Mucinoses
In this group of disorders, there is deposition of glycosaminoglycans, previously referred to as mucopolysaccharides (‘mucin’), within the skin, especially the dermis. Most frequently, the deposit is composed of hyaluronic acid. While several of the entities are idiopathic, underlying disorders include autoimmune thyroid disease, a monoclonal gammopathy, and diabetes mellitus.
Scleredema
• Symmetric diffuse induration of the skin, usually limited to the upper back and posterior neck, that may require palpation to be appreciated; a peau d'orange appearance may be present with prominent follicular orifices, and occasionally there is blanching erythema in the sites of involvement (Fig. 38.1).
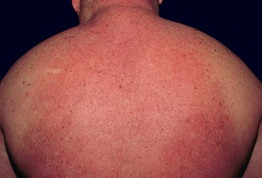
Fig. 38.1 Scleredema in association with diabetes mellitus. Diffuse induration of the upper back and neck with overlying erythema.
• While scleredema is often asymptomatic, some patients may complain of tightness or decreased range-of-motion; occasionally there is also involvement of the face and upper extremities and rarely, the muscles, eyes, or heart.
• The three major types have different associations: type I – preceding streptococcal infections; type II – monoclonal gammopathy; and type III – diabetes mellitus, with men representing the majority of patients.
• DDx: systemic sclerosis (diffuse form), scleromyxedema, and other sclerodermoid disorders (see Table 35.4); occasionally, cellulitis if erythema is present.
• Rx: sometimes there is spontaneous resolution, especially with type I disease, but control of underlying diabetes mellitus does not lead to improvement; anecdotal therapies include phototherapy (e.g. UVA1, PUVA) and electron beam therapy.
Scleromyxedema/Papular Mucinosis
• A spectrum of clinical findings that varies from multiple linear arrays of firm, 2- to 3-mm, waxy, skin-colored papules (Fig. 38.2) to diffuse induration of the skin with thickened folds, including leonine facies (Fig. 38.3; Table 38.1); involvement is symmetric and often widespread.
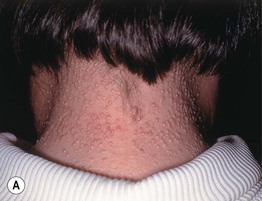
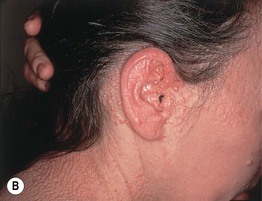
Fig. 38.2 Scleromyxedema/papular mucinosis. A, B Numerous monomorphic, firm, skin-colored papules which can have a linear arrangement (most obvious on the upper back).
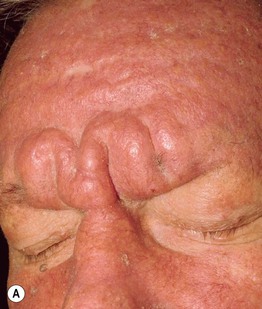
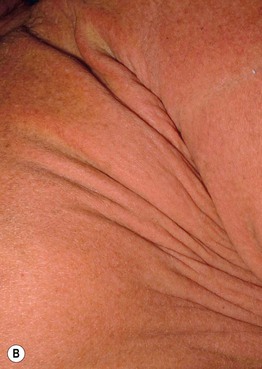
Fig. 38.3 Scleromyxedema/papular mucinosis. Thickening of the skin of the forehead (A) and trunk (B), leading to deep furrows and folds. Scleromyxedema is one of the causes of leonine facies. Courtesy, Joyce Rico, MD.
Table 38.1
Leonine facies – associated dermatologic diseases.
Additional causes include sarcoidosis, mastocytosis, multicentric reticulohistocytosis, and progressive nodular histiocytosis.

• Associated with an underlying monoclonal gammopathy; in addition to skin stiffness, there can be decreased range-of-motion of joints and contractures as well as myositis, peripheral neuropathy, and encephalopathy (dermato-neuro syndrome).
• DDx: systemic sclerosis, scleredema; if primarily papules, primary systemic amyloidosis, lipoid proteinosis, and especially the various types of skin-limited (localized) mucinoses, e.g. acral persistent papular mucinosis, self-healing cutaneous mucinosis, the discrete papular form of lichen myxedematosus.
• Rx: similar to that of multiple myeloma (see primary systemic amyloidosis, Chapter 39), systemic retinoids, PUVA, UVA1.
Pretibial Myxedema
• In the vast majority of patients, associated with hyperthyroidism, primarily due to Graves' disease, an autoimmune disorder with circulating anti-thyroid-stimulating hormone receptor autoantibodies; lesions may appear following treatment of the thyroid disease, i.e. when the patient is euthyroid or hypothyroid.
• Favors the shins but can involve the foot and presents as indurated, waxy nodules or plaques that vary from skin-colored to red-brown (Fig. 38.4); there can be a prominence of follicular openings (peau d'orange appearance) and occasionally elephantiasis develops.
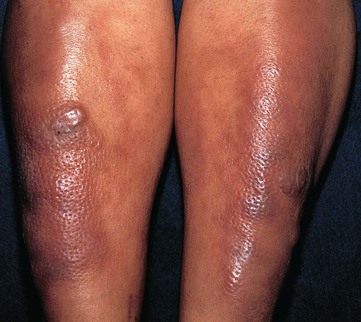
Fig. 38.4 Pretibial myxedema. Purple-brown plaques on the shins of a patient with Graves' disease. A peau d'orange appearance is present due to prominent follicular openings. Courtesy, Franco Rongioletti, MD, and Alfredo Rebora, MD.
• Additional clinical findings include exophthalmos, goiter, and thyroid acropachy.
• DDx: obesity-associated lymphedematous mucinosis (no history of hyperthyroidism), lymphedema, lipedema, lichen amyloidosis.
• Rx: although lesions may clear spontaneously over a period of several years, treatment of the underlying thyroid disease usually has no effect; anecdotal therapies include topical and intralesional CS, pneumatic compression, surgical shave removal, octreotide.
Generalized Myxedema
• As a result of profound hypothyroidism, the skin is diffusely dry, cool, and pale, with a waxy appearance; the hair and nails can be brittle, leading to a diffuse non-scarring alopecia of the scalp and alopecia of the lateral eyebrows.
• Additional mucocutaneous findings include eczema craquelé, acquired ichthyosis, carotenoderma, and a puffiness of the hands and the face, including the eyelids; the tongue may be enlarged.
• In the congenital form, mental retardation, dwarfism, poor muscle tone, constipation, and somnolence are characteristic findings.
• Because the most common underlying disease in adults is Hashimoto's thyroiditis, women are more commonly affected; in addition to the skin changes outlined above, patients may gain weight, have cold intolerance and constipation, feel sluggish, and can occasionally develop cutaneous xanthomas.
Self-Healing Cutaneous Mucinosis
• Acute eruption of multiple firm papules and nodules favoring the face (especially the forehead and periorbital region), scalp, and periarticular areas.
• No underlying disorder and characterized by spontaneous resolution over months to years.
Reticular Erythematous Mucinosis (REM)
• Persistent erythematous papules of the central chest and central back that can form a net-like pattern and/or coalesce into plaques (Fig. 38.5); may be photo-aggravated.
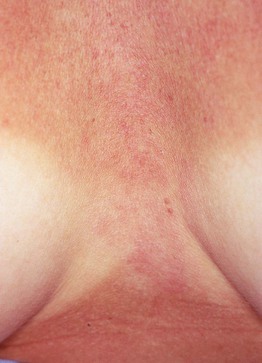
Fig. 38.5 Reticular erythematous mucinosis (REM). Grouped pink papules on the central chest with no surface changes; there is a subtle annular and reticulated configuration. Note the significant tan.
• Overlaps with lupus erythematosus (LE) tumidus, Jessner's benign lymphocytic infiltrate (minimal to no dermal mucin), and papulonodular mucinosis (see below).
• Rx: topical or intralesional CS, antimalarials, e.g. hydroxychloroquine, chloroquine, sunscreens.
Cutaneous Lupus Mucinosis/Papulonodular Mucinosis (of Gold)
• Occurs in the setting of autoimmune connective tissue diseases, with LE >> dermatomyositis or systemic sclerosis; ~75% of patients with LE who develop these lesions have systemic involvement.
• Skin-colored to erythematous papules and nodules that may require side-lighting to appreciate; favors the back, V of the chest and upper extremities (Fig. 38.6).
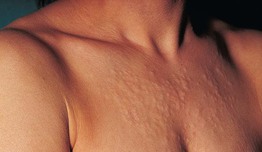
Fig. 38.6 Cutaneous lupus mucinosis/papulonodular mucinosis. Skin-colored papules and nodules leading to a ‘lumpy’ appearance to the skin that is best appreciated by side-lighting. Courtesy, Franco Rongioletti, MD, and Alfredo Rebora, MD.
• Overlaps with LE tumidus, reticular erythematous mucinosis, and Jessner's benign lymphocytic infiltrate (minimal to no dermal mucin).
• Rx: antimalarials, e.g. hydroxychloroquine, chloroquine, topical or intralesional CS, sunscreens.
Follicular Mucinosis (Alopecia Mucinosis)
• In contrast to the other disorders in this chapter, here the mucin is deposited within the epithelium of hair follicles rather than in the dermis.
• In the primary form, there are pink to violet-brown plaques, primarily in the head and neck region, that have associated alopecia and sometimes scale (Fig. 38.7A); in some patients, there are grouped follicular papules (Fig. 38.7B), and in patients with darkly pigmented skin, lesions may be hypopigmented.
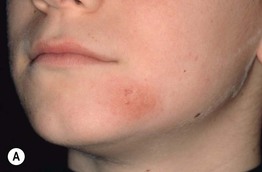
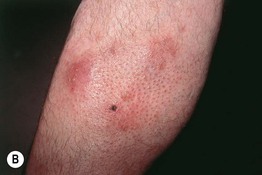
Fig. 38.7 Follicular mucinosis. A Pink plaque containing follicular papules in a young boy. B Grouped follicular papules on the leg of an older adult in association with violet-brown plaques; note the associated alopecia. The hemorrhagic crust is the site of a previous biopsy. A, Courtesy, Lorenzo Cerroni, MD.
• The primary form most commonly occurs in children and young adults and represents a benign, self-limited disease; in older adults, especially when the lesions are more widespread and persistent, the possibility of coexisting mycosis fungoides needs to be considered.
• In addition to the characteristic histologic finding of mucin deposition within the follicular epithelium, it is important to comment on the presence or absence of atypical lymphocytes.
• DDx: cutaneous LE, tinea faciei or capitis, facial discoid dermatosis, various forms of dermatitis; if diagnosed histologically, consider an incidental finding (e.g. associated with atopic dermatitis).
• Rx: for primary, observation until spontaneous resolution, topical or intralesional CS, antimalarials; if associated with mycosis fungoides, treat the latter (see Chapter 98).
Other Entities
Digital mucous cyst is covered in Chapter 90. Cutaneous mucin deposits can also be seen within tumors (e.g. basal cell carcinomas, cutaneous metastases) and inflammatory disorders (e.g. granuloma annulare, cutaneous LE, dermatomyositis).
For further information see Ch. 46. From Dermatology, Third Edition.