CHAPTER 21 Muscle tone
What is normal muscle tone?
Muscle tone is often referred to as a state of readiness in a muscle at rest (resting tone) which provides us with a background level of tone from which we can function efficiently. It is defined by the resistance to passive movement, which is an expression of the stiffness of the muscle fibres (Brodal 2004). Normal tone should be high enough to keep you up against gravity but low enough to allow movement.
![]() Caution
Caution
There is huge variation of normal within this definition. The ability to differentiate abnormal muscle tone can only come from an appreciation of this normal range and this requires the therapist to handle individuals with an intact nervous system.
When the limb of an individual with an intact central nervous system is moved passively the following characteristics are evident:
In terms of muscle tone this requires the individual to reduce their muscle tone to a level that allows the limb to be moved freely (follow) but then to immediately recruit sufficient activity so that the limb remains in a position when released (placing).
Muscle tone is considered to depend physiologically on two factors:
Non-neural factors
This is a consequence of the mechanical-elastic properties of the soft tissues (compliance or stiffness of soft tissue structures) and incorporates the thixotropic properties (viscosity) of the muscle and the muscle length. These factors contribute a significant component to the normal resting tone of a muscle which explains how we are able to stand still with only minimal corrective bursts of postural muscle activity (Simons and Mense 1998). These non-neural factors can be influenced by age, temperature and exercise.
Neural factors
The neural factors relate to the degree of activation of the contractile apparatus of the muscle. Our muscles are constantly contracting or active and it is the nervous system that controls the appropriate level of this background activity. The level of muscle contraction is a result of the output from the alpha motor neuron (AMN) in the ventral horn of the spinal cord (S2.13) which innervates the muscle itself. The AMN output is dictated by the final outcome of competing inhibitory and excitatory synapses from various inputs related to both the peripheral and central nervous systems. These include:
It is the final assimilation of all these inputs at the level of the spinal cord which dictates the output from the alpha motor neuron and translates into the precise level of muscle tone.
What is abnormal muscle tone?
Individuals who have a neurological lesions affecting the central nervous system (CNS) may lose the ability to control the level of muscle tone and may present with resting tone that is either too low (hypotonia) or too high (hypertonia) (Brodal 2004). It is also common to see both these characteristics present in an individual patient.
In CNS lesions, muscle weakness (S3.30) is evident in association with both hypotonia (reduced muscle tone) and hypertonia (increased muscle tone). The relationship between these concepts is complex but it appears likely that both altered tone states directly contribute to a reduction in force production (weakness) of the muscle. The pathophysiology which defines alterations in muscle tone will also lead to a dysfunction in the timing or pattern of motor unit recruitment or the number of units able to be recruited. This will lead to a presentation of muscle weakness during certain movements. It should also be noted that when altered tone exists over a prolonged period, the outcome may be disuse of the part, and further muscle weakness may occur as a consequence of sarcomere loss and reduction in cross-sectional area (S3.30).
In terms of assessment, a comparison of the conceptual definitions gives the therapist a simplified tool by which to differentiate muscle tone and weakness. Muscle tone is defined as the resistance to passive movement, representing the background level of tension or stiffness in a muscle (Moore and Kowalske 2000). Therefore it should be assessed in a muscle at rest. Muscle weakness on the other hand is defined as the inability to generate sufficient force to overcome the resistance of a task and therefore by definition should be assessed during movement activities.
Hypotonia
Definition
Hypotonia, or low tone, is a reduced level of muscle stiffness, providing little or no resistance when moved passively and which cannot be ‘placed’ on termination of the movement. The limb feels heavy when handled and tendon reflexes are reduced or absent. Patients with hypotonia will have difficulty staying up against gravity and when attempting to move present with areas of postural instability and ineffective muscle recruitment that makes movement effortful. An absence of muscle tone is referred to as flaccidity.
Pathophysiology of hypotonia
Hypotonia presents in many pathologies involving the central nervous system, e.g. multiple sclerosis, traumatic brain injury and cerebrovascular accident (CVA). Where an acute insult occurs, the nervous system may go into a state of neural shock (Kwakkel et al. 2003). The shock results in reduced neuronal conduction (S2.6) and a breakdown in communication within the nervous system. If the motor systems are affected, an insufficient number of alpha motor neurons can be recruited and hypotonia presents. Over time, as the nervous system recovers the neural shock subsides, neural transmission is resumed and muscle tone begins to return. However, there is no guarantee that it will return to normal.
If the patient still presents with hypotonia after a 4-week period, the presentation is sometimes termed ‘prolonged muscular flaccidity’ (Kwakkel et al. 2003). In CVA, the prognosis for the final outcome is poor if this state remains beyond 3 months (Formisano et al. 2005). The definitive cause of prolonged muscular flaccidity is unclear in the current literature. It has been hypothesized to result from a reduction in the levels of arousal and central drive leading to insufficient excitation at the alpha motor neuron. However, the cortical loops associated with the basal ganglia and cerebellum are also found to be severely affected in patients with prolonged muscular flaccidity (Pantano et al. 1995).
Hypertonia
Hypertonia, or high tone, is an increase in muscle stiffness with an increased resistance to passive movement. Patients often present with effortful movement that is often ineffective. Hypertonia is sub-divided into:
Rigidity defined
Traditionally, rigidity is defined as an increased resistance to passive movement which is constant throughout the range of movement. The resistance occurs throughout the full range of a passive movement and will be present in all muscles (including the face). The resistance is described as ‘lead-pipe’ (constant through range) or ‘cogwheel’ (resistance followed by a period of ‘give’) (Fung and Thompson 2002; Xia and Rymer 2004). As a result of rigidity affecting all muscle groups, patients often present with a lack of rotation, especially in the trunk (Wright et al. 2007). Recent studies have shown that rigidity is also velocity dependent (Mak et al. 2007; Xia et al. 2009). Voluntary movement is difficult both to initiate and arrest. Tendon reflexes are usually normal.
Pathophysiology of rigidity
Rigidity is one of the cardinal symptoms in Parkinson’s disease (PD) but can be seen in any patient with a lesion of the basal ganglia. The presentation of increased resistance to passive movement in rigidity is a consequence of neural and non-neural factors.
Neural factors
The neural factors are a result of damage to the basal ganglia (S2.11) and particularly, the dopamine-producing cells of the substantia nigra (SN). The dopaminergic neurons of the SN project to the striatum and normally modulate the activity of both the direct and indirect pathways within the basal ganglia (S2.11), having the opposite effect on each. The direct pathway facilitates the initiation and selection of the correct voluntary movement programmes to achieve a task, while the indirect pathway helps to prevent any unwanted movement programmes. In PD, the loss of dopaminergic cells in the SN means that the ability to modulate motor programme selection is lost and there is inappropriate competition between the correct and incorrect movement programmes being sent to the cortex. At a muscular level, this presents as inappropriate co-contraction (Xia and Rymer 2004; Xia et al. 2009) attributed to inadequate reciprocal inhibition (Meunier et al. 2000). Consequently, a hypokinetic movement disorder presents, or in simple terms a lack of movement.
Non-neural
Altered muscle activity and joint movement leads to structural and functional changes in the musculoskeletal system. Muscles lose sarcomeres, becoming shorter, stiffer and more thixotropic and collagen production may be altered and disorganized. This structural change is considered to significantly contribute to the resistance to passive movement (Bhakta 2000; Chung et al. 2004; Vattanasilp et al. 2000).
Hypertonia (related to spasticity) defined
Hypertonia (related to spasticity) is notoriously difficult to understand for the novice therapist. This is primarily because in clinical practice the term ‘spasticity’ is often used interchangeably with hypertonia. This is misleading. Spasticity is defined as velocity- and length-dependent increase in the tonic stretch reflex with exaggerated tendon reflexes and is described as a range of positive and negative features (Table 21.1), one of which is hypertonia (Lance 1980; Platz et al. 2005; Burridge et al. 2005). Therefore, for clarity, this text will use the term ‘hypertonia (related to spasticity)’. Hypertonia (related to spasticity) is defined as an increase in resistance to a passive movement that increases with the velocity of the movement and then fades away as the muscle is held in a constant stretch, when it is described as ‘clasp knife’. The clinical presentation is a feeling of stiffness during part of or all of the range of movement and the patient’s limb may be held in an abnormal posture. The pattern of hypertonia (related to spasticity) may be present in any muscle group, however common presentations have been linked with lesions of different levels of the brain:
Table 21.1 The positive and negative features of spasticity
| Positive features | Negative features |
|---|---|
| Hyper-reflexia (S3.22) | Weakness (S3.30) |
| Hypertonia | Inability to fractionate |
| Gross movement patterns (S3.18) | Poor selective movement |
| Associated reactions (S3.18) | |
| Abnormal co-contraction | |
| Clonus (S3.18) |
Clinical observation seems to indicate that voluntary movement, increased effort and increased sensory stimulation may further increase hypertonia. However, evidence shows that in terms of reflex activity, this is not the case (Sharp and Brouwer 1997; Ada et al. 1998; Burne et al. 2005).
Pathophysiology of hypertonia (related to spasticity)
Hypertonia (related to spasticity) may be seen in patients with a lesion of the CNS. However, the nature of the pathology will dictate whether the onset is immediate (traumatic brain injury) or slowly evolving (CVA, multiple sclerosis, spinal cord injury) (Edwards 2002). The presentation of increased resistance to passive movement is related to a combination of neural and non-neural factors:
Neural factors
In terms of neural factors, hypertonia (related to spasticity) results from an increased excitability of the alpha motor neuron at the level of the spinal cord. This could occur as a consequence of (1) damage to inhibitory pathways (medullary or medial reticulospinal tract) or (2) increased activity of the excitatory pathways (pontine or lateral reticulospinal tract).
Non-neural
Altered muscle activity and joint movement leads to structural and functional changes in the musculoskeletal system. Muscles lose sarcomeres, becoming shorter, stiffer and more thixotropic and collagen production may be altered and disorganized. This structural change is considered to significantly contribute to the resistance to passive movement (Bhakta 2000; Chung et al. 2004; Vattanasilp et al. 2000).
In the literature, there remains uncertainty as to the relevant contributions of neural and non-neural factors. Electromyography studies show that the reflex-mediated increase in muscle tone reaches its maximum between 1 and 3 months post-lesion (Bhakta 2000; Teasell and Heitzner 1998), whereas others state that reflexic activity is only evident when a limb is moved quickly (Vattanasilp et al. 2000). However, after 3 months, the increased resistance to passive stretch is proposed to be primarily due to the intrinsic non-neural stiffness of the muscle (Bhakta 2000; Chung et al. 2004; Vattanasilp et al. 2000).
Why do I need to assess muscle tone?
It is important to assess muscle tone because of its potential effect on functional ability. Hypotonia appears to be a negative prognostic indicator in CVA and also prolongs the rehabilitation process (Formisano et al. 2005). A direct correlation between hypertonia and the level of disability has not been established (Sommerfeld et al. 2004) and little is known about hypertonia in a contracting muscle. In fact, some evidence implies that movement disorders observed in patients who present with hypertonia are the result of weakness in the agonist muscle rather than hypertonia in the antagonist. It is therefore unclear how, or if, hypertonia contributes directly to the movement disorders itself. However, a detrimental effect on function has been associated with the secondary side-effects of hypertonia, which include pain (Pizzi 2005), contracture (Watkins et al. 2002; Pizzi 2005), limitation of range of movement (Lin and Sabbahi 1999) and muscle weakness (Maruishi et al. 2001).
How do I assess muscle tone?
Observation
Patient
The therapist may start their assessment of muscle tone in any posture but will need to assess in various postures to gain a true insight into the patient’s deficit.
Therapist
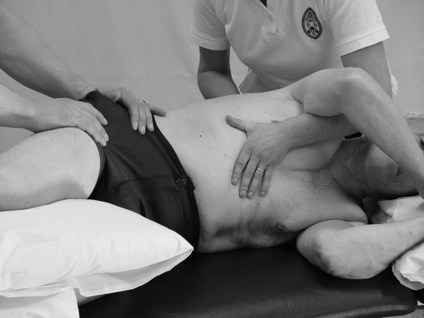
Passive movements
Therapist
This tool assesses the resistance to passive movement and therefore adheres closely to the definition of altered muscle tone. The therapist is evaluating the overall outcome of both the neural and non-neural components of muscle tone. The test should be carried out with the muscle at rest, therefore ensure that the patient is comfortable and supported.
![]() Caution
Caution
Some patients may find it very difficult to fully relax. The consequent tension in the muscles is not hypertonia.
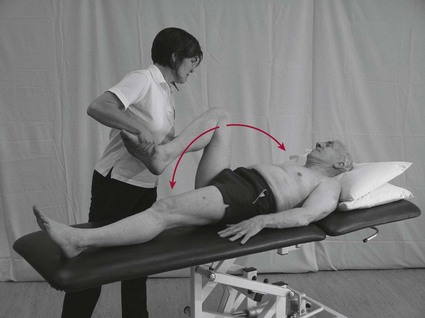
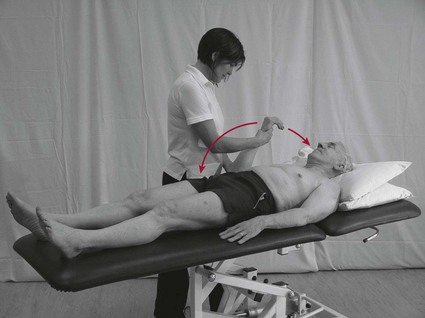
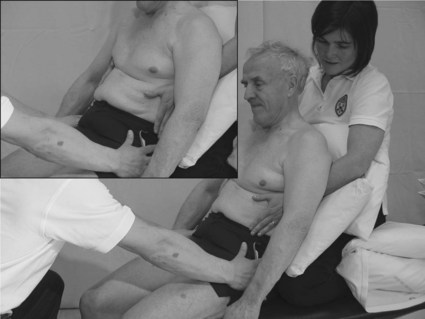
Limb testing
Trunk testing
This involves performing a passive movement to the patient’s trunk.
Reflex testing
Therapist
Reflex testing (S3.22) is carried out to evaluate or confirm the integrity of the reflex pathway and the reflexic properties of the muscle. This may tell us in part about the neural component of muscle tone but it does not tell us about the overall stiffness of a muscle. Therefore it is an inappropriate tool to use for testing muscle tone in isolation. In terms of hypo-reflexia, the peripheral or central nervous system could be implicated. A hyper-reflexic muscle may confirm the involvement spasticity, however caution is advised when directly relating this finding to hypertonia as the evidence indicates that there is a low correlation between the existence of hypertonia and increased tendon jerk reflexes (S2.22) (Teasell and Heitzner 1998).
Recording
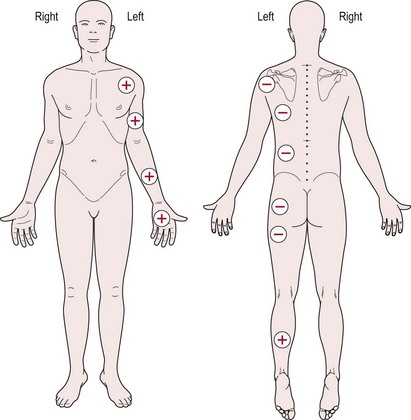
When recording findings, the therapist may use a body chart (Fig. 21.6) or a text description (Table 21.2).
Example
See Figure 21.6 and Table 21.2.
Table 21.2 Example of a text description recording (muscle tone)
Analysis
The identification of severe hypotonia or hypertonia is often uncomplicated. However, in moderate and mild severity, diagnosis is more difficult. The differential diagnosis of rigidity and spasticity will primarily be based upon the area of brain damaged. However, based on the pathophysiology of altered muscle tone which identifies both neural and non-neural components, the therapist should use a combination of assessment tools before coming to a conclusion. The therapist should also assess the patient for any other (treatable) factors which may be influencing muscle tone, such as, pain (musculoskeletal or systemic), soft tissue adaptation (from poor seating), medication or emotional stress. These should be alleviated as a priority.
Analysis of the example shown in Figure 21.6 and Table 21.2 leads to the hypothesis that hypotonia exists through the left trunk, shoulder and hip girdles, with hypertonia evident in the flexor muscles of the left elbow, wrist and hand and in the extensor muscles of the left ankle.
References and Further Reading
Ada L, O’Dwyer N. Do associated reactions in the upper limb after stroke contribute to contracture? Clinical Rehabilitation. 2001;15:186-194.
Ada L, Vattanasilp W, O’Dwyer N, et al. Does spasticity contribute to walking dysfunction after stroke? Journal of Neurology Neurosurgery and Psychiatry. 1998;64:628-635.
Bhakta BB. Management of spasticity in stroke. British Medical Bulletin. 2000;56:476-485.
Bhakta BB, Cozens JA, Chamberlain MA, et al. Quantifying associated reactions in the paretic arm in stroke and their relationship to spasticity. Clinical Rehabilitation. 2001;15:195-206.
Brodal P. The central nervous system: structure and function, ed 3. Oxford: Oxford University Press; 2004.
Burne JA, Carleton VL, O’Dwyer NJ. The spasticity paradox: movement disorder or disorder of resting limbs? Journal of Neurology Neurosurgery and Psychiatry. 2005;76:47-54.
Burridge JH, Wood DE, Hermens HJ, et al. Theoretical and methodological considerations in the measurement of spasticity. Disability and Rehabilitation. 2005;271/2:69-80.
Chung SG, van Rey E, Bai Z, et al. Biomechanic changes in passive properties of hemiplegic ankles with spastic hypertonia. Archives of Physical Medicine and Rehabilitation. 2004;85:1638-1646.
Corden DM, Lippold OC, Buchanan K, et al. Long-latency component of the stretch reflex in human muscle is not mediated by intramuscular stretch receptors. Journal of Neurophysiology. 2000;84:184-188.
Edwards S. Neurological physiotherapy. Edinburgh: Churchill Livingstone; 2002.
Formisano R, Pantano P, Buzzi MG, et al. Late motor recovery is influenced by muscle tone changes after stroke. Archives of Physical Medicine and Rehabilitation. 2005;86:308-311.
Fung VS, Thompson PD. Rigidity and spasticity. In: Jankovic JJ, Tolosa E, editors. Parkinson’s disease and movement disorders. ed 4. Philadelphia: Lippincott Williams and Wilkins; 2002:473-482.
Kandel ER, Schwartz JH, Jessell TM. Principles of neural science, ed 4. New York: McGraw-Hill; 2000.
Kwakkel G, Kollen BJ, van der Grond J, et al. Probability of regaining dexterity in the flaccid upper limb: impact of severity of paresis and time since onset in acute stroke. Stroke. 2003;34:2181-2186.
Lance JW. Spasticity: disordered motor control. In: Feldman RG, Young RR, Koella WP, editors. Spasticity: disordered motor control. Chicago: Year Book Medical; 1980:485-494.
Lin F-M, Sabbahi M. Correlation of spasticity with hyperactive stretch reflexes and motor dysfunction in hemiplegia. Archives of Physical Medicine and Rehabilitation. 1999;80:526-530.
Magee DJ. Orthopaedic physical assessment, ed 4. Canada: Elsevier Sciences; 2002.
Mak MK, Wong EC, Hui-Chan CW. Quantitative measurement of trunk rigidity in parkinsonian patients. Journal of Neurology. 2007;254:202-209.
Maruishi M, Mano Y, Sasaki T, et al. Cerebral palsy in adults: independent effects of muscle strength and muscle tone. Archives of Physical Medicine and Rehabilitation. 2001;82:637-641.
Meunier S, Pol S, Houeto JL, et al. Abnormal reciprocal inhibition between antagonist muscles in Parkinson’s disease. Brain. 2000;123:1017-1026.
Moore DP, Kowalske KJ. Neuromuscular rehabilitation and electrodiagnosis of myopathy. Archives of Physical Medicine and Rehabilitation. 2000;81:S-32-S-35.
Nielsen JB, Crone C, Hultborn H. The spinal pathophysiology of spasticity – from a basic science point of view. Acta Physiologica. 2007;1892:171-18010.
Pantano P, Formisano R, Ricci M, et al. Prolonged muscular flaccidity after stroke: morphological and functional brain alterations. Brain. 1995;118:1329-1338.
Platz T, Eickhof C, Nuyens G, et al. Clinical scales for the assessment of spasticity associated phenomena and function: a systematic review of the literature. Disability and Rehabilitation. 2005;271/2:7-18.
Pizzi A, Carlucci G, Falsini C, et al. Evaluation of upper-limb spasticity after stroke: a clinical and neurophysiologic study. Archives of Physical Medicine and Rehabilitation. 2005;86:410-415.
Rathore SS, Hinn AR, Cooper LS, et al. Characterization of incident stroke signs and symptoms: findings from the Atherosclerosis Risk in Communities Study. Stroke. 2002;33:2718-2721.
Sharp SA, Brouwer BJ. Isokinetic strength training of the hemiparetic knee: effects on function and spasticity. Archives of Physical Medicine and Rehabilitation. 1997;78:1231-1236.
Sheean G. The pathophysiology of spasticity. European Journal of Neurology. 2002;9:3-9.
Simons DG, Mense S. Understanding and measurement of muscle tone as related to clinical muscle pain. Pain. 1998;75:1-17.
Sommerfeld DK, EekE U-B, Svensson A-K, et al. Spasticity after stroke: its occurrence and association with motor impairments and activity limitations. Stroke. 2004;35:134-140.
Teasell RW, Heitzner JD. The painful hemiplegic shoulder. Physical Medicine and Rehabilitation: State of the Art. 1998;12:489-500.
Vattanasilp W, Ada L, Crosbie J. Contribution of thixotropy spasticity and contracture to ankle stiffness after stroke. Journal of Neurology Neurosurgery and Psychiatry. 2000;69:34-39.
Watkins C, Leathley M, Gregson J, et al. Prevalence of spasticity post stroke. Clinical Rehabilitation. 2002;165:515-522.
Woollacott AJ, Burne JA. The tonic stretch reflex and spastic hypertonia after spinal cord injury. Experimental Brain Research. 2006;1742:386-396.
Wright WG, Gurfinkel VS, Nutt J, et al. Axial hypertonicity in Parkinson’s disease: direct measurements of trunk and hip torque. Experimental Neurology. 2007;208:38-46.
Xia R, Rymer WZ. Reflex reciprocal facilitation of antagonist muscles in spinal cord injury. Spinal Cord. 2004;43:14-21.
Xia R, Sun S, Threlkeld J. Analysis of interactive effect of stretch reflex and shortening reaction on rigidity in Parkinson’s disease. Clinical Neurophysiology. 2009;120:1400-1407.