Urticaria and Angioedema
• Urticaria and angioedema can occur at any age and are estimated to have an overall lifetime prevalence of 10–25%.
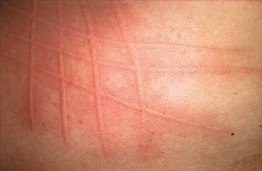
• Urticaria (hives) is characterized by wheals: evanescent, pale to pink-red, edematous papules or plaques (Fig. 14.1); lesions often have central clearing, a peripheral erythematous flare, and associated pruritus.
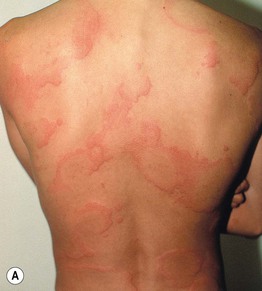
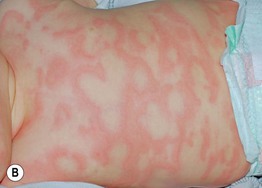
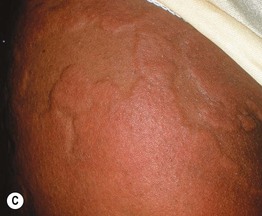
Fig. 14.1 Wheals. Wheals can be small or large in size (A) as well as annular or polycyclic (B), but they still retain the classic central pallor and erythematous flare. C Occasionally, more uniform edematous plaques are seen. B, Courtesy, Julie V. Schaffer, MD.
• Individual wheals last <24 hours, which can be documented by outlining them with ink.
• Angioedema represents deeper dermal and subcutaneous or submucosal swelling (Fig. 14.2); affected areas are ill-defined, have minimal or no overlying erythema, and may be painful as well as pruritic.
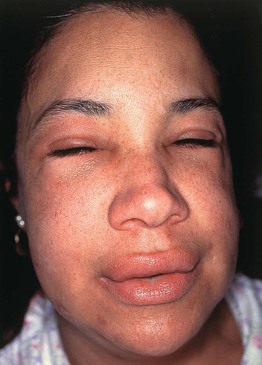
Fig. 14.2 Angioedema. The swelling is deeper than in wheals and may affect mucosal surfaces. Note the swelling of the lips and periorbital region and the lack of erythema. Courtesy, Clive E. H. Grattan, MD.
• In addition to the skin/subcutis, angioedema can affect the mouth and respiratory or gastrointestinal tract; an area of swelling may persist for several days.
• A classification scheme and DDx for urticaria and angioedema are presented in Table 14.1; patients with angioedema may have associated urticaria, including physical urticaria.
Table 14.1
Classification and differential diagnosis of urticaria and angioedema.

* Urticaria occurring less frequently than this over a long period is referred to as episodic or recurrent.
† Individual lesions tend to last >24 hours; urticarial vasculitis features burning/pain, purpura upon resolution, and a subgroup associated with hypocomplementation and autoimmune connective tissue disease (e.g. SLE).
** Consider for chronic urticaria with associated symptoms such as fevers, pain, and arthralgias.
SLE, systemic lupus erythematosus.
• Urticaria and urticaria-associated angioedema result from the release of histamine and other proinflammatory and vasoactive substances from mast cells; this leads to extravasation of plasma, vasodilatation, and pruritus.
• Stimuli for mast cell degranulation are shown in Fig. 14.3.
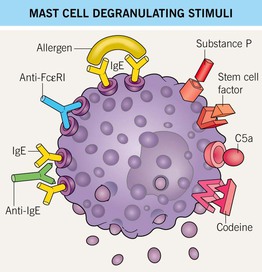
Fig. 14.3 Mast cell degranulating stimuli. Both immunologic and non-immunologic stimuli can lead to release of mediators. Stem cell factor is also known as KIT ligand. Autoantibodies against the high-affinity IgE receptor (FcεRI) and the Fc portion of IgE are implicated in chronic autoimmune urticaria.
Spontaneous (‘Ordinary’) Urticaria: Acute and Chronic
• Although both can occur at any age, acute urticaria is most common in children, whereas chronic urticaria has a peak in the fourth decade of life and a female : male ratio of ~2 : 1.
• The most frequent causes of acute and chronic urticaria are listed in Table 14.2.
Table 14.2
Causes of acute and chronic spontaneous urticaria.

FcεRI, high-affinity IgE receptor (present on mast cells); IgE, immunoglobulin E; URI, upper respiratory tract infection.
• Acute urticaria in young children often presents with large annular or polycyclic lesions (urticaria ‘multiforme’; see Figs. 14.1B and 3.3A) that tend to resolve with a transient dusky purplish hue, which can lead to misdiagnosis as erythema multiforme.
• Urticaria can result in sleep disturbances and anxiety.
• Chronic autoimmune urticaria is associated with an increased risk of other autoimmune conditions, such as thyroid disorders and celiac disease.
• An approach to the diagnosis of chronic urticaria is outlined in Fig. 14.4; extensive laboratory evaluations (e.g. for food allergies) are extremely low-yield and are not recommended.
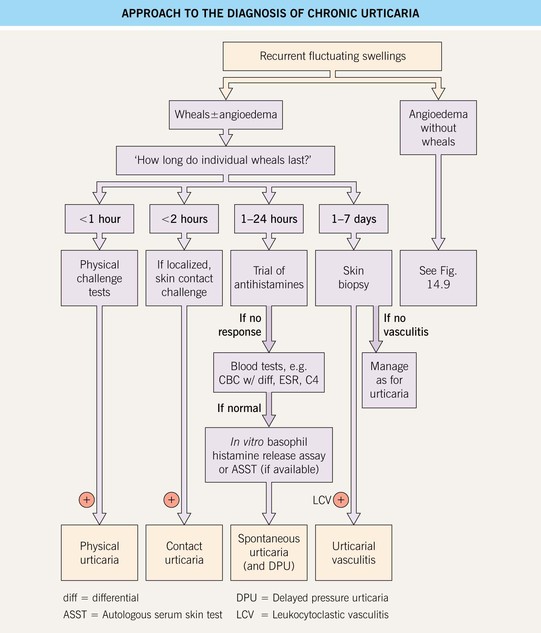
Fig. 14.4 Approach to the diagnosis of chronic urticaria. In a positive ASST, a localized wheal and flare response occurs upon intradermal injection of autologous serum, providing evidence of functional histamine-releasing factors in the blood. Regulations regarding blood products limit the availability of this test. Courtesy, Clive E. H. Grattan, MD.
• Rx: a stepwise therapeutic approach is presented in Fig. 14.5; long-acting antihistamines are the mainstay of treatment, and systemic corticosteroids should be avoided.
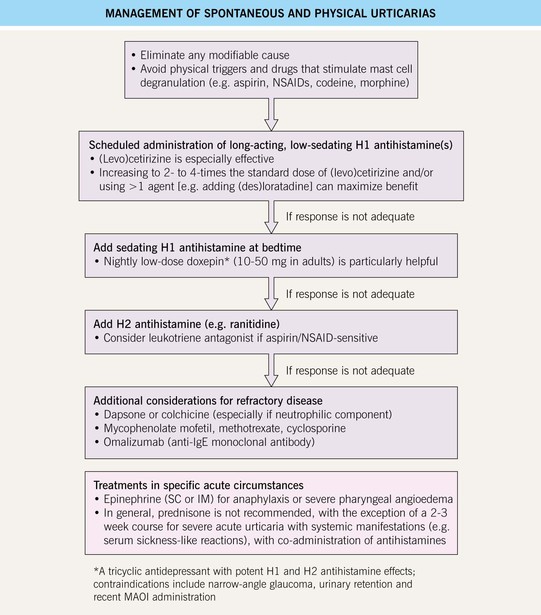
Fig. 14.5 Management of spontaneous and physical urticarias. IM, intramuscular; IVIg, intravenous immunoglobulin; MAOI, monoamine oxidase inhibitor; SC, subcutaneous.
Physical (Inducible) Urticaria
• Different forms of physical urticaria may coexist with one another and/or chronic spontaneous urticaria.
• Rx: see Fig. 14.5.
Dermographism (‘Skin Writing’)
• Affects at least 10% of the general population; may lead to symptoms such as pruritus.
• Linear or irregularly shaped wheals develop at sites of scratching or friction (Fig. 14.6); lesions typically resolve within an hour.
• Can elicit via stroking the skin, e.g. with a thin wooden stick or tongue depressor.
Delayed Pressure Urticaria
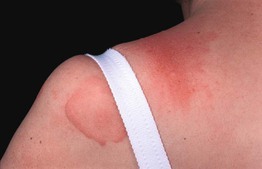
• Pruritic and/or painful erythema and swelling (Fig. 14.7) develop 0.5–12 hours after sustained pressure to the skin (e.g. due to tight clothing or shoes); may last several days, sometimes with associated arthralgias and malaise.
Cold Urticaria
• Wheals ± angioedema develop within minutes of cold exposure, with maximal hiving upon rewarming; systemic reactions (e.g. anaphylaxis) may occur with aquatic activities.
• Can elicit via ice cube test (Fig. 14.8; 1- to 10-minute application within glove, then rewarming).
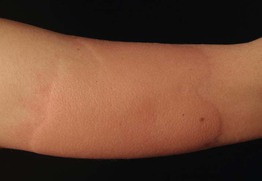
Fig. 14.8 Cold urticaria. Wheals developed on the forearm after placement of an ice cube for 10 minutes, followed by rewarming. Courtesy, Thomas Schwarz, MD.
• Usually primary; <5% of cases are associated with cryoglobulins or cryofibrinogen.
• Rare early-onset variants with autosomal dominant inheritance and a negative ice cube test: cryopyrin-associated periodic syndrome (see Table 3.2), familial atypical cold urticaria (wheals upon evaporative cooling; PLCG2 mutations).
Cholinergic Urticaria
• Multiple small (2–3 mm), monomorphic, pruritic wheals with an erythematous flare develop within 15 minutes of sweat-inducing stimulus (e.g. physical exertion, emotional stress, hot bath); favors the upper body but may be widespread.
• DDx: adrenergic urticaria (blanched halo rather than flare), heat urticaria (can occur without sweating), exercise-induced urticaria/anaphylaxis (only with exercise, not a hot bath), aquagenic urticaria (upon contact with water of any temperature).
Solar Urticaria
• Pruritus and wheals within 5–10 minutes of exposure to UVA and/or visible light > UVB (see Chapter 73).
Contact Urticaria
• Immunologic contact urticaria presents with localized pruritus and hives within 30 minutes of handling fresh vegetables/fruits or contact with latex in sensitized individuals; occasionally generalizes, and ‘protein contact dermatitis’ may occur with repeated exposure (especially in atopic patients).
• Evaluation of suspected type 1 latex allergy initially involves a blood test for specific IgE; if negative, a prick test with latex extract can be performed in a controlled setting and, if there is no reaction, confirmed with a usage test (e.g. wearing the suspect glove).
• ‘Oral allergy syndrome’ presents with intraoral itching and swelling in individuals with a pollen allergy upon ingestion of cross-reacting fresh fruits or vegetables.
• Non-immunologic contact urticaria results from exposure to plants containing toxins (e.g. histamine) within sharp ‘hairs’ on their leaves (e.g. stinging nettles).
Schnitzler's Syndrome
• Chronic urticaria ± pruritus associated with a monoclonal gammopathy (IgM >> IgG).
• Other features include fevers, arthralgias, bone pain, lymphadenopathy, leukocytosis, and an increased ESR; patients may develop a lymphoproliferative malignancy.
• Rx: prednisone, anakinra, and rituximab, as well as treatment of the underlying disorder.
Hereditary Angioedema (HAE)
• HAE due to deficiency (type I) or dysfunction (type II) of the complement C1 esterase inhibitor is an uncommon autosomal dominant disorder that presents with episodic nonpruritic angioedema lasting 2–3 days, often beginning in early childhood and triggered by trauma; although not associated with true urticaria, attacks are occasionally preceded or accompanied by transient, nonpruritic, serpiginous erythematous patches.
• Type I/II HAE favors the extremities and gastrointestinal tract (may mimic an acute abdomen), and airway compromise due to laryngeal edema can occur.
• Type III HAE is a later-onset form with more frequent facial involvement that develops primarily in teenage girls and young women.
• Pathogenesis of HAE is related to excessive generation of bradykinin, which leads to increased vascular permeability.
• Evaluation and DDx: outlined in Fig. 14.9.
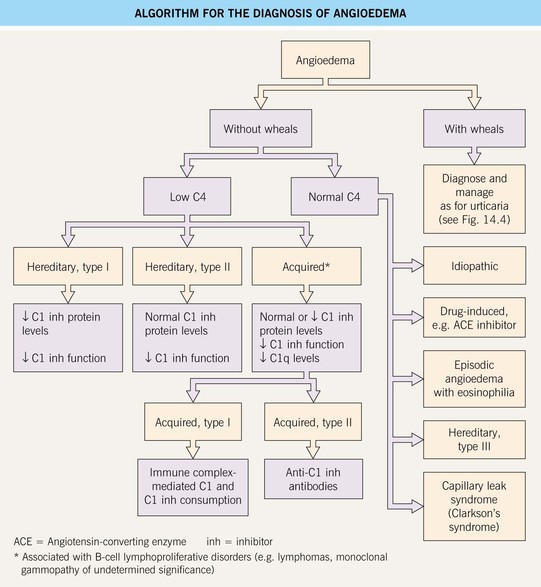
Fig. 14.9 Algorithm for the diagnosis of angioedema. Episodic angioedema with eosinophilia as well as weight gain and fever is known as Gleich syndrome. Systemic capillary leak syndrome can lead to life-threatening hypotension and is associated with an IgG monoclonal gammopathy.
• Rx: acute attacks or short-term prophylaxis (e.g. for surgical or dental procedures) – intravenous C1 inhibitor concentrate > subcutaneous ecallantide (kallikrein inhibitor) or icatibant (bradykinin B2 receptor antagonist); long-term treatment – androgens (e.g. oral danazol) > antifibrinolytic agents; antihistamines, epinephrine, and corticosteroids are not effective.
For further information see Ch. 18. From Dermatology, Third Edition.