporis.
Pityriasis Lichenoides et Varioliformis Acuta (PLEVA) and Pityriasis Lichenoides Chronica (PLC)
• PLEVA, also known as Mucha–Habermann disease, and PLC exist along a clinicopathologic spectrum such that patients can have characteristic lesions of both disorders, either concurrently or in tandem.
• In both forms, there are recurrent crops of papules with individual lesions spontaneously resolving over weeks (PLEVA) to months (PLC); only occasionally is there an obvious trigger (e.g. viral infection, medication); the entire course of the disorder can last for years.
• PLEVA occurs more commonly in younger age groups; it is characterized by widespread erythematous papules that are often crusted but may be vesicular or pustular (Fig. 7.3A–C).
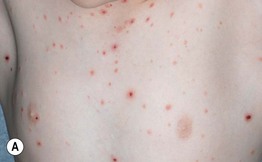
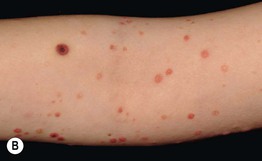
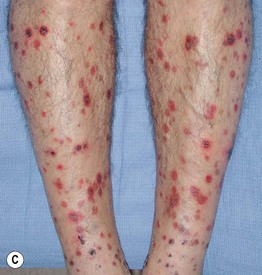
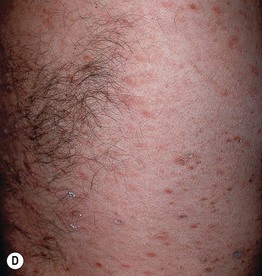
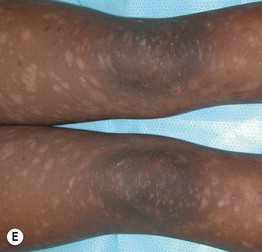
Fig. 7.3 Clinical spectrum of pityriasis lichenoides. In the acute form (PLEVA), widespread erythematous papules and papulovesicles are admixed with crusted lesions (A, B); sometimes there can be an ulcerative component (C). Lesions can heal with varioliform scars. Individuals with the chronic form (PLC) develop multiple red-brown papules, some of which have scale (D); these lesions often heal with hypopigmentation, especially in patients with darkly pigmented skin (E). A, Courtesy, Julie V. Schaffer, MD; B, Courtesy, Thomas Schwarz, MD.
• The onset of PLEVA can be abrupt, and recurrences typically occur for months to years; there is an unusual ulcerative form that is accompanied by fever, lymphadenopathy, arthritis, and mucosal involvement.
• PLC is characterized by pink to red-brown papules with scale and can resolve with post-inflammatory guttate hypopigmentation (Fig. 7.3D,E).
• Histologically, parakeratosis, an interface dermatitis with necrotic keratinocytes, and extravasation of red blood cells are seen; the infiltrate is composed of T cells that are often monoclonal; in PLEVA, the infiltrate may be wedge-shaped and neutrophils may be seen.
• DDx: PLEVA – varicella or other viral exanthem, e.g. Coxsackie, disseminated zoster without a dermatome (more limited duration), lymphomatoid papulosis (often fewer larger lesions), arthropod reactions, small vessel vasculitis; PLC – small plaque parapsoriasis, pityriasis rosea, secondary syphilis, guttate psoriasis, lichen planus.
• Rx: topical CS, prolonged courses of antibiotics (e.g. erythromycin, tetracyclines), phototherapy (e.g. NBUVB); severe cases may require MTX in consultation with a dermatologist.
Pityriasis Rosea
• Occurs more commonly in adolescents and young adults; in general, individuals are healthy and have no systemic complaints/symptoms.
• The etiology is unknown, but viral infections may serve as a trigger.
• Lesions increase in number and extent over a few weeks but then spontaneously resolve; classically, the initial lesion, known as the ‘herald patch,’ is often the largest (Fig. 7.4).
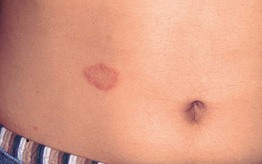
Fig. 7.4 Pityriasis rosea – herald patch. It typically precedes the development of a more widespread eruption. Courtesy, Kalman Watsky, MD.
• The distribution is that of a 1920s bathing suit – proximal extremities and trunk; occasionally, an inverse pattern is seen in which the majority of lesions are in the axillae and/or groin (Fig. 7.5).
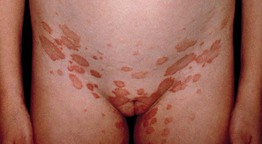
Fig. 7.5 Inverse pityriasis rosea. In this variant, the lesions are limited to the groin and/or axillae. The long axes of the lesions follow the lines of cleavage.
• Pink to salmon-colored papules or plaques are round or oval in shape (Fig. 7.6), with their long axes following Langer's lines of cleavage (Fig. 7.7), creating a ‘Christmas tree’ pattern on the trunk; scale, both fine white centrally and as a collarette at the edge of the lesion, is the most common secondary change, but occasionally crusting, vesicles, purpura, or even pustules may be seen.
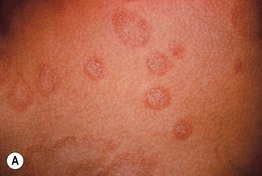
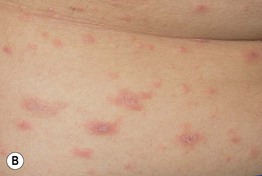
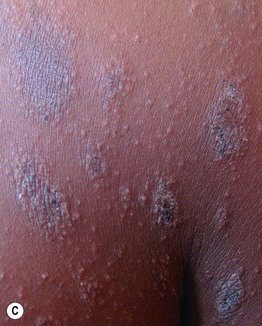
Fig. 7.6 Pityriasis rosea. A, B Both round and oval-shaped plaques can be seen as well as fine white scale and collarettes of scale. C In patients with more darkly pigmented skin, central hyperpigmentation can develop and there may be a more follicular pattern. B, Courtesy, Julie V. Schaffer, MD; C, Courtesy, Aisha Sethi, MD.
• The average duration is 6–8 weeks, with some cases lasting for months.
• Histologically, mounds of parakeratosis are seen, accompanied by spongiosis and a mild perivascular and interstitial lymphocytic infiltrate; extravasation of red blood cells may occur.
• DDx: guttate psoriasis, secondary syphilis (preceding chancre, usually genital; accompanied by malaise, lymphadenopathy, other mucocutaneous signs such as condyloma latum, palmoplantar lesions; positive Venereal Disease Research Laboratory [VDRL] or rapid plasma reagin [RPR] test), pityriasis lichenoides chronica (especially if persistent), nummular dermatitis (if vesicular), pityriasis rosea-like drug eruptions (e.g. ACE inhibitors, metronidazole).
• Rx: topical anti-pruritic lotions or CS (for the minority of patients with associated pruritus), natural sunlight, 14-day course of erythromycin, 10-day course of azithromycin, NBUVB.
Pityriasis Rubra Pilaris
• One of the dermatologic disorders that can lead to an erythroderma (Fig. 7.8), often with an onset in the head and neck region; peaks of incidence – first to second decade of life and sixth decade of life.
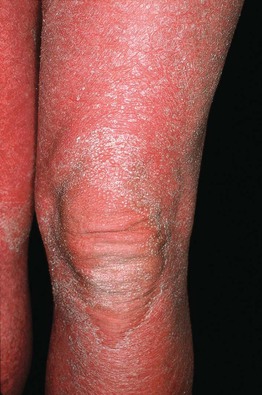
Fig. 7.8 Erythroderma due to pityriasis rubra pilaris. Within areas of erythema, follicular hyperkeratosis (knee) may be more difficult to appreciate than in areas of relative sparing (compare to Fig. 7.9A).
• It is characterized by a salmon or orange-red color, islands of sparing, follicular papules (including within the relatively spared areas and on the dorsal fingers), and a waxy keratoderma (Fig. 7.9).
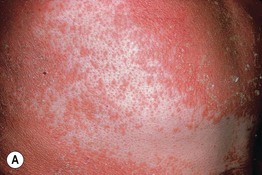
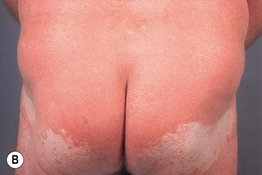
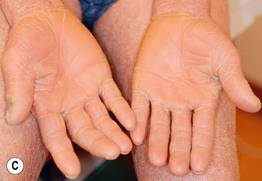
Fig. 7.9 Pityriasis rubra pilaris. A Follicular papules within islands of sparing and confluent orange-red scaly plaques. B The islands of sparing may be sharply demarcated; note the salmon color of the plaques. C Waxy keratoderma, again with an orange hue. C, Courtesy, Irwin Braverman, MD.
• May be exacerbated by exposure to UV light; classic forms spontaneously resolve within 3–5 years (Fig. 7.10).
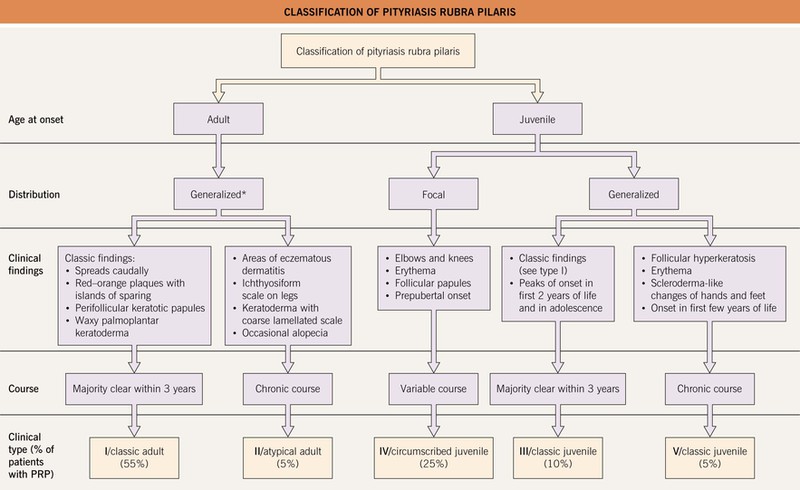
Fig. 7.10 Classification of pityriasis rubra pilaris (PRP). *A generalized distribution of PRP, often with findings similar to type I, may be seen in association with elongated follicular spines, acne conglobata, and hidradenitis suppurativa in HIV-infected individuals; this has been referred to as type VI PRP or the HIV-associated follicular syndrome.
• Five major forms have been described, with distinctions based on age of onset and distribution, with the adult classic form being the most common (Fig. 7.10); occasionally PRP is familial and can be due to CARD14 mutations.
• Histologically, there is alternating ortho- and parakeratosis, both vertically and horizontally, within the stratum corneum (checkerboard pattern); additional findings are follicular plugging with a shoulder of parakeratosis, acantholysis within the epidermis, and variable inflammation.
• DDx: other causes of erythroderma, in particular psoriasis and Sézary syndrome, and an unusual form of dermatomyositis seen more often in Asians (Wong type); in children, also progressive symmetric erythrokeratoderma; early on, seborrheic dermatitis.
• Rx: oral isotretinion, acetretin, methotrexate, tumor necrosis factor-α inhibitors (mixed results); response should be seen within 6 months.
Pityriasis Rotunda
• Seen primarily in the Far East, Mediterranean basin, and Africa; favors individuals with darker skin phototypes.
• Large, asymptomatic, circular and polycyclic patches with scale that are often hyperpigmented; the lesions are also well demarcated and lack inflammation clinically, occurring on the trunk and extremities.
• Associated with malnutrition and secondarily internal malignancies or systemic infections; occasionally, familial, especially in Caucasians.
• Histologically, resembles ichthyosis vulgaris with hyperkeratosis and a reduced granular layer.
• DDx: leprosy, large plaque parapsoriasis, tinea corporis, tinea versicolor.
Granular Parakeratosis
• Originally described in the axillae of adults (primarily women), but can involve other intertriginous zones and in infants, the diaper area.
• Red-brown plaques with scale, often thick, that may be related to chronic irritation (Fig. 7.11); there may be secondary maceration and pruritus.
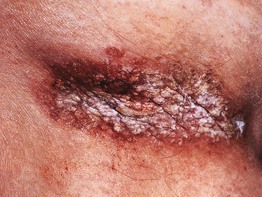
Fig. 7.11 Granular parakeratosis. Brownish-red papules that have coalesced into a keratotic plaque in the axilla. Courtesy, David Mehregan, MD.
• Diagnostic histologic findings of marked compact parakeratosis with retained keratohyaline granules within the stratum corneum.
• DDx: other causes of intertrigo (e.g. seborrheic dermatitis, inverse psoriasis, candidiasis), irritant or allergic contact dermatitis, erythrasma, Hailey–Hailey disease.
• Rx: discontinuation of topical irritants (e.g. mineral salt-containing crystals used as ‘natural’ deodorants, biodegradable diapers), mild topical CS.
For further information see Ch. 9. From Dermatology, Third Edition.