Uropygial Gland Disease Conditions
Basic Information 
Definition
Disease conditions that affect the uropygial gland, a bilobed secretory gland located on the uropygium
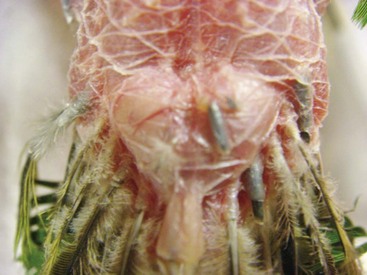
Uropygial Gland Disease Conditions Normal appearance of the bilobed uropygial gland on this feather-picking parrot.
The uropygial area is located dorsally over the pygostyle, on the midline, at the base of the tail. Secretions of this gland are an important component in maintaining feathers’ condition.
Epidemiology
Species, Age, Sex
All species that have a uropygial gland and all ages and both sexes can be affected by uropygial gland disease presentations.
Genetics and Breed Predisposition
None specific, but certain avian species (e.g., Amazon parrots, hyacinth macaws) do not have a uropygial gland; therefore, they would not be susceptible to disease conditions associated with this gland.
Etiology and Pathophysiology
• The uropygial gland, often referred to as the oil or preen gland, is an epidermal holocrine gland localized on the uropygium of most birds. It is composed of two lobes separated by an interlobular septum and covered by an external capsule. A dorsocaudally oriented papilla contains one, two, or multiple ducts and a tuft of down feathers at the openings. The nerve supply of the gland has both a medullar and a sympathetic origin. The gland is vascularized by branches of the caudal artery.
• Composition of avian uropygial gland secretions is very complex and may vary with species, gender, season, diet, and hormonal regulation. The secretion is a complex mixture of ester waxes, fatty acids, lipids, and wax alcohols. Secretions are spread among the plumage by preening. Contact of the beak with the papilla induces a flow of secretion.
• Possible roles of uropygial gland secretions:
 Antimicrobial activity against feather-degrading bacteria and fungi
Antimicrobial activity against feather-degrading bacteria and fungi
 Antiabrasive effects to prevent feather barbules from breaking and to maintain plumage in good condition when the feathers are drawn through the bill during preening
Antiabrasive effects to prevent feather barbules from breaking and to maintain plumage in good condition when the feathers are drawn through the bill during preening
 As protection against feather-degrading ectoparasites such as feather lice
As protection against feather-degrading ectoparasites such as feather lice
 Hydrophobic properties, which have a role in plumage waterproofing in some species
Hydrophobic properties, which have a role in plumage waterproofing in some species
 Conversion of provitamin D to vitamin D by ultraviolet light and ingestion by further preening
Conversion of provitamin D to vitamin D by ultraviolet light and ingestion by further preening
 Sex-linked changes in the ultraviolet appearance of the plumage
Sex-linked changes in the ultraviolet appearance of the plumage
 Excretory functions of several pesticides and pollutants
Excretory functions of several pesticides and pollutants
 The fact that some bird species lack a preen gland suggests that preen oil is not universally important, or that they may use alternative strategies for feather maintenance.
The fact that some bird species lack a preen gland suggests that preen oil is not universally important, or that they may use alternative strategies for feather maintenance.
Diagnosis 
Differential Diagnosis
• Glandular metaplasia and hyperkeratosis due to hypovitaminosis A
• Neoplasia: adenoma, adenocarcinoma, squamous cell carcinoma, papilloma
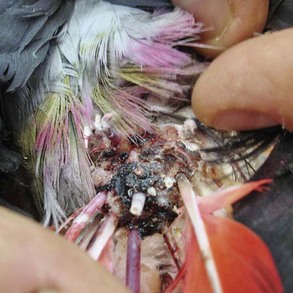
Uropygial Gland Disease Conditions Large tumor of the uropygial gland in a parakeet. Surgical excision often is incomplete and recurrence is common; aggressive radiation offers a good follow-up option after removal of the bulk of the mass.
• Granulomas: fungi, foreign bodies
• Trauma, rupture of the gland, chronic ulcerative dermatitis of the uropygial and periuropygial area
Initial Database
• Complete blood count (CBC): in most cases unremarkable; slight leukocytosis or monocytosis may be observed in cases with inflammation or secondary infection
• Plasma biochemistry panel: no specific biochemistry abnormalities noted
• Cytologic examination/cultures: Cytologic examination can be performed on gland secretions or ulcerations. The main purpose is to determine whether an infection is present with inflammatory cells and bacteria (monomorphic intracellular) or neoplasia (neoplastic cells present). Culture and sensitivity should be performed as appropriate.
Treatment 
Therapeutic Goal
Resolution of the disease condition and return of normal function of the uropygial gland
Acute General Treatment
• Treatment of a uropygial gland problem will depend on the diagnosis.
 Digital pressure in cases of impacted, abscessed, or metaplastic glands may be helpful in exuding the contents. Application of hot compresses may help in liquefying the content before expulsion.
Digital pressure in cases of impacted, abscessed, or metaplastic glands may be helpful in exuding the contents. Application of hot compresses may help in liquefying the content before expulsion.
 Wound care and cleaning are necessary if ulceration or erosion is noted. Adherent dressings (e.g., 3M Tegaderm, 3M Tegaderm-Foam-Adhesive-Dressing, 3M Tegaderm-Hydrocolloid-Thin-Dressing [3M, St Paul, Minn]) should be considered whenever possible with an infected or extensive wound in this area. Treatments that can be used alone or in combination with surgery are described later.
Wound care and cleaning are necessary if ulceration or erosion is noted. Adherent dressings (e.g., 3M Tegaderm, 3M Tegaderm-Foam-Adhesive-Dressing, 3M Tegaderm-Hydrocolloid-Thin-Dressing [3M, St Paul, Minn]) should be considered whenever possible with an infected or extensive wound in this area. Treatments that can be used alone or in combination with surgery are described later.
• For impacted uropygial glands, an incision over the affected lobe(s) with subsequent removal of the impacted material; the incision should be left to heal by secondary intention
Chronic Treatment
• Topical chemotherapy (e.g., 5-fluorouracil application)
• Intratumoral chemotherapy (e.g., carboplatin, cisplatin)
• Radiation therapy involves administration of ionizing radiation to tumor cells. Strontium 90 ophthalmic applicator therapy has been used to apply 100 Gy in the treatment of uropygial tumors.
• Cryotherapy has several advantages: minimal systemic effects, minimal postoperative bleeding, and safe repeat treatments.
Drug Interactions
• Any chemotherapy and radiation therapy should be administered by a trained oncology specialist. Chemotherapeutic and radiation therapeutic agents present a serious health hazard for people around the patient during treatment application.
• If chemotherapeutic and radiation therapy is not administered correctly and at the proper dose, the patient may die or suffer permanent injury.
Recommended Monitoring
• Monitor diseased uropygial gland for treatment response.
• Repeat CBC and plasma chemistry panel when radiation or chemotherapy is being used.
• Analgesic/antiinflammatory medication is required in cases of suspected pain and inflammation.
• Monitor appetite, fecal output, and behavior during treatment period, until the disease condition has resolved.
Pearls & Considerations 
Comments
• Some avian species (e.g., some macaw species, Amazon parrots) do not have a uropygial gland.
• With many avian species, the uropygial gland may be removed without adverse consequences.
• The uropygial gland is very important for water birds to maintain the health and condition of their feathers while swimming.
• The uropygial gland is vascular; care should be taken when excising the gland to reduce hemorrhage associated with removal.
• A definitive diagnosis is necessary to establish a proper treatment protocol for the patient.
Altman, RB. Soft tissue surgical procedures. In: Altman RB, et al, eds. Avian medicine and surgery. Philadelphia: WB Saunders; 1997:704–732.
Filippich, LJ. Tumor control in birds. Semin Avian Exotic Pet Med. 2004; 13:25–43.
Lucas, AM, et al. Avian anatomy: integument, part II, agriculture handbook 362. Washington DC: U. S. Government Printing Office; 1972.
Nemetz, LP, et al. Strontium-90 therapy for uropygial neoplasia. Proc Conf Assoc Avian Vet. 2004; 25:15–20.