52 Eosinophilic folliculitis and furunculosis
INTRODUCTION
Canine eosinophilic furunculosis is an uncommon condition with an acute onset. It is usually confined to the nose and the muzzle, although it can occur on the pinna and the trunk. The severity of the lesions varies and many dogs will exhibit signs of pruritus. In most cases, it is thought to result from an acute hypersensitivity reaction to arthropod antigens. The condition is similar to mosquito-bite hypersensitivity in cats.
CASE HISTORY
Most dogs are presented with a history of a sudden onset of symptoms. Only when questioned is the owner likely to report a possible recent exposure to insects.
CLINICAL EXAMINATION
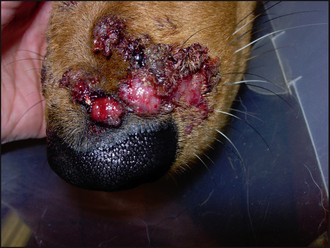
A physical examination revealed enlarged submandibular lymph nodes, but all other parameters were within normal limits. Multiple nodules, some with an ulcerated surface and some with a haemorrhagic crust, were present on the bridge of the nose (Fig. 52.1). The dog resented examination of this site. None of the other sites were affected in this case.
The most likely differential diagnoses based on the history were:
An adverse drug reaction can also have a sudden onset, but the dog in this case had not been medicated for over 12 months. Other less likely diagnoses include:
However, the onset in these conditions is slow and the lesions progressively worsen. Furthermore, they usually involve multiple sites, so they can easily be ruled out during the case work-up.
CASE WORK-UP
The case work-up should include, or rule out, the differential diagnoses. In this case, the following tests were performed:
The excision biopsy and one punch biopsy were placed in pots containing 10% formal saline and submitted for histology.
A biopsy sample is required to culture certain bacterial organisms and fungi, so the second punch biopsy was placed in a sterile pot, in sterile saline to keep it moist, and was submitted for bacterial and fungal culture. In this case, there was no bacterial growth on aerobic and anaerobic culture after 72 hours, and no fungal growth after 3 weeks of incubation.
A tentative diagnosis of canine eosinophilic furunculosis was made, based on the history, clinical signs and the cytological findings before the results of bacteriology and histology were known. Treatment was started to provide relief to the dog, as this condition is intensely pruritic and in some cases painful.
Histological examination then revealed epidermal ulceration with moderate epidermal acanthosis, intense eosinophilic infiltrate around the intact and disrupted hair follicles, and fragments of keratin present in the dermis. Dermal oedema and haemorrhage were also present. These changes were consistent with eosinophilic furunculosis. Fungal elements were not demonstrated on Periodic acid–Schiff (PAS)-stained histological sections.
In recurring cases, further evaluation of the role of insects may be determined by intradermal testing using insect antigens. However, due to the limited availability of these allergens for intradermal testing and the wide range of insects that could have been involved, it was not undertaken in this case.
DIAGNOSIS
Canine eosinophilic furunculosis was confirmed on histology but the trigger for the condition was not determined, although an insect bite was implicated.
PROGNOSIS
The prognosis for this condition is good, although the owner has to be warned of possible recurrences if the dog is exposed to the allergens again. Rapid, appropriate glucocorticoid therapy is indicated in more severely affected cases because scarring may result if treatment is excessively delayed.
AETIOPATHOGENESIS
A hypersensitivity response to arthropod venom is the most likely cause of the symptoms in these cases, even though in most cases the actual exposure is not seen by the owner. Wasps, bees, mosquitoes, spiders, hornets, black flies, stable flies and other stinging insects have all been implicated.
In dogs, Type I and IV hypersensitivity mechanisms are thought to be involved, although in humans Type III and Type IV mechanisms have been proposed for arthropod-bite reactions. Type III and Type IV reactions are implicated for tick-bite reactions in dogs.
Exposure to insect venom in sensitized individuals leads to mast cell degranulation and the consequent release of inflammatory mediators. These mediators are involved in further recruitment of inflammatory cells, in particular eosinophils, to the site. The eosinophils in turn produce toxins, enzymes and cytokines, all of which lead to extensive tissue damage and help to perpetuate the lesions (see Chapter 36).
EPIDEMIOLOGY
Eosinophilic furunculosis is an uncommon condition that is seen in dogs of any age, although more than half the reported cases are in dogs less than 2 years old. This age distribution may arise because it is the younger, less experienced, dogs that are more likely to disturb insect nests.
There is no reported sex or breed predisposition, but it is thought that larger breeds, living outdoors, may be more prone to it than smaller, indoor, dogs. A higher incidence has been observed in the warmer months, when insect activity is at its highest; however, it is reported in winter months and in dogs living indoors.
TREATMENT
Systemic glucocorticoids are indicated in all cases for rapid response, although resolution without treatment has been reported. The treatment of choice is prednisolone administered at 1 mg/kg daily, ideally until resolution of lesions, then reduced to alternate days, and gradually tapered off and withdrawn. Most cases respond within 48 hours and resolve within 3 weeks.
Topical ointments or gels containing corticosteroids can be applied to the lesions; however, topical treatment alone is not sufficient to provide complete and quick relief to the dog.
Sedatives such as acetylpromazine may be prescribed for the first few days to stop self-trauma, if one is unable to make a tentative diagnosis based on surface cytology and needs to wait for results before starting glucocorticoids.
Treatment in this case
Treatment was started with prednisolone at 1 mg/kg for 10 days which was then reduced to 0.5 mg/kg every alternate day for 2 weeks until resolution of lesions when glucocorticoid therapy was withdrawn.
Cases should be monitored for evidence of secondary bacterial infection and antibacterial treatment started if required.
This is one of the few conditions that have both a sudden onset of severe lesions and pruritus. In most cases the history and clinical signs are suggestive of the condition, and in most cases a tentative diagnosis can be made by simple in-house cytology. Treatment should be started immediately, after obtaining the appropriate biopsy samples necessary to confirm the diagnosis.