Body Mechanics and Patient Mobility
Objectives
1. State the principles of body mechanics.
2. Explain the rationale for use of appropriate body mechanics.
3. Discuss considerations related to mobility for older adults.
4. Discuss the complications of immobility.
5. Demonstrate the use of assistive devices for proper positioning.
6. State the nursing interventions used to prevent complications of immobility.
7. Demonstrate placement of patient in various positions, such as Fowler's, supine (dorsal), Sims', side-lying, prone, dorsal recumbent, and lithotomy positions.
8. State the assessment for the patient's neurovascular status, including the phenomenon of compartment syndrome.
9. Describe and demonstrate range-of-motion exercises and explain their purpose.
10. Identify complications caused by inactivity.
11. Relate appropriate body mechanics to the techniques for turning, moving, and lifting the patient.
12. Discuss use of the continuous passive motion machines.
13. Discuss the nursing process and how it relates to patient mobility.
Key Terms
http://evolve.elsevier.com/Cooper/foundations/
The two concepts of body mechanics and patient mobility are directly related to one another. Nursing personnel must learn and practice proper principles of body mechanics to prevent injury to themselves and injury to their patients. When assisting patients in mobility, nurses must be constantly aware of their own body mechanics. According to the Bureau of Labor Statistics (www.bls.gov), nursing personnel (which includes unlicensed assistive personnel [UAP], such as certified nurse assistants [CNAs], orderlies) rank second in the number of occupational injuries requiring days away from work. Nurses fall just below the top five occupations that require days away from work due to injuries. The vast majority of these injuries are classified as musculoskeletal disorders (MSDs), with back injuries prominent among health care personnel.
Most injuries occur when nursing personnel perform tasks that require repetitive movement, uncomfortable posture, and exertion to assist patients in activities such as feeding, dressing, bathing, toileting, repositioning, and ambulation. Awareness of proper ergonomic principles (ergonomics is the science of matching workplace conditions and job demands to the capabilities of workers, especially in regard to MSDs and their prevention) and good body mechanics helps prevent injury.
Mechanical lifting devices (sling and standing lifts) and assistive patient-handling equipment, such as roller boards, sliders, friction-reduction pads, transfer chairs, and gait belts, work by taking on the energy and force that otherwise are imposed on the nurse during the lifting, transferring, or repositioning of a patient. Regular use of lifts and other assistive devices reduces the risk of injury (see the Evidence-Based Practice box).
Safe patient transfer requires adequate staffing, the right mix of personnel, and appropriate, readily available, well-maintained patient-lifting equipment. The licensed practical/vocational nurse (LPN/LVN) is responsible for being competent in the appropriate and safe use of equipment and for ensuring that UAP are knowledgeable regarding proper use of assistive devices.
Equally important is the use of appropriate body mechanics or movements that protect large muscle groups from injury and provide safety for patients during ambulation assistance. Special care should be taken in the care of older adults (see Life Span Considerations for Older Adults box regarding mobility). Assistive devices such as splints, crutches, braces, canes, gait belts, and walkers are available to aid in promotion of patient activity. Also important is the need to teach the patient appropriate positioning for home care and to help a family member to learn how to assist the patient at home.
Use of Appropriate Body Mechanics
Understanding of body mechanics (the area of physiology for the study of muscle action and how muscles function in maintaining the posture of the body and prevention of injury during activity) includes knowledge of how certain muscle groups are used. The nurse uses body mechanics daily in making beds, assisting the patient to walk, carrying supplies and equipment, lifting, providing patient care, and carrying out other procedures.
For prevention of injury to the nurse and the patient, principles of body mechanics for health care workers (Table 8-1) should be followed by all health care professionals and personnel. Patients should also be taught principles of good body mechanics to protect themselves. The appropriate use of body mechanics should consistently be practiced in the workplace and in one's personal life so that MSDs do not occur. Maintenance of appropriate body alignment is the key factor in proper body mechanics. The term alignment refers to the relationship of various body parts to each other. Alignment helps balance and helps coordinate movements smoothly and effectively.
Table 8-1
Body Mechanics for Health Care Workers
| ACTION | RATIONALE |
| When planning to move a patient, arrange for adequate help. Use mechanical aids if help is unavailable. | Two workers lifting together divide the workload by 50%. |
| Encourage patient to assist as much as possible. | This promotes patient's abilities and strength while keeping workload to a minimum. |
| Keep back, neck, pelvis, and feet aligned. Avoid twisting. | Twisting increases risk of injury. |
| Flex knees; keep feet shoulder length apart. | A broad base of support increases stability. |
| Position yourself close to patient (or object being lifted). | This minimizes strain and undue stress on the lifter. Holding an object or patient away from the body increases the workload. |
| Use arms and legs (not back). | The leg muscles are stronger larger muscles capable of greater work without injury. |
| Slide patient toward yourself using a pull sheet. | Sliding requires less effort than lifting. Pull sheet keeps to a minimum any shearing forces, which can damage patient's skin. |
| Set (tighten) abdominal and gluteal muscles in preparation for move. | Preparing muscles for the load limits strain to the least possible level.* |
| Person with the heaviest load coordinates efforts of team involved by counting to 3. | Simultaneous lifting keeps the load for any one lifter to a minimum. |
* Back injuries are still the most common occupational injury among nurses.
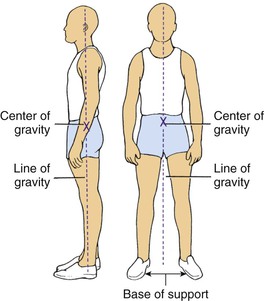
Maintenance of a wide base of support (a stance with feet shoulder width apart) when standing is one of the basic concepts of good body mechanics and alignment that should be followed because it helps in providing better stability (Figure 8-1). Better stability prevents the nurse from losing proper balance while carrying out patient care, which could result in strain or injury to muscles.
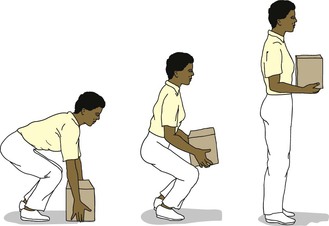
The skeletal muscles and the nervous system maintain equilibrium, or balance, which facilitates appropriate body alignment when lifting, bending, moving, and performing other activities. Bending one's knees and hips before attempting these activities protects the back from the stress and potential injury inherent in the physical work of nursing. When stooping, the hips and knees should be flexed or bent and appropriate body alignment maintained (i.e., the back kept straight). Bending from the waist should be avoided because this will, in time, strain the lower back (Figure 8-2). The nurse should work at a height or level that is comfortable to help prevent undue stress and strain on the back muscles. This can be easily accomplished by adjusting the height of the bed to a level appropriate for the nurse's height.
Use of large muscle groups (such as arm and shoulder muscles, hips, and thigh muscles) helps in performing a bigger workload more safely. The more muscle groups used, the more evenly the workload is distributed. If the base of support is widened in the direction of movement, less effort is needed to carry out an activity. To avoid twisting the spine, the nurse should stand directly in front of the person or object being worked with.
Nurses have numerous other ways to protect themselves and the patient from injury. Carrying objects close to the midline of the body (see Figure 8-2), avoiding reaching too far, avoiding lifting when other means of movement are available (such as sliding, rolling, pushing, or pulling), using devices instead of or in combination with lifting, and using alternating periods of rest and activity are just a few of the ways to prevent injury. Knowing the maximum weight that is safe to carry is also important. Many facilities suggest a 50-lb weight limit on lifting for their staff.
Nurses should assess their own abilities and limitations and those of the person helping, if working in pairs. Correct use of body mechanics is essential to providing efficient care while preventing injury (Box 8-1).
 Positioning of Patients
Positioning of Patients
Positioning of patients is a common intervention performed by nursing personnel. Many positions can be used to prevent patients from development of complications (Skill 8-1 and the Patient Teaching box on mobility). Inappropriate positioning poses the risk of causing permanent disability.
Mobility Versus Immobility
Mobility is a person's ability to move around freely in his or her environment. Moving about serves many purposes, including exercising, expressing emotion, attaining basic needs, performing recreational activities, and completing activities of daily living (ADLs; those activities of physical self-care such as bathing, dressing, and eating). In addition, mobility is fundamental to maintaining the body's normal physiologic activities. For normal physical mobility, the body's nervous, muscular, and skeletal systems must be intact, functioning, and used regularly. Although a person may welcome a rare day to lie in bed and rest, the person who is immobile (experiencing immobility, the inability to move around freely) is predisposed to a wide variety of complications (Box 8-2).
Many types of health problems potentially lead to a decline in a patient's mobility. Patients with certain illnesses, injuries, or surgeries sometimes experience a period of immobilization as a result of changes in medical and physical status. In some cases, immobilization is also used therapeutically to limit the movement of the whole body or a body part, and some patients are under ambulation restrictions.
Interventions to prevent complications of immobility are varied, and many do not require a physician's order (see Box 8-2).
Various assistive devices help maintain correct body positioning and prevent complications that commonly arise when a patient needs prolonged bed rest (Table 8-2). Several of the devices are especially useful in the care of patients who have a loss of sensation, mobility, or consciousness (Figures 8-3 to 8-5).
Table 8-2
Assistive Devices for Proper Positioning
| DEVICE | REASON FOR USE |
| Pillow | Provides support of body or extremity; elevates body part; splints incisional area to reduce postoperative pain during activity or coughing and deep breathing |
| Foot boots or foot boards | Maintain feet in dorsiflexion, which prevents plantar flexion (foot drop) |
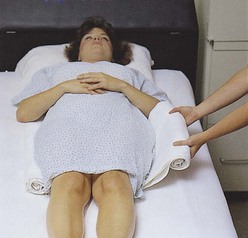
| Trochanter roll (see Figure 8-3) | Prevents external rotation of legs when patient is in supine position; possible to make with a bath blanket |
| Sandbag | Provides support and shape to body contours; immobilizes extremity; maintains specific body alignment |
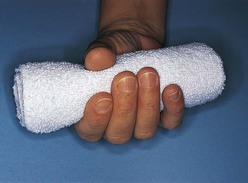
| Hand roll (see Figure 8-4) | Maintains thumb slightly adducted and in opposition to fingers; maintains fingers in slightly flexed position |
| Hand-wrist splint | Individually molded for patient to maintain proper alignment of thumb; slightly adducted in opposition to fingers; maintains wrist in slight dorsiflexion |
| Trapeze bar (see Figure 8-5) | Enables patient to raise trunk from bed; enables patient to transfer from bed to wheelchair; allows patient to perform exercises that strengthen upper arms |
| Side rail | Helps weak patient to roll from side to side or to sit up in bed |
| Bed board | Provides additional support to mattress and improves vertebral alignment |
| Wedge pillow | Also called abductor pillow (triangular pillow made of heavy foam); used to maintain the legs in abduction after total hip replacement surgery |
Modified from Potter PA, Perry AG, Stocket PA: Basic nursing: Essentials for practice, ed 7, St. Louis, 2011, Mosby.
Neurovascular Function
One of the responsibilities of the nurse is frequent monitoring of the patient's neurovascular function, or circulation, movement, and sensation (CMS) assessment. The LPN/LVN checks for skin color, temperature, movement, sensation, pulses, capillary refill, and pain. The affected limb should be compared with the unaffected one (Table 8-3).
Table 8-3
Assessment of Neurovascular Status
| CHARACTERISTIC | ASSESSMENT TECHNIQUE | NORMAL FINDINGS |
| Skin color | Inspect the color of the skin distal to the injury. | The skin color should match that of the unaffected body part. |
| Skin temperature | Palpate the area distal to the injury to determine whether any change in skin temperature has occurred compared with other body parts. | The skin is warm to the touch. |
| Movement | Ask the patient to move the affected area or the area distal to the injury, unless contraindicated. | The patient is able to move with minimal difficulty and with minimal, if any, discomfort. |
| Move the area distal to the injury if the patient is unable to move the body part on his or her own. | No difference in comfort is found compared with the patient actively moving the body part. | |
| Sensation | Ask the patient if numbness or tingling is present (paresthesia), and assess with proper devices as necessary, such as a cotton-tipped applicator or tongue blade. | No numbness or tingling occurs; no difference in sensation is seen in the affected and unaffected body parts. |
| Assess sensation with a cotton-tipped applicator, tongue blade, or other device as indicated. | Loss of sensation may indicate nerve or circulatory impairment. | |
| Pulses | Palpate the pulses distal to the site of injury. | Pulses are strong and easily palpated; no difference is found in the affected and unaffected extremities. |
| Capillary refill | Press the nail beds distal to the injury until blanching occurs (or until the skin near the nail blanches, if nails are thick and brittle); pressure should be applied for approximately 3 to 5 sec. | Blood returns (return to usual color) within 3 sec (5 sec for older adult patients). |
| Pain | Ask the patient about the location, the nature, and the frequency of pain and to rate the pain with a pain scale. | The patient should have no or minimal reports of pain. |
This assessment is especially important when compression from external devices, such as casts and bulky dressings, creates the risk of acute compartment syndrome, which has the potential to cause extensive tissue damage. Acute compartment syndrome occurs in the extremities, especially the legs, where a sheath of inelastic fascia partitions blood vessel, nerve, and muscle tissue. Normally, the pressure in this compartment is less than capillary pressure. However, compression created by external pressure or the accumulation of excessive tissue fluid from severe burns, fractures, crushing injuries, or severely bruised muscles increases compartmental pressure and in some cases leads to compartment syndrome. Ischemic tissue necrosis is likely to occur within 4 to 8 hours unless this pressure is relieved and compartment syndrome reversed (American Academy of Orthopaedic Surgeons, 2009).
Symptoms of acute compartment syndrome include pain within the muscle, especially when stretched, that is more intense than expected from the injury or causative factor; tingling and burning or a feeling of pins and needles in the affected area (paresthesias); and a full or tight feeling in the muscle. Numbness and paralysis are late signs of compartment syndrome and may be indicative of permanent damage.
Acute compartment syndrome is an emergency situation. The earlier compartment syndrome is treated, the better the prognosis. If acute compartment syndrome is caused by an external device, such as a cast or tight bandage, the pressure should be removed immediately by cutting away these devices. If the syndrome is caused by other factors, surgical intervention may be required. A fasciotomy may be necessary, in which the surgeon makes an incision into the skin and fascia to release the pressure. This incision is sometimes left open until swelling subsides.
Chronic compartment syndrome is not an emergency situation and is usually caused by exercise that involves repetitive movement, such as bicycling or running. The symptoms include pain and cramping during exercise, visible muscle bulging, and numbness. These symptoms are usually alleviated by discontinuing the activity and by rest.
Performance of Range-of-Motion Exercises
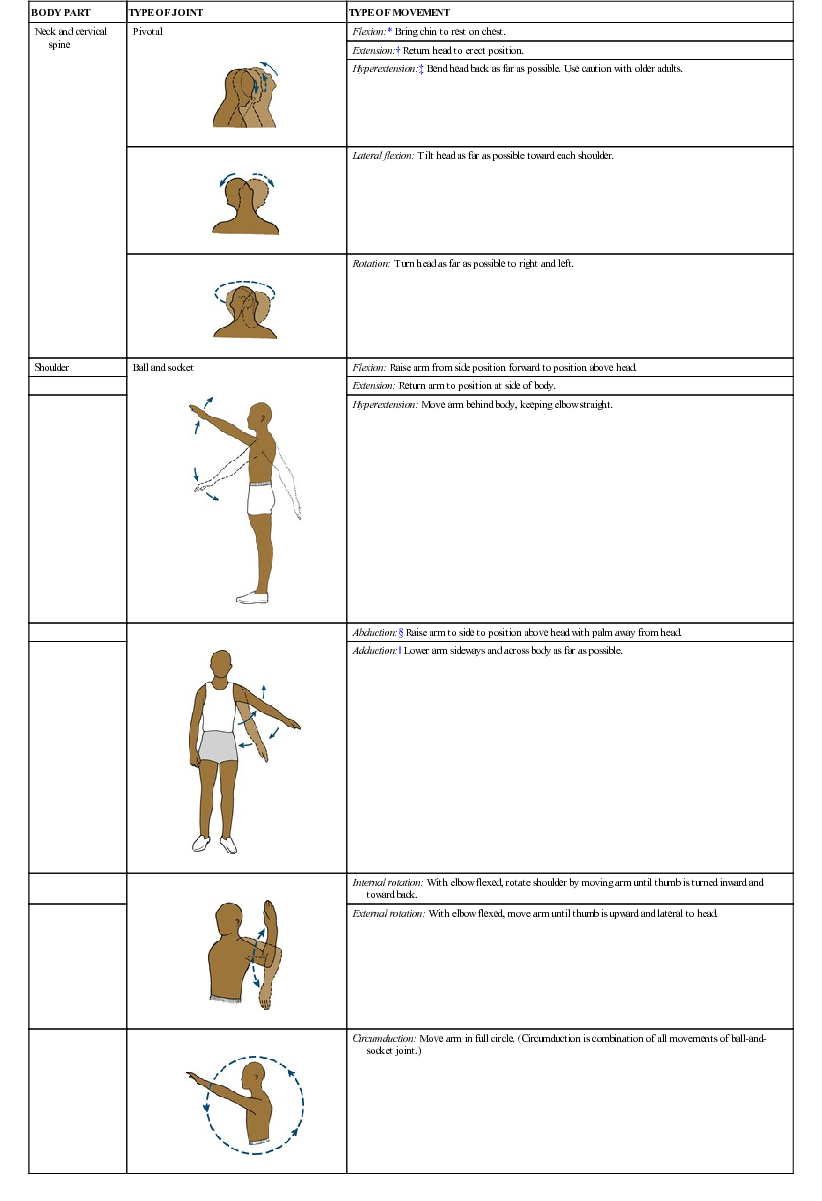
Regardless of whether the causes of immobility are permanent or temporary, the immobilized patient needs some type of exercise to prevent excessive muscle atrophy and joint contracture. The nurse and other health care personnel, including members of the physical therapy department, help the patient with decreased mobility to perform range-of-motion (ROM; movement of the body that involves the muscles and joints in natural directional movements) exercises. Passive ROM exercise is performed by caregivers, and active ROM by patients. The designated joint (any one of the connections between bones) is moved actively or passively to the point of resistance or pain, with avoidance of injury. ROM exercises are increased with subsequent exercises as tolerated (Table 8-4 and Skill 8-2). ![]()
Table 8-4
Joint Range-of-Motion Exercises
| BODY PART | TYPE OF JOINT | TYPE OF MOVEMENT |
| Neck and cervical spine | Pivotal | Flexion:* Bring chin to rest on chest. |
| Extension:† Return head to erect position. | ||
| Hyperextension:‡ Bend head back as far as possible. Use caution with older adults. | ||
 | Lateral flexion: Tilt head as far as possible toward each shoulder. | |
 | Rotation: Turn head as far as possible to right and left. | |
| Shoulder | Ball and socket | Flexion: Raise arm from side position forward to position above head. |
| Extension: Return arm to position at side of body. | ||
| Hyperextension: Move arm behind body, keeping elbow straight. | ||
 | Abduction:§ Raise arm to side to position above head with palm away from head. | |
| Adduction:‖ Lower arm sideways and across body as far as possible. | ||
 | Internal rotation: With elbow flexed, rotate shoulder by moving arm until thumb is turned inward and toward back. | |
| External rotation: With elbow flexed, move arm until thumb is upward and lateral to head. | ||
 | Circumduction: Move arm in full circle. (Circumduction is combination of all movements of ball-and-socket joint.) | |
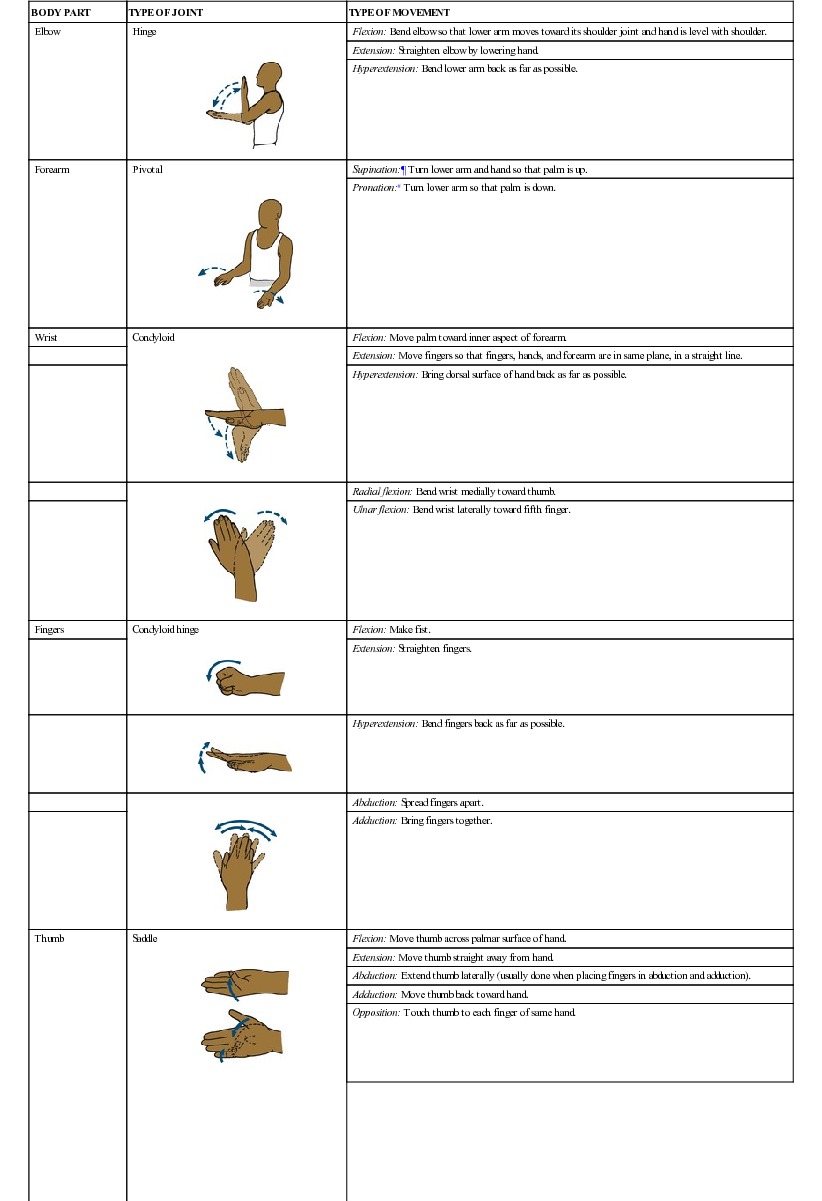
| Elbow | Hinge | Flexion: Bend elbow so that lower arm moves toward its shoulder joint and hand is level with shoulder. |
| Extension: Straighten elbow by lowering hand. | ||
| Hyperextension: Bend lower arm back as far as possible. | ||
| Forearm | Pivotal | Supination:¶ Turn lower arm and hand so that palm is up. |
| Pronation:# Turn lower arm so that palm is down. | ||
| Wrist | Condyloid | Flexion: Move palm toward inner aspect of forearm. |
| Extension: Move fingers so that fingers, hands, and forearm are in same plane, in a straight line. | ||
| Hyperextension: Bring dorsal surface of hand back as far as possible. | ||
 | Radial flexion: Bend wrist medially toward thumb. | |
| Ulnar flexion: Bend wrist laterally toward fifth finger. | ||
| Fingers | Condyloid hinge | Flexion: Make fist. |
| Extension: Straighten fingers. | ||
 | Hyperextension: Bend fingers back as far as possible. | |
 | Abduction: Spread fingers apart. | |
| Adduction: Bring fingers together. | ||
| Thumb | Saddle | Flexion: Move thumb across palmar surface of hand. |
| Extension: Move thumb straight away from hand. | ||
| Abduction: Extend thumb laterally (usually done when placing fingers in abduction and adduction). | ||
| Adduction: Move thumb back toward hand. | ||
| Opposition: Touch thumb to each finger of same hand. | ||
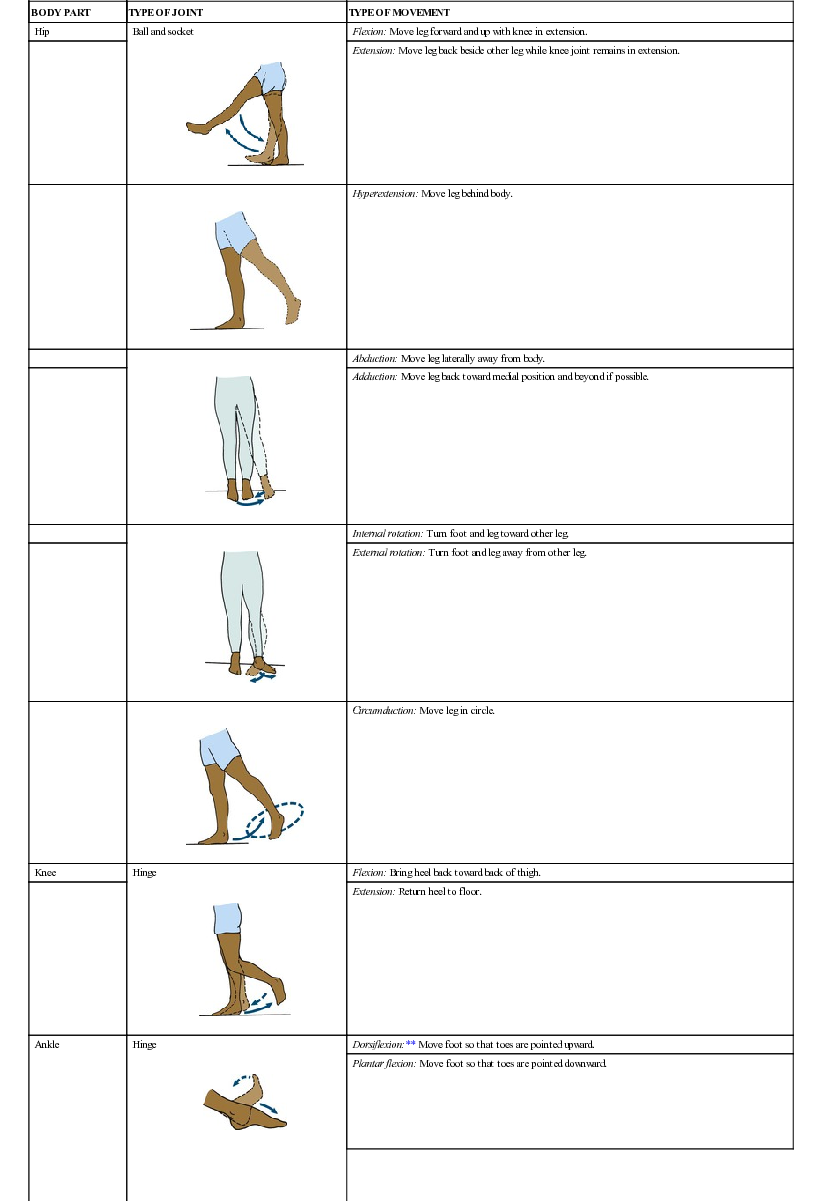
| Hip | Ball and socket | Flexion: Move leg forward and up with knee in extension. |
| Extension: Move leg back beside other leg while knee joint remains in extension. | ||
 | Hyperextension: Move leg behind body. | |
 | Abduction: Move leg laterally away from body. | |
| Adduction: Move leg back toward medial position and beyond if possible. | ||
 | Internal rotation: Turn foot and leg toward other leg. | |
| External rotation: Turn foot and leg away from other leg. | ||
 | Circumduction: Move leg in circle. | |
| Knee | Hinge | Flexion: Bring heel back toward back of thigh. |
| Extension: Return heel to floor. | ||
| Ankle | Hinge | Dorsiflexion:** Move foot so that toes are pointed upward. |
| Plantar flexion: Move foot so that toes are pointed downward. | ||
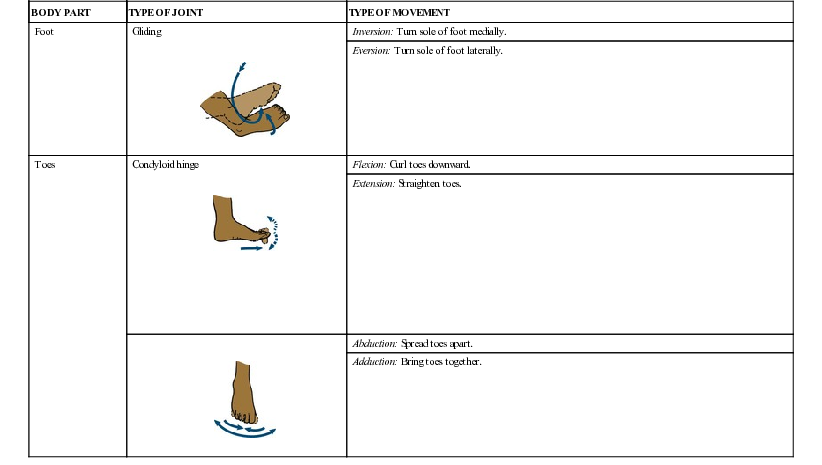
| Foot | Gliding | Inversion: Turn sole of foot medially. |
| Eversion: Turn sole of foot laterally. | ||
| Toes | Condyloid hinge | Flexion: Curl toes downward. |
| Extension: Straighten toes. | ||
 | Abduction: Spread toes apart. | |
| Adduction: Bring toes together. |
* Flexion: Movement of certain joints that decreases angle between two adjoining bones.
† Extension: Movement of certain joints that increases angle between two adjoining bones.
‡ Hyperextension: Extreme or abnormal extension.
§ Abduction: Movement of limb away from body.
‖ Adduction: Movement of limb toward axis of body.
¶ Supination: Kind of rotation that allows palm of hand to turn up.
# Pronation: Palm of hand turned down.
** Dorsiflexion: To bend or flex backward.
Figures from Potter PA, Perry AG: Fundamentals of nursing: Concepts, process, and practice, ed 6, St. Louis, 2006, Mosby.
Modified from Potter PA, Perry AG: Basic nursing: Essentials for practice, ed 7, St. Louis, 2012, Mosby.
Some patients who are weak or partially paralyzed are able to move a limb partially through ROM and the nurse may then assist the patient to finish the full ROM. This is referred to as passive assisted ROM. Active assisted ROM occurs when the patient uses the strong arm to exercise the weaker or paralyzed arm. The LPN/LVN best meets the needs of the patient by encouraging the patient to be as independent as possible.
Assessment by the nurse and the physical therapy department determines the patient's current mobility status. The patient who is able to move about freely independently performs ADLs and active ROM exercises. Patients who are partially immobile or unable to move about freely (from paraplegia, quadriplegia, weakness, or fatigue) need the nurse and other health care personnel to assist with passive ROM exercises.
Encourage and assess active ROM every day (see Life Span Considerations for Older Adults box). The total amount of activity required to prevent physical disuse syndrome (a state in which an individual is at risk for deterioration of body systems due to prescribed or unavoidable inactivity) is only about 2 hours for every 24-hour period. Schedule this activity throughout the day to prevent the patient from remaining inactive for long periods (Ackley and Ladwig, 2011).
Continuous Passive Motion Machines
Continuous passive motion (CPM) machines flex and extend joints for passive mobilization without the strain of active exercises (Figure 8-6). This therapy is frequently used immediately after total knee replacement surgery (knee arthroplasty), but CPM can also be used in outpatient or home physical therapy programs. The CPM machine's settings must be adjusted according to the health care provider's orders for the degree and the speed of flexion and extension for each individual patient to prevent damage to the joint or surgical site. Some recent studies question the necessity of CPM machines and encourage the use of immediate physical therapy instead.
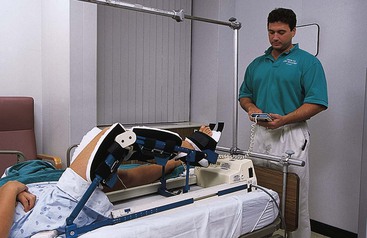
CPM machines can be used on joints other than the knee, including the hip, the shoulder, and the ankle. Mobilization of the joint prevents complications, such as joint contracture, atrophy of surrounding muscles, and thromboembolism.
With use of a CPM machine, consider the following (Perry et al., 2012):
• Older adults who need CPM therapy after discharge sometimes must enter a rehabilitation facility or have home care because the equipment is not easy to manipulate.
• Older adults with fragile skin are at a high risk of skin impairment from pressure of the CPM machine. Closely monitor pressure points such as the heel.
• Physical therapy is frequently used in addition to the CPM therapy.
• If the patient is using CPM at home, ensure that the patient and the family members assisting with care are given instructions on use of the CPM machine, prescribed settings, and parameters for contacting the physician.
• The goals of CPM therapy are to increase or maintain mobility by improving joint range of motion and to prevent skin breakdown at pressure points.
• Care of the patient during CPM therapy can be delegated to assistive personnel, but assessment of the patient must not be. Assessment remains a nursing responsibility.
Moving the Patient
A common nursing action is assisting patients in movement. Patients may need assistance in various ways, such as moving the patient up in bed, out of bed, or from a chair or wheelchair; turning the patient; and assisting the patient in and out of the bed for ambulation (Skill 8-3). For some situations, the nurse uses mechanical equipment for lifting patients, such as the hydraulic lift, roller board, and gurney lift. The nurse should first mentally think through the lift in an effort to be prepared for lifting the patient and then physically perform the lift. The nurse must ensure that patients do not become too dependent on assistance with mobility. Frequent assessment of the patient's ability to assist with mobility is necessary to prevent overdependence. The LPN/LVN should also assess the patient for pain and administer pain medications before activities that cause further pain (Box 8-3 and Coordinated Care box).
Use of the Lift for Moving Patients
Mechanical devices, such as the patient lift with a sling (Figure 8-7), are useful for moving patients safely and protecting the nurse's back and for full-weight lifting of patients who cannot assist. Follow agency policy for use of the lift (Skill 8-4).
 Nursing Process for Patient Mobility
Nursing Process for Patient Mobility
The role of the LPN/LVN in the nursing process as stated is that the LPN/LVN.
• Participates in planning care for patients based on patient needs.
• Reviews the patient's plan of care and recommends revisions as needed.
• Reviews and follows defined prioritization for patient care.
• Uses clinical pathways, care maps, or care plans to guide and review patient care.
 Assessment
Assessment
Assessment focuses on ROM, muscle strength, activity tolerance, gait, and posture. Observation during ADLs enables the nurse to estimate the patient's fatigability, muscle strength, and ROM. Further assessment helps determine the type of assistance the patient needs to change position or transfer from bed to chair or wheelchair. These assessments give the LPN/LVN an understanding of the patient's overall level of mobility and coordination (see the Cultural Considerations box).
It is acceptable to delegate the skills of safe and effective transfer from bed to chair to UAP who have successfully demonstrated good body mechanics and safe transfer techniques for patients involved.
Teaching patients how to use assistive devices requires critical thinking and knowledge application unique to a nurse. However, UAP are able to assist ambulatory patients with assistive devices.
• Have patient wear shoes with a nonskid surface during ambulation.
• Be sure the area is free of clutter, wet areas, and rugs that may slide or buckle.
• Ensure UAP know how to use an intravenous (IV) pole to assist in ambulation for patients with continuous IV therapy.
• Be sure the patient uses the correct gait and weight bearing during ambulation.
• Ease patients to a sitting position in a chair or on the floor if they become dizzy or faint.
• Alert the LPN/LVN if a patient becomes dizzy or lightheaded or suffers a fall.
The skill of performing ROM exercises can be delegated to UAP. Patients with spinal cord or orthopedic trauma or surgery usually require exercise by nurses or physical therapists. When delegating this skill, the nurse should instruct UAP to perform exercises slowly and provide adequate support to the joint being exercised. In addition, the nurse should remind UAP not to exercise joints beyond the point of resistance or to the point of fatigue or pain. In addition, if muscle spasms occur, exercise should stop until the spasms have subsided.
The nurse may delegate the skill of safe and effective transfer with a mechanical lift to UAP who have demonstrated ability to use good body mechanics and safe transfer techniques and equipment (mechanical lift).
 Nursing Diagnosis
Nursing Diagnosis
Assessment enables the nurse to cluster relevant data and develop actual or potential (risk) nursing diagnoses related to the patient's needs. The nursing diagnoses are stated along with the probable causes “related to (r/t).” Identification of the cause of the problem further individualizes the care plan and leads to selection of appropriate care.
 Expected Outcomes and Planning
Expected Outcomes and Planning
The nurse should set goals and expected outcomes with the patient to direct interventions. Care planning is individualized to the patient, with the patient's most immediate needs taken into consideration. These goals are based on the nursing diagnosis formulated.
 Implementation
Implementation
Nursing interventions should be individualized according to the level of risk to the patient. The nurse, the patient, and other members of the health care team work together to determine the most effective interventions (Nursing Care Plan 8-1). While implementing the established goals, the nurse should also assess the patient's readiness to learn and teach appropriate body mechanics (see the Home Care Considerations box on mobility).
The nurse is aware of the patient's motor deficits, ability to aid in transfer, and body weight. As suggested by the National Institute for Occupational Safety and Health's (NIOSH) Division of Safety Research, health care personnel should never attempt to lift more than 35 pounds of a patient's body weight (Howard, 2010). For the safety of the staff and the patient, additional assistance should always be secured when the transferability of a patient is in doubt.
Many special problems are to be considered in transfer. Patients who have been immobile for several days or longer may be weak or have vertigo (dizziness) and sometimes have orthostatic hypotension (a drop in blood pressure) when transferred. A patient with neurologic deficits perhaps has paresis (muscle weakness) or paralysis unilaterally or bilaterally, which complicates safe transfer. A flaccid arm can easily sustain injury during transfer if unsupported. The nurse must be creative when necessary in the transfer of trauma patients. As a general rule, a gait (transfer) belt should be used and assistance obtained for mobilization of such patients.
 Evaluation
Evaluation
The success of interventions is evaluated with a comparison of the patient's response with the outcome established for each nursing goal, such as the following:
1. Ask the patient to rate fatigue on a scale of 1 to 10 (determines need for additional pain control).
2. Note the patient's behavioral response to transfer (reveals level of motivation and self-care potential).
For evaluation of the patient's perception of the interventions, knowledge of the patient's expectations concerning joint mobility, posture, or body alignment is necessary first. What is acceptable or anticipated on the nurse's part is sometimes vastly different from what the patient and family members anticipate or are able to accept.
























