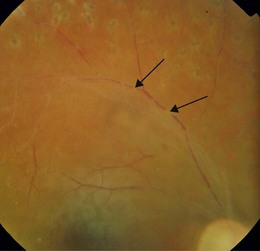
Confirming death
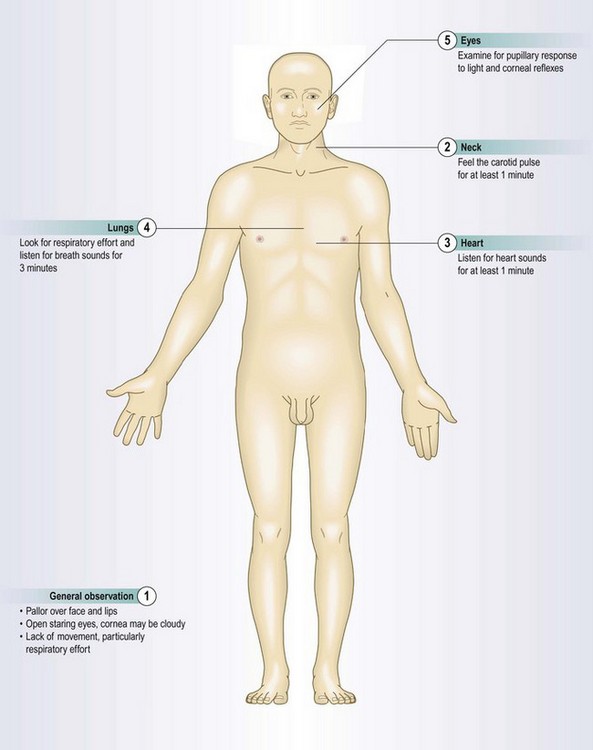
Examination to confirm death
Definition
In the UK there is no legal definition of death. It is the clinician’s responsibility to declare when a patient has died. Death is defined by the UK Academy of Medical Royal Colleges as: ‘the irreversible loss of the capacity for consciousness, combined with irreversible loss of the capacity to breathe’. For practical purposes, death has occurred if there is absence of spontaneous cardiac function, respiratory effort and central nervous system activity.
Death used to be synonymous with the sudden and unexpected loss of spontaneous cardiac activity and respiration (cardiopulmonary arrest). Appropriate and prompt treatment can, however, successfully resuscitate some people in this category (Ch. 19).
Timing
The exact timing of death is rarely predictable, but is sometimes anticipated and accepted, e.g. in a patient with advanced metastatic cancer. Some patients with very severe chronic or terminal illness do not wish to have resuscitative efforts performed. In some countries, including the UK, the applicability of a ‘do not attempt resuscitation’ (DNAR) directive may be discussed with the patient and close relatives. The outcome of this discussion should be clearly recorded in the notes, made known to relevant medical and nursing staff and reviewed regularly. The presence of a DNAR order does not in any way imply withdrawal of treatment: it should focus attention on the general care of the patient, including adequate analgesia.
Confirmation
Confirming death has major medicolegal implications and obligations. Your approach and manner should always be professional. Although death may appear obvious, carefully and systematically examine the body. Misdiagnosis is especially likely in situations where vital functions and general metabolism are greatly reduced (Box 20.1).
Investigations
In certain situations, additional investigations may be available and confirmatory: for example, an electrocardiograph monitor trace showing asystole, absence of pulsatile flow from an intra-arterial line, or of contractile motion on echocardiography.
Brainstem death
Modern resuscitative devices and techniques can maintain the function of the heart, lungs and visceral organs, even when brainstem function has stopped. Patients receiving mechanical ventilation require additional tests to confirm brainstem death, which should be carried out by two experienced doctors on two occasions 24 hours apart. Prior to such testing establish that the patient has irreversible brain injury of known cause producing deep coma and apnoea requiring artificial ventilation and that excludes potentially reversible causes (Box 20.1).
What to do after you have confirmed death
Record the death in the patient’s medical notes, with the date and time at which you pronounced life extinct. If possible, state what you believe to be the cause of death. Sign the notes legibly; include your designation.
Inform the close family or next of kin about the death as soon as possible. Wherever possible, do this in person rather than by telephone. Breaking bad news is difficult: always speak to the bereaved in a quiet and private environment, avoid interruption (ask someone to take your telephone and pager) and, wherever possible, involve a nurse or counsellor to act as a witness and provide future support if required. Relatives need time to understand and accept the situation. Use great care and sensitivity to try to support them. Inform the family doctor as soon as is reasonable. The followers of some faiths have procedures and rituals that should be followed after a death and which require the involvement of an appropriate religious leader.
If appropriate, ask about the deceased’s wishes for organ donation. Some people carry an organ donor card stating their wishes. In the UK there is an organ donor register, which allows people to indicate their wishes for organ donation after death. You can check this register to confirm the deceased’s wishes.
Where the circumstances of death are unexpected or where death has occurred in suspicious or prescribed circumstances, the legal authorities must be informed. Examples include suspected overdose, deaths related to alcohol or after surgery or if there is to be a post mortem examination. Do not give a death certificate until the coroner, procurator fiscal or other authority has agreed that you should do so (Box 20.3).