Environmental and Sports-Related Skin Diseases
Cutaneous Injury Due to Heat Exposure
Thermal Burns
• Traumatic injury to the skin caused by an external heat source.
• The depth of the burn injury depends on the temperature of and the amount of contact time with the heat source as well as the thickness of the affected skin.
• The burn depth determines the severity and classification of the injury, its potential for healing and need for surgical intervention (Table 74.1).
Table 74.1
Classification and treatment of thermal burns.
Based on the 2009 American Burn Association revised classification system for burns. http://www.ameriburn.org/Chapter14.pdf
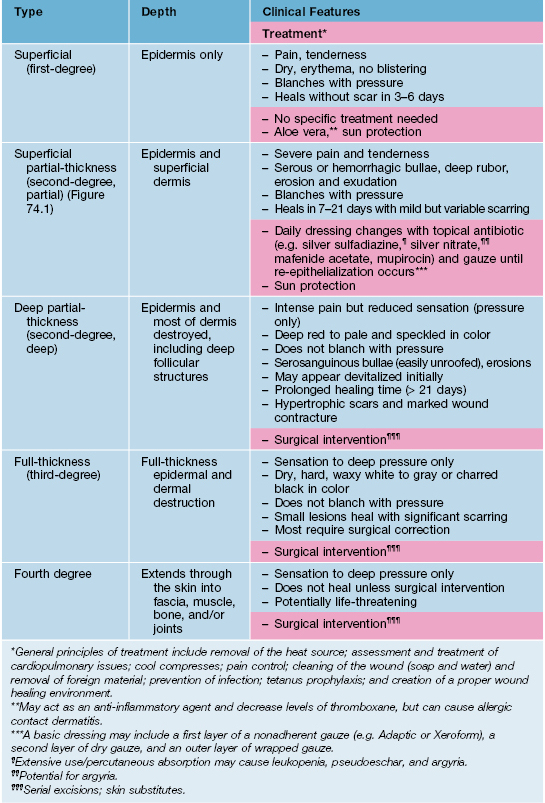
• In 2009, the American Burn Association replaced the traditional classification of burn wounds (i.e. first-, second-, third-degree) with a system that reflects the need for surgical intervention (see Table 74.1; Fig. 74.1).
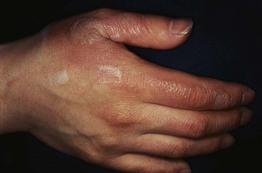
Fig. 74.1 Thermal burn. This superficial partial-thickness burn is characterized by bullae that contain serous fluid. Courtesy, Kalman Watsky, MD.
• An exact classification of the burn injury may not be possible upon initial presentation and may take up to 3 weeks to determine; burns may be deeper than initially suspected when occurring on thinner skin (e.g. in pediatric and elderly patients; on ears, volar forearms, medial thighs, and perineum).
• The extent of burn injury is expressed as a percentage of the body surface area (BSA) involved and is essential for guiding therapy and determining a patient's disposition (e.g. hospital admission for a partial-thickness burn involving >10% BSA in an individual 10–50 years of age).
• The most accurate method for estimating BSA involvement in adults and children is the Lund–Browder chart (http://www.tg.org.au/etg_demo/phone/etg-lund-and-browder.pdf); the ‘rule of nines’ method is perhaps more expeditious in adults, but it cannot be used for children (Fig. 74.2).
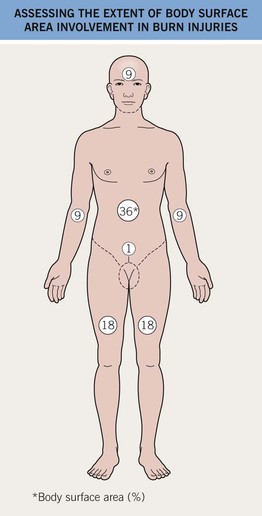
Fig. 74.2 Assessing the extent of body surface area involvement in burn injuries: Rule of nines. In adults, an estimate of burn extent is often based on this surface area distribution chart. Infants and children have a relatively increased head : trunk surface area ratio and this chart is ineffective for them. These estimates are also used for primary cutaneous disorders. The most accurate method of estimating the BSA involvement of burn injury in adults and children is with the Lund–Browder chart (http://www.tg.org.au/etg_demo/phone/etg-lund-and-browder.pdf).
• General principles of treatment are outlined in Table 74.1.
Erythema Ab Igne
• Localized areas of reticulated erythema and hyperpigmentation due to chronic exposure to heat that is below the threshold for a thermal burn.
• Multiple heat sources have been implicated (Table 74.2).
Table 74.2
Heat sources reported to cause erythema ab igne.
| • Heating pads | • Steam radiators |
| • Hot water bottles | • Heated car seats |
| • Electric stove/heater | • Heated reclining chairs |
| • Open fires | • Heating blanket |
| • Coal stoves | • Hot bricks |
| • Peat fires | • Infrared lamps |
| • Wood stoves | • Microwave popcorn |
| • Sauna belt | • Laptop computer* |
* Anterior thighs >> abdomen.
Courtesy, Mary Beth Cole, MD, and Michael Smith, MD.
• Most commonly seen in the lumbosacral region (due to heating pads applied to relieve pain from degenerative spinal disease); more recently seen on the anterior thighs from heated batteries in laptop computers.
• In long-standing erythema ab igne (latency period ≥30 years) there is an associated risk of malignant degeneration, resulting in thermal keratoses and SCC.
• Early lesions: asymptomatic, initially transient, blanchable macular erythema in a broad, reticulated pattern that corresponds to the venous plexus; size and shape approximates that of the heat source (Fig. 74.3A).
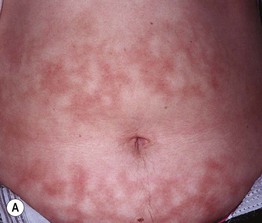
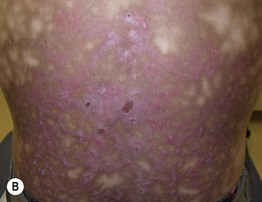
Fig. 74.3 Erythema ab igne. A Early phase with pink reticulated patches predominating over reticulated hyperpigmentation. B Later phase with large area of reticulated hyperpigmentation and superimposed pink keratotic plaques centrally. A, Courtesy, Jeffrey Callen, MD; B, Courtesy, Peter Klein, MD.
• Later lesions: dusky reticulated hyperpigmentation; lesions are fixed and no longer blanchable (Fig. 74.3B).
• End stage: may become keratotic and bullae may appear.
• DDx: livedo reticularis, cutis marmorata, poikiloderma (e.g. due to CTCL, dermatomyositis, several genodermatoses); the latter has a tighter net-like pattern.
• Rx: remove the heat source; if applicable, identify and treat the underlying source of pain.
Burns Associated with MRI and Fluoroscopy
MRI
• MRI may produce first-, second-, or third-degree burns due to metal or wire contact with skin, creating a closed-loop conduction system.
• The shape and size of the burns are determined by the conductor causing the injury (e.g. circular burns under ECG electrodes).
Fluoroscopy
• Fluoroscopy, especially when performed repeatedly in patients with cardiovascular disease, may result in radiation-induced injury (radiodermatitis).
• This radiodermatitis may be acute, but with time continued changes can develop, e.g. hair loss, desquamation, permanent erythema, and ulceration (Fig. 74.4).
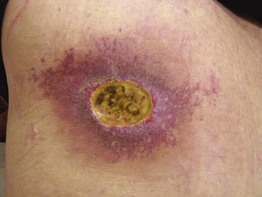
Fig. 74.4 Fluoroscopy-induced radiation dermatitis. The left upper back is a characteristic location for patients who have undergone attempts at coronary artery revascularization (e.g. angioplasty, stent placement). Courtesy, Jeffrey Callen, MD.
Cutaneous Injury Due to Cold Exposure
Frostbite
• Can occur when the skin temperature drops below about –2°C (28°F).
• Tissue freezing, vasoconstriction, and inflammatory mediator release are key features of its pathophysiology.
• There are four categories of severity based on depth of tissue injury; these are only recognizable upon rewarming (Fig. 74.5).
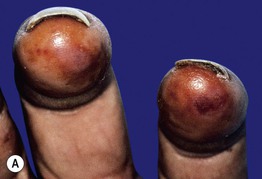
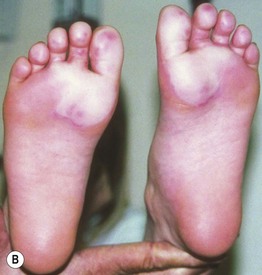
Fig. 74.5 Frostbite. A Erythema, edema, and hemorrhage are seen on the fingertips in a first-degree frostbite (frostnip); full recovery is expected, with only mild desquamation. B Bullae filled with clear fluid on the distal plantar surfaces in a second-degree frostbite; many such patients develop long-term sensory neuropathies. In third-degree frostbite there is full-thickness dermal loss with hemorrhagic bullae or waxy, dry, mummified skin. In fourth-degree frostbite there is full-thickness loss of the entire part, with skin, muscle, tendon, and bone damage; amputation may occur. A, Courtesy, Michael L. Smith, MD; B, Courtesy, Timothy Givens, MD.
• Symptomatically, early erythema, edema, and numbness are replaced by marked hyperemia and pain.
• Rx: rapid rewarming in a warm water bath is the cornerstone of treatment, followed by appropriate wound care.
Pernio (Chilblains)
• An abnormal inflammatory response to cold, damp, nonfreezing conditions.
• Classically presents with single or multiple erythematous to blue-violet macules, papules, or nodules distributed symmetrically on distal toes (Fig. 74.6) and fingers, and less often on the remainder of the foot or hand, nose and ears.
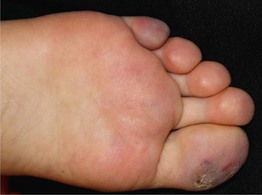
Fig. 74.6 Pernio. Violaceous macules and patches, primarily on the toes but also on the plantar surface of the foot; note the associated scaling. Courtesy, Jean L. Bolognia, MD.
• In severe cases, blistering and ulceration may be seen.
• Patients describe pruritus, burning, or pain; histology demonstrates a perivascular and perieccrine lymphohistiocytic infiltrate.
• Lesions typically resolve in 1–3 weeks but can take much longer or become chronic in elderly patients with venous insufficiency.
• DDx: chilblain lupus; frostbite; lupus pernio (a variant of sarcoidosis involving mainly the nose and ears) (Table 74.3).
Table 74.3
Differential diagnosis and evaluation of skin lesions induced by nonfreezing cold exposure.
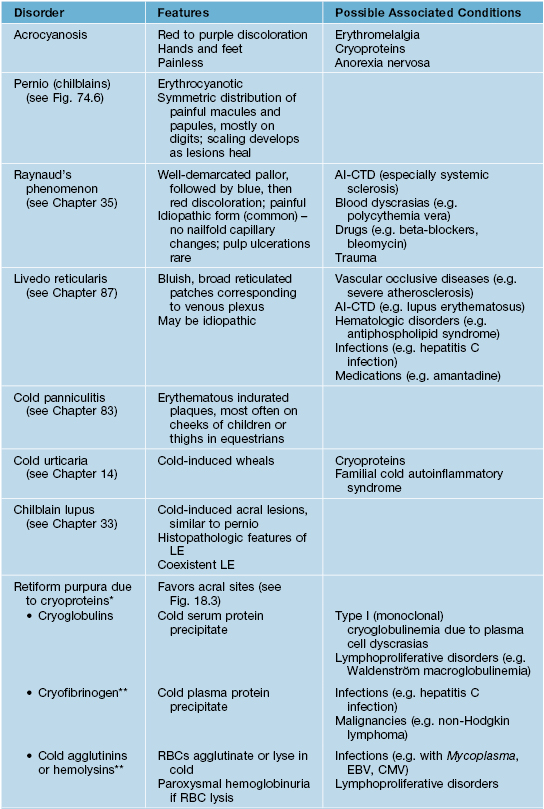
* Acrocyanosis, Raynaud's phenomenon, livedo reticularis, and cold urticaria can also be observed in association with cryoproteins.
** Rarely cause cold-related occlusion syndromes.
AI-CTD, autoimmune connective tissue disease; CMV, cytomegalovirus; EBV, Epstein–Barr virus; RBC, red blood cell; CBC, complete blood count; ANA, anti-nuclear antibody.
Courtesy, Michael L. Smith, MD.
• Rx: adequate clothing; avoidance of cold, damp conditions; keeping feet dry; avoidance of smoking; and use of nifedipine in recalcitrant cases.
Cutaneous Injury Due to Chemical Exposure
Chemical Hair Discoloration
• May be a voluntary cosmetic change or the result of chemical or metal exposure (Table 74.4).
• Most hair discoloration normalizes over time upon discontinuation of the offending exposure.
• Numerous anecdotal treatment remedies have been described, e.g. hot oil, hydrogen peroxide, and various shampoos (e.g. alkaline or EDTA-based).
Chronic Arsenical Dermatoses
• Chronic arsenic exposure most often occurs via contaminated drinking water or occupational exposure; long latency period (up to 40 years).
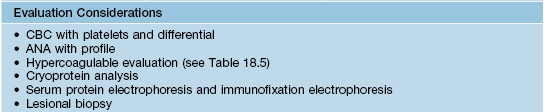
• Chronic arsenicism is characterized by mottled hyperpigmentation with areas of hypopigmentation (Fig. 74.7A); arsenical keratoses on the palms and soles (Fig. 74.7B–C); multiple non-melanoma skin cancers (particularly Bowen's disease); peripheral neuropathy and internal malignancies (e.g. bladder, lung, liver).
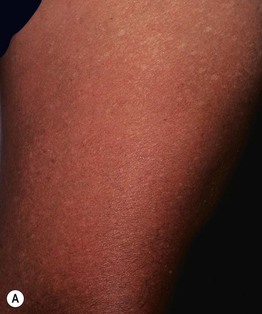
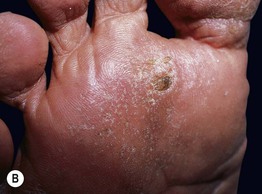
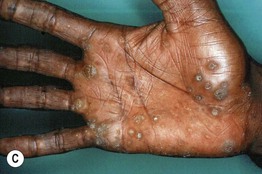
Fig. 74.7 Cutaneous manifestations of chronic arsenicism. A Guttate hypopigmentation superimposed on hyperpigmentation resembles ‘raindrops on a dusty road.’ B, C Arsenical keratoses on the plantar and palmar surface. A, Courtesy, John Steinbaugh, MD; C, Courtesy, Jeffrey Callen, MD.
Cutaneous Findings Resulting from Toxic and Heavy Metal Exposure
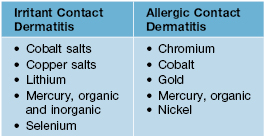
• Various toxic and heavy metals are known to cause irritant and/or allergic contact dermatitis, including the following (Table 74.5):
– Beryllium is a metal known to cause dermatitis and sarcoidosis-like granulomas of the skin and lung.
– Gold, as an elemental salt, can cause a variety of cutaneous eruptions (Table 74.6).
– Mercury, in elemental, inorganic, or organic forms, may cause acrodynia, tattoo reaction (cinnabar), granulomas, exanthems, cutaneous hyperpigmentation, allergic and irritant contact dermatitis, baboon syndrome.
– Cutaneous contact with silver may result in argyria, irritant contact dermatitis, or skin ulceration.
– Thallium, in its soluble form, may cause alopecia, acneiform papules, hyperkeratotic plaques on hands and feet, and Mee's lines in nails.
Table 74.6
Cutaneous eruptions associated with gold exposure (as an elemental salt).
| Most Common | Less Common |
| • Lichen planus, lichenoid drug eruption • Allergic contact dermatitis • Pityriasis rosea-like eruptions • Erosive stomatitis | • Chrysiasis • Erythema nodosum • Erythema multiforme, toxic epidermal necrolysis • Exfoliative dermatitis |
• For most cutaneous exposures to these toxic and heavy metals, effective treatment requires prompt soap and/or water washing; an exception is lithium, in which washing is contraindicated and gentle brushing off is preferred.
Cutaneous Findings of Frictional and Traumatic Injury to the Skin
Corns and Calluses
• Keratotic lesions resulting from repeated trauma and the subsequent cycle of friction, pressure, and thickening (Fig. 74.8).
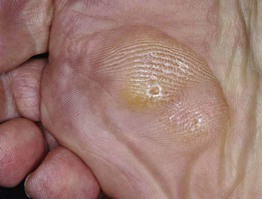
Fig. 74.8 Callus plus hard corns. Calluses are broad based and have increased skin markings while corns are round, more sharply defined papules with a central translucency and an interruption in dermatoglyphics. The skin overlying the second and third metatarsal heads is a common location for such lesions. Courtesy, Jean L. Bolognia, MD.
• Contributing factors include ill-fitting footwear, bony protuberances, abnormal biomechanical foot function, and specific activities that involve repetitive activity.
• Hard corns are usually located on the dorsal aspects of the toes, while soft corns are typically found in the interdigital web spaces.
• Corns and calluses can often be mistaken for verrucae; gentle paring of the lesions with a blade and noticing the lesion's effect on dermatoglyphics can help distinguish between these three entities (Table 74.7).
Table 74.7
Distinguishing features of verrucae, corns, and calluses.
| Lesion | Paring Revelations | Effect on Dermatoglyphics |
| Verruca | Thrombosed capillaries, multiple bleeding points | Interrupted |
| Corn | Central translucent, whitish-yellow core | Interrupted |
| Callus | Layers of yellowish keratin | Accentuated |
• Treatment involves both symptomatic relief and correction of the underlying biomechanical problem:
1. Paring of the callosity with removal of the corn's central core may bring immediate relief of discomfort, followed by periodic foot filing.
2. Application of keratolytic agents (e.g. 40% salicylic acid pads; 6% salicylic acid, 10–40% urea, or 12% ammonium lactate creams), from daily to twice weekly, depending on strength.
3. Soft cushions (e.g. silicone sheet, sheep skin) and donut-shaped corn pads.
– Biomechanical correction – properly-fitted footwear and use of appropriate orthotics.
– Recalcitrant lesions – consider x-ray to look for exostoses and referral to orthopedic or podiatric surgeon.
Black Heel (Talon Noir)
• Black macules on the palms or soles due to hemoglobin within the thickened stratum corneum (Fig. 74.9).
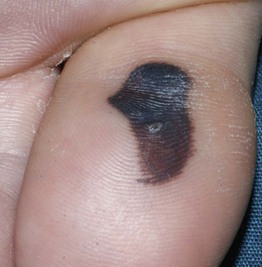
Fig. 74.9 Black heel (talon noir) and palm. This black color is due to hemoglobin within the thickened stratum corneum of plantar skin. Courtesy, Julie V. Schaffer, MD.
• Secondary to impact trauma and resolves with paring or spontaneously with time.
• Harmless, but because of its dark color must be differentiated from acral cutaneous melanoma (does not resolve with gentle paring).
Chondrodermatitis Nodularis Helicis (CNH)
• A tender, inflammatory process of the ear that primarily affects patients older than 50 years of age; initiated by ischemia-related inflammation of the cartilage.
• Presents with a skin-colored to erythematous, dome-shaped papule or nodule with a central crust or keratin-filled crater; often exquisitely tender (Fig. 74.10).
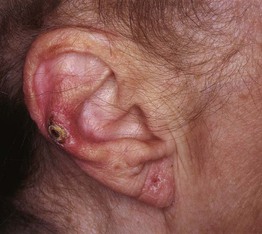
Fig. 74.10 Chondrodermatitis nodularis helicis (CNH). Tender, erythematous papulonodule with central scale-crust on the mid antihelix of an older woman. This represented the site most susceptible to pressure-induced ischemia. Courtesy, Kalman Watsky, MD.
• Most often a unilateral process affecting the most protuberant portion of the ear, primarily the upper helical rim or the middle to lower antihelical rim.
• DDx: SCC, KA, BCC, AK, cutaneous horn, weathering nodule, verruca, calcinosis cutis, gouty tophus; often distinguished via biopsy.
• Rx: mostly anecdotal and not standardized (e.g. intralesional CS, topical antibiotics, specially designed CNH pillows for sleeping, cryosurgery, electrodesiccation and curettage, CO2 laser ablation); full-thickness excision is the most definitive and favored treatment for particularly bothersome lesions.
Acanthoma Fissuratum
• Results from ill-fitting eyeglass frames that create a frictional injury to the postauricular sulcus or the upper lateral nose (Fig. 74.11).
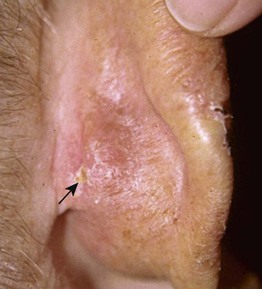
Fig. 74.11 Acanthoma fissuratum. Thin pink plaque with scale of the postauricular sulcus. Note the linear fissure (arrow). Courtesy, Mary Beth Cole, MD, and Michael L. Smith, MD.
• Presents as a firm or sometimes soft, skin-colored to erythematous nodule or plaque with a central vertical groove or fissure; occasionally tenderness, serous discharge, or slight hyperkeratosis.
• DDx: BCC, SCC, chronic dermatitis or benign acanthoma; biopsy is occasionally necessary to exclude a non-melanoma skin cancer.
Weathering Nodules of the Ears
• Multiple, bilateral, firm (feels like cartilage), asymptomatic, whitish, 2- to 3-mm papules located along the inner rim of the helices in older males >> females (Fig. 74.12).
Fig. 74.12 Weathering nodules. Multiple asymptomatic, small, whitish papules along the helix of an older man with photodamage. Courtesy, Jean L. Bolognia, MD.
• Associated consistently with a history of significant sun exposure and actinic damage.
• DDx: CNH, gouty tophi, calcinosis cutis, elastotic nodules, granuloma annulare.
Sports-Related Dermatoses
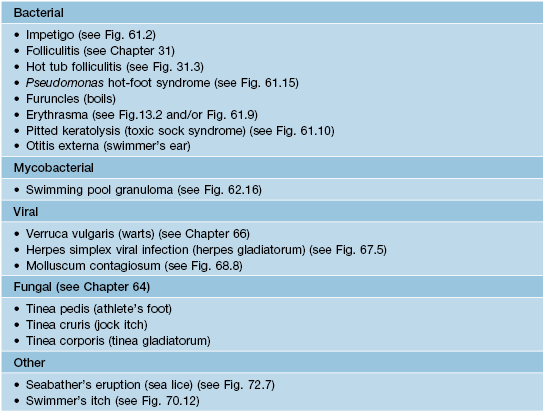
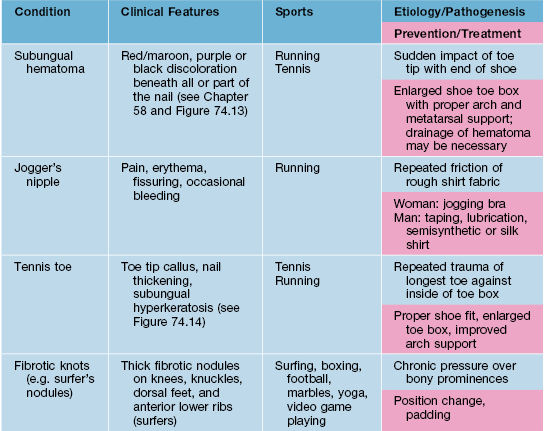
• Participation in sports is often associated with a number of cutaneous injuries, dermatoses, or infections, related to acute and chronic mechanical trauma (Tables 74.8 and 74.9; Fig. 74.13 and 74.14).
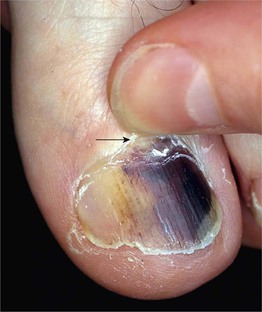
Fig. 74.13 Subungual hematoma. A common sports-related (e.g. tennis, running, basketball) injury due to the sudden impact of the toe tip with the end of the shoe. Note the subungual dark purplish discoloration, which may be misdiagnosed as melanoma. Clues to the diagnosis of subungual hematoma include: a normal-appearing proximal nail plate upon gentle retraction of the cuticle (arrow); characteristic dermoscopic features (e.g. red-brown to purplish-black round globules); and determination that the discoloration grows out distally. Courtesy, Jean L. Bolognia, MD.
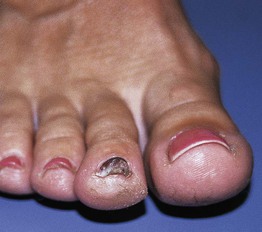
Fig. 74.14 Chronic ‘tennis toe.’ Chronic and repeated trauma of the longer second toe against the end of the tennis shoe toe box during sudden stops creates the distal callus formation and nail plate thickening known as ‘tennis toe.’ Courtesy, Michael L. Smith, MD.
For further information see Ch. 88. From Dermatology, Third Edition.