CHAPTER 31 Myotomes
What is a myotome?
A myotome is defined as the group of muscles supplied by one spinal nerve root level. There are 31 pairs of spinal nerves (S2.13) each contributing to the innervations of many muscles (e.g. C5 innervates parts of supraspinatus, infraspinatus, deltoid and biceps). The muscles supplied by a single nerve root level are generally involved in a common muscle action/s and it is this muscle action that is assessed. The list below identifies a simplified version of the actions associated with each spinal nerve root level (Grieve 2004).
Why do I need to assess myotomes?
Assessing a myotome gives information related to nerve integrity, in other words, whether the nerve pathway from the spinal cord to the muscle is intact. The assessment evaluates the strength of the muscle contraction, however it should be remembered that a weak muscle could be the result of a lesion anywhere along the nerve pathway but also of the muscle itself. Knowledge of the muscles supplied by the spinal nerve root (myotome) and the peripheral nerve allows the therapist to differentiate between lesions of each (Petty 2006). A complete lesion of the peripheral nerve will lead to complete paralysis of the muscles innervated by that nerve. Therefore, weakness will be evident immediately on testing and muscle atrophy will occur over time. However, the presentation of a lesion to a single nerve root will be more difficult to recognize because the muscle itself will still be innervated by other unaffected root levels within the peripheral nerve. For example, the biceps muscle is supplied by the musculocutaneous nerve (C5/6/7). Therefore, any lesion affecting C6 nerve root will present as minor weakness because sufficient motor units can be recruited via the remaining root levels C5/7. However, if the therapist provides resistance over a period of time (5–10 seconds) the weakness may become evident.
![]() Caution
Caution
A motor loss related to a single myotome may be indicative of a lesion at the spinal nerve root but must be confirmed by a similar finding for that particular root level for dermatomes (S3.24) and reflexes (S3.22).
In terms of neurologically impaired patients, the clinical presentation of any motor loss only requires assessment using myotomes when there is involvement of either the spinal cord specifically or the peripheral nervous system, e.g. spinal cord injury (SCI) and Guillain–Barré syndrome (GBS). As neither of these pathologies affects the spinal nerve root in isolation, myotome testing is less clinically useful as a diagnostic tool, however it is a very useful way of mapping the motor loss. The map produced gives the therapist a highly relevant outcome measure, by which the extent and level of motor loss can first be estimated and then re-evaluated. This is especially important in recovering conditions, such as GBS and in SCI, where a rising level of motor loss may reflect a serious deterioration of the injury.
How do I assess a myotome?
Patient
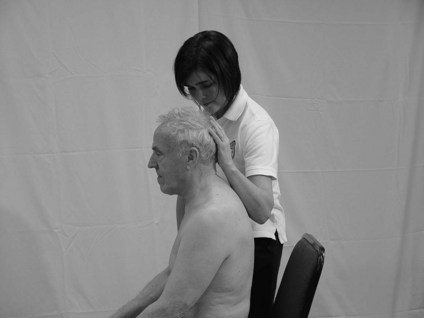
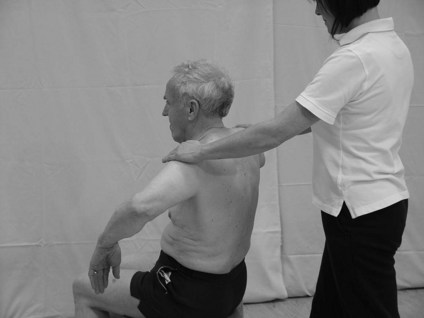
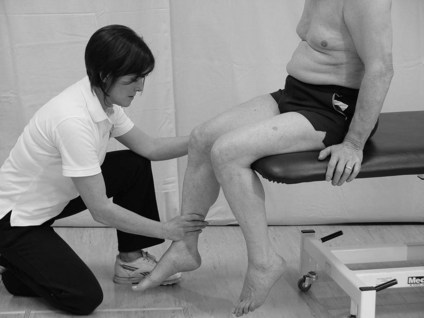
For testing the upper limb, the posture of sitting should be acceptable. To complete the lower limb assessment sitting, supine or prone may be necessary.
Therapist
Recording
The therapist should note all the muscle actions that present with weakness. A simple statement of what was assessed and a list of abnormal findings is sufficient. In the case of GBS and SCI, the loss may be extensive but detailed analysis is crucial and may be easier to record on a body chart.
Analysis
The findings of weakness related to a single myotome should be analysed along with any abnormal findings from dermatome testing and reflexes. The findings from all three assessments can be used to identify specifically the level and extent of a lesion or if relevant to differentiate a spinal nerve root deficit.