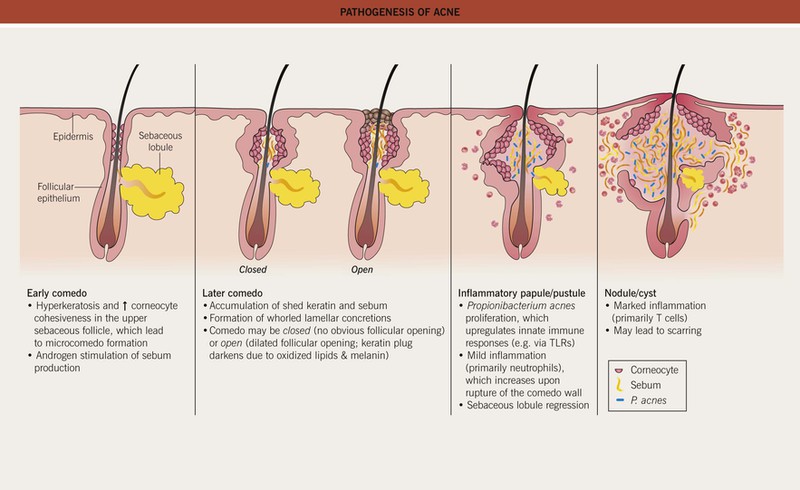
Acne Vulgaris
• Common pilosebaceous disorder that occurs in ~85% of individuals 12–24 years of age and 15–35% of adults (especially women) in their 30s–40s.
• Clinical presentations range from mild comedones to severe, explosive eruptions of suppurative nodules associated with systemic manifestations.
• May result in scarring and psychosocial repercussions such as anxiety, depression, and social withdrawal.
• A tendency to develop moderate to severe acne can run in families.
• Multiple factors affecting the pilosebaceous unit contribute to acne pathogenesis (Fig. 29.1), a process that typically begins when androgen production increases at adrenarche.
• The relationship between diet and acne is controversial, with some evidence of possible associations with milk intake (especially skim milk) and a high glycemic index diet.
Clinical Features and Variants of Acne
• Favors the face and upper trunk, sites with well-developed sebaceous glands.
– Closed comedones (whiteheads) are small (~1 mm), skin-colored papules without an obvious follicular opening (Fig. 29.2A,B).
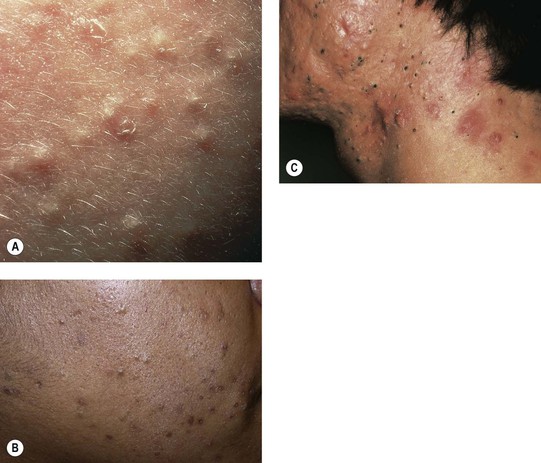
Fig. 29.2 Comedonal acne vulgaris. A Closed comedones highlighted by side lighting. B Open and closed comedones as well as post-inflammatory hyperpigmentation on the cheek. C Prominent open comedones in a patient with scarring cystic acne. A, Courtesy, Ronald P. Rapini, MD; B, Courtesy, Andrew Zaenglein, MD, and Diane Thiboutot, MD.
– Open comedones (blackheads) have a dilated follicular opening filled with a keratin plug, which has a black color due to oxidized lipids and melanin (Fig. 29.2B,C).
– Erythematous papules and pustules (Fig. 29.3A).
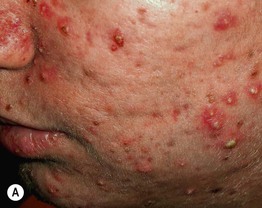
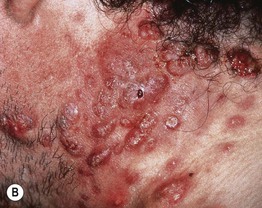
Fig. 29.3 Inflammatory acne vulgaris. A Papules, obvious pustules, and atrophic scars are present. B Severe nodulocystic acne. This form is best treated with low doses of isotretinoin initially (± a preceding course of oral antibiotics) to avoid precipitating a flare. A, Courtesy, Andrew Zaenglein, MD, and Diane Thiboutot, MD.
– Nodules and cysts filled with pus or serosanguinous fluid; may coalesce and form sinus tracts (Fig. 29.3B).
– Acne conglobata (severe nodulocystic acne) is classified in the follicular occlusion tetrad along with dissecting cellulitis of the scalp, hidradenitis suppurativa, and pilonidal cysts (see Chapter 31); it is also a part of pyogenic arthritis, pyoderma gangrenosum, and acne conglobata (PAPA) and pyoderma gangrenosum, acne, and suppurative hidradenitis (PASH) syndromes.
• Inflammatory acne commonly results in post-inflammatory hyperpigmentation, especially in patients with darker skin, which fades slowly over time (Fig. 29.4A); nodulocystic acne (and less frequently other inflammatory > comedonal forms) often leads to pitted (Fig. 29.4B) or hypertrophic scars (the latter especially on the trunk; see Fig. 81.4).
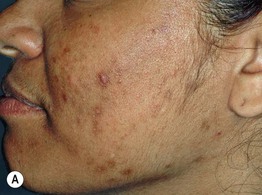
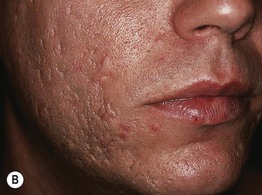
Fig. 29.4 Sequelae of acne. A Post-inflammatory hyperpigmentation. Such pigmentary changes are most common in patients with darker skin colors. B ‘Ice-pick’ scarring secondary to nodulocystic acne. A, Courtesy, Andrew Zaenglein, MD, and Diane Thiboutot, MD.
Post-Adolescent Acne
• Age >25 years; favors women.
• Tends to flare in the week prior to menstruation; up to one-third of these women have hyperandrogenism.
• Typically features papulonodules on the lower face, jawline, and neck.
Acne Excoriée
• Favors teenage girls and young women.
• Habitual picking at comedones and inflammatory papules, resulting in crusted erosions (often linear/angular) and potential scarring (see Fig. 5.3).
• Some patients have an underlying obsessive–compulsive or anxiety disorder.
Acne Fulminans
• Favors boys 13 to 16 years of age.
• Sudden development of numerous, markedly inflamed nodular lesions on the face, trunk, and upper arms.
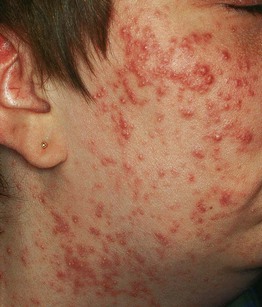
• Coalescence into painful, oozing, friable plaques with hemorrhagic crusting, erosion/ulceration, and eventual scarring (Fig. 29.5).
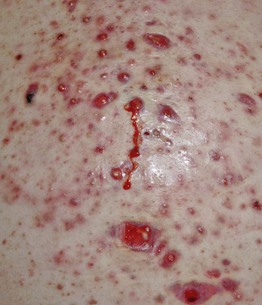
Fig. 29.5 Acne fulminans. Inflamed, friable papulopustules and plaques with erosions, oozing, and formation of granulation tissue. Courtesy, Julie V. Schaffer, MD.
• Systemic manifestations include fever, malaise, myalgias, arthralgias, osteolytic bone lesions (most often of clavicles and sternum), and hepatosplenomegaly.
• Laboratory findings: leukocytosis and increased ESR > anemia, microscopic hematuria, and proteinuria.
• DDx: an acne fulminans-like flare occasionally develops upon initiation of isotretinoin therapy for acne, and acne fulminans can be associated with synovitis, acne, pustulosis, hyperostosis, and osteitis (SAPHO) syndrome (see Chapter 21).
• Rx: isotretinoin (low dose initially with slow escalation) plus prednisone.
Solid Facial Edema (Morbihan's Disease)
• Woody induration ± erythema of the central face in the setting of chronic inflammation due to acne vulgaris or rosacea (Fig. 29.6).
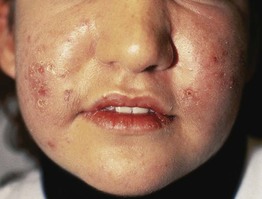
Fig. 29.6 Solid facial edema due to acne vulgaris. There is soft tissue swelling in the central portion of the face. Courtesy, Andrew Zaenglein, MD, and Diane Thiboutot, MD.
Neonatal Acne (Neonatal Cephalic Pustulosis) (See Chapter 28)
• Facial papulopustular eruption thought to be triggered by Malassezia spp.; comedones are not present.
Infantile Acne
• Ages 3 months to 2 years; favors boys.
• Facial comedones, papulopustules, and cysts as in classic acne (Fig. 29.7); may result in scarring.
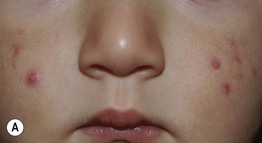
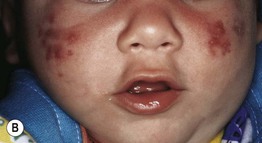
Fig. 29.7 Infantile acne. Presentations can range from scattered papulopustules (A) to multiple coalescing papulonodules and inflammatory cysts (B). If the latter child failed to improve with a topical retinoid plus an oral antibiotic, consideration would be given to oral isotretinoin. Courtesy, Kalman Watsky, MD.
• Reflects physiologic elevation of androgen levels in infants 6–12 months of age (especially boys); patients often have a family history of severe acne.
• Rx: similar to adolescent acne; typically resolves within 1–2 years, becoming quiescent until puberty.
Contact Acne
• Acne mechanica: comedogenesis due to chronic friction/occlusion from objects such as chin straps, helmets, collars, and musical instruments (e.g. ‘fiddler’s neck’ in a violinist).
• Acne cosmetica, pomade acne, and occupational acne: comedogenesis caused by exposure to follicle-occluding substances in cosmetics, hair products (favoring forehead and temples), and materials used in the workplace (e.g. cutting oils, coal tar derivatives).
Chloracne
• Results from exposure (usually occupational) to halogenated aromatic hydrocarbons (e.g. polychlorinated dibenzodioxins and dibenzofurans) in agents such as herbicides and insecticides.
• Comedones and cystic papulonodules develop within 2 months of exposure, favoring malar and retroauricular areas of the face (see Fig. 12.18) as well as the axillae and scrotum; often persists for years.
Drug-Induced Acne and Acneiform Eruptions
• Systemic CS can trigger an eruption of monomorphous follicular papulopustules favoring the upper trunk (Fig. 29.8).
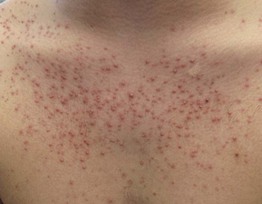
Fig. 29.8 Acneiform eruption secondary to systemic corticosteroid therapy. Abrupt eruption of monomorphous follicular papulopustules on the trunk. Courtesy, Scott Jackson, MD, and Lee T. Nesbitt, Jr., MD.
• Acneiform eruptions represent a frequent side effect of epidermal growth factor receptor (EGFR) inhibitors (e.g. cetuximab, erlotinib) used to treat solid tumors; patients present with follicular pustules and papules on the face (Fig. 29.9), scalp, and upper trunk, usually 1–3 weeks after beginning treatment, which may correlate with a therapeutic response.
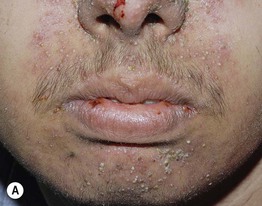
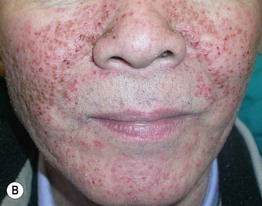
Fig. 29.9 Acneiform eruptions due to epidermal growth factor receptor inhibitors. A, B Numerous monomorphous follicular pustules and crusted papules on the face of two patients treated with erlotinib. A, Courtesy, Julie V. Schaffer, MD; B, Courtesy, Andrew Zaenglein, MD, and Diane Thiboutot, MD.
• Other common causes of drug-induced acne include anabolic steroids, bromides (found in sedatives and cold remedies), iodides (found in contrast dyes and supplements), isoniazid (Fig. 29.10), lithium, phenytoin, and progestins.
Acne Associated with a Syndrome
• Examples include Apert, PAPA, PASH, and SAPHO (see Ch. 21) syndromes.
Evaluation and Treatment of Acne
• Table 29.1 lists key components in the history and physical examination of an acne patient.
Table 29.1
History and physical examination of the acne patient.
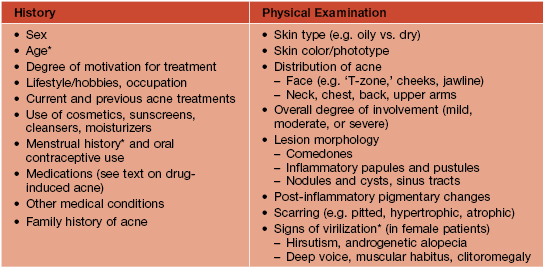
* Hyperandrogenism should be suspected in children who develop acne between 2 and 7 years of age, in older adolescents/women with irregular menses, and in female patients with signs of virilization; evaluation often includes serum levels of testosterone (total and free), DHEAS, and 17-hydroxyprogesterone (see Fig. 57.10) as well as hand/wrist x-rays to evaluate bone age in prepubertal children.
• DDx: presented in Table 29.2.
Table 29.2
Differential diagnosis of acne vulgaris.
Folliculotropic mycosis fungoides can mimic comedonal or inflammatory acne.
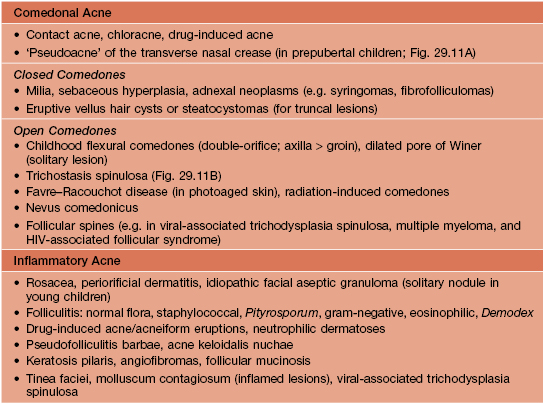
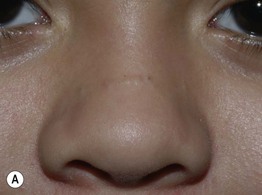
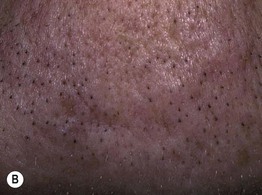
Fig. 29.11 Disorders in the differential diagnosis of comedonal acne vulgaris. A ‘Pseudoacne’ of the transverse nasal crease in a young child. Note the milia and comedones located along this anatomical demarcation line. B Trichostasis spinulosa. Multiple vellus hairs and keratinous debris are found within the dilated follicular orifices. A, Courtesy, Julie V. Schaffer, MD; B, Courtesy, Judit Stenn, MD.
• Rx: outlined in Table 29.3.
Table 29.3
Treatment of acne vulgaris.
Lack of response should prompt consideration of noncompliance and alternative diagnoses. In general, monotherapy with a topical or oral antibiotic should be avoided. Laser (e.g. 1450-nm diode), light (e.g. blue, intense pulsed), or photodynamic therapies may be of benefit to some patients but are not first-line, and superficial chemical peels (e.g. 20–30% salicylic acid, 30–50% glycolic acid) are occasionally useful to reduce comedones.

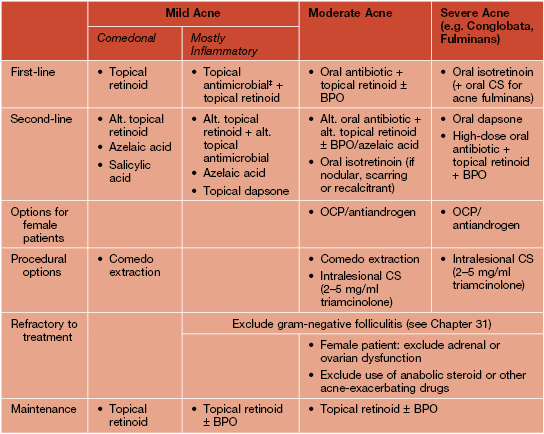
* Tretinoin is photolabile and inactivated by BPO (so generally applied at night, separately from BPO); tazarotene is the most irritating of the topical retinoids (see text) and is pregnancy category X.
** Can bleach clothing/bedding and cause contact dermatitis (irritant > allergic); unlike topical antibiotics, bacterial resistance does not occur.
† Increased effectiveness when used in conjunction with BPO or a retinoid.
§ Severe teratogenicity; in the United States, prescribers and patients must register in a risk management program (iPLEDGE™) that requires monthly visits. The most common side effects are cheilitis > mucosal dryness (ocular, nasal) and xerosis (Fig. 29.12).
‡ BPO ± a topical antibiotic may also be used as monotherapy, especially as an initial treatment in a younger patient.
Alt, alternative; EE, ethinyl estradiol; OCP, oral contraceptive pill.
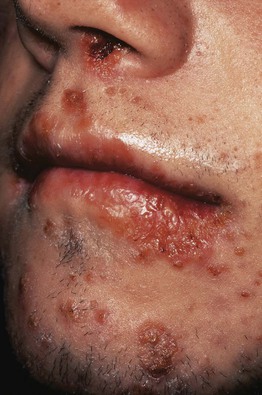
Fig. 29.12 Impetigo in a patient receiving isotretinoin. Multiple serous crusts are evident. Dryness and fragility of the skin, lips, and nasal mucosa in patients treated with isotretinoin increase susceptibility to staphylococcal infections.
• Once active acne has been successfully treated, intralesional CS (for hypertrophic scars) or surgical modalities (e.g. fractional or traditional laser resurfacing, dermabrasion, fillers) can be used for residual scarring if needed.
Tips for Topical Therapy
• Lack of compliance is often an issue, with common reasons including irritated skin, busy schedules, and giving up when the response is not rapid; substantial benefit typically requires 6–8 weeks of treatment.
• The main side effect of topical medications is irritation, which is most problematic in adolescents with atopic dermatitis and adults.
• Patients should be advised to avoid harsh scrubs, other irritating agents (e.g. toners, acne products that are not part of the regimen), and manipulation of lesions, especially inflammatory papulonodules and closed comedones.
• Even if planning combination therapy, a gradual initial approach can improve tolerance in patients with sensitive skin; for example, a single agent may be used for the first 2–3 weeks (starting every other day for retinoids), followed by slow introduction of a second medication (e.g. transitioning from alternate days to daily).
• Simplifying the regimen and considering combination products (e.g. benzoyl peroxide + adapalene or clindamycin; tretinoin + clindamycin) may improve compliance, especially in less-motivated adolescents.
• In general, topical medications (especially retinoids) should be used to the entire acne-prone region rather than as ‘spot treatment’ of individual lesions.
• Patients should be instructed to select noncomedogenic products (e.g. moisturizers, sunscreens, make-up) and to avoid having oily hair or using pomades that may contribute to acne.
• Having patients bring everything that they apply to their face to a visit may help to determine the source of problems.
For further information see Ch. 36. From Dermatology, Third Edition.