CHAPTER 32 Balance
What is balance?
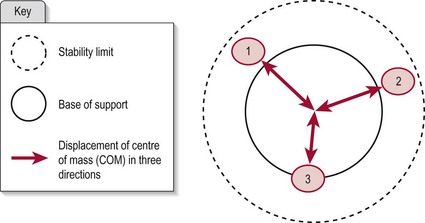
In biomechanical terms, balance is a state whereby the projection of the centre of mass (COM) falls within the stability limits of the base of support (BOS). The stability limit being the point at which balance is lost and corrective action is required. Balance is a core component of all functional activities and as such, incorporates both the concepts of posture (arrested movement) and movement. The control of posture and movement in attaining a state of balance is often termed postural control and describes the motor action that occurs following the integration of sensory, perceptual, cognitive and motor processes. The aims of postural control are:
Sensory input and balance
The state of balance is maintained through complex postural control mechanisms which are reliant on adequate sensory input. The principal input systems to balance are the vestibular system (S2.10), the visual system (S2.10) and the somatosensory systems (S3.23) (Massion et al. 2004). Visual input provides a reference for upright vertical but is also essential in predicting forthcoming threats to balance from the environment. The somatosensory system, primarily proprioception, provides a reference for the body’s position in relation to the supporting surface and to other body parts and finally the vestibular system provides a reference for head position and movement of the head in relation to gravity.
Integration
Integration of this sensory information for an appropriate motor response is facilitated by various higher centres, including: the brain stem and cranial nerves (S2.10); the cerebellum (S2.12); reticular formation (S2.10) and the cerebral cortex (S2.7). The amount of cognitive processing by the cortex for postural control is usually minimal, with its contribution depending on the complexity of the task and the capability of the individual’s postural control system. For example, postural control relies on accurate sensory input, but also on the ability of the central nervous system (CNS) to attend to the relevant sensory cues and to prioritize or weight the input according to its relevance to the context and task (Horak 2006). The CNS also intervenes if a sensory conflict exists when it must weight the sources and reject the potential source of error (Karnath et al. 2000b).
Motor output and balance
During movement there is inevitably a displacement of the COM in relation to the BOS. This occurs whether the movement involves the trunk, the upper limb, the lower limb, turning the head or simply breathing. What determines whether the displacement leads to a fall is the motor response by which balance is recovered. These motor adjustments are flexible and varied and dependent on the task, the environmental context and the individual. An appropriate motor response requires a certain level of muscle strength, endurance and an available range of movement (Cholewicki et al. 1997; Ebenbichler and Oddsson 2001; Hodges and Richardson 1997) but also fine grading of agonists, antagonists and synergistic muscles, appropriate co-contraction and a high level of reciprocal innervation.
Although postural control mechanisms are varied, certain patterns of activation are described, however in an adult these are integrated into movement and may not always be evident:
Movement strategies
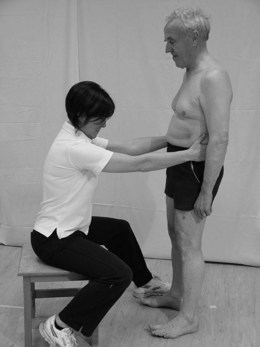
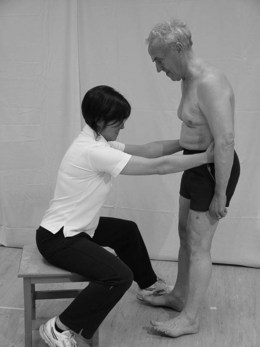
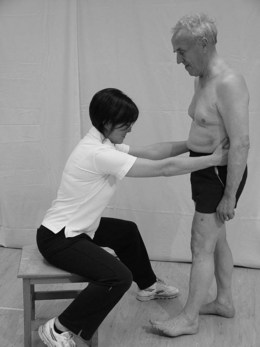
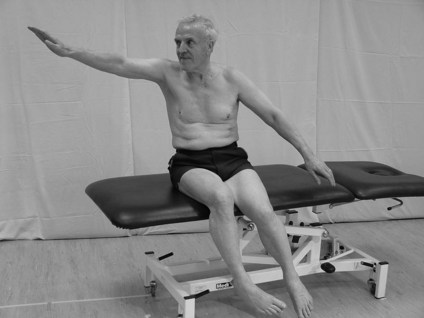
An individual can slow down the displacement of the COM by rapidly generating muscle torque at the ankles, hips or other joints around a fixed BOS. For anteroposterior displacements of the COM the predominant torque is generated via an ankle strategy (Fig. 32.1) although a hip strategy (Fig. 32.2) may also be present. For a mediolateral displacement, the hip strategy is dominant (Maki and McIlroy 2006). These strategies occur in a feed forward manner to maintain balance and are continuously interchangeable during movement. However, if the perturbation is large and these strategies are unsuccessful, the individual may actually change the BOS by stepping (Fig. 32.3) or using an outstretched arm. Although the latter response is often referred to as protective it can also occur during small perturbations as a normal strategy for balance.
Balance reactions
Equilibrium reactions
These are subtle changes in muscle tone required to maintain equilibrium and are analogous with postural sway (Fig. 32.4). When people stand with their eyes closed, postural sway may increase by 20–70% (Lord and Menz 2000).
Righting reactions
The existence of righting reactions in a mature adult is debated as it is proposed that they become integrated with equilibrium reactions by age 3 months. However, as the debate appears to be one of terminology and is as yet unresolved, this text describes the two phenomena separately.
Righting reactions occur in response to displacement of the COM beyond the stability limits in an attempt to regain equilibrium. They are a basic component in maintaining equilibrium while changing between positions and hence during movement. Righting reactions may involve the head (moving on the trunk to maintain the head in vertical), the trunk (in response to weight transfer or head/limb movement) or limb movement (acting as a counter balance to offset the displacement of COM) (Fig. 32.5).
Why do we need to assess balance?
Balance impairments have been shown to increase the risk of falls (S3.34) resulting in high economic costs and social problems (Lamb et al. 2003; Harris et al. 2005; Belgen et al. 2006). Balance problems in neurologically impaired patients are common, being associated with the following impairments:
Motor dysfunction
Musculoskeletal
Biomechanics
Sensory dysfunction
Altered sensory integration
![]() Clinical hints and tips
Clinical hints and tips
It is interesting that in healthy subjects our perceived stability limit and the consequent motor response may be altered if we fear a threat to our balance (e.g. icy ground or wet floor). This is highly relevant in patients who readily lose confidence and as a consequence, they may limit themselves functionally over time.
How do I assess balance?
The state of balance is primarily a background to performing a movement and in the main is automatically controlled. Therefore it should be assessed in this context, that is, during performance of a task or function. However, several options are available to the therapist.
Functional observation
Patient
In order to assess balance in context the patient should be requested to perform a functional activity. The choice of activity will be dependent on the patient’s ability.
Therapist
Recording
A simple text description of the therapist’s assessment and findings is sufficient. This should include the patient’s functional ability to balance and some description related to the quality of the motor response.
Example
Patient is sitting – Pt is able to sit unsupported for a limited time (10 seconds) and maintains this posture using excessive activity around both hips. Postural sway is normal.
Patient was able to lift both hands off his lap for approx. 2 seconds, during which he became anxious. Further assessment was inappropriate.
Analysis
Postural control is hugely complex and therefore simple balance measures are unlikely to identify the specific deficits of the sensorimotor processes. Comprehensive assessment is required to evaluate the potential impairments implicated in a deficit of balance. Therefore the findings from your balance assessment must be considered in conjunction with the findings from other assessment tools (S3.19–34). Particular attention should be paid to vision (S3.27) and sensory testing (S3.23) and if a lesion of the vestibular system is suspected, referral to a specialist unit is advised. However, trunk stability, muscle tone, alignment, pain, strength, range of movement and cognition/perception may also be linked to reduced balance.
In the above example, the patient maintains balance in sitting using an ineffective compensatory strategy. His underlying balance deficit is related to hypotonia of his trunk, based on other findings. He also appears to have developed an altered perception of his stability limits as he becomes anxious without apparent need. This could limit the voluntary use of his upper limbs in the future.
Outcome measures
Research
Posturography refers to any technique used to quantify postural control in standing. These objective quantitative measures of balance can assess with greater sensitivity than observation by the therapist (De Oliveira 2008). Postural reactions can be quantified on force platforms with the sensory environment being manipulated to challenge different systems of balance. However, the output from a force platform does not tell the therapist about the quality of the postural control mechanisms.
References and Further Reading
Au-Yeung SS, Ng JT, Lo SK. Does balance or motor impairment of limbs discriminate the ambulatory status of stroke survivors? American Journal of Physical Medicine and Rehabilitation. 2003;824:279-283.
Belgen B, Beninato M, Sullivan PE, et al. The association of balance capacity and falls self-efficacy with history of falling in community-dwelling people with chronic stroke. Archives of Physical Medicine and Rehabilitation. 2006;874:554-561.
Bonan IV, Colle FM, Guichard JP, et al. Reliance on visual information after stroke, Part I: Balance on dynamic posturography. Archives of Physical Medicine Rehabilitation. 2004;852:268-273.
Bonan IV, Guettard E, Leman MC. Subjective visual vertical perception relates to balance in acute stroke. Archives of Physical Medicine Rehabilitation. 2006;875:642-646.
Brown LA, Sleik RJ, Winder TR. Attentional demands for static postural control after stroke. Archives of Physical Medicine Rehabilitation. 2002;8312:1732-1735.
Brown LA, Cooper SA, Doan JB, et al. Parkinsonian deficits in sensory integration for postural control: temporal response to changes in visual input. Parkinsonism Related Disorders. 2006;12:376-381.
Chen IC, Cheng PT, Hu AL, et al. Balance evaluation in hemiplegic stroke patients. Chan Gung Medical. 2000;J236:339-347.
Cholewicki J, Panjabi M, Khachatryan A. Stabilizing function of trunk flexor and extensor muscles around a neutral spine posture. Spine. 1997;22:2207-2212.
Danells CJ, Black SE, Gladstone DJ, et al. Poststroke ‘pushing’: Natural history and relationship to motor and functional recovery. Stroke. 2004;3512:2873-2878.
De Haart M, Geurts AC, Huidekoper SC, et al. Recovery of standing balance in postacute stroke patients: a rehabilitation cohort study. Archives of Physical Medicine Rehabilitation. 2004;856:886-895.
De Nunzio AM, Nardone A, Schieppati M. The control of equilibrium in Parkinson’s disease patients: delayed adaptation of balancing strategy to shifts in sensory set during a dynamic task. Brain Research Bulletin. 2007;74:258-270.
De Oliveira CB, de Medeiros IR, Frota NA, et al. Balance control in hemiparetic stroke patients: main tools for evaluation. Journal of Rehabilitation Research and Development. 2008;468:1216-1228.
Ebenbichler G, Oddsson L. Sensory-motor control of the lower back: implications for rehabilitation. Medicine and Science in Sports and Exercise. 2001;33:1889-1898.
Garland SJ, Ivanova TD, Mochizuki G. Recovery of standing balance and health-related quality of life after mild or moderately severe stroke. Archives of Physical Medicine Rehabilitation. 2007;882:218-227.
Gustafson Y. Falls and injuries after stroke: time for action!. Stroke. 2003;342:494-501.
Harris JE, Eng JJ, Marigold DS, et al. Relationship of balance and mobility to fall incidence in people with chronic stroke. Physical Therapy. 2005;852:150-158.
Hodges P, Richardson C. Relationship between limb movement speed and associated contraction of the trunk muscles. Ergonomics. 1997;40:1220-1230.
Horak FB. Postural orientation and equilibrium: what do we need to know about neural control of balance to prevent falls? Age Ageing. 2006;35(Suppl 2):7-11.
Horak FB, Henry SM, Shumway-Cook A. Postural perturbations: new insights for treatment of balance disorders. Physical Therapy. 1997;775:517-533.
Karnath HO, Broetz D. Understanding and treating ‘pusher syndrome’. Physical Therapy. 2003;8312:1119-1125.
Karnath HO, Ferber S, Dichgans J. The origin of contraversive pushing: evidence for a second graviceptive system in humans. Neurology. 2000;559:1298-1304.
Karnath HO, Ferber S, Dichgans J. The neural representation of postural control in humans. Proceedings of the National Academy of Science USA. 2000;9725:13931-13936.
Karatas M, Cetin N, Bayramoglu M, et al. Trunk muscle strength in relation to balance and functional disability in unihemispheric stroke patients. American Journal of Physical Medicine and Rehabilitation. 2004;832:81-87.
Lamb SE, Ferrucci L, Volapto S, et al. Risk factors for falling in home-dwelling older women with stroke: the Women’s Health and Aging Study. Stroke. 2003;342:494-501.
Lord SR, Menz HB. Visual contributions to postural stability in older adults. Gerontology. 2000;46:306-310.
Maki BE, McIlroy WE. The role of limb movements in maintaining upright stance: the ‘change-in-support’ strategy. Physical Therapy. 1997;775:488-507.
Maki BE, McIlroy WE. Control of rapid limb movements for balance recovery: age-related changes and implications for fall prevention. Age and Ageing. 2006;35-S2:12-18.
Mancini M, Rocchi L, Horak FB, et al. Effects of Parkinson’s disease and levodopa on functional limits of stability. Clinical Biomechanics. 2008;23:450-458.
Massion J, Alexandrov A, Frolov A. Why and how are posture and movement coordinated? Progress in Brain Research. 2004;1432:13-27.
Niam S, Cheung W, Sullivan PE, et al. Balance and physical impairments after stroke. Archives of Physical Medicine Rehabilitation. 1999;80(10):1227-1233.
Oie KS, Kiemel T, Jeka JJ. Multisensory fusion: simultaneous re-weighting of vision and touch for the control of human posture. Brain Research Cognitive Brain Research. 2002;141:164-176.
Oxford Dictionary. Online www.askoxford.com/?view=uk
Peterka JR. Sensorimotor integration in human postural control. Journal of Neurophysiology. 2002;883:1097-1118.
Peterka RJ, Loughlin PJ. Dynamic regulation of sensorimotor integration in human postural control. Journal of Neurophysiology. 2004;911:410-423.
Stapleton T, Ashburn A, Stack E. A pilot study of attention deficits balance control and falls in the acute stage following stroke. Clinical Rehabilitation. 2001;15:437-444.
Stokes M. Physical management in neurological rehabilitation, ed 2. Edinburgh: Elsevier/Mosby; 2004.
Tyson SF, DeSouza LH. Reliability and validity of functional balance tests post stroke. Clinical Rehabilitation. 2004;188:916-923.
Tyson SF, Hanley M, Chillala J, et al. Balance disability after stroke. Physical Therapy. 2006;861:30-38.
Vaugoyeau M, Viel S, Assaiante C, et al. Impaired vertical postural control and proprioceptive integration deficits in Parkinson’s disease. Neuroscience. 2007;146:852-863.
Verheyden G, Vereeck L, Truijen S, et al. Trunk performance after stroke and the relationship with balance gait and functional ability. Clinical Rehabilitation. 2006;205:451-458.
Yelnik AP, Lebreton FO, Bonan IV, et al. Perception of verticality after recent cerebral hemispheric stroke. Stroke. 2002;339:2247-2253.