The respiratory history
Presenting symptoms (see List 9.1)
COUGH AND SPUTUM
Cough is a common presenting respiratory symptom. It occurs when deep inspiration is followed by explosive expiration. Flow rates of air in the trachea approach the speed of sound during a forceful cough. Coughing enables the airways to be cleared of secretions and foreign bodies.
The duration of a cough is important (see Questions box 9.1). Find out when the cough first became a problem. A cough of recent origin, particularly if associated with fever and other symptoms of respiratory tract infection, may be due to acute bronchitis or pneumonia. A chronic cough (of more than 8 weeks duration) associated with wheezing may be due to asthma; sometimes asthma can present with just cough alone. A change in the character of a chronic cough may indicate the development of a new and serious underlying problem (e.g. infection or lung cancer).
A differential diagnosis of cough based on its character is shown inTable 9.1 and on its duration is shown in List 9.2.
TABLE 9.1
Differential diagnosis of cough based on its character
| Origin | Character | Causes |
| Nasopharynx/larynx | Throat clearing, chronic | Postnasal drip, acid reflux |
| Larynx | Barking, painful, acute or persistent | Laryngitis, pertussis (whooping cough), croup |
| Trachea | Acute, painful | Tracheitis |
| Bronchi | Intermittent, sometimes productive, worse at night | Asthma |
| Worse in morning | Chronic obstructive pulmonary disease (COPD) | |
| With blood | Bronchial malignancy | |
| Lung parenchyma | Dry then productive | Pneumonia |
| Chronic, very productive | Bronchiectasis | |
| Productive, with blood | Tuberculosis | |
| Irritating and dry, persistent | Interstitial lung disease | |
| Worse on lying down, sometimes with frothy sputum | Pulmonary oedema | |
| ACE inhibitors | Dry, scratchy, persistent | Medication-induced |
A cough associated with a postnasal drip or sinus congestion or headaches may be due to the upper airway cough syndrome, which is the single most common cause of chronic cough. Although patients with this problem often complain of a cough, when asked to demonstrate their cough they do not cough but clear the throat. This annoys chest doctors (who feel their time is valuable) intensely.
An irritating, chronic dry cough can result from oesophageal reflux and acid irritation of the lungs. There is some controversy about these as causes of true cough. A similar dry cough may be a feature of late interstitial lung disease or associated with the use of the angiotensin-converting enzyme (ACE) inhibitors—drugs used in the treatment of hypertension and cardiac failure. Cough that wakes a patient from sleep may be a symptom of cardiac failure or of the reflux of acid from the oesophagus into the lungs that can occur when a person lies down. A chronic cough that is productive of large volumes of purulent sputum may be due to bronchiectasis.
Some patients feel the need to cough after an ectopic heartbeat. There may be an associated sensation of a missed heartbeat.
Patients’ descriptions of their cough may be helpful. In children, a cough associated with inflammation of the epiglottis may have a muffled quality and cough related to viral croup is often described as ‘barking’. Cough caused by tracheal compression by a tumour may be loud and brassy. Cough associated with recurrent laryngeal nerve palsy has a hollow sound because the vocal cords are unable to close completely; this has been described as a bovine cough. A cough that is worse at night is suggestive of asthma or heart failure, while coughing that comes on immediately after eating or drinking may be due to incoordinate swallowing or oesophageal reflux or, rarely, a tracheo-oesophageal fistula.
It is an important (though perhaps a somewhat unpleasant task) to enquire about the type of sputum produced and then to look at it, if it is available. Be warned that some patients have more interest in their sputum than others and may go into more detail than you really want. A large volume of purulent (yellow or green) sputum suggests the diagnosis of bronchiectasis or lobar pneumonia. Foul-smelling dark-coloured sputum may indicate the presence of a lung abscess with anaerobic organisms. Pink frothy secretions from the trachea, which occur in pulmonary oedema, should not be confused with sputum. It is best to rely on the patient’s assessment of the taste of the sputum, which, not unexpectedly, is foul in conditions like bronchiectasis or lung abscess.
HAEMOPTYSIS
Haemoptysis (coughing up of blood) can be a sinister sign of lung disease (see Table 9.2) and must always be investigated. It must be distinguished from haematemesis (vomiting of blood) and from nasopharyngeal bleeding (see Table 9.3).
TABLE 9.2
Causes (differential diagnosis) of haemoptysis and typical histories
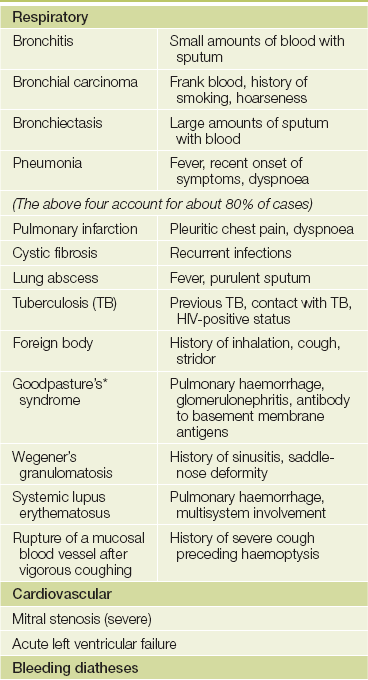
Note: Exclude spurious causes, such as nasal bleeding or haematemesis.
*Ernest W Goodpasture (1886–1960), pathologist at Johns Hopkins, Baltimore. He described this syndrome in 1919.
TABLE 9.3
Features distinguishing haemoptysis from haematemesis and nasopharyngeal bleeding
| Favours haemoptysis | Favours haematemesis | Favours nasopharyngeal bleeding |
| Mixed with sputum | Follows nausea | Blood appears in mouth |
| Occurs immediately after coughing | Mixed with vomitus; follows dry retching |
Ask how much blood has been produced. Mild haemoptysis usually means less than 20 mL in 24 hours. It appears as streaks of blood discolouring sputum. Massive haemoptysis is more than 250 mL of blood in 24 hours and represents a medical emergency. Its most common causes are carcinoma, cystic fibrosis, bronchiectasis and tuberculosis.
BREATHLESSNESS (DYSPNOEA)
The awareness that an abnormal amount of effort is required for breathing is called dyspnoea. It can be due to respiratory or cardiac disease, or lack of physical fitness or sometimes to anxiety (see List 9.3). Careful questioning about the timing of onset, severity and pattern of dyspnoea is helpful in making the diagnosis (see Questions box 9.2 and List 9.4).1 The patient may be aware of this only on heavy exertion or have much more limited exercise tolerance. Dyspnoea can be graded from I to IV based on the New York Heart Association classification:
| Class I | Disease present but no dyspnoea or dyspnoea only on heavy exertion. |
| Class II | Dyspnoea on moderate exertion. |
| Class III | Dyspnoea on minimal exertion. |
| Class IV | Dyspnoea at rest. |
It is more useful, however, to determine the amount of exertion that actually causes dyspnoea—that is, the distance walked or the number of steps climbed.
The association of dyspnoea with wheeze suggests airways disease, which may be due to asthma or chronic obstructive pulmonary disease (COPD; see List 9.5). The duration and variability of the dyspnoea are important. Dyspnoea that worsens progressively over a period of weeks, months or years may be due to interstitial lung disease (ILD). Dyspnoea of more rapid onset may be due to an acute respiratory infection (including bronchopneumonia or lobar pneumonia) or to pneumonitis (which may be infective or secondary to a hypersensitivity reaction). Dyspnoea that varies from day to day or even from hour to hour suggests a diagnosis of asthma. Dyspnoea of very rapid onset associated with sharp chest pain suggests a pneumothorax (see List 9.6). Dyspnoea that is described by the patient as inability to take a breath big enough to fill the lungs and associated with sighing suggests anxiety. Dyspnoea that occurs on moderate exertion may be due to the combination of obesity and a lack of physical fitness (‘deconditioning’; a not uncommon occurrence).
WHEEZE
A number of conditions can cause a continuous whistling noise that comes from the chest (rather than the throat) during breathing. These include asthma or COPD, infections such as bronchiolitis and airways obstruction by a foreign body or tumour. Wheeze is usually maximal during expiration and is accompanied by prolonged expiration. This must be differentiated from stridor (see below), which can have a similar sound, but is loudest over the trachea and occurs during inspiration.
CHEST PAIN
Chest pain due to respiratory disease is usually different from that associated with myocardial ischaemia (page 95). The pleura and central airways have pain fibres and may be the source of respiratory pain. Pleural pain is characteristically pleuritic in nature: sharp and made worse by deep inspiration and coughing. It is typically localised to one area of the chest. It may be of sudden onset in patients with lobar pneumonia, pulmonary embolism and infarction or pneumothorax, and is often associated with dyspnoea. The sudden onset of pleuritic chest pain and dyspnoea is an urgent diagnostic problem, as all three of these conditions may be life-threatening if not treated promptly.
Other presenting symptoms
Bacterial pneumonia is an acute illness in which prodromal symptoms (fever, malaise and myalgia) occur for a short period (hours) before pleuritic pain and dyspnoea begin. Viral pneumonia is often preceded by a longer (days) prodromal illness. Patients may occasionally present with episodes of fever at night. Tuberculosis, pneumonia and lymphoma should always be considered in these cases. Occasionally, patients with tuberculosis present with episodes of drenching sweating at night.
Hoarseness or dysphonia (an abnormality of the voice) may sometimes be considered a respiratory system symptom. It can be due to transient inflammation of the vocal cords (laryngitis), vocal cord tumour or recurrent laryngeal nerve palsy.
Sleep apnoea is an abnormal increase in the periodic cessation of breathing during sleep. Patients with obstructive sleep apnoea (OSA, where airflow stops during sleep for periods of at least 10 seconds and sometimes for more than 2 minutes, despite persistent respiratory efforts) typically present with daytime somnolence, chronic fatigue, morning headaches and personality disturbances. Very loud snoring may be reported by anyone within earshot. These patients are often obese and hypertensive. The Epworth sleepiness scale is a way of quantifying the severity of sleep apnoea (see List 9.7). Patients with central sleep apnoea (where there is cessation of inspiratory muscle activity) may also present with somnolence but do not snore excessively (see Table 9.4).
TABLE 9.4
Abnormal patterns of breathing
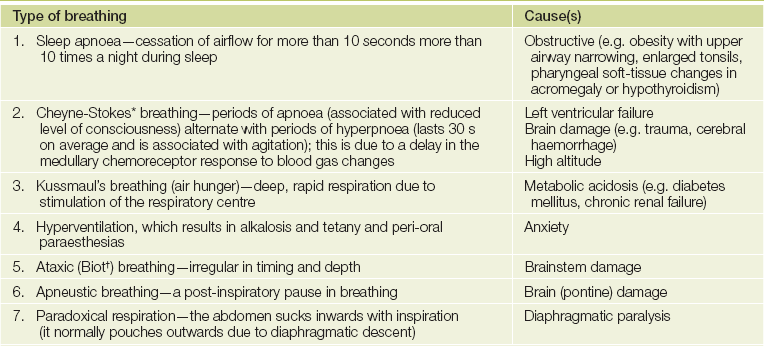

*John Cheyne (1777-1836), Scottish physician who worked in Dublin, described this in 1818. William Stokes (1804-1878), Irish physician, described it in 1854.
†Camille Biot (1878-1936), French physician.
Some patients respond to anxiety by increasing the rate and depth of their breathing. This is called hyperventilation. The result is an increase in CO2 excretion and the development of alkalosis—a rise in the pH of the blood. These patients may complain of variable dyspnoea; they have more difficulty breathing in than out. The alkalosis results in paraesthesias of the fingers and around the mouth, light-headedness, chest pain and a feeling of impending collapse.
Treatment
It is important to find out what drugs the patient is using (see List 9.8), how often they are taken and whether they are inhaled or swallowed. The patient’s previous and current medications may give a clue to the current diagnosis. Bronchodilators and inhaled steroids are prescribed for COPD and asthma. A patient’s increased use of bronchodilators suggests poor control of asthma and the need for review of treatment. Chronic respiratory disease, including sarcoidosis, hypersensitivity pneumonias and asthma, may have been treated with oral steroids. Oral steroid use may predispose to tuberculosis or pneumocystis pneumonia. Patients with chronic lung conditions like cystic fibrosis or bronchiectasis will often be very knowledgeable about their treatment and can describe the various forms of physiotherapy that are essential for keeping their airways clear.
Find out whether home oxygen has been prescribed. An oxygen concentrator or oxygen cylinder may be used and the oxygen administered by a mask or with nasal prongs. The flow rate is usually 2 L/minute or more and oxygen may be prescribed for 24 hours a day in some cases. Portable oxygen cylinders and rechargeable concentrators are available. Home oxygen is expensive and the rules for its prescription are quite strict. Usually arterial blood gas measurements that show low oxygen concentrations are required before oxygen can be prescribed. For safety reasons patients must have given up smoking before home oxygen can be allowed.
Pulmonary rehabilitation courses are now commonly prescribed for patients with chronic lung disease. They involve graded exercise programs and information about ways of dealing with chronic respiratory symptoms. Find out if this has been recommended and whether it has been helpful.
Almost every class of drug can produce lung toxicity. Examples include pulmonary embolism from use of the oral contraceptive pill, interstitial lung disease from cytotoxic agents (e.g. methotrexate, cyclophosphamide, bleomycin), bronchospasm from beta-blockers or non-steroidal anti-inflammatory drugs (NSAIDs), and cough from ACE inhibitors. Some medications known to cause lung disease may not be mentioned by the patient because they are illegal (e.g. cocaine), are used sporadically (e.g. hydrochlorothiazide), can be obtained over the counter (e.g. tryptophan) or are not taken orally (e.g. timolol; beta-blocker eye drops for glaucoma). The clinician therefore needs to ask about these types of drug specifically.
Past history
Always ask about previous respiratory illness, including pneumonia, tuberculosis or chronic bronchitis, or abnormalities of the chest X-ray that have previously been reported to the patient. Many previous respiratory investigations may have been memorable, such as bronchoscopy, lung biopsy and video-assisted thoracoscopy. Spirometry, with or without challenge testing for asthma, may have been performed. Many severe asthmatics perform their own regular peak flow testing (page 163). Ask about the results of any of these investigations. Patients with the acquired immunodeficiency syndrome (AIDS) have a high risk of developing Pneumocystis jiroveci (carinii) pneumonia and indeed other chest infections, including tuberculosis.
Occupational history
In no other body system assessment are the patient’s present and previous occupations of more importance (see Table 9.5).2 A detailed occupational history is essential. The occupational lung diseases or pneumoconioses cause interstitial lung disease by damaging the alveoli and small airways. Prolonged exposure to substances whose use is now heavily restricted is usually required. Cigarette smoking has an additive effect for these patients. These occupational conditions are now rare, and the most common occupational lung disease is asthma.
TABLE 9.5
Occupational lung disease (pneumoconioses)
| Substance | Disease |
| Coal | Coal worker’s pneumoconiosis |
| Silica | Silicosis |
| Asbestos | Asbestosis |
| Talc | Talcosis |
Ask about exposure to dusts in mining industries and factories (e.g. asbestos, coal, silica, iron oxide, tin oxide, cotton, beryllium, titanium oxide, silver, nitrogen dioxide, anhydrides). Heavy exposure to asbestos can lead to asbestosis (see List 9.9), but even trivial exposure can result in pleural plaques or mesothelioma (malignant disease of the pleura). The patient may be unaware that his or her occupation involved exposure to dangerous substances; for example, factories making insulating cables and boards very often used asbestos until 25 years ago. Asbestos exposure can result in the development of asbestosis, pleural plaques, mesothelioma or carcinoma of the lung up to 30 years later. Relatives of people working with asbestos may be exposed when handling work clothes. Only very minor exposure is required for patients to develop the disease and sometimes considerable detective work is needed to work out the source of exposure. Finding the source of exposure can be important as a public health matter.
Work or household exposure to animals, including birds, is also relevant (e.g. Q fever or psittacosis, which are infectious diseases caught from animals).
Exposure to organic dusts can cause a local immune response to organic antigens and result in extensive allergic alveolitis. Within a few hours of exposure, patients develop flu-like symptoms. These often include fever, headache, muscle pains, dyspnoea without wheeze and dry cough. The culprit antigens may come from mouldy hay, humidifiers or air conditioners, among others (see Table 9.6).
TABLE 9.6
| Disorder | Source |
| Bird fancier’s lung | Bird feathers and excreta |
| Farmer’s lung | Mouldy hay or straw (Aspergillus fumigatus) |
| Byssinosis | Cotton or hemp dust |
| Cheese worker’s lung | Mouldy cheese (Aspergillus clavatus) |
| Malt worker’s lung | Mouldy malt (Aspergillus clavatus) |
| Humidifier fever | Air-conditioning (thermophilic Actinomycetes) |
It is most important to find out what the patient actually does when at work, the duration of any exposure, use of protective devices and whether other workers have become ill. An improvement in symptoms over the weekend is a valuable clue to the presence of occupational lung disease, particularly occupational asthma. This can occur as a result of exposure to spray paints or plastic or soldering fumes.
Social history
A smoking history must be routine, as it is the major cause of COPD3 and lung cancer (see List 1.2, page 11). It also increases the risk of spontaneous pneumothorax and of Goodpasture’s syndrome. It is necessary to ask how many packets of cigarettes per day the patient has smoked and how many years the patient has smoked. An estimate should be made of the number of packet-years of smoking (see Chapter 1). Occupation may further affect cigarette smokers; for example, asbestos workers who smoke are at an especially high risk of lung cancer. Passive smoking is now regarded as a significant risk for lung disease and the patient should be asked about exposure to other people’s cigarette smoke at home and at work.
Many respiratory conditions are chronic and may interfere with the ability to work and exercise as well as interfering with normal family life. In some cases involving occupational lung disease there may be compensation matters affecting the patient. Ask about these problems and whether the patient has been involved in a pulmonary rehabilitation program. Housing conditions may be inappropriate for a person with a limited exercise tolerance or an infectious disease.
An enquiry about the patient’s alcohol consumption is important. Drinking large amounts of alcohol in binges can sometimes result in aspiration pneumonia, and alcoholics are more likely to develop pneumococcal or Klebsiella pneumonia. Intravenous drug users are at risk of lung abscess and drug-related pulmonary oedema. Sexual orientation or history of intravenous drug use may be related to an increased risk of HIV infection and susceptibility to infection. Such information may influence the decision about whether to advise treatment at home or in hospital.
Family history
A family history of asthma or other atopic diseases, cystic fibrosis, lung cancer or emphysema should be sought. Alpha1-antitrypsin deficiency, for example, is an inherited disease, and those affected are extremely susceptible to the development of emphysema. A family history of infection with tuberculosis is also important. A number of pulmonary diseases may have a familial or genetic association. These include carcinoma of the lung and pulmonary hypertension.
References
1. Schmitt, BP, Kushner, MS, Wiener, SL. The diagnostic usefulness of the history of the patient with dyspnea. J Gen Intern Med. 1986; 1:386–393. [History alone was correct three out of four times when deciding the cause of dyspnoea in defined circumstances.].
2. Anonymous. Obtaining an exposure history. Agency for Toxic Substances and Disease Registry. United States Department of Health and Human Services, Public Health Service, Atlanta, Georgia. Am Fam Phys. 1993; 48:483–491.
3. Broekhuizen, BD, Sachs, AP, Oostvogels, R, Hoes, AW, Verheij, TJ, Moons, KG. The diagnostic value of history and physical examination for COPD in suspected or known cases: a systematic review. Fam Pract. 2009; 26(4):260–268. [Items of diagnostic value for COPD included a history of dyspnoea, wheezing and smoking. Items of value on examination included audible wheezing and forced expiratory time. However, the data were heterogeneous.].
 denotes symptoms for the possible diagnosis of an urgent or dangerous problem.
denotes symptoms for the possible diagnosis of an urgent or dangerous problem.