Other Eczematous Eruptions
The major forms of dermatitis include atopic (see Chapter 10), contact (see Chapter 12), seborrheic, asteatotic (xerotic), stasis, and nummular. Dermatitis of special sites – i.e. hands, feet, lips, diaper area, and major body folds – is reviewed in Chapter 13, and pityriasis alba is reviewed in Chapters 10 and 54.
Seborrheic Dermatitis
• Common disorder with both an infantile and an adult form (Figs. 11.1 and 11.2); unusual in children.
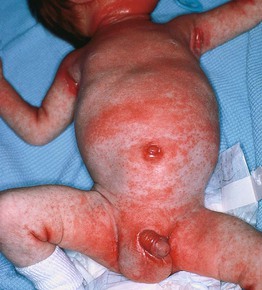
Fig. 11.1 Infantile seborrheic dermatitis. Glistening red plaques of the neck, axillary and inguinal folds as well as the penis and umbilicus. Note disseminated lesions on the trunk and extremities. Courtesy, Robert Hartman, MD.
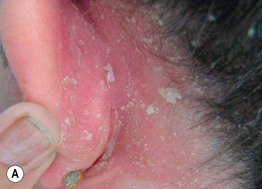
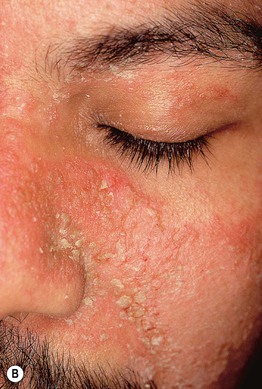
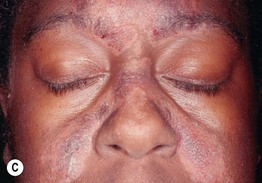
Fig. 11.2 Adult seborrheic dermatitis of the scalp, ear, and face. A Fairly sharply demarcated pink plaque with white and greasy scale. Note the fissure in the retroauricular fold. B Thin pink-orange plaques with yellow, greasy scale, especially of the melolabial fold and eyebrows. C Symmetric red-brown to violet plaques of the central forehead, nasal bridge, and medial cheeks with an associated hypopigmented figurate rim. A, Courtesy, Norbert Reider, MD, and Peter O Fritsch, MD; C, Courtesy, Jeffrey Callen, MD.
• Possibly related to components of sebum and Malassezia spp.
• Severe or recalcitrant seborrheic dermatitis can be a sign of underlying HIV infection or neurologic disorder.
• In adults, tends to be a chronic relapsing disorder; stress or tapering of systemic CS can lead to a flare.
• Symmetric distribution pattern that includes sites of greater sebum production – scalp, ears (external canal, retroauricular fold), medial eyebrows, upper eyelids, nasolabial folds, central chest – and major body folds.
• Lesions are pink-yellow to red-brown in color, depending on the underlying skin phototype, and they often have greasy scale, especially in the head and neck region; occasionally annular in configuration.
• On the scalp, involvement tends to be more diffuse, with well-circumscribed plaques with thicker silvery scale more characteristic of psoriasis.
• In some patients, the lesions of the scalp, ears, and major body folds have features of both seborrheic dermatitis and psoriasis, leading to the term ‘sebopsoriasis’.
• DDx: psoriasis, contact dermatitis, other causes of diaper dermatitis (see Fig. 13.4), intertrigo (see Fig. 13.2) or blepharitis, tinea versicolor (presternal), tinea capitis (especially in children), atopic dermatitis, pityriasis amiantacea and dermatomyositis (scalp); may coexist with rosacea.
• Rx: topical anti-fungal creams and daily shampooing (e.g. ketoconazole, ciclopirox, selenium sulfide or zinc-containing shampoo alternating with a gentle shampoo), mild topical CS on the face and in body folds and moderate-strength topical CS for the scalp and ears; topical calcineurin inhibitors (e.g. tacrolimus ointment).
Asteatotic Eczema (Xerotic Eczema, Eczema Craquelé)
• Arises in areas of dry skin, especially during winter months, in dry climates and in older adults.
• The areas of dermatitis resemble a ‘dried riverbed’ or ‘crazy-paving’ with superficial cracking of the skin (Fig. 11.3).
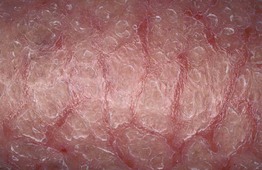
Fig. 11.3 Asteatotic eczema (eczema craquelé). The distal lower extremity has obvious inflammation and xerosis with adherent white scale (pseudo-ichthyosis) as well as a crisscross pattern of superficial cracks and fissures said to resemble a dried riverbed. Courtesy, Louis A. Fragola, MD.
• May be associated with pruritus; stinging can occur with application of water-based topical agents, including those that contain lactic or glycolic acid.
• Favors the shins, thighs, lower flanks, and posterior axillary line; may become more widespread but with sparing of the face, palms, and soles.
• Involvement of the posterior axillary line seen in chronic GVHD; when widespread, consider the possibility of an underlying systemic lymphoma.
• DDx: stasis dermatitis ± autosensitization, ichthyosis vulgaris, adult atopic dermatitis, allergic or irritant contact dermatitis.
• Rx: decrease frequency of bathing and use of soaps, liberal use of water-in-oil emollients, mild topical CS ointments.
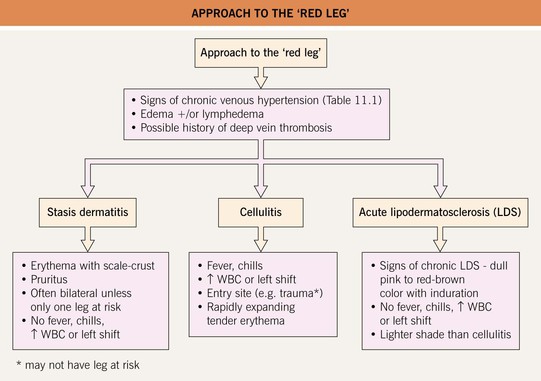
Stasis Dermatitis
• Pruritic dermatitis with scale-crust and sometimes oozing that favors the shins and calves; historically often begins near the medial malleolus.
• Patients often have a history of chronic lower extremity edema and may have a history of deep vein thromboses and/or recurrent cellulitis.
• Often accompanied by other signs of chronic venous hypertension (Table 11.1).
Table 11.1
Cutaneous signs of chronic venous hypertension.

* Need to exclude causes of hypercoagulability.
• One of the more common causes of autosensitization (Fig. 11.4).
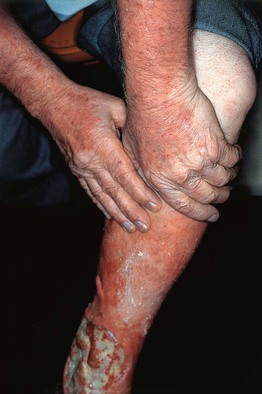
Fig. 11.4 Autosensitization dermatitis. There is dermatitis of the extensor surfaces of the upper extremities in this patient with allergic contact dermatitis to neomycin as well as stasis dermatitis and venous ulceration. Courtesy, Jean Bolognia, MD.
• DDx: allergic contact dermatitis, irritant contact dermatitis, asteatotic eczema, nummular dermatitis; may accompany other causes of the red leg, especially cellulitis and acute or chronic lipodermatosclerosis (Fig. 11.5), but the latter lack the clinical and histologic findings of dermatitis.
• Rx: exclude superimposed allergic contact dermatitis (e.g. neomycin, preservatives in topical creams) or component of infectious eczematous dermatitis if draining ulcer; open wet dressings for a few days, mild topical CS ointments, leg elevation, pressure stockings (after excluding arterial insufficiency via ankle–brachial index), endovascular ablation of large varicosities, water-in-oil emollients for maintenance therapy.
Autosensitization Dermatitis (Id Reaction)
• More widespread distribution of dermatitis that follows by days to weeks the development of localized areas of dermatitis, e.g. allergic contact dermatitis, stasis dermatitis, inflammatory tinea infections.
• Can also represent a rebound phenomenon when there has been too rapid a taper of systemic CS, as in 6-day taper of prednisone or methylprednisolone (Medrol® dose pack) for poison ivy.
• Favored sites of involvement (in addition to primary site): extensor aspects of extremities (see Fig. 11.4), palms and soles, usually in a symmetric pattern.
• In children with tinea capitis, the id reaction often involves the head and neck region.
• Areas of dermatitis, often ill-defined, can be accompanied by excoriated papules (Fig. 11.6).
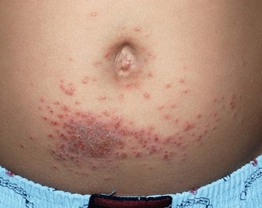
Fig. 11.6 Id reaction in a child due to allergic contact dermatitis (ACD) to nickel. Square-shaped area of ACD due to nickel in a buckle surrounded by multiple crusted edematous papules. Courtesy, Julie V. Schaffer, MD.
• DDx: atopic dermatitis, widespread contact dermatitis (e.g. textiles), Gianotti–Crosti syndrome, drug eruption to systemic anti-fungal medication (tinea capitis id), eczematous drug eruptions (e.g. calcium channel blockers [unusual]).
• Rx: in addition to aggressively treating the primary dermatitis, topical CS and oral antihistamines usually suffice; occasionally, when severe, systemic CS.
Infectious Eczematous (Eczematoid) Dermatitis
• Dermatitis that initially involves the skin surrounding a site of infection, usually bacterial, which is weeping or has drainage (e.g. otitis externa, infected leg ulcer, toe web infection).
• An id reaction can develop and treatment of both the infection and the dermatitis is recommended.
Nummular Eczema (Nummular Dermatitis)
• Markedly pruritic, coin-shaped lesions of dermatitis, usually measuring 2 or 3 cm in diameter (Fig. 11.7).
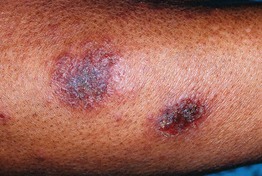
Fig. 11.7 Nummular eczema. Coin-shaped lesions of acute and subacute dermatitis that are fairly well demarcated. There is often marked pruritus. Courtesy, Kalman Watsky, MD.
• Occurs primarily on the extremities, classically the legs in men and the arms in women.
• Favors adults and can develop in the absence of an atopic diathesis; a chronic relapsing course is common.
• DDx: atopic dermatitis, autosensitization dermatitis, impetigo, stasis dermatitis, allergic contact dermatitis, tinea corporis, vesicular pityriasis rosea, mycosis fungoides.
• Rx: in addition to topical CS and calcineurin inhibitors, often requires phototherapy to clear.
Dyshidrotic Eczema (Acute and Recurrent Vesicular Hand Dermatitis)
• Firm, pruritic vesicles of the palms > soles as well as the lateral and medial aspects of the digits (Fig. 11.8); chronic and recurrent.
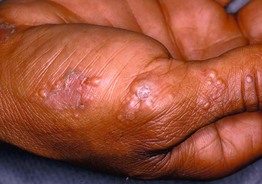
Fig. 11.8 Dyshidrotic eczema. Clusters of firm vesicles along the lateral aspect of the thumb and hypothenar eminence. Courtesy Louis A. Fragola, MD.
• Intact vesicles due to edema within the epidermis are more long-lived because of the thick stratum corneum in acral sites.
• When the vesicles are small and grouped, they are said to have an appearance similar to tapioca pudding.
• When larger vesicles develop, the term pompholyx is sometimes used.
• Can flare with stress, allergic or irritant contact dermatitis and administration of IVIg; seen in patients with atopic dermatitis and hyperhidrosis.
• DDx: id reaction (overlap), inflammatory tinea pedis or manuum, allergic contact dermatitis, scabies, dyshidrosiform bullous pemphigoid; if secondarily infected, palmoplantar pustulosis; when localized to a single digit, whitlow (herpes simplex infection) or blistering digital dactylitis (staphylococcal or group A streptococcal infection).
• Rx: exclude allergic or irritant contact dermatitis; topical CS, topical calcineurin inhibitors, bath PUVA; occasionally, when severe, systemic CS.
Juvenile Plantar Dermatosis
• Favors the plantar surface of the forefeet in prepubertal children, usually with an atopic diathesis.
• The skin is dry and scaly with mild inflammation and a characteristic glazed appearance (Fig. 11.9).
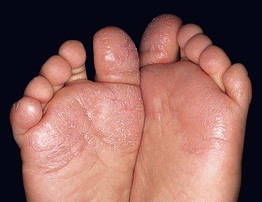
Fig. 11.9 Juvenile plantar dermatosis in a child. Erythema and scaling of the plantar surface of the forefoot, especially the ball of the foot and the great and fifth toes. Note the glazed appearance of the skin of the left foot. Courtesy, Kalman Watsky, MD.
• Thought to be related to hydration of the stratum corneum from wearing shoes made of impermeable materials and subsequent shearing of skin due to friction.
• DDx: other causes of foot dermatitis (see Table 13.1), especially psoriasis, allergic contact dermatitis (e.g. rubber, chromates in leather), tinea pedis (interdigital toe webs involved), atopic dermatitis.
• Rx: permeable socks and shoes, emollients, CS ointments, removal of wet socks along with wet shoes.
Infective Dermatitis
• Rare disorder of childhood or adolescence associated with human T-cell lymphotropic virus type 1 (HTLV-1) infection.
• Dermatitis of the scalp, ears, eyelid margins, paranasal skin, axillae, and groin that clears with oral antibiotics.
For further information see Ch. 13. From Dermatology, Third Edition.