ELBOW JOINT
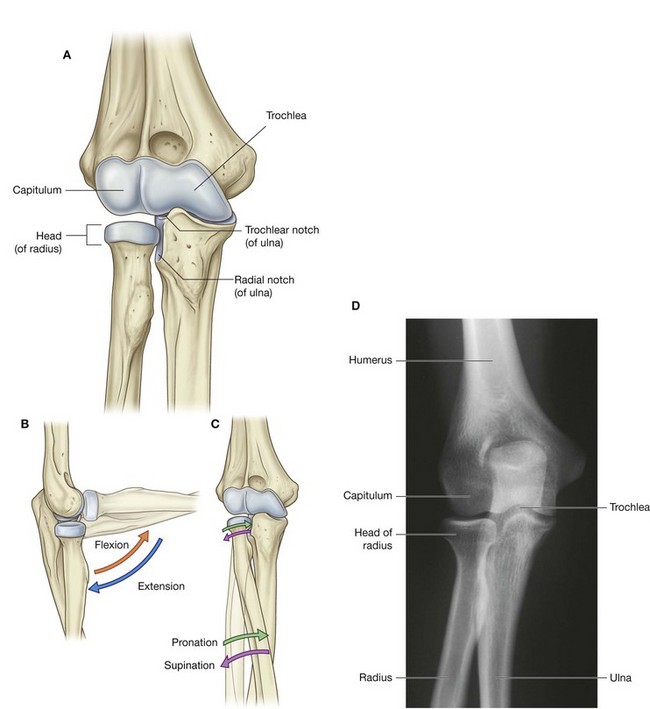
The elbow joint is a complex joint involving three separate articulations, which share a common synovial cavity (Fig. 7.71).

The joints between the trochlear notch of the ulna and the trochlea of the humerus and between the head of the radius and the capitulum of the humerus are primarily involved with hinge-like flexion and extension of the forearm on the arm and, together, are the principal articulations of the elbow joint.

The joint between the head of the radius and the radial notch of the ulna, the proximal radio-ulnar joint, is involved with pronation and supination of the forearm.
The articular surfaces of the bones are covered with hyaline cartilage.
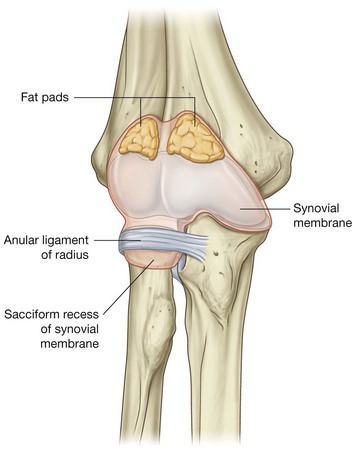
The synovial membrane originates from the edges of the articular cartilage and lines the radial fossa, the coronoid fossa, the olecranon fossa, the deep surface of the joint capsule, and the medial surface of the trochlea (Fig. 7.72).
The synovial membrane is separated from the fibrous membrane of the joint capsule by pads of fat in regions overlying the coronoid fossa, the olecranon fossa, and the radial fossa. These fat pads accommodate the related bony processes during extension and flexion of the elbow. Attachments of the brachialis and triceps brachii muscles to the joint capsule overlying these regions pull the attached fat pads out of the way when the adjacent bony processes are moved into the fossae.
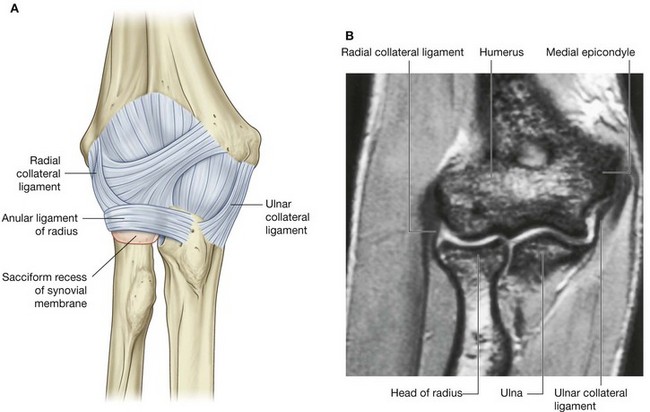
The fibrous membrane of the joint capsule overlies the synovial membrane, encloses the joint, and attaches to the medial epicondyle and the margins of the olecranon, coronoid, and radial fossae of the humerus (Fig. 7.73). It also attaches to the coronoid process and olecranon of the ulna. On the lateral side, the free inferior margin of the joint capsule passes around the neck of the radius from an anterior attachment to the coronoid process of the ulna to a posterior attachment to the base of the olecranon.
The fibrous membrane of the joint capsule is thickened medially and laterally to form collateral ligaments, which support the flexion and extension movements of the elbow joint (Fig. 7.73).
In addition, the external surface of the joint capsule is reinforced laterally where it cuffs the head of the radius with a strong anular ligament of radius. Although this ligament blends with the fibrous membrane of the joint capsule in most regions, they are separate posteriorly. The anular ligament of radius also blends with the radial collateral ligament.
The anular ligament of radius and related joint capsule allow the radial head to slide against the radial notch of the ulna and pivot on the capitulum during pronation and supination of the forearm.
The deep surface of the fibrous membrane of the joint capsule and the related anular ligament of radius that articulate with the sides of the radial head are lined by cartilage. A pocket of synovial membrane (sacciform recess) protrudes from the inferior free margin of the joint capsule and facilitates rotation of the radial head during pronation and supination.
Vascular supply to the elbow joint is through an anastomotic network of vessels derived from collateral and recurrent branches of the brachial, profunda brachii, radial, and ulnar arteries.
The elbow joint is innervated predominantly by branches of the radial and musculocutaneous nerves, but there may be some innervation by branches of the ulnar and median nerves.
In the clinic
Elbow joint injury
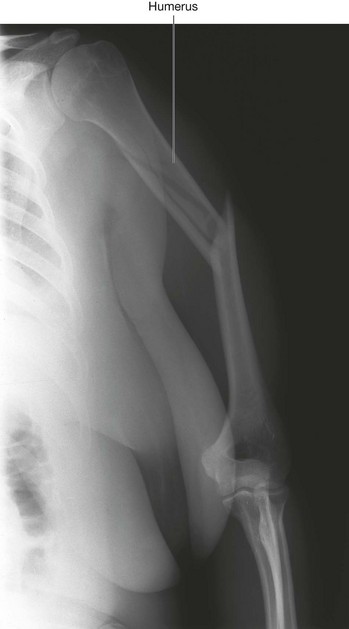
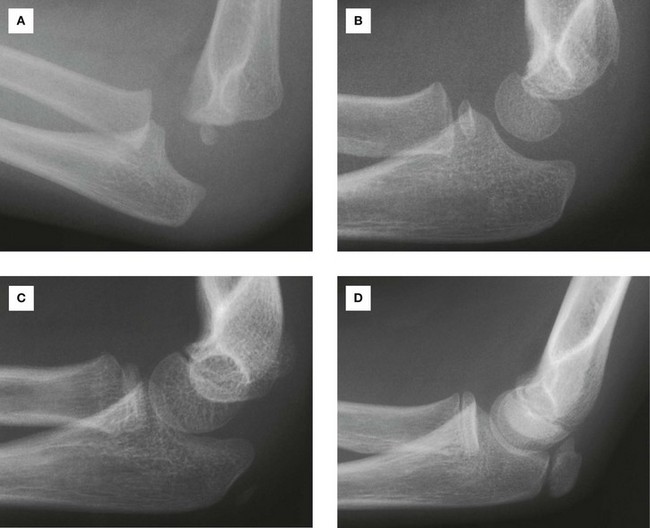
The elbow joint can be injured in many ways; the types of injuries are age dependent. When a fracture or soft tissue trauma is suspected, a plain lateral and an anterior–posterior radiograph are obtained. In an adult it is usually not difficult to interpret the radiograph, but in children additional factors require interpretation.
As the elbow develops in children, numerous secondary ossification centers appear before and around puberty. It is easy to mistakenly interpret these as fractures. In addition, it is also possible for the epiphyses and apophyses to be “pulled off” or disrupted. Therefore, when interpreting a child’s radiograph of the elbow, the physician must know the child’s age (Fig. 7.74). Fusion occurs at around the time of puberty. An understanding of the normal epiphyses and apophyses and their normal relationship to the bones will secure a correct diagnosis. The approximate ages of appearance of the secondary ossification centers around the elbow joint are:

capitulum—1 year;

head (of radius)—5 years;

medial epicondyle—5 years;

trochlea—11 years;

olecranon—12 years;

lateral epicondyle—13 years.
In the clinic
Supracondylar fracture of the humerus
Elbow injuries in children may result in a transverse fracture of the distal end of the humerus, above the level of the epicondyles. This fracture is termed a supracondylar fracture. The distal fragment and its soft tissues are pulled posteriorly by the triceps muscle. This posterior displacement effectively “bowstrings” the brachial artery over the irregular proximal fracture fragment. In children, this is a relatively devastating injury: the muscles of the anterior compartment of the forearm are rendered ischemic and form severe contractions, significantly reducing the function of the anterior compartment and flexor muscles (Volkmann’s ischemic contracture).
In the clinic
Transection of the radial or ulnar arteries
Adult patients may transect the radial or ulnar arteries because these vessels are relatively subcutaneous. A typical method of injury is when the hand is forced through a plate glass window. Fortunately, the dual supply to the hand enables the surgeon to tie off either the ulnar or the radial artery, without significant consequence.
In the clinic
Pulled elbow
Pulled elbow is a disorder that typically occurs in children under 5 years of age. It is commonly caused by a sharp pull of the child’s hand, usually when the child is pulled up a curb. The not-yet-developed head of the radius and the laxity of the anular ligament of radius allow the head to sublux from this cuff of tissue. Pulled elbow is extremely painful, but can be treated easily by simple supination and compression of the elbow joint by the clinician. When the radial head is relocated the pain subsides immediately and the child can continue with normal activity.
In the clinic
Fracture of the head of radius
A fracture of the head of radius is a common injury and can cause appreciable morbidity. It is one of the typical injuries that occur with a fall on the outstretched hand. On falling, the force is transmitted to the radial head, which fractures. These fractures typically result in loss of full extension, and potential surgical reconstruction may require long periods of physiotherapy to obtain a full range of movement at the elbow joint.
A lateral radiograph of a fracture of the head of radius typically demonstrates the secondary phenomenon of this injury. When the bone is fractured, fluid fills the synovial cavity, elevating the small pad of fat within the coronoid and olecranon fossae. These fat pads appear as areas of lucency on the lateral radiograph—the “fat pad” sign. This radiological finding is useful because fracture of the head of radius is not always clearly visible. If there is an appropriate clinical history, tenderness around the head of radius and positive fat pad sign, a fracture can be inferred clinically even if no fracture can be identified on the radiograph, and appropriate treatment can be instituted.
In the clinic
Epicondylitis
It is not uncommon for people who are involved in sports such as golf and tennis to develop an overuse strain of the origins of the flexor and extensor muscles of the forearm. The pain is typically around the epicondyles and usually resolves after rest. If pain and inflammation persist, surgical division of the extensor or flexor origin from the bone may be necessary. Typically, in tennis players this pain occurs on the lateral epicondyle and common extensor origin (tennis elbow), whereas in golfers it occurs on the medial epicondyle and common flexor origin.
In the clinic
Elbow arthritis
Osteoarthritis is extremely common and is usually most severe in the dominant limb. From time to time an arthritic elbow may undergo such degenerative change that small bone fragments appear in the articular cavity. Given the relatively small joint space, these fragments can result in an appreciable reduction in flexion and extension, and typically lodge within the olecranon and coronoid fossae.
In the clinic
Ulnar nerve injury
Posterior to the medial epicondyle of the humerus the ulnar nerve is bound in a fibro-osseous tunnel (the cubital tunnel) by a retinaculum. Older patients may develop degenerative changes within this tunnel, which compresses the ulnar nerve when flexed. The repeated action of flexion and extension of the elbow may cause local nerve damage, resulting in impaired function of the ulnar nerve. Accessory muscles and localized neuritis in this region secondary to direct trauma may also produce ulnar nerve damage.
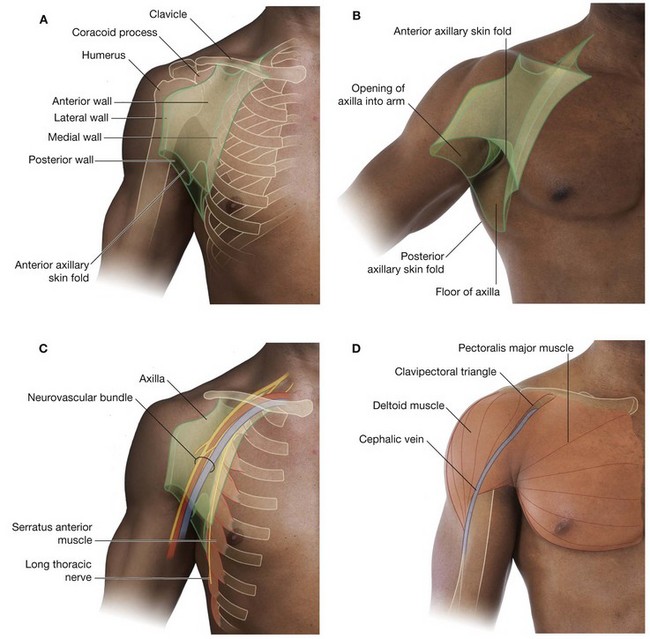
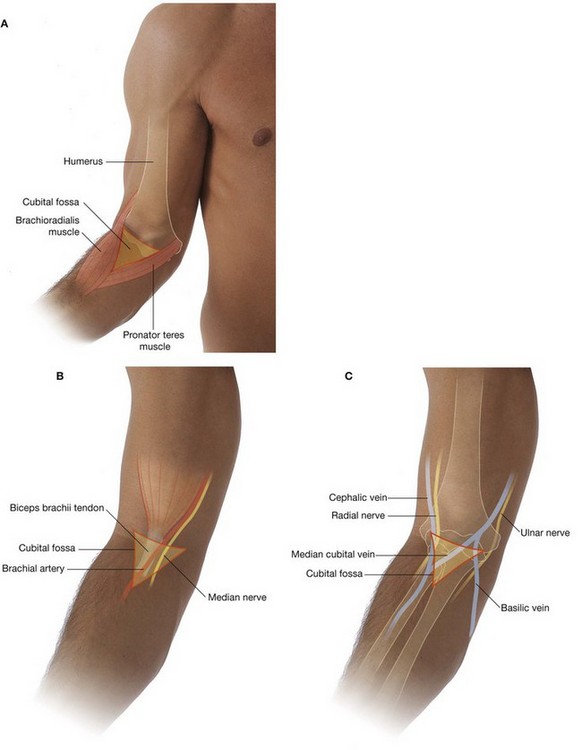
CUBITAL FOSSA
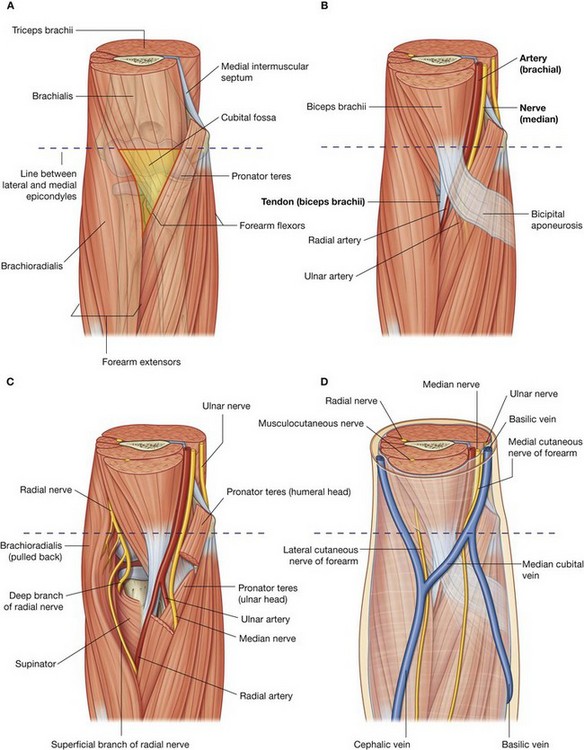
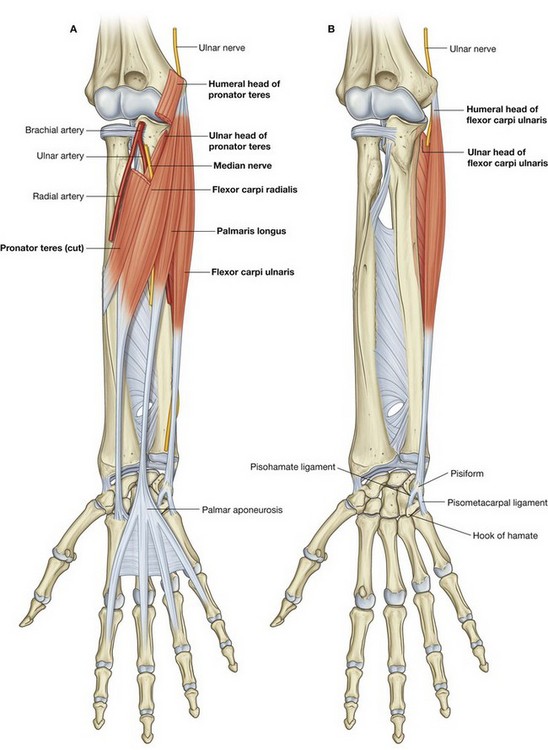
The cubital fossa is an important area of transition between the arm and the forearm. It is located anterior to the elbow joint and is a triangular depression formed between two forearm muscles:

the brachioradialis muscle originating from the lateral supraepicondylar ridge of the humerus;

the pronator teres muscle originating from the medial epicondyle of the humerus (
Fig. 7.75A).
The base of the triangle is an imaginary horizontal line between the medial and lateral epicondyles. The bed or floor of the fossa is formed mainly by the brachialis muscle.
The major contents of the cubital fossa, from lateral to medial, are:

the tendon of the biceps brachii muscle;

the brachial artery; and
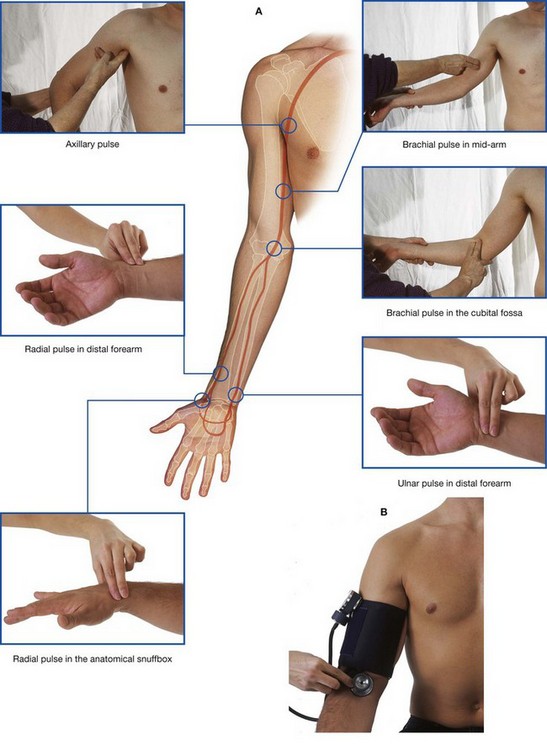
The brachial artery normally bifurcates into the radial and ulnar arteries in the apex of the fossa, although this bifurcation may occur much higher in the arm, even in the axilla (Fig. 7.75B). When taking a blood pressure reading from a patient, the clinician places the stethoscope over the brachial artery in the cubital fossa.
The median nerve lies immediately medial to the brachial artery and leaves the fossa by passing between the ulnar and humeral heads of the pronator teres muscle (Fig. 7.75C).
The brachial artery and the median nerve are covered and protected anteriorly in the distal part of the cubital fossa by the bicipital aponeurosis (Fig. 7.75B). This flat connective tissue membrane passes between the medial side of the tendon of the biceps brachii muscle and deep fascia of the forearm. The sharp medial margin of the bicipital aponeurosis can often be felt.
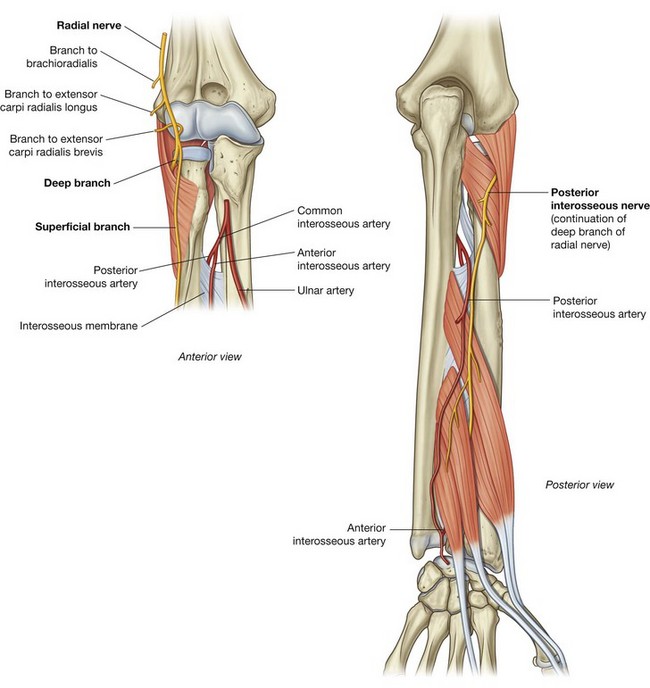
The radial nerve lies just under the lip of the brachioradialis muscle, which forms the lateral margin of the fossa (Fig. 7.75C). In this position, the radial nerve divides into superficial and deep branches:

the superficial branch continues into the forearm just deep to the brachioradialis muscle;

the deep branch passes between the two heads of the supinator muscle (see p. 747 and
Fig. 7.90) to access the posterior compartment of the forearm.
The ulnar nerve does not pass through the cubital fossa. Instead, it passes posterior to the medial epicondyle.
The roof of the cubital fossa is formed by superficial fascia and skin. The most important structure within the roof is the median cubital vein (Fig. 7.75D), which passes diagonally across the roof and connects the cephalic vein on the lateral side of the upper limb with the basilic vein on the medial side. The bicipital aponeurosis separates the median cubital vein from the brachial artery and median nerve. Other structures within the roof are cutaneous nerves—the medial cutaneous and lateral cutaneous nerves of the forearm.
In the clinic
Construction of a dialysis fistula
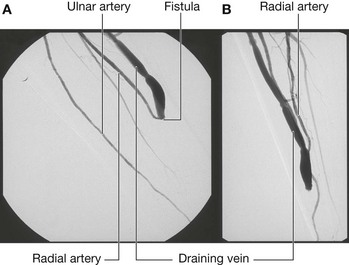
Many patients throughout the world require renal dialysis for kidney failure. The patient’s blood is filtered and cleaned by the dialysis machine. Blood therefore has to be taken from patients into the filtering device and then returned to them. This process of dialysis occurs over many hours and requires considerable flow rates of 250–500 ml per minute. To enable such large volumes of blood to be removed from and returned to the body, the blood is taken from vessels that have a high flow. As no veins in the peripheral limbs have such high flow, a surgical procedure is necessary to create such a system. In most patients, the radial artery is anastomosed (joined) to the cephalic vein (Fig. 7.76) at the wrist, or the brachial artery is anastomosed to the cephalic vein at the elbow. Some surgeons place an arterial graft between these vessels.
After six weeks, the veins increase in size in response to their arterial blood flow and are amenable to direct cannulation or dialysis.
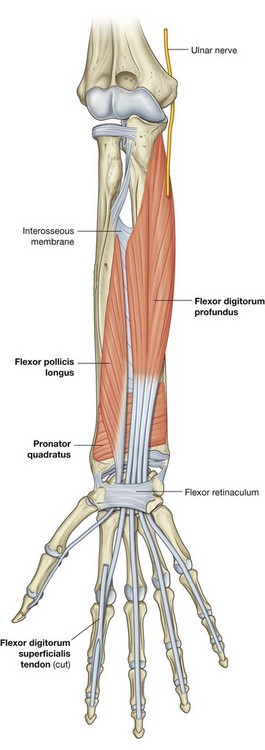
FOREARM
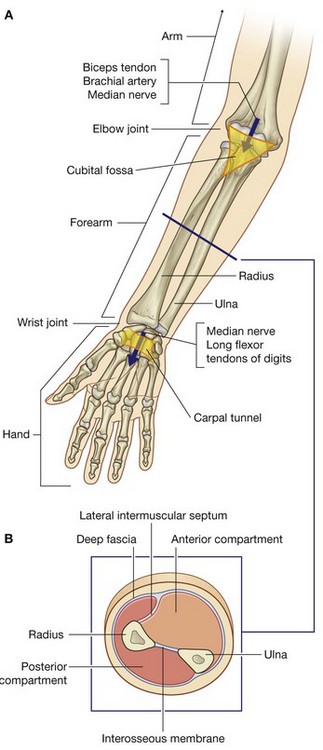
The forearm is the part of the upper limb that extends between the elbow joint and the wrist joint. Proximally, most major structures pass between the arm and forearm through, or in relation to, the cubital fossa, which is anterior to the elbow joint (Fig. 7.77). The exception is the ulnar nerve, which passes posterior to the medial epicondyle of the humerus.
Distally, structures pass between the forearm and the hand through, or anterior to, the carpal tunnel (Fig. 7.77). The major exception is the radial artery, which passes dorsally around the wrist to enter the hand posteriorly.
The bone framework of the forearm consists of two parallel bones, the radius and the ulna (Figs. 7.78 and 7.79). The radius is lateral in position and is small proximally, where it articulates with the humerus, and large distally, where it forms the wrist joint with the carpal bones of the hand.
The ulna is medial in the forearm, and its proximal and distal dimensions are the reverse of those for the radius: the ulna is large proximally and small distally. Proximal and distal joints between the radius and the ulna allow the distal end of the radius to swing over the adjacent end of the ulna, resulting in pronation and supination of the hand.
As in the arm, the forearm is divided into anterior and posterior compartments (Fig. 7.77). In the forearm, these compartments are separated by:

a lateral intermuscular septum, which passes from the anterior border of the radius to deep fascia surrounding the limb;

an interosseous membrane, which links adjacent borders of the radius and ulna along most of their length; and

the attachment of deep fascia along the posterior border of the ulna.
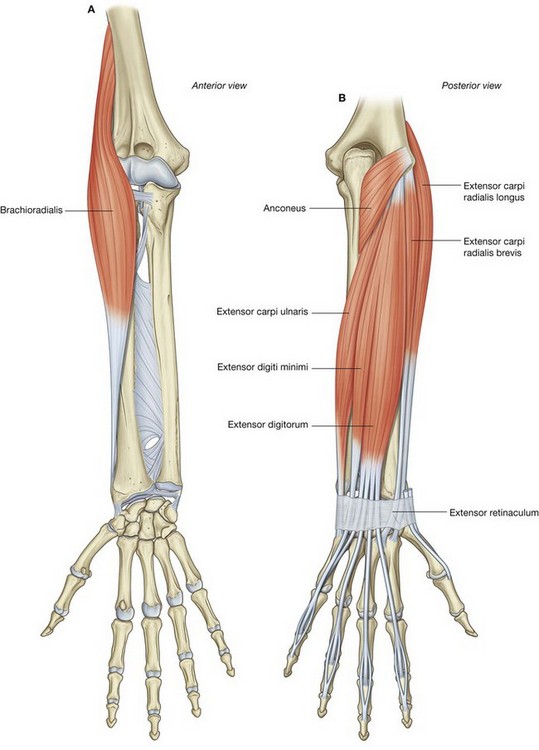
Muscles in the anterior compartment of the forearm flex the wrist and digits and pronate the hand. Muscles in the posterior compartment extend the wrist and digits and supinate the hand. Major nerves and vessels supply or pass through each compartment.
Bones
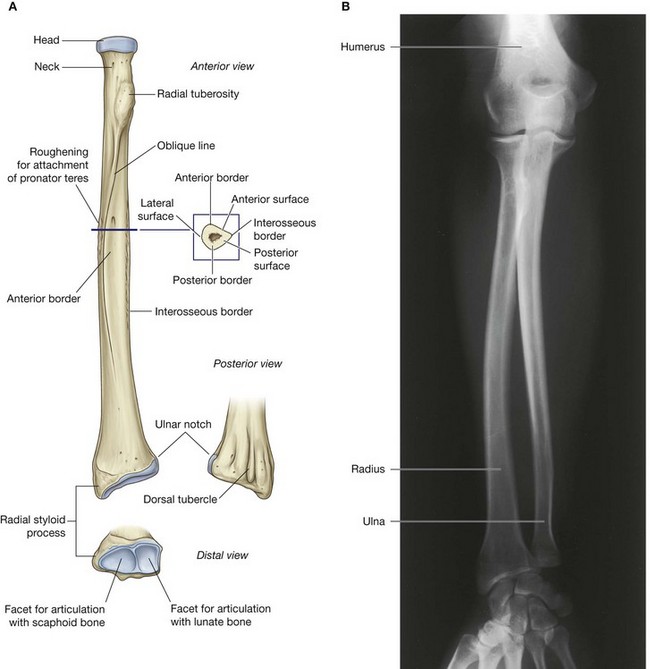
Shaft and distal end of radius
The shaft of the radius is narrow proximally, where it is continuous with the radial tuberosity and neck, and much broader distally, where it expands to form the distal end (Fig. 7.78).
Throughout most of its length, the shaft of the radius is triangular in cross-section, with:

three borders (anterior, posterior, and interosseous); and

three surfaces (anterior, posterior, and lateral).
The anterior border begins on the medial side of the bone as a continuation of the radial tuberosity. In the superior third of the bone, it crosses the shaft diagonally, from medial to lateral, as the oblique line of the radius. The posterior border is distinct only in the middle third of the bone. The interosseous border is sharp and is the attachment site for the interosseous membrane, which links the radius to the ulna.
The anterior and posterior surfaces of the radius are generally smooth, whereas an oval roughening for the attachment of pronator teres marks approximately the middle of the lateral surface of the radius.
Viewed anteriorly, the distal end of the radius is broad and somewhat flattened anteroposteriorly (Fig. 7.78). Consequently, the radius has expansive anterior and posterior surfaces and narrow medial and lateral surfaces. Its anterior surface is smooth and unremarkable, except for the prominent sharp ridge that forms its lateral margin.
The posterior surface of the radius is characterized by the presence of a large dorsal tubercle, which acts as a pulley for the tendon of one of the extensor muscles of the thumb (extensor pollicis longus). The medial surface is marked by a prominent facet for articulation with the distal end of the ulna (Fig. 7.78). The lateral surface of the radius is diamond shaped and extends distally as a radial styloid process.
The distal end of the bone is marked by two facets for articulation with two carpal bones (the scaphoid and lunate).
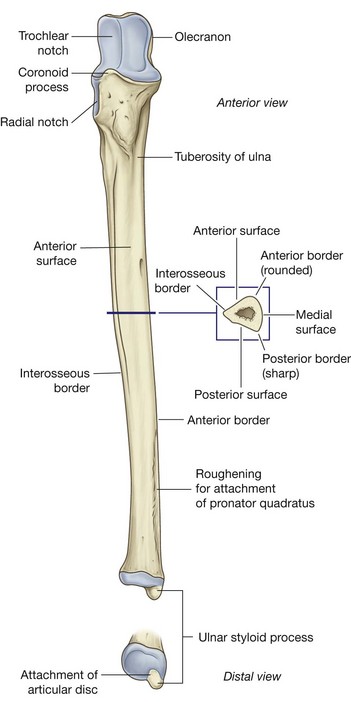
Shaft and distal end of ulna
The shaft of the ulna is broad superiorly where it is continuous with the large proximal end and narrow distally to form a small distal head (Fig. 7.79). Like the radius, the shaft of the ulna is triangular in cross-section and has:

three borders (anterior, posterior, and interosseous); and

three surfaces (anterior, posterior, and medial).
The anterior border is smooth and rounded.
The posterior border is sharp and palpable along its entire length.
The interosseous border is also sharp and is the attachment site for the interosseous membrane, which joins the ulna to the radius.
The anterior surface of the ulna is smooth, except distally where there is a prominent linear roughening for the attachment of the pronator quadratus muscle. The medial surface is smooth and unremarkable. The posterior surface is marked by lines, which separate different regions of muscle attachments to bone.
The distal end of the ulna is small and characterized by a rounded head and the ulnar styloid process (Fig. 7.79). The anterolateral and distal part of the head is covered by articular cartilage. The ulnar styloid process originates from the posteromedial aspect of the ulna and projects distally.
In the clinic
Fractures of the radius and ulna
The radius and ulna are attached to the humerus proximally and the carpal bones distally by a complex series of ligaments and muscles. Although they are both separate bones in many respects, they behave as one. When a severe injury occurs to the forearm it usually involves both bones, resulting in either fracture of both bones or more commonly a fracture of one bone and a dislocation of the other. Commonly, the mechanism of injury and the age of the patient determine which of these are likely to occur.
There are three classic injuries to the radius and ulna:

Monteggia’s fracture is a fracture of the proximal third of the ulna and an anterior dislocation of the head of the radius at the elbow;

Galeazzi’s fracture is a fracture of the distal third of the radius associated with subluxation (partial dislocation) of the head of the ulna (distal ulna) at the wrist joint;

Colles’ fracture is a fracture, and posterior displacement, of the distal end of the radius.
Whenever a fracture of the radius or ulna is demonstrated radiographically, further images of the elbow and wrist should be obtained to exclude dislocations.
Joints
Distal radio-ulnar joint
The distal radio-ulnar joint occurs between the articular surface of the head of the ulna, with the ulnar notch on the end of the radius, and with a fibrous articular disc, which separates the radio-ulnar joint from the wrist joint (Fig. 7.80).
The triangular-shaped articular disc is attached by its apex to a roughened depression on the ulna between the styloid process and the articular surface of the head, and by its base to the angular margin of the radius between the ulnar notch and the articular surface for the carpal bones.
Synovial membrane is attached to the margins of the distal radio-ulnar joint and is covered on its external surface by a fibrous joint capsule.
The distal radio-ulnar joint allows the distal end of the radius to move anteromedially over the ulna.
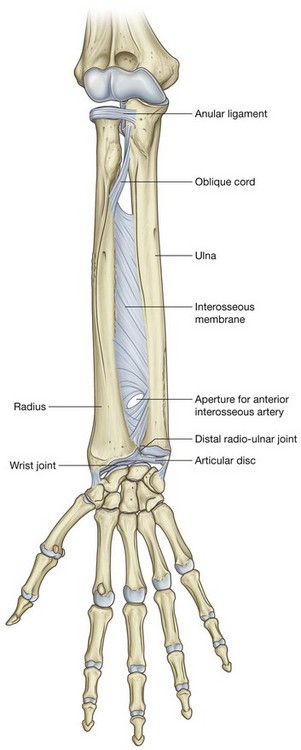
Interosseous membrane
The interosseous membrane is a thin fibrous sheet that connects the medial and lateral borders of the radius and ulna, respectively (Fig. 7.80). Collagen fibers within the sheet pass predominantly inferiorly from the radius to the ulna.
The interosseous membrane has a free upper margin, which is situated just inferior to the radial tuberosity, and a small circular aperture in its distal third. Vessels pass between the anterior and posterior compartments superior to the upper margin and through the inferior aperture.
The interosseous membrane connects the radius and ulna without restricting pronation and supination and provides attachment for muscles in the anterior and posterior compartments. The orientation of fibers in the membrane is also consistent with its role in transferring forces from the radius to the ulna and ultimately, therefore, from the hand to the humerus.
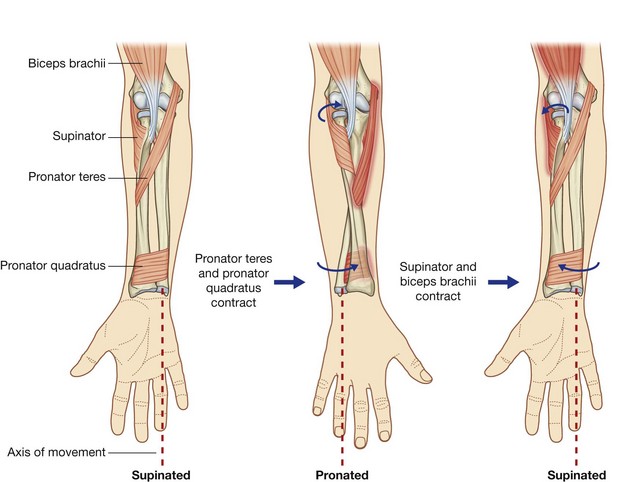
Pronation and supination
Pronation and supination of the hand occur entirely in the forearm and involve rotation of the radius at the elbow and movement of the distal end of the radius over the ulna (Fig. 7.81).
At the elbow, the superior articular surface of the radial head spins on the capitulum while, at the same time, the articular surface on the side of the head slides against the radial notch of the ulna and adjacent areas of the joint capsule and anular ligament of radius. At the distal radio-ulnar joint, the ulnar notch of the radius slides anteriorly over the convex surface of the head of the ulna. During these movements, the bones are held together by:

the anular ligament of radius at the proximal radio-ulnar joint;

the interosseous membrane along the lengths of the radius and ulna; and

the articular disc at the distal radio-ulnar joint (
Fig. 7.81).
Because the hand articulates predominantly with the radius, the translocation of the distal end of the radius medially over the ulna moves the hand from the palm-anterior (supinated) position to the palm-posterior (pronated) position.
Two muscles supinate and two muscles pronate the hand (Fig. 7.81).
Muscles involved in pronation and supination
Biceps brachii.
The biceps brachii muscle, the largest of the four muscles that supinate and pronate the hand, is a powerful supinator as well as a flexor of the elbow joint. It is most effective as a supinator when the forearm is flexed.
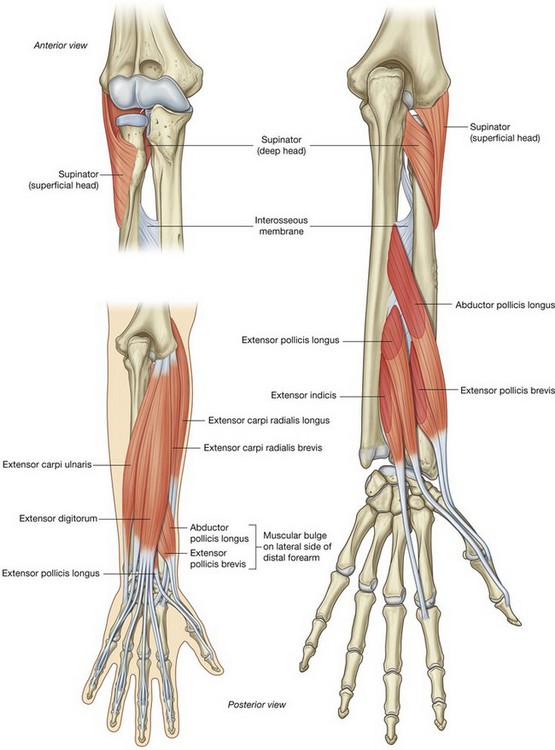
Supinator.
The second of the muscles involved with supination is the supinator muscle. Located in the posterior compartment of the forearm, it has a broad origin, from the supinator crest of the ulna and the lateral epicondyle of the humerus and from ligaments associated with the elbow joint.
The supinator muscle curves around the posterior surface and the lateral surface of the upper third of the radius to attach to the shaft of the radius superior to the oblique line.
The tendon of the biceps brachii muscle and the supinator muscle both become wrapped around the proximal end of the radius when the hand is pronated (Fig. 7.81). When they contract, they unwrap from the bone, producing supination of the hand.
Pronator teres and pronator quadratus.
Pronation results from the action of the pronator teres and pronator quadratus muscles (Fig. 7.81). Both these muscles are in the anterior compartment of the forearm:

the pronator teres runs from the medial epicondyle of the humerus to the lateral surface of the radius, approximately midway along the shaft;

the pronator quadratus extends between the anterior surfaces of the distal ends of the radius and ulna.
When these muscles contract, they pull the distal end of the radius over the ulna, resulting in pronation of the hand (Fig. 7.81).
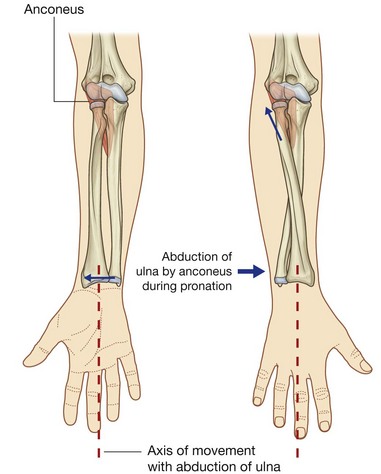
Anconeus.
In addition to hinge-like flexion and extension at the elbow joint, some abduction of the distal end of the ulna also occurs and maintains the position of the palm of the hand over a central axis during pronation (Fig. 7.82). The muscle involved in this movement is the anconeus muscle, which is a triangular muscle in the posterior compartment of the forearm that runs from the lateral epicondyle to the lateral surface of the proximal end of the ulna.
HAND
The hand (Fig. 7.91) is the region of the upper limb distal to the wrist joint. It is subdivided into three parts:

the wrist (carpus);

the metacarpus;

and the digits (five fingers including the thumb).
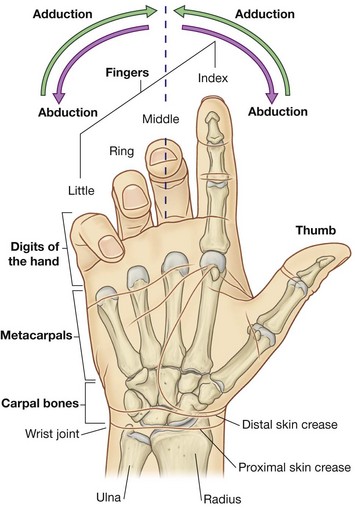
The five digits consist of the laterally positioned thumb and, medial to the thumb, the four fingers—the index, middle, ring, and little fingers.
In the normal resting position, the fingers form a flexed arcade, with the little finger flexed most and the index finger flexed least. In the anatomical position, the fingers are extended.
The hand has an anterior surface (palm) and a dorsal surface (dorsum of hand).
Abduction and adduction of the fingers are defined with respect to the long axis of the middle finger (Fig. 7.91). In the anatomical position, the long axis of the thumb is rotated 90° to the rest of the digits so that the pad of the thumb points medially; consequently, movements of the thumb are defined at right angles to the movements of the other digits of the hand.
The hand is a mechanical and sensory tool. Many of the features of the upper limb are designed to facilitate positioning the hand in space.
Bones
There are three groups of bones in the hand:

the eight
carpal bones are the bones of the wrist;

the five
metacarpals (
I to V) are the bones of the metacarpus;

the
phalanges are the bones of the digits—the thumb has only two, the rest of the digits have three (
Fig. 7.92).
The carpal bones and metacarpals of the index, middle, ring, and little fingers (metacarpals II to V) tend to function as a unit and form much of the bony framework of the palm. The metacarpal bone of the thumb functions independently and has increased flexibility at the carpometacarpal joint to provide opposition of the thumb to the fingers.
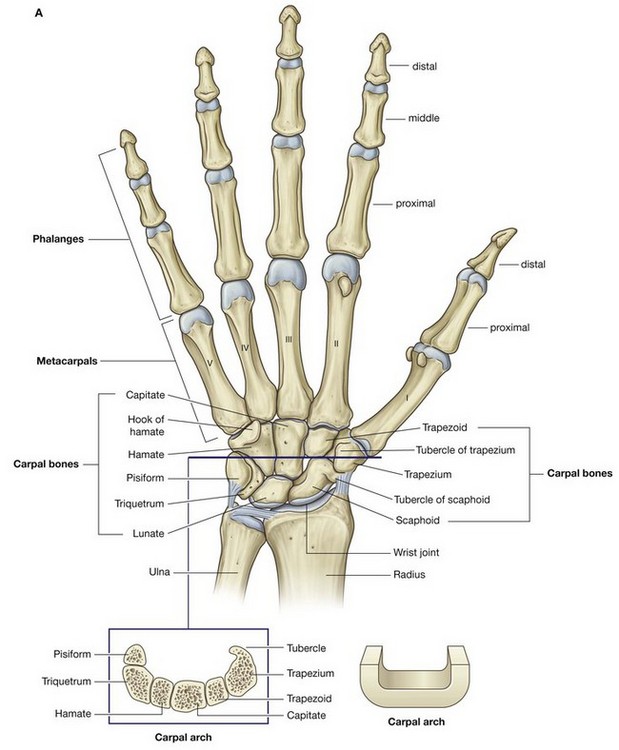
Carpal bones
The small carpal bones of the wrist are arranged in two rows, a proximal and a distal row, each consisting of four bones (Fig. 7.92).
Proximal row
From lateral to medial and when viewed from anteriorly, the proximal row of bones consists of:

the boat-shaped
scaphoid;

the
lunate, which has a crescent shape;

the three-sided
triquetrum bone; and
The pisiform is a sesamoid bone in the tendon of the flexor carpi ulnaris and articulates with the anterior surface of the triquetrum.
The scaphoid has a prominent tubercle on its lateral palmar surface that is directed anteriorly.
Distal row
From lateral to medial and when viewed from anteriorly, the distal row of carpal bones consists of:

the irregular four-sided
trapezium bone;

the four-sided
trapezoid;

the
capitate, which has a head; and
The trapezium articulates with the metacarpal bone of the thumb and has a distinct tubercle on its palmar surface that projects anteriorly.
The largest of the carpal bones, the capitate, articulates with the base of metacarpal III.
The hamate, which is positioned just lateral and distal to the pisiform, has a prominent hook (hook of hamate) on its palmar surface that projects anteriorly.
Articular surfaces
The carpal bones have numerous articular surfaces (Fig. 7.92). All of them articulate with each other, and the carpal bones in the distal row articulate with the metacarpals of the digits. With the exception of the metacarpal of the thumb, all movements of the metacarpal bones on the carpal bones are limited.
The expansive proximal surfaces of the scaphoid and lunate articulate with the radius to form the wrist joint.
Carpal arch
The carpal bones do not lie in a flat plane; rather, they form an arch, whose base is directed anteriorly (Fig. 7.92). The lateral side of this base is formed by the tubercles of the scaphoid and trapezium. The medial side is formed by the pisiform and the hook of hamate.
The flexor retinaculum attaches to, and spans the distance between, the medial and lateral sides of the base to form the anterior wall of the so-called carpal tunnel. The sides and roof of the carpal tunnel are formed by the arch of the carpal bones.
Metacarpals
Each of the five metacarpal bones is related to one digit:

metacarpal I is related to the thumb;

metacarpals II to V are related to the index, middle, ring, and little fingers, respectively (
Fig. 7.92).
Each metacarpal consists of a base, a shaft (body), and distally, a head.
All of the bases of the metacarpals articulate with the carpal bones; in addition, the bases of the metacarpal bones of the fingers articulate with each other.
All of the heads of the metacarpal bones articulate with the proximal phalanges of the digits. The heads form the knuckles on the dorsal surface of the hand when the fingers are flexed.
Phalanges
The phalanges are the bones of the digits (Fig. 7.92):

the thumb has two—a
proximal and a
distal phalanx;

the rest of the digits have three—a
proximal, a
middle, and a
distal phalanx.
Each phalanx has a base, a shaft (body), and distally, a head.
The base of each proximal phalanx articulates with the head of the related metacarpal bone.
The head of each distal phalanx is nonarticular and flattened into a crescent-shaped palmar tuberosity, which lies under the palmar pad at the end of the digit.
Joints
Wrist joint
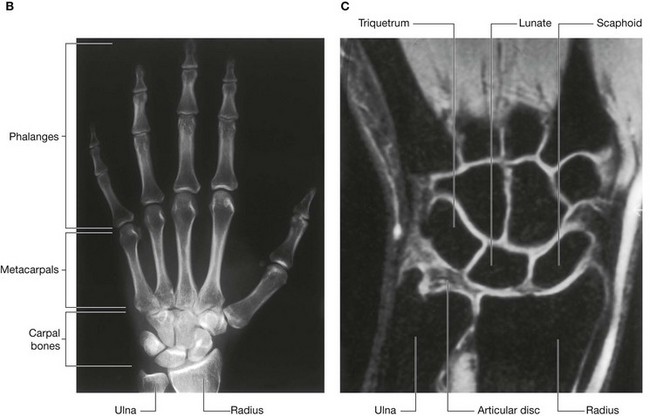
The wrist joint is a synovial joint between the distal end of the radius and the articular disc overlying the distal end of the ulna, and the scaphoid, lunate, and triquetrum (Fig. 7.92). Together, the articular surfaces of the carpals form an oval shape with a convex contour, which articulates with the corresponding concave surface of the radius and articular disc.
The wrist joint allows movement around two axes. The hand can be abducted, adducted, flexed, and extended at the wrist joint.
Because the radial styloid process extends further distally than does the ulnar styloid process, the hand can be adducted to a greater degree than it can be abducted.
The capsule of the wrist joint is reinforced by palmar radiocarpal, palmar ulnocarpal, and dorsal radiocarpal ligaments. In addition, radial and ulnar collateral ligaments of the wrist joint span the distance between the styloid processes of the radius and ulna and the adjacent carpal bones. These ligaments reinforce the medial and lateral sides of the wrist joint and support them during flexion and extension.
Carpal joints
The synovial joints between the carpal bones share a common articular cavity. The joint capsule of the joints is reinforced by numerous ligaments.
Although movement at the carpal joints (intercarpal joints) is limited, they do contribute to the positioning of the hand in abduction, adduction, flexion, and, particularly, extension.
Carpometacarpal joints
There are five carpometacarpal joints between the metacarpals and the related distal row of carpal bones (Fig. 7.92).
The saddle joint, between metacarpal I and the trapezium, imparts a wide range of mobility to the thumb that is not a feature of the rest of the digits. Movements at this carpometacarpal joint are flexion, extension, abduction, adduction, rotation, and circumduction.
The carpometacarpal joints between metacarpals II to V and the carpal bones are much less mobile than the carpometacarpal joint of the thumb, allowing only limited gliding movements. Movement of the joints increases medially, so metacarpal V slides to the greatest degree. This can be best observed on the dorsal surface of the hand as it makes a fist.
Metacarpophalangeal joints
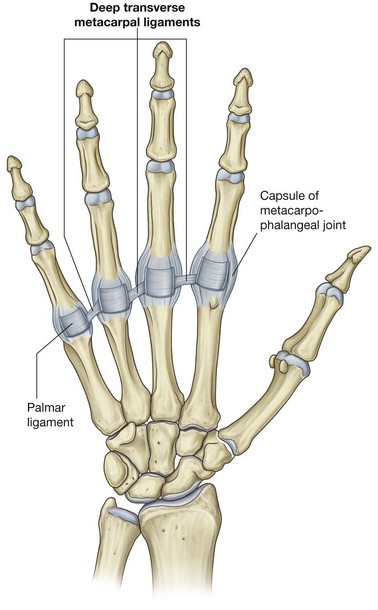
The joints between the distal heads of the metacarpals and the proximal phalanges of the digits are condylar joints, which allow flexion, extension, abduction, adduction, circumduction, and limited rotation (Fig. 7.92). The capsule of each joint is reinforced by the palmar ligament and by medial and lateral collateral ligaments.
Deep transverse metacarpal ligaments
The three deep transverse metacarpal ligaments (Fig. 7.93) are thick bands of connective tissue connecting the palmar ligaments of the metacarpophalangeal joints of the fingers to each other. They are important because, by linking the heads of the metacarpal bones together, they restrict the movement of these bones relative to each other. As a result, they help form a unified skeletal framework for the palm of the hand.
Significantly, a deep transverse metacarpal ligament does not occur between the palmar ligament of the metacarpophalangeal joint of the thumb and the palmar ligament of the index finger. The absence of this ligament, and the presence of a saddle joint between metacarpal I and the trapezium, are responsible for the increased mobility of the thumb relative to the rest of the digits of the hand.
Interphalangeal joints of hand
The interphalangeal joints of the hand are hinge joints that allow mainly flexion and extension. They are reinforced by medial and lateral collateral ligaments and palmar ligaments.
In the clinic
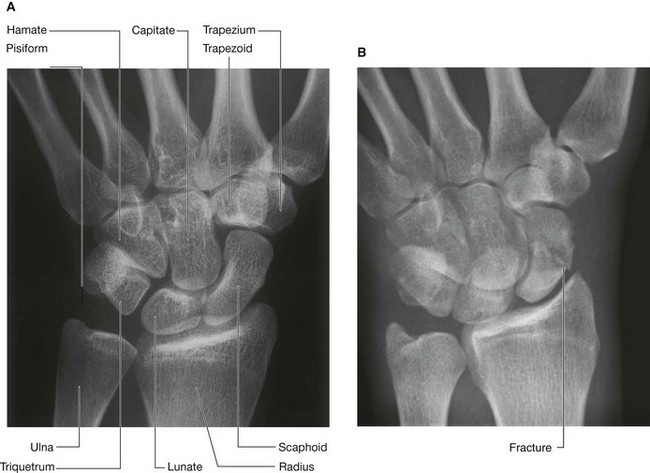
Fracture of the scaphoid and avascular necrosis of the proximal scaphoid
The commonest carpal injury is a fracture across the waist of the scaphoid bone (Fig. 7.94). It is uncommon to see other injuries. In approximately 10% of individuals, the scaphoid bone has a sole blood supply from the radial artery, which enters through the distal portion of the bone to supply the proximal portion. When a fracture occurs across the waist of the scaphoid, the proximal portion therefore undergoes avascular necrosis. It is impossible to predict which patients have this blood supply.
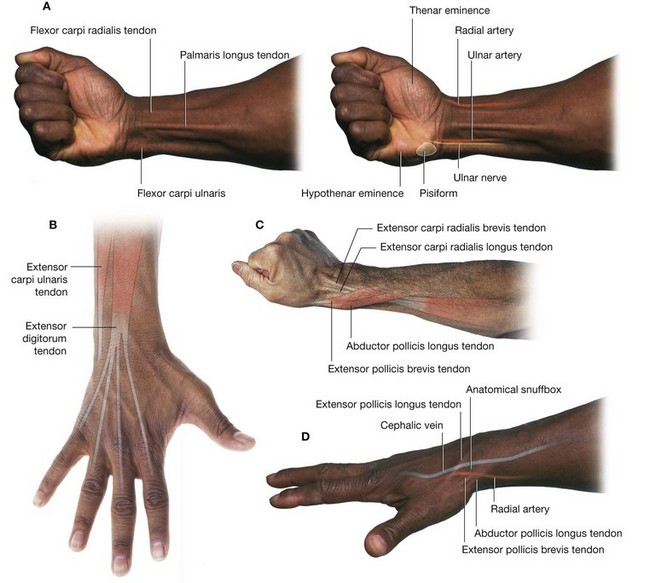
Carpal tunnel and structures at the wrist
The carpal tunnel is formed anteriorly at the wrist by a deep arch formed by the carpal bones and the flexor retinaculum (Fig. 7.92).
The base of the carpal arch is formed medially by the pisiform and the hook of the hamate and laterally by the tubercles of the scaphoid and trapezium.
The flexor retinaculum is a thick connective tissue ligament that bridges the space between the medial and lateral sides of the base of the arch and converts the carpal arch into the carpal tunnel.
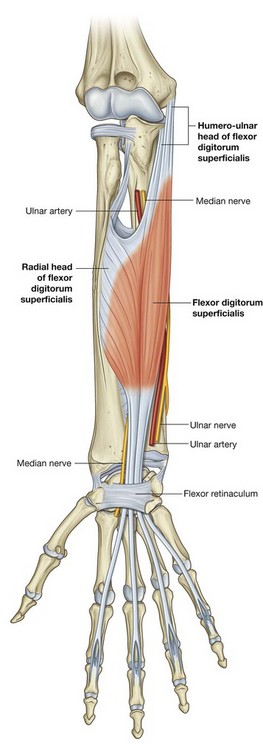
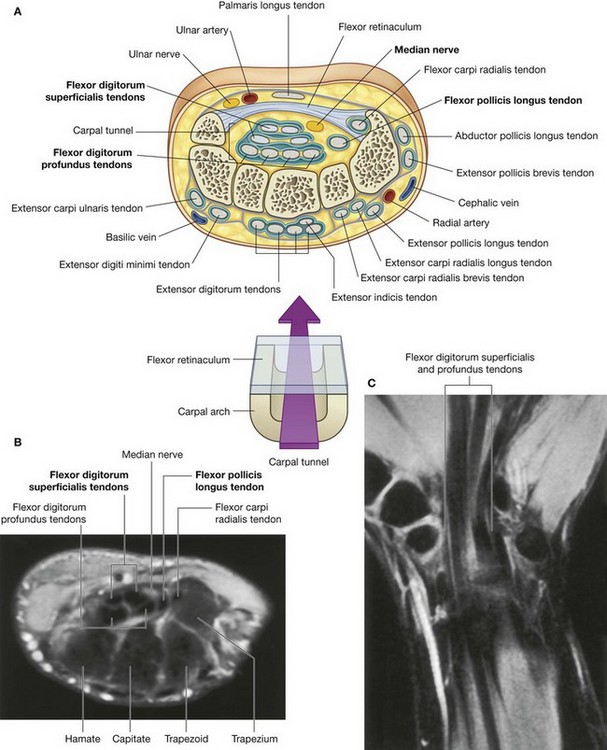
The four tendons of the flexor digitorum profundus, the four tendons of the flexor digitorum superficialis, and the tendon of the flexor pollicis longus pass through the carpal tunnel, as does the median nerve (Fig. 7.95).
The flexor retinaculum holds the tendons to the bony plane at the wrist and prevents them from “bowing.”
Free movement of the tendons in the carpal tunnel is facilitated by synovial sheaths, which surround the tendons. All the tendons of the flexor digitorum profundus and flexor digitorum superficialis are surrounded by a single synovial sheath; a separate sheath surrounds the tendon of the flexor pollicis longus. The median nerve is anterior to the tendons in the carpal tunnel.
The tendon of the flexor carpi radialis is surrounded by a synovial sheath and passes through a tubular compartment formed by the attachment of the lateral aspect of the flexor retinaculum to the margins of a groove on the medial side of the tubercle of trapezium.
The ulnar artery, ulnar nerve, and the tendon of the palmaris longus pass into the hand anterior to the flexor retinaculum and therefore do not pass through the carpal tunnel (Fig. 7.95). The tendon of the palmaris longus is not surrounded by a synovial sheath.
The radial artery passes dorsally around the lateral side of the wrist and lies adjacent to the external surface of the scaphoid.
The extensor tendons pass into the hand on the medial, lateral, and posterior surfaces of the wrist in six compartments defined by an extensor retinaculum and lined by synovial sheaths (Fig. 7.95):

the tendons of the extensor digitorum and extensor indicis share a compartment and synovial sheath on the posterior surface of the wrist;

the tendons of the extensor carpi ulnaris and extensor digiti minimi have separate compartments and sheaths on the medial side of the wrist;

the tendons of the abductor pollicis longus and extensor pollicis brevis muscles, the extensor carpi radialis longus and extensor carpi radialis brevis muscles, and the extensor pollicis longus muscle pass through three compartments on the lateral surface of the wrist.
In the clinic
Carpal tunnel syndrome
Carpal tunnel syndrome is an entrapment syndrome caused by pressure on the median nerve within the carpal tunnel. The etiology of this condition is often obscure, though in some instances the nerve injury may be a direct effect of increased pressure on the median nerve caused by overuse, swelling of the tendons and tendon sheaths (e.g., rheumatoid arthritis), and cysts arising from the carpal joints. Increased pressure in the carpal tunnel is thought to cause venous congestion that produces nerve edema and anoxic damage to the capillary endothelium of the median nerve itself.
Patients typically report pain and pins and needles in the distribution of the median nerve. Weakness and loss of muscle bulk of the thenar muscles may also occur. Gently tapping over the median nerve (in the region of the flexor retinaculum) readily produces these symptoms (Tinel’s sign).
Initial treatment is aimed at reducing the inflammation and removing any repetitive insults that produce the symptoms. If this does not lead to improvement, nerve conduction studies will be necessary to confirm nerve entrapment, which may require surgical decompression of the flexor retinaculum.
Palmar aponeurosis
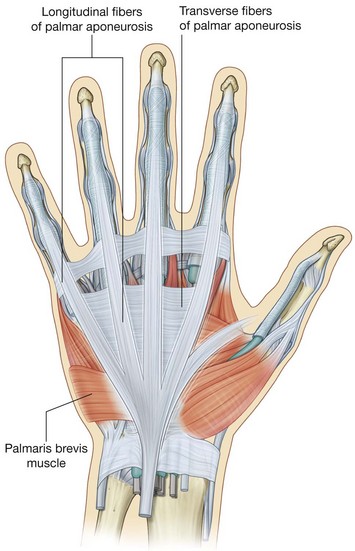
The palmar aponeurosis is a triangular condensation of deep fascia that covers the palm and is anchored to the skin in distal regions (Fig. 7.96).
The apex of the triangle is continuous with the palmaris longus tendon, when present; otherwise, it is anchored to the flexor retinaculum. From this point, fibers radiate to extensions at the base of the digits that project into each of the index, middle, ring, and little fingers and, to a lesser extent, the thumb.
Transverse fibers interconnect the more longitudinally arranged bundles that continue into the digits.
Vessels, nerves, and long flexor tendons lie deep to the palmar aponeurosis in the palm.
Palmaris brevis
The palmaris brevis, a small intrinsic muscle of the hand, is a quadrangular-shaped subcutaneous muscle that overlies the hypothenar muscles, ulnar artery, and superficial branch of the ulnar nerve at the medial side of the palm (Fig. 7.96). It originates from the palmar aponeurosis and flexor retinaculum and inserts into the dermis of the skin on the medial margin of the hand.
The palmaris brevis deepens the cup of the palm by pulling on skin over the hypothenar eminence and forming a distinct ridge. This may improve grip.
The palmaris brevis is innervated by the superficial branch of the ulnar nerve.
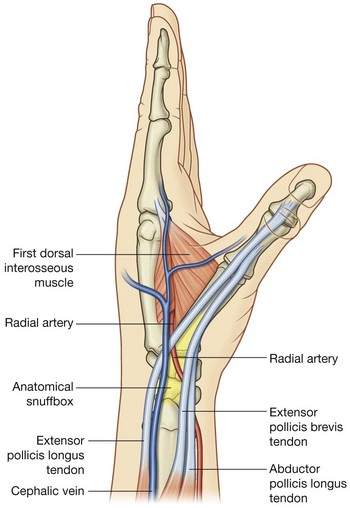
Anatomical snuffbox
The “anatomical snuffbox” is a term given to the triangular depression formed on the posterolateral side of the wrist and metacarpal I by the extensor tendons passing into the thumb (Fig. 7.97). Historically, ground tobacco (snuff) was placed in this depression before being inhaled into the nose. The base of the triangle is at the wrist and the apex is directed into the thumb. The impression is most apparent when the thumb is extended:

the lateral border is formed by the tendons of the abductor pollicis longus and extensor pollicis brevis;

the medial border is formed by the tendon of the extensor pollicis longus;

the floor of the impression is formed by the scaphoid and trapezium, and the distal ends of the tendons of the extensor carpi radialis longus and extensor carpi radialis brevis.
The radial artery passes obliquely through the anatomical snuffbox, deep to the extensor tendons of the thumb and lies adjacent to the scaphoid and trapezium.
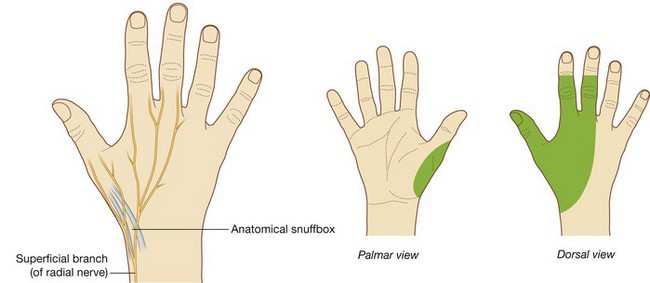
Terminal parts of the superficial branch of the radial nerve pass subcutaneously over the snuffbox as does the origin of the cephalic vein from the dorsal venous arch of the hand.
In the clinic
Snuffbox
The anatomical snuffbox is an important clinical region. When the hand is in ulnar deviation, the scaphoid becomes palpable within the snuffbox. This position enables the physician to palpate the bone to assess for a fracture. The pulse of the radial artery can also be felt in the snuffbox.
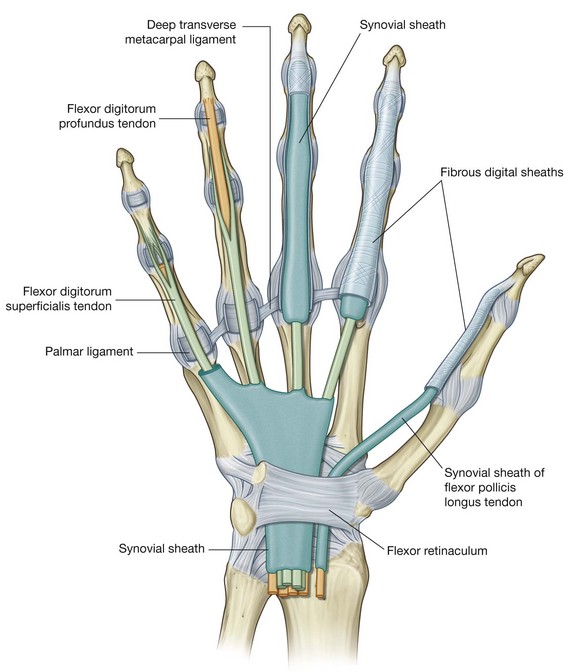
Fibrous digital sheaths
After exiting the carpal tunnel, the tendons of the flexor digitorum superficialis and profundus muscles cross the palm and enter fibrous sheaths on the palmar aspect of the digits (Fig. 7.98). These fibrous sheaths:

begin proximally, anterior to the metacarpophalangeal joints, and extend to the distal phalanges;

are formed by fibrous arches and cruciate (cross-shaped) ligaments, which are attached posteriorly to the margins of the phalanges and to the palmar ligaments associated with the metacarpophalangeal and interphalangeal joints; and

hold the tendons to the bony plane and prevent the tendons from bowing when the digits are flexed.
Within each tunnel, the tendons are surrounded by a synovial sheath. The synovial sheaths of the thumb and little finger are continuous with the sheaths associated with the tendons in the carpal tunnel (Fig. 7.98).
Extensor hoods
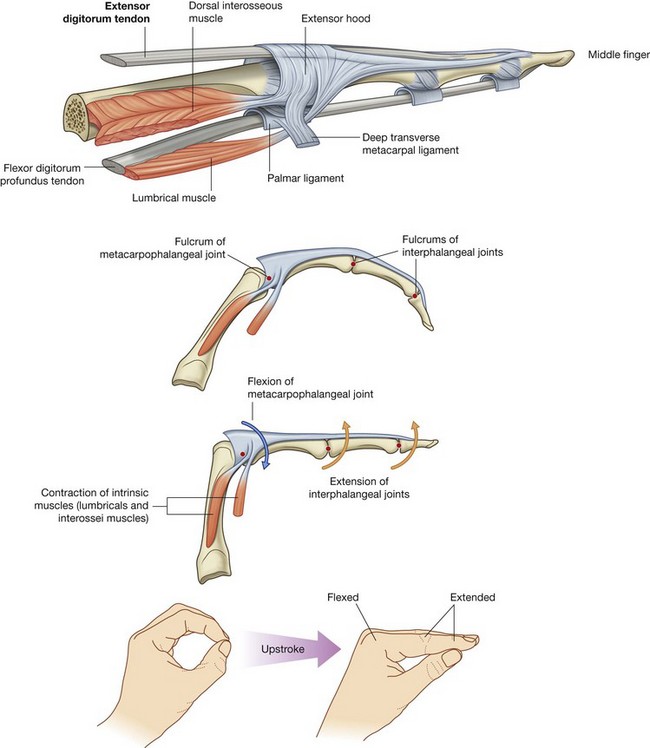
The tendons of the extensor digitorum and extensor pollicis longus muscles pass onto the dorsal aspect of the digits and expand over the proximal phalanges to form complex “extensor hoods” or “dorsal digital expansions” (Fig. 7.99A). The tendons of the extensor digiti minimi, extensor indicis, and extensor pollicis brevis muscles join these hoods.
Each extensor hood is triangular, with:

the apex attached to the distal phalanx;

the central region attached to the middle phalanx (index, middle, ring, and little fingers) or proximal phalanx (thumb); and

each corner of the base wrapped around the sides of the metacarpophalangeal joint—in the index, middle, ring, and little fingers, the corners of the hoods attach mainly to the deep transverse metacarpal ligaments; in the thumb, the hood is attached on each side to muscles.
In addition to other attachments, many of the intrinsic muscles of the hand insert into the free margin of the hood on each side. By inserting into the extensor hood, these intrinsic muscles are responsible for complex delicate movements of the digits that could not be accomplished with the long flexor and extensor tendons alone.
In the index, middle, ring, and little fingers, the lumbrical, interossei, and abductor digiti minimi muscles attach to the extensor hoods. In the thumb, the adductor pollicis and abductor pollicis brevis muscles insert into and anchor the extensor hood.
Because force from the small intrinsic muscles of the hand is applied to the extensor hood distal to the fulcrum of the metacarpophalangeal joints, the muscles flex these joints (Fig. 7.99B). Simultaneously, the force is transferred dorsally through the hood to extend the interphalangeal joints. This ability to flex the metacarpophalangeal joints, while at the same time extending the interphalangeal joints, is entirely due to the intrinsic muscles of the hand working through the extensor hoods. This type of precision movement is used in the upstroke when writing a t (Fig. 7.99C).
Muscles
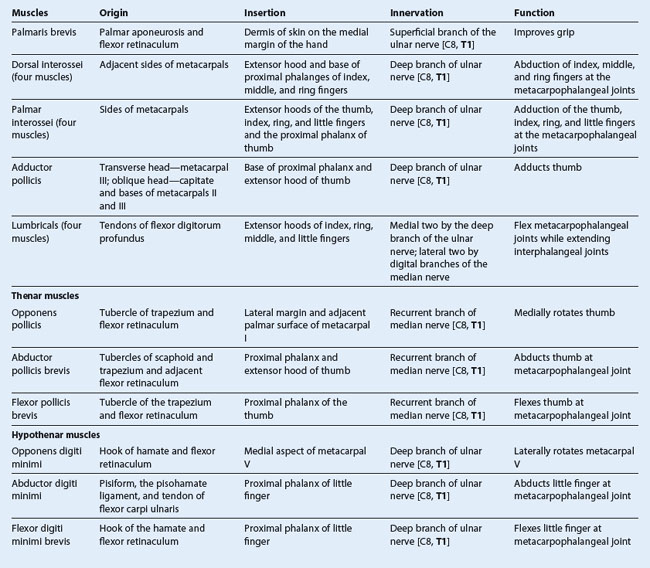
The intrinsic muscles of the hand are the palmaris brevis (described on p. 759; Fig. 7.96), interossei, adductor pollicis, thenar, hypothenar, and lumbrical muscles (Figs. 7.100-7.104). Unlike the extrinsic muscles that originate in the forearm, insert in the hand, and function in forcefully gripping (“power grip”) with the hand, the intrinsic muscles occur entirely in the hand and mainly execute precision movements (“precision grip”) with the fingers and thumb.
All of the intrinsic muscles of the hand are innervated by the deep branch of the ulnar nerve except for the three thenar and two lateral lumbrical muscles, which are innervated by the median nerve. The intrinsic muscles are predominantly innervated by spinal cord segment T1 with a contribution from C8.
The interossei are muscles between and attached to the metacarpals (Figs. 7.100 and 7.101). They insert into the proximal phalanx of each digit and into the extensor hood and are divided into two groups, the dorsal interossei and the palmar interossei. All of the interossei are innervated by the deep branch of the ulnar nerve. Collectively, the interossei abduct and adduct the digits and contribute to the complex flexion and extension movements generated by the extensor hoods.
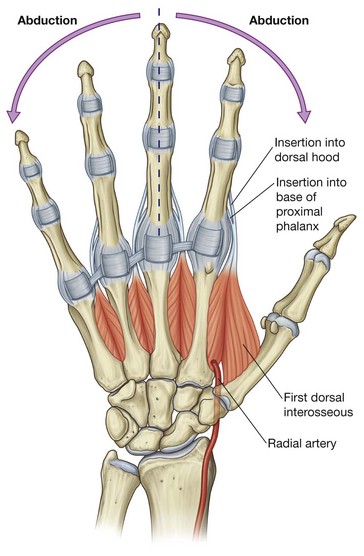
Dorsal interossei
Dorsal interossei are the most dorsally situated of all of the intrinsic muscles and can be palpated through the skin on the dorsal aspect of the hand (Fig. 7.100). There are four bipennate dorsal interosseous muscles between, and attached to, the shafts of adjacent metacarpal bones (Fig. 7.100). Each muscle inserts both into the base of the proximal phalanx and into the extensor hood of its related digit.
The tendons of the dorsal interossei pass dorsal to the deep transverse metacarpal ligaments:

the first dorsal interosseous muscle is the largest and inserts into the lateral side of the index finger;

the second and third dorsal interossei insert into the lateral and medial sides, respectively, of the middle finger;

the fourth dorsal interosseous muscle inserts into the medial side of the ring finger.
In addition to generating flexion and extension movements of the fingers through their attachments to the extensor hoods, the dorsal interossei are the major abductors of the index, middle, and ring fingers, at the metacarpophalangeal joints (Table 7.15).
The middle finger can abduct medially and laterally with respect to the long axis of the middle finger and consequently has a dorsal interosseous muscle on each side. The thumb and little finger have their own abductors in the thenar and hypothenar muscle groups, respectively, and therefore do not have dorsal interossei.
The radial artery passes between the two heads of the first dorsal interosseous muscle as it passes from the anatomical snuffbox on the posterolateral side of the wrist into the deep aspect of the palm.
Palmar interossei
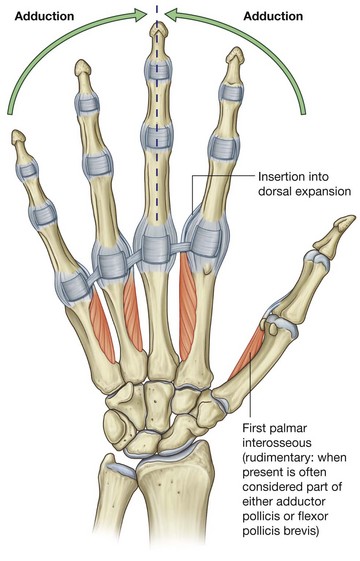
The four palmar interossei are anterior to the dorsal interossei, and are unipennate muscles originating from the metacarpals of the digits with which each is associated (Fig. 7.101).
The first palmar interosseous muscle is rudimentary and often considered part of either the adductor pollicis or the flexor pollicis brevis. When present, it originates from the medial side of the palmar surface of metacarpal I and inserts into both the base of the proximal phalanx of the thumb and into the extensor hood. A sesamoid bone often occurs in the tendon attached to the base of the phalanx.
The second palmar interosseous muscle originates from the medial surface of metacarpal II and inserts into the medial side of the extensor hood of the index finger.
The third and fourth palmar interossei originate from the lateral surfaces of metacarpals IV and V and insert into the lateral sides of the respective extensor hoods.
Like the tendons of the dorsal interossei, the tendons of the palmar interossei pass dorsal to the deep transverse metacarpal ligaments.
The palmar interossei adduct the thumb, index, ring, and little fingers with respect to a long axis through the middle finger. The movements occur at the metacarpophalangeal joints. Because the muscles insert into the extensor hoods, they also produce complex flexion and extension movements of the digits (Table 7.15).
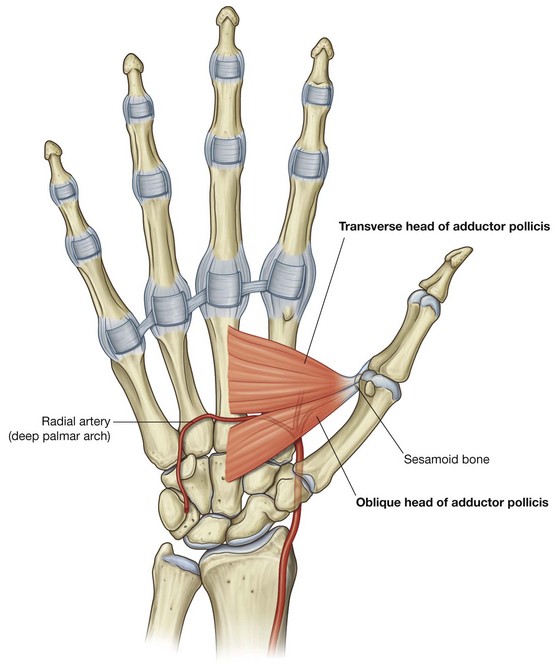
Adductor pollicis
The adductor pollicis is a large triangular muscle anterior to the plane of the interossei that crosses the palm (Fig. 7.102). It originates as two heads:

a
transverse head from the anterior aspect of the shaft of metacarpal III;

an
oblique head, from the capitate and adjacent bases of metacarpals II and III.
The two heads converge laterally to form a tendon, which often contains a sesamoid bone, that inserts into both the medial side of the base of the proximal phalanx of the thumb and into the extensor hood.
The radial artery passes anteriorly and medially between the two heads of the muscle to enter the deep plane of the palm and form the deep palmar arch.
The adductor pollicis is a powerful adductor of the thumb and opposes the thumb to the rest of the digits in gripping (Table 7.15).
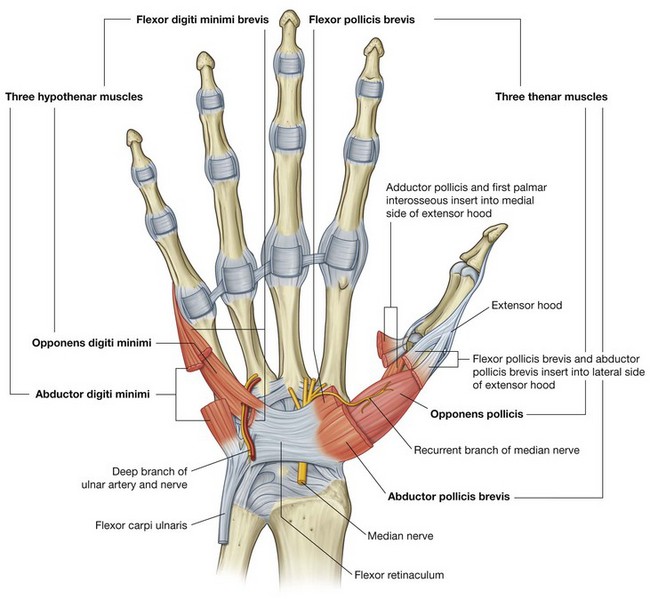
Thenar muscles
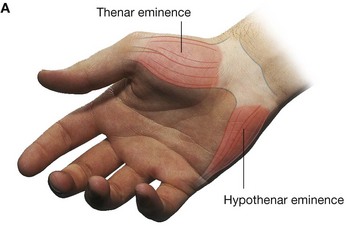
The three thenar muscles (the opponens pollicis, flexor pollicis brevis, and abductor pollicis brevis muscles) are associated with opposition of the thumb to the fingers and with delicate movements of the thumb (Fig. 7.103) and are responsible for the prominent swelling (thenar eminence) on the lateral side of the palm at the base of the thumb.
The thenar muscles are innervated by the recurrent branch of the median nerve.
Opponens pollicis
The opponens pollicis muscle is the largest of the thenar muscles and lies deep to the other two (Fig. 7.103). Originating from the tubercle of the trapezium and the adjacent flexor retinaculum, it inserts along the entire length of the lateral margin and adjacent lateral palmar surface of metacarpal I.
The opponens pollicis rotates and flexes metacarpal I on the trapezium, so bringing the pad of the thumb into a position facing the pads of the fingers (Table 7.15).
Abductor pollicis brevis
The abductor pollicis brevis muscle overlies the opponens pollicis and is proximal to the flexor pollicis brevis muscle (Fig. 7.103). It originates from the tubercles of the scaphoid and trapezium and from the adjacent flexor retinaculum, and inserts into the lateral side of the base of the proximal phalanx of the thumb and into the extensor hood.
The abductor pollicis brevis abducts the thumb, principally at the metacarpophalangeal joint. Its action is most apparent when the thumb is maximally abducted and the proximal phalanx is moved out of line with the long axis of the metacarpal bone (Table 7.15).
Flexor pollicis brevis
The flexor pollicis brevis muscle is distal to the abductor pollicis brevis (Fig. 7.103). It originates mainly from the tubercle of the trapezium and adjacent flexor retinaculum, but it may also have deeper attachments to other carpal bones and associated ligaments. It inserts into the lateral side of the base of the proximal phalanx of the thumb. The tendon often contains a sesamoid bone.
The flexor pollicis brevis flexes the metacarpophalangeal joint of the thumb (Table 7.15).
Hypothenar muscles
The hypothenar muscles (the opponens digiti minimi, abductor digiti minimi, and flexor digiti minimi brevis) contribute to the swelling (hypothenar eminence) on the medial side of the palm at the base of the little finger (Fig. 7.103). The hypothenar muscles are similar to the thenar muscles in name and in organization.
Unlike the thenar muscles, the hypothenar muscles are innervated by the deep branch of the ulnar nerve and not by the recurrent branch of the median nerve.
Opponens digiti minimi
The opponens digiti minimi muscle lies deep to the other two hypothenar muscles (Fig. 7.103). It originates from the hook of the hamate and from the adjacent flexor retinaculum and it inserts into the medial margin and palmar surface of metacarpal V. Its base is penetrated by the deep branches of the ulnar nerve and ulnar artery.
The opponens digiti minimi rotates metacarpal V toward the palm; however, because of the simple shape of the carpometacarpal joint and the presence of a deep transverse metacarpal ligament, which attaches the head of metacarpal V to that of the ring finger, the movement is much less dramatic than that of the thumb (Table 7.15).
Abductor digiti minimi
The abductor digiti minimi muscle overlies the opponens digiti minimi (Fig. 7.103). It originates from the pisiform bone, the pisohamate ligament, and the tendon of the flexor carpi ulnaris, and inserts into the medial side of the base of the proximal phalanx of the little finger and into the extensor hood.
The abductor digiti minimi is the principal abductor of the little finger (Table 7.15).
Flexor digiti minimi brevis
The flexor digiti minimi brevis muscle is lateral to the abductor digiti minimi (Fig. 7.103). It originates from the hook of the hamate bone and the adjacent flexor retinaculum and inserts with the abductor digiti minimi muscle into the medial side of the base of the proximal phalanx of the little finger.
The flexor digiti minimi brevis flexes the metacarpophalangeal joint.
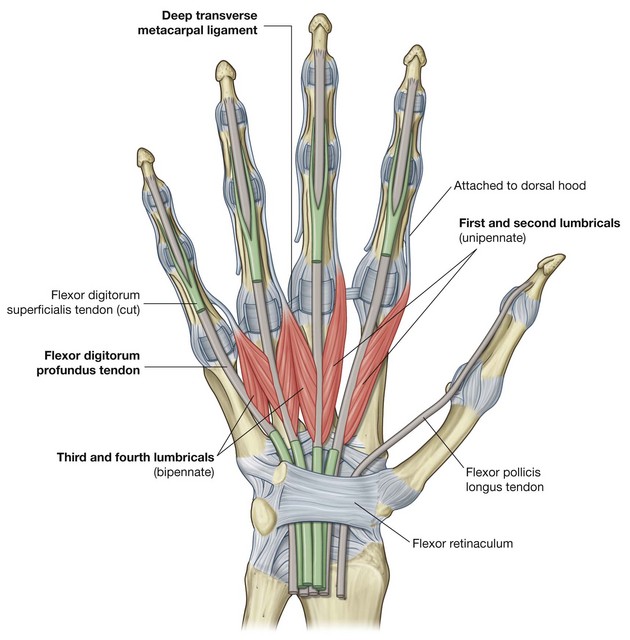
Lumbrical muscles
There are four lumbrical (worm-like) muscles, each of which is associated with one of the fingers. The muscles originate from the tendons of the flexor digitorum profundus in the palm:

the medial two lumbricals are bipennate and originate from the flexor digitorum profundus tendons associated with the middle and ring fingers and the ring and little fingers, respectively;

the lateral two lumbricals are unipennate muscles, originating from the flexor digitorum profundus tendons associated with index and middle fingers, respectively.
The lumbricals pass dorsally around the lateral side of each finger, and insert into the extensor hood (Fig. 7.104). The tendons of the muscles are anterior to the deep transverse metacarpal ligaments.
The lumbricals are unique because they link flexor tendons with extensor tendons. Through their insertion into the extensor hoods, they participate in flexing the metacarpophalangeal joints and extending the interphalangeal joints.
The medial two lumbricals are innervated by the deep branch of the ulnar nerve; the lateral two lumbricals are innervated by digital branches of the median nerve (Table 7.15).
Arteries and veins
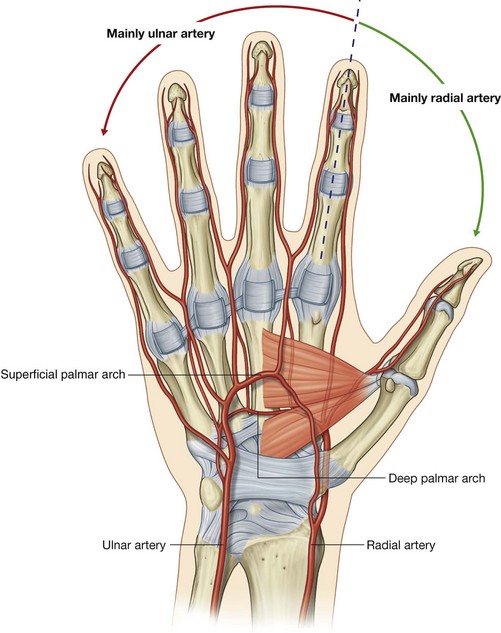
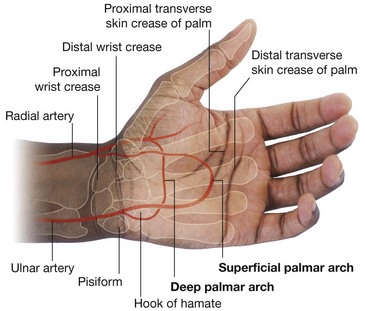
The blood supply to the hand is by the radial and ulnar arteries, which form two interconnected vascular arches (superficial and deep) in the palm (Fig. 7.105). Vessels to the digits, muscles, and joints originate from the two arches and the parent arteries:

the radial artery contributes substantially to the supply of the thumb and the lateral side of the index finger;

the remaining digits and the medial side of the index finger are supplied mainly by the ulnar artery.
Ulnar artery and superficial palmar arch
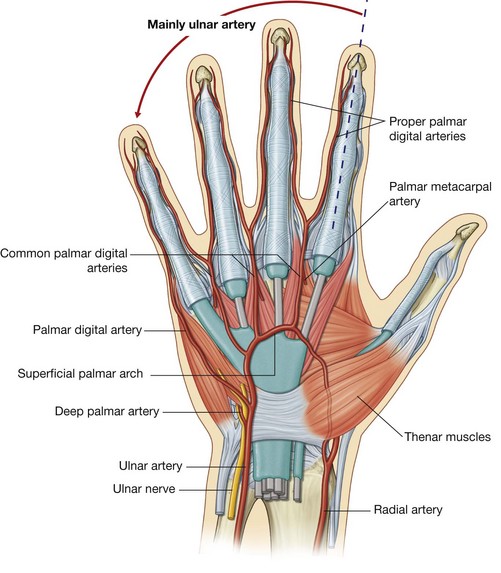
The ulnar artery and ulnar nerve enter the hand on the medial side of the wrist (Fig. 7.106). The vessel lies between the palmaris brevis and the flexor retinaculum and is lateral to the ulnar nerve and the pisiform bone. Distally, the ulnar artery is medial to the hook of the hamate bone and then swings laterally across the palm, forming the superficial palmar arch, which is superficial to the long flexor tendons of the digits and just deep to the palmar aponeurosis. On the lateral side of the palm, the arch communicates with a palmar branch of the radial artery.
One branch of the ulnar artery in the hand is the deep palmar branch (Figs. 7.105 and 7.106), which arises from the medial aspect of the ulnar artery, just distal to the pisiform, and penetrates the origin of the hypothenar muscles. It curves medially around the hook of the hamate to access the deep plane of the palm and to anastomose with the deep palmar arch derived from the radial artery.
Branches from the superficial palmar arch include:

a palmar digital artery to the medial side of the little finger; and

three large,
common palmar digital arteries, which ultimately provide the principal blood supply to the lateral side of the little finger, both sides of the ring and middle fingers, and the medial side of the index finger (
Fig. 7.106); they are joined by palmar metacarpal arteries from the deep palmar arch before bifurcating into the
proper palmar digital arteries, which enter the fingers.
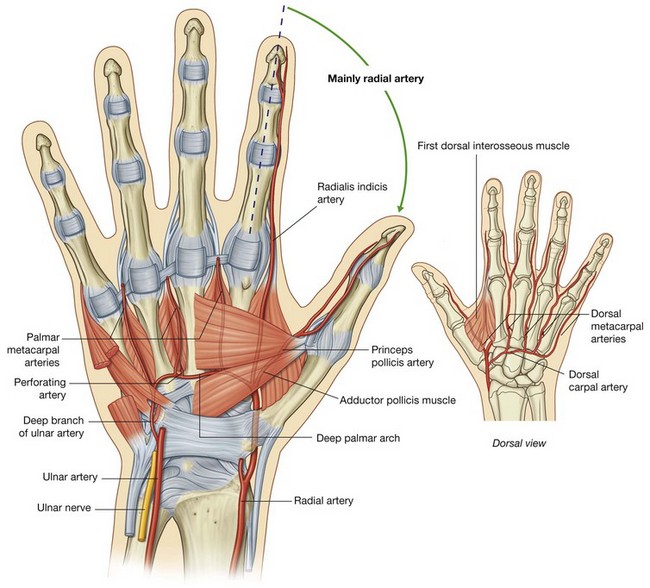
Radial artery and deep palmar arch
The radial artery curves around the lateral side of the wrist, passes over the floor of the anatomical snuffbox and into the deep plane of the palm by penetrating anteriorly through the back of the hand (Fig. 7.105). It passes between the two heads of the first dorsal interosseous muscle and then between the two heads of the adductor pollicis to access the deep plane of the palm and form the deep palmar arch.
The deep palmar arch passes medially through the palm between the metacarpal bones and the long flexor tendons of the digits. On the medial side of the palm, it communicates with the deep palmar branch of the ulnar artery (Figs. 7.105 and 7.107).
Before penetrating the back of the hand, the radial artery gives rise to two vessels:

a
dorsal carpal branch, which passes medially as the
dorsal carpal arch, across the wrist and gives rise to
dorsal metacarpal arteries, which subsequently divide to become small dorsal digital arteries, which enter the fingers;

the
first dorsal metacarpal artery, which supplies adjacent sides of the index finger and thumb.
Two vessels, the princeps pollicis artery and the radialis indicis artery, arise from the radial artery in the plane between the first dorsal interosseous and adductor pollicis. The princeps pollicis artery is the major blood supply to the thumb, and the radialis indicis artery supplies the lateral side of the index finger.
The deep palmar arch gives rise to:

three
palmar metacarpal arteries, which join the common palmar digital arteries from the superficial palmar arch; and

three
perforating branches, which pass posteriorly between the heads of origin of the dorsal interossei to anastomose with the dorsal metacarpal arteries from the dorsal carpal arch.
In the clinic
Allen’s test
To test for adequate anastomoses between the radial and ulnar arteries, compress both the radial and ulnar arteries at the wrist, then release pressure from one or the other, and determine the filling pattern of the hand. If there is little connection between the deep and superficial palmar arteries, only the thumb and lateral side of the index finger will fill with blood (become red) when pressure on the radial artery alone is released.
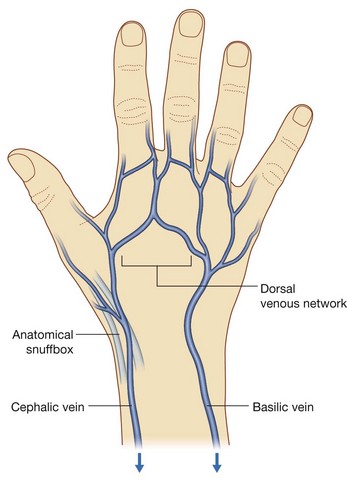
Veins
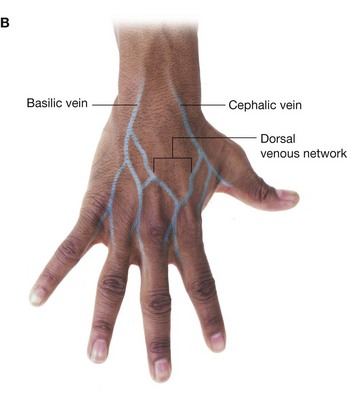
As generally found in the upper limb, the hand contains interconnected networks of deep and superficial veins. The deep veins follow the arteries; the superficial veins drain into a dorsal venous network on the back of the hand over the metacarpal bones (Fig. 7.108).
The cephalic vein originates from the lateral side of the dorsal venous network and passes over the anatomical snuffbox into the forearm.
The basilic vein originates from the medial side of the dorsal venous network and passes into the dorsomedial aspect of the forearm.
In the clinic
Venipuncture
In many patients, venous access is necessary for obtaining blood for laboratory testing and administering fluid and intravenous drugs. The ideal sites for venous access are typically in the cubital fossa and in the cephalic vein adjacent to the anatomical snuffbox. The veins are simply distended by use of a tourniquet. A tourniquet should be applied enough to allow the veins to become prominent. For straightforward blood tests the antecubital vein is usually the preferred site, and although it may not always be visible, it is easily palpated. The cephalic vein is generally the preferred site for short-term intravenous cannula.
Nerves
The hand is supplied by the ulnar, median, and radial nerves (Figs. 7.109-7.111). All three nerves contribute to cutaneous or general sensory innervation. The ulnar nerve innervates all intrinsic muscles of the hand except for the three thenar muscles and the two lateral lumbricals, which are innervated by the median nerve. The radial nerve only innervates skin on the dorsolateral side of the hand.
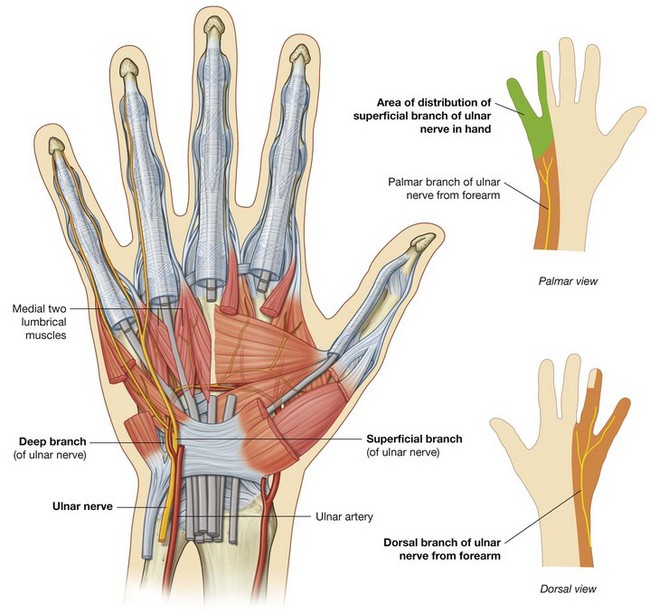
Ulnar nerve
The ulnar nerve enters the hand lateral to the pisiform and posteromedially to the ulnar artery (Fig. 7.109). Immediately distal to the pisiform, it divides into a deep branch, which is mainly motor and a superficial branch, which is mainly sensory.
The deep branch of the ulnar nerve passes with the deep branch of the ulnar artery (Fig. 7.109). It penetrates and supplies the hypothenar muscles to reach the deep aspect of the palm, arches laterally across the palm, deep to the long flexors of the digits, and supplies the interossei, adductor pollicis, and the two medial lumbricals. In addition, the deep branch of the ulnar nerve contributes small articular branches to the wrist joint.
As the deep branch of the ulnar nerve passes across the palm, it lies in a fibro-osseous tunnel (Guyon’s canal) between the hook of the hamate and the flexor tendons. Occasionally, small outpouchings of synovial membrane (ganglia) from the joints of the carpus compress the nerve within this canal, producing sensory and motor symptoms.
The superficial branch of the ulnar nerve innervates the palmaris brevis muscle and continues across the palm to supply skin on the palmar surface of the little finger and the medial half of the ring finger (Fig. 7.109).
In the clinic
Ulnar nerve injury
The ulnar nerve is most commonly injured at two sites: the elbow and the wrist.

At the elbow, the nerve lies posterior to the medial epicondyle.

At the wrist, the ulnar nerve passes superficial to the flexor retinaculum and lies lateral to the pisiform bone.
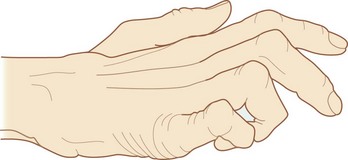
Ulnar nerve lesions are characterized by “clawing” of the hand, in which the metacarpophalangeal joints of the fingers are hyperextended and the interphalangeal joints are flexed because the function of most of the intrinsic muscles of the hand is lost (Fig. 7.110).
Clawing is most pronounced in the medial fingers because the function of all intrinsic muscles of these digits is lost while in the lateral two digits, the lumbricals are innervated by the median nerve. Function of the adductor pollicis muscle is also lost.
In lesions of the ulnar nerve at the elbow, function of the flexor carpi ulnaris muscle and flexor digitorum profundus to the medial two digits is lost as well. Clawing of the hand, particularly of the little and ring fingers, is worse with lesions of the ulnar nerve at the wrist than at the elbow because interruption of the nerve at the elbow paralyzes the ulnar half of the flexor digitorum profundus, which leads to lack of flexion at the distal interphalangeal joints in these fingers.
Ulnar nerve lesions at the elbow and wrist result in impaired sensory innervation on the palmar aspect of the medial one and one-half digits.
Damage to the ulnar nerve at the wrist or at a site proximal to the wrist can be distinguished by evaluating the status of function of the dorsal branch (cutaneous) of the ulnar nerve, which originates in distal regions of the forearm. This branch innervates skin over the dorsal surface of the hand on the medial side.
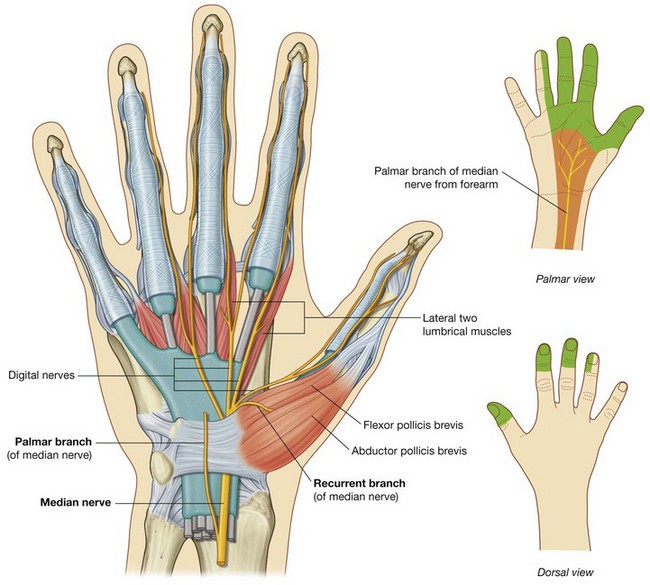
Median nerve
The median nerve is the most important sensory nerve in the hand because it innervates skin on the thumb, index and middle fingers, and lateral side of the ring finger (Fig. 7.111). The nervous system, using touch, gathers information about the environment from this area, particularly from the skin on the thumb and index finger. In addition, sensory information from the lateral three and one-half digits enables the fingers to be positioned with the appropriate amount of force when using precision grip.
The median nerve also innervates the thenar muscles that are responsible for opposition of the thumb to the other digits.
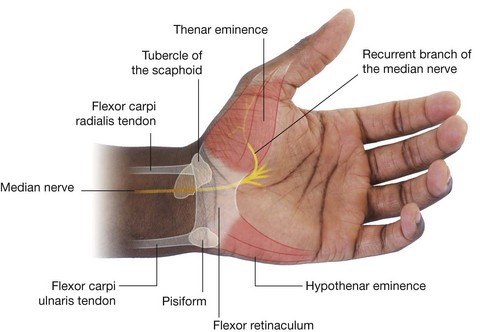
The median nerve enters the hand by passing through the carpal tunnel and divides into a recurrent branch and palmar digital branches (Fig. 7.111).
The recurrent branch of the median nerve innervates the three thenar muscles. Originating from the lateral side of the median nerve near the distal margin of the flexor retinaculum, it curves around the margin of the retinaculum and passes proximally over the flexor pollicis brevis muscle. The recurrent branch then passes between the flexor pollicis brevis and abductor pollicis brevis to end in the opponens pollicis.
The palmar digital nerves cross the palm deep to the palmar aponeurosis and the superficial palmar arch and enter the digits. They innervate skin on the palmar surfaces of the lateral three and one-half digits and cutaneous regions over the dorsal aspects of the distal phalanges (nail beds) of the same digits. In addition to skin, the digital nerves supply the lateral two lumbrical muscles.
Superficial branch of the radial nerve
The only part of the radial nerve that enters the hand is the superficial branch (Fig. 7.112). It enters the hand by passing over the anatomical snuffbox on the dorsolateral side of the wrist. Terminal branches of the nerve can be palpated or “rolled” against the tendon of the extensor pollicis longus as they cross the anatomical snuffbox.
The superficial branch of the radial nerve innervates skin over the dorsolateral aspect of the palm and the dorsal aspects of the lateral three and one-half digits distally to approximately the terminal interphalangeal joints.
In the clinic
Radial nerve injury
Around the elbow joint the radial nerve divides into its two terminal branches—the superficial branch and the deep branch nerve.
The most common radial nerve injury is damage to the nerve in the radial groove of the humerus, which produces a global paralysis of the muscles of the posterior compartment resulting in wrist drop. Radial nerve damage can result from fracture of the shaft of the humerus as the radial nerve spirals around in the radial groove. The typical injury produces reduction of sensation in the cutaneous distribution, predominantly over the posterior aspect of the hand. Severing the posterior interosseous nerve (continuation of deep branch of radial nerve) may paralyze the muscles of the posterior compartment of the forearm, but the nerve supply is variable. Typically, the patient may not be able to extend the fingers.
The distal branches of the superficial branch of the radial nerve can be readily palpated as “cords” passing over the tendon of the extensor pollicis longus in the anatomical snuffbox. Damage to these branches is of little consequence because they supply only a small area of skin.
Clinical cases
Case 1 SHOULDER PROBLEM AFTER FALLING ON AN OUTSTRETCHED HAND
A 45-year-old man came to his physician complaining of pain and weakness in his right shoulder. The pain began after a fall on his outstretched hand approximately 6 months previously. The patient recalled having some minor shoulder tenderness but no other specific symptoms. He was otherwise fit and well.
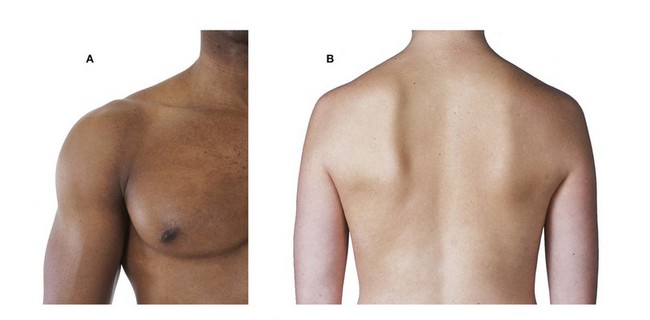
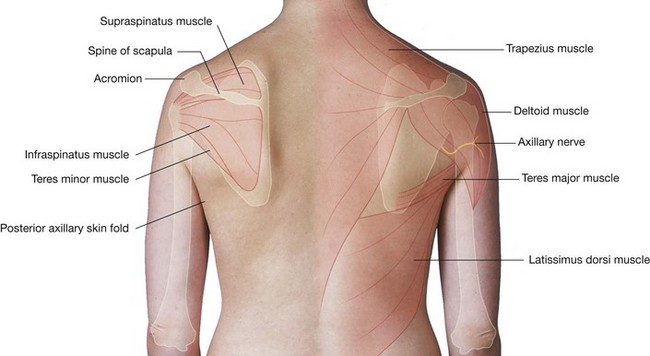
On examination of the shoulder, there was marked wasting of the muscles in the supraspinous and infraspinous fossae. The patient found initiation of abduction difficult and there was a weakness of lateral rotation of the humerus.
The wasted muscles were the supraspinatus and infraspinatus. The cause of the muscle wasting was disuse.
Muscle atrophy (wasting) occurs through a variety of disorders. Disuse atrophy is one of the most common causes. Examples of disuse atrophy include the loss of muscle bulk after fracture immobilization in a plaster cast. The opposite effect can also be demonstrated—when muscles are overused they become bulkier (hypertrophy).
The supraspinatus and infraspinatus muscles are supplied by the suprascapular nerve (C5, C6), which originates from the superior trunk of the brachial plexus. Given that only these muscles were involved, it is highly likely that the muscle atrophy is caused by denervation. Denervation may result from a direct nerve transection, nerve compression, or a pharmacologic effect on the nerve.
The typical site for compression of the suprascapular nerve is the spinoglenoid notch (greater scapular notch) on the lateral margin of the spine of the scapula adjacent to the glenohumeral joint. The notch is bounded by soft tissue, which creates a fixed space through which the suprascapular nerve passes.
The patient’s apparent minor injury damaged the fibrocartilaginous glenoid labrum, which allowed a cyst to form and pass along the anterosuperior border of the scapula to enter the spinoglenoid notch. The cyst then extended upward, so compressing the suprascapular nerve.
Surgical excision of the damaged glenoid labrum and removal improved the patient’s symptoms.
Case 2 WINGED SCAPULA
A 57-year-old woman underwent a right mastectomy for a breast cancer. The surgical note reported that all of the breast tissue had been removed, including the axillary process. In addition, the surgeon had dissected all lymph nodes within the axilla with their surrounding fat. The patient made an uneventful recovery.
At the first follow-up appointment, the patient’s husband told the surgeon that she had now developed a bony “spike” on her back. The surgeon was intrigued and asked the patient to reveal this spike. At examination, the spike was the inferior angle of the scapula, which appeared to be sticking out posteriorly. Raising the arms accentuated this structure.
The medial border of the scapula was accentuated and it was noted that there was some loss of bulk of the serratus anterior muscle, which attaches to the tip of the scapula.
The nerve to this muscle was damaged.
During the surgery on the axilla, the long thoracic nerve was damaged as it passed down the lateral thoracic wall on the external surface of the serratus anterior, just deep to the skin and subcutaneous fascia.
Although it is unlikely that the patient will improve because the nerve was transected, she was happy that she had an adequate explanation for the spike.
Case 3 BRACHIAL PLEXUS NERVE BLOCK
A surgeon wished to carry out a complex procedure on a patient’s wrist, and asked the anesthesiologist whether the whole arm could be numbed while the patient was awake. Within 20 minutes the anesthesiologist had carried out the procedure after injecting 10 ml of local anesthetic into the axilla. The surgeon went ahead with the operation and the patient did not feel a thing.
The anesthetic was injected into the axillary sheath.
It would be almost impossible to anesthetize the wrist in the forearm because local anesthetic would have to be placed accurately around the ulnar, median, and radial nerves. Furthermore, all of the cutaneous branches of the forearm would also have to be anesthetized individually, which would take a considerable amount of time and probably produce subtotal anesthesia.
The nerves of the upper limb originate from the brachial plexus, which surrounds the axillary artery within the axilla. Importantly, the axillary artery, axillary vein, and brachial plexus lie within the sleeve-like covering of fascia, termed the axillary sheath. By injecting the anesthetic into the space enclosed by the axillary sheath, all of the nerves of the brachial plexus were paralyzed.
It is possible with a patient’s arm abducted and externally rotated (palm behind the head) to easily palpate the axillary artery and therefore locate the position of the axillary sheath. Once the axillary artery has been identified, a small needle can be placed beside the vessel and local anesthetic can be injected on both sides of it. The local anesthetic tracks along the axillary sheath in this region. The brachial plexus surrounding the axillary artery is therefore completely anesthetized and an effective local anesthetic “block” is achieved.
“Could there be any complications?” asks the patient.
Potential complications are a direct needle spike of the branches of the brachial plexus, damage to the axillary artery, and inadvertent arterial injection of the local anesthetic. Fortunately, these are rare in skilled hands.
Case 4 COMPLICATION OF A FRACTURED FIRST RIB
A 25-year-old woman was involved in a motor vehicle accident and thrown from her motorcycle. When she was admitted to the emergency room, she was unconscious. A series of tests and investigations were performed, one of which included chest radiography. The attending physician noted a complex fracture of the first rib on the left.
Many important structures that supply the upper limb pass over rib I.
It is important to test the nerves that supply the arm and hand, although this is extremely difficult to do in an unconscious patient. However, some muscle reflexes can be determined using a tendon hammer. Also, it may be possible to test for pain reflexes in patients with altered consciousness levels. Palpation of the axillary artery, brachial artery, radial artery, and ulnar artery pulses is necessary because a fracture of the first rib can sever and denude the subclavian artery, which passes over it.
A chest drain was immediately inserted because the lung had collapsed. The fractured first rib had damaged the visceral and parietal pleurae, allowing air from a torn lung to escape into the pleural cavity. The lung collapsed, and the pleural cavity filled with air, which impaired lung function.
A tube was inserted between the ribs, and the air was sucked out to re-inflate the lung.
The first rib is a deep structure at the base of the neck. It is not uncommon for ribs to be broken after minor injuries, including sports injuries. However, rib I, which lies at the base of the neck, is surrounded by muscles and soft tissues that provide it with considerable protection. Therefore a patient with a fracture of the first rib has undoubtedly been subjected to a considerable force, which usually occurs in a deceleration injury. Other injuries should always be sought and the patient should be managed with a high level of concern for deep neck and mediastinal injuries.
Case 5 CARPAL TUNNEL SYNDROME?
A 35-year-old woman comes to her physician complaining of tingling and numbness in the fingertips of the first, second, and third digits (thumb, index, and middle fingers). The symptoms were provoked by arm extension. Local anesthesia was also present around the base of the thenar eminence.
The problem was diagnosed as median nerve compression.
The median nerve is formed from the lateral and medial cords of the brachial plexus anterior to the axillary artery and passes into the arm anterior to the brachial artery. At the level of the elbow joint it sits medial to the brachial artery, both of which are medial to the tendon of biceps. In the forearm the nerve courses through the anterior compartment and passes deep to the flexor retinaculum. It innervates most of the muscles of the forearm, the thenar muscles, the two lateral lumbricals, and the skin over the palmar surface of the lateral three and one-half digits and over the lateral side of the palm and the middle of the wrist.
The median nerve was believed to be trapped below the flexor retinaculum (carpal tunnel syndrome).
Carpal tunnel syndrome is a common problem in young to middle-aged patients. Typically the nerve becomes compressed within the carpal tunnel and may be associated with a number of medical conditions, such as thyroid disease and pregnancy. Occasionally a small ganglion or a tumor situated within the carpal tunnel can also compress the nerve. Other possibilities include tenosynovitis in patients with rheumatoid arthritis.
Nerve conduction studies were performed to confirm the clinical findings.
Nerve conduction studies are a series of tests that send small electrical impulses along the length of a variety of nerves in order to measure the speed at which the nerve conducts these pulses. The speed of the nerve pulse can be measured and is referred to as the latency. In our patient it was noted that the nerve had normal latency to the elbow joint; however, below the elbow joint there was increased latency.
The nerve conduction studies indicate the compression site at the elbow joint.
The clinical findings are not consistent with carpal tunnel syndrome. the clinician should have been alerted to this problem, given that the patient experienced numbness over the thenar eminence of the hand. This clue indicates an understanding of the anatomy. Compression of the nerve within the carpal tunnel does not produce this numbness, because the small cutaneous branch that supplies this region is proximal to the flexor retinaculum.
The etiology of the nerve compromise was the ligament of Struthers.
The ligament of Struthers is an embryological remnant of the coracobrachialis muscle and is an extremely rare finding. Occasionally it may ossify and cross the nerve, artery, and vein to produce compression in arm extension. Although this is very rare and unusual, it illustrates the complex course of the median nerve.
Case 6 IMMOBILIZING EXTENSOR DIGITORUM
After a hard day’s studying, two medical students decided to meet for coffee. The more senior student said to the freshman that he would bet him $50 that he could not lift a matchbook with a finger. The freshman placed $50 on the table and the bet was on. The senior medical student told the freshman to make a fist and place it in a palm-downward position, so that the middle phalanges of the fingers were in direct contact with the bar counter. He was then told to extend his middle finger so that it stuck forward while maintaining the middle phalanges of the index finger, the ring finger, and the little finger on the bar surface.
A matchbook was placed on top of the freshman’s middle fingernail and he was told to flip it. He couldn’t. He lost the $50.
Extension of the index, middle, ring, and little fingers is performed by the extensor digitorum muscle.
Placing the fist in a palm-down position on the table and pressing the middle phalanges onto the table effectively immobilizes the action of the extensor digitorum. The freshman was therefore unable to elevate his middle finger (which was sticking out). It is important to remember that if this same procedure is carried out leaving the index or little finger free to move, they do. This is because these two digits are extended not only by the extensor digitorum muscle, but also by the extensor indicis and extensor digiti minimi muscles, respectively.
Case 7 TORN SUPRASPINATUS TENDON
A 70-year-old woman came to an orthopedic surgeon with right shoulder pain and failure to initiate abduction of the shoulder. Further examination revealed loss of muscle bulk in the supraspinous fossa. The supraspinatus muscle was damaged.
Abduction of the humerus at the glenohumeral joint is initiated by the supraspinatus muscle. After the shoulder has been abducted to 10°–15°, the deltoid muscle continues the movement. The patient was able to abduct her arm by lowering and tilting the glenohumeral joint inferiorly to enable the deltoid to obtain its mechanical advantage.
The loss of muscle bulk in the supraspinous fossa suggested muscle atrophy.
Muscle atrophy occurs when a muscle is not used. The orthopedic surgeon thought that there was a tear of the supraspinatus tendon beneath the acromion. If this was so, the muscle would atrophy.
The diagnosis was confirmed by ultrasound scan.
The patient was seated on a stool and her right shoulder was uncovered. The patient’s hand was placed over her right buttock, a position that acts to externally rotate and extend the shoulder, exposing the supraspinatus tendon for ultrasound scan examination. The ultrasound revealed a completely torn tendon with fluid in the subacromial subdeltoid bursa (Fig. 7.125). The patient underwent a surgical repair and made a good recovery.
Case 8 HOW TO EXAMINE THE HAND
A resident was asked to carry out a clinical assessment of a patient’s hand. He examined the following:
Musculoskeletal system
The musculoskeletal system includes the bones, joints, muscles, and tendons. The resident looked for abnormalities and muscle wasting. Knowing which areas are wasted identifies the nerve that supplies them. She palpated the individual bones and palpated the scaphoid with the wrist in ulnar deviation. She examined the movement of joints because they may be restricted by joint disease or inability of muscular contraction.
Circulation
Palpation of both radial and ulnar pulses is necessary. The resident looked for capillary return to assess how well the hand was perfused.
Examination of the nerves
The three main nerves to the hand should be tested:
Median nerve
The median nerve innervates the skin on the palmar aspect of the lateral three and one-half digits, the dorsal aspect of the distal phalanx, half of the middle phalanges of the same fingers, and a variable amount on the radial side of the palm of the hand. Median nerve damage results in wasting of the thenar eminence, absence of abduction of the thumb, and absence of opposition of the thumb.
Ulnar nerve
The ulnar nerve innervates the skin of the anterior and posterior surfaces of the little finger and the ulnar side of the ring finger, the skin over the hypothenar eminence, and a similar strip of skin posteriorly. Sometimes the ulnar nerve innervates all the skin of the ring finger and the ulnar side of the middle finger.
An ulnar nerve palsy results in wasting of the hypothenar eminence, absent flexion of the distal interphalangeal joints of the little and ring fingers, and absent abduction and adduction of the fingers. The thumb is unaffected.
Radial nerve
The radial nerve innervates a small area of skin over the lateral aspect of metacarpal I and the back of the first web space.
The radial nerve also produces extension of the wrist and extension of the metacarpophalangeal and interphalangeal joints and of the digits.
A very simple examination would include tests for the median nerve by opposition of the thumb, for the ulnar nerve by abduction and adduction of the digits, and for the radial nerve by extension of the wrist and fingers and feeling on the back of the first web space.
Case 9 SHOULDER JOINT PROBLEM
A 35-year-old baseball pitcher came to the clinic with a history of a recurrent dislocation of the shoulder (Fig. 7.126). An MRI scan was performed to assess the shoulder joint prior to any treatment.
The MRI demonstrates the anatomical structures in multiple planes, allowing the physician to obtain an overview of the shoulder and to assess any intra- or extra-articular structures that may have been damaged and require surgical repair.
The MRI demonstrated a divot in the posterior superior aspect of the humeral head and a small fragment of bone and glenoid labrum that had become separated in the anterior-inferior aspect of the glenoid cavity.
Shoulder dislocation is not an uncommon problem and may occur as a “once-off” or with repetitive injury may be recurrent. Recurrent dislocations may be bilateral and symmetric (a memory aid is “torn loose or born loose”).
The MRI findings are typical for an anterior inferior dislocation, which is the most common type; moreover the MRI demonstrates the injuries that occur within the joint at the time of dislocation. These injuries include the abutment of the posterior superior aspect of the humeral head on the anterior inferior aspect of the glenoid cavity. This type of injury, when recurrent, may avulse a small fragment of the glenoid labrum, and in some cases this may attach to a small fragment of bone (the Bankart lesion). When the shoulder is relocated, the integrity of the capsular attachment antero-inferiorly has been disrupted, potentially making the shoulder somewhat prone to further dislocation.
An arthroscopic repair was performed.
Arthroscopy of the shoulder is an established method for assessing the shoulder joint. Portals of entry are anterior and posterior and small holes in the capsule are made percutaneously. The shoulder joint is filled with saline, which distends it, allowing the arthroscope to move around the joint and inspect the joint surfaces, including the labrum. The labrum and its bony fragment were reattached and sutured using anchor sutures (somewhat similar to staples.) The anterior aspect of the capsule was also tightened.
The patient made an uneventful recovery.
After the procedure the arm was held in internal rotation and remained adducted. Gentle exercise and physiotherapy were performed and the patient returned back to playing baseball.