Hepatic Lipidosis
Basic Information 
Definition
Hepatopathy induced by metabolic changes that lead to an excessive accumulation of triglycerides in liver tissue, with resulting cholestasis and hepatic dysfunction
Epidemiology
Genetics and Breed Predisposition
Amazon parrots, galah cockatoos, cockatoos, budgerigars, lorikeets
Risk Factors
Given the complexity of lipid metabolism (avian lipid metabolism pathways and regulation are not fully understood), a multitude of factors may predispose a bird to hepatic lipidosis.
• Overfeeding of neonates (cockatoos, macaws) using a high-energy ration
• Multinutrient-deficient diet, especially essential fatty acids (linoleic acid), essential and sulfur amino acids (choline, methionine, cysteine), lipotrophic factors that promote metabolism of fat (l-carnitine), and vitamins such as biotin, vitamin E, vitamins B1, B2, B6, and B12, and folic acid
 Impaired fatty acid beta-oxidation
Impaired fatty acid beta-oxidation
 Impaired synthesis and secretion of very low-density lipoproteins (VLDLs) essential for normal hepatic lipid metabolism and transport
Impaired synthesis and secretion of very low-density lipoproteins (VLDLs) essential for normal hepatic lipid metabolism and transport
• Restricted exercise, sedentary lifestyle
• Increased lipogenesis such as estrogen-induced lipogenesis during active egg laying, increased activity of hormone-sensitive lipase with diabetes mellitus, stress-associated hepatic lipogenesis and peripheral lipolysis (promoted by catecholamines, corticosteroids, and thyroxine), and estrogenic-like action of pesticides
• Acute release of fatty acids from adipose stores in an overweight and anorectic bird does not seem to promote fatty liver syndrome as observed in cats.
Clinical Presentation
History, Chief Complaint
The bird may be presented for anorexia, dyspnea, nonspecific sickness, green stools, regurgitation, or polyuria-polydipsia. History frequently points out an improper nutritional background. Upon physical examination, the bird is often noted to be obese or slightly overweight.
Physical Exam Findings
• Lethargy, weakness, weight loss
• Hepatic enlargement that may be palpable or visible through the skin
• Dyspnea due to hepatic enlargement and/or intracoelomic fat accumulation
• Abdominal distention due to hepatic enlargement and/or ascites (usually with concurrent heart disease)
• Biliverdinuria (increased renal excretion of biliverdin) due to cholestasis
• Poor feather condition: pigment changes, stress bars
• Neurologic signs due to hepatic encephalopathy (rare)
• Polyuria, diarrhea, regurgitation, and/or vomiting
• Melena, bloody droppings in case of coagulopathy (final stage)
• Some integument conditions of poorly understood pathogenesis are occasionally associated with lipid hepatopathy:
Etiology and Pathophysiology
The general disease signs are various but consistent with hepatic failure, enlargement, or insufficiency. The course of the disease is generally chronic, but clinical illness may appear acute. Concurrent conditions associated with poor nutrition may also be present. The laying hen may die acutely of fatty liver hemorrhagic syndrome resulting from rupture of hepatic blood vessels during egg laying. It should be stressed that other forms of lipid deposition (e.g., atherosclerosis; fat deposition in kidneys, skin, abdomen, lungs, and spleen) that lead to other physical findings can be found concurrently with hepatic lipidosis.
Diagnosis 
Differential Diagnosis
Any hepatobiliary disease, particularly if chronic and noninfectious, that could induce hepatomegaly
• Hepatic congestion, portal hypertension
• Hepatotoxins: mycotoxins (e.g., aflatoxins produced by Aspergillus spp., ochratoxins), plants, drugs (e.g., antifungals, volatile anesthetics, some antibiotics, steroids), pesticides, heavy metals, environmental toxins, vitamin A
• Hepatic neoplasia or metastasis to liver
• Amyloidosis (rarely reported in psittacines)
• Iron storage disease, especially in lorikeets, Sturnidae, and Ramphastidae
• Infectious hepatitis: bacterial (Chlamydophila psittaci, Mycobacteria spp., Gram-negative hepatitis), viral (polyomavirus, herpesvirus, adenovirus, reovirus), and parasitic (trematodes, protozoa)
Initial Database
Complete blood count (CBC) often shows a mild nonregenerative anemia and mild leukocytosis or leukopenia. CBC helps to rule out inflammatory hepatopathies.
• Clinical pathologic examination should target and evaluate recent hepatocellular damage, hepatic function, lipid metabolism, and electrolytes.
• Aspartate aminotransferase (AST): high sensitivity but low specificity should always be interpreted with creatine kinase (CK) values. Plasma activities may be normal in very advanced cases and are not consistently increased in hepatic lipidosis.
• Glutamate dehydrogenase (GLDH): mitochondrial enzyme, low sensitivity but high specificity, accurate elevation in cases of severe hepatocellular damage
• Bile acids: high sensitivity and high specificity, test hepatic function, moderate to high elevation
• Total protein (TP), albumin, coagulation factors, uric acid: decreased with impairment of hepatic production
• Hypoglycemia may be seen because of impaired gluconeogenesis, starvation, or chronic disease; elevation in cases of diabetes mellitus
• Lipemic serum and hyperlipidemia are common with elevation in triglycerides and cholesterol due to impaired lipid metabolism. Lipemic serum can strongly interfere with some biochemical tests.
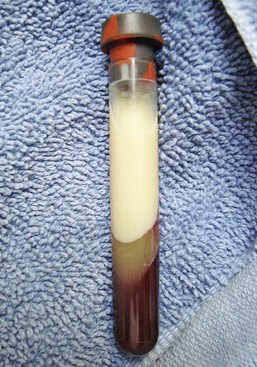
Hepatic Lipidosis
Severe hypercholesterolemia in a bird. This can often be seen in birds on a high-fat diet. (Photo courtesy Jörg Mayer, The University of Georgia, Athens.)
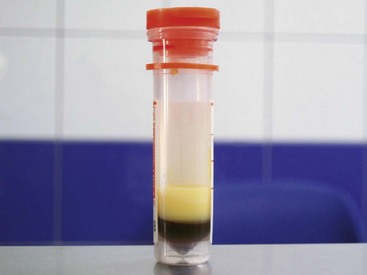
Hepatic Lipidosis
Severely lipemic serum from a cockatiel diagnosed with hepatic lipidosis; such lipemia interferes strongly with biochemistry. (Courtesy Hugues Beaufrère and Clinique Vétérinaire Brasseur.)
• Hypokalemia could also be present if the bird has regurgitated, has vomited, or is polyuric.
Advanced or Confirmatory Testing
 Radiographs frequently reveal an enlarged liver with compression of coelomic air sacs and concomitant overinflation of axillary diverticuli of interclavicular air sacs. Ascites may be present but is rarely important without concurrent heart disease. Cardiomegaly should be ruled out.
Radiographs frequently reveal an enlarged liver with compression of coelomic air sacs and concomitant overinflation of axillary diverticuli of interclavicular air sacs. Ascites may be present but is rarely important without concurrent heart disease. Cardiomegaly should be ruled out.
 Ultrasonographic examination of the liver in affected birds shows an enlarged liver with rounded margins and diffuse alteration of parenchyma, which is hyperechoic. Ascites may be confirmed as well. Ultrasound examination is especially useful to rule out liver congestion, in which biopsy could lead to a fatal hemorrhage.
Ultrasonographic examination of the liver in affected birds shows an enlarged liver with rounded margins and diffuse alteration of parenchyma, which is hyperechoic. Ascites may be confirmed as well. Ultrasound examination is especially useful to rule out liver congestion, in which biopsy could lead to a fatal hemorrhage.
 Endoscopy allows visualization of the liver via a lateral approach, through entry into the ventral hepatic peritoneal cavity from the left or right caudal thoracic air sacs, or by a direct approach, via the ventral midline. Livers exhibiting lipidosis are enlarged with pale or mottled yellow parenchyma and rounded margins.
Endoscopy allows visualization of the liver via a lateral approach, through entry into the ventral hepatic peritoneal cavity from the left or right caudal thoracic air sacs, or by a direct approach, via the ventral midline. Livers exhibiting lipidosis are enlarged with pale or mottled yellow parenchyma and rounded margins.
 Definitive diagnosis of hepatic lipidosis requires a liver biopsy that may be taken using endoscopy, ultrasound, or surgery. Histologically, hepatic lipidosis is characterized by vacuolation and degeneration of hepatocytes. A prognosis may be determined by assessing the degree of degeneration, vacuolation, and inflammation present in the sample.
Definitive diagnosis of hepatic lipidosis requires a liver biopsy that may be taken using endoscopy, ultrasound, or surgery. Histologically, hepatic lipidosis is characterized by vacuolation and degeneration of hepatocytes. A prognosis may be determined by assessing the degree of degeneration, vacuolation, and inflammation present in the sample.
 Birds with severe hepatic lipidosis are in metabolic crisis, and anesthesia for collection of a liver biopsy is inappropriate until the patient is stabilized.
Birds with severe hepatic lipidosis are in metabolic crisis, and anesthesia for collection of a liver biopsy is inappropriate until the patient is stabilized.
Treatment 
Therapeutic Goals
• Stabilize and improve patient’s physical condition.
• Improve nutritional status of patient.
• Treat secondary conditions that may be leading to patient’s poor physical health.
• Develop a plan for gradual weight loss and improved nutritional offerings.
• Improve status of liver function.
• Increase patient exercise if appropriate, to consume energy and to stimulate enteric motility.
• Limit stress, which may promote storage of triglycerides in the liver.
Acute General Treatment
 Fluid replacement is important because dehydration compromises hepatic circulation. Avoid lactated fluids because a bird with severe hepatic lipidosis could present lactate intolerance. Avoid excessive glucose or dextrose infusion, which is thought to potentiate triglyceride accumulation by inhibiting beta-oxidation of fatty acids.
Fluid replacement is important because dehydration compromises hepatic circulation. Avoid lactated fluids because a bird with severe hepatic lipidosis could present lactate intolerance. Avoid excessive glucose or dextrose infusion, which is thought to potentiate triglyceride accumulation by inhibiting beta-oxidation of fatty acids.
 Supplement fluids with water-soluble vitamins, and with potassium if hypokalemic.
Supplement fluids with water-soluble vitamins, and with potassium if hypokalemic.
 Consider administration of vitamin K1.
Consider administration of vitamin K1.
 Hypoproteinemic birds may require the addition of colloids (hetastarch, oxyglobin) 10-15 mL/kg/d IV or a 5 mL/kg bolus.
Hypoproteinemic birds may require the addition of colloids (hetastarch, oxyglobin) 10-15 mL/kg/d IV or a 5 mL/kg bolus.
 Ascitic fluid should not be removed by abdominocentesis because this would deplete protein stores, except if the bird is severely dyspneic. Just remove as needed for diagnostic purposes.
Ascitic fluid should not be removed by abdominocentesis because this would deplete protein stores, except if the bird is severely dyspneic. Just remove as needed for diagnostic purposes.
 Place the bird in an incubator with oxygen if very depressed or dyspneic.
Place the bird in an incubator with oxygen if very depressed or dyspneic.
 Hepatic encephalopathy, if present, may be managed with lactulose 150-650 mg/kg q 12 h. Supplementation with proteins should be limited.
Hepatic encephalopathy, if present, may be managed with lactulose 150-650 mg/kg q 12 h. Supplementation with proteins should be limited.
 Ascites should be controlled with furosemide 1-2 mg/kg as needed, generally once to twice daily.
Ascites should be controlled with furosemide 1-2 mg/kg as needed, generally once to twice daily.
 Vomiting, regurgitation, and nausea can be addressed with antiemetic drugs: metoclopramide 0.5 mg/kg q 6 h, metopimazine 0.5-1 mg/kg q 24 h.
Vomiting, regurgitation, and nausea can be addressed with antiemetic drugs: metoclopramide 0.5 mg/kg q 6 h, metopimazine 0.5-1 mg/kg q 24 h.
 Chronic egg laying or reproductive status should be suppressed with leuprolide acetate 500-1000 mcg/kg q 14 d or hCG 500-1000 IU q 3-5 wk.
Chronic egg laying or reproductive status should be suppressed with leuprolide acetate 500-1000 mcg/kg q 14 d or hCG 500-1000 IU q 3-5 wk.
 Ursodeoxycholic acid has been shown to have cytoprotective, antiinflammatory, antioxidant, and antifibrotic effects on hepatocytes, and to increase the production of glutathione. This drug is used in human medicine for cholestasis and attenuation of hepatotoxicity, and in feline medicine for cholangiohepatitis. However, no real benefit has been demonstrated in feline or human medicine in triglyceride accumulation disorders. Dosage: 15 mg/kg q 24 h
Ursodeoxycholic acid has been shown to have cytoprotective, antiinflammatory, antioxidant, and antifibrotic effects on hepatocytes, and to increase the production of glutathione. This drug is used in human medicine for cholestasis and attenuation of hepatotoxicity, and in feline medicine for cholangiohepatitis. However, no real benefit has been demonstrated in feline or human medicine in triglyceride accumulation disorders. Dosage: 15 mg/kg q 24 h
Chronic Treatment
 Providing a well-balanced diet free of toxins is the single most important treatment in hepatic lipidosis; formulated diets with correct quantities of fresh fruits and vegetables are highly suggested.
Providing a well-balanced diet free of toxins is the single most important treatment in hepatic lipidosis; formulated diets with correct quantities of fresh fruits and vegetables are highly suggested.
 Supplement proteins to reduce lipid accumulation in the liver unless hepatic encephalopathy is a concern. Several recovery or neonatal psittacine formulas have a high content of proteins and should be used for nutritional support in birds suffering from hepatic lipidosis (e.g., Recovery Formula, Harrison Bird Food, crude protein 35%; Exact, Kaytee, crude protein 22%; A21, Nutribird, Versele-laga, crude protein 21%; Neonate formula, Harrison Bird Food, crude protein 26%).
Supplement proteins to reduce lipid accumulation in the liver unless hepatic encephalopathy is a concern. Several recovery or neonatal psittacine formulas have a high content of proteins and should be used for nutritional support in birds suffering from hepatic lipidosis (e.g., Recovery Formula, Harrison Bird Food, crude protein 35%; Exact, Kaytee, crude protein 22%; A21, Nutribird, Versele-laga, crude protein 21%; Neonate formula, Harrison Bird Food, crude protein 26%).
 Avoid excessive energy intake.
Avoid excessive energy intake.
 Inhibit peripheral lipolysis by providing at least the resting energy requirement for ideal body weight.
Inhibit peripheral lipolysis by providing at least the resting energy requirement for ideal body weight.
 Carbohydrate supplementation is contraindicated because it inhibits beta-oxidation of fatty acids.
Carbohydrate supplementation is contraindicated because it inhibits beta-oxidation of fatty acids.
 Gavage feed the bird if anorectic as many times as necessary to ensure intake of the correct balance and quantity of food. Vitamins may be added to the feeding as required.
Gavage feed the bird if anorectic as many times as necessary to ensure intake of the correct balance and quantity of food. Vitamins may be added to the feeding as required.
• Supporting lipid metabolism with dietary supplementation
 Supplementation with vitamins (especially B complex, biotin, E, and vitamin K1) and essential amino acids
Supplementation with vitamins (especially B complex, biotin, E, and vitamin K1) and essential amino acids
 Supplementation in lipotrophic factors: choline and methionine 40-50 mg/kg q 24 h
Supplementation in lipotrophic factors: choline and methionine 40-50 mg/kg q 24 h
 l-Carnitine 100-250 mg/kg q 24 h could be helpful in that it is an important component of the mitochrondrial membrane, and it transports fatty acid in the matrix, where beta-oxidation occurs. This agent is regularly used in the management of feline lipidosis, even though its use is controversial because carnitine deficiency has not been demonstrated in cats with hepatic lipidosis.
l-Carnitine 100-250 mg/kg q 24 h could be helpful in that it is an important component of the mitochrondrial membrane, and it transports fatty acid in the matrix, where beta-oxidation occurs. This agent is regularly used in the management of feline lipidosis, even though its use is controversial because carnitine deficiency has not been demonstrated in cats with hepatic lipidosis.
 Other antioxidant agents could be tried such as silymarin 50/75 mg/kg q 12 h.
Other antioxidant agents could be tried such as silymarin 50/75 mg/kg q 12 h.
 N-acetylcysteine (NAC) and S-adenosyl-methionine (SAMe) 15-20 mg/kg q 24 h may help to prevent oxidative stress and stabilize hepatocellular membranes. Both are glutathione precursors and contain sulfur amino acids. NAC and SAMe may assist in lipid metabolism and other aspects of metabolism of the liver. SAMe is also a precursor of l-carnitine.
N-acetylcysteine (NAC) and S-adenosyl-methionine (SAMe) 15-20 mg/kg q 24 h may help to prevent oxidative stress and stabilize hepatocellular membranes. Both are glutathione precursors and contain sulfur amino acids. NAC and SAMe may assist in lipid metabolism and other aspects of metabolism of the liver. SAMe is also a precursor of l-carnitine.
Possible Complications
• Use furosemide with caution in hypokalemic birds.
• Anabolic steroids (stanozolol) should be avoided because they can inhibit bile flow and seem to increase the risk of hepatic lipidosis in cats. Anabolic steroids and glucocorticoids also have an inhibitory influence on beta-oxidation.
• Tetracyclines (e.g., doxycycline) have lipogenic effects on hepatocytes in many mammals and consequently should be used with caution in birds suffering from hepatic lipidosis.
Recommended Monitoring
• Control weight; an obese bird should lose weight gradually.
• Reassess liver damage and function at regular intervals using hepatic biochemistry and by monitoring clinical improvement.
• A recheck liver biopsy may be indicated after completion of therapy.
• Assess the progress of diet conversion as well as body weight at regular rechecks until stable.
Pearls & Considerations 
Comments
• Certain bird species are susceptible to hepatic lipidosis; owners of these species should be aware of the bird’s chances of developing this disease.
• Owners with young obese birds should have the animals monitored on a regular basis for subclinical signs of hepatic lipidosis through blood testing.
Center, SA. Feline hepatic lipidosis. Vet Clin North Am (Small Anim Pract). 2006; 35:225–269.
Fudge, AM. Testing the liver and the gastrointestinal function. In: Fudge AM, ed. Laboratory medicine: avian and exotic pets. Philadelphia: WB Saunders; 2000:47–55.
Lumeij, J. Hepatology. In: Ritchie BW, et al, eds. Avian medicine: principles and application. Lake Worth, FL: Wingers Publishing; 1994:522–537.
Scherk, MA, et al, Toxic, metabolic, infectious, and neoplastic liver diseases. Textbook of veterinary internal medicine. ed 6. Ettinger, SJ, et al, eds. Textbook of veterinary internal medicine; vol 2. Elsevier/Saunders, St Louis, 2005.:1464–1477.