CHAPTER 25 Trunk stability
What is trunk stability?
The terms trunk/central and spinal stability are synonymous and are used interchangeably in clinical practice. Core stability is the equivalent lay term. In essence, trunk stability is a reflection of an individual’s postural control, the ability to orientate and stabilize the body using appropriate balance strategies and responses (Raine et al. 2009). As such, trunk stability is an essential core component of balance, the ability to maintain the centre of mass (COM) within the base of support (BOS) (S3.32) and functional activities, by which it provides proximal stability to allow for the coordinated free movement of the limbs and head (Brown 2006; Massion et al. 2004). Trunk stability is also important in controlling and supporting the spinal segments, so reducing the stresses upon soft tissue structures and helping to avoid injury and pain.
Trunk stability mainly incorporates muscle activation related to the trunk, head/neck and proximal limb girdles. However, it is also described as a muscular ‘box’ that is made up of the diaphragm superiorly, the pelvic floor and gluteal muscles inferiorly, the abdominals anteriorly and the back extensors posteriorly. The therapist should remain aware of the ‘box’ as a whole in terms of strategies they may use to facilitate treatment (through contraction of the pelvic floor) and tricks that the patient may use to achieve false stability (breath holding).
This section will focus upon the core trunk muscles which are commonly divided into two groups according to their functional anatomy (Bergmark 1989):
The global stabilizers
These muscles are anatomically superficial and their action does not have an influence at a segmental level. They are composed primarily of Type IIx (fast glycolytic fibres) muscle fibres which can generate larger forces but are fast fatiguing. The function of the global stabilizers is primarily trunk movement, although they do contribute to general trunk stability.
The local stabilizers
These muscles are anatomically deep and have attachments to each individual spinal vertebra. This allows them to act at a segmental level (between adjacent vertebrae) providing a strong basis for trunk stability. The local stabilizers are composed primarily of Type I (slow oxidative fibres) muscle fibres, which produce low forces but are fatigue resistant. These muscles therefore function as postural muscles. They also have smaller motor units which are easily activated due to their low neural threshold and therefore tend to be recruited first (Henneman principle) during functional activities. In theory, this means that the local stabilizers are activated prior to the surrounding global muscles which have larger motor units. This pre-setting of trunk stability is crucial in providing a stable base upon which limb movement can be based and may be part of an anticipatory response to a perceived COM displacement (MacDonald et al. 2006). The anticipatory activation will be built into a learned movement plan.
The anatomical and physiological features of the local muscle stabilizers make them perfectly adapted to perform their specific trunk stability function, however the nervous system also influences the fine control of these muscles. The force of contraction required to provide segmental stability is estimated to be 3% of maximum contraction (Cholewicki and McGill 1996). As antigravity postural muscles, this background level of activity is controlled by the vestibular and reticular systems (S2.10).
The balance of activity between the abdominal (TAb/IOf) and back extensor (MT) pair is vital in terms of the level and timing of activation. A neutral position of the pelvis and lumbar spine is considered to be highly correlated with the co-contraction of this muscle pair (O’Sullivan 2006). In postures of either anterior pelvic tilt with lumbar spine hyperextension or posterior tilt with lumbar spine flexion the local muscles are switched off and over time become deconditioned (O’Sullivan 2006). This is highly relevant in a population of neurologically impaired patients who often spend many hours sitting in poor postures in inadequate seating.
Why do I need to assess trunk stability?
Trunk instability results in less efficient movement, a limited ability to explore the environment (Cristea et al. 2003) and demands compensatory muscle activity to maintain an upright position. The latter may present as abnormal fixation of the trunk or, in extreme cases, excessive use of the upper limbs, and leads to effortful movement for the individual. Poor trunk stability resulting in deviations in posture may also cause abnormal stresses and potential damage to soft tissue structures leading to pain and further functional loss. Often rehabilitation focuses on improving general trunk stability without specific attention to the interaction between the local and global stabilizers. More focus on segmental stability initially may have the potential to improve the movement sequences and the functional outcome for the individual.
In a neurologically impaired patient, poor trunk stability has been linked with a poor functional outcome in multiple sclerosis (Lanzetta et al. 2004), cerebrovascular accident (CVA) (Hsieh et al. 2002) and Parkinson’s disease (PD) (Dibble and Lange 2006; Nardone and Schieppati 2006).
In CVA, trunk instability has also been linked with poor postural control in standing (Palmer et al. 1996; Slijper et al. 2002) and in sitting (Dickstein et al. 2004) and is viewed as a negative prognostic indicator for recovery. Proprioception (position sense) (Mergner et al. 2003; Peterka 2002) and reduced strength (Karatas et al. 2004) in the trunk have been found to be causal in CVA (Ryerson et al. 2008) and in PD (Vaugoyeau et al. 2007).
How do I assess trunk stability?
Observation during functional activities
Patient
Any trunk instability may have already been noted during the second section of the objective assessment (S3.18). However, as the demands on trunk stability appear to be task specific the therapist should ensure they have investigated a range of functional activities.
Therapist
The therapist observes the patient during a functional activity.
Assessment of the local muscle stabilizers
Patient
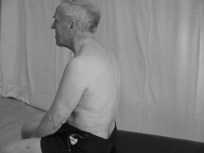
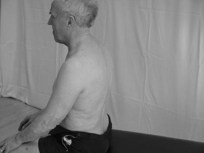
Initially in terms of patient safety, it is wise to begin assessing the patient in a sitting position. However, for higher level patients, a further assessment when standing may also be pertinent.
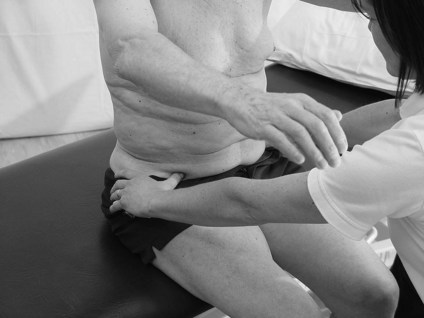
Therapist: observe and palpate
![]() Clinical hints and tips
Clinical hints and tips
Although MT is found at all levels of the vertebral column it is at its thickest in the cervical and lumbar areas and it is superficial from level L3 down.
Anatomically, in cadavers, the TAb and IOf muscles have been found to be fused at this palpation point (Marshall and Murphy 2003). The therapist should be aware they are palpating both muscles, however this is deemed clinically acceptable when considering that they are also functionally compatible.
![]() Clinical hints and tips
Clinical hints and tips
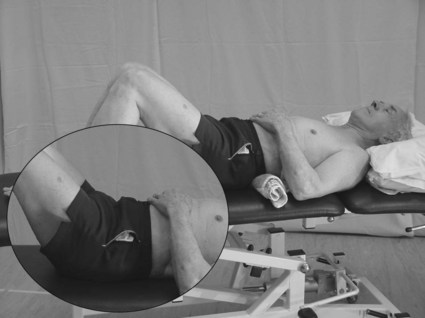
During a simple bilateral arm raise through shoulder flexion the COM is displaced forward and therefore stabilizer activity is greatest in the back extensors. During a unilateral leg lift through hip flexion, the COM is initially displaced backwards and therefore the greatest stabilizer activity is recorded in the abdominals to maintain the alignment of the pelvis.
Therapist: realign pelvis/lumbar spine
Therapist: assessment of individual muscle components
If the patient is still unable to recruit the appropriate muscles with the pelvis/lumbar spine in a neutral alignment then the therapist should evaluate the patient’s ability to activate the local muscle components individually.
Transversus abdominus (TAb)
Multifidus (MT)
Recording
A simple heading and text description of all the therapist’s findings is acceptable, or notation with a key on a body chart.
Example
Trunk stability: patient presents with exaggerated postural sway during all upper limb activities. Postural sway increases with eyes closed. Patient is able to isolate both local stabilizers appropriately in sitting with effort and focused attention. Muscle tone in the trunk appears normal however proprioception is reduced.
Analysis
The findings from an assessment of trunk stability should be considered in relation to other assessment tools (S3.19–34) and especially postural control/balance as the two are highly integrated. Analysis and synthesis of all this information may allow the therapist to predict a possible cause of the trunk instability.
In terms of the above example, the cause of the increased postural sway is likely to be altered sensory feedback (proprioception). This is reinforced when vision is withdrawn and the patient presents with an increase in sway.
References and Further Reading
Bergmark A. Stability of the lumbar spine: a study in mechanical engineering. Acta Orthopaedica Scandinavica. 1989;230(Suppl):20-24.
Brown TD. Getting to the core of the matter. Strengthening and Conditioning Journal. 2006;282:1524-1604.
Cholewicki J, McGill S. Mechanical stability of the in vivo lumbar spine: implications for injury and chronic low back pain. Clinical Biomechanics. 1996;11:1-15.
Cristea MC, Mitnitski AB, Feldman AG, et al. Interjoint coordination dynamics during reaching in stroke. Experimental Brain Research. 2003;1513:289-300.
Dibble LE, Lange M. Predicting falls in individuals with Parkinson disease: a reconsideration of clinical balance measures. Journal of Neurologic Physical Therapy. 2006;30:60-67.
Dickstein R, Sheffi S, Markovici E. Anticipatory postural adjustment in selected trunk muscles in post stroke hemiparetic patients. Archives of Physical Medicine and Rehabilitation. 2004;85:228-234.
Hsieh CL, Sheu CF, Hsueh IP, et al. Trunk control as an early predictor of comprehensive activities of daily living function in stroke patients. Stroke. 2002;33:2626-2630.
Karatas M, Cetin N, Bayramoglu M, et al. Trunk muscle strength in relation to balance and functional disability in unihemispheric stroke patients. American Journal of Physical Medicine and Rehabilitation. 2004;83:81-87.
Lanzetta D, Cattaneo D, Pellegatta D, et al. Trunk control in unstable sitting posture during functional activities in healthy subjects and patients with multiple sclerosis. Archives of Physical Medicine and Rehabilitation. 2004;85:279-283.
MacDonald DA, Moseley GL, Hodges PW. The lumbar multifidus: does the evidence support clinical belief? Manual Therapy. 2006;11:254-263.
Marshall P, Murphy B. The validity and reliability of surface EMG to assess the neuromuscular response of the abdominal muscles to rapid limb movement. Journal of Electromyography and Kinesiology. 2003;13:477-489.
Massion J, Alexandrov A, Frolov A. Why and how are posture and movement coordinated? Progress in Brain Research. 2004;1432:13-27.
Mergner T, Mauer C, Peterka RA. Multisensory posture control model of human upright stance. Progress in Brain Research. 2003;142:189-201.
Nardone A, Schieppati M. Balance in Parkinson’s disease under static and dynamic conditions. Movement Disorders. 2006;21:1515-1520.
O’Sullivan PB, Dankearts W, Burnett AF, et al. Effect of different upright sitting postures on spinal-pelvic curvature and trunk muscle activation in a pain free population. Spine. 2006;3119:E707-E712.
Palmer E, Downes L, Ashby P. Associated postural adjustments are impaired by a lesion of the cortex. Neurology. 1996;46:471-475.
Peterka JR. Sensorimotor integration in human postural control. Journal of Neurophysiology. 2002;883:1097-1118.
Raine S, Meadows L, Lynch-Ellerington M. Bobath concept theory and clinical practice in neurological rehabilitation. Oxford: Wiley Blackwell; 2009.
Ryerson S, Byl NN, Brown DA, et al. Altered trunk position sense and its relation to balance functions in people post-stroke. Journal of Neurologic Physical Therapy. 2008;321:14-20.
Slijper H, Latash M, Rao N, et al. Task specific modulation of anticipatory postural adjustments in individuals with hemiparesis. Clinical Neurophysiology. 2002;113:642-655.
Vaugoyeau M, Viel S, Assaiante C, et al. Impaired vertical postural control and proprioceptive integration deficits in Parkinson’s disease. Neuroscience. 2007;146:852-863.