CHAPTER 20 Postural alignment
What is postural alignment?
Postural alignment refers to the relationship between body segments and in basic terms refers to the structure of the musculoskeletal system, bones, joints and muscles. The alignment of the musculoskeletal system, within normal limits, is important in terms of minimizing stresses on soft tissue, minimizing muscle effort and providing sensory information to the centres involved in motor control (the control of movement). Hence, the musculoskeletal alignment plays a significant role in facilitating efficient movement during functional activities (Lennon 2003; Mayston 2000a,b; Carr and Shepherd 2003).
The importance of sensory feedback to successful motor control is well established (Kandel et al. 2000), with all decisions made by the nervous system being based upon the sensory feed forward/feedback it receives. A successful outcome is therefore reliant upon receiving sufficient accurate sensory information, a large amount of which comes from the somatosensory receptors (S3.23) embedded in the musculoskeletal system. In the main, this information relates to proprioception (S3.23), joint and muscle position and movement sense. Therefore it is the alignment of the musculoskeletal system which informs the nervous system of its present state for the planning of movement and also its ongoing state during movement when outcome can be monitored.
The alignment of body segments is therefore critical in both posture (arrested movement) and movement itself. The relationship between posture and movement can be viewed as integral in terms of body segment alignment with similar patterns or strategies observed in both. To appreciate any deviations from a normal range, the therapist requires knowledge of the normal parameters of posture and movement patterns and the range of normal presentations.
Why do I need to assess postural alignment?
A deviation from the most efficient alignment of the musculoskeletal system can occur as a direct effect of various neurological impairments, e.g. as a result of hypertonia, hypotonia (S3.21); pain (S3.29); weakness (S3.30) or altered sensation (S3.23). The malalignment of one body segment may also produce further deviations from normal range in other segments. For example, hypotonia involving the shoulder complex will directly result in reduced stability at the glenohumeral joint and possibly a subluxation. However, the changes in biomechanics will also immediately influence the alignment of both the upper limbs and the trunk as the patient finds strategies to compensate and remain balanced. The extra effort required to move and the stresses on soft tissue may later produce pain which will further limit the biomechanics of the movement. Over time, soft tissue adaptation occurs and the new compensatory strategies become learned via the physiological processes of neuroplasticity (Ungerleider et al. 2002; Marrone 2007).
Following a change in the musculoskeletal alignment of a body, there is a corresponding change in the somatosensory feedback to the nervous system. In the case of patients with a neurological deficit, they may be further disadvantaged by having a direct lesion involving the sensory system which may limit the amount and accuracy of the feedback. Potentially this could lead to an inaccurate motor plan being implemented and ultimately an inefficient, unsuccessful movement.
In terms of treatment, the therapist will aim to facilitate a musculoskeletal alignment that is within normal limits for both posture and movement.
How do I assess postural alignment?
Observation
As the patterns of musculoskeletal alignment are similar for posture and movement, the initial assessment can be carried out in a static posture. The assessment of alignment during movement is covered in the second part of the objective assessment section whereby the therapist performs a movement analysis of a functional task (S3.18).
Patient
The posture chosen will vary according to the patient’s ability. For example, for a patient recently admitted with no sitting balance it will be safer in a supported sitting or supine position.
![]() Clinical hints and tips
Clinical hints and tips
Keep in mind that until you have more experience the process may take some time and sitting or standing for a long period may be uncomfortable for some people.
The same malalignments can often be observed in any posture, but will be more pronounced when the patient is in a more challenging posture, such as sitting and standing.
Therapist
![]() Caution
Caution
Do not to start analysing the data until you have recorded all your findings from the individual body segments. You may start to question correctly that a deviation in one segment is occurring because of the influence of another, however waiting until the full picture is available will improve your overall analysis and conclusions.
Recording
When recording the findings there are a few viable options to choose from. Namely:
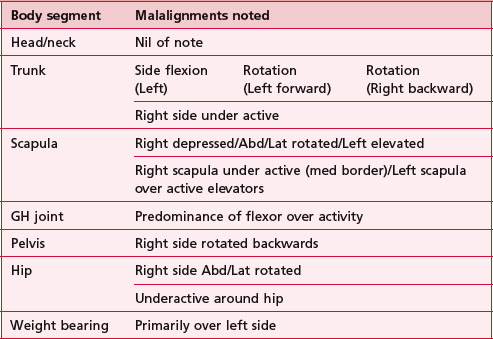
Table 20.1 Text description of the postural alignment assessment of patient X (pt X)
Analysis
Having completed the assessment, the therapist should have identified any deviations outside the normal limits expected. During the analysis of this data, the therapist should start to hypothesize the relationship between any deviations presented and begin to try and predict which may be causal and which may be a compensation in response. Gathering more information from the remaining objective assessment tools will be necessary before the reason for the deviations can be established.
Example
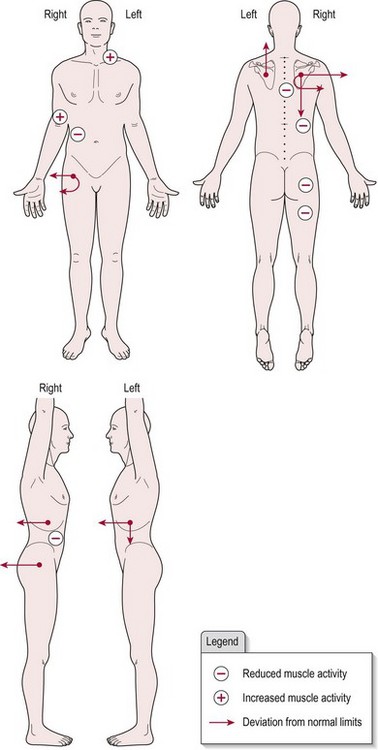
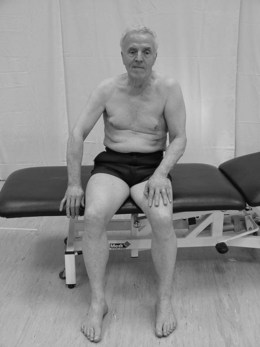
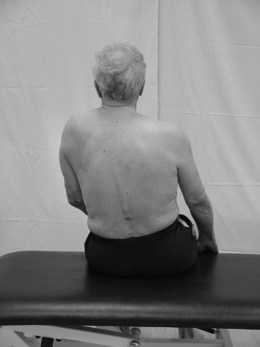
The body chart (Fig. 20.3) represents patient X shown in Figures 20.1 and 20.2 who has suffered a right hemiplegia. Following analysis of all the objective markers and examination of the body chart the following is hypothesized. The right pelvis, hip, trunk and shoulder complex are seen to be rotated backwards probably due to hypotonia. In response, the patient works harder with the left side, especially the shoulder complex (elevation) and forward trunk rotation in an attempt to maintain an upright posture against gravity. The latter is a normal response to the deviation imposed by the hypotonia on the right. Therefore treatment would be most effective aimed at the hypotonia with the assumption that the compensatory activity would then no longer be required.
Outcome measures
Research
Objective tools capable of measuring the alignment of structures of the musculoskeletal system include:
References and Further Reading
Carr J, Shepherd R. Stroke rehabilitation guidelines for exercise and training to optimize motor skill. Edinburgh: Butterworth-Heinemann; 2003.
Kandel ER, Schwartz JH, Jessell TM. Principles of neural science, ed 4. New York: McGraw-Hill Health professions Division; 2000.
Lennon S. Physiotherapy practice in stroke rehabilitation: a survey. Disability and Rehabilitation. 2003;259:455-461.
Marrone DF. Ultrastructural plasticity associated with hippocampal learning: a meta analysis. Neurobiology of Learning and Memory. 2007;873:361-371.
Mayston M. Handling and spasticity letter to the editor. Physiotherapy. 2000;86:559.
Mayston M. Compensating for CNS dysfunction letter to the editor. Physiotherapy. 2000;86:612.
SiliconCOACH. SiliconCOACH coaching solutions for a digital age [online]. New Zealand www.siliconcoach.com, 2004. (Accessed 1 September 2006)
Ungerleider LG, Doyon J, Karni A. Imaging brain plasticity during motor skill learning. Neurobiology of Learning and Memory. 2002;783:553-564.