The Past, Present, and Future
1 Contrast present-day concepts of maternity and child care with those of the past.
2 Recall the contributions of persons in history to the fields of maternity and pediatric care.
3 List the organizations concerned with setting standards for the nursing care of maternity and pediatric patients.
4 Name two international organizations concerned with maternity and pediatric care.
5 List three federal programs that assist mothers and infants.
6 State the influence of the federal government on maternity and pediatric care.
7 Discuss how culture affects childbirth and child care.
8 List four reasons why statistics are important.
9 Discuss common terms used in expressing vital statistics.
10 State two types of health care delivery systems in the United States.
11 Discuss the role of the advanced practice nurse.
12 List the five steps of the nursing process.
13 Understand the legal responsibilities of the nurse to report certain diseases or condition to the public health authorities.
14 Contrast a nursing care plan with a clinical pathway.
15 Define the Nursing Interventions Classification (NIC) and its relationship to the nursing process.
16 Describe the Nursing Outcomes Classification (NOC) and its influence on the nursing process.
17 Compare and contrast nursing and medical diagnosis frameworks with focus on North American Nursing Diagnosis Association International (NANDA-I) taxonomy.
19 Discuss the role of critical thinking in the nursing process and in clinical judgment.
20 Discuss the role of critical thinking as it relates to test taking and lifelong learning.
21 Discuss the objectives of Healthy People 2020 as it relates to maternity and pediatric care.
22 Examine the importance of documentation as a nursing responsibility.
23 Describe the role of the community health nurse as a health care provider.
![]() http://evolve.elsevier.com/Leifer
http://evolve.elsevier.com/Leifer
The word obstetrics is derived from the Latin term obstetrix, which means “stand by.” It is the branch of medicine that pertains to care of women during pregnancy, childbirth, and the postpartum period (puerperium). Maternity nursing is the care given by the nurse to the expectant family before, during, and following birth.
A physician specializing in the care of women during pregnancy, labor, birth, and the postpartum period is an obstetrician. These physicians perform cesarean deliveries and treat women with known or suspected obstetric problems as well as attend normal deliveries. Many family physicians and certified nurse-midwives also deliver babies.
Pediatrics is defined as the branch of medicine that deals with the child’s development and care and the diseases of childhood and their treatment. The word is derived from the Greek pais, paidos, meaning “child,” and iatreia, “cure.”
Family-centered care recognizes the strength and integrity of the family and places it at the core of planning and implementing health care. The family members as caregivers and decision makers are an integral part of both obstetric and pediatric nursing. The philosophy, goals, culture, and ethnic practices of the family contribute to their ability to accept and maintain control over the health care of family members. This control is called empowerment. The nurse’s role in maternity and pediatric family-centered care is to enter into a contract or partnership with the family to achieve the goals of health for its members.
The Past
The skill and knowledge related to obstetrics have evolved over centuries. The earliest records concerning childbirth are in the Egyptian papyruses (circa 1550 bc). Later advances were made by Soranus, a Greek physician who practiced in second-century Rome and who is known as the father of obstetrics. He instituted the practice of podalic version, a procedure used to rotate a fetus to a breech, or feet-first, position. Podalic version is important in the vaginal delivery of the second infant in a set of twins. In this procedure the physician reaches into the uterus and grasps one or both of the infant’s feet to facilitate delivery. Planned cesarean birth is safer than podalic version and today is used more often.
With the decline of the Roman Empire and the ensuing Dark Ages, scientific exploration and associated medical improvements came to a halt. During the nineteenth century, however, Karl Credé (1819-1892) and Ignaz Semmelweis (1818-1865) made contributions that improved the safety and the health of mother and child during and after childbirth. In 1884 Credé recommended instilling 2% silver nitrate into the eyes of newborns to prevent blindness caused by gonorrhea. Credé’s innovation has saved the eyesight of incalculable numbers of babies.
Semmelweis’s story is a classic in the history of maternity care. In the 1840s he worked as an assistant professor in the maternity ward of the Vienna general hospital. There he discovered a relationship between the incidence of puerperal fever (or “childbed fever”), which caused many deaths among women in lying-in wards, and the examination of new mothers by student doctors who had just returned from dissecting cadavers. Semmelweis deduced that puerperal fever was septic, contagious, and transmitted by the unwashed hands of physicians and medical students. Semmelweis’s outstanding work, written in 1861, is titled The Causes, Understanding, and Prevention of Childbed Fever. Tragically, not until 1890 was his teaching finally accepted.
Louis Pasteur (1822-1895), a French chemist, confirmed that puerperal fever was caused by bacteria and could be spread by improper handwashing and contact with contaminated objects. The simple, but highly effective, procedure of handwashing continues to be one of the most important means of preventing the spread of infection in the hospital and the home today.
Joseph Lister (1827-1912), a British surgeon influenced by Pasteur, experimented with chemical means of preventing infection. He revolutionized surgical practice by introducing antiseptic surgery.
Pediatrics
Methods of child care have varied throughout history. The culture of a society has a strong influence on standards of child care. Many primitive tribes were nomads. Strong children survived, whereas the weak were left to die. This practice of infanticide (French and Latin infans, “infant,” and caedere, “to kill”) helped to ensure the safety of the group. As tribes became settled, more attention was given to children, but they were still frequently valued only for their productivity. Certain peoples, such as the Egyptians and the Greeks, were advanced in their attitudes. The Greek physician Hippocrates (460-370 bc) wrote of illnesses peculiar to children.
In the Middle Ages, the concept of childhood did not exist. Infancy lasted until about age 7 years, at which time the child was assimilated into the adult world. The art of that time depicts children wearing adult clothes and wigs. Most children did not attend school.
Christianity had a considerable impact on child care. In the early seventeenth century, several children’s asylums were founded by Saint Vincent de Paul. Many of these eventually became hospitals, although their original concern was for the abandoned. The first children’s hospital was founded in Paris in 1802. In the United States, numerous homeless children were cared for by the Children’s Aid Society, founded in New York City in 1853. In 1855 the first pediatric hospital in the United States, The Children’s Hospital of Philadelphia, was founded.
Abraham Jacobi (1830-1919) is known as the father of pediatrics because of his many contributions to the field. The establishment of pediatric nursing as a specialty paralleled that of departments of pediatrics in medical schools, the founding of children’s hospitals, and the development of separate units for children in foundling homes and general hospitals. By the 1960s, separate pediatric units were also common in hospitals. Parents were restricted by rigid visiting hours that allowed parent-infant contact for only a few hours each day; when medically indicated, nursing mothers were allowed to enter the pediatric unit for 1 hour at a time to breastfeed their infants.
Obstetric and Pediatric Care in the United States
The immigrants who reached the shores of North America brought with them a wide variety of practices and beliefs about the birth process. Many practices were also contributed by the Native American nations. Most deliveries in the early United States were attended by a midwife or relative. One physician, Samuel Bard, who was educated outside the United States, is credited with writing the first American textbook for midwives in 1807.
As a young Harvard physician, Oliver Wendell Holmes (1809-1894) wrote a paper detailing the contagious nature of puerperal fever but he, like Semmelweis, was widely criticized by his colleagues. Eventually, the “germ theory” became accepted, and more mothers and babies began to survive childbirth in the hospital.
Before the 1900s most babies were born at home. Only very ill patients were cared for in lying-in hospitals. Maternal and child morbidity and mortality were high in such institutions because of crowded conditions and unskilled nursing care. Hospitals began to develop training programs for nurses. As the medical profession grew, physicians developed a closer relationship with hospitals. This, along with the advent of obstetric instruments and anesthesia, caused a shift to hospital care during childbirth. By the 1950s, hospital practice in obstetrics was well-established. By 1960, more than 90% of births in the United States occurred in hospitals.
However, hospital care during that time did not embrace the family-centered approach. Often the father waited in a separate room during the labor and birth of his child. The mother was often sedated with “twilight sleep” and participated little during labor and delivery. After birth the infant was not reunited with the parents for several hours, which resulted in a delay of parent-infant bonding.
Organizations concerned with setting standards for maternity and pediatric nursing developed. These included the American College of Nurse-Midwives (ACNM); the Association of Women’s Health, Obstetric, and Neonatal Nurses (AWHONN), which was formerly the Nurses Association of the American College of Obstetricians and Gynecologists (NAACOG); and the Division of Maternal Nursing within the American Nurses Association (ANA). The American Academy of Pediatrics (AAP), made up of pediatricians from across the nation, has established a position of leadership in setting health standards for children.
Government Influences in Maternity and Pediatric Care
Legislation: The high mortality of mothers and infants motivated action by the federal government to improve care. The following is a chronological list of some of the important milestones in United States history related to maternity and pediatric care and safety:
• The Sheppard-Towner Act of 1921 provided funds for state-managed programs for maternity care.
• Title V of the Social Security Act, passed in 1935, provided funds for maternity care.
• The Fair Labor Standards Act, passed in 1938, established a general minimum working age of 16 years and a minimum working age of 18 years for jobs considered hazardous. More importantly, this act paved the way for the establishment of national minimum standards for child labor and provided a means of enforcement.
• The National Institutes of Health (NIH) established support for maternity research and education (1962).
• Head Start programs were established to increase educational exposure of preschool children (1966).
• The Women’s, Infant’s and Children’s (WIC) program was established to provide supplemental food and education for families in need of assistance (1966).
• The National Center for Family Planning was established to provide contraceptive information (1970).
• In 1974, the government passed the Child Abuse Prevention and Treatment Act (CAPTA).
• In 1975, the Education for All Handicapped Children Act provided for support and public education of handicapped children.
• The Title V amendment of the Public Health Services Act established maternal-infant care centers in public clinics (1981).
• In 1982, the Community Mental Health Center was funded; and the Missing Children’s Act was passed, providing a nationwide clearinghouse for missing children.
• The Family and Medical Leave Act (FMLA) of 1993 enabled employees to take 12 weeks of unpaid leave to care for newborns or family members who were ill without losing benefits or pay status in their jobs.
• Title XIX of the Medicaid program increased access to care by indigent women (1993).
• The Health Information Portability and Accountability Act (HIPAA), enacted in 2003, set standards to protect patients’ health information. Patients are allowed access to their medical records and control over how their personal information is disclosed.
• The Health Information Technology for Economic and Clinical Health Act (HITECH) was enacted in 2009 to extend HIPAA regulations by protecting electronic health records.
Laws requiring the licensing of physicians and pharmacists indirectly affect the health of children and of the general public. Protection is also afforded by the Pure Food and Drug Act, which has allowed for governmental control over medicines, poisons, and the purity of foods. Programs for disaster relief, care and rehabilitation of handicapped children, foster child care, family counseling, family day care, protective services for abused or neglected children, and education of the public are maintained and supported by governmental and private agencies. State licensing bureaus control the regulation of motor vehicles. Car seats for infants and children are currently mandatory. Protection of the public by law enforcement agencies is important because automobile accidents rank among the leading causes of injury and death in children.
The Children’s Bureau: Lillian Wald, a nurse who was interested in the welfare of children, is credited with suggesting the establishment of a federal children’s bureau. Once the Children’s Bureau was established in 1912, it focused its attention on the problem of infant mortality. This program was then followed by one that dealt with maternal mortality. These programs eventually led to birth registration in all states. In the 1930s, the Children’s Bureau investigations led to the development of hot lunch programs in many schools. Today the Children’s Bureau is administered under the auspices of the Department of Health and Human Services.
White House Conferences: The First White House Conference on Children and Youth was called by President Theodore Roosevelt in 1909. It continues to be held every 10 years. In the White House Conference on Child Health and Protection of 1930, the Children’s Charter was written (Box 1-1). The charter lists 17 statements related to the needs of children in the areas of education, health, welfare, and protection and is considered one of the most important documents in child care history. This declaration has been widely distributed throughout the world.
The 1980 White House Conference on Families focused on involving the states at the grassroots level. A series of statewide hearings were held to identify the most pressing problems of families in the various localities. A tremendous range of viewpoints on many subjects was shared, and specific recommendations were made.
International Year of the Child: The year 1979 was designated as the International Year of the Child (IYC). Its purpose was to focus attention on the critical needs of the world’s 1.5 billion children and to inspire the nations, organizations, and individuals of the world to consider how well they provide for children (U.S. Commission of the International Year of the Child, 1980). At this time, the United Nations reaffirmed the Declaration of the Rights of the Child (Box 1-2). Two international organizations concerned with children are the United Nations International Children’s Fund (UNICEF) and the World Health Organization (WHO).
Department of Public Health: The Department of Public Health bears a great deal of responsibility for the prevention of disease and death during childhood. Preventive efforts are made on national, state, and local levels. This department sees to the inspection of the water, milk, and food supplies of communities and enforces the maintenance of proper sewage and garbage disposal. Epidemics are investigated and, when necessary, persons capable of transmitting diseases are isolated. The Department of Public Health is also concerned with the inspection of housing.
The Present
In family-centered childbearing, the family is recognized as a unique system. Every family member is affected by the birth of a child; therefore, family involvement during pregnancy and birth is seen as constructive and, indeed, necessary for bonding and support. To accommodate family needs, alternative birth centers, birthing rooms, rooming-in units, and mother-infant coupling have been developed. These arrangements are alternatives to the previous standard of separate areas for labor and delivery, which made it necessary to transport a mother from one area to another and fragmented her care.
The three separate sections of the maternity unit—labor-delivery, postpartum, and newborn nursery—have merged. The whole sequence of events may take place in one suite of labor, delivery, and recovery (LDR) rooms. The patient is not moved from one area to another, but receives care during labor and delivery and then remains in the same room to recover and care for her new infant. The rooms are often decorated to look homelike.
Freestanding birthing centers outside the traditional hospital setting are popular with low-risk maternity patients. These birthing centers provide comprehensive care, including antepartum, labor-delivery, postpartum, mothers’ classes, lactation classes, and follow-up family planning. Home birth using midwives is not a current widespread practice, because malpractice insurance is expensive and emergency equipment for unexpected complications is not available.
Financial Considerations
Cost containment is the efficient and effective use of resources. It includes monitoring and regulating expenditures of funds and involves the institution’s budget. At first, cost containment influenced maternity care by requiring the discharge of mother and newborn in 24 hours or less after delivery. As a result of problems that occurred, current legislation allows a 48-hour hospital stay for vaginal deliveries and a stay of 4 days for a cesarean section.
Changing Perceptions of Childbearing
Current maternity practice focuses on a high-quality family experience. Childbearing is seen as a normal and healthy event. Parents are prepared for the changes that take place during pregnancy, labor, and delivery. They are also prepared for the changes in family dynamics after the birth. Treating each family according to its individual needs is considered paramount.
During the 1950s, the hospital stay for labor and delivery was 1 week. The current average stay in uncomplicated cases is 2 days. Routine follow-up of the newborn takes place within 2 weeks. A nurse visits the homes of infants and mothers who appear to be at high risk.
Midwives
Throughout history, women have played an important role as birth attendants or midwives. The first school of nurse-midwifery opened in New York City in 1932. There are many accredited programs across the United States, all located in or affiliated with institutions of higher learning. The certified nurse-midwife (CNM) is a registered nurse who has graduated from an accredited midwife program and is nationally certified by the American College of Nurse-Midwives. The CNM provides comprehensive prenatal and postnatal care and attends uncomplicated deliveries. The CNM ensures that each patient has a backup physician who will assume her care should a problem occur.
Role of the Consumer
Consumerism has played an important part in family-centered childbirth. In the early 1960s, the natural childbirth movement awakened expectant parents to the need for education and involvement. Prepared childbirth, La Leche League (breastfeeding advocates), and Lamaze classes gradually became accepted. Parents began to question the routine use of anesthesia and the exclusion of fathers from the delivery experience.
Today, a father’s attendance at birth is common. Visiting hours are liberal, and extended contact with the newborn is encouraged. The consumer continues to be an important instigator of change. Consumer groups, with the growing support of professionals, have helped to revise restrictive policies once thought necessary for safety. It has been demonstrated that informed parents can make wise decisions about their own care during this period if they are adequately educated and given professional support.
Cultural Considerations
Culture is a body of socially inherited characteristics that one generation hands down to the next. Culture consists of values, beliefs, and practices shared by members of the group. Culture becomes a patterned expression of the thoughts and actions (called traditions) and affects the way patients respond to health care.
The United States is a culturally diverse nation, and nurses must develop cultural awareness and cultural sensitivity to practices and values that differ from their own. Only this way nurses can develop the cultural competence that will enable them to adapt health care practices to meet the needs of patients from various cultures.
The cultural background of the expectant family strongly influences its adaptation to the birth experience. Nursing Care Plan 1-1 lists nursing interventions for selected diagnoses that pertain to cultural diversity. One way in which the nurse gains important information about an individual’s culture is to ask the pregnant woman what she considers normal practice. Data collection questions might include the following:
• How does the woman view her pregnancy (as an illness, a vulnerable time, or a healthy time)?
• Does she view the birth process as dangerous? Why?
• Is birth a public or private experience for her?
• In what position does she expect to deliver (i.e., squatting, lithotomy, or some other position)?
• What type of help does she need before and after delivery?
• What role does her immediate or extended family play in relation to the pregnancy and birth?
Such information helps to promote understanding and individualizes patient care. It also increases the satisfaction of the patient and the nurse regarding the quality of care provided. Cultural influences on nursing care are discussed in Chapter 6.
Technology and Specialty Expertise
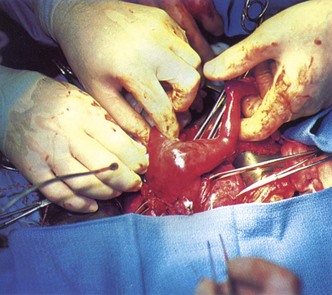
Technological advances have enabled many infants to survive who might otherwise have died (Figure 1-1). High-risk prenatal clinics and the neonatal intensive care unit offer the 1-lb preemie an opportunity to survive. Children with heart problems are now treated by a pediatric cardiologist. Much of the complex surgery needed by the newborn with a congenital defect is provided by the pediatric surgeon. Emotional problems are managed by pediatric psychiatrists. Many hospital laboratories are well equipped to test pediatric specimens. Chromosomal studies and biochemical screening have made identification of risks and family counseling more significant than ever. The field of perinatal biology has advanced to the forefront of pediatric medicine.
The medical profession and allied health agencies work as a team to ensure the total well-being of the patient. Children with defects previously thought to be incompatible with life are taken to special diagnostic and treatment centers where they receive expert attention and care. After discharge, many of these children are being cared for in their homes. The number of chronically disabled children is growing. Some are dependent on sophisticated hospital equipment such as ventilators and home monitors. The required nursing care at home may call for the suctioning of a tracheostomy, central line care, and other highly technical skills. Parents must be carefully educated and continually supported. Although this type of care is cost-effective and psychologically sound for the child, respite care is extremely important, because 24-hour-a-day care is extremely taxing for the family, both physically and psychologically.
Genomics
Genomics is the study of the functions of all of the genes in the human body, with a focus on their interactions with each other and the environment. The Human Genome Project has identified all genetic material present in the human body. The door is now open for medical researchers to identify genes responsible for specific congenital disorders and develop “gene therapy” to replace missing genes or alter defective genes (Figure 1-2). This knowledge, combined with technological advances, can result in earlier diagnosis, earlier intervention, and an integration of genomic knowledge in patient education as well as therapy.
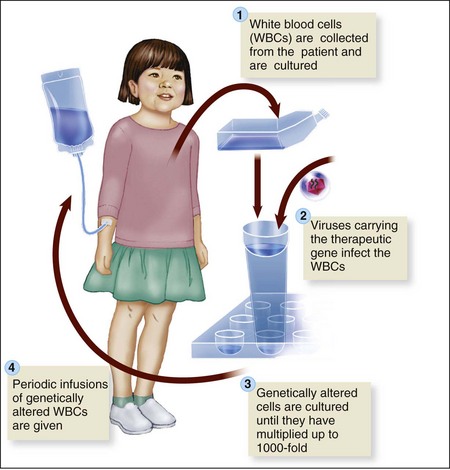
FIGURE 1-2 Gene therapy. One goal of gene replacement therapy is to alter the existing body cells to eliminate the cause of a genetic disease. The therapeutic or missing gene can be combined with a virus that can enter the infant’s system. This is called gene augmentation. In gene replacement therapy, new therapeutic genes are combined with viruses that can enter the human genome.
Health Care Delivery Systems
Cost containment is a major motivating factor in current health care, especially when health costs rise without decreases in morbidity and mortality. Many hospitals are merging to increase their buying power and reduce duplication of services.
Insurance reimbursement has become an important consideration in health care. The federal government has had to revise its Medicare and Medicaid programs. Among other changes, it instituted diagnosis-related groups (DRGs). These refer to a Medicare system that determines payment for a hospital stay based on the patient’s diagnosis. This mandate has had a tremendous impact on health care delivery. Patients are being discharged earlier from the hospital, and more care is being given in skilled nursing facilities and in the home. Some insurance companies are employing nurses in the role of case managers. Nurses remaining in institutions also may be required to assume the role of case managers and to become more flexible through cross-training. Nurses are expected to be concerned with keeping hospital costs down while maintaining the quality of care. Many suggest that the future of nursing may depend on how well nurses can demonstrate their value and cost-effectiveness.
Health maintenance organizations (HMOs) and preferred provider organizations (PPOs) have emerged as alternative medical care delivery systems. Insurers and providers of care have united to hold costs down yet remain competitive. Historically, a two-tiered system evolved: one tier (private insurance, HMOs and PPOs) served people with greater financial resources, and the other tier (Medicare and Medicaid) served people with fewer resources. With recent federal legislative changes, a large percentage of persons who were uninsured will have access to health care via the Healthcare Reform Act of 2010. Box 1-3 defines managed care systems.
Nursing Care
Procedural modifications for the nurse have been made, including adherence to standard precautions during the labor and delivery process (see Appendix A), during umbilical cord care, and in the nursery. More emphasis on data entry and retrieval makes it necessary for nursing personnel to be computer-literate. Sociologically, families have become smaller, the number of single parents is increasing, child and spouse abuse is rampant, and more mothers work outside of the home to help support the family. These developments present special challenges to maternal and child health nurses. Careful assessment and documentation to detect abuse are necessary, and nurses must be familiar with community support services for women and children in need. Nurses must also be flexible and promote policies that make health care more available for working parents. Teaching must be integrated into care plans and individually tailored to the family’s needs and its cultural and ethnic background.
Pediatric Nurses as Advocates
An advocate is a person who intercedes or pleads on behalf of another. Pediatric nurses are increasingly assuming the role of child advocate. Advocacy may be required for the child’s physical and emotional health and may include other family members. Hospitalized children frequently cannot determine or express their needs. When nurses believe that the child’s best interests are not being met, they must seek assistance. This usually involves taking the problem to the multidisciplinary team. Nurses must document their efforts to seek instruction and direction from their head nurse or supervisors, or the physician.
Health Promotion
Health promotion continues to assume increased importance. Preventing illness or disability is cost-effective; more importantly, it saves the family from stress, disruptions, and financial burden. Healthy children are spending fewer days in the hospital. Many conditions are treated in same-day surgery, ambulatory settings, or emergency departments. Rather than being distinct, hospital and home care have become interdependent.
Many chronically ill children are living into adulthood, creating the need for more support services. Medically fragile and technology-dependent children may change the typical profile of chronically ill children. The nurse is often the initiator of support services to these patients through education and referral. Ideally these services will assist the child to become as independent as possible, lead a productive life, and be integrated into society. In the past the term mainstream was used to describe the process of integrating a physically or mentally challenged child into society. The term full inclusion, signifying an expansion of the mainstream policy, is being used more frequently today. Early infant intervention programs for children with developmental disabilities attempt to reduce or minimize the effects of the disability. These services may be provided in a clinic or in the home. The need for in-home, family-centered pediatric care will continue to grow with the number of children with chronic illness who survive.
Quality of life is particularly relevant. Organ transplants have saved some children; however, the complications, limited availability, and expense of these transplants create moral and ethical dilemmas. Older children with life-threatening conditions must be included in planning modified advance directives with their families and the medical team.
These developments, along with the explosion of information, an emphasis on individual nurses’ accountability, new technology, and use of computers in health care, make it especially imperative for nurses to maintain their knowledge and skills at the level necessary to provide safe care. Employers often offer continuing education classes for their employees. Most states require proof of continuing education for the renewal of nursing licenses.
Advanced Practice Nurses
In keeping with the current practice of focusing on prevention of illness and maintenance of health rather than the treatment of illness, the specialty of pediatric nurse practitioner (PNP) was born. The PNP provides ambulatory and primary care for patients. The school nurse or child life specialist expands the accessibility of preventive health care to the well child.
The clinical nurse specialist (CNS) provides care in the hospital or community to specific specialty patients, such as cardiac, neurological, or oncological care. CNSs conduct primary research and facilitate necessary changes in health care management of their patients. Often the PNP and the CNS are called advanced practice nurses, and they have a registered nurse (RN) license as well as an advanced degree. Advanced practice nurses can specialize in obstetrics, pediatrics, or neonatal care. Box 1-4 lists some specialties that have developed in maternal-child care.
Nursing Tools
The Nursing Process: The nursing process was developed in 1963. This term referred to a series of steps describing the systematic problem-solving approach nurses used to identify, prevent, or treat actual or potential health problems. In 1973, the ANA developed standards relating to this nursing process that have been nationally accepted and include the following:
1. Assessment: Collection of patient data, both subjective and objective
2. Diagnosis: Analysis of data in terms of NANDA nursing diagnoses (see inside back cover)
3. Planning: Preparation of a plan of care designed to achieve stated outcomes
Outcomes identification: Identification of individualized expected patient outcomes
4. Implementation: Carrying out of interventions identified in the plan of care
5. Evaluation: Evaluation of outcome progress and redesigning of the plan if necessary
The nursing process is a framework of action designed to meet the individual needs of patients. It is problem-oriented and goal-directed and involves the use of critical thinking, problem solving, and decision making. The nursing process is expressed in an individualized nursing care plan. Diagnoses approved by NANDA-I are listed on the inside back cover. Table 1-1 differentiates between medical and nursing diagnoses.
Table 1-1
Comparison of Medical and Nursing Diagnoses
| MEDICAL DIAGNOSIS | NURSING DIAGNOSIS |
| Acquired immunodeficiency syndrome (AIDS) | Imbalanced nutrition: less than body requirements related to anorexia and evidenced by weight loss |
| Gestational diabetes mellitus | Deficient knowledge related to gestational diabetes mellitus (GDM) and its effects on pregnant woman and fetus; manifested by crying, anxiety |
| Cystic fibrosis | Ineffective airway clearance related to mucus accumulation; manifested by rales, fatigue |
Nursing Care Plans: The nursing care plan is developed as a result of the nursing process. It is a written instrument of communication among staff members that focuses on individualized patient care. See Nursing Care Plan 1-1 for an example of a care plan. Other sample care plans for maternity and pediatric nursing are provided throughout this text. Certain terms used in care plans are important to understand (Box 1-5).
A nursing care plan is a “picture” of a typical clinical situation that may be encountered by the graduate nurse. Specific data concerning the patient are obtained. These data can be used as clues to solve the mystery or problem concerning the patient (this phase is called collection). These clues help the nurse identify the problems of the patient. By organizing all the clues and identifying several problems, the nurse then prioritizes the problems identified. This phase of care planning is called analysis. When the priority problem is identified, the nurse can use knowledge, experience, and resources such as doctors’ prescriptions, textbooks, journals, or the Internet to decide on a plan of action to solve the problem. This phase is called planning. The actual nursing activities necessary to solve the problem are called nursing interventions. The nursing interventions are planned with specific outcomes or goals in mind. An outcome or goal is the positive resolution of the patient’s problem. The nursing interventions are the basis of the nursing or bedside care provided to the patient. After the nursing care is provided, the nurse reevaluates the original problem to determine if the goal was met or the outcome achieved. If goals have not been met, the nurse suggests revision of interventions.
Clinical Pathways: Clinical pathways, also known as critical pathways, care maps, or multidisciplinary action plans, are collaborative guidelines that define multidisciplinary care in terms of outcomes within a timeline. Fundamentally, the pathway identifies expected progress within a set timeline and benchmarks by which to recognize this progress. This expected progress of the patient becomes a standard of care; therefore, clinical pathways are based on research rather than on tradition. By setting specific recovery goals that the patient is expected to reach each day, deviations are readily identified. These deviations are called variances. If the patient’s progress is slower than expected, the outcome (goal) is not achieved within the timeline and a negative variance occurs, and discharge from the hospital may be delayed. The use of clinical pathways improves the quality of care and reduces unnecessary hospitalization time. It is an essential component of managed care and promotes coordination of the entire health care team. Sample clinical pathways are presented throughout the chapters in this text.
Statistics: Statistics refers to the process of gathering and analyzing numerical data. Statistics concerning birth, illness (morbidity) and death (mortality) provide valuable information for determining or projecting the needs of a population or subgroup and for predicting trends. In the United States, vital statistics are compiled for the country as a whole by the National Center for Health Statistics and are published in the Centers for Disease Control and Prevention (CDC) annual report, Vital Statistics of the United States, and in the pamphlet Morbidity and Mortality Weekly Report (MMWR). Statistics are issued by each state’s bureaus of vital statistics as well. Other independent agencies also supply statistics regarding various specialties.
A maternity nurse may use statistical data to become aware of reproductive trends, to determine populations at risk, to evaluate the quality of prenatal care, or to compare relevant information from state to state and country to country. Box 1-6 lists some frequently used terms in vital statistics.
Statistics show, for example, that sudden infant death syndrome (SIDS) was the second leading cause of death under the age of 1 year in 1980, but was the third in 2005. Respiratory distress syndrome was the third leading cause of death under 1 year of age in 1980 and the eighth leading cause of death in 2005 (National Center for Health Statistics, 2007). Go to the Evolve website for more detailed information on infant deaths in the United States in 1980 and 2005. Research, education, and nursing care account for many of the positive changes in these statistical reports.
Table 1-2 compares the national birth rates for 2002 to 2006. Statistics show that there may be a relationship between the lack of prenatal care and the infant mortality rates. To promote early prenatal care and decrease the numbers of low-birth-weight infants, there would seem to be a need for public education. National maternal death rates per 100,000 live births have decreased from 73.7 in 1950 to 7.6 in 2002 (National Center for Health Statistics, 2007).
Table 1-2
Birth Rate Statistics in the United States, 2002 to 2006
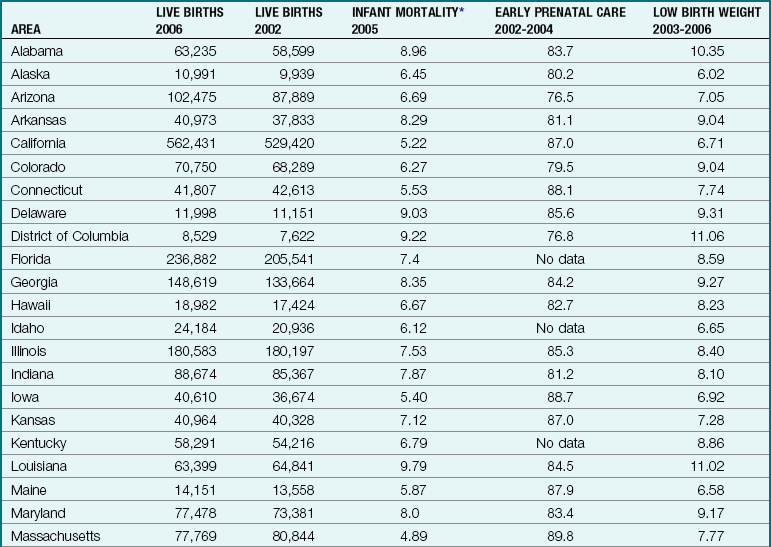
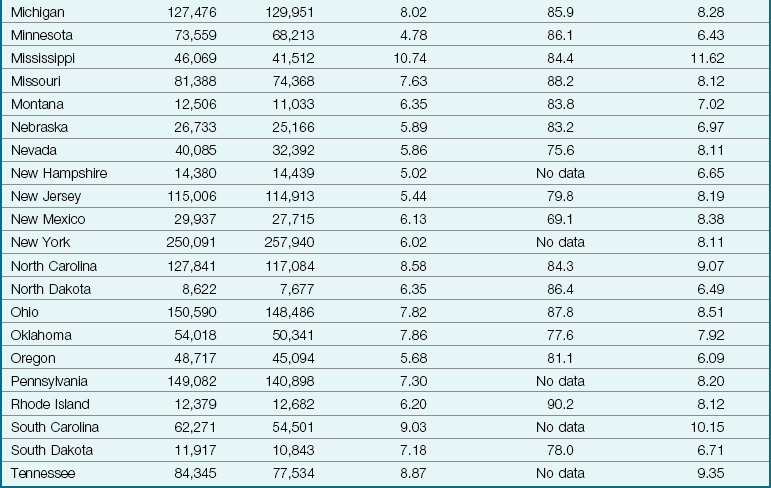
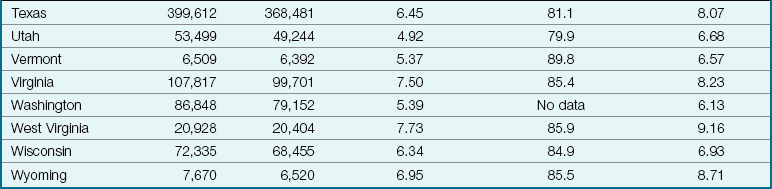
*Infant mortality rates are death under 1 year per 1000 live births in specified area.
Data from Health, United States (2007) with chartbook on trends in the health of Americans and National Vital Statistics Report 52(19). Retrieved May 9, 2009, from www.cdc.gov/nchs/data/hus/hus06trend.pdf.
Critical Thinking: Nurses have job-specific knowledge and skills they incorporate into their daily nursing practice by applying thought. General thinking involves random or memorized thoughts. An example of general thinking would be memorizing the steps in a clinical procedure or skill. Critical thinking, however, is purposeful, goal-directed thinking based on scientific evidence rather than assumption or memorization.
The way a nurse solves the problems of a patient is not always found in a textbook or in class lectures. Sometimes the nurse must consider factors that are specific to the individual patient or affected by individual situation. For example, the cultural background of the patient or the age of the patient influences how effective a given intervention will be. If the problem is a protein deficiency and the nurse selects the intervention to teach the importance of meat in the diet, the intervention will be ineffective—that is, it will not have a positive outcome—if this patient is a vegetarian, because meat will not be eaten. Thus critical thinking must enter the picture for optimum nursing care to be provided. Critical thinking entails applying creativity and ingenuity to solve a problem: combining basic standard principles with data specific to the patient. The basic steps in preparing a care plan involve critical thinking and are outlined in Box 1-7.
Critical thinking organizes the approach to discovery and involves the reflection and integration of information that enables the nurse to arrive at a conclusion or make a judgment. An example of critical thinking would be modifying the steps in a clinical procedure or skill so that the individual patient’s needs are met but the basic principles of the skill are not violated (e.g., sterile technique). With critical thinking, problem solving is effective and problem prevention occurs. General thinking can occur naturally, but critical thinking is a skill that must be learned.
Because critical thinking is an active process, the regular use of critical thinking can assist in moving general information into long-term memory and can increase creativity. Critical thinking skills help the nurse adapt to new situations that occur every day and aid in clinical decision making about care. Critical thinking can improve the care nurses give to patients, improve test scores (through critical thinking about a scenario in the question), and improve working conditions by enabling the nurse to analyze and find creative ways to improve existing policies and practices.
The nursing process and critical thinking: The nursing process (assessment, diagnosis, outcomes identification, planning, implementation, and evaluation) is a tool for effective critical thinking. When a nurse uses the nursing process in critical thinking, a clinical judgment can be made that is specific to the data collected and the clinical situation. In every clinical contact, a nurse must identify actual and potential problems and make decisions about a plan of action that will result in a positive patient outcome; know why the actions are appropriate; differentiate between those problems that the nurse can handle independently and those that necessitate contacting other members of the health care team; and prioritize those actions (Box 1-8).
Differentiating between actions that can be carried out independently and those requiring collaboration with other health care providers is based on the scope of practice of the licensed practical or vocational nurse (LPN/LVN). The scope of practice of the LPN/LVN is published by the state board of nursing.
NIC, NOC, and NANDA-I: Nursing Interventions Classification (NIC) by Bulechek and colleagues (2008), Nursing Outcomes Classification (NOC) by Moorhead and colleagues (2008), and the North American Nursing Diagnosis Association International (NANDA-I, 2009) Nursing Diagnoses: Definitions and Classification are companions that aid in the critical thinking aspect of patient care. They provide a standardization of language concerning patient status and nursing activities that enables nurses to work in the managed care environment, improve quality of care, reduce costs, promote research, and facilitate the development of a reimbursement system for nursing services rendered.
NIC and NOC codes make possible the collection of electronic data for the purposes of research and reimbursement. Nursing Care Plan 1-1 includes NIC and NOC entries to demonstrate how they are incorporated into the typical care plan. The specific codes assigned to NIC and NOC are not included in this text because the registered nurse is responsible for the coding. However, the LPN/LVN is responsible for understanding and working with NIC and NOC terminology.
NIC: NIC specifies actions that nurses perform to help patients toward a goal or outcome. The focus is on the action of the nurse. Physiological interventions such as suctioning and psychosocial interventions such as reducing fears and anxieties are useful in the prevention as well as the treatment of illness. There is a relationship between nursing diagnosis (NANDA-I), nursing interventions (NIC), and nursing outcomes (NOC). Nursing outcomes are different from nursing goals because nursing goals are either met or unmet. Nursing outcomes are described on a continuum. This makes it possible to measure outcomes as they are influenced by nursing actions.
Using critical thinking to improve test scores: Attending class, reading the text, and studying are the basis of learning, and evaluation of learning is achieved by testing. Weekly tests evaluate short-term learning. Final examinations evaluate long-term learning or retention of learning. Retained learning is subject to later recall and therefore is most useful in nursing practice after graduation from nursing school. Recalling facts that have been retained is what makes critical thinking in nursing practice possible. For a nurse to recognize or analyze abnormal findings, the normal findings must be recalled and used for comparison. An intervention can then be formulated.
Using critical thinking in studying involves the following:
• Understanding facts before trying to memorize them
• Prioritizing information to be memorized
• Relating facts to other facts (clusters, patterns, groups)
• Using all five senses to study (read, write, draw, listen to tapes, see pictures of symptoms)
• Reading critically (identifying key concepts and using critical thinking) when working with sample questions during study
Documentation
Documentation, or charting, has always been a legal responsibility of the nurse and continues to be a National Patient Safety Goal of The Joint Commission (TJC). When a medication is given or a treatment performed, it must be accurately documented on the patient’s chart. Charting responsibilities also include head-to-toe assessment of the patient and a recording of both data pertinent to the diagnosis and the response to treatment.
The forms of charting required by different hospitals in different areas of the country that guide the nurse toward comprehensive charting have been many. A traditional problem was when several members of the multidisciplinary health care team would access the chart at the same time. While the nurse was recording a medication administered, the medication record was “tied up” until the recording was complete. While a physician was reviewing the chart and the progress of the patient, the records were tied up until the conference was completed.
Electronic documentation was developed to decrease the number of medical errors caused by illegible handwriting and is now used by most hospitals in the country. Electronic documentation is paperless, and a bar-coding system is often used to document medication administration at the patient’s bedside. Security features are usually built in, and integrated prompts encourage accurate and comprehensive documentation by requiring certain entries be made before the user can progress further through the system. Critical ranges can be programmed into the computer so the nurse is alerted to deviations from the norm as information is recorded. Using electronic documentation, all caregivers have simultaneous access to patient records on all patients at all times from various locations. The adaptation of computer-based programs and their application in the hospital setting has motivated all nurses to become computer-literate.
SBAR Communication
Another TJC National Patient Safety goal involves improving communication between members of the health care team. One technique of communication concerning the patient between the members of the health care team is the use of SBAR (or S-BAR), a formal method of providing end-of-shift reports. The SBAR process includes discussion of these elements:
• Situation: The status of the patient on the unit
• Background: The background or relevant history of the patient that may influence care
• Assessment: An analysis of the problem or continuing patient need based on assessments made or orders written
• Recommendation: What the current patient need is and the outcome goals
Community-Based Nursing
Nursing care within the community and in the home is not a new concept in maternal-child nursing. In the first part of the twentieth century, the work of Lillian Wald, founder of the Henry Street Settlement, brought home health care to poor children. Margaret Sanger’s work as a public health nurse opened access to care for poor pregnant women and was the seed for the development of modern Planned Parenthood programs.
The community is now the major health care setting for all patients, and the challenge is to provide safe, caring, cost-effective, high-quality care to mothers, infants, and families. This challenge involves the nurse, who can advocate on behalf of patients and influence government, business, and the community to recognize the need for supporting preventive care of maternal-infant patients to ensure a healthy population for the future. The nurse must work with the interdisciplinary health care team to identify needs within the community and create cost-effective approaches to comprehensive preventive and therapeutic care.
The role of the nurse as an educator within the community is facilitated by involving schools, churches, health fairs, websites, and the media. Some registered nurses are branching out into the community as private practitioners, such as lactation consultants for new mothers. The nursing care plan is expanding to become a family care plan because the nurse is providing care to the patient in the home. Growth and development of the family and family lifestyles are discussed in Chapter 15, and the family care plan is presented in Chapter 9. Creativity, problem solving, coordination of multidisciplinary caregivers, case management, assessment, and referral are just some of the essential skills required of a nurse providing community-based care to maternal-infant patients.
Preventive care is only one aspect of current and future home care and community-based nursing. Therapeutic care is also provided in the home setting, and the nurse must educate the family concerning care, monitoring, and the potential needs for professional referral. Specialized care such as fetal monitoring of high-risk pregnant women, apnea monitoring of high-risk newborns, diabetic glucose monitoring, heparin therapy, and total parenteral nutrition can be safely accomplished in the home setting, often supported by telephone access to a nurse manager.
The home health care team, as advocated by the American Academy of Pediatrics Committee on Children with Disabilities, includes a pediatrician; nurses; occupational, physical, and respiratory therapists; speech therapists; home teachers; social workers; and home health aides. The American Academy of Home Health Care Physicians has expressed a medical commitment to the concept of home care for the future.
The Future
The revolution in health care involves the conflict between cost containment and quality of care. When health care became a profitable business industry, cost containment and managed care were born. Managed care openly evaluates care given and can result in increased quality. Quality assurance committees are investigating the routine management of patients, especially in the area of preventive care and tests.
The federal government enacted a health care reform plan in 2010 to reduce the cost of health care while making it more accessible to all. Access to care also depends on the availability of resources within a community. Figure 1-3 demonstrates that as of 2004, there are many areas within the United States that do not have adequate resources for maternal-child health care.
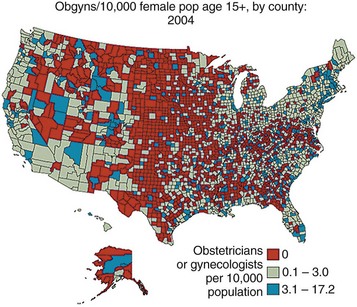
FIGURE 1-3 Obstetricians or gynecologists per 10,000 females aged 15 and over by county in the United States, 2004.
Health insurance plays an important role in health care delivery. Having health insurance does not necessarily ensure access to care, since the insurance company often must approve (or deny) the expenditure before a test or care is provided. Historically, families that could not afford health insurance often did not seek preventive health care such as prenatal care, infant immunizations, and well-baby check-ups. The Healthcare Reform Act of 2010 helps to facilitate access to healthcare that was previously unavailable. Managed care and utilization review committees that review the appropriateness of health care services also have an impact on physicians’ management of patients. Continued study is needed to determine the effect of managed care on the quality of health care and cost containment. Nurses are involved in the health care reform movement as patient advocates to ensure quality of care.
Future Roles for Nurses
The future role of the nurse will involve providing health care in a variety of settings and working closely with the multidisciplinary health care team. The nurse will function as a caregiver, teacher, collaborator, advocate, manager, and researcher. Competence in care and accountability to patient, family, community, and profession are core responsibilities of the nurse in the twenty-first century. Nurses will take a key role in shaping the health care picture of tomorrow.
Healthy People 2020
Healthy People 2020 updates the previous decade’s statement of national health promotion and disease prevention objectives facilitated by the federal government (U.S. Department of Health and Human Services, 2010). The report identifies objectives designed to use the vast knowledge and technology of health care that was developed in the twentieth century to improve the health and quality of life of Americans in the twenty-first century. The objectives fall under broad categories of effort: health promotion, health protection, preventive services, and the development of surveillance and data systems. The specific goals include increasing the span of healthy life, reducing health disparities among Americans, and achieving access to preventive care for all Americans. Some priority areas include maternal and infant health, immunizations, prevention of sexually transmitted infections, oral health, nutrition, and physical fitness. It is a “vision for the new century” to achieve a nation of healthy people (see Health Promotion box on p. 11).
Get Ready for the NCLEX® Examination!
Key Points
• In 1840 Ignaz Semmelweis suggested that handwashing was an important concept in preventing infection. This simple procedure is still a cornerstone of nursing care.
• The American Nurses Association (ANA) has written standards of maternal-child health practices.
• HIPAA regulations mandate maintaining confidentiality concerning patient medical records and personal information.
• The Fair Labor Standards Act, passed in 1938, regulates the use of child labor.
• Lillian Wald, a nurse, is credited with suggesting the establishment of the Children’s Bureau.
• The White House Conferences on Children and Youth investigate and report on matters pertaining to children and their families among all classes of people.
• The Children’s Charter of 1930 is considered one of the most important documents in child care history.
• The United Nations Declaration of the Rights of the Child calls for freedom, equality of opportunity, social and emotional benefits, and enhancement of each child’s potential.
• Labor, delivery, and recovery (LDR) rooms provide family-centered birthing and promote early parent-infant bonding.
• The culture of a society has a strong influence on family and child care.
• The cultural background of the expectant family plays an important role in its members’ adaptation to the birth experience.
• The educational focus for the childbearing family is that childbirth is a normal and healthy event.
• The nurse must understand the culture and tradition of the family and its influence on health practices.
• Advanced practice nurses are registered nurses with advanced degrees who are certified and specialize, manage patient care, and conduct research.
• The nursing process consists of five steps: assessment, nursing diagnosis, planning (with outcomes identification), implementation, and evaluation. It is an organized method in nursing practice and a means of communication among staff members.
• Diagnosis-related groups (DRGs), a form of cost containment, continue to affect nursing practice.
• The nursing care plan is a written instrument of communication that uses the nursing process to formulate a plan of care for a specific patient. It uses nursing diagnoses and involves critical thinking and problem solving.
• Clinical pathways are collaborative guidelines that define multidisciplinary care in terms of outcomes within a timeline.
• Statistics refers to gathering and analyzing numerical data.
• Birth rate refers to the number of live births per 1000 population in 1 year.
• In the United States, vital statistics are compiled for the country as a whole by the National Center for Health Statistics.
• Critical thinking is an active process that involves recall of information that is stored in long-term memory so that judgments based on facts can be analyzed and prioritized for use in clinical decision making.
• The use of critical thinking skills increases the ability of the nurse to make clinical decisions that meet individual needs of patients. The use of critical thinking skills can also improve test scores. The use of critical thinking also stimulates creativity that can improve quality of care and the work environment.
• Utilization review committees, quality assurance committees, the American Academy of Pediatrics Committee on Children with Disabilities, the American Academy of Home Care Physicians, and the Association of Women’s Health Obstetric and Neonatal Nurses (AWHONN) are some of the organizations that set and maintain standards of maternity and pediatric care.
• Nurses have legal and ethical responsibilities to report specific conditions to local public health agencies to protect the patient and the community.
• Charting is the legal responsibility of the nurse and includes a head-to-toe assessment and data pertinent to the diagnosis and the response of the patient to treatment.
• SBAR is a technique of communicating patient information among staff at the end of one shift and the beginning of the next.
• Healthy People is a statement of national health promotion that is a vision for the twenty-first century. The objectives are designed to use technology and knowledge to improve health care and quality of life.
• Home health care involves therapy, monitoring, teaching, and referral.
Additional Learning Resources
![]() Go to your Study Guide for additional learning activities to help you master this chapter content.
Go to your Study Guide for additional learning activities to help you master this chapter content.
![]() Go to your Evolve website (http://evolve.elsevier.com/Leifer) for the following FREE learning resources:
Go to your Evolve website (http://evolve.elsevier.com/Leifer) for the following FREE learning resources:
• Answer Guidelines for Critical Thinking Questions
• Answers and Rationales for Review Questions for the NCLEX® Examination
• Glossary with English and Spanish pronunciations
• Interactive Review Questions for the NCLEX® Examination
• Patient Teaching Plans in English and Spanish
• American Academy of Home Care Physicians: www.aahcp.org
• American Academy of Pediatrics: www.aap.org
• National Center for Health Statistics: www.cdc.gov/nchs
• National Human Genome Research Institute: www.genome.gov
• World Health Organization: www.who.int
Review Questions for the NCLEX® Examination
1. The number of deaths of infants younger than age 28 days per 1000 live births is termed the:
2. Which nursing action is the priority when a patient arrives at the clinic?
3. An organization that sets standards of practice for nursing is the:
1. American Medical Association (AMA).
2. American Nurses Association (ANA).
4. One advantage of electronic charting, which is used in most hospitals, is that it:
1. relieves the nurse of responsibilities to write.
2. enables many caregivers to access the chart at the same time.
5. Which source would the nurse use to determine if a specific nursing activity is within the scope of practice of an LPN/LVN?
 , p. 3)
, p. 3) , p. 3)
, p. 3) , p. 2)
, p. 2) , p. 2)
, p. 2) , p. 2)
, p. 2) , p. 2)
, p. 2) , p. 12)
, p. 12) ) (p. 16)
) (p. 16)