Chapter 616 Abnormalities of the Lids
Ptosis
In blepharoptosis, the upper eyelid droops below its normal level. Congenital ptosis is usually a result of a localized dystrophy of the levator muscle in which the striated muscle fibers are replaced with fibrous tissue. The condition may be unilateral or bilateral and can be transmitted as a dominant trait.
Parents often comment that the eye looks smaller because of the drooping eyelid. The lid crease is decreased or absent where the levator muscle would normally insert below the skin surface. Because the levator is replaced by fibrous tissue, the lid does not move downward fully in downgaze (lid lag). If the ptosis is severe, affected children often attempt to raise the lid by lifting their brow or adapting a chin-up head posture to maintain binocular vision. Marcus Gunn jaw-winking ptosis accounts for 5% of ptosis in children. In this syndrome, an abnormal synkinesis exists between the 5th and 3rd cranial nerves; this causes the eyelid to elevate with movement of the jaw. The wink is produced by chewing or sucking and may be more noticeable than the ptosis itself.
Although ptosis in children is often an isolated finding, it may occur in association with other ocular or systemic disorders. Systemic disorders include myasthenia gravis, muscular dystrophy, and botulism. Ocular disorders include mechanical ptosis secondary to lid tumors, blepharophimosis syndrome, congenital fibrosis syndrome, combined levator/superior rectus maldevelopment, and congenital or acquired 3rd nerve palsy. A small degree of ptosis is seen in Horner syndrome (Chapter 614). A complete ophthalmic and systemic examination is therefore important in the evaluation of a child with ptosis.
Amblyopia may occur in children with ptosis. The amblyopia may be secondary to the lid’s covering the visual axis (deprivation) or induced astigmatism (anisometropia). When amblyopia occurs, it should generally be treated before treating the ptosis.
Treatment of ptosis in a child is indicated for elimination of an abnormal head posture, improvement in the visual field, prevention of amblyopia, and restoration of a normal eyelid appearance. The timing of surgery depends on the degree of ptosis, its cosmetic and functional severity, the presence or absence of compensatory posturing, the wishes of the parents, and the discretion of the surgeon. Surgical treatment is determined by the amount of levator function that is present. A levator resection may be used in children with moderate to good function. In patients with poor or absent function, a frontalis suspension procedure may be necessary. This technique requires that a suspension material be placed between the frontalis muscle and the tarsus of the eyelid. It allows patients to use their brow and frontalis muscle more effectively to raise their eyelid. Amblyopia remains a concern even after surgical correction and should be monitored closely.
Epicanthal Folds
These vertical or oblique folds of skin extend on either side of the bridge of the nose from the brow or lid area, covering the inner canthal region. They are present to some degree in most young children and become less apparent with age. The folds may be sufficiently broad to cover the medial aspect of the eye, making the eyes appear crossed (pseudoesotropia). Epicanthal folds are a common feature of many syndromes, including chromosomal aberrations (trisomies) and disorders of single genes.
Lagophthalmos
This is a condition in which complete closure of the lids over the globe is difficult or impossible. It may be paralytic because of a facial palsy involving the orbicularis muscle, or spastic, as in thyrotoxicosis. It may be structural when retraction or shortening of the lids results from scarring or atrophy consequent to injury (burns) or disease. For example, children with various craniosynostosis syndromes can have problematic lagophthalmos. Infants with collodion membrane may have temporary lagophthalmos caused by the restrictive effect of the membrane on the lids. Lagophthalmos may accompany proptosis or buphthalmos (enlarged cornea due to elevated intraocular pressure) when the lids, although normal, cannot effectively cover the enlarged or protuberant eye. A degree of physiologic lagophthalmos may occur normally during sleep, but functional lagophthalmos in an unconscious or debilitated patient can be a problem.
In patients with lagophthalmos, exposure of the eye may lead to drying, infection, corneal ulceration, or perforation of the cornea; the result may be loss of vision, even loss of the eye. In lagophthalmos, protection of the eye by artificial tear preparations, ophthalmic ointment, or moisture chambers is essential. Gauze pads are to be avoided because the gauze may abrade the cornea. In some cases, surgical closure of the lids (tarsorrhaphy) may be necessary for long-term protection of the eye.
Lid Retractions
Pathologic retraction of the lid may be myogenic or neurogenic. Myogenic retraction of the upper lid occurs in thyrotoxicosis, in which it is associated with 3 classic signs: a staring appearance (Dalrymple sign), infrequent blinking (Stellwag sign), and lag of the upper lid on downward gaze (von Graefe sign).
Neurogenic retraction of the lids may occur in conditions affecting the anterior mesencephalon. Lid retraction is a feature of the syndrome of the sylvian aqueduct. In children, it is commonly a sign of hydrocephalus. It may occur with meningitis. Paradoxical retraction of the lid is seen in the Marcus Gunn jaw-winking syndrome. It may also be seen with attempted eye movement after recovery from a 3rd nerve palsy, if aberrant regeneration of the oculomotor nerve fibers has occurred.
Simple staring and the physiologic or reflexive lid retraction (“eye popping”), in contrast to pathologic lid retractions, occur in infants in response to a sudden reduction in illumination or as a startle reaction.
Ectropion, Entropion, and Epiblepharon
Ectropion is eversion of the lid margin; it may lead to overflow of tears (epiphora) and subsequent maceration of the skin of the lid, inflammation of exposed conjunctiva, or superficial exposure keratopathy. Common causes are scarring consequent to inflammation, burns, or trauma, or weakness of the orbicularis muscle as a result of facial palsy; these forms may be corrected surgically. Protection of the cornea is essential. Ectropion is also seen in certain children who have faulty development of the lateral canthal ligament; this may occur in Down syndrome.
Entropion is inversion of the lid margin, which may cause discomfort and corneal damage because of the inward turning of the lashes (trichiasis). A principal cause is scarring secondary to inflammation such as occurs in trachoma or as a sequela of Stevens-Johnson syndrome. There is also a rare congenital form. Surgical correction is effective in many cases.
Epiblepharon is commonly seen in childhood and may be confused with entropion. In epiblepharon, a roll of skin beneath the lower eyelid lashes causes the lashes to be directed vertically and to touch the cornea (Fig. 616-1). Unlike entropion, the eyelid margin itself is not rotated toward the cornea. Epiblepharon usually resolves spontaneously. If corneal scarring begins to occur, surgical correction may be necessary.
Blepharospasm
This spastic or repetitive closure of the lids may be caused by irritative disease of the cornea, conjunctiva, or facial nerve; fatigue or uncorrected refractive error; or common tic. Thorough ophthalmic examination for pathologic causes, such as trichiasis, keratitis, conjunctivitis, or foreign body, is indicated. Local injection of botulinum toxin may give relief but frequently must be repeated.
Blepharitis
This inflammation of the lid margins is characterized by erythema and crusting or scaling; the usual symptoms are irritation, burning, and itching. The condition is commonly bilateral and chronic or recurrent. The two main types are staphylococcal and seborrheic. In staphylococcal blepharitis, ulceration of the lid margin is common, the lashes tend to fall out, and conjunctivitis and superficial keratitis are often associated. In seborrheic blepharitis, the scales tend to be greasy, the lid margins are less red, and ulceration usually does not occur. The blepharitis is often of mixed type.
Thorough daily cleansing of the lid margins with a cloth or moistened cotton applicator to remove scales and crusts is important in the treatment of both forms. Staphylococcal blepharitis is treated with an antistaphylococcal antibiotic applied directly to the lid margins. When a child also has seborrhea, concurrent treatment of the scalp is important.
Pediculosis of the eyelashes may produce a clinical picture of blepharitis. The lice can be smothered with ophthalmic-grade petrolatum ointment applied to the lid margin and lashes. Nits should be mechanically removed from the lashes. It should be remembered that pediculosis represents a sexually transmitted disease.
Hordeolum
Infection of the glands of the lid may be acute or subacute; tender focal swelling and redness are noted. The usual agent is Staphylococcus aureus. When the meibomian glands are involved, the lesion is referred to as an internal hordeolum; the abscess tends to be large and may point through either the skin or the conjunctival surface. When the infection involves the glands of Zeis or Moll, the abscess tends to be smaller and more superficial and points at the lid margin; it is then referred to as an external hordeolum or stye.
Treatment is frequent warm compresses and, if necessary, surgical incision and drainage. In addition, topical antibiotic preparations are often used. Untreated, the infection may progress to cellulitis of the lid or orbit, requiring the use of systemic antibiotics.
Chalazion
A chalazion is a granulomatous inflammation of a meibomian gland characterized by a firm, nontender nodule in the upper or lower lid. This lesion tends to be chronic and differs from internal hordeolum in the absence of acute inflammatory signs. Although many chalazia subside spontaneously, excision may be necessary if they become large enough to distort vision (by inducing astigmatism by exerting pressure on the globe) or to be a cosmetic blemish. Patients who experience frequent chalazia formation, or those who have significant corneal changes secondary to the underlying blepharitis, may benefit from systemic, low dose erythromycin or azithromycin treatment.
Coloboma of the Eyelid
This cleftlike deformity may vary from a small indentation or notch of the free margin of the lid to a large defect involving almost the entire lid. If the gap is extensive, ulceration and corneal opacities may result from exposure. Early surgical correction of the lid defect is recommended. Other deformities frequently associated with lid colobomas include dermoid cysts or dermolipomas on the globe; they often occur in a position corresponding to the site of the lid defect. Lid colobomas may also be associated with extensive facial malformation, as in mandibulofacial dysostosis (Franceschetti or Treacher Collins syndrome).
Tumors of the Lid
A number of lid tumors arise from surface structures (the epithelium and sebaceous glands). Nevi may appear in early childhood; most are junctional. Compound nevi tend to develop in the prepubertal years and dermal nevi at puberty. Malignant epithelial tumors (basal cell carcinoma, squamous cell carcinoma) are rare in children, but the basal cell nevus syndrome and the malignant lesions of xeroderma pigmentosum and of Rothmund-Thomson syndrome may develop in childhood.
Other lid tumors arise from deeper structures (the neural, vascular, and connective tissues). Capillary hemangiomas are especially common in children (Fig. 616-2). Many tend to regress spontaneously, although they may show alarmingly rapid growth in infancy. In many cases, the best management of such hemangiomas is patient observation, allowing spontaneous regression to occur (Chapter 642). In the case of a rapidly expanding lesion, which may cause amblyopia by obstructing the visual axis or inducing astigmatism, corticosteroid, interferon, or surgical treatment should be considered. Recently, systemic propranalol has shown benefit as well. Nevus flammeus (port-wine stain), a noninvoluting hemangioma, occurs as an isolated lesion or in association with other signs of Sturge-Weber syndrome. Affected patients should be monitored for the development of glaucoma. Lymphangiomas of the lid appear as firm masses at or soon after birth and tend to enlarge slowly during the growing years. Associated conjunctival involvement, appearing as a clear, cystic, sinuous conjunctival mass, may provide a clue to the diagnosis. In some cases, there is also orbital involvement. The treatment is surgical excision.
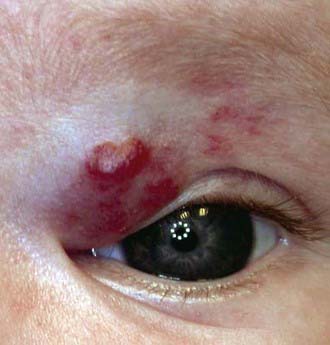
Figure 616-2 Capillary hemangioma of the eyelid.
(Courtesy of Amy Nopper, MD, and Brandon Newell, MD.)
Plexiform neuromas of the lids occur in children with neurofibromatosis, often with ptosis as the first sign. The lid may take on an S-shaped configuration. The lids may also be involved by other tumors, such as retinoblastoma, neuroblastoma, and rhabdomyosarcoma of the orbit; these conditions are discussed elsewhere.
Dray JP, Leibovitch I. Congenital ptosis and amblyopia: a retrospective study of 130 cases. J Pediatr Ophthalmol Strabismus. 2002;39:222-225.
Drolet BA, Esterly NB, Frieden IJ. Hemangiomas in children. N Engl J Med. 1999;341:173-181.
Gusek-Schneider GC, Martus P. Stimulus deprivation amblyopia in human congenital ptosis: a study of 100 patients. Strabismus. 2000;8:261-270.
Meisler DM, Raizman MB, Traboulsi EI. Oral erythromycin treatment for childhood blepharokeratitis. J AAPOS. 2000;4:379-380.
Plager DA, Snyder SK. Resolution of astigmatism after surgical resection of capillary hemangiomas in infants. Ophthalmology. 1997;104:1102-1106.
Sterker I, Grafe G. Periocular hemangiomas in childhood—functional and esthetic results. Strabismus. 2004;12:103-110.