Nail Disorders
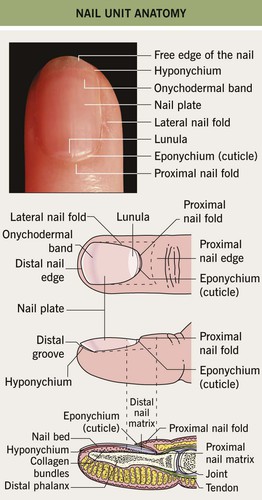
• The nail matrix, which is the growth area, has proximal and distal components (Fig. 58.1).
– The proximal nail matrix forms the top (surface) of the nail plate.
– The distal nail matrix forms the underside of the nail plate; therefore, biopsies of the distal matrix are less likely to produce a deformity of the surface of the nail plate.
• Fingernails grow ~1 mm per month and are replaced every 6 months.
• Toenails grow ~0.5 mm per month and are replaced every 12 months.
• Therefore, nail plate abnormalities such as Beau's lines that are due to insults to the nail matrix can be dated by their distance from the cuticle.
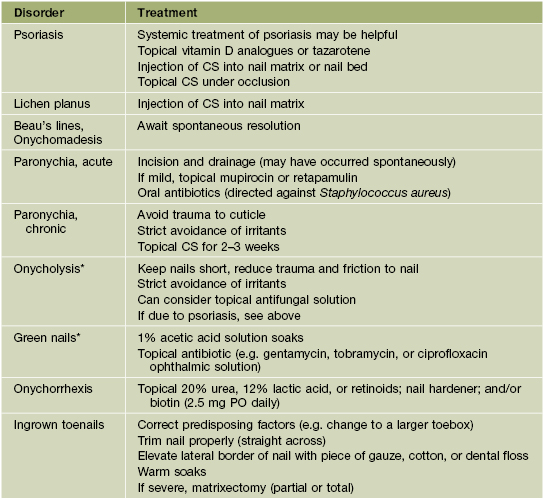
• Rx of common nail disorders is given in Table 58.1.
Onycholysis
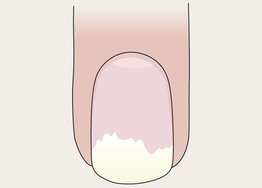
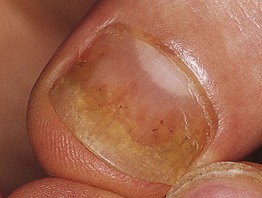
• Distal nail plate detachment, causing nail to look white to yellow-white (Fig. 58.2).
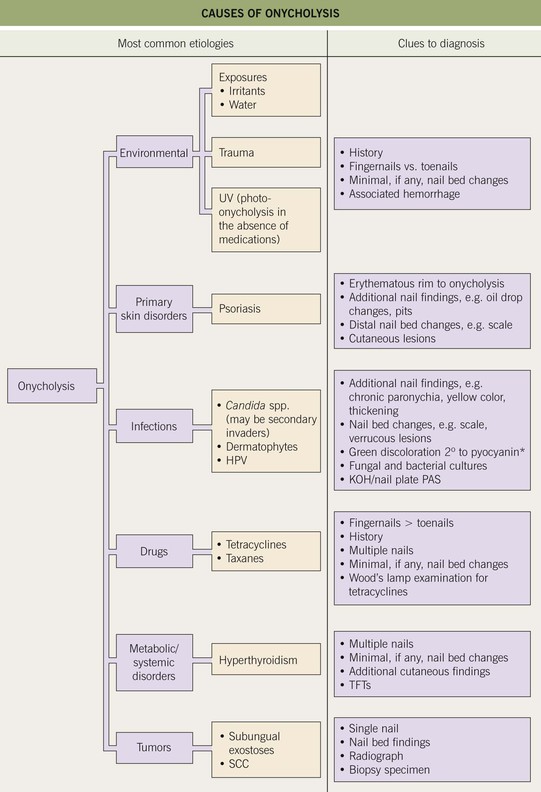
Fig. 58.2 Causes of onycholysis. *Due to secondary colonization with Pseudomonas aeruginosa. SCC, squamous cell carcinoma; TFTs, thyroid function tests.
• Chronic exposure to water and irritants (e.g. soaps) is a common cause.
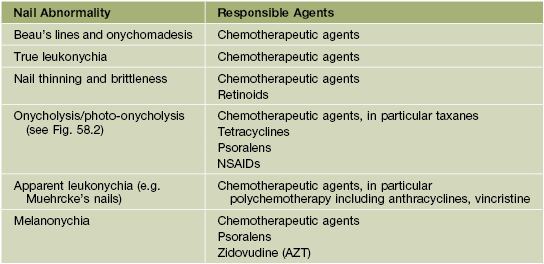
• Associated with psoriasis, onychomycosis, hyperthyroidism, and medications (Table 58.2).
Onychomadesis
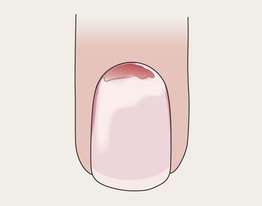
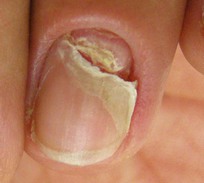
• Proximal detachment of nail plate.
• When single digit, often due to trauma.
• Consider systemic cause (e.g. high fever, chemotherapy, post-erythroderma, post-viral) if multiple nails involved.
Pitting in Psoriasis
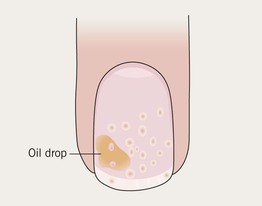
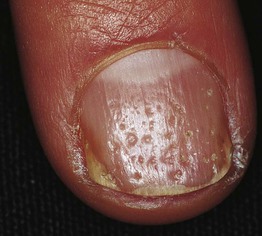
• Punctate depressions in the nail plate.
• Admixed with oil drop changes and other signs of nail psoriasis such as onycholysis, subungual debris (see Chapter 6).
Darier Disease
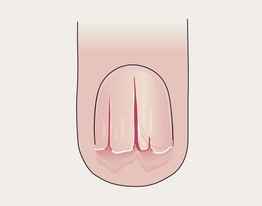
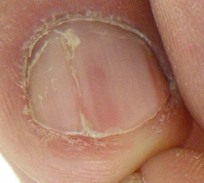
Trachyonychia
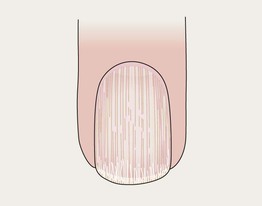
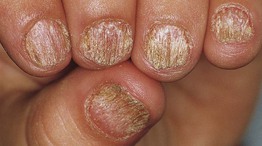
• Rough, ‘sandpaper’ nails, often thin.
• Associated with alopecia areata or lichen planus >> psoriasis.
• May affect most or all nails, especially in children; often termed ‘20-nail dystrophy’.
Lichen Planus
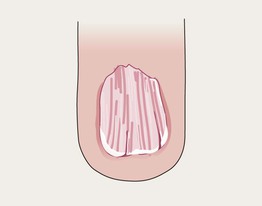
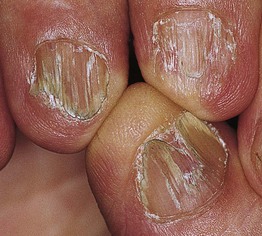
• Nail thinning/atrophy, especially laterally.
• Sometimes dorsal pterygium (see below).
• See Chapter 9.
True Leukonychia
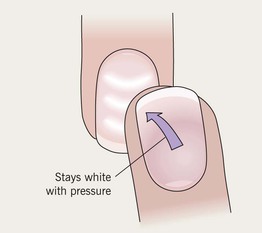
• White discoloration of nail.
• Punctate > linear > diffuse.
• Linear bands may be transverse or longitudinal (see Darier disease).
Apparent Leukonychia
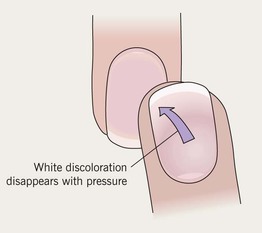
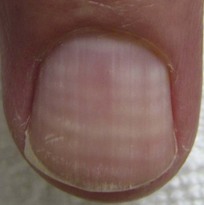
• Nail plate appears white due to alterations in nail bed (e.g. edema).
• Secondary to drugs or systemic disease (e.g. hypoalbuminemia leads to Muehrcke's lines).
• Terry's nails: only distal several millimeters of nail plate unaffected; associated with liver disease.
• Lindsay's nails: proximal half of nail is white and distal nail is red; associated with renal disease.
Beau's Lines
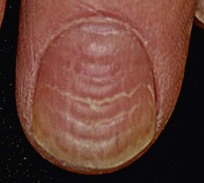
• Transverse depressions in the nail plate.
• Consider systemic insult (e.g. high fever, chemotherapy) if multiple nails involved.
Longitudinal Melanonychia
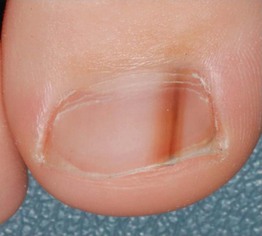
• Longitudinal brown-to-black band.
• Multiple bands common in darker skin types (physiologic); also can be due to trauma (Table 58.3).
• Single band may be a sign of nail melanoma (Table 58.4).
Table 58.4
ABCDEF rule for clinical suspicion of nail melanoma.

Adapted from Levit EK, et al. The ABC rule for clinical detection of subungual melanoma. J. Am. Acad. Dermatol. 2000;42:269–274.
• When melanoma is suspected, the nail matrix must be biopsied (see Fig. 58.1).
Onychorrhexis
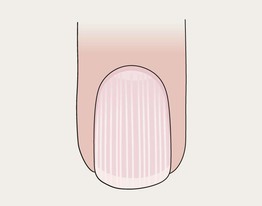
• Thinning and longitudinal ridging.
• May develop fissuring or notching.
Onychoschizia
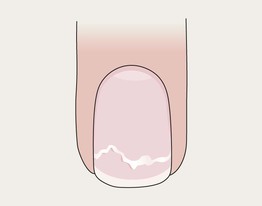
• Lamellar splitting of distal nail into multiple layers.
Pitting in Alopecia Areata
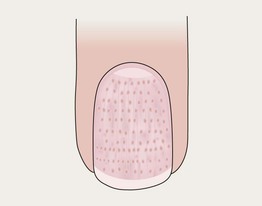
• Punctate depressions in nail plate; geometric or ‘scotch-plaid’ pattern.
• Compared to psoriasis, pits are smaller and more numerous.
Proximal Nail Fold Telangiectasias
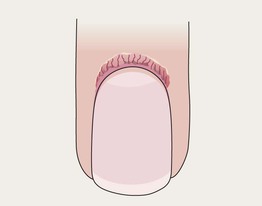
• Capillary prominence ± cuticular hemorrhages.
• Associated with lupus erythematosus and Osler–Weber–Rendu syndrome.
• Also associated with dermatomyositis and scleroderma, with a slightly different appearance (see below).
Proximal Nail Fold Telangiectasias with Capillary Dropout
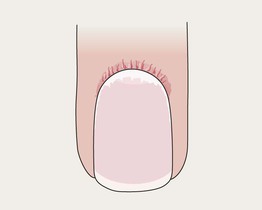
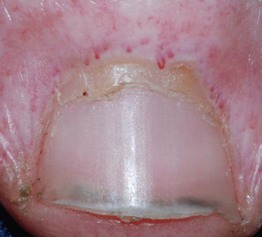
• Capillary dropout alternating with dilated capillary loops.
• Associated with dermatomyositis and scleroderma.
• In dermatomyositis, ragged cuticles may also be present.
• In scleroderma, ventral pterygium (loss of distal subungual space) may be seen.
Clubbing
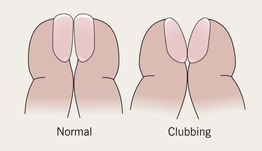
• Bulbous digits with watch-glass nails (> 180° angle between proximal nail fold and nail).
• Most commonly seen in thyroid acropachy and in association with cardiovascular and bronchopulmonary disorders.
Splinter Hemorrhages
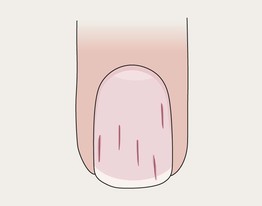
• Thin, longitudinal, dark-red subungual lines.
• Usually secondary to trauma.
Subungual Hematoma
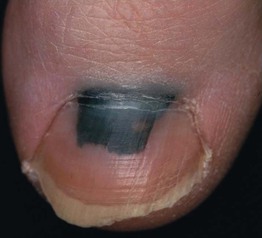
• Purple-red to black color beneath nail plate.
• Moves distally with nail growth.
• Secondary to trauma; if cuticle pushed back, band of normal nail growth may be seen.
Green Nail
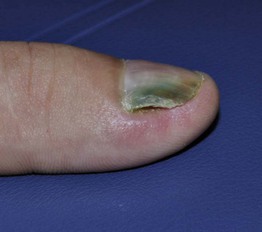
• Blue-green to green-black discoloration secondary to Pseudomonas aeruginosa.
• Usually in association with onycholysis (creates a favorable moist environment).
Paronychia, Acute
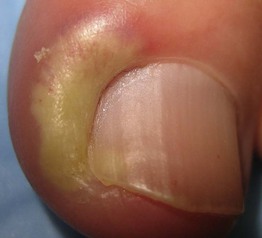
• Swollen nail fold with erythema and pain, sometimes with pustular drainage.
• Caused by bacteria (especially staphylococci).
• Recurrent episodes may be caused by herpes simplex virus infection (herpetic whitlow).
Paronychia, Chronic
• Chronic proximal nail fold inflammation with loss of cuticle (natural sealant).
• Exacerbated by exposure to water and irritants or overaggressive nail grooming.
Median Nail Dystrophy (Tic Deformity)
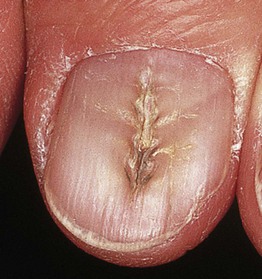
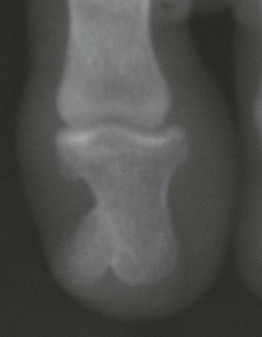
Nail Patella Syndrome
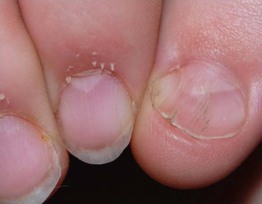
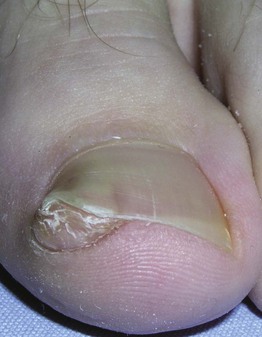
Ingrown Toenails
• Painful inflammation of lateral fold with growth of granulation tissue.
• Can be side effect of drugs.
• Rx: see Table 58.1.
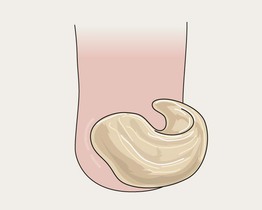
Onychogryphosis
Yellow Nail Syndrome
• Yellow coloration of all or most fingernails > toenails.
• Loss of cuticle, onychomadesis, overcurvature of nail plate.
Tumors
• Various cysts, hyperplasias, and tumors may be seen on the distal digits, including fibromas (Fig. 58.3), myxoid cysts (Fig. 58.4), pyogenic granuloma (Fig. 58.5), glomus tumor (associated with paroxysmal pain) (see Chapter 94), Bowen's disease (Fig. 58.6), keratoacanthoma (symptoms include pain, rapid growth), melanoma (signs include longitudinal melanonychia [Fig. 58.7], Hutchinson's sign = pigmentation of proximal cuticle).
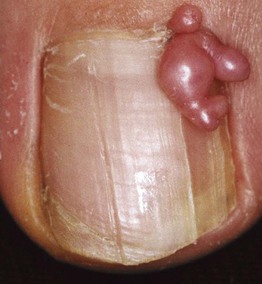
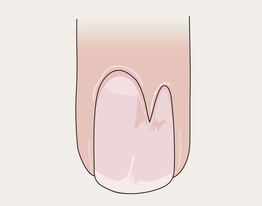
Fig. 58.3 Periungual fibroma producing a longitudinal groove due to matrix compression. Courtesy, Antonella Tosti, MD.
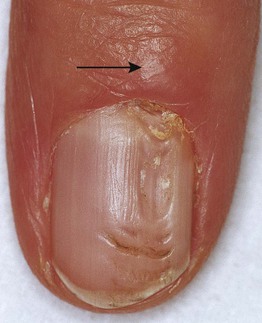
Fig. 58.4 Myxoid cyst. The longitudinal nail groove is a result of the compression of the nail matrix by the cyst (arrow). Courtesy, Antonella Tosti, MD.
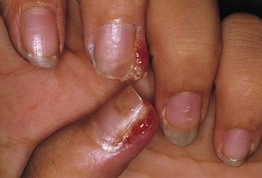
Fig. 58.5 Multiple periungual pyogenic granulomas in a patient taking indinavir. Similar lesions can be seen in patients receiving systemic retinoids or epidermal growth factor receptor inhibitors. Courtesy, Antonella Tosti, MD.
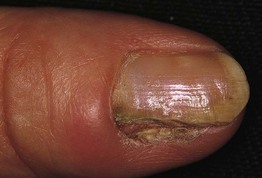
Fig. 58.6 Bowen's disease. The lateral portion of the nail plate is absent. The nail bed shows hyperkeratosis with scaling and fissuring of the epithelium. Courtesy, Antonella Tosti, MD.
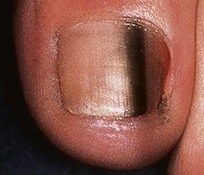
Fig. 58.7 Melanoma in situ of the nail. Darkly pigmented band in the nail bed and matrix. Courtesy, Frank O Nestle, MD.
For further information see Ch. 71. From Dermatology, Third Edition.
Additional details: onycholysis due to psoriasis; onychomadesis after an episode of acute paronychia; apparent leukonychia represents Muehrcke’s lines; multiple Beau’s lines were due to repeated cycles of systemic chemotherapy; proximal nail fold telangiectasias and ragged cuticles due to dermatomyositis.
Additional courtesies: Antonella Tosti, Julie V Schaffer, and Jean L Bolognia.