Chapter 32 Microbiology of dental caries
Dental caries is a chronic endogenous infection caused by the normal oral commensal flora. The carious lesion is the result of demineralization of enamel – and later of dentine – by acids produced by plaque microorganisms as they metabolize dietary carbohydrates. However, the initial process of enamel demineralization is usually followed by remineralization, and cavitation occurs when the former process overtakes the latter. Once the surface layer of enamel has been lost, the infection invariably progresses to dentine, with the pulp becoming firstly inflamed and then necrotic.
Caries is defined as localized destruction of the tissues of the tooth by bacterial fermentation of dietary carbohydrates.
Epidemiology
Dental caries (with periodontal disease) is one of the most common human diseases and affects the vast majority of individuals. Although caries was not uncommon in the developing world, the recent affluence in these regions has resulted in a remarkable upsurge in caries due to the ready and cheap availability of fermentable carbohydrates. In contrast, caries prevalence is falling overall in the developed world due to the increasing awareness of cariogenic food sources and the general improvement in oral hygiene and the dental care delivery systems. Caries of enamel surfaces is particularly common up to the age of 20 years, after which it tends to stabilize. However, in later life, root surface caries becomes increasingly prevalent, due to gingival recession, exposing the vulnerable cementum to cariogenic bacteria.
Classification
Dental caries can be classified with respect to the site of the lesion (Fig. 32.1):
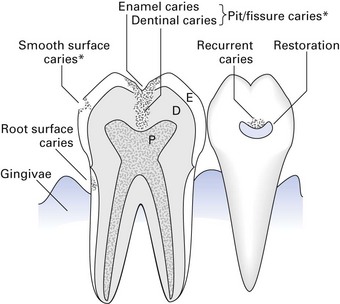
Fig. 32.1 Nomenclature of dental caries. D, dentine; E, enamel; P, pulp. *Also termed occlusal caries.
Clinical presentation
The primary lesion of caries is a well-demarcated, chalky-white lesion (Fig. 32.2) in which the surface continuity of enamel has not been breached. This ‘white-spot’ lesion can heal or remineralize, and this stage of the disease is therefore reversible. However, as the lesion develops, the surface becomes roughened and cavitation occurs. If the lesion is not treated, the cavitation spreads into dentine and eventually may destroy the dental pulp, finally leading to the development of a periapical abscess and purulent infection (see Chapter 34).
Diagnosis
Diagnosis is usually by a combination of:
Aetiology
The major factors involved in the aetiology of caries (Fig. 32.3) are:
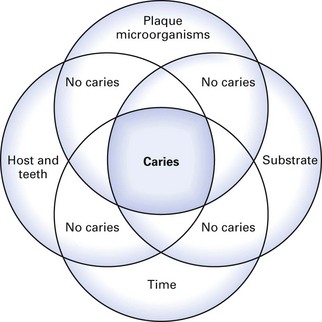
Fig. 32.3 Interplay of major aetiological factors in dental caries (all four factors must act simultaneously for caries to occur).
Host factors
Tooth structure
The structure of enamel, and of dentine in root caries, is important: some areas of the same tooth are much more susceptible to carious attack than others, possibly because of differences in mineral content (especially fluoride).
Flow rate and composition of saliva
The mechanical washing action of saliva is a very effective mechanism in the removal of food debris and unattached oral microorganisms. It has a high buffering capacity, which tends to neutralize acids produced by plaque bacteria on tooth surfaces, and it is supersaturated with calcium and phosphorus ions, which are important in the remineralization of white-spot lesions. Saliva also acts as a delivery vehicle for fluoride.
Diet
There is a direct relationship between dental caries and the intake of carbohydrates. The most cariogenic sugar is sucrose, and the evidence for its central role in the initiation of dental caries includes:
Sucrose is highly soluble and diffuses easily into dental plaque, acting as a substrate for the production of extracellular polysaccharides and acids. Cariogenic streptococci produce water-insoluble glucan from sucrose, which, in addition to facilitating initial adhesion of the organisms to the tooth surface, serve as a nutritional source and a matrix for further plaque development. The relationship between sucrose and dental caries is complex and cannot be simply explained by the total amount of sugar consumed. The frequency of sugar intake rather than the total amount of sugar consumed appears to be of decisive importance. Also relevant are the stickiness and concentration of the sucrose consumed, both factors influencing the period for which sugar is retained in close contact with the enamel surface.
Carbohydrates other than sucrose, e.g. glucose and fructose, are also cariogenic, but less so than sucrose. Polyol carbohydrates, ‘sugar alcohols’ (e.g. xylitol), with low cariogenicity have been produced and are sought after as sugar substitutes in products such as chewing gum and baby foods.
Microbiology
Microorganisms in the form of dental plaque are a prerequisite for the development of dental caries. The different types of plaque and the factors involved in their development are described in Chapter 31.
Specific and non-specific plaque hypothesis
Although mutans streptococci have been recognized as the major group of organisms involved in caries, there is some controversy as to whether one or more specific groups of bacteria are principally involved in caries – the specific plaque hypothesis – or whether the disease is caused by a heterogeneous mixture of non-specific bacteria – the non-specific plaque hypothesis.
There is conflicting opinion for and against the specific plaque hypothesis:
Given the extreme variation in the composition of supragingival plaque from the same site in the same mouth at different times, it is unlikely that the initiation and progression of all carious lesions are associated with specific organisms such as Streptococcus mutans. Further, other plaque bacteria also possess some of the biochemical characteristics thought to be important in cariogenicity. Therefore, it seems likely that combinations of bacteria other than mutans streptococci and lactobacilli may be able to initiate carious lesions, and the plaque flora may be non-specific in nature. The current evidence implies that some bacteria (mutans streptococci, Lactobacillus spp. and Actinomyces spp.) may be more important than others in the initial as well as subsequent events leading to both enamel and root surface caries.
The role of mutans streptococci
There is a vast literature on the role of the mutans streptococci in caries. ‘Streptococcus mutans’ is a loosely applied group name for a collection of seven different species (S. mutans, S. sobrinus, S. criceti, S. ferus, S. ratti, S. macacae and S. downei) and eight serotypes (a–h). S. mutans serotypes c, e, f and S. sobrinus serotypes d, g are the species most commonly found in humans, with serotype c strains being the most prevalent, followed by d and e. The others are rarely encountered. The evidence for the aetiological role of mutans streptococci in dental caries includes the following:
Note: not all strains of mutans streptococci possess all of the above properties; thus, some strains are more cariogenic than others. Caries may therefore be an infectious disease in a minority, with a highly pathogenic strain being transmitted from one individual to another. Despite this apparently strong relationship between S. mutans and caries, a number of longitudinal studies in children have failed to find such a strong correlation.
The role of lactobacilli
Lactobacilli were previously believed to be the causative agents of dental caries. They were considered to be candidate organisms for caries because of:
On the negative side, however, lactobacilli are rarely isolated from plaque before the development of caries, and they are often absent from incipient lesions.
Although the role of lactobacilli in the carious process is not well defined, it is believed that:
The role of Actinomyces spp.
Actinomyces spp. are associated with the development of root surface caries (root lesions differ from enamel caries in that the calcified tissues are softened without obvious cavitation). The evidence for the involvement of Actinomyces viscosus in root surface caries is based on:
Despite the fact that Actinomyces spp. (especially A. viscosus) predominate in the majority of plaque samples taken from root surface lesions, some studies have reported both mutans streptococci and Lactobacillus spp. in these lesions. Furthermore, the sites from which these organisms were isolated appeared to have a higher risk of developing root surface caries than other sites. The role of Actinomyces spp. in caries is therefore not clear.
The role of Veillonella
Veillonella is a Gram-negative anaerobic coccus that is present in significant numbers in most supragingival plaque samples. As Veillonella spp. require lactate for growth, but are unable to metabolize normal dietary carbohydrates, they use lactate produced by other microorganisms and convert it into a range of weaker and probably less cariogenic organic acids, e.g. propionic acid. Hence, this organism may have a beneficial effect on dental caries. This protective effect has been demonstrated in vitro and in animal experiments, but not in humans.
Plaque metabolism and dental caries
Plaque metabolism is a complex subject and the following is a very simplified account.
The main source of nutrition for oral bacteria is saliva. Although the carbohydrate content of saliva is generally low, increased levels (up to 1000-fold) are seen after a meal. To make use of these transient increases in food levels, oral bacteria have developed a number of regulatory mechanisms, which act at three levels:
The bacterial metabolism of carbohydrate is critical in the aetiology of caries as the acidic end products are responsible for enamel demineralization. The process begins when dietary sucrose is broken down by bacterial extracellular enzymes such as glucosyl and fructosyl transferases, with the release of glucose and fructose, respectively. These monosaccharides are then converted into polysaccharides that are either water-soluble or water-insoluble – glucans and fructans, respectively. Glucans are mostly used as a major bacterial food source; the insoluble fructans contribute to the plaque matrix while facilitating the adhesion and aggregation of plaque bacteria and serving as a ready, extracellular food source. Some of the sucrose is transported directly into bacteria as the disaccharide or disaccharide phosphate, which is metabolized intracellularly by invertase or sucrose phosphate hydrolase into glucose and fructose. During glycolysis, glucose is degraded immediately by bacteria via the Embden–Meyerhof pathway, with the production of two pyruvate molecules from each molecule of glucose. The pyruvate can be degraded further:
Different species produce acids at different rates and vary in their ability to survive under such conditions. The mutans group streptococci, being the most acidogenic and aciduric (acid-tolerant), are the worst offenders and reduce the plaque pH to low levels, creating hostile conditions for other plaque bacteria. The resultant overall fall in pH to levels below 5.5 initiates the process of enamel demineralization. This characteristic fall in plaque pH, followed by a slow return to the original value in about an hour, produces a curve that is termed the ‘Stephan curve’.
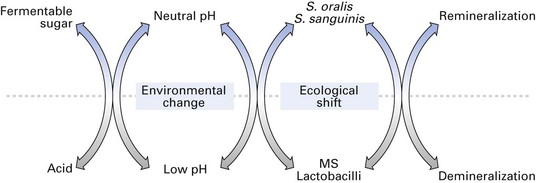
Ecological plaque hypothesis
A key feature of a number of caries studies is the absence of mutans streptococci at caries sites, suggesting that bacteria other than the latter can contribute to the disease process. Conversely, in some studies where mutans streptococci were found in high numbers, there was apparently no demineralization of the underlying enamel. This may be due to the presence of lactate-consuming species such as Veillonella, or to the production of alkali at low pH by organisms such as Streptococcus salivarius and Streptococcus sanguinis. These and other related findings have led to the development of the ‘ecological plaque hypothesis’ of caries (Fig. 32.4). According to this proposal, cariogenic flora found in natural plaque are weakly competitive and comprise only a minority of the total community. With a conventional diet, levels of such potential cariogenic bacteria are clinically insignificant, and the processes of remineralization and demineralization are in equilibrium. If, however, the frequency of intake of fermentable carbohydrates increases, then the plaque pH level falls and remains low for prolonged periods, promoting the growth of acid-tolerant (aciduric) bacteria while gradually eliminating the communal bacteria that are acid-labile. Prolonged low pH conditions also initiate demineralization. This process would turn the balance in the plaque community in favour of mutans streptococci and lactobacilli. The hypothesis also explains, to some extent, the dynamic relationship between the bacteria and the host, so that alterations in major host factors such as salivary flow on plaque development can be taken into account.
Management of dental caries
The conventional approach to the treatment of dental caries was to remove and replace diseased tissue with an inert restoration. This approach made no attempt to cure the disease, and the patient often returned some months later requiring further fillings due to new or recurrent caries. In contrast, the modern philosophy in caries management highlights:
The result of such measures should be less, rather than more, demand for restorative treatment by individual patients.
Patient evaluation
In patients with a low incidence of caries, a case history and clinical and radiographic examination are probably adequate for treatment planning. However, for patients with rampant or recurrent caries, or where expensive crown and bridge work is planned, additional investigations are necessary. These include:
Microbiological tests in caries assessment
Saliva samples can be used to establish the numbers of S. mutans and Lactobacillus spp. in the oral cavity, as follows:
Simplified detection kits for estimation of both lactobacilli and S. mutans in saliva are available. The results correlate well with laboratory plate counts, and the tests can be performed in the dental clinic without special facilities (Fig. 32.5).

Fig. 32.5 Dip slide test to detect mutans streptococci in saliva: a high density of white colonies indicates a higher caries risk.
The presence of high salivary levels of S. mutans or lactobacilli does not necessarily mean that the patient has an increased risk of developing dental caries, as it is a disease of multifactorial aetiology. Other factors, such as diet, buffering capacity, fluoride content of enamel and degree of oral hygiene, should also be considered. Further, the presence of large numbers of cariogenic organisms in saliva does not imply that all teeth are caries-prone, as the salivary organisms may have originated from a few foci with high caries activity. Therefore, these tests at best give a generalized approximation of the caries risk. It should be noted that the microbiological tests used in caries assessment differ from conventional tests used in medical microbiology, where the presence of a pathogen indicates a positive diagnosis (e.g. syphilis). The main uses of microbiology tests in caries assessment are:
Microbiology of root surface caries
Approximately 60% of individuals in the West aged 60 years or older now have root caries. This has arisen mainly because of the reduction in enamel caries and the consequential retention of teeth later into life, accompanied by gingival recession. The soft cemental surfaces thus exposed are highly susceptible to microbial colonization by virtue of their irregular and rough surfaces.
Early studies showed a high prevalence of Actinomyces naeslundii, Actinomyces odontolyticus and Rothia dentocariosa from human root surface caries. However, more recent data suggest a stronger association between lactobacilli, mutans streptococci and root caries. Indeed, the presence of lactobacilli is considered to be predictive of subsequent development of such lesions. The latter organisms, together with pleomorphic Gram-positive rods, are also frequent in the deeper dentinal parts of the lesion. Recent molecular analysis of deep dentinal surfaces of root caries lesions, to some extent, confirm previous findings and indicate S. mutans, lactobacilli and R. dentocariosa to be the predominant species. However, these organisms were associated with a vast number (>40) of new taxa!
Prevention of dental caries
The major approaches to prevention of caries are:
The rationale for these procedures is outlined below.
Sugar substitutes
Artificial sweeteners or sugar substitutes cannot be absorbed and metabolized to produce acids by the vast majority of plaque bacteria. Two types of sugar substitute are available:
Fluoridation
Fluoride can be delivered to the tooth tissue in many ways. When administered systemically during childhood, it is incorporated during amelogenesis. The best delivery vehicle is the domestic water supply (at a concentration of 1 ppm); failing this, tablets, topical applications of fluoridated gel or fluoridated toothpaste may be used.
Fissure sealants
Sealants prevent caries in pits and fissures by eliminating stagnation areas and blocking potential routes of infection. Early lesions that are well sealed can be effectively arrested by this technique, whereas more extensive lesions may extend into pulp, as the trapped cariogenic bacteria are able to use the carious dentinal matrix as a source of nutrition.
Control of cariogenic plaque flora
Control may be achieved by mechanical cleansing, antimicrobial therapy, immunization and replacement therapy.
Mechanical cleansing techniques
Conventional tooth-brushing with a fluoridated toothpaste is not very successful in reducing the caries incidence as it is entirely dependent on the motivation and skill of the patient. Further, it is unlikely that mechanical cleansing even with flossing, interdental brushes and wood sticks will affect pit and fissure caries.
Antimicrobial agents
Chlorhexidine as a 0.2% mouthwash is by far the most effective antimicrobial in plaque control:
Unfortunately, because of the problems of tooth staining and unpleasant taste, chlorhexidine is normally only used for short-term therapy.
Active immunization against dental caries
Using either cell wall-associated antigens (antigen I/II) or glucosyl transferases (extracellular enzymes) from mutans streptococci is effective in reducing experimental dental caries in rats and monkeys. The vaccine may produce its protective effect by:
However, convincing proof that any of these mechanisms prevents the development of dental caries in vivo is lacking. Vaccination trials on humans have been unsuccessful because of fears of possible side effects, which would be unacceptable as caries is not a life-threatening disease. (The antibodies that develop after immunization with most antigens of S. mutans tend to cross-react with heart tissue, and the possibility that heart damage could result has made human vaccine trials very difficult.) Furthermore, the incidence of dental caries is falling in the West and the disease can be adequately controlled using other techniques.
A caries vaccine could, however, be useful for developing countries with limited dental services and increasing prevalence of caries, and also for prevention of disease in high-risk groups, for instance, children with mental or physical disabilities.
Passive immunization
Experimental studies indicate that when the natural levels of oral mutans streptococci are suppressed by chlorhexidine, topical application of monoclonal antibodies against antigen I/II of mutans streptococci prevents recolonization by the organisms. Transgenic plants could be used to produce dimeric antibodies with specificity to antigen I/II of streptococci that are stable in the mouth and persist for longer periods than the monomeric antibody. These new developments have heightened the hopes of an alternative caries-preventive strategy for the future.
Replacement therapy
Experimental studies indicate that genetically engineered, low-virulence mutants of mutans streptococci that are deficient in glucosyl transferase or deficient in lactate dehydrogenase activity can be ‘seeded’ into the oral environment. These organisms can replace their more virulent counterparts and prevent their re-emergence. The term probiotic therapy or probiotics is now used for approaches where the offending pathogen is replaced artificially by innocuous commensals that are allowed to obtain a permanent foothold in the locale (e.g. oral cavity, intestines, vagina). It is feasible that replacement therapy of this nature may be exploited to control cariogenic flora in the future. However, assurances of the safety of these replacement strains are needed by both the public and the authorities before these methods are realized.
Key facts
Bowden G.H.W. Microbiology of root surface caries. Journal of Dental Research. 1990;69:1205-1210.
Fejerskov O., Ekstrand J., Burt B.A., editors. Fluoride in dentistry, 2nd ed., Copenhagen: Munksgaard, 1996.
Kidd E.A.M., Fejerskov O. Dental caries: The disease and its clinical management. Copenhagen: Blackwell Munksgaard; 2003.
Marsh P.D., Marin M.V. Oral microbiology, 5th ed. London: Churchill Livingstone; 2009.
Russell M.W., Chiders N.K., Michalek S.M., Smith D.J., Taubman M.A. A caries vaccine? The state of the science of immunization against dental caries. Caries Research. 2004;38:230-235.
Shen S., Samaranayake L.P., Yip H.K., Dyson J.E. Bacterial and yeast flora of root surface caries in elderly, ethnic Chinese. Oral Diseases. 2002;8:207-217.
Review questions (answers on p. 354 & p. 355)
Please indicate which answers are true, and which are false.