Approach to the patient
Being a ‘good’ doctor
From your first day as a student you have professional obligations placed upon you by the public, the law and your colleagues which continue throughout your working life. Patients want more than merely intellectual and technical proficiency. To be a good doctor or nurse it is much easier if you genuinely like and are interested in people. Most patients want a doctor who listens to them and over 70 separate qualities have been listed as being important. Fundamentally, though, we all want doctors who:
• respect people, healthy or ill, regardless of who they are
• support patients and their loved ones when and where needed
• always ask courteous questions, let people talk and listen to them carefully
• promote health as well as treat disease
• give unbiased advice, let people participate actively in all decisions related to their health and healthcare, assess each situation carefully and help whatever the situation
• use evidence as a tool, not as a determinant of practice
• humbly accept death as an important part of life; and help people make the best possible arrangements when death is close
• work cooperatively with other members of the healthcare team
• are proactive advocates for their patients, mentors for other health professionals and ready to learn from others, regardless of their age, role or status.
Doctors also need a balanced life and to care for themselves and their families. In short, we want doctors who are happy and healthy, caring and competent, and who care for people throughout their life.
One way to reconcile these expectations with your inexperience and incomplete knowledge or skills is to put yourself in the situation of the patient and/or relatives. Consider how you would wish to be cared for in the patient’s situation, acknowledging that you are different and your preferences may not be the same. Most clinicians approach and care for patients differently once they have their own or a relative’s experience as a patient. Doctors, nurses and everyone involved in healthcare have a profound influence on how patients experience illness and their sense of dignity. When you are dealing with patients, always consider your:
Confidentiality and consent
As a student and as a doctor or nurse you will be given private and intimate information about patients and their families. This information is confidential, even after a patient’s death. This is a general rule, although its legal application varies between countries. In the UK, follow the guidelines issued by the General Medical Council (Box 1.1). There are exceptions to the general rules governing patient confidentiality, where failure to disclose information would put the patient or someone else at risk of death or serious harm, or where disclosure might assist in the prevention, detection or prosecution of a serious crime. If you find yourself in this situation, contact the senior doctor in charge of the patient’s care immediately and inform him or her of the situation.
Take all reasonable steps to ensure that consultation and examination of a patient is private. Never discuss patients where you can be overheard or leave patients’ records, either on paper or on screen, where they can be seen by other patients, unauthorised staff or the public. Always obtain consent or other valid authority before undertaking any examination or investigation, providing treatment or involving patients in teaching or research. Even where you have been given signed consent to disclose information about the patient, only disclose what is being asked for. If you have any doubts discuss your report with the patient so that he is clear about what information is going to a third party.
Clearly record your findings in the patient’s case notes immediately after the consultation. These case notes are confidential and must be stored securely. They also constitute a legal document that could be used in a court of law. Keeping accurate and up-to-date case notes is an essential part of good patient care (p. 38). Remember that what you write may be seen by the patient, as in many countries, including the UK, patients can ask for and receive access to their medical records.
Personal responsibilities
Always look after yourself and maintain your own health. Register with a general practitioner (GP). Do not self-diagnose and self-treat. If you know, or think that you might have, a serious condition you could pass on to patients, or if your judgement or performance could be affected by a condition or its treatment, consult your GP and be guided as to the need for secondary referral. Heed your doctor’s advice regarding investigations, treatment and changes to your working practice. Protect yourself, your patients and your colleagues by being immunised against common but serious communicable diseases where vaccines are available, e.g. hepatitis B.
Your professional position is a privileged one; do not use it to establish or pursue a sexual or improper emotional relationship with a patient or someone close to the patient. Do not give medical care to anyone with whom you have a close personal relationship. Do not express your personal beliefs, including political, religious or moral ones, to your patients in ways that exploit their vulnerability or could cause them distress.
Dress and demeanour
The way you dress is important in establishing a successful patient–doctor relationship. Your dress style and demeanour should never make your patient or colleagues uncomfortable or distract them. Smart, sensitive and modest dress is appropriate; expressing your personality is not. Exposing your chest, midriff and legs may not only create offence but impede communication. Have short or three-quarter-length sleeves or roll long sleeves up, away from your wrists, before examining patients or carrying out procedures. This allows you to clean your hands effectively and reduces the risk of cross-infection. Tie back long hair and keep any jewellery simple and limited to allow effective hand washing. Some medical schools and hospitals require students and staff to wear white coats or ‘scrubs’ for reasons of professionalism, identification and as a barrier to infection. If this is the case, these must be clean and smart and you should always wear a name badge which can be read easily, i.e. not at your waist.
Whenever you see a patient or relative, introduce yourself fully and clearly. A friendly smile helps to put your patient at ease.
How you speak to, and address, a patient depends upon the patient’s age, background and cultural environment. Many older patients prefer not to be called by their first name, and it is best to ask patients how they would prefer to be addressed.
Communication skills
A consultation is a meeting of two experts: you as the clinician and the patient as an expert on his own body and mind. Excellent communication skills allow you to identify a patient’s problem rapidly and accurately and improve patient satisfaction (p. 7). Poor communication skills are associated with increased medicolegal vulnerability and clinician burnout. Improve your skills by videoing yourself consulting with a patient (having obtained informed signed consent) and review this with a senior clinician using one of the many techniques developed for this. Continually seek to improve your communication skills. These will develop with experience but can always be improved.
Most doctors and nurses work in teams with colleagues in other professions. Working in teams does not change your personal accountability for your conduct and the care you provide. Try to act as a positive role model and motivate and inspire your colleagues. Always respect the skills and contributions of your colleagues and communicate effectively with them particularly when handing over care.
Expectations and respect
The literary and media stereotypes of doctors frequently involve miraculous intuition, the confirmation of rare and brilliant diagnoses and the performance of dramatic life-saving interventions. Reality is different. Medicine often involves seeing and treating patients with common conditions and chronic diseases where we may only be able to provide palliation or simply bear witness to patients’ suffering. The best doctors are humble and recognise that humans are infinitely more complex, demanding and fascinating than one can imagine. They understand that much so-called medical ‘wisdom’ is at best incomplete, and often simply wrong.
If a patient under your care has suffered harm or distress, act immediately to put matters right, if that is possible. Apologise and explain fully and promptly to the patient what has happened, and the likely effects. Patient complaints about their care or treatment are often the result of a breakdown in communication and they have a right to expect a prompt, open, constructive and honest response. Do not allow a patient’s complaint to affect adversely the care or treatment you provide.
Hand washing and cleanliness
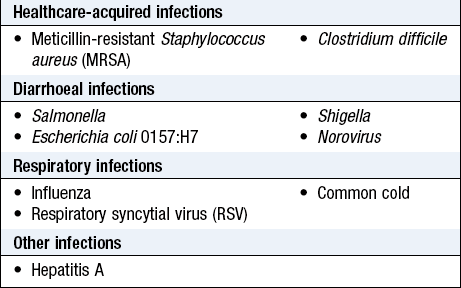
Transmission of microorganisms from the hands of healthcare workers is the main source of cross-infection in hospitals, primary care surgeries and nursing homes. Healthcare-acquired infections complicate up to 10% of hospital admissions and in the UK 5000 people die from them each year (Box 1.2).
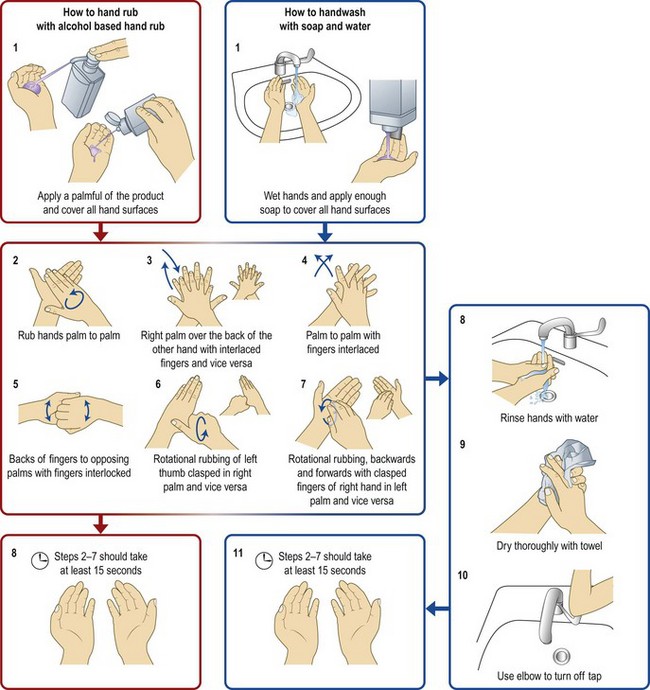
Hand washing is the single most effective way to prevent the spread of infection. It is your responsibility to prevent the spread of infection and routinely wash your hands after every clinical examination. Do not be put off by lack of hand hygiene agents or facilities for hand washing, or being short of time.
• If your hands are visibly soiled, wash thoroughly with soap and water.
• If your hands are not obviously dirty, wash with soap and water or use an alcohol-based rub or gel.
• Always wear surgical gloves when you may be in contact with blood, mucous membranes or non-intact skin.
While washing with alcohol-based gels will remove most microorganisms, e.g. meticillin-resistant Staphylococcus aureus (MRSA), Escherichia coli, Salmonella), when dealing with patients with influenza, norovirus or Clostridium difficile infection, always clean hands with liquid soap and water (Fig. 1.1).