Other Vesiculobullous Diseases
There are a number of disorders that can present with vesicles and bullae, including exaggerated insect bite reactions (see Chapter 20), autoimmune and inherited blistering diseases (see Chapters 23–26), porphyrias (see Chapter 41), the Stevens–Johnson syndrome–toxic epidermal necrolysis spectrum (see Chapter 16), and phototoxicity, from sunburn to phototoxic drug reactions (e.g. due to doxycycline). This chapter examines a miscellaneous group of disorders, several of which favor the lower extremities, whereas Chapter 28 reviews vesiculobullous diseases in newborns and infants.
Friction Blisters
• Most commonly develop on the heels, soles, and palms; the blister develops within the epidermis, contains clear or hemorrhagic fluid (‘blood blister’), and heals spontaneously without scarring.
• Due to repeated friction (e.g. prolonged walking in ill-fitting shoes) and repetitive actions (e.g. raking leaves).
• DDx: if exaggerated response, can consider inherited blistering disease, in particular the localized form of epidermolysis bullosa simplex (see Chapter 26).
• Rx: if significant fluid accumulation, drainage of fluid can relieve pressure; the roof of the blister should be left in place to act as a ‘natural Band-Aid’; secondary soft tissue infection is unusual in immunocompetent individuals.
Edema Bullae (Edema Blisters)
• The bullae are bland (i.e. non-inflammatory), initially tense, and may reach several centimeters in diameter; they arise within areas of significant edema and contain sterile, usually clear but occasionally blood-tinged, fluid.
• The most common location is the distal lower extremities, often in the setting of an acute exacerbation of chronic edema in an elderly patient; in patients with anasarca and those who are bedridden, the distribution can be more widespread (Fig. 27.1).
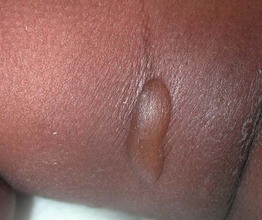
Fig. 27.1 Edema bullae on the thigh of an infant. The bullae are tense and are surrounded by edema. Desquamation from a ruptured bulla is also seen.
• DDx: bullosis diabeticorum and bullous pemphigoid, including the variant localized to the lower extremities; if there is surrounding erythema, warmth and tenderness, then bullous cellulitis needs to be excluded.
• Rx: as bullae resolve in concert with the edema, only drainage of larger bullae needs to be considered (see below).
Bullosis Diabeticorum (Diabetic Bullae)
• In patients with diabetes mellitus, tense bland bullae arise rather suddenly within normal-appearing skin (Fig. 27.2); the diameter varies from 0.5 to several centimeters; the blister fluid is sterile and clear, but may be more viscous than that of friction or edema blisters.
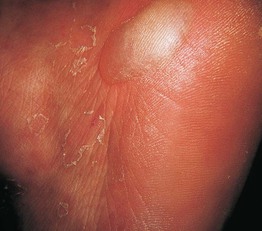
Fig. 27.2 Bullosis diabeticorum. A tense blister on the palm as well as desquamation at sites of previous bullae. Courtesy, José M. Mascaró Jr., MD.
• Most commonly develops on the distal extremities (lower > upper) of adults and may be accompanied by peripheral neuropathy.
• DDx: bullous pemphigoid, epidermolysis bullosa acquisita, porphyria cutanea tarda, pseudoporphyria, bullous impetigo, and if significant edema, edema bullae; given the increased risk of soft tissue infections in diabetics, the possibility of bullous cellulitis needs to be excluded if there is surrounding erythema.
• Rx: placing a small window in a dependent location in the roof of the blister allows for both drainage and preservation of the blister roof; no further treatment is required for uncomplicated lesions, as they spontaneously heal over 3–6 weeks.
Delayed Postburn/Postgraft Blisters
• Tense vesicles or bullae may develop within areas of previous thermal burns as well as within recipient or donor skin graft sites; occur weeks to months after initial injury has healed.
• Possible explanation is enhanced fragility due to a less mature basement membrane zone within the healing wound.
• DDx: limited given specific distribution, but includes ischemia within graft recipient sites, herpetic infections, bullous impetigo, and occasionally autoimmune bullous diseases (locus minoris resistentiae phenomenon).
• Rx: supportive as lesions heal spontaneously, but can recur.
Coma Bullae (Coma Blisters)
• Tense cutaneous vesicles and bullae can appear within 2 or 3 days of prolonged pressure secondary to immobilization (Figs. 27.3 and 27.4); there is often preceding blanchable erythema.
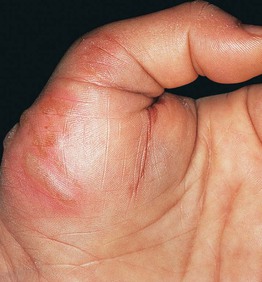
Fig. 27.3 Coma bullae. Blisters developed in an area of pressure in a previously comatose patient. Courtesy, José M. Mascaró Jr., MD.
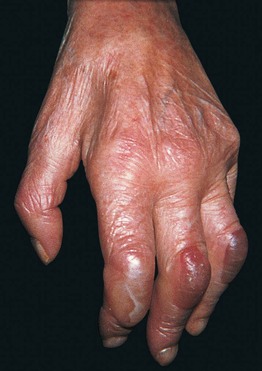
Fig. 27.4 Neurologic blisters. Tense blisters on the dorsal aspect of the fingers on the hemiplegic side of a patient with a previous cerebrovascular accident. Courtesy, José M. Mascaró Jr., MD.
• The bullae develop at sites of maximum pressure and therefore often develop in the skin overlying joints or bony prominences.
• The prolonged pressure may occur in the setting of a coma, whose cause can vary from drug-induced to metabolic (e.g. hepatic encephalopathy); immobility can also result from neurologic disorders, especially cerebral vascular accidents.
• Characteristic histologic finding of necrosis of eccrine sweat glands, presumably secondary to local hypoxia.
• DDx: usually limited if history of immobilization obtained and distribution pattern limited to pressure points appreciated.
• Rx: supportive as lesions heal over 1 or 2 weeks; prevention requires frequent repositioning of the patient.
For further information see Ch. 33. From Dermatology, Third Edition.