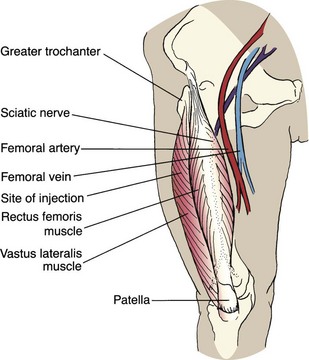
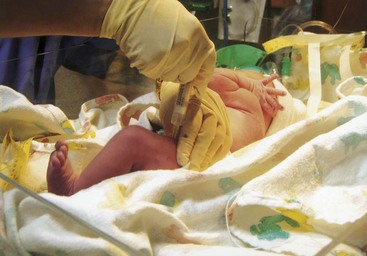
Nursing Care of Mother and Infant During Labor and Birth
1 Define each key term listed.
2 Discuss specific cultural beliefs the nurse may encounter when providing care to a woman in labor.
3 Compare the advantages and disadvantages for each type of childbearing setting: hospital, freestanding birth center, and home.
4 Describe the four components (“four Ps”) of the birth process: powers, passage, passenger, and psyche.
5 Describe how the four Ps of labor interrelate to result in the birth of an infant.
6 Explain the normal processes of childbirth: premonitory signs, mechanisms of birth, and stages and phases of labor.
7 Explain common nursing responsibilities during the labor and birth.
8 Explain how false labor differs from true labor.
9 Determine appropriate nursing care for the intrapartum patient, including the woman in false labor and the woman having a vaginal birth after cesarean (VBAC).
10 Describe the care of the newborn immediately after birth.
![]() http://evolve.elsevier.com/Leifer
http://evolve.elsevier.com/Leifer
Childbirth is a normal physiological process that involves the health of the mother and a fetus who will become part of our next generation. The nursing care is unique because every nursing intervention involves the welfare of two patients and the use of skills from medical-surgical and pediatric nursing, psychosocial and communication skills, and specific skills involved in obstetric care. In addition, labor and delivery are often a family affair, with fathers, grandparents, and others closely involved. The details of this experience are often remembered for a long time by each family participant.
The privacy and rights of the mother must be protected, the policies and procedures of the institution must be considered, and the nurse must be familiar with the scope of practice set out by the state board of nursing. Recent changes in the management of labor and delivery include practices related to induction and augmentation of labor, fetal monitoring techniques, maternal positions, types of analgesia offered, and assistive devices such as vacuum extraction.
This chapter provides information concerning the birth process and the nursing responsibilities during labor and delivery.
Cultural Influence on Birth Practices
The needs of the woman giving birth may be influenced by her cultural background, which may be very different from that of the nurse but must be understood and respected. In a multicultural environment, nothing is routine. Patient and cultural preferences require flexibility on the part of the nurse. Women of most cultures prefer the presence of a support person at all times during labor and delivery, and that can include the father or family as well as professional staff. The United States is a multicultural society. Table 6-1 lists common traditional birth practices of selected cultures. The practices of these cultural groups may vary depending on the amount of time they have been in the United States and the degree to which they have assimilated into the culture.
Table 6-1
Birth Practices of Selected Cultural Groups
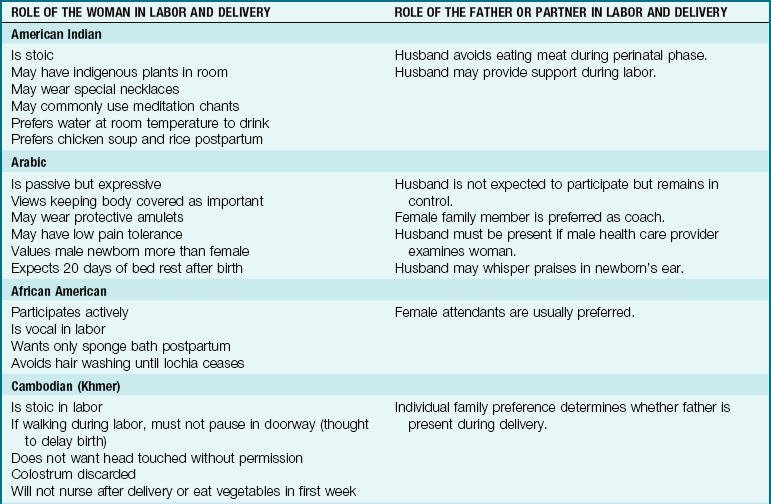
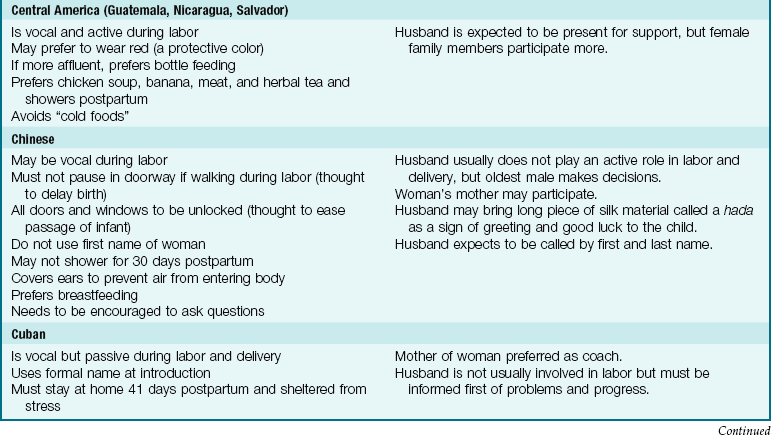
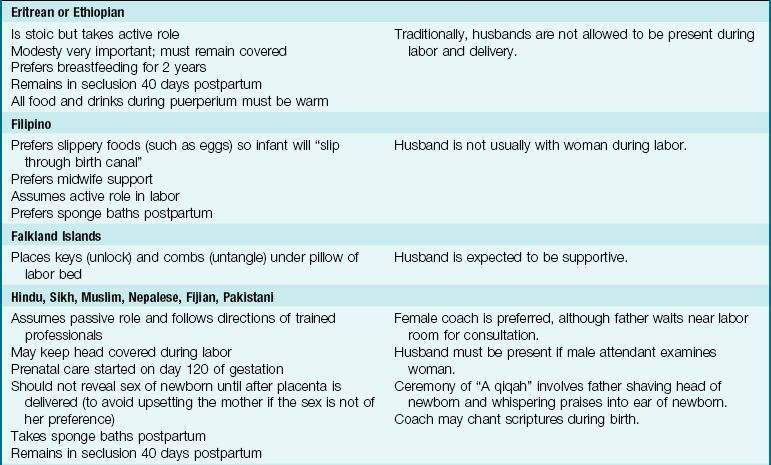
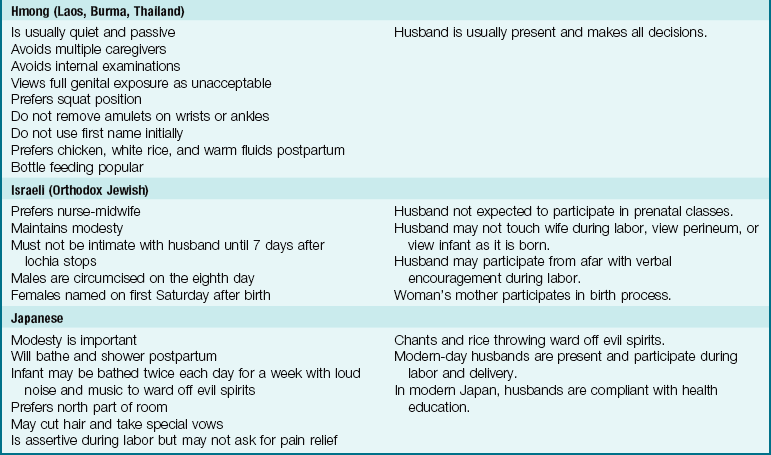
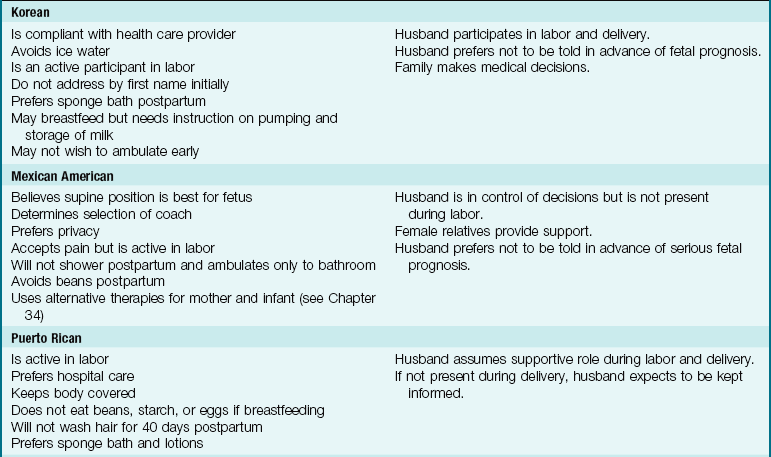
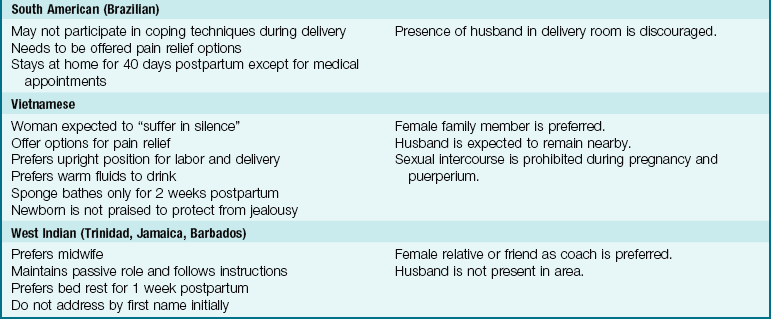
Note: Use professional translators whenever possible. Family members may not convey taboo topics accurately.
Data from Lipson, J.G., & Dibble, S.L. (2005). Culture and nursing care (2nd ed.). San Francisco: University of California, San Francisco, School of Nursing; Lowdermilk, D.L., & Perry, S.E., (2007). Maternity and women’s health care (9th ed.). St. Louis: Mosby; Perry, S.E., Hockenberry, M.J., Lowdermilk, D.L., & Wilson, D. (2010). Maternal and child nursing care (4th ed.). St. Louis: Mosby; Murasaki, S. (1996). Diary of Lady Murasaki. New York: Penguin Books.
Settings for Childbirth
Depending on facilities available in the area and the risks for complications, a woman can choose among three settings in which to deliver her child. Most women give birth in the hospital, whereas others choose freestanding birth facilities or their own home with a nurse-midwife or lay midwife in attendance.
Hospitals
The woman who chooses a hospital birth may have a “traditional” setting, in which she labors, delivers, and recovers in separate rooms. After the recovery period, she is transferred to the postpartum unit. A more common setting for hospital maternity care is the birthing room, often called a labor-delivery-recovery (LDR) room. The woman labors, delivers, and recovers all in the same room. She is then transferred to the postpartum unit for continuing care. The appearance of the birthing room is more homelike than institutional. The fully functional birthing bed has wood trim that hides its utilitarian purpose (Figure 6-1). The beds have receptacles for various fittings, such as a “squat bar,” which facilitates squatting during second-stage labor. The foot of the bed can be detached or rolled away to reveal foot supports or stirrups.
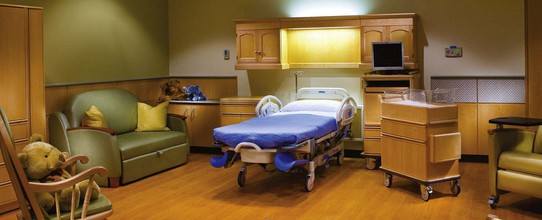
FIGURE 6-1 Typical labor, delivery, and recovery (LDR) room. Homelike furnishings can be quickly adapted to provide essential equipment when woman enters the active phase of labor. (Courtesy Hill-Rom Services, Inc., Batesville, IN.)
Another hospital birth setting is a single-room maternity care arrangement, often called a labor-delivery-recovery-postpartum (LDRP) room. It is similar to the LDR room, but the mother and infant remain in the same room until discharge.
Advantages of hospital-based birth settings include the following:
Freestanding Birth Centers
Some communities have birth centers that are separate from, although usually near, hospitals and are similar to outpatient surgical centers. Many birth centers are operated by full-service hospitals and are close enough for easy transfer if the mother, fetus, or newborn develops complications. Certified nurse-midwives often attend the births. Advantages of freestanding birth centers include the following:
Home
Some women give birth at home. Many factors enter into their decision, and most families have carefully weighed the pros and cons of their choice. Advantages of a home birth include the following:
• Control over persons who will or will not be present for the labor and birth, including children
• No risk of acquiring pathogens from other patients
• A low-technology birth, which is important to some families
Disadvantages vary with the location and may include the following:
• Limited choice of birth attendants (most physicians and nurse-midwives choose not to attend home births; in many communities, only lay midwives are available [whose training, abilities, and licensure status vary widely])
• Significant delay in reaching emergency care if the mother or child develops life-threatening complications
• Possibility of no preestablished relationship with a physician in the case of an emergency arises that necessitates the woman or newborn to be transferred to a hospital
Components of the Birth Process
Four interrelated components, often called the “four Ps,” make up the process of labor and birth: the powers, the passage, the passenger, and the psyche. These factors are discussed in detail in the following sections.
Other factors that influence the progress of labor include preparation, such as attendance at prenatal classes; position, horizontal or vertical; professional help, such as knowledgeable nurses in attendance who explain and coach; the place or setting, because a lack of privacy and changes in shift personnel can interrupt rapport; procedures, such as internal examinations; and people, such as the presence of supportive family members (VandeVusse, 1999).
The Powers
The powers of labor are forces that cause the cervix to open and that propel the fetus downward through the birth canal. The two powers are the uterine contractions and the mother’s pushing efforts.
Uterine Contractions
Uterine contractions are the primary powers of labor during the first of the four stages of labor (from onset until full dilation of the cervix). Uterine contractions are involuntary smooth muscle contractions; the woman cannot consciously cause them to stop or start. However, their intensity and effectiveness are influenced by a number of factors, such as walking, drugs, maternal anxiety, and vaginal examinations.
Effect of Contractions on the Cervix: Contractions cause the cervix to efface (thin) and dilate (open) to allow the fetus to descend in the birth canal (Figure 6-2). Before labor begins, the cervix is a tubular structure about 2 to 3.8 cm long. Contractions simultaneously push the fetus downward as they pull the cervix upward (an action similar to pushing a ball out the cuff of a sock). This causes the cervix to become thinner and shorter. Effacement is determined by a vaginal examination and is described as a percentage of the original cervical length. When the cervix is 100% effaced, it feels like a thin, slick membrane over the fetus.
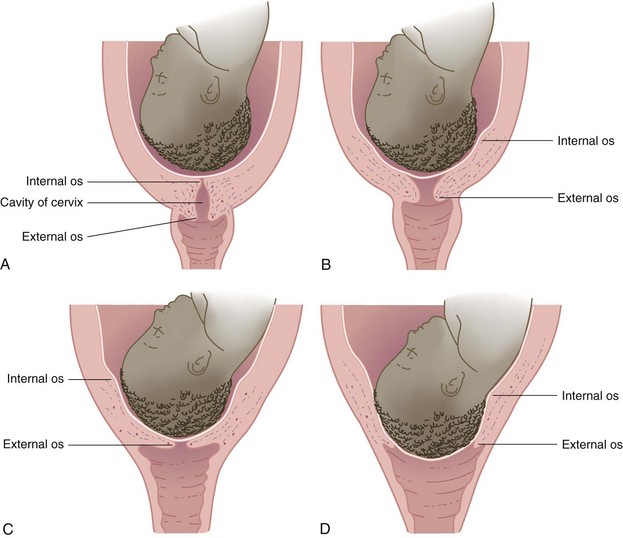
FIGURE 6-2 Cervical effacement and dilation. A, No effacement, no dilation. B, Early effacement and dilation. C, Complete effacement, some dilation. D, Complete dilation and effacement.
Dilation of the cervix is determined during a vaginal examination. Dilation is described in centimeters, with full dilation being 10 cm (Figure 6-3). Both dilation and effacement are estimated by touch rather than being precisely measured.
Phases of Contractions: Each contraction has the following three phases (Figure 6-4):
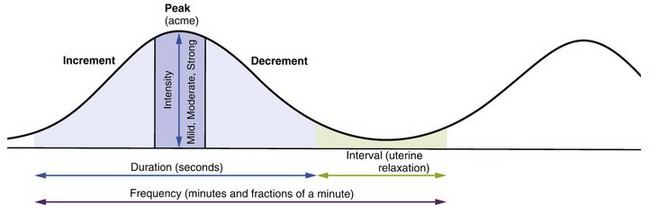
FIGURE 6-4 Contraction cycle. Each contraction can be likened to a bell shape, with an increment, peak (acme), and decrement. The frequency of contractions is the average time from the beginning of one to the beginning of the next. The duration is the average time from the beginning to the end of one contraction. The interval is the period of uterine relaxation between contractions.
Contractions are also described by their average frequency, duration, intensity, and interval.
Frequency: Frequency is the elapsed time from the beginning of one contraction until the beginning of the next contraction. Frequency is described in minutes and fractions of minutes, such as “contractions every 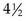 minutes.” Contractions occurring more often than every 2 minutes may reduce fetal oxygen supply and should be reported.
minutes.” Contractions occurring more often than every 2 minutes may reduce fetal oxygen supply and should be reported.
Duration: Duration is the elapsed time from the beginning of a contraction until the end of the same contraction. Duration is described as the average number of seconds for which contractions last, such as “duration of 45 to 50 seconds.” Persistent contraction durations longer than 90 seconds may reduce fetal oxygen supply and should be reported.
Intensity: Intensity is the approximate strength of the contraction. In most cases, intensity is described in words such as “mild,” “moderate,” or “strong,” which are defined as follows:
• Mild contractions: Fundus is easily indented with the fingertips; the fundus of the uterus feels similar to the tip of the nose.
• Moderate contractions: Fundus can be indented with the fingertips but with more difficulty; the fundus of the uterus feels similar to the chin.
• Firm contractions: Fundus cannot be readily indented with the fingertips; the fundus of the uterus feels similar to the forehead.
Interval: The interval is the amount of time the uterus relaxes between contractions. Blood flow from the mother into the placenta gradually decreases during contractions and resumes during each interval. The placenta refills with freshly oxygenated blood for the fetus and removes fetal waste products. Persistent contraction intervals shorter than 60 seconds may reduce fetal oxygen supply.
Maternal Pushing
When the woman’s cervix is fully dilated, she adds voluntary pushing to involuntary uterine contractions. The combined powers of uterine contractions and voluntary maternal pushing in stage 2 of labor propel the fetus downward through the pelvis. Most women feel a strong urge to push or bear down when the cervix is fully dilated and the fetus begins to descend. However, factors such as maternal exhaustion or sometimes epidural analgesia (see Chapter 7) may reduce or eliminate the natural urge to push. Some women feel a premature urge to push before the cervix is fully dilated because the fetus pushes against the rectum. This should be discouraged because it may contribute to maternal exhaustion and fetal hypoxia.
The Passage
The passage consists of the mother’s bony pelvis and the soft tissues (cervix, muscles, ligaments, and fascia) of her pelvis and perineum (see Chapter 2 for a review of the structure of the bony pelvis).
Bony Pelvis
The pelvis is divided into the following two major parts: (1) the false pelvis (upper, flaring part); (2) the true pelvis (lower part). The true pelvis, which is directly involved in childbirth, is further divided into the inlet at the top, the midpelvis in the middle, and the outlet near the perineum. It is shaped somewhat like a curved cylinder or a wide, curved funnel. The measurements of the maternal bony pelvis must be adequate to allow the fetal head to pass through, or cephalopelvic disproportion (CPD) will occur, and a cesarean birth may be indicated.
Soft Tissues
In general, women who have had previous vaginal births deliver more quickly than women having their first births because their soft tissues yield more readily to the forces of contractions and pushing efforts. This advantage is not present if the woman’s prior births were cesarean. Soft tissue may not yield as readily in older mothers or after cervical procedures that have caused scarring.
The Passengers
The passengers are the fetus, the placenta (afterbirth), amniotic membranes, and amniotic fluid. Because the fetus usually enters the pelvis head first (cephalic presentation), the nurse should understand the basic structure of the fetal head.
The Fetus
Fetal Head: The fetal head is composed of several bones separated by strong connective tissue, called sutures (Figure 6-5). A wider area called a fontanelle is formed where the sutures meet. The following two fontanelles are important in obstetrics:
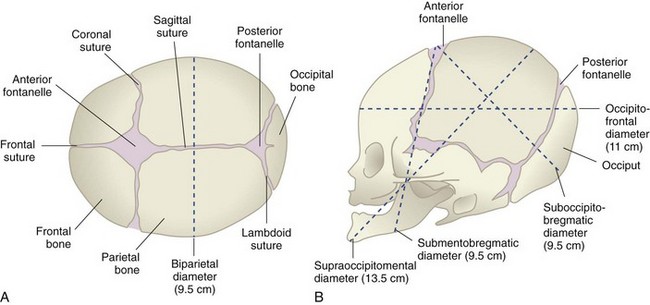
FIGURE 6-5 The fetal skull, showing sutures, fontanelles, and important measurements. A, Superior view. Note that the anterior fontanelle has a diamond shape; the posterior fontanelle is triangular. The biparietal diameter is an important fetal skull measurement. B, Lateral view. The measurements of the fetal skull are important to determine if cephalopelvic disproportion will be a problem. The mechanisms of labor allow the fetal head to rotate so that the smallest diameter of the head passes through the pelvis as it descends.
1. The anterior fontanelle, a diamond-shaped area formed by the intersection of four sutures (frontal, sagittal, and two coronal)
2. The posterior fontanelle, a tiny triangular depression formed by the intersection of three sutures (one sagittal and two lambdoid)
The sutures and fontanelles of the fetal head allow it to change shape as it passes through the pelvis (molding). They are important landmarks in determining how the fetus is oriented within the mother’s pelvis during birth.
The main transverse diameter of the fetal head is the biparietal diameter, which is measured between the points of the two parietal bones on each side of the head. The anteroposterior diameter of the fetal head can vary depending on how much the head is flexed or extended.
Lie: Lie describes how the fetus is oriented to the mother’s spine (Figure 6-6). The most common orientation is the longitudinal lie (greater than 99% of births), in which the fetus is parallel to the mother’s spine. The fetus in a transverse lie is at right angles to the mother’s spine. The transverse lie may also be called a shoulder presentation. In an oblique lie, the fetus is between a longitudinal lie and a transverse lie.
Attitude: The fetal attitude is normally one of flexion, with the head flexed forward and the arms and the legs flexed. The flexed fetus is compact and ovoid and most efficiently occupies the space in the mother’s uterus and pelvis. Extension of the head, the arms, and/or the legs sometimes occurs, and labor may be prolonged.
Presentation: Presentation refers to the fetal part that enters the pelvis first. The cephalic presentation is the most common. Any of the following four variations of cephalic presentations can occur, depending on the extent to which the fetal head is flexed (Figure 6-7):
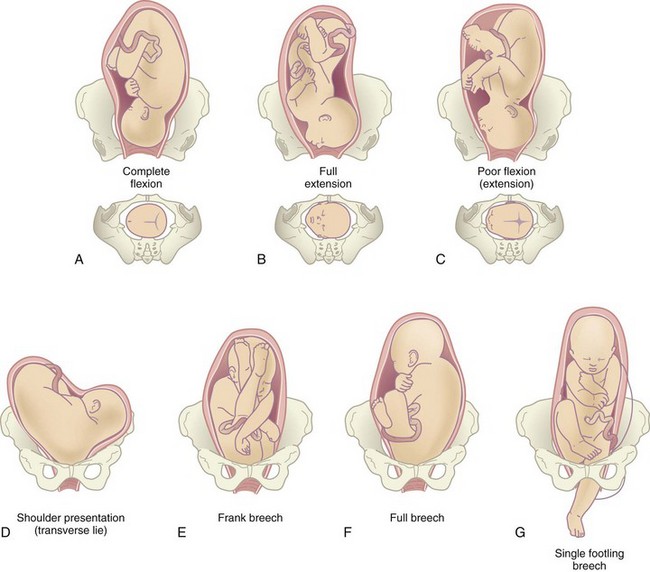
FIGURE 6-7 Fetal presentations. A, Cephalic vertex. B, Cephalic face. C, Cephalic brow. D, Shoulder. E, Frank breech. F, Full or complete breech. G, Footling breech (can be single or double). The vertex presentation in which the fetal chin is flexed on the chest is the most common and favorable for a vaginal birth because it allows the smallest diameter of the head to go through the bony pelvis of the mother. Note how the anterior and posterior fontanelles can be used to determine fetal presentation and position in the pelvis.
1. Vertex presentation: The fetal head is fully flexed. This is the most favorable cephalic variation because the smallest possible diameter of the head enters the pelvis. It occurs in about 96% of births.
2. Military presentation: The fetal head is neither flexed nor extended.
3. Brow presentation: The fetal head is partly extended. The longest diameter of the fetal head is presenting. This presentation is unstable and tends to convert to either a vertex or a face presentation.
4. Face presentation: The head is fully extended and the face presents.
The next most common presentation is the breech, which can have the following three variations (see Figure 6-7, E to G):
1. Frank breech: The fetal legs are flexed at the hips and extend toward the shoulders; this is the most common type of breech presentation. The buttocks present at the cervix.
2. Full or complete breech: A reversal of the cephalic presentation, with flexion of the head and extremities. Both feet and the buttocks present at the cervix.
3. Footling breech: One or both feet are present first at the cervix.
Many women with a fetus in the breech presentation have cesarean births because the head, which is the largest single fetal part, is the last to be born and may not pass through the pelvis easily because flexion of the fetal head cannot occur (see Figure 8-6, p. 190). After the fetal body is born, the head must be delivered quickly so the fetus can breathe; at this point, part of the umbilical cord is outside the mother’s body and the remaining part is subject to compression by the fetal head against the bony pelvis.
When the fetus is in a transverse lie, the fetal shoulder enters the pelvis first. A fetus in this orientation must be delivered by cesarean section because it cannot safely pass through the pelvis.
Position: Position refers to how a reference point on the fetal presenting part is oriented within the mother’s pelvis. The term occiput is used to describe how the head is oriented if the fetus is in a cephalic vertex presentation. The term sacrum is used to describe how a fetus in a breech presentation is oriented within the pelvis. The shoulder and back are reference points if the fetus is in a shoulder presentation.
The maternal pelvis is divided into four imaginary quadrants: right and left anterior and right and left posterior. If the fetal occiput is in the left front quadrant of the mother’s pelvis, it is described as left occiput anterior. If the sacrum of a fetus in a breech presentation is in the mother’s right posterior pelvis, it is described as right sacrum posterior.
Abbreviations describe the fetal presentation and position within the pelvis (Box 6-1). Three letters are used for most abbreviations:
1. First letter: Right or left side of the woman’s pelvis. This letter is omitted if the fetal reference point is directly anterior or posterior, such as occiput anterior (OA).
2. Second letter: Fetal reference point (occiput for vertex presentations; mentum [chin] for face presentations; and sacrum for breech presentations).
3. Third letter: Front or back of the mother’s pelvis (anterior or posterior). Transverse (T) denotes a fetal position that is neither anterior nor posterior.
Figure 6-8 shows various fetal presentations and positions.
The Psyche
Childbirth is more than a physical process; it involves the woman’s entire being. Women do not recount the births of their children in the same manner that they do surgical procedures. They describe births in emotional terms, such as those they use to describe marriages, anniversaries, religious events, or even deaths. Families often have great expectations about the birth experience, and the nurse can promote a positive childbearing experience by incorporating as many of the family’s birth expectations as possible.
A woman’s mental state can influence the course of her labor. For example, the woman who is relaxed and optimistic during labor is better able to tolerate discomfort and work with the physiological processes. By contrast, marked anxiety can increase her perception of pain and reduce her tolerance of it. Anxiety and fear also cause the secretion of stress compounds from the adrenal glands. These compounds, called catecholamines, inhibit uterine contractions and divert blood flow from the placenta.
A woman’s cultural and individual values influence how she views and copes with childbirth.
Normal Childbirth
The specific event that triggers the onset of labor remains unknown. Many factors probably play a part in initiating labor, which is an interaction of the mother and fetus. These factors include stretching of the uterine muscles, hormonal changes, placental aging, and increased sensitivity to oxytocin. Labor normally begins when the fetus is mature enough to adjust easily to life outside the uterus yet still small enough to fit through the mother’s pelvis. This point is usually reached between 38 and 42 weeks after the mother’s last menstrual period.
Signs of Impending Labor
Signs and symptoms that labor is about to start may occur from a few hours to a few weeks before the actual onset of labor.
Braxton Hicks Contractions
Braxton Hicks contractions are irregular contractions that begin during early pregnancy and intensify as full term approaches. They often become regular and somewhat uncomfortable, leading many women to believe that labor has started (see the discussion of true and false labor later in this chapter). Although Braxton Hicks contractions are often called “false” labor, they play a part in preparing the cervix to dilate and in adjusting the fetal position within the uterus.
Increased Vaginal Discharge
Fetal pressure causes an increase in clear and nonirritating vaginal secretions. Irritation or itching with the increased secretions is not normal and should be reported to the physician or certified nurse-midwife (CNM) because these symptoms are characteristic of infection.
Bloody Show
As the time for birth approaches, the cervix undergoes changes in preparation for labor. It softens (“ripens”), effaces, and dilates slightly. When this occurs, the mucous plug that has sealed the uterus during pregnancy is dislodged from the cervix, tearing small capillaries in the process. Bloody show is thick mucus mixed with pink or dark brown blood. It may begin a few days before labor, or a woman may not have bloody show until labor is under way. Bloody show may also occur if the woman has had a recent vaginal examination or intercourse.
Rupture of the Membranes
The amniotic sac (bag of waters) sometimes ruptures before labor begins. Infection is more likely if many hours elapse between rupture of the membranes and birth because the amniotic sac seals the uterine cavity against organisms from the vagina. In addition, the fetal umbilical cord may slip down and become compressed between the mother’s pelvis and the fetal presenting part. For these two reasons, women should go to the birth facility when their membranes rupture, even if they have no other signs of labor.
Mechanisms of Labor
As the fetus descends into the pelvis, it undergoes several positional changes so that it adapts optimally to the changing pelvic shape and size. Many of these mechanisms, also called cardinal movements, occur simultaneously (Figure 6-9).
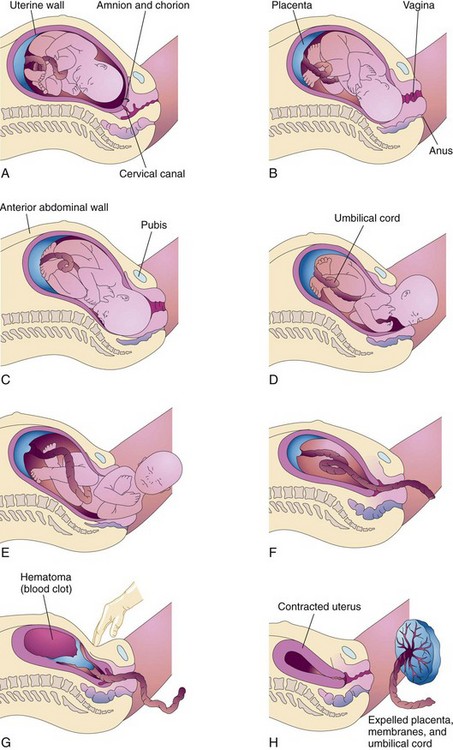
FIGURE 6-9 Mechanisms of labor are also called cardinal movements. The positional changes allow the fetus to fit through the pelvis with the least resistance. A, Descent, engagement, and flexion. B, Internal rotation. C, Beginning extension. D, Birth of the head by complete extension. E, External rotation, birth of shoulders and body. F, Separation of placenta begins. G, Complete separation of placenta from uterine wall. H, Placenta is expelled and uterus contracts.
Descent
Descent is required for all other mechanisms of labor to occur and for the infant to be born. Descent occurs as each mechanism of labor comes into play. Station describes the level of the presenting part (usually the head) in the pelvis. Station is estimated in centimeters from the level of the ischial spines in the mother’s pelvis (a 0 [zero] station). Minus stations are above the ischial spines, and plus stations are below the ischial spines (Figure 6-10). As the fetus descends, the minus numbers decrease (e.g., −2, −1) and the plus numbers increase (e.g., +1, +2).
Engagement
Engagement occurs when the presenting part (usually the biparietal diameter of the fetal head) reaches the level of the ischial spines of the mother’s pelvis (presenting part is at a 0 station or lower). Engagement often occurs before the onset of labor in a woman who has not previously given birth (a nullipara); if the woman has had prior vaginal births (a multipara), engagement may not occur until well after labor begins.
Flexion
The fetal head should be flexed to pass most easily through the pelvis. As labor progresses, uterine contractions increase the amount of fetal head flexion until the fetal chin is on the chest.
Internal Rotation
When the fetus enters the pelvis head first, the head is usually oriented so the occiput is toward the mother’s right or left side. As the fetus is pushed downward by contractions, the curved, cylindrical shape of the pelvis causes the fetal head to turn until the occiput is directly under the symphysis pubis (occiput anterior [OA]).
Extension
As the fetal head passes under the mother’s symphysis pubis, it must change from flexion to extension so it can properly negotiate the curve. To do this, the fetal neck stops under the symphysis, which acts as a pivot. The head swings anteriorly as it extends with each maternal push until it is born.
External Rotation
When the head is born in extension, the shoulders are crosswise in the pelvis and the head is somewhat twisted in relation to the shoulders. The head spontaneously turns to one side as it realigns with the shoulders (restitution). The shoulders then rotate within the pelvis until their transverse diameter is aligned with the mother’s anteroposterior pelvis. The head turns farther to the side as the shoulders rotate within the pelvis.
Admission to the Hospital or Birth Center
Intrapartum nursing care begins before admission by educating the woman about the appropriate time to come to the facility. Nursing care includes admission assessments and the initiation of necessary procedures. Many women have false labor and are discharged after a short observation period.
When to Go to the Hospital or Birth Center
During late pregnancy the woman should be instructed about when to go to the hospital or birth center. There is no exact time, but the general guidelines are as follows:
• Contractions: The woman should go to the hospital or birth center when the contractions have a pattern of increasing frequency, duration, and intensity. The woman having her first child is usually advised to enter the facility when contractions have been regular (every 5 minutes) for 1 hour. Women having second or later children should go sooner, when regular contractions are 10 minutes apart for a period of 1 hour.
• Ruptured membranes: The woman should go to the facility if her membranes rupture or if she thinks they may have ruptured.
• Bleeding other than bloody show: Bloody show is a mixture of blood and thick mucus. Active bleeding is free flowing, bright red, and not mixed with thick mucus.
• Decreased fetal movement: The woman should be evaluated if the fetus is moving less than usual. Many fetuses become quiet shortly before labor, but decreased fetal activity can also be a sign of fetal compromise or fetal demise (death).
• Any other concern: Because these guidelines cannot cover every situation, the woman should contact her health care provider or go to the birth facility for evaluation if she has any other concerns.
Admission Data Collection
The nurse should observe the appropriate infection control measures when providing care in any clinical area. Water-repellent gowns, eye shields, and gloves are worn in the delivery area, and the newborn infant is handled with gloves until after the first bath. General guidelines for wearing protective clothing in the intrapartal area can be found in Appendix A.
When a woman is admitted, the nurse establishes a therapeutic relationship by welcoming her and her family members. The nurse continues developing the therapeutic relationship during labor by determining the woman’s expectations about birth and helping to achieve them. Some women have a written birth plan that they have discussed with their health care provider and the facility personnel. The woman’s partner and other family members she wants to be part of her care are included. From the first encounter, the nurse conveys confidence in the woman’s ability to cope with labor and give birth to her child.
The three major assessments performed promptly on admission are the following: (1) fetal condition, (2) maternal condition, and (3) impending (nearness to) birth.
Fetal Condition
The fetal heart rate (FHR) is assessed with a fetoscope (stethoscope for listening to fetal heart sounds), a hand-held Doppler transducer, or an external fetal monitor. When the amniotic membranes are ruptured, the color, amount, and odor of the fluid are assessed and the FHR is recorded.
Maternal Condition
The temperature, pulse, respirations, and blood pressure are assessed for signs of infection or hypertension.
Impending Birth
The nurse continually observes the woman for behaviors that suggest she is about to give birth, including the following:
• Bearing down with contractions
• Bulging of the perineum or the fetal presenting part becoming visible at the vaginal opening
If it appears that birth is imminent, the nurse does not leave the woman but summons help or uses the call bell. Gloves should be applied in case the infant is born quickly. Emergency delivery kits (called “precip trays” for “precipitous birth”) containing essential equipment are in all delivery areas. The student should locate this tray early in the clinical experience because one cannot predict when it will be needed. The nurse’s priority is to prevent injury to the mother and infant. The nurse should don gloves and a cover gown and assist with the delivery until help arrives (Skill 6-1).
Additional Data Collection
If the maternal and fetal conditions are normal and if birth is not imminent, other data can be gathered in a more leisurely way. Most birth facilities have a preprinted form to guide admission assessments. Women who have had prenatal care should have a prenatal record on file for retrieval of that information. Examples of assessment data needed are as follows:
• Basic information should be obtained: the woman’s reason for coming to the facility, the name of her health care provider, medical and obstetrical history, allergies, food intake, any recent illness, and medication use (including illicit substances).
• Woman’s plans for birth should be determined.
• Status of labor should be evaluated. A vaginal examination is done by the registered nurse, CNM, or physician to determine cervical effacement and dilation and fetal presentation, position, and station. Contractions are assessed for frequency, duration, and intensity by palpation and/or with an electronic fetal monitor.
• Woman’s general condition should be evaluated by performing a brief physical examination. Any edema, especially of the fingers and face, and any abdominal scars should be further explored. Fundal height is measured (or estimated by an experienced nurse) to determine if it is appropriate for her gestation. Reflexes are checked to identify hyperactivity that may occur with gestational hypertension (GH).
Admission Procedures
Several procedures may be done when a woman is admitted to a birth facility. Some common procedures are described in the following sections.
Permission and Consent Forms
The mother signs permission and/or consent forms for care of herself and her infant during labor, delivery, and the postbirth period. Permission for an emergency cesarean delivery may be included. All signatures must be witnessed by the health care provider and the nurse who confirms that proper information was given to the patient.
Laboratory Tests
A blood sample for measurement of hematocrit and a midstream urine specimen for determination of glucose and protein levels are common tests performed upon admission. The hematocrit test is often omitted if a woman has had regular prenatal care and a recent evaluation. The woman who did not have prenatal care will have additional tests that may include a complete blood count, urinalysis, a drug screen, tests for sexually transmitted infections, and others as indicated.
Intravenous Infusion
An intravenous (IV) line is started to allow the administration of fluids and drugs. The woman may have a constant fluid infusion, or venous access may be maintained with a saline lock to permit greater patient mobility in early labor.
Perineal Prep
A perineal prep is occasionally done to remove pubic hair that would interfere with the repair of a laceration or episiotomy. Its use has declined because it does not prevent infection as was once believed. If done, it is restricted to a small area of the perineum (“miniprep”).
Determining Fetal Position and Presentation
The nurse may assist the health care provider in determining the fetal position and presentation by abdominal palpations called Leopold’s maneuver (Figure 6-11). Sometimes performance of this technique at the time of admission reveals a previously unidentified multifetal pregnancy. Leopold’s maneuver is also helpful in locating the fetal back, which is the best location for hearing the FHR, and thus determining optimal placement of the fetal monitor sensor.
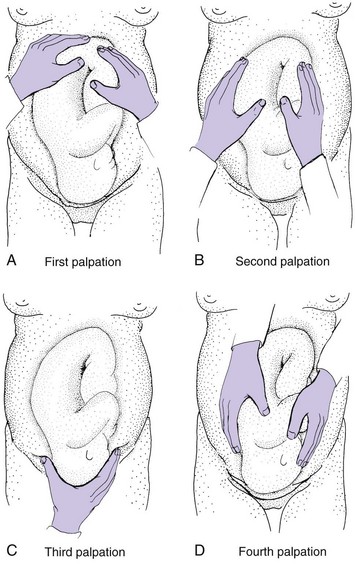
FIGURE 6-11 Leopold’s maneuver. A, Presentation. Hands are placed on either side of the maternal abdomen to palpate the uterine fundus to determine if a round, hard object is felt at the fundus (the fetal head, indicating a breech presentation) or a soft, irregular contour (the fetal buttocks, indicating a vertex presentation). B, Position. Hands are placed on either side of the maternal abdomen. Support one side of the abdomen while palpating the other side. Palpating a hard, smooth contour indicates location of the fetal back, while feeling soft, irregular objects indicates the small parts or extremities. C, Confirm presentation. The suprapubic area is palpated to determine that the vertex or head is presenting. Feeling a hard, round area that does not move may indicate the head is engaged. D, Attitude. Attitude of the fetal head is determined by palpating the maternal abdomen with fingers pointing toward the maternal feet. The hand is moved downward toward the symphysis pubis. Feeling a hard, round object on the same side as the fetal back indicates the fetus is in extension. Feeling the hard, round object opposite the fetal back indicates the head is in flexion.
Nursing Care of the Woman in False Labor
True labor is characterized by changes in the cervix (effacement and dilation), which is the key distinction between true and false labor. Table 6-2 lists other characteristics of true and false labor.
Table 6-2
Comparison of False Labor and True Labor
| FALSE LABOR (PRODROMAL LABOR OR PRELABOR) | TRUE LABOR |
| Contractions are irregular or do not increase in frequency, duration, and intensity. | Contractions gradually develop a regular pattern and become more frequent, longer, and more intense. |
| Walking tends to relieve or decrease contractions. | Contractions become stronger and more effective with walking. |
| Discomfort is felt in the abdomen and groin. | Discomfort is felt in the lower back and the lower abdomen; often feels like menstrual cramps at first. |
| Bloody show is usually not present. | Bloody show is often present, especially in women having their first child. |
| There is no change in effacement or dilation of the cervix. | Progressive effacement and dilation of the cervix occur. |
A better term for false labor might be prodromal labor, because these contractions help prepare the woman’s body and the fetus for true labor. Many women are observed for a short while (1 to 2 hours) if their initial assessment suggests that they are not in true labor and their membranes are intact. The mother and fetus are assessed during observation as if labor were occurring. Most facilities run an external electronic fetal monitor strip for at least 20 minutes to document fetal well-being. The woman can usually walk about when not being monitored. If she is in true labor, walking often helps to intensify the contractions and bring about cervical effacement and dilation.
After the observation period the woman’s labor status is reevaluated by the health care provider, who performs another vaginal examination. If there is no change in the cervical effacement or dilation, the woman is usually sent home to await true labor. Sometimes, if it is her first child and she lives nearby, the woman in very early labor is sent home because the latent phase of most first labors is quite long (see Table 6-6).
Each woman in false labor (or early latent-phase labor) is evaluated individually. Factors to be considered include the number and the duration of previous labors, distance from the facility, and availability of transportation.
If the woman’s membranes are ruptured, she is usually admitted even if labor has not begun because of the risk for infection or a prolapsed umbilical cord (see Chapter 8).
The woman in false labor is often frustrated and needs generous reassurance that her symptoms will eventually change to true labor. No one stays pregnant forever, although it sometimes feels that way to a woman who has had several false alarms and is tired of being pregnant. Guidelines for coming to the facility should be reinforced before she leaves.
Nursing Care Before Birth
After admission to the labor unit, nursing care consists of the following elements:
Monitoring the Fetus
Intrapartum care of the fetus includes assessment of FHR patterns and the amniotic fluid. In addition, several observations of the mother’s status, such as vital signs and contraction pattern, are closely related to fetal well-being because they influence fetal oxygen supply.
Fetal Heart Rate
The FHR can be assessed by intermittent auscultation, by using a fetoscope or Doppler transducer, or by continuous electronic fetal monitoring. (See Skill 6-2 for the procedure for assessing FHR.) Electronic fetal monitoring is more widely used in the United States, but intermittent auscultation is a valid method of intrapartum fetal assessment when performed according to established intervals and with a 1 : 1 nurse-patient ratio.
Intermittent Auscultation: Intermittent auscultation allows the mother greater freedom of movement, which is helpful during early labor and is the method used during home births and in most birth centers. However, unlike continuous monitoring, intermittent auscultation does not automatically record the results, so the nurse must provide careful documentation. Intermittent auscultation of the FHR should be performed as noted in Skill 6-2 and Box 6-2. Figure 6-12 shows the approximate locations of the fetal heart sounds according to various presentations and positions of the fetus. Any FHR outside the normal limits and any slowing of the FHR that persists after the contraction ends is promptly reported to the health care provider.
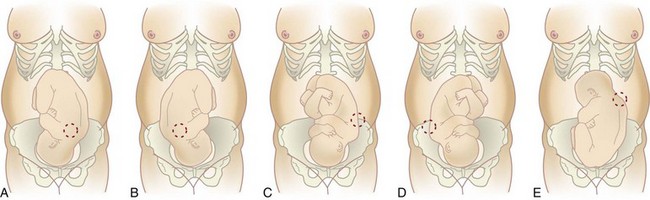
FIGURE 6-12 Determining placement of fetoscope or sensor to assess fetal heart rate (FHR). Approximate the location of the strongest fetal heart sound when the fetus is in various positions and presentations. The fetal heart sounds are heard best in the lower abdomen in a cephalic (vertex) presentation and higher on the abdomen when the fetus is in a breech presentation (E). A, LOA; B, ROA; C, LOP; D, ROP; E, LSA.
Continuous Electronic Fetal Monitoring: Continuous electronic fetal monitoring (EFM) allows the nurse to collect more data about the fetus than intermittent auscultation. FHR and uterine contraction patterns are continuously recorded. Most hospitals use continuous EFM because the permanent recording becomes part of the mother’s chart. Some monitors make use of telemetry (like a cordless telephone) and permit the woman to walk while a transmitter sends the data back to the monitor at the nurses station to be recorded. In the absence of that capability, intermittent monitoring is a variation that promotes walking during labor. An initial recording of at least 30 minutes is obtained, and then the fetus is remonitored at regular intervals of 30 to 60 minutes (see Skill 6-2).
EFM can be performed with external or internal devices. Internal devices require that the membranes be ruptured and the cervix dilated 1 to 2 cm for device insertion. Internal devices are disposable to reduce transmission of infection. A small spiral electrode applied to the fetal presenting part allows internal FHR monitoring. Two types of devices are used for internal contraction monitoring. One uses a fluid-filled catheter connected to a pressure-sensitive device on the monitor. The other uses a solid catheter with an electronic pressure sensor in its tip.
External fetal heart monitoring is done with a Doppler transducer, which uses sound waves to detect motion of the fetal heart and calculate the rate, just as the hand-held model does. Contractions are sensed externally with a tocotransducer (“toco”), which has a pressure-sensitive button. The toco is positioned over the mother’s upper uterus (fundus), about where the nurse would palpate contractions by hand (Skill 6-3).
Evaluating Fetal Heart Rate Patterns: The FHR is recorded on the upper grid of the paper strip and is expressed as beats per minute (beats/min, or bpm); the uterine contraction pattern is recorded on the lower grid. Both grids must be evaluated together for accurate interpretation of FHR patterns. The FHR is evaluated for baseline rate, baseline variability, episodic changes, and periodic changes. Episodic changes are those changes in the FHR that are not associated with uterine contractions. Periodic changes are those changes in the FHR that are associated with uterine contractions, such as accelerations and decelerations.
• Baseline fetal heart rate is the average FHR that occurs for at least 2 minutes during a 10-minute period of time. It is assessed while there are no uterine contractions. The baseline FHR should be 110 beats/min to 160 beats/min for at least a 2-minute period (ACOG, 2009).
• Fetal bradycardia occurs when the FHR is below 110 beats/min for 10 minutes or longer (ACOG, 2009). Causes of fetal bradycardia can be fetal hypoxia, maternal hypoglycemia, maternal hypotension, or prolonged umbilical cord compression. When bradycardia is accompanied by a loss of baseline variability or by late decelerations, immediate intervention is required for a favorable outcome.
• Fetal tachycardia is a baseline FHR greater than 160 beats/min that lasts 10 minutes or longer (ACOG, 2009). It can be caused by fetal hypoxia, maternal fever, or maternal dehydration. When fetal tachycardia occurs along with loss of baseline variability or with late decelerations, immediate intervention is required.
• Baseline variability describes fluctuation or constant changes in the baseline fetal heart rate within a 10-minute window (Figure 6-13). Variability causes a recording of the FHR to have a sawtooth appearance with larger, undulating, wavelike movements.
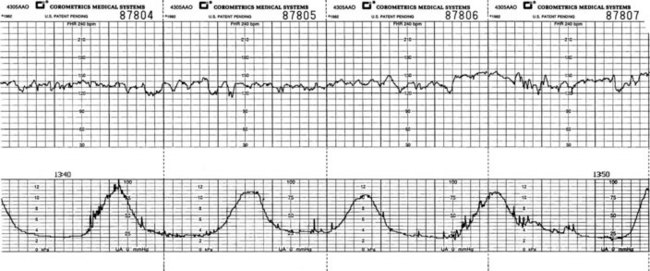
FIGURE 6-13 Recording of the fetal heart rate (FHR) in the upper grid and the uterine contractions in the lower grid. Note the sawtooth appearance of the FHR tracing that is due to the constant changes in the rate (variability). Note: The space between each dark black line on the strip represents 1 minute. The small squares, or the space between each light black line, represents 10 seconds.
• Moderate variability, defined as changes of 6 beats/min to 25 beats/min from the baseline fetal heart rate, is desirable since it indicates good oxygenation of the central nervous system (CNS) and fetal well-being.
• Marked variability occurs when there is more than 25 beats of fluctuation over the FHR baseline and can indicate cord prolapse or maternal hypotension.
• Absent variability is less than 6 beats/min change from baseline for a 10-minute period and is typically caused by uteroplacental insufficiency but can also be caused by maternal hypotension, cord compression, and fetal hypoxia. Nursing interventions for marked or absent variability include positioning the mother on her side, increasing regular IV-fluid flow rate to improve maternal circulation, administer oxygen at 8 to 10 L/min by mask, and notifying the health care provider.
• Episodic changes are those changes in the FHR that are not associated with uterine contractions.
• Periodic changes are temporary changes in the baseline rate associated with uterine contractions. Periodic changes include accelerations (rate increases) and any of three types of decelerations (rate decreases) (Box 6-3).
Accelerations: Accelerations are temporary, abrupt rate increases of at least 15 beats/min above the baseline FHR that last less than 30 seconds. This pattern suggests a fetus that is well oxygenated and is known as a “reassuring pattern.” Accelerations occur with fetal movement and are the basis for interpretation of the non–stress test (NST). An acceleration that lasts 2 to 10 minutes is considered a prolonged acceleration. An acceleration that lasts longer than 10 minutes may be considered a baseline FHR change (Adams & Bianchi, 2008).
Early decelerations: Early decelerations are temporary, gradual rate decreases during contractions; the FHR always returns to the baseline rate by the end of the contractions. The peak of deceleration occurs at the same time as the peak of the contraction. This results from compression of the fetal head and is a reassuring sign of fetal well-being.
Variable decelerations: Variable decelerations are abrupt decreases of 15 beats/min below baseline, lasting 15 seconds to 2 minutes. These decreases begin and end abruptly; on the monitor they are V-, W-, or U-shaped (Figure 6-14). They do not always exhibit a consistent pattern in relation to contractions. Variable decelerations suggest that the umbilical cord is being compressed, often because it is around the fetal neck (nuchal cord) or because there is inadequate amniotic fluid to cushion the cord. If the FHR decreases to 70 beats/min or the decrease lasts more than 60 seconds and is recurrent the health care provider should be notified immediately.
Late decelerations: Late decelerations of the FHR look similar to early decelerations, except that they begin after the beginning of the contraction and do not return to the baseline FHR until after the contraction ends (Figure 6-15). Late decelerations suggest that the placenta is not delivering enough oxygen to the fetus (uteroplacental insufficiency). This is known as a “nonreassuring pattern.” Late decelerations under 15 beats/min below baseline is a CNS response to fetal hypoxia. The occurrence of late decelerations greater than 45 beats/min below baseline may be due to placental aging (postmaturity) or fetal heart depression and is an ominous sign. Late decelerations that are accompanied by decreased variability are nonreassuring and require immediate intervention.
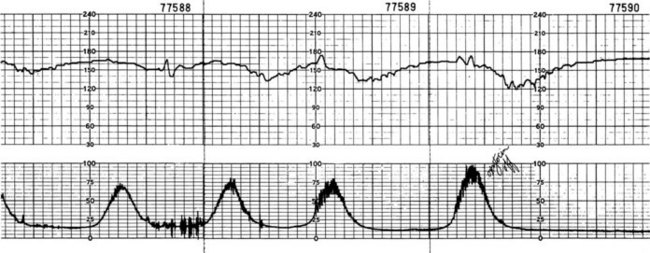
FIGURE 6-15 Late decelerations, showing their pattern of slowing, which persists after the contraction ends. The usual cause is reduced blood flow from the placenta (uteroplacental insufficiency [UPI]). Measures to correct this include repositioning the woman, giving oxygen, increasing nonmedicated intravenous fluid and stopping administration of oxytocin if it is being given, and giving drugs to reduce uterine contractions.
Prolonged decelerations: Prolonged decelerations are abrupt FHR decreases of at least 15 beats/min from baseline that last longer than 2 minutes but less than 10 minutes (ACOG, 2009). The FHR may drop to 90 beats/min during the 2- to 10-minute period. This is caused by cord compression or prolapse, maternal supine hypotension, or regional anesthesia. A prolonged deceleration that lasts longer than 10 minutes may be considered a change in the baseline rate (Adams & Bianchi, 2008).
Recurrent decelerations: Recurrent decelerations are decelerations that occur in more than 50% of uterine contractions in a 20-minute period.
Nursing Response to Monitor Patterns: The significance of and therefore the nursing response to FHR changes depends on the pattern or category identified (Table 6-3). Accelerations and early decelerations are reassuring and thus necessitate no intervention other than continued observation. Repositioning the woman is usually the first response to a pattern of variable decelerations. Changing the mother’s position can relieve pressure on the umbilical cord and improve blood flow through it. The woman is turned to her side. Other positions, such as the knee-chest or a slight Trendelenburg (head-down) position may be tried if the side-lying positions do not restore the pattern to a reassuring one. If membranes have ruptured, an amnioinfusion technique, in which IV fluid is infused into the amniotic cavity through an intrauterine pressure catheter, may be done to add a fluid cushion around the cord.
Table 6-3
Fetal Heart Rate Categories and Nursing Care
| CATEGORY | FETAL HEART RATE TRACINGS | NURSING RESPONSIBILITIES |
| I | Normal baseline rate and variability | Provide routine labor care. |
| II | Variable | Provide close observation and documentation. |
| III | Abnormal | Prompt interventions are indicated to have a positive outcome for woman and fetus. |
Late decelerations are initially treated by measures to increase maternal oxygenation and blood flow to the placenta. The specific measures depend on the most likely cause of the pattern and may include the following:
• Repositioning to prevent supine hypotension (see Chapter 4)
• Giving oxygen 8 to 10 L/min by face mask to increase the amount in the mother’s blood
• Increasing the amount of IV fluid infused to expand the blood volume and make more available for the placenta; this is often needed if regional analgesia or anesthesia causes hypotension
• Stopping oxytocin (Pitocin) infusion because the drug intensifies contractions and reduces placental blood flow
• Preparing to give tocolytic drugs to decrease uterine contractions
The health care provider is notified of any nonreassuring pattern after initial steps are taken to correct it.
Inspection of Amniotic Fluid
The membranes may rupture spontaneously, or the health care provider may rupture them artificially in a procedure called an amniotomy. The color, the odor, and the amount of fluid are recorded. The normal color of amniotic fluid is clear, possibly with flecks of white vernix (fetal skin protectant). The amount of amniotic fluid is usually estimated as scant (only a trickle), moderate (about 500 mL), or large (about 1000 mL or more). Green-stained fluid may indicate the fetus has passed meconium (the first stool) before birth, a situation associated with fetal compromise that can cause respiratory problems at birth. Cloudy or yellow amniotic fluid with an offensive odor may indicate an infection and should be reported immediately.
The FHR should be assessed for at least 1 full minute after the membranes rupture and must be recorded and reported. Marked slowing of the rate or variable decelerations suggests that the fetal umbilical cord may have descended with the fluid gush and is being compressed.
A nitrazine test or fern test may be performed if it is not clear whether the mother’s membranes have ruptured. Nitrazine paper is a pH paper; alkaline amniotic fluid turns it dark blue-green or dark blue. In the fern test, a sample of amniotic fluid is spread on a microscope slide and allowed to dry. It is then viewed under the microscope; the crystals in the fluid look like tiny fern leaves (Skill 6-4). Commercial high tech strips are available, such as AmniSure that involve swabbing vaginal secretions and inserting the swab in a vial to determine the pH of the vaginal fluid.
Monitoring the Woman
Intrapartum care of the woman includes assessing her vital signs, contractions, progress of labor, intake and output, and responses to labor.
Vital Signs
The temperature is checked every 4 hours, or every 2 hours if it is elevated or if the membranes have ruptured (frequency varies among facilities). A temperature of 38° C (100.4° F) or higher should be reported. If the temperature is elevated, the amniotic fluid is assessed for signs of infection. IV antibiotics are usually given to a woman who has a fever because of the risk that the infant will acquire group B streptococcus (GBS) infection. The pulse, blood pressure, and respirations are assessed every hour. Maternal hypotension (particularly if the systolic pressure is below 90 mm Hg) or hypertension (greater than 140/90 mm Hg) can reduce blood flow to the placenta.
Contractions
Contractions can be assessed by palpation and/or by continuous EFM. Some women have sensitive abdominal skin, especially around the umbilicus. When palpation is used to evaluate contractions, the entire hand is placed lightly on her uterine fundus (Figure 6-16). The nurse should keep the fingers still when palpating contractions. Moving the fingers over the uterus can stimulate contractions and give an inaccurate idea of their true frequency (Skill 6-5 and Table 6-4).
Table 6-4
| UTERINE ACTIVITY | DESCRIPTION |
| Normal | Five contractions within 10 minutes averaged over a 30-minute period |
| Tachysystole (increased uterine activity) | More than five contractions within 10 minutes for two consecutive 10-minute periods |
| Hyperstimulation | Exaggerated uterine response with late FHR decelerations or fetal tachycardia >160 beats/min or other nonreassuring FHR changes |
Relate the uterine contractions to the occurrence of fetal heart rate (FHR) decelerations or loss of variability.
Macones, G., Hankins, G., Spong, C., Hauth, J., & Moore, T. (2008). The 2008 NICHHD workshop report on EFM update of definition, interpretation, and research guidelines. Journal OB-GYN 112(3), 661-666.
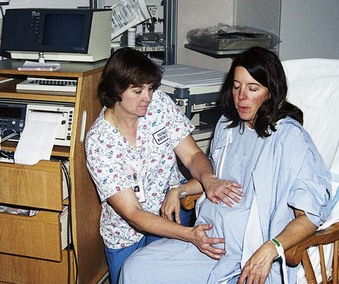
FIGURE 6-16 The nurse helps the mother maintain control and use breathing techniques during active labor. The use of an electronic monitor for fetal heart rate and contractions is not a substitute for personal hands-on care during labor. Note that the nurse places the entire hand on the fundus to determine the intensity of the contraction.
Progress of Labor
The health care provider does a vaginal examination periodically to determine how labor is progressing. The cervix is evaluated for effacement and dilation. The descent of the fetus is determined in relation to the ischial spines (station) (see Figure 6-10). There is no set interval for doing vaginal examinations. The observant nurse watches for physical and behavioral changes associated with progression of labor to reduce the number of vaginal examinations needed. Vaginal examinations are limited to prevent infection, especially if the membranes are ruptured. They are also uncomfortable.
Intake and Output
Women in labor do not usually need strict measurement of intake and output, but the time and approximate amount of each urination are recorded. The woman may not sense a full bladder, so she should be checked every 1 or 2 hours for a bulge above the symphysis pubis. A full bladder is a source of vague discomfort and can impede fetal descent. It often causes discomfort that persists after an epidural block has been initiated.
Policies about oral intake vary among birth facilities. Ice chips are usually allowed to moisten the mouth, unless it is likely that the woman will have a cesarean birth. Many facilities allow Popsicles or hard, sugarless lollipops.
Response to Labor
The nurse assesses the woman’s response to labor, including her use of breathing and relaxation techniques, and supports adaptive responses. Nonverbal behaviors that suggest difficulty coping with labor include a tense body posture and thrashing in bed. The health care provider is notified if the woman requests added pain relief, such as epidural analgesia.
Helping the Woman Cope with Labor
Coping is a dynamic process in which emotions and stress affect and influence each other; coping changes the relationship between the individual and the environment. Adjustment is the outcome of coping at a specific point in time. The nurse must understand the physiology of the normal process of labor to recognize abnormalities. The nurse collects, records, and interprets data during labor, such as FHR responses to uterine contractions (see the discussion of electronic fetal monitoring on pp. 132-137), maternal physical responses (e.g., vital signs and duration of contractions), and psychological responses (e.g., anxiety and tension). The nurse also maintains open communication with the health care provider and provides general hygiene and comfort measures for the mother according to the needs presented. In addition to consistent assessment of the fetal and maternal conditions, the nurse helps the woman to cope with labor by comforting, positioning, teaching, and encouraging her (Figure 6-17). Another aspect of intrapartum nursing is care of the woman’s partner.
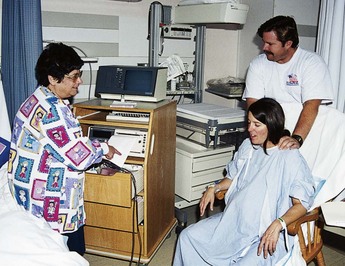
FIGURE 6-17 The nurse explains the external electronic fetal monitor to the woman. The uterine activity sensor is placed on her upper abdomen, over the uterine fundus. The Doppler transducer is placed over her lower abdomen, or wherever the fetal heart rate (FHR) is clearest. The woman and partner are kept informed of progress.
Childbirth is a normal and natural process but today, with modern medicine and technology, few women in the hospital setting give birth without some intervention. These routine interventions includes limited oral intake, IV fluids, bed rest, external or internal fetal monitoring, separation of mother and infant immediately after birth, and elective cesarean sections. The Lamaze Institute for normal birth (2007) recommends six basic principles to use as a guide for maternity care whenever possible:
1. Labor should begin on its own.
2. The woman should have freedom of movement.
3. The woman should have a birth support person or doula.
4. No interventions should be performed simply because they are routine.
The nurse should provide continuous labor support in a hands-on, in-person manner rather than relying on monitors viewed from outside the labor room.
Labor Support
The environment of the labor room can be controlled by having the woman listen to familiar music brought from home, which can produce a calming effect. The recommended positions of comfort for the laboring woman include sitting upright on a rocking chair or birthing ball, which uses the natural force of gravity to promote fetal descent. The “towel-pull” involves the woman pulling on a towel that is secured to the foot of the bed during contractions, which uses the abdominal muscles and aids in expulsion efforts. The lateral Sims position encourages rest and helps prevent pressure on the sacrum.
Body support can be provided by use of pillows to prevent back strain. This position can also be used to facilitate anterior rotation of the fetus when the woman lies on the side of the fetal spine. The “lunge,” in which the mother places her foot on a chair and turns that leg outward, helps the femur press on the ischium to increase pelvic space and facilitates rotation of the fetus that is in occiput posterior (OP) position. The lunge is held for three seconds and repeated.
Squatting during a contraction increases the diameter of the pelvis, facilitating fetal rotation and descent (Adams & Bianchi, 2008). In addition to controlling the environment, using nonpharmacological pain relief techniques such as touch, effleurage, massage, back pressure, application of heat or cold, and various relaxation techniques are effective means of labor support. Emotional support, encouragement, communication concerning progress, and promoting positive thoughts are also essential.
Teaching
Teaching the laboring woman and her partner is an ongoing task of the intrapartum nurse. Even women who attended prepared childbirth classes often find that the measures they learned are inadequate or have to be adapted. Positions or breathing techniques different from those learned in class can be tried. A woman should usually try a change in technique or position for two or three contractions before abandoning it.
Many women are discouraged when their cervix is about 5 cm dilated because it has taken many hours to reach that point. They think they are only halfway through labor (full dilation is 10 cm); however, a 5-cm dilation signifies that about two thirds of the labor is completed because the rate of progress increases. Laboring women often need support and reassurance to overcome their discouragement at this point.
The nurse must often help the woman avoid pushing before her cervix is fully dilated. She can be taught to blow out in short puffs when the urge to push is strong before the cervix is fully dilated. Pushing before full dilation can cause maternal exhaustion and fetal hypoxia, thus slowing progress rather than speeding it.
When the cervix is fully dilated, stage 2 of labor begins, and the nurse teaches or supports effective pushing techniques. If the woman is pushing effectively and the fetus is tolerating labor well, the nurse should not interfere with her efforts. The woman takes a deep breath and exhales at the beginning of a contraction. She then takes another deep breath and pushes with her abdominal muscles while exhaling. Prolonged breath holding while pushing can impair fetal blood circulation (Valsalva’s maneuver). The woman should push for about 4 to 6 seconds at a time. If she is in a semisitting position in bed, she should pull back on her knees, with her hands behind her thighs, or use the hand-holds on the bed.
Providing Encouragement
Encouragement is a powerful tool for intrapartum nursing care because it helps the woman to summon inner strength and gives her courage to continue. After each vaginal examination, she is told of the progress in cervical change or fetal descent. Liberal praise is given if she successfully uses techniques to cope with labor. Her partner needs encouragement as well since labor coaching is a demanding job. Some women may use a doula, a person whose only job is to support and encourage the woman in the task of giving birth (Figure 6-18).
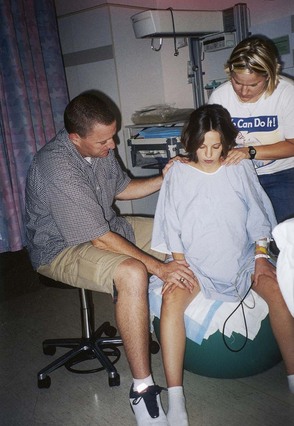
FIGURE 6-18 The doula. The laboring woman sits on a birthing ball as her partner provides encouragement and the doula massages her shoulders. (Courtesy Pat Spier, RN-C.)
The nurse’s caring presence cannot be overlooked as a source of support and encouragement for the laboring woman and her partner. Many women feel dependent during labor and are more secure if the nurse is in their room or nearby. Just being present helps, even if no specific care is given, because they see the nurse as the expert.
Supporting the Partner
Partners, or coaches, vary considerably in the degree of involvement with which they are comfortable. The labor partner is most often the infant’s father but may be the woman’s mother or friend. Some partners are truly coaches and take a leading role in helping the woman cope with labor (Figure 6-19). Others are willing to assist if they are shown how, but they will not take the initiative. Still other couples are content with the partner’s encouragement and support but do not expect him or her to have an active role. The partner should be permitted to provide the type of support comfortable for the couple. The nurse does not take the partner’s place but remains available as needed. The partner should be encouraged to take a break and periodically eat a snack or meal. Many partners are reluctant to leave the woman’s bedside, but they may faint during the birth if they have not eaten. A chair or stool near the bed allows the partner to sit down as much as possible.
Stages and Phases of Labor
Women giving birth display common physical and behavioral characteristics in each of the four stages of labor. Those who receive an epidural analgesic during labor may not exhibit the behaviors and sensations associated with each stage and phase. The nurse must also realize that women are individuals and that each responds to labor in her own way. Table 6-6 summarizes the stages and phases of labor, the related behavioral changes, and the nursing care responsibilities.
Vaginal Birth After Cesarean
It was once thought that a woman who had a cesarean delivery for one infant must have a surgical birth for every subsequent infant. Today, physicians carefully select women who are appropriate candidates for vaginal birth after cesarean (VBAC). (See p. 181 for more information about cesarean birth and subsequent vaginal births.)
Nursing care for women who plan to have a VBAC is similar to that for women who have had no cesarean births. The main concern is that the uterine scar will rupture (see p. 195), which can disrupt the placental blood flow and cause hemorrhage. Observation for signs of uterine rupture should be part of the nursing care for all laboring women, regardless of whether they have had a previous cesarean birth.
Women having a VBAC often need more support than other laboring women. They are often anxious about their ability to cope with labor’s demands and to deliver vaginally, especially if they have never done so. If their cesarean birth occurred during rather than before labor, they may become anxious when they reach the same point in the current labor. The nurse must provide empathy and support to help the woman cross this psychological barrier. However, the nurse cannot promise the woman that a repeat cesarean birth will not be needed, because one may be required for many reasons.
Nursing Care During Birth
There is no exact time when the woman should be prepared for delivery. In general, the woman having her first child is prepared for delivery when about 3 to 4 cm of the fetal head is visible (crowning) at the vaginal opening. The multiparous woman is usually prepared when her cervix is fully dilated but before crowning has occurred. If the woman must be transferred to a delivery room rather than give birth in a LDR room, she should be moved early enough to avoid a last-minute rush.
If the woman does not have full sensation or movement of the legs because of an epidural anesthetic, padded stirrups may be used, and the woman should be observed closely for excess pressure behind the knee, which can cause thrombophlebitis (blood clot).
A woman can give birth in many different positions. The “traditional” position—semisitting and using foot supports—improves access to her perineum but may not be the most comfortable for her or the best one to expel the infant. She may give birth in a side-lying position, squatting, standing, or in other positions.
Nursing Responsibilities
Health care providers do not usually need a scrub nurse during the birth. The registered nurse who cares for the woman during labor usually continues to do so in a “circulating” capacity during delivery. Typical delivery responsibilities include the following:
• Preparing the delivery instruments and infant equipment (Figure 6-20)

FIGURE 6-20 The table contains the sterile instruments that the health care provider will use for delivery. The table is kept covered with a sterile sheet in the labor, delivery, and recovery (LDR) room until it is ready for use.
• Doing the perineal scrub prep (Figure 6-21)
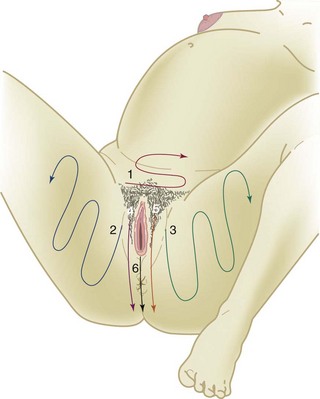
FIGURE 6-21 Perineal scrub preparation is done just before birth. Numbers and arrows indicate the order and the direction of each stroke. A clean sponge is used for each step.
• Administering drugs to the mother or infant
• Providing initial care to the infant, such as suctioning secretions from the airway with a bulb syringe, drying the skin, and placing the infant in a radiant warmer to maintain body heat
• Assessing the infant’s Apgar score (see Table 6-7, p. 152)
Table 6-7
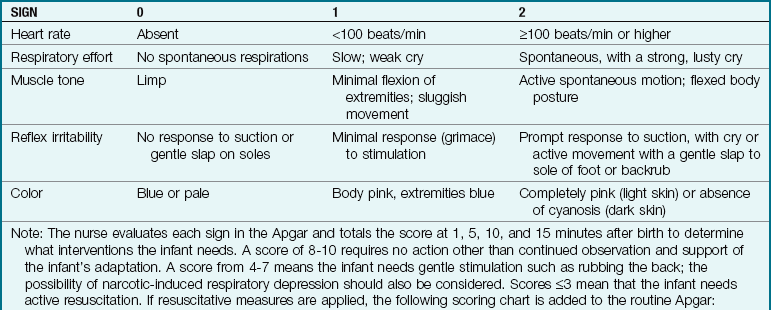

ETT, Endotracheal tube; NCPAP, nasal continuous positive airway pressure; PPV, positive pressure ventilation.
• Examining the placenta to be sure it is intact and recording if it was expelled via the Schultze or the Duncan mechanism (Figure 6-22)
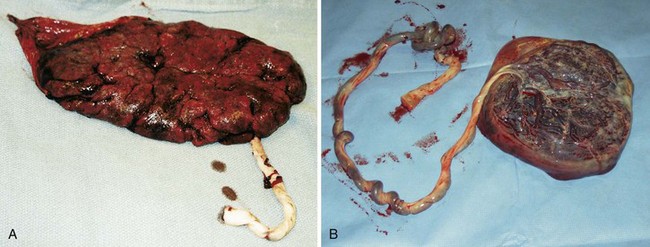
FIGURE 6-22 The placenta after delivery. A, Duncan’s delivery. The maternal side of the placenta, which is dull and rough, is delivered first. B, Schultze delivery. The fetal side of the placenta, which is shiny and smooth, is delivered first. (Courtesy Pat Spier, RN-C.)
• Assessing the infant for obvious abnormalities
• Making a note if the infant has a stool or urinates
• Identifying the mother and infant with like-numbered identification bands (the father or other support person usually receives a band as well; infant footprints and the mother’s fingerprints are often obtained)
• Promoting parent-infant bonding and initial breastfeeding by encouraging parents to hold and explore the infant while maintaining the infant’s body temperature (observe for eye contact, fingertip or palm touch of the infant, and talking to the infant, all of which are associated with initial bonding; these observations continue throughout the postpartum period)
Figure 6-23 on pp. 148-149 shows an infant being born in the vertex presentation in a spontaneous vaginal birth.
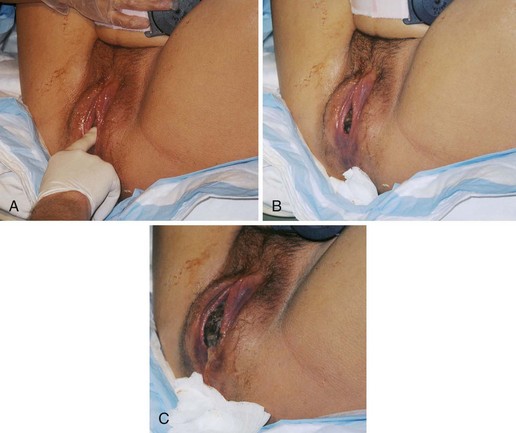
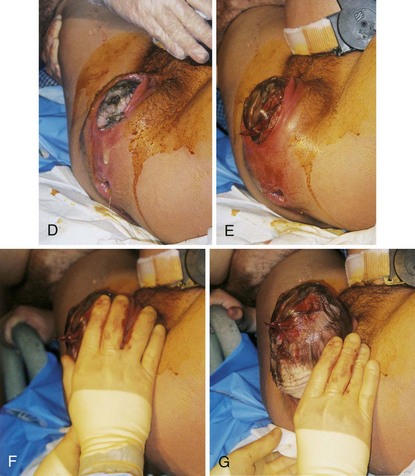
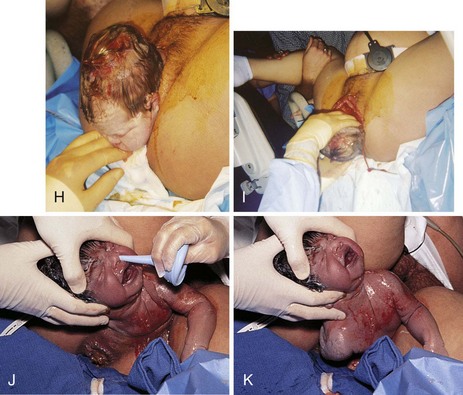
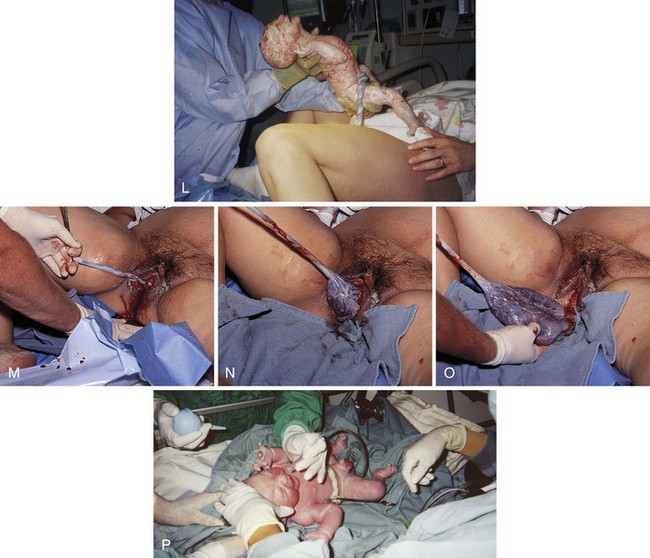
FIGURE 6-23 Vaginal birth of a fetus in vertex presentation. A, The health care provider palpates the fontanelle of the fetus to confirm the position of the head. B, A portion of the fetal head is visible during a contraction. This is called crowning. C, The perineum bulges, and more of the fetal head is visible as the woman bears down. Amniotic fluid drips from the vaginal orifice. D, The perineum has been cleansed with an antimicrobial solution as the fetal head begins extension. Head born by extension. Note the distention of the perineum and anus. E, The head is about to be delivered by extension. Note the thinning, redness, and distention of the perineal area. An episiotomy may be performed at this stage to enlarge the vaginal opening. Also note the fetal monitor that is in place on the mother’s abdomen that allows for continuous monitoring of the fetal heart rate (FHR). F, The health care provider supports the perineum as the head emerges. G, The health care provider checks for cord around the neck. H, The perineum is covered as the head is born. I, The health care provider exerts gentle pressure on the head to release the anterior shoulder from under the symphysis pubis. J, The health care provider uses a bulb syringe to clear the infant’s airway. Newborn cries; color is cyanotic. K, The posterior shoulder and chest is delivered. L, The newborn infant, covered with thick white vernix, is lifted onto the abdomen of the mother, where the cord is cut. M-O, Delivery of placenta. P, Newborn is placed in the radiant warmer where gentle resuscitative measures, such as bulb syringe suctioning and whiffs of oxygen, are provided. Note that the caregivers are wearing gloves while caring for the unwashed newborn. (A to I courtesy Pat Spier, RN-C.)
Immediate Postpartum Period: The Third and Fourth Stages of Labor
The third stage of labor is the expulsion of the placenta. The nurse examines the placenta and monitors the woman’s vital signs (see Table 6-6). The fourth stage of labor is the first 1 to 4 hours after birth of the placenta or until the mother is physiologically stable. Nursing care during the fourth stage of labor includes the following general care:
Nursing Care Immediately After Birth
Facility protocols will vary, but a common schedule for assessing the mother during the fourth stage is every 15 minutes for 1 hour, every 30 minutes during the second hour, and hourly until transfer to the postpartum unit. After transfer to the postpartum unit, applicable routine assessments are made every 4 to 8 hours. The following should be included at each assessment during the fourth stage:
• Vital signs (temperature may be taken hourly if normal)
• Location and firmness of the uterine fundus (see Chapter 9)
• Amount and color of lochia (see Chapter 9)
• Presence and location of pain
• Fullness of the bladder or urine output from a catheter
• Condition of the perineum for vaginal birth
• Condition of dressing for cesarean birth or tubal ligation
• Level of sensation and ability to move lower extremities if an epidural or spinal block was used
Observing for Hemorrhage
The uterine fundus is assessed for firmness, height in relation to the umbilicus, and position (midline or deviated to one side). Refer to Chapter 9 for assessment of the fundus. Vaginal bleeding should be dark red (lochia rubra). No more than one pad should be saturated in an hour, and the woman should not pass large clots. A continuous trickle of bright red blood suggests a bleeding laceration. The blood pressure, pulse rate, and respirations are checked to identify a rising pulse rate or falling blood pressure, which suggest shock. An oral temperature is taken and reported if it is 38° C (100.4° F) or higher or if the woman has a higher risk for infection.
Observing for Bladder Distention
The bladder is assessed for distention, which may occur soon after birth. The woman often does not feel the urge to urinate because of the effects of the anesthetic, perineal trauma, and loss of fetal pressure against the bladder. If her bladder is full, the uterus will be higher than expected and often displaced to one side. A full bladder inhibits uterine contraction and can lead to hemorrhage. Catheterization will be needed if the woman cannot urinate.
Promoting Comfort
Many women have a shaking chill after birth yet deny that they are cold. A warm blanket over the woman makes her feel more comfortable until the chill subsides. The warm blanket also maintains the infant’s warmth while parents get acquainted.
An ice pack may be placed on the mother’s perineum to reduce bruising and edema. A glove can be filled with ice and wrapped in a wash cloth. Perineal pads that incorporate a chemical cold pack are often used. These pads do not absorb as much lochia as those without the cold pack, and this must be considered when evaluating the quantity of bleeding. Cold applications are continued for at least 12 hours. A warm pack pad may be used after the first 12 to 24 hours to encourage blood flow to the area.
The infant usually stays with the mother or parents during recovery if there are no complications. The priority care involves promoting respiratory function and maintaining the temperature. (See Chapter 9 for care of the newborn after the fourth stage of labor [phase 2] and Chapter 12 for an in-depth discussion of the normal newborn [phase 3].)
Care of the Newborn Immediately After Delivery
Care of the newborn after delivery is divided into the following “transition phases” that are involved in adapting to extrauterine life:
• Phase 1: The immediate care after birth; from birth to 1 hour (usually in delivery room) (discussed in the next section)
• Phase 2: From 1 to 3 hours after birth; usually in the transition nursery or postpartum unit (see Chapter 9)
• Phase 3: From 2 to 12 hours after birth; usually in the postpartum unit if rooming-in with the mother (see Chapter 12)
Phase 1: Care of the Newborn
Initial care of the newborn includes the following:
• Maintaining thermoregulation
• Maintaining cardiorespiratory function
• Observing for urination and/or passage of meconium
• Identifying the mother, the father or partner, and the newborn
• Performing a brief assessment for major anomalies
• Encouraging bonding and, as the case may be, breastfeeding
The infant will be covered in blood and amniotic fluid at birth. All caregivers should wear gloves when handling the newborn until after the first bath.
Maintaining Thermoregulation: A critical factor in the transition of the newborn is maintaining a neutral thermal environment in which heat loss is minimal and oxygen consumption needs are the lowest. Hypothermia (low body temperature) can cause hypoglycemia (low blood glucose level) because glucose is used by the infant’s body to generate heat. Hypoglycemia is associated with the development of neurological problems in the newborn. Hypothermia can also cause cold stress, in which the increased metabolic rate required to generate body heat causes increased respiratory rate and oxygen consumption. If the infant cannot supply the increased demand for oxygen, hypoxia will result and cause further problems.
Essential nursing interventions to maintain a neutral thermal environment include the following:
• Drying the infant with a towel to prevent heat loss caused by evaporation of amniotic fluid on the skin: the body and head should be gently dried with a warm towel.
• Placing infant in radiant warmer: a skin probe can be placed on the right upper abdomen (over the spleen or liver) to act as a thermostat to the radiant warmer so that the proper setting of heat will be supplied (Figure 6-24).
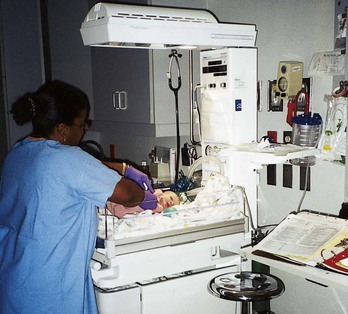
FIGURE 6-24 The nurse applies the sensor and assesses the newborn in the radiant warmer. Note: This nurse is wearing purple nitrite (latex-free) gloves when handling the newborn. (Some newborns can be allergic to latex.)
• Placing a hat on the infant’s head after the head is dried: the head is the largest body surface area in the newborn, and significant heat loss can occur if the moist head is left open to room air.
• Wrapping the infant in warm blankets when taken out of the warmer (see Skill 22-1); skin-to-skin (kangaroo) contact between mother and newborn during bonding (see Skill 13-2) or breastfeeding can also prevent heat loss.
An incubator may be necessary if the infant is unable to stabilize body temperature. The first bath is delayed until the infant’s temperature is stabilized at 36.5° C to 37° C.
Maintaining Cardiorespiratory Function: Physiological changes in the cardiopulmonary circulation in the newborn are discussed in Chapter 12. Respiratory support immediately after delivery includes the following:
• The face, nose, and mouth are gently wiped to remove mucus and excess amniotic fluid.
• Gentle bulb suctioning of secretions from nose and mouth is performed to clear airways. At birth the infant may be placed on the mother’s abdomen. Suctioning may be initiated by the health care provider before cutting the cord. Further need for suctioning is determined when the infant is placed in the radiant warmer.
• A cord clamp is applied when the infant is stabilized in the radiant warmer (Figure 6-25).
Spontaneous breathing usually begins within a few seconds after birth. The infant’s color at birth may be cyanotic (blue) but quickly turns pink (often except for the hands and feet). As the infant cries, the skin color will be pink. Acrocyanosis is the bluish color of hands and feet of the newborn that is normal and is caused by sluggish peripheral circulation. Administration of oxygen by face mask may be performed until the infant is crying vigorously.
Some signs of respiratory distress that should be immediately reported include the following:
• Persistent cyanosis (other than the hands and feet)
• Grunting respirations: a noise heard without a stethoscope as the infant exhales
• Retractions: under the sternum or between the ribs
• Sustained respiratory rate higher than 60 breaths/min
• Sustained heart rate greater than 160 beats/min or less than 110 beats/min
Narcan (naloxone) is kept on hand to reverse narcotic-induced respiratory depression.
Performing Apgar Scoring: Dr. Virginia Apgar devised a system for evaluating the infant’s condition and any need for resuscitation at birth (Table 6-7). Five factors are evaluated at 1 minute and 5 minutes after birth and are ranked in order of importance:
If resuscitative measures are required during the Apgar scoring, a separate chart indicating the interventions are attached to the routine Apgar form (see Table 6-7).
The Apgar score is not a predictor of future intelligence or abilities and disabilities. It was meant to identify only the infant’s condition and any need for neonatal resuscitation measures. Equipment, medications, and personnel must be readily available for resuscitation at any birth because the need cannot always be anticipated.
Identifying the Infant: Wristbands with preprinted numbers are placed on the mother, the infant, and often the father or other support person in the birthing room as the primary means of identifying the infant. The nurse should check to be sure that all numbers in the set are identical. Other identifying information is completed, such as mother’s name, the birth attendant’s name, the date and time of birth, the sex of the infant, and usually the mother’s hospital identification number. The bands are applied relatively snugly on the infant and have only a finger’s width of slack because infants lose weight after birth.
The nurse must check the preprinted wristband numbers to see that they match every time the infant returns to the mother after a separation or the mother goes to the nursery to retrieve her infant. The nurse should either look at the numbers to see that they are identical or have the mother read her own band number while looking at the infant’s band.
Footprints of the infant and one or both index fingerprints of the mother are often taken. Many birth facilities take a photograph of the infant in the birthing room or very soon after admission and record birthmarks or unique features. This is primarily for identification of the infant in the event of an abduction and for keepsake purposes.
Observing Urinary Function and Passage of Meconium: Newborns may not urinate for as long as 24 hours after delivery. If the infant voids in the LDR room, it must be documented on the chart. Meconium, the first stool of the newborn, may be passed anytime within 12 to 24 hours. If meconium is passed in the LDR room, it should be documented in the chart. The infant cannot be discharged to the home until documentation is made that the gastrointestinal and genitourinary tracts are functioning. Passing meconium and voiding help determine the status of these systems.
Promoting Maternal-Infant Bonding: Every attempt should be made to facilitate maternal-infant contact. As soon as the infant is dried and warmed and cardiorespiratory function is stable, the infant should be warmly wrapped and placed in the mother’s arms or in skin-to-skin contact with the mother. The infant is alert in the first hour of life, and therefore this is the best time to initiate breastfeeding and bonding. This practice is supported by the awarding of “baby-friendly hospital” designations to those facilities that encourage skin to skin contact and breastfeeding immediately after birth in the LDR room (Figure 6-26). Breastfeeding is discussed in Chapter 9. Referral to a nurse who is a lactation specialist may be initiated if the mother needs assistance with breastfeeding.
Administering Medications: After the first hour of life the infant begins a sleep pattern with decreased motor activity. This is the best time to place the infant in the warmer for medication administration before leaving the delivery room.
Eye care: All newborn infants are given specific eye care to prevent ophthalmia neonatorum, which is caused by Neisseria gonorrhoeae. The American Academy of Pediatrics also recommends protection against Chlamydia trachomatis. Therefore, erythromycin eye ointment (administered from single-dose tubes) is placed in each eye (Skill 6-6). Eye care is given 1 hour after birth (so that the infant and mother can bond in that first hour), but it must be given and charted before the infant leaves the delivery room.
Vitamin K (AquaMEPHYTON): Newborns need vitamin K to assist in blood clotting. Vitamin K is naturally produced from intestinal flora, which is absent in the newborn. One single dose of vitamin K is injected into the vastus lateralis muscle (thigh) before the infant leaves the delivery room, usually at age 1 hour (Skill 6-7).
Observing for Major Anomalies: The nurse notes signs of injury or anomalies while performing other assessments and care. The infant’s movements and facial expressions during crying are observed for symmetry and equality of movement. The head and face should be assessed for trauma, especially if forceps were used. A small puncture wound is usually apparent on the scalp if an internal spiral electrode was used for fetal monitoring. If the infant was born vaginally in a breech presentation, the buttocks may be bruised.
Many anomalies, such as spina bifida (open spine) or a cleft lip (see Chapter 14), are immediately obvious. The fingers and toes should be counted to identify abnormal numbers or webbing. The feet are observed for straightness; if deviated, it should be determined if they can be returned to the straight position. Length of arms and legs should be checked for equality. Urination or meconium passage is assessed, both of which confirm patency.
A detailed assessment for anomalies and gestational age is completed on admission to the newborn nursery or postpartum unit. See discussion of phases 2 and 3 of newborn care in Chapters 9 and 12.
Cord Blood Banking
Blood from the placenta and umbilical cord has traditionally been treated as a waste product and discarded. Cord blood, like bone marrow, contains regenerative stem cells that can be used for transplant to replace diseased cells or to treat many malignant or genetic diseases in children and adults; they are less likely to cause a potentially fatal rejection response. Private cord blood banks have been established in the United States and are accredited by the American Association of Blood Banks.
Families can register and store their infant’s cord blood for as long as 15 years for later use. The cost of collection and storage is usually not covered by insurance. Informed consent is essential before collection of cord blood, and privacy of information must be maintained. The cord blood is collected after the healthy infant is delivered and the cord has been clamped and cut. Collection is usually performed by a phlebotomist with appropriate equipment to prevent contamination, and the cord blood bank is notified in advance. The blood must be transported within 48 hours of collection for cryopreservation.
Each unit of cord blood must contain a minimum of 40 mL for use in children and 70 mL for use in adults. In 2004 a bill was introduced in the U.S. Congress to establish a national network of cord blood stem cell banking under the direction of the national Health Resources and Services Administration (HRSA), and in 2008, the American College of Obstetricians and Gynecologists (ACOG) updated the policy recognizing the use of umbilical cord blood as an accepted emerging therapy. It is no longer considered an experimental therapy (Einstein & Merkatz, 2008). The data for umbilical cord blood transplantation in children are encouraging, but continued research is needed to demonstrate evidence of success in adults.
Get Ready for the NCLEX® Examination!
Key Points
• The four components, or “four Ps,” of the birth process are the powers, the passage, the passenger, and the psyche. All interrelate during labor to either facilitate or impede birth.
• True labor and false labor have several differences; however, the conclusive difference is that true labor results in cervical change (effacement and/or dilation).
• The woman should go to the hospital if she is having persistent, regular contractions (every 5 minutes for nulliparas, and every 10 minutes for multiparas); if her membranes rupture; if she has bleeding other than normal bloody show; if fetal movement decreases; or for other concerns not covered by the basic guidelines.
• Three key assessments on admission are fetal condition, maternal condition, and nearness to birth.
• There are four stages of labor, and each stage has different characteristics. The first stage is the stage of dilation, lasting from labor’s onset to full (10 cm) cervical dilation. First-stage labor is subdivided into three phases: latent, active, and transition. Second-stage labor, the stage of expulsion, extends from full cervical dilation until birth of the infant. The third stage, the placental stage, is from the birth of the infant until the placenta is delivered. The fourth stage is the immediate postbirth recovery period and includes the first 1 to 4 hours after placental delivery.
• The main fetal risk during first- and second-stage labor is fetal compromise caused by interruption of the fetal oxygen supply. The main maternal risk during fourth-stage labor is hemorrhage caused by uterine relaxation.
• Nursing care during the first and second stages focuses on observing the fetal and maternal conditions and on assisting the woman to cope with labor.
• Continuous electronic fetal monitoring is most common in hospital births, but intermittent auscultation is a valid method of fetal assessment.
• The normal baseline FHR should be between 110 to 160 beats/min.
• A fetal heart rate tracing demonstrates the relationship between the baseline fetal heart rate and uterine contractions.
• Periodic changes in the FHR are temporary changes from the baseline rate associated with uterine contractions that occur in a pattern over time. The presence of accelerations and moderate variability in the FHR pattern is reassuring that the fetus is well oxygenated.
• Abnormal FHR patterns must be reported to the health care provider promptly to ensure a favorable outcome.
• Laboring women can assume many positions. Upright positions add gravity to the forces promoting fetal descent. Hands-and-knees or leaning-forward positions promote normal internal rotation of the fetus if “back labor” is a problem (see Chapter 8). Squatting facilitates fetal descent during the second stage. The supine position should be discouraged because it causes the heavy uterus to compress the mother’s main blood vessels, which can reduce fetal oxygen supply.
• The immediate care of the newborn after birth includes maintaining warmth, maintaining cardiorespiratory function, assessing for major anomalies, encouraging parent-infant bonding, and providing proper identification and documentation.
Additional Learning Resources
![]() Go to your Study Guide for additional learning activities to help you master this chapter content.
Go to your Study Guide for additional learning activities to help you master this chapter content.
![]() Go to your Evolve website (http://evolve.elsevier.com/Leifer) for the following FREE learning resources:
Go to your Evolve website (http://evolve.elsevier.com/Leifer) for the following FREE learning resources:
• Answer Guidelines for Critical Thinking Questions
• Answers and Rationales for Review Questions for the NCLEX® Examination
• Glossary with English and Spanish pronunciations
• Interactive Review Questions for the NCLEX® Examination
• Patient Teaching Plans in English and Spanish
• Coping with labor: www.lamaze.org
• Multilingual facts for prenatal health: www.safemotherhood.org
• Safer childbirth around the world: www.asia-initiative.org
Review Questions for the NCLEX® Examination
1. To determine the frequency of uterine contractions, the nurse should note the time from the:
1. beginning to end of the same contraction.
2. end of one contraction to the beginning of the next contraction.
3. beginning of one contraction to the beginning of the next contraction.
4. contraction’s peak until the contraction begins to relax.
2. Excessive anxiety and fear during labor may result in a(n):
3. A woman who is pregnant with her first child phones an intrapartum facility and says her “water broke.” The nurse should tell her to:
1. wait until she has contractions every 5 minutes for 1 hour.
2. take her temperature every 4 hours and come to the facility if it is over 38° C (100.4° F).
4. A laboring woman suddenly begins making grunting sounds and bearing down during a strong contraction. The nurse should initially:
1. leave the room to find an experienced nurse to assess the woman.
2. look at her perineum for increased bloody show or perineal bulging.
5. A woman in active labor has contractions every 3 minutes lasting 60 seconds, and her uterus relaxes between contractions. The electronic fetal monitor shows the FHR to reach 90 beats/min for periods lasting 20 seconds during a uterine contraction. The appropriate priority nursing action is to:
Critical Thinking Question
1. A para 0, gravida 1 woman is admitted in active labor. She states she has completed prenatal care and wishes for a natural, unmedicated childbirth. However, she states she now does not feel she can cope with the increasing levels of pain and asks if it is okay if she takes pain medication. What is the best response of the nurse?
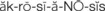 , p. 151)
, p. 151)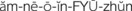 , p. 137)
, p. 137) , p. 137)
, p. 137)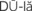 , p. 143)
, p. 143) , p. 120)
, p. 120)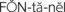 , p. 123)
, p. 123) , p. 135)
, p. 135) , p. 152)
, p. 152) , p. 136)
, p. 136)
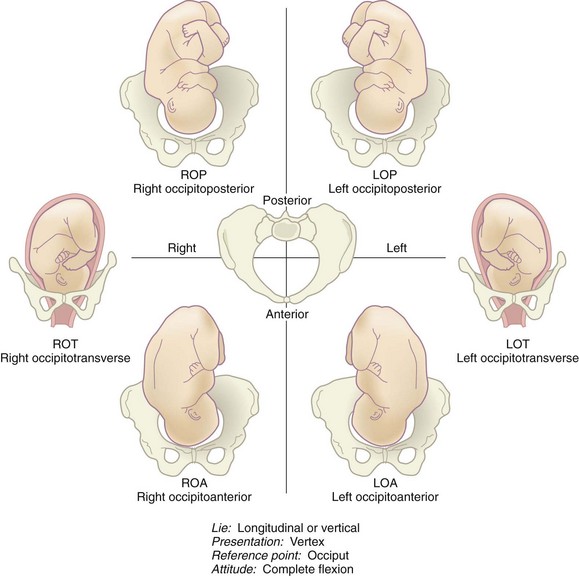
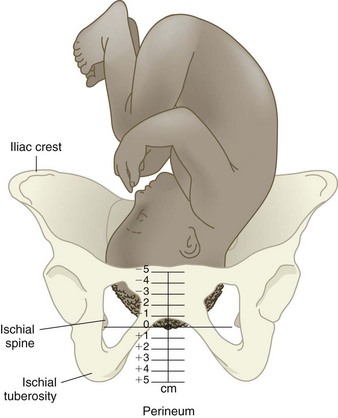
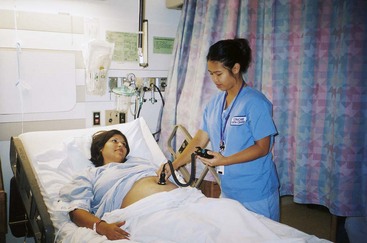
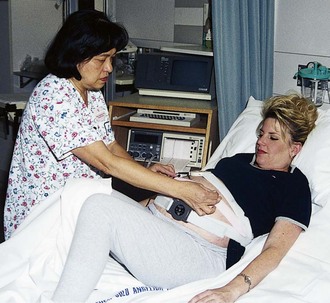
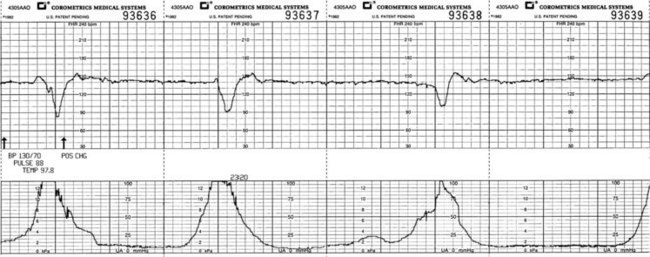
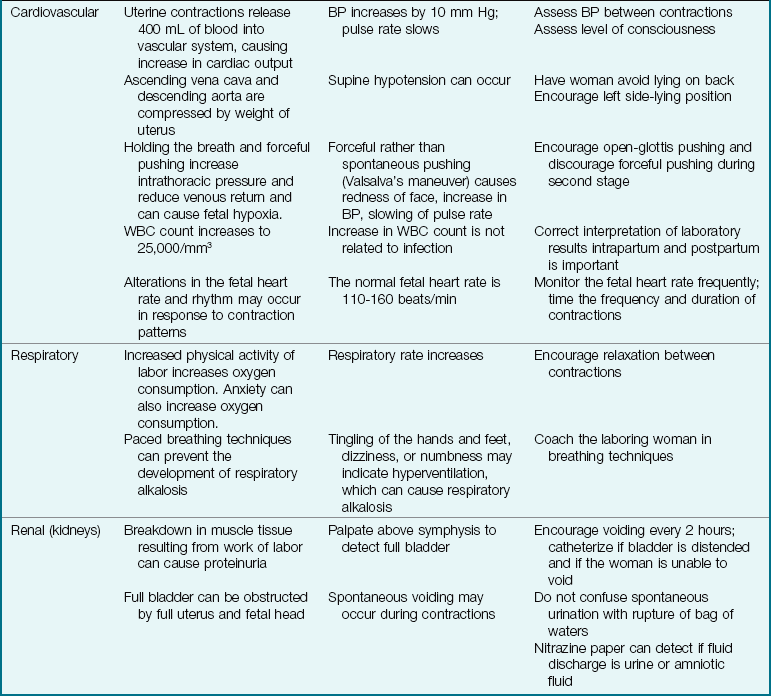
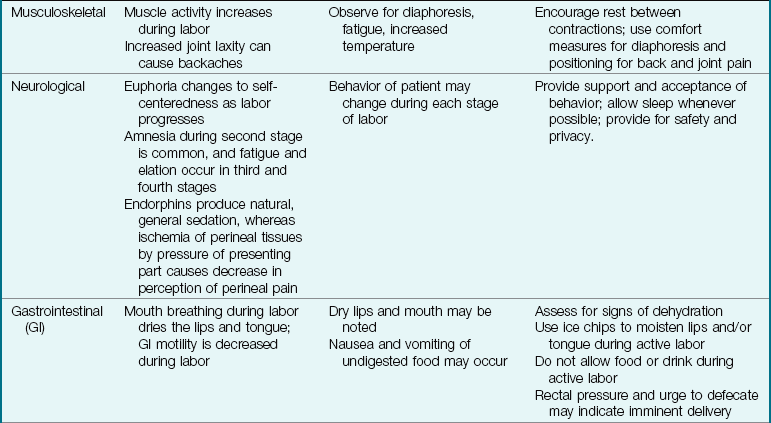


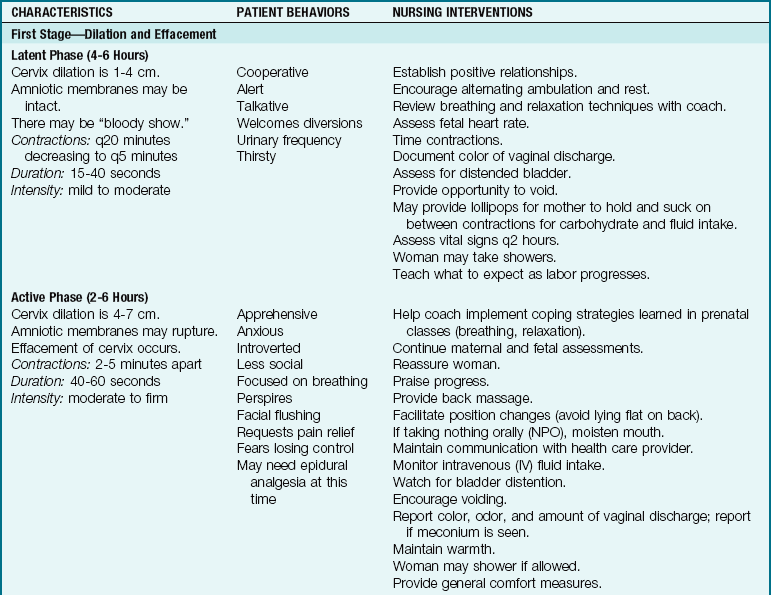
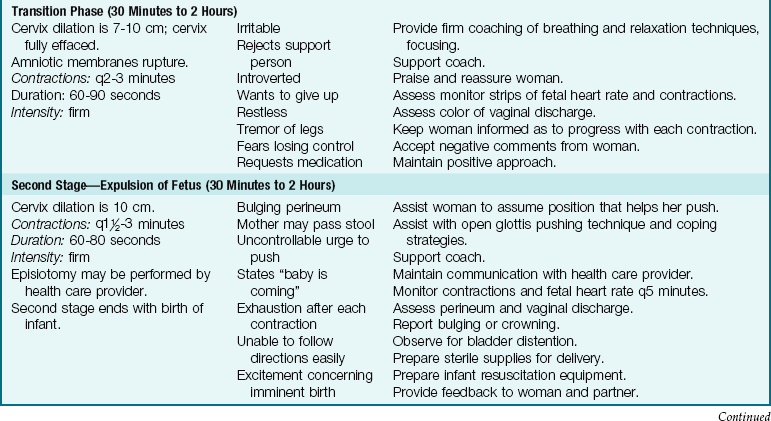
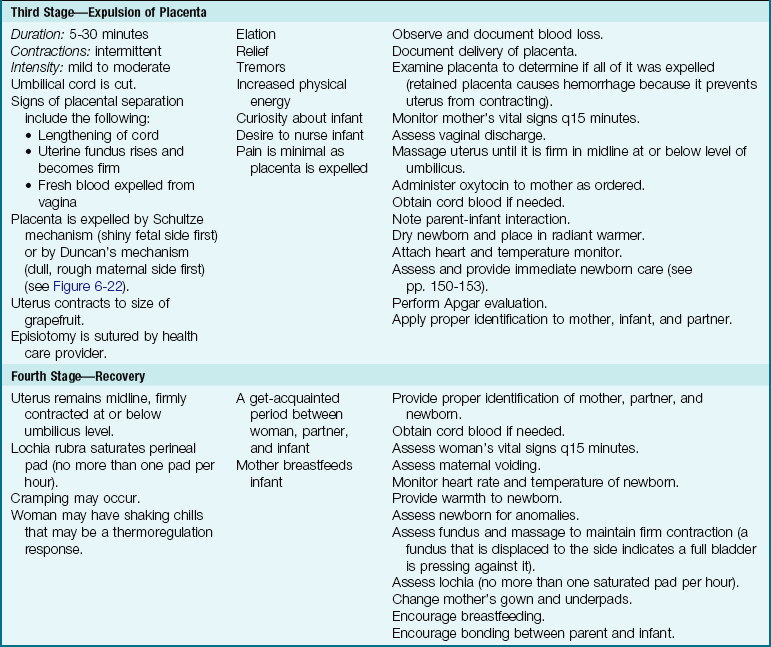
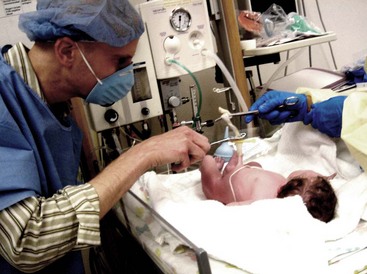
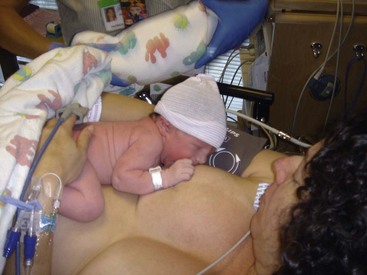
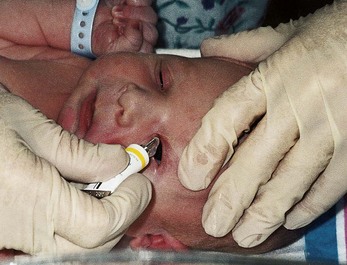
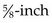 , 25-gauge needle is often used. A small needle reaches the muscle but potentially prevents striking the bone.
, 25-gauge needle is often used. A small needle reaches the muscle but potentially prevents striking the bone.