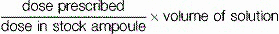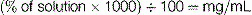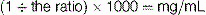10 Medicines management
• To provide an overview of policy and procedure associated with medicines management
• To provide an Introduction to the commonest medicines used for patients in medical placements
• To consider how to assess the effect of the medicines administered
• To identify opportunities to develop knowledge and skills in medicines management throughout the patient journey
Introduction
Regardless of your field of nursing or year of training, you will have learning outcomes that focus on medicines management because it is one of the Nursing and Midwifery Council (NMC) Essential Skills Clusters (NMC 2010) from year 1 to entry to the register. Box 10.1 provides some examples of the Essential Skills Cluster – Medicines Management (NMC 2010).
Box 10.1 Examples of the Essential Skills Cluster – Medicines Management
At the end of the first year, a student nurse needs to be competent in medicines calculations for tablets, capsules, liquid medicines and injections and International System of Units (SI) conversion.
By the end of the third year, many skills are identified such as the following:
 Drug pathways and how they act.
Drug pathways and how they act.
 Related anatomy and physiology.
Related anatomy and physiology.
(NMC 2010)
In every ward you are placed on, all of your patients will have one thing in common – a prescription chart. Some patients will have very few medications prescribed while others may have more than one chart. Medications can be a daunting area for students and you may wonder when you should start to learn about medications.
You need to start being involved in administering medication to your individual patients as early as possible, or as appropriate to your individual course of study and practice requirements. Many medications you come across will belong to common groups of drugs, for example antibiotics, analgesics and cardiac drugs. You need to start learning some of the common medications used, side effects, cautions and routes. It can be quite nerve wracking at first and you may find that your hands shake as you try to dispense medications into the receptacle in front of a qualified nurse. You may also feel that you are very slow and that you are holding up your mentor and making patients wait.
You are not alone, but it is not something that should be rushed. It is essential that you know what you are doing and why you are doing it, and it must always be under supervision. If you have not yet covered this topic in theory at university, then please refer to the NMC, university and trust guidelines for the administration of medications.
Read the NMC Standards for Medicines Management (2008a), your university and placement guidelines, and then discuss your role in medicines management with your mentor.
Nurse prescribing and patient group directives
Within your medical placements you may be exposed to a range of nurses who have completed an advanced course in nurse prescribing. Only those who have undergone appropriate training and are registered with the NMC as an independent prescriber can prescribe (NMC 2006). It must also be judged that it is part of the nurse's role. Some clinical nurse specialists, advanced nurse practitioners, practice nurses, district nurses, health visitors and community matrons will have completed this course and will have undergone intensive supervision and academic assessment to meet the competencies required (Kaufman 2010).
Ask your mentor if there are any practitioners within your area who are nurse prescribers and find out if you can spend some time with them to discuss their role and how it fits in with day-to-day medicine administration by nurses in placement.
Self-administration
In some of your medical placements, patients may be self-administering their medication and there should be a policy within the organisation that supports this practice. Nurses must assess that the patient is willing to do this, has the knowledge and is not forgetful or confused before self-administering their medication. It can work very effectively for patients as they do not need to wait for a nurse to administer their medication and they are able to have control over this aspect of their care. Within the essential skills clusters, there is an expectation that student nurses will ‘involve people and carers in administration and self-administration of medicines’ (NMC 2010) and from your second year this will be one of your learning outcomes under the supervision and guidance of your mentor.
There is also an assessment that can be undertaken when admitting or discharging a patient. Nurses can make arrangements for medication to be packaged in different ways to aid compliance. This can be arranged on discharge to allow health and social care practitioners within the community to help patients take their medicines. The NMC expects nurses to continually assess their patients regarding the appropriateness of the medication compliance aid. Patients who have been taking long-term medication are usually very knowledgeable about their medication. The following are examples of compliance aids:
• Blister packs: the medication is packaged with the days of the week highlighted.
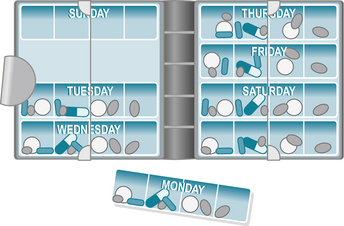
• Dosette boxes: the medication will be placed in a box with separate compartments for days and times by a nurse to ensure that the patient does not get muddled about which medication to take and when. This is very helpful when a patient has multiple medications to take every day (Fig. 10.1).
Covert administration
Covert administration of medicines means administering medicines to your patient without their knowledge, for example disguising it in food or drink. This is not considered good practice (NMC 2008a). If your patient is refusing their medicines, it is important that you first establish why they do not want to take them. Often it will be because they don't know what they are or why they need to take them. Spending some time explaining the medicines and reassuring your patient may be all that is needed for your patient to agree to take their prescribed medicines.
An interesting article for you to read:
Griffith R, Griffiths H, Jordan S (2003). Administration of medicines part 1: the law and nursing. Nursing Standard 18(2):47–51. Online. Available at: http://nursingstandard.rcnpublishing.co.uk/archive/article-administration-of-medicines-part-1-the-law-and-nursing (accessed July 2011).
If you are not sure about the medicines, use this as an opportunity to brush up on your own knowledge. Your patient may be having difficulty swallowing their tablets and it may be possible to order them in a different preparation, for example as a liquid. Crushing medication could also affect its metabolism/absorbance and may alter the affect of the drug. This could cause harm to the patient.
It may be that your patient does not understand the importance of the medicines and the potential side effects of not taking them. In this case, the team looking after the patient will need to determine if the patient has capacity to decide whether to take the medicines (see Ch. 6 for a discussion on capacity). Within the Essential Skills Clusters (NMC 2010) there is an expectation that ‘people can trust the newly registered graduate nurse to work within the legal and ethical frameworks that underpin safe and effective medicines management’.
If it is decided that a patient does not have the capacity to make the decision, the multidisciplinary team, along with those who know the patient best (e.g. relatives/carers), must make a decision in the best interests of the patient and this may be to administer medicines covertly. If this is the case, how and when the medicines are given must be decided and documented clearly in the patient's notes. This decision must also be regularly reviewed.
As you progress in your nurse training, your learning outcomes will incorporate ethical issues in relation to medicines and consent. You will need to be able to demonstrate that you are aware of religious, cultural and ethical beliefs pertaining to medications and that you are sensitive to these issues.
This Website provides information to patients regarding Ramadan and there is a comprehensive section relating to medicines:
http://www.nhs.uk/Livewell/healthyRamadan/Pages/Healthyramadanhome.aspx (accessed July 2011).
Medicines management for controlled drugs
Since the fourth report of The Shipman Inquiry (2004) there has been tighter legislation in relation to controlled drugs, and nurses need to familiarise themselves with the latest NMC, Department of Health and local trust and university policies. As a student, you will be placed in a variety of placements – community, independent sector and acute sector trusts – and will need to make sure that you are aware of the placement policies regarding controlled drugs. The NMC (2008a) emphasises that student nurses must be involved in the administration of all medicines when they are deemed competent by a registrant and also feel confident and competent themselves. One of the essential skill outcomes states that ‘people can trust the newly registered graduate nurse to safely order, receive, store and dispose of medicines (including controlled drugs) in any setting’ (NMC 2010).
Controlled drugs are kept in a double-locked cupboard and the nurse in charge will hold a separate set of keys to this cupboard. These keys are not to be left on hooks in the office nor on the ward desk, but on the person of the key holder at all times.
The national guidance for drugs considered to be controlled drugs can be found here:
Read the controlled drugs policy for the hospital you are placed in and note the role of the student nurse in the administration of controlled drugs. Compare this with your university administration of medicines policy, which you will have used in any clinical simulation activities concerning medicines management, and discuss this with your mentor.
Quiz: management of controlled drugs
Here is a quiz to help you with the above activity.
(Answers on p. 197.)
10.1. Are student nurses allowed to give any medication without supervision?
10.2. Which of these policies do student nurses need to read and understand prior to taking part in drug administration?
10.3. A staff nurse checks paracetamol with you in the clinical room and then asks you to take the medication to Mrs Smith in bed 8. Would you say yes or no? Explain your answer.
10.4. Mrs Patel is confused and refusing her antibiotic which she really needs. The staff nurse crushes the tablet and disguises it in a spoon of porridge and asks you to give this to the patient. Would you agree to this? Explain your answer.
10.5. Your patient requires a subcutaneous injection of insulin which the staff nurse allows you to draw up under his/her supervision. The staff nurse then takes you to the patient and allows you to administer the injection. Would you agree to do this? Explain your answer.
10.6. You have just undertaken a blood glucose measurement which is 10 mmol. The patient is on an insulin infusion which is currently running at 1 mL/hour. The prescription states that the infusion should run at 2 mL/hour if the blood glucose is 10 mmol. You inform the staff nurse and she tells you to increase the rate on the pump. Would you agree to do this? Explain your answer.
10.7. What is a controlled drug?
10.8. Who would need to be present when preparing and administering a controlled drug?
10.9. Where are controlled drugs kept?
10.10. Who has the keys for the controlled drugs?
10.11. When can a student nurse administer medications under supervision?
10.12. A patient is prescribed 0.1 mg thyroxine. The registered nurse asks you to come along to observe. The nurse checks the medication against the prescription chart and then counts out 10 × 100 μg tablets. She asks you to come with her and administer them to the patient. What is your response?
As a student nurse, you will need to become involved with medications under the direct supervision of a registered nurse wherever you are placed. As a third year student nurse, you will be required to be assessed undertaking a medicines management assessment as part of your nursing programme. Details of medicines management assessments are given in Box 10.2.
Box 10.2 Medicines management assessments
 Prepare the medicines trolley or use patients' own dispensary appropriately.
Prepare the medicines trolley or use patients' own dispensary appropriately.
 Check the prescription sheets and initially identify medication to be given at the prescribed time.
Check the prescription sheets and initially identify medication to be given at the prescribed time.
 Check that prescriptions are written in accordance with the medicines administration policy of the practice area.
Check that prescriptions are written in accordance with the medicines administration policy of the practice area.
 Explain details of side effects of medications to the assessor and explain how these side effects can be managed if they occur.
Explain details of side effects of medications to the assessor and explain how these side effects can be managed if they occur.
 Administer medication to patients with regard to the local medicines policies and NMC Standards for Medicines Management (2008).
Administer medication to patients with regard to the local medicines policies and NMC Standards for Medicines Management (2008).
 Ascertain the patient's understanding of the reasons for the administration of medications.
Ascertain the patient's understanding of the reasons for the administration of medications.
 Ensure that oral medicines have been ingested by the patient.
Ensure that oral medicines have been ingested by the patient.
 Demonstrate/describe the actions to be taken in situations of non-compliance of patients with prescribed medication.
Demonstrate/describe the actions to be taken in situations of non-compliance of patients with prescribed medication.
 Be able to give an account of the legislation governing the administration and storage of scheduled poisons and controlled drugs.
Be able to give an account of the legislation governing the administration and storage of scheduled poisons and controlled drugs.
 Be able to discuss the role of the student nurse in the administration of controlled drugs.
Be able to discuss the role of the student nurse in the administration of controlled drugs.
 Be able to discuss and demonstrate the procedure to follow when administering blood and blood products.
Be able to discuss and demonstrate the procedure to follow when administering blood and blood products.
 Be able to explain what the term ‘patient group directive’ means.
Be able to explain what the term ‘patient group directive’ means.
This can seem daunting and you may feel that you already have enough to cope with, including exams, objective structured clinical examinations, assignments and practice-based assessments. It is important for you to consider what type of learner you are. There are many strategies for learning about medications. Some of the following may help:
• Make sure that you administer the medications for your group of patients according to trust, university and NMC guidelines. You will be doing this under the supervision of the registered nurse.
• Become involved with the administration of controlled drugs – make sure that you understand the policy for administering this medication. Who is able to sign the controlled drugs book? Who holds the keys to the controlled drug cupboard? Are the keys kept with the other medication keys or are they a separate bunch? How often do these medications need to be checked and by whom?
• Many patients will be given intravenous drugs. Make sure you look at and understand the policy for this and the training that is required for this procedure, as well as the rationale for the patient having to have these.
• When you administer medications to patients, do they have a right to be informed about each medication? Remember that they are partners in their care.
• Think about the dose, route, side effects and contraindications for the medications.
• Identify the different groups of drugs and three drugs that belong to each group. You will find that each group of drugs often has side effects in common.
• Maybe think of a mnemonic to help you learn the drug side effects.
• You could learn about three drugs a day and make notes about them.
• You may find it easier to link medications to patients' conditions.
• Try to find a book related to medicines that you find readable and easy to understand.
• Remember that everyone learns in a different way. Your mentor may also be able to give you advice.
• Ask your mentor to undertake a mock drug assessment with you. This could highlight your strengths and help you to understand where you need to develop.
List the different routes of medication that can be administered and give examples of the routes and medication that you have been actively involved in administering within your practice area.
Ask your mentor about administering drugs via a syringe driver. If possible, try to observe medication for a syringe driver being prepared by a staff nurse and see how the syringe driver is set up with the patient.
Determine what key skills are required to prepare and administer this kind of medication. If you are a third-year student, it may be appropriate for some of these to be included in your learning outcomes (see Further reading list for clinical skills texts that may be useful).
Drug calculations
It is really important to ensure that you are competent and accurate when undertaking calculations for medications. If you get the dose wrong, this could harm the patient – too low a dose could be ineffective and too high a dose could be toxic.
Drug calculations need practice and it is important that you let your mentor know if this is something you struggle with. Mentors can only help if they know what you need help with. Many nurses worry about calculations. They may not be natural mathematicians! However, calculations are something you can learn. If you know the formula, then you can work out the dose for the medication. You are never alone on a ward and there is always someone to check your calculation with.
Acknowledging our limitations is part of the NMC Code (2008b), however there is a level of competence that needs to be achieved by a registered nurse before they can administer medications. Once you qualify, you will find that this competence is frequently tested by organisations to ensure patient safety.
Within all fields of nursing, the essential skills clusters expect student nurses to be competent in ‘basic medicines calculations relating to: tablets and capsules, liquid medicines, injections including unit dose, sub-and multiple unit dose and SI unit conversion’.
Calculating drug dosages
Here are some common formulae used in calculations. (Refer to Table 10.1 for a list of common abbreviations and concentrations.)
Table 10.1 Abbreviations and concentrations
| Abbreviations | |
|---|---|
| g | gram |
| mg | milligrams |
| mcg/μg | micrograms |
| ng | nanograms |
| L | litre |
| mL | millilitre |
| mmol | millimole |
| Concentrations | |
|---|---|
| 1 g | 1000 mg |
| 1 mg | 1000 mcg |
| 1 mcg | 1000 ng |
Calculating amount of a solution needed to obtain a prescribed dose
Working out the amount of a solution you need to obtain the prescribed dose is achieved using the following formulae:
Calculating concentrations of drugs in solution
To work out the concentration of a solution (i.e. how many mg there are per mL), we use the following formula:
Working out the amount of drug in a solution
Some drugs that are presented in a ‘percentage’ solution will have the amount of drug per mL stated, either on the ampoule or in the accompanying literature. However, the following formula can be used to work out the amount of drug present in a given volume of fluid when it is presented in a percentage form:
Drug dosages in ratios
Some concentrations of drugs are presented as ratios (e.g. adrenaline (epinephrine) is available in concentrations of 1:1000 and 1:10 000):
• A 1:1000 solution means that 1 g is dissolved in 1000 mL.
The following formula can also be used:
What knowledge of medications is required?
Apart from the calculations, you need to consider the medications that are commonly used on your medical placements. For entry to the register, you will need to apply ‘knowledge of basic pharmacology, how medicines act and interact in the systems of the body and their therapeutic action’ (NMC 2010). It is easier to start with groups of medications, and the list in Box 10.3 is by no means exhaustive.
Once you have sorted out the groups of medications, specify the actual medications that are used on your ward. You need to know the general doses, routes and side effects of the drugs.
Quiz
Ask yourself the following questions about the bronchodilator salbutamol.
(Answers on p. 197.)
10.13. What is the action of bronchodilators?
10.14. What routes can you use to administer salbutamol?
10.15. What is the usual dose for a salbutamol nebuliser?
Consider the action of antibiotics: what are they commonly used for?
Common antibiotics include amoxicillin, cefuroxime, ciprofloxacin, metronidazole, vancomycin and gentamicin. It is important to check blood levels prior to administration and to reduce the dose in renal failure.
Side effects include diarrhoea, allergy, rash, nausea, vomiting and anaphylaxis. It is imperative to know how to treat anaphylaxis as this is a medical emergency.
Quiz: medications
(Answers on p. 197.)
10.18. What are the side effects of opiates?
10.19. What two observations should you look at before administering cardiac drugs?
10.20. What are the side effects of antibiotics?
10.21. Name four groups of laxatives.
10.22. What groups do the following drugs belong to?
10.23. What do you need to consider if a patient is on long-term steroids? What impact might this have on your nursing care?
10.24. What information might a patient who is taking salbutamol require?
10.25. Are there any special requirements for patients who are taking vancomycin or gentamicin?
10.26. What blood test do patients who are taking warfarin require and what is the antidote?
10.27. When, in relation to food, do you give a patient flucloxacillin?
Medicines management is an essential skill or nurses, and wherever you are in your placement you will be involved in the administration of medications under the supervision of a registered nurse. Despite all of the policies, guidance and knowledge for the administration of medications, errors still occur.
Assessing the effect of medication you have given
When you are undertaking the administration of medicines during your medical placement, you will more than likely be administering analgesia to your patients. If a patient is prescribed analgesia, should you, as the nurse, administer it just because it is prescribed or should you assess the patient prior to administering the medication? This will provide your patient with an opportunity to tell you about any pain they are experiencing and will empower them to take an active role in their management. It is important that you understand how the patient is feeling prior to administering analgesia so that you can understand how effective the analgesia has been and document this. It can be difficult to assess pain in those who cannot respond verbally, however there can be physiological changes in respiration, blood pressure and pulse rate, nausea and sweating. Visually, the patient's body language, emotions or facial expression could also indicate that they are in pain. There are various pain assessment tools available including verbal descriptors, numerical rating scales and visual analogue scales that can help you to assess and evaluate pain.
When administering analgesia, it is important to think about the following:
• How much pain is the patient experiencing? Measure and record it in the nursing notes.
• Does the analgesia you are administering take the pain away?
• Could you offer anything else – repositioning, heat?
• Is the patient requesting analgesia before the next dose is due?
• Is the patient experiencing any side effects that you can help to reduce, e.g. offering aperients for constipation?
Refer to the example of visual analogue used at Newham University Hospital NHS Trust (Fig. 10.2).
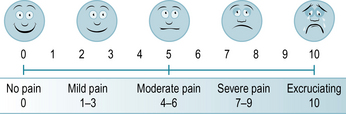
Fig 10.2 Example of visual analogue to help assess and evaluate pain used at Newham University Hospital NHS Trust
You are looking after a 74-year-old man who is rehabilitating on an intermediate care ward recovering from pneumonia, which has left him very weak. You are about to administer his medicines under the supervision of a registered nurse. He is prescribed digoxin 125 μg once a day and bisoprolol 10 mg once a day. Before you administer the digoxin, you take his pulse and find that it is 52 bpm. What should you do?
(Answer on p. 198.)
Mrs Wells is a 73-year-old lady who is rehabilitating on a stroke unit. She has diabetes and usually takes three short-acting insulin injections a day and a longer acting insulin at night. At handover, the night staff inform you and your mentor that they have not been able to give the night dose of insulin because her blood sugar has been very low, requiring the patient to have sugary drinks and snacks. The doctor was informed overnight. The blood sugar prior to breakfast is within normal limits. Your mentor asks you about the actions that need to be taken by a registered nurse.
(Answers on p. 198.)
Summary
In this chapter you have explored the policies and procedures in relation to medicines management and considered the commonest medicines that your medical patients may have been prescribed. The role of the nurse in the administration of medicines is an important one and keeping up to date during your career is a must. Medication policies change and it is important that you always read and check the medicines policies in each placement area. You will become more confident and knowledgeable throughout your training but you will never know everything there is to know about medicines, as medical research continues to develop new medicines.
Brooker C., Waugh A. Foundations of nursing practice: fundamentals of holistic care. Edinburgh: Mosby; 2007.
Kaufman G. Developing patient group directions for medicines management. Nursing Standard. 2010;24(48):50–56.
Nursing and Midwifery Council. Standards of proficiency for nurse and midwife prescribers. London: NMC; 2006.
Nursing and Midwifery Council. Standards for medicines management. London: NMC; 2008.
Nursing and Midwifery Council. The code: standards of conduct, performance and ethics for nurses and midwives. London: NMC; 2008.
Nursing and Midwifery Council. Essential skills clusters. London: NMC; 2010.
The Shipman Inquiry. Fourth report. The regulation of controlled drugs in the community. London: Department of Health; 2004. Online. Available at http://www.shipman-inquiry.org.uk/reports.asp
Bennett J., Dawoud D., Maben J. Effects of interruptions to nurses during medication administration. Nursing Manage. 2010;16(9):22–23.
Crocker C. Following the patient journey to improve medicines management and reduce errors. Nursing Times. 2009;105(46):12–15.
Dougherty L. Delivery of intravenous therapy. Nursing Standard. 2002;16(16):45–52.
Elliot M., Liu Y. The nine rights of medication administration. British Journal of Nursing. 2010;19(5):300–305.
Hyde L. Legal and professional aspects of intravenous therapy. Nursing Standard. 2002;16(26):39–42.
Jenkins K., Kirk M. Heart failure and chronic kidney disease: an integrated approach. Renal Care. 2010;36:127–135.
Jordan S., Griffiths H., Griffith R.A. Administration of medicines part 2: pharmacology. Nursing Standard. 2003;18(3):45–54.
Kirby M. A spoonful of sugar: helping older patients to take their medicines. British Journal of Primary Care Nursing: Cardiovascular Disease and Diabetes. 2008;5(1):21–23.
McIntosh K. Medicines management. Nursing Times. 2008;104(44):18–20.
Tingle J. Patient safety and health quality: recent reports from the CQC. British Journal of Nursing. 2010;19(7):45–55.
Nursing and Midwifery Council. Standards for pre-registration nursing education. London: NMC; 2010.
Answers
10.3. No, because you need the staff nurse to witness and supervise you to ensure that the medication is given to the correct patient.
10.4. No, for two reasons: i) disguising medication is not considered good practice by the NMC (2008a); ii) crushing the medication may alter the therapeutic properties of the medication.
10.5. Yes, if you are competent and the patient consents.
10.6. No, because as a student nurse you are not allowed to administer medications unsupervised.
10.7. Some prescription medicines contain drugs that are controlled under the Misuse of Drugs legislation. These are called controlled drugs.
10.8. Depending on the organisation this can vary, but if there are two registered nurses available, they should check the controlled drug with the student nurse as witness. Always check your university and organisational policy in relation to controlled drugs.
10.9. Controlled drugs are kept in a double-locked cupboard
10.12. No, because this would be a drug error – 0.1 mg thyroxine = 100 μg thyroxine, therefore only one tablet is required.
10.13. Bronchodilators cause the bronchi to dilate.
10.15. 2.5–5 mg via a nebuliser, repeated up to 4 times a day.
10.16. Tachycardia, arrhythmia, headache, nausea, gastric irritation.
10.18. Commonly respiratory depression, constipation, itchiness, nausea, vomiting.
10.19. Blood pressure and pulse.
10.20. Anaphylactic shock, rash, diarrhoea, nausea and vomiting at toxic levels.
10.21. Osmotic, bulk forming, enemas, suppositories and stimulating.
10.23. Cushings syndrome, diabetes, gastric ulceration, thinning of the skin, hypertension, Addision's crisis.
• You would assess the patient for any history of gastric ulceration/irritation prior to administering steroids. If this is a problem for the patient, a proton pump inhibitor could then be prescribed by the doctor to prevent this side effect and maybe enteric-coated steroids prescribed.
• Check urinalysis for glucose.
• Weigh the patient to assess if the patient has gained weight and ask if they have noticed any changes in their appearance.
• Patient information and health education: the patient should be informed about the need to reduce steroids gradually under the supervision of a doctor to prevent Addison's crisis.
• The action of the medication.
• Help with their inhaler technique or what to do with their nebuliser mask once the medication has finished.
• Side effects that they might experience: palpitations, tremors, headaches, anxiety.
• Peak flow: technique, information, peak flow diary.
10.25. Blood levels need to be taken to prevent toxic levels building up. Doctors usually need to gain microbiology consent prior to prescribing these.
10.26. The International normalised ratio test (INR). The antidote to warfarin is vitamin K, given in tablet or injectable form.
10.27. 30 minutes before food.
Case history 10.1 After discussion and under the supervision of a registered nurse, you could do the following. Omit both medicines for the time being, as both will reduce the heart rate, and contact the doctor to determine what she would like you to do. Ensure that the patient is kept fully informed and that every action you take is documented accurately in the nursing notes. The doctor may prescribe a lower dose of digoxin and ask you to omit the beta blocker, or she may ask you to omit both for today and say that they will review the patient on the ward round. Your role is to understand how the medications could affect your patient and inform the doctor if you feel that administering them might be contraindicated.
Case history 10.2 Ensure the patient has her breakfast, administer insulin for the morning and contact the diabetic nurse specialist and doctor to review the blood sugar. Ask the patient how she is feeling. Document any actions you take in the nursing notes and keep the patient informed of what is going on with her medication.