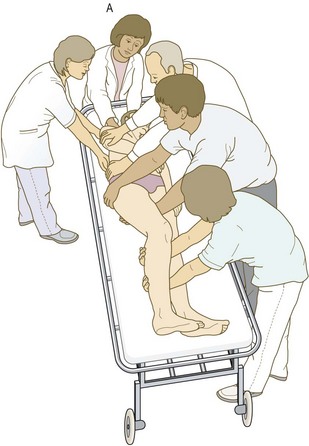
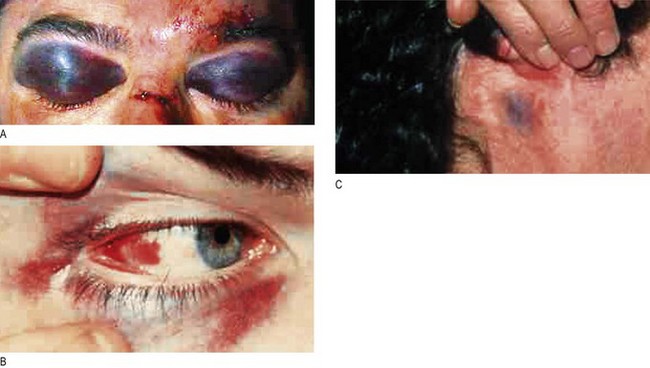
The critically ill
Examination of the critically ill patient
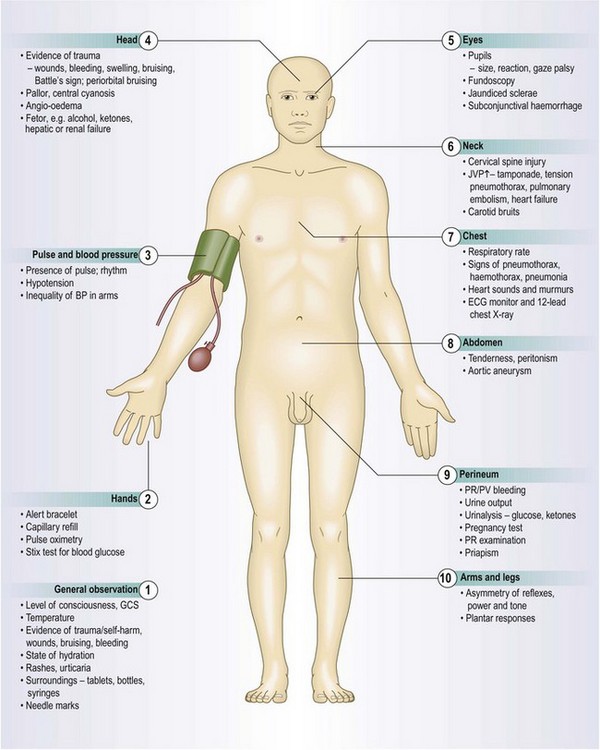
Approach to the critically ill patient
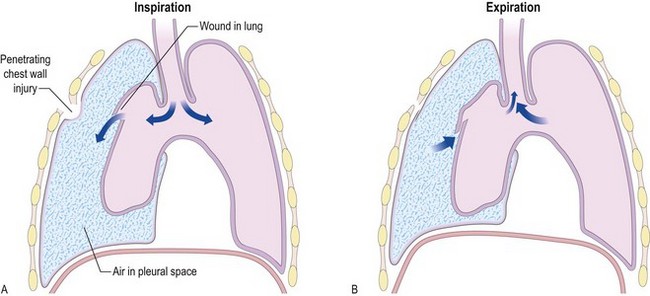
Systematic examination is inappropriate for critically ill patients as immediate intervention may be needed to save life, e.g. in cardiac arrest or tension pneumothorax, or to halt processes which untreated, would lead to death, e.g. hypovolaemic shock. Examination and interventions are often performed simultaneously.
Rapidly identify the main problems affecting the patient and use the resources available to gain control of the situation. Your aim is to stabilise the patient’s condition and address life-threatening problems. This temporary phase should always be followed by a full history and clinical examination when the patient is ‘stable’ to make a full diagnosis, perform specialist investigations and institute definitive therapy.
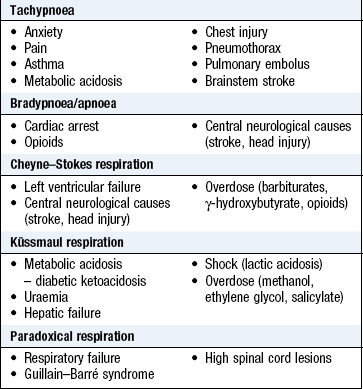
The clinical manifestations of critical illness (Box 19.1)
Critical illness can present as:
• acute respiratory compromise affecting Airway or Breathing (Box 19.2)
• acute cardiovascular compromise, detectable as reduced Circulation (Box 19.3)
• altered conscious state manifest as neurological Disability (Box 19.4).
Initially, you may not be aware of events or the timeframe preceding the current state. Concentrating on the system which appears most likely to be causing the problem may be misleading, wastes time and further compromises the patient. Use a simple and safe ABCD approach to address and correct conditions using a logical framework.
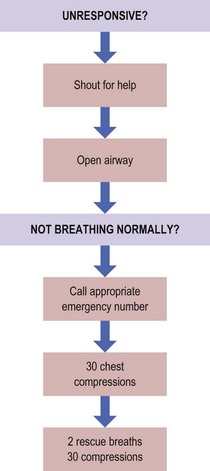
The ABCD approach
This has four interlinked phases:
Seek senior, experienced help immediately. If you have to work alone, only proceed to the next item once you have adequately completed the preceding one. A team can deal with the separate elements simultaneously, but the leader should ensure that all components are covered and if a patient’s condition deteriorates, should immediately review the ABCD sequence.
Communicating with others in order to get help requires careful, concise delivery of information that can be difficult in an emotionally charged resuscitation. A useful and widely used format with which to structure your thoughts is SBAR (situation, background, assessment, recommendation: Box 19.5).
Preparation
Information gathering: The patient may be unable to give a history, so use all possible sources of information (Box 19.6). Include previous primary care or hospital records, relatives, friends, bystanders and emergency or ambulance personnel. Look for diabetic/steroid/anticoagulant cards and medications, and Alert bracelets/necklaces (Fig. 3.3). If possible, contact the patient’s GP, who is often a key source of current and background information.
Managing your resources: Identify your available resources: which staff can help? What is their level of seniority and experience and what can they do? If you have others to help you, identify roles and responsibilities. If you are team leader, communicate your thinking to the whole team clearly and frequently.
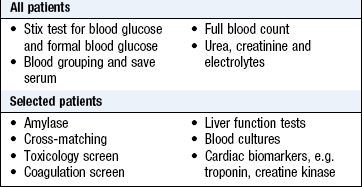
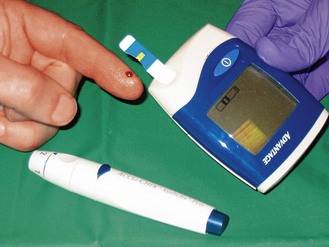
Investigations
See Box 19.15.
Secondary survey
The secondary survey reassesses the patient after the primary survey is complete. This is a systematic, detailed top-to-toe examination that fully documents additional signs and identifies injuries in the trauma patient. Only start the secondary survey once you are confident that there is no immediate need for further resuscitation and the patient does not require immediate transfer for definitive care, e.g. to theatre for a patient with a ruptured abdominal aortic aneurysm. Continually re-evaluate to assess the response to treatment. If the patient deteriorates or you are unsure about clinical status, return to the primary survey.
Give adequate analgesia to all patients in pain. There is no ‘standard’ dose. Slowly titrate an opioid drug, e.g. morphine IV in 1–2 mg aliquots to achieve pain relief. The amount needed varies according to the patient’s response and adverse effects, e.g. respiratory depression, hypotension.
Investigations
Specific investigations will depend upon the presentation involved, e.g. CT for head injury. A 12-lead ECG and chest X-ray are standard and in patients with blunt trauma the initial X-rays should, as a minimum, include views of the cervical spine, chest and pelvis. Perform a urinary pregnancy test in all women of child-bearing age.
Ensure tetanus prophylaxis for all trauma patients who are non-immune. Give IV antibiotic therapy to patients with presumed meningococcal disease, septic shock and open fractures.
Document all investigations, therapy and response to treatment. Stop the assessment process if the patient needs immediate definitive care or investigation. Let the receiving team know exactly which stage of the assessment process you have reached when you hand over care of the patient.
Definitive treatment
Once stable, the patient is moved to a critical care area, theatre, scanning room or another hospital. This is high-risk and there must be sufficiently trained staff accompanying the patient. The critically ill patient needs to be adequately monitored and as ‘stable’ as possible. All relevant documentation and investigation results should accompany the patient, with clear lines of communication between clinicians.
If you discover that the patient is terminally ill and that this crisis is not unexpected, it may not be appropriate for the patient to be given aggressive or ‘heroic’ treatment. It may be difficult to recognise and prepare for a patient’s death but it is essential and humane. Communicate with the family, the GP and the senior clinician previously involved in the patient’s care. Care for the patient in a dignified manner, with the emphasis on analgesia, relief of distressing symptoms and the highest quality of nursing care.