The Complete Health Assessment
Putting It All Together
http://evolve.elsevier.com/Jarvis/
• Complete Physical Examination Form
• Head-to-Toe Examination of the Adult
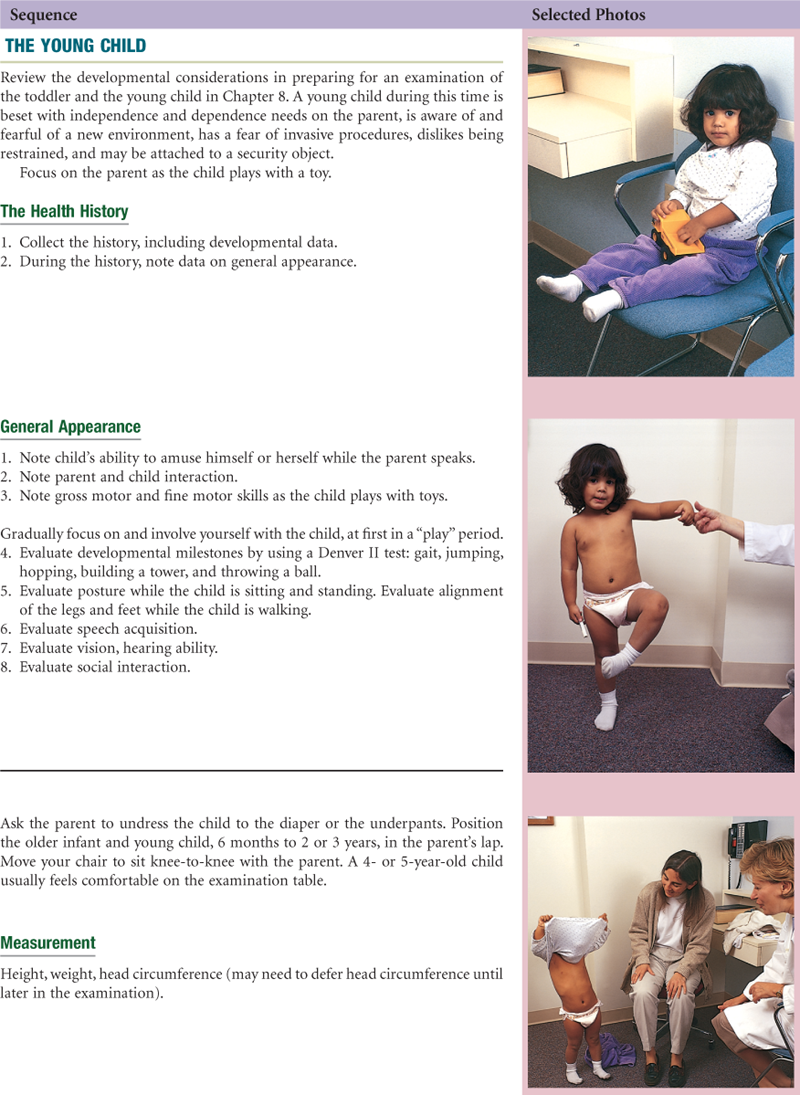
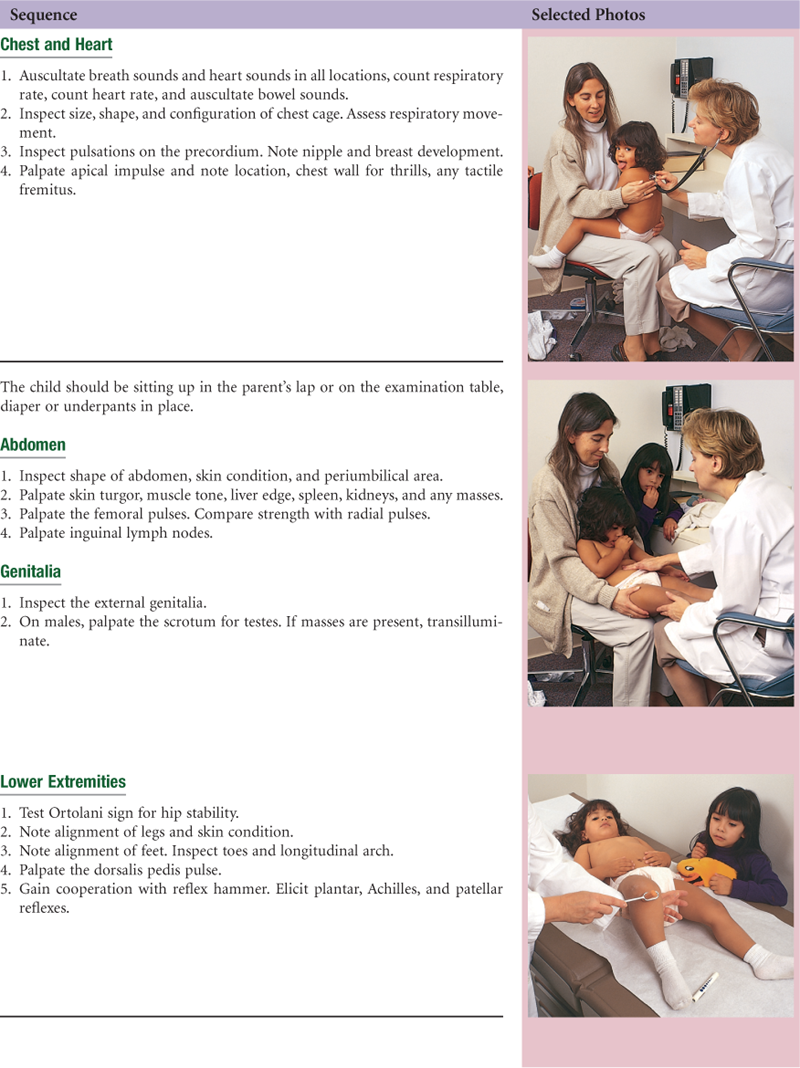
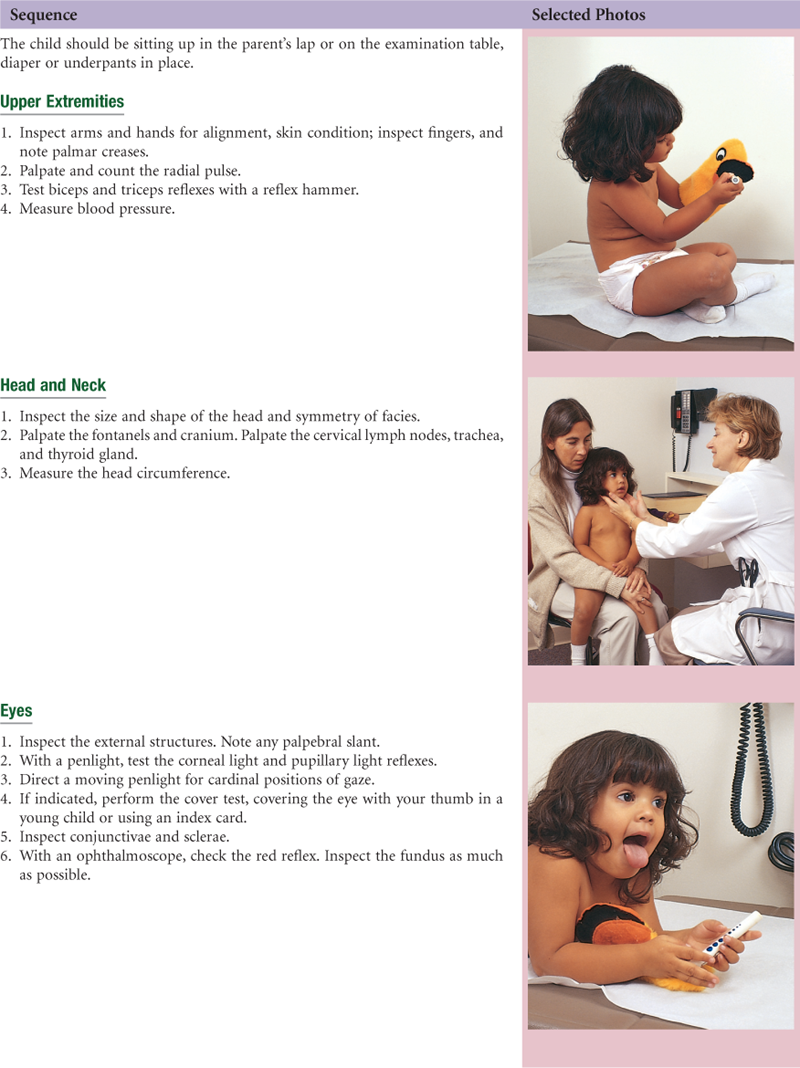
• Head-to-Toe Examination of the Child
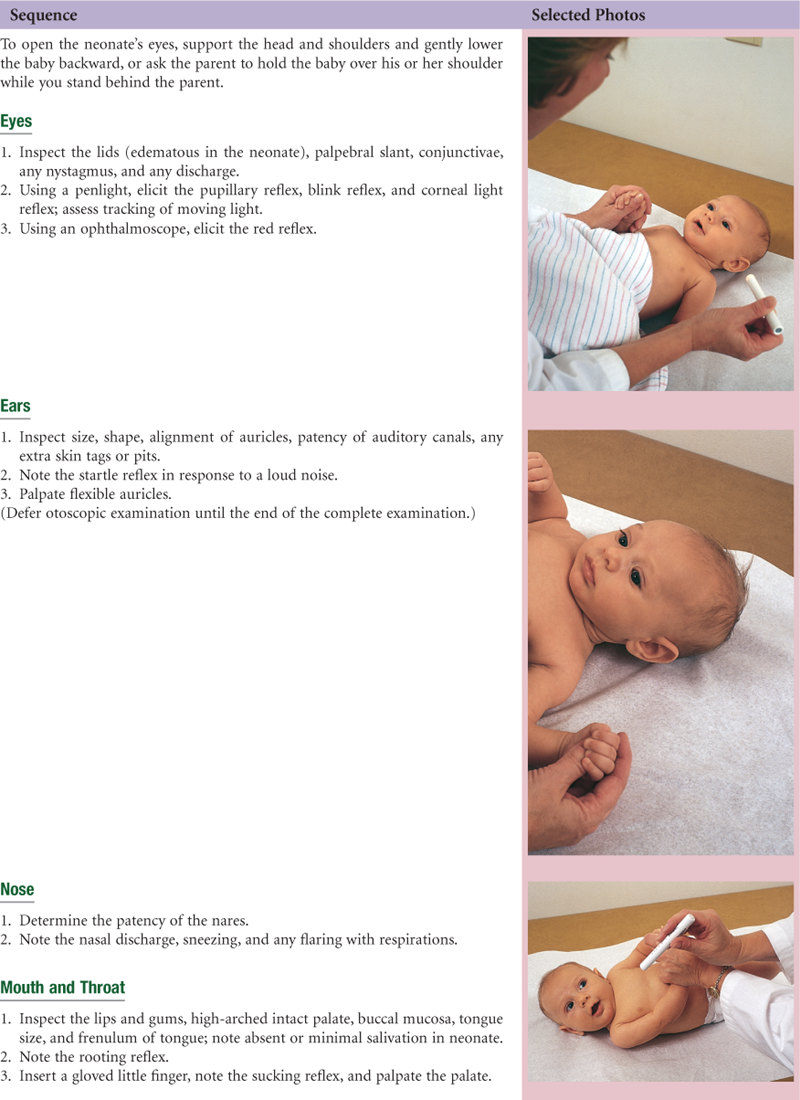
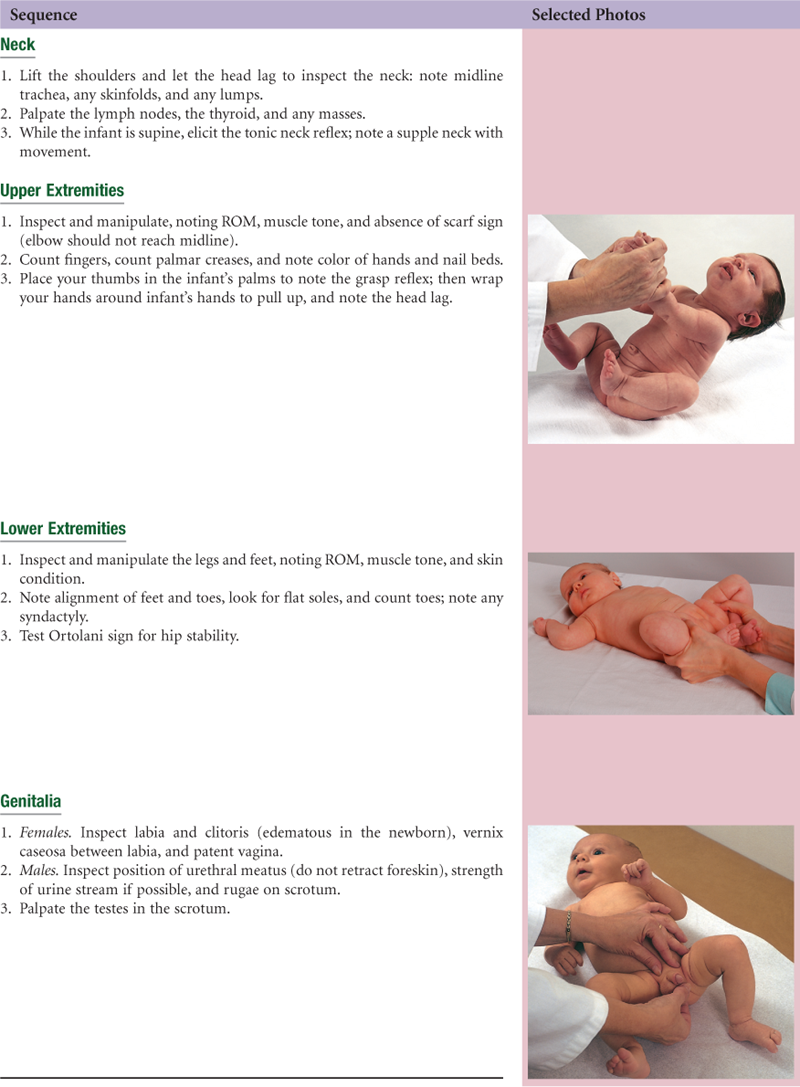
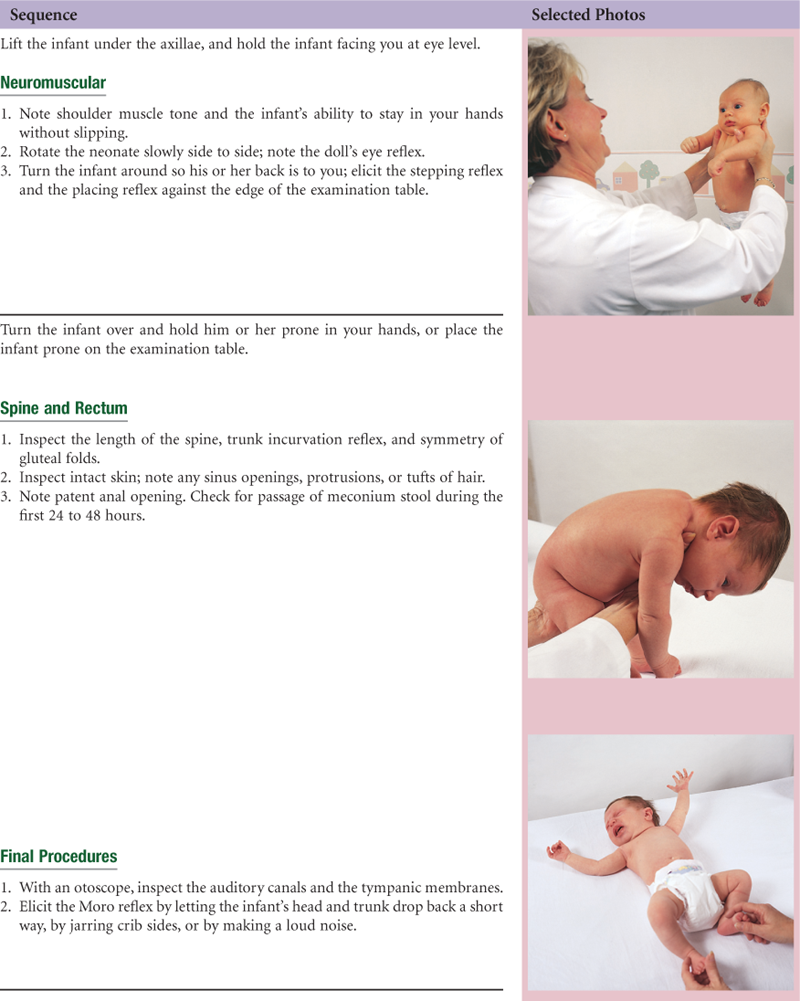
• Head-to-Toe Examination of the Neonate
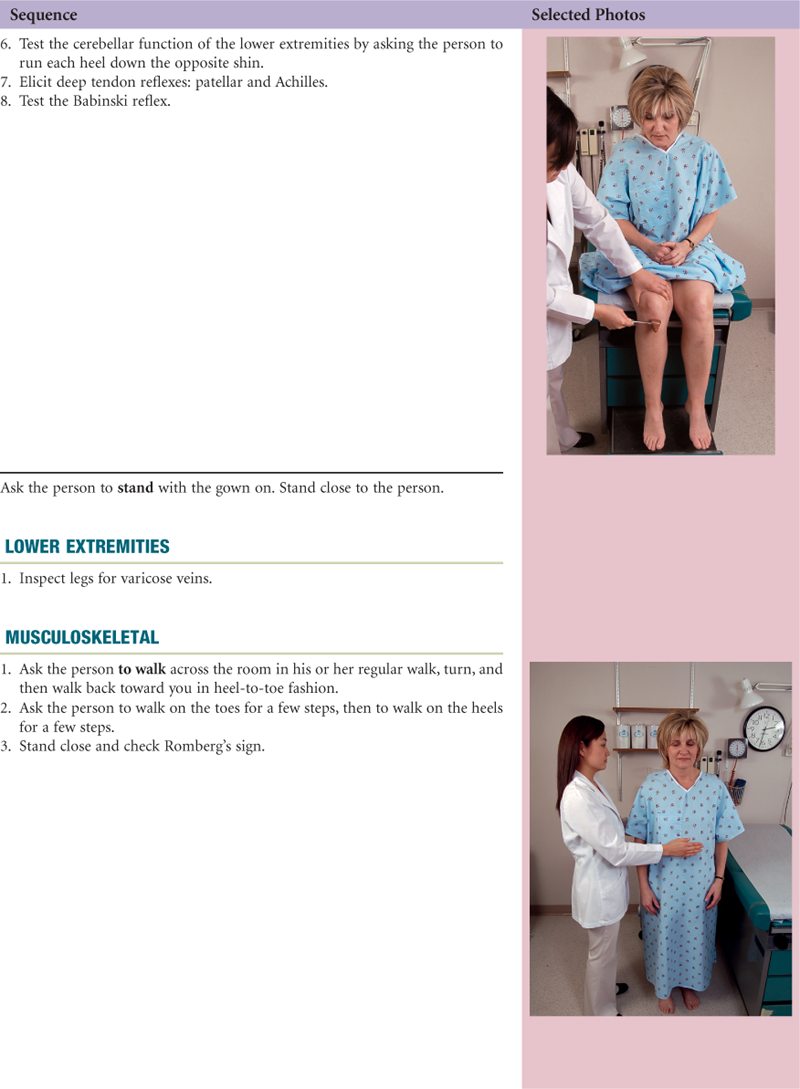
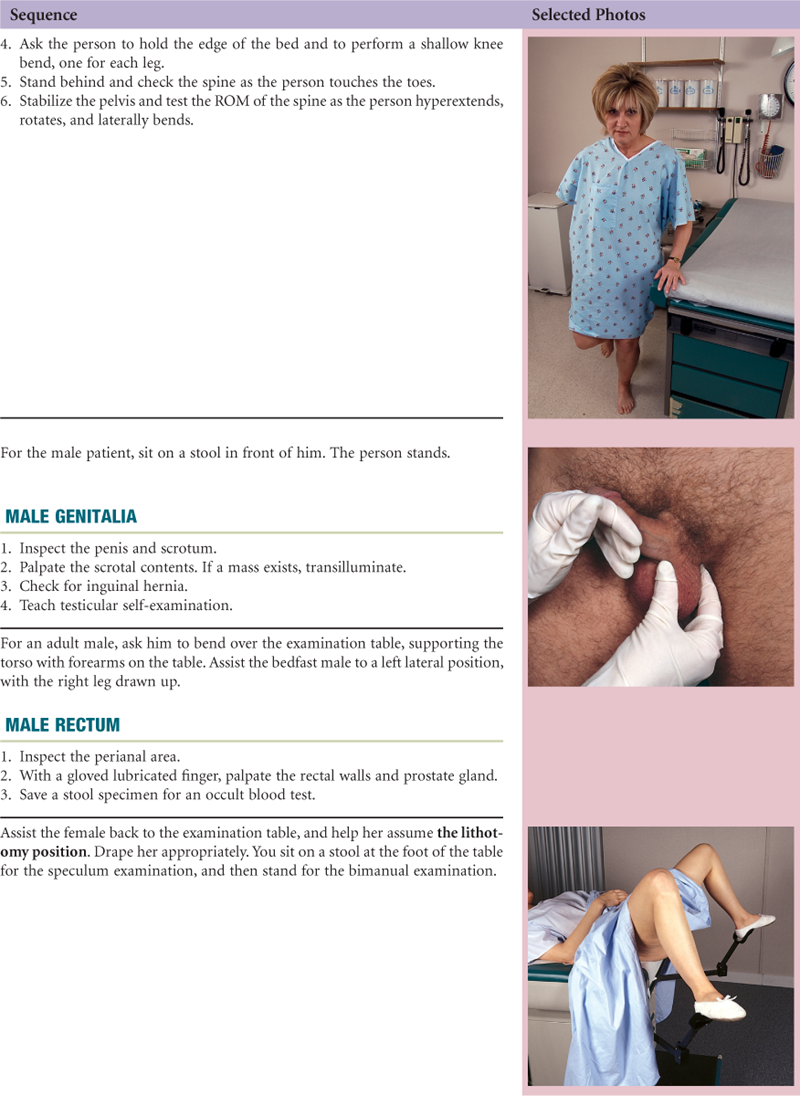
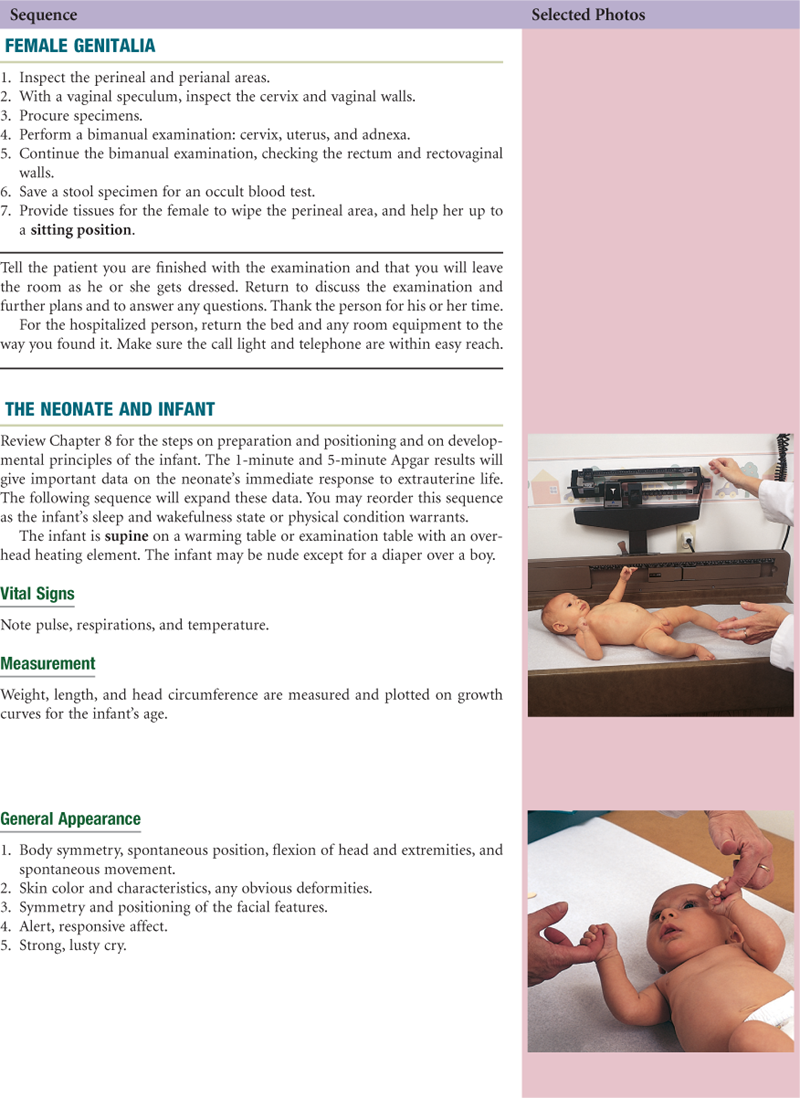
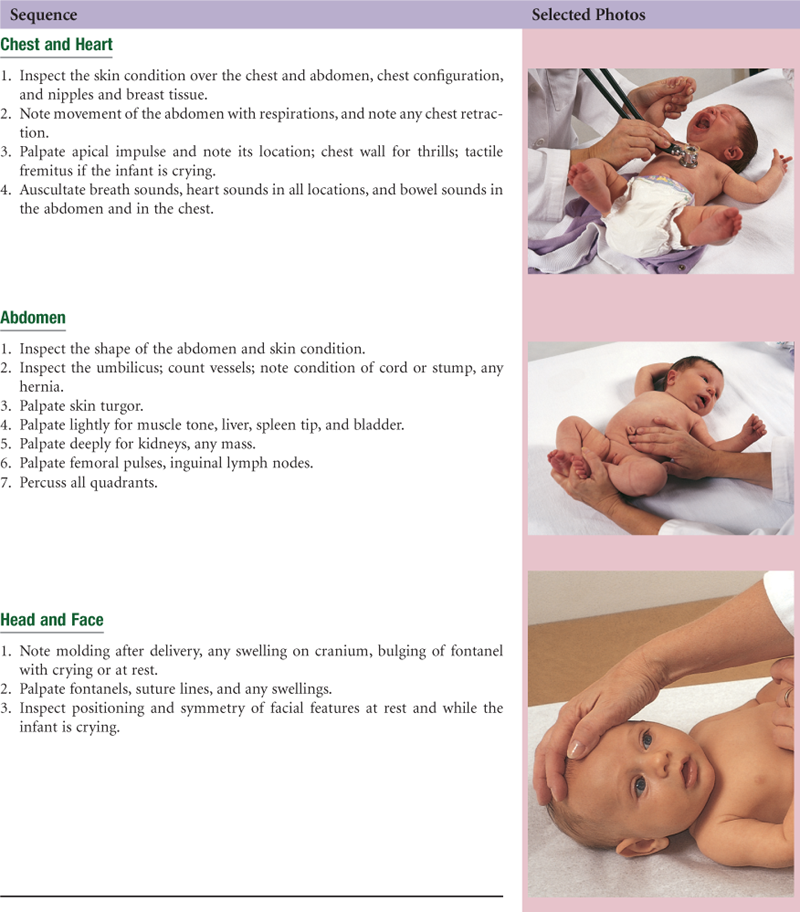
The choreography of the complete history and physical examination is the art of arranging all the separate steps you have learned so far into a fluid whole. Your first examination may seem awkward and contrived; you may have to pause and think of what comes next rather than just gather data. Repeated rehearsals will make the choreography smoother. You will come to the point at which the procedure flows naturally, and even if you forget a step, you will be able to insert it gracefully into the next logical place.
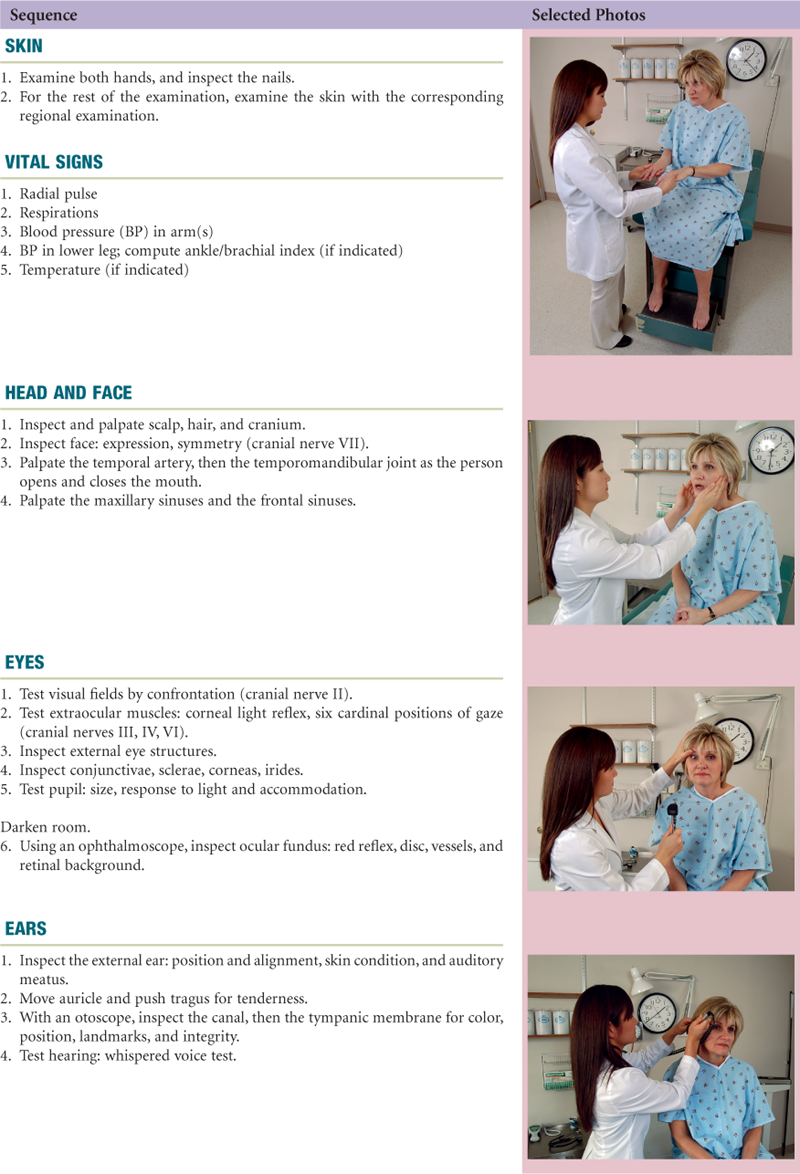
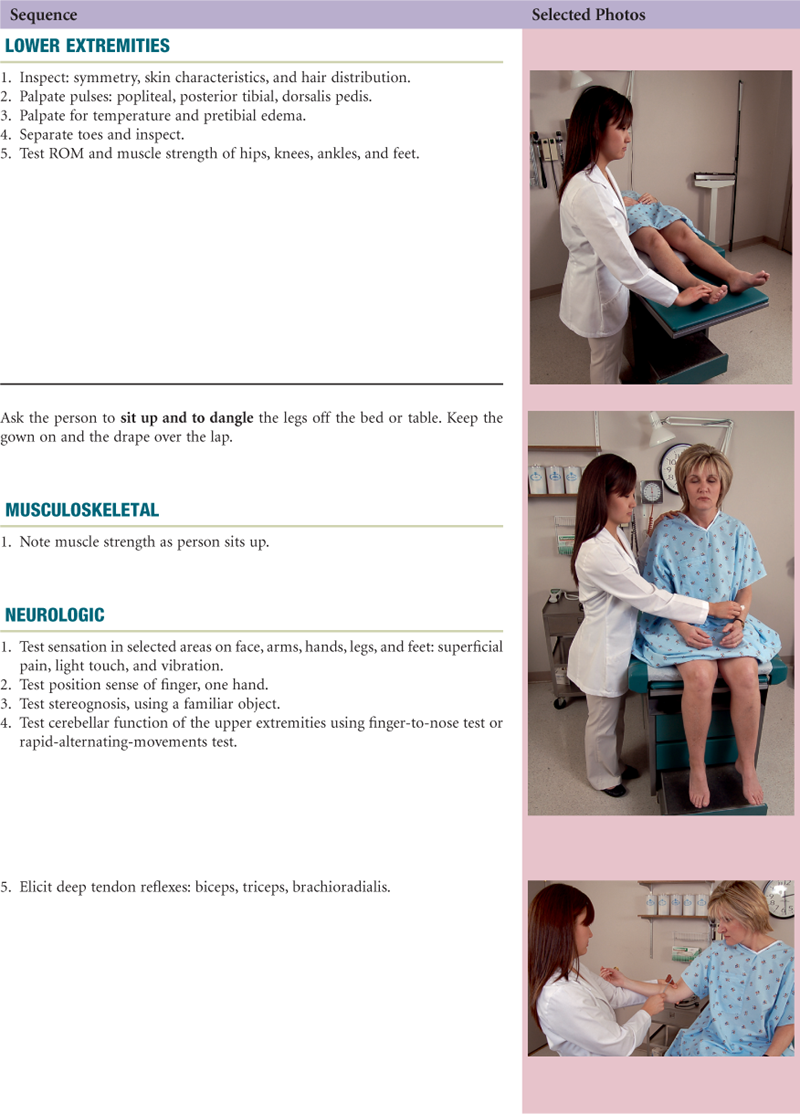
The following examination sequence is one suggested route. It is intended to minimize the number of position changes for the patient and for you. With experience, you may wish to adapt this and arrange a sequence that feels natural for you.
A complete examination is performed at a patient’s first entry in an outpatient setting or initial admission to the hospital. Perform all the steps listed here for a complete examination. With experience, you will learn to strike a balance between which steps you must retain to be thorough and which corners you may safely cut when time is pressing. The steps for the follow-up or shift assessment are described in the next chapter.
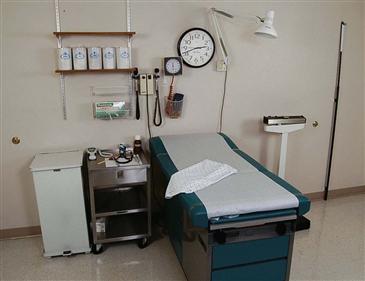
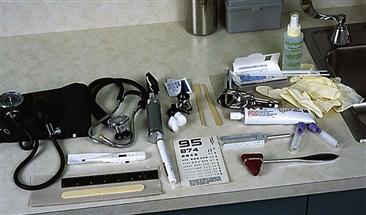
Have all equipment prepared and accessible before the examination. Review Chapter 8 for the list of necessary equipment, the setting, the patient’s emotional state, your demeanor, and the preparation of the patient considering his or her age.





 Documentation and Critical Thinking
Documentation and Critical Thinking
Recording the Data
Record the data from the history and physical examination as soon after the event as possible. Memory fades as the day develops, especially when you are responsible for the care of more than one person.
It is difficult to strike a balance between recording too much data and recording too little. It is important to remember that, from a legal perspective, if it is not documented, it was not done. Data important for the diagnosis and treatment of the person’s health should be recorded, as well as data that contribute to your decision-making process. This includes charting relevant normal or negative findings.
On the other hand, a listing of every assessment parameter described in this text yields an unwieldy, unworkable record. One way to keep your record complete yet succinct is to study your writing style. Use short, clear phrases. Avoid redundant introductory phrases such as “The patient states that….” Avoid redundant descriptions such as “No inguinal, femoral, or umbilical hernias.” Just write, “No hernias.”
Use simple line drawings to describe your findings. You do not need artistic talent; draw a simple sketch of a tympanic membrane, breast, abdomen, or cervix, and mark your findings on it. A clear picture is worth many sentences of words.
Study the following complete history and physical examination for a sample write-up. Note that the subject is the same young woman introduced in Chapter 1 of this text.
Health History
Biographic Data
| Name: Ellen K. | Birth date: 1/18/ |
| Address: 123 Center St. | Birthplace: Springfield |
| Marital Status: Single | Race: White |
Ellen K. is a 23-year-old single white female cashier at a tavern, currently unemployed for 6 months.
Source. Ellen, seems reliable.
Reason for Seeking Care. “I’m coming in for alcohol treatment.”
History of Present Illness. First alcoholic drink, age 16. First intoxication, age 17, drinking one or two times per week, a 6-pack per occasion. Attending high school classes every day, but grades slipping from A−/B+ average to C− average. At age 20, drinking two times per week, six to nine beers per occasion. At age 22, drinking two times per week, a 12-pack per occasion, and occasionally a 6-pack the next day to “help with the hangover.” During this year, experienced blackouts, failed attempts to cut down on drinking, was physically sick the morning after drinking, and was unable to stop drinking once started. Also, incurred three driving-under-the-influence (DUI) legal offenses. Last DUI 1 month PTA; last alcohol use just before DUI, 18 beers that occasion. Abstinent since that time.
Past Health
Childhood Illnesses. Chickenpox at age 6. No measles, mumps, croup, pertussis. No rheumatic fever, scarlet fever, or polio.
Accidents. (1) Auto accident, age 12; father driving, Ellen thrown from car, right leg crushed. Hospitalized at Memorial; surgery for leg pinning to repair multiple compound fractures. (2) Auto accident, age 21; head hit dashboard, no loss of consciousness, treated and released at Memorial Hospital ED. (3) Auto accident, age 23; “car hit median strip,” no injuries, not seen at hospital.
Chronic Illnesses. None.
Hospitalizations. Age 12, Memorial Hospital, surgery to repair right leg as described; Dr. M.J. Carlson, surgeon.
Obstetric History. Gravida 0/Para 0/Abortion 0.
Immunizations. Childhood immunizations up to date. Last tetanus “probably high school.” No TB skin test.
Last Examinations. Yearly pelvic examinations at health department since age 15, told “normal.” High school sports physical as sophomore. Last dental examination as high school junior; last vision test for driver’s license age 16; never had ECG, chest x-ray study.
Allergies. No known allergies.
Current Medications. Birth control pills, low-estrogen type, 1/day, for 5 years. No other prescription or over-the-counter medications.
Family History
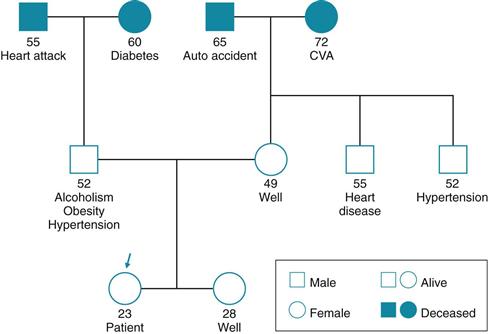
Ellen is second youngest child, parents divorced 8 years, father has chronic alcoholism. See Family genogram below.
Review of Systems
General Health. Reports usual health “OK.” No recent weight change; no fatigue, weakness, fever, sweats.
Skin. No change in skin color, pigmentation, or nevi. No pruritus, rash, lesions. Has bruise now over right eye, struck by boyfriend 1 week PTA. No history skin disease. Hair: no loss, change in texture. Nails: no change. Self-care: Stays in sun “as much as I can.” No use of sunscreen. Goes to tanning beds at hair salon twice/week during winter.
Head. No unusually frequent or severe headaches; no head injury, dizziness, syncope, or vertigo.
Eyes. No difficulty with vision or double vision. No eye pain, inflammation, discharge, lesions. No history glaucoma or cataracts. Wears no corrective lenses.
Ears. No hearing loss or difficulty. No earaches; no infections now or as child; no discharge, tinnitus, or vertigo. Self-care: No exposure to environmental noise; cleans ears with washcloth.
Nose. No discharge; has two or three colds per year; no sinus pain, nasal obstruction, epistaxis, or allergy.
Mouth and Throat. No mouth pain, bleeding gums, toothache, sores or lesions in mouth, dysphagia, hoarseness, or sore throat. Has tonsils. Self-care: Brushes teeth twice/day, no flossing.
Neck. No pain, limitation of motion, lumps, or swollen glands.
Breasts. No pain, lump, nipple discharge, rash, swelling, or trauma. No history breast disease in self, mother, or sister. No surgery. Self-care: Does not do breast self-examination.
Respiratory. No history of lung disease; no chest pain with breathing; no wheezing or shortness of breath. Colds sometimes “go to my chest”; treats with over-the-counter cough medicine and aspirin. Occasional early-morning cough, nonproductive. Smokes cigarettes 2 PPD × 2 years; prior use 1 PPD × 4 years. Never tried to quit. Works in poorly ventilated tavern; “Everybody smokes.”
Cardiovascular. No chest pain, palpitation, cyanosis, fatigue, dyspnea with exertion, orthopnea, paroxysmal nocturnal dyspnea, nocturia, edema. No history of heart murmur, hypertension, coronary artery disease, or anemia.
Peripheral Vascular. No pain, numbness or tingling, swelling in legs. No coldness, discoloration, varicose veins, infections, or ulcers. Legs are unequal in length as sequelae of accident age 12. Self-care: Usual work as cashier involves standing for 8-hour shifts; no support hose.
Gastrointestinal. Appetite good with no recent change. No food intolerance, heartburn, indigestion, pain in abdomen, nausea, or vomiting. No history of ulcers, liver or gallbladder disease, jaundice, appendicitis, or colitis. Bowel movement 1/day, soft, brown; no rectal bleeding or pain. Self-care: No use of vitamins, antacids, laxatives. Diet recall—see Functional Assessment.
Urinary. No dysuria, frequency, urgency, nocturia, hesitancy, or straining. No pain in flank, groin, suprapubic region. Urine color yellow; no history kidney disease.
Genitalia. Menarche age 11. Last menstrual period April 18. Cycle usually q 28 days, duration 4 to 5 days, flow moderate, no dysmenorrhea. No vaginal itching, discharge, sores, or lesions.
Sexual health. In relationship now that includes intercourse. This boyfriend has been her only sexual partner for 2 years; had one other partner before that. Uses birth control pills to prevent pregnancy; partner uses no condoms. Concerned that boyfriend may be having sex with other women but has not confronted him. Not aware of any STI contact. Never been tested for AIDS. History of sexual abuse by father from ages 12 to 16 years; abuse did not include intercourse. Ellen is unwilling to discuss further at this time.
Musculoskeletal. No history of arthritis, gout. No joint pain, stiffness, swelling, deformity, or limitation of motion. No muscle pain or weakness. Bone trauma at age 12; has sequela of unequal leg lengths, right leg shorter, walks with limp. Self-care: No walking or running for sport or exercise “because of leg.” Able to stand as cashier. Uses lift pad in right shoe to equalize leg length.
Neurologic. No history of seizure disorder, stroke, fainting. Has had blackouts with alcohol use. No weakness, tremor, paralysis, problems with coordination, difficulty speaking or swallowing. No numbness or tingling. Not aware of memory problem, nervousness or mood change, depression. Had counseling for sexual abuse in the past. Denies any suicidal ideation or intent during adolescent years or now.
Hematologic. No bleeding problems in skin, no excessive bruising. Not aware of exposure to toxins, never had blood transfusion, never used needles to shoot drugs.
Endocrine. Paternal grandmother with diabetes. No increase in hunger, thirst, or urination; no problems with hot or cold environments; no change in skin or appetite; no nervousness.
Functional Assessment
Self-Concept. Graduated from high school. Trained “on-the-job” as bartender; also worked as cashier in tavern. Unemployed now, on public aid, does not perceive she has enough money for daily living. Lives with older sister. Raised as Presbyterian, believes in God, does not attend church. Believes self to be “honest, dependable.” Believes limitations are “smoking, weight, drinking.”
Activity-Exercise. Typical day: Arises 9 AM, light chores or TV, spends day looking for work, running errands, with friends, bedtime at 11 PM. No sustained physical exercise. Believes self able to perform all ADLs; limp poses no problem in bathing, dressing, cooking, household tasks, mobility, driving a car, or work as cashier. No mobility aids. Hobbies are fishing, boating, snowmobiling; however, currently has no finances to engage in most of these.
Sleep-Rest. Bedtime 11 PM. Sleeps 8 to 9 hours. No sleep aids.
Nutrition. 24-hour recall: Breakfast—none; lunch—bologna sandwich, chips, diet soda; dinner—hamburger, French fries, coffee; snacks—peanuts, pretzels, potato chips, “bar food.” This menu is typical of most days. Eats lunch at home alone. Most dinners at fast-food restaurants or in tavern. Shares household grocery expenses and cooking chores with sister. No food intolerances.
Alcohol. See History of Present Illness. Denies use of street drugs. Cigarettes: Smokes 2 PPD × 2 years; prior use 1 PPD × 4 years. Never tried to quit. Boyfriend smokes cigarettes.
Interpersonal Relationships. Describes family life growing up as chaotic. Father physically abusive toward mother and sexually abusive toward Ellen. Parents divorced because of father’s continual drinking. Few support systems currently. Estranged from mother; “Didn’t believe me about my father.” Father estranged from entire family. Gets along “OK” with sister. Relationship with boyfriend chaotic; has hit her twice in the past. Ellen has never pressed legal charges. No close women friends. Most friends are “drinking buddies” at tavern.
Coping and Stress Management. Believes housing adequate, adequate heat and utilities, and neighborhood safe. Believes home has no safety hazards. Does not use seat belts. No travel outside 60 miles of hometown.
Identifies current stresses to be drinking, legal problems with DUIs, unemployment, financial worries. Considers her drinking to be problematic.
Perception of Health
Identifies alcohol as a health problem for herself; feels motivated for treatment. Never been interested in physical health and own body before; “Now I think it’s time I learned.” Expects health care providers to “Help me with my drinking. I don’t know beyond that.” Expects to stay at this agency for 6 weeks; “Then, I don’t know what.”
Physical Examination
Measurement
Height: 163 cm (5′4″); Weight: 68.6 kg (151 lb); Waist circumference: 32 inches
BP: 142/100 mm Hg right arm, sitting
140/96 mm Hg right arm, lying
138/98 mm Hg left arm, lying
Temp: 37° C; Pulse: 76 bpm, regular; Respirations: 16 per min, unlabored
General Survey. Ellen K. is a 23-year-old white female, not currently under the influence of alcohol or other drugs, who articulates clearly, ambulates without difficulty, and is in no distress.
Head-To-Toe Examination
Skin. Uniformly tan-pink in color, warm, dry, intact; turgor good. No lesions, birthmarks, edema. Resolving 2-cm yellow-green hematoma present over right eye; no swelling; ocular structures not involved. Hair: normal distribution and texture, no pest inhabitants. Nails: no clubbing, biting, or discolorations. Nail beds: pink and firm with prompt capillary refill.
Head. Normocephalic, no lesions, lumps, scaling, parasites, or tenderness. Face: symmetric, no weakness, no involuntary movements.
Eyes. Acuity by Snellen chart: right eye 20/20; left eye 20/20−1. Visual fields full by confrontation. EOMs intact, no nystagmus. No ptosis, lid lag, discharge, or crusting. Corneal light reflex symmetric; no strabismus. Conjunctivae clear. Sclerae white; no lesion or redness. Pupils: 3 mm resting, 2 mm constricted, and = bilaterally. PERRLA.
Fundi: discs flat with sharp margins. Vessels present in all quadrants without crossing defects. Background has even color, no hemorrhage or exudates.
Ears. Pinna: no mass, lesions, scaling, discharge, or tenderness to palpation. Canals clear. Tympanic membrane: pearly gray, landmarks intact, no perforation. Whispered words heard bilaterally.
Nose. No deformities or tenderness to palpation. Nares patent. Mucosa pink, no lesions. Septum midline, no perforation. No sinus tenderness.
Mouth. Mucosa and gingivae pink, no lesions or bleeding. Right lower 1st molar missing, multiple dark spots on most teeth, gums receding on lower incisors. Tongue symmetric, protrudes midline, no tremor. Pharynx pink, no exudate. Uvula rises midline on phonation. Tonsils 1+. Gag reflex present.
Neck. Neck supple with full ROM. Symmetric; no masses, tenderness, lymphadenopathy. Trachea midline. Thyroid nonpalpable, not tender. Jugular veins flat @ 45 degrees. Carotid arteries 2+ and = bilaterally; no bruits.
Spine and Back. Normal spinal profile; no scoliosis. No tenderness over spines; no CVA tenderness.
Thorax and Lungs. AP < transverse diameter. Chest expansion symmetric. Tactile fremitus equal bilaterally. Lung fields resonant. Diaphragmatic excursion 4 cm and = bilaterally. Breath sounds diminished. Expiratory wheeze in posterior chest at both bases, scattered rhonchi in posterior chest at both bases, do not clear with coughing.
Breasts. Symmetric; no retraction, discharge, or lesions. Contour and consistency firm and homogeneous. No masses or tenderness, no lymphadenopathy.
Heart. Precordium: no abnormal pulsations, no heaves. Apical impulse at 5th ICS in left MCL, no thrills. S1–S2 are not diminished or accentuated, no S3 or S4. Systolic murmur, grade ii/vi, loudest at left lower sternal border, no radiation, present supine and sitting.
Abdomen. Flat, symmetric. Skin smooth with no lesions, scars, or striae. Bowel sounds present, no bruits. Tympany predominates in all quadrants. Liver span 7 cm in right MCL. Abdomen soft, no organomegaly, no masses or tenderness, no inguinal lymphadenopathy.
Extremities. Color tan-pink; no redness, cyanosis, lesions other than surgical scar. Scar right lower leg, anterior, 28 cm × 2 cm wide, well healed. No edema, varicosities. No calf tenderness. All peripheral pulses present, 2+ and = bilaterally. Asymmetric leg length—right leg 3 cm shorter than left.
Musculoskeletal. Temporomandibular joint: no slipping or crepitation. Neck: full ROM, no pain. Vertebral column: no tenderness, no deformity or curvature; full extension, lateral bending, rotation. Arms symmetric, legs measure as described, extremities have full ROM, no pain or crepitation. Muscle strength: able to maintain flexion against resistance and without tenderness.
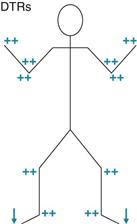
Neurologic. Mental status: Appearance, behavior, speech appropriate. Alert and oriented to person, place, time. Thought coherent. Remote and recent memories intact. Cranial nerves II through XII intact. Sensory: Pinprick, light touch, vibration intact. Stereognosis: Able to identify key. Motor: No atrophy, weakness, or tremors. Gait: Has limp, able to tandem walk with shoes on. Negative Romberg’s sign. Cerebellar: Finger-to-nose smoothly intact. DTRs: See stick gram.
Genitalia. External genitalia: no lesion, discharge. Internal genitalia: vaginal walls pink, no lesion. Cervix: pink, nulliparous os, no lesions, small amount nonodorous clear discharge. Specimens for Pap test, GC/chlamydia, trichomoniasis, moniliasis obtained. Swabbing mucosa with acetic acid shows no acetowhitening.
Bimanual: no pain on moving cervix; uterus midline; no enlargement, masses, or tenderness. Adnexa—ovaries not enlarged, no tenderness. Anus—no hemorrhoids, fissures, or lesions. Rectal wall intact, no masses or tenderness. Stool soft, brown; hematest negative.
Assessment
Alcohol dependence, severe, with physiologic dependence
Nicotine dependence with physiologic dependence
Hypertension
Systolic heart murmur
Ineffective airway clearance R/T tracheobronchial secretions and obstruction
Right orbital contusion (resolving)
Risk for trauma
Self-care deficit: oral hygiene R/T lack of motivation
Deficient knowledge about alcoholism disease process, treatment options, support systems R/T lack of exposure
Deficient knowledge about balanced diet R/T lack of exposure and substance abuse
Dysfunctional family processes: alcoholism
Chronic low self-esteem R/T effects of alcoholism, sexual abuse, physical abuse