Disorders of Eccrine and Apocrine Glands
Eccrine and apocrine glands represent the two major types of sweat glands (see Fig. 91.1).
Eccrine Glands
• Functional from birth and activated by thermal stimuli via the hypothalamic sweat center; while their major function is thermoregulation by evaporative heat loss, they are also activated by emotional stimuli.
• Innervated by sympathetic fibers that have acetylcholine as their major neurotransmitter.
• Generalized distribution, with greatest concentration on the palms and soles.
• The eccrine duct opens directly onto the skin surface, and the excretory product is a clear hypotonic fluid that is mostly water but also contains NaCl.
Apocrine Glands
• Unclear function in humans; functional development requires androgens.
• More limited distribution – primarily axillae, nipples/areolae, and umbilical and anogenital regions; modified apocrine glands are found in the external auditory canals and eyelid margins.
• The apocrine duct drains into the superficial portion of the hair follicle (see Fig. 91.1).
• ‘Decapitation’ of apocrine gland cells produces an odorless and viscous fluid; however, its degradation by flora on the skin surface can lead to an odor.
Hyperhidrosis
• Excessive production of eccrine sweat is usually due to primary cortical (emotional) hyperhidrosis and the favored sites are the axillae or palms and soles (Fig. 32.1) > the face (Fig. 32.2); involvement is bilateral and symmetric.
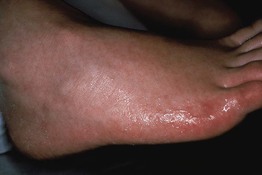
Fig. 32.1 Volar hyperhidrosis (primary cortical). The palmoplantar skin displays excessive eccrine sweat production, including the portions that extend onto the sides of the hands, feet, and digits. Its onset is during childhood as opposed to axillary hyperhidrosis, which has its onset around puberty.
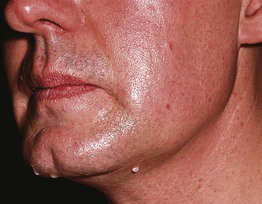
Fig. 32.2 Primary cortical (emotional) hyperhidrosis involving the face. Sweat droplets are evident on the upper cutaneous lip, jawline, and chin. Reproduced from Hurley HJ. Hyperhidrosis. Curr. Opin. Dermatol. 1997;4:105–114. Philadelphia: Rapid Science Publishers.
• Secondary cortical hyperhidrosis is associated with genodermatoses, including palmoplantar keratodermas and epidermolysis bullosa simplex; associated odor reflects maceration and degradation of keratin by bacteria.
• Secondary hypothalamic (thermoregulatory) hyperhidrosis can be due to a number of systemic diseases, from infections to neoplasms (Table 32.1).
Table 32.1
Causes of secondary hypothalamic hyperhidrosis.

CNS, central nervous system; CVA, cerebrovascular accident; MAOI, monoamine oxidase inhibitor; RSD, reflex sympathetic dystrophy, also referred to as complex regional pain syndrome; SSRI, selective serotonin reuptake inhibitor. Linezolid is an MAOI.
• Secondary medullary (gustatory) hyperhidrosis can be physiologic as exemplified by the facial sweating that occurs with spicy foods or pathologic as occurs in Frey's syndrome (Fig. 32.3); in the former, taste receptors send afferent impulses, whereas in the latter, disrupted nerves for sweat aberrantly connect with nerves for salivation.
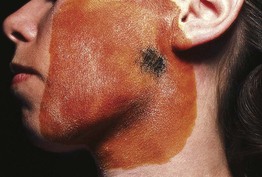
Fig. 32.3 Gustatory sweating in the auriculotemporal (Frey's) syndrome, as a consequence of parotid surgery. The blue-black area represents sweating (starch–iodine technique). Salivary stimulation induced this sweating response. Reproduced from Hurley HJ. Hyperhidrosis. Curr. Opin. Dermatol. 1997;4:105–114. Philadelphia: Rapid Science Publishers.
• Injuries or diseases affecting the spinal cord can result in segmental hyperhidrosis.
• In addition to embarrassment, hyperhidrosis can lead to overhydration of the skin and a higher risk of bacterial and fungal infections.
• Sweating only during waking hours points to primary cortical (emotional) hyperhidrosis; after consideration of possible underlying etiologies, topical antiperspirants containing aluminum chloride (e.g. Certain-Dri®) or aluminum chloride hexahydrate (e.g. Xerac-AC® [6.25%], Drysol® [20%]) can be applied, and if necessary, initially preceded by oral glycopyrrolate or oxybutynin.
• Injection of botulinum toxin type A every ~6 months is very effective for primary cortical (emotional) hyperhidrosis (Fig. 32.4); tap water iontophoresis is less effective.
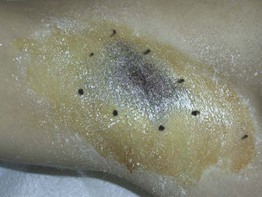
Fig. 32.4 Delineation of area for injections of botulinum toxin A for axillary hyperhidrosis (starch–iodine technique). Blue-black areas represent foci of sweating. In the case of onabotulinumtoxin A, a total of 50–100 U is injected, utilizing 10–15 injection sites. Courtesy, Alastair Carruthers, MD, and Jean Carruthers, MD.
Hypohidrosis (and Anhidrosis)
• There are multiple etiologies of hypohidrosis and anhidrosis including the following:
– A side effect of medications with anticholinergic properties (e.g. atropine, tricyclic antidepressants, glycopyrrolate).
– Manifestation of inherited disorders, in particular ectodermal dysplasias (see Chapter 52), as well as acquired disorders such as Sjögren's syndrome.
– Neurologic disorders, from tumors or infarcts of the hypothalamus, pons, or medulla to peripheral neuropathies.
• Increased risk of developing hyperthermia.
• Evaluation includes colorimetric testing (see Fig. 32.4) and biopsy of affected skin.
Bromhidrosis (Foul-Smelling Sweat)
• Eccrine variant associated with degradation of sweat by resident microflora; most commonly involves the feet.
• Apocrine variant associated with degradation of odiferous substances (e.g. triglycerides) by skin flora.
• The smell can be rancid (Corynebacterium) or sweaty (Micrococcus).
Chromhidrosis
• Colored sweat can be intrinsic and due to the lipofuscin content of apocrine sweat (yellow, green, black) or extrinsic and due to staining of sweat by clothing or chromogenic bacteria (e.g. Corynebacterium) or fungi.
Sweat Retention Disorders
Miliaria
• Excessive sweating leads to maceration and blockage of eccrine ducts; can be exacerbated by occlusion, e.g. clothing, athletic equipment, prolonged bed rest.
• Classically divided into three major types: (1) crystallina – tiny, superficial, short-lived, clear vesicles (Fig. 32.5A; see Fig. 28.3); (2) rubra (prickly heat) – pruritic erythematous papulovesicles and occasionally pustules that favor the upper trunk (Fig. 32.5B); and (3) profunda – white papules due to excessive sweating in a hot climate (rare); these three forms reflect ductal occlusion within the stratum corneum, mid-epidermis, and dermal–epidermal junction, respectively.
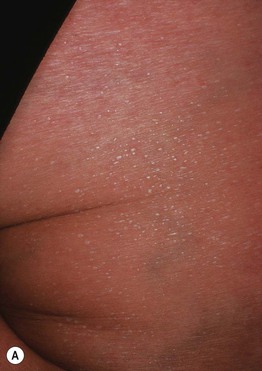
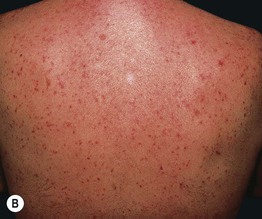
Fig. 32.5 A Miliaria crystallina. Multiple small superficial vesicles with clear fluid. B Miliaria rubra. Multiple erythematous nonfollicular papules and papulovesicles on the back.
• If extensive, decrease in eccrine function can give rise to hyperpyrexia.
• DDx: miliaria rubra needs to be distinguished from folliculitis, Grover's disease, neutrophilic eccrine hidradenitis, and cutaneous candidiasis.
Fox–Fordyce Disease (Apocrine Miliaria)
• Occlusion then rupture of apocrine sweat gland ducts in the axillae > anogenital or periareolar region > periumbilical or presternal area; seen primarily in women ages 15–35 years.
• Multiple skin-colored papules that are follicular, dome-shaped, and often pruritic (Fig. 32.6).
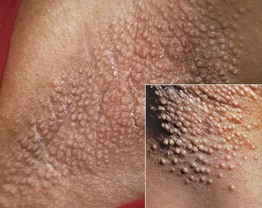
Fig. 32.6 Fox–Fordyce disease. Monomorphic skin-colored papules in the axillary vault. The dome shape is appreciated in the insert.
• May improve with oral contraceptive pills (OCPs) or pregnancy.
Hidradenitis
Neutrophilic Eccrine Hidradenitis
• Most commonly related to administration of chemotherapy (e.g. cytarabine) and is thought to result from excretion of the drug(s) into the eccrine sweat, leading to a toxic insult.
• Erythematous papules and plaques that may have clinical overlap with Sweet's syndrome (Fig. 32.7).
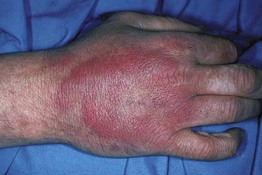
Fig. 32.7 Neutrophilic eccrine hidradenitis. Pink annular plaque on the dorsal hand. Courtesy, Jami L. Miller, MD.
• Rx: spontaneously resolves but sometimes a short course of systemic CS is prescribed once an infectious process such as cellulitis or septic emboli is excluded.
Idiopathic Palmoplantar Hidradenitis
• Occurs following vigorous physical activity, primarily in healthy children.
• Thought to be precipitated by rupture of eccrine glands.
• Erythematous, tender nodules appear suddenly, most often on the soles (Fig. 32.8), and then spontaneously resolve over days to weeks.
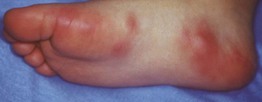
Fig. 32.8 Idiopathic palmoplantar hidradenitits. Tender erythematous papules and nodules on the plantar surface. Courtesy, Michael L. Smith, MD.
• DDx: Pseudomonas hot-foot syndrome, pernio, symmetric lividity of the soles, delayed pressure urticaria.
Other
Keratolysis Exfoliativa
• Common disorder in healthy individuals; affects the palms >> soles.
• Multiple annular and semi-annular collarettes of white scale that usually measure <5 mm, but may be larger (Fig. 32.9); no preceding vesicles or inflammation clinically.
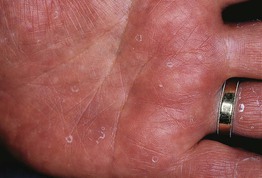
Fig. 32.9 Keratolyis exfoliativa. Small annular collarettes of scale on the palm. Courtesy, Jean L. Bolognia, MD.
• Recurrent and sometimes associated with hyperhidrosis.
• Rx: nonspecific; effectiveness of topical agents, e.g. 12% ammonium lactate, 20% urea, is limited.
For further information see Chs. 35 and 39. From Dermatology, Third Edition.